Abstract
Background
Previous work has evaluated the effect of remote ischaemic conditioning (RIC) in a number of clinical conditions (e.g. cardiac surgery and acute kidney injury), but only one analysis has examined blood pressure (BP) changes. While individual studies have reported the effects of acute bouts and repeated RIC exposure on resting BP, efficacy is equivocal. We conducted a systematic review and meta-analysis to evaluate the effects of acute and repeat RIC on BP.
Methods
A systematic search was performed using PubMed, Web of Science, EMBASE, and Cochrane Library of Controlled Trials up until October 31, 2020. Additionally, manual searches of reference lists were performed. Studies that compared BP responses after exposing participants to either an acute bout or repeated cycles of RIC with a minimum one-week intervention period were considered.
Results
Eighteen studies were included in this systematic review, ten examined acute effects while eight investigated repeat effects of RIC. Mean differences (MD) for outcome measures from acute RIC studies were: systolic BP 0.18 mmHg (95%CI -0.95, 1.31; p = 0.76), diastolic BP -0.43 mmHg (95%CI -2.36, 1.50; p = 0.66), MAP -1.73 mmHg (95%CI -3.11, −0.34; p = 0.01) and HR -1.15 bpm (95%CI -2.92, 0.62; p = 0.20). Only MAP was significantly reduced. Repeat RIC exposure showed non-significant change in systolic BP -3.23 mmHg (95%CI -6.57, 0.11; p = 0.06) and HR -0.16 bpm (95%CI -7.08, 6.77; p = 0.96) while diastolic BP -2.94 mmHg (95%CI -4.08, −1.79; p < 0.00001) and MAP -3.21 mmHg (95%CI -4.82, −1.61; p < 0.0001) were significantly reduced.
Conclusions
Our data suggests repeated, but not acute, RIC produced clinically meaningful reductions in diastolic BP and MAP.
Keywords: Blood pressure, Acute remote ischaemic conditioning, Repeat remote ischaemic conditioning, RIC
Abbreviations: BP, blood pressure; CABG, coronary artery bypass grafting; CI, confidence interval; HR, heart rate; MD, mean difference; VEGF, vascular endothelial growth factor; RIC, Remote ischaemic conditioning; SD, standard deviation; T2DM, type 2 diabetes mellitus
Highlights
-
•
Question: Does acute or repeat remote ischaemic conditioning (RIC) lower blood pressure?
-
•
Findings: Acute RIC significantly reduced MAP. Repeat RIC significantly reduced DBP and MAP by around 3mmHg. This is clinically meaningful.
-
•
Meaning: Repeat RIC is effective in reducing diastolic and mean arterial blood pressures.
1. Introduction
Uncontrolled hypertension is a major cardiovascular risk factor. People with hypertension have decreased arteriole and capillary density within their tissues. This condition is known as rarefaction and increases peripheral resistance resulting in elevated blood pressure, vessel damage and systemic inflammation [1]. The treatment and management of hypertension is a major public health concern since prevalence continues to rise significantly with age [[2], [3], [4]].
Hypertension treatment options include pharmacological and lifestyle modification interventions [5,6]. However, treatment responses and adherence continue to be variable as management is ongoing [[7], [8], [9]]. Regular exercise participation rates remain low due to financial cost, lack of time and motivation [[10], [11], [12], [13], [14]]. Therefore, identification of a novel, beneficial, time efficient and cost-effective intervention is of great importance.
Remote ischaemic conditioning (RIC) is a simple emerging intervention, requiring minimal time commitment, that has been shown to induce stimulation of angiogenesis within the existing vasculature via the activation of physiological or functional non-pathological processes in the myocardium [15] and the repeated exposure has the potential to modify cardiovascular disease (CVD) risk factors [16].
First shown in 1993 [17], RIC was developed to protect from myocardial injury during coronary artery bypass grafting (CABG). RIC is usually executed by the application of an inflated blood pressure cuff that elicits repeated brief episodes of ischaemic conditioning alternated with periods of reperfusion (deflated cuff). RIC deprives a vascular bed, tissue or organ of blood flow in order to condition it towards a permanent or prolonged restricted blood flow as a means of protection against future hypoxia [16,18,19]. The application of RIC usually comprises 3–4 repetitions of 5-min cuff inflation at 200 mmHg intermittently spread with 5-min of deflation [16] in either a remote organ [20] or limb [21].
The safety of RIC has been shown in patients with anterior ST-segment elevation myocardial infarction who had reduced enzymatic infarct size with an improved cardiac magnetic resonance imaging (MRI) and ST-segment resolution [22,23]. Pilcher et al. [24] in their systematic review and meta-analysis showed the cardioprotective efficacy of RIC in open cardiac surgery demonstrating a significantly reduced concentration of postoperative troponin. The magnitude of troponin release following cardiac surgery has independently been linked with a high risk of mortality [25,26]. Meng et al. [27] also showed the efficacy and safety of RIC in octo- and non-agenarians with symptomatic intracranial arterial stenosis to prevent stroke occurrence and recurrence.
Single session RIC performed immediately preceding exercise improved athletic performance in both competitive athletes [28] and recreationally active young individuals [29,30]. Similarly, in people with multiple sclerosis a single session of RIC resulted in an immediate improvement in 6-min walk distance [31].
More importantly, the relationship between BP and RIC has received attention following Madias’ self-experimentation case study reporting mean reduction in both systolic (>6 mmHg) and diastolic (>3 mmHg) BP at 60 min following acute bouts of RIC as a normotensive, middle-aged adult [32]. Subsequent work by Madias and Koulouridis [33] improving on the initial work of Madias, which may have had minor design flaws [32], confirmed the hypotensive effect of repeated RIC compared to control. Further work showed a sustained BP lowering effect during RIC, which remained for 5–10 days after cessation of therapy [19]. Adopting RIC as an adjunct therapeutic modality for controlling blood pressure may be appropriate.
There have been a number of reviews and meta-analyses that have assessed the clinical outcomes of RIC during cardiac surgery [[24], [25], [26],[34], [35], [36], [37], [38], [39], [40], [41], [42], [43]]. By including cohort and non-RCTs, previous meta-analyses have provided weaker level evidence. While some individual studies have reported the effects of repeated RIC on resting BP, there has not been a consensus on its efficacy [16] and an updated systematic review using only RCTs in the meta-analysis is indicated as new studies are now available. The aim of this work was to evaluate the effect of acute and repeated exposure RIC on BP.
2. Methods
This systematic review and meta-analysis was registered with the International Prospective Register of Systematic Reviews (PROSPERO) [CRD42020180784] [44].
2.1. Search strategy
A systematic literature search was conducted to identify potential studies for inclusion. PubMed, Web of Science, EMBASE from 1966 up until October 31, 2020 and the Cochrane controlled trials registry were searched. Reference lists from systematic reviews and eligible studies were searched for additional studies. The search strategy included a combination of the following terms: (remote ischaemic preconditioning) or (remote ischaemic conditioning) or (physiological ischaemia training) or (limb occlusion) or (cuff inflation) and (blood pressure) (Supplementary Table S1).
2.2. Inclusion and exclusion criteria
We included RCTs, cohort, crossover studies in adult (over 18 years) humans that investigated blood pressure response after exposing participants to acute or repeated RIC by the application of BP cuff inflation or medical tourniquet in a remote limb. RIC studies that completely prevented blood flow, for repeated ischaemic cycles were included. We included acute studies and studies that assessed the repeated effects of RIC using a minimum intervention duration of one week. We included studies in adult participants, with or without known CVD (i.e. both healthy and diseased adult populations).
We excluded studies that did not report any desired outcome of interest.
Authors were contacted to provide missing data where necessary. Two reviewers (BB, MP) assessed all identified articles independently for eligibility, and two reviewers (GD, NS) were consulted for any disagreement to be resolved.
2.3. Comparisons
We compared data from studies that utilized a “remote ischaemic conditioning intervention group” versus either [non-exposed control, or sham group, or another intervention group] OR a comparison between pre-versus post-remote ischaemic interventions.
2.4. Outcome measures
The outcome measures were change in blood pressure (systolic and diastolic BP, MAP) and heart rate.
2.5. Data extraction
Data was extracted using a data extraction form purposely designed for this review. The extracted data was checked and discussed by all authors. Extracted data from each study included first author's name and year of publication, country, study design, population, participants' baseline characteristics (age, gender proportion and sample size), protocol characteristics, duration and frequency of protocol, change in the desired outcome variables, number of withdrawal participants and intervention compliance.
2.6. Analyses
A descriptive analysis of extracted data was undertaken for all studies included in the review. However, only RCT data was pooled for meta-analyses. The change in means after the intervention were obtained by subtracting the pre-intervention means from the post-intervention means. The change in SD of the corresponding means were calculated adopting the formula [45] for calculating change in means' SD, using a correlation of 0.5 for all studies. A random effects model was used for the pooled analyses. Forest plots was generated to provide visual representation of the effect of RIC on outcome measures. Egger's plots were provided to evaluate the publication bias by visual inspection [46].
Statistical heterogeneity (I2) was assessed and the values of 25%, 50%, and 75% corresponded to low, moderate, and high degrees of heterogeneity [47]. The level of statistical significance was set at p < 0.05 CIs. The meta-analyses were carried out using Review Manager version 5.4, The Cochrane Collaboration software package [48].
2.7. Quality assessment
The methodological quality of the included studies was assessed using the JADAD scale [49]. Three domains were assessed based on study description as randomisation (score: 0–2), blinding (score: 0–2), and an account of withdrawals and dropouts (score: 0–1) for a total score of 5. Any study with a total score ≤2 or ≥3 was described as low or high quality, respectively.
3. Results
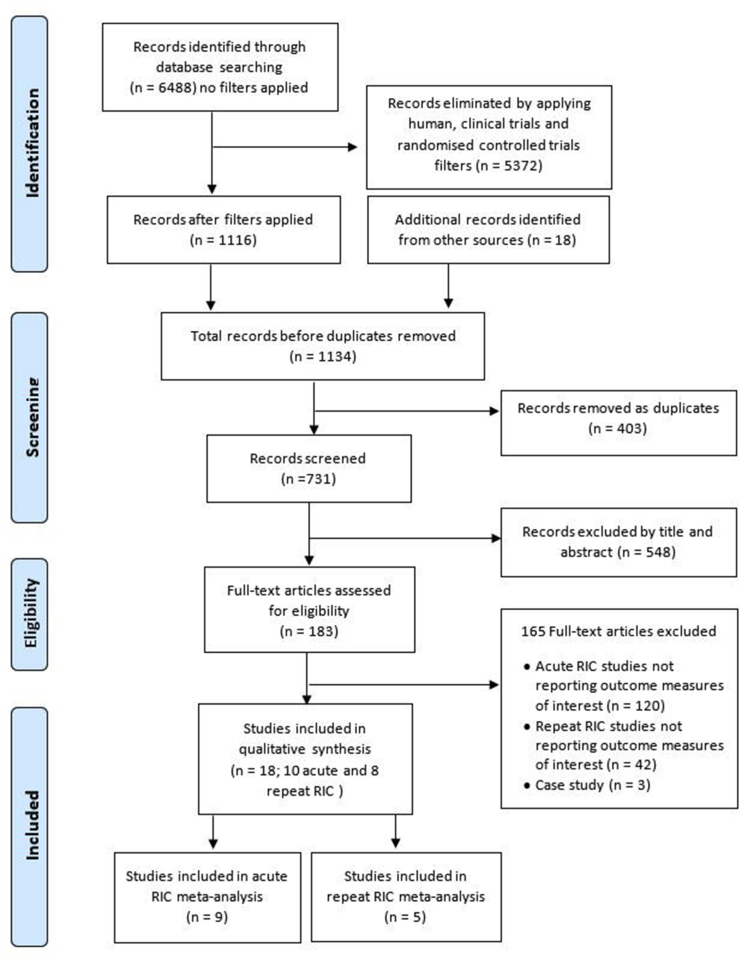
The systematic database search identified a total of 6488 records without any filters applied. A total of 1116 records remained after human, clinical and randomised controlled trial filters were applied. An additional 18 records were found in reference lists from systematic reviews and references of papers found in the initial search. After removal of duplicates, 731 articles were screened by title and abstract leaving 183 publications (Fig. 1). Of these, 165 full-text publications were excluded for not meeting inclusion criteria with reasons indicated in the PRISMA flow diagram. Eighteen (10 acute and 8 repeat RIC) studies were deemed eligible for inclusion in the systematic review.
Fig. 1.
PRISMA flow diagram.
3.1. Study characteristics
Ten acute RIC exposure studies [31,[50], [51], [52], [53], [54], [55], [56], [57], [58]] were considered in this systematic review including one cohort study [50]. Nine studies (10 comparisons) were eligible for pooling meta-analytically for acute RIC effect. Three studies [50,51,56] were conducted in healthy individuals, one study each in patients with multiple sclerosis [31] and peripheral artery disease [53], three other studies [52,54,55] were conducted in patients undergoing surgery. One study was conducted in coronary heart disease patients [58] and a crossover study in both healthy adults and patients with coronary heart disease [57]. The duration of the follow-up after RIC application ranged from 10-min to 28 h; while in two studies [51,57], the duration before post-measurement was not clearly described. Acute RIC protocols varied from 3 to 4 cycles with 5-min cuff inflation-induced ischaemia at similar pressure of 200 mmHg or 30–50 mmHg above each participant's predetermined systolic BP across studies. The characteristics of the acute RIC effect included studies are summarized in Table 1.
Table 1.
Acute RIC – Characteristics of included studies.
| Study/Year/Country | Design/MA inclusion | Population – Age (yr) – Sex |
Outcome measures | Duration before post-measurement | Treatment groups and protocol | Ischaemic pressure and Devicea | Withdrawal Compliance |
|---|---|---|---|---|---|---|---|
| Chotiyarnwong 2020 [31] UK |
RCT Yes |
76 Multiple sclerosis 45.8 31 M; 44 F |
6MWT, Borg RPE, gait speed, BP, HR | 10 min | RIC = 38 (21 M; 17 F) 3x (5 min cuff inflation x 5 min deflation) unilateral arm |
30 mmHg above resting SBP | None |
| CON sRIC = 37 (10 M; 27 F) 3x (5 min cuff inflation x 5 min deflation) unilateral arm |
30 mmHg below resting DBP | 1 | |||||
| Guo 2019 [50] China |
Cohort Self-controlled No |
50 Healthy adults 34.5 ± 12.0 22 M; 26 F |
dCA parameters, MAP, HR, VEGF, GDNF, BDNF, CNF, β-NGF, inflammation-related biomarkers | 2 h | RIC = 48 4x (5 min cuff inflation x 5 min deflation), unilateral arm and leg |
200 mmHg Automatic BP device |
None 2 low coherence |
| CON = 48 No intervention | |||||||
| Incognito 2017 [51] Canada |
RCT Yes |
37 Healthy men 24 ± 5 37 M; 0 F |
MAP, HR, SV, CO, TVC, MSNA |
No clear time description | RIC = 21 3x (5 min cuff inflation x 5 min deflation), unilateral left arm |
200 mmHg | None |
| CON sRIC = 16 3x (5min cuff inflation x 5 min deflation), unilateral left arm |
20 mmHg | ||||||
| Kepler 2019 [52] Estonia |
RCT Yes |
90 Vascular Surgery 66.5 66 M; 24 F |
PWV, AIx, BP, HR, elasticity indices of arteries | 20–28 h post-op | RIC = 44 (36 M; 8 F) 4x (5 min cuff inflation x 5 min deflation), unilateral arm |
200 mmHg or 20 mmHg above SBP ≥ 180 mmHg | None |
| CON sRIC = 46 (30 M; 16 F) 4x (5min cuff inflation x 5 min deflation), unilateral arm |
10–20 mmHg | ||||||
| Kuusik 2019 [53] Estonia |
RCT Yes |
102 Peripheral artery disease 65.6 81 M; 21 F |
PWV, AIx, PP, SVR, BP, HR, elasticity indices of arteries | 24 h | RIC = 47 (33 M; 14 F) 4x (5min cuff inflation x 5 min deflation), unilateral arm |
200 mmHg or 20 mmHg above SBP ≥ 180 mmHg | 7 |
| CON sRIC = 55 (48 M; 7 F) 4x (5min cuff inflation x 5 min deflation), unilateral arm |
20 mmHg | 2 | |||||
| Li 2013 [54] China |
RCT Yes |
62 Abdominal aortic aneurysm repair 64.5 55 M; 7 F |
a/A ratio, A-aDO2 PaCO2, PaO2, IR, arterial pH, lung compliance, CVP, MAP, HR, biomarkers of intestinal injury, oxidative stress and inflammation |
30 min | RIC = 31 (29 M; 2 F) 3x (5min cuff inflation x 5 min deflation), unilateral left arm |
200 mmHg | None |
| CON = 31 (26 M; 5 F) deflated cuff for 30 min | 0 mmHg | ||||||
| Li 2014 [55] China |
RCT Yes |
216 Thoracic pulmonary resection under one-lung ventilation 57.5 158 M; 58 F |
a/A ratio, A-aDO2 PaCO2, PaO2/FiO2, IR, arterial pH, lung compliance, CVP, MAP, HR, biomarkers of oxidative stress & inflammation, incidence of in-hospital complications |
30 min | RIC = 108 (82 M; 26 F) 3x (5min cuff inflation x 5 min deflation), unilateral left arm |
200 mmHg Automated cuff-inflator |
None |
| CON = 108 (76 M; 32 F) deflated cuff for 30 min | 0 mmHg Automated cuff-inflator |
||||||
| Muller 2019 [56] Germany |
RCT (Crossover) Yes |
40 Healthy adults 25.6 ± 2.8 17 M; 23 F |
BP, HR, arterial stiffness (Central systolic BP and PWV) | 30 min | RIC = 40 3x (5min cuff inflation x 5 min deflation), unilateral leg (right thigh) |
200 mmHg | None |
| CON sRIC = 40 3x (5min cuff inflation x 5 min deflation), unilateral right arm |
40 mmHg | ||||||
| Xu 2018 [58] China |
RCT Yes |
17 Coronary heart disease RIC 65.88 ± 4.99 CON 65.25 ± 5.52 6 M; 11 F |
BP, HR | No clear time description | RIC = 9 3x (5min cuff inflation x 5 min deflation), unilateral leg (left thigh) |
Not specified (vascular Doppler revealed no blood flow) | None |
| CON = 8 deflated cuff | Unrestricted blood flow | ||||||
| Zagidulin 2016 [57] Russia |
RCT (Crossover) Yes |
20 Healthy adults 58.2 ± 2.49 16 M; 4 F |
BP, HR and HR variability, oxygen saturation, arterial stiffness, PWV | No clear time description | RIC = 20 3x (5min cuff inflation x 5 min deflation), unilateral arm |
50 mmHg above participant's predetermined SBP | None |
| CON sRIC = 20 3x (5min cuff inflation x 5 min deflation), unilateral arm |
Participant's predetermined DBP | ||||||
| 30 Coronary heart disease 63.9 ± 1.6 21 M; 9 F |
No clear time description | RIC = 30 3x (5min cuff inflation x 5 min deflation), unilateral arm |
50 mmHg above participant's predetermined SBP | None | |||
| CON sRIC = 30 3x (5min cuff inflation x 5 min deflation), unilateral arm |
Participant's predetermined DBP |
A-aDO2: alveolar–arterial oxygen tension difference, a/A ratio: arterial–alveolar ratio, BP: blood pressure, BDNF: brain-derived neurotrophic factor, CNF: ciliary neurotrophic factor, β-NGF: beta-nerve growth factor, CO: cardiac output, CON: control, CVP: central venous pressure, dCA: dynamic cerebral autoregulation, GDNF: glial cell line–derived neurotrophic factor, F: female, HR: heart rate, RI: respiratory index M: male, MA: meta-analysis, MAP: mean arterial pressure, MSNA: muscle sympathetic nerve activity, PaCO2: arterial carbon dioxide partial pressure, PaO2: arterial oxygen partial pressure, PaO2/FIO2: ratio of arterial oxygen partial pressure to fractional inspired oxygen, PD: phase difference, PP: pulse pressure, PWV: pulse wave velocity, RIC, remote ischaemic conditioning; RPE: rate of perceived exertion, 6MWT: 6-min walk test, SV: stroke volume, SVR: systemic vascular resistance, TVC: total vascular conductance, VEGF: vascular endothelial growth factor, yr: years.
All studies used a manual BP cuff (sphygmomanometer) unless stated otherwise. Cuff deflation = reperfusion; cuff inflation = ischaemia.
Eight repeat RIC exposure studies [[59], [60], [61], [62], [63], [64], [65], [66]] were considered in this systematic review including two cohort studies [60,65]. Only 5 RCTs [59,[61], [62], [63],66] were pooled in the meta-analysis for reported repeat RIC effect. Five studies [[60], [61], [62],65,66] conducted repeated RIC in healthy individuals while three others conducted repeated RIC in patient with chronic heart disease [59], compensated chronic heart failure [64] and type 2 diabetes mellitus (T2DM) [63]. The study duration spanned from one week to 3 months; the frequency of RIC administration ranged from a daily application to 3 times per week. Repeated RIC protocols varied from 3 to 6 cycles with 3- to 5-min cuff inflation-induced ischaemia at similar pressure of 200–220 mmHg across studies. Participants’ compliance to RIC protocols varied from 92 to 100% and male subjects were in the majority of included studies. The characteristics of the repeat RIC exposure included studies are summarized in Table 2.
Table 2.
Repeat RIC – Characteristics of included studies.
| Study/Year/Country | Design/MA inclusion | Population – Age (years) – Sex |
Outcome measures | Duration Frequency per week |
Treatment groups and protocol | Ischaemic pressure Device∗ | Withdrawal Compliance |
|---|---|---|---|---|---|---|---|
| Banks 2016 [65] Canada |
Cohort No |
10 Sedentary healthy adults 18 - 35 (24 ± 4) 6 M and 4 F |
BP, HR, peak VO2, cardiac and skeletal muscle energetics | 9 days Daily |
4x (5 min caff inflation x 5 min caff deflation) unilateral right arm | 200 mmHg | None 100% |
| Chen 2019 [59] China |
RCT Yes |
55 Coronary heart disease 50–70 (64.44 ± 8.28) 31 M and 24 F |
BP, MAP, cardiac structure and function, VEGF |
3 months 5 days per week |
RIC = 18 (9 M; 9 F) 3x (3 min cuff inflation x 5 min cuff deflation) bilateral arm |
Not reported | Not reported 92% |
| 3 months 2 session daily for 5 days per week |
IET = 19 (11 M; 8 F) 10x (1 min 40–50% MVC x 1 min rest) bilateral HGT as one session |
40–50% MVC handgrip dynamometer | |||||
| CON = 18 (11 M; 7 F) No exercise but only drug treatment |
|||||||
| Herrod 2019 [66] UK |
RCT Yes |
30 Healthy pre-menopausal sedentary women 20 - 50 (37.9 ± 7.9) |
BP, FMD, CPET parameters | 4 weeks 3 days per week |
RIC = 10 3x (3 min cuff inflation x 3 min cuff deflation) unilateral right arm |
200 mmHg | None 100% |
| IET = 10 4x (2 min 30% MVC x 2 min rest) unilateral right arm HGT |
30% MVC handgrip dynamometer | ||||||
| CON = 10 No intervention |
|||||||
| Jones 2014 [60] UK |
Cohort No |
13 Active healthy men 22 ± 2 |
FMD, MAP, CVC | 7 days Daily |
4x (5 min cuff inflation x 5 min deflation), unilateral dominant arm | 220 mmHg | None 100% |
| Jones 2015 [61] UK |
RCT Yes |
18 Active healthy men RIC 22.4 ± 2.3 CON 26.0 ± 4.8 |
FMD, MAP, CVC, peak VO2 | 8 weeks 3 days per week |
RIC = 8 4x (5min cuff inflation x 5 min deflation), unilateral arm |
220 mmHg | 2 (1 each group) 96% |
| CON = 8 No intervention |
|||||||
| Kimura 2007 [62] Japan |
RCT Yes |
30 Healthy men PC arm 28.1 ± 3.9 CL arm 27.3 ± 4.0 |
FBF, VEGF, BP, HR, serum lipid profile | 4 weeks Daily |
RICPC arm = 10 6x (5min cuff inflation x 5 min deflation) per day, preconditioned arm |
200 mmHg | None 100% |
| RICCL arm = 10 6x (5min cuff inflation x 5 min deflation) per day, contralateral arm |
200 mmHg | ||||||
| CON = 10 No intervention |
|||||||
| Maxwell 2019 [63] UK |
RCT Yes |
21 T2DM RIC 58.8 ± 7.4 CON 59.7 ± 9.6 13 M and 8 F |
FMD, BP, MAP, PetCO2, partial pressure of end tidal carbon dioxide, MCAv, CbVC | 7 days Daily |
RIC = 11 (6 M; 5 F) 4x (5min cuff inflation x 5 min deflation), unilateral arm |
220 mmHg | None 96% |
| CON = 10 (7 M; 3 F) No intervention |
|||||||
| Pryds 2017 [64] Denmark |
RCT (parallel group study) No |
43 Cardiovacular disease RIC1 66 ± 9.7 RIC2 63.1 ± 6.3 |
LVF, CPET parameters, skeletal muscle function, BP, HR, NT-proBNP |
4 weeks Daily |
RIC1 = 22 CIHF (20 M; 2 F) 4x (5 min cuff inflation x 5 min deflation), unilateral |
Auto RIC device | None |
| RIC2 = 21 matched CON non-CIHF (17 M; 4 F) 4x (5 min cuff inflation x 5 min deflation) unilateral |
Auto RIC device | None |
Cuff deflation = reperfusion; Cuff inflation = ischaemia.
BP: blood pressure, CPET: cardiopulmonary exercise test, CbVC: cerebral vascular conductance, CIHF: chronic ischaemic heart failure, CL arm: contralateral arm, CVC: cutaneous vascular conductance, FBF: forearm blood flow, FMD: flow-mediated dilatation, HG: handgrip training, IET: isometric exercise training, LVF: left ventricular function, MAP: mean arterial pressure, MCAv: middle cerebral artery velocity, NT-proBNP: N-terminal pro-brain natriuretic peptide, PetCO2: partial pressure of end tidal carbon, PC arm: preconditioned, RIC: remote ischaemic conditioning, T2DM: type 2 diabetes mellitus, VEGF: vascular endothelial growth factor.
3.2. Acute RIC exposure
BP parameters and HR were available in all the acute RIC exposure included studies except three studies [50,54,55] that reported only MAP and HR results.
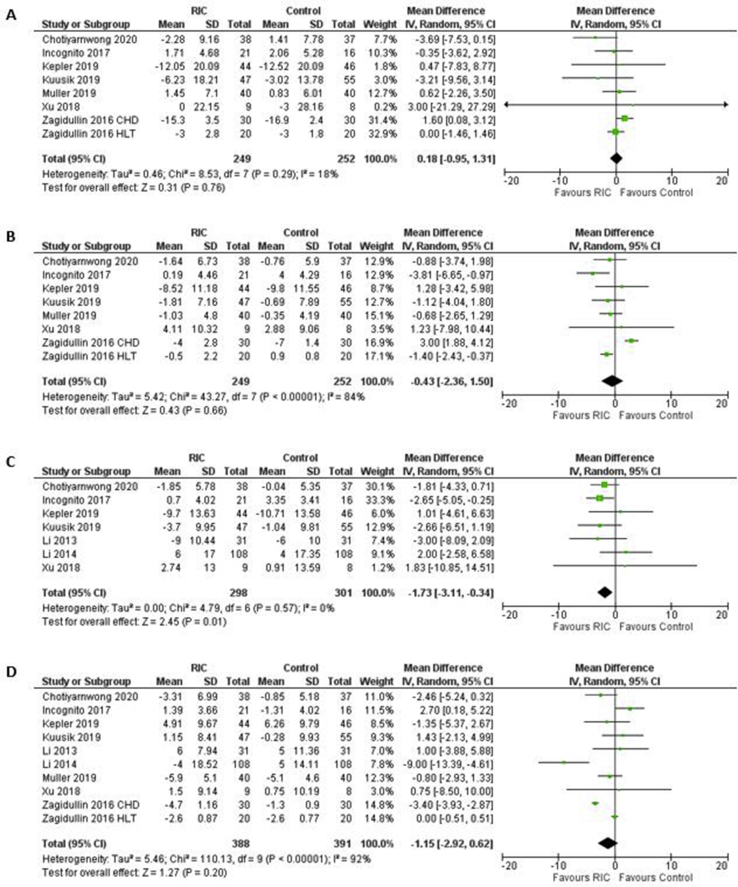
Systolic and diastolic BP data were available in 7 studies [31,[51], [52], [53],[56], [57], [58]] and 8 comparisons were included in the meta-analysis. There was no significant change in systolic BP (MD = 0.18 mmHg [95%CI -0.95 to 1.31; p = 0.76]) and diastolic BP (MD = −0.43 mmHg [95%CI -2.36 to 1.50; p = 0.66]). Seven studies reported MAP [31,[51], [52], [53], [54], [55],58] and there was a significant reduction in MAP with MD -1.73 mmHg (95%CI -3.11 to −0.34; p = 0.01). Nine studies (10 comparisons) reported HR; there was no significant change in HR (MD -1.15 bpm [95%CI -2.92 to 0.62; p = 0.20]). See Fig. 2 for changes in BP and HR after acute RIC exposure.
Fig. 2.
Changes in systolic and diastolic BP, MAP and HR after acute RIC exposure. Forest plots showing the effects of acute RIC exposure on systolic BP (A), diastolic BP (B), MAP (C) and HR (D). A p-value < 0.05 represents a significant pooled mean difference of overall effect. Horizontal lines across each present 95% CI for each study. The diamond represents the 95% CI for pooled estimates of effect of mean difference. CHD: chronic heart disease group; HLT: healthy group; IV: inverse variance; RIC: remote ischaemic conditioning; SD: standard deviation; Total: number of participants.
3.3. Repeat RIC exposure
Outcome measures of interest were reported by 5 repeat RIC exposure studies [59,[61], [62], [63],66] and were included in data pooling.
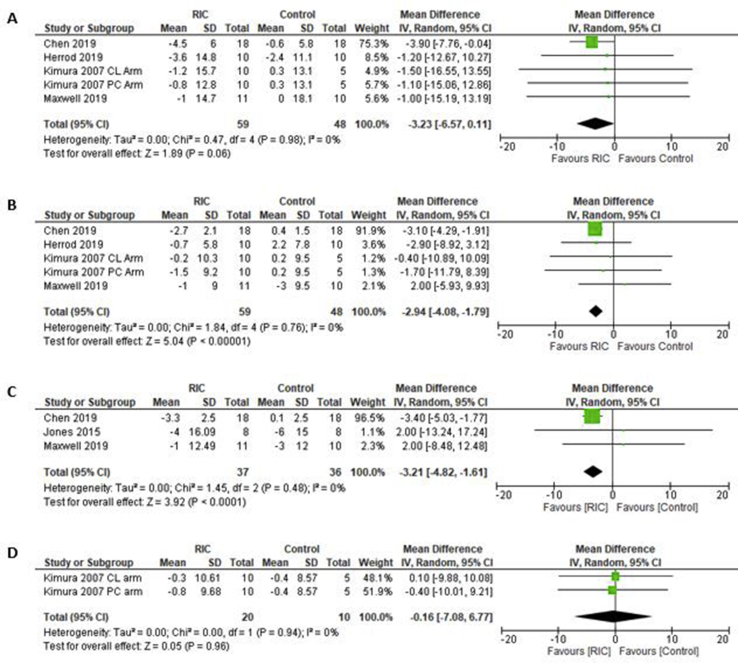
Systolic and diastolic BP data were available in 4 studies [59,62,63,66] with 5 comparisons, totaling 107 participants. Systolic BP was non-significantly reduced with MD -3.23 mmHg (95%CI -6.57 to 0.11; p = 0.06); whereas diastolic BP was significantly reduced with MD -2.94 mmHg (95%CI -4.08 to –1.79; p < 0.00001). MAP was reported in 3 studies [59,61,63], totaling 73 participants, and significantly reduced with MD -3.21 mmHg (95%CI -4.82 to −1.61; p < 0.0001). Only one study [62] (2 comparisons) reported HR; there was no change in MD with −0.16 bpm (95%CI -7.08 to 6.77; p = 0.96) (Fig. 3).
Fig. 3.
Changes in systolic and diastolic BP, MAP and HR after repeat RIC exposure. Forest plots showing the effects of repeat RIC exposure on systolic blood pressure (A) and diastolic BP (B), MAP (C) and HR (D). A p-value < 0.05 represents a significant pooled mean difference of overall effect. Horizontal lines across each present 95% CI for each study. The diamond represents the 95% CI for pooled estimates of effect of mean difference. CL: contralateral arm; IV: inverse variance; PC: preconditioned; SD: standard deviation; Total: number of participants.
Three studies were included in the qualitative synthesis. The cohort study by Banks et al. [65] reported no change in systolic and diastolic BP in healthy adults after 9 days of RIC intervention. A parallel group study conducted by Pryds et al. [64] showed a significant reduction in systolic BP and non-significant reduction in diastolic BP. One cohort study by Jones et al. [60] reported reduced MAP after 7 days of RIC intervention that was sustained 8 days post RIC intervention in healthy men. Two studies reported on HR [64,65] with no significant changes post intervention.
3.4. Sub-analyses
The sub-analysis of all studies – acute versus repeat RIC – showed a non-significant reduction in systolic and diastolic BP and HR. Only MAP was significantly reduced with MD -2.36 mmHg (95%CI -3.41 to −1.31; p < 0.0001) (Supplementary Fig. S1).
For acute RIC, a sub-analysis of healthy patients versus patients receiving hypertension treatment revealed a significant decrease in DBP in the healthy patients (3 studies) with MD -1.6 mmHg (95%CI -2.91 to −0.29; p = 0.02); HR decreased in patients receiving hypertension treatment (7 studies) with MD -2.25 bpm (95%CI -4.38 to −0.12; p = 0.04) (Supplementary Fig. S2).
For repeat RIC, a sub-analysis of healthy patients versus patients receiving hypertension treatment revealed a significant decrease in SBP and MAP for patients receiving treatment (2 studies) with SBP MD -3.7 mmHg (95%CI -7.42 to 0.02; p = 0.05) and MAP MD -3.27 mmHg (95%CI -4.89 to −1.66; p = 0.05) (Supplementary Fig. S3).
3.5. Heterogeneity and publication bias
In general, acute and repeat RIC exposure studies demonstrated a low heterogeneity (I2 = 0%–18%. Heterogeniety was high in acute RIC exposure studies for diastolic BP (I2 = 84%) and HR (I2 = 91%). Egger plots showed minimal evidence of bias (Supplementary Figs. S4 and S5).
3.6. Study quality
The median JADAD scores for acute RIC and repeat RIC exposure included studies were 4 out of a maximum of 5. All trials were of high quality with only two acute RIC exposure studies and two repeat RIC exposure studies not describing the method of randomisation or blinding (Supplementary Tables S2 and S3).
4. Discussion
Our work expands on the previous work of Epps et al. [16] on repeat RIC for improved cardiovascular function. The major findings of this systematic review were: First, the meta-analyses from all studies suggested that acute and repeat RIC exposure decreases MAP; second, repeat RIC exposure has the potential to lower diastolic blood pressure; and third, relatively fewer studies have been conducted on repeat RIC exposure, compared to acute RIC. This analysis may currently be underpowered due to the limited number of studies and sample sizes included in this meta-analysis.
Our analysis of acute RIC exposure showed that the typical delivery method was 3–4 cycles of 5-min ischaemic periods interspersed with 5-min reperfusion periods in each single session. However, 3 cycles of alternated ischaemic and reperfusion periods per session was adopted in the majority of studies. In contrast, for chronic effects, although our analyses did not clarify the optimal delivery method for repeat RIC exposure, it appears that the majority of the studies adopted four RIC cycles of 5-min (ischaemic period) interspersed with 5-min reperfusion or rest intervals during each session. Sessions were performed either daily or at least 3 days per week in the case of repeat RIC exposure, except in two studies [59,66] which used a 3 times 3-min ischaemia protocol. Preferably, 4 times 5-min exposure appears to be most common application method, at least for lowering blood pressure in people with chronic disease. This intervention shows promise as an adjunct treatment for hypertension management. Despite the relatively few studies, most individual studies have reported anti-hypertensive effects of systolic, diastolic and mean arterial blood pressure following participants’ exposure to repeat RIC. The anti-hypertensive effect was sustained for at least one week after cessation of exposure to RIC [60,63].
Repeat remote ischaemic conditioning delivers clinically meaningful blood pressure reductions and has potential as an adjunct therapeutic modality for controlling blood pressure. Repeat RIC is easy to use/apply, appropriate for people with mobility issues, and requires less time commitment (about 35 min per session) than aerobic exercise. Moreover, repeat RIC can be performed anywhere at an individual's convenience providing exceptional flexibility. While RIC has mostly been utilized in a clinical setting, as no adverse events have been reported, there is no obvious reason why individuals cannot obtain a blood pressure cuff and self-administer the RIC protocol. Madias [19], for example, made extensive, self-administered, use of RIC when collecting data for publication.
4.1. Effect of acute versus repeat RIC outcome responses
Our meta-analysis showed no significant changes in systolic and diastolic BP or HR following acute RIC exposure but MAP was significantly reduced. It is possible that a single session of RIC is insufficient to reduce blood pressure. It is widely accepted that in the period immediately following physiological stress (e.g. exercise or RIC) there is an acute hypotensive response that can be quite pronounced, but blood pressure often returns to baseline levels within a matter of hours [67]. It is therefore perhaps unsurprising to note that the acute RIC response is less than that observed from repeated exposure; the acute response is likely to be both more variable and transient, which may explain the higher heterogeneity. In contrast, the accumulated repeat effect confirms the anti-hypertensive benefit of repeat RIC. The magnitude of the reduction is similar to those reported by other exercise modalities (e.g. endurance exercise) [68]. There were observed reductions (~3 mmHg) in systolic and diastolic blood pressure and MAP across the included studies combining both healthy individuals and patients with chronic disease. Some of these patients were treated with anti-hypertension medication which is unlikely to have influenced the magnitude of RIC's pressor effect. For both, acute and repeat RIC, the sub-analyses of healthy versus patients treated with anti-hypertension medication showed mixed results. For healthy individuals DBP decreased with acute but not repeat RIC. For patients receiving hypertension treatment SBP and MAP decreased with repeat RIC. The limited number of studies and patient numbers are most likely responsible. Moreover, exercise training increases an individual's ability to exercise in terms of intensity and duration that may augment the acute response providing more and lasting post-exercise hypotensive effect over time, which explains the possible interaction between acute and chronic exercise [67]. These results show promise for future research to substantiate these benefits.
Overall, repeat RIC significantly reduced diastolic BP and MAP by about 3 mmHg. This should be considered clinically meaningful since a reduction in diastolic BP is beneficial for individuals with isolated elevation of diastolic BP. This is equally important as reducing systolic BP as isolated elevation of diastolic BP is more closely related to end-organ damage [69]. Staley et al. [70] found increased diastolic BP to be associated with the reduction of executive functioning performance in cognitively healthy older adults which highlights increased DBP as a risk factor for neurodegeneration. Also, a higher DBP has been associated with a higher bleeding risk in patients with nonvalvular atrial fibrillation [71]. Although, systolic BP has been known to have greater effect for BP control [72], both systolic and diastolic BP independently influenced cardiovascular outcomes, therefore diastolic BP should not to be overlooked [73].
Qualitative synthesis revealed that there were observed BP reductions in individual repeat RIC studies [60,64], with the exception of the Banks et al. [65] study. Banks et al. [65] reported no change in BP, although they exposed participants to repeated RIC similar to Jones et al. [60] and Maxwell et al. [63] using the 4 × (5 min cuff inflation x 5 min deflation) for a duration of approximately one week with equal frequency. A possible explanation for these conflicting results could be the (1) difference in populations with respect to the gender distribution that was predominantly male compared to Banks et al. [65]; (2) Ischaemic inflation pressure difference applied during the RIC exposure. Both Jones et al. [60] and Maxwell et al. [63] employed 220 mmHg inflation pressure while Banks et al. [65] used the standard 200 mmHg ischaemic inflation pressure; (3) the occurrence of a possible “floor” effect for BP reduction as participants of the Banks et al. study had lower systolic BP at baseline; and (4) method of BP measurement employed since the position (both body and arm) assumed by an individual influences variations in BP measurements [74,75] – the varying distances between the heart level and the arm support of the chair, can be large depending on the height of the person (e.g. it can be larger than 25 cm in tall persons) [75]. BP devices use a different measuring technique (i.e. auscultatory, automated, oscillometric and ultrasound) and the location has an effect on the BP measurement. Although the brachial artery is the standard location for BP measurement, other devices measure pressure at the wrist and fingers. However, it is important to know that at different parts of the arterial tree, systolic and diastolic pressures differ considerably – while systolic pressure rises more in distal arteries, diastolic pressure declines [74]. Regardless, the use of BP monitoring devices may be preferred in certain situations.
4.2. Limitations
The major limitations of this review are (i) the small sample size in the included studies; and (ii) not all studies provided data suitable for pooling. Another significant limitation is the fact that we could not perform sub-analysis to determine the difference in result with regards to the effect of age, population (health and unhealthy), frequency of RIC exposure and duration of study. Although, the protocols for RIC application varied across studies, this allowed the differing protocols characteristics to be related to the presence or absence of beneficial effect on the blood pressure variables. Our study may have been underpowered by the sample size to detect a statistically significant mean reduction difference in systolic blood pressure.
5. Conclusions
The available literature indicates that acute RIC exposure does not alter blood pressure, but repeated RIC may have beneficial anti-hypertensive effects. Our work suggests repeat RIC may be a safe, effective, economical and simple therapy to manage blood pressure, offering venue flexibility and manageable time commitment, for both healthy and clinical individuals that could be adopted as an adjunct treatment modality. Given the limited data availability on the effects of RIC exposure in blood pressure management as well as other cardiovascular variables, more research is warranted.
Funding
None.
Declaration of competing interest
None of the authors declare any conflicts of interest.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.ijchy.2021.100081.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- 1.Marek-Trzonkowska N., Kwieczyńska A., Reiwer-Gostomska M., Koliński T., Molisz A., Siebert J. Arterial hypertension is characterized by imbalance of pro-angiogenic versus anti-angiogenic factors. PloS One. 2015;10(5) doi: 10.1371/journal.pone.0126190. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.GBD 2017 Causes of Death Collaborators Global, regional, and national age-sex-specific mortality for 282 causes of death in 195 countries and territories, 1980–2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2018;392(10159):1736–1788. doi: 10.1016/s0140-6736(18)32203-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Harrap S.B., Lung T., Chalmers J. New blood pressure guidelines pose difficult choices for Australian physicians. Circ. Res. 2019;124(7):975–977. doi: 10.1161/CIRCRESAHA.118.314637. [DOI] [PubMed] [Google Scholar]
- 4.Nguyen B., Bauman A., Ding D. Association between lifestyle risk factors and incident hypertension among middle-aged and older Australians. Prev. Med. 2019;118:73–80. doi: 10.1016/j.ypmed.2018.10.007. [DOI] [PubMed] [Google Scholar]
- 5.Whelton P.K., Carey R.M., Aronow W.S., Casey D.E., Collins K.J., Himmelfarb C.D., DePalma S.M., Gidding S., Jamerson K.A., Jones D.W. 2017 ACC/AHA/AAPA/ABC/ACPM/AGS/APhA/ASH/ASPC/NMA/PCNA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults. A report of the American College of Cardiology/American Heart Association task force on clinical practice guidelines. J. Am. Coll. Cardiol. 2018;71(19):e127–e248. doi: 10.1016/j.jacc.2017.11.006. [DOI] [PubMed] [Google Scholar]
- 6.Williams B., Mancia G., Spiering W., Agabiti Rosei E., Azizi M., Burnier M., Clement D.L., Coca A., De Simone G., Dominiczak A. 2018 ESC/ESH guidelines for the management of arterial hypertension. The task force for the management of arterial hypertension of the European society of cardiology (ESC) and the European society of hypertension (ESH) Eur. Heart J. 2018;39(33):3021–3104. doi: 10.1093/eurheartj/ehy339. [DOI] [PubMed] [Google Scholar]
- 7.Aucott L., Poobalan A., Smith W.C.S., Avenell A., Jung R., Broom J. Effects of weight loss in overweight/obese individuals and long-term hypertension outcomes: a systematic review. Hypertension. 2005;45(6):1035–1041. doi: 10.1161/01.HYP.0000165680.59733.d4. [DOI] [PubMed] [Google Scholar]
- 8.Selçuk K.T., Çevik C., Mercan Y., Koca H. Hypertensive patients' adherence to pharmacological and non-pharmacological treatment methods, in Turkey. Int. J. Community Med. Public Health. 2017;4(8):2648–2657. doi: 10.18203/2394-6040.ijcmph20173308. [DOI] [Google Scholar]
- 9.Stevens V.J., Obarzanek E., Cook N.R., Lee I.-M., Appel L.J., West D.S., Milas N.C., Mattfeldt-Beman M., Belden L., Bragg C. Long-term weight loss and changes in blood pressure: results of the Trials of Hypertension Prevention, phase II. Ann. Intern. Med. 2001;134(1):1–11. doi: 10.7326/0003-4819-134-1-200101020-00007. [DOI] [PubMed] [Google Scholar]
- 10.Carraca E.V., Mackenbach J.D., Lakerveld J., Rutter H., Oppert J.M., De Bourdeaudhuij I., Compernolle S., Roda C., Bardos H., Teixeira P.J. Lack of interest in physical activity - individual and environmental attributes in adults across Europe: the SPOTLIGHT project. Prev. Med. 2018;111:41–48. doi: 10.1016/j.ypmed.2018.02.021. [DOI] [PubMed] [Google Scholar]
- 11.Moschny A., Platen P., Klaaßen-Mielke R., Trampisch U., Hinrichs T. Barriers to physical activity in older adults in Germany: a cross-sectional study. Int. J. Behav. Nutr. Phys. Activ. 2011;8(1):121. doi: 10.1186/1479-5868-8-121. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Reichert F.F., Barros A.J., Domingues M.R., Hallal P.C. The role of perceived personal barriers to engagement in leisure-time physical activity. Am. J. Publ. Health. 2007;97(3):515–519. doi: 10.2105/AJPH.2005.070144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Schutzer K.A., Graves B.S. Barriers and motivations to exercise in older adults. Prev. Med. 2004;39(5):1056–1061. doi: 10.1016/j.ypmed.2004.04.003. [DOI] [PubMed] [Google Scholar]
- 14.Trost S.G., Owen N., Bauman A.E., Sallis J.F., Brown W. Correlates of adults' participation in physical activity: review and update. Med. Sci. Sports Exerc. 2002;34(12):1996–2001. doi: 10.1249/01.MSS.0000038974.76900.92. [DOI] [PubMed] [Google Scholar]
- 15.Shen M., Gao J., Li J., Su J. Effect of ischaemic exercise training of a normal limb on angiogenesis of a pathological ischaemic limb in rabbits. Clin. Sci. (Lond.) 2009;117(5):201–208. doi: 10.1042/cs20080212. [DOI] [PubMed] [Google Scholar]
- 16.Epps J., Dieberg G., Smart N.A. Repeat remote ischaemic pre-conditioning for improved cardiovascular function in humans: a systematic review. Int. J. Cardiol. Heart Vasc. 2016;11:55–58. doi: 10.1016/j.ijcha.2016.03.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Przyklenk K., Bauer B., Ovize M., Kloner R.A., Whittaker P. Regional ischemic 'preconditioning' protects remote virgin myocardium from subsequent sustained coronary occlusion. Circulation. 1993;87(3):893–899. doi: 10.1161/01.cir.87.3.893. [DOI] [PubMed] [Google Scholar]
- 18.Heusch G., Botker H.E., Przyklenk K., Redington A., Yellon D. Remote ischemic conditioning. J. Am. Coll. Cardiol. 2015;65(2):177–195. doi: 10.1016/j.jacc.2014.10.031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Madias J.E. Sustained blood pressure lowering effect of twice daily remote ischemic conditioning sessions in a normotensive/prehypertensive subject. Int. J. Cardiol. 2015;182:392–394. doi: 10.1016/j.ijcard.2014.12.159. [DOI] [PubMed] [Google Scholar]
- 20.Pell T.J., Baxter G.F., Yellon D.M., Drew G.M. Renal ischemia preconditions myocardium: role of adenosine receptors and ATP-sensitive potassium channels. Am. J. Physiol. 1998;275(5):H1542–H1547. doi: 10.1152/ajpheart.1998.275.5.H1542. [DOI] [PubMed] [Google Scholar]
- 21.Kharbanda R.K., Mortensen U.M., White P.A., Kristiansen S.B., Schmidt M.R., Hoschtitzky J.A., Vogel M., Sorensen K., Redington A.N., MacAllister R. Transient limb ischemia induces remote ischemic preconditioning in vivo. Circulation. 2002;106(23):2881–2883. doi: 10.1161/01.cir.0000043806.51912.9b. [DOI] [PubMed] [Google Scholar]
- 22.Crimi G., Pica S., Raineri C., Bramucci E., De Ferrari G.M., Klersy C., Ferlini M., Marinoni B., Repetto A., Romeo M., Rosti V., Massa M., Raisaro A., Leonardi S., Rubartelli P., Oltrona Visconti L., Ferrario M. Remote ischemic post-conditioning of the lower limb during primary percutaneous coronary intervention safely reduces enzymatic infarct size in anterior myocardial infarction: a randomized controlled trial, JACC Cardiovasc. Interv. 2013;6(10):1055–1063. doi: 10.1016/j.jcin.2013.05.011. [DOI] [PubMed] [Google Scholar]
- 23.McLeod S.L., Iansavichene A., Cheskes S. Remote ischemic perconditioning to reduce reperfusion injury during acute ST-segment–elevation myocardial infarction: a systematic review and meta-analysis. J. Am. Heart Assoc. 2017;6(5) doi: 10.1161/JAHA.117.005522. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Pilcher J.M., Young P., Weatherall M., Rahman I., Bonser R.S., Beasley R.W. A systematic review and meta-analysis of the cardioprotective effects of remote ischaemic preconditioning in open cardiac surgery. J. R. Soc. Med. 2012;105(10):436–445. doi: 10.1258/jrsm.2012.120049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Domanski M.J., Mahaffey K., Hasselblad V., Brener S.J., Smith P.K., Hillis G., Engoren M., Alexander J.H., Levy J.H., Chaitman B.R. Association of myocardial enzyme elevation and survival following coronary artery bypass graft surgery. J. Am. Med. Assoc. 2011;305(6):585–591. doi: 10.1001/jama.2011.99. [DOI] [PubMed] [Google Scholar]
- 26.Adabag A.S., Rector T., Mithani S., Harmala J., Ward H.B., Kelly R.F., Nguyen J.T., McFalls E.O., Bloomfield H.E. Prognostic significance of elevated cardiac troponin I after heart surgery. Ann. Thorac. Surg. 2007;83(5):1744–1750. doi: 10.1016/j.athoracsur.2006.12.049. [DOI] [PubMed] [Google Scholar]
- 27.Meng R., Ding Y., Asmaro K., Brogan D., Meng L., Sui M., Shi J., Duan Y., Sun Z., Yu Y., Jia J., Ji X. Ischemic conditioning is safe and effective for octo- and nonagenarians in stroke prevention and treatment. Neurotherapeutics. 2015;12(3):667–677. doi: 10.1007/s13311-015-0358-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Jean-St-Michel E., Manlhiot C., Li J., Tropak M., Michelsen M.M., Schmidt M.R., McCrindle B.W., Wells G.D., Redington A.N. Remote preconditioning improves maximal performance in highly trained athletes. Med. Sci. Sports Exerc. 2011;43(7):1280–1286. doi: 10.1249/MSS.0b013e318206845d. (Remote ischemic preconditioning)(Report) [DOI] [PubMed] [Google Scholar]
- 29.Cruz R.S.d.O., Aguiar R.A.d., Turnes T., Pereira K.L., Caputo F. Effects of ischemic preconditioning on maximal constant-load cycling performance. J. Appl. Physiol. 2015;119(9):961–967. doi: 10.1152/japplphysiol.00498.2015. [DOI] [PubMed] [Google Scholar]
- 30.Cruz R.S.d.O., Aguiar R.A.d, Turnes T., Salvador A.F., Caputo F. Effects of ischemic preconditioning on short-duration cycling performance. Appl. Physiol. Nutr. Metabol. 2016;41:825+. doi: 10.1139/apnm-2015-0646. [DOI] [PubMed] [Google Scholar]
- 31.Chotiyarnwong C., Nair K., Angelini L., Buckley E., Mazza C., Heyes D., Ramiz R., Baster K., Ismail A., Das J., Ali A., Lindert R., Sharrack B., Price S., Paling D. Effect of remote ischaemic preconditioning on walking in people with multiple sclerosis: double-blind randomised controlled trial. BMJ Neurology Open. 2020;2(1) doi: 10.1136/bmjno-2019-000022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Madias J.E. Effect of serial arm ischemic preconditioning sessions on the systemic blood pressure of a normotensive subject. Med. Hypotheses. 2011;76(4):503–506. doi: 10.1016/j.mehy.2010.12.002. [DOI] [PubMed] [Google Scholar]
- 33.Madias J.E., Koulouridis I. Effect of repeat twice daily sessions of remote ischemic conditioning over the course of one week on blood pressure of a normotensive/prehypertensive subject. Int. J. Cardiol. 2014;176(3):1076–1077. doi: 10.1016/j.ijcard.2014.07.132. [DOI] [PubMed] [Google Scholar]
- 34.Deng Q.-W., Xia Z.-Q., Qiu Y.-X., Wu Y., Liu J.-X., Li C., Liu K.-X. Clinical benefits of aortic cross-clamping versus limb remote ischemic preconditioning in coronary artery bypass grafting with cardiopulmonary bypass: a meta-analysis of randomized controlled trials. J. Surg. Res. 2015;193(1):52–68. doi: 10.1016/j.jss.2014.10.007. [DOI] [PubMed] [Google Scholar]
- 35.Piercy K.L., Troiano R.P., Ballard R.M., Carlson S.A., Fulton J.E., Galuska D.A., George S.M., Olson R.D. The physical activity guidelines for Americans. J. Am. Med. Assoc. 2018;320(19):2020–2028. doi: 10.1001/jama.2018.14854. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Sardar P., Chatterjee S., Kundu A., Samady H., Owan T., Giri J., Nairooz R., Selzman C.H., Heusch G., Gersh B.J., Abbott J.D., Mukherjee D., Fang J.C. Remote ischemic preconditioning in patients undergoing cardiovascular surgery: evidence from a meta-analysis of randomized controlled trials. Int. J. Cardiol. 2016;221:34–41. doi: 10.1016/j.ijcard.2016.06.325. [DOI] [PubMed] [Google Scholar]
- 37.Takagi H., Manabe H., Kawai N., Goto S.-n., Umemoto T. Review and meta-analysis of randomized controlled clinical trials of remote ischemic preconditioning in cardiovascular surgery. Am. J. Cardiol. 2008;102(11):1487–1488. doi: 10.1016/j.amjcard.2008.07.036. [DOI] [PubMed] [Google Scholar]
- 38.Takagi H., Umemoto T. Remote ischemic preconditioning for cardiovascular surgery: an updated meta-analysis of randomized trials. Vasc. Endovasc. Surg. 2011;45(6):511–513. doi: 10.1177/1538574410379654. [DOI] [PubMed] [Google Scholar]
- 39.Wang S., Li H., He N., Sun Y., Guo S., Liao W., Liao Y., Chen Y., Bin J. Impact of remote ischaemic preconditioning on major clinical outcomes in patients undergoing cardiovascular surgery: a meta-analysis with trial sequential analysis of 32 randomised controlled trials. Int. J. Cardiol. 2017;227:882–891. doi: 10.1016/j.ijcard.2016.11.278. [DOI] [PubMed] [Google Scholar]
- 40.Xie J., Zhang X., Xu J., Zhang Z., Klingensmith N.J., Liu S., Pan C., Yang Y., Qiu H. Effect of remote ischemic preconditioning on outcomes in adult cardiac surgery: a systematic review and meta-analysis of randomized controlled studies. Anesth. Analg. 2018;127(1):30–38. doi: 10.1213/ANE.0000000000002674. [DOI] [PubMed] [Google Scholar]
- 41.Zhou C., Jeon Y., Meybohm P., Zarbock A., Young P.J., Li L., Hausenloy D.J. Renoprotection by remote ischemic conditioning during elective coronary revascularization: a systematic review and meta-analysis of randomized controlled trials. Int. J. Cardiol. 2016;222:295–302. doi: 10.1016/j.ijcard.2016.07.176. [DOI] [PubMed] [Google Scholar]
- 42.Zhou C., Liu Y., Yao Y., Zhou S., Fang N., Wang W., Li L. β-blockers and volatile anesthetics may attenuate cardioprotection by remote preconditioning in adult cardiac surgery: a meta-analysis of 15 randomized trials. J. Cardiothorac. Vasc. Anesth. 2013;27(2):305–311. doi: 10.1053/j.jvca.2012.09.028. [DOI] [PubMed] [Google Scholar]
- 43.King N., Dieberg G., Smart N.A. Remote ischaemic pre-conditioning does not affect clinical outcomes following coronary Artery bypass grafting. a systematic review and meta-analysis. Clin. Trials Regul. Sci. Cardiol. 2016;17(C):1. doi: 10.1016/j.ctrsc.2016.03.001. (Author abstract) [DOI] [Google Scholar]
- 44.Baffour-Awuah B., Smart N., Dieberg G., Pearson M. 2020. The Effect of Repeat Remote Ischaemic Conditioning on Blood Pressure Response: a Systematic Review and Meta-Analysis.https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD42020180784 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Schünemann H.J., Vist G.E., Higgins J.P., Santesso N., Deeks J.J., Glasziou P., Akl E.A., Guyatt G.H. Chapter 15: interpreting results and drawing conclusions. In: Higgins J., Thomas J., Chandler J., Cumpston M., Li T., Page M., Welch V., editors. Cochrane Handbook for Systematic Reviews of Interventions Version 6.0. John Wiley & Sons; Chichester (UK): 2019. [Google Scholar]
- 46.Egger M., Smith G.D., Schneider M., Minder C. Bias in meta-analysis detected by a simple, graphical test. Br. Med. J. 1997;315(7109):629–634. doi: 10.1136/bmj.315.7109.629. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Higgins J.P., Thompson S.G., Deeks J.J., Altman D.G. Measuring inconsistency in meta-analyses. Br. Med. J. 2003;327(7414):557–560. doi: 10.1136/bmj.327.7414.557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Review Manager (RevMan) [Computer Program] 2020. https://training.cochrane.org/online-learning/core-software-cochrane-reviews/revman/revman-5-download/download-and-installation [Google Scholar]
- 49.Jadad A.R., Moore R.A., Carroll D., Jenkinson C., Reynolds D.J.M., Gavaghan D.J., McQuay H.J. Assessing the quality of reports of randomized clinical trials: is blinding necessary?, Control. Clin. Trials. 1996;17(1):1–12. doi: 10.1016/0197-2456(95)00134-4. [DOI] [PubMed] [Google Scholar]
- 50.Guo Z.N., Guo W.T., Liu J., Chang J., Ma H., Zhang P., Zhang F.L., Han K., Hu H.H., Jin H. Changes in cerebral autoregulation and blood biomarkers after remote ischemic preconditioning. Neurology. 2019;93(1):e8–e19. doi: 10.1212/WNL.0000000000007732. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Incognito A.V., Doherty C.J., Lee J.B., Burns M.J., Millar P.J. Ischemic preconditioning does not alter muscle sympathetic responses to static handgrip and metaboreflex activation in young healthy men. Physiol. Rep. 2017;5(14) doi: 10.14814/phy2.13342. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Kepler T., Kuusik K., Lepner U., Starkopf J., Zilmer M., Eha J., Lieberg J., Vähi M., Kals J. The effect of remote ischaemic preconditioning on arterial stiffness in patients undergoing vascular surgery: a randomised clinical trial. Eur. J. Vasc. Endovasc. Surg. 2019;57(6):868–875. doi: 10.1016/j.ejvs.2018.12.002. [DOI] [PubMed] [Google Scholar]
- 53.Kuusik K., Kepler T., Zilmer M., Eha J., Vahi M., Kals J. Effects of remote ischaemic preconditioning on arterial stiffness in patients undergoing lower limb angiographic procedures: a randomised clinical trial. Eur. J. Vasc. Endovasc. Surg. 2019;58(6):875–882. doi: 10.1016/j.ejvs.2019.06.004. [DOI] [PubMed] [Google Scholar]
- 54.Li C., Li Y.S., Xu M., Wen S.H., Yao X., Wu Y., Huang C.Y., Huang W.Q., Liu K.X. Limb remote ischemic preconditioning for intestinal and pulmonary protection during elective open infrarenal abdominal aortic aneurysm repair: a randomized controlled trial. Anesthesiology. 2013;118(4):842–852. doi: 10.1097/ALN.0b013e3182850da5. [DOI] [PubMed] [Google Scholar]
- 55.Li C., Xu M., Wu Y., Li Y.S., Huang W.Q., Liu K.X. Limb remote ischemic preconditioning attenuates lung injury after pulmonary resection under propofol-remifentanil anesthesia: a randomized controlled study. Anesthesiology. 2014;121(2):249–259. doi: 10.1097/aln.0000000000000266. [DOI] [PubMed] [Google Scholar]
- 56.Muller J., Taebling M., Oberhoffer R. Remote ischemic preconditioning has no short term effect on blood pressure, heart rate, and arterial stiffness in healthy young adults. Front. Physiol. 2019;10 doi: 10.3389/fphys.2019.01094. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Zagidullin N., Scherbakova E., Safina Y., Zulkarneev R., Zagidullin S. The impact of remote ischemic preconditioning on arterial stiffness and heart rate variability in patients with angina pectoris. J. Clin. Med. 2016;5(7) doi: 10.3390/jcm5070060. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Xu Y., Yu Q., Yang J., Yuan F., Zhong Y., Zhou Z., Wang N. Acute hemodynamic effects of remote ischemic preconditioning on coronary perfusion pressure and coronary collateral blood flow in coronary heart disease. Acta Cardiol. Sin. 2018;34(4):299–306. doi: 10.6515/ACS.201807_34(4).20180317A. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Chen W., Ni J., Qiao Z., Wu Y., Lu L., Zheng J., Chen R., Lu X. Comparison of the clinical outcomes of two physiological ischemic training methods in patients with coronary heart disease. Open Med. 2019;14:224–233. doi: 10.1515/med-2019-0016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Jones H., Hopkins N., Bailey T.G., Green D.J., Cable N.T., Thijssen D.H. Seven-day remote ischemic preconditioning improves local and systemic endothelial function and microcirculation in healthy humans. Am. J. Hypertens. 2014;27(7):918–925. doi: 10.1093/ajh/hpu004. [DOI] [PubMed] [Google Scholar]
- 61.Jones H., Nyakayiru J., Bailey T.G., Green D.J., Cable N.T., Sprung V.S., Hopkins N.D., Thijssen D.H. Impact of eight weeks of repeated ischaemic preconditioning on brachial artery and cutaneous microcirculatory function in healthy males. Eur. J. Prev. Cardiol. 2015;22(8):1083–1087. doi: 10.1177/2047487314547657. [DOI] [PubMed] [Google Scholar]
- 62.Kimura M., Ueda K., Goto C., Jitsuiki D., Nishioka K., Umemura T., Noma K., Yoshizumi M., Chayama K., Higashi Y. Repetition of ischemic preconditioning augments endothelium-dependent vasodilation in humans: role of endothelium-derived nitric oxide and endothelial progenitor cells, Arterioscler. Thromb. Vasc. Biol. 2007;27(6):1403–1410. doi: 10.1161/ATVBAHA.107.143578. [DOI] [PubMed] [Google Scholar]
- 63.Maxwell J.D., Carter H.H., Hellsten Y., Miller G.D., Sprung V.S., Cuthbertson D.J., Thijssen D.H.J., Jones H. Seven-day remote ischaemic preconditioning improves endothelial function in patients with type 2 diabetes mellitus: a randomised pilot study. Eur. J. Endocrinol. 2019;181(6):659–669. doi: 10.1530/EJE-19-0378. [DOI] [PubMed] [Google Scholar]
- 64.Pryds K., Nielsen R., Jorsal A., Hansen M., Ringgaard S., Refsgaard J., Petersen A., Bøtker H., Schmidt M. Effect of long-term remote ischemic conditioning in patients with chronic ischemic heart failure. Basic Res. Cardiol. 2017;112(6):1–11. doi: 10.1007/s00395-017-0658-6. [DOI] [PubMed] [Google Scholar]
- 65.Banks L., Wells G.D., Clarizia N.A., Jean-St-Michel E., McKillop A.L., Redington A.N., McCrindle B.W. Short-term remote ischemic preconditioning is not associated with improved blood pressure and exercise capacity in young adults. Appl. Physiol. Nutr. Metabol. 2016;41(8):903–906. doi: 10.1139/apnm-2016-0024. [DOI] [PubMed] [Google Scholar]
- 66.Herrod P.J.J., Blackwell J.E.M., Moss B.F., Gates A., Atherton P.J., Lund J.N., Williams J.P., Phillips B.E. The efficacy of 'static' training interventions for improving indices of cardiorespiratory fitness in premenopausal females. Eur. J. Appl. Physiol. 2019;119(3):645–652. doi: 10.1007/s00421-018-4054-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Hamer M. The anti-hypertensive effects of exercise. Sports Med. 2006;36(2):109–116. doi: 10.2165/00007256-200636020-00002. [DOI] [PubMed] [Google Scholar]
- 68.Cornelissen V.A., Buys R., Smart N.A. Endurance exercise beneficially affects ambulatory blood pressure: a systematic review and meta-analysis. J. Hypertens. 2013;31(4):639–648. doi: 10.1097/HJH.0b013e32835ca964. [DOI] [PubMed] [Google Scholar]
- 69.Blank S.G., Mann S.J., James G.D., West J.E., Pickering T.G. Isolated elevation of diastolic blood pressure. Hypertension. 1995;26(3):383–389. doi: 10.1161/01.HYP.26.3.383. [DOI] [PubMed] [Google Scholar]
- 70.Staley S B., Wei Q G., Amano S., Nolty A., Harrington M. C-09 diastolic blood pressure and executive function in healthy older adults. Arch. Clin. Neuropsychol. 2019;34(6) doi: 10.1093/arclin/acz034.171. 1036-1036. [DOI] [Google Scholar]
- 71.Yu Y., Li M., Zhou W., Wang T., Zhu L., Hu L., Bao H., Cheng X. Diastolic blood pressure achieved at target systolic blood pressure (120-140 mm Hg) and dabigatran-related bleeding in patients with nonvalvular atrial fibrillation: a real-world study. Anatol. J. Cardiol. 2020;24(4):267–273. doi: 10.14744/AnatolJCardiol.2020.11823. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Baffour-Awuah B., Dieberg G., Pearson M.J., Smart N.A. Blood pressure control in older adults with hypertension: a systematic review with meta-analysis and meta-regression. IJCHy. 2020;6:100040. doi: 10.1016/j.ijchy.2020.100040. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Flint A.C., Conell C., Ren X., Banki N.M., Chan S.L., Rao V.A., Melles R.B., Bhatt D.L. Effect of systolic and diastolic blood pressure on cardiovascular outcomes. N. Engl. J. Med. 2019;381(3):243–251. doi: 10.1056/NEJMoa1803180. [DOI] [PubMed] [Google Scholar]
- 74.Ogedegbe G., Pickering T. Principles and techniques of blood pressure measurement. Cardiol. Clin. 2010;28(4):571–586. doi: 10.1016/j.ccl.2010.07.006. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Netea R.T., Lenders J.W.M., Smits P., Thien T. Both body and arm position significantly influence blood pressure measurement. J. Hum. Hypertens. 2003;17(7):459–462. doi: 10.1038/sj.jhh.1001573. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.