Abstract
A healthy 32-year-old G3P3 woman with an unknown last menstrual period presented to the emergency department with intense abdominal pain and pain in the right chest that radiated down the right arm. Further workup showed that she had a ruptured ectopic pregnancy with significant haemoperitoneum. After successful laparoscopic evacuation of the ectopic pregnancy and haemoperitoneum, the patient subsequently developed a right ovarian vein thrombosis 4 weeks after the procedure. She was treated with anticoagulation, and further haematological studies did not show any significant findings. Postpartum ovarian vein thrombosis is extremely rare and can be life- threatening if not accurately diagnosed and treated with anticoagulation or surgical management in a timely manner.
Keywords: obstetrics and gynaecology, venous thromboembolism, pregnancy
Background
Ectopic pregnancy is a fairly common condition occurring in approximately 1 out of every 50 births according to the American Academy of Family Physicians. It is also the most common cause of life-threatening pathologies in the first trimester of pregnancy.1 Recent data have shown that since the implementation of the transvaginal ultrasound and screening using the beta subunit of human chorionic gonadotropin (HCG), fatality rates from ruptured ectopic pregnancies have decreased from 35.5 deaths per 10 000 in 1970 to 3.8 per 10 000.2 Ectopic implantation of the conceptus is most commonly found in the fallopian tube.3 The constellation of symptoms of tubal ectopic pregnancies could initially be difficult to detect due to many diseases presenting in a similar manner. The decision to work up an acute ectopic rupture is also challenging due to a variety of clinical presentations. However, initial workup in a woman with an unknown last menstrual period and signs of acute abdominal pain should warrant further investigation. One study showed that only 55% of ectopic pregnancies were discovered by the attending emergency department (ED) physician, and of those 55% discovered, 60% had already ruptured at the time of surgical intervention.4 In addition, one retrospective study showed that the risk of tubal rupture has been shown to be more common in women with no history of ectopic pregnancy.5
We present here a case report of a 32-year-old G3P3 otherwise healthy woman who presented to the ED with pleuritic chest pain and intense right upper and lower quadrant pain. She also reported a 2-week history of vaginal bleeding, with an unknown date of last true menstrual period. She was diagnosed with an ectopic pregnancy in the right fallopian tube that had ruptured with resulting haemoperitoneum. Four weeks after successful laparoscopic removal of the ectopic pregnancy, the patient developed a right ovarian vein thrombosis (OVT) measuring 9 cm in diameter. CT scans have been shown to be effective in clinching the diagnosis. However, without an appropriate history to suggest the diagnosis or even suspect it, the diagnosis becomes much harder.
Case presentation
A 32-year-old G3P3 woman presented to the ED at 18:50 with intermittent right-sided, moderate, stabbing chest tightness that was positional in nature and worse when lying down or when breathing deeply. She also reported moderate periumbilical abdominal pain that started earlier that day and had been constant. She stated that she had experienced vaginal bleeding for the past 2 weeks but was unsure of the date of her last true menstrual period. She denied radiation of pain, nausea, vomiting, fever, chills, weakness or diaphoresis. Medical history included endometriosis and three vaginal deliveries. The patient reported using intrauterine device (IUD) for contraception.
On physical examination, the patient was ill-appearing and tachycardic (107 beats per minute), but otherwise vital signs were stable. Pelvic examination was deferred. Tenderness to palpation was appreciated at the right chest wall, right upper quadrant and periumbilical area. Re-evaluation at 24:00 revealed abdominal guarding. The patient had a total white cell count of 11.2×109 g/L and haemoglobin of 11.4×103 g/L.
Investigations
Due to the pleuritic nature of her symptoms, the ED physician undertook diagnostic workup for pulmonary embolism (PE) versus acute pathology of the abdomen. CT angiogram of the chest showed no evidence of acute PE, consolidation or pleural effusion. Coagulation studies including prothrombin time, international normalised ratio and partial thromboplastin time were all normal. Pregnancy test was positive with a quantitative beta-HCG of 929. The clinical picture of ruptured ectopic pregnancy was further supported by transvaginal ultrasound showing no intrauterine pregnancy, with free fluid throughout the pelvis representing a potential haemoperitoneum. CT of the abdomen (with/without contrast) showed a large amorphous hyperdensity in the pelvis anterior and superior to the uterus, with fluid extending along bilateral paracolic gutters, with moderate perihepatic and perisplenic free fluid. In addition, there was a 5.6×4.5 cm right adnexal cyst. After the diagnosis of ruptured ectopic pregnancy with haemoperitoneum was confirmed, the patient was taken to the operating room for laparoscopic right salpingectomy with evacuation of haemoperitoneum and drainage of right ovarian cyst with removal of IUD.
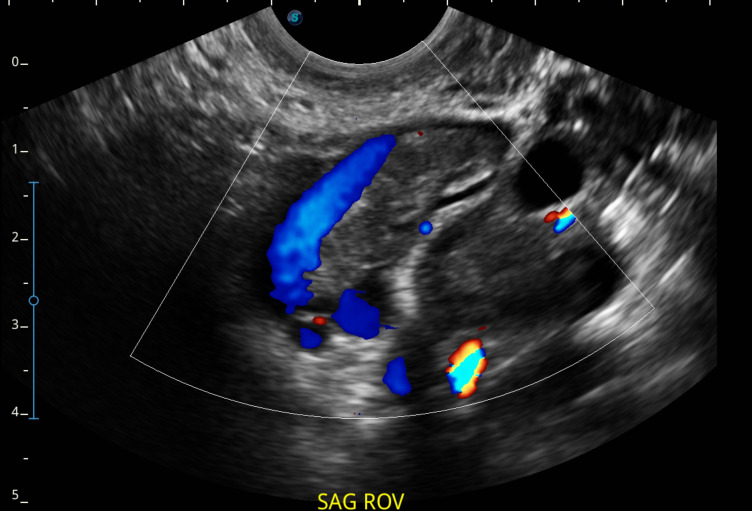
Postoperatively, the patient did seemingly well until she presented to the clinic 4 weeks later with right-sided pelvic pain that she rated as an 8/10. The patient reported vaginal bleeding but denied vomiting or nausea. Since removal of her IUD, she reported using condoms for contraception and had no history of tobacco use. Physical examination was positive for mild tenderness to palpation of the right ovary but was otherwise insignificant, and the laparoscopic surgical incisions were healing well and showed no signs of infection. Pregnancy test done in the office was negative, and transvaginal ultrasound showed right ovarian vein varices with sluggish flow and areas of non-occluding thrombus (figure 1) consistent with the diagnosis of right OVT.
Figure 1.
Right ovarian vein varices with sluggish flow and areas of non-occluding thrombus.
Treatment
PE can also be a sequela of postpartum ovarian vein thrombosis (POVT). Some studies have shown the rates of occurrence of PE after being diagnosed with a POVT to be around 0.15%–0.33%.3 A CT was done and showed no evidence of a clot. While negative for an acute PE, this provides further support for the use of intravenous or oral anticoagulants for patients who have had a POVT. Although the diagnosis may initially prove difficult to make, swift management with anticoagulation therapy such as low-molecular-weight heparin or Xarelto has been shown to be effective in select case studies. While the duration of anticoagulation therapy has been controversial, mortality rates have been shown to decrease from 25% to 5% in patients who have been managed with anticoagulation.3 Surgical management of POVT is an option for patients who have contraindications to anticoagulants.
Outcome and follow-up
After the diagnosis of an OVT was confirmed via imaging studies, the patient underwent coagulation studies that proved to be unrevealing. The patient was started on appropriate anticoagulation medication and has since been stable with no recurrence or residual symptoms.
Discussion
Thromboembolism is a known and well-established complication of gynaecological surgery.6 In addition, a history of endometriosis, as in this case, is known to further increase coagulopathies postoperatively.6 Thrombus occurs in the right ovarian vein in 70%–90% of cases due to its length and absence of functioning valves.7 The pathophysiology of a thromboembolism and OVT is the same, both involving Virchow’s triad of venous stasis, endothelial damage and hypercoagulability.7 In theory, a ruptured ectopic pregnancy would at the very least potentiate endothelial damage, leading to systemic release of clotting factors which could increase the risk of thrombosis in the ipsilateral or contralateral ovarian vein.
Patients with POVT typically present with right lower quadrant pain and fever. Nausea and vomiting are common but not specific. A palpable mass in the iliac fossa is a less common finding.8 If POVT is suspected, ultrasound should be the initial imaging study. An ultrasound can confirm the diagnosis but should not be used to exclude the diagnosis as ovarian veins can only be visualised in 52% of cases on the right and 23% of cases on the left.9 If clinical suspicion for POVT remains high, a spiral CT scan or magnetic resonance angiography (MRA) should be requested for definitive diagnosis.10 Contrast-enhanced CT of the abdomen and pelvis is currently the most acceptable modality for initial diagnosis. It has a sensitivity of 77.8% and specificity of 62.5% for diagnosing OVT. MRA is technically diagnostically superior to CT in diagnosing OVT with a sensitivity and specificity close to 100%, but is rarely used due to the availability of CT imaging.11 12 On CT, POVT can be identified as a dilated tubular retroperitoneal structure that contains central low-attenuation areas.13
A retrospective study carried out at the Mayo clinic examined around 40 patients with OVT and found 20% with a history of pelvic surgery.14 The established link between gynaecological surgery and thromboembolism, compounded with the possibility for endothelial damage sensitive to a ruptured ectopic pregnancy, further corroborates the need to keep OVT on the differential diagnosis. In a healthy adult patient, preoperative evaluation of haemostasis is not recommended.15 This seems to hold true in patients undergoing laparoscopic salpingectomy based on the fact that the patient presented in this case had normal coagulation studies preoperatively. The pairing of normal coagulation studies and the development of OVT has been previously documented.16 Given that thrombosis is a known complication for gynaecological surgery, our hope is that clinicians can use this case report to increase awareness of POVT and consider its diagnosis when confronted with a similar patient presentation.
Learning points.
Clinicians are at an inherent disadvantage when confronted with a postpartum ovarian vein thrombosis due to its low incidence and lack of clinical data.
The presence of vague abdominal complaints following pelvic laparoscopic surgery should warrant a further investigation of ovarian vein thrombosis, with imaging (transvaginal ultrasound, contrast-enhanced CT) being the most useful tool in helping to define the problem.
If the diagnosis of an ovarian vein thrombosis is confirmed, swift anticoagulation should be administered to treat this potentially life-threatening disease process. Surgical treatment should be considered, if needed.
Footnotes
Contributors: DET, the first author, researched, edited, drafted and revised the manuscript. JDM researched, edited and drafted the manuscript. JS, the mentor, edited the manuscript, provided documentation and kept in communication with the patient.
Funding: The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests: None declared.
Provenance and peer review: Not commissioned; externally peer reviewed.
References
- 1.Murray H, Baakdah H, Bardell T, et al. Diagnosis and treatment of ectopic pregnancy. CMAJ 2005;173:905–12. 10.1503/cmaj.050222 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Lozeau A-M, Potter B. Diagnosis and management of ectopic pregnancy. Am Fam Physician 2005;72:1707–14. [PubMed] [Google Scholar]
- 3.Kumar V, Gupta J. Tubal ectopic pregnancy. BMJ Clin Evid 2015;2015:1406. [PMC free article] [PubMed] [Google Scholar]
- 4.Stovall TG, Kellerman AL, Ling FW, et al. Emergency department diagnosis of ectopic pregnancy. Ann Emerg Med 1990;19:1098–103. 10.1016/S0196-0644(05)81511-2 [DOI] [PubMed] [Google Scholar]
- 5.Saxon D, Falcone T, Mascha EJ, et al. A study of ruptured tubal ectopic pregnancy. Obstet Gynecol 1997;90:46–9. 10.1016/S0029-7844(97)00180-4 [DOI] [PubMed] [Google Scholar]
- 6.Mann WJ. Complications of gynecologic surgery, 2019. [Google Scholar]
- 7.Togan T, Turan H, Cifci E, et al. Ovarian and renal vein thrombosis: a rare cause of fever outer the postpartum period. Case Rep Obstet Gynecol 2015;2015:1–4. 10.1155/2015/817862 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Basili G, Romano N, Bimbi M, et al. Postpartum ovarian vein thrombosis. JSLS 2011;15:268–71. 10.4293/108680811X13071180406673 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Savader SJ, Otero RR, Savader BL. Puerperal ovarian vein thrombosis: evaluation with CT, us, and MR imaging. Radiology 1988;167:637–9. 10.1148/radiology.167.3.3283835 [DOI] [PubMed] [Google Scholar]
- 10.Twickler DM, Setiawan AT, Evans RS, et al. Imaging of puerperal septic thrombophlebitis: prospective comparison of Mr imaging, CT, and sonography.. AJR Am J Roentgenol 1997;169:1039–43. 10.2214/ajr.169.4.9308461 [DOI] [PubMed] [Google Scholar]
- 11.Jenayah AA, Saoudi S, Boudaya F, et al. Ovarian vein thrombosis. Pan Afr Med J 2015;21:251. 10.11604/pamj.2015.21.251.6908 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Gupta A, Gupta N, Blankstein J, et al. Ovarian vein thrombosis as a complication of laparoscopic surgery. Case Rep Obstet Gynecol 2015;2015:1–4. 10.1155/2015/682941 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Virmani V, Kaza R, Sadaf A, et al. Ultrasound, computed tomography, and magnetic resonance imaging of ovarian vein thrombosis in obstetrical and nonobstetrical patients. Can Assoc Radiol J 2012;63:109–18. 10.1016/j.carj.2010.08.002 [DOI] [PubMed] [Google Scholar]
- 14.Wysokinska EM, Hodge D, McBane RD. Ovarian vein thrombosis: incidence of recurrent venous thromboembolism and survival. Thromb Haemost 2006;96:126–31. 10.1160/TH06-03-0151 [DOI] [PubMed] [Google Scholar]
- 15.Smetana GW. Preoperative medical evaluation of the healthy adult patient, 2020. [Google Scholar]
- 16.Kodali N, Veytsman I, Martyr S, et al. Diagnosis and management of ovarian vein thrombosis in a healthy individual: a case report and a literature review. J Thromb Haemost 2017;15:242–5. 10.1111/jth.13584 [DOI] [PubMed] [Google Scholar]