To the editor:
Mild eosinophilia is not uncommon in hemodialysis patients. It is historically related in most cases to allergic reactions to the extracorporeal circuit components and more rarely to various conditions ranging from infections to malignancies.1,2
We report on six patients (Table 1) who developed an acute severe eosinophilia (median peak of eosinophil count, 8.6 ± 3.3 G/) that was induced by the insertion of tunneled central venous catheters. The link between eosinophilia and central venous catheters is substantiated by causality assessment,3 based first on chronological criteria (Figure 1): while eosinophil blood count was normal for several years, it dramatically increased after the catheter insertion, persisted at high levels as long as the catheter was left in place and resolved shortly after catheter withdrawal. Besides, in patients 3 and 4, eosinophilia recurred after a further venous catheter insertion. Furthermore, comprehensive etiological work-up (parasites culture and serological tests, autoantibodies tests, bone marrow aspiration, tests for FIP1L1-PDGFRA and BCR-ABL rearrangements, thoraco-abdominal and pelvic CT-scan) for underlying malignancy, infection, allergy or autoimmune disease and assessment for medications and dialysis membrane replacement, failed to identify any alternative cause for eosinophilia (semiological criteria for causality).4,S1
Table 1.
Characteristics of six dialysis patients with tunneled catheter-related eosinophilia
| Patient Gender, Age (y) |
Type of venous catheter (brand) | Time from catheter insertion to Eo (days) | Eo peak (G/L) (time from catheter, days) | Eo related manifestations | Eo duration (months) | Eo recovery time after catheter withdrawal (days) |
|---|---|---|---|---|---|---|
|
P1 M, 48 |
Tunneled jugular catheter (HEMOTECH®) | 90 (first available test after catheter) | 10 (183) | Ulcerative colitis Pulmonary nodules (Figure 2) |
13 | 15 |
|
P2 M, 50 |
Tunneled jugular catheter (HEMOTECH®) Intermittent use of fistula |
322 (first available test after catheter) | 4.8 (336) | Urticarial rash | 12.5 | 0 |
|
P3 F, 57 |
Tunneled jugular catheter (OPTIMED®) | 277 | 1.9 (281) | No | 0.5 | NA |
| Tunneled jugular catheter (VYGON®) | 68 (first available test after catheter) | 1.8 (68) | No | 6 | 30 | |
| Tunneled jugular catheter (HEMOTECH®) | 18 | 5.2 (40) | No | 1 | 15 | |
| Tunneled jugular catheter (HEMOTECH®) | 21 | 8.5 (37) | No | 1.5 | NA | |
|
P4 M, 57 |
Tunneled jugular catheter (VYGON®) | 37 | 2 (112) | No | 3 | 4 |
| Tunneled jugular catheter (VYGON®) | 32 | 14.3 (37) | Pruritus, sweats | 8.5 | 1 | |
|
P5 F, 54 |
Palindrome catheter (METRONIC®) | 93 | 6.1 (387) | Pruritus, sweats and urticarial rash | 14 | 21 (renal transplantation) |
|
P6 M, 37 |
Tunneled jugular catheter (HEMOTECH®) | 47 | 9.8 (1230) | Pruritus, sweats and urticarial rash | 39 | NA (renal transplantation) |
Eo, eosinophilia; F, female; M, male; NA, not available; P, patient; y, year
Figure 1.
Time evolution of eosinophilscounts in six patients with hemodialysis catheter induced eosinophilia.
The cases presented here are peculiar for the severity of eosinophilia. It was associated to rather mild symptoms in the majority of patients, mostly pruritus, sweating and urticarial rash during dialysis sessions. However, in one patient, eosinophilia was associated to the occurrence of pulmonary nodules, eosinophilic alveolitis and colitis (Figure 2). In this patient, as well as in two additional ones, eosinophilia work-up led to a significant delay in the access to renal transplantation, due to temporary contraindication. In two other patients, severe reactions with hypotension, dyspnea occurred repeatedly after start of dialysis session.
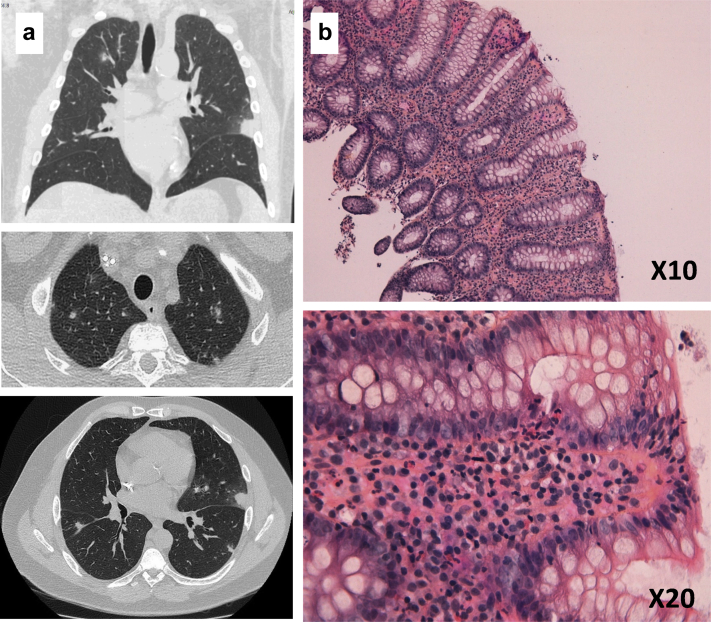
Figure 2.
Patient 1 had severe eosinophilia associated to the occurrence of pulmonary nodules (a), eosinophilic alveolitis and colitis (b).
To the best of our knowledge, this is the first description of severe eosinophilia induced by dialysis catheter. Nephrologists should be aware that indwelling venous catheter is a potential reversible cause of severe eosinophilia in hemodialysis patients whose mechanism remains to be understood. This will help avoiding useless etiological investigations and, more importantly, delays in the access to renal transplantation for these patients.
Footnotes
Supplementary Reference.
Supplementary Material
References
- 1.Hildebrand S., Corbett R., Duncan N., Ashby D. Increased prevalence of eosinophilia in a hemodialysis population: Longitudinal and case control studies. Hemodial Int. 2016;20(3):414–420. doi: 10.1111/hdi.12395. [DOI] [PubMed] [Google Scholar]
- 2.Gauckler P., Shin J.I., Mayer G., Kronbichler A. Eosinophilia and Kidney Disease: More than Just an Incidental Finding? J Clin Med. 2018;7(12) doi: 10.3390/jcm7120529. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Miremont-Salamé G., Théophile H., Haramburu F. Causality assessment in pharmacovigilance: The French method and its successive updates. Therapie. 2016 Apr;71(2):179–186. doi: 10.1016/j.therap.2016.02.010. [DOI] [PubMed] [Google Scholar]
- 4.Gotlib J. World Health Organization-defined eosinophilic disorders: 2017 update on diagnosis, risk stratification, and management. Am J Hematol. 2017;92(11):1243–1259. doi: 10.1002/ajh.24880. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.