Abstract
Covid-19 due to Sars-Cov-2 infection has reached pandemic proportion. Many healthcare workers are involved in managing both COVID-suspected and confirmed cases. It is mandatory for healthcare workers to have droplet and contact precautions by means of Personal protective equipment (PPE), facemask, face shield or eye protection. Prolonged usage of medical mask results in various adverse effects. This study is an attempt to know the common effects of prolonged face mask in healthcare workers and its resultant quality-of-life (QOL). To study the common effects of prolonged face mask and its impact on QOL of healthcare workers during the COVID 19 crisis. This was a prospective cross-sectional study conducted over 6 months among 2750 healthcare workers. A questionnaire requesting demographic details and most common side effects after prolonged usage of face mask was circulated. We also attached a short form-12 (sf-12) questionnaire to assess its impact on QOL. Out of 2750 personnel, 299 were excluded. Male preponderance was noted. Study was conducted on candidates using 3ply mask or above. Age range was between 18 and 65 years with mean age being 37.61 ± 15.23 in mask users < 5 h per day, 32.2 ± 10.02 in 5–10 h group and 30.19 ± 8.15 in 10 h group. 8.48% (n = 174) had comorbidities. QOL impacted. The complaints with face mask use definitely are troublesome with increase in severity with duration of mask usage. This definitely has a proportional impact on the healthcare workers’ QOL.
Keywords: COVID-19, Healthcare workers, Face mask, Side effects, QOL, Sf-12, PPE, Audit, Symptomatology
Introduction
COVID-19 caused by SARS-CoV2 originated from Wuhan city in China in November 2019 soon reaching pandemic proportions [1, 2]. Many patients presented with sore throat, high fever, dry cough, breathing problems, decreased smell and taste sensation and easy fatigability [3]. WHO defines a healthcare worker as, “people involved in actions with the primary intent of enhancing health of the patient” [4]. It includes doctors, nursing and midwifery professionals, cleaners, other staff who work in health facilities, social workers, and community health workers [4]. All health workers and care givers involved in managing a COVID-19 confirmed or suspected patient should have droplet and contact precautions before entering the room where they are admitted [5]. The principles to be followed are, to perform hand hygiene before putting on and after removing PPE (Personal protective equipment)—use PPE which is appropriate, medical mask, facial protection (face-shield) or eye protection (goggles), and to avoid contamination of mucous membranes—long-sleeved gown, clean, nonsterile medical gloves are worn. Health workers and caregivers working in clinical areas with COVID-19 suspected or confirmed cases should continuously wear a facemask during all routine activities throughout the entire shift [6].
A mask is said to be a surgical mask if it is flat or which can be pleated and are fixed to head with help of straps that can either go around the ears or around head or both. It aims to balance adequate breathability, high filtration [7, 8]. Filtering facepiece respirators (FFR) like medical masks offer a balance of filtration and breathability. Medical masks filter 3 µm droplets while respirators must filter 0.075 µm solid particles [9, 10]. An important difference between these masks is that the way of filtration it is being tested. Respirators are tested for filtration across the entire surface whereas medical masks are tested on a cross section. An N95 respirator consists of multiple layers, made from polypropylene. The two outer layers of the mask are of fabric and are spun bonded [11]. It measures about 20–50 g/m2 in density and acts as protection against outside environment. A prefiltration layer is present between the spun bond layers which is about 250 g/m2 in density after which filtration layer is placed. A high efficiency layer is the last layer which is melt-blown electret and it is the layer which determines the filtration efficiency [12].
The practice of using face mask by all healthcare givers and professionals, working in a clinical setup throughout the entire shift in a day is known as continuous face mask use. Face masks are removed or changed only if it is damaged, wet or soiled; or removed by healthcare workers for drinking or eating [13].
Aim
To study the common effects of prolonged face mask and its impact on QOL of healthcare workers during the COVID 19 crisis.
Methodology
A prospective cross-sectional study was conducted on 2750 healthcare workers in and around Chennai, from April to September 2020 between the age of 18–65 years on side effects of prolonged facemask usage. Customized questionnaire was circulated electronically to professionals and graduates; and hard copy was given to high school population for whom junior residents and secretary from Department of ENT provided with vernacular support and helped to fill the questionnaire. It comprised of demographic details, whether using recommended 3ply mask (or higher) or not, hours of using mask per day. 299 of them were excluded (n = 2451) because of native mask use, use of kerchiefs and improper wearing of masks. Based on the duration of mask usage, they were grouped into < 5 h, 5–10 h and > 10 h.
Nasal and airway symptoms like nasal block, nasal dryness, watery nasal discharge, sneezing/nasal irritability, nasal bridge abrasion, breathing difficulty, nasal bleeding and mouth breathing; non-nasal symptoms like headache, fatigability, acne over mask line, periauricular pain, fogging/malposition of spectacles, prickly heat, itching around eye were documented. History regarding risk factors like pre-existing airway disease, comorbidities, personal habits such as smoking and alcohol intake, COVID-19 positive relatives; COVID status of participants like usage of medications or supplements as precautionary measures, COVID-19 positive treatment and COVID related airway symptoms were obtained.
All questions were answerable as No/Yes. A clinical symptom scale was made giving a value of “0” for “No” and “1” for “Yes”. A maximum score of 20 was given. It was graded as 0-no symptoms, 1 to 7-mild symptoms, 8 to 14-moderate symptoms, 15 to 20-severe symptoms. The quality-of-life (QOL) assessment and its impact on mask users was calculated using Short Form-12 (sf-12) questionnaire [14]—easy to respond and less time-consuming. Data tabulation was done using MS Excel. Continuous data was given as mean ± standard deviation, categorical data was given as number (percent). Pearson’s correlation was done. Statistical evaluation was done using IBM SPSS statistics for Windows v26 (Armonk NY: IBM Corp). P value < 0.05 was considered statistically significant.
Inclusion Criteria
Age between 18 and 65 years
Healthcare workers
Usage of 3ply face mask or higher
Exclusion Criteria
Known case of anemia/sinusitis
Usage of non-surgical masks
Previous facial/airway surgeries
Improper usage
Treatment for facial conditions
Results and Discussion
Demographic data noted (Table 1). N = 2451, of which 1737 (70.8%) were males and 714 (29.2%) were females. Overall male:female was 2.4:1. Age-wise & gender-wise distribution across groups depicted in Figs. 1 and 2. Age range was between 18 and 65 years.
Table 1.
Demographic details
| Sr. no. | Parameter (n = 2451) | Group | Value (n,%/m ± SD) |
|---|---|---|---|
| 1 | Age range (years) | 18–65 | |
| 2 | Mean age (years) |
< 5 h 5–10 h > 10 h |
37.61 ± 15.23 32.2 ± 10.02 30.19 ± 8.15 |
| 3 | Mean age (years) | Overall | 33.34 ± 11.13 |
| 4 | Male:female | 2.4:1 | |
| 5 | Co-morbidities |
Hypertension Diabetes mellitus Type 2 Bronchial asthma Pulmonary Tuberculosis Coronary Artery Disease Seizure Thyroid disorder |
68 (2.7%) 60 (2.4%) 11 (.4%) 16 (.6%) 20 (.8%) 5 (.2%) 34 (1.38%) |
| 6 | Habits |
Smoking Alcohol intake |
556 (22.68%) 312 (12.72%) |
| 7 | Educational status |
Professionals Graduates High-school |
421 (17.2%) 1069 (43.4%) 969 (39.4%) |
Fig. 1.
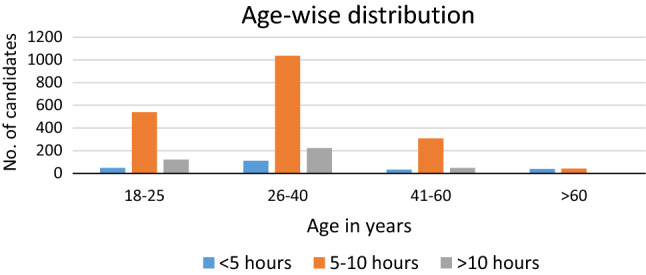
Age-wise distribution
Fig. 2.
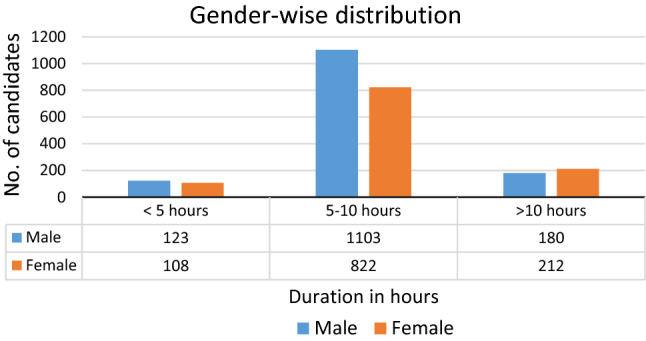
Gender-wise distribution
Clinical symptom score/severity represented in Figs. 3 and 4. Co-morbidity and habit profile shown in Figs. 5 and 6. Candidates’ educational qualification noted (Fig. 7).
Fig. 3.
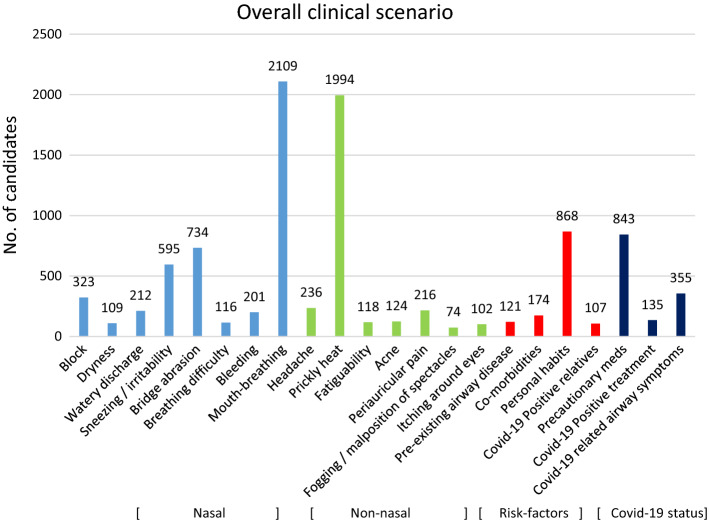
Overall clinical symptoms
Fig. 4.
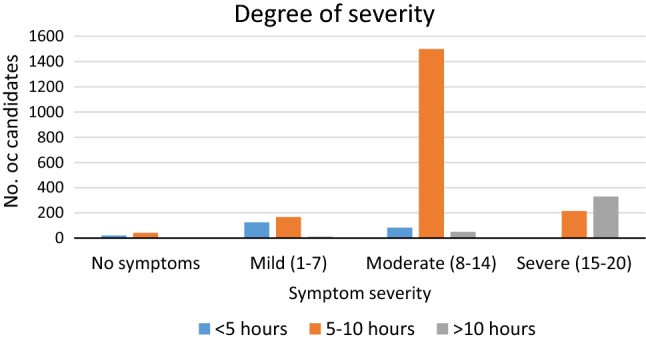
Symptom severity
Fig. 5.
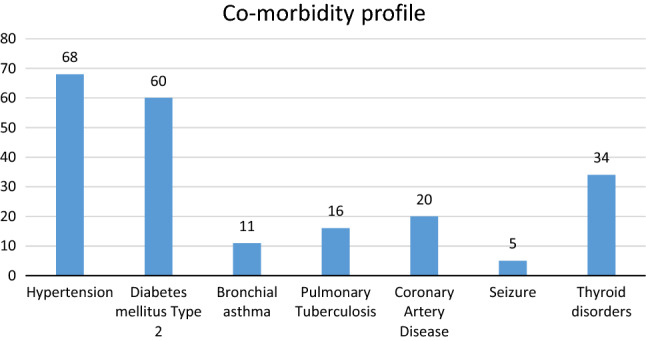
Co-morbidity profile
Fig. 6.
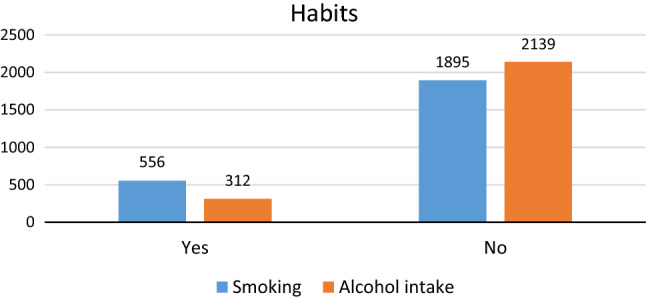
Habits profile
Fig. 7.
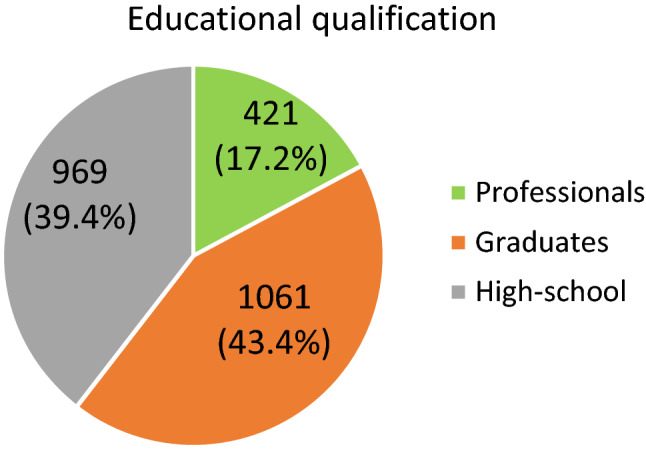
Educational profile of study population
Sf-12 observations and correlation values depicted in Table 2, Fig. 8.
Table 2.
sf-12 analytics
| Sr. no. | Parameter (n = 2451) | Value (n,% / m ± SD) | |
|---|---|---|---|
| Minimum | Maximum | ||
| 1 | PCS-12 | 28.53 | 55.23 |
| 2 | Mean PCS-12 | 41.88 ± 18.87 | |
| 3 | MCS-12 | 33.41 | 44.81 |
| 4 | Mean MCS-12 | 39.11 ± 8.06 | |
| 5 | Correlation co-efficient—Rho (symptom score Vs sf-12) | ||
|
< 5 h − 0.914 |
5–10 h − 0.887 |
> 10 h − 0.679 |
|
Fig. 8.
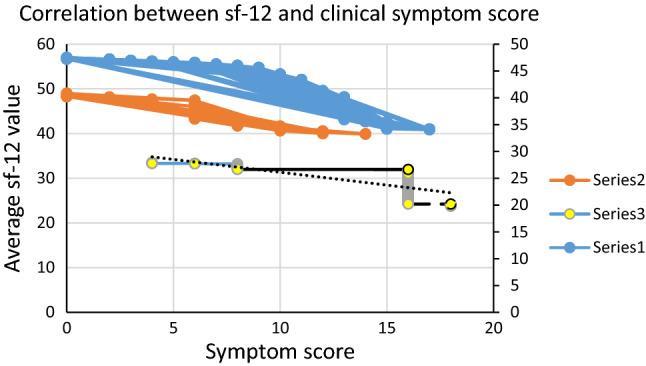
Correlation values. Series 1—< 5 h, Series 2—5–10 h, Series 3—> 10 h
This was a prospective cross-sectional study conducted on healthcare workers involved in managing COVID patients. The study sample size was 2451. Rosner et al. [15] studied the adverse effects of prolonged mask use among healthcare professionals during COVID-19 on a sample of 343. However, Salari et al. [16] provided a systematic review and meta-analysis of 14 centres with a total sample size 44,531.
Our study included personnel using only 3ply mask or higher grades. Use of local alternative masks was an exclusion criterion as its efficiency had not been standardized [7, 8]. The CDC had encouraged the use of cloth masks in the community to prevent asymptomatic spread of Covid-19 [17]. However, since this was an hospital population with a variety of Covid-19 affects and cloth masks provided inferior protection [18]. Reuse of N95 and equivalent respirators has been tested in laboratory settings, but clinical effectiveness and safety of mask re-use in practice are still debatable [19–21]. Godoy et al. [22] studied various mask materials and concluded that, in contrast to 3 M respirators, EX101 did not lose charge on outer layer and worked at a different level of mechanical barrier. Ou et al. [23] and Wang et al. [24] observed that use of mask in general reduces transmission rates during pandemic scenario air/droplet transmission. Study by Lazzarino et al. [25] conveys that face mask usage for prolonged period causes breathing difficulty, as a fraction of carbon dioxide exhaled is inhaled in each cycle of respiration. This in turn increases the frequency and depth of breathing thus increasing the carbon dioxide toxicity. This data was not verified by our study.
The age range of participants in this study was 18–65 years. Overall mean age was 33.43 ± 11.13 years. Mean age of < 5 h group was 37.61 ± 15.23, 5–10 h group was 32.2 ± 10.02 and > 10 h was 30.19 ± 8.15 years respectively. Lim et al. [26] study on Headaches and the N95 face‐mask amongst healthcare providers demonstrated consensual observations with age range of 21–58 years and mean age of 31 ± 7 years.
In contrast to our study with a male preponderance (M:F = 2.4:1), a pilot study by Zhu et al. [27] on effects of long-duration mask usage showed a massive female preponderance (M:F = 1:5.4).
Most common airway symptoms observed [Fig. 3] in the study participants was mouth-breathing (86.04%) followed by nasal irritability (24.27%). Non-nasal symptoms were prickly heat in head and neck region (81.35%) followed by nasal bridge abrasion (29.9%). In another study by Rosner et al. [15], however, the common symptoms were headache (71.4%), acne (53.1%), skin breakdown (51%), impaired cognition (23.6%). Degree of severity of the symptoms was also made mention of [Fig. 4]. In a study by Salunke et al. [28], a simple scale of ABCD was proposed to assess Covid-19 patients presenting at the emergency department.
Our study documented risk-factors of all healthcare workers. 174 (8.48%) had various co-morbidities as mentioned above, in addition to pre-existing airway disease (121, 4.9%), personal habits—smoking and alcohol intake (868, 35.4%) and having Covid-19 positive relatives (107, 4.3%) (Fig. 5). In updates released on Covid-19 risk by WHO and Centres for Disease Control and Prevention (CDC) [29, 30], individuals with similar profile are classified as high- / increased-risk groups.
In a study making a note on pre-existing airway disease in Covid-19 scenario [31], candidates having bronchial asthma was 4% (n = 36) in comparison to our study showing only 0.4% (n = 11) which was around 1/3rd of the observed value.
Detailing the co-morbidity profile, [Table 1, Fig. 5] our study showed individuals with systemic hypertension (HTN) to be 2.7% (n = 68); diabetes mellitus type 2 (T2DM)—2.4% (n = 60); coronary artery disease (CAD)—0.8% (n = 20); seizure—0.2% (n = 5) and thyroid disorders—1.38% (n = 34). In studies by Chew et al. [31], Driggin et al. [32] and Nguyen et al. [33] detailing co-morbidities, a higher prevalence of co-morbidities was noted. Ong et al. [34] also studied co-morbidities and psychological affects in Covid-19 frontline health workers but with a smaller sample (n = 158).
Pulmonary tuberculosis history was available for 0.6% (n = 16) [Fig. 5] of the candidates. All had completed their treatment for a minimum of 8 months. In a study by Torun et al. [35], a lesser mortality was noted in patients who already had either BCG vaccination or was frequently exposed to pulmonary tuberculosis patients.
Smoking (22.68%, 556) and alcohol intake history (12.72%, 312) [Fig. 6], was available for 35.4% (n = 868) workers. Cattaruzza et al. [36] had observed a positive relation between smokers and severe Covid-19 (OR = 2.25) and that smokers had a relatively bad prognosis if they developed Covid-19 lung symptoms. However, a direct influence on the disease nature due to alcohol consumption was elaborated in studies by Testino et al. [37], Ruuskanen et al. [38] and Egbe et al. [39]. This line of study was beyond the scope of this article. In Ong et al.’s [34] demographics, only 1.2% (n = 2) were smokers.
4.3% (n = 107) of the participants had 1/more relatives with Covid-19 positivity. We considered this a risk-factor and all the exposed candidates were sent for Covid-19 reverse transcriptase—polymerase chain reaction (RTPCR) test and advised further treatment accordingly after notification to institute’s infection control committee. Islam et al. [40] studied stress levels making mention of how management of Covid-19 positive relatives contributed to higher stress levels.
Educational qualification of study participants represented [Table 1, Fig. 7] were professionals 17.20% (n = 421), graduates 43.40% (n = 1069), high school population 39.40% (n = 969) whereas in a study done by Ong et al. [34], there were 32.3% (n = 51) doctors, 64.6% (n = 102) nurses and 3.2% (n = 5) paramedical personnel. High-school group needed some extra vernacular support to complete questionnaires.
SF-12 questionnaire [14] was used to assess the QOL. In mask users, the observed physical health composite scores (PCS-12) were 55.23, 40.86 and 28.53 in < 5 h, 5–10 h and > 10 h respectively and the mental health composite scores (MCS-12) were 44.81, 39.63 and 33.41 in < 5 h, 5–10 h and > 10 h respectively [Table 2]. The mean overall scores were 41.88 ± 18.87 for PCS-12 and 39.11 ± 8.06 for MCS-12. These values portray an average / below-average QOL in frontline healthcare workers. This questionnaire evaluated only the physical and emotional construct and did not delve into psychological construct. In contrast, apart from sf-12, Jelena et al. [41] and An et al. [42] studied QOL using Short Form-36 (sf-36), Pittsburgh Sleep Quality Index (PSQI), Health-related QOL (HrQOL) tools. Data on psychological affect and sleep quality was also documented.
QOL was assessed across all cadre of healthcare workers whereas An Y et al. [42] studied impact only on nursing staffs. In our study, correlation between SF-12 tool and symptom scale was done for each group (< 5/5–10/ > 10 h) gave coefficients (Rho) − 0.914, − 0.887 and − 0.679 respectively [Fig. 8]. All values suggested a moderate negative correlation implying that higher the symptom score, lesser was the QOL (Table 2). In study by Do et al. [43] correlating eHeal scale psychometric properties of Covid-19 healthcare personnel showed positive correlation (Rho = 0.8).
Limitations
This was an observational study and not interventional, so the natural symptom course could not be elaborated. Only hospital-population studied. Pediatric population not included. No follow-up. We evaluated physical and emotional status and impact on QOL and not the psychological status of the participants.
Conclusion
Majority of healthcare workers are involved in managing Covid-19 patients. It is mandatory to have PPE (including facemasks) throughout the shift. Wearing PPEs continuously results in many adverse effects. Mouth-breathing likely alters the breathing pattern and changes respiratory milieu. This should be emphasized among continuous facemask users and conscious effort should be put on nasal breathing while using PPE. This would probably go a long way in reducing the airway symptoms associated with prolonged facemask usage and give better compliance among healthcare workers.
Effective use of facemask along with recommended precautions will definitely help bring Covid-19 spread to a halt. QOL will definitely improve among face mask users if awareness is adequately disbursed via audio-visual clips and flyers. Adequate hydration, using mild moisturizer creams at bed time, washing face frequently, using correct fitting masks can alleviate the adverse effects of prolonged face mask usage.
Funding
No external funding.
Code Availability
MS Excel was used. Computed with IBM SPCC v26.
Declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
Cleared.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Lai CC, Shih TP, Ko WC, Tang HJ, Hsueh PR. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and corona virus disease-2019 (COVID-19): the epidemic and the challenges. Int J Antimicrob Agents. 2020;17:105924. doi: 10.1016/j.ijantimicag.2020.105924. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Arpin N, Talbot PJ. Coronaviruses and their diseases. Boston, MA: Springer; 1990. Molecular characterization of the 229E strain of human coronavirus; pp. 73–80. [DOI] [PubMed] [Google Scholar]
- 3.Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, Liu L, Shan H, Lei CL, Hui DS, Du B. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–1720. doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Dal Poz MR, Kinfu Y, Dräger S, Kunjumen T, Diallo K (2006) Counting health workers: definitions, data, methods and global results. Geneva, World Health Organization. (Background paper for The world health report 2006; available at: http://www.who.int/hrh/documents/en/)
- 5.World Health Organization (2020) Advice on the use of masks in the context of COVID-19: interim guidance. World Health Organization
- 6.World Health Organization (2020) Infection prevention and control during health care when COVID-19 is suspected: interim guidance. World Health Organization
- 7.European Standards (2019) UNE EN 14683:2019+AC:2019. Medical face masks -requirements and test methods. (https://www.en-standard.eu/une-en-14683-2019-ac2019-medical-face-masks-requirements-and-test-methods/, Accessed 24 Oct 2020)
- 8.F23 Committee, n.d. Specification for performance of materials used in medical face masks. ASTM International. (https://doi.org/10.1520/F2100-19E01, Accessed 24 Oct 2020)
- 9.National Institute for Occupational Safety and Health (NIOSH) (1996) NIOSH guide to the selection and use of particulate respirators. Department of Health and Human Services (DHHS) NIOSH publication number 96-101. (http://www.cdc.gov/niosh/userguid.html, Accessed 24 Oct 2020)
- 10.CEN, E., 2001. 149: 2001 norm: Respiratory protective devices—filtering half masks to protect against particles—Requirements, testing, marking. European Committee for Standardization. (https://shop.bsigroup.com/ProductDetail?pid=000000000030178264, Accessed 24 Oct 2020)
- 11.Thomasnet.com. (2020) How to make N95 masks—a manufacturing guide. [online] Available at: <https://www.thomasnet.com/articles/plant-facility-equipment/how-to-make-n95-masks/> [Accessed 19 Sep 2020]
- 12.U.S. Food and Drug Administration (2020) N95 Respirators, surgical masks, and face masks. [online] Available at: <https://www.fda.gov/medical-devices/personal-protective-equipment-infection-control/n95-respirators-surgical-masks-and-face-masks> [Accessed 19 Sep 2020]
- 13.Klompas M, Morris CA, Sinclair J, Pearson M, Shenoy ES. Universal masking in hospitals in the covid-19. Era N Engl J Med. 2020;382(21):e63. doi: 10.1056/NEJMp2006372. [DOI] [PubMed] [Google Scholar]
- 14.Ware JE, Keller SD, Kosinski M. SF-12: how to score the SF-12 physical and mental health summary scales. New England Medical Center: Health Institute; 1995. [Google Scholar]
- 15.Rosner E. Adverse effects of prolonged mask use among healthcare professionals during COVID-19. J Infect Dis Epidemiol. 2020;6:130. [Google Scholar]
- 16.Salari N, Hosseinian-Far A, Jalali R, Vaisi-Raygani A, Rasoulpoor S, Mohammadi M, Rasoulpoor S, Khaledi-Paveh B. Prevalence of stress, anxiety, depression among the general population during the COVID-19 pandemic: a systematic review and meta-analysis. Glob Health. 2020;16(1):1–1. doi: 10.1186/s12992-019-0531-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.U.S. Centers for Disease Control (2020) Recommendation regarding the use of cloth face coverings, especially in areas of significant community-based transmission. https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/cloth-facecover.html. Accessed 25 Oct 2020
- 18.U.S. Centers for Disease Control (2020) Interim infection prevention and control recommendations for patients with suspected or confirmed coronavirus disease 2019 (COVID-19) in healthcare settings. https://www.cdc.gov/coronavirus/2019-ncov/hcp/infection-controlrecommendations.html. Accessed 25 Oct 2020
- 19.World Health Organization (2020) Shortage of personal protective equipment endangering health workers worldwide. https://www.who.int/news-room/detail/03-03-2020-shortage-of-personal-protectiveequipment-endangering-health-workersworldwide. Accessed 25 Oct 2020
- 20.ECRI (2020) Clinical evidence assessment: Safety of extended use and reuse of N95 respirators. https://assets.ecri.org/PDF/COVID-19-Resource-Center/COVID-19-ClinicalCare/COVID-ECRI-N95-Respiratorsupdated.pdf. Accessed 25 Oct 2020
- 21.U.S. Centers for Disease Control (2020) Decontamination and reuse of filtering facepiece respirators. https://www.cdc.gov/coronavirus/2019-ncov/hcp/ppe-strategy/decontaminationreuse-respirators.html. Accessed 25 Oct 2020
- 22.Godoy LR, Jones AE, Anderson TN, Fisher CL, Seeley KM, Beeson EA, Zane HK, Peterson JW, Sullivan PD. Facial protection for healthcare workers during pandemics: a scoping review. BMJ Glob Health. 2020;5(5):e002553. doi: 10.1136/bmjgh-2020-002553. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ou Q, Pei C, Kim SC, Abell E, Pui DY. Evaluation of decontamination methods for commercial and alternative respirator and mask materials–view from filtration aspect. J Aerosol Sci. 2020;1(150):105609. doi: 10.1016/j.jaerosci.2020.105609. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Wang J, Pan L, Tang S, Ji JS, Shi X. Mask use during COVID-19: a risk adjusted strategy. Environ Pollut. 2020;25:115099. doi: 10.1016/j.envpol.2020.115099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Lazzarino AI, Steptoe A, Hamer M, Michie S (2020) Covid-19: Important potential side effects of wearing face masks that we should bear in mind. BMJ 369 [DOI] [PubMed]
- 26.Lim EC, Seet RC, Lee KH, Wilder-Smith EP, Chuah BY, Ong BK. Headaches and the N95 face-mask amongst healthcare providers. ActaNeurolScand. 2006;113(3):199–202. doi: 10.1111/j.1600-0404.2005.00560.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Zhu JH, Lee SJ, Wang DY, Lee HP. Effects of long-duration wearing of N95 respirator and surgical facemask: a pilot study. J Lung PulmResp Res. 2014;4:97–100. [Google Scholar]
- 28.Salunke AA, Pathak SK, Dhanwate A, et al. A proposed ABCD scoring system for patient's self assessment and at emergency department with symptoms of COVID-19. Diabetes MetabSyndr. 2020;14(5):1495–1501. doi: 10.1016/j.dsx.2020.07.053. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Coronavirus Disease 2019 (COVID-19) [Internet] (2020) Centers for disease control and prevention. [cited 12 Nov 2020]. Available from: https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/people-with-medical-conditions.html
- 30.Coronavirus disease (COVID-19) [Internet] (2020) Who.int. [cited 12 Nov 2020]. Available from: https://www.who.int/emergencies/diseases/novel-coronavirus-2019/question-and-answers-hub/q-a-detail/q-a-coronaviruses
- 31.Chew NW, Lee GK, Tan BY, Jing M, Goh Y, Ngiam NJ, Yeo LL, Ahmad A, Khan FA, Shanmugam GN, Sharma AK. A multinational, multicentre study on the psychological outcomes and associated physical symptoms amongst healthcare workers during COVID-19 outbreak. Brain BehavImmun. 2020;88:559–565. doi: 10.1016/j.bbi.2020.04.049. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Driggin E, Madhavan MV, Bikdeli B, Chuich T, Laracy J, Biondi-Zoccai G, Brown TS, Der Nigoghossian C, Zidar DA, Haythe J, Brodie D. Cardiovascular considerations for patients, health care workers, and health systems during the COVID-19 pandemic. J Am CollCardiol. 2020;75(18):2352–2371. doi: 10.1016/j.jacc.2020.03.031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Nguyen LH, Drew DA, Graham MS, Joshi AD, Guo CG, Ma W, Mehta RS, Warner ET, Sikavi DR, Lo CH, Kwon S. Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study. Lancet Public Health. 2020;5(9):e475–e483. doi: 10.1016/S2468-2667(20)30164-X. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Ong JJ, Bharatendu C, Goh Y, Tang JZ, Sooi KW, Tan YL, Tan BY, Teoh HL, Ong ST, Allen DM, Sharma VK. Headaches associated with personal protective equipment—a cross-sectional study among frontline healthcare workers during COVID-19. Headache J Head Face Pain. 2020;60(5):864–877. doi: 10.1111/head.13811. [DOI] [PubMed] [Google Scholar]
- 35.Torun S, Ozkaya S, Sen N, Kanat F, Karaman I, Yosunkaya S, Dikis OS, Asan A, Eroglu SA, Atal SS, Ayten O (2020) The Characteristics of health care workers with COVID-19 and relationship Between COVID-19 mortality and BCG/tuberculosis history: a multi-center study. medRxiv
- 36.Cattaruzza MS, Zagà V, Gallus S, D’Argenio P, Gorini G. Tobacco smoking and COVID-19 pandemic: old and new issues. A summary of the evidence from the scientific literature. Acta Bio MedicaAteneiParmensis. 2020;91(2):106. doi: 10.23750/abm.v91i2.9698. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Testino G, Leone S, Borro P. Alcoholic liver disease and the hepatitis C virus: an overview and a point of view. Minerva Med. 2016;107(5):300–313. [PubMed] [Google Scholar]
- 38.Ruuskanen O, Lahti E, Jennings LC, Murdoch DR. Viral pneumonia. The Lancet. 2011;377(9773):1264–1275. doi: 10.1016/S0140-6736(10)61459-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Egbe CO, Londani M, Parry CD, Myers B, Shuper PA, Nkosi S, Morojele NK. Tobacco use and nicotine dependence among people living with HIV who drink heavily in South Africa: a cross-sectional baseline study. BMC Public Health. 2019;19(1):1684. doi: 10.1186/s12889-019-8047-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Islam SD, Bodrud-Doza M, Khan RM, Haque MA, Mamun MA. Exploring COVID-19 stress and its factors in Bangladesh: a perception-based study. Heliyon. 2020;6(7):e04399. doi: 10.1016/j.heliyon.2020.e04399. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Stojanov J, Malobabic M, Stanojevic G, Stevic M, Milosevic V, Stojanov A. Quality of sleep and health-related quality of life among health care professionals treating patients with coronavirus disease-19. The Int J Soc Psychiatry. 2020 doi: 10.1177/0020764020942800. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.An Y, Yang Y, Wang A, Li Y, Zhang Q, Cheung T, Ungvari GS, Qin MZ, An FR, Xiang YT. Prevalence of depression and its impact on quality of life among frontline nurses in emergency departments during the COVID-19 outbreak. J Affect Disord. 2020;1(276):312–315. doi: 10.1016/j.jad.2020.06.047. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Do BN, Tran TV, Phan DT, Nguyen HC, Nguyen TT, Duong V (2020) Health literacy, eHealth literacy, adherence to infection prevention and control procedures, lifestyle changes, suspected COVID-19 symptoms among health care workers: an online survey during the lockdown. J Med Internet Res [DOI] [PMC free article] [PubMed]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
MS Excel was used. Computed with IBM SPCC v26.