Abstract
Background
Determinants of vaccine acceptance are multifactorial, complex, and in most cases, context-dependent. We determined the prevalence of COVID-19 vaccination intention (VI) and fear of its adverse effects (FAE) as well as their associated factors in Latin America and the Caribbean (LAC).
Methods
We conducted a secondary cross-sectional analysis of a database collected by the University of Maryland and Facebook. We included participants aged 18 and over from LAC surveyed, January 15 to February 1, 2021. We evaluated VI, FAE, sociodemographic characteristics, COVID-19 symptomatology, compliance with community mitigation strategies, food and economic insecurity, mental health evaluation and the influence in VI when recommended by different stakeholders. We calculated crude and adjusted prevalence ratios with their 95%CIs.
Results
We analyzed 472,521 responses by Latin American adults, finding a VI and FAE prevalence of 80.0% and 81.2%, respectively. We found that female and non-binary genders were associated with a lower probability of VI and a higher probability of FAE. Besides, living in a town, village or rural area and economic insecurity was associated with a higher FAE probability. The fears of becoming seriously ill, a family member becoming seriously ill from COVID-19 and having depressive symptoms were associated with a higher probability of VI and FAE.
Conclusion
Eight out of 10 adults in LAC have VI and FAE. The factors identified are useful for the development of communication strategies to reduce FAE frequency. It is necessary to guarantee mass vaccination and support the return of economic activities.
Keywords: COVID-19, SARS-CoV-2, COVID-19 vaccines, Vaccination, Vaccination refusal, Latin America
1. Introduction
The Coronavirus Disease 2019 (COVID-19) pandemic continues to affect the population worldwide. On April 12, 2021, more than 136.2 million cases and more than 2.94 million deaths have been reported from COVID-19 globally [1]. Latin America and the Caribbean (LAC) is one of the regions with the highest number of cases and mortality from COVID-19. Vulnerability to the pandemic is being exacerbated by the structural challenges posed by poverty, severe inequality and the region's already insufficient social protection and health systems and safety nets [2]. For example, by April 12, 2021, countries in this region such as Brazil (2nd place: 353,137 deaths), Mexico (3rd place: 209,338 deaths), Colombia (11th place: 65,889), Argentina (13th place: 57,779) and Peru (15th place: 54,903), lead the count of deaths from COVID-19 in the world [1].
Vaccines are health technologies widely used for disease prevention, recognizing that their use reduces the number of deaths from preventable causes and costs in health systems [[3], [4], [5]]. They are considered a highly cost-effective measure in health, preventing two to three million deaths per year [6]. In the context of the COVID-19 pandemic, vaccines have been developed as an additional tool to reduce the impact of the infection due the Severe Acute Respiratory Syndrome coronavirus 2 (SARS-CoV-2). To date, more than 50 vaccine candidates have been developed in the world against SARS-CoV-2 [7]. Some of them are already approved by the leading regulatory institutions such as the Food and Drug Administration (FDA) and European Medicines Agency (EMA), allowing vaccination campaigns in several countries worldwide.
Even though vaccines are essential for controlling transmissible diseases such as COVID-19; the growing spread of anti-vaccine movements and mistrust towards immunization programs have undermined vaccine effectiveness during the last decades, a situation that has been identified by the World Health Organization (WHO) as one of the top 10 threats to global health [6]. There are different motivations for reluctance to vaccination, including fear of its adverse effects (FAE), misinformation about the vaccine and its effects, or distrust of medical personnel or the health system, among others [8]. Likewise, sociodemographic factors such as age, gender, and residence area could be associated differently with vaccine intention depending on the context where they are researched [9,10]. Although the pandemic has overwhelmed health systems resulting in high mortality and morbidity rates, surveys have identified vaccine-hesitant subgroups [[9], [10], [11], [12]].
Vaccine hesitancy is not a new phenomenon and predates the pandemic. By June 2020, surveys carried in countries affected by the pandemic describe that around 20% would not be willing to be vaccinated against COVID-19 [9,13]. Among the arguments described, the possibility of adverse events due to the vaccine administration stands out [14]. So far, there is little evidence about the VI against COVID-19 in LAC, a region characterized by access barriers to achieving immunization coverage goals such as socioeconomic inequalities, the influence of beliefs and attitudes and FAE [15]. The determinants of the acceptance of vaccination are multiple and depend on the context in which they are evaluated [8]. Therefore, this study aimed to determine the prevalence of VI and FAE of the COVID-19 vaccine and its associated factors in LAC. This information is critical for designing targeted strategies and policies to increase the VI against COVID-19 in the region.
2. Methods
2.1. Study design and data sources
We conducted a secondary analysis of a database collected by the University of Maryland and the social network Facebook® (Facebook, Inc), based on a survey designed to evaluate the respondents' features in the context of the COVID-19 pandemic. The survey includes demographic information, contact report, self-report of COVID-19 symptoms, assessment of food and economic security, mental health and a module on vaccination attitudes. The survey was conducted for the first time on April 23, 2020, and is conducted daily in more than 200 countries or territories translated into each country's primary language.
2.2. Population and sample
The surveyed population included participants aged 18 and over who were Facebook® users. For the analysis, we included the LAC participants who answered the survey from January 15 to February 1, 2021, reaching a total number of 784,460 adults. We excluded those participants who did not have the variables of interest for this analysis, for which we analyzed 472,521 adults from 20 LAC countries.
3. Variables
3.1. Outcomes
3.1.1. Vaccination intention
We evaluated the VI using the following question: If a vaccine to prevent COVID-19 were offered to you today, would you choose to get vaccinated? This question had four possible answers: yes, definitely; yes, probably; no, probably and no, definitely. We dichotomized the variable considering the last two alternatives to the non-VI for COVID-19 and the first two alternatives as to the VI.
3.1.2. Fear of adverse effects of vaccination
Besides, we evaluated the FAE of vaccination using the following question: How concerned are you that you would experience a side effect from a COVID-19 vaccination? This question had four possible answers: very concerned, moderately concerned, slightly concerned and not at all concerned. We dichotomized the variable considering the first four alternatives regarding the presence of FAE and the last alternative as the absence.
3.2. Independent variables
3.2.1. Sociodemographic characteristics
We included gender (male, female, non-binary), age (18–24, 25–34, 35–44, 45–54, 55–64, 65–74, 75 or more years) and the residential area of the participant (city, town, rural area).
3.2.2. COVID-19 symptoms and compliance with community mitigation strategies
We evaluated the presence of suspicious COVID-19 symptoms, defined as three or more of the following symptoms in the last 24 h: fever, cough, difficulty breathing, fatigue, nasal discharge, muscle pain, sore throat, chest pain, nausea, loss of smell, eye pain, and headache.
We included compliance with the three main community mitigation strategies: hand washing, use of a mask, and physical distancing. We defined the compliance with physical distancing when the participant reported not having been in direct contact (including touching, shaking hands, hugging, kissing) for no more than 1 min in the last 24 h and not having been within 2 m of any person with whom you are not currently living. We considered handwashing compliance when participants reported having washed their hands at least once in the last 24 h. Besides, we considered a mask using compliance when participants reported wearing it in public (at least once) during the last seven days. We created a variable considering compliance with the three community mitigation strategies.
3.2.3. Food and economic insecurity
Food security was assessed by the following question: How worried are you about having enough to eat in the next week? This question had four possible answers: very worried, somewhat worried, not very worried, and not worried at all. The variable was dichotomized, considering the first three alternatives as food insecurity.
Financial security was assessed by the following question: How worried are you about your household's finances in the next month? This question had four alternatives: very worried, somewhat worried, not very worried, and not worried at all. The variable was dichotomized, considering the first three responses as economic insecurity.
3.2.4. Mental health evaluation
We evaluated the presence of depressive symptoms using the following question adapted from the Kessler Psychological Distress Scale (K10): In the past seven days, how often did you feel so depressed that nothing could cheer you up? This question had five possible answers: all the time, most of the time, some of the time, a little of the time and none of the time [16]. We generated a dichotomous variable considering the last alternative as the absence of depressive symptoms and the first four alternatives regarding the presence of depressive symptoms.
We included evaluating anxiety symptoms, measured by the following question adapted from the Kessler Psychological Distress Scale (K10): During the last seven days, how often did you feel so nervous that nothing could calm you down? This question had five alternatives: all the time, most of the time, some of the time, a little of the time and none of the time [16]. We generated a dichotomous variable considering the last alternative as the absence of anxiety symptoms and the other four alternatives to the presence of anxiety symptoms.
Likewise, we evaluated the participant's fear to become seriously ill or his fear that a family member would become seriously ill from COVID-19, which was evaluated using the following question: How worried are you that you or someone in your immediate family might become seriously ill from coronavirus (COVID-19)? The question had the following possible answers: very worried, somewhat worried, not too worried and not worried at all. We created a dichotomous variable considering the last alternative as the absence of fear of the participant or a family member would become seriously ill from COVID-19 and the remaining three as the presence of fear.
3.2.5. Probability of vaccination acceptance when recommended by different stakeholders
We assessed the influence that friends and family, local health workers, the World Health Organization (WHO), government health officials, and politicians could have on the participants VI. That was evaluated using the following question: would you be more or less likely to get a COVID-19 vaccination if it were recommended to you by each of the following. These questions had three answers: more likely, about the same and less likely. We considered the last two alternatives as to the lack of influence for the VI and the first alternative to influence the VI.
3.3. Statistical analysis
We downloaded the Microsoft Excel® 2010 format database and imported it into the statistical package STATA® v14.0 (StataCorp, TX, USA). We carried out the statistical analyses considering the complex sampling of the survey using the svy command.
We described the qualitative variables using absolute frequencies and weighted proportions according to the survey's complex sampling with their respective 95% confidence intervals (95%CI). Likewise, we performed the bivariate analysis between the covariates of interest and the outcome variables, using Pearson's Chi-square test with Rao-Scott correction. Also, we performed generalized linear models from the Poisson family with a logarithmic link function to evaluate the factors associated with VI and FAE. We calculated crude (cPR) and adjusted (aPR) prevalence ratios with their 95%CI. We used a statistical criterion (p < 0.05) to select the variables for the adjusted model. Also, we evaluated the possible collinearity between the covariates included in the final model.
3.4. Ethical considerations
The participants gave informed consent before starting the survey. The study is exempt from an institutional review board ethical approval since it used secondary data, and the database does not contain any sensitive data or personal identifiers. Hence, the integrity of the participants was not compromised. We obtained the data by signing a research data use agreement with the University of Maryland. The data was downloaded without identifiers. The participants gave their informed consent before starting the survey.
4. Results
4.1. Characteristics of the study sample
We analyzed a sample of 472,521 LAC adults from January 15 to February 1, 2021. We found that 49.6% (n = 205,569) were male, 65.9% (n = 331,835) were under 45 years of age and 79.4% (n = 390,122) lived in a city. Likewise, 22.3% (n = 110,075) had suspicious symptoms of COVID-19, while 49.8% (n = 236,617) complied with the community mitigation strategies, 71.2% (n = 328,732) had food insecurity and 85.3% (n = 401,377) had economic insecurity. 95.1% (n = 453,513) reported fear to get seriously ill or that a member of their family would be seriously ill from COVID-19, as well as 43.9% (n = 219,796) had anxiety symptoms. 41.6% (n = 198,556) and 60.3% (n = 298,914) reported that the recommendation by family and friends, as well as local doctors could influence their VI, respectively. We found that 80.0% (n = 391,597) reported VI and 81.2% (n = 382,507) had FAE (Table 1 ).
Table 1.
Descriptive analysis of the study sample (n = 472,521).
| Total |
|||
|---|---|---|---|
| Characteristics |
Absolute frequency of participants surveyed |
Weighted proportion according to each category |
|
| n | % | 95%CI | |
| Gender | |||
| Male | 205,569 | 49.6 | 49.0–50.1 |
| Female | 263,026 | 49.4 | 48.9–50.0 |
| Non-binary | 3926 | 1.0 | 0.9–1.1 |
| Age (years) | |||
| 18–24 | 86,687 | 19.5 | 18.6–20.3 |
| 25–34 | 134,279 | 25.9 | 25.2–26.5 |
| 35–44 | 110,869 | 20.5 | 20.2–20.9 |
| 45–54 | 76,091 | 17.6 | 17.2–17.9 |
| 55–64 | 46,323 | 9.8 | 9.3–10.4 |
| 65–74 | 15,592 | 5.9 | 5.4–6.5 |
| 75 years or older | 2680 | 0.9 | 0.8–1.0 |
| Living area | |||
| City | 390,122 | 79.4 | 75.8–82.6 |
| Town | 53,353 | 13.2 | 10.7–16.2 |
| Village or rural area | 29,046 | 7.4 | 6.5–8.4 |
| COVID-19 symptomatology | |||
| No | 362,446 | 77.7 | 76.6–78.8 |
| Yes | 110,075 | 22.3 | 21.2–23.4 |
| Compliance with community mitigation strategies | |||
| No | 235,904 | 50.2 | 49.1–51.4 |
| Yes | 236,617 | 49.8 | 48.6–50.9 |
| Food insecurity | |||
| No | 143,789 | 28.8 | 27.1–30.5 |
| Yes | 328,732 | 71.2 | 69.5–72.9 |
| Economic insecurity | |||
| No | 71,144 | 14.7 | 14.1–15.4 |
| Yes | 401,377 | 85.3 | 84.6–85.9 |
| Fear of becoming seriously ill or that a family member becomes seriously ill from COVID-19 | |||
| No | 19,008 | 4.9 | 4,1–6,0 |
| Yes | 453,513 | 95.1 | 94.7–95.5 |
| Anxiety symptomatology | |||
| No | 252,725 | 56.1 | 55.2–57.1 |
| Yes | 219,796 | 43.9 | 42.9–44.8 |
| Depressive symptomatology | |||
| No | 238,497 | 52.7 | 51.8–53.6 |
| Yes | 234,024 | 47.3 | 46.4–48.2 |
| Probability of vaccination acceptance when recommended by friends and family | |||
| Less likely/about the same | 273,965 | 58.4 | 57.2–59.6 |
| More likely | 198,556 | 41.6 | 40.4–42.8 |
| Probability of vaccination acceptance when recommended by local health workers | |||
| Less likely/about the same | 173,607 | 39.7 | 37.2–42.3 |
| More likely | 298,914 | 60.3 | 57.7–62.8 |
| Probability of vaccination acceptance when recommended by the WHO | |||
| Less likely/about the same | 150,856 | 34.4 | 31.9–36.9 |
| More likely | 321,665 | 65.6 | 63.1–68.1 |
| Probability of vaccination acceptance when recommended by government health officials | |||
| Less likely/about the same | 234,300 | 51.4 | 49.5–53.2 |
| More likely | 238,221 | 48.6 | 46.8–50.5 |
| Probability of vaccination acceptance when recommended by politicians | |||
| Less likely/about the same | 423,381 | 89.8 | 89.3–90.3 |
| More likely | 49,140 | 10.2 | 9.7–10.7 |
| Vaccination intention | |||
| No | 80,924 | 20.0 | 18.4–21.7 |
| Yes | 391,597 | 80.0 | 78.3–81.6 |
| Fear of adverse effects of vaccination | |||
| No | 90,014 | 18.9 | 15.8–22.2 |
| Yes | 382,507 | 81.2 | 77.8–84.2 |
95%CI: 95% confidence intervals; WHO: World Health Organization.
4.2. Bivariate analysis according to vaccination intention and fear of adverse effects of the vaccine
We found statistically significant differences between the VI and the included covariates, except for food insecurity (p = 0.554) (Table 2 ). Likewise, we found statistically significant differences between FAE and the independent variables included, except for compliance with community mitigation strategies (p = 0.530) (Table 3 ). The bivariate analysis, according to the outcomes, is described in Table 2, Table 3
Table 2.
Descriptive and bivariate analysis of the study sample characteristics according to vaccination intention (n = 472,521).
| Vaccination intention |
|||||||
|---|---|---|---|---|---|---|---|
| No |
Yes |
||||||
| Characteristics | Absolute frequency of participants surveyed | Weighted proportion according to each category | Absolute frequency of participants surveyed | Weighted proportion according to each category | P-value | ||
| n | % | 95%CI | n | % | 95%CI | ||
| Gender | <0.001 | ||||||
| Male | 33,117 | 19.1 | 17.8–20.4 | 172,452 | 80.9 | 79.6–82.2 | |
| Female | 46,758 | 20.7 | 18.6–23.0 | 216,268 | 79.2 | 77.0–81.4 | |
| Non-binary | 1049 | 29.8 | 26.9–31.8 | 2877 | 70.2 | 67.2–73.1 | |
| Age (years) | 0.004 | ||||||
| 18–24 | 14,068 | 20.1 | 18.1–22.3 | 72,619 | 79.9 | 77.7–81.9 | |
| 25–34 | 22,560 | 20.7 | 18.9–22.7 | 111,719 | 79.3 | 77.3–81.1 | |
| 35–44 | 19,145 | 19.9 | 18.5–21.4 | 91,724 | 80.1 | 78.6–81.5 | |
| 45–54 | 13,525 | 19.7 | 18.0–21.4 | 62,566 | 80.3 | 78.6–82.0 | |
| 55–64 | 8274 | 19.0 | 17.7–20.4 | 38,049 | 81.0 | 79.6–82.3 | |
| 65–74 | 2783 | 18.8 | 17.3–20.5 | 12,809 | 81.2 | 79.5–82.7 | |
| 75 years or older | 569 | 22.3 | 20.0–24.8 | 2111 | 77.7 | 75.2–80.0 | |
| Living area | <0.001 | ||||||
| City | 64,081 | 19.0 | 17.5–20.7 | 326,041 | 81.0 | 79.3–82.5 | |
| Town | 10,260 | 22.5 | 20.2–25.0 | 43,093 | 77.5 | 75.0–79.8 | |
| Village or rural area | 6583 | 25.8 | 24.2–27.6 | 22,463 | 74.2 | 72.4–75.8 | |
| COVID-19 symptomatology | <0.001 | ||||||
| No | 62,748 | 20.3 | 18.7–21.9 | 299,698 | 79.7 | 78.1–81.3 | |
| Yes | 18,176 | 19.1 | 17.4–20.8 | 91,899 | 80.9 | 79.2–82.6 | |
| Compliance with community mitigation strategies | 0.005 | ||||||
| No | 39,073 | 19.6 | 17.8–21.4 | 196,831 | 80.4 | 78.6–82.2 | |
| Yes | 41,851 | 20.4 | 18.9–22.0 | 194,766 | 79.6 | 78.0–81.1 | |
| Food insecurity | 0.554 | ||||||
| No | 23,755 | 19.8 | 17.9–21.8 | 120,034 | 80.2 | 78.2–82.1 | |
| Yes | 57,169 | 20.1 | 18.5–21.7 | 271,563 | 79.9 | 78.3–81.5 | |
| Economic insecurity | <0.001 | ||||||
| No | 12,652 | 21.5 | 19.7–23.5 | 58,492 | 78.5 | 76.5–80.3 | |
| Yes | 68,272 | 19.7 | 18.2–21.4 | 333,105 | 80.3 | 78.6–81.8 | |
| Fear of becoming seriously ill or that a family member becomes seriously ill from COVID-19 | <0.001 | ||||||
| No | 7942 | 44.7 | 42.9–46.5 | 11,066 | 55.3 | 53.5–57.1 | |
| Yes | 72,982 | 18.7 | 17.2–20.4 | 380,531 | 81.3 | 79.6–82.8 | |
| Anxiety symptomatology | <0.001 | ||||||
| No | 49,705 | 22.4 | 20.8–24.1 | 203,020 | 77.6 | 75.9–79.2 | |
| Yes | 31,219 | 16.9 | 15.3–18.6 | 188,577 | 83.1 | 81.4–84.7 | |
| Depressive symptomatology | <0.001 | ||||||
| No | 45,844 | 22.0 | 20.5–23.5 | 192,653 | 78.0 | 76.5–79.5 | |
| Yes | 35,080 | 17.8 | 16.1–19.7 | 198,944 | 82.2 | 80.3–83.9 | |
| Probability of vaccination acceptance when recommended by friends and family | <0.001 | ||||||
| Less likely/about the same | 65,346 | 27.6 | 25.5–29.9 | 208,619 | 72.4 | 70.1–74.5 | |
| More likely | 15,578 | 9.2 | 8.4–10.1 | 182,978 | 90.8 | 89.9–91.6 | |
| Probability of vaccination acceptance when recommended by local health workers | <0.001 | ||||||
| Less likely/about the same | 66,128 | 41.4 | 39.6–43.3 | 107,479 | 58.6 | 56.7–60.4 | |
| More likely | 14,796 | 5.8 | 5.3–6.5 | 284,118 | 94.2 | 93.5–94.7 | |
| Probability of vaccination acceptance when recommended by the WHO | <0.001 | ||||||
| Less likely/about the same | 63,448 | 45.6 | 44.3–47.0 | 87,408 | 54.4 | 53.0–55.7 | |
| More likely | 17,476 | 6.6 | 5.9–7.3 | 304,189 | 93.4 | 92.7–94.1 | |
| Probability of vaccination acceptance when recommended by government health officials | <0.001 | ||||||
| Less likely/about the same | 72,026 | 34.5 | 32.6–36.4 | 162,274 | 65.5 | 63.6–67.4 | |
| More likely | 8898 | 4.7 | 4.2–5.2 | 229,323 | 95.3 | 94.8–95.8 | |
| Probability of vaccination acceptance when recommended by politicians | <0.001 | ||||||
| Less likely/about the same | 78,518 | 21.5 | 19.8–23.3 | 344,863 | 78.5 | 76.7–80.2 | |
| More likely | 2406 | 6.6 | 5.7–7.7 | 46,734 | 93.4 | 92.3–94.3 | |
95%CI: 95% confidence intervals, WHO: World Health Organization.
Table 3.
Descriptive and bivariate analysis of the study sample characteristics according to the fear of vaccination's adverse effects (n = 472,521).
| Fear of adverse effects of vaccination |
|||||||
|---|---|---|---|---|---|---|---|
| No |
Yes |
||||||
| Characteristics | Absolute frequency of participants surveyed | Weighted proportion according to each category | Absolute frequency of participants surveyed | Weighted proportion according to each category | P-value | ||
| n | % | 95%CI | n | % | 95%CI | ||
| Gender | <0.001 | ||||||
| Male | 45,310 | 21.9 | 18.9–25.2 | 160,259 | 78.1 | 74.8–81.1 | |
| Female | 44,083 | 15.6 | 12.6–19.3 | 218,943 | 84.4 | 80.7–87.4 | |
| Non-binary | 621 | 16.7 | 13.8–20.1 | 3305 | 83.3 | 79.9–86.2 | |
| Age (years) | <0.001 | ||||||
| 18–24 | 15,320 | 16.9 | 14.3–19.8 | 71,367 | 83.1 | 80.2–85.7 | |
| 25–34 | 23,231 | 16.1 | 13.5–19.2 | 111,048 | 89.9 | 80.8–86.5 | |
| 35–44 | 21,131 | 18.3 | 15.3–21.8 | 89,738 | 81.7 | 78.2–84.5 | |
| 45–54 | 15,388 | 20.0 | 16.8–23.7 | 60,703 | 80.0 | 76.3–83.2 | |
| 55–64 | 10,632 | 23.3 | 19.5–27.6 | 35,691 | 76.7 | 72.4–80.5 | |
| 65–74 | 3667 | 25.6 | 22.1–29.5 | 11,925 | 74.4 | 70.5–77.9 | |
| 75 years or older | 645 | 24.5 | 20.8–28.6 | 2035 | 75.5 | 71.4–79.2 | |
| Living area | <0.001 | ||||||
| City | 78,884 | 20.1 | 16.8–23.9 | 311,238 | 78.9 | 76.1–83.2 | |
| Town | 6668 | 12.2 | 11.4–13.0 | 46,685 | 87.8 | 87.0–88.6 | |
| Village or rural area | 4462 | 15.8 | 14.3–17.6 | 24,584 | 84.2 | 82.4–85.7 | |
| COVID-19 symptomatology | <0.001 | ||||||
| No | 72,735 | 19.7 | 16.6–23.3 | 289,711 | 80.3 | 76.7–83.4 | |
| Yes | 17,279 | 15.5 | 13.0–18.3 | 92,796 | 84.5 | 81.7–87.0 | |
| Compliance with community mitigation strategies | 0.530 | ||||||
| No | 44,971 | 18.8 | 15.7–22.4 | 190,933 | 81.2 | 77.6–84.3 | |
| Yes | 45,043 | 18.7 | 15.8–22.0 | 191,574 | 81.3 | 78.0–84.2 | |
| Food insecurity | <0.001 | ||||||
| No | 41,840 | 29.4 | 25.4–33.7 | 101,949 | 70.6 | 66.3–74.6 | |
| Yes | 48,174 | 14.5 | 12.1–17.2 | 280,558 | 85.5 | 82.8–87.9 | |
| Economic insecurity | <0.001 | ||||||
| No | 22,045 | 31.5 | 27.7–35.5 | 49,099 | 68.5 | 64.5–72.3 | |
| Yes | 67,969 | 16.6 | 13.8–19.8 | 333,408 | 83.4 | 80.2–86.2 | |
| Fear of becoming seriously ill or that a family member becomes seriously ill from COVID-19 | <0.001 | ||||||
| No | 6375 | 33.9 | 32.1–35.6 | 12,633 | 66.1 | 64.4–67.9 | |
| Yes | 83,639 | 18.0 | 14.9–21.6 | 369,874 | 82.0 | 78.4–85.1 | |
| Anxiety symptomatology | <0.001 | ||||||
| No | 52,593 | 20.7 | 17.8–23.9 | 200,132 | 79.3 | 76.1–82.2 | |
| Yes | 37,421 | 16.3 | 13.1–20.0 | 182,375 | 83.7 | 80.0–86.9 | |
| Depressive symptomatology | <0.001 | ||||||
| No | 49,055 | 20.6 | 17.7–23.7 | 189,442 | 79.4 | 76.3–82.3 | |
| Yes | 40,959 | 16.7 | 13.5–20.5 | 193,065 | 83.3 | 79.5–86.5 | |
| Probability of vaccination acceptance when recommended by friends and family | <0.001 | ||||||
| Less likely/about the same | 49,925 | 17.6 | 14.8–20.9 | 224,040 | 82.4 | 79.1–85.2 | |
| More likely | 40,089 | 20.3 | 17.1–24.0 | 158,467 | 79.7 | 76.0–82.9 | |
| Probability of vaccination acceptance when recommended by local health workers | <0.001 | ||||||
| Less likely/about the same | 19,756 | 11.3 | 10.4–12.7 | 153,851 | 88.7 | 87.3–89.9 | |
| More likely | 70,258 | 23.6 | 19.8–27.9 | 228,656 | 76.4 | 72.1–80.2 | |
| Probability of vaccination acceptance when recommended by the WHO | <0.001 | ||||||
| Less likely/about the same | 16,221 | 10.9 | 10.1–11.7 | 134,635 | 89.1 | 88.3–89.9 | |
| More likely | 73,793 | 22.9 | 19.0–27.3 | 247,872 | 77.1 | 72.7–81.0 | |
| Probability of vaccination acceptance when recommended by government health officials | <0.001 | ||||||
| Less likely/about the same | 32,012 | 13.4 | 11.3–15.8 | 202,288 | 86.6 | 84.2–88.7 | |
| More likely | 58,002 | 24.4 | 20.7–28.6 | 180,219 | 75.6 | 71.4–79.3 | |
| Probability of vaccination acceptance when recommended by politicians | <0.001 | ||||||
| Less likely/about the same | 74,713 | 17.4 | 14.5–20.7 | 348,668 | 82.6 | 79.3–85.5 | |
| More likely | 15,301 | 31.0 | 27.3–35.0 | 33,839 | 69.0 | 65.0–72.7 | |
95%CI: 95% confidence intervals; WHO: World Health Organization.
4.3. Prevalence of vaccination intention by country
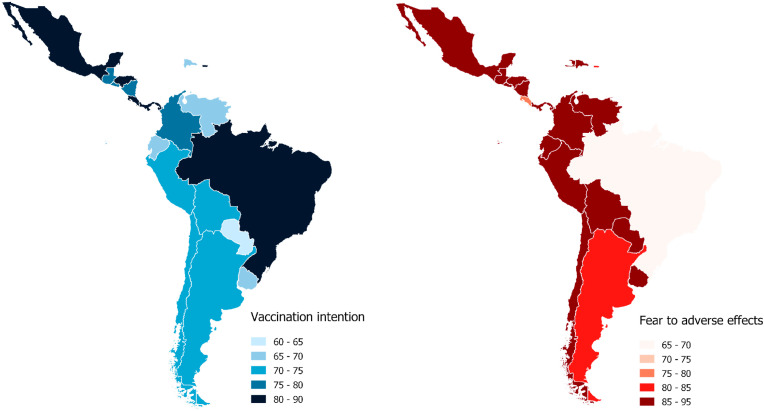
The countries with the highest prevalence of VI were Mexico (88.4%), Puerto Rico U.S. (85.0%), Costa Rica (84.1%), Brazil (83.1%) and Honduras (80.5%). On the other hand, those with the lowest prevalence of VI were Haiti (43.2%), Paraguay (64.6%), Dominican Republic (65.8%), Uruguay (65.9%) and Venezuela (68.8%) (Fig. 1 ).
Fig. 1.
Prevalence of vaccination intention and fear of adverse effects of the vaccine according to Latin American and the Caribbean.
4.4. Prevalence of fear to adverse effects of the vaccine according to countries
We found that the countries with the highest prevalence of FAE were Venezuela (92.7%), Bolivia (91.3%), Ecuador (90.9%), Peru (90.5%) and the Dominican Republic (90.3%). On the other hand, those with the lower frequency of FAE were Brazil (68.2%), Costa Rica (79.8%), Puerto Rico, U.S. (80.8%), Argentina (84.5%) and Paraguay (84.5%) (Fig. 1).
4.5. Probability of vaccination intention when recommended by different stakeholders
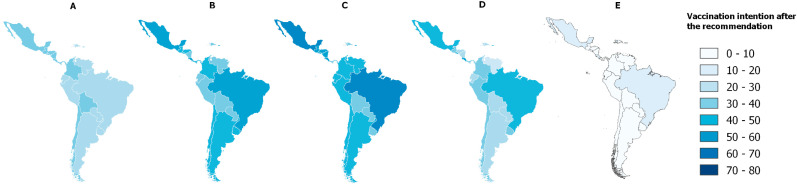
The countries with the highest prevalence of VI based on the recommendation of friends and family were Mexico (49.1%), Puerto Rico (47.1%) and Nicaragua (47.0%). Also, the countries with the highest prevalence of VI based on the recommendation of local health workers were Brazil (69.1%), Costa Rica (66.9%) and Puerto Rico (66.1%). The countries with the highest prevalence of VI based on the recommendation by the WHO were Brazil (73.8%), Mexico (73.6%) and Costa Rica (66.9%) and Puerto Rico (66.4%). Furthermore, the countries with the highest prevalence of VI based on the recommendation by the government health officials were Costa Rica (62.0%), Mexico (56.0%) and Puerto Rico (54.5%). Finally, the countries with the highest prevalence of VI based on the recommendation by politicians were Puerto Rico (17.7%), Haiti (16.4%) and Costa Rica (13.2%) (Fig. 2 and supplementary material).
Fig. 2.
Prevalence of the vaccination intention after the recommendation by: (A). Friends and family; (B). Local health workers; (C). The World Health Organization; (D). Government health officials; (E). Politicians.
4.6. Factors associated with the vaccination intention
In the adjusted regression model, we found that female gender (aRP = 0.97; 95%CI: 0.95–0.97; p < 0.001) and non-binary gender (aRP = 0.93; 95%CI: 0.90.0.95; p < 0.001), compared to males, were associated with a lower prevalence of VI. Likewise, living in a village or rural area (aRP = 0.96; 95%CI: 0.95–0.97; p < 0.001) was associated with a lower probability of VI when compared to a city. Also, compliance with community mitigation strategies (aRP = 0.99; 95%CI: 0.98–0.99; p = 0.008) was associated with a lower prevalence of VI. Likewise, being afraid of getting seriously ill or being afraid that a family member would get seriously sick from COVID-19 (aRP = 1.28; 95%CI: 1.26–1.30; p < 0.001) and displaying depressive symptoms (aRP = 1.03; 95%CI: 1.03–1.04; p < 0.001), were all associated with a higher prevalence of VI. We found that the recommendations of family and friends (aRP = 1.08; 95%CI: 1.07–1.09; p < 0.001), local doctors (aRP = 1.29; 95%CI: 1.26–1.31; p < 0.001), WHO (aRP = 1.44; 95%CI: 1.41–1.47; p < 0.001) and government health officials (aRP = 1.10; 95%CI: 1.09–1.11; p < 0.001) were associated with a higher probability of VI, while the recommendations by politicians (aRP = 0.93; 95%CI: 0.92–0.94; p < 0.001), was associated with a lower probability of VI (Table 4 ).
Table 4.
Crude and adjusted generalized linear models of the Poisson family with a logarithmic link to evaluate the factors associated with vaccination intention and the fear of adverse effects of vaccination in the study sample.
| Vaccination intention |
Fear of adverse effects of vaccination |
|||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Crude |
Adjusted |
Crude |
Adjusted |
|||||||||
| Characteristics | cPR | 95%CI | P value | aPR | 95%CI | P value | cPR | 95%CI | P value | aPR | 95%CI | P value |
| Gender | ||||||||||||
| Male | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| Female | 0.98 | 0.96–0.99 | 0.026 | 0.97 | 0.95–0.97 | <0.001 | 1.08 | 1.07–1.09 | <0.001 | 1.07 | 1.06–1.07 | <0.001 |
| Non-binary | 0.87 | 0.84–0.90 | <0.001 | 0.93 | 0.90–0.95 | <0.001 | 1.07 | 1.03–1.10 | <0.001 | 1.04 | 1.01–1.06 | 0.001 |
| Age (years) | ||||||||||||
| 18–24 | Reference | – | – | Reference | – | – | Reference | – | – | |||
| 25–34 | 0.99 | 0.98–1.00 | 0.059 | 1.00 | 1.00–1.02 | 0.002 | 1.01 | 1.01–1.02 | <0.001 | |||
| 35–44 | 1.00 | 0.99–1.01 | 0.622 | 0.98 | 0.97–0.99 | 0.001 | 1.00 | 0.99–1.01 | 0.707 | |||
| 45–54 | 1.01 | 0.99–1.02 | 0.394 | Not includeda | 0.96 | 0.95–0.98 | <0.001 | 0.99 | 0.98–0.99 | 0.029 | ||
| 55–64 | 1.01 | 1.00–1.03 | 0.075 | 0.92 | 0.90–0.94 | <0.001 | 0.96 | 0.95–0.98 | 0.001 | |||
| 65–74 | 1.02 | 1.00–1.04 | 0.088 | 0.89 | 0.87–0.92 | <0.001 | 0.95 | 0.93–0.97 | <0.001 | |||
| 75 years or older | 0.97 | 0.94–1.00 | 0.059 | 0.91 | 0.88–0.94 | <0.001 | 0.97 | 0.94–1.00 | 0.077 | |||
| Living area | ||||||||||||
| City | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| Town | 0.96 | 0.93–0.98 | 0.001 | 1.00 | 0.98–1.01 | 0.659 | 1.10 | 1.06–1.14 | <0.001 | 1.08 | 1.05–1.11 | <0.001 |
| Village or rural area | 0.92 | 0.90–0.93 | <0.001 | 0.96 | 0.95–0.97 | <0.001 | 1.05 | 1.02–1.09 | 0.001 | 1.04 | 1.02–1.06 | <0.001 |
| COVID-19 symptomatology | ||||||||||||
| No | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| Yes | 1.02 | 1.01–1.02 | <0.001 | 1.00 | 1.00–1.01 | 0.148 | 1.05 | 1.04–1.07 | <0.001 | 1.02 | 1.01–1.03 | <0.001 |
| Compliance with community mitigation strategies | ||||||||||||
| No | Reference | – | – | Reference | Reference | – | – | Not includeda | ||||
| Yes | 0.99 | 0.98–0.99 | 0.003 | 0.99 | 0.98–0.99 | 0.008 | 1.00 | 1.00–1.01 | 0.541 | |||
| Food insecurity | ||||||||||||
| No | Reference | – | – | Not includeda | Reference | – | – | Not includedb | ||||
| Yes | 1.00 | 0.98–1.01 | 0.549 | 1.21 | 1.17–1.25 | <0.001 | ||||||
| Economic insecurity | ||||||||||||
| No | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| Yes | 1.02 | 1.01–1.03 | <0.001 | 0.99 | 0.99–1.00 | 0.072 | 1.22 | 1.19–1.25 | <0.001 | 1.16 | 1.14–1.19 | <0.001 |
| Fear of becoming seriously ill or that a family member becomes seriously ill from COVID-19 | ||||||||||||
| No | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| Yes | 1.47 | 1.43–1.51 | <0.001 | 1.28 | 1.26–1.30 | <0.001 | 1.24 | 1.21–1.27 | <0.001 | 1.21 | 1.19–1.23 | <0.001 |
| Anxiety symptomatology | ||||||||||||
| No | Reference | – | – | Not includedc | Reference | – | – | Not includedc | ||||
| Yes | 1.07 | 1.06–1.08 | <0.001 | 1.06 | 1.05–1.06 | <0.001 | ||||||
| Depressive symptomatology | ||||||||||||
| No | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| Yes | 1.05 | 1.05–1.06 | <0.001 | 1.03 | 1.03–1.04 | <0.001 | 1.05 | 1.04–1.06 | <0.001 | 1.01 | 1.01–1.02 | 0.018 |
| Probability of vaccination acceptance when recommended by friends and family | ||||||||||||
| Less likely/about the same | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| More likely | 1.25 | 1.23–1.28 | <0.001 | 1.08 | 1.07–1.09 | <0.001 | 0.98 | 0.96–0.98 | <0.001 | 1.04 | 1.03–1.05 | <0.001 |
| Probability of vaccination acceptance when recommended by local health workers | ||||||||||||
| Less likely/about the same | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| More likely | 1.61 | 1.57–1.65 | <0.001 | 1.29 | 1.26–1.31 | <0.001 | 0.86 | 0.83–0.90 | <0.001 | 0.92 | 0.90–0.94 | <0.001 |
| Probability of vaccination acceptance when recommended by the WHO | ||||||||||||
| Less likely/about the same | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| More likely | 1.72 | 1.68–1.76 | <0.001 | 1.44 | 1.41–1.47 | <0.001 | 0.87 | 0.83–0.91 | <0.001 | 0.91 | 0.88–0.95 | <0.001 |
| Probability of vaccination acceptance when recommended by government health officials | ||||||||||||
| Less likely/about the same | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| More likely | 1.46 | 1.42–1.49 | <0.001 | 1.10 | 1.09–1.11 | <0.001 | 0.87 | 0.85–0.90 | <0.001 | 0.96 | 0.95–0.97 | <0.001 |
| Probability of vaccination acceptance when recommended by politicians | ||||||||||||
| Less likely/about the same | Reference | – | – | Reference | – | – | Reference | – | – | Reference | – | – |
| More likely | 1.19 | 1.17–1.21 | <0.001 | 0.93 | 0.92–0.94 | <0.001 | 0.83 | 0.82–0.85 | <0.001 | 0.90 | 0.89–0.91 | <0.001 |
95%CI: 95% confidence intervals; cPR: Crude prevalence ratio; aPR: Adjusted prevalence ratio; WHO: World Health Organization.
Not included due to not having a statistically significant association in the crude model.
Not included due to collinearity with economic insecurity.
Not included due to collinearity with the fear of becoming ill or that a family member could become seriously ill from COVID-19.
4.7. Factors associated with fear of adverse effects of the vaccine in the study sample
In the adjusted regression model, we found that female gender (aRP = 1.07; 95%CI: 1.06–1.07; p < 0.001) and non-binary gender (aRP = 1.04; 95%CI: 1.01–1.06; p = 0.001), compared to the male gender, were associated with a higher prevalence of FAE. Likewise, living in a town (aRP = 1.08; 95%CI: 1.05–1.11; p < 0.001), village or rural area (aRP = 1.04; 95%CI: 1.02–1.06; p < 0.001), compared to a city, was associated with a greater frequency of FAE. In addition, economic insecurity (aRP = 1.16; 95%CI: 1.14–1.19; p < 0.001), fear of getting seriously ill or that a family member gets seriously sick from COVID-19 (aRP = 1.21; 95%CI: 1.19–1.23; p < 0.001), having suspicious symptoms of COVID-19 (aRP = 1.02; 95%CI: 1.01–1.03; p < 0.001) and having depressive symptoms (aRP = 1.01; 95%CI: 1.01–1.02; p = 0.018), were associated with a higher prevalence of FAE.
On the other hand, being between 25 and 34 years old (aRP = 1.01; 95%CI: 1.01–1.02; p < 0.001) compared to those aged 18–24 years, was associated with a greater probability of FAE. Likewise, 45–54 (aRP = 0.99; 95%CI: 0.98–0.99; p = 0.029), 55–64 (aRP = 0.96; 95%CI: 0.95–0.98; p = 0.001), 65–74 (aRP = 0.95; 95%CI: 0.93–0.97; p < 0.001), compared to those aged 18–24 years, was associated with a lower frequency of FAE. We found that recommendations from family and friends (aRP = 1.04; 95%CI: 1.03–1.05; p < 0.001) were associated with a higher prevalence of FAE, while recommendations by local doctors (aRP = 0.92; 95%CI: 0.90–0.94; p < 0.001), WHO (aRP = 0.91; 95%CI: 0.88–0.95; p < 0.001), government health officials (aRP = 0.96; 95%CI: 0.95–0.97; p < 0.001) and politicians (aRP = 0.90; 95%CI: 0.89–0.91; p < 0.001), was associated with a lower probability of FAE (Table 4).
According to the countries included, the proportion of vaccination intention and fear to adverse effects of vaccination is available in the Supplementary Table S1. According to the countries included, the proportion of influence on the vaccination intention is described in Table S2.
5. Discussion
5.1. Main findings
This work aimed to evaluate the prevalence and factors associated with VI and FAE. The findings show that approximately eight out of ten participants had VI; however, there was a similar FAE frequency. Furthermore, we found that female and non-binary participants had a lower probability of VI. On the other hand, the fear of becoming seriously ill or that a family member becomes seriously ill from COVID-19, having depressive symptoms, and the recommendations from family and friends, local health workers, WHO and government health officials were associated with a higher prevalence of VI. However, recommendations from politicians were associated with a lower probability of VI.
Besides, we found that female or non-binary gender living in a town, village or rural area was associated with a higher FAE prevalence. On the other hand, being over 35 years of age was associated with a lower probability of FAE and, in contrast, economic insecurity, fear of becoming seriously ill, or a family member becoming seriously ill from COVID-19 and depressive symptoms with a greater probability of FAE. Finally, friends and family's recommendations were associated with a higher probability of FAE. In contrast, recommendations by local health workers, WHO, government health officials, and politicians were associated with a lower frequency of FAE. The current study is one of the first aiming to evaluate the VI in the LAC region; the findings can help identify higher-risk groups to design targeted strategies to increase VI and reduce FAE.
5.2. Comparison with previous studies
To date, most studies have been conducted in North America [[17], [18], [19], [20]], Europe [11,21,22], Asia [23,24] and Australia [25]. In general terms, our results show a higher prevalence of VI in the LAC region compared to its peers. However, some studies have found that almost 84% of Chinese adults were willing to receive a COVID-19 vaccine [23]. This prevalence is higher than the reported in our study for Brazil and Honduras, which were in our top five countries with the highest VI. Regarding the associated factors, our study shows that women were less likely to accept a COVID19 vaccine as in Europe [11,22], Australia [25], and the US [17]. Similarly, fear or perceived severity of COVID-19 [18,19] and healthcare providers' recommendations also increased the probability of VI in some studies conducted in US adults [19].
On the other hand, even though the fear of adverse effects has been described as an essential barrier to vaccination for COVID-19 [26], we found few studies assessing this topic [27,28]. Although associated factors were not evaluated, it has been reported that fear of adverse effects was the leading cause for rejecting the COVID-19 vaccine. Similar conclusions were reported during and after outbreaks of vaccine-preventable diseases [[29], [30], [31]]. Recently in another cross-sectional study in Colombia, assessing perceptions of COVID-19 vaccination among physicians found that around 91% of them are willing to get vaccinated [32].
5.3. Interpretation of the results
We found that female and non-binary genders, compared to males, were associated with a lower probability of VI and a higher probability of FAE. This finding goes in line with previous studies [10,18,[33], [34], [35]], where males had a greater frequency of VI; this might be explained by several factors such as the exposure that mothers have to anti-vaxxer groups, the exclusion of pregnant and lactating women in the COVID-19 vaccine trials and the, as well as men having a lower acceptance of conspiracy beliefs about the disease [10,34,36]. In LAC, man's role as family chief has been described [37,38]; besides, to a growing financial crisis given the pandemic's economic insecurity, the most vulnerable groups require urgent access to the vaccine to be able to sustain their households [9]. Economic insecurity was associated with a higher prevalence of FAE; in contrast, high vaccination coverage would be necessary to reactivate economic activities. Therefore, it urges to design and implement effective communication strategies to increase the population's confidence in COVID-19 vaccination while refuting falsehoods about the vaccine effects and other conspiracy theories [18]. Other possible causes of a low VI frequency could be the belief that vaccines are unnecessary and the unknown or short duration of immunity [12].
Furthermore, we found that living in towns, village or rural areas was associated with a greater FAE frequency, a finding that seems to be consistent with previous studies [10]. Distrust in vaccines and conspiracy beliefs are more robust in people with lower education levels and regions with higher poverty rates [[39], [40], [41]], such as LAC's rural regions. In these areas, health promotion activities do not have adequate coverage increasing the risk of misinformation; therefore, increasing resistance to immunization strategies and community mitigation strategies. It is necessary to reinforce and adapt communication strategies towards these populations [39].
LAC is one of the most affected regions by the pandemic; some of these countries rank among the countries reporting the most coronavirus-related deaths per inhabitant in the world. The pandemic effects have been devastating for their health systems, which in many cases are fragmented and nowadays have collapsed [40]. The collapse of the healthcare system leads to fear of suffering severe COVID-19 disease, for which vaccination represents the hope of being able to defeat the pandemic and reduce the high mortality rates [41]. After witnessing the positive outcomes of experiences such as the Israeli one [42], the message on the need for LAC countries of a high coverage campaign for COVID19 has been reinforced, which would explain the high frequency of VI. However, this occurs with a high frequency of FAE, which persists in the population due to mistrust regarding vaccines' safety and the short time these products were developed [43].
We found that the recommendation by friends and family increased the VI, but also the FAE. This situation could be due to the immediate environment's information to contain fake news or non-corroborated information that would generate mistrust [43,44]. Likewise, excessive exposure to false and fatalistic news can generate resistance to vaccination and lead to vaccination rejection [39]. However, given the need to return to daily activities and observing that the number of people vaccinated increases in developed countries, the desire to have vaccines soon could become more assertive.
Also, we found that a recommendation from local health workers, government health officials and WHO increases the VI and decreases the FAE. That is important to identify groups that could potentially serve as communication agents to increase vaccination acceptance in the population. Due to the health systems' inadequate response capacity during the pandemic, the self-medication practice gained popularity [45]. There is a vast culture of self-medication in the LAC region, which is even promoted by communication media. Besides, in countries as Peru and Bolivia, the use of unproven therapies such as chlorine dioxide became relevant, increasing the popularity of extremist anti-vaccine groups [46]. It is relevant to have community strategies based on scientific information and adapted according to the population group of interest [47,48]. The health personnel and the minister of health of each country must provide confidence to the population and communicate the vaccination benefits [43,49].
We find that politicians recommendations decreased the VI and FAE. This situation could be due to the population believes that the measures taken to combat the pandemic have been affected by political decisions or by personal pursuits objectives by political groups [43]. In this way, there was a politicization of the pandemic, which generates distrust in the population at a government's sanitary recommendation [18]. However, due to the constant corruption scandals to which the LAC political class has been linked, including clandestine vaccination, outside the context of a clinical trial and influence traffic such as Peru and Argentina [50,51]. These events would generate rejection towards vaccination but the loss of FAE.
We found differences in the prevalence of VI and FAE among countries. Likewise, the high frequency of VI was not consistent with the low frequency of FAE in all countries. Only Puerto Rico U.S., Costa Rica and Brazil had the highest VI with the lowest FAE presence among the countries. These countries were also the ones with the highest frequency of VI after a recommendation of the WHO, local health workers and government officials. Thus, it is likely that sociocultural factors, the dissemination of information campaigns by the government, the strength of the anti-vaxxer movements and the politicization of vaccination can influence the differences in VI and FAE in other countries [12,36].
5.4. The relevance of our findings
It is important to identify groups that may have less VI or greater FAE to intervene rapidly. The best strategy to control the pandemic is mass vaccination; many countries have already started the vaccination process, prioritizing vulnerable groups [52]. Although the VI prevalence is high, the FAE frequency is similar, which could compromise LAC countries' national immunization strategies. Besides, LAC countries have a more substantial vaccination scheme than European or North American countries [15]; therefore, vaccination campaigns and strategies could be successful, and the population could accept them.
During the COVID-19 pandemic, due to the disease's fear, the population used multiple information resources, including television, radio, social media, local doctors and scientists who did scientific divulgation [43]. However, due to the pandemic's spread, the lack of adequate and accessible treatment, and the media's contradictions, the population achieved an “infodemic” [53,54]. This situation led to the belief in uncorroborated information that could generate mistrust or rejection of COVID-19 vaccines. In this way, it is crucial to work on disseminating transparent and adequate information regarding vaccines' safety and efficacy with local doctors, health officials, and scientists who can provide confidence to the population [43,47]. Likewise, it is crucial to prevent political corruption acts concerning vaccines' proper use from generating rejection in the population. International health agencies, including the WHO, and especially the Pan American Health Organization (PAHO), should consider these results to promote vaccination in the region of the Americas.
5.5. Strengths and limitations
The study has limitations. Although the data collected from a multinational study with a significant sample was analyzed, the participants are users of a network, which implies that the data obtained comes from a sample with internet access and social media users, not representing a population without these characteristics. Likewise, the variables included for this analysis and its definition are subordinated to the survey. Additionally, there may be other confounders for the association between the variables studied and the VI or FAE, which were not measured by the survey and should be included in future studies. Besides, the data was obtained by self-report, so there may be a sub-record of information. Finally, due to the study's design, causality between the variables evaluated cannot be established. Despite this, this study has strengths such as the large sample that includes 20 LAC countries, which characterizes the study's problem for this population. Likewise, the respondents are users of social media widely known and used in LAC (and four out of every five Internet users in this region have a Facebook profile). Also, as a limitation, we have no access to variables such as racial and ethnic minorities, and certainly, possible variation in uptake based on race and ethnicity would be present, as has been previously reported [55].
6. Conclusions
Despite the high prevalence of VI, the study found a similar FAE frequency. The identified factors can be used to design and develop strategies to promote vaccination, aiming to reduce the FAE. Guaranteeing a mass vaccination to reduce the human impact of COVID-19 is essential. Moreover, when people are suffering the neglect in LAC, and support the return of economic activities.
Ethical approval
Not required as a retrospective analysis of data, blinded personal identification data. The participants gave informed consent before starting the survey. The study is exempt from an institutional review board ethical approval since it used secondary data, and the database does not contain any sensitive data or personal identifiers. Hence, the integrity of the participants was not compromised. We obtained the data by signing a research data use agreement with the University of Maryland. The data was downloaded without identifiers. The participants gave their informed consent before starting the survey.
Funding
This research received no specific grant from any funding agency in the public, commercial, or not-for-profit sectors.
Authors' contributions
All authors made substantial contributions to the study's conception and design, analysis and interpretation. CRediT author statement:
CRediT authorship contribution statement
Diego Urrunaga-Pastor: Conceptualization, Methodology, Writing – original draft. Guido Bendezu-Quispe: Conceptualization, Methodology, Writing – original draft. Percy Herrera-Añazco: Conceptualization, Methodology, Writing – original draft. Angela Uyen-Cateriano: Methodology, Writing – review & editing. Carlos J. Toro-Huamanchumo: Conceptualization, Methodology, Writing – original draft. Alfonso J. Rodriguez-Morales: Methodology, Writing – original draft, Writing – review & editing. Adrian V. Hernandez: Methodology, Writing – review & editing. Vicente A. Benites-Zapata: Conceptualization, Methodology, Writing – original draft.
Declaration of competing interest
The authors declare that they have no competing interests.
Acknowledgements
The authors would like to thank the University of Maryland and Facebook, Inc for conducting and made the survey dataset available.
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.tmaid.2021.102059.
Appendix A. Supplementary data
The following is the Supplementary data to this article:
References
- 1.Johns Hopkins University COVID-19 dashboard by the center for systems science and engineering (CSSE) at Johns Hopkins University (JHU) 2021. https://coronavirus.jhu.edu/map.html
- 2.CEPAL N. Health and the economy: a convergence needed to address COVID-19 and retake the path of sustainable development in Latin America and the Caribbean 2020.
- 3.Zhou F., Shefer A., Wenger J., Messonnier M., Wang L.Y., Lopez A., et al. Economic evaluation of the routine childhood immunization program in the United States, 2009. Pediatrics. 2014;133:577–585. doi: 10.1542/peds.2013-0698. [DOI] [PubMed] [Google Scholar]
- 4.Ozawa S., Clark S., Portnoy A., Grewal S., Brenzel L., Walker D.G. Return on investment from childhood immunization in low- and middle-income countries, 2011-20. Health Aff Proj Hope. 2016;35:199–207. doi: 10.1377/hlthaff.2015.1086. [DOI] [PubMed] [Google Scholar]
- 5.Orenstein W.A., Ahmed R. Simply put: vaccination saves lives. Proc Natl Acad Sci U S A. 2017;114:4031–4033. doi: 10.1073/pnas.1704507114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.World Health Organization Ten threats to global health in 2019. 2019. https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019
- 7.World Health Organization COVID-19 vaccines. 2021. https://www.who.int/emergencies/diseases/novel-coronavirus-2019/covid-19-vaccines
- 8.World Health Organization Vaccine hesitancy: a growing challenge for immunization programmes. 2015. https://www.who.int/news/item/18-08-2015-vaccine-hesitancy-a-growing-challenge-for-immunization-programmes
- 9.Lazarus J.V., Ratzan S.C., Palayew A., Gostin L.O., Larson H.J., Rabin K., et al. A global survey of potential acceptance of a COVID-19 vaccine. Nat Med. 2020:1–4. doi: 10.1038/s41591-020-1124-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Sallam M. COVID-19 vaccine hesitancy worldwide: a concise systematic review of vaccine acceptance rates. Vaccines. 2021;9:160. doi: 10.3390/vaccines9020160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Peretti-Watel P., Seror V., Cortaredona S., Launay O., Raude J., Verger P., et al. A future vaccination campaign against COVID-19 at risk of vaccine hesitancy and politicisation. Lancet Infect Dis. 2020;20:769–770. doi: 10.1016/S1473-3099(20)30426-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Lin C., Tu P., Beitsch L.M. Confidence and receptivity for COVID-19 vaccines: a rapid systematic review. Vaccines. 2021;9:16. doi: 10.3390/vaccines9010016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Lin Y., Hu Z., Zhao Q., Alias H., Danaee M., Wong L.P. Understanding COVID-19 vaccine demand and hesitancy: a nationwide online survey in China. PLoS Neglected Trop Dis. 2020;14 doi: 10.1371/journal.pntd.0008961. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Fadda M., Albanese E., Suggs L.S. When a COVID-19 vaccine is ready, will we all be ready for it? Int J Publ Health. 2020:1–2. doi: 10.1007/s00038-020-01404-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Guzman-Holst A., DeAntonio R., Prado-Cohrs D., Juliao P. Barriers to vaccination in Latin America: a systematic literature review. Vaccine. 2020;38:470–481. doi: 10.1016/j.vaccine.2019.10.088. [DOI] [PubMed] [Google Scholar]
- 16.Andrews G., Slade T. Interpreting scores on the Kessler psychological distress scale (K10) Aust N Z J Publ Health. 2001;25:494–497. doi: 10.1111/j.1467-842x.2001.tb00310.x. [DOI] [PubMed] [Google Scholar]
- 17.Latkin C.A., Dayton L., Yi G., Colon B., Kong X. Mask usage, social distancing, racial, and gender correlates of COVID-19 vaccine intentions among adults in the US. PloS One. 2021;16 doi: 10.1371/journal.pone.0246970. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Ruiz J.B., Bell R.A. Predictors of intention to vaccinate against COVID-19: results of a nationwide survey. Vaccine. 2021;39:1080–1086. doi: 10.1016/j.vaccine.2021.01.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Reiter P.L., Pennell M.L., Katz M.L. Acceptability of a COVID-19 vaccine among adults in the United States: how many people would get vaccinated? Vaccine. 2020;38:6500–6507. doi: 10.1016/j.vaccine.2020.08.043. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Taylor S., Landry C.A., Paluszek M.M., Groenewoud R., Rachor G.S., Asmundson G.J. A proactive approach for managing COVID-19: the importance of understanding the motivational roots of vaccination hesitancy for SARS-CoV2. Front Psychol. 2020;11:2890. doi: 10.3389/fpsyg.2020.575950. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Sherman S.M., Smith L.E., Sim J., Amlôt R., Cutts M., Dasch H., et al. COVID-19 vaccination intention in the UK: results from the COVID-19 vaccination acceptability study (CoVAccS), a nationally representative cross-sectional survey. Hum Vaccines Immunother. 2020:1–10. doi: 10.1080/21645515.2020.1846397. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Paul E., Steptoe A., Fancourt D. Attitudes towards vaccines and intention to vaccinate against COVID-19: implications for public health communications. Lancet Reg Health-Eur. 2021;1:100012. doi: 10.1016/j.lanepe.2020.100012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Chen M., Li Y., Chen J., Wen Z., Feng F., Zou H., et al. An online survey of the attitude and willingness of Chinese adults to receive COVID-19 vaccination. Hum Vaccines Immunother. 2021:1–10. doi: 10.1080/21645515.2020.1853449. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Yu Y., Lau J.T., Lau M., Wong M., Chan P.K. Understanding the prevalence and associated factors of behavioral intention of COVID-19 vaccination under specific scenarios combining effectiveness, safety, and cost in the Hong Kong Chinese general population. Int J Health Pol Manag. 2021 doi: 10.34172/ijhpm.2021.02. In press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Rhodes A., Hoq M., Measey M.-A., Danchin M. Intention to vaccinate against COVID-19 in Australia. Lancet Infect Dis. 2020 doi: 10.1016/S1473-3099(20)30724-6. In press. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Fisk R.J. Barriers to vaccination for COVID-19 control—experience from the United States. Glob Health J. 2021;5(1):51–55. doi: 10.1016/j.glohj.2021.02.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Scott E.M., Stein R., Brown M.F., Hershberger J., Scott E.M., Wenger O.K. Vaccination patterns of the northeast Ohio Amish revisited. Vaccine. 2021;39:1058–1063. doi: 10.1016/j.vaccine.2021.01.022. [DOI] [PubMed] [Google Scholar]
- 28.Neumann-Böhme S., Varghese N.E., Sabat I., Barros P.P., Brouwer W., van Exel J., et al. A European survey on willingness to be vaccinated against COVID-19. Springer; 2020. Once we have it, will we use it? [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Fournet N., Mollema L., Ruijs W.L., Harmsen I.A., Keck F., Durand J.Y., et al. Under-vaccinated groups in Europe and their beliefs, attitudes and reasons for non-vaccination; two systematic reviews. BMC Publ Health. 2018;18:1–17. doi: 10.1186/s12889-018-5103-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Rehmet S., Ammon A., Pfaff G., Bocter N., Petersen L.R. Cross-sectional study on influenza vaccination, Germany, 1999–2000. Emerg Infect Dis. 2002;8:1442. doi: 10.3201/eid0812.010497. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Rachiotis G., Mouchtouri V.A., Kremastinou J., Gourgoulianis K., Hadjichristodoulou C. Low acceptance of vaccination against the 2009 pandemic influenza A (H1N1) among healthcare workers in Greece. Euro Surveill. 2010;15:19486. [PubMed] [Google Scholar]
- 32.Alvarado-Socarras JL, Vesga-Varela AL, Quintero-Lesmes DC, Fama-Pereira MM, Serrano-Diaz NC, Vasco M, et al. Perception of COVID-19 vaccination amongst physicians in Colombia. Vaccines. 2021;9(3):287. doi: 10.3390/vaccines9030287. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Malik A.A., McFadden S.M., Elharake J., Omer S.B. Determinants of COVID-19 vaccine acceptance in the US. EClinicalMedicine. 2020;26:100495. doi: 10.1016/j.eclinm.2020.100495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Wong L.P., Alias H., Wong P.-F., Lee H.Y., AbuBakar S. The use of the health belief model to assess predictors of intent to receive the COVID-19 vaccine and willingness to pay. Hum Vaccines Immunother. 2020;16:2204–2214. doi: 10.1080/21645515.2020.1790279. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Abu-Farha R.K., Alzoubi K.H., Khabour O.F. Public willingness to participate in COVID-19 vaccine clinical trials: a study from Jordan. Patient Prefer Adherence. 2020;14:2451. doi: 10.2147/PPA.S284385. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Sallam M., Dababseh D., Eid H., Al-Mahzoum K., Al-Haidar A., Taim D., et al. High rates of COVID-19 vaccine hesitancy and its association with conspiracy beliefs: a study in Jordan and Kuwait among other Arab countries. Vaccines. 2021;9:42. doi: 10.3390/vaccines9010042. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Wilson T.D. Violence against women in Latin America. Lat Am Perspect. 2014;41:3–18. doi: 10.1177/0094582X13492143. [DOI] [Google Scholar]
- 38.Bott S., Guedes A., Goodwin M., Mendoza J.A. Pan American Health Organization; Washington, DC: 2012. Violence against women in Latin America and the Caribbean: a comparative analysis of population-based data from 12 countries.https://stacks.cdc.gov/view/cdc/22295 [Google Scholar]
- 39.French J., Deshpande S., Evans W., Obregon R. Key guidelines in developing a pre-emptive COVID-19 vaccination uptake promotion strategy. Int J Environ Res Publ Health. 2020;17:5893. doi: 10.3390/ijerph17165893. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Atun R., de Andrade L.O.M., Almeida G., Cotlear D., Dmytraczenko T., Frenz P., et al. Health-system reform and universal health coverage in Latin America. Lancet. 2015;385:1230–1247. doi: 10.1016/S0140-6736(14)61646-9. [DOI] [PubMed] [Google Scholar]
- 41.Lazarus J.V., Ratzan S.C., Palayew A., Gostin L.O., Larson H.J., Rabin K., et al. A global survey of potential acceptance of a COVID-19 vaccine. Nat Med. 2020:1–4. doi: 10.1038/s41591-020-1124-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Dagan N., Barda N., Kepten E., Miron O., Perchik S., Katz M.A., et al. BNT162b2 mRNA covid-19 vaccine in a nationwide mass vaccination setting. N Engl J Med. 2021 doi: 10.1056/NEJMoa2101765. 0:null. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Mannan D.K.A., Farhana K.M. Social Science Research Network; Rochester, NY: 2020. Knowledge, attitude and acceptance of a COVID-19 vaccine: a global cross-sectional study. [DOI] [Google Scholar]
- 44.Ali S.H., Foreman J., Tozan Y., Capasso A., Jones A.M., DiClemente R.J. Trends and predictors of COVID-19 information sources and their relationship with knowledge and beliefs related to the pandemic: nationwide cross-sectional study. JMIR Public Health Surveill. 2020;6 doi: 10.2196/21071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Molento M.B. COVID-19 and the rush for self-medication and self-dosing with ivermectin: a word of caution. One Health. 2020;10:100148. doi: 10.1016/j.onehlt.2020.100148. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Mostajo-Radji M. Pseudoscience in the times of crisis: how and why chlorine dioxide consumption became popular in Latin America during the COVID-19 pandemic. 2020. [DOI]
- 47.Qiao S., Friedman D.B., Tam C.C., Zeng C., Li X. Vaccine acceptance among college students in South Carolina: do information sources and trust in information make a difference? MedRxiv. 2020 doi: 10.1101/2020.12.02.20242982. 2020.12.02.20242982. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Charron J., Gautier A., Jestin C. Influence of information sources on vaccine hesitancy and practices. Med Maladies Infect. 2020;50:727–733. doi: 10.1016/j.medmal.2020.01.010. [DOI] [PubMed] [Google Scholar]
- 49.Alvarado-Socarras J.L., Vesga-Varela A.L., Quintero-Lesmes D.C., Fama-Pereira M.M., Serrano-Diaz N.C., Vasco M., et al. 2021 2021. Perception of COVID-19 vaccination amongst physicians in Colombia, january. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Chauvin L. Peruvian COVID-19 vaccine scandal spreads. Lancet. 2021;397:783. doi: 10.1016/S0140-6736(21)00508-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Lissardy G. BBC News Mundo; 2021. Escándalos con la vacuna del coronavirus: cómo la lucha contra la covid-19 desnuda viejos vicios de América Latina. [Google Scholar]
- 52.Los países de América Latina donde todavía no han llegado vacunas contra covid-19 (y cuándo se espera que lo hagan) BBC News Mundo; 2021. [Google Scholar]
- 53.Patwa P., Sharma S., Pykl S., Guptha V., Kumari G., Akhtar M.S., et al. 2020. Fighting an infodemic: COVID-19 fake news dataset. ArXiv201103327 Cs. [Google Scholar]
- 54.Alvarez-Risco A., Mejia C.R., Delgado-Zegarra J., Del-Aguila-Arcentales S., Arce-Esquivel A.A., Valladares-Garrido M.J., et al. The Peru approach against the COVID-19 infodemic: insights and strategies. Am J Trop Med Hyg. 2020 doi: 10.4269/ajtmh.20-0536. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Tirupathi R., Muradova V., Shekhar R., Salim S.A., Al-Tawfiq J.A., Palabindala V. COVID-19 disparity among racial and ethnic minorities in the US: a cross sectional analysis. Trav Med Infect Dis. 2020;38:101904. doi: 10.1016/j.tmaid.2020.101904. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.