To the editor,
We read with interest the manuscript entitled “Anakinra treatment in critically ill COVID-19 patients: a prospective cohort study” by Kooistra et al. [1] reporting the potential efficacy of anakinra (ANA) to control the hyperinflammation in COVID-19 patients.
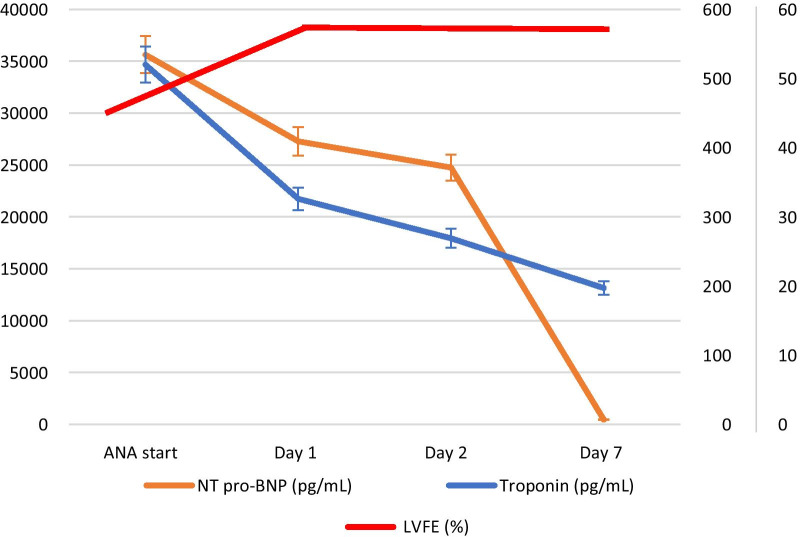
In our clinical practice, we adopted the early use of intravenous ANA for the treatment of cardiac disfunction in Pediatric Inflammatory Multisystem Syndrome temporally associated with SARS CoV-2 infection (PIMS-TS) patients. During the second COVID-19 wave, 9 PIMS-TS children were admitted to Meyer Children’s University Hospital in Florence (mean age of 10.2 y [IQR] 8.5–13). Echocardiography revealed a left ventricular ejection fraction (LVEF) ≤ 40% in 5/9 patients. In these 5 children, ANA was adopted as first-line therapy and administered as continuous intravenous infusion at 10 mg/kg/day (400 mg/day maximum dose). Within the first day of ANA therapy, fractionated IVIG (2 g/kg) and intravenous steroids (one methylprednisolone pulses [30 mg/kg/day, maximum 1 g/day] in 3 consecutive days followed by 1 mg/kg/day intravenous methylprednisolone) were subsequently associated. At median time of 24 h (range 12–36 h) from starting ANA, all patients restored LVEF to > 55% along with a progressive reduction of troponin and N-terminal pro B-type natriuretic peptide (NT pro-BNP) values (Fig. 1). A concomitant reduction until discontinuation of inotropic support was obtained together with the recovery of clinical sings and inflammatory parameters.
Fig. 1.
Trend of mean NT pro-BNP and troponin values in relation to PIMS-TS patients’ LVEF after starting anakinra (ANA)
In order to prevent the inflammatory rebound, ANA therapy was tapered in 2 weeks, then switched subcutaneously and stopped after 5 weeks (range 4–6).
One month after discharge, echocardiography reported stably normal findings.
The early use of ANA prompted a rapid and sub-stained LEVF improvement over one day from admission. Our results further support the assumption that an aggressive, early and overtime immunomodulatory approach in PIMS-TS patients with myocardial involvement may induce a faster time to recovery, as quickly damping the cytokine storm [2, 3]. However, the cumulative effect of ANA in combination with subsequent IVIG and steroid use could be advocated as effective in restoring a normal LVEF. Due to the poor peripheral perfusion and hemodynamic instability into the early phases of PIMS-TS, continuous intravenous infusion may be the preferable administration route. Subcutaneous injections might be considered as maintenance therapy after achieving stable conditions [3].
Future randomized controlled trials and long-term follow-up could test the hypothesis that a step-down immunomodulatory approach could be preferred in PIMS-TS patients experiencing myocardial disfunction to avoid a further progression and/or the onset of sequalae over time.
Acknowledgements
Not applicable.
Authors' contributions
MVM collected the data. GS and MVM designed the study. MVM wrote the first draft of the manuscript. All the authors revised and accepted the manuscript.
Funding
No funding was secured for this study.
Availability of data and materials
The complete clinical reports of each patient are available for the reviewers if requested.
Declarations
Ethics approval and consent to participate
Not applicable.
Consent for publication
All authors agreed for pblication.
Competing interests
The authors have no example conflicts of interest to disclose..
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Kooistra EJ, Waalders NJB, Grondman I, Janssen NAF, de Nooijer AH, Netea MG, et al. Anakinra treatment in critically ill COVID-19 patients: a prospective cohort study. Crit Care. 2020;24(1):688. doi: 10.1186/s13054-020-03364-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Belhadjer Z, Méot M, Bajolle F, Khraiche D, Legendre A, Abakka S, et al. Acute heart failure in multisystem inflammatory syndrome in children in the context of global SARS-CoV-2 pandemic. Circulation. 2020;142(5):429–436. doi: 10.1161/CIRCULATIONAHA.120.048360. [DOI] [PubMed] [Google Scholar]
- 3.Belhadjer Z, Auriau J, Méot M, Oualha M, Renolleau S, Houyel L, et al. Addition of corticosteroids to immunoglobulins is associated with recovery of cardiac function in multi-inflammatory syndrome in children. Circulation. 2020;142(23):2282–2284. doi: 10.1161/CIRCULATIONAHA.120.050147. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Evans C, Davies P. SARS-CoV-2 paediatric inflammatory syndrome. Paediatr Child Health. 2021;31(3):110–115. doi: 10.1016/j.paed.2020.12.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Ramcharan T, Nolan O, Lai CY, Prabhu N, Krishnamurthy R, Richter AG, et al. Paediatric inflammatory multisystem syndrome: temporally associated with SARS-CoV-2 (PIMS-TS): cardiac features, management and short-term outcomes at a UK Tertiary Paediatric Hospital. Pediatr Cardiol. 2020;41(7):1391–1401. doi: 10.1007/s00246-020-02391-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Gorelik M, Lee Y, Abe M, Andrews T, Davis L, Patterson J, et al. IL-1 receptor antagonist, anakinra, prevents myocardial dysfunction in a mouse model of Kawasaki disease vasculitis and myocarditis. Clin Exp Immunol. 2019;198(1):101–110. doi: 10.1111/cei.13314. [DOI] [PMC free article] [PubMed] [Google Scholar]