SUMMARY:
While back pain presents less frequently in children than in adults, it still poses a significant clinical challenge with respect to making a firm diagnosis and developing an effective treatment plan. When children have back pain and medical attention is sought, an underlying pathology is usually suspected. Pediatric patients are evaluated, first, with a complete clinical history and examination and, second, by an imaging work-up that is based on initial findings, including the child's age and size, signs and symptoms, and suspected etiology. This article describes 1) the epidemiology of back pain in children, 2) the imaging work-up used, and 3) the correlation of imaging findings with disease entities that may cause back pain in the pediatric patient. The list of diseases giving rise to back pain is not meant to be exhaustive but rather reflective of the most commonly identified pathologies and disorders among young children and adolescents, from athletic injuries to lethal cancers.
Back pain in children presents less frequently than in adults. The incidence of back pain in adults has been estimated to be as high as 60%–80%1; the actual incidence of back pain in children, however, is unknown. Back pain in children presenting to the emergency department was originally thought to be an uncommon complaint,2 reflecting significant underlying pathology compared with adults. Although recent studies have shown an increased prevalence of back pain in children,3–7 relatively few patients receive medical attention.8
As a rule, when children present with back pain, clinicians typically suspect more serious underlying disease; this traditionally held view, in turn, has led to the practice of doing extensive work-ups to determine possible etiologies.9 More recent studies have demonstrated lower rates of identifiable disease.10,11
This review article covers the epidemiology, clinical evaluation, imaging work-up, and imaging findings of entities causing back pain in children.
Epidemiology
The prevalence of back pain in children and adolescents varies widely from 12% to 50%. Jones et al8 reported an average lifetime prevalence of back pain of 40.2% in 500 children between 10 and 16 years of age. Burton et al12 demonstrated a lifetime prevalence increase from 12% at 11 years of age to 50% at 15 years of age. A cross-sectional study performed in a Danish population showed a dramatic increase in the prevalence of low back pain in the early teen years.9 Sato et al4 recently reported a lifetime prevalence of 28.8% in Japanese children, increasing to 42.5% in junior high school. By 18 years of age in girls and 20 years of age in boys, Leboeuf-Yde and Kyvik13 demonstrated that >50% of these children had experienced at least 1 episode of low back pain.
The difficulty in determining the prevalence of back pain in the pediatric population in part may be related to the following: 1) differences among practitioners in defining back pain, 2) variability in the time period assessed,14,15 and 3) the small number of prospective studies on the epidemiology of low back pain in children.16 For example, while some articles refer to back pain in general11,15,17,18 others refer exclusively to low back pain4,5,19 or to nonspecific back pain.20,21
Back pain in children is often the manifestation of a benign process; in some cases, however, it may suggest a serious pathology such as a neoplasm or an infectious process. Unfortunately, organic pathology (benign or malignant) is not always identifiable; this problem, in turn, frequently leads to extensive diagnostic work-ups in children described as having nonspecific or mechanical back pain.17,19 In a recent prospective study, Bhatia et al17 examined the rate of pediatric back pain diagnosed and the value of the various tests used in making diagnoses. In this study, 78% of patients had no definitive final diagnosis, including those with disorders that might have been treatable but were not identified. Similarly, Auerbach et al19 found a high prevalence of mechanical back pain (53%) with negative findings on radiographs, SPECT, CT, and MR imaging.
Prevalence is also influenced by the subgroup studied and, in general, tends to increase with age and is higher in girls than in boys.12,16 The adolescent athlete, for example, belongs to a different subgroup than the young child because back pain in the adolescent more often results from acute injury or, more commonly, overuse injury.22–24
Clinical Evaluation
In evaluating the child with back pain, the clinician must first take a detailed clinical history and perform a thorough physical examination before further diagnostic studies are recommended. There is general agreement among physicians that children and adolescents with back pain who have no significant physical findings, short duration of pain, and a history of minor injury can be conservatively treated without radiographic or laboratory studies.5,18
Characterization of the pain, including the mechanism of onset, duration, and frequency, is essential to making accurate diagnoses. Important features such as the site of pain; radiation of pain; acute or chronic pain; remitting or unremitting pain (often seen with infection or malignancy); exacerbating and relieving factors, such as time of onset (eg, nighttime pain); pain that worsens with spinal movement; and pain associated with recent onset of scoliosis should be considered.11,15,18,23 Pain associated with constitutional symptoms such as fever, malaise, and night sweats may indicate underlying infection or malignancy. Pain that improves with aspirin or nonsteroidal anti-inflammatory drugs may be associated with an underlying osteoid osteoma. Other considerations include lifestyle, psychological and social factors, hobbies, sports activities, interference with school, school backpack weight, and family history of back pain.15,25,26
The clinician should recognize symptoms and signs that may represent serious pathology and may warrant further urgent investigation (Table 1).15 “Red flags” in the history include pain in prepubertal children, especially <5 years of age; acute trauma; progression of symptoms with time; functional disability; pain lasting >4 weeks; history of malignancy or tuberculosis exposure; recurrent or worsening pain; early morning stiffness and/or gelling; night pain that prevents or disrupts sleep; radicular pain; fever; weight loss; malaise; postural changes (eg, kyphosis or scoliosis); and limp or altered gait. Red flags in the physical examination include fever, tachycardia, weight loss, bruising, lymphadenopathy or abdominal mass, altered spine shape or mobility, vertebral or intervertebral tenderness, limp or altered gait, abnormal neurologic symptoms, and bladder or bowel dysfunction.11,15,18,23,27,28 In a study by Feldman et al,11 the correlation between the type and location of pain, scoliosis, and an abnormal neurologic examination was evaluated for its predictive value in making a specific diagnosis. Their results showed that when both radicular pain and abnormal findings on a neurologic examination were present, the specificity and positive predictive value of making a specific diagnosis were 100%. Night pain also had a very high specificity (95%) for determining a specific diagnosis. Lumbar back pain was the most sensitive (67%) and had the largest negative predictive value (75%) of the variables identified.
Table 1:
Symptoms and signs that may indicate serious underlying pathology in children with back pain—red flags
| History | Examination |
|---|---|
| Prepubertal children especially <5 years | Fever, tachycardia |
| Functional disability | Weight loss, bruising, lymphadenopathy, or abdominal mass |
| Duration >4 weeks | Altered spine shape or mobility |
| Recurrent or worsening pain | Vertebral or intervertebral tenderness |
| Early morning stiffness and/or gelling | Limp or altered gait |
| Night pain | Neurologic symptoms |
| Fever, weight loss, malaise | Bladder or bowel dysfunction |
| Postural changes: kyphosis or scoliosis | |
| Limp or altered gait |
Reproduced with permission from BMJ Publishing Group Ltd & Royal College of Paediatrics and Child Health.15
Laboratory tests are indicated for patients who have a high suspicion for infection or systemic illness and should include inflammatory markers and a complete routine blood panel. Blood cultures sent before antibiotic therapy may be useful in identifying an organism in 30% of cases of vertebral osteomyelitis or diskitis.22 Assessment of acute-phase reactants, full blood count with blood film, and LDH levels are indicated if malignancy is suspected. Abdominal sonography and urinary catecholamines may aid in the diagnosis of neuroblastoma.15
Imaging Evaluation
There is no standard imaging work-up for back pain in children. Various algorithms have been used and are proposed for routine clinical practice.11,15,17,19 Imaging evaluation is reserved for those patients with symptoms and signs suggesting an underlying pathology. Conventional radiographs are used as the initial diagnostic screening test. The choice of CT, MR imaging, or bone scintigraphy depends, however, on the clinical presentation, suspected underlying pathology, and the child's age.15
Conventional Radiography
Spine radiography may not be recommended initially in patients who have had benign findings on physical and neurologic examination and whose symptoms are of short duration.18 When indicated, radiographs are a good initial diagnostic tool for the evaluation of back pain in children and should include both anteroposterior and lateral views of the spine. Collimation to the precise area of interest often helps. Oblique views are not routinely obtained in children, however, in part because of concerns regarding exposure to radiation and in part because subtle fractures are often missed on radiography. In the recent study by Feldman et al,11 plain radiography demonstrated a high diagnostic yield. Among patients who had a specific diagnosis in his study, 68% were diagnosed by plain radiographs.
Nuclear Medicine, CT, and MR imaging
After plain radiography, the imaging technique best suited for imaging back pain in children is subject to debate. The clinician must be especially mindful of the amount of radiation exposure associated with each diagnostic technique—an important consideration in imaging children. The use of CT in children, for example, has increased significantly in the past 2 decades. Although CT is an excellent diagnostic tool, there is some evidence that repeated scanning (and associated ionizing radiation) may place some children at risk for fatal cancers. The principles of ALARA should be applied to reduce radiation exposure.29 As a rule, the use of CT in children should be kept to a minimum, and when indicated, imaging should be restricted to the smallest FOV necessary.30 When possible, imaging modalities that do not emit ionizing radiation, such as MR imaging, should be used in the pediatric population.
In the setting of persistent back pain with negative findings on plain radiographs, 99mTc-MDP SPECT has been the criterion standard. However, the use of 18F with PET has been shown recently to provide exquisite detail.31 Radionuclide imaging can detect abnormalities (eg, spondylolysis, stress fractures)32 or bone lesions (eg, osteoid osteoma). In a study by Auerbach et al, 19 negative findings on a SPECT scan were 100% predictive of MBP in patients with <6 weeks of pain. MBP was diagnosed when there was no demonstrable cause of back pain and findings on all imaging studies (SPECT, CT, MR imaging) were negative. Spondylolysis, however, was more often detected by SPECT compared with MR imaging.
Achieving an effective radiation dose with SPECT is also of paramount importance, especially in cases in which a fracture requires further CT evaluation and exposes the child to yet more radiation.33 In addition, SPECT may not identify other organic causes of back pain such as bone tumors, soft-tissue tumors, or soft-tissue infections. Until recently at our institution, back pain in the young athlete has been evaluated by a SPECT bone scan followed by CT of the affected area. These patients are now evaluated by MR imaging, and in cases in which there is some evidence of spondylolysis, the extent of healing is assessed by follow-up CT for up to 4 months following the initial diagnosis. This approach has recently been explored by Dunn et al,33 who concluded that MR imaging should be used as the first-line imaging technique for evaluating adolescents with back pain, specifically when acute spondylolysis is suspected, because the presence of marrow edema is detected with great clarity on both sagittal STIR and fat-saturated T2 images.
CT is widely accepted as the criterion standard for the evaluation of osseous structures, and it is considered the imaging technique of choice for characterizing fractures, monitoring healing, and detecting progression.23,33 CT alone fails, however, to detect early stress reaction and other relevant spinal abnormalities. In such cases, helical imaging is performed through the area of interest followed by 2D reconstruction of the images generated with this technique. 3D reconstruction models have become increasingly important in the preoperative evaluation of spinal trauma and scoliosis and in presurgical orthopedic planning.
MR imaging is the technique of choice in diagnosing intraspinal or paraspinal pathology, especially in younger children whose clinical histories and physical examinations are characterized by the several red flags mentioned previously. Indeed, increasing numbers of institutions use MR imaging as the first-line imaging technique when serious underlying pathology is suspected in a child with back pain.15 MR imaging is useful in evaluating soft tissue, bone marrow, and intraspinal contents, including disk disease, spinal tumors, infection, and congenital anomalies. More recently, it has been favored for evaluating bone marrow edema (evident, for example, in stress fractures) or for assessing spondylolysis.33 On the basis of the suspected underlying abnormality, the examination is tailored accordingly. In all cases, the decision to use MR imaging must be weighed carefully against the relatively high cost of this type of study, the need to sedate younger children before and during a given examination, and the potential for adverse reactions to anesthesia and/or side effects arising from its administration.
In the sections that follow, imaging sequences are presented as they relate to specific conditions associated with back pain. Some of the common etiologies of back pain are described in the sections below. This discussion is not meant to be exhaustive and is summarized in Table 2.
Table 2:
Etiology of back pain in children and adolescents
| Back Pain |
|---|
|
Traumatic/Musculoskeletal Disorders
The spine in early childhood and adolescence is anatomically different from that of the adult. These differences include increased cartilage/bone ratio, the presence of secondary ossification centers, and soft-tissue hyperelasticity. The vertebral bodies are in part cartilaginous, and the intervertebral disk spaces appear larger. This ratio reverses with age. Vertebral apophyses are secondary centers of ossification that develop at the superior and inferior surfaces of the vertebral bodies. These apophyses become radiographically apparent between 8 and 12 years of age and fuse by adulthood.23
The adolescent athlete can have acute injuries (macrotrauma) or overuse injuries (microtrauma). Overuse injuries can result from sports that involve rapid and repetitive hyperextension, hyperflexion, and rotatory motion. Flexion-based injuries include disk degeneration, atypical Scheuermann disease, and internal disk derangement. Extension-based injuries include, but are not limited to, spondylotic processes.23
Traumatic spinal injuries have been classified according to the Denis 3-column theory.34 The 3 columns described in this theory are the anterior (containing the anterior longitudinal ligament and the anterior half of the vertebral body and annulus), the middle (the posterior half of the vertebral body and annulus), and the posterior (the posterior arch and stabilizing ligaments). If a single column is involved, the injury is considered stable. Two-column involvement indicates instability. Posterior column injuries include spondylolysis and spondylolisthesis, facet syndrome, lordotic low back pain, and sacroiliac inflammation. Anterior column injuries include disk herniation, Scheuermann kyphosis, and atypical Scheuermann disease.23
Stress fractures of the lumbar spine are relatively common. The main components of lumbar motion occur at the L3–L4 and L5–S1 levels. Although fractures of the pedicle and sacrum can occur, pars fractures (spondylolysis) are more frequent.24
Spondylolysis and Spondylolisthesis
Spondylolysis is a defect or disruption in the pars interarticularis of the vertebral arch. Bilateral spondylolysis is more frequent than unilateral spondylolysis, and L5 is the most commonly affected vertebral level.35 A large prospective study of spondylolysis reported a prevalence of 4.4% in children and 6% in the general population.36 The etiology of spondylolysis is controversial, with both developmental defects and trauma proposed as risk factors.23,37 Most frequently, spondylolysis is associated with repetitive microtrauma, occurring in the adolescent during spinal growth. An increased incidence of spondylolysis is seen in adolescent athletes who practice sports with repetitive and excessive hyperextension such as gymnastics, diving, ballet, and soccer.38,39 In the general population, spondylolysis is more frequent in males, though young female athletes are also at risk for spondylolysis.39 Other risk factors include spina bifida occulta, sacral anatomy, and family history.37,40,41
Imaging Evaluation
There is no general consensus for the imaging evaluation in suspected cases of spondylolysis. As previously mentioned, until recently at our institution, bone scans have been initially obtained, followed by CT of the affected area. MR imaging is now performed initially; in cases in which spondylosis is confirmed, a follow-up CT to assess healing may be performed for up to 4 months following the initial diagnosis. However, if the findings of the MR imaging study are initially negative and if the patient continues in pain with no response to physical therapy, then the physician may order a bone scan (SPECT).
The diagnostic imaging work-up for suspected spondylolysis is typically initiated with plain radiographs. Although this technique has a low sensitivity for detecting spondylolysis, it can detect spondylolisthesis, which, in the presence of bilateral pars defects, is characterized by the anterior slippage of a given vertebra over the one below it.42 The amount of slippage is graded by measuring the degree of displacement of the vertebral body relative to the inferior vertebral body. Grade 1 represents <25% displacement; grade 2, 25%–50% displacement; grade 3, 50%–75% displacement; and grade 4, 75%–100% displacement. Grade 5 (spondyloptosis) refers to complete displacement of the vertebral body anteriorly, with inferior displacement to the level of the vertebral body below (Fig 1). On oblique plain films of the lumbar spine, a lucency can be seen in the pars interarticularis. In addition, ipsilateral pedicle hypertrophy and/or sclerosis can be present. An oblique lucency at the base of the laminae may be seen on the lateral view.
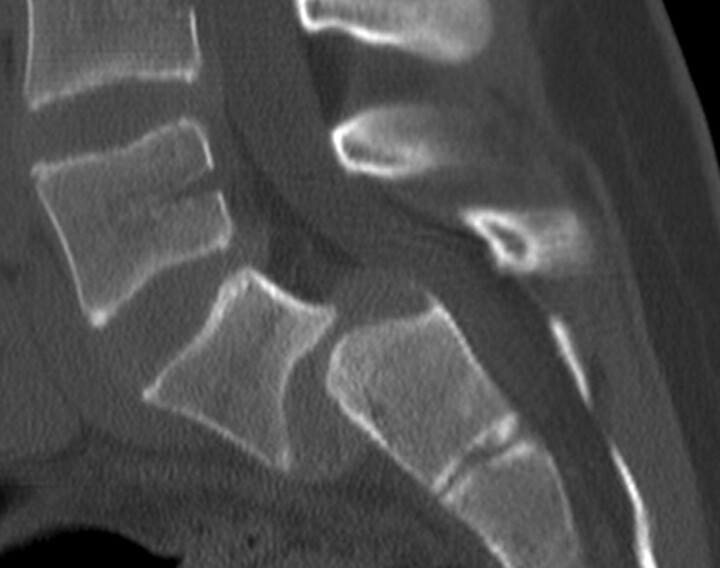
Fig 1.
Spondylolisthesis in a 12-year-old girl. Sagittal 2D CT reconstruction image demonstrates grade 3 anterolisthesis of L5 on S1.
SPECT bone scans are very sensitive for detecting spondylolysis, revealing areas of bone turnover; and the findings are generally positive for a prolonged period.19 On SPECT, spondylolysis will present as increased radiotracer uptake in the posterior elements (the pars interarticularis, lamina, or pedicle) (Fig 2A). These findings may suggest stress reaction, stress fracture, or a symptomatic spondylolytic defect.
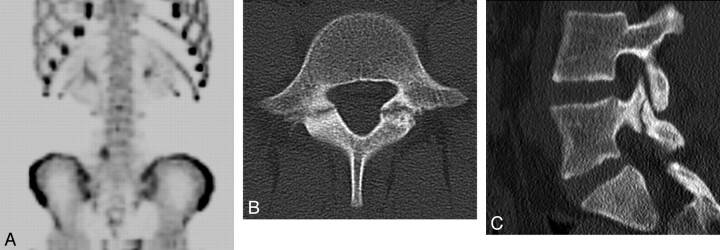
Fig 2.
Spondylolysis in a 13-year-old girl. A, 99mTc-MDP SPECT scan demonstrates increased uptake in the region of the right pars interarticularis of L5. B, Axial helical CT image demonstrates bilateral spondylolysis at L5. C, Sagittal 2D reconstruction image shows extension of the right pars fracture into the right L5 superior facet.
CT scans have been considered the criterion standard for characterizing fractures and for detailing bone morphology and anatomy.33,43 The CT technique consists of a limited helical scan (3-mm section thickness with reconstruction to 0.75 mm) from the pedicle of the vertebra above to the pedicle of the vertebra below the level or levels of interest. On CT, fractures arising from a stress reaction may present with localized sclerosis without trabecular or cortical disruption. In addition, cortical or trabecular disruption of the pars interarticularis with minimal sclerosis or lysis of the fracture gap may be seen (Fig 2B). Visualization of the pars defect may be aided by sagittal reformations (Fig 2C).
MR imaging evaluation of spondylolysis consists of sagittal T1-weighted images and sagittal T2-weighted images with fat saturation (or STIR), axial T1-weighted images, and nonangled axial FSE T2-weighted images with fat saturation (or STIR) of the lumbosacral spine. On MR imaging, a spondylolytic defect with focal decreased signal intensity of the pars interarticularis on sagittal and axial T1-weighted imaging may be present. Incomplete fractures propagate in an inferior-to-superior direction.33 There may be high signal intensity on STIR or T2-weighted fat-saturated MR images, consistent with marrow edema. MR imaging is less useful for demonstrating the healing response of incomplete fractures. Neither MR imaging nor CT, however, can reliably distinguish whether an incomplete fracture is in an evolutionary or reparative phase.33 Saifuddin and Burnett44 have proposed the following widely used MR imaging classification for spondylolysis: grade 0 (normal): normal marrow, intact cortical margins; grade 1 (stress reaction): marrow edema, intact cortical margins; grade 2 (incomplete fracture): marrow edema, cortical fracture incompletely extending through the pars; grade 3 (complete active fracture): marrow edema and fracture completely extending through the pars (Fig 3A); and grade 4 (fracture nonunion): no marrow edema, fracture completely extending through the pars.
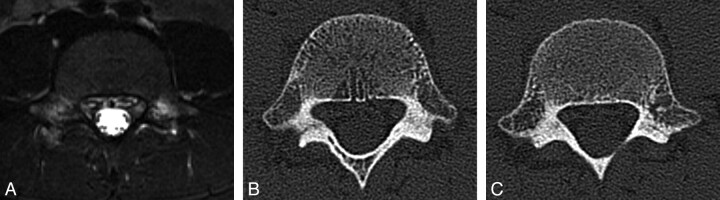
Fig 3.
Spondylolysis in an 8-year-old boy. A, Axial T2-weighted image with fat saturation demonstrates hyperintense signal intensity consistent with bone marrow edema in the region of the pars defects bilaterally. B, Axial CT image demonstrates a complete pars defect of L5 on the right. C, Axial CT image demonstrates an incomplete pars defect of L5 on the left.
The evolution of spondylolysis has been described in 4 stages45: The first stage consists of a stress reaction that is radiologically inapparent but visible on bone scintigraphy and MR imaging.43 The second stage, early spondylolysis, represents a range of features including hairline fractures and bony resorption evident on CT. The third stage represents a complete pars fracture with or without fragmentation—also referred to as progressive spondylolysis (Fig 3B, -C). The fourth stage, referred to as terminal spondylolysis, is characterized by nonunion of the fracture and sclerosis.
Once a firm diagnosis of spondylosis is made, the patient is generally treated with a brace, and participation in sports is restricted. Activity is limited to physical therapy and certain forms of exercise (eg, stationary biking and modified swimming). On subsequent visits, the patient is reassessed, and if asymptomatic with hyperextension, a return to sports may be considered. If pain persists, however, further imaging and treatment may be indicated.23
Vertebral Body Fractures
Thoracolumbar fractures are more common in older children and adolescents, while cervical fractures are more common in younger children. In athletes, acute fractures of the thoracolumbar spine are rare.23 Plain films are useful in assessing the degree of compression of the vertebral body. Compression of <25% indicates stability, with a single anterior column involvement. CT is indicated if the compression approaches 50%, which may be indicative of anterior and middle column involvement. In children, injury may be present without evidence of radiographic abnormality. In these situations, diagnosis is often elusive, and MR imaging is indicated for evaluation of intraspinal abnormalities.
Disk Degeneration and Herniation
Intervertebral disk degeneration, a fairly common finding in children with low back pain, is seen in approximately 50% of symptomatic patients, compared with 20% in asymptomatic patients.46 MR imaging shows loss of disk height and decreased signal intensity on T2-weighted images. The finding of disk degeneration has no impact on treatment, however.
Intervertebral disk herniations in children are similar to those in adults with 3 exceptions: 1) The size of disk herniations is larger in children than adults, 2) traumatic disk herniation in adolescents is frequently accompanied by a fracture of the adjacent vertebral endplate (apophyseal ring fracture), and 3) pediatric disk herniations are often calcified.47 Most children with disk herniation are asymptomatic, and most patients recover completely without surgical intervention. As mentioned previously, disk herniations may be associated with apophyseal ring fractures. Apophyseal ring fractures, also known as endplate avulsion fractures, are more frequently seen in the lumbosacral spine and are best appreciated on CT and MR imaging. On CT, there is an arc-shaped or rectangular bone fragment posterior to the dorsal endplate margin.48 On MR imaging, apophyseal fractures manifest as bone marrow edema in the donor vertebral body with the disk extending into the defect. On T2-weighted images, the disk between the fragment and the vertebral body is hyperintense. The bone fragment appears hypointense on T1-weighted images. Disk desiccation can occur with time, appearing hypointense on T2-weighted images.49 Surgical intervention depends on clinical symptoms.48–50
Scheuermann Kyphosis (Juvenile Kyphosis)
Scheuermann kyphosis is an osteochondrosis presenting as an abnormality of the vertebral epiphyseal growth plates.18 This condition presents as a form of adolescent thoracic or thoracolumbar kyphosis characterized by anterior wedging of 3 or more contiguous vertebrae of 5° or greater resulting in a thoracic kyphosis greater than 35°, with the apex more commonly seen between T7 and T9. Other radiologic criteria for the diagnosis of Scheuermann kyphosis include irregular upper and lower endplates with Schmorl nodes, disk-height loss, and associated apophyseal ring fractures (Fig 4). Etiologies for this condition include genetic factors, repetitive microtrauma, osteoporosis, osteochondrosis, necrosis ring apophysis, and tight hamstrings.23
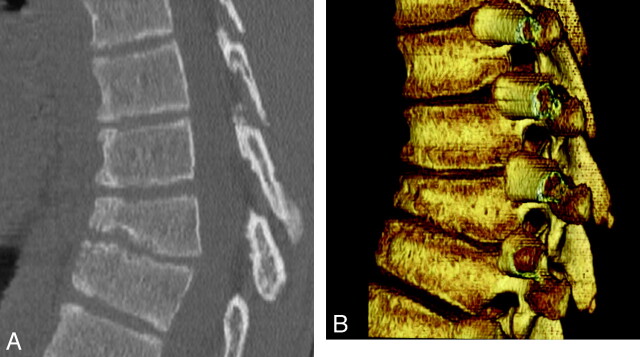
Fig 4.
Scheuermann kyphosis in a 15-year-old boy. A, Sagittal 2D CT reconstruction image demonstrates midthoracic kyphosis with anterior wedging of at least 3 consecutive vertebrae with presence of Schmorl nodes. B, Sagittal 3D CT reconstruction image demonstrates midthoracic kyphosis with anterior wedging of at least 3 consecutive vertebrae with the presence of Schmorl nodes.
Patients present with pain typically localized to the midscapular region located over the kyphotic deformity. The pain usually intensifies gradually, though without an episode of precipitating trauma; it generally worsens after activity and improves with rest. Conservative treatment is strongly recommended in patients who have spinal growth remaining and who have responded well to therapy (ie, physical therapy and sometimes the use of a brace).22,23
The initial diagnostic imaging evaluation consists of plain radiographs. CT and MR imaging may be indicated to confirm or further delineate disease (Fig 5). They may also be helpful in detecting associated apophyseal ring fractures. Atypical Scheuermann kyphosis (lumbar type) occurs at the thoracolumbar level with the apex situated between T10 and T12. There is a greater incidence reported in males22 and among athletes who participate in sports requiring repetitive flexion such as wrestling and football.22
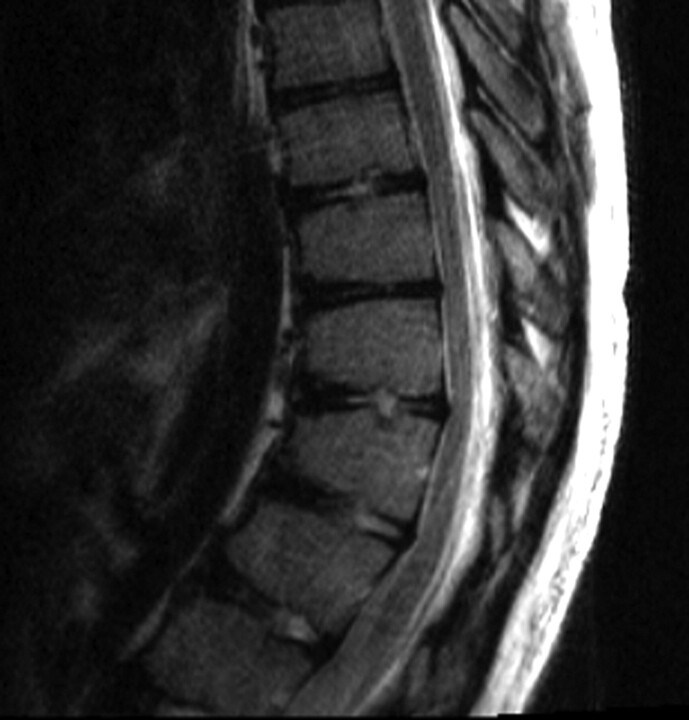
Fig 5.
Scheuermann kyphosis in a 14-year-old boy. Sagittal T2-weighted image demonstrates thoracic kyphosis with mild anterior wedging of the T10–T12 vertebral bodies with slight disk space irregularity and Schmorl nodes. Minimal annular bulges slightly indent the ventral aspect of the thecal sac.
Disk Calcification
Intervertebral disk calcification is a rare entity in childhood. The etiology remains unknown, though inflammation and trauma have been suggested as possible causes. Intervertebral disk calcification can be an incidental finding or can present with symptoms such as pain, stiffness, decreased range of motion, muscle spasm, tenderness, and torticollis. Some patients present with fever and increased ESR.51–53 In general, the symptoms are relatively brief, rarely lasting longer than several weeks.52 Neurologic complications may occur, however, when the calcification herniates through the fibrous annulus, causing nerve root or spinal cord compression. Anterior or posterior herniation of the calcified intervertebral disk material may also develop. Dysphagia associated with anterior disk protrusion has been described.54
Disk calcification is most frequently found in the cervical spine, less frequently in the thoracic spine, and only rarely in the lumbar spine.52 Symptoms are seen most frequently with calcification of the cervical spine, typically at the level of C7–T1, though multiple levels can be affected.51 Boys seem to be slightly more often affected than girls.52,53,55 The average age at diagnosis is 7–8 years, with a range of 7 days to 20 years.51,53,56
Disk calcification in children can be seen as part of a syndrome or disease, such as Morquio syndrome, I cell disease, Patau syndrome, congenital or acquired vertebral fusion, hyperparathyroidism and other hypercalcemic states, osteomyelitis, tuberculosis, and diskitis.56
Disk calcification, while often difficult to identify, is usually seen on plain film or CT as an attenuated, round, oval, flattened, or fragmented calcification in the nucleus pulposus (Fig 6). CT or MR imaging may also demonstrate an associated disk herniation. On MR imaging, calcification can appear as decreased signal intensity on T2-weighted images or as hyperintense on T1-weighted images.
Fig 6.
Disk calcification in a 6-year-old boy. A, Axial CT image demonstrates posterior extrusion of a calcified disk. B, Sagittal 2D CT reconstruction image demonstrates calcification in the central portion of the disk.
Disk calcification in children is considered a self-limiting condition with a good prognosis. Dai et al52 have reported that in a series of 17 cases of disk calcification, the calcific deposits had completely resolved. While the severity of the symptoms is often not correlated with the radiographic findings, conservative treatment is generally recommended, even in the setting of disk herniation.52 At times, however, surgery is a preferable course, especially in patients with intractable pain and progressive neurologic deficit.57
Infectious Disorders
Spinal infection may involve the vertebral body, intervertebral disk, paravertebral soft tissues, epidural space, leptomeninges, or the spinal cord. Infectious processes of the spine in children include vertebral osteomyelitis, sacroiliac pyarthrosis, diskitis, epidural abscess, meningitis, arachnoiditis, myelitis, and spinal cord abscess.58–60
Diskitis
Diskitis is an inflammatory process or infection of the intervertebral disk. Diskitis has a bimodal distribution occurring in young children between 6 months and 4 years of age, with a second subtler peak from 10 to 14 years of age.61 Although the pathophysiology of diskitis is not entirely understood, it is thought to be related to the presence of vascular channels that terminate in the cartilaginous portion of the disk and disappear later in a life, thus making the disk susceptible to infection. Abundant intraosseous arterial anastomoses during childhood are thought to promote clearance of micro-organisms or entrapped emboli, making the vertebral body less susceptible to infarction from septic emboli.62,63 Most experts attribute the etiology to an infectious process.
Diskitis occurs typically in the lumbar region, most often at the L2–L3 and L3–L4 levels. Clinical presentation varies widely, making the diagnosis difficult. Symptoms and signs may include, among others, fever, back pain, irritability, and refusal to walk or sit up. Mild leukocytosis and an elevated ESR and C-reactive protein level are usually present; results of blood cultures can often be negative.64 In one-third to one-half of patients, however, results of blood cultures or biopsy materials are positive and the infectious agent is almost always Staphylococcus aureus.60
While findings of radiographs of the spine are usually normal in the early stages of disease, findings of bone scintigraphy can be positive as soon as 1–2 days after the onset of symptoms, demonstrating increased uptake in the intervertebral bodies on each side of the disk involved. However, bone scintigraphy is not specific and cannot differentiate diskitis from other causes of back pain. The earliest time interval between the onset of symptoms and a positive radiograph has been 12 days. In the series of Fernandez et al,60 of 33 children with diskitis, 76% had abnormalities detected on spine radiographs and the most frequent finding was decreased height of the disk space and erosion of adjacent vertebral endplates.
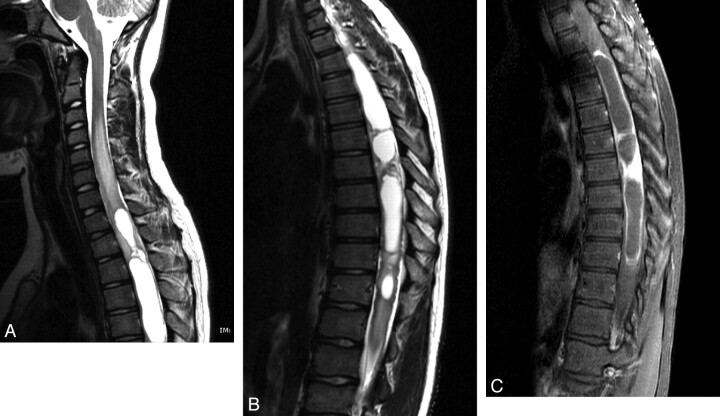
MR imaging is the study of choice because it can detect diskitis early on. MR imaging findings include loss of the normal hyperintense signal intensity of the disk on T2-weighted images, narrowing or complete absence of the disk, and abnormal increased T2-weighted signal intensity in the adjacent vertebral bodies, consistent with marrow edema (Fig 7A).65 There may be contrast enhancement of the disk and adjacent vertebral body (Fig 7B). MR imaging detects disk extrusion and the formation of paraspinal and epidural abscesses. Any evaluation for suspected diskitis should exclude spinal cord compression.58,65,66 Follow-up radiographs will show persistent narrowing of the intervertebral disk space and sclerosis at adjacent vertebral bodies weeks or months after the initial diagnosis. Most patients, moreover, will be asymptomatic within 3 weeks following antibiotic treatment, and in such cases, disk space height can sometimes be restored.
Fig 7.
Vertebral osteomyelitis and diskitis in a 7-year-old boy. A, Sagittal T2-weighted image with fat saturation shows marked disk space narrowing at L2–L3 with hypointense T2 signal intensity within the disk. There is increased T2 prolongation in adjacent vertebral bodies. B, Sagittal T1-weighted MR image with fat saturation with gadolinium shows diffuse enhancement in the L2–L3 vertebral bodies and intervening disk space.
Vertebral Osteomyelitis
In children, osteomyelitis occurs more frequently in the long bones than it does in the spine. When it does present in the spine (vertebral osteomyelitis), it is thought to occur when micro-organisms lodge in the low-flow end-organ vasculature adjacent to the subchondral plate region. A history of trauma has been associated with vertebral osteomyelitis and diskitis.67,68 Possible infectious causes include bacteria (S aureus)60 and tuberculosis in endemic areas.69 Other etiologies include coccidioidomycosis, blastomycosis, and actinomycosis. The clinical presentation of the older child with vertebral osteomyelitis includes fever and back pain in the lumbar, thoracic, or cervical regions. Initially, plain radiographs may demonstrate localized rarefaction of 1 vertebral body and, later, destruction of bone, usually anteriorly with osteophytic formation.60,63
Diskitis and vertebral osteomyelitis often, however, cannot be differentiated in the early stage of the disease process. Nuclear medicine bone scans and CT are not useful in providing a specific diagnosis of vertebral osteomyelitis. MR imaging is the technique of choice for the assessment of vertebral osteomyelitis, with high sensitivity and specificity. MR imaging should include T1-weighted images and T2-weighted images with fat saturation (or STIR) in the sagittal and axial planes. Bone marrow edema, an early nonspecific finding, presents as low signal intensity on T1-weighted and high signal intensity on STIR or T2-weighted images with fat saturation (Fig 7A).64 Fat-suppressed T1-weighted images with contrast can detect early cases of spinal infection and can determine accurately the extent of disease (Fig 7B).64
It is often difficult to differentiate osteomyelitis from leukemia/lymphoma or metastatic disease. These entities usually affect several noncontiguous vertebral bodies, do not involve the disk space, and may not produce a paraspinal mass.35
Neoplastic Disorders
Neoplasms of the spine can be classified according to the site of origin. Neoplasms involving the spinal column include primary tumors of the vertebra, such as aneurysmal bone cysts, LCH, giant cell tumors, Ewing sarcoma, osteoid osteoma and osteoblastoma, and, rarely, osteosarcomas.70,71 Intraspinal tumors can originate from the spinal cord (intramedullary) or outside the spinal cord (extramedullary). Intramedullary tumors account for 35%–40% of all intraspinal tumors in children.72 The most common histologic types are astrocytomas (45%–60%) and ependymomas (30%–35%).73 Astrocytomas present more frequently in younger children and decrease in frequency into adulthood, while ependymomas become more predominant with age.74 In a series of intramedullary spinal cord tumors in patients younger than 3 years of age, no ependymomas were reported.75 Other intramedullary tumors include gangliocytomas, gangliogliomas, germinomas, primitive neuroectodermal tumors, and LCH. Extramedullary tumors account for approximately two-thirds of all intraspinal tumors and can be extradural (50%) or intradural (10%–15%).76 Again, according to the site of origin, these can be meningeal (meningiomas), from the nerve roots/nerve root sheaths (neurofibromas and schwannomas); extraspinal tumors that invade the epidural space (neuroblastoma-ganglioneuroblastoma-ganglioneuroma spectrum); or lymphomas or primitive neuroectodermal tumors.47,77
Pain is the most frequent presenting symptom for spinal tumors and can be diffuse or radicular.72,74,78 Pain can be present in approximately 25%–30% of cases: It has been described as dull and aching and localized to the bone segments adjacent to the tumor. Different symptoms can occur depending on the age of the child. Young children and infants can present with severe pain, motor regression, weakness, or frequent falls, whereas older children can present with clumsiness, progressive scoliosis, or gait disturbance.79 Pain usually precedes the development of other symptoms such as weakness, gait deterioration, torticollis, sensory disturbance, and sphincter dysfunction.74 Malignant tumors are characterized by symptoms that are shorter in duration compared with benign lesions and have an increased incidence of associated neurologic deficits.78 Nocturnal pain that awakens the child from sleep can be associated with intramedullary tumors and is thought to arise from venous congestion and dural distention caused by the recumbent position. Nocturnal pain should be considered a red flag for the clinician.72,74
We will present examples of some of the specific tumors that can be associated with back pain.
Spinal Column Tumors
Primary Neoplasms
Osteoid Osteoma.
Osteoid osteoma, a benign osteoblastic lesion of unknown etiology, was first described by Jaffe in 1935.80 This lesion consists of a nidus of osteoid matrix and a stroma of loose vascular connective tissue. The nidus may be calcified and surrounded by sclerotic reactive bone, usually measuring <15 mm. Of all osteoid osteomas, 10% are localized in the spine. Osteoid osteoma is more frequently found in boys; most affected children are 10–12 years of age at the time of diagnosis.
Back pain in children with osteoid osteoma is more intense at night and can be alleviated by aspirin. This lesion often presents as painful scoliosis of the thoracic and lumbar spine secondary to muscle spasm, which differs from nonpainful idiopathic juvenile scoliosis localized in the thoracic spine. The lesion is usually on the concave side of the curve.81,82
The radiologic appearance of spinal osteoid osteoma is similar to that of other parts of the skeleton characterized by a radiolucent nidus, which may contain central calcification surrounded by sclerotic bone. These lesions are usually localized to the posterior elements, most often in the lamina and pedicles, but can also occur in the transverse and spinous processes (Fig 8).81,83
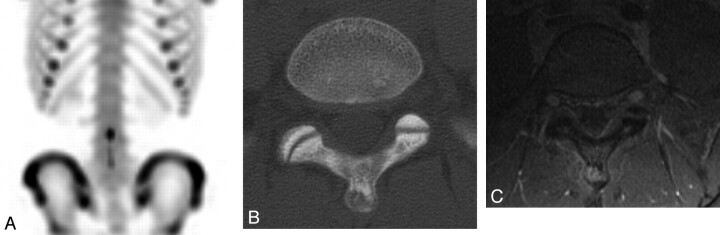
Fig 8.
Osteoid osteoma in a 14-year-old girl. A, 99mTc-MDP SPECT scan demonstrates mild increased uptake in the spinous process of L5. B, Axial CT image shows a lucency in the tip of the spinous process of L5 with surrounding sclerosis and a tiny sclerotic nidus. C, Axial T1-weighted MR image with gadolinium demonstrates homogeneous enhancement of the lesion at the tip of the spinous process of L5.
Although bony sclerosis in osteoid osteoma can be detected on conventional radiography, targeted CT is the preferred cross-sectional technique for the demonstration and precise localization of the lucent nidus (Fig 8B).84 99mTc bone scintigraphy is accepted as the most accurate technique for detection of suspected osteoid osteoma, showing marked uptake of the bone tracer (Fig 8A).81,85
On MR imaging, osteoid osteoma can have a very heterogeneous and variable appearance. The nidus appears isointense on T1-weighted images and hypointense on T2-weighted FSE sequences. Matrix mineralization can present as a focal signal-intensity void. Perinidal edema is usually present and is graded according to location and extension.86 MR imaging is also useful in determining any involvement of the spinal canal and cord.11 Dynamic gadolinium-enhanced MR imaging can often improve the conspicuity of osteoid osteomas over thin-section CT (Fig 8C).87,88 Before surgical or percutaneous treatment (ie, excision, laser treatment, or thermocoagulation), precise localization of the lesion must be determined. CT-guided RFA, a minimally invasive and safe method, has been proved an effective treatment for spinal osteoid osteoma.89,90 Surgery is usually reserved for lesions causing nerve root compression. Another therapeutic approach is gamma probe−guided surgery, which is typically used when RFA is not applicable and complete resection is difficult.91
Osteoblastoma.
Osteoblastoma, also known as giant osteoid osteoma, contains a fibrovascular stroma with numerous osteoblasts, osteoid tissue, well-formed woven bone, and giant cells. Osteoblastoma is usually >2 cm in diameter. Forty percent of all osteoblastomas occur in the spine, specifically in the neural arch, and can often extend to the vertebral body. An associated soft-tissue mass can be present. A neurologic deficit also may be present in approximately 25%–50% of cases. On imaging, osteoblastoma can show progression and aggressive features with bone destruction and a soft-tissue mass but no surrounding bone edema. Osteoblastomas can recur.92
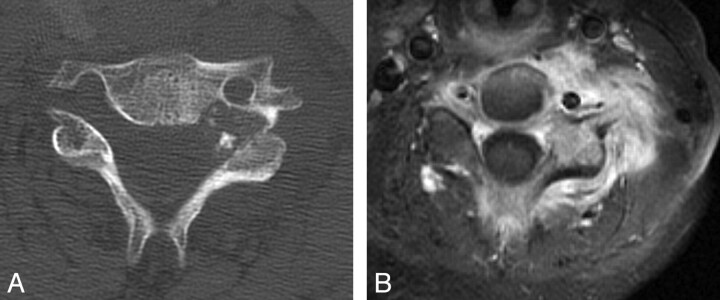
In patients with osteoblastoma, pain at night is not as severe as it is in osteoid osteoma and is not relieved by aspirin. Neurologic deficits occur more frequently in osteoblastomas. CT can demonstrate a geographic lesion with sclerotic borders (Fig 9A). On MR imaging, most lesions have T2-weighted hypointense areas consistent with immature chondroid matrix, hypercellularity, calcifications, and hemosiderin on histologic analysis. Enhancement with gadolinium is often present, which may be lobular, marginal, or septal (Fig 9B).93 Treatment is curettage with bone graft or methylmethacrylate placement. Preoperative embolization may be extremely helpful.92,94
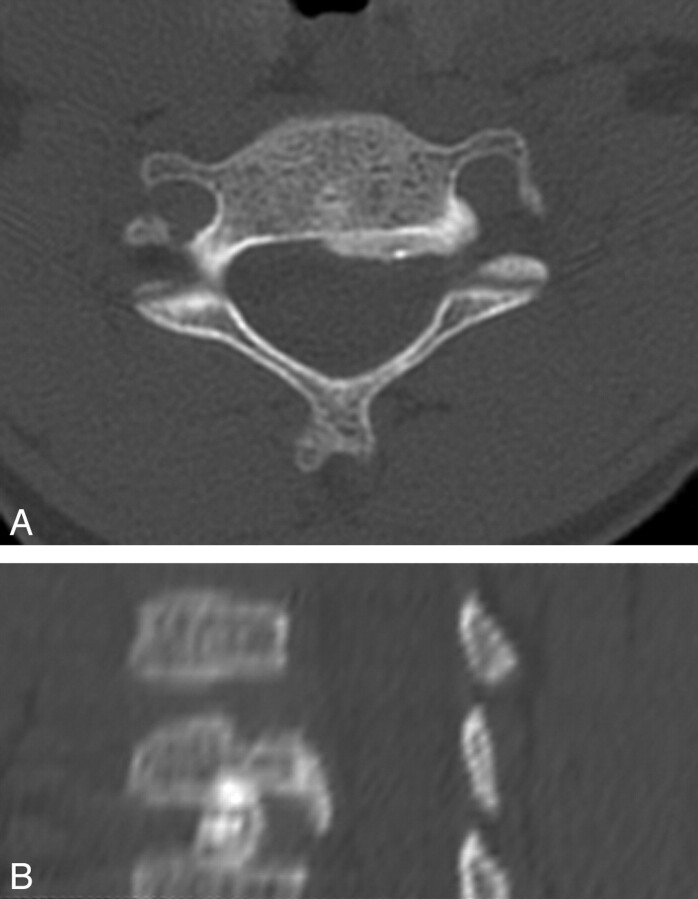
Fig 9.
Osteoblastoma in a 12-year-old boy. A, Axial CT image demonstrates an expansile lytic lesion in the pedicle of the C5 vertebra, which involves the C4–C5 facet joint and the left transverse foramen. B, Axial T1-weighted image with gadolinium and fat saturation demonstrates extensive enhancement in the adjacent bone and the left paraspinal soft tissues of the cervical spine, with extension into the epidural space.
LCH.
LCH (previously termed “histiocytosis X”) comprises a group of rare disorders of unknown etiology, characterized by abnormal proliferation of histiocytes in a variety of organs, causing tissue destruction. This cellular infiltration can affect the bone, skin, and internal organs. Traditionally, LCH has been classified according to certain clinical manifestations, on the age of presentation, and on the severity and distribution of disease. Three main forms described in the order of severity are the following: eosinophilic granuloma, Hand-Schüller-Christian disease, and Letterer-Siwe disease. Eosinophilic granuloma, the most frequent and benign, can manifest as a unifocal or multifocal osseous lesion, with or without soft-tissue involvement, presenting at any age. Hand-Schüller-Christian disease presents in children or young adults; it manifests with the characteristic triad of exophthalmos, osteolytic skull lesions, and diabetes insipidus. Acute disseminated LCH (Letterer-Siwe disease), usually seen in children <3 years of age, can affect multiple organs and systems with a lethal outcome.95
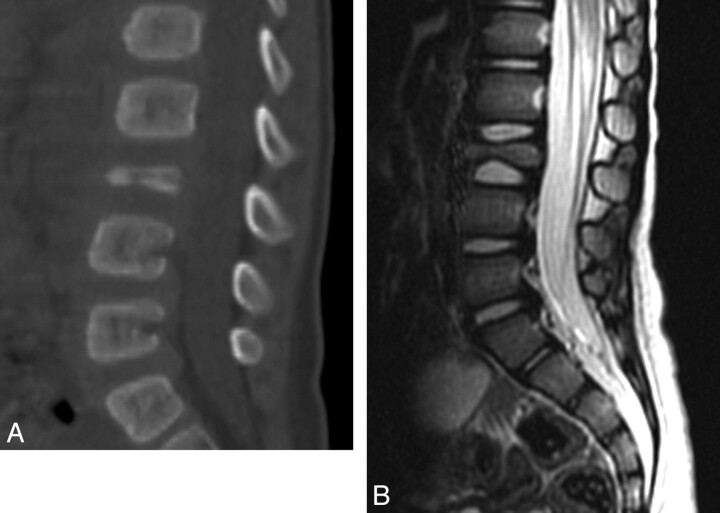
When the spine is involved, LCH most frequently presents with local back pain; the thoracic vertebrae is the most commonly affected region (54%), followed by the lumbar spine (35%) and cervical spine (11%). There may be associated leukocytosis and fever. On conventional radiography, LCH can present as a lytic nonsclerotic destructive vertebral lesion; as a vertebra plana (with preserved adjacent disks and posterior elements rarely involved); or as scoliosis, which is far less common. On CT, the nonsclerotic destructive osseous lesion can present with a paraspinal enhancing soft-tissue mass. Epidural extension may occur. A collapsed vertebra plana is a typical form of presentation (Fig 10A).
Fig 10.
LCH−vertebra plana in an 18-month-old boy. A, Sagittal 2D CT reconstruction image of the lumbar spine shows a collapsed L3 vertebral body. B, Sagittal T2-weighted MR image of the lumbar spine demonstrates a vertebra plana deformity with significant decreased height of the L3 vertebral body and preservation of the adjacent intervertebral disks.
MR imaging is the technique of choice for staging LCH and monitoring response to therapy.96 LCH may manifest as a homogeneously enhancing soft-tissue mass that is hypointense on T1-weighted images and hyperintense on T2-weighted images, with or without a pathologic fracture. When a vertebra plana is present, the classic appearance is 2 vertebral disks in apposition without an intervening normal vertebral body (Fig 10B). The differential diagnosis for vertebra plana includes histiocytosis; tumors; and infections such as tuberculosis, leukemia, lymphoma, trauma, Gaucher disease, and neurofibromatosis.
Treatment for histiocytosis varies and can include conservative management, curettage with allograft implantation, chemotherapy, steroids, and external beam radiation therapy. Spontaneous regression of single spinal lesions with conservative treatment also has been described.97
Ewing Sarcoma.
Ewing sarcoma most commonly affects the spine as metastatic disease from a primary tumor elsewhere in the body but can also present as a primary osseous lesion that is centered in the vertebral body, in the posterior elements, or in the sacrum. Spinal canal invasion is common.98 Rarely, Ewing sarcoma can present as an extraosseous lesion located in the epidural region.99 Clinically, Ewing sarcoma can present with local pain. Neurologic deficits, including muscle weakness and sensory deficiencies, can be present at the time of initial presentation. Bladder and bowel dysfunction are usually late manifestations. Constitutional symptoms, however, are rare.98,100
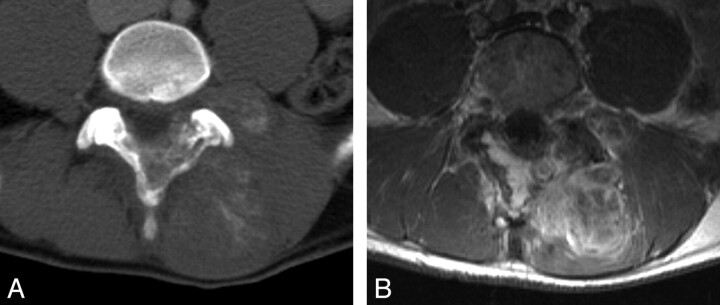
On conventional radiography and CT, Ewing sarcoma presents as a permeative osteolytic lesion with a “moth-eaten” appearance. An extraosseous noncalcified soft-tissue mass can be present in 50% of cases (Fig 11A). Although CT can differentiate Ewing sarcoma from osteosarcoma by confirming the absence of a tumor matrix, it may also underestimate soft-tissue involvement. MR imaging is an excellent tool for delineating soft-tissue extension and invasion into the spinal canal. Ewing sarcoma appears T1-hypointense to normal bone; and on T2-weighted images, it varies from hypointense to hyperintense. Moderate enhancement of the lesion is present with areas of necrosis (Fig 11B).101 Lymphoma and neuroblastoma can have a similar radiographic appearance.
Fig 11.
Ewing sarcoma of the lumbar spine in a 17-year-old boy. A, Post-contrast-enhanced axial CT image demonstrates a large partially calcified mass in the paraspinal musculature at the L3–L5 levels. The mass involves the adjacent spinous process and extends into the spinal canal. B, Axial T1-weighted postgadolinium MR image shows extensive enhancement of the mass with epidural extension.
Secondary Neoplasms
Lymphoma and Leukemia
Spinal involvement of lymphomas and leukemias in children is relatively rare. More often the spine is involved in disseminated disease. Metastases are typically located in the epidural or paravertebral space, though bony and leptomeningeal spread can occur.102 In 4% of all patients with lymphoma, an epidural lesion can be the initial site of presentation.103 Primary spinal lymphoma, most often non-Hodgkin disease, has been reported in children.104,105 Children with acute myelogenous leukemia can present with a solid spinal tumor in the epidural compartment, known as granulocytic sarcoma (chloromas).106,107 Several cases of granulocytic sarcomas have been reported in patients without leukemia.108,109 Chloromas are highly vascularized lesions composed of immature granulocytes.110 On MR imaging, these lesions are isointense to hyperintense on T1-weighted images and isointense to hypointense on T2-weighted images (Fig 12 ) and may demonstrate moderate-to-marked contrast enhancement.110 These tumors tend to respond rapidly to first-line therapies (ie, chemotherapy and radiation).108
Fig 12.
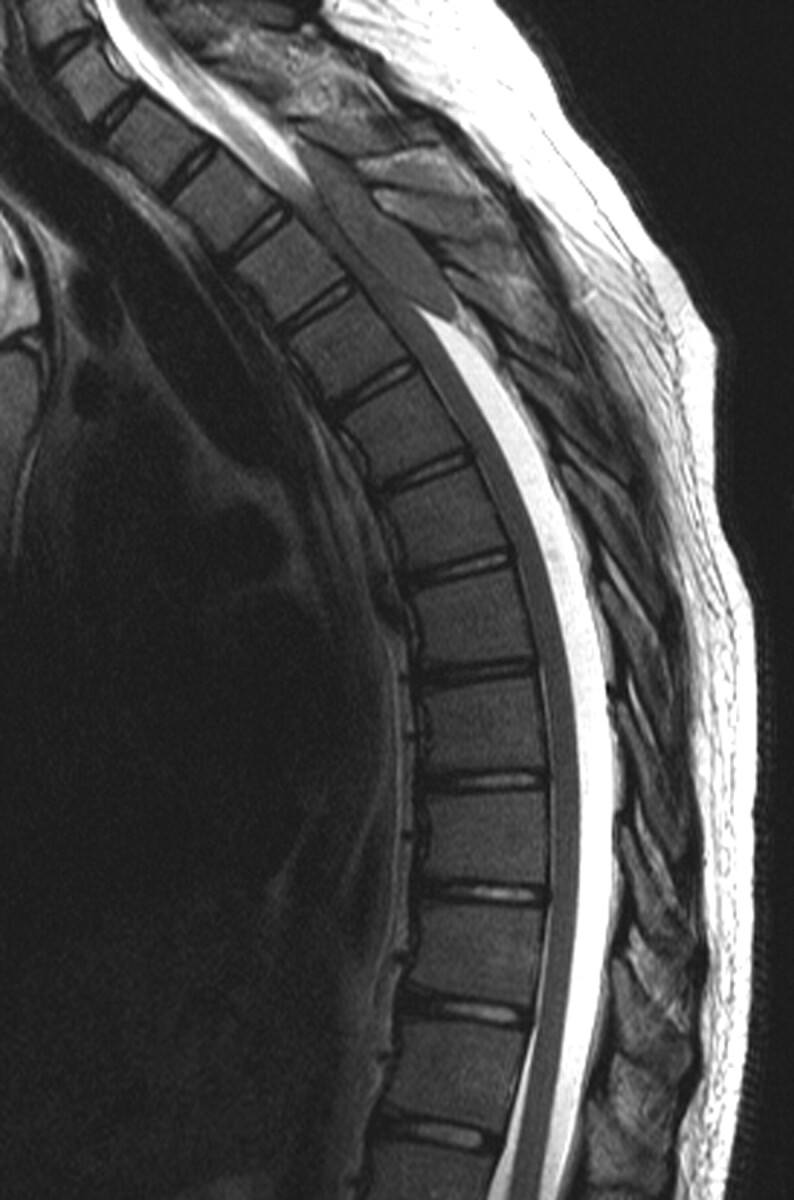
Lymphoblastic lymphoma in a 15-year-old boy. Sagittal T2-weighted MR image demonstrates an intraspinal extradural well-circumscribed hypointense lesion at the T2–T4 level with compression of the spinal cord with hypointensity diffusely in the vertebral bodies.
Unlike the high T1 signal intensity seen in the bone marrow of healthy children, the bone marrow in children with lymphoma and leukemia is low in signal intensity on T1-weighted images (Fig 13). It is unclear if this is the result of leukemic infiltration and/or increased activity of the bone marrow or is secondary to treatment.47 Low signal intensity, however, is not a reliable marker in children younger than 5 years of age because bone marrow in toddlers and infants may still have active hematopoiesis (red marrow), which typically exhibits low signal intensity on T1-weighted images.111 Moreover, following the administration of gadolinium, bone marrow in young children can enhance heterogeneously and should not be confused with tumor infiltration.47 Pathologic vertebral compression fractures can be a manifestation of acute lymphoblastic leukemia in childhood,112,113 secondary to severe osteoporosis and occurring in 1%–7% of patients diagnosed with this cancer.112
Fig 13.
Acute lymphoblastic leukemia in a 3-year-old boy. A, Sagittal T1-weighted MR image demonstrates diffuse abnormal low signal intensity in the lumbar spine bone marrow consistent with a diffuse infiltrative process. B, Sagittal T1-weighted image of a healthy 3-year-old boy with normal higher T1 signal intensity of the vertebral body marrow relative to the intervertebral disks.
Intramedullary Spinal Cord Tumors
Astrocytoma.
Astrocytoma is the most common spinal cord tumor of childhood, comprising 30%–35% of intraspinal tumors and >60% of intramedullary tumors. Astrocytomas are classified pathologically into 4 grades based on the WHO classification: pilocytic astrocytoma (grade 1), fibrillary astrocytoma (grade 2), anaplastic astrocytoma (grade 3), and glioblastoma multiforme (grade 4). In children, 80%–90% of intramedullary astrocytomas are most often low-grade astrocytomas. The most common histologic types are pilocytic astrocytoma and fibrillary astrocytoma. Although uncommon, high-grade neoplasms (WHO grades 3 and 4) may also occur.114 Astrocytomas are slow-growing tumors that may present clinically with back pain, paresthesias, and spasticity. Subarachnoid dissemination may occur. Astrocytomas most often occur in the cervical and thoracic spinal cord and tend to be eccentrically located. Intramedullary astrocytomas affecting the entire cord (ie, holocord tumor) have also been reported (Fig 14).115
Fig 14.
Astrocytoma in an 11-year-old boy. A, Sagittal T2 MR image of the cervical and upper thoracic spine demonstrates a partly cystic and solid intramedullary spinal cord tumor. B, Sagittal T2 MR image of the thoracic spine demonstrates a partly cystic and solid intramedullary spinal cord tumor. C, Sagittal T1-weighted postcontrast MR image shows enhancement of the solid portions of the tumor and peripheral enhancement of the cystic components.
On conventional radiography, occasionally enlargement of the spinal canal or scoliosis is seen. CT may show expansion and remodeling of the bone.
MR imaging is the technique of choice for evaluating intramedullary spinal cord tumors, effectively demonstrating cord expansion that typically spans fewer than 4 vertebral levels. Tumors of this type appear hypointense to isointense on T1-weighted images and hyperintense on T2-weighted images (Fig 14A, -B). Cysts, necrosis, and occasionally hemorrhage may be present. Edema or a syrinx may be seen above and below the level of the lesion. Contrast enhancement is usually intense and can be homogeneous, heterogeneous, partial, or total (Fig 14C).72,102
Differential diagnoses of intramedullary lesions include ependymoma, ganglioglioma, and hemangioblastoma; autoimmune or inflammatory myelitis (acute transverse myelitis, multiple sclerosis, and infectious myelitis); and vascular diseases such as cord ischemia or infarction.
Ependymoma.
Ependymoma is uncommon in children except in association with neurofibromatosis type 2 and is usually a WHO grade 2 tumor. These tumors are slow-growing, presenting more often in adolescence with a slight male predilection. The origin of ependymomas is presumably from the ependymal cell remnants of the central canal. As a result, the extension of this tumor is circumferential and vertical along the central canal and centrally located in the cord, causing expansion of the gray matter.72,102 On conventional radiography and CT, there may be spinal canal widening, posterior vertebral body scalloping, widened interpediculate distance with thinning of the pedicles, and scoliosis (though uncommon).
On MR imaging, ependymomas are T1 hypointense or isointense and T2 hyperintense with well-circumscribed lesions and are characterized by expansion of the spinal cord. Hemorrhage and cysts can be present. In ≤20% of cases, deposits of hemosiderin may be seen in the cranial and caudal margins of the lesion, a so-called “cap sign.”116 Cord edema can also be present. Enhancement of the solid component is usually intense and well-delineated.
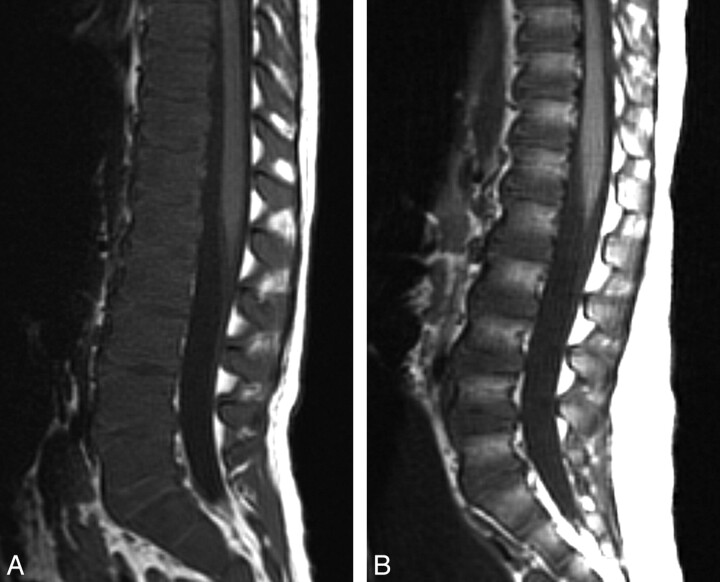
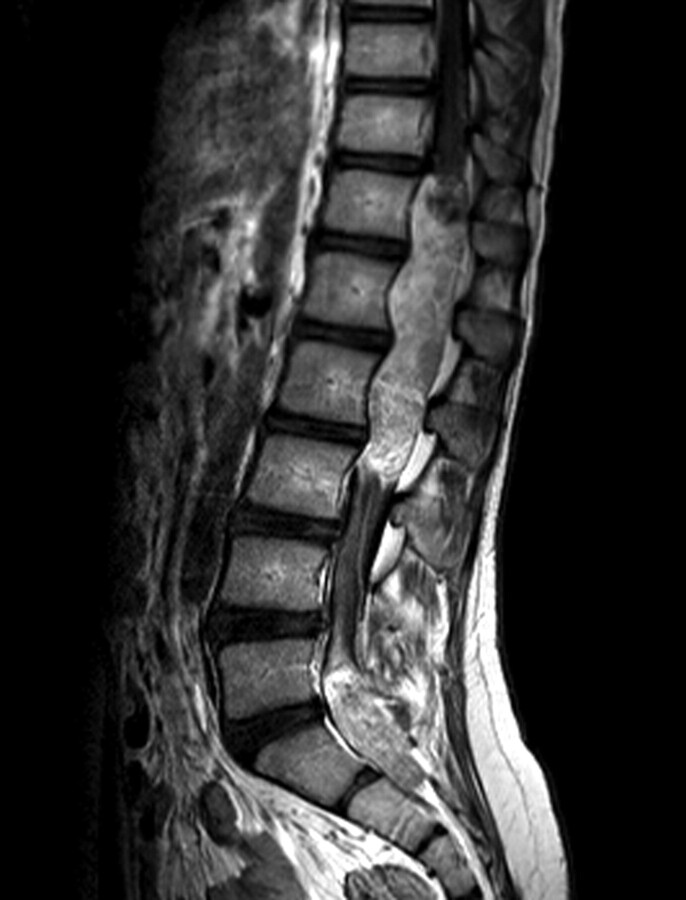
Myxopapillary ependymomas, a distinct variant of spinal ependymomas, are categorized as WHO grade 1 lesions and occur most commonly in the lumbosacral region. These tumors originate within the terminal filum or the conus medullaris, are rare in children, and account for 13% of all spinal ependymomas. Although myxopapillary ependymomas are considered benign, they tend to be more aggressive in children than in adults. The most common symptom in the series of Bagley et al was pain.117 Other symptoms include motor, sensory, urinary, and gait abnormalities. Tumor spread may occur via the subarachnoid space, invade locally, or rarely metastasize outside the central nervous system. MR imaging findings in myxopapillary ependymomas are nonspecific; however, certain features may suggest this type of tumor, including an intradural extramedullary thoracolumbar mass spanning several vertebral levels in the lumbar and sacral canal. These tumors tend to be T1 hypointense and T2 hyperintense and almost always enhance homogeneously after intravenous contrast administration (Fig 15).117
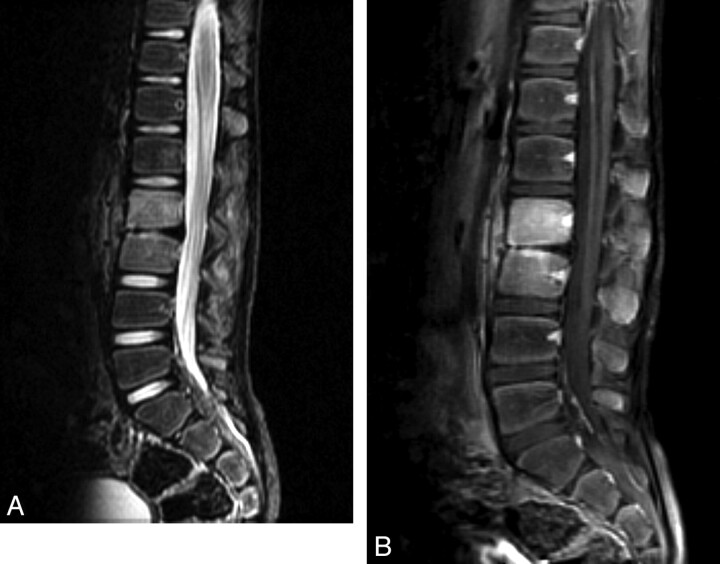
Fig 15.
Myxopapillary ependymoma in a 12-year-old boy. Sagittal T1-weighted postcontrast MR image demonstrates an intradural extramedullary mass lesion extending from the T12 to L3 levels and a second lesion at the L5–S2 level with diffuse enhancement. There is associated scalloping of the posterior aspects of the lumbar vertebral bodies.
Ganglioglioma.
Ganglioglioma is an intramedullary tumor that constitutes nearly 30% of intramedullary tumors in children younger than 3 years of age.75,110 In a series of 27 patients with gangliogliomas, Patel et al118 reported the average age as 12 years. Gangliogliomas are composed of a mixture of neoplastic mature neuronal elements (ganglion cells) and neoplastic glial elements.118 They are typically low-grade tumors (WHO grades 1 and 2), with a low rate of malignant transformation; however, they tend to recur locally. These tumors are located most commonly in the cervical and thoracic cord. Gangliogliomas tend to span an average of 8 vertebral segments, compared with an average of 4 vertebral bodies in astrocytomas and ependymomas. Holocord involvement has been described more frequently in gangliogliomas and is most likely related to the slow growth of this tumor.118
On imaging, gangliogliomas tend to be eccentrically located; 46% of these tumors harbor cysts. Calcification is the single most suggestive feature of gangliogliomas, which may be otherwise indistinguishable from astrocytomas and ependymomas.110,119 The solid portions of this tumor are isointense to hypointense on T1-weighted images and heterogeneous with areas of isointensity and hyperintensity on T2-weighted images. Contrast enhancement can be focal or patchy or occasionally absent. Perifocal edema can vary from absent or limited118 to extensive.110
Because most of the intramedullary tumors are benign, Jallo et al72 offer a rationale for radical surgery, thus obviating radiation and chemotherapy in these patients. However, given that the prognosis for malignant intramedullary tumors is usually poor, surgery in these children should be limited to conservative debulking. In addition, surgery on these neoplasms can be safely performed by using modern surgical adjuncts such as the ultrasonic aspirator, contact laser, and neurophysiologic monitoring.72
Acknowledgments
We thank Nancy Drinan for her editorial assistance and Cynthia Dubé for her assistance with manuscript preparation.
Abbreviations
- ALARA
as low as reasonably achievable
- ESR
erythrocyte sedimentation rate
- FSE
fast spin-echo
- 18F
fluorine 18
- LCH
Langerhans cell histiocytosis
- LDH
lactate dehydrogenase
- MBP
mechanical back pain
- PET
positron-emission tomography
- RFA
radio-frequency ablation
- SPECT
single-photon emission computed tomography
- STIR
short tau inversion recovery
- 99mTc-MDP
technetium 99m methylene diphosphonate
- WHO
World Health Organization
References
- 1. Kelsey JL, White AA, 3rd. Epidemiology and impact of low-back pain. Spine 1980;5:133–42 [DOI] [PubMed] [Google Scholar]
- 2. Selbst SM, Lavelle JM, Soyupak SK, et al. Back pain in children who present to the emergency department. Clin Pediatr (Phila) 1999;38:401–06 [DOI] [PubMed] [Google Scholar]
- 3. Watson KD, Papageorgiou AC, Jones GT, et al. Low back pain in schoolchildren: the role of mechanical and psychosocial factors. Arch Dis Child 2003;88:12–17 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Sato T, Ito T, Hirano T, et al. Low back pain in childhood and adolescence: a cross-sectional study in Niigata City. Eur Spine J 2008;17:1441–47.Epub 2008 Oct 1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Szpalski M, Gunzburg R, Balague F, et al. A 2-year prospective longitudinal study on low back pain in primary school children. Eur Spine J 2002;11:459–64 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Salminen JJ, Pentti J, Terho P. Low back pain and disability in 14-year-old schoolchildren. Acta Paediatr 1992;81:1035–39 [DOI] [PubMed] [Google Scholar]
- 7. Kristjansdottir G. Prevalence of self-reported back pain in school children: a study of sociodemographic differences. Eur J Pediatr 1996;155:984–86 [DOI] [PubMed] [Google Scholar]
- 8. Jones MA, Stratton G, Reilly T, et al. A school-based survey of recurrent non-specific low-back pain prevalence and consequences in children. Health Educ Res 2004;19:284–89 [DOI] [PubMed] [Google Scholar]
- 9. Harreby M, Nygaard B, Jessen T, et al. Risk factors for low back pain in a cohort of 1389 Danish school children: an epidemiologic study. Eur Spine J 1999;8:444–50 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10. Fribourg D, Delgado E. Occult spinal cord abnormalities in children referred for orthopedic complaints. Am J Orthop 2004;33:18–25 [PubMed] [Google Scholar]
- 11. Feldman DS, Straight JJ, Badra MI, et al. Evaluation of an algorithmic approach to pediatric back pain. J Pediatr Orthop 2006;26:353–57 [DOI] [PubMed] [Google Scholar]
- 12. Burton AK, Clarke RD, McClune TD, et al. The natural history of low back pain in adolescents. Spine 1996;21:2323–28 [DOI] [PubMed] [Google Scholar]
- 13. Leboeuf-Yde C, Kyvik KO. At what age does low back pain become a common problem? A study of 29,424 individuals aged 12–41 years. Spine 1998;23:228–34 [DOI] [PubMed] [Google Scholar]
- 14. Watson KD, Papageorgiou AC, Jones GT, et al. Low back pain in schoolchildren: occurrence and characteristics. Pain 2002;97:87–92 [DOI] [PubMed] [Google Scholar]
- 15. Davis PJ, Williams HJ. The investigation and management of back pain in children. Arch Dis Child Educ Pract Ed 2008;93:73–83 [DOI] [PubMed] [Google Scholar]
- 16. Jones GT, Macfarlane GJ. Epidemiology of low back pain in children and adolescents. Arch Dis Child 2005;90:312–16 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Bhatia NN, Chow G, Timon SJ, et al. Diagnostic modalities for the evaluation of pediatric back pain: a prospective study. J Pediatr Orthop 2008;28:230–33 [DOI] [PubMed] [Google Scholar]
- 18. Bernstein RM, Cozen H. Evaluation of back pain in children and adolescents. Am Fam Physician 2007;76:1669–76 [PubMed] [Google Scholar]
- 19. Auerbach JD, Ahn J, Zgonis MH, et al. Streamlining the evaluation of low back pain in children. Clin Orthop Relat Res 2008;466:1971–77 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Masiero S, Carraro E, Celia A, et al. Prevalence of nonspecific low back pain in schoolchildren aged between 13 and 15 years. Acta Paediatr 2008;97:212–16 [DOI] [PubMed] [Google Scholar]
- 21. Mirovsky Y, Jakim I, Halperin N, et al. Non-specific back pain in children and adolescents: a prospective study until maturity. J Pediatr Orthop B 2002;11:275–78 [DOI] [PubMed] [Google Scholar]
- 22. Kim HJ, Green DW. Adolescent back pain. Curr Opin Pediatr 2008;20:37–45 [DOI] [PubMed] [Google Scholar]
- 23. Curtis C, d'Hemecourt P. Diagnosis and management of back pain in adolescents. Adolesc Med State Art Rev 2007;18:140–64,x [PubMed] [Google Scholar]
- 24. Micheli LJ, Curtis C. Stress fractures in the spine and sacrum. Clin Sports Med 2006;25:75–88,ix [DOI] [PubMed] [Google Scholar]
- 25. Combs JA, Caskey PM. Back pain in children and adolescents: a retrospective review of 648 patients. South Med J 1997;90:789–92 [DOI] [PubMed] [Google Scholar]
- 26. Korovessis P, Koureas G, Papazisis Z. Correlation between backpack weight and way of carrying, sagittal and frontal spinal curvatures, athletic activity, and dorsal and low back pain in schoolchildren and adolescents. J Spinal Disord Tech 2004;17:33–40 [DOI] [PubMed] [Google Scholar]
- 27. Rubinstein SM, van Tulder M. A best-evidence review of diagnostic procedures for neck and low-back pain. Best Pract Res Clin Rheumatol 2008;22:471–82 [DOI] [PubMed] [Google Scholar]
- 28. Nigrovic P. Evaluation of the child with back pain. In: Basow DS.ed. UpToDate. Waltham, Massachusetts, 2009 [Google Scholar]
- 29. Shah NB, Platt SL. ALARA: is there a cause for alarm? Reducing radiation risks from computed tomography scanning in children. Curr Opin Pediatr 2008;20:243–47 [DOI] [PubMed] [Google Scholar]
- 30. Goske MJ, Applegate KE, Boylan J, et al. The “Image Gently” campaign: increasing CT radiation dose awareness through a national education and awareness program. Pediatr Radiol 2008;38:265–69 [DOI] [PubMed] [Google Scholar]
- 31. Grant FD, Fahey FH, Packard AB, et al. Skeletal PET with 18F-fluoride: applying new technology to an old tracer. J Nucl Med 2008;49:68–78 [DOI] [PubMed] [Google Scholar]
- 32. Connolly LP, Drubach LA, Connolly SA, et al. Young athletes with low back pain: skeletal scintigraphy of conditions other than pars interarticularis stress. Clin Nucl Med 2004;29:689–93 [DOI] [PubMed] [Google Scholar]
- 33. Dunn AJ, Campbell RS, Mayor PE, et al. Radiological findings and healing patterns of incomplete stress fractures of the pars interarticularis. Skeletal Radiol 2008;37:443–50 [DOI] [PubMed] [Google Scholar]
- 34. Denis F. Spinal instability as defined by the three-column spine concept in acute spinal trauma. Clin Orthop Relat Res 1984:65–76 [PubMed] [Google Scholar]
- 35. Oestreich AE, Young LW, Poussaint TY. Scoliosis circa 2000: radiologic imaging perspective. II. Treatment and follow-up. Skeletal Radiol 1998;27:651–56 [DOI] [PubMed] [Google Scholar]
- 36. Beutler WJ, Fredrickson BE, Murtland A, et al. The natural history of spondylolysis and spondylolisthesis: 45-year follow-up evaluation. Spine 2003;28:1027–35,discussion 35 [DOI] [PubMed] [Google Scholar]
- 37. McTimoney CA, Micheli LJ. Current evaluation and management of spondylolysis and spondylolisthesis. Curr Sports Med Rep 2003;2:41–46 [DOI] [PubMed] [Google Scholar]
- 38. d'Hemecourt PA, Gerbino PG, 2nd, Micheli LJ. Back injuries in the young athlete. Clin Sports Med 2000;19:663–79 [DOI] [PubMed] [Google Scholar]
- 39. d'Hemecourt PA, Zurakowski D, Kriemler S, et al. Spondylolysis: returning the athlete to sports participation with brace treatment. Orthopedics 2002;25:653–57 [DOI] [PubMed] [Google Scholar]
- 40. Wang Z, Parent S, Mac-Thiong JM, et al. Influence of sacral morphology in developmental spondylolisthesis. Spine 2008; 33: 2185– 91 [DOI] [PubMed] [Google Scholar]
- 41. Sairyo K, Goel VK, Vadapalli S, et al. Biomechanical comparison of lumbar spine with or without spina bifida occulta: a finite element analysis. Spinal Cord 2006;44:440–44.Epub 2005 Nov 29 [DOI] [PubMed] [Google Scholar]
- 42. Lonstein JE. Spondylolisthesis in children: cause, natural history, and management. Spine 1999;24:2640–48 [DOI] [PubMed] [Google Scholar]
- 43. Campbell RS, Grainger AJ, Hide IG, et al. Juvenile spondylolysis: a comparative analysis of CT, SPECT, and MRI. Skeletal Radiol 2005;34:63–73 [DOI] [PubMed] [Google Scholar]
- 44. Saifuddin A, Burnett SJ. The value of lumbar spine MRI in the assessment of the pars interarticularis. Clin Radiol 1997;52:666–71 [DOI] [PubMed] [Google Scholar]
- 45. Ralston S, Weir M. Suspecting lumbar spondylolysis in adolescent low back pain. Clin Pediatr (Phila) 1998;37:287–93 [DOI] [PubMed] [Google Scholar]
- 46. Erkintalo MO, Salminen JJ, Alanen AM, et al. Development of degenerative changes in the lumbar intervertebral disk: results of a prospective MR imaging study in adolescents with and without low-back pain. Radiology 1995;196:529–33 [DOI] [PubMed] [Google Scholar]
- 47. Barkovich AJ. Pediatric Neuroimaging. Philadelphia: Lippincott Williams & Wilkins; 2005:279 [Google Scholar]
- 48. Chang CH, Lee ZL, Chen WJ, et al. Clinical significance of ring apophysis fracture in adolescent lumbar disc herniation. Spine 2008; 33: 1750– 54 [DOI] [PubMed] [Google Scholar]
- 49. Peh WC, Griffith JF, Yip DK, et al. Magnetic resonance imaging of lumbar vertebral apophyseal ring fractures. Australas Radiol 1998;42:34–37 [DOI] [PubMed] [Google Scholar]
- 50. Yen CH, Chan SK, Ho YF, et al. Posterior lumbar apophyseal ring fractures in adolescents: a report of four cases. J Orthop Surg (Hong Kong) 2009;17:85–89 [DOI] [PubMed] [Google Scholar]
- 51. Beluffi G, Fiori P, Sileo C. Intervertebral disc calcifications in children. Radiol Med 2009;114:331–41 [DOI] [PubMed] [Google Scholar]
- 52. Dai LY, Ye H, Qian QR. The natural history of cervical disc calcification in children. J Bone Joint Surg Am 2004;86-A:1467–72 [DOI] [PubMed] [Google Scholar]
- 53. Lernout C, Haas H, Rubio A, et al. Pediatric intervertebral disk calcification in childhood: three case reports and review of literature. Childs Nerv Syst 2009;25:1019–23.Epub 2009 May 8 [DOI] [PubMed] [Google Scholar]
- 54. Jawish R, Ponet M. Dysphagia disclosing a cervical disk calcification in a child: apropos of a case and review of the literature [in French]. Chir Pediatr 1990;31:127–30 [PubMed] [Google Scholar]
- 55. Ventura N, Huguet R, Salvador A, et al. Intervertebral disc calcification in childhood. Int Orthop 1995;19:291–94 [DOI] [PubMed] [Google Scholar]
- 56. Girodias JB, Azouz EM, Marton D. Intervertebral disk space calcification: a report of 51 children with a review of the literature. Pediatr Radiol 1991;21:541–46 [DOI] [PubMed] [Google Scholar]
- 57. Gerlach R, Zimmermann M, Kellermann S, et al. Intervertebral disc calcification in childhood: a case report and review of the literature. Acta Neurochir (Wien) 2001;143:89–93 [DOI] [PubMed] [Google Scholar]
- 58. Marin C, Sanchez-Alegre ML, Gallego C, et al. Magnetic resonance imaging of osteoarticular infections in children. Curr Probl Diagn Radiol 2004;33:43–59 [DOI] [PubMed] [Google Scholar]
- 59. Mahboubi S, Morris MC. Imaging of spinal infections in children. Radiol Clin North Am 2001;39:215–22 [DOI] [PubMed] [Google Scholar]
- 60. Fernandez M, Carrol CL, Baker CJ. Discitis and vertebral osteomyelitis in children: an 18-year review. Pediatrics 2000;105:1299–304 [DOI] [PubMed] [Google Scholar]
- 61. Wenger DR, Bobechko WP, Gilday DL. The spectrum of intervertebral disc-space infection in children. J Bone Joint Surg Am 1978;60:100–08 [PubMed] [Google Scholar]
- 62. Early SD, Kay RM, Tolo VT. Childhood diskitis. J Am Acad Orthop Surg 2003;11:413–20 [DOI] [PubMed] [Google Scholar]
- 63. Offiah AC. Acute osteomyelitis, septic arthritis and discitis: differences between neonates and older children. Eur J Radiol 2006;60:221–32 [DOI] [PubMed] [Google Scholar]
- 64. James SL, Davies AM. Imaging of infectious spinal disorders in children and adults. Eur J Radiol 2006;58:27–40 [DOI] [PubMed] [Google Scholar]
- 65. Herman TE, Siegel MJ. Thoracic discitis. Clin Pediatr (Phila) 2009;48:120–23 [DOI] [PubMed] [Google Scholar]
- 66. du Lac P, Panuel M, Devred P, et al. MRI of disc space infection in infants and children: report of 12 cases. Pediatr Radiol 1990;20:175–78 [DOI] [PubMed] [Google Scholar]
- 67. Correa AG, Edwards MS, Baker CJ. Vertebral osteomyelitis in children. Pediatr Infect Dis J 1993;12:228–33 [DOI] [PubMed] [Google Scholar]
- 68. Spiegel PG, Kengla KW, Isaacson AS, et al. Intervertebral disc-space inflammation in children. J Bone Joint Surg Am 1972;54:284–96 [PubMed] [Google Scholar]
- 69. Andronikou S, Jadwat S, Douis H. Patterns of disease on MRI in 53 children with tuberculous spondylitis and the role of gadolinium. Pediatr Radiol 2002;32:798–805 [DOI] [PubMed] [Google Scholar]
- 70. Fenoy AJ, Greenlee JD, Menezes AH, et al. Primary bone tumors of the spine in children. J Neurosurg 2006;105:252–60 [DOI] [PubMed] [Google Scholar]
- 71. Dormans JP, Moroz L. Infection and tumors of the spine in children. J Bone Joint Surg Am 2007;89Suppl 1:79–97 [DOI] [PubMed] [Google Scholar]
- 72. Jallo GI, Freed D, Epstein F. Intramedullary spinal cord tumors in children. Childs Nerv Syst 2003;19:641–49 [DOI] [PubMed] [Google Scholar]
- 73. Schellinger KA, Propp JM, Villano JL, et al. Descriptive epidemiology of primary spinal cord tumors. J Neurooncol 2008;87:173–79 [DOI] [PubMed] [Google Scholar]
- 74. Houten JK, Weiner HL. Pediatric intramedullary spinal cord tumors: special considerations. J Neurooncol 2000;47:225–30 [DOI] [PubMed] [Google Scholar]
- 75. Constantini S, Houten J, Miller DC, et al. Intramedullary spinal cord tumors in children under the age of 3 years. J Neurosurg 1996;85:1036–43 [DOI] [PubMed] [Google Scholar]
- 76. Berger M.ed. Pediatric Neuro-Oncology. Philadelphia: Saunders; 1992 [Google Scholar]
- 77. Rosemberg S, Fujiwara D. Epidemiology of pediatric tumors of the nervous system according to the WHO 2000 classification: a report of 1,195 cases from a single institution. Childs Nerv Syst 2005; 21: 940– 44 [DOI] [PubMed] [Google Scholar]
- 78. Schick U, Marquardt G. Pediatric spinal tumors. Pediatr Neurosurg 2001;35:120–27 [DOI] [PubMed] [Google Scholar]
- 79. Barkovich AJ. Pediatric Neuroradiology. Philadelphia: Lippincott Williams & Wilkins; 2005:774 [Google Scholar]
- 80. Jaffe H. “Osteoid-osteoma”: a benign osteoblastic tumor composed of osteoid and atypical bone. Arch Surg 1935; 31: 709– 28 [Google Scholar]
- 81. Azouz EM, Kozlowski K, Marton D, et al. Osteoid osteoma and osteoblastoma of the spine in children: report of 22 cases with brief literature review. Pediatr Radiol 1986;16:25–31 [DOI] [PubMed] [Google Scholar]
- 82. Saifuddin A, White J, Sherazi Z, et al. Osteoid osteoma and osteoblastoma of the spine: factors associated with the presence of scoliosis. Spine 1998;23:47–53 [DOI] [PubMed] [Google Scholar]
- 83. Jackson RP, Reckling FW, Mants FA. Osteoid osteoma and osteoblastoma: similar histologic lesions with different natural histories. Clin Orthop Relat Res 1977:303–13 [PubMed] [Google Scholar]
- 84. Yamamoto K, Asazuma T, Tsuchihara T, et al. Diagnostic efficacy of thin slice CT in osteoid osteoma of the thoracic spine: report of two cases. J Spinal Disord Tech 2005;18:182–84 [DOI] [PubMed] [Google Scholar]
- 85. Ransford AO, Pozo JL, Hutton PA, et al. The behaviour pattern of the scoliosis associated with osteoid osteoma or osteoblastoma of the spine. J Bone Joint Surg Br 1984;66:16–20 [DOI] [PubMed] [Google Scholar]
- 86. Harish S, Saifuddin A. Imaging features of spinal osteoid osteoma with emphasis on MRI findings. Eur Radiol 2005;15:2396–403 [DOI] [PubMed] [Google Scholar]
- 87. Liu PT, Chivers FS, Roberts CC, et al. Imaging of osteoid osteoma with dynamic gadolinium-enhanced MR imaging. Radiology 2003;227:691–700 [DOI] [PubMed] [Google Scholar]
- 88. Zampa V, Bargellini I, Ortori S, et al. Osteoid osteoma in atypical locations: the added value of dynamic gadolinium-enhanced MR imaging. Eur J Radiol 2009;71:527–35 [DOI] [PubMed] [Google Scholar]
- 89. Hoffmann RT, Jakobs TF, Kubisch CH, et al. Radiofrequency ablation in the treatment of osteoid osteoma: 5-year experience. Eur J Radiol 2010;73:374–79Epub 2009 Jan 13 [DOI] [PubMed] [Google Scholar]
- 90. Vanderschueren GM, Obermann WR, Dijkstra SP, et al. Radiofrequency ablation of spinal osteoid osteoma: clinical outcome. Spine 2009;34:901–04 [DOI] [PubMed] [Google Scholar]
- 91. Hempfing A, Hoffend J, Bitsch RG, et al. The indication for gamma probe-guided surgery of spinal osteoid osteomas. Eur Spine J 2007;16:1668–72 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92. Zileli M, Cagli S, Basdemir G, et al. Osteoid osteomas and osteoblastomas of the spine. Neurosurg Focus 2003; 15:E5. [PubMed] [Google Scholar]
- 93. Jee WH, Park YK, McCauley TR, et al. Chondroblastoma: MR characteristics with pathologic correlation. J Comput Assist Tomogr 1999;23:721–26 [DOI] [PubMed] [Google Scholar]
- 94. Emmez H, Kaymaz M, Tokgoz N, et al. Progression of a lumbar spinal osteoblastoma. Neurol Med Chir (Tokyo) 2005;45:379–83 [DOI] [PubMed] [Google Scholar]
- 95. Lichtenstein L. Histiocytosis X: integration of eosinophilic granuloma of bone, Letterer-Siwe disease, and Schuller-Christian disease as related manifestations of a single nosologic entity. AMA Arch Pathol 1953;56:84–102 [PubMed] [Google Scholar]
- 96. Brown CW, Jarvis JG, Letts M, et al. Treatment and outcome of vertebral Langerhans cell histiocytosis at the Children's Hospital of Eastern Ontario. Can J Surg 2005;48:230–36 [PMC free article] [PubMed] [Google Scholar]
- 97. Bavbek M, Atalay B, Altinors N, et al. Spontaneous resolution of lumbar vertebral eosinophilic granuloma. Acta Neurochir (Wien) 2004;146:165–67 [DOI] [PubMed] [Google Scholar]
- 98. Ilaslan H, Sundaram M, Unni KK, et al. Primary Ewing's sarcoma of the vertebral column. Skeletal Radiol 2004;33:506–13 [DOI] [PubMed] [Google Scholar]
- 99. Hsieh CT, Chiang YH, Tsai WC, et al. Primary spinal epidural Ewing sarcoma: a case report and review of the literature. Turk J Pediatr 2008;50:282–86 [PubMed] [Google Scholar]
- 100. Marco RA, Gentry JB, Rhines LD, et al. Ewing's sarcoma of the mobile spine. Spine 2005;30:769–73 [DOI] [PubMed] [Google Scholar]
- 101. Vezina G. Spine. In: Barkovich AJ. ed. Diagnostic Imaging: Pediatric Neuroradiology. Salt Lake City: Amirsys;2007:90– 92 [Google Scholar]
- 102. Binning M, Klimo P, Jr, Gluf W, et al. Spinal tumors in children. Neurosurg Clin N Am 2007;18:631–58 [DOI] [PubMed] [Google Scholar]
- 103. Chahal S, Lagera JE, Ryder J, et al. Hematological neoplasms with first presentation as spinal cord compression syndromes: a 10-year retrospective series and review of the literature. Clin Neuropathol 2003;22:282–90 [PubMed] [Google Scholar]
- 104. Mora J, Wollner N. Primary epidural non-Hodgkin lymphoma: spinal cord compression syndrome as the initial form of presentation in childhood non-Hodgkin lymphoma. Med Pediatr Oncol 1999;32:102–05 [DOI] [PubMed] [Google Scholar]
- 105. Raco A, Cervoni L, Salvati M, et al. Primary spinal epidural non-Hodgkin's lymphomas in childhood: a review of 6 cases. Acta Neurochir (Wien) 1997;139:526–28 [DOI] [PubMed] [Google Scholar]
- 106. Mostafavi H, Lennarson PJ, Traynelis VC. Granulocytic sarcoma of the spine. Neurosurgery 2000;46:78–83;discussion 84 [PubMed] [Google Scholar]
- 107. Meltzer JA, Jubinsky PT. Acute myeloid leukemia presenting as spinal cord compression. Pediatr Emerg Care 2005;21:670–72 [DOI] [PubMed] [Google Scholar]
- 108. Takeda M, Yamaguchi S, Eguchi K, et al. Spinal epidural granulocytic sarcoma in a child precedent to clinical manifestation of acute myeloid lymphoma: case report. Neurol Med Chir (Tokyo) 2009;49:221–24 [DOI] [PubMed] [Google Scholar]
- 109. Shiozawa Y, Kiyokawa N, Saito M, et al. Granulocytic sarcoma of the spine in a child without bone marrow involvement: a case report and literature review. Eur J Pediatr 2005;164:616–20 [DOI] [PubMed] [Google Scholar]
- 110. Rossi A, Gandolfo C, Morana G, et al. Tumors of the spine in children. Neuroimaging Clin N Am 2007;17:17–35 [DOI] [PubMed] [Google Scholar]
- 111. Sze G, Baierl P, Bravo S. Evolution of the infant spinal column: evaluation with MR imaging. Radiology 1991;181:819–27 [DOI] [PubMed] [Google Scholar]
- 112. Bertuna G, Fama P, Lo Nigro L, et al. Marked osteoporosis and spontaneous vertebral fractures in children: don't forget, it could be leukemia. Med Pediatr Oncol 2003;41:450–51 [DOI] [PubMed] [Google Scholar]
- 113. Goldbloom EB, Cummings EA, Yhap M. Osteoporosis at presentation of childhood ALL: management with pamidronate. Pediatr Hematol Oncol 2005;22:543–50 [DOI] [PubMed] [Google Scholar]
- 114. Wilson PE, Oleszek JL, Clayton GH. Pediatric spinal cord tumors and masses. J Spinal Cord Med 2007;30(suppl 1):S15–20 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115. Schittenhelm J, Ebner FH, Tatagiba M, et al. Holocord pilocytic astrocytoma: case report and review of the literature. Clin Neurol Neurosurg 2009;111:203–07 [DOI] [PubMed] [Google Scholar]
- 116. Nemoto Y, Inoue Y, Tashiro T, et al. Intramedullary spinal cord tumors: significance of associated hemorrhage at MR imaging. Radiology 1992;182:7939–46 [DOI] [PubMed] [Google Scholar]
- 117. Bagley CA, Kothbauer KF, Wilson S, et al. Resection of myxopapillary ependymomas in children. J Neurosurg 2007;106:261–67 [DOI] [PubMed] [Google Scholar]
- 118. Patel U, Pinto RS, Miller DC, et al. MR of spinal cord ganglioglioma. AJNR Am J Neuroradiol 1998;19:879–87 [PMC free article] [PubMed] [Google Scholar]
- 119. Miller DC, Lang FF, Epstein FJ. Central nervous system gangliogliomas. Part 1. Pathology. J Neurosurg 1993;79:859–66 [DOI] [PubMed] [Google Scholar]