Abstract
Background:
Neuroimmunology/multiple sclerosis is a rapidly evolving, but still poorly defined subspecialty. Fellowship training is not standardized, and there is substantial variability across sites. Outcomes of fellowship training have not yet been studied. We therefore examined early career choices of neuroimmunology/MS fellowship program graduates and solicited the perspective of current and recent trainees on their fellowship experience as well as opportunities to improve neuroimmunology education.
Methods:
We developed a questionnaire to collect information about fellowship training experiences and current medical practice. We identified recent graduates based on records from US training programs and the National MS Society and electronically sent the survey to current trainees and recent graduates (within the last 5 years).
Results:
We identified 179 current/recent trainees and successfully reached 157 with survey distributions. Ninety-five individuals (60.5%) returned surveys. Most graduates assumed an academic practice (68%) focused mostly or exclusively on MS and other CNS neuroimmune diseases (55%), and practiced in regions where there were ≥5 other neuroimmunology specialists (51%). Graduates felt well-prepared to manage diagnoses of MS and neuromyelitis optica spectrum disorders but their comfort with rarer CNS neuroimmune diseases varied substantially. Basic immunology, neuro-rheumatology, grant writing and neuro-rehabilitation were identified as high impact areas for cross-disciplinary didactic training. The majority of recent trainees (57%) favored standardizing a core neuroimmunology curriculum, and 48% favored developing a subspecialty certification.
Conclusions:
This is the first study to examine practice outcomes and trainee experiences for neuroimmunology training programs. We anticipate that these data will help educators define a core curriculum for the subspecialty and identify complementary skill sets that enhance the traditional clinic-based model of teaching.
Keywords: Neuroimmunology, Multiple sclerosis, Graduate medical education
1. Introduction
Neuroimmunology is a rapidly growing subspecialty. Its growth has been fueled by the increasing specificity with which autoimmune syndromes can be identified (Lopez-Chiriboga and Clardy, 2017; Linnoila and Pittock, 2016) as well as by the expansion of immunomodulatory treatment options for multiple sclerosis (MS) and other central nervous system (CNS) neuroimmune disorders (Pittock et al., 2019; Cree et al., 2019; Yamamura et al., 2019; Comi et al., 2017). Each immunomodulatory therapy comes with unique side effects and toxicities, and it is becoming essential for patient safety that prescribing physicians have comprehensive knowledge of both the diagnostic differential and the nuances of treatment options. Moreover, most CNS autoimmune conditions are relapsing, chronic diseases that span decades. The neurology clinic frequently becomes the patient’s primary medical home, and their neurologists are required to develop targeted skills in complementary sub-disciplines including neuro-rehabilitation, urogynecology, psychiatry and pain management, or to build multidisciplinary care teams incorporating members of these specialties (Soelberg Sorensen et al., 2019; Gallien et al., 2014).
The evolution in diagnostic sensitivity, immunomodulatory treatments and multidisciplinary management necessitates practitioners of neuroimmunology to delineate the scope of their subspecialty and reach consensus about how mastery of the field should be achieved and demonstrated. We previously surveyed nearly 70 training programs in the United States and described training practices (Obeidat et al., 2020). While most programs reported that their trainees received training in a variety of CNS demyelinating disorders, there was substantial heterogeneity in curriculum content across the sites. Outcomes for the current model of neuroimmunology graduate training are not known. Building on this work, we surveyed recent graduates to determine their practice patterns and to establish how successfully their graduate programs prepared them for clinical practice. Further, we solicited opinions from current trainees and recent graduates on what content should be included in a neuroimmunology curriculum. We also asked for their views on several hot topics including whether neuroimmunology fellowship training curriculum should be standardized and whether the subspecialty should pursue formal certification.
2. Methods
We identified 179 neurologists who were enrolled in or within 5 years of graduation from a clinical neuroimmunology/MS fellowship as of August 2019. We identified participants by (1) direct contact with programs and (2) records of National MS Society clinical fellowship awardees. We obtained trainees’ contact information via communication with their training programs and the member directory of the American Academy of Neurology. Contact information were accurate for 157 neurologists.
We designed a survey using the secure, web-based Qualtrics platform and emailed it to all recent graduates and current trainees (Appendix A). We requested information from graduates about their current employment and scope of practice. We also asked trainees and graduates about their training experience, preparedness for independent practice, and opinions on areas where fellowship training could be improved. An open-ended question requested additional comments about training or other related topics. Survey reminders were sent periodically to survey nonresponders.
We used SPSS v.26 (IBM Corp) for statistical analyses. Missing data were dropped. The Yale University Institutional Review Board determined this protocol to be exempt under federal regulation 45 CFR 46.104(d)(4).
3. Results
3.1. Outcomes of neuroimmunology/MS training programs
Ninety-five neurologists returned surveys (60.5% response rate), with 88 individuals completing all assigned questions. Among respondents, 83 had completed fellowship within the last 5 years and 10 were still in training. Two individuals reported that it had been more than 5 years since graduation.
Most graduates joined an academic institution (54/80, 68%). Seventeen reported being employed by a hospital system (21%), while only 4 individuals entered private practice (5%). Clinical activities comprised the largest proportion of full time effort (FTE), primarily outpatient (median 60%, range 10–100%) and to a lesser extent, inpatient care (median 15%, range 0–60%). Administrative responsibilities occupied a median of 10% of FTE (range 0–45%). While most neuroimmunologists incorporated some research into their practice (39/65 reported spending >10% effort on research), only 11/65 had ≥50% research effort. Research activities occupied a median of 17% FTE (range 0–90%). Those who completed longer fellowships spent a higher proportion of their effort on research (Spearman’s rho 0.467, p<0.0001 correlating quartiles of FTE with years of fellowship training).
Graduates continued to function as subspecialists, with 24% (19/80) seeing exclusively MS/neuroimmunology patients and an additional 31% seeing mostly MS/neuroimmunology. The majority continued to practice in subspecialist-rich regions, with 51% (41/80) reporting at least five other fellowship trained neuroimmunologists in their geographic region (within 100 miles). Five individuals (6%) reported being the only neuroimmunologist in their region. Table A.1 shows details of practice outcomes.
3.2. Graduate experience of neuroimmunology training
Most graduates (69/76, 91%) felt that their training programs prepared them “extremely well” or “very well” for their subsequent employment. The duration of fellowship training ranged from 1–4 years, with the majority (43/80, 54%) completing a one-year fellowship. Almost all fellows (79/86, 92%) participated in clinical research during training and received programmatic support to attend at least one national meeting (75/86, 87%). Thirteen percent of fellows (11/86) participated in non-subspecialty clinics (e.g. General Neurology) to help support their salaries during training.
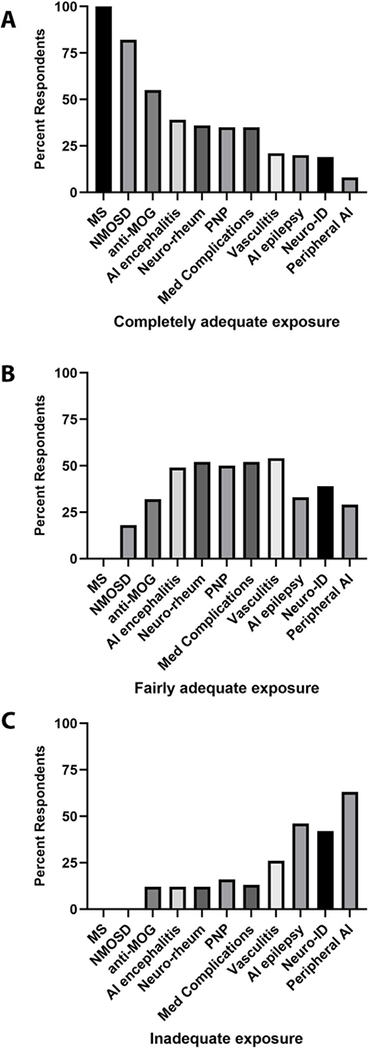
A variety of diagnoses were encompassed by neuroimmunology/MS training programs, with opportunities for exposure to rare diseases varying by program. All graduates felt fully equipped to manage MS, and most also reported a strong background in neuromyelitis optica spectrum disorders (NMOSD) and anti-MOG associated disorders (Fig. 2). Other disease areas showed more heterogeneity but overall, graduates felt fairly well prepared to manage autoimmune encephalitis, neurologic complications of systemic autoimmune diseases and biologic medications, paraneoplastic disorders and vasculitis. On the other hand, a large proportion of graduates did not feel equipped to manage autoimmune epilepsy, neuro-infectious diseases and peripheral autoimmune conditions.
Fig. 2.
Self-reported exposure to neuro-immunologic diagnoses during fellowship training. n = 82–84 respondents. Med complications was defined as “neurologic complications of biologic drugs”. MS: multiple sclerosis, NMO: neuromyelitis optica, MOG: myelin-oligodendrocyte glycoprotein, AI: autoimmune, PNP: paraneoplastic, ID: infectious disease.
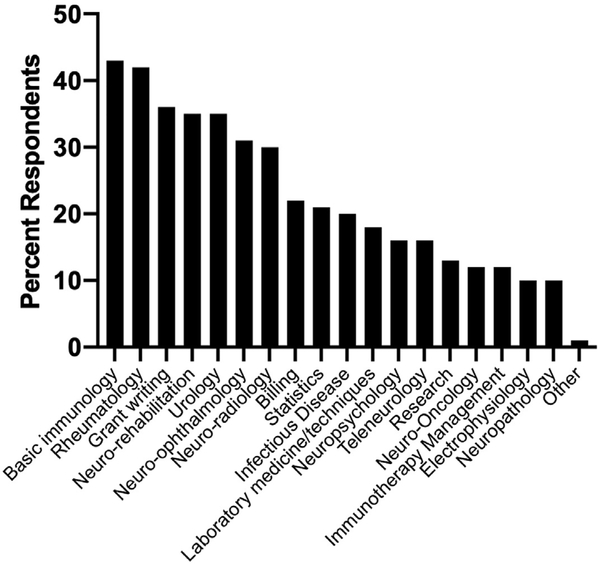
Graduates identified several areas where additional training would have enhanced their transition to independence. 69% (52/76) felt only “somewhat prepared” or “not prepared” to handle logistical issues pertaining to patient care, including insurance appeals, prior authorizations, disability paperwork and similar problems. Also, many trainees felt that dedicated training in subjects beyond the traditional neuroimmunology/MS clinic would have further enhanced their learning. Formal training in basic immunology (47%), rheumatology (45%), grant writing (39%), neuro-rehabilitation (38%), urology (38%), neuro-ophthalmology (33%) and neuro-radiology (32%) were of particular interest (Fig. 1).
Fig. 1.
Supplementary curricular options. Respondents were asked to identify areas where additional training would have enhanced their education. n = 88 completed surveys.
3.3. Future directions for the neuroimmunology/MS subspecialty
The majority of respondents (48/84, 57%) felt that a standardized core curriculum would enhance neuroimmunology/MS training. Another 41% (n = 34) were undecided, with only 2 individuals opposed to standardizing a core curriculum. Interestingly, a large proportion of recent graduates also supported pursuing subspecialty certification (41/85, 48%). Thirteen individuals were opposed to subspecialty certification, while the rest (31/85, 37%) were neutral.
Forty-three respondents provided free text comments on the topic of subspecialty certification (representative comments clustered by theme in Appendix B). Commonly identified drawbacks to subspecialty certification centered around inconveniences to the subspecialist, including the introduction of additional testing requirements (n = 11), cost (n = 17) and time/administrative burden (n = 4). There was a concern that certification might result in loss of flexibility for customized training based on individual career goals, which was perceived as a strength of the current model (n = 6). Several respondents also pointed out that lack of evidence-based guidelines and the rapidly changing nature of neuroimmunology would hinder the creation and maintenance of certification standards. A few were concerned that certifying neuroimmunology/MS as a subspecialty could paradoxically impair patients’ ability to access qualified care providers and effective treatments. On the other hand, there were perceived benefits of subspecialty certification. Many felt that certification would validate the subspecialty and clearly differentiate fellowship-trained neuroimmunologists (n = 14). Many viewed content standardization (n = 13) as an additional benefit and felt that clearly identifying the experts in this field would improve patient safety (n = 11). A few individuals mentioned the potential for improved reimbursements (n = 3), lobbying power (n = 1) and financial support for trainees (n = 2) which might accompany certification. Finally, several felt that maintaining certification would help to ensure neuroimmunology specialists stayed abreast of the rapidly evolving field (n = 3).
4. Discussion
We previously examined the scope of neuroimmunology and MS fellowship training in the USA (Obeidat et al., 2020). Here, we further explored the outcomes of neuroimmunology training programs along with the perspective of recent graduates on ways to further enhance training in MS and neuroimmunology.
4.1. Outcomes for neuroimmunology/MS training programs
Recent graduates of US neuroimmunology/MS fellowships were predominantly employed by academic institutions and appear to be geographically clustered. This mirrors the trend for the training programs themselves, which are disproportionately on the East and West Coasts (Obeidat et al., 2020). This trend has implications for patient access to care. Moreover, although research is integral to most training programs and nearly all trainees participated in research, far fewer continued to devote substantial effort to research as attendings. This observation is surprising, given that most were employed by universities, and may warrant further evaluation. It is possible that trainees pursuing a research career were not fully captured by our sample, which was targeted towards clinical fellows and did not include individuals in research-based postdoctoral training. Nevertheless, 47% of our respondents spent 2 years or longer in fellowship. Such multi-year training typically signifies commitment to achieving substantial research or educational goals (e.g. masters’ degree) during fellowship. That research was not a primary focus after graduation could suggest that employers are not supporting research effort for new hires, or that more senior neuroimmunologists are receiving the majority of clinical research opportunities. Also of note, few trainees entered private practice, and many clinical trials rely on private practices for recruitment. This could have implications on the future recruitment and conduct of clinical trials if fellowship-trained neurologists are not entering the private practice workforce. Further investigation is warranted.
4.2. Training experience: curriculum & opportunities for improvement
Neuroimmunology/MS fellowship training has historically focused on MS and NMOSD, and reassuringly, almost all graduates reported excellent training in these areas (Fig. 2). Nevertheless, the scope of the subspecialty continues to expand. There is now consensus that autoimmune encephalitis and other diseases associated with pathologic autoantibodies fall within the scope of the subspecialty, and CNS complications of systemic autoimmune diseases or biologic medications (such as checkpoint inhibitors) are also encompassed. Graduates of neuroimmunology/MS training programs are expected to have the knowledge and basic capacity to manage the breadth of autoimmune CNS disease (Obeidat et al., 2020).
Gaining competency in diagnosing and managing rarer CNS neuroimmune conditions poses challenges for many trainees, as exposure to these conditions varies substantially across centers. A subset of training programs has particular expertise in non-MS neuroimmune diseases, and graduates from these programs often narrow their scope of practice accordingly. Nevertheless, the national demand for neuroimmunologic care is such that all training programs must build the capacity to impart expertise across the spectrum of CNS neuroimmune disease. Opportunity exists for national collaborations that leverage center-based expertise to provide standardized didactic and case-based teaching around these rare diagnoses.
Both program directors (Obeidat et al., 2020) and recent graduates favored the development and implementation of a core, standardized neuroimmunology curriculum, while maintaining program-level flexibility and trainee-centered customization. Such a curriculum would identify a core group of diagnoses and skills for which all fellows would be expected to gain mastry. In addition to covering the CNS neuroimmune diseases discussed previously, such a curriculum would incorporate cross-disciplinary training on topics designed to complement fellows’ typical neurology experiences (Fig. 1). Such topics should include cross-disciplinary teaching (e.g. from rheumatologists or urologists) as well as more mundane information such as how to manage insurance-related barriers to care and billing. Providing additional education on how to function in private practice might help improve patient access to fellowship-trained neuroimmunologists. While individual programs would have autonomy in determining the best methods for implementing this curriculum, many of these topics could be addressed systematically by building a nationally available, shared library of didactic and case-based teaching material, or by utilizing video conferencing technology to host live conferences nationally or regionally. Existing programs, such as the monthly case conferece hosted by the National MS Society, could be leveraged or expanded to facilitate this. Developing and implementing such a core curriculum will be the next step in the evolution of the subspecialty.
The issue of subspecialty certification has been under discussion by the Neuroimmunology/MS community for many years, without consensus. Opinions on this subject have not previously been solicited from the more junior members of the community. Surprisingly, more recent graduates favored certification (48%) than opposed it (13%), with a large proportion remaining undecided. One important consideration remains a potential loss of training flexibility with increasing standardization. Neuroimmunology/MS fellowships have historically afforded trainees the discretion to tailor their training experience to their personal career goals by pursuing targeted electives (e.g. research training or Botox injections). Standardization efforts will need to focus on defining the scope of training and establishing minimal competencies; individual-level flexibility for personalized training should be maintained. The pros/cons of certification expressed by this cohort of junior neuroimmunologists (Appendix B) will help inform this ongoing national conversation.
While we achieved a 60% response rate to our survey, it is possible that individuals practicing in certain environments (e.g. private practice, rural areas) may have been less likely to respond. Additionally, while we confidently identified trainees from large training programs and those supported by non-profit funds (National MS Society), it is possible that some trainees from small centers or those funded by for-profit sources may have been missed. Selection bias is therefore possible, which could impact the reported practice patterns. Moreover, these data reflect practice trends within the United States only. Nevertheless, these data uniquely delineate outcomes of neuroimmunology training for a large number of trainees and generate critical information about the educational needs of neuroimmunology practitioners. This information will be foundational to ongoing work on developing a standardized neuroimmunology curriculum and thus enhancing the care of patients with CNS neuroimmune conditions.
Supplementary Material
Acknowledgments
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Table A1.
Demographics for neuroimmunology program graduates.
| Demographics for neuroimmunology program graduates n = 80 | |
| Years since graduation, n (%) | |
| ≤1 | 29 (36) |
| 2 | 16 (20) |
| 3 | 19 (24) |
| 4 | 8 (10) |
| 5 | 8 (10) |
| Years in fellowship, n (%) | |
| 1 | 43 (54) |
| 2 | 26 (33) |
| 3 | 10 (13) |
| 4 | 1 (1) |
| Current practice, n (%) | |
| Academic physician | 54 (68) |
| Hospital employed | 17 (21) |
| Private practice | 4 (5) |
| Other | 5 (6) |
| Proportion of Neuroimmunology/MS seen in clinical practice, n (%) | |
| 100% | 19 (24) |
| 75% | 25 (31) |
| 50% | 17 (21) |
| <50% | 14 (18) |
| Missing | 4 (5) |
| Percent effort, median (range) | |
| Outpatient | 60 (10–100) |
| Inpatient | 15 (0–60) |
| Research/Academic | 17 (0–90) |
| Administrative | 10 (0–45) |
| Other neuroimmunologists within 100 miles (n,%) | |
| 0 | 5 (6) |
| <5 | 30 (38) |
| ≥5 | 41 (51) |
| Missing | 4 (5) |
Footnotes
Disclosures
Ahmed ZObeidat reports personal compensation for consulting, speaking or serving on steering committees or advisory boards for Genzyme, Biogen, Novartis, Alexion Pharmaceuticals, Genentech, Celgene, EMD Serono, Bristol Myers Squibb, Research support from the Center for Immunology at the Medical College of Wisconsin and Research Affairs Committee and serving on the editorial board of the International Journal of MS Care.
Le H Hua reports personal compensation for speaking, consulting or advisory board activities from Biogen, Genzyme, Novartis, Celgene/Bristol Myers Squibb, Genetech and EMD Serono.
Erin ELongbrake reports personal compensation for consulting for Biogen, Celegene/Bristol Myers Squibb, Genentech, Alexion, Genzyme, EMD Serono. Research support from the Race to Erase MS and NIH K23NS107624.
Supplementary materials
Supplementary material associated with this article can be found, in the online version, at doi:10.1016/j.msard.2020.102296.
References
- Comi G, Radaelli M, Soelberg Sorensen P, 2017. Evolving concepts in the treatment of relapsing multiple sclerosis. Lancet 389, 1347–1356. [DOI] [PubMed] [Google Scholar]
- Cree BAC, Bennett JL, Kim HJ, et al. , 2019. Inebilizumab for the treatment of neuromyelitis optica spectrum disorder (N-MOmentum): a double-blind, randomised placebo-controlled phase 2/3 trial. Lancet 394, 1352–1363. [DOI] [PubMed] [Google Scholar]
- Gallien P, Gich J, Sanchez-Dalmau BF, Feneberg W, 2014. Multidisciplinary management of multiple sclerosis symptoms. Eur. Neurol 72 (Suppl 1), 20–25. [DOI] [PubMed] [Google Scholar]
- Linnoila J, Pittock SJ, 2016. Autoantibody-associated central nervous system neurologic disorders. Semin. Neurol 36, 382–396. [DOI] [PubMed] [Google Scholar]
- Lopez-Chiriboga AS, Clardy SL, 2017. Emerging subspecialties in neurology: autoimmune neurology. Neurology 89, e129–e133. [DOI] [PubMed] [Google Scholar]
- Obeidat AZ, Jassam YN, Hua LH, et al. , 2020. Education research: multiple sclerosis and neuroimmunology fellowship training status in the United States. Neurology 94, 495–500. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Pittock SJ, Berthele A, Fujihara K, et al. , 2019. Eculizumab in aquaporin-4-positive neuromyelitis optica spectrum disorder. N. Engl. J. Med 381, 614–625. [DOI] [PubMed] [Google Scholar]
- Soelberg Sorensen P, Giovannoni G, Montalban X, Thalheim C, Zaratin P, Comi G, 2019. The multiple sclerosis care unit. Mult. Scler 25, 627–636. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yamamura T, Kleiter I, Fujihara K, et al. , 2019. Trial of satralizumab in neuromyelitis optica spectrum disorder. N. Engl. J. Med 381, 2114–2124. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.