Abstract
Sporotrichosis is a frequent subcutaneous mycosis in Madagascar. Extracutaenous forms are exceptional and are usually seen in immunosuppressed hosts. We report a case of an aggressive clinical evolution of lymphocutaneous sporotrichosis with osteoarticular involvement in an immunocompetent patient. Therapy with oral itraconazole 200 mg twice daily for 12 months improved the lesion. Early diagnosis of Sporothrix schenkii infection is critical to prevent complications including osteoarticular involvement, disseminated forms and death.
Keywords: Sporotrichosis, Sporothrix shenckii, Osteoarticular, Involvement
1. Introduction
Sporotrichosis is an invasive infection caused by the members of the genus Sporothrix schenkii sensu lato, a dimorphic fungus with global distribution. However, it is more commonly reported from tropical and subtropical areas given the tempered, and humid climate favors its growth [1]. Sporothrix is endemic in Madagascar, with an estimated prevalence of 37% [2]. Lymphocutaneous sporotrichosis is the most common variety. However, osteoarticular lesions are rare [3]. We report one case of osteoarticular sporotrichosis with good response to itraconazole, from 63 cases of sporotrichosis collected in 4 years.
2. Case presentation
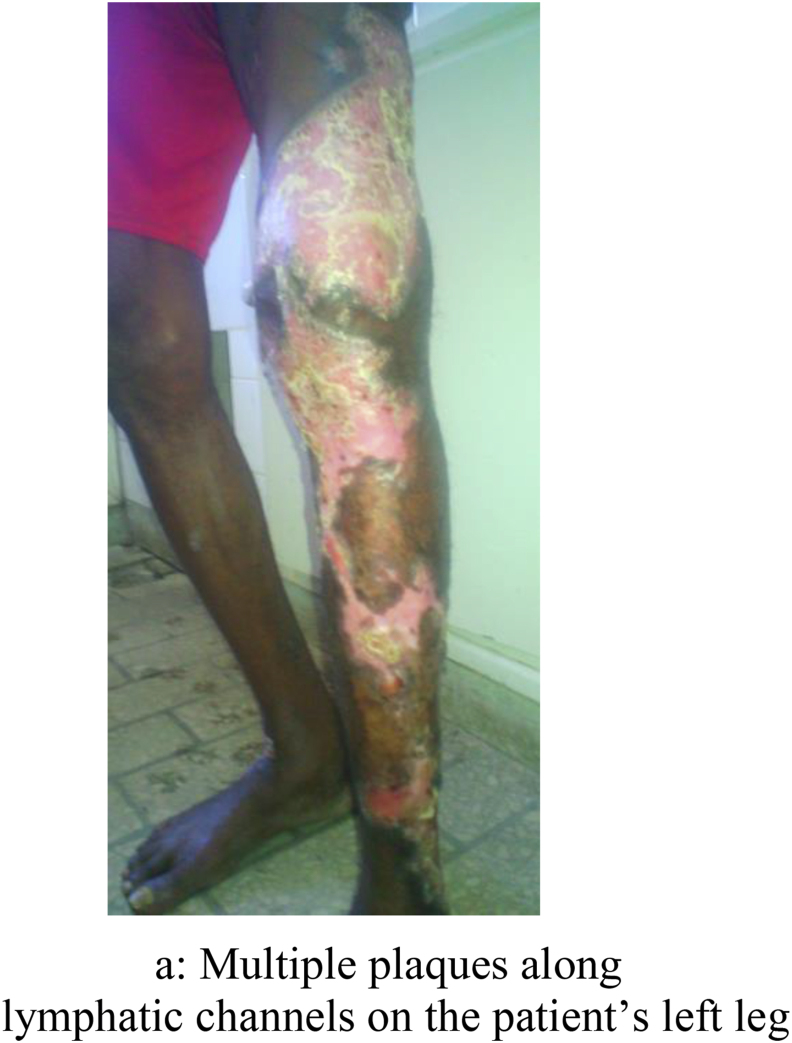
A 34-year-old previously healthy man, farmer, presented with plaques and multiple nodules on the left lower limb (day 0). He lived in rural Madagascar. Six months before, he had noted painless nodule on his left ankle after a traumatic inoculation by plants. Nodule gradually progressed to a plaque with granulomatous appearance and exudation; simultaneously new nodules appeared along the left leg. He complained of severe pain requiring opioids for analgesia. On examination, he was afebrile and vital signs were stable. Physical examination on day 0 revealed multiple plaques along lymphatic channels on the patient's left leg, with crusted ulcer area on the left popliteal fossa (Fig. 1a, Fig. 1ba and b). Furthermore, he presented left knee effusion with limited passive and active range of motion to 15°. Laboratory evaluation on day 0 showed a white cell count of 9000 per cubic millimeter (60% neutrophils and 35% lymphocytes), erythrocyte sedimentation rate (ESR) of 40mm/h, and a C-reactive protein (CRP) of 30mg/L. Serum creatinine and liver testing were within normal limits, and a hemoglobin A1c was 6%. An HIV test was negative. Periodic acid-Schiff stain from skin biopsy demonstrated budding yeast (Fig. 2). Due to the degree of knee involvement and intense pain, imaging tests were requested on day 0. Left knee radiography revealed diffuse joint space narrowing (Fig. 3) and ultrasound showed joint effusion. Fungal culture of a skin biopsy and synovial fluid yielded dark colonies for Sporothrix sp on Sabouraud dextrose agar (SDA) on day +9 (Fig. 4). Microscopic examination show delicate hyphae with clusters of pyriform conidia (Fig. 5). PCR was positive for Sporothrix schenckii sensu stricto. Therapy with oral itraconazole 200 mg twice daily (initiated on day +9) for 12 months improved the lesion and functional impairment of the knee, with no recurrence of sporotrichosis four years after the episode.
Fig. 1a.
Multiple plaques along lymphatic channels on the patient's left leg.
Fig. 1b.
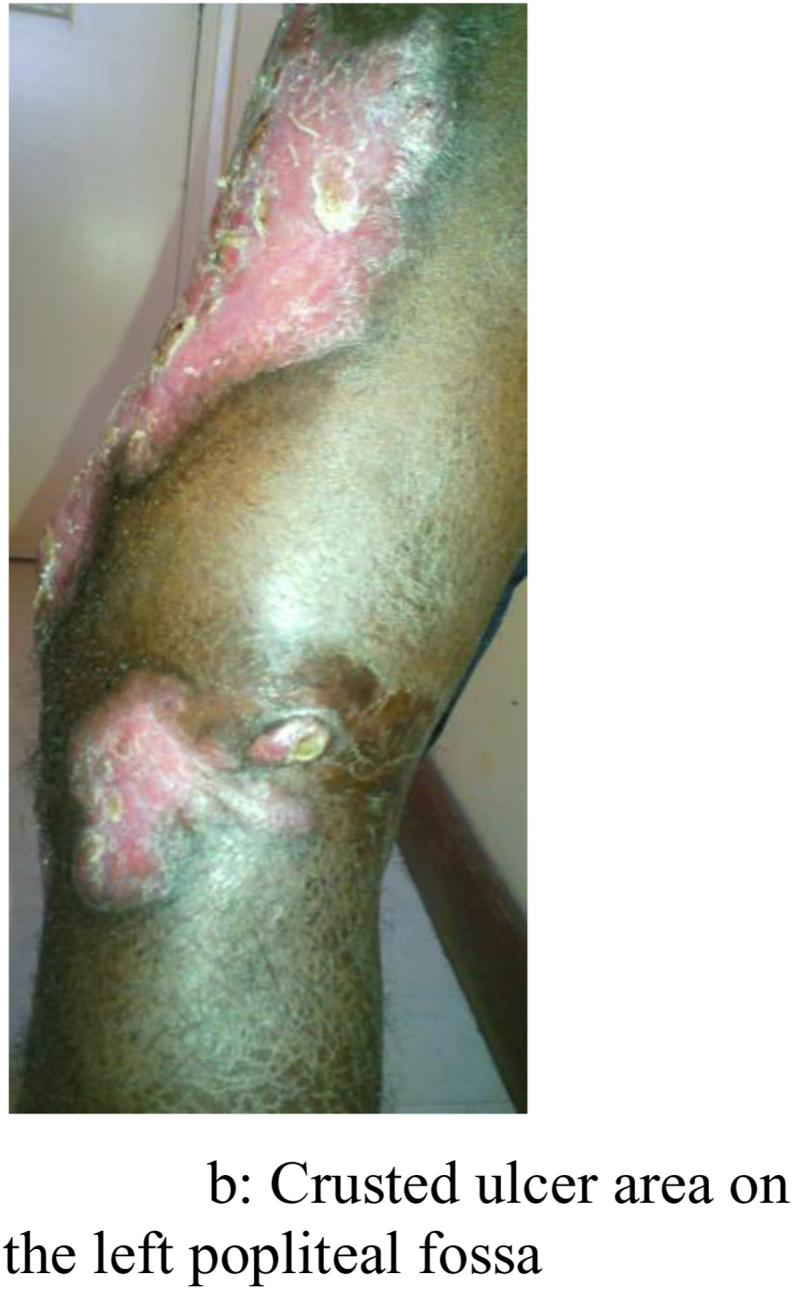
Crusted ulcer area on the left popliteal fossa.
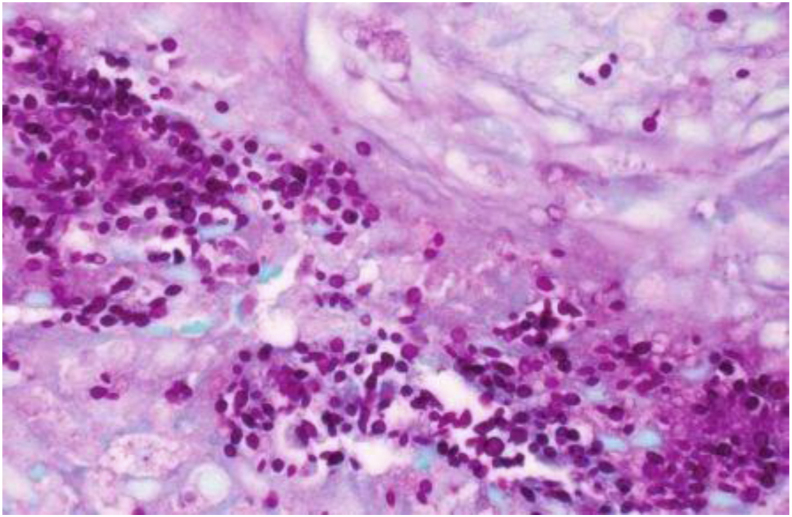
Fig. 2.
PAS stain from skin biopsy showing budding yeast.
Fig. 3.
Diffuse joint space narrowing.
Fig. 4.
Dark colonies on Sabouraud dextrose agar.
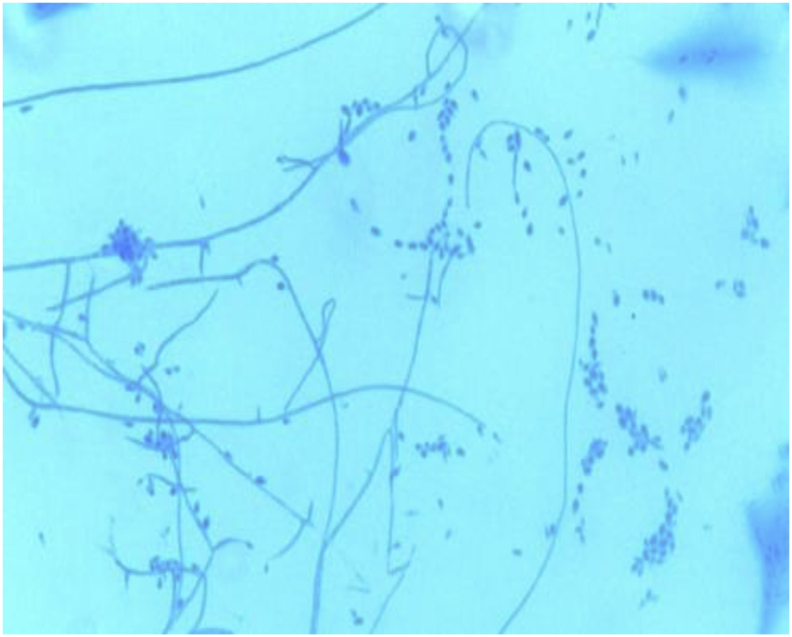
Fig. 5.
Delicate hyphae with clusters of pyriform conidia on microscopic examination.
3. Discussion and conclusion
This case represents unusual form of sporotrichosis. It demonstrates an aggressive clinical evolution of this disease with osteoarticular involvement and a challenge to successful medical treatment.
Sporotrichosis is a disease of worldwide distribution most commonly found in tropical regions, like Madagascar. It is almost endemic in rural areas and professionals handling plants or plant material such as farmers, gardeners, florists, foresters. Like in our case, the majority of patients are between 20 and 50 years of age; the most active years of life when the individual is probably exposed maximally to injuries [4].
The cutaneous and lymphocutaneous forms of sporotrichosis are the most common forms of clinical presentation. Osteoarticular lesions are rare, representing 3–4% of cases [5], and particularly affect immunocompromised, alcoholic and diabetic patients [6,7]. However, our case has no immunosuppression factor. The infection can occur after local or hematogenous dissemination. As shown in our case, local spread can occur when overlying skin lesions progress resulting in underlying erosive bone disease. Initial manifestations are tenosynovitis, joint effusion, bursitis, and synovial cyst formation [8]. The time to diagnosis in our case was 6 months; it seems earlier than this reported in previously cases [5,9,10]. Due to this early diagnosis of Sporothrix schenkii infection, there are no extensive destructive changes which occur in the affected joints because of delayed diagnosis.
Clinical suspiscion is the key for early diagnosis. Few years ago, the diagnosis of sporotrichosis was established only by fungal culture or histopathology findings. In our case, the diagnosis was confirmed by PCR-based strategy with identification of fungal species which is effective, fast, accurate and highly sensitive.
A higher dose and longer duration of itraconazole is recommended for osteoarticular sporotrichosis: oral itraconazole 200 mg twice daily for at least 12 months [8], with success rates varying between 60% and 80% [11]. Among cutaneous-osteoarticular cases, successful response was observed when Itraconazole is combined with sulfamethoxazole/trimethoprim (800mg/160mg) twice daily [12].
Early diagnosis of Sporothrix schenkii infection is critical to prevent complications including septic arthritis, systemic infection and death.
Ethics approval and consent to participate
Ethical approval was granted by Ethics Committee of the University Hospital Joseph Raseta Befelatanana, Antananarivo Madagascar. Written informed consent for publication of their clinical details was obtained from the patient.
Funding statement
No funding.
Declaration of competing interest
The authors declare that no competing interests exist.
Acknowledgements
None.
References
- 1.Quintal D. Sporotrichosis infection on mines of the Witwatersrand. J. Cutan. Med. Surg. 2000;4(1):51–54. doi: 10.1177/120347540000400113. [DOI] [PubMed] [Google Scholar]
- 2.T Rasamoelina, N Rakotozandrindrainy, M Raberahona, F Rapelanoro Rabenja, M Rakoto Andrianarivelo, M Andrianarison et al. Chromoblastomycosis and sporotrichosis in Madagascar: epidemiology, molecular diagnostic and perspectives. 10.1016/j.mycmed.2016.04.035. [DOI] [PubMed]
- 3.Carrada-Bravo T. New observations on the epidemiology of sporotrichosis and Sporothrix schenkii complex. Rev Latinoameric Patol Clin. 2012;59:88–100. [Google Scholar]
- 4.Mahajan V.K., Sharma N.L., Sharma R.C., Gupta M.L., Garg G., Kanga A.K. Cutaneous sporotrichosis in Himachal Pradesh, India. Mycoses. 2005;48(1):25–31. doi: 10.1111/j.1439-0507.2004.01058.x. * [DOI] [PubMed] [Google Scholar]
- 5.Barbaryan A., Atrouni W.E., Bailuc S., Jones M.W., Bhakta M., Mahmoud K.H. Isolated Sporothrix schenkii monoarthritis. Case Rep Inf Dis. 2018 doi: 10.1155/2018/9037657. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Appenzeller S., Amaral T.N., Amstalden E.M., Bertolo M.B., Neto J.F., Samara A.M. Sporothrix schenkii infection presented as monoarthritis: report of two cases and review of the literature. Clin. Rheumatol. 2006;25:926–928. doi: 10.1007/s10067-005-0095-z. [DOI] [PubMed] [Google Scholar]
- 7.Edwards C., Reuther W.L., Greer D.L. Disseminated osteoarticular sporotrichosis: treatment in a patient with acquired immunodeficiency syndrome. South. Med. J. 2000;93:803–806. [PubMed] [Google Scholar]
- 8.Kauffman C.A., Bustamante B., Chapman S.W., Pappas P.G. Clinical practice guidelines for the management of sporotrichosis: 2007 update by the Infectious Diseases Society of America. Clin. Infect. Dis. 2007;45:1255–1265. doi: 10.1086/522765. [DOI] [PubMed] [Google Scholar]
- 9.Patel Rina, Busby L.P., Motamedi D. Delayed diagnosis in a case of smoldering sporotrichal monoarthropathy. Radiology Case. 2019;13(1):17–23. doi: 10.3941/jrcr.v13i1.3520. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Crout J.E., Brewer N.S., Tompkins R.B. Sporotrichosis arthritis: clinical features in seven patients. Ann. Intern. Med. 1977 doi: 10.7326/0003-4819-86-3-294. [DOI] [PubMed] [Google Scholar]
- 11.Hu S., Chung W.H., Hung S.I., Ho H.C., Wang Z.W., Chen C.H. Detection of Sporotrhix schenkii in clinical samples by a nested PCR assay. J. Clin. Microbiol. 2003;41(4):1414–1418. doi: 10.1128/JCM.41.4.1414-1418.2003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Bonifaz A., Tirado-Sanchez A. Cutaneous disseminated and extracutaneous sporotrichosis: current status of a complex disease. J Fungi (Basel) 2017;10(1):6. doi: 10.3390/jof3010006. 3. [DOI] [PMC free article] [PubMed] [Google Scholar]