Abstract
Traumatic posterior dislocations of the shoulder can result in bony defects, labral tears, and cartilage injuries of the glenohumeral joint. Although traditional Hill-Sachs lesions from anterior dislocations are more commonly identified, reverse Hill-Sachs lesions caused by posterior dislocation often leads to recurrent engagement of the humeral head with the glenoid and significantly greater damage to the humeral chondral surface. In severe traumatic cases, concomitant damage of the capsulolabral soft tissues, such as circumferential labral lesions, can lead to chronic shoulder instability and residual glenoid bone loss. These lesions further add to the complexity of managing patients with posterior dislocations of the shoulder because of the challenges of achieving adequate anatomic reduction and tensioning of the capsulolabral junction, while also using a combination of arthroscopic and open-labral repair techniques. In the setting of reverse Hill-Sachs lesions treatment, it is important to address the bony and cartilage defect. The purpose of this Technical Note is to describe our preferred technique for arthroscopic repair of circumferential lesions of the glenoid labrum causing multidirectional instability with concomitant reverse Hill-Sachs Lesion treatment with fresh talus osteochondral allograft.
Technique Video
The patient was initially positioned into the lateral decubitus position for diagnostic arthroscopy and to repair the circumferential labral tear in a left shoulder. Standard diagnostic arthroscopy was performed using a posterior portal, mid-glenoid portal, and an accessory posterolateral portal. The repair began at the 7 o’clock position. The accessory posterolateral portal was used for both suture passage, as well as suture anchor placement. A combination of suture anchors were used to repair the labral tear extending from the 9 o’clock position posterior to the 4 o’clock position anterior in this case. Anchors were first placed 3 mm apart beginning at the 7 o’clock position and proceeding to the 9 o’clock position posteriorly. The anteroinferior labral tear extending anteriorly to the 4 o’clock position is then addressed and fixated. The patient was then repositioned into the beach chair position and re-draped. The anterior portal site was extended into a deltopectoral incision. The subscapularis tendon was identified and the upper half of the subscapularis tendon was sharply taken down in a subscapularis peel technique. This allowed visualization of the glenohumeral joint exposing the large defect deep on the anteromedial surface of the humeral head, just medial to the lesser tuberosity. The edges of the defect were sharply debrided using a combination of Cobb elevator, sagittal saw, curette, and rongeur into a pie-shaped fashion to allow for talus allograft placement. On the back table, the talus allograft was cut in a custom fashion using a sagittal saw to match the defect. K-wires were placed to assist with fixation. The allograft was brought up to the surgical field, and rasp and burr were used to match the defect and the allograft perfectly and gently tamped into position. Preliminary K-wire fixation was used to hold the allograft into position. Using the K-wires for guidance, three headless compression screws were placed to fixate the allograft.
Glenohumeral joint instability is a common pathology in young, active individuals, with posterior shoulder instability comprising a relatively small subset of this group.1 Posterior shoulder dislocation has been reported to account for roughly 2% to 5% of shoulder dislocations and usually result from a direct force applied to the abducted and extended arm in internal rotation.2, 3, 4 In this patient population, coexistent injuries such as soft tissue laxity, glenoid bone loss, and osteochondral lesions of the humeral head are more common than previously thought and can further complicate diagnostic workup and treatment.1,5 Reverse Hill-Sachs lesions (rHSLs) were identified by magnetic resonance imaging (MRI) in up to 86% of patients with first-time traumatic posterior shoulder dislocation6 and are associated with significantly greater cartilage damage than traditional HSLs.7
In cases of chronic posterior instability, copathologies such as posterior humeral avulsion of the glenohumeral ligament (pHAGL) and localized labral damage are commonly present alongside rHSLs, necessitating recognition and subsequent treatment. In cases with more severe labrum damage, a circumferential or pan-labral lesion can be seen. Circumferential labral lesions are uncommon, representing 2.4% of all labral lesions8 and are thought to result from an initial traumatic insult resulting in an isolated lesion that eventually progresses to a circumferential lesion after multiple instability events.8,9 Pan-labral lesions result in recurrent instability, substantial shoulder pain, and positive provocative tests for labral tear in all directions and remain symptomatic in the absence of recent instability events.9
For these reasons, it is imperative to address both the bony humeral head defect and circumferential labral repair to prevent recurrent shoulder instability and reengagement of a large rHSL with the posterior glenoid rim. Also, an rHSL has significant cartilage involvement and can compromise up to 45° of the articular surface of the humeral head.7,10 In isolation, outcomes of both reconstruction of rHSLs and arthroscopic repairs of circumferential lesions of the glenoid labrum have demonstrated improvement in objective and subjective measures9,11 and no difference in shoulder stability and function when compared to anterior labral repair alone.12 To date, no outcomes have been reported on the simultaneous treatment of rHSLs and circumferential labral lesions. In this Technical Note, we describe our preferred technique for soft tissue management of posterior shoulder instability completed via multiportal arthroscopic repair of circumferential lesions of the glenoid labrum, followed by an anatomic reconstruction of the humeral head with an unmatched talus allograft for the management of a large reverse Hill-Sachs lesion (Video 1).
Surgical Technique
Patient Positioning in the Lateral Decubitus Position
Within the preoperative area, antibiotics are given, and an interscalene nerve block is performed using ultrasound guidance. Once in the operating room the patient is initially placed in the supine position on the operating table, and an examination is done with the patient under general anesthesia. The patient is then placed in the lateral decubitus position for the initial diagnostic arthroscopy and posterior stabilization procedure. All bony prominences are well padded, and the arm is placed in an arm sleeve (Arthrex Inc., Naples, FL) under 10 pounds of balanced suspension. To note, the patient will be later repositioned and redraped in the beach chair position for the open aspect of the case, using the same beanbag flattened.
Portal Placement and Diagnostic Arthroscopy
A standard diagnostic arthroscopy is performed to evaluate the glenoid, humeral head, labrum, biceps tendon, and rotator cuff using the posterior viewing portal. After the diagnostic arthroscopy, anterosuperior, mid-glenoid, and posterolateral portals are placed under direct visualization, and 5 mm cannulas are placed. The mid-glenoid portal should be made approximately 1 cm lateral from the joint line of the humeral head and 2 to 3 cm inferior and 1 to 2 cm medial from the posterolateral acromial angle. This portal along with the accessory posterolateral are used for both suture passage and anchor placement for the posterior labral repair.13 This case shows a 4 o’clock to 9 o’clock labral tear (Fig 1). A large reverse Hill-Sachs lesion can also be appreciated about the humeral head (Fig 2).
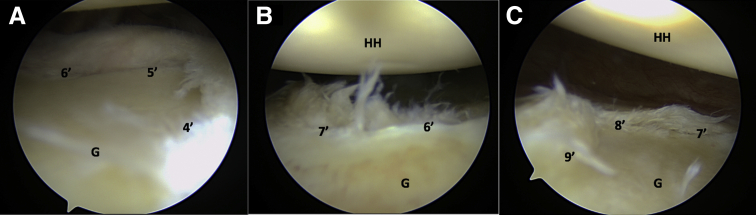
Fig 1.
Arthroscopic view from the anterosuperior portal of the circumferential lesion of the glenoid labrum in a left shoulder in lateral decubitus position. The lesion can be seen extending from the 4 o’clock position (A) to the 6 o’clock (B) and 9 o’clock (C) positions, causing multidirectional instability. The labrum is prepped and mobilized using an elevator through the posterior portal, and a shaver is used to debride the loose frayed tissue to achieve a stable capsulolabral rim. HH, humeral head; G, glenoid; L, labrum.
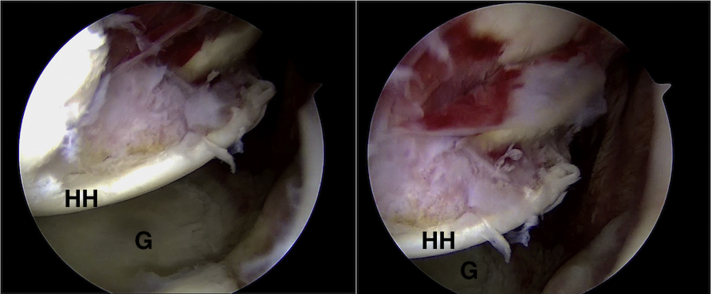
Fig 2.
Arthroscopic views from the anterosuperior portal of a large reverse Hill-Sachs lesion in a left shoulder in the lateral decubitus position. HH, humeral head; G, glenoid.
Circumferential Labral Repair
The labrum is addressed first, and a probe is used to further delineate the labral tear. With the arthroscope in the posterior portal, the anterior-inferior labrum is debrided and prepared using a combination of a elevators, radiofrequency wand, shaver, and a power rasp. Adequate mobilization is noted once the muscle belly of the subscapularis is visualized. An elevator is introduced through the posterior portal to elevate the labrum and posterior capsule layer off the face and neck of the glenoid. After mobilization of the posterior labrum, a shaver is introduced to debride the loose frayed tissue. The bony surfaced is then prepared using a shaver on burr mode providing a freshened surfaced for healing of the labral repair.
The capsulolabral repair is addressed starting at the 7 o’clock position. The repair is continued from the 9 o’clock position, posteriorly, to the 4 o’clock position, anteriorly. To note, the appropriate number of anchors is determined by the extent of the labral tear (Fig 3). Examination consisting of the anterior and posterior load and shift is performed under direct visualization to insure restoration of global stability. In this case, the superior labrum is noted to have an unstable tear extending into the biceps insertion. A radiofrequency wand is used to detach the biceps tendon from the superior labrum for a later biceps tenodesis. The arthroscope is removed, and all wounds are closed in a layered fashion with absorbable suture, which is sterilely covered.
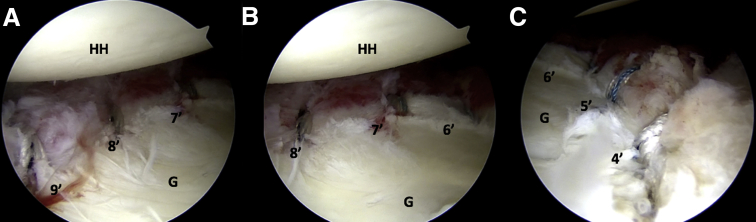
Fig 3.
Arthroscopic views from the anterosuperior portal of the circumferential lesion of the glenoid labrum in a left shoulder in lateral decubitus position. The repair begins at the 7 o’clock position and proceeds sequentially to the 9 o’clock position to stabilize the posteroinferior aspect of the lesion first (A and B). The anteroinferior lesion is then addressed from the 7 o’clock to 4o’clock position (C). The number of anchors placed are dictated by the extent of the lesions, as anchors are placed 3 mm apart to achieve adequate fixation. HH, humeral head; G, glenoid; L, labrum.
Patient Repositioning to Beach Chair Position
The patient is repositioned from the lateral decubitus to the supine position. With the patient in the supine position, the head of the bed is elevated approximately 45°, the beanbag is deflated, and then inflated flat. The arm is reprepped and redraped in standard sterile fashion. A well-padded Mayo stand is used to assist for arm positioning. An incision is made over the deltopectoral interval, and dissection is continued deeply until the cephalic vein is identified. The vein is protected and mobilized laterally. The clavipectoral fascia is then incised, and the interval between the deltoid and the conjoined tendon is bluntly dissected. The undersurface of the deltoid is freed from all attachments to the rotator cuff and a Kolbel retractor is inserted underneath the deltoid laterally and conjoined tendon medially to allow for visualization. In addition, two Hohmann retractors are place superiorly to further improve visualization. The long head of the biceps tendon and the bicipital groove is identified, and the bicipital sheath is opened. The previously tenotomized tendon is retrieved, and with gentle tension a soft tissue tenodesis is performed to the pectoralis major tendon. Overhanging tendon can be transacted just proximal to the tenodesis site. The bicipital groove is followed proximally into the rotator interval, and a curved mayo scissors is used to open the interval.
The subscapularis attachment on the lesser tuberosity can be clearly delineated, noting both the proximal and distal borders of the tendon. The bicipital groove is cleared of all remaining soft tissues and the lateral most aspect of the subscapularis footprint is identified. A peel technique is used to release the upper two thirds of the subscapularis and capsule as a single unit. A blunt retractor is then placed inferiorly to protect the axillary nerve. With adduction and external rotation, the reverse Hills-Sachs defect is clearly visible just medial to the lesser tuberosity. The upper border of the subscapularis tendon is tagged using a no. 2 FiberWire suture, and the lesion should be debrided down to a cancellous bed of humeral bone. Once this is done, the edges of the defect can be sharply debrided using a combination of a Cobb elevator, sagittal saw, curette, and osteotomes. After this step, measurements (width, length, and depth) of the defect are taken by a ruler for preparation of the osteochondral allograft. The overall configuration of the defect is usually a lemon wedge in shape, and the talus will be shaped as a wedge to fill the defect. Bone wax may be used to size the defect and reconstruct on the back table.
Talus Allograft Preparation and Fixation
The base of the fresh allograft is removed with an oscillating saw (Fig 4). The graft is cut matching the dimensions of the prepared humeral defect. Bone wax mold can help facilitate preparation. Cutting the graft 1 to 2 mm larger than the resected lesion allows for a press fit match into the previously prepared lesion. K-wires are placed to aid with fixation and manipulation of the fresh talus allograft. After placing the K-wires, the graft is gently tamped into the matched position on the humeral head and the previously placed K-wires are advanced for temporary fixation of the allograft. Care is taken to ensure that the articular margin of the humeral head and fresh talus osteochondral allograft are matched as closely as possible. The K-wires are overdrilled, and three 2.5 mm headless compression screws (Acutrak; Acumed, Hillsboro, OR) are placed providing stable fixation of the fresh talus allograft (Figs 5 and 6).
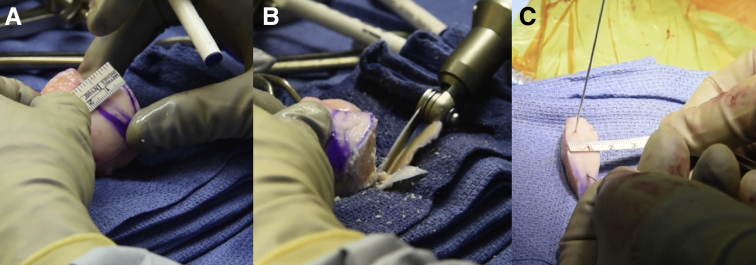
Fig 4.
Fresh talus allograft preparation. The fresh talus allograft is prepared on the back table and begins with measuring the dimensions of the defect with a ruler and marked with a surgical pen (A). The base of the fresh talus allograft is removed with an oscillating saw and the graft is cut matching the dimensions of the prepared humeral defect. A towel clamp can be used to stabilize the graft while cutting. Cutting the graft 1 to 2 mm larger than the resected lesion allows for a press fit match into the previously prepared lesion of the shoulder (B). K-wires are placed to aid with fixation and manipulation of the fresh talus allograft (C).
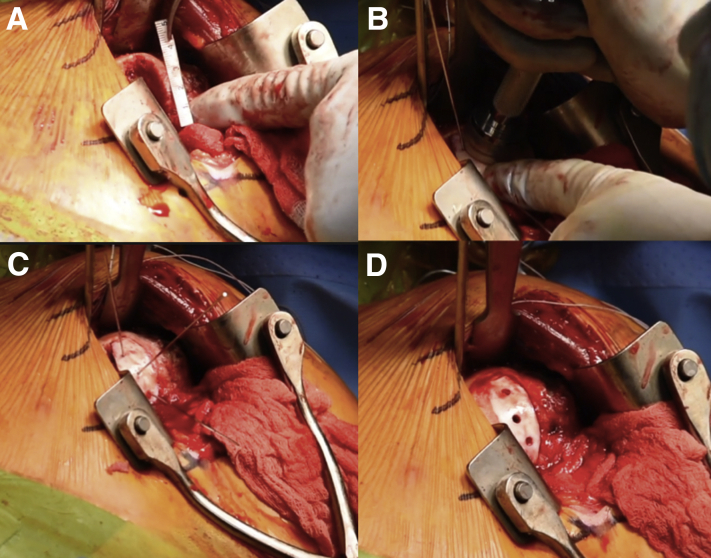
Fig 5.
Fresh talus allograft fixation in a left shoulder. The defect is again measured to ensure proper sizing of the allograft (A). After graft preparation, the graft is gently tamped into the matched position on the humeral head, and the previously placed K-wires are advanced for temporary fixation of the allograft (B). Care is taken to ensure that the articular margin of the humeral head and fresh talus osteochondral allograft are matched as closely as possible (C). The K-wires are overdrilled and three 2.5 mm headless compression screws (Acutrak; Acumed, Hillsboro, OR) are placed providing stable fixation of the fresh talus allograft (D).
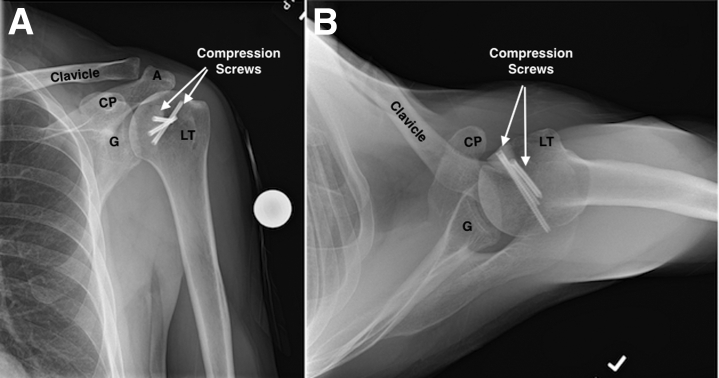
Fig 6.
(A) Anteroposterior and (B) axial postoperative standard radiographs showing final fresh talus allograft fixation in a left shoulder. The radiographs show filling of the bony defect with the fresh talus allograft using three 2.5 mm headless compression screws (Acutrak; Acumed, Hillsboro, OR). CP, coracoid process; G, glenoid; LT, lesser tuberosity; A, acromion.
Subscapularis Tendon Repair and Closure
The upper border of the subscapularis tendon and capsule is repaired back to its anatomic footprint on the lesser tuberosity. This is achieved by using a SpeedBridge technique (Arthrex). Two medial Suturetak (Arthrex) suture anchors in a Speedbridge configuration (Arthrex) and two lateral-row 4.75 mm SwiveLock suture anchors are placed in the lesser tuberosity footprint. This allows for excellent fixation of the subscapularis tendon back to its anatomic footprint. The wound is then thoroughly irrigated and closed in a layered fashion. The patient is immobilized in a padded abduction sling.
Discussion
This Technical Note describes our preferred technique for arthroscopic repair of circumferential lesions of the glenoid labrum with concomitant rHSL treatment with fresh talus allograft. The goal of this procedure is to restore posterior shoulder stability by reattaching the extensively torn glenoid labrum to its native location. Moreover, restoring the anatomic osseous architecture of the humeral head through the use of a talus allograft prevents its engagement with the posterior rim of the glenoid and ultimately decreases the likelihood of recurrent posterior instability events. This technique presents a novel treatment option in cases of chronic or traumatic posterior glenohumeral instability presenting with complex concomitant soft tissue and bony injuries.
Several techniques have been described for the treatment of reverse Hill Sachs lesions. The McLaughlin procedure and its modified variants involve subscapularis tendon and lesser tuberosity osseous transfer to fill in the anterior defect.14 However, limitations to this nonanatomic procedure consist of restrictions in internal shoulder rotation and lack of the ability to reproduce the native cartilage surface. Furthermore, although fresh humeral osteochondral allograft has also been proposed as an effective option to replicate the normal shoulder anatomy, there may be an increased risk in infection because grafts closer to the donor midline have an increased rate of harvest contamination.15 Because rHSLs have been reported to be associated with greater cartilage damage than traditional HSLs, fresh talus allograft has emerged as a viable procedure to best reproduce the native curvature and cartilage surface of the humeral head, while also serving to minimize infection because of its peripherally located harvest site (Table 1).16 However, there is a paucity of literature regarding outcomes of combined circumferential labral repair and humeral or glenoid bone grafting procedures, and future studies are needed to elucidate whether multidirectional lesions impact the outcomes of bony augmentation procedures.
Table 1.
Advantages and Disadvantages of Circumferential Labral Repair and Anatomic Reconstruction of the Humeral Head with Fresh Talus Allograft
| Arthroscopic circumferential labral repair |
| Advantages |
| Arthroscopic Repair allows for stepwise suture placement and adequate tensioning and reduction of the labrum |
| Inferior to superior repair improves visualization for anchor placement |
| Disadvantages |
| Patient repositioning and re-draping is required when performed with RHSL procedure |
| Multiple portals may increase risk of neurovascular injury |
| Anatomic reconstruction of the humeral head |
| Advantages |
| Talus allograft offers cartilaginous surface to recreate humeral head anatomy |
| Talus allograft reproduces native curvature of humeral head anatomy |
| Disadvantages |
| Several team members needed to aid with graft prep, repositioning, and retraction |
| Fresh talus allografts may not be available in certain regions |
| Open technique increases risk of infection |
| Risk of nonunion |
Posterior instability represents only a small subset of all instability cases, which can pose challenging treatment dilemmas for surgeons. In the setting of traumatic posterior shoulder instability, reverse Bankart lesions have been reported in the majority of cases, with an incidence of up to 66%.6 Although less common, these patients may present with more extensive lesions that extend into the inferior, anterior, and superior portions of the glenoid labrum. These types of complex circumferential labral tears were first described by Powell et al.17 as pan-labral SLAP-IX lesions and have also been classified as triple (anterior, posterior, type II SLAP) labral lesions.
Interestingly, Lo and Burkhart8 originally proposed that triple labral lesions most likely result from a primary pathology of anterior instability. Although such lesions may involve the posterior labrum, it is thought that damage to the posterior capsule and labrum in these cases most likely result from “contrecoup” injuries associated with anterior instability. It was also noted in the same study that patients presenting with rHSLs may represent true cases of traumatic, posterior instability, which applies to the case described in this Technical Note. In the absence of additional soft tissue or bony injuries, reliable outcomes have been reported after isolated arthroscopic repair of circumferential or extensive (≥180°) labral tears.
Although data in the literature is currently limited regarding short- to long-term outcomes for the treatment of rHSLs with and without concomitant soft tissue damage, it is suggested that management for these lesions relies on the same concepts as traditional HSL treatment.15 Therefore it is possible that failure to address concomitant soft tissue lesions may lead to recurrent shoulder instability, persistent pain, and ultimately failure of the bony augmentation procedure. Additionally, because circumferential lesions of the glenoid labrum are difficult to diagnose before surgery.
Because of limitations of physical examination and radiologic interpretation, circumferential lesions of the glenoid labrum can be difficult to diagnose before surgery and result in inadequate recognition, planning, and treatment.9 In cases with concomitant circumferential labral lesions, Tokish et al.9 emphasized the importance of pertinent patient history and physical examination to help differentiate from unidirectional lesions on initial presentation. The authors reported that 100% of patients reported multiple instability events that could reflect the corresponding pathogenesis of a multidirectional lesion. Furthermore, patients uniquely remain symptomatic after initial instability events, and physical examination tests often result in positive provocative test results in all directions.9 It has also been suggested that magnetic resonance imaging with contrast may be beneficial for identification when suspicious of circumferential lesions, especially in cases with concomitant bony lesions.
Depending on the extent of the tear, the stepwise surgical approach for circumferential tears involve the combination of individual labral repair techniques. In this case, arthroscopic repair of the circumferential labral lesion begins at the 7 o’clock position. This position allows for adequate anatomic reduction and subsequent tensioning of the capsulolabral rim and further improves visualization because the intraarticular soft tissues tend to swell as surgical time lapses (Table 1). Additionally, accessory portals, including a mid-glenoid portal and posterolateral portal, are necessary for optimal visualization and anchor trajectory for posterior and inferior aspects of the lesion. It is the senior author’s recommendation to address the posterior aspect of the lesion first, because the working space is diminished if the anterior portion is repaired first, subsequently increasing the difficulty of completing the repair (Table 2). Therefore the anterior Bankart lesion is fixated last, which allows for solid anatomic fixation throughout 360°.
Table 2.
Pearls and Pitfalls of Circumferential Labral Repair and Anatomic Reconstruction of the Humeral Head with Fresh Talus Allograft
| Circumferential labral repair |
| Pearls |
| Begin labral repair at 7 o’clock position and work posteriorly first |
| Complete labral repair at anteroinferior position |
| Initial mobilization of the capsulolabral rim allows for adequate reduction of labrum |
| Use of multiple accessory portals improves visualization and anchor trajectory for tears around the glenoid |
| Cannulas help facilitate suture passage and interchanging of viewing portals |
| Magnetic resonance imaging arthrogram may aid with identification |
| Pitfalls |
| Over constraint causes difficulty in anatomic reduction and labral tensioning |
| Failure to use accessory portals may affect trajectory of anchor placement and cause damage to glenoid cartilage with shallow placement |
| Failure to address lesions on the humeral side may lead to recurrent shoulder instability and operative failure |
| Care should be taken to avoid tangling of sutures with the use of multiple anchors |
| Anterosuperior anchor placement may result in over constraint and loss of shoulder external rotation |
| Anatomic reconstruction of the humeral head |
| Pearls |
| Preoperative computed tomography with 3D reconstruction should be used for surgical planning and graft sizing |
| Careful shaping and measurement helps ensure accurate graft size and fit |
| Partial subscapularis tendon peel technique improves visualization of the bony defect |
| Bone wax may be used to size the defect and reconstruct on the back table |
| Pitfalls |
| Inaccurate shaping and failure to achieve press fit of talus allograft may negatively affect patient outcomes |
This Technical Note describes our preferred surgical technique for arthroscopic repair of circumferential lesions of the glenoid labrum with concomitant rHSL treatment with fresh talus allograft. We believe this technique provides a viable and reproducible strategy to concurrently address both soft tissue and osseous lesions of this complex injury and improves patient satisfaction with recurrent multidirectional instability. However, future studies are needed to evaluate the efficacy of fresh talus allograft for the treatment of reverse Hill-Sachs Lesions and the effects of concomitant soft tissue labral injury on patient outcomes.
Footnotes
The authors report the following potential conflicts of interest or sources of funding: M.T.P. receives personal fees from Arthrex, the Joint Research Foundation (JRF), SLACK Inc, and Arthrosurface, outside the submitted work; is an editorial or governing board member for Arthroscopy, Knee, Orthopedics, and SLACK Inc; and is a board or committee member for AANA, AAOS, AOSSM, ASES, ISAKOS, the San Diego Shoulder Institute, and the Society of Military Orthopaedic Surgeons. Full ICMJE author disclosure forms are available for this article online, as supplementary material.
Supplementary Data
The patient was initially positioned into the lateral decubitus position for diagnostic arthroscopy and to repair the circumferential labral tear in a left shoulder. Standard diagnostic arthroscopy was performed using a posterior portal, mid-glenoid portal, and an accessory posterolateral portal. The repair began at the 7 o’clock position. The accessory posterolateral portal was used for both suture passage, as well as suture anchor placement. A combination of suture anchors were used to repair the labral tear extending from the 9 o’clock position posterior to the 4 o’clock position anterior in this case. Anchors were first placed 3 mm apart beginning at the 7 o’clock position and proceeding to the 9 o’clock position posteriorly. The anteroinferior labral tear extending anteriorly to the 4 o’clock position is then addressed and fixated. The patient was then repositioned into the beach chair position and re-draped. The anterior portal site was extended into a deltopectoral incision. The subscapularis tendon was identified and the upper half of the subscapularis tendon was sharply taken down in a subscapularis peel technique. This allowed visualization of the glenohumeral joint exposing the large defect deep on the anteromedial surface of the humeral head, just medial to the lesser tuberosity. The edges of the defect were sharply debrided using a combination of Cobb elevator, sagittal saw, curette, and rongeur into a pie-shaped fashion to allow for talus allograft placement. On the back table, the talus allograft was cut in a custom fashion using a sagittal saw to match the defect. K-wires were placed to assist with fixation. The allograft was brought up to the surgical field, and rasp and burr were used to match the defect and the allograft perfectly and gently tamped into position. Preliminary K-wire fixation was used to hold the allograft into position. Using the K-wires for guidance, three headless compression screws were placed to fixate the allograft.
References
- 1.Owens B.D., Duffey M.L., Nelson B.J., DeBerardino T.M., Taylor D.C., Mountcastle S.B. The Incidence and characteristics of shoulder instability at the United States Military Academy. Am J Sports Med. 2007;35:1168–1173. doi: 10.1177/0363546506295179. [DOI] [PubMed] [Google Scholar]
- 2.Kowalsky M.S., Levine W.N. Traumatic posterior glenohumeral dislocation: classification, pathoanatomy, diagnosis, and treatment. Orthop Clin North Am. 2008;39:519–533. doi: 10.1016/j.ocl.2008.05.008. [DOI] [PubMed] [Google Scholar]
- 3.Hatzis N., Kaar T.K., Wirth M.A., Rockwood C.A. The often overlooked posterior dislocation of the shoulder. Tex Med. 2001;97:62–67. [PubMed] [Google Scholar]
- 4.Robinson C.M., Aderinto J. Posterior shoulder dislocations and fracture-dislocations. J Bone Jt Surg. 2005;87:639–650. doi: 10.2106/JBJS.D.02371. [DOI] [PubMed] [Google Scholar]
- 5.Rouleau D.M., Hebert-Davies J. Incidence of associated injury in posterior shoulder dislocation: systematic review of the literature. J Orthop Trauma. 2012;26:246–251. doi: 10.1097/BOT.0b013e3182243909. [DOI] [PubMed] [Google Scholar]
- 6.Saupe N., White L.M., Bleakney R. Acute traumatic posterior shoulder dislocation: MR findings. Radiology. 2008;248:185–193. doi: 10.1148/radiol.2481071003. [DOI] [PubMed] [Google Scholar]
- 7.Moroder P., Tauber M., Scheibel M. Defect characteristics of reverse Hill-Sachs lesions. Am J Sports Med. 2016;44:708–714. doi: 10.1177/0363546515621286. [DOI] [PubMed] [Google Scholar]
- 8.Lo I.K.Y., Burkhart S.S. Triple labral lesions: pathology and surgical repair technique-report of seven cases. Arthrosc J Arthrosc Relat Surg Off Publ Arthrosc Assoc N Am Int Arthrosc Assoc. 2005;21:186–193. doi: 10.1016/j.arthro.2004.09.022. [DOI] [PubMed] [Google Scholar]
- 9.Tokish J.M., McBratney C.M., Solomon D.J., Leclere L., Dewing C.B., Provencher M.T. Arthroscopic repair of circumferential lesions of the glenoid labrum. J Bone Joint Surg Am. 2009;91:2795–2802. doi: 10.2106/JBJS.H.01241. [DOI] [PubMed] [Google Scholar]
- 10.Frank R.M., Romeo A.A., Provencher M.T. Posterior glenohumeral instability: evidence-based Treatment. J Am Acad Orthop Surg. 2017;25:610–623. doi: 10.5435/JAAOS-D-15-00631. [DOI] [PubMed] [Google Scholar]
- 11.Guehring M., Lambert S., Stoeckle U., Ziegler P. Posterior shoulder dislocation with associated reverse Hill-Sachs lesion: treatment options and functional outcome after a 5-year follow up. BMC Musculoskelet Disord. 2017;18:442. doi: 10.1186/s12891-017-1808-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Wall A., McGonigle O., Gill T.J. Arthroscopic circumferential labral repair for patients with multidirectional instability: a comparative outcome study. Orthop J Sports Med. 2019;7 doi: 10.1177/2325967119890103. 232596711989010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Provencher M., Aman Z., Peebles L. Placing Knotless Suture Anchor through Mid-Glenoid Portal. J Med Insight. 2014 doi: 10.24296/jomi/f2. Published online. [DOI] [Google Scholar]
- 14.McLaughlin H.L. Posterior dislocation of the shoulder. J Bone Joint Surg Am. 1952;24 A:584–590. [PubMed] [Google Scholar]
- 15.Provencher M.T., Frank R.M., LeClere L.E. The Hill-Sachs lesion: diagnosis, classification, and management. J Am Acad Orthop Surg. 2012;20:242–252. doi: 10.5435/JAAOS-20-04-242. [DOI] [PubMed] [Google Scholar]
- 16.Provencher M.T., Sanchez G., Schantz K. Anatomic Humeral head reconstruction with fresh osteochondral talus allograft for recurrent glenohumeral instability with reverse Hill-Sachs lesion. Arthrosc Tech. 2017;6:e255–e261. doi: 10.1016/j.eats.2016.10.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Powell S.E., Nord K.D., Ryu R.K.N. The diagnosis, classification, and treatment of SLAP lesions. Oper Tech Sports Med. 2004;12:99–110. [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
The patient was initially positioned into the lateral decubitus position for diagnostic arthroscopy and to repair the circumferential labral tear in a left shoulder. Standard diagnostic arthroscopy was performed using a posterior portal, mid-glenoid portal, and an accessory posterolateral portal. The repair began at the 7 o’clock position. The accessory posterolateral portal was used for both suture passage, as well as suture anchor placement. A combination of suture anchors were used to repair the labral tear extending from the 9 o’clock position posterior to the 4 o’clock position anterior in this case. Anchors were first placed 3 mm apart beginning at the 7 o’clock position and proceeding to the 9 o’clock position posteriorly. The anteroinferior labral tear extending anteriorly to the 4 o’clock position is then addressed and fixated. The patient was then repositioned into the beach chair position and re-draped. The anterior portal site was extended into a deltopectoral incision. The subscapularis tendon was identified and the upper half of the subscapularis tendon was sharply taken down in a subscapularis peel technique. This allowed visualization of the glenohumeral joint exposing the large defect deep on the anteromedial surface of the humeral head, just medial to the lesser tuberosity. The edges of the defect were sharply debrided using a combination of Cobb elevator, sagittal saw, curette, and rongeur into a pie-shaped fashion to allow for talus allograft placement. On the back table, the talus allograft was cut in a custom fashion using a sagittal saw to match the defect. K-wires were placed to assist with fixation. The allograft was brought up to the surgical field, and rasp and burr were used to match the defect and the allograft perfectly and gently tamped into position. Preliminary K-wire fixation was used to hold the allograft into position. Using the K-wires for guidance, three headless compression screws were placed to fixate the allograft.
The patient was initially positioned into the lateral decubitus position for diagnostic arthroscopy and to repair the circumferential labral tear in a left shoulder. Standard diagnostic arthroscopy was performed using a posterior portal, mid-glenoid portal, and an accessory posterolateral portal. The repair began at the 7 o’clock position. The accessory posterolateral portal was used for both suture passage, as well as suture anchor placement. A combination of suture anchors were used to repair the labral tear extending from the 9 o’clock position posterior to the 4 o’clock position anterior in this case. Anchors were first placed 3 mm apart beginning at the 7 o’clock position and proceeding to the 9 o’clock position posteriorly. The anteroinferior labral tear extending anteriorly to the 4 o’clock position is then addressed and fixated. The patient was then repositioned into the beach chair position and re-draped. The anterior portal site was extended into a deltopectoral incision. The subscapularis tendon was identified and the upper half of the subscapularis tendon was sharply taken down in a subscapularis peel technique. This allowed visualization of the glenohumeral joint exposing the large defect deep on the anteromedial surface of the humeral head, just medial to the lesser tuberosity. The edges of the defect were sharply debrided using a combination of Cobb elevator, sagittal saw, curette, and rongeur into a pie-shaped fashion to allow for talus allograft placement. On the back table, the talus allograft was cut in a custom fashion using a sagittal saw to match the defect. K-wires were placed to assist with fixation. The allograft was brought up to the surgical field, and rasp and burr were used to match the defect and the allograft perfectly and gently tamped into position. Preliminary K-wire fixation was used to hold the allograft into position. Using the K-wires for guidance, three headless compression screws were placed to fixate the allograft.