Abstract
A 69-year-old man presented with a left pleural effusion. Even after repeated drainage, the pleural effusion had been increasing for more than two years. Thoracoscopy unexpectedly showed a pleural mass on the parietal pleura, and it was completely removed. The diagnosis was pleural capillary hemangioma, and the effusion has not recurred after the resection. Pleural hemangioma is one of the crucial differential diagnoses of refractory pleural effusion.
Keywords: Capillary hemangioma, Pleural effusion, Refractory, Nonspecific pleuritis
Highlights
-
•
Not a few cases are followed as non-specific pleuritis.
-
•
Pleural hemangioma causes refractory but curable pleural effusion.
-
•
If a pleural effusion remains over a year, thoracoscopy is recommended.
1. Case report
A 69-year-old man presented with a left pleural effusion. Laboratory data showed slightly increased white blood cells (9170/μL) and C-reactive protein (0.99 mg/dL). The carcinoembryonic antigen level was high (10.2 ng/mL), but it decreased spontaneously. brain natriuretic protein was not increased (<5.8 pg/mL). Positron emission tomography-computed tomography did not show fluorodeoxyglucose uptake. The pleural effusion was exudative and lymphocyte-dominant (99%). On evaluation of the effusion, the cytology was class II, and the carcinoembryonic antigen level level was not increased (3.3 ng/mL), which was unlikely for a malignant pleural effusion. Adenosine deaminase was not increased (20.2 U/L), and acid-fast bacteria stain and sputum and pleural effusion cultures were negative, which was unlikely for a tuberculous pleural effusion. Even after repeated drainage, the effusion had been increasing for more than two years. Accordingly, thoracoscopy and pleural biopsy were performed. Pleural biopsy did not show any specific findings, but a pleural mass was unexpectedly found on the parietal pleura and removed completely (Fig. 1).
Fig. 1.
Thoracoscopic findings.
A pleural mass was found unexpectedly on the parietal pleura and removed completely.
There were increased small capillaries (CD34-positive), with no abnormalities of endothelial cells or mitoses (Fig. 2).
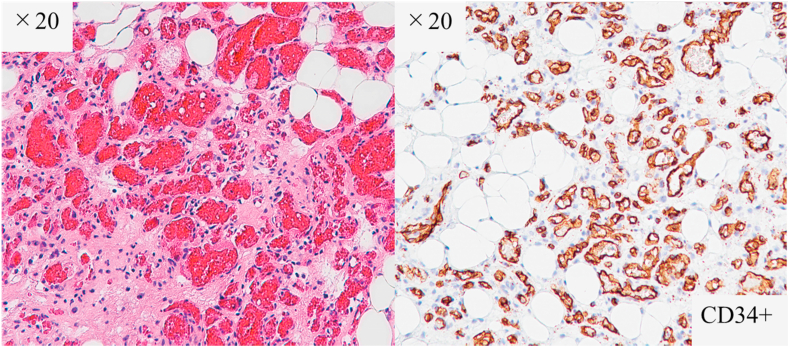
Fig. 2.
Pathological findings.
There were increased small capillaries (CD34-positive), with no abnormalities of endothelial cells or mitoses evident.
providing supported that the mass was a malformation rather than a tumor, and it was diagnosed as a pleural capillary hemangioma. After the surgery, the pleural effusion resolved and did not recur.
2. Discussion
A pleural biopsy is performed to evaluate a pleural effusion, but about 30% of the cases are of unknown etiology and diagnosed as nonspecific pleuritis [1].
Generally, hemangioma is a frequently used term, but the definition of the diagnosis is controversial. For convenience, the diagnosis has been made according to the size of increased vessels, such as cavernous hemangioma. Recently, in the International Society for the Study of Vascular Anomalies classification [2], abnormalities of endothelial cells or mitoses and the lesion's development are considered, and the present case was classified as a capillary malformation.
Capillary hemangiomas usually emerge on or under the skin, and, to the best of our knowledge, cases of pleural origin have been only a few. Every case was accompanied by a pleural effusion, but the mechanism of the effusion is not well known. A hemangioma is considered to result from genetic abnormalities related to the genesis, development, and remodeling of vessels [3]. The vulnerability or abnormal function of increased vessel walls are suggested to make pleural effusion. For the treatment of hemangiomas, dissection, laser radiation, and sclerotherapy are considered. For pleural hemangiomas, dissection could be reasonable and radical, and no recurrences of the pleural effusions were seen after dissection in the reported cases [4].
In the clinical course of nonspecific pleuritis, malignancies could ultimately be identified, and one year of follow-up has been considered sufficient [5]. If a pleural effusion remains after one year of follow-up, thoracoscopy is recommended and could lead to an unexpected diagnosis as this capillary hemangioma case.
3. Conclusion
Though extremely rare, pleural hemangioma is one of the crucial differential diagnoses of refractory pleural effusion.
Formatting of funding sources
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author statement
Kazumasa Akagi: Conceptualization, Investigation, Writing – original draft preparation, Toyoshi Matsutake: Writing-Reviewing and Editing, Kiyoyasu Fukushima: Writing-Reviewing and Editing, Hiroshi Mukae: Supervision, Hirokazu Kurohama: Resources, Writing-Reviewing and Editing. Hirofumi Matsumoto: Resources, Writing-Reviewing and Editing
Declaration of competing interest
None.
References
- 1.Davis H.E., Nicholson J.E., Rahman N.M., Wilkinson E.M., Davies R.J.O., Lee Y.C.G. Outcome of patients with nonspecific pleuritis/fibrosis on thoracoscopic pleural biopsies. Eur. J. Cardio. Thorac. Surg. 2010;38(4):472–477. doi: 10.1016/j.ejcts.2010.01.057. [DOI] [PubMed] [Google Scholar]
- 2.International society for the Study of vascular Anomalies classification 2018 [internet] https://www.issva.org/classification [cited 2020 July 19] Available from:
- 3.Mimura H., Akita S., Fujino A., Jinnin M., Ozaki M., Osuga K. Japanese clinical practice guidelines for vascular Anomalies 2017. Pediatr. Int. 2020;62(3):257–304. doi: 10.1111/ped.14077. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Sindhwani G., Khanduri R., Nadia S., Jethani V. Pleural haemangioma: a rare cause of recurrent pleural effusion. Respir. Med. Case Rep. 2016;17:24–26. doi: 10.1016/j.rmcr.2015.12.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.DePew Z.S., Verma A., Wigle D., Mullon J.J., Nichols F.C., Maldonado F. Nonspecific pleuritis: optimal duration of follow up. Ann. Thorac. Surg. 2014;97(6):1867–1871. doi: 10.1016/j.athoracsur.2014.01.057. [DOI] [PubMed] [Google Scholar]