Abstract
Acute respiratory distress syndrome (ARDS) in COVID‐19 is associated with high mortality. Mesenchymal stem cells are known to exert immunomodulatory and anti‐inflammatory effects and could yield beneficial effects in COVID‐19 ARDS. The objective of this study was to determine safety and explore efficacy of umbilical cord mesenchymal stem cell (UC‐MSC) infusions in subjects with COVID‐19 ARDS. A double‐blind, phase 1/2a, randomized, controlled trial was performed. Randomization and stratification by ARDS severity was used to foster balance among groups. All subjects were analyzed under intention to treat design. Twenty‐four subjects were randomized 1:1 to either UC‐MSC treatment (n = 12) or the control group (n = 12). Subjects in the UC‐MSC treatment group received two intravenous infusions (at day 0 and 3) of 100 ± 20 × 106 UC‐MSCs; controls received two infusions of vehicle solution. Both groups received best standard of care. Primary endpoint was safety (adverse events [AEs]) within 6 hours; cardiac arrest or death within 24 hours postinfusion). Secondary endpoints included patient survival at 31 days after the first infusion and time to recovery. No difference was observed between groups in infusion‐associated AEs. No serious adverse events (SAEs) were observed related to UC‐MSC infusions. UC‐MSC infusions in COVID‐19 ARDS were found to be safe. Inflammatory cytokines were significantly decreased in UC‐MSC‐treated subjects at day 6. Treatment was associated with significantly improved patient survival (91% vs 42%, P = .015), SAE‐free survival (P = .008), and time to recovery (P = .03). UC‐MSC infusions are safe and could be beneficial in treating subjects with COVID‐19 ARDS.
Keywords: cell transplantation, cellular therapy, clinical trials, mesenchymal stem cells, respiratory tract, transplantation, umbilical cord

Lessons learned
Two intravenous infusions of umbilical cord mesenchymal stem cells (UC‐MSCs), at a dose of 100 million cells per infusion, given 72 hours apart, are safe in COVID‐19 patients with acute respiratory distress syndrome.
This double blind randomized controlled trial in 24 subjects demonstrated fewer serious adverse events in the UC‐MSC treatment group compared with the control group.
UC‐MSC treatment was associated with a significant decrease in a set of inflammatory cytokines involved in the COVID‐19 “cytokine storm.”
UC‐MSC treatment was associated with significantly improved patient survival and time to recovery.
The observed findings strongly support further investigation in a larger trial designed to estimate and establish efficacy.
Significance statement
This study was a double‐blind, randomized, controlled, early phase clinical trial of umbilical cord mesenchymal stem cell treatment in 24 subjects with COVID‐19 acute respiratory distress syndrome. This study demonstrated fewer serious adverse events in the treatment group compared with control. Exploratory efficacy analyses provide evidence of significantly improved patient survival and time to recovery. The observed findings strongly support further investigation in a larger trial designed to estimate and establish efficacy. These observations will inform physicians influencing clinical practice and future research in the fields of acute respiratory distress syndrome, COVID‐19, and other immune‐related disorders.
1. INTRODUCTION
Coronavirus disease 2019 (COVID‐19), a pneumonia‐like disease caused by the virus severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2), reached pandemic proportions in early 2020. 1 , 2 A subset of subjects infected by SARS‐CoV‐2 develop severe COVID‐19 requiring hospitalization. 3 , 4 Severe COVID‐19 is believed to result from hyperinflammation, overactive immune response triggering cytokine storm, and a prothrombotic state, collectively determined as immunothrombosis, all elicited by SARS‐CoV‐2 infection. 5 , 6 , 7 , 8 Subjects progressing to acute respiratory distress syndrome (ARDS) require high‐flow oxygen therapy, intensive care, and frequently, mechanical ventilation. 3 , 4 , 9 , 10 , 11 , 12 Mortality in patients with COVID‐19 and ARDS was reported to be 52.4%. 10 There is an urgent need for novel therapies that can attenuate the excessive inflammatory response associated with the immunopathological cytokine storm and immunothrombosis, that can accelerate the recovery of functional lung tissue, and that can abate mortality in patients with severe COVID‐19.
Mesenchymal stem cells, also known as mesenchymal stromal cells or medicinal signaling cells (MSCs), 13 have been shown to modulate overactive immune and hyperinflammatory processes, promote tissue repair, and secrete antimicrobial molecules. 14 , 15 , 16 These cells, with established safety profile when administered intravenously, 17 have been studied for treatment of autoimmune diseases (eg, type 1 diabetes [T1D]), 18 , 19 systemic lupus erythematous, 20 inflammatory disorders, 21 and steroid‐refractory graft‐vs‐host‐disease (GvHD). 22 MSCs have been reported to limit inflammation and fibrosis in the lungs, 23 , 24 and have generated variable yet promising results in ARDS of viral 25 and nonviral etiology. 26 , 27 , 28 , 29 Multiple ongoing trials are now testing MSCs in patients with severe COVID‐19, and pilot uncontrolled trials have reported promising results. 16 , 30 , 31 , 32 , 33 , 34 MSCs can be isolated and expanded from multiple tissues, including the umbilical cord (UC). UC‐MSCs constitute a cell type of choice in cell therapy trials, including for COVID‐19. 15 , 30 , 31 , 32 , 33 , 34 , 35 The experience accumulated thus far indicates that allogeneic UC‐MSC administration is safe in a multitude of diseases. 36 These cells can be derived from umbilical cords discarded after delivery and quickly expanded to clinically relevant numbers. 37 They express low levels of class I and class II human leukocyte antigen, which may reduce alloreactivity. 37 Our Current Good Manufacturing Practice (cGMP) manufacturing facility is now scaling up UC‐MSC manufacturing to support upcoming multisite clinical trials, where large numbers of cell doses will be required.
The objective of this study was to establish safety and explore efficacy of allogenic UC‐MSC infusions in hospitalized patients with ARDS secondary to COVID‐19. Here we report the results at 1 month of follow‐up of a double‐blind randomized controlled trial (RCT) testing this cell‐based therapy approach.
2. MATERIALS AND METHODS
2.1. Trial design
This double‐blind, phase 1/2a randomized controlled trial was an academic, investigator‐initiated trial performed at UHealth System/Jackson Health System (UHS/JHS), in Miami, Florida. This trial was designed to evaluate safety and explore efficacy endpoints of allogeneic UC‐MSCs in patients with COVID‐19 and ARDS.
Regulatory, ethical, and institutional review board approvals were obtained by the Western Institutional Review Board and UHS/JHS Human Subject Research Office/Institutional Review Board in accordance with local institutional requirements.
Additional details are provided in the supplemental online Methods.
2.2. Participants
The trial was conducted in accordance with the principles of the Declaration of Helsinki and consistent with the Good Clinical Practice guidelines of the International Conference on Harmonisation.
Subjects diagnosed with COVID‐19 ARDS were eligible for inclusion if they met the eligibility criteria listed in Table S1 within 24 hours of enrollment. The investigations were performed with informed consent.
2.3. Randomization
Twenty‐four subjects hospitalized for COVID‐19 were randomized 1:1 to either UC‐MSC treatment (n = 12) or to the control group (n = 12). Patients were assigned to treatment group using a stratified, blocked randomized design.
Additional details are provided in the supplemental online Methods.
2.4. Blinding
The study was double‐blinded: neither the patient nor the assessing physician was aware of treatment assignment, and the staff responsible for product administration were blinded to group assignment.
2.5. UC‐MSC investigational product
UC‐MSCs were manufactured as previously described. 38 UC‐MSCs were culture‐expanded from a previously established and characterized master cell bank (MCB) derived from the subepithelial lining of a UC, collected from a healthy term delivery (kindly provided by Jadi Cell and Amit Patel, M.D.). 37 , 39 The MCB and its source tissue were tested according to the applicable U.S. Food and Drug Administration (FDA) regulations and American Association of Blood Banks (AABB) and Foundation for the Accreditation for Cellular Therapy (FACT) standards for cellular therapies.
In preparation for infusion, frozen UC‐MSCs were quickly thawed and slowly diluted in Plasma‐LyteA supplemented with human serum albumin and heparin (vehicle solution). The final volume of UC‐MSC suspension or vehicle solution (control) for infusion was 50 mL. Cell dose (100 ± 20 × 106), cell viability by trypan blue (>80%), cell surface marker expression by flow cytometric analysis (CD90/CD105 > 95%, CD34/CD45 < 5%), endotoxin (<1.65 EU/mL), Gram stain (negative), and 14‐day sterility (negative) were used as product release criteria. The vehicle solution was tested for 14‐day sterility, Gram stain, and endotoxin. The UC‐MSC suspension or vehicle solution was infused within 3 hours of preparation for infusion.
Additional details are provided in the supplemental online Methods.
2.6. Interventions
Subjects in the UC‐MSC treatment group received two intravenous infusions of 100 ± 20 × 106 UC‐MSCs each, in 50 mL vehicle solution containing human serum albumin and heparin, infused over 10 ± 5 minutes, at days 0 and 3. Subjects in the control group (n = 12) received two infusions of 50 mL vehicle solution, at day 0 and day 3. Best standard of care was provided in both groups following the current institutional COVID‐19 guidelines.
Additional details are provided in the supplemental online Methods.
2.7. Outcomes
2.7.1. Primary endpoints
Primary endpoints were the following: (a) safety, defined by the occurrence of prespecified infusion‐associated adverse events (AEs) within 6 hours from each infusion; (b) cardiac arrest or death within 24 hours postinfusion; and (c) incidence of AEs.
2.7.2. Secondary endpoints
Secondary endpoints included exploratory efficacy defined by clinical outcomes and laboratory testing and mechanistic analyses.
Clinical outcomes included the following: (a) survival at day 28 after treatment; (b) time to recovery, defined as time to discharge or, if the subject was hospitalized, no longer requiring supplemental oxygen and no longer requiring COVID‐19‐related medical care; and (c) AEs, serious AEs (SAEs), and clinical outcomes assessed for 31 days after the first infusion, corresponding to 28 days after the last infusion.
Laboratory testing and mechanistic analyses included the following: (a) viral load by SARS‐CoV‐2 real‐time polymerase chain reaction (RT‐PCR) in peripheral blood plasma samples and (b) inflammatory cytokines, chemokines, and growth factors in peripheral blood plasma.
Primary and secondary endpoints are presented in detail in the supplemental online Methods.
2.8. Plasma preparation from peripheral blood
Whole blood was collected from randomized subjects at day 0 (immediately pretreatment) and at day 6 after treatment initiation. Whole blood was collected into EDTA‐treated tubes, transferred on ice, and processed for plasma separation within 4 hours. Whole blood was centrifuged at 2000g for 15 minutes at 4°C. The plasma (top fraction) was collected, aliquoted into cryogenic tubes, and stored at −80°C until processing.
2.9. Analysis of viral load by SARS‐CoV‐2 RT‐PCR
The RealStar SARS‐COV‐2 RT‐PCR kit (Altona Diagnostics GmbH, Hamburg, Germany) was used to detect the SARS‐CoV‐2‐specific S gene and quantify the number of copies per mL of plasma. The assay was performed following the manufacturer's instruction, using plasma samples collected from the randomized subjects on day 0 and day 6.
2.10. Analysis of inflammatory cytokines, chemokines, and growth factors in peripheral blood plasma
A protein array (RayBio Q‐Series, RayBiotech, Peachtree Corners, Georgia) was used to determine plasma levels of a set of inflammatory cytokines, chemokines, and growth factors (granulocyte‐macrophage colony‐stimulating factor [GM‐CSF], interferon [IFN]g, interleukin [IL]‐2, IL‐5, IL‐6, IL‐7, tumor necrosis factor [TNF]a, TNFb, platelet‐derived growth factor [PDGF]‐BB, regulated on activation, normal T cell expressed and secreted, RANTES). The assay was performed using plasma samples collected from the randomized subjects on day 0 and day 6. On the processing day, 1 mL of plasma per sample was thawed in a 37°C water bath and supplemented with 10 μL of 100× Halt Protease and Phosphatase inhibitor cocktail (Thermo Fisher Scientific, Waltham, Massachusetts). Each plasma sample was diluted 1:2 with sample diluent and assayed following the manufacturer's instructions. The fluorescent signals were visualized via a laser scanner equipped with a Cy3 wavelength (green channel) and converted to concentrations (pg/mL) using the standard curve generated per array.
2.11. Statistical methods
Comparisons of AEs, SAEs, demographics, clinical characteristics, comorbidities, and concomitant treatments between the two groups were performed using Fisher's exact test and Wilcoxon two‐sample tests for categorical and continuous variables, respectively. Survival, survival in absence of SAE (SAE‐free survival), and time to recovery were estimated in each group with Kaplan‐Meier survival estimates. Log‐rank tests were used to compare hazards between groups. For the analyses of viral load, P values were calculated using the Wilcoxon rank‐sum test on SAS 9.4. The data were nonnormally distributed. For the analyses of inflammatory cytokines, chemokines, and growth factors, group data at a specific day were analyzed via nonparametric unpaired Mann‐Whitney t test; for the analyses on longitudinal changes in each group, data at day 0 and day 6 were analyzed via nonparametric paired Wilcoxon t test.
2.12. Registration
This trial was registered with ClinicalTrials.gov identifier NCT04355728 (https://clinicaltrials.gov/ct2/show/NCT04355728?term=NCT04355728&draw=2&rank=1).
2.13. Clinical trial protocol
The clinical trial protocol is included in the Data S1.
3. RESULTS
3.1. Participant flow
Participant flow is shown in Figure 1.
FIGURE 1.
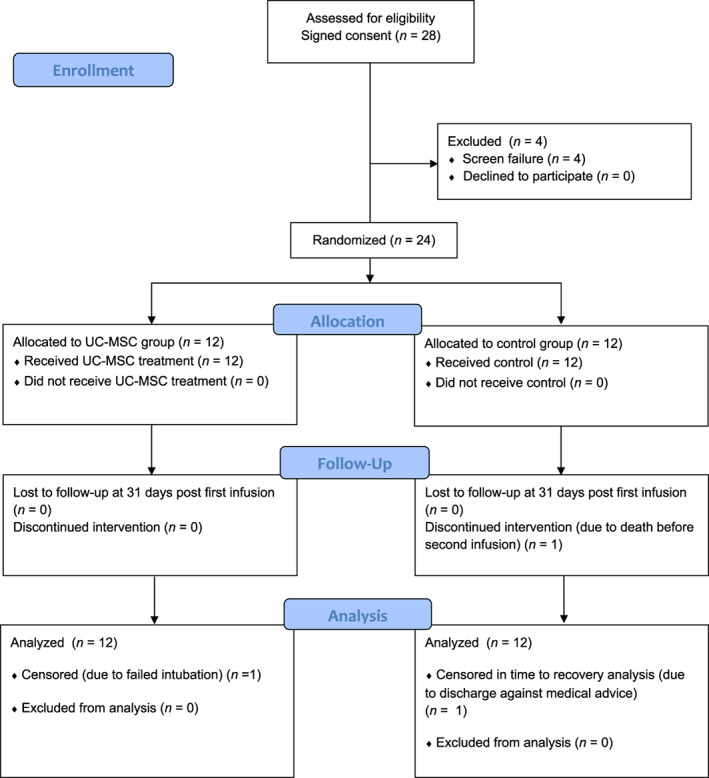
Enrollment and randomization. UC‐MSC, umbilical cord mesenchymal stem cell
3.2. Recruitment
From 25 April 2020, to 21 July 2020, a total of 28 subjects were enrolled. Four subjects were subsequently determined to be ineligible because of screen failure. Twenty‐four subjects were randomized (Figure 1). At enrollment, 11 subjects (46%) were receiving invasive mechanical ventilation, and 13 (54%) were on high flow oxygen therapy via noninvasive ventilation (including high flow nasal cannula, continuous positive airways pressure, or bilevel positive airways pressure) prior to initiation of treatment.
Demographics and baseline characteristics for enrolled subjects, along with stratification, randomization, and concomitant treatment information are presented in Table 1 and Table S2.
TABLE 1.
Baseline characteristics and concomitant treatments during index of hospitalization by treatment group
| Characteristics and treatments | UC‐MSC (n = 12) | Control (n = 12) | P value |
|---|---|---|---|
| Sex, n (%) | .41 | ||
| Male | 5 (41.7) | 8 (66.7) | |
| Female | 7 (58.3) | 4 (33.3) | |
| Age, mean ± SD, years | 58.58 ± 15.93 | 58.83 ± 11.61 | .97 |
| Race, n (%) | 0.99 | ||
| White | 11 (91.7) | 10 (83.3) | |
| African American | 1 (8.3) | 2 (16.7) | |
| Ethnicity, n (%) | 0.99 | ||
| Hispanic or Latino | 11 (91.7) | 11 (91.7) | |
| Non‐Hispanic | 1 (8.3) | 1 (8.3) | |
| PaO2/FiO2 ratio at enrollment, median (IQR) | 124 (68‐164) | 108.5 (68.5‐165.5) | .67 |
| ARDS severity stratification, n (%) | 0.99 | ||
| Mild‐to‐moderate | 3 (25) | 3 (25) | |
| Moderate‐to‐severe | 9 (75) | 9 (75) | |
| BMI, mean ± SD, kg/m2 | 34.5 ± 4.5 | 29.6 ± 3.5 | .01 |
| Smoker (former), n (%) | 0 | 2 (16.7) | .48 |
| Comorbidities, n (%) | |||
| Diabetes | 5 (41.7) | 6 (50) | 0.99 |
| Hypertension | 7 (58.3) | 9 (75) | .67 |
| Obesity (BMI >30) | 11 (91.7) | 5 (41.7) | .03 |
| Cancer | 0 | 1 (8.3) | 0.99 |
| Heart disease | 1 (8.3) | 3 (25) | .59 |
| Concomitant treatments, n (%) | |||
| Heparin | 12 (100) | 12 (100) | 0.99 |
| Only prophylactic dose heparin a | 9 (75) | 7 (58.3) | .67 |
| Therapeutic dose heparin b | 3 (25) | 5 (41.7) | .67 |
| Remdesivir | 9 (75) | 7 (58.3) | .67 |
| Convalescent plasma | 3 (25) | 4 (33.3) | 0.99 |
| Corticosteroids | 10 (83.3) | 9 (75) | 0.99 |
| Tocilizumab | 1 (8.3) | 4 (33.3) | .32 |
| Hydroxychloroquine | 1 (8.3) | 2 (18.2) | .59 |
| Alteplase | 0 | 2 (16.7) | .48 |
Note: Age and BMI are normally distributed. PaO2/FiO2 ratio at enrollment is non‐normally distributed. t test, Wilcoxon two‐sample test, and Fisher's exact test were used for continuous normal, continuous non‐normal and categorical variables, respectively.
Abbreviations: ARDS, acute respiratory distress syndrome; BMI, body mass index; FiO2, fraction of inspired oxygen; IQR, interquartile range; PaO2, partial pressure of oxygen; UC‐MSC, umbilical cord mesenchymal stem cell.
Prophylactic dose heparin: either prophylactic unfractionated heparin, subcutaneous injection, 5000 units two to three times daily (up to 15 000 units) or prophylactic enoxaparin 40 to 60 mg daily.
Therapeutic dose heparin: either full dose unfractionated heparin, intravenous, titrated to a goal of activated partial thromboplastin time, or full dose enoxaparin 1 mg/kg twice daily.
Two cases required special considerations. Subject #11 died for reasons unrelated to COVID‐19 after failed endotracheal intubation. Therefore, this subject was considered as censored in the data analysis for time to COVID‐19‐related death and time to recovery outcomes. Subject #24 left the hospital against medical advice 11 days after second infusion and was thus considered as censored in the time to recovery analysis. This patient eventually recovered at home and was confirmed alive at 31 days after the first infusion.
A Data Safety Monitoring Board reviewed all safety data.
At the time of this writing, all subjects have been followed for 31 days after the first infusion, corresponding to 28 days after the second infusion.
3.3. Baseline data
Twelve subjects were randomized to the UC‐MSC treatment group (age 59 ± 16 years; 7 women [58%]) and 12 to the control group (age 59 ± 12 years; 4 women [33%]) (Table 1; Table S2). The age of enrolled subjects was 59 ± 14 years (mean ± SD).
Three subjects in each group were stratified to the mild‐to‐moderate ARDS severity stratum, and nine subjects in each group into the moderate‐to‐severe stratum. There were no significant differences in concomitant treatments between the groups (Table 1; Table S2). The only differences observed in baseline characteristics and comorbidities were in body mass index and obesity, which were higher in the UC‐MSC treatment group (Table 1; Table S2). The analysis was by original assigned groups.
3.4. Investigational product
An average of 98.7 × 106 UC‐MSCs were administered per infusion. The viability of UC‐MSCs (investigational product) at the time of product release for administration was found to be 96.2% ± 1.8% by trypan blue and 88.4% ± 7.6% by flow cytometry using fixable viability stain. Apoptosis, assessed by activated caspase‐3, was found to be 2.4% ± 3.7%, by flow cytometry (Figure S1). No differences in cell dose, cell viability, or degree of apoptosis were observed between UC‐MSCs (investigational product) prepared for the first or second infusion. Stability studies demonstrated stability of the UC‐MSC investigational product for up to 8 hours after thawing and preparation, as assessed by cell count, viability by trypan blue and flow cytometry, and apoptosis assessed by flow cytometry. Cell surface marker analysis demonstrated a typical surface marker profile characteristic of MSCs: CD90 of 97.9% ± 2.6%, CD105 of 98.1% ± 1.4%, and CD34/CD45 of 2.2% ± 4.9% (Figure S1).
3.5. Outcomes and estimations
A total of nine deaths were documented by day 28 after the second infusion. Two deaths occurred in the UC‐MSC treatment group and seven deaths in the control group. One subject (Subject #11) in the UC‐MSC treatment group died as a result of a failed endotracheal intubation. This outcome was deemed to be unrelated to the patient's COVID‐19 disease. Therefore, data analyses for this subject were censored at the time of failed endotracheal intubation.
The details of all deaths are presented in Table S3.
3.6. Adverse events
Two serious adverse events (SAEs) were observed in the UC‐MSC group and 16 SAEs in the control group, affecting 2 of 12 and 8 of 12 subjects, respectively (P = .04; Fisher's exact test). There were significantly more subjects experiencing SAEs in the control group than in the UC‐MSC treatment group. The adverse events in all subjects are summarized in Table 2.
TABLE 2.
Summary of all adverse events for randomized subjects
| Topics | UC‐MSC treatment, n (%) | Controls, n (%) | Total (n = 24; 12 per group), n (%) | Fisher's exact test |
|---|---|---|---|---|
| Number of AEs reported | 35 | 53 | 88 | |
| Number of subjects with AEs a | 8 | 11 | 19 | NS |
| Number of SAEs reported | 2 | 16 | 18 | |
| Number of subjects with SAEs a | 2 | 8 | 10 | P = .04 |
| Number of AEs by severity b | ||||
| Mild | 13 (37) | 13 (24) | 26 (30) | |
| Moderate | 18 (51) | 21 (40) | 39 (44) | |
| Severe | 4 (12) | 19 (36) | 23 (26) | |
| Subjects with AEs by severity c , d | ||||
| Mild | 7 (44) | 5 (25) | 12 (33) | NS |
| Moderate | 7 (44) | 8 (40) | 15 (42) | NS |
| Severe | 2 (12) | 7 (35) | 9 (25) | NS |
| Number of AEs by relatedness to treatment b | ||||
| Unrelated | 31 (89) | 45 (85) | 76 (86) | |
| Unlikely | 3 (9) | 7 (13) | 10 (11) | |
| Possible | 1 (3) | 1 (2) | 2 (3) | |
| Probable | 0 (0) | 0 (0) | 0 (0) | |
| Definite | 0 (0) | 0 (0) | 0 (0) | |
| Subjects with AEs by relatedness to treatment c , d | ||||
| Unrelated | 8 (80) | 10 (67) | 18 (72) | NS |
| Unlikely | 1 (10) | 4 (26) | 5 (20) | NS |
| Possible | 1 (10) | 1 (7) | 2 (8) | NS |
| Probable | 0 (0.0) | 0 (0.0) | 0 (0.0) | NS |
| Definite | 0 (0.0) | 0 (0.0) | 0 (0.0) | NS |
Abbreviations: AE, adverse event; SAE, serious adverse event; NS, not significant; UC‐MSC, umbilical cord mesenchymal stem cell.
Subjects who experience one or more AEs or SAEs are counted only once.
Percentages are based on number of AEs reported for each treatment group.
Subjects are counted only once within a particular severity grade or relatedness category.
Percentages are based on n for each treatment group.
3.7. Primary endpoint
The primary endpoint was safety, defined as the occurrence of prespecified infusion‐associated AEs within 6 hours after infusion in addition to cardiac arrest or death within 24 hours after infusion. Prespecified infusion‐associated AEs are outlined in Table 3. One subject in each group developed infusion‐associated AEs. UC‐MSC treatment was found to be safe, as it did not lead to an increase in prespecified infusion‐associated AEs. In the UC‐MSC treatment group, the only reported adverse event occurred in a subject with bradycardia, who experienced worsening of bradycardia and required transient vasopressor treatment. In the control group, all prespecified infusion‐associated AEs occurred in the same subject, who experienced cardiac arrest 2 hours after infusion of vehicle solution. In each group, one subject developed infusion‐associated AEs.
TABLE 3.
Primary endpoint: Safety
| Adverse event | Adverse events | |
|---|---|---|
| UC‐MSC treatment (n = 12), n (%) | Control (n = 12), n (%) | |
| 1a. An increase in vasopressor dose | 1 a | 1 |
| 1b. In patients receiving mechanical ventilation: worsening hypoxemia | 0 | 0 |
| 1c. In patients receiving high flow oxygen therapy: worsening hypoxemia, as indicated by requirement of intubation and mechanical ventilation | 0 | 0 |
| 1d. New cardiac arrhythmia requiring cardioversion | 0 | 1 |
| 1e. New ventricular tachycardia, ventricular fibrillation, or asystole | 0 | 1 |
| 1f. A clinical scenario consistent with transfusion incompatibility or transfusion‐related infection | 0 | 0 |
| 2. Cardiac arrest or death within 24 h postinfusion | 0 | 0 |
Note: Safety: as defined by the occurrence of prespecified infusion‐associated adverse events within 6 hours (1a‐1f) and occurrence of cardiac arrest or death within 24 hours postinfusion (2).
The vasopressor dose increase was ordered by the primary treating physician before the infusion started, but it was not given until hours later, after the infusion.
3.8. Secondary endpoints
At 31 days after the first infusion (corresponding to 28 days after the last infusion), patient survival was significantly improved in the UC‐MSC vs the control group: 10 of 11 (91%) vs 5 of 12 (42%), respectively (P = .015). The hazard ratio for death comparing the control group with UC‐MSC treatment group was 8.76 (95% confidence interval [CI]: 1.07‐71.4), indicating that the control group had a higher risk of death. Kaplan‐Meier estimates are presented in Figure 2A (survival).
FIGURE 2.
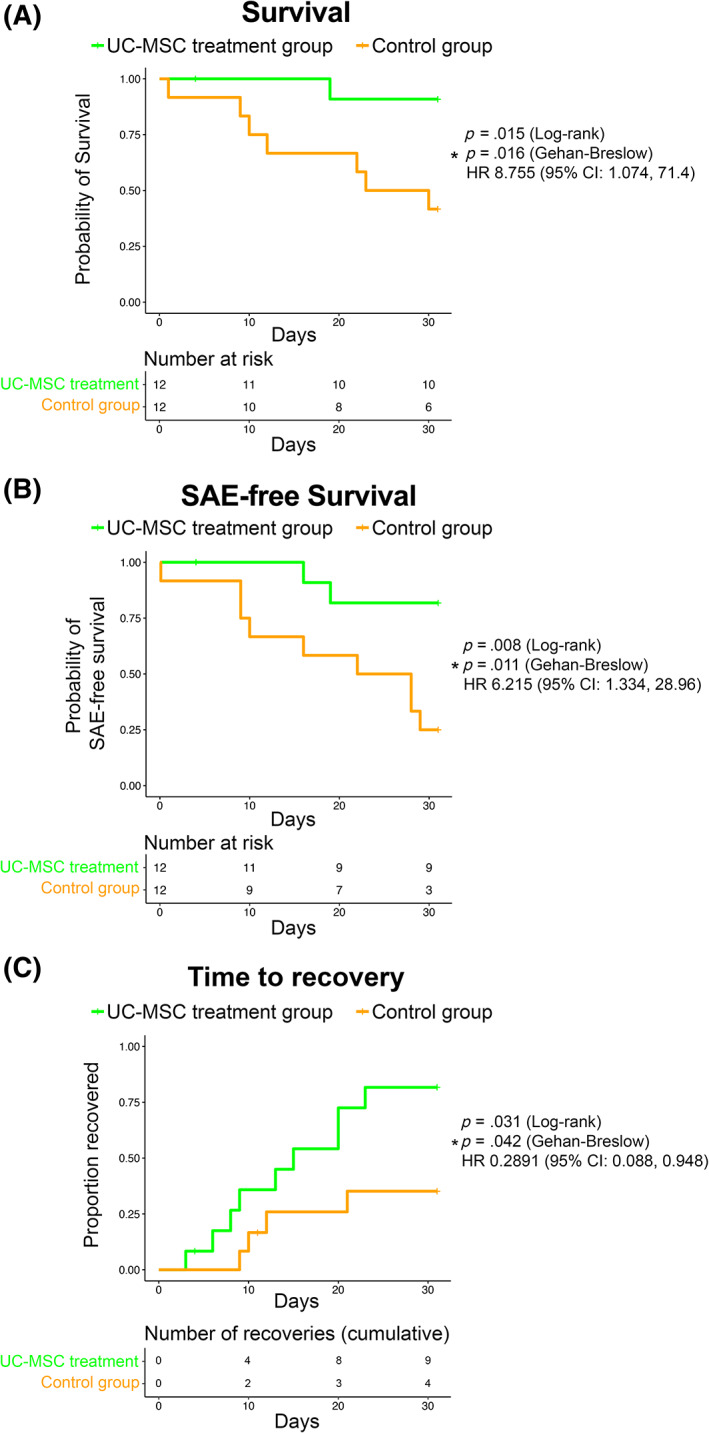
Kaplan‐Meier curves. A, Survival. At 31 days after the first infusion (corresponding to 28 days after the last infusion), patient survival was 91% vs 42% in the UC‐MSC and control group, respectively (P = .015). The difference between the groups was statistically significant. B, SAE‐free survival. SAE‐free survival was significantly improved in the UC‐MSC treatment group compared with the control group (P = .008). SAEs affected two vs eight patients in the UC‐MSC and control group, respectively. C, Time to recovery. Time to recovery was significantly shorter in the UC‐MSC treatment group compared with the control group (P = .031). Censoring was limited to dropout from study, and the event of interest was recovery. In the case of death, the patient's time to recovery was considered censored at the end of study observation; thus the patient conservatively remained in the risk set for all Kaplan‐Meier estimation throughout the study period. CI, confidence interval; HR, hazard ratio; SAE, serious adverse event; UC‐MSC, umbilical cord mesenchymal stem cell
SAE‐free survival was significantly improved in the UC‐MSC treatment group (P = .0081). The hazard ratio for SAE, comparing the control group with the UC‐MSC treatment group, was 6.22 (95% CI: 1.33‐28.96), indicating that the control group experienced an increased risk of SAEs. Kaplan‐Meier estimates are presented in Figure 2B (SAE‐free survival).
Time to recovery was significantly shorter in the UC‐MSC treatment group (P = .0307). The hazard ratio for recovery comparing the control group with the UC‐MSC treatment group was 0.29 (95% CI: 0.09‐0.95); this is evidence of a lower rate of recovery for the control group. Kaplan‐Meier estimates are presented in Figure 2C (time to recovery).
3.9. Analysis of viral load in peripheral blood plasma
The median viral load at day 0 or day 6 did not differ significantly between the UC‐MSC treatment and control group. The P values were .196 and .136 for day 0 and day 6, respectively (Figure S2).
3.10. Analysis of inflammatory cytokines and chemokines levels in peripheral blood plasma
The blood plasma levels of 10 inflammation‐related proteins were assessed by quantitative enzyme‐linked immunosorbent assay in both UC‐MSC treatment and control groups on days 0 and 6. Baseline levels of proteins tested were comparable in both UC‐MSC and control groups (Figure 3; day 0 column, unpaired t tests), with the exception of IL‐6, which showed higher baseline levels in the control group (P < .05, an imbalance between groups possibly resulting from the small sample size). At 6 days after treatment initiation, we observed significant differences between the groups, and a consistent decrease in inflammatory markers only in the UC‐MSC treatment group. In a comparison between groups at day 6, we observed significant differences in the concentration of GM‐CSF, IFNg, IL‐5, IL‐6, IL‐7, TNFa, TNFb, PDGF‐BB, and RANTES (P < .05); median values of these molecules were lower in the UC‐MSC group (Figure 3; day 6 column, unpaired t tests). The difference in IL‐2 resulted very close to statistical significance (P = .051) (Figure 3; day 6 column, IL‐2). In the longitudinal analysis, inflammatory cytokine concentrations showed marked and statistically significant decreases from day 0 to day 6 only in the UC‐MSC treatment group (Figure 3; UC‐MSC treatment and control columns, paired t tests).
FIGURE 3.
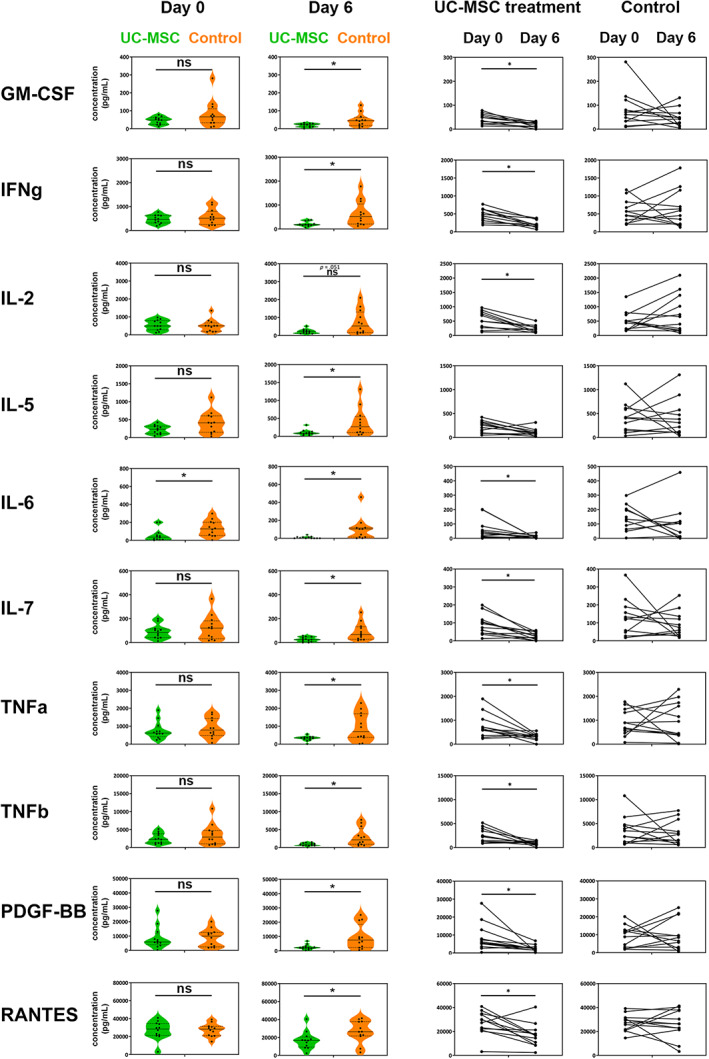
Analysis of inflammatory cytokines, chemokines, and growth factors in plasma of randomized subjects. In the comparison between groups at day 6 and in the longitudinal analysis from day 0 to day 6, inflammatory cytokine concentrations showed marked and statistically significant decreases from day 0 to day 6 only in the UC‐MSC treatment group. The overall “signature” of the response in the UC‐MSC treatment group is characterized by a reduction of the levels of key inflammatory molecules involved in the COVID‐19 “cytokine storm,” including IFNg, IL‐6, and TNFa cytokines and RANTES chemokine. GM‐CSF and PDGF‐BB also decreased significantly only in the UC‐MSC treatment group. ns, not significant; UC‐MSC, umbilical cord mesenchymal stem cell
4. DISCUSSION
Severe COVID‐19 is believed to result from a hyperinflammatory state and overactive immune response with cytokine storm and immunothrombosis elicited by SARS‐CoV‐2 infection. 5 , 40 , 41 Patients with severe COVID‐19 frequently develop ARDS, which is associated with poor prognosis. 4 , 40 Mortality in COVID‐19 is associated with ARDS and multiple organ failure. 42 Mortality in patients with COVID‐19 and ARDS was reported to be 52.4%. 10 Various treatment modalities have been investigated and recently reported, including dexamethasone 11 and convalescent plasma. 43 Yet, there remains a need for therapies that can modulate the inflammatory response, shorten the course of disease, and further improve survival.
UC‐MSCs may have beneficial effects in patients with severe COVID‐19 by modulating immune responses and altering the immunopathogenic cytokine storm. 30 , 31 , 32 The cells used in this trial were derived from the subepithelial lining of the umbilical cord and can be rapidly expanded for clinical applications under strict Good Manufacturing Practice conditions. 37 UC‐MSCs were reported to be safe in clinical trials in other disease states and have been safely administered across histocompatibility barriers. 44 , 45 , 46 Because of their immunomodulatory functions, UC‐MSCs have already been tested in the treatment of autoimmune and inflammatory disorders. Clinical applications using UC‐MSCs processed at our cGMP facility have been authorized by the FDA in subjects with T1D (IND#018302) and Alzheimer's disease (IND#18200).
Several clinical trials have been conducted to test MSCs as treatment of ARDS, mainly focused on determining safety. 25 , 26 , 27 , 28 , 29 Variable results have been reported, possibly because of differences in trial design and quality of the cell product used. Improved outcomes were recently reported in patients with COVID‐19 pneumonia treated with angiotensin converting enzyme ‐ 2 (ACE‐2)‐negative MSCs. 30 Additional pilot studies of UC‐MSCs for COVID‐19 also reported promising results. 31 , 32 , 33
Based on previous encouraging results by other groups, 30 , 31 , 32 , 33 our experience with cell therapy clinical protocols, and the urgent need to develop effective therapeutic strategies, the purpose of this RCT was to determine safety and explore efficacy of UC‐MSCs for treatment of subjects with ARDS secondary to COVID‐19 (ClinicalTrials.gov identifier: NCT04355728).
The current report presents, for the first time, the results of a double‐blind, phase 1/2a RCT testing UC‐MSCs in 24 subjects with COVID‐19 and ARDS. There was overall balance in the distribution of baseline characteristics, comorbidities, or concomitant treatments between the groups. No serious adverse events related to UC‐MSC infusion were observed. There was no observed difference in number of subjects experiencing infusion‐associated adverse events. At 28 days after the last infusion, patient survival was 91% in the UC‐MSC group and 42% in the control group (P = .015). Two SAEs were reported in the UC‐MSC group and 16 in the control group, affecting two and eight patients, respectively (P = .04). SAE‐free survival (P = .008) and time to recovery (P = .03) were significantly improved in the UC‐MSC treatment group.
This study was not intended as an efficacy trial, but instead as an early phase study to establish safety. We relied on randomization to protect against imbalance in biasing preliminary estimates of efficacy. Stratified, blocked randomization was employed to evenly represent ARDS severity and changing standard of care over time between groups. Even with blocked randomization, confounding may exist because, with small numbers, there is still potential for imbalance. Table 1 and Table S2 illustrate overall balance in the distribution of demographic and clinical factors thought to be associated with COVID‐19 trajectory. The only differences observed at baseline, in body mass index and obesity, would be expected to worsen COVID‐19 outcomes in the UC‐MSC treatment group. 47 , 48 The viral load at baseline did not differ significantly between the UC‐MSC treatment and the control group. An important change in inclusion criteria is worthy of discussion. The study was initially designed to enroll patients receiving invasive mechanical ventilation. At the time of study inception, there were concerns regarding the potential for high flow oxygen therapy and noninvasive mechanical ventilation to increase aerosolization and infection risk in health care workers. Such concerns led practitioners to avoid these therapies and prompted infection control leadership to restrict them in our study sites. Subsequent studies called these concerns into question, 49 and high flow oxygen became broadly used. At that time, it appeared appropriate to include in our trial patients of similar disease severity but who were being treated with a different modality, and on 22 June 2020, we made a change in our inclusion criteria to reflect this. Subsequent studies have shown that high flow oxygen therapy is associated with a reduction in the proportion of patients who receive invasive mechanical ventilation, but no difference in mortality. 12 This supports the idea that the change of inclusion criteria did not necessarily alter the severity of patients enrolled but rather just reflects the secular trends and treatment patterns in the care of patients with a novel disease.
The inferences we make from the efficacy results observed in this phase 1/2a trial in 24 subjects, including the outcome of survival, are still subject to limitations of sample size and potential bias because of factors we were not yet aware of. However, results do provide preliminary evidence of a remarkable effect, which substantiates the need for further investigation in a larger, stratified, and adjusted clinical trial. In addition, based on our results and those from previously reported clinical trials, synergistic combination strategies could be explored, with agents that have shown a beneficial effect at similar stages of COVID‐19 disease progression, such as dexamethasone 11 and convalescent plasma. 43
The overall “signature” of the response in the UC‐MSC treatment group is characterized by a reduction of the levels of key inflammatory molecules involved in the COVID‐19 “cytokine storm,” including IFNg, IL‐6, and TNFa cytokines and RANTES chemokine. 50 In parallel, a reduction in GM‐CSF was observed. GM‐CSF is the main activator of the proinflammatory M1 macrophage phenotype; hence, its reduction could lead to macrophage polarization toward alternatively activated M2 macrophages. 51 The levels of PDGF‐BB also resulted significantly reduced in the UC‐MSC treatment group. Notably, PDGF‐BB stimulates mesenchymal cell activation, airway smooth muscle cell proliferation and migration, lung fibroblast cytokine production, and activation of nociceptive neurons. 52 , 53 , 54 Hence, it is possible that the administration of allogeneic MSCs could accelerate the steps of tissue repair in the lungs, decreasing the need for further mesenchymal cell activation.
The positive response in subjects receiving UC‐MSC treatment seems to be more closely associated to a decrease in inflammatory cytokines, rather than a change in viral load.
The observations made in this study could be of assistance for future studies in the field of COVID‐19, ARDS, hyperinflammatory states, overactive immune responses, and autoimmunity. In addition, the preferential targeting of lung tissue after intravenous infusion could make UC‐MSCs particularly appealing for ARDS secondary to trauma, microbial infection, and pulmonary GvHD.
5. CONCLUSION
The results of this trial indicate that UC‐MSC infusions in COVID‐19 with ARDS are safe. Moreover, UC‐MSC treatment was associated with a significant reduction in SAEs, mortality, and time to recovery, compared with controls.
CONFLICT OF INTEREST
The authors declared no potential conflicts of interest.
author contributions
G.L.: conception/design, collection and/or assembly of data, data analysis and interpretation, manuscript writing, final approval of manuscript; E.L.: conception/design, manuscript writing, final approval of manuscript, other (UC‐MSC manufacture); D.C.: collection and/or assembly of data, manuscript writing, final approval of manuscript; S.M.C.: conception/design, data analysis and interpretation, manuscript writing, final approval of manuscript; R.A.A.: conception/design, manuscript writing, final approval of manuscript, other (implementation of the study); D.K.: collection and/or assembly of data, manuscript writing, final approval of manuscript; A.A.G.: collection and/or assembly of data, manuscript writing, final approval of manuscript, other (implementation of the study), other (clinical monitoring); R.P.: collection and/or assembly of data, manuscript writing, final approval of manuscript, other (implementation of the study), other (clinical monitoring); P.R.: conception/design, collection and/or assembly of data, manuscript writing, final approval of manuscript; A.C.M.: manuscript writing, final approval of manuscript, other (implementation of the study); K.H.: manuscript writing, final approval of manuscript, other (protocol preparation), other (regulatory compliance and coordination); C.A.B.: collection and/or assembly of data, manuscript writing, final approval of manuscript, other (implementation of the study); H.K.: collection and/or assembly of data, manuscript writing, final approval of manuscript, other (implementation of the study); L. Rafkin: manuscript writing, final approval of manuscript, other (protocol preparation), other (regulatory compliance and coordination); D.B.: conception/design, manuscript writing, final approval of manuscript, other (clinical monitoring); A.P. and K.G.: manuscript writing, final approval of manuscript, other (implementation of the study); C.L. and X.W.: manuscript writing, final approval of manuscript, other (UC‐MSC manufacture); A.M.A.M. and S.W.M.: data analysis and interpretation, manuscript writing, final approval of manuscript; L. Roque: manuscript writing, final approval of manuscript, other (protocol preparation), other (regulatory compliance and coordination); B.M.: manuscript writing, final approval of manuscript, other (regulatory compliance and coordination); N.S.K., E.G., X.X., J.T., A.I.C., and M.K.G.: conception/design, manuscript writing, final approval of manuscript; R.A.: conception/design, manuscript writing, final approval of manuscript, other (clinical monitoring); C.R.: conception/design, manuscript writing, final approval of manuscript, other (principal investigator), other (clinical monitoring).
Supporting information
Data S1. Supporting Information.
Figure S1. Immunophenotype, viability and apoptosis of UC‐MSC. Flow cytometry analysis demonstrated a surface marker profile characteristic of MSCs, with high proportion of viable cells and low proportion of apoptotic cells.
Figure S2. Xxxxxxxxxxx.
Table S1. Eligibility criteria.
Table S2. Demographic, stratification, and randomization information.
Table S3. Deaths.
Table S4. Flow cytometry reagents.
acknowledgments
The authors wish to thank the North America's Building Trades Unions (NABTU), The Cure Alliance, the Diabetes Research Institute Foundation (DRIF), the Barilla Group and Family, the Fondazione Silvio Tronchetti Provera, the Simkins Family Foundation, and Ugo Colombo for funding this clinical trial; Dr. Amit N Patel for the invaluable contributions to UC‐MSC manufacturing and infusion protocols over the years; Jadi Cell for providing the initial UC‐MSC master cell bank (cells provided at no cost by JadiCell ‐ US Patent # 9,803,176 B2) used in this trial, further expanded at the Diabetes Research Institute (DRI) cGMP Facility to generate the Investigational Product; Drs. George Burke and Ronald Goldberg for serving as Medical Monitor and DSMB Chair; the DRI‐Cell Transplant Center cGMP Staff; Joana R.N. Lemos for the help with data analysis; Melissa Willman for the help in experimental design; and the Clinical Translational Research Site at the Miami Clinical and Translational Science Institute (UL1TR000460) from the National Center for Advancing Translational Sciences and the National Institute on Minority Health and Health Disparities. The trial was supported by unrestricted donations from the North America's Building Trades Unions (NABTU), The Cure Alliance, the Diabetes Research Institute Foundation (DRIF), the Barilla Group and Family, the Fondazione Silvio Tronchetti Provera, the Simkins Family Foundation, and Ugo Colombo. This publication was supported by the Clinical Translational Research Site Grants Number UL1TR000460 and UL1TR002736 from the National Center for Advancing Translational Sciences (NCATS). The contents of this publication are solely the responsibility of the authors and do not necessarily represent the official views of the NIH. The funding sources had no roles in study design, patient recruitment, data collection, data analysis, data interpretation, or writing the report. None of the authors has been paid to write this article by a pharmaceutical company or other agency. The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit this manuscript for publication.
Lanzoni G, Linetsky E, Correa D, et al. Umbilical cord mesenchymal stem cells for COVID‐19 acute respiratory distress syndrome: A double‐blind, phase 1/2a, randomized controlled trial. STEM CELLS Transl Med. 2021;10:660–673. 10.1002/sctm.20-0472
Funding information National Center for Advancing Translational Sciences, Grant/Award Numbers: UL1TR002736, UL1TR000460; Ugo Colombo; Simkins Family Foundation; Fondazione Silvio Tronchetti Provera; Barilla Group and Family; Diabetes Research Institute Foundation (DRIF); The Cure Alliance; North America's Building Trades Unions (NABTU)
DATA AVAILABILITY STATEMENT
Individual participant data will be available. In particular, individual participant data that underlie the results reported in this article, after deidentification (text, tables, figures), will be available. Study protocol, statistical analysis plan, and analytic code will be available. Data will be available immediately after publication and ending 2 years after article publication. Data will be shared with investigators whose proposed use of the data has been approved by an independent review committee (“learned intermediary”) identified for this purpose, to achieve aims in the approved proposal. Proposals may be submitted up to 24 months after article publication. After 24 months the data will be available in the University of Miami's data warehouse but without investigator support other than deposited metadata. Information regarding submitting proposals and accessing data may be found at http://www.regenmedtrials.org or may be requested to Camillo Ricordi, cricordi@med.miami.edu and Giacomo Lanzoni, glanzoni@med.miami.edu.
references
- 1. Zhou P, Yang XL, Wang XG, et al. A pneumonia outbreak associated with a new coronavirus of probable bat origin. Nature. 2020;579:270‐273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Wu JT, Leung K, Bushman M, et al. Estimating clinical severity of COVID‐19 from the transmission dynamics in Wuhan, China. Nat Med. 2020;26:506‐510. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Centers for Disease Control and Prevention . Interim Clinical Guidance for Management of Patients with Confirmed Coronavirus Disease (COVID‐19). https://www.cdc.gov/coronavirus/2019-ncov/hcp/clinical-guidance-management-patients.html. Updated June 20, 2020. Accessed on November 23, 2020.
- 4. Berlin DA, Gulick RM, Martinez FJ. Severe Covid‐19. N Engl J Med. 2020;383:2451‐2460. [DOI] [PubMed] [Google Scholar]
- 5. Kox M, Waalders NJB, Kooistra EJ, Gerretsen J, Pickkers P. Cytokine levels in critically ill patients with COVID‐19 and other conditions. JAMA. 2020;324:1565‐1567. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Lucas C, Wong P, Klein J, et al. Longitudinal analyses reveal immunological misfiring in severe COVID‐19. Nature. 2020;584:463‐469. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Del Valle DM, Kim‐Schulze S, Huang HH, et al. An inflammatory cytokine signature predicts COVID‐19 severity and survival. Nat Med. 2020;26:1636‐1643. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. Patel BV, Arachchillage DJ, Ridge CA, et al. Pulmonary angiopathy in severe COVID‐19: physiologic, imaging, and hematologic observations. Am J Respir Crit Care Med. 2020;202:690‐699. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Wiersinga WJ, Rhodes A, Cheng AC, Peacock SJ, Prescott HC. Pathophysiology, transmission, diagnosis, and treatment of coronavirus disease 2019 (COVID‐19): a review. JAMA. 2020;324:782‐793. [DOI] [PubMed] [Google Scholar]
- 10. Wu C, Chen X, Cai Y, et al. Risk factors associated with acute respiratory distress syndrome and death in patients with coronavirus disease 2019 pneumonia in Wuhan, China. JAMA Intern Med. 2020;180:934‐943. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11. WHO Rapid Evidence Appraisal for COVID‐19 Therapies (REACT) Working Group , JAC S, Murthy S, Diaz JV, et al. Association between administration of systemic corticosteroids and mortality among critically ill patients with COVID‐19: a meta‐analysis. JAMA. 2020;324:1330‐1341. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Demoule A, Vieillard Baron A, Darmon M, et al. High‐flow nasal cannula in critically iii patients with severe COVID‐19. Am J Respir Crit Care Med. 2020;202:1039‐1042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Caplan AI. Mesenchymal stem cells: time to change the name! stem cells translational med. 2017;6:1445‐1451. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Caplan AI, Correa D. The MSC: an injury drugstore. Cell Stem Cell. 2011;9:11‐15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Laroye C, Gibot S, Huselstein C, et al. Mesenchymal stromal cells for sepsis and septic shock: lessons for treatment of COVID‐19. stem cells translational med. 2020;9:148‐1494. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16. Atala A, Henn A, Lundberg M, et al. Regen med therapeutic opportunities for fighting COVID‐19. stem cells translational med. 2020; 10.1002/sctm.20-0245 [Epub ahead of print]. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Thompson M, Mei SHJ, Wolfe D, et al. Cell therapy with intravascular administration of mesenchymal stromal cells continues to appear safe: an updated systematic review and meta‐analysis. EClinicalMedicine. 2020;19:100249. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Cai J, Wu Z, Xu X, et al. Umbilical cord mesenchymal stromal cell with autologous bone marrow cell transplantation in established type 1 diabetes: a pilot randomized controlled open‐label clinical study to assess safety and impact on insulin secretion. Diabetes Care. 2016;39:149‐157. [DOI] [PubMed] [Google Scholar]
- 19. Carlsson PO, Schwarcz E, Korsgren O, le Blanc K. Preserved beta‐cell function in type 1 diabetes by mesenchymal stromal cells. Diabetes. 2015;64:587‐592. [DOI] [PubMed] [Google Scholar]
- 20. Wen L, Labopin M, Badoglio M, et al. Prognostic factors for clinical response in systemic lupus erythematosus patients treated by allogeneic mesenchymal stem cells. Stem Cells Int. 2019;2019:7061408. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21. Garcia‐Olmo D, Garcia‐Arranz M, Herreros D, et al. A phase I clinical trial of the treatment of Crohn's fistula by adipose mesenchymal stem cell transplantation. Dis Colon Rectum. 2005;48:1416‐1423. [DOI] [PubMed] [Google Scholar]
- 22. Le Blanc K, Frassoni F, Ball L, et al. Mesenchymal stem cells for treatment of steroid‐resistant, severe, acute graft‐versus‐host disease: a phase II study. Lancet. 2008;371:1579‐1586. [DOI] [PubMed] [Google Scholar]
- 23. Moodley Y, Vaghjiani V, Chan J, et al. Anti‐inflammatory effects of adult stem cells in sustained lung injury: a comparative study. PLoS One. 2013;8:e69299. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Harrell CR, Sadikot R, Pascual J, et al. Mesenchymal stem cell‐based therapy of inflammatory lung diseases: current understanding and future perspectives. Stem Cells Int. 2019;2019:4236973. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Chen J, Hu C, Chen L, et al. Clinical study of mesenchymal stem cell treating acute respiratory distress syndrome induced by epidemic influenza A (H7N9) infection, a hint for COVID‐19 treatment. Engineering (Beijing). 2020;6:1153‐1161. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Yip HK, Fang WF, Li YC, et al. Human umbilical cord‐derived mesenchymal stem cells for acute respiratory distress syndrome. Crit Care Med. 2020;48:e391‐e399. [DOI] [PubMed] [Google Scholar]
- 27. Matthay MA, Calfee CS, Zhuo H, et al. Treatment with allogeneic mesenchymal stromal cells for moderate to severe acute respiratory distress syndrome (START study): a randomised phase 2a safety trial. Lancet Respir Med. 2019;7:154‐162. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Zheng G, Huang L, Tong H, et al. Treatment of acute respiratory distress syndrome with allogeneic adipose‐derived mesenchymal stem cells: a randomized, placebo‐controlled pilot study. Respir Res. 2014;15:39. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29. Zhao R, Su Z, Wu J, Ji HL. Serious adverse events of cell therapy for respiratory diseases: a systematic review and meta‐analysis. Oncotarget. 2017;8:30511‐30523. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Leng Z, Zhu R, Hou W, et al. Transplantation of ACE2(−) mesenchymal stem cells improves the outcome of patients with COVID‐19 pneumonia. Aging Dis. 2020;11:216‐228. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Liang B, Chen J, Li T, et al. Clinical remission of a critically ill COVID‐19 patient treated by human umbilical cord mesenchymal stem cells: a case report. Medicine (Baltimore). 2020;99:e21429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Guo Z, Chen Y, Luo X, He X, Zhang Y, Wang J. Administration of umbilical cord mesenchymal stem cells in patients with severe COVID‐19 pneumonia. Crit Care. 2020;24:420. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Meng F, Xu R, Wang S, et al. Human umbilical cord‐derived mesenchymal stem cell therapy in patients with COVID‐19: a phase 1 clinical trial. Signal Transduct Target Ther. 2020;5:172. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34. Qu W, Wang Z, Hare JM, et al. Cell‐based therapy to reduce mortality from COVID‐19: systematic review and meta‐analysis of human studies on acute respiratory distress syndrome. stem cells translational med. 2020;9:1007‐1022. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35. Can A, Coskun H. The rationale of using mesenchymal stem cells in patients with COVID‐19‐related acute respiratory distress syndrome: what to expect. stem cells translational med. 2020;9:1287‐1302. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36. Can A, Celikkan FT, Cinar O. Umbilical cord mesenchymal stromal cell transplantations: a systemic analysis of clinical trials. Cytotherapy. 2017;19:1351‐1382. [DOI] [PubMed] [Google Scholar]
- 37. Patel AN, Vargas V, Raveloo P, et al. Mesenchymal stem cell population isoalted from the subepithelial layer of umbilical cord tissue. Cell Transplant. 2013;22:513‐519. [DOI] [PubMed] [Google Scholar]
- 38. Lanzoni G, Linetsky E, Correa D, et al. Umbilical cord‐derived mesenchymal stem cells for COVID‐19 patients with acute respiratory distress syndrome (ARDS). CellR4. 2020;e2839. 10.32113/cellr4_20204_2839 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39. Patel A, inventor. Methods and compositions for the clinical derivation of an allogenic cell and therapeutic uses. US patent 9,803,176 B2. October 31, 2017.
- 40. Matthay MA, Leligdowicz A, Liu KD. Biological mechanisms of COVID‐19 ARDS. Am J Respir Crit Care Med. 2020;202:1489‐1491. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41. McElvaney OJ, McEvoy NL, McElvaney OF, et al. Characterization of the inflammatory response to severe COVID‐19 illness. Am J Respir Crit Care Med. 2020;202:812‐821. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42. McGonagle D, O'Donnell JS, Sharif K, et al. Immune mechanisms of pulmonary intravascular coagulopathy in COVID‐19 pneumonia. Lancet Rheumatol. 2020;2:e437‐e445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43. Liu STH, Lin HM, Baine I, et al. Convalescent plasma treatment of severe COVID‐19: a propensity score‐matched control study. Nat Med. 2020;26:1708‐1713. [DOI] [PubMed] [Google Scholar]
- 44. Tuma J, Carrasco A, Castillo J, et al. RESCUE‐HF trial: retrograde delivery of allogeneic umbilical cord lining subepithelial cells in patients with heart failure. Cell Transplant. 2016;25:1713‐1721. [DOI] [PubMed] [Google Scholar]
- 45. Bartolucci J, Verdugo FJ, Gonzalez PL, et al. Safety and efficacy of the intravenous infusion of umbilical cord mesenchymal stem cells in patients with heart failure: a phase 1/2 randomized controlled trial (RIMECARD trial [randomized clinical trial of intravenous infusion umbilical cord mesenchymal stem cells on Cardiopathy]). Circ Res. 2017;121:1192‐1204. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46. Deng D, Zhang P, Guo Y, Lim TO. A randomised double‐blind, placebo‐controlled trial of allogeneic umbilical cord‐derived mesenchymal stem cell for lupus nephritis. Ann Rheum Dis. 2017;76:1436‐1439. [DOI] [PubMed] [Google Scholar]
- 47. Kang Z, Luo S, Gui Y, et al. Obesity is a potential risk factor contributing to clinical manifestations of COVID‐19. Int J Obes (Lond). 2020;44:2479‐2485. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48. Soeroto AY, Soetedjo NN, Purwiga A, et al. Effect of increased BMI and obesity on the outcome of COVID‐19 adult patients: a systematic review and meta‐analysis. Diabetes Metab Syndr. 2020;14:1897‐1904. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49. Li J, Fink JB, Ehrmann S. High‐flow nasal cannula for COVID‐19 patients: low risk of bio‐aerosol dispersion. Eur Respir J. 2020;55:2000892. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50. Tang Y, Liu J, Zhang D, Xu Z, Ji J, Wen C. Cytokine storm in COVID‐19: the current evidence and treatment strategies. Front Immunol. 2020;11:1708. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51. Castro‐Dopico T, Fleming A, Dennison TW, et al. GM‐CSF calibrates macrophage defense and wound healing programs during intestinal infection and inflammation. Cell Rep. 2020;32:107857. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52. Kardas G, Daszyńska‐Kardas A, Marynowski M, Brząkalska O, Kuna P, Panek M. Role of platelet‐derived growth factor (PDGF) in asthma as an immunoregulatory factor mediating airway remodeling and possible pharmacological target. Front Pharmacol. 2020;11:47. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53. van Steensel L, Paridaens D, Dingjan GM, et al. Platelet‐derived growth factor‐BB: a stimulus for cytokine production by orbital fibroblasts in Graves' ophthalmopathy. Invest Ophthalmol Vis Sci. 2010;51:1002‐1007. [DOI] [PubMed] [Google Scholar]
- 54. Barkai O, Puig S, Lev S, et al. Platelet‐derived growth factor activates nociceptive neurons by inhibiting M‐current and contributes to inflammatory pain. Pain. 2019;160:1281‐1296. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data S1. Supporting Information.
Figure S1. Immunophenotype, viability and apoptosis of UC‐MSC. Flow cytometry analysis demonstrated a surface marker profile characteristic of MSCs, with high proportion of viable cells and low proportion of apoptotic cells.
Figure S2. Xxxxxxxxxxx.
Table S1. Eligibility criteria.
Table S2. Demographic, stratification, and randomization information.
Table S3. Deaths.
Table S4. Flow cytometry reagents.
Data Availability Statement
Individual participant data will be available. In particular, individual participant data that underlie the results reported in this article, after deidentification (text, tables, figures), will be available. Study protocol, statistical analysis plan, and analytic code will be available. Data will be available immediately after publication and ending 2 years after article publication. Data will be shared with investigators whose proposed use of the data has been approved by an independent review committee (“learned intermediary”) identified for this purpose, to achieve aims in the approved proposal. Proposals may be submitted up to 24 months after article publication. After 24 months the data will be available in the University of Miami's data warehouse but without investigator support other than deposited metadata. Information regarding submitting proposals and accessing data may be found at http://www.regenmedtrials.org or may be requested to Camillo Ricordi, cricordi@med.miami.edu and Giacomo Lanzoni, glanzoni@med.miami.edu.


