Abstract
This study aimed to assess the feasibility of a home‐based exercise programme and examine the effects on the healing rates of venous leg ulcers. A 12‐week randomised controlled trial was conducted investigating the effects of an exercise intervention compared to a usual care group. Participants in both groups (n = 13) had active venous ulceration and were treated in a metropolitan hospital outpatients clinic in Australia. Data were collected on recruitment from medical records, clinical assessment and questionnaires. Follow‐up data on progress in healing and treatments were collected fortnightly for 12 weeks. Calf muscle pump function data were collected at baseline and 12 weeks from recruitment. Range of ankle motion data were collected at baseline, 6 and 12 weeks from recruitment. This pilot study indicated that the intervention was feasible. Clinical significance was observed in the intervention group with a 32% greater decrease in ulcer size (P = 0·34) than the usual care group, and a 10% (P = 0·74) improvement in the number of participants healed in the intervention group compared to the usual care group. Significant differences between groups over time were observed in calf muscle pump function parameters [ejection fraction (P = 0·05), residual volume fraction (P = 0·04)] and range of ankle motion (P = 0·01). This pilot study is one of the first to examine and measure clinical healing rates for participants involved in a home‐based progressive resistance exercise programme. Further research is warranted with a larger multi‐site study.
Keywords: Calf muscle pump, Healing rates, Range of ankle motion, Resistance exercise, Venous leg ulcers
Introduction
Venous leg ulcers are a major health concern in the older population (1), affecting 1–3% of the population aged over 60 years 2, 3. Leg ulcers may persist for years and may have a profound impact on the well‐being of the individual (3). Patients with venous leg ulcers have been reported as being less physically active than age‐matched controls 4, 5, which may increase their risk of disease‐related comorbidities (6).
Chronic venous insufficiency and associated venous hypertension may lead to calf muscle changes such as muscle fibre atrophy (7), abnormal gait (8) and reduced strength and functioning of the calf muscle 9, 10. This impairment of calf muscle pump function further worsens venous hypertension. There is evidence to suggest that exercise may improve calf muscle function in this patient population 10, 11, 12, 13. Studies have used a resistance training approach as a means for developing muscular strength and endurance of the calf muscle to ascertain whether this results in an improvement in calf muscle pump efficiency (10, 11, 12, 13, 14, 15). Only one study (11) has tested the feasibility of improving calf muscle pump function by exercise in patients with venous ulceration.
Current chronic venous ulcer management recommendations include the use of specific dressings with compression bandaging and leg elevation. There is considerable variation in healing rates within the literature from the use of compression bandaging. Multilayered compression bandaging has been reported to help heal from 23% to 56% (16) and 69% (17) after 12 weeks of treatment. Up to 15–30% of chronic venous leg ulcers do not respond to compression treatment (18) and remain unhealed, even after a year of treatment (19). Additional strategies are required in these patients.
A recent study (20) reported that venous leg ulcer patients viewed physical activity as a positive factor in life. However, they felt limited by barriers such as pain, fear of injury or lack of time due to time‐consuming ulcer care and care of family members. Importantly, this study highlighted a key message that patients reported information from caregivers regarding physical activity or exercise was insufficient or contradictory. This indicates that wound care practitioners need evidence to support what type of exercise is safe to recommend to patients and if there is a benefit directly related to healing and functional well‐being outcomes.
The primary aim of this study was to assess the feasibility of a home‐based progressive resistance exercise programme and examine the effects on the healing rates of venous leg ulcers. The secondary aim was to determine whether this exercise programme improves calf muscle pump function and ankle range of motion.
Method
Study design and sampling
A randomised controlled trial (RCT) was undertaken to determine the feasibility of a home‐based progressive resistance exercise programme in comparison with usual care on the effects on calf muscle pump function and healing rates for venous leg ulcer patients. The study was an open‐label RCT (ACTRN12611000469910), and recruitment and data collection were conducted between April and December 2008.
To determine the appropriate sample size, the results from a previous study (21) were used, whereby a 25% difference was found in acute wound healing rates for older healthy adults between a group receiving an exercise intervention compared to a group not receiving an exercise intervention. In light of this study, a 20% greater number of completely healed participants was considered to be clinically significant for the intervention group. No previous studies had been published on leg ulcer patients and the impact of exercise on improving healing rates. However, on a practical level, the sample size (60), given the time frame of the study required to observe a 20% change, was unrealistic, and therefore a 30% change between groups was calculated with a sample size of 40 estimated as necessary to detect a between‐group change of 30% in healed at 90% power with an α of 0·05.
Participants were randomised after signed informed consent was obtained, according to a predetermined computer‐generated randomisation scheme, into one of two groups: a control (usual care) or intervention (exercise) group. An independent source prepared the envelopes, and then the principal researcher was required to select the next envelope. Envelopes contained a sheet of paper with either A or B on it. The participant prior to seeing the selection was informed that A corresponded to the usual care group and B corresponded to the exercise intervention. It was stressed to the participants that this process was random. The envelope was chosen and the participant's allocation was recorded. A team of wound care nurses at the clinic were trained in the compression techniques protocol for consistency as participants were all required to be in high‐compression bandaging. Standard hospital protocol for venous leg ulcer patients was general maintenance of bandaging, leg elevation and performing leg and/or ankle exercises.
The sample included participants recruited from the Princess Alexandra Hospital (PAH) Vascular Outpatients' Clinic Queensland, Australia. All participants at the clinic were screened for inclusion in the study. The case definition for venous ulceration was any break in the skin on the lower leg that had been present for 6 weeks or more, no other causative aetiology being present, appearing clinically venous and having an ankle brachial pressure index (ABPI) ≥0·8 ≤1·3. Participants were included if they were 18 years or older, were able to give informed consent, met the case definition, tolerated compression and were able to move their ankle with relatively little pain. Participants were excluded if they had any clinical signs of cellulitis.
Data collection and measures
Data on demographics, health, medical history and ulcer characteristics were collected from medical records and patient questionnaires at baseline. Information on variables known to influence ulcer healing, that is ulcer size, duration and age (22), was collected to include in the final analysis. Data on progress in healing and treatments were collected fortnightly for 12 weeks from baseline. Data on calf muscle pump function and range of ankle motion (ROAM) were collected via physical assessment at baseline, 6 and 12 weeks from recruitment.
Progress in wound healing was measured fortnightly with the following methods: the ulcer area was calculated from wound tracings and use of a portable digital planimetry device, that is Visitrak Digital (Smith & Nephew Medical Limited, Hull, England) as previously validated (23) to determine ulcer areas and percentage area reduction. Incidence of complete wound healing, where wound healing is defined as complete epithelialisation maintained for 2 weeks, was also measured. The Pressure Ulcer Scale for Healing (PUSH) tool (24) was used to provide a broader measure of healing than examining area alone, covering area, exudate and the type of wound bed tissue, and clinical data related to healing progress such as presence of oedema, eczema, inflammation and signs of infection were also collected. A record was kept each week on how many days the compression system was worn. The wound healing outcome measure was the incidence of complete wound closure at the completion of the study (12 weeks after initiation of exercise intervention).
Calf muscle pump function measurements were made with the use of air plethysmography (APG)‐1000 (ACI Medical, San Marcos, CA). The ejection fraction (EF) and residual volume fraction (RVF) were measured as previously described (25). All measurements were made without the use of a thigh tourniquet. The air plethysmograph was inflated with air to 6 mmHg and connected to a pressure transducer, amplifier and recorder. The air plethysmograph was fitted, with the participant in the supine position and the leg elevated (45°) to empty the veins, with the heel supported by a foam box. The air chamber was inflated to 6 mmHg and the leg was kept in this position for 5 minutes once the leg had equilibrated with the cuff and room pressure. A baseline was obtained and calibration was performed by injecting 100 ml of air into the cuff before then removing it. The participant was asked to stand with the weight on the opposite leg, holding onto a frame and the foot being examined was resting on the ground. An increase in the leg volume was observed in the recordings due to venous filling. The participant was asked to remain stationary until a plateau was reached indicating that the veins were full. This increase represents the functional venous volume (VV). The participant was then asked to perform one tip‐toe (heel raise) movement; this was done several times until similar ejections were being achieved (EF). After completing the EF test, the participant was asked to stand with no weight on the tested limb until the veins were full and a volume plateau was reached. The participant was then asked to perform 10 tip‐toe movements approximately 1 second apart. The participant then returned to the initial position on the examination table with limb elevated to 45° until the VV stabilised (RVF).
ROAM was measured in degrees by goniometry [baseline plastic 360° ISOM (STFR), NY] with the participants sitting with their knees at a 45° angle; this was validated by Back et al. (26) in relation to chronic venous insufficiency. ROAM is the combined total of plantar flexion and dorsiflexion. Plantar flexion and dorsiflexion are reported as maximal angular deviations of the sole of the foot from the ‘neutral’ position, defined as 90° on a 0–180° scale, that is perpendicular to the body. Normal ROAM at the ankle is approximately 57 +/− 2°, which in patients with active ulceration is decreased to only 21 +/− 4°(26).
An activity diary was used to measure self‐reported levels of physical activity undertaken for those involved in the study. The activity diary was to be completed by all participants on a daily basis and reviewed at the wound clinic upon each visit. An activity diary was used in a similarly designed study for venous leg ulcer patients (27).
Procedure
On admission to the outpatient leg ulcer clinic, patients were assessed, and if suitable, were invited to participate in the trial. An information package on the study was provided by the principal researcher and an appointment for laboratory screening was made.
All participants undertook a laboratory screening test at the PAH Vascular Lab booked the same week when participants had been recruited. During this test, a venous duplex ultrasound scan was performed to confirm venous incompetence or obstruction and ABPI was performed to exclude peripheral arterial disease.
Following randomisation and prior to the beginning of the first series of baseline measurements, all participants whether in the control or intervention group attended an individual introduction session. During this session, participants were given detailed instructions on the correct technique for the APG and ROAM tests. The aim of the APG familiarisation was to teach participants how to conduct the test without anything touching the pressure cuff, thus ensuring stable pre‐programme baseline measures. Participants in the intervention group participated in a home‐based progressive resistance exercise programme for 12 weeks. These exercises could be reproduced in the participants' own homes without the use of any additional equipment and were similar to the interventions used in two previous trials to improve calf muscle pump function 10, 11. The author prescribed the exercises weekly face‐to‐face at outpatient leg ulcer clinic visits and/or over the phone, if additional support was required. All participants in the intervention group received an individualised exercise programme which followed the exercise protocol in Appendix 1. The exercise protocol was designed with the intention that all participants started at the same level and only graduated to the next level upon successful completion of the current level for at least 3 days or until encouraged by the author that they were ready for the next level of resistance. Stretching was recommended prior to and following each exercise session. These stretches targeted the calf and hamstring musculature and were performed in both of the lower limbs. Participants were instructed to perform each stretch to the point that elicits comfortable tension, but no pain. At the point of tension, each stretch was held for 20 seconds.
Usual care group
The participants assigned to the usual care group were required to perform all the screening tests prior to the study, the calf muscle pump and fitness tests, questionnaires at baseline and the activity diary throughout the study. Participants randomised to usual care did not receive any form of specific exercise training beyond standard general advice given as part of hospital protocol and were therefore instructed not to change their physical activity habits during the 12‐week period. At the completion of the study, if participants in the non‐intervention group had not healed they were given the opportunity to be involved in an individualised exercise programme at the end of the 12 weeks.
Statistical methods
Data analysis was conducted using the software package SPSS for Windows Release 17.0 (SPSS Inc., Chicago, IL). Baseline demographic, health and ulcer characteristics were analysed to check for comparability of the two groups. Descriptive analyses were undertaken for all variables. A chi‐square test for independence was used to identify if there was a significant difference between the numbers in each group, healed by week 12. A Mann–Whitney U‐test was used to identify if there were significant differences between groups for percentage reduction in healing rates over time. To test for the effect of the intervention over time, a two‐way analysis of variance (ANOVA) was conducted on the remaining outcome variables. Group (intervention versus control) was the between‐subject factor and time (pre‐test, week 6, week 12) was the within‐subject or repeated‐measures factor. Due to the small sample size, further tests were conducted to check the assumptions of the statistical tests to be used. The results showed that using Mauchly's test, the Sphericity assumptions of repeated measures for ANOVA were met. Furthermore, tests of homogeneity of variance of assumptions also confirmed that this assumption was met.
Ethics
Ethical approval for the study was obtained from the Queensland University of Technology Human Research Ethics Committee and the PAH and complied with the Helsinki Declaration ethical rules for human experimentation. Participants' freedom to withdraw consent at any time was offered.
Results
Thirteen patients were recruited into the study with 2 not completing the protocol due to intolerance of compression therapy, giving only 11 patients for analysis due to limited patients attending the wound clinic. The planned sample size of 40 was unable to be met due to time constraints of the project. The flow of participants through the study is shown in Figure 1. There were no adverse effects in either the intervention or usual care group.
Figure 1.
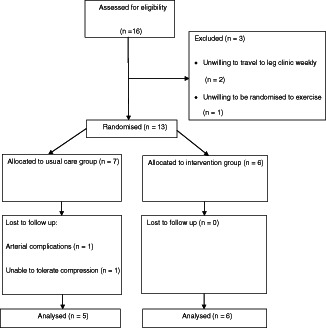
Flow of participants through study.
Baseline demographic characteristics, comorbidities and ulcer characteristics are shown in Table 1. There were no significant differences between groups for age, gender, health variables or ulcer characteristics.
Table 1.
Baseline demographic, health and ulcer characteristics
| Entire cohort | Control | Intervention | |
|---|---|---|---|
| Number | 11 | 5 | 6 |
| Males | 6 | 3 | 3 |
| Females | 5 | 2 | 3 |
| Age (years) * | 64·9 (13) | 63·6 (20) | 66 (6) |
| BMI (kg/m2) * | 33·9 (9) | 36·7 (12·3) | 31·7 (6·6) |
| ABPI * | 1·05 (0.1) | 1·05 (0·07) | 1·05 (0·1) |
| Ulcer duration (weeks) * | 26·5 (16) | 34·8 (17) | 19·5 (14) |
| Ulcer area (cm2) * | 4·2 (4·7) | 3·2 (3·9) | 5·1 (5·5) |
| Previous medical history | |||
| Osteoarthritis | 5 | 2 | 3 |
| Hypertension | 4 | 1 | 3 |
| Heart disease | 1 | 0 | 1 |
| Stroke | 1 | 1 | 0 |
| Medications | |||
| Antihypertensives | 5 | 1 | 4 |
| Antidepressants | 3 | 0 | 3 |
| Analgesics | 5 | 2 | 3 |
| Lasix | 1 | 0 | 1 |
| Current smoker | 1 | 1 | 0 |
| Mobility (with aid) | 4 | 2 | 2 |
| Depression score * | 4·27 (3·8) | – | – |
| Quality of life score * | 8·55 (1·6) | – | – |
ABPI, ankle brachial pressure index; BMI, body mass index.
*Data are means (SD).
Wound healing outcomes
A chi‐square test for independence was used to identify if there was a significant difference between the numbers in each group, healed by week 12. Results showed that 50% of the intervention group had completely healed, in comparison with 40% of the usual care group (χ 2 = 0·11, P = 0·74). A Mann–Whitney U‐test was used to identify if there were significant differences between groups for percentage reduction in healing rates over time. Results observed a 45% reduction in ulcer area size for those in the usual care group, and 77% for those in the intervention group (P = 0·34). A repeated‐measures ANOVA showed no significant difference between groups over time for the PUSH scores at week 12 (P = 0·35).
Calf muscle pump outcomes
Seven participants were included in this analysis as some participants were not able to complete the APG measure due to difficulty in the required testing procedure for various reasons. The change from baseline to week 12 follow‐up in each of the calf muscle pump functioning measures is shown in Table 2.
Table 2.
Air plethysmography values at baseline and 12 weeks later
| Calf muscle pump parameters | Normal values | Intervention | Control | ||
|---|---|---|---|---|---|
| Baseline * (n = 4) | Week 12 * (n = 4) | Baseline * (n = 3) | Week 12 * (n = 3) | ||
| Venous volume (ml) | 80–150 † | 129·33 (42) | 129·73 (42) | 140 (42) | 142·83 (44) |
| Ejection fraction (%) | >60% † <40% poor † | 55 (9) | 66·55 (12) | 60·33 (14) | 61·53 (15) |
| Venous filling index (ml/s) | <2·0 † | 2·63 (1·7) | 1·55 (1·1) | 2·3 (1·2) | 1·77 (0·8) |
| Residual volume fraction | <35 ‡ | 44·92 (8) | 33·06 (12) | 39·67 (13) | 38·45 (15) |
The results showed that there was an overall improvement in calf muscle function in the exercise group. A repeated‐measures ANOVA showed that EF had an interaction effect between group and time (F 1,5 = 6·7, P = 0·05) and a main effect for time (F 1,5 = 10·17, P = 0·02). To examine the interaction effect, paired t‐tests were conducted and showed that the intervention group had a significant increase between baseline and week 12 [t(3) = −3·5, P = 0·03], whereas no significant difference was detected for the usual care group [t(2) = −0·96, P = 0·44]. RVF showed an interaction effect between group and time (F 1,5 = 7·02, P = 0·04) and a main effect for time (F 1,5 = 10·54, P = 0·02). To examine the interaction effect, paired t‐tests were conducted and showed that the intervention group had a significant decrease between baseline and week 12 [t(3) = 3·63, P = 0·03], whereas no significant difference was detected for the usual care group [t(2) = 0·9, P = 0·46]. However, venous filling index (VFI) showed no interaction effect between group and time (F 1,5 = 0·29, P = 0·61) and no main effect for group (F 1,5 = 0·004, P = 0·95) or time (F 1,5 = 2·57, P = 0·17).
Range of ankle motion
The change from baseline to week 6 to week 12 for ROAM is shown in Table 3. A repeated‐measures ANOVA showed for ROAM an interaction effect between group and time (F 2,7 = 11·49, P = 0·01), and a main effect for time (F 2,7 = 11·49, P = 0·01). To examine the interaction effect, post hoc paired t‐tests were conducted and showed that the intervention group had a significant increase between baseline and week 12 [t(9) = −3·2, P = 0·01], no significant difference was observed between baseline and week 6 [t(9) = −2·0, P = 0·07] or week 6 and week 12 [t(9) = −1·6, P = 0·15].
Table 3.
Range of ankle motion values at baseline and 12 weeks later
| Intervention | Control | |||||
|---|---|---|---|---|---|---|
| Baseline * (n = 6) | Week 6 (n = 6) | Week 12 * (n = 6) | Baseline (n = 5) | Week 6 (n = 56) | Week 12 * (n = 5) | |
| Plantar flexion | 18·3 (4) | 23 (5) | 23·5 (4) | 16·5 (6) | 16·5 (6) | 16·5 (6) |
| Dorsi flexion | 6·1 (3) | 7 (3) | 8·3 (2) | 7 (2) | 7 (2·5) | 7 (2·5) |
| Total range of motion | 24·5 (5) | 28·8 (8) | 31·8 (6) | 23·5 (8) | 23·5 (8) | 23·5 (8) |
*Data are means (SD); no significant differences found between control and intervention groups.
Activity diary
The activity diaries were given to all participants at the beginning of the study. Participants recorded the type of exercise, duration, level of perceived exertion, level of enjoyment and symptoms. Log sheets were to be completed and given back to the researcher at the end of the study.
Of the participants in the usual care group, only one of five participants completed the activity diary, despite regular reminders. This is in direct contrast to all the participants in the intervention group (n = 6).
Discussion
This research was a pilot study to assess the feasibility of conducting a home‐based progressive resistance exercise programme for participants experiencing venous leg ulcers. The intervention was deemed feasible with all participants in the intervention group completing the 12‐week study period with no deleterious effects noted. There was, however, no significant difference observed over time between groups in relation to healing. Participants in the intervention group had significant improvement in their calf muscle pump efficiency and ROAM over the 12‐week home‐based progressive resistance exercise programme compared to those in usual care.
Although not statistically significant, participants who received a home‐based progressive resistance exercise programme in addition to usual care had a 32% greater decrease in ulcer size than the usual care group, and a 10% improvement in the number of participants healed in the intervention group compared to the usual care group. This difference could be viewed as clinically significant or may reflect variance between patients. It is noted that the lower than anticipated enrolment significantly reduced the power of this study to detect whether the observed difference was statistically significant. Future studies with larger sample sizes are needed to determine statistical and clinical significance. The only other study to measure healing as an outcome in an ankle exercise study is by Jull et al. (11). These authors found the mean change in ulcer area from baseline to week 12 was not significant between groups; however, healing was improved in the usual care group by 15·9%. In their study at 12 weeks, 38% of participants in the exercise group had completely healed and 53% in the usual care group had healed; no reason for the difference in observations was mentioned by the authors.
It has been suggested that structured exercise programmes are associated with improvements in calf muscle pump function 10, 11, 12, 13. The findings of this research are consistent within the literature.
Participants in the intervention group showed significant improvement in calf muscle pump function, specifically an increase in EF and a decrease in RVF. However, no significant changes were observed for VFI in either study group. It is interesting to consider at what point in time improvements in EF and RVF occurred. Yang et al. (10) showed a significant increase in EF and a decrease in RVF after a 6‐week programme. However, unlike the current study, Yang et al. (10) used non‐parametric tests to analyse the data and these patients did not have open venous ulcerations but had recently healed ulcers; additionally, there was no between‐group effect as all patients were in an exercise group. Kan and Delis (12) were able to show a significant difference between the control and exercise groups in relation to EF, following an intensive 8‐day exercise programme. However, the VFI and RVF did not change significantly. Padberg et al. (13) noted RVF and EF improved in the exercise group after a 6‐month programme, while the VFI remained unchanged in both the control and exercise groups. The significant increase in EF in this study is supported by the most recent study (11), which also showed a significantly greater improvement in EF of the calf muscle in the exercise group compared with the usual care group after a 12‐week home‐based progressive exercise programme. Although there was no significant change for VFI in this study, the results of this study are consistent with all the other studies in this area 10, 11, 12, 13, 14, 15.
Participants in the intervention group showed significant improvement over the 12 weeks for ROAM, whereas there was no change for the usual care group receiving usual care. The results further suggest that the exercise intervention needed to be conducted for at least 12 weeks as this is when the significance for ROAM was observed. Further research is warranted to determine if venous ulceration causes decreased ROAM. Perhaps, ROAM is caused by a lack of mobility, osteoarthritis or a past sporting injury and these musculoskeletal changes result in venous ulceration.
Decreased ROAM is associated with delayed healing of venous ulcers (28. The mean increase in ROAM was 30%, which was statistically significant between groups over the 12 weeks. This result is consistent with Davies et al. (27). These authors observed a significant difference following 12 and 24 weeks; however, unlike the current study no usual care group was utilised.
The ROAM shown in this patient population is comparable to the literature (26). In the study by Barwell et al. (28), only 13% of patients who had less than 35° ROAM had healed at 24 weeks, compared with 60% of those who had over 35°. Artificially restricting the movement of the ankle joint has been shown to decrease the effectiveness of the calf muscle pump in healthy volunteers walking on a treadmill (29). This warrants further investigation of targeting increased ankle mobility and perhaps a longer study period time to be able to assess this relationship.
From the field notes taken by the author and the activity diaries, the participants in the intervention group often communicated that the resistance programme activity was achievable, convenient and enjoyable. The close individual support and encouragement that all patients received during the programme may have contributed to the individual basis at which participants progressed through the intensity of the resistance programme. In addition, the short duration of training possibly meant that interest in the programme did not wane. The main reason for not adhering to a session was sickness and/or pain.
Unfortunately, only one usual care group participant returned the activity diary; therefore, a comparison between daily activity levels between the groups was not possible. Few daily activity diaries have been described in the literature (30), although one was used by Davies et al. (27) in their home‐based intervention for increasing ROAM, it was not described. In the current study, it may have been that it was too burdensome for participants to fill out, as previously reported (30).
The major limitation of this study was that subject numbers were insufficient to be powered to detect differences in all measured variables. Recruitment of participants occurred from only one site. Despite this hospital being one of the largest vascular centres in Queensland, recruitment was slow, which is indicative of this patient population (31), and there were time constraints on the study. All eligible patients were shared between this study and a National Health and Medical Research Council (NHMRC)‐funded study. Second, the APG test is highly patient dependent, with many unable to adequately perform the exercise part of the test (25). Third, there is little information in the literature to indicate how effective resistance exercises are with multilayer compression bandaging on as in this study. Fourth, although insignificant statistical differences were observed between mean ulcer duration at baseline, the mean for the intervention group was less than the usual care group, possibly resulting in a mitigating factor in the rate of healing in the intervention group. Finally, there is difficulty in generalising the current findings given that only participants who lived in close proximity to the recruitment site were utilised for the study.
Despite evidence to suggest that exercise improves calf muscle pump efficiency, few studies have assessed the impact on healing rates. Clinical guidelines in Australia currently recommend calf muscle and ankle exercises for adults with venous leg ulcers. However, anecdotal evidence suggests few clinicians actually recommend specific exercise as an adjunct therapy of current wound treatment. If, as this pilot study has demonstrated, a simple home‐based exercise programme is feasible for patients, this may possibly be included as a minimum for health professionals to recommend to their clients to engage in self‐management principles of wound care, thereby empowering patients. Further to this, wound professionals may need to refer patients to physiotherapists and/or accredited exercise physiologists for lifestyle modification and exercise advice and programmes.
Acknowledgement
The authors acknowledge Bronwen Woodward, Carissa Ceccato, Megan Pratt and Kylie Armstrong and the vascular staff at the Princess Alexandra Hospital for their contribution.
Exercise protocol
Stage 1: seated heel‐rises (both legs)
10 × 3 sets three times per day everyday
15 × 3 sets three times per day everyday
20 × 3 sets three times per day everyday
25 × 3 sets three times per day everyday
Stage 2: standing heel‐rises (both legs)
10 × 3 sets three times per day everyday
15 × 3 sets three times per day everyday
20 × 3 sets three times per day everyday
25 × 3 sets three times per day everyday
Stage 3: one‐legged heel‐rises
10 × 3 sets three times per day everyday
15 × 3 sets three times per day everyday
20 × 3 sets three times per day everyday
25 × 3 sets three times per day everyday
References
- 1. Harrison M, Graham I, Friedberg E, Lorimer K, Vandevelde‐Coke S. Assessing the population with leg and foot ulcers. Can Nurse 2001;97:18–23. [PubMed] [Google Scholar]
- 2. Graham ID, Harrison MB, Nelson EA, Lorimer K, Fisher A. Prevalence of lower‐limb ulceration: a systematic review of prevalence studies. Adv Skin Wound Care 2003;16:305–16. [DOI] [PubMed] [Google Scholar]
- 3. Heit JA, Rooke TW, Silverstein MD, Mohr DN, Lohse CM, Petterson TM, O'Fallon WM, Melton LJ 3rd. Trends in the incidence of venous stasis syndrome and venous ulcer: a 25‐year population‐based study. J Vasc Surg 2001;33:1022–7. [DOI] [PubMed] [Google Scholar]
- 4. Heinen M, Van Der Vleuten C, De Rooij M, Uden C, Evers A, Van Achterberg T. Physical activity and adherence to compression therapy in patients with venous leg ulcers. Arch Dermatol 2007;143:1283–8. [DOI] [PubMed] [Google Scholar]
- 5. Roaldsen KS, Rollman O, Torebark E, Olsson E, Stanghelle JK. Functional ability in female leg ulcer patients – a challenge for physiotherapy. Physiother Res Int 2006;11:191–203. [DOI] [PubMed] [Google Scholar]
- 6. Persoon A, Heinen MM., Van Der Vleuten CJM, De Rooij MJ, Van De Kerkhof PCM and Van Achterberg T. Leg ulcers: a review of their impact on daily life. J Clin Nurs 2004;13:341–54. [DOI] [PubMed] [Google Scholar]
- 7. Qiao T, Liu C, Ran F. The impact of gastrocnemius muscle cell changes in chronic venous insufficiency. Eur J Vasc Endovasc Surg 2005;30:430–6. [DOI] [PubMed] [Google Scholar]
- 8. Van Uden CJT, Van der Vleuten CJM, Kooloos JGM, Haenen JH, Wollersheim H. Gait and calf muscle endurance in patients with chronic venous insufficiency. Clin Rehabil 2005;19:339–44. [DOI] [PubMed] [Google Scholar]
- 9. Orsted HL, Radke L, Gorst R. The impact of musculoskeletal changes on the dynamics of the calf muscle pump. Ostomy Wound Manage 2001;47:18. [PubMed] [Google Scholar]
- 10. Yang D, Vandongen YK, Stacey MC. Effect of exercise on calf muscle pump function in patients with chronic venous disease. Br J Surg 1999;86:338–41. [DOI] [PubMed] [Google Scholar]
- 11. Jull A, Parag V, Walker N, Maddison R, Kerse N, Johns T. The PREPARE pilot RCT of home‐based progressive resistance exercises for venous leg ulcers. J Wound Care 2009;18:497–503. [DOI] [PubMed] [Google Scholar]
- 12. Kan M, Delis K. Hemodynamic effects of supervised calf muscle exercise in patients with venous leg ulceration: a prospective controlled study. Arch Surg 2001;136:1364–9. [DOI] [PubMed] [Google Scholar]
- 13. Padberg FT Jr, Johnston MV, Sisto SA. Structured exercise improves calf muscle pump function in chronic venous insufficiency: a randomized trial. J Vasc Surg 2004;39:79–87. [DOI] [PubMed] [Google Scholar]
- 14. Heinen M, Borm G, van der Vleuten C, Evers A, Oostendorp R, van Achterberg T. The Lively Legs self‐management programme increased physical activity and reduced wound days in leg ulcer patients: results from a randomized controlled trial. Int J Nurs Stud 2012;49:151–61. [DOI] [PubMed] [Google Scholar]
- 15. Zajkowski PJ, Draper T, Bloom J, Henke PK, Wakefield TW. Exercise with compression stockings improves reflux in patients with mild chronic venous insufficiency. Phlebology 2006;21:100–4. [Google Scholar]
- 16. Harrison MB, Graham ID, Lorimer K, Friedberg E, Pierscianowski T, Brandys T. Leg‐ulcer care in the community, before and after implementation of an evidence‐based service. Can Med Assoc J 2005;172:1447–52. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Franks PJ, Moffatt CJ. Factors associated with healing leg ulceration with high compression. Age Ageing 1995;24:407. [DOI] [PubMed] [Google Scholar]
- 18. O'Meara S, Cullum N, Nelson E. Compression for venous leg ulcers. Cochrane Database Syst Rev 2009;CD000265. [DOI] [PubMed] [Google Scholar]
- 19. Kurd SK, Hoffstad OJ, Bilker WB, Margolis DJ. Evaluation of the use of prognostic information for the care of individuals with venous leg ulcers or diabetic neuropathic foot ulcers. Wound Repair Regener 2009;17:318–25. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Roaldsen KS, Biguet G, Elfving B. Physical activity in patients with venous leg ulcer–between engagement and avoidance. A patient perspective. Clin Rehabil 2011;25:275–86. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Emery CF, Kiecolt‐Glaser JK, Glaser R, Malarkey WB, Frid DJ. Exercise accelerates wound healing among healthy older adults: a preliminary investigation. J Gerontol A 2005;60A:1432–6. [DOI] [PubMed] [Google Scholar]
- 22. Margolis DJ, Knauss J, Bilker W. Epidemiology and Health Services Research Medical conditions associated with venous leg ulcers. Br J Dermatol 2004;150:267–73. [DOI] [PubMed] [Google Scholar]
- 23. Sugama J, Matsui Y, Sanada H, Konya C, Okuwa M, Kitagawa A. A study of the efficiency and convenience of an advanced portable Wound Measurement System (VISITRAK). J Clin Nurs 2007;16:1265–9. [DOI] [PubMed] [Google Scholar]
- 24. Stotts NA, Rodeheaver GT, Thomas DR, Frantz RA, Bartolucci AA, Sussman C, Ferrel BA, Cuddigan J, Maklebust JA. An instrument to measure healing in pressure ulcers: development and validation of the Pressure Ulcer Scale for Healing (PUSH). J Gerontol A 2001;56A:M795. [DOI] [PubMed] [Google Scholar]
- 25. Araki CT, Back TL, Padberg FT, Thompson PN, Jamil Z, Lee BC, Duran WN, Hobson RW 2nd. The significance of calf muscle pump function in venous ulceration. J Vasc Surg 1994;20:872. [DOI] [PubMed] [Google Scholar]
- 26. Back TL, Padberg FT Jr, Araki CT, Thompson PN, Hobson RW II. Limited range of motion is a significant factor in venous ulceration. J Vasc Surg 1995;22:519–23. [DOI] [PubMed] [Google Scholar]
- 27. Davies JA, Bull RH, Farrelly IJ, Wakelin MJ. A home‐based exercise programme improves ankle range of motion in long‐term venous ulcer patients. Phlebology 2007;22:86–9. [DOI] [PubMed] [Google Scholar]
- 28. Barwell JR, Taylor M, Deacon J, Davies C, Whyman MR, Poskitt KR. Ankle motility is a risk factor for healing of chronic venous leg ulcers. Phlebology 2001;16:38–40. [Google Scholar]
- 29. Kugler C, Strunk M, Rudofsky G. Venous pressure dynamics of the healthy human leg. J Vasc Res 2001;38:20–9. [DOI] [PubMed] [Google Scholar]
- 30. Moore R, Berlowitz D, Denehy L, Jackson B, McDonald CF. Comparison of pedometer and activity diary for measurement of physical activity in chronic obstructive pulmonary disease. J Cardiopulm Rehab Prev 2009;29:57–61. [DOI] [PubMed] [Google Scholar]
- 31. Edwards H, Courtney M, Finlayson K, Lindsay E, Lewis C, Shuter P, Chang A. Chronic venous leg ulcers: effect of a community nursing intervention on pain and healing. Nurs Stand 2005;19:47–54. [DOI] [PubMed] [Google Scholar]


