Abstract
This chapter explores ways to reduce the risk of severe acute respiratory syndrome coronavirus-2 transmission to women and staff within gynaecology outpatient clinics. The likely routes of transmission are discussed, namely through droplets, aerosols and fomites. Using the ‘hierarchy of control’ categories, elimination, substitution, engineering, administration and personal protective equipment, practical strategies for modifying virus exposure are presented. The management of specific clinical conditions are reviewed based on advice prepared by the specialist societies in conjunction with each other and the Royal College of Obstetricians and Gynaecologists. The need to maintain at least a minimal level of gynaecological services is recognised and that this should provide safe, equitable and effective care. Ways to reduce clinic attendance are discussed with the substitution of face-to-face with remote consultations and when this is relevant. Current recommendations for ambulatory procedures, which include colposcopy and hysteroscopy, are considered so that best use is made of reduced resources.
Keywords: Hierarchy of control, Personal protective equipment, Triaging referrals, Remote consultation, Gynaecological services
Routes of virus transmission
The past months have seen the arrival of a wealth of new evidence in relation to transmission of severe acute respiratory syndrome coronavirus-2 (SARS-CoV-2) and coronavirus disease-2019 (COVID-19). During this period, many hospitals in the UK have postponed all non-urgent care to ensure that resources are made available to aid with the pandemic. However, this strategy is not feasible in the long term and services need to resume as much as possible, whilst the safety of patients and staff is ensured.
To minimise risk, virus transmission modes must be understood. A recent meta-analysis found that peak viral load levels are within the first 5 days of symptom development [1], which indicates that the height of infectiousness could be prior to clinical detection. Furthermore, those who are asymptomatic or with minimal symptoms may still have large viral loads [1]. All areas should therefore be treated as ‘COVID-19 minimised’ as opposed to ‘COVID-19 free’. Given the risk of asymptomatic patients carrying high viral loads of SARS-CoV-2, women attending gynaecology clinics should be treated as suspected carriers to minimise transmission risk.
The primary mode of SARS-CoV-2 transmission, whether through respiratory droplets or aerosols, is debated. Experimental data show that SARS-CoV-2 could be transmitted through aerosols and that both droplets and aerosols are generated during speech, sneezing and coughing with a span of approximately 7–8 m [2]. Although SARS-CoV-2-positive air samples do not equate to viable virus and higher infection risk, the evidence in support of airborne transmission is on the rise, and this route should be considered in infection prevention strategies [3].
SARS-CoV-2 within droplets was found to remain viable for 72 h on plastic and stainless steel and 84 h on glass [3], indicating the plausibility of fomite spread.
Respiratory droplets appear to carry the highest risk of SARS-CoV-2 transmission, with other methods of transmission such as through aerosols or fomites being plausible but of unclear certainty. Transmission is more strongly associated with indoor spaces and prolonged close contact [4]. Preventing the spread of the virus should involve minimising risk through all potential transmission routes.
Hierarchy of control
Having established potential transmission routes of SARS-CoV-2, it is useful to consider how patients present to the gynaecology clinic and by following patient pathways identify ways of mitigating the risk of virus transfer. The ‘hierarchy of control’ provides a structured approach and in decreasing order of effectiveness consists of elimination, substitution, engineering, administration and personal protective equipment (PPE) [4].
Elimination
‘Elimination’ is regarded as the priority here and consists of the limitation of interactions between patients with each other and hospital staff to reduce nosocomial infection. Such actions include avoiding face-to-face encounters, fewer people attending at any one time when attendance is unavoidable and minimising the duration of interactions.
Triage of GP referrals to gynaecology into locally agreed categories allows the number of patients offered a face-to-face appointment to be reduced and controlled [5]. When insufficient information is available, a telephone consultation is likely to be useful and with the benefit of discussing direct with the patient possible investigations and treatment options [6].
Targeting patients with suspected gynaecological cancer symptoms is important to ensure that otherwise treatable cancers are not ignored, whilst ensuring vulnerable patients are not inappropriately exposed to infection. However, ‘two-week wait’ referral services should be maintained even if reduced [7].
Though some benign gynaecological conditions may require urgent attention, the treatment of others may be safely deferred; clear pathways for assessment should be established [8].
Substitution
Patients with a gynaecological condition who are not seen face-to-face still require care and attention. The Royal College of Obstetricians and Gynaecologists (RCOG) advise ensuring that a minimal level of service is available providing ‘safe, equitable, effective and quality care for all women’ [5]. Telephone consultations can substitute for many face-to-face encounters [5]. Such a service could rapidly commence and would be accessible to most patients. Family members may be involved by using speakerphone facilities; where understanding and speaking of English is a factor, online interpreting services can be integrated into the consultation.
Video consultations may aid in building rapport. Although randomised studies are small, the current evidence suggests that they are an effective consultation method with patients and staff reporting high satisfaction levels [9]. However, they are more complicated to set up, involve training and require the patient to have access to appropriate technology, which introduces a problem for some. Gynaecological services that favour remote consultations include fertility services and menopause clinics [10,11].
Engineering
The Japanese government adopted avoidance of the ‘three Cs: closed spaces with poor ventilation, crowded places with many people nearby and close-contact settings such as close-range conversations’ [12]. Adequate ventilation can reduce indoor infections by the dilution of SARS-CoV-2 aerosol particles [13]. Simple measures, such as opening windows, and encouraging natural ventilation, reduce transmission of other aerosol-transmitted diseases, including tuberculosis [14]. However, caution is necessary in gynaecology outpatients to balance the risks of infection prevention with thermal discomfort or potential loss of privacy.
Administration
To reduce the risk of fomite transmission, surfaces, particularly those that are touched frequently, should be cleaned thoroughly and for 1 min with 70%–90% ethanol, 0.5% hydrogen peroxide or 0.1% sodium hypochlorite [15,16]. Single-use cleaning equipment should be used where possible [17] and the ‘one wipe, one surface, one direction, dispose’ policy adopted when wiping surfaces to prevent recontamination [18].
Although there is insufficient evidence to support the frequency of cleaning different surfaces, interim guidance suggests at least twice daily for waiting areas, three times daily for shared toilets and after each patient visit for consultation rooms. A good overall standard of cleanliness is required, even in areas not frequently used [16]. Care should be taken to avoid splashes [17].
Ample provision of hand sanitiser for both staff and patient use is recommended. Alcohol-based hand rub with a minimum of 60% ethanol was found to inactivate viruses and should be applied for 20–30 s using a seven-step technique [19,20]. Soap and water are another option for staff, with 15 s of handwashing leading to a 90% reduction of bacterial contamination and 30 s leading to 99% [21]. Following this, complete hand drying is essential to ensure there is no persistence of the virus. Paper towels surpass electric hand dryers in terms of hygiene and friction dislodges microorganisms from the hands [22].
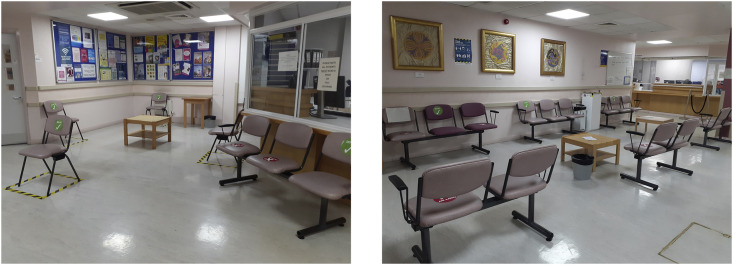
Physical distancing is enabled with fewer people in the department with protection against contraction of SARS-CoV-2 roughly doubling for every additional metre of distance maintained, with 2 m the recommended minimum distance [23]. This applies to all shared spaces, including waiting areas and break rooms. Patients should be advised to arrive on time for the scheduled appointment and not earlier; staggering appointments avoids several patients checking in at the same time. Seating arrangements should enable physical distancing (see Fig. 1 ). Placing seats back-to-back stops patients directly facing each other; though intuitive, there is no study to support that this avoids transmission. Similarly, one-way systems, although often employed, are not supported by clear evidence and may not be feasible in healthcare settings [4].
Fig. 1.
Outpatient clinic arrangements illustrating adequate spacing between seats.
Personal protective equipment
Appropriate PPE has been a pillar in the fight against COVID-19 and has provided healthcare staff with a high level of protection but must comply with health and safety requirements outlined in the Regulation (EU) 2016/425 [24].
Facemasks and respirators
N95 respirator masks are designed to protect a person from the surrounding environment, whereas surgical masks protect the environment from a person. Respirators generally provide more efficient protection than surgical masks [25]. The standards for particulate respirators vary; disposable respirators must comply with EN 149:2001+A1:2009, whereas reusable respirators must comply with EN140:1998 and EN143:2000 [26].
There are disadvantages to N95 respirators; fit testing is a vital part of ensuring an adequate seal to provide effectiveness. Furthermore, respirators often require more adjustment because of discomfort, with these adjustments leading to contamination [27]. In outpatient settings, both surgical masks and N95 respirators provide equivalent protection [28]. Surgical masks are sufficient unless aerosol-generating procedures are performed or when encountering a known infectious person.
Patients attending the outpatient department are required to wear a face covering. Recent supply shortages resulted in the recommendation that surgical masks should be kept for healthcare professionals [29]. Homemade face coverings, typically made of cloth, vary in efficacy in preventing transmission, though any mask appears beneficial when compared with no mask at all [30].
Exemptions from mask wearing divide into physiological and psychological reasons. Physiological exemptions include those with pre-existing respiratory conditions; however, they are at a higher risk of developing severe COVID-19, and therefore, for those with respiratory illness, exemption from mask wearing is not recommended [31]. Psychological exemptions include those who are unable to tolerate or understand masks [32].
Other protection
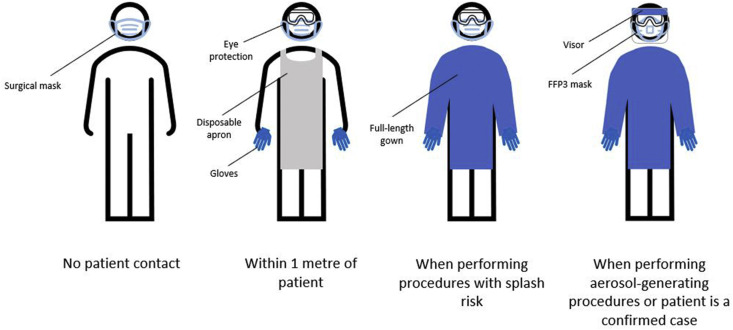
Gloves, gowns/aprons and eye protection also form vital components of effective PPE (see Fig. 2 ). A meta-analysis concerning the transmission of SARS coronavirus 1 and PPE use found significantly reduced odds ratios when wearing masks, gloves and gowns separately and combined [33].
Fig. 2.
Illustration of the PPE to be worn in various circumstances.
PPE requirements depend on whether the wearer will be within 1 m of patients. Staff without close patient contact need only wear a surgical mask. Staff with close patient contact should wear a surgical mask, eye protection, gloves and a disposable apron [34]; all gloves should comply with EN ISO 374-5:2016, gowns and disposable aprons must comply with EN 14126:2003 [26]. Long-sleeved gowns should be used when undertaking aerosol-generating procedures or ‘when there is a risk of extensive splashing of blood and/or other body fluids’, with an additional waterproof apron if the gown is not fluid-resistant [35]. A Cochrane review concluded with very low certainty that gowns may provide better protection than aprons [36]; however, this was only based on one study and further evidence is needed to guide recommendations.
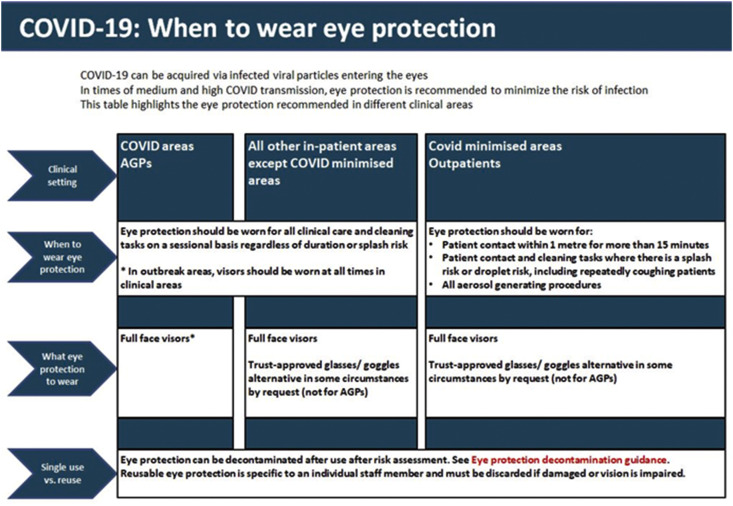
Eye protection includes safety glasses, goggles, face visors and panels that sit on top of facemasks and was found to reduce the transmission of coronaviruses in a meta-analysis [23]. Simulation studies have found that both visors and goggles protect against other viruses when compared with no eye protection; however, they were not directly compared (see Fig. 3 ) [36]. Prescription eyeglasses provided no additional protection in a simulation model and were comparable to no eye protection at all [37]; however, many goggles fit over prescription eyeglasses. Goggles or face visors are the preferred and recommended form of eye protection [28], but more research is required to determine their efficacy. Uncertainty exists around whether wearing both would be beneficial; at the present time, one form of eye protection is felt to be sufficient. The standard EN 166:2001 concerns all eye protection, which must comply with this standard prior to use in healthcare settings [26].
Fig. 3.
Recommendations for eye protection to be worn during the COVID-19 pandemic.
Gloves and gowns should be changed between patients. Facemasks worn to prevent the spread of one's own respiratory secretions (for example from talking or coughing) can be reused until soiled, damaged or hard to breathe through, but when used for protection from others' splashes and respiratory secretions should be changed between patients [38]. Eye protection may be cleaned with soap and water followed by disinfection with either sodium hypochlorite 0.1% or 70% alcohol wipes between uses [39].
Access to all required PPE should be provided in clinical settings. Training in donning and doffing minimises inadvertent contamination and should be provided. Double gloving may reduce contamination risks during this process but the benefits are unclear, and the certainty of evidence very low [36]; again, further research is required to guide recommendations.
Specific clinical conditions
Introduction
Some gynaecological conditions can seriously damage health if treatment is deferred, with cancers an obvious example. However, even benign conditions can significantly harm health; therefore, a minimal level of service is required at all times [5].
When referral for gynaecological services is considered, it is recommended that patient assessment through remote consultation is initially undertaken, with appropriate medical advice offered to minimise the need for women to visit their healthcare providers and reduce the risk of person-to-person viral transmission.
Patients should be informed that for any face-to-face attendance, they should wear a face covering unless exempt, and they should defer the appointment if they have suspected or confirmed COVID-19 infection and self-isolate until no longer infectious.
Principles for the management of women with gynaecological disorders during the COVID-19 pandemic have been provided (see Box 1 ) [5]. Taking these into account, the management of specific gynaecological disorders will be considered.
Box 1. Guidance for the provision of gynaecology services during the COVID-19 pandemic [5].
For delivery of safe, equitable, effective and quality gynaecological care, the minimum level of service requires:
-
•
Evidence-based, equitable, safe, compassionate and respectful care wherever, whenever and however it takes place
-
•
Clear pathways for accessible patient advice and help
-
•
Protection of women from nosocomial infection, particularly those potentially vulnerable to severe effects of COVID-19
-
•
Continued gynaecology care with minimal disruption for those at high risk
-
•
Maintaining essential and urgent cancer treatments [40].
-
•
Protection and support of all staff with adherence to national guidance on infection prevention and control
Alt-text: Box 1
Ambulatory procedures
Concerns about performing ambulatory procedures in the outpatient clinic primarily focus on possible spread of the SARS-CoV-2 virus as a consequence of aerosol production or contamination by infected bodily fluids or smoke. Viral RNA has been identified in the lower genital tract, urine, faeces and blood, but with low prevalence; consequently, the risk of virus dissemination from these body fluids appears to be minimal [41]. Therefore, gynaecological procedures should not pose a risk to healthcare workers.
In view of the prevalence of asymptomatic carriers of SARS-CoV-2, the duration of many ambulatory procedures beyond 15 min and the close proximity to the patient, as well as staff to each other, PPE worn by staff should include eye protection (goggles or visor), in addition to facemask, gloves and gown [34]. Consideration should be given to patients who become distressed during a procedure by allowing them to temporarily remove their face covering. When obtaining written consent, consider the pen used by a patient (see Box 2 ).
Box 2. When confirming patient consent:
-
•
Ask them to use their own pen
-
•
Otherwise, wipe the pen before and after use with antiviral solution
Alt-text: Box 2
Gynaecological cancers
General principles
A framework for the management of the diagnosis and treatment of women with a gynaecological cancer has been provided (see Box 3 ) [6]. It acknowledges the compromise of cancer service facilities due to staff sickness and reduced treatment options to protect patients from nosocomial infection. The varied impact of the COVID-19 pandemic across the UK means that decisions about services will need to be made locally by gynaeoncology multidisciplinary teams [6].
Box 3. General principles for the management of gynaecological cancer during the Covid-19 pandemic [6].
-
•
Prioritise treatment for those most in need
-
•
Make decisions within gynaecological MDT frameworks and communicate clearly with patients
-
•
Deviations from normal standards of care may be appropriate, which depend upon what is safely deliverable
-
•
Document MDT-directed changes
-
•
Continue to track patients with cancer diagnosis
-
•
Minimise hospital face-to-face visits, consider remote communication for follow-up and/or patient-initiated consultations
Alt-text: Box 3
Most women (>90%) referred to gynaecology fast track services do not have cancer despite having a ‘red-flag’ symptom or suspicious lesion [42]. Principles for safe and effective triaging of suspected cancer referrals is provided to ensure that priority is given to urgent referrals, with a safety net provided for downgraded referrals or when the standard investigations are deferred or not performed (see Box 4 ) [43]. This should reduce clinic attendance and allow appropriate physical distancing between patients, particularly within waiting areas. Streaming patients directly to a test may also minimise interactions and appointments within health services [6].
Box 4. Safe and effective triaging of cancer referrals [43].
-
•
Continue to not downgrade referrals without consulting the referring health professional
-
•
Prioritise particularly urgent referrals and introduce greater communication between primary and secondary care
-
•
For downgraded or avoided referrals, ensure safety-netting in case of patient deterioration or increased cancer risk
Alt-text: Box 4
Support from primary care is required to ensure the appropriateness of the referral. When the clinical need is unclear, initial remote contact with patients may establish whether investigation can be safely deferred or that a visit to the clinic is actually appropriate. Assessment of patients' vulnerability, particularly for those who are shielding, enables balancing the risk of patients acquiring a nosocomial infection versus delay in the diagnosis and treatment of a gynaecological cancer [44].
It remains important to see a patient in person when breaking bad news [6]. The support of a gynaeoncological clinical nurse specialist is pertinent, particularly when seeing a patient on their own, as this will help enable transparent communication and if necessary, signposting to appropriate services. A family member or friend included on the speakerphone may help mitigate their absence.
Abnormal uterine bleeding and cancer
Postmenopausal bleeding
New guidance for the investigation of postmenopausal bleeding (PMB) has been published (see Box 5 ) [44]. Deferring investigation may be considered for women with few risk factors for endometrial cancer and with probable residual ovarian activity: age <55 years [44], body mass index (BMI) < 35, <2 years since the menopause and period-like blood loss. Such patients should be advised to report persistent or heavier bleeding.
Box 5. Investigation of postmenopausal bleeding (PMB) during the COVID-19 pandemic [44].
-
•
Minimise hospital attendances, offer relevant procedures at a single visit
-
•
A normal cervix on speculum examination and negative cervical smear excludes cervical cancer
-
•
First-line test - TVS measurement of endometrial thickness (ET)
-
•
Where ET <4 mm on TVS, women can be discharged because endometrial cancer risk is low
-
•
Where ET >4 mm perform endometrial biopsy alone, particularly if limited access to hysteroscopy
-
•
Allocate experienced hysteroscopists to minimise need for further investigation
-
•
Consider “insufficient sample” on endometrial biopsy as normal, provided biopsy device insertion >6 cm into cavity and consistent with TVS. Women should seek advice if bleeding recurs
-
•
Consider hysteroscopy for failed or non-diagnostic endometrial biopsy for directed biopsy or endometrial polypectomy
-
•
Offer choice of anaesthesia and treatment settings for hysteroscopy: advise minimised risk of exposure to SARS-CoV-2 as outpatient; if inpatient, consider conscious sedation or regional anaesthesia, rather than GA, to prevent aerosol generation
-
•
Consider LNG-IUS insertion at the time of endometrial biopsy or hysteroscopy when there is a high risk of endometrial hyperplasia or cancer
Alt-text: Box 5
Irregular bleeding on hormone replacement therapy
Unscheduled bleeding whilst taking hormone replacement therapy (HRT) is no longer listed as a suspected gynaecological cancer symptom [7]. The risk of endometrial cancer is lower in women on combined HRT than for women with PMB not taking HRT [45]. However, the symptom is often troublesome and causes anxiety and concern. The problem in the UK was compounded by the limited availability of certain HRT preparations [11], with consequent modifications to therapy, which resulted in new irregular vaginal bleeding. Nevertheless, women should be advised to seek advice if the blood loss continues beyond 6 months despite additional progestogen therapy (see Box 6 ) [11] and particularly if it fails to cease within 6 weeks of stopping HRT [46]. Assessment of the endometrium by TVS may be indicated, with an endometrial biopsy as appropriate.
Box 6. Management of irregular bleeding on HRT during the Covid-19 pandemic [11].
Modifying progestogen intake may control unscheduled bleeding:
Continuous combined HRT regimens:
-
•
Increase progestogen e.g. utrogestan 100 mg daily to 200 mg daily
-
•
Add utrogestan, medroxyprogesterone acetate, or norethisterone when progestogen is within combined preparation or Mirena IUS
-
•
Change to cyclical intake of progestogen if unscheduled bleeding continues
Cyclical HRT regimens:
-
•
Increase progestogen dose: e.g. utrogestan from 200 mg to 300 mg for 12 days a month
-
•
Increase duration of progestogen e.g. from 14 to 21 days for a 28-day HRT cycle
Alt-text: Box 6
Intermenstrual bleeding
Similar concern arises about the association of endometrial cancer with intermenstrual bleeding; though it only warrants investigation in women with persistent loss for more than 3 consecutive months. Nevertheless, patients can be reassured that the risk of endometrial cancer is small and that symptoms often resolve spontaneously [47]. Many women can be managed remotely and offered a trial without hormonal contraceptives for those using them or a trial with hormonal contraceptives for those who are not. The risk of cancer increases with age and is reflected in the criteria for referral to secondary care (see Box 7 ) [44].
Box 7. Management of intermenstrual bleeding (IMB) during the Covid-19 pandemic [44].
-
•
See within 30 days: women ≥40 years with persistent IMB (>3 consecutive months, no hormonal contraceptives)
-
•
May see beyond 30 days: women <40 years or women ≥40 years of age on hormonal contraceptives, with persistent IMB (>3 consecutive months)
-
•Within secondary care consider:
-
oCervical biopsy
-
oTVS
-
oEndometrial biopsy
-
oHysteroscopy±directed endometrial biopsy
-
o
Alt-text: Box 7
Appropriate genital swabs should be taken if sexually transmitted infection is possible. In addition, cervical cancer should be suspected if the woman also has postcoital bleeding (PCB) and/or an offensive vaginal discharge.
Postcoital bleeding and cervical cancer
Women who present with persistent PCB may initially be managed remotely within primary care with advice that cervical cancer is extremely unlikely if their cervical screening tests are up to date and high-risk human papilloma virus (HPV) negative [44]; if aged <26 years clarify whether they received the HPV vaccine. When the cervical smear test is overdue, the woman should be seen, the cervix examined and the test performed. Sexually transmitted disease should be considered and appropriately investigated and managed.
Referral to secondary care to be seen within 2 weeks is indicated when: the appearance of the cervix is consistent with cervical cancer and the woman is aged <35 years with abnormal, absent or overdue smears or is aged >35 years regardless of her smear history. A more relaxed timeframe of attendance within 42 days is appropriate, when the woman has a satisfactory smear history and is aged <35 years [44]. Investigations should follow local protocols and testing resources, with the consideration of endometrial investigation in postmenopausal women with PCB, particularly with a normal appearing cervix.
Abnormal cervical smears
Guidance is provided for the continuation of colposcopy services [48]. Women who need colposcopy are those with a recent cervical smear report showing: a high-grade (moderate or worse) abnormality, borderline changes in endocervical cells, possible glandular neoplasia and suspicion of invasive disease. Women with suspected cervical cancer should be seen in a weekly rapid access clinic.
Advice should be offered remotely, following local guidelines by healthcare professionals with suitable expertise, for low-grade abnormalities such as minor cytological changes and persistent HPV, to mimimise attendance in clinics.
Colposcopy
As with any patient attending an outpatient clinic, women with suspected or confirmed COVID-19 disease should not attend, but their colposcopic examination deferred until they are no longer infectious. The exception to this is for women with significant symptoms indicating cervical cancer; in these circumstances, staff must wear full PPE (see Fig. 2) during the consultation and examination.
Cervical abnormalities may be excised electrosurgically using standard smoke extraction facilities because the smoke produced is unlikely to contain SARS-CoV-2 particles [41]. However, laser ablation and excision with vaporisation of tissue should not be used [48].
Suspicious abdominal mass and ovarian cancer
As with other clinical symptoms that may indicate cancer, when assessing an abdominal mass hospital attendances need minimising. Patients' symptoms can be established remotely and preferably within primary care, with attention particularly to women >50 years old with persistent abdominal symptoms, increased urinary urgency and/or frequency [7].
Standard guidance continues, therefore women should be referred urgently if physical examination identifies ascites or an abdominal or pelvic mass that is not obviously fibroids [7]. Fibroids may be evident from previous scans, and the patient's knowledge about this may help avoid an inappropriate hospital visit.
Given the current situation, an abdominal examination may not have taken place, however, assessment of the Ca125 level remains pertinent. Local facilities vary but a drive-in, COVID-19-secure phlebotomy service may be available. A ‘straight-to test’ strategy is advocated, therefore symptomatic women with a substantially raised Ca125 level should be directed for an urgent computed tomography scan of the abdomen and pelvis rather than an initial ultrasound scan (USS), thus reducing the number of hospital visits [6].
The use of magnetic resonance imaging or USS assessment using the IOTA rules is advised when there is concern about a mass but with a low cancer risk [6]. The risk of malignancy index (RMI) can be calculated using the USS findings, and women in whom it is relatively low (<200) could be considered for virtual assessment and follow-up during the pandemic period [6].
Vulval and vaginal cancers
Guidelines state to consider referral ‘in women with an unexplained vulval lump, ulceration or bleeding’ [7]. Despite only 1300 new vulval cancers diagnosed annually in the UK [49], this is not reflected in the relatively high number of fast-track referrals for vulval conditions [42]. With the increased use of remote communication in primary and secondary care, photographic images may assist diagnosis and images sent by patients can be forwarded securely. Given the low overall risk of malignancy, most vulval conditions may be managed symptomatically, with only referral of women who fail to respond to treatment.
Little is known about how rare vaginal cancers present, but suspicious features include an unexplained palpable mass in or at the entrance to the vagina [7]. Unexplained, persistent vaginal bleeding should prompt a vaginal examination for a possible cancer; anecdotally, metastatic thyroid cancer or melanoma may present with a vaginal secondary.
Benign gynaecology
Heavy menstrual bleeding
Guidance has been produced for managing women with abnormal uterine bleeding during the COVID-19 pandemic [44]. It is advised that women with heavy menstrual bleeding (HMB) are managed initially by remote communication, establishing the severity of symptoms, the likelihood of anaemia and the possible cause. Women may be reassured that the risk of malignancy is negligible [47].
For women with torrential bleeding or in whom severe anaemia is suspected, emergency care may be required with appropriate treatment (see Box 8 ).
Box 8. Medical treatment for severe HMB during the Covid-19 pandemic [44].
For women with acute, severe vaginal bleeding consider:
-
•
Oral tranexamic acid, 1 g tds or qds (maximum 4 g/24 h)
-
•Oral high dose progestogens to rapidly suppress acute bleeding as single 21-day course, repeated cyclically days 5–26 monthly [51], or continuously to induce amenorrhoea:
-
oNorethisterone, 5 mg tds
-
oMedroxyprogesterone acetate, 10 or 20 mg tds
-
o
-
•
GnRHa, intramuscular injection of 4-week duration or nasally twice daily
-
•
Oral iron, intravenous iron infusion, or blood transfusion according to the severity of anaemia and associated symptoms
-
•
Address prolapsed cervical fibroid or haematological disorder if present
Alt-text: Box 8
When anaemia is unlikely, oral medical treatments as opposed to an LNG-IUS are preferable to reduce face-to-face interactions [44]. Guidance for the referral of women with less acute HMB is provided (see Box 9 ) [44].
Box 9. Non-acute, HMB management during the Covid-19 pandemic [44].
Refer women when non-acute, ongoing HMB resistant to oral treatments.
-
•See within 30 days if:
-
oConsidered unmanageable by the woman
-
oRisk factors for atypical hyperplasia or cancer: PCOS, morbid obesity (BMI ≥40), obesity (BMI ≥35) in women >40 years and Lynch syndrome
-
oSignificant anaemia
-
o
-
•See beyond 30 days if:
-
oConsidered manageable by the woman
-
oNo significant anaemia
-
o
Alt-text: Box 9
Diagnostic assessment of women referred to secondary care would usually commence after history and examination, with hysteroscopic investigation and possibly following a pelvic USS, if indicated [50]. If access to USS is limited, then a pelvic examination should be offered. This may reveal an obvious cause, such as a large fibroid uterus or even a prolapsed cervical fibroid. Removal of a prolapsed fibroid is possible within an outpatient setting, provided there is sufficient vaginal access as outlined below. If access to hysteroscopy is limited, then an endometrial biopsy should be taken to exclude endometrial cancer or hyperplasia.
Women with a large fibroid uterus and anaemia may benefit from gonadotrophin-releasing hormone agonist (GnRHa) injections, with the addition of hormonal add-back therapy to minimise menopausal side effects (see Box 10 ). Primary care may provide the injections depending upon local arrangements. The duration of treatment will depend on local facilities and access to surgical treatments, the patient's vulnerabilities and her wishes.
Box 10. Gonadotrophin-releasing analogues (GnRHa) for the management of anaemia, pain and pressure symptoms during the Covid-19 pandemic [44].
Introduce or continue outpatient GnRHa injection service and
-
•
Initially offer patients 4-week duration GnRHa
-
•
Move to a 12-week therapy if well tolerated
-
•
Consider nasal spray
-
•
Monitor for hypertension
-
•Offer for:
-
oHMB with severe anaemia
-
oAcute and chronic pain from endometriosis or adenomyosis
-
oLarge fibroids with pressure symptoms
-
o
-
•
Manage menopausal symptoms and bone demineralisation with hormonal add-back therapy
-
•
Oral tibolone 2.5 mg daily often suitable
Alt-text: Box 10
Hysteroscopy services
Diagnostic and operative hysteroscopy services are normally provided within an outpatient setting in conscious women with or without local anaesthetic. There is no evidence that operative hysteroscopic procedures with the use of electrosurgery or tissue removal systems (TRS) carry an increased risk of transmission of SARS-CoV-2 through contamination or the generation of aerosols [41]. Therefore, these services may continue during pandemic restrictions and enable women to undergo urgent investigations and treatments for uterine disorders. The range of services might need curtailing during times of greatest restriction, for example endometrial ablation for HMB replaced by medical treatments to reduce hospital attendances. However, there is a balance to be struck between, for example, a single visit for an outpatient endometrial ablation as opposed to multiple attendances for GnRHa injections.
Whilst all women should be offered a choice of anaesthesia and treatment settings for hysteroscopic procedures, they should be advised that an outpatient setting avoids hospital admission, thereby minimising the risk of exposure to SARS-CoV-2.
Infection control practices for hysteroscopic procedures in an outpatient setting include the use of PPE and complying with local and national protocols (see Fig. 2). Also, best practices should be adopted as currently advised (see Box 11 ) [41].
Box 11. Best practice for hysteroscopic services to minimise SARS-CoV-2 transmission [41].
-
•
Minimise blood, urine, genital tract fluids and faecal contamination
-
•
Avoid complications requiring further health care interventions
-
•
Use mechanical instruments or tissue removal systems, if safe and effective alternative to electrosurgery, to avoid generating surgical smoke
-
•
Where electrosurgery is used, extract surgical smoke using active suction through closed circuit outflow
Alt-text: Box 11
Removal of prolapsed cervical fibroids
Prolapsed cervical fibroids can cause severe and acute menstrual blood loss with anaemia. Provided that the fibroid is accessible vaginally and the patient is amenable, it can be removed in an ambulatory setting in the outpatient clinic with local anaesthesia, and therefore avoiding a general anaesthetic. Electrosurgical instruments, such as a colposcopic diathermy loop with smoke extraction can be used to excise the vaginal portion of the fibroid and then the removal of the remaining intrauterine stump using a hysteroscopic TRS once access to the uterine cavity is possible. A gaping cervical os may need clamping to obtain uterine distension.
Menopause services
The continued need for menopause services is recognised [11]. Remote consultations are already a feature of some menopause services; expansion or introduction of these will ensure minimal face-to-face encounters [11]. Women with new symptoms require access to information, advice and treatment, and those already receiving HRT need continued access to prescriptions; both groups will need to know the local pathways for obtaining medication. Reduced access to some HRT preparations has created difficulties in the UK for GPs and patients, but regular updates are provided about their availability [11].
The management of unscheduled bleeding on HRT is discussed above.
Chronic pelvic pain
Patients with chronic pelvic pain, sometimes as a consequence of endometriosis or adenomyosis, may be awaiting definitive surgical treatment but have found this to be postponed, seemingly indefinitely, by the COVID-19 pandemic. Treatment with oral progestogens, as for HMB (see Box 8), and non-steroidal medication may prove sufficient. However, episodic, cyclical or continuous severe pain that does not respond to these measures may be managed with GnRHa injections, with the addition of add-back therapy (see Box 10). Again, the use of a 12-week duration therapy will reduce the number of clinical interactions.
Urogynaecology
Patients who attend urogynaecology clinics generally present with non-urgent conditions such as prolapse and/or urinary incontinence. A large proportion of these patients are aged >60 years making them more vulnerable should they contract COVID-19. Fortunately, there are few situations when an emergency admission to hospital is required. Guidance is available for the care of women with urogynaecological disorders. Patients who require a face-to-face consultation or review are identified along with when they need to be seen [52].
Urinary retention
Patients with urinary retention need urgent attention within 12 h of presentation to prevent long-term bladder problems. Where the residual volume is over the normal range for the local hospital guidance, patients should be taught self-catheterisation and followed up remotely to reduce the need for further hospital visits. The alternative is to insert an indwelling catheter and arrange a return visit for a trial without catheter at a convenient date. This is generally within 7 days but could be deferred.
Vaginal pessaries
Occasionally, patients may develop a severe problem arising from a vaginal pessary, such as fistulation and this needs to be addressed within 7 days, often for pessary removal. Such problems are usually secondary to either a Gelhorn or shelf pessary.
Women with a vaginal pessary require regular follow-up. An initial telephone consultation may establish whether any problems indicating ulceration are present, such as vaginal bleeding or pain. If so, the women should be reviewed within 30 days. If vaginal bleeding is a concern and the uterus is present, then the patient would need assessment for PMB as above. Women with vaginal discharge or bleeding should be advised how to make contact and seek advice.
Provided all remains well, the woman can be reassured that a delay of a few months for a pessary change will not cause harm. Routine vaginal ring pessary changes can be safely deferred for up to 6 months from when the change was due. However, this should not be beyond 3 months for Shaatz, Gelhorn, shelf and double pessaries, otherwise the risk of ulceration and incarceration increases.
New referrals with prolapse or incontinence
A woman with new onset procidentia may require assessment within 30 days if she experiences bladder and bowel problems. However, if the problem is long-standing and causing minimal inconvenience, this can be delayed.
Most new referrals to urogynaecology clinics can be deferred until concerns about the COVID-19 pandemic are relaxed. For urinary incontinence, a virtual consultation will permit an assessment of the type of incontinence and for preliminary advice to be given, and this may enable the commencement of initial treatment.
Physical examination is essential for women with a prolapse to understand their condition and offer advice about management and treatment options, therefore a telephone consultation is of limited value and the appointment is best deferred.
Suprapubic catheters
Suprapubic catheters in women are usually changed at regular intervals, but this can be safely delayed by 3 months. A hospital visit might be avoided if a local district nurse can perform this for the patient at home.
Urogynaecological procedures
The advice regarding urogynaeclogical procedures is that they are non-urgent and therefore should be suspended for the duration of the COVID-19 pandemic [53]. This includes bladder instillations, Botox injections, percutaneous tibial nerve stimulation, insertion of urethral bulking agents and diagnostic cystoscopy for non-cancer-related symptoms. These procedures can be resumed with the relaxation of pandemic restrictions.
Fertility services
Fertility units throughout the UK closed during the first lockdown. However, with the easing of pressures on the NHS, individual units reopened once their COVID-19 treatment commencement strategy was approved [53]. During subsequent lockdowns, it was felt safe for fertility units to continue [54].
Remote communication is effective for the initial assessment of fertility patients with discussion about treatment options. Many fertility treatments and procedures are undertaken within an ambulatory setting; detailed guidance to recommence these is available [54]. The importance of clear and effective communication with individuals seeking fertility treatment during the pandemic is emphasised [53]. A new consideration is the benefit of vaccination against SARS-CoV-2 before treatment is started, to avoid potential complications of COVID-19 during a subsequent pregnancy [53].
Summary
Strategies for minimising the risk of SARS-CoV-2 transmission are discussed using the ‘hierarchy of control’ categories and applying them to gynaecology outpatient clinics and ambulatory services. Triaging of referrals and targeting women with the greatest need reduces hospital attendances and supports the provision of safe, equitable, effective and quality care for all women. Fewer patients attending clinics and reconfiguration of seating arrangements in waiting areas enables safe physical distancing. Many opportunities for hand sanitisation or hand washing and a scrupulous cleaning regime reduce viral transmission. Careful doffing, donning and wearing of appropriate PPE helps maintain staff and patient safety.
The continuation of gynaecological services is necessary, with emergency and urgent care maintained, including care of patients with cancer, whilst minimising the risk of nosocomial infection. Remote methods of communication have proved invaluable at establishing contact with patients and providing care, whilst minimising clinic attendance. Specialist advice is available to manage gynaecological disorders during the COVID-19 pandemic. Alternative treatments are advocated to mitigate the consequences of less access to the usual surgical procedures, with the aim to make best use of all available resources. Patients who require physical examination for a non-urgent condition may have their assessment safely deferred.
Outpatient hysteroscopy and colposcopy services may safely continue; it is advisable that these are undertaken by experienced clinicians to minimise the likelihood of complications, which require further healthcare interventions. Avoidance of inpatient episodes and the need for a general anaesthetic is advised.
Declaration of competing interest
Natalie Farmer: None.
Mary Connor receives teaching honoraria and consultancy fees from Medtronic Medical Device Company, Covidien AG, Victor von Bruns-Strasse 19 8212, Neuhausen am Rheinfall, Switzerland.
Practice points.
-
•
SARS-CoV-2 transmission is probably primarily by droplet and aerosols; therefore, virus transmission is likely to be minimised by the reduction of patient attendance.
-
•
Attention to the clinic environment by ensuring adequate ventilation, maintaining high standards of cleanliness and ensuring staff wear appropriate personal protective equipment, will help reduce transmission between patients and staff.
-
•
Substitute face-to-face encounters with virtual consultations when examination or procedures are unlikely; use to establish the level of vulnerability and assess whether deferring investigation is appropriate.
-
•
Joint guidelines published by the RCOG advocate the achievement of as much as possible during a single visit e.g. consider the insertion of LNG-IUS during hysteroscopy or endometrial biopsy, when endometrial hyperplasia or uterine cancer is likely.
-
•
Manage anaemia from heavy menstruation with oral preparations; actively respond to acute, severe anaemia and offer non-surgical treatment to prevent recurrence.
-
•
Guidelines from the RCOG and BSGE advise that outpatient ambulatory care should be provided by experienced clinicians to minimise the need for inpatient episodes.
-
•
Advice from the BSUG is that non-urgent conditions, such as prolapse and urinary incontinence, can be safely deferred until SARS-CoV-2 infection risk eases.
Research agenda.
-
•
Risk of SARS-CoV-2 transmission using various forms of eye protection e.g. goggles versus face shields
-
•
Risk of SARS-CoV-2 transmission wearing single versus double pair of gloves
-
•
Summary of research into exemptions to wear face masks/coverings
-
•
Future developments in patient-initiated follow-up in gynaecology outpatient clinics
References
- 1.Cevik M., Tate M., Lloyd O., Maraolo A.E., Schafers J., Ho A. SARS-CoV-2, SARS-CoV, and MERS-CoV viral load dynamics, duration of viral shedding, and infectiousness: a systematic review and meta-analysis. Lancet Microbe. 2021;2:e13–e22. doi: 10.1016/S2666-5247(20)30172-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Hui K.P.Y., Cheung M.-C., Perera R.A.P.M., Ng K.-C., Bui C.H.T., Ho J.C.W., et al. Tropism, replication competence, and innate immune responses of the coronavirus SARS-CoV-2 in human respiratory tract and conjunctiva: an analysis in ex-vivo and in-vitro cultures. Lancet Respir Med. 2020;8:687–695. doi: 10.1016/S2213-2600(20)30193-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.van Doremalen N., Bushmaker T., Morris D.H., Holbrook M.G., Gamble A., Williamson B.N., et al. Aerosol and surface stability of SARS-CoV-2 as compared with SARS-CoV-1. N Engl J Med. 2020;382:1564–1567. doi: 10.1056/NEJMc2004973. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Environmental and Modelling Group Transmission of SARS-CoV-2 and mitigating measures: EMG-SAGE. 4th June 2020. https://assets.publishing.service.gov.uk/government/uploads/system/uploads/attachment_data/file/892043/S0484_Transmission_of_SARS-CoV-2_and_Mitigating_Measures.pdf
- 5.RCOG Framework for staffing of obstetrics and gynaecology units during the COVID-19 pandemic. 2020. https://www.rcog.org.uk/globalassets/documents/guidelines/2020-05-22-framework-for-staffing-of-obstetrics-and-gynaecology-units-during-the-covid-19-pandemic.pdf
- BGCS BGCS framework for care of patients with gynaecological cancer during the COVID-19 Pandemic. 2020. https://www.bgcs.org.uk/wp-content/uploads/2020/03/BGCS-covid-guidance-v1.-22.03.2020.pdf
- 7.National Institute for Health and Care Excellence Suspected cancer: recognition and referral [NG12] 2015. https://www.nice.org.uk/guidance/ng12/resources/suspected-cancer-recognition-and-referral-pdf-1837268071621 [PubMed]
- RCOG Restoration and recovery: priorities for obstetrics and gynaecology. 2020. https://www.rcog.org.uk/globalassets/documents/guidelines/2020-06-26-restoration-and-recovery---priorities-for-obstetrics-and-gynaecology.pdf
- 9.Car J., Koh G.C.H., Foong P.S., Wang C.J. Video consultations in primary and specialist care during the covid-19 pandemic and beyond. BMJ. 2020;371:m3945. doi: 10.1136/bmj.m3945. [DOI] [PubMed] [Google Scholar]
- Murugesu S., Galazis N., Jones B.P., Chan M., Bracewell-Milnes T., Ahmed-Salim Y., et al. Evaluating the use of telemedicine in gynaecological practice: a systematic review. BMJ Open. 2020;10 doi: 10.1136/bmjopen-2020-039457. [DOI] [PMC free article] [PubMed] [Google Scholar]
- BMS, RCOG, RCGP, FSRH Joint BMS/RCOG/RCGP/FSRH framework for restoration of menopause services in response to COVID-19. 2020. https://www.fsrh.org/documents/bms-fsrh-rcgp-rcog-restoration-menopause-covid19/
- 12.Muto K., Yamamoto I., Nagasu M., Tanaka M., Wada K. Japanese citizens' behavioral changes and preparedness against COVID-19: an online survey during the early phase of the pandemic. PloS One. 2020;15 doi: 10.1371/journal.pone.0234292. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Azuma K., Yanagi U., Kagi N., Kim H., Ogata M., Hayashi M. Environmental factors involved in SARS-CoV-2 transmission: effect and role of indoor environmental quality in the strategy for COVID-19 infection control. Environ Health Prev Med. 2020;25:1–16. doi: 10.1186/s12199-020-00904-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Escombe A.R., Ticona E., Chávez-Pérez V., Espinoza M., Moore D.A.J. Improving natural ventilation in hospital waiting and consulting rooms to reduce nosocomial tuberculosis transmission risk in a low resource setting. BMC Infect Dis. 2019;19 doi: 10.1186/s12879-019-3717-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Kampf G., Todt D., Pfaender S., Steinmann E. Persistence of coronaviruses on inanimate surfaces and their inactivation with biocidal agents. J Hosp Infect. 2020;104:246–251. doi: 10.1016/j.jhin.2020.01.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.WHO Cleaning and disinfection of environmental surfaces: interim guidance. 2020. https://www.who.int/publications-detail/cleaning-and-disinfection-of-environmental-surfaces-inthe-context-of-covid-19
- 17.European Centre for Disease Prevention and Control Disinfection of environments in healthcare and non- healthcare settings potentially contaminated with SARS-CoV-2. 2020. https://www.ecdc.europa.eu/en/publications-data/disinfection-environments-covid-19
- 18.Edwards N.W.M., Best E.L., Goswami P., Wilcox M.H., Russell S.J. Recontamination of healthcare surfaces by repeated wiping with Biocide-Loaded wipes: “one wipe, one surface, one direction, dispose” as best practice in the clinical environment. Int J Mol Sci. 2020;21:9659. doi: 10.3390/ijms21249659. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Kamming D., Gardam M., Chung F. Anaesthesia and SARS. Br J Anaesth. 2003;90:715–718. doi: 10.1093/bja/aeg173. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.WHO WHO guidelines on hand hygiene in health care: a summary first global patient safety challenge clean care is safer care. Patient Saf. 2009 http://whqlibdoc.who.int/publications/2009/9789241597906_eng.pdf [PubMed] [Google Scholar]
- 21.CDC Guideline for hand hygiene in health-care settings. 2002. https://www.cdc.gov/mmwr/PDF/rr/rr5116.pdf
- 22.Huang C., Ma W., Stack S. The hygienic efficacy of different hand-drying methods: a review of the evidence. Mayo Clin Proc. 2012;87:791–798. doi: 10.1016/j.mayocp.2012.02.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Chu D.K., Akl E.A., Duda S., Solo K., Yaacoub S., Schünemann H.J., et al. Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. Lancet. 2020;395:1973–1987. doi: 10.1016/S0140-6736(20)31142-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.European Parliament, Council of the European Union Regulation (EU) 2016/425 of the European Parliament and of the Council of 9 March 2016 on personal protective equipment and repealing Council Directive 89/686/EEC. 2016. https://eur-lex.europa.eu/legal-content/EN/TXT/?uri=CELEX:32016R0425
- 25.Bałazy A., Toivola M., Adhikari A., Sivasubramani S.K., Reponen T., Grinshpun S.A. Do N95 respirators provide 95% protection level against airborne viruses, and how adequate are surgical masks? Am J Infect Contr. 2006;34:51–57. doi: 10.1016/j.ajic.2005.08.018. [DOI] [PubMed] [Google Scholar]
- 26.European Commission List of COVID-19 essential protective personal equipment (PPE) 2020. https://ec.europa.eu/info/sites/info/files/list-covid-19-essential-ppe_en.pdf
- 27.Smith J.D., MacDougall C.C., Johnstone J., Copes R.A., Schwartz B., Garber G.E. Effectiveness of N95 respirators versus surgical masks in protecting health care workers from acute respiratory infection: a systematic review and meta-analysis. CMAJ (Can Med Assoc J) 2016;188:567–574. doi: 10.1503/cmaj.150835. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Garcia Godoy L.R., Jones A.E., Anderson T.N., Fisher C.L., Seeley K.M.L., Beeson E.A., et al. Facial protection for healthcare workers during pandemics: a scoping review. BMJ Glob Health. 2020;5:1–9. doi: 10.1136/bmjgh-2020-002553. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.CDC Coronavirus disease 2019 (COVID-19). How to protect yourself & others. 2021. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/prevention.html
- 30.The Royal Society, The British Academy Face masks and coverings for the general public: behavioural knowledge, effectiveness of cloth coverings and public messaging. 2020. https://royalsociety.org/-/media/policy/projects/set-c/set-c-facemasks.pdf?la=en-GB&hash=A22A87CB28F7D6AD9BD93BBCBFC2BB24
- 31.Soriano J.B., Anzueto A., Anticevich S.B., Kaplan A., Miravitlles M., Usmani O., et al. Face masks, respiratory patients and COVID-19. Eur Respir J. 2020;56:2003325. doi: 10.1183/13993003.03325-2020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Department of Health & Social Care Face coverings: when to wear one, exemptions, and how to make your own. 2020. https://www.gov.uk/government/publications/face-coverings-when-to-wear-one-and-how-to-make-your-own/face-coverings-when-to-wear-one-and-how-to-make-your-own#exemptions
- Jefferson T., Foxlee R., Del Mar C., Dooley L., Ferroni E., Hewak B., et al. Physical interventions to interrupt or reduce the spread of respiratory viruses: systematic review. BMJ. 2008;336:77–80. doi: 10.1136/bmj.39393.510347.BE. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Health and Safety Executive HSE rapid evidence review PART ONE: equivalence of N95 and FFP2 masks. 2020. https://www.hse.gov.uk/coronavirus/assets/docs/face-mask-equivalence-aprons-gown-eye-protection.pdf
- 35.Health and Safety Executive HSE rapid evidence review PART TWO: aprons, gowns and eye protection. 2020. https://www.hse.gov.uk/coronavirus/assets/docs/face-mask-equivalence-aprons-gown-eye-protection.pdf
- 36.Verbeek J.H., Rajamaki B., Ijaz S., Sauni R., Toomey E., Blackwood B., et al. Personal protective equipment for preventing highly infectious diseases due to exposure to contaminated body fluids in healthcare staff. Cochrane Database Syst Rev. 2020 May 15;5 doi: 10.1002/14651858.CD011621.pub5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Mansour A.A.I., Even J.L., Phillips S., Halpern J.L. Eye protection in Orthopaedic surgery: an in vitro study of various forms of eye protection and their effectiveness. J Bone Jt Surg. 2009;91:1050–1054. doi: 10.2106/JBJS.H.00460. [DOI] [PubMed] [Google Scholar]
- 38.CDC Strategies for optimizing the supply of facemasks. 2020. https://www.cdc.gov/coronavirus/2019-ncov/hcp/ppe-strategy/face-masks.html
- 39.Coia J.E., Ritchie L., Adisesh A., Makison Booth C., Bradley C., Bunyan D., et al. Guidance on the use of respiratory and facial protection equipment. J Hosp Infect. 2013;85:170–182. doi: 10.1016/j.jhin.2013.06.020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- NHS England Clinical guide for the management of cancer patients during the coronavirus pandemic. 2020. https://www.uhb.nhs.uk/coronavirus-staff/downloads/pdf/CoronavirusCancerManagement.pdf
- 41.BSGE R.C.O.G. Joint RCOG/BSGE Statement on gynaecological endoscopy during the COVID-19 pandemic. 2020. https://www.rcog.org.uk/globalassets/documents/guidelines/2020-12-21-joint-rcog-bsge-gynaecological-endoscopy.pdf
- 42.Bansal J.K., Goldrick I.G., Manchanda R., Olaitan A. vol. 9. Dove Press; 2017. (Rapid-access gynecological oncology clinic outcomes in North London, UK). 19–23. [Google Scholar]
- 43.NHS England and NHS Improvement Letter: cancer alliance information on managing cancer referrals. 2020. https://www.england.nhs.uk/coronavirus/wp-content/uploads/sites/52/2020/03/cancer-alliance-information-on-managing-cancer-referrals-19-march-2020.pdf
- RCOG, BSGE, BGCS Joint RCOG, BSGE and BGCS guidance for the management of abnormal uterine bleeding in the evolving Coronavirus (COVID-19) pandemic. 2020. https://www.bgcs.org.uk/wp-content/uploads/2020/03/Joint-RCOG-BSGE-BGCS-guidance-for-management-of-abnormal-uterine-bleeding-AUB-in-the-evolving-Coronavirus-COVID-19-pandemic.pdf
- 45.Clarke M.A., Long B.J., Del Mar Morillo A., Arbyn M., Bakkum-Gamez J.N., Wentzensen N. Association of endometrial cancer risk with postmenopausal bleeding in women: a systematic review and meta-analysis. JAMA Intern Med. 2018;178:1210–1222. doi: 10.1001/jamainternmed.2018.2820. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.National Institute for Health and Care Excellence Referral guidelines for suspected cancer: clinical guideline [CG27] 2005. https://www.nice.org.uk/guidance/cg27/documents/cg27-referral-for-suspected-cancer-review-decision2
- 47.Pennant M.E., Mehta R., Moody P., Hackett G., Prentice A., Sharp S.J., et al. Premenopausal abnormal uterine bleeding and risk of endometrial cancer. BJOG An Int J Obstet Gynaecol. 2017;124:404–411. doi: 10.1111/1471-0528.14385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.BSCCP, RCOG Colposcopy guidance during COVID-19 pandemic. 2020. https://www.rcog.org.uk/globalassets/documents/guidelines/2020-04-17-colposcopy-guidance-during-covid-19-pandemic.pdf
- 49.Cancer Research UK Vulval cancer statistics. 2020. https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/vulval-cancer
- 50.National Institute for Health and Care Excellence Heavy menstrual bleeding: assessment and management [NG88] 2020. https://www.nice.org.uk/guidance/ng88 [PubMed]
- 51.Bofill Rodriguez M., Lethaby A., Low C., Cameron I.T. Cyclical progestogens for heavy menstrual bleeding. Cochrane Database Syst Rev. 2019;(8) doi: 10.1002/14651858.CD001016.pub3. Art. No.: CD001016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Jha S., Pradhan A. BSUG guidance on management of urogynaecological conditions and vaginal pessary use during the covid 19 pandemic. 2020. https://www.rcog.org.uk/globalassets/documents/guidelines/2020-04-09-bsug-guidance-on-management-of-urogynaecological-conditions-and-vaginal-pessary-use-during-the-covid-19-pandemic.pdf
- 53.Human Fertilisation & Embryology Authority FAQ coronavirus (COVID-19) 2021. https://portal.hfea.gov.uk/media/1661/covid-19-clinic-faqs-15-january-2021.pdf
- 54.Human Fertilisation & Embryology Authority Coronavirus (COVID-19) guidance for professionals. 2021. https://www.hfea.gov.uk/treatments/covid-19-and-fertility-treatment/coronavirus-covid-19-guidance-for-professionals