Abstract
Background and objectives
Thousands of healthcare workers (HCWs) have been infected with 2019 novel coronavirus pneumonia (COVID‐19) during the COVID‐19 pandemic. Laboratory personnel in blood transfusion departments may be infected with severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2) if laboratory biosafety protection is insufficient. Therefore, we investigated the current situation of laboratory biosafety protection in blood transfusion departments to determine how to improve the safety of laboratory processes.
Materials and methods
An online survey was conducted in blood transfusion departments from 1st to 6th May 2020 in China. A total of 653 individuals completed the questionnaire. The questionnaire was designed with reference to COVID‐19 laboratory biosafety summarized in Annex II. All responses were summarized using only descriptive statistics and expressed as frequencies and ratios [n (%)].
Results
Most participants were concerned about COVID‐19. Some participants had inadequate knowledge of COVID‐19. Two participants stated that there were laboratory personnel infected with SARS‐CoV‐2 in their departments. A total of 31 (4.7%) participants did not receive any safety and security training. In terms of laboratory biosafety protection practices, the major challenges were suboptimal laboratory safety practices and insufficient laboratory conditions.
Conclusion
The major deficiencies were insufficient security and safety training, and a lack of personal protective equipment, automatic cap removal centrifuges and biosafety cabinets. Consequently, we should enhance the security and safety training of laboratory personnel to improve their laboratory biosafety protection practices and ensure that laboratory conditions are sufficient to improve the safety of laboratory processes.
Keywords: laboratory biosafety protection, COVID‐19, SARS‐CoV‐2, blood transfusion department
Introduction
In December 2019, pneumonia of an unknown aetiology was reported in Wuhan, China [1]. The disease was subsequently named COVID‐19 by the World Health Organization (WHO) [2]. On 11th March 2020, the WHO declared COVID‐19 to be a pandemic as the highly infectious severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2) rapidly spread worldwide [3].
Healthcare workers (HCWs) are essential to fight this pandemic. However, HCWs involved in the treatment of COVID‐19 patients are at high risk of infection, including laboratory personnel in medical technology departments. Thousands of HCWs have been infected with SARS‐CoV‐2 during the pandemic, and some have even died [4, 5, 6]. As a type of medical technology department, blood transfusion departments in China perform pretransfusion testing, including pretransfusion compatibility testing and infectious disease screening. Pretransfusion compatibility testing can be performed with the traditional tube method or automated and semi‐automated testing platforms that use column agglutination. Enzyme immunosorbent assays and chemiluminescent immunoassays are used to detect infectious diseases. Nucleic acid testing has also been performed in a few hospitals. Van Doremalen et al. reported that aerosol transmission of SARS‐CoV‐2 is plausible [7]. Moreover, there is growing evidence that aerosol transmission of SARS‐CoV‐2 is possible in confined settings with poor ventilation and upon long exposure to high concentrations of aerosols [8]. The WHO acknowledged that some medical procedures can produce very small droplets (called aerosolized droplet nuclei or aerosols) containing SARS‐CoV‐2 [9], which may pose an infectious risk to medical staff. Although most COVID‐19 patients had detectable viral RNA in respiratory swabs, some studies have shown that a small proportion of them had detectable SARS‐CoV‐2 RNA in blood [10, 11], which may aerosolize to generate infectious virus‐containing droplets or particles. Hence, exposure to other personnel who may be asymptomatically infected with SARS‐CoV‐2, aerosols generated during specimen pretreatment (e.g. centrifugation) and nosocomial airborne transmission may be the main causes of COVID‐19 infection among laboratory workers during outbreaks. In addition, various serological tests performed in blood transfusion laboratories, such as those that use test tubes and microcolumn gels, involve centrifugation, which increases the risk of producing aerosols containing viruses. Therefore, staff in blood transfusion laboratories are also at risk of COVID‐19 infection.
According to a previous study [12], great uncertainty concerning biohazard risks related to SARS‐CoV‐2 and inadequate resources such as surgical masks, protective suits and laboratory equipment pose great challenges for processes in clinical chemistry laboratories. Therefore, we sought to identify the existing problems and propose areas for improvement by investigating the current situation of laboratory biosafety protection in blood transfusion departments. Specifically, we investigated attitudes to and knowledge of COVID‐19; the rate of COVID‐19 infection among laboratory staff; knowledge of laboratory biosafety protection; and laboratory biosafety protection practices in pretransfusion testing during the COVID‐19 pandemic in Chinese blood transfusion departments. To the best of our knowledge, this is the first report concerning the rate of COVID‐19 infection and its prevention in blood transfusion departments.
Materials and methods
Study population and participants
This study was conducted online by issuing electronic questionnaires. All participants were guaranteed anonymity and provided informed consent. During the study period (1st to 6th May 2020), 653 participants from blood transfusion departments in China completed the questionnaire.
Study questionnaire
The study questionnaire consisted of four sections. The first section included five questions concerning the demographic characteristics of participants, such as their gender, age, degrees, work experience and geographical distribution. The second section included five questions concerning participants’ attitude to and knowledge of COVID‐19, such as anxiety levels about COVID‐19 and the transmission routes, symptoms, the causative pathogen, and COVID‐19 treatments. The third section included six questions concerning the rate of COVID‐19 infection and participants’ knowledge of laboratory biosafety protection in blood transfusion departments. The fourth section included 12 questions concerning laboratory biosafety protection practices in pretransfusion testing. Detailed questionnaire information is provided in Annex I.
Ethical approval
This cross‐sectional observational study was approved by the Ethics Committee of the Third Xiangya Hospital of Central South University (2020‐S351).
Statistical analysis
All responses were summarized using only descriptive statistics and expressed as frequencies and ratios [n (%)].
Results
Demographic characteristics of the study participants
A total of 653 participants completed the questionnaire [235 males (35.99%) and 418 females (64.01%)]. The study participants had various degrees, including college, bachelor, master and doctorate degrees. Participants were aged from 18 years to older than 60 years. A total of 538 (82.39%) participants had more than 5 years of work experience (Fig. 1). The study participants were from 34 provinces of China (Fig. 2).
Fig. 1.
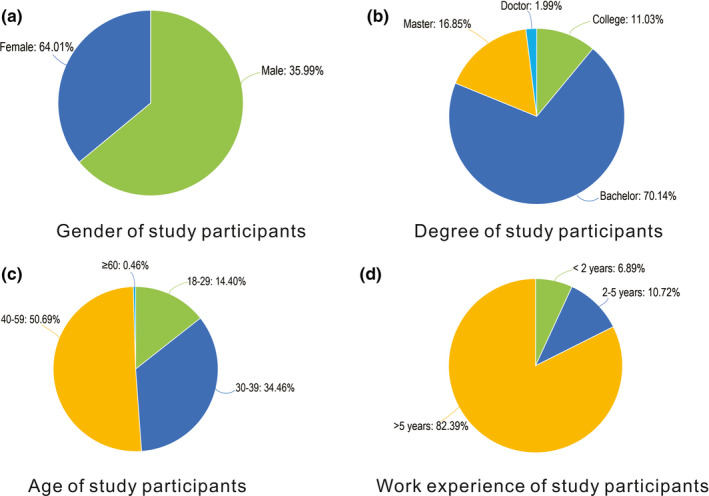
Demographic characteristics of the study participants. (A) Gender, (B) degree, (C) age and (D) work experience of the study participants.
Fig. 2.
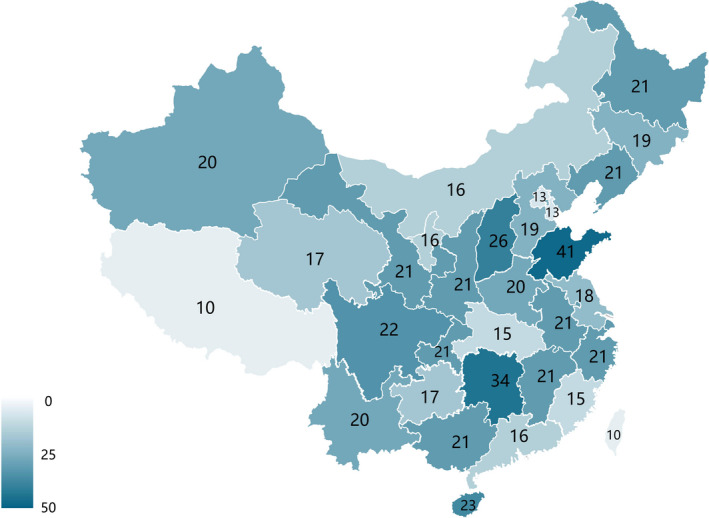
The geographical distribution of the study participants.
Participants’ attitude to and knowledge of COVID‐19
Participants’ attitude to and knowledge of COVID‐19 are shown in Table 1. Most participants (66.9%) were concerned about COVID‐19. In terms of the common transmission routes of SARS‐CoV‐2, 97.5% and 99.7% of participants knew that SARS‐CoV‐2 can be transmitted through close contact and respiratory transmission, respectively, but 292 (44.7%) participants believed that SARS‐CoV‐2 can be transmitted through blood transfusion. A substantial number of participants incorrectly answered questions about the pathogen of COVID‐19. For example, 187 (28.6%) and 129 (19.8%) participants thought the pathogen responsible for COVID‐19 is SARS‐CoV and MERS‐CoV, respectively. More than 80% of participants knew the manifestations of COVID‐19, including fever, cough, fatigue and no symptoms. A total of 98% participants knew that COVID‐19 is treated with symptomatic and supportive treatment.
Table 1.
Participants’ attitude to and knowledge of COVID‐19.
| Question | Response | Frequency, n (%) |
|---|---|---|
| Are you worried about COVID‐19? | Very much | 57 (8.7) |
| A little | 437 (66.9) | |
| Not at all | 159 (24.3) | |
| What is the transmission route of SARS‐CoV‐2? | Close contact | 637 (97.5) |
| Blood transfusion | 292 (44.7) | |
| Respiratory transmission | 651 (99.7) | |
| What are the symptoms of COVID‐19? | Fever | 563 (86.2) |
| Cough | 553 (84.7) | |
| Fatigue | 547 (83.8) | |
| What is the pathogen of COVID‐19? | SARS‐CoV | 187 (28.6) |
| SARS‐CoV‐2 | 287 (44.0) | |
| MERS‐CoV | 129 (19.8) | |
| What are the treatments for COVID‐19? | Market vaccine | 9 (1.4) |
| Specific medicine | 4 (0.6) | |
| Symptomatic and supportive treatment | 640 (98.0) |
This article is being made freely available through PubMed Central as part of the COVID-19 public health emergency response. It can be used for unrestricted research re-use and analysis in any form or by any means with acknowledgement of the original source, for the duration of the public health emergency.
The rate of COVID‐19 infection and knowledge of laboratory biosafety protection in blood transfusion departments
The rate of COVID‐19 infection and knowledge of laboratory biosafety protection in blood transfusion departments are shown in Table 2. A total of two (0.3%) participants stated that there were personnel infected with COVID‐19 (nosocomial infection) in their departments. Meanwhile, 31 (4.7%) participants did not receive safety and security training about COVID‐19 in their departments. In terms of risk assessment of laboratory procedures, nearly all participants knew the risks of SARS‐CoV‐2 transmission involving contagion, droplet transmission in specimen reception and aerosol transmission caused by removing caps, centrifugation and vigorous shaking. Laboratory biosafety protection mainly involves personal biosafety protection and laboratory space and facility protection. Most participants had adequate knowledge of personal biosafety protection levels. In terms of laboratory space and facility protection, nearly all participants undertook measures such as ventilating the laboratory, partitioning items and separating clean and dirty items. However, only 60–80% of participants undertook measures such as guaranteeing sufficient experimental supplies and instrument maintenance, suggesting that laboratory personnel should pay more attention to laboratory space and facility protection.
Table 2.
The rate of COVID‐19 infection among laboratory staff and knowledge of laboratory biosafety protection in blood transfusion departments.
| Question | Response | Frequency, n (%) |
|---|---|---|
| Is anyone in your department infected with COVID‐19 (nosocomial infection)? | Yes | 2 (0.3) |
| No | 651 (99.7) | |
| Have you received safety and security training about COVID‐19? | Yes | 622 (95.3) |
| No | 31 (4.7) | |
| What are the risks for SARS‐CoV‐2 transmission in laboratories? | Respiratory droplet transmission | 628 (96.2) |
| Close contact transmission | 615 (94.2) | |
| Aerosol transmission | 641 (98.2) | |
| Blood transfusion transmission | 292 (44.7%) | |
| Which situations pose a risk of COVID‐19 infection? | Specimen reception | 643 (98.5) |
| Specimen centrifugation, removing caps or shaking | 651 (99.7) | |
| What are the levels of personal biosafety protection a ? | Level 1 personal biosafety protection | 530 (81.2) |
| Level 2 personal biosafety protection | 629 (96.3) | |
| Level 3 personal biosafety protection | 562 (86.1) | |
| What laboratory space and facility protection measures are there in your laboratory? | Laboratory ventilation | 644 (98.6) |
| Item partitioning | 598 (91.6) | |
| Separating clean and dirty items | 638 (97.7) | |
| Guaranteeing sufficient experimental supplies | 509 (77.9) | |
| Ultraviolet radiation disinfection | 638 (97.7) | |
| Maintenance of laboratory equipment | 402 (61.6) |
Level 1: a medical surgical mask, gloves, a laboratory coat, a medical protective cap and seven‐step hand‐washing.
Level 2: a medical surgical mask or N95 mask, gloves, an isolation gown, a medical protective cap and seven‐step hand‐washing.
Level 3: a medical surgical mask or N95 mask, gloves, a face shield, safety glasses, a protective suit, a medical protective cap and seven‐step hand‐washing.
Levels of personal biosafety protection:
This article is being made freely available through PubMed Central as part of the COVID-19 public health emergency response. It can be used for unrestricted research re-use and analysis in any form or by any means with acknowledgement of the original source, for the duration of the public health emergency.
Laboratory biosafety protection practices during pretransfusion testing
Laboratory biosafety protection practices during pretransfusion testing are shown in Table 3. A total of 523 (80.1%) participants manipulated COVID‐19 patient specimens in a biosafety level 2 (BSL‐2) laboratory. The pretransfusion testing procedure involves reception of the specimen, centrifugation and manipulation of the specimen, disposal of the specimen and waste and disinfection of the laboratory environment after testing. Attention must be paid to laboratory biosafety protection during each of these steps. During testing of COVID‐19 patient specimens, only 225 (34.5%) participants used level 3 personal biosafety protection, and 430 (65.8%) participants stated that their departments lacked personal protective equipment (PPE). This indicates that some laboratory personnel did not use level 3 personal biosafety protection due to a lack of PPE including surgical masks, gloves and protective suits. During sample reception, most participants disinfected the surface of the plastic bag containing the specimen and application form, the inner layer of the plastic bag, the specimen tubes and the application form with 75% ethanol. Frequent hand hygiene is a personal protection measure that laboratory personnel should adhere to. A total of 608 (93.1%) participants performed seven‐step hand‐washing before entering and leaving the laboratory and on any occasion when contamination was known or suspected to be present on the hands; however, 45 (6.9%) participants did not strictly adhere to hand hygiene practices. Removal of the cap from the specimen tube is an aerosol‐generating procedure, and automatic cap removal centrifugation can avoid aerosol generation. However, only 194 (29.7%) participants had an automatic cap removal centrifuge in their departments. Only 349 (53.4%) participants removed specimens more than 10 min after the centrifuge had stopped, and 45 (6.9%) participants removed specimens immediately. When abnormal sounds occurred during centrifugation, only 463 (71.0%) participants used personal level 3 biosafety protection and 573 (87.7%) participants removed specimens more than 30 min after the centrifuge had stopped. When faced with laboratory contamination (including broken or overturned specimen tubes) caused by blood specimens of patients with confirmed COVID‐19, nearly all participants closed the laboratory and covered the contaminated area with 5500 mg/L effective chlorine disinfectant wipes for more than 30 min, but only 339 (51.9%) participants fumigated the laboratory with peroxyacetic acid following large spills. A total of 478 (73.2%) participants performed manual tests of specimens in a biosafety cabinet (BSC); however, 130 (19.9%) participants lacked a BSC in their departments. In addition, 45 (6.9%) participants did not perform manual tests of specimens in a BSC because they felt it was inconvenient. After all manipulations were completed, a few participants did not disinfect laboratory supplies, equipment, countertops or the space with appropriate disinfectants or ultraviolet radiation. Meanwhile, a few participants did not seal the specimen tube with a cap in a double yellow medical garbage bag or disinfect the surface of the garbage bag with 75% ethanol. Fortunately, all participants autoclaved the waste after the storage period.
Table 3.
Laboratory biosafety protection practices during pretransfusion testing.
| Question | Response | Frequency, n (%) |
|---|---|---|
| Do you perform all manipulations of COVID‐19 patient specimens in a BSL‐2 or higher‐level laboratory? | Yes | 523 (80.1) |
| No | 130 (19.9) | |
| Which of the following personal biosafety protection levels do you use when testing blood specimens of COVID‐19 patients? | Level 1 personal biosafety protection | 89 (13.6) |
| Level 2 personal biosafety protection | 339 (51.9) | |
| Level 3 personal biosafety protection | 225 (34.5) | |
| Does your department lack PPE? | Yes | 430 (65.8) |
| No | 223 (34.2) | |
| Which of the following do you perform during specimen reception? | Disinfect the surface of the plastic bag containing the specimens and application form with 75% ethanol | 603 (92.3) |
| Disinfect the inner layer of the plastic bag, specimen tubes and the application form | 568 (87.0) | |
| When do you perform seven‐step hand‐washing? | Before entering and leaving the laboratory, after handling any specimen and on any occasion when contamination is known or suspected to be present on the hands | 608 (93.1) |
| Only after handling any specimen | 9 (1.4) | |
| I do not perform seven‐step hand‐washing | 36 (5.5) | |
| Is there an automatic cap removal centrifuge in your department? | Yes | 194 (29.7) |
| No | 459 (70.3) | |
| How long do you wait to remove the specimen after the centrifuge stops? | 0 min | 45 (6.9) |
| 5–10 min | 259 (39.7) | |
| More than 10 min | 349 (53.4) | |
| How do you respond when abnormal sounds occur during centrifugation? | Use personal level 3 biosafety protection | 463 (71.0) |
| Remove the specimen more than 30 min after the centrifuge has stopped | 573 (87.7) | |
| How do you handle laboratory contamination (including broken or overturned specimen tubes) caused by blood specimens of patients with confirmed COVID‐19? | Close the laboratory and cover the contaminated area with 5500 mg/L effective chlorine disinfectant wipes for more than 30 min | 638 (97.7) |
| Fumigate the laboratory with peroxyacetic acid following large spills | 339 (51.9) | |
| Do you perform manual tests in a BSC? | Yes | 478 (73.2) |
| No, the department lacks a BSC | 130 (19.9) | |
| No, the manipulation is inconvenient in a BSC | 45 (6.9) | |
| What disinfection do you perform after testing? | Disinfect laboratory instruments and supplies with 75% ethanol | 553 (84.7) |
| Wipe laboratory countertops, the floor and equipment with 75% ethanol or 500 mg/L effective chlorine disinfectant | 618 (94.6) | |
| Disinfect the laboratory space with ultraviolet lamps for more than 30 min | 613 (93.9) | |
| Seal specimens inside double yellow medical garbage bags | 588 (90.0) | |
| How do you dispose specimens after testing? | Disinfect the surface of the above bags with 75% ethanol | 533 (81.6) |
| Autoclave waste after storage | 578 (88.5) |
BSC, biosafety cabinet; PPE, personal protective equipment (a surgical mask, gloves, a protective suit, safety glasses, a face shield, etc.).
This article is being made freely available through PubMed Central as part of the COVID-19 public health emergency response. It can be used for unrestricted research re-use and analysis in any form or by any means with acknowledgement of the original source, for the duration of the public health emergency.
Discussion
The COVID‐19 pandemic has posed an unprecedented challenge for medical staff including laboratory personnel. According to a previous study, clinical laboratories are facing major challenges including limited guidance and inadequate medical protection resources [12 pp1439–1440]. Blood transfusion departments have performed pretransfusion testing during the COVID‐19 pandemic. Personnel in these departments may be infected with SARS‐CoV‐2 due to frequent contact with potentially infected blood specimens and other personnel who are asymptomatically infected. Therefore, it is crucial to ensure that laboratory processes are safe and effective.
In the current study, 653 participants completed the questionnaire. The participants spanned a range of ages, had different degrees including college, bachelor, master and doctorate degrees, and had a variety of work experience. Additionally, the participants were from each of the 34 provinces in China, meaning that their responses to our questionnaire represent laboratory personnel in blood transfusion departments across China.
Participants’ attitude to and knowledge of COVID‐19 play an important role in establishing prevention awareness and promoting positive behaviours to a certain extent [13, 14 pp186]. More than half of participants were concerned about COVID‐19. Nearly all participants knew the common transmission routes of SARS‐CoV‐2 [15, 16]. However, 292 (44.7%) participants believed that SARS‐CoV‐2 can be transmitted through blood transfusion. Currently, there is no evidence to support this [17, 18]. However, only 287 (44.0%) participants knew that the pathogen of COVID‐19 is SARS‐CoV‐2 [19], and some thought that it is SARS‐CoV or MERS‐CoV. When we sought clarification from participants regarding this finding, a lack of knowledge regarding the causative pathogen of COVID‐19 was confirmed. Therefore, knowledge of COVID‐19 among laboratory personnel in blood transfusion departments in China must be improved via training and education.
According to interim guidance, titled ‘Laboratory biosafety guidance related to the novel coronavirus (2019‐nCoV)’, issued by the WHO (https://www.who.int/docs/default‐source/coronaviruse/laboratory‐biosafety‐novel‐coronavirus‐version‐1‐1.pdf?sfvrsn=912a9847_2), all personnel should receive safety and security training; all procedures should be performed based on risk assessment; and initial processing (before inactivation) of all specimens should be performed in a validated BSC. In our study, 4.7% of participants did not receive safety and security training about COVID‐19 in their departments, including 23 (3.5%) individuals who replied that their hospitals did not provide training to all employees and eight (1.2%) individuals who were unable to attend training due to scheduling conflicts. This means that such training was inadequate in these departments and some laboratory personnel were unqualified to perform pretransfusion testing of COVID‐19 patients, which is an obstacle to ensuring laboratory processes are safe. Nearly all participants knew the risks of SARS‐CoV‐2 transmission involving contagion, droplet transmission and aerosol transmission due to specimen reception, centrifugation, vigorous shaking and removal of caps [20, 21]. Personal biosafety protection plays an important role in decreasing infection of HCWs with COVID‐19 [22, 23, 24]. Most participants had adequate knowledge of laboratory biosafety protection levels. A safe laboratory environment is essential for laboratory personnel [20 pp581]. However, some participants did not perform measures such as ventilating the laboratory, partitioning items, separating clean and dirty items, guaranteeing sufficient experimental supplies, disinfecting with ultraviolet radiation and maintaining laboratory equipment. This may be related to the safety and security training of participants and some participants’ inadequate knowledge of COVID‐19.
Patients can have suspected or confirmed COVID‐19 or even be infected with SARS‐CoV‐2 but not display symptoms. Laboratory personnel may be infected with SARS‐CoV‐2 during laboratory processes involving specimen reception before testing, centrifugation and manipulation of specimens and disposal of specimens and waste. Therefore, laboratory biosafety protection measures are vital to avoid infection of laboratory personnel. According to recommendations of the International Federation of Clinical Chemistry and Laboratory Medicine (IFCC) Taskforce, COVID‐19 specimens should be handled in a BSL‐2 laboratory [21]. However, 130 (19.9%) participants did not perform pretransfusion testing in a BSL‐2 laboratory, meaning that the laboratory conditions in some blood transfusion departments in China did not meet the requirements for COVID‐19 testing. Due to the presence of asymptomatic or undiagnosed COVID‐19 patients and the highly contagious nature of COVID‐19, use of appropriate personal biosafety protection is universally recommended to avoid COVID‐19 infection [25]. However, some participants did not perform proper disinfection during specimen reception, and only 225 (34.5%) participants used level 3 personal biosafety protection when testing specimens of COVID‐19 patients. Additionally, 430 (65.8%) participants stated that their departments lacked PPE, suggesting that the reason why most participants did not use level 3 personal biosafety protection was a lack of PPE. The characteristics of SARS‐CoV‐2 transmission, especially aerosol transmission, play an important role in infection of laboratory personnel. Therefore, personnel should be cautious about generating aerosols during all laboratory manipulations such as centrifugation, testing, vigorous shaking and removal of caps. An automatic cap removal centrifuge avoids aerosol generation during removal of specimen caps. However, only 194 (29.7%) participants had an automatic cap removal centrifuge in their departments, meaning that insufficient laboratory equipment is a challenge for ensuring laboratory procedures are safe. According to the recommendation of the Chinese Society of Laboratory Medicine (http://www.cslm.org.cn/cn/news.asp?id=73.html), laboratory personnel should remove specimens more than 10 min after the centrifuge has stopped, and, if abnormal sounds occur during centrifugation, laboratory personnel should use level 3 personal biosafety protection and remove specimens more than 30 min after the centrifuge has stopped. Nevertheless, only 349 (53.4%) participants removed specimens more than 10 min after the centrifuge had stopped, and 463 (71.0%) participants used level 3 personal biosafety protection, and 573 (87.7%) participants removed specimens more than 30 min after the centrifuge had stopped when abnormal sounds occurred during centrifugation. According to the recommendation of the WHO, COVID‐19 specimens must be handled in a BSC using standard precautions, especially during manual specimen tests. However, 130 (19.9%) participants lacked a BSC in their departments, and 45 (6.9%) participants did not perform manual specimen tests in a BSC because it was inconvenient, indicating that laboratory facilities are insufficient and laboratory personnel do not have adequate laboratory biosafety knowledge. After all manipulations were completed, a few participants did not disinfect the laboratory, indicating that they did not pay attention to the specimen disposal procedure after testing. Hand hygiene is vital in laboratory biosafety protection. Furthermore, strict adherence of laboratory staff to hand hygiene measures is required to prevent inadvertent transmission of pathogens to themselves or others [20, 23]. However, 6.9% of participants did not strictly adhere to seven‐step hand‐washing. In conclusion, laboratory biosafety protection practices of some laboratory personnel in Chinese blood transfusion departments were poor, which may have been due to their inadequate laboratory biosafety knowledge and insufficient laboratory facilities such as a BSC, an automatic cap removal centrifuge and PPE. Moreover, two (0.3%) participants stated that there were personnel infected with COVID‐19 in their departments. We contacted these two participants to investigate the reasons why these personnel were infected. One participant stated that the infected personnel did not use level 3 personal protection during testing of COVID‐19 specimens due to a lack of PPE and did not receive security and safety training about COVID‐19. The other participant stated that the infected personnel did not perform manual tests of specimens in a BSC.
Limitations
This is the first study to focus on the rate of COVID‐19 infection and its control in blood transfusion departments. There are several limitations of our study. First, the limited number of questions does not reflect the imprecise current situation of laboratory biosafety protection. Second, the responses provided likely reflect a snapshot of national practices at the time of survey and may change over time. Hospital blood transfusion departments in China order blood components from blood centres and distribute them to recipients when necessary. Blood processing, including preparation and modification of components, is performed in blood centres and is prohibited in hospital blood transfusion departments. Therefore, the risks associated with blood products are beyond the scope of this study.
Conclusion
In this study, some participants thought that SARS‐CoV‐2 can be transmitted through blood transfusion and did not know the pathogen of COVID‐19, meaning that knowledge of COVID‐19 among laboratory personnel must be improved via training and education. Some personnel did not have adequate knowledge of laboratory biosafety protection and were unqualified to work in a laboratory during the COVID‐19 pandemic because they did not receive security and safety training. During pretransfusion testing of COVID‐19 patients, some participants did not strictly perform laboratory biosafety protection. This was because some laboratory personnel were unqualified and laboratory facilities such as a BSC, an automatic cap removal centrifuge and PPE were lacking. Meanwhile, two participants stated that there were personnel infected with COVID‐19 in their departments. This may have been due to insufficient laboratory biosafety protection. Consequently, on the one hand, we should enhance security and safety training of laboratory personnel to improve their laboratory biosafety protection knowledge and practices. On the other hand, we should ensure that there is sufficient equipment such as a BSC, an automatic cap removal centrifuge and PPE in blood transfusion departments to guarantee that laboratory procedures are safe.
Conflict of interest
The authors declare that they have no conflicts of interest relevant to the manuscript.
Author contributions
Haiting Liu, Leping Liu, Rong Gui and Rong Huang were involved in questionnaire design. Leping Liu, Xueling Shang, Sai Chen, Xisheng Li and Junhua Zhang were involved in sample processing, data acquisition and analysis and manuscript writing. Haiting Liu wrote the manuscript. Rong Gui and Rong Huang edited the manuscript.
Supporting information
Annex I The detailed questionnaire information
Annex II Recommendations of COVID‐19 laboratory biosafety
Acknowledgements
We warmly thank all the participants. This research was funded by the Fundamental Research Funds for the Central Universities of Central South University (grant number 2019zzts829), the Fundamental Research Funds for the Universities of Hunan Province (grant number 1021‐0001017106) and the National Natural Science Foundation of China (NSFC) (grant numbers 81573091 and 81602801).
Contributor Information
Rong Gui, Email: aguirong@163.com, Email: ronghuang1989@csu.edu.cn.
Rong Huang, Email: aguirong@163.com, Email: ronghuang1989@csu.edu.cn.
References
- 1. Zhang YZ, Chen N, Zhou M, et al.: Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Nature 2020; 395:507–13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Lai CC, Shih TP, Ko WC, et al.: Severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2) and coronavirus disease‐2019 (COVID‐19): The epidemic and the challenges. Radiology 2020; 55:105924 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Muniyappa R, Gubbi S: COVID‐19 pandemic, coronaviruses, and diabetes mellitus. Am J Physiol Endocrinol Metab 2020; 318:E736‐e41 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Jin YH, Huang Q, Wang YY, et al.: Perceived infection transmission routes, infection control practices, psychosocial changes, and management of COVID‐19 infected healthcare workers in a tertiary acute care hospital in Wuhan: a cross‐sectional survey. Mil Med Res 2020; 7:24 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Huang L, Lin G, Tang L, et al.: Special attention to nurses' protection during the COVID‐19 epidemic. Crit Care 2020; 24:120 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Chu J, Yang N, Wei Y, et al.: Clinical characteristics of 54 medical staff with COVID‐19: A retrospective study in a single center in Wuhan, China. J Med Virol 2020; 92:807–813 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. van Doremalen N, Bushmaker T, Morris DH, et al.: Aerosol and surface stability of HCoV‐19 (SARS‐CoV‐2) compared to SARS‐CoV‐1. N Engl J Med 2020; 382:1564–1567 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Asadi S, Bouvier N, Wexler AS, et al. The coronavirus pandemic and aerosols: Does COVID‐19 transmit via expiratory particles? Aerosol Sci Technol 2020; 1–4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. https://www.who.int/zh/emergencies/diseases/novel‐coronavirus‐2019/question‐and‐answers‐hub/q‐a‐detail/q‐a‐how‐is‐covid‐19‐transmitted.
- 10. Kiely P, Hoad VC, Seed CR, et al.: Severe acute respiratory syndrome coronavirus‐2: implications for blood safety and sufficiency. Vox Sang 2020. 10.1111/vox.13009 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. Peng L, Liu J, Xu W, et al.: SARS‐CoV‐2 can be detected in urine, blood, anal swabs, and oropharyngeal swabs specimens. J Med Virol 2020; 92(9):1676–1680. 10.1002/jmv.25936 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Loh TP, Horvath AR, Wang CB, et al.: Laboratory practices to mitigate biohazard risks during the COVID‐19 outbreak: an IFCC global survey. Clin Chem Lab Med 2020; 58(9):1433–1440. 10.1515/cclm-2020-0711 [DOI] [PubMed] [Google Scholar]
- 13. Pambuccian SE: The COVID‐19 pandemic: implications for the cytology laboratory. J Am Soc Cytopathol 2020; 9:202–11 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Zhang M, Zhou M, Tang F, et al.: Knowledge, attitude, and practice regarding COVID‐19 among healthcare workers in Henan. China. J Hosp Infect 2020; 105:183–7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Guo YR, Cao QD, Hong ZS, et al.: The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID‐19) outbreak ‐ an update on the status. Mil Med Res 2020; 7:11 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Shereen MA, Khan S, Kazmi A, et al.: COVID‐19 infection: Origin, transmission, and characteristics of human coronaviruses. J Adv Res 2020; 24:91–8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Chang L, Yan Y, Wang L: Coronavirus disease 2019: coronaviruses and blood safety. Transfus Med Rev 2020; 34:75–80 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Cho HJ, Koo JW, Roh SK, et al.: COVID‐19 transmission and blood transfusion: A case report. J Infect Public Health 2020; 13(11):1678–1679. 10.1016/j.jiph.2020.05.001 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Gorbalenya AE, Baker SC, Baric RS, et al.: The species Severe acute respiratory syndrome‐related coronavirus: classifying 2019‐nCoV and naming it SARS‐CoV‐2. Nat Microbiol 2020; 5:536–544 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Ağalar C, Öztürk Engin D: Protective measures for COVID‐19 for healthcare providers and laboratory personnel. Turk J Med Sci 2020; 50:578–84 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Lippi G, Adeli K, Ferrari M, et al.: Biosafety measures for preventing infection from COVID‐19 in clinical laboratories: IFCC Taskforce Recommendations. Clin Chem Lab Med 2020; 58:1053–62 [DOI] [PubMed] [Google Scholar]
- 22. Zhang Z, Liu S, Xiang M, et al.: Protecting healthcare personnel from 2019‐nCoV infection risks: lessons and suggestions. Front Med 2020; 14:229–31 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Ferioli M, Cisternino C, Leo V, et al.: Protecting healthcare workers from SARS‐CoV‐2 infection: practical indications. Eur Respir Rev 2020; 29:200068 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Mourya DT, Sapkal G, Yadav PD, et al.: Biorisk assessment for infrastructure & biosafety requirements for the laboratories providing coronavirus SARS‐CoV‐2/(COVID‐19) diagnosis. Indian J Med Res 2020; 151:172–6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Hellewell J, Abbott S, Gimma A, et al.: Feasibility of controlling COVID‐19 outbreaks by isolation of cases and contacts. Lancet Glob Health 2020; 8:e488–e496 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Annex I The detailed questionnaire information
Annex II Recommendations of COVID‐19 laboratory biosafety


