Abstract
The renin–angiotensin–aldosterone system and its metabolites play an important role in homeostasis of body, especially the cardiovascular system. In this study, we discuss the imbalance of multiple systems during the infection and the importance of therapeutic choice, dosing, and laboratory monitoring of cardiac and anti-coagulant therapies in COVID-19 patients. The crosstalk between angiotensin, kinin-kallikrein system, as well as inflammatory and coagulation systems plays an essential role in COVID-19. Cardiac complications and coagulopathies imply the crosstalks between the mentioned systems. We believe that the blockage of bradykinin can be a good option in the management of COVID-19 and CVD in patients and that supportive treatment of respiratory and cardiologic complications is needed in COVID-19 patients. Ninety-one percent of COVID-19 patients who were admitted to hospital with a prolonged aPTT were positive for lupus anticoagulant, which increases the risk of thrombosis and prolonged aPTT. Therefore, the question that is posed at this juncture is whether it is safe to use the prophylactic dose of heparin particularly in those with elevated D‐dimer levels. It should be noted that timing is of high importance in anti-coagulant therapy; therefore, we should consider the level of D-dimer, fibrinogen, drug-drug interactions, and risk factors during thromboprophylaxis administration. Fibrinogen is an independent predictor of resistance to heparin and should be considered before thromboprophylaxis. Alteplase and Futhan might be a good choice to assess the condition of heparin resistance. Finally, the treatment option, dosing, and laboratory monitoring of anticoagulant therapy are critical decisions in COVID-19 patients.
Keywords: SARS-CoV-2, Bradykinin, Coagulation, Cytokine storm, Cardiac complications
Introduction
COVID-19 is caused by the single positive stranded RNA virus known as severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), which enters into human body via the mucosa of respiratory or digestive tracts or eyes using cell receptors such as angiotensin-converting enzyme 2 (ACE2). SARS-CoV-2 mainly penetrates into the cells via the interaction of spike protein (S protein) and ACE2. Interestingly, S protein needs processing before its interaction process is mediated by proteases such as transmembrane protease serine 2 (TMPRSS2), cellular protease furin and cathepsin L [1, 2]. Recent studies have indicated that SARS-CoV-2 uses other cell receptors such as CD26, Ezrin, Neuropilin-1 (NRP-1), and Extracellular matrix metalloproteinase inducer (EMMPRIN)/CD147 for its entry. It has also been reported that disintegrin and metalloproteinase 17 (ADAM17) as a zinc metalloprotease play a catalytic role on ACE2, mediate ACE2 processing, and increase viral cell entry [3–5]. The main problem of COVID-19 is that the binding of SARS-CoV-2 to ACE2 leads to ACE2 downregulation, which increases the production of Ang II but reduces angiotensin 1–7, leading, in turn, to lung dysfunction [6, 7]. Additionally, ACE2 is an interferon stimulated gene (ISG) that is increased during cytokine storm and augments viral entry [8]. In another hand, COVID-19 virus disrupts renin–angiotensin–aldosterone system (RAAS) and coagulation systems, decreasing the capacity of removing poisonous metabolites and increasing the cardiovascular considerations of patients [9–11]. In this comprehensive review, we discuss the challenging aspect of COVID-19, namely the imbalanced mechanisms such as inflammation, RAAS and coagulation as well as implication of cardiac complications. We also discuss the benefits of candidate CVD drugs against SARS-CoV-2.
COVID-19 and the imbalance problem
Imbalanced renin–angiotensin aldosterone system (RAAS) and therapeutic challenges
Initially, SARS-CoV-2 cell entry and infection depend on ACE2/TMPRSS2 co-expression as well as ACE2 expression (12). ACE2 is activated and downregulated by S protein and is involved in SARS-CoV-2 entry into epithelial cells and myocardium [13]. Decreased ACE2 expression induces heart injury that reflects the protective effect of cellular ACE2 [14]. In fact, ACE2 is a double-edged sword and a major regulator of blood pressure as well as fluid and electrolyte balance. ACE2 is involved in the conversion of Ang I into Ang II, which exerts its effects through angiotensin II type 1 and type 2 receptors (AT1R and AT2R) [15]. Notably, AT1R is responsible for the activation of vasoconstrictive pathways while AT2R stimulates vasodilation to ensure balance. Importantly, overactivation of ACE/Ang II/AT1R axis is associated with the pathogenesis of proliferation, oxidative stress, inflammation, and fibrosis leading to the onset of pathological disorders including lung, renal and cardiovascular diseases. On the other hand, ACE2 is known to activate the inhibitory arm of RAAS as it converts Ang II into angiotensin (1–7), which counteracts the harmful actions of Ang II via activation of AT2R and G-coupled receptor Mas receptor (MasR) [16, 17]. AngII and AT1R interaction increases sodium and water conservation, aldosterone release, and myocardial remodeling [18]. However, studies have shown that the decrease in plasma Ang II/Ang 1–7 ratio induces ACE2 function. SARS-CoV-2 not only decreases ACE2 expression but also increases Ang II/ANg 1–7 ratio [19]. Liu et al. revealed that Ang II levels increase in COVID-19 patients such that anti-hypertensive AT1R blockers (ARBs) can reduce disease severity in the elderly [20]. ACE2 converts angiotensin I (Ang I) and II (Ang II) to Ang 1–9 and Ang 1–7, although Ang II binds to Ang II receptor type 1 (AT1R) and induces inflammation [21]. However, Ang 1–7 plays a protective role via binding to Mas-1 receptor (Mas-1R) and suppressing the inflammation via production of anti-inflammatory cytokines [22], and elevated levels of AngII might induce a positive feedback loop, increasing inflammation, coagulation and thrombosis risk [23]. SARS-CoV-2 entry and replication lead to inflammatory responses and inflammatory component production, as well as RAAS imbalance and change in AngII/Ang (1–7) ratio [24]. Since ACE2 expression is upregulated by RAAS inhibitors, viral entry and viral load seem to increase by these drugs and worse the situation [19]. However, Conversano et al. indicated that these therapeutic approaches are not an independent predictor of poor outcome and using these types of treatments are harmless [25]. Studies on Recombinant Human Angiotensin-converting Enzyme 2 (rhACE2) injection indicated successful results in clinical grade, and it can significantly block SARS-CoV-2 in early stages [26] see Fig. 1.
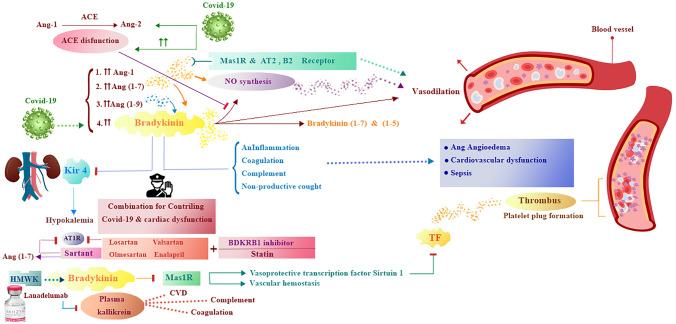
Fig. 1.
Importantly, overactivation of ACE/Ang II/AT1R axis is associated with the pathogenesis of proliferation, oxidative stress, inflammation and fibrosis leading to the onset of pathological disorders including lung, renal and cardiovascular diseases. Increased level of bradykinin and its metabolites enhances inflammation, coagulation and the complement system, and these three systems play an important role in angioedema, cardiovascular dysfunction and sepsis which occur in COVID‐19 patients. Excessive vasodilation happens as a result of Ang (1–7) activation, synthesis of nitric oxide and agonism of AT2, B2, MAS receptors as well as accumulated bradykinin. Ang (1–7) and Ang (1–9) increase bradykinin levels. Bradykinin stimulates renal Na+ and K+ excretion via inhibiting the K+ channel (Kir4.1) in kidney and leads to hypokalemia. Based on recent studies, the accumulation of bradykinin is as important as Ang-II, and it should be balanced in the body to control the harmful effects in COVID-19 patients. Bradykinin is the inflammatory product of coagulation system consisting of factor XII (FXII), plasma prekallikrein (PPK) and high molecular weight kininogen (HK). Bradykinin Receptor B1 (BDKRB1) plays a major role in the outbreak and maintenance of the inflammatory response. Although kinin-kallikrein system crosstalks to RAS, coagulation system and finally the thrombosis leads to organ failure
Imbalanced kallikrein system
In addition to its effects on RAAS and ACE inhibitors, ACE-2 has been shown to cause active bradykinin hydrolysis and thus increased levels of bradykinin and nonproductive coughs as a result of fluid extravasation and leukocyte recruitment to the lung. Studies on serum level of bradykinin have shown its increase in COVID-19 [27]. Increased bradykinin level and its metabolites enhance inflammation, coagulation and the complement system, and these three systems play an important role in angioedema, cardiovascular dysfunction and sepsis which occur in COVID‐19 patients [28]. Interestingly, bradykinin is a major contributor to the innate inflammatory response, and it plays an important role in the increased level of inflammatory cytokines such as TNF-a and IL-1 [29, 30]. Studies on ACE dysfunction indicated the increase of metabolites such as Ang-1, Ang (1–9), Ang (1–7) and bradykinin. Excessive vasodilation happens as a result of Ang (1–7) activation, synthesis of nitric oxide and agonism of AT2, B2, MAS receptors as well as accumulated bradykinin [31]. Interestingly, Ang (1–7) and Ang (1–9) increase bradykinin levels [32, 33]. Bradykinin stimulates renal Na+ and K+ excretion via inhibiting the K+ channel (Kir4.1) in kidney and leads to hypokalemia [34]. Hypokalemia and hypomagnesemia are two common events observed in COVID-19 patients. Therefore, further studies are needed for finding prognostic and diagnostic molecules to monitor cardiac and cardiovascular dysfunctions in early stages of COVID-19 [35]. Based on recent studies, the accumulation of bradykinin is as important as Ang-II, and it should be balanced in the body to control the harmful effects in COVID-19 patients. Bradykinin is the inflammatory product of the coagulation system consisting of factor XII (FXII), plasma prekallikrein (PPK) and high molecular weight kininogen (HK). Therefore, it is linked to the intrinsic coagulation system via factor XI (FXI) [36]. Bradykinin Receptor B1 (BDKRB1) plays a major role in the outbreak and maintenance of the inflammatory response. Although the kinin-kallikrein system crosstalks to RAS, the coagulation system and finally the thrombosis lead to organ failure [37]. The interaction between kinin-kallikrein and RAAS has a thromboregulatory role independent of the contact pathway and the decrease in bradykinin increases Mas1R expression. This is important in the vascular homeostasis by decreasing thrombosis via increasing the production of vasoprotective transcription factor Sirtuin 1, inhibiting tissue factor (TF) expression, and inhibiting platelet activation [38]. Plasma kallikrein plays an essential role in the cleavage of high molecular weight kininogen (HMWK) into bradykinin and is involved in coagulation, activation of complement system, and CVD [39–42]. Several studies on plasma kallikrein inhibitors in CVD have indicated promising results [43]. Lanadelumab is a monoclonal antibody (mAb) used for the treatment of angioedema that can block plasma kallikrein formation [44, 45]. Lanadelumab can decrease cytokine and coagulation storm and balance complement activation, and COVID-19 patients can benefit from this medicine besides anti-viral therapy [46].
Imbalanced inflammatory responses and cytokine storm
Mortality rates are high among COVID-19 patients when they suffer from diseases such as hypertension, diabetes, and CVD [47]. Strong evidence suggests that COVID-19 patients develop a higher risk of arrhythmic events (7.3%) and heart palpitations. After acute respiratory distress syndrome (ARDS), the prevalence of malignant ventricular arrhythmias rose to 44.4% [48]. Recent studies indicate that myocardial damage might be the main factor of enhanced arrhythmia risk in COVID-19 patients [49, 50]. Cytokine storm is the main factor in the development of myocardial damage and arrhythmia among COVID-19 patients [51]. Increased troponin level is a useful biomarker in targeting cardiac myocyte damage particularly in those with severe COVID-19 disease, which can be helpful in the management of cardiac damage in these patients [52]. COVID-19 is associated with CD4+ and CD8+ T-cell lymphopenia, which increases the imbalance of proinflammatory and anti-inflammatory cytokines [53, 54]. Cytokine storm or cytokine release syndrome (CRS) seems to be the main reason of lung injury and multiple organ failure in SARS-CoV-2 infection [55]. Studies on proinflammatory cytokines indicate that tumor necrosis factor (TNF) α, interleukin 1β (IL-1β), IL-6, L-2, IL-8, IL-17, granulocyte-colony stimulating factor (G-CSF), interferon gamma-induced protein-10, monocyte chemoattractant protein-1 (MCP-1), and macrophage inflammatory proteins 1-α (MIP-1a) significantly increase in SARS-CoV-2 patients [56]. Higher plasma levels of IL-2, IL-7, IL-10, GCSF, IP-10, MCP-1, MIP-1A, and TNF-α are related to cytokine storm and disease severity [57]. Hypersecretion of proinflammatory cytokines plays a critical role in severe conditions, and thus immunosuppressive drugs such as steroids, IL-6 or IL-1 antagonists, Tocilizumab and Selinexor might be effective in balancing severe conditions and decreasing mortality [58, 59]. Targeting the cytokine storm and the imbalanced immune responses can be crucial in COVID-19 treatment and decreasing multiorgan dysfunction [56, 60]. NLRP3 inflammasome might be the major reason of cytokine storm and multi-organ damage in COVID-19 infection. COVID-19 can directly activate NLRP3 and induce IL-1β secretion. Immune response and antiviral response are able to eradicate the infection. However, in immunological dysfunction cases, hyper-inflammation evoke the cytokine storm leading to the lung injury and ARDS development. Therefore, targeting NLRP3 inflammasome can be an appropriate approach in COVID-19 treatment protocols [61]. Activation of NLRP3 inflammasome provokes an immune response via intracellular caspase, which leads to imbalanced proinflammatory cytokine release, humoral response, and complement cascade. NLRP3 inflammasome is a good drug target in SARS-CoV-2 treatment [62]. See Fig. 2.
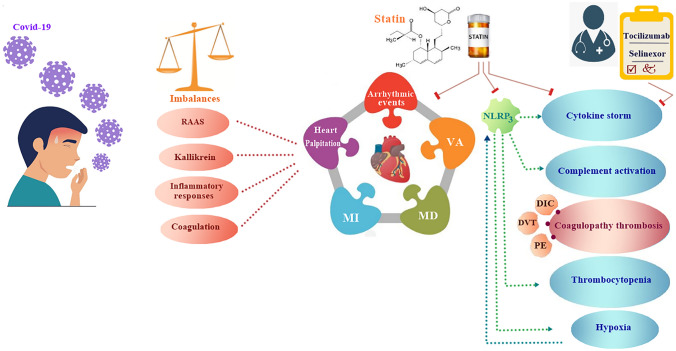
Fig. 2.
COVID-19 patients face multiple-system imbalances. The main imbalances were detected in RAAS, Kallikrein, inflammatory and coagulation systems. These imbalances lead to several cardiac complications such as: Heart palpitation, arrhythmic events, ventricular arrhythmias (VA), myocardial damage (MD) and myocardial infraction (MI). NLRP3 inflammasome might be the major reason of cytokine storm and multi-organ damage in COVID-19 infection; therefore, targeting NLRP3 inflammasome can be a good approach in COVID-19 treatment protocols. Activation of NLRP3 inflammasome provokes an immune response via intracellular caspase, which leads to imbalanced proinflammatory cytokines release, humoral response, and the complement cascade. NLRP3 inflammasome is a good drug target in SARS-CoV-2 treatment so Statin can be one of our best choices in COVID-19 treatment because it affects NLRP3, Cardiac complications and cytokine storm. Additionally, Tocilizumab and Selinexor are strong choices in managing cytokine storm
Imbalanced coagulation system and cardiac complications
Several studies have reported thrombosis in SARS-CoV-2 patients and suggested that the induced infection might be associated with a coagulopathy and enhanced risk of thrombosis [63]. A recent retrospective analysis of 21 COVID-19-related mortality indicated that 71.8% of these cases had disseminated intravascular coagulation (DIC), highlighting the importance of studies on coagulopathy and thrombotic events [23]. Coagulation abnormalities and thromboembolic complications were reported in SARS-CoV-2 patients, including increased D-dimer levels and DIC [64], deep venous thrombosis (DVT), pulmonary embolism (PE) [65], and thrombocytopenia [66]. Prothrombin time (PT), international normalized ratio (INR), thrombin time (TT), activated partial thromboplastin time (aPTT), fibrinogen (FIB), D-Dimer (DD) [67] and Von Willebrand factor (VWF) are critical tests in monitoring the coagulation system in COVID-19 patients, especially in the severe stage and can help us in monitoring the coagulopathy and thrombosis condition [68, 69]. Various factors affect the risk of thrombosis in intravascular coagulation, the contact activation system and the kinin-kallikrein system, which are major systems in the regulation of thrombosis. Additionally, among the antigen presenting cells (APCs), neutrophils release not only inflammatory cytokines but also various bioactive molecules activating FXII of the intrinsic pathway and platelets (PLTs) and mediating coagulation [70, 71].
Tissue factor
TF activation mediates impaired fibrin removal, disseminated intravascular coagulation (DIC), fibrin consumption, and decreased platelet counts [72]. A cohort study indicated that 71% of patients who eventually died from COVID-19 experienced DIC and that thrombotic complication is an important event in SARS-CoV-2 pandemic [73]. Moreover, alternatively spliced TF promotes plaque angiogenesis via hypoxia-inducible factor-1α (HIF-1α) [74], and conversely, hypoxia might induce TF expression (75). HIF-1α increases NLRP3 inflammasome activation in lung injury, and early inhibition of NLRP3 activation might be an effective approach in ARDS treatment [76]. Recent studies indicate that HIF-1α expression might be correlated with thrombus formation [77], which can also induce TF expression and play an important role in coagulation among pulmonary diseases [78].
In Ebola infection, we face a similar condition of cytokine storm and coagulopathy due to plasma membrane surface [79]. Statin is a low cost CVD drug that can downregulate NLRP3 and downstream mediators such as IL1β in CVD and atherosclerosis patients [80]. Local physicians in Sierra Leone used statins and ARBs to maintain the endothelial barrier integrity and treated approximately 100 consecutive Ebola patients with atorvastatin and irbesartan [81, 82]. A cohort retrospective study on 13,981 COVID-19 patients indicated that statin decreases the risk of mortality due to its immunomodulatory effects [67]. See Figs. 1 and 2.
Complement system
The complement system is a mediator of innate immune response. This system is highly activated in the lungs of COVID-19 patients. N protein activates mannose-binding protein-associated serine protease 2 (MASP-2) and initiates the complement cascade via mannose binding lectin (MBL) pathway [83]. Complement overactivation leads to diffused thrombotic microangiopathy (TMA), organ dysfunction, and thrombocytopenia, with C5a playing a main role in cardiac dysfunction [84–87]. SARS-CoV-2 associated tissue injury is related to cytokine storm that affects lung parenchymal cells and decreases oxygen uptake. Thrombotic events, intravascular coagulation and the activation of the complement induced by the virus in lungs as well as other organs play an important role in thrombus formation, multiple organ failure and mortality [88]. Multi-organ damage seems to cause cardiac and kidney injury [89]. Besides, the complement interacts with TF activity in endothelium [90] and C5a induces TF activity on endothelial cells [91]. The crosstalk between the complement system and the coagulation system contributes to hemolytic and thrombotic disease, and thrombin associated with platelet membrane initiates C3 convertase formation, leading to complement sequence. Interestingly, the activated complement system on platelet surface increases aggregation and serotonin secretion, which works as a positive feedback enhancing complement system activation [92]. Membrane Attack Complex (MAC) activates platelets, enhances binding of coagulation factors Va and Xa, and augments the release of factor V from platelets and von Willebrand factor (VWF) from endothelial cells [93]. Noticeably, COVID-19 activates the complement via MBL and classic pathway [94], C5a induces TF activity on endothelial cells [91], and MAC induces the secretion of von Willebrand factor (VWF) from endothelial cells, which increases platelet adhesion and triggers the coagulation cascade [95]. In addition, MAC activates platelets and enhances coagulation activation. Finally, this sequence of events leads to extensive formation of thrombus and multi-organ dysfunction.
Studies on C5 complement inhibitor and anti-C5 monoclonal antibody eculizumab showed effective response in reversing both renal and cardiac dysfunction in COVID-19 patients [96]. Another study on complement C3 inhibitor AMY-101 reported that this intervention could control complement-mediated inflammatory damage among COVID-19 patients [97]. Avdoralimab (Innate Pharma, Marseille, France) is an anti-C5aR monoclonal antibody inhibiting C5a activity in clinical stage, preventing C5a-mediated myeloid cell recruitment and activation and controlling lung inflammation associated with ARDS in COVID-19 patients [98]. Recombinant human C1 esterase inhibitor (C1-INH) is a specific inhibitor of classical complement pathway and a candidate for clinical trial in COVID-19 patients [99]. Narsoplimab is a novel human monoclonal antibody with anticoagulant effect that targets MASP-2, inhibits MBL pathway of the complement and decreases endothelial damage, thrombotic events and ARD in COVID-19 patients [100]. The balance of complement as a therapeutic approach should be considered in COVID-19 treatment (Fig. 2).
Candidate CVD drugs against SARS-CoV-2
Combination of ARBs such as sartans (sacubitril/valsartan) and ACE inhibitor
ARBs such as sartans (sacubitril/valsartan) are potent drugs that can inhibit angiotensin-mediated AT1R activation, upregulate ACE2, and increase Ang 1–7 production [101]. Since Ang-II decreases NO and bradykinin levels, it enhances the formation of endothelin and is a potent vasoconstrictor such that Ang-II receptor blockers such as Valsartan, Olmesartan, Losartan, and Enalapril (which considered as ACE inhibitor) might be effective in controlling the infection and should not increase the risk of myocardial infraction [102–104]. Based on a study on ACE-knockout mice, Ang-II remained unchanged due to 14-fold increase in chymase activity [105]. Therefore, ARBs and Ang-II inhibitors seem to be better choices in combination or in comparison with ACE inhibitors in SARS-CoV-2 treatment [106]. By May 10, 2020, nine trials had been registered on clinicaltrials.gov to demonstrate the therapeutic benefits of ARBs for treating COVID-19 infections, two dealing with Ang 1–7 but none with Ang II [107].
In vitro studies on exogenous Ang II have revealed a novel vasopressor agent that can downregulate ACE2 via the AT1-ERK/p38 MAP kinase pathway [108]. Based on several studies, exogenous Ang II might be a good therapeutic approach in COVID-19 treatment via ACE2 downregulation. Several studies indicate that ACE2 downregulation is not favorable for COVID-19 patients and that it causes several organ dysfunctions; thus, ACE2 might have protective effects in organs and could be a major mechanism leading to cardiac and lung injury [109]. ACE2 agonists affect AT1R [108, 110]. Ang II binding to AT1R leads to aldosterone and vasopressin release from adrenal gland and hypothalamus to increase sodium and free water reabsorption in the kidney and finally increase mean arterial pressure (MAP) and It also increases vascular tone and vasodilatation via affecting bradykinin system, which can be an independent risk factor for CVD and heart disease [111, 112]. Additionally, inflammatory effects of AngII are mediated via activation of nuclear factor kappa-B (NF-κB) and its synergic effect on the production of several inflammatory cytokines such as IL1-β [113, 114]. Also, combination of a neprilysin inhibitor (NEPi) and an ARB (sacubitril/valsartan) might be effective in SARS-CoV-2 treatment [115]. Neprilysin inhibitor–angiotensin II receptor blocker combination (sacubitril/valsartan) seems to be a rational combination for adoption in SARS-CoV-2 patients. See Fig. 1.
Bradykinin receptor B1, B2 inhibitors and bradykinin antagonists
Losartan increases bradykinin levels via blocking AT1R [116]. ACE inhibitors rapidly activate mTORC1 via bradykinin [117]. Activation of Bradykinin Receptor B1 (BDKRB1) and B2R on endothelial cells in the lungs of SARS-CoV-2 patients makes the lung prone to angioedema, and inhibiting BDKB1R and B2R might be effective in attenuating acute respiratory distress syndrome (ARDS) as well as lung injury among COVID-19 patients [118]. Moreover, BDKRB1 is mostly expressed by cytokines and immunopathological conditions [119]. Recent studies on targeting BDKRB1 have indicated a potent pharmacological target for treatment of inflammatory lung disorders, pulmonary hypertension, and CVD [120–122]. Xiaowei Zhou et al. presented a novel bradykinin antagonist (RR-18) from the skin gland secretions of Hejiang frog as immune defense peptides that can be useful in the treatment of chronic inflammation [123] (Fig. 2).
Candidate anti-coagulation drugs against SARS-CoV-2
Based on a study conducted by Litao Zhang et al. D‐dimer levels higher than 2.0 µg/mL (fourfold increase) could effectively predict in‐hospital mortality of COVID-19 patients, which means D‐dimer level could be an early biomarker to improve the management of the disease [124]. Approximately 31% of COVID-19 patients in ICU face thrombotic complications, highlighting the need for pharmacological thrombosis prophylaxis in all COVID-19 patients admitted to ICU [2]. Several studies have confirmed that mortality might be a function of the thrombosis observed in segmental and subsegmental pulmonary arterial vessels. Thus, understanding and the management of thrombotic complications in COVID-19 patients can be a effective step in the management of the disease [125]. Low‐molecular weight heparin (LMWH) is a prophylactic anticoagulant for decreasing mortality in critically ill patients with sepsis‐induced hypercoagulation, and it can be useful in viral infections like COVID-19 [126]. Although high-dose heparin might be dangerous as a result of the hemorrhagic component of microangiopathy, only randomized clinical trials can answer whether high-dose heparin promotes the incidence of major bleeding (which occurred in some Italian COVID-19 patients). Marco Cattaneo et al. believe that 40 mg Lovenox (enoxaparin) is useful for decreasing PE, DVT and thromboprophylaxis of COVID-19 patients [127]. Another study on the incident of heparin induced thrombocytopenia (HIT), a life-threatening complication of heparin exposure, indicated that HIT increased among COVID-19 patients treated with heparin [128]. A recent study conducted by Chen Shi et al. reported heparin changes in the percentage of lymphocytes, levels of D-dimer and fibrinogen degradation products (FDP) and IL-6 levels. Thus, LMWH can improve coagulopathy and inflammation via decreasing IL-6 and increasing lymphocyte percentage [129]. Systemic treatment-dose anti-coagulant decreases mortality in COVID-19, but the risk of bleeding should be considered. According to one study, 29.8% of the patients who received treatment-dose anti-coagulant were more likely to need invasive mechanical ventilation compared to those who received prophylactic dose anti-coagulant or did not receive 8.1% and PT, aPTT, lactate dehydrogenase (LDH), ferritin, C reactive protein (CRP), and D-dimer values were higher among individuals who received anti-coagulant [130]. COVID-19–associated coagulopathy should be managed by thromboembolic prophylaxis in severe COVID-19, and if bleeding does occur, the management of DIC and bleeding should be considered according to the standard guidelines [63]. COVID‐19 patients with elevated D-dimer level should receive prophylactic anticoagulation therapy to decrease the risk of VET and PE. In a study on 199 COVID‐19 patients a D‐dimer value of 1 μg/ml was associated with an increased hazard ratio of 18·4 mortality and based on International Society on Thrombosis and Haemostasis (ISTH), elevated D‐dimers (arbitrarily defined as 3–fourfold increase) should be hospitalized even in the absence of other symptoms [131]. Bowles et al. reported that 91% of COVID-19 patients who were admitted to hospital with a prolonged aPTT were positive for lupus anticoagulant, which increases the risk of thrombosis via antiphospholipid syndrome. They also indicated that prolonged aPTT should not be a barrier to the use of anti-coagulant in the management of DVT and PE in COVID-19 patients [132]. Denote timing is very important in anti-coagulant therapy, so we should consider these points:
Considering the level of D-dimer (more than 1.0 μg/ml predicts the risk of VT) is a precious indicator for heparin administration [133].
Thromboprophylaxis should be administered from hospitalization until 7–14 days after discharge (specially for patients with risk factors such as, previous venous thromboembolism (VTE), active cancer, body mass index (BMI) > 30 and etc.) [134].
Intermediate-dose LMWH (i.e., enoxaparin 4000 IU subcutaneously every 12 h) can be considered on patients with multiple risk factors for VTE [134].
Drug-drug interactions between anticoagulants, antiplatelet agents, cardiac drugs, lupus anticoagulant inhibitors, and anti-complement should be considered.
Fibrinogen is an independent predictor of resistance to heparin [135], so the levels of fibrinogen should be considered to estimate the patient’s resistance to heparin before administration of heparin to COVID-19 patients.
COVID-19 patients with a history of a previous stroke or CVD need higher doses of coagulants, and the precise dose and the anti-coagulant should be clearly defined in COVID-19 protocols.
Higher levels of fibrinogen should be considered to increase the risk of thrombosis because it increases blood viscosity which, in turn, increases the risk of CVD and cardiac complications [136], so D-dimer plus fibrinogen should be considered for monitoring cardiac complications and CVD in COVID-19 patients.
Thrombolysis with Alteplase [Tissue plasminogen activator (tPA)] might be a good choice for heparin resistant patients [137], which should be considered in future studies of COVID-19.
Nafamostat mesylate (Futhan), is a synthetic serine protease inhibitor which has anticoagulation and antiviral effects, and it inhibits the proteolysis of fibrinogen into fibrin [138]. This should be considered in future studies of COVID-19 especially in heparin resistant individuals. During administration of Unfractionated heparin (UFH) and low-molecular-weight heparin (LMWH), we should consider UFH binding to endothelial cells, platelet factor 4, and platelets [139]. Therefore, it might cause pharmacokinetic and pharmacodynamics complications during administration with other medicines in COVID-19.
We need more trails on antiphospholipid antibodies in COVID-19, and antagonist of these antibodies might be a better choice in the management of thrombosis and coagulopathy in COVID-19 patients.
Conclusion and future prospective
Decreased levels of ACE2 during SARS-CoV-2 entry might be one of the main reasons of tissue damage because it impairs not only the imbalance angiotensin system but also Kallikrein–Kinin System, inflammatory system and coagulation. The crosstalk between these systems should be clarified in order to manage the disease. Cardiac complications and coagulopathies have been reported in COVID-19 patients, which implies the importance of the crosstalks between the mentioned systems. The important point is related to the secret of the initiation of coagulopathies in COVID-19 infection.
Since RAAS inhibitors upregulate ACE2 expression and ARBs inhibit Ang II-AT1R interaction, COVID-19 patients might benefit from the combination of RAAS inhibitors, ARBs, and statin. We believe that the blockage of bradykinin can be a good option in the management of COVID-19 and CVD patients, and supportive treatment of respiratory and cardiologic complications are needed in COVID-19 patients. Inhibiting BDKB1R and B2R might be effective in decreasing ARDS and lung injury in COVID-19 patients. It is worth restating that 91% of COVID-19 patients who were admitted to hospital with a prolonged aPTT were positive for lupus anticoagulant which increases the risk of thrombosis and prolonged aPTT. Heparin is a good choice for the management of the thrombosis in COVID-19 patients. In the meantime, denote timing is very important in anti-coagulant therapy, so we should consider the level of D-dimer, fibrinogen, Drug-drug interaction and risk factors such as previous venous thromboembolism (VTE), active cancer, body mass index (BMI) > 30, etc. during thromboprophylaxis administration. Fibrinogen is an independent predictor of resistance to heparin, so we should consider this factor before Thromboprophylaxis administration. Alteplase, Futhan might be a good choice in a heparin resistance condition. Finally, our therapeutic choice, dosing, and laboratory monitoring of anti-coagulant therapy in COVID-19 patients are critical decisions which can be life-saving or life-threatening.
Acknowledgements
We wish to thank our colleagues in Ahvaz Jundishapur University of Medical Sciences, Ahvaz, Iran and Dr Kreso Bendelja Institute of Immunology Location Cali, Colombia Department of Cellular Immunology for his kind comments on this manuscript.
Author contributions
H.H discussed the cardiac drugs in COVID-19 treatment, Z.D.Z managed the whole manuscript and presented the figures and the hypothesis, imbalance, N.S revised the manuscript, M.M revised cytokine storm, and designed the figures in Photoshop.
Funding
No fund was received for this study.
Declarations
Conflict of interest
This manuscript is a review article and does not involve a research protocol requiring approval by the relevant institutional review board or ethics committee. Authors declare no complicit of interest.
Ethical approval
This article does not contain any studies with human participants or animals performed by any of the authors.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Matsuyama S, Nao N, Shirato K, Kawase M, Saito S, Takayama I, et al. Enhanced isolation of SARS-CoV-2 by TMPRSS2-expressing cells. Proc Natl Acad Sci. 2020;117(13):7001–7003. doi: 10.1073/pnas.2002589117. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Klok F, Kruip M, Van der Meer N, Arbous M, Gommers D, Kant K, et al. Incidence of thrombotic complications in critically ill ICU patients with COVID-19. Thromb Res. 2020 doi: 10.1016/j.thromres.2020.04.041. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Radzikowska U, Ding M, Tan G, Zhakparov D, Peng Y, Wawrzyniak P, et al. Distribution of ACE2, CD147, cyclophilins, CD26 and other SARS-CoV-2 associated molecules in human tissues and immune cells in health and disease. bioRxiv. 2020;27:325. doi: 10.1111/all.14429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Segars J, Katler Q, McQueen DB, Kotlyar A, Glenn T, Knight Z, et al. Prior and novel coronaviruses, COVID-19, and human reproduction: what is known? Fertil Steril. 2020 doi: 10.1016/j.fertnstert.2020.04.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Cantuti-Castelvetri L, Ojha R, Pedro LD, Djannatian M, Franz J, Kuivanen S, et al. Neuropilin-1 facilitates SARS-CoV-2 cell entry and provides a possible pathway into the central nervous system. bioRxiv. 2020 doi: 10.1101/2020.06.07.137802. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Zamai L. Yin-Yang balance of ACE/ACE2 pathways: the rational for administration of ACE2 pathway inhibitors in patients infected by SARS-CoV-2. Preprints. 2020 doi: 10.20944/preprints202003.0338.v3. [DOI] [Google Scholar]
- 7.Wösten-van Asperen RM, Lutter R, Specht PA, Moll GN, van Woensel JB, van der Loos CM, et al. Acute respiratory distress syndrome leads to reduced ratio of ACE/ACE2 activities and is prevented by angiotensin-(1–7) or an angiotensin II receptor antagonist. J Pathol. 2011;225(4):618–627. doi: 10.1002/path.2987. [DOI] [PubMed] [Google Scholar]
- 8.Zhuang MW, Cheng Y, Zhang J, Jiang XM, Wang L, Deng J, et al. increasing host cellular receptor—angiotensin-converting enzyme 2 (ACE2) expression by coronavirus may facilitate 2019-nCoV (or SARS-CoV-2) infection. J Med Virol. 2020;92:2693–2701. doi: 10.1002/jmv.26139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Zheng Y-Y, Ma Y-T, Zhang J-Y, Xie X. Reply to:‘interaction between RAAS inhibitors and ACE2 in the context of COVID-19’. Nat Rev Cardiol. 2020;17(5):313–314. doi: 10.1038/s41569-020-0369-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Thachil J. All those D-dimers in COVID-19. J Thromb Haemost. 2020 doi: 10.1111/jth.14939. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Mehra MR, Desai SS, Kuy S, Henry TD, Patel AN. Cardiovascular disease, drug therapy, and mortality in COVID-19. N Engl J Med. 2020 doi: 10.1056/NEJMoa2007621. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]
- 12.Zhou L, Niu Z, Jiang X, Zhang Z, Zheng Y, Wang Z, et al. Systemic analysis of tissue cells potentially vulnerable to SARS-CoV-2 infection by the protein-proofed single-cell RNA profiling of ACE2, TMPRSS2 and Furin proteases. SSRN. 2020 doi: 10.2139/ssrn.3589839. [DOI] [Google Scholar]
- 13.La Vignera S, Cannarella R, Condorelli RA, Torre F, Aversa A, Calogero AE. Sex-specific SARS-CoV-2 mortality: among hormone-modulated ACE2 expression, risk of venous thromboembolism and hypovitaminosis D. Int J Mol Sci. 2020;21(8):2948. doi: 10.3390/ijms21082948. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Zhang Y, Xiao M, Zhang S, Xia P, Cao W, Jiang W, et al. Coagulopathy and antiphospholipid antibodies in patients with Covid-19. N Engl J Med. 2020;382(17):e38. doi: 10.1056/NEJMc2007575. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Ribeiro-Oliveira A, Jr, Nogueira AI, Pereira RM, Boas WWV, dos Santos RAS, e Silva ACS. The renin–angiotensin system and diabetes: an update. Vasc Health Risk Manage. 2008;4(4):787. [PMC free article] [PubMed] [Google Scholar]
- 16.Nehme A, Zouein FA, Deris Zayeri Z, Zibara K. An update on the tissue renin angiotensin system and its role in physiology and pathology. J Cardiovasc Dev Dis. 2019;6(2):14. doi: 10.3390/jcdd6020014. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Imai Y, Kuba K, Rao S, Huan Y, Guo F, Guan B, et al. Angiotensin-converting enzyme 2 protects from severe acute lung failure. Nature. 2005;436(7047):112–116. doi: 10.1038/nature03712. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Pedersen HD, Koch J, Poulsen K, Jensen AL, Flagstad A. Activation of the renin-angiotensin system in dogs with asymptomatic and mildly symptomatic mitral valvular insufficiency. J Vet Intern Med. 1995;9(5):328–331. doi: 10.1111/j.1939-1676.1995.tb01092.x. [DOI] [PubMed] [Google Scholar]
- 19.Perrotta F, Matera MG, Cazzola M, Bianco A. Severe respiratory SARS-CoV2 infection: does ACE2 receptor matter? Respir Med. 2020;168:105996. doi: 10.1016/j.rmed.2020.105996. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Liu Y, Huang F, Xu J, Yang P, Qin Y, Cao M, et al. Anti-hypertensive Angiotensin II receptor blockers associated to mitigation of disease severity in elderly COVID-19 patients. medRxiv. 2020;12:e0188975. [Google Scholar]
- 21.Das U. Angiotensin-II behaves as an endogenous pro-inflammatory molecule. JAPI. 2005;53:472–474. [PubMed] [Google Scholar]
- 22.Khajah MA, Fateel MM, Ananthalakshmi KV, Luqmani YA. Anti-inflammatory action of angiotensin 1–7 in experimental colitis may be mediated through modulation of serum cytokines/chemokines and immune cell functions. Dev Comp Immunol. 2017;74:200–208. doi: 10.1016/j.dci.2017.05.005. [DOI] [PubMed] [Google Scholar]
- 23.Zou Y, Guo H, Zhang Y, Zhang Z, Liu Y, Wang J, et al. Analysis of coagulation parameters in patients with COVID-19 in Shanghai, China. Biosci Trends. 2020 doi: 10.5582/bst.2020.03086. [DOI] [PubMed] [Google Scholar]
- 24.Wehbe Z, Hammoud S, Soudani N, Zaraket H, El-Yazbi A, Eid AH. Molecular insights into SARS COV-2 interaction with cardiovascular disease: role of RAAS and MAPK signaling. Front Pharmacol. 2020;11:836. doi: 10.3389/fphar.2020.00836. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Conversano A, Melillo F, Napolano A, Fominskiy E, Spessot M, Ciceri F, et al. RAAs inhibitors and outcome in patients with SARS-CoV-2 pneumonia. A case series study. Hypertension. 2020 doi: 10.1161/HYPERTENSIONAHA.120.15312. [DOI] [PubMed] [Google Scholar]
- 26.Monteil V, Kwon H, Prado P, Hagelkrüys A, Wimmer RA, Stahl M, et al. Inhibition of SARS-CoV-2 infections in engineered human tissues using clinical-grade soluble human ACE2. Cell. 2020 doi: 10.1016/j.cell.2020.04.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.van de Veerdonk F, Netea MG, van Deuren M, van der Meer JW, de Mast Q, Bruggemann RJ, et al. Kinins and cytokines in COVID-19: a comprehensive pathophysiological approach. Preprints. 2020 doi: 10.20944/preprints202004.0023.v1. [DOI] [Google Scholar]
- 28.Colarusso C, Terlizzi M, Pinto A, Sorrentino R. A lesson from a saboteur: high-MW kininogen impact in coronavirus-induced disease 2019. Br J Pharmacol. 2020 doi: 10.1111/bph.15154. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Joseph K, Kaplan AP. Formation of bradykinin: a major contributor to the innate inflammatory response. Adv Immunol. 2005;86:159–208. doi: 10.1016/S0065-2776(04)86005-X. [DOI] [PubMed] [Google Scholar]
- 30.Ferreira S, Lorenzetti B, Poole S. Bradykinin initiates cytokine-mediated inflammatory hyperalgesia. Br J Pharmacol. 1993;110(3):1227–1231. doi: 10.1111/j.1476-5381.1993.tb13946.x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Li P, Chappell MC, Ferrario CM, Brosnihan KB. Angiotensin-(1–7) augments bradykinin-induced vasodilation by competing with ACE and releasing nitric oxide. Hypertension. 1997;29(1):394–398. doi: 10.1161/01.hyp.29.1.394. [DOI] [PubMed] [Google Scholar]
- 32.Abbas A, Gorelik G, Carbini L, Scicli A. Angiotensin-(1–7) induces bradykinin-mediated hypotensive responses in anesthetized rats. Hypertension. 1997;30(2):217–221. doi: 10.1161/01.hyp.30.2.217. [DOI] [PubMed] [Google Scholar]
- 33.Flores-Muñoz M, Smith N, Haggerty C, Milligan G, Nicklin S. Angiotensin1-9 antagonises pro-hypertrophic signalling in cardiomyocytes via the angiotensin type 2 receptor. J Physiol. 2011;589(4):939–951. doi: 10.1113/jphysiol.2010.203075. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Zhang D-D, Gao Z-X, Vio CP, Xiao Y, Wu P, Zhang H, et al. Bradykinin stimulates renal Na+ and K+ excretion by inhibiting the K+ channel (Kir4. 1) in the distal convoluted tubule. Hypertension. 2018;72(2):361–369. doi: 10.1161/HYPERTENSIONAHA.118.11070. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Sattar Y, Ullah W, Rauf H. COVID-19 cardiovascular epidemiology, cellular pathogenesis, clinical manifestations and management. Int J Cardiol Heart Vasc. 2020;29:100589. doi: 10.1016/j.ijcha.2020.100589. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Hofman Z, de Maat S, Hack CE, Maas C. Bradykinin: inflammatory product of the coagulation system. Clin Rev Allergy Immunol. 2016;51(2):152–161. doi: 10.1007/s12016-016-8540-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Nicolau LA, Magalhães PJ, Vale ML. What would sérgio ferreira say to your physician in this war against COVID-19: how about kallikrein/kinin system? Med Hypotheses. 2020;143:109886. doi: 10.1016/j.mehy.2020.109886. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Fang C, Schmaier AH. Novel anti-thrombotic mechanisms mediated by mas receptor as result of balanced activities between the Kallikrein/Kinin and the renin-angiotensin systems. Pharmacol Res. 2020;160:105096. doi: 10.1016/j.phrs.2020.105096. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Berrettini M, Lammle B, White T, Heeb MJ, Schwarz H, Zuraw B, et al. Detection of in vitro and in vivo cleavage of high molecular weight kininogen in human plasma by immunoblotting with monoclonal antibodies. Blood. 1986 doi: 10.1182/blood.V68.2.455.bloodjournal682455. [DOI] [PubMed] [Google Scholar]
- 40.Wuepper KD, Cochrane CG. Effect of plasma kallikrein on coagulation in vitro. Proc Soc Exp Biol Med. 1972;141(1):271–276. doi: 10.3181/00379727-141-36757. [DOI] [PubMed] [Google Scholar]
- 41.Irmscher S, Döring N, Halder LD, Jo EA, Kopka I, Dunker C, et al. Kallikrein cleaves C3 and activates complement. J Innate Immun. 2018;10(2):94–105. doi: 10.1159/000484257. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Govers-Riemslag J, Smid M, Cooper J, Bauer K, Rosenberg R, Hack C, et al. The plasma kallikrein–kinin system and risk of cardiovascular disease in men. J Thromb Haemost. 2007;5(9):1896–1903. doi: 10.1111/j.1538-7836.2007.02687.x. [DOI] [PubMed] [Google Scholar]
- 43.Kolte D, Shariat-Madar Z. Plasma kallikrein inhibitors in cardiovascular disease. Cardiol Rev. 2016;24(3):99–109. doi: 10.1097/CRD.0000000000000069. [DOI] [PubMed] [Google Scholar]
- 44.Banerji A, Riedl MA, Bernstein JA, Cicardi M, Longhurst HJ, Zuraw BL, et al. Effect of lanadelumab compared with placebo on prevention of hereditary angioedema attacks: a randomized clinical trial. JAMA. 2018;320(20):2108–2121. doi: 10.1001/jama.2018.16773. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Banerji A, Busse P, Shennak M, Lumry W, Davis-Lorton M, Wedner HJ, et al. Inhibiting plasma kallikrein for hereditary angioedema prophylaxis. N Engl J Med. 2017;376(8):717–728. doi: 10.1056/NEJMoa1605767. [DOI] [PubMed] [Google Scholar]
- 46.Challener CA (2019) FDA marks record year for new drug approvals. Pharm Technol 43(1):30–33
- 47.Yang J, Zheng Y, Gou X, Pu K, Chen Z, Guo Q, et al. Prevalence of comorbidities and its effects in patients infected with SARS-CoV-2: a systematic review and meta-analysis. Int J Infect Dis. 2020;94:91–95. doi: 10.1016/j.ijid.2020.03.017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Driggin E, Madhavan MV, Bikdeli B, Chuich T, Laracy J, Biondi-Zoccai G, et al. Cardiovascular considerations for patients, health care workers, and health systems during the COVID-19 pandemic. J Am Coll Cardiol. 2020;75(18):2352–2371. doi: 10.1016/j.jacc.2020.03.031. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Kochi AN, Tagliari AP, Forleo GB, Fassini GM, Tondo C. Cardiac and arrhythmic complications in patients with COVID-19. J Cardiovasc Electrophysiol. 2020;31(5):1003–1008. doi: 10.1111/jce.14479. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Bhatla A, Mayer MM, Adusumalli S, Hyman MC, Oh E, Tierney A, et al. COVID-19 and cardiac arrhythmias. Heart Rhythm. 2020;17:1439–1444. doi: 10.1016/j.hrthm.2020.06.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Sun X, Wang T, Cai D, Hu Z, Liao H, Zhi L, et al. Cytokine storm intervention in the early stages of COVID-19 pneumonia. Cytokine Growth Factor Rev. 2020 doi: 10.1016/j.cytogfr.2020.04.002. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Lippi G, Lavie CJ, Sanchis-Gomar F. Cardiac troponin I in patients with coronavirus disease 2019 (COVID-19): evidence from a meta-analysis. Prog Cardiovasc Dis. 2020 doi: 10.1016/j.pcad.2020.03.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Fathi N, Rezaei N. Lymphopenia in COVID-19: therapeutic opportunities. Cell Biol Int. 2020 doi: 10.1002/cbin.11403. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Pedersen SF, Ho Y-C. SARS-CoV-2: a storm is raging. J Clin Investig. 2020 doi: 10.1172/JCI137647. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Coperchini F, Chiovato L, Croce L, Magri F, Rotondi M. The cytokine storm in COVID-19: an overview of the involvement of the chemokine/chemokine-receptor system. Cytokine Growth Factor Rev. 2020 doi: 10.1016/j.cytogfr.2020.05.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Cao X. COVID-19: immunopathology and its implications for therapy. Nat Rev Immunol. 2020;20(5):269–270. doi: 10.1038/s41577-020-0308-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Fu Y, Cheng Y, Wu Y. Understanding SARS-CoV-2-mediated inflammatory responses: from mechanisms to potential therapeutic tools. Virol Sin. 2020 doi: 10.1007/s12250-020-00207-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Gaborit BJ, Bergmann J-F, Mussini C, Arribas JR, Behrens G, Walmsley S, et al. Plea for multitargeted interventions for severe COVID-19. Lancet Infect Dis. 2020 doi: 10.1016/S1473-3099(20)30312-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Zhang C, Wu Z, Li J-W, Zhao H, Wang G-Q. The cytokine release syndrome (CRS) of severe COVID-19 and Interleukin-6 receptor (IL-6R) antagonist Tocilizumab may be the key to reduce the mortality. Int J Antimicrob Agents. 2020;55:105954. doi: 10.1016/j.ijantimicag.2020.105954. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Roshanravan N, Seif F, Ostadrahimi A, Pouraghaei M, Ghaffari S. Targeting cytokine storm to manage patients with COVID-19: a mini-review. Arch Med Res. 2020 doi: 10.1016/j.arcmed.2020.06.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Huang Q, Wu X, Zheng X, Luo S, Xu S, Weng J. Targeting inflammation and cytokine storm in COVID-19. Pharmacol Res. 2020 doi: 10.1016/j.phrs.2020.105051. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Shah A. Novel coronavirus-induced NLRP3 inflammasome activation: a potential drug target in the treatment of COVID-19. Front Immunol. 2020 doi: 10.3389/fimmu.2020.01021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Connors JM, Levy JH. COVID-19 and its implications for thrombosis and anticoagulation. Blood. 2020;135(23):2033–2040. doi: 10.1182/blood.2020006000. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Levi M, Thachil J, Iba T, Levy JH. Coagulation abnormalities and thrombosis in patients with COVID-19. Lancet Haematol. 2020;7(6):e438. doi: 10.1016/S2352-3026(20)30145-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Al-Ani F, Chehade S, Lazo-Langner A. Thrombosis risk associated with COVID-19 infection. A scoping review. Thromb Res. 2020 doi: 10.1016/j.thromres.2020.05.039. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Lippi G, Plebani M, Henry BM. Thrombocytopenia is associated with severe coronavirus disease 2019 (COVID-19) infections: a meta-analysis. Clin Chim Acta. 2020 doi: 10.1016/j.cca.2020.03.022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Zhang X-J, Qin J-J, Cheng X, Shen L, Zhao Y-C, Yuan Y, et al. In-hospital use of statins is associated with a reduced risk of mortality among individuals with COVID-19. Cell Metab. 2020 doi: 10.1016/j.cmet.2020.06.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Goshua G, Pine AB, Meizlish ML, Chang C-H, Zhang H, Bahel P, et al. Endotheliopathy in COVID-19-associated coagulopathy: evidence from a single-centre, cross-sectional study. Lancet Haematol. 2020 doi: 10.1016/S2352-3026(20)30216-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Jin X, Duan Y, Bao T, Gu J, Chen Y, Li Y, et al. The values of coagulation function in COVID-19 patients. medRxiv. 2020;3:265. doi: 10.1371/journal.pone.0241329. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Heestermans M, Salloum-Asfar S, Salvatori D, Laghmani EH, Luken BM, Zeerleder SS, et al. Role of platelets, neutrophils, and factor XII in spontaneous venous thrombosis in mice. Blood. 2016;127(21):2630–2637. doi: 10.1182/blood-2015-10-672766. [DOI] [PMC free article] [PubMed] [Google Scholar] [Retracted]
- 71.Wu Y. Contact pathway of coagulation and inflammation. Thromb J. 2015;13(1):17. doi: 10.1186/s12959-015-0048-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Asakura H, Suga Y, Yoshida T, Ontachi Y, Mizutani T, Kato M, et al. Pathophysiology of disseminated intravascular coagulation (DIC) progresses at a different rate in tissue factor-induced and lipopolysaccharide-induced DIC models in rats. Blood Coagul Fibrinol. 2003;14(3):221–228. doi: 10.1097/01.mbc.0000061290.28953.57. [DOI] [PubMed] [Google Scholar]
- 73.Beun R, Kusadasi N, Sikma M, Westerink J, Huisman A. Thromboembolic events and apparent heparin resistance in patients infected with SARS-CoV-2. Int J Lab Hematol. 2020 doi: 10.1111/ijlh.13230. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Giannarelli C, Alique M, Rodriguez DT, Yang DK, Jeong D, Calcagno C, et al. Alternatively spliced tissue factor promotes plaque angiogenesis through the activation of hypoxia-inducible factor-1α and vascular endothelial growth factor signaling. Circulation. 2014;130(15):1274–1286. doi: 10.1161/CIRCULATIONAHA.114.006614. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Monteiro RQ, Lima LG, Gonçalves NP, De Souza MRA, Leal AC, Demasi MAA, et al. Hypoxia regulates the expression of tissue factor pathway signaling elements in a rat glioma model. Oncol Lett. 2016;12(1):315–322. doi: 10.3892/ol.2016.4593. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Sherman MA, Suresh MV, Dolgachev VA, McCandless LK, Xue X, Ziru L, et al. Molecular characterization of hypoxic alveolar epithelial cells after lung contusion indicates an important role for HIF-1α. Ann Surg. 2018;267(2):382. doi: 10.1097/SLA.0000000000002070. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Kim S, Jun JH, Kim J, Kim DW, Jang YH, Lee WJ, et al. HIF-1α and VEGF expression correlates with thrombus remodeling in cases of intravascular papillary endothelial hyperplasia. Int J Clin Exp Pathol. 2013;6(12):2912. [PMC free article] [PubMed] [Google Scholar]
- 78.Semenza GL. Oxygen-regulated transcription factors and their role in pulmonary disease. Respir Res. 2000;1(3):7. doi: 10.1186/rr27. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Kennedy JR. Phosphatidylserine’s role in Ebola’s inflammatory cytokine storm and hemorrhagic consumptive coagulopathy and the therapeutic potential of annexin V. Med Hypotheses. 2020;135:109462. doi: 10.1016/j.mehy.2019.109462. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Koushki K, Shahbaz SK, Mashayekhi K, Sadeghi M, Zayeri ZD, Taba MY, et al. Anti-inflammatory action of statins in cardiovascular disease: the role of inflammasome and toll-like receptor pathways. Clin Rev Allergy Immunol. 2020 doi: 10.1007/s12016-020-08791-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Fedson DS, Jacobson JR, Rordam OM, Opal SM. Treating the host response to Ebola virus disease with generic statins and angiotensin receptor blockers. MBio. 2015 doi: 10.1128/mBio.00716-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Fedson DS, Rordam OM. Treating Ebola patients: a ‘bottom up’approach using generic statins and angiotensin receptor blockers. Int J Infect Dis. 2015;36:80–84. doi: 10.1016/j.ijid.2015.04.019. [DOI] [PubMed] [Google Scholar]
- 83.Gao T, Hu M, Zhang X, Li H, Zhu L, Liu H, et al. Highly pathogenic coronavirus N protein aggravates lung injury by MASP-2-mediated complement over-activation. medRxiv. 2020;25:777. [Google Scholar]
- 84.Jacobs E, Ortiz C, Licht C. the role of complement in the pathogenesis of HUS and the TMA spectrum disorders. Curr Pediatr Rep. 2019;7(1):1–11. [Google Scholar]
- 85.De Voeght A, Calmes D, Beck F, Sylvestre J-B, Delvenne P, Peters P, et al. Thrombotic microvascular injury is not mediated by thrombotic microangiopathy despite systemic complement activation in Covid-19 patients. medRxiv. 2020;9:e01753. [Google Scholar]
- 86.Niederbichler AD, Hoesel LM, Westfall MV, Gao H, Ipaktchi KR, Sun L, et al. An essential role for complement C5a in the pathogenesis of septic cardiac dysfunction. J Exp Med. 2006;203(1):53–61. doi: 10.1084/jem.20051207. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.Gavriilaki E, Sakellari I, Gavriilaki M, Anagnostopoulos A. Thrombocytopenia in COVID-19: pathophysiology matters. Ann Hematol. 2020 doi: 10.1007/s00277-020-04183-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Noris M, Benigni A, Remuzzi G. The case of complement activation in COVID-19 multiorgan impact. Kidney Int. 2020 doi: 10.1016/j.kint.2020.05.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Guan W-j, Ni Z-Y, Hu Y, Liang W-h, Ou C-q, He J-X, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. 2020;382(18):1708–1720. doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Saadi S, Holzknecht RA, Patte CP, Stern DM, Platt JL. Complement-mediated regulation of tissue factor activity in endothelium. J Exp Med. 1995;182(6):1807–1814. doi: 10.1084/jem.182.6.1807. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 91.Ikeda K, Nagasawa K, Horiuchi T, Tsuru T, Nishizaka H, Niho Y. C5a induces tissue factor activity on endothelial cells. Thromb Haemost. 1997;77(02):394–398. [PubMed] [Google Scholar]
- 92.Luo S, Hu D, Wang M, Zipfel PF, Hu Y. Complement in hemolysis-and thrombosis-related diseases. Front Immunol. 2020 doi: 10.3389/fimmu.2020.01212. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 93.Fletcher-Sandersjöö A, Bellander B-M. Is COVID-19 associated thrombosis caused by overactivation of the complement cascade? A literature review. Thromb Res. 2020 doi: 10.1016/j.thromres.2020.06.027. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Polycarpou A, Howard M, Farrar CA, Greenlaw R, Fanelli G, Wallis R, et al. Rationale for targeting complement in COVID-19. EMBO Mol Med. 2020 doi: 10.15252/emmm.202012642. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 95.Albrecht EA, Chinnaiyan AM, Varambally S, Kumar-Sinha C, Barrette TR, Sarma JV, et al. C5a-induced gene expression in human umbilical vein endothelial cells. Am J Pathol. 2004;164(3):849–859. doi: 10.1016/S0002-9440(10)63173-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Valga F, Vega-Díaz N, Macia M, Monzón T, Rodriguez-Perez JC. Targeting complement in severe coronavirus disease 2019 to address microthrombosis. Clin Kidney J. 2020 doi: 10.15252/emmm.202012642. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Mastaglio S, Ruggeri A, Risitano AM, Angelillo P, Yancopoulou D, Mastellos DC, et al. The first case of COVID-19 treated with the complement C3 inhibitor AMY-101. Clin Immunol. 2020;215:108450. doi: 10.1016/j.clim.2020.108450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 98.Carvelli J, Demaria O, Vély F, Batista L, Benmansour NC, Fares J, Carpentier S, Thibult ML, Morel A, André P, Represa A. Identification of immune checkpoints in COVID-19
- 99.Jodele S, Köhl J. Tackling COVID-19 infection through complement-targeted immunotherapy. Br J Pharmacol. 2020 doi: 10.1111/bph.15187. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Rambaldi A, Gritti G, Micò MC, Frigeni M, Borleri G, Salvi A, et al. Endothelial injury and thrombotic microangiopathy in COVID-19: treatment with the lectin-pathway inhibitor narsoplimab. Immunobiology. 2020;225:152001. doi: 10.1016/j.imbio.2020.152001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Acanfora D, Ciccone MM, Scicchitano P, Acanfora C, Casucci G. Neprilysin inhibitor–angiotensin II receptor blocker combination (sacubitril/valsartan): rationale for adoption in SARS-CoV-2 patients. Eur Heart J—Cardiovasc Pharmacother. 2020 doi: 10.1093/ehjcvp/pvaa028. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Speth RC. Response to recent commentaries regarding the involvement of angiotensin-converting enzyme 2 (ACE2) and renin-angiotensin system blockers in SARS-CoV-2 infections. Drug Dev Res. 2020 doi: 10.1002/ddr.21672. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Furuhashi M, Moniwa N, Takizawa H, Ura N, Shimamoto K. Potential differential effects of renin-angiotensin system inhibitors on SARS-CoV-2 infection and lung injury in COVID-19. Hypertens Res. 2020 doi: 10.1038/s41440-020-0478-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.McDonald MA, Simpson SH, Ezekowitz JA, Gyenes G, Tsuyuki RT. Angiotensin receptor blockers and risk of myocardial infarction: systematic review. BMJ. 2005;331(7521):873. doi: 10.1136/bmj.38595.518542.3A. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Singh R, Leehey DJ. Effect of ACE inhibitors on angiotensin II in rat mesangial cells cultured in high glucose. Biochem Biophys Res Commun. 2007;357(4):1040–1045. doi: 10.1016/j.bbrc.2007.04.038. [DOI] [PubMed] [Google Scholar]
- 106.Laurentius A, Mendel B, Prakoso R. Clinical outcome of renin-angiotensin-aldosterone system blockers in treatment of hypertensive patients with COVID-19: a systematic review and meta-analysis. Egypt Heart J. 2021;73(1):1–12. doi: 10.1186/s43044-021-00135-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Speth RC. Angiotensin II administration to COVID-19 patients is not advisable. Crit Care. 2020;24(1):296. doi: 10.1186/s13054-020-03032-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Koka V, Huang XR, Chung AC, Wang W, Truong LD, Lan HY. Angiotensin II up-regulates angiotensin I-converting enzyme (ACE), but down-regulates ACE2 via the AT1-ERK/p38 MAP kinase pathway. Am J Pathol. 2008;172(5):1174–1183. doi: 10.2353/ajpath.2008.070762. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Tomasoni D, Italia L, Adamo M, Inciardi RM, Lombardi CM, Solomon SD, et al. COVID 19 and heart failure: from infection to inflammation and angiotensin II stimulation. Searching for evidence from a new disease. Eur J Heart Fail. 2020 doi: 10.1002/ejhf.1871. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Busse LW, Chow JH, McCurdy MT, Khanna AK. COVID-19 and the RAAS—a potential role for angiotensin II? Crit Care. 2020 doi: 10.1186/s13054-020-02862-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Maimaiti N, Wen L, Li X, Wang L, Abulimiti A, Tao W, et al. Secondary hypertension. Singapore: Springer; 2010. Renal parenchymal hypertension; pp. 125–185. [Google Scholar]
- 112.DeMers D, Wachs D. Physiology, mean arterial pressure. Treasure Island: StatPearls Publishing; 2020. [PubMed] [Google Scholar]
- 113.Pueyo ME, Gonzalez W, Nicoletti A, Savoie F, Arnal J-F, Michel J-B. Angiotensin II stimulates endothelial vascular cell adhesion molecule-1 via nuclear factor-κB activation induced by intracellular oxidative stress. Arterioscler Thromb Vasc Biol. 2000;20(3):645–651. doi: 10.1161/01.atv.20.3.645. [DOI] [PubMed] [Google Scholar]
- 114.Alique M, Sánchez-López E, Rayego-Mateos S, Egido J, Ortiz A, Ruiz-Ortega M. Angiotensin II, via angiotensin receptor type 1/nuclear factor-κB activation, causes a synergistic effect on interleukin-1-β-induced inflammatory responses in cultured mesangial cells. J Renin-Angiotensin-Aldosterone Syst. 2015;16(1):23–32. doi: 10.1177/1470320314551564. [DOI] [PubMed] [Google Scholar]
- 115.Ruilope LM, Tamargo J, Ruiz-Hurtado G. Renin–angiotensin system inhibitors in the COVID-19 pandemic: consequences of antihypertensive drugs. Eur Heart J. 2020;41(22):2067–2069. doi: 10.1093/eurheartj/ehaa487. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Campbell DJ, Krum H, Esler MD. Losartan increases bradykinin levels in hypertensive humans. Circulation. 2005;111(3):315–320. doi: 10.1161/01.CIR.0000153269.07762.3B. [DOI] [PubMed] [Google Scholar]
- 117.Luo H, Wu P-F, Cao Y, Jin M, Shen T-T, Wang J, et al. Angiotensin-converting enzyme inhibitor rapidly ameliorates depressive-type behaviors via bradykinin-dependent activation of mTORC1. Biol Psychiatry. 2020 doi: 10.1016/j.biopsych.2020.02.005. [DOI] [PubMed] [Google Scholar]
- 118.van de Veerdonk FL, Netea MG, van Deuren M, van der Meer JW, de Mast Q, Brüggemann RJ, et al. Kallikrein-kinin blockade in patients with COVID-19 to prevent acute respiratory distress syndrome. Elife. 2020;9:e57555. doi: 10.7554/eLife.57555. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 119.Marceau F, Bachelard H, Bouthillier J, Fortin J-P, Morissette G, Bawolak M-T, et al. Bradykinin receptors: agonists, antagonists, expression, signaling, and adaptation to sustained stimulation. Int Immunopharmacol. 2020;82:106305. doi: 10.1016/j.intimp.2020.106305. [DOI] [PubMed] [Google Scholar]
- 120.Murugesan P, Hildebrandt T, Bernlöhr C, Lee D, Khang G, Doods H, et al. Inhibition of kinin B1 receptors attenuates pulmonary hypertension and vascular remodeling. Hypertension. 2015;66(4):906–912. doi: 10.1161/HYPERTENSIONAHA.115.05338. [DOI] [PubMed] [Google Scholar]
- 121.Vasquez-Pinto LM, Nantel F, Sirois P, Jancar S. Bradykinin B1 receptor antagonist R954 inhibits eosinophil activation/proliferation/migration and increases TGF-β and VEGF in a murine model of asthma. Neuropeptides. 2010;44(2):107–113. doi: 10.1016/j.npep.2009.11.001. [DOI] [PubMed] [Google Scholar]
- 122.Heitsch H. The therapeutic potential of bradykinin B2 receptor agonists in the treatment of cardiovascular disease. Expert Opin Investig Drugs. 2003;12(5):759–770. doi: 10.1517/13543784.12.5.759. [DOI] [PubMed] [Google Scholar]
- 123.Xie Z, Li Z, Shao Y, Liao C. Discovery and development of plasma kallikrein inhibitors for multiple diseases. Eur J Med Chem. 2020;190:112137. doi: 10.1016/j.ejmech.2020.112137. [DOI] [PubMed] [Google Scholar]
- 124.Zhang L, Yan X, Fan Q, Liu H, Liu X, Liu Z, et al. D-dimer levels on admission to predict in-hospital mortality in patients with Covid-19. J Thromb Haemost. 2020;18(6):1324–1329. doi: 10.1111/jth.14859. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 125.Lax SF, Skok K, Zechner P, Kessler HH, Kaufmann N, Koelblinger C, et al. Pulmonary arterial thrombosis in COVID-19 with fatal outcome: results from a prospective, single-center, clinicopathologic case series. SSRN Electron J. 2020 doi: 10.2139/ssrn.3586685. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 126.Lindahl U, Li JP. Heparin–an old drug with multiple potential targets in Covid-19 therapy. J Thromb Haemost. 2020 doi: 10.1111/jth.14898. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 127.Cattaneo M, Bertinato EM, Birocchi S, Brizio C, Malavolta D, Manzoni M, et al. Pulmonary embolism or pulmonary thrombosis in COVID-19? Is the recommendation to use high-dose heparin for thromboprophylaxis justified? Thromb Haemost. 2020 doi: 10.1055/s-0040-1712097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 128.Patell R, Khan A, Bogue T, Merrill M, Koshy A, Bindal P, et al. Heparin induced thrombocytopenia antibodies in COVID-19. Am J Hematol. 2020 doi: 10.1002/ajh.25935. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 129.Shi C, Wang C, Wang H, Yang C, Cai F, Zeng F, et al. The potential of low molecular weight heparin to mitigate cytokine storm in severe COVID-19 patients: a retrospective clinical study. medrxiv. 2020 doi: 10.1101/2020.03.28.20046144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Paranjpe I, Fuster V, Lala A, Russak AJ, Glicksberg BS, Levin MA, et al. Association of treatment dose anticoagulation with in-hospital survival among hospitalized patients with COVID-19. J Am Coll Cardiol. 2020;76(1):122. doi: 10.1016/j.jacc.2020.05.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 131.Kollias A, Kyriakoulis KG, Dimakakos E, Poulakou G, Stergiou GS, Syrigos K. Thromboembolic risk and anticoagulant therapy in COVID-19 patients: emerging evidence and call for action. Br J Haematol. 2020;189(5):846–847. doi: 10.1111/bjh.16727. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 132.Bowles L, Platton S, Yartey N, Dave M, Lee K, Hart DP, et al. Lupus anticoagulant and abnormal coagulation tests in patients with Covid-19. N Engl J Med. 2020 doi: 10.1056/NEJMc2013656. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 133.Artifoni M, Danic G, Gautier G, Gicquel P, Boutoille D, Raffi F, et al. Systematic assessment of venous thromboembolism in COVID-19 patients receiving thromboprophylaxis: incidence and role of D-dimer as predictive factors. J Thromb Thrombolysis. 2020 doi: 10.1007/s11239-020-02146-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 134.Marietta M, Ageno W, Artoni A, De Candia E, Gresele P, Marchetti M, et al. COVID-19 and haemostasis: a position paper from Italian Society on Thrombosis and Haemostasis (SISET) Blood Transfus. 2020;18(3):167. doi: 10.2450/2020.0083-20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 135.Kawatsu S, Sasaki K, Sakatsume K, Takahara S, Hosoyama K, Masaki N, et al. Predictors of heparin resistance before cardiovascular operations in adults. Ann Thorac Surg. 2018;105(5):1316–1321. doi: 10.1016/j.athoracsur.2018.01.068. [DOI] [PubMed] [Google Scholar]
- 136.Mora S, Rifai N, Buring JE, Ridker PM. Additive value of immunoassay-measured fibrinogen and high-sensitivity C-reactive protein levels for predicting incident cardiovascular events. Circulation. 2006;114(5):381–387. doi: 10.1161/CIRCULATIONAHA.106.634089. [DOI] [PubMed] [Google Scholar]
- 137.Absar S, Choi S, Yang VC, Kwon YM. Heparin-triggered release of camouflaged tissue plasminogen activator for targeted thrombolysis. J Control Release. 2012;157(1):46–54. doi: 10.1016/j.jconrel.2011.09.060. [DOI] [PubMed] [Google Scholar]
- 138.Chen X, Xu Z, Zeng S, Wang X, Liu W, Qian L, et al. The molecular aspect of antitumor effects of protease inhibitor nafamostat mesylate and its role in potential clinical applications. Front Oncol. 2019;9:852. doi: 10.3389/fonc.2019.00852. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 139.Hirsh J, Raschke R. Heparin and low-molecular-weight heparin: the seventh ACCP conference on antithrombotic and thrombolytic therapy. Chest. 2004;126(3):188S–203S. doi: 10.1378/chest.126.3_suppl.188S. [DOI] [PubMed] [Google Scholar]