Abstract
The current pandemic caused by the new severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) has become a public health emergency. To date, March 1, 2021, coronavirus disease 2019 (COVID-19) has caused about 114 million accumulated cases and 2.53 million deaths worldwide. Previous pieces of evidence suggest that SARS-CoV-2 may affect the central nervous system (CNS) and cause neurological symptoms in COVID-19 patients. It is also known that angiotensin-converting enzyme-2 (ACE2), the primary receptor for SARS-CoV-2 infection, is expressed in different brain areas and cell types. Thus, it is hypothesized that infection by this virus could generate or exacerbate neuropathological alterations. However, the molecular mechanisms that link COVID-19 disease and nerve damage are unclear. In this review, we describe the routes of SARS-CoV-2 invasion into the central nervous system. We also analyze the neuropathologic mechanisms underlying this viral infection, and their potential relationship with the neurological manifestations described in patients with COVID-19, and the appearance or exacerbation of some neurodegenerative diseases.
Keywords: SARS-CoV-2, storm cytokine syndrome, neuroinflammation, blood-brain barrier, neurological alterations, neurodegenerative diseases, Alzheimer's disease
Introduction
Coronavirus disease 2019 (COVID-19) was first reported in December 2019 in Wuhan, in Hubei province, China (1). In March 2020, the world health organization (WHO) declared the COVID-19 a pandemic. Almost a year later, on March 1, 2021, more than 114 million cases and 2.53 million deaths have been reported (2–4). Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the causative agent of COVID-19, is 100 nm with an oval shape and covered with crown-shaped glycoprotein spikes (5). It is transmitted through respiratory droplets from infected individuals or contact with fomites. Once SARS-CoV-2 enters the body, the onset of symptoms ranges from 2 to 14 days. Patients can manifest clinically from asymptomatic or mild symptoms to moderate or severe symptoms (6, 7). Mild to moderate symptoms manifest as fever, dry cough, nasal congestion, sore throat, runny nose, fatigue, myalgias, diarrhea, anosmia, and ageusia as main symptoms (6, 7). The severe condition is characterized by atypical pneumonia, which can be observed as “ground-glass opacification” with bilateral multi-lobular consolidations by imaging studies (8). Between 5 and 30% of patients develop acute respiratory distress syndrome, characterized by rapid onset and with generalized inflammation in the lungs, requiring invasive life support therapy, such as mechanical ventilation (6, 7). There is increasing evidence that these critically ill COVID-19 patients suffer a so-called “cytokine storm syndrome,” characterized by the release of many pro-inflammatory cytokines [interleukin (IL)-1β and IL-6] and a low number of T cells into the bloodstream (9). The mean period from the onset of the symptoms to death is around 13 days [interquartile range (IQR) 11–18 days], and this depends on advanced age (>65 years) and comorbidities such as diabetes mellitus (DM), hypertension, cardiovascular disease, or chronic obstructive pulmonary disease (COPD) (10). These comorbidities are also risk factors for severity and transfer to intensive care unit (ICU), endotracheal intubation, and death in patients with COVID-19 (11). However, there may be bias in the epidemiological data due to the in-hospital stay of the patient, as well as the human development index of each country. SARS-CoV-2 also may be able to invade multiple organs, including the nervous system, and thus cause multiple organ dysfunction syndrome (MODS) (12). The neurological manifestations are beginning to take on unquestionable importance, mainly in the critical patient (13, 14). Neurological manifestations of COVID-19 and other coronavirus infections involve febrile seizures, disorientation, difficulty in speaking, encephalitis, and stroke (15–18). The mechanisms by which SARS-CoV-2 can spread, infect, cause damage to nerve cells and finally affect both the central (CNS) and peripheral (PNS) nervous system, are not yet understood. This review will analyze the potential mechanisms by which SARS-CoV-2 can invade the CNS and PNS and generate a neurotoxic environment that may trigger or worsen neurological disorders.
SARS-CoV-2: Structure and Mechanism of Infection
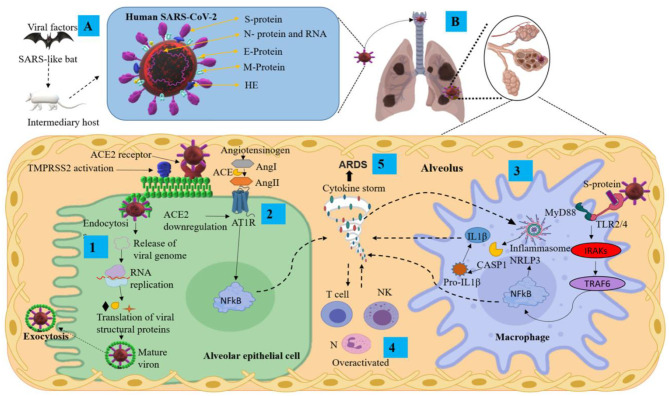
The coronaviruses (CoVs) belong to the Orthocoronaviridae subfamily; order: Nidovirales; subordination: Cornidovirineae; family: Coronaviridae (19). They can be grouped into four genera, including α/β/γ/δ-CoV: α and β infect mammals and γ/δ infect birds (20). CoVs are large, positive-stranded RNA viruses, and they are enveloped with a lipid membrane derived from a host cell. The protein protruding from the virus membrane is the spike (S) protein, giving the virus the appearance of a solar corona (1) (Figure 1A). Coronaviruses have single-stranded RNA of between 26.4 and 31.7 kilobases, making them the largest of RNA viruses (21). CoVs have several main structural proteins (Figure 1A): nucleocapsid (N) proteins, which surround the RNA genome; membrane (M) proteins (also known as E1 membrane glycoprotein or matrix protein) (20); envelope (E) proteins, involved in virus assembly, and S protein, which mediates virus entry into host cells. Some CoVs also encode an envelope-associated hemaglutinin-esterase protein (HE) used as an invading mechanism (22).
Figure 1.
Pathological mechanisms of SARS-CoV-2 in the pulmonary alveolus. (A) Mode of transmission and main structural proteins of SARS-CoV-2. (B) Mechanisms of SARS-CoV-2 infection and pulmonary inflammatory immune response. ACE2, angiotensin-converting enzyme 2; Ang, angiotensin; ARDS, acute respiratory distress syndrome; AT1R, angiotensin II type I receptor; CASP1, aaspase 1; E protein, envelope small membrane protein; HE, hemagglutinin esterase; IL1β, interleukin 1 beta; IRAKs, interleukin-1 receptor-associated kinases; M protein, membrane protein; MyD88, myeloid differentiation primary response 88; N protein, nucleoprotein; N, neutrophils; NF-κB, nuclear factor Kappa B; NK, natural killer cells; NLRP3, nucleotide-binding domain-, leucine-rich repeat-containing receptor, pyrin domain-containing 3; RNA, ribonucleic acid; S protein, spike protein; TMPRSS2, transmembrane serine protease 2; TRAF6, tumor necrosis factor receptor-associated factor 6.
The S protein is the main antigenic component of SARS-CoV-2 structural proteins and is comprised of two subunits, S1 and S2 (23). This protein is multifunctional, contributing to host receptor binding, pathogenesis, and cell tropism. The S protein binds to host receptors on target cells, inducing virion particle endocytosis, and then catalyzes the fusion between host and viral membranes, allowing the virus genome penetration into the host cytoplasm (24). The S1 domain has a high-affinity association with the host receptor angiotensin-converting enzyme 2 (ACE2) (25). The receptor-binding domain (RBD) of the S protein binds to the extracellular peptidase domain of ACE2, mediating cell entry (25, 26). SARS-CoV-2 uses the SARS-CoV receptor ACE2 for entry and the transmembrane serine protease 2 (TMPRSS2) for S protein priming. The endosomal cysteine proteases cathepsin B and L (CatB/L) can be used to mature the S protein (27, 28). However, while TMPRSS2 is indispensable for viral spread and pathogenesis, the CatB/L activity is not essential (Figure 1B step 1). Once the virus enters the host cell, viral replication begins with translation of the replicase-polymerase gene and assembly of the replication-transcription complex. This complex also transcribes the genomic regions to structural proteins. New virions are assembled in the endoplasmic reticulum and Golgi apparatus released from the cell (Figure 1B step 1) (29). Finally, the newly assembled SARS-CoV-2 virions possess protein S on the surface and are ready to infect any cell that expresses the ACE2 receptor with no further requirement for TMPRSS2 activity (30).
SARS-CoV2 Pathophysiology
The SARS-CoV-2 pathophysiology is not yet clear. It has been suggested that it can be similar to SARS-CoV (31, 32) with two possible responses (32):
1) After the viral infection occurs, active viral replication and dissemination through ACE2 receptors occurs with the associated host antiviral responses. SARS-CoV-2 downregulates ACE2 receptors, with loss of their catalytic effect at the membrane surface. Inflammation and thrombosis have been related to enhanced and unimpeded angiotensin II effects through the ACE-Angiotensin II-AT1 receptor axis (33) (Figure 1B step 2). The SARS-CoV-2 infection can lead to an acute immune response. This response is driven by inflammatory alveolar and monocyte-derived macrophages that can be activated by pathogen-associated molecular patterns (PAMPs) and damage-associated molecular patterns (DAMPs) released by infected pneumocytes (34–36). Subsequently, several pro-inflammatory mediators such as tumor necrosis factor-alpha (TNF-α) and IL-1β, secreted by alveolar macrophages, initiate the acute inflammatory cascade that triggers cell death and damage. Aside from PAMP/DAMP production, the recruitment of immune cells and activation of the nucleotide-binding domain leucine-rich repeat-containing receptor, pyrin domain-containing 3 (NLRP3), establish a pro-inflammatory positive feedback cascade (32, 34, 35) (Figure 1B steps 3 and 4). This localized inflammatory cell death could lead to a hyper-inflammatory microenvironment and spread to the vasculature, inducing leakage, edema, and pneumonia in COVID-19 patients (35, 37). Serum of COVID-19 patients is characterized by increased levels of the following: IL-2, IL-7, IL-10, TNF-α, protein monocyte chemoattractant-1 (MCP1; also known as C-C motif chemokine ligand 2 CCL2), granulocyte colony-stimulating factor (G-CSF), macrophage inflammatory protein 1 alpha (MIP1α; also known as CCL3), C-X-C motif chemokine ligand 10 (CXCL10), C-reactive protein (CRP), D-dimers and ferritin (19, 38–40).
2) The SARS-CoV-2 infection can also lead to the generation of adaptive immunity and neutralizing antibody (NAb). The virus-NAb complex can trigger Fc receptor (FcR)-mediated inflammatory response and acute lung injury. SARS-CoV-2 can infect cells that have FcRs, which provide the ability for antibody-mediated internalization. This mechanism can occur in macrophages, monocytes, or B cells even without ACE2 and TMPRSS2 expression, and especially during infection (41). The internalization of the virus–antibody immune complexes can also promote tissue damage and inflammation by activating myeloid cells via FcRs (42). Both primary and secondary responses culminate in the postulated pathogenesis of SARS-CoV-2 infection (32). Interestingly, it has been suggested that fatal COVID-19 is characterized as a cytokine release syndrome (CRS) induced by a cytokine storm and associated with adverse outcomes of acute respiratory distress syndrome (ARDS) (Figure 1B step 5) and high mortality rate (43, 44).
For mechanistic insights into the life cycle of SARS-CoV-2, the mouse hepatitis virus (MHV) represents a suitable comparator. MHV is a βCoV very similar to SARS-CoV, MERS-CoV, and SARS-CoV-2 (45). Therefore, an MHV animal model could contribute to the elucidation of the neuropathological mechanisms of SARS-CoV-2 in the following aspects: (1) MHV can invade and replicate in the CNS, triggering lesions in the white matter (45); (2) Infection with MHV induces meningoencephalitis in an acute stage and subsequently subacute chronic inflammatory demyelination in the brain and spinal cord (46); (3) CD4 and CD8 T lymphocytes, especially γδ T cells, play an important role in the MHV-induced demyelination process (47); (4) MHV can be translocated from the initial inoculation brain area to the spinal cord through the transit of viral particles in glial and neural cells, as well as by mechanisms that involve the fusion of lipid membranes (48); (5) After intranasal MHV-CoV inoculation in mice, the virus can access the CNS through the olfactory nerve and spread from this area to neuroanatomically interconnected structures such as the limbic system and the brainstem (49).
Potential Neuroinvasive Pathways of SARS-CoV-2
There are four possible routes by which SARS-CoV-2 could enter the CNS: (1) the hematopoietic pathway and subsequent rupture of the blood-brain barrier (BBB); (2) via blood-cerebrospinal fluid (B-CSF); (3) transsynaptic viral spreading; (4) through the entry to circumventricular organs (CVO). In this section, we will discuss the four routes in greater detail.
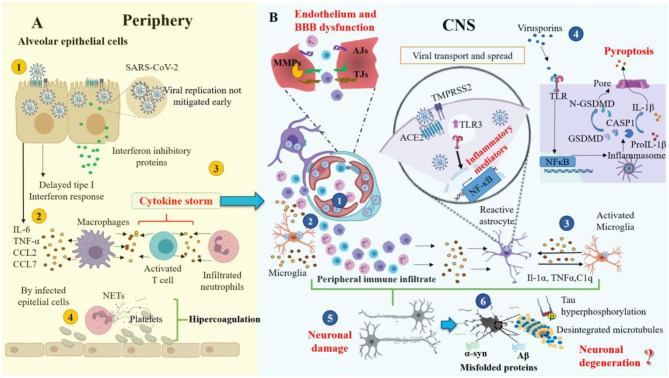
1) Coronaviruses access the bloodstream via the airway and infect immune cells, which may cross BBB facilitated by pro-inflammatory cytokines and chemokines (Figure 2B step 1). The mechanism by which infected immune cells cross the BBB may occur via intercellular adhesion molecule 1 (ICAM-1) mediated transport that is upregulated by TNF-α, followed by activation of matrix metalloproteinases (MMPs) such as MMP9, which specifically influences cellular leakage and membrane degradation (50). Besides, SARS-CoV-2 tropism, toward the CNS endothelial cells (BECs) favors BBB disruption; by entering the cytosol of the astrocyte via the receptor; the virus increases the release of pro-inflammatory cytokines, such as IL-2, IL-6, IL-7, IL-8, TNFα, CCL2, CCL3, CCL7, and CXCL10. The reactive astrocyte could lead to activation of microglia and the peripheral immune infiltrate such as macrophages, neutrophils, and lymphocytes (Figure 2B step 2) (51–54), which could end in neurotoxicity. DM, hypertension, and metabolic syndrome are risk factors for both contracting COVID-19 and a poor prognosis in patients. These comorbidities also contribute to vascular and BBB alteration (55), increase neuroinflammation, and exacerbate neuropathology (56).
2) The CSF circulation comprises both a directional CSF flow and a pulsatile to and from movement throughout the entire brain and which involves a local fluid exchange between blood, interstitial fluid, and CSF (57). It has been suggested that viral infection may occur via B-CSF and alter gene expression in the choroid plexus. This process activates the nuclear factor kappa (NF-kB), upregulates MMP9, and affects B-CSF permeability and immune cell trafficking (MMP8, TNFα, IL6, IL1B, MCP1, intercellular adhesion molecule 1 (ICAM1) (58), leading to a neuroinflammatory environment.
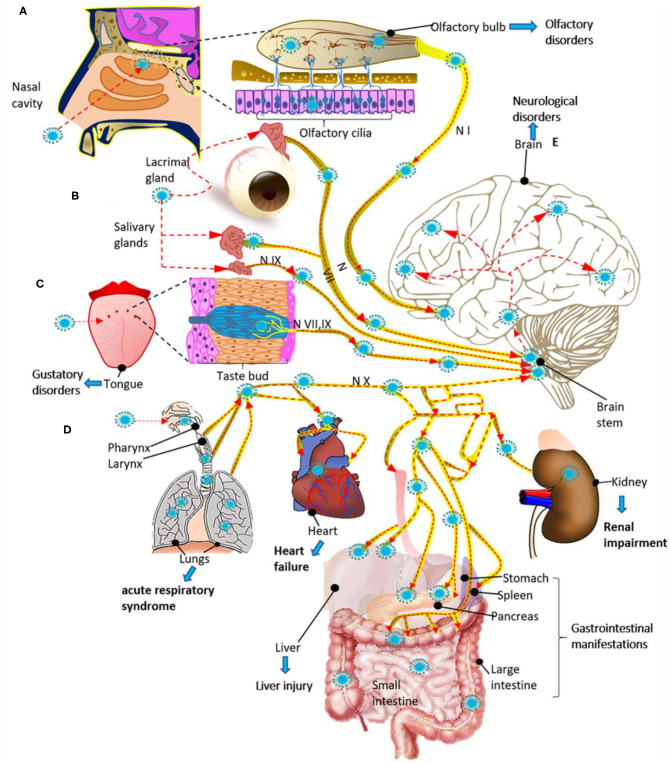
3) Another entry route to the CNS for SARS-CoV-2 could be through axonal transport and transneuronal spread from olfactory, gustatory, trigeminal, and vagal nerves, allowing the virus to infect the brainstem in the early stages of infection (Figures 3A–D) (52, 59). The transneuronal pathway is one of the potential routes that would allow SARS-CoV-2 to enter through the primary sensory neurons, which communicate with the mitral cells. Mitral cells have projections toward the ventricle and the medulla, and this favors the transfer of the virus from the cerebrospinal fluid toward the lymphatic system within the CNS and toward the PNS (60). The virus could also enter the CNS following the transneuronal olfactory bulb pathway and is reflected by changes at the level of the olfactory nerve, bulb, and cortex (61–63). It has been proposed that SARS-CoV-2 could spread retrogradely through transsynaptic transfer, using an exocytosis/endocytosis mechanism or via rapid axonal transport, which would move the virus along the microtubules to the neuronal soma (64). Supporting this hypothesis, it has been shown that some CoVs and other viruses such as rabies and hemagglutinating encephalomyelitis can enter and spread to the CNS via retrograde transsynaptic pathways (65–67), from peripheral nerve endings through membranous-coating-mediated endocytosis and exocytosis (66). Mechanisms have also been described by which viruses can enter and leave axons, both retrograde and anterograde, through coupled transport mediated by vesicles or separate transport which is not mediated by vesicles (68). For this reason, it would be interesting in the future to know if SARS-CoV2 uses transsynaptic transport and to trace neural circuits, using specific labeling techniques.
4) Finally, we suggest that SARS-CoV-2 might enter the CNS through CVOs. CVOs include the subfornical organ, the paraventricular nucleus, the nucleus tractus solitarius (NTS), and the rostral ventrolateral medulla, all of which express ACE2. Besides, these CVOs are highly vascularized and lack a BBB (69). Therefore, these areas would be more susceptible to the virus, triggering neurovascular damage, as we have discussed previously.
Figure 2.
Schematic representation of the pathophysiological mechanisms of SARS-CoV-2. (A) Peripheral pathological events triggered by SARS-CoV-2 infection. (B) Possible CNS pathological mechanisms caused by the severe peripheral hyperinflammation associated with COVID-19. ACE2, angiotensin-converting enzyme 2 receptor; AJs, adherent junctions; Aβ; amyloid-beta; BBB, blood-brain barrier; C1q, the complement component 1q; CASP1, caspase1; CCL, chemokine (C-C motif) ligand; CNS, central nervous system; CXCL10, C–X–C motif chemokine 10; GSDMD, gasdermin-D; IL, interleukin; MMPs, metalloproteinases; NETs, neutrophil extracellular traps; NF-κB, Nuclear factor Kappa B; N-GSDMD, N-terminal gasdermin; NLRP3, nucleotide-binding domain-, leucine-rich repeat-containing receptor, pyrin domain-containing 3; TJs, tight junctions; TLR3, toll-like receptor 3; TNF-α, tumor necrosis factor-alpha; α-syn, alpha-synuclein.
Figure 3.
Potential routes for infection and spread of SARS-CoV-2 to systemic organs and the central nervous system through the cranial nerves (N). (A) SARS-CoV-2 could enter through the olfactory mucosa (causing anosmia), spread through the olfactory nerve (N I) and end in the olfactory cortex. (B) SARS-CoV-2 could also enter through the lacrimal and salivary glands, spread through the facial (N VII) and glossopharyngeal (N IX) nerves, and end in their respective brain stem nuclei. (C) The infection could spread from the taste buds (triggering ageusia) through the N VII and N IX nerves ending in the NTS located in the brain stem. (D) SARS-CoV-2 could also enter through the respiratory tract, reach the respiratory system and via the vagus nerve (N X), spread to other systemic organs innervated by this nerve, and end in the brain stem. (E) Finally, once the virus reaches the brain stem, it can spread to the brain through neuroanatomically interconnected pathways. The SARS-Cov2 infection can cause multiple organ dysfunction syndrome (A–E). The red dashed arrows indicate the possible dissemination route for SARS-CoV-2 through the cranial nerves.
Once SARS-CoV-2 enters the CNS, it could bind to CNS cells, such as neurons, astrocytes, oligodendrocytes, and microglia (70), due to the presence of ACE2 (28, 71) and TMPRSS2 (72) receptors and probably via binding to other receptors (Table 1). It is important to highlight that the expression of ACE2 is low in the human brain, with a higher expression in certain areas such as thalamus and choroid plexus. ACE2 also has access to peptides in the circulation in the cerebrospinal and interstitial fluid, and it is present in pericytes and smooth muscle cells of human brain vessels (95). ACE2 receptors have been reported in other organs, mainly enterocytes, renal tubules, gallbladder, cardiomyocytes, male reproductive cells, placental trophoblasts, ductal cells, eye, and vasculature. In the respiratory system, its expression is limited (96). ACE2 plays a role in attenuating microvascular pathology and protecting against atherogenesis, endothelial dysfunction, thrombus formation, oxidative stress, and inflammatory cascades responsible for monocyte-endothelial cell interaction (71, 97).
Table 1.
Receptors or proteins related to SARS-CoV-2 infection in the nervous system.
| Receptor or protein | Expression in nerve cells | Neuroanatomic areas of gene expression* | Pathological effects on the nervous system | References |
|---|---|---|---|---|
| ACE2 | Neurons, astrocytes, microglia, BECs, OLGs | PG, Acb, Hy, SC, Cd, SN, Cb, HiF, FroCx, Amg, Pu and ACC | The direct binding of SARS-CoV-2 to the ACE2 receptor could trigger microvascular dysfunction, disrupt coagulation processes, cause neuronal depolarization, and increase expression of glutamate and MMPs, resulting in neuroinflammation, seizures, and hemorrhages. | (56, 58, 69, 73–75) |
| TMPRSS2 | PG, Hy, Cb, Amg, Cd, HiF, SN, Acb, ACC, FroCx, Pu and SC. | It acts as a co-receptor for ACE2 and cleaves S protein, facilitating viral binding to the ACE2 receptor and its activation. Therefore, it promotes the same effects described for ACE-2. | (76–78) | |
| DPP4 | Astrocytes (in murine) | FroCx, SC, ACC, PG, SN, Hy, HiF, Amg, Cb, Acb, Cd and Pu. | It is strongly associated with MERS-CoV. The murine models for DPP4 receptor infected with MERS-CoV have shown neuronal damage and peripheral immune infiltrates. | (79–81) |
| TLR4 | Astrocytes, microglia | Cd, SN, Acb, Amg, Pu, SC, ACC, FroCx, y, HiF and Cb. | Molecular docking studies have demonstrated the binding of the native S protein of SARS-CoV-2 to TLR1, TLR4, and TLR6. However, TLR4 is most likely to recognize molecular patterns from SARS-CoV-2 to induce inflammatory responses. In CNS, it could promote the neuroinflammation environment. | (82, 83) |
| ATR1 | Neurons, astrocytes | PG, SN, Hy, Cb SC,HiF, Cd, Acb, Pu, Amg, FroCx and ACC | It has been suggested that SARS-CoV-2 causes lung damage by increasing Ang II production. The hyperactivation of Ang II/ATR1/ACE signaling results in increased expression of pro-inflammatory cytokines, macrophage activation, and possibly BBB dysfunction. | (84–87) |
| ITGB1 | Microglia | SC, PG, SN, Hy, HiF,Pu, Cd, Amg, FroCx, Acb, ACC and Cb. | It has been suggested that ITGB1 could bind to S protein through the RGD or KGE motif. ITGB1 mainly activates the MI3K/MAPK pathways, inducing an inflammatory response. | (24, 88, 89) |
| CatB and CatL | Microglia, neurons, astrocytes. | Cat B: FroCx, PG, SC, Cb, Hy, Acb, ACC, Cd, SN, Pu, HiF and Amg Cat: PG, SC, FroCx, Cb, SN, Hy, Cd, Acb, Pu, ACC, HiF and Amg | It has been suggested that S protein priming is partly dependent on the endosomal proteases, CatB and CatL. Nevertheless, TMPRSS2 is essential for viral entry into primary target cells and viral spread in the infected host. Also, CatB and CatL can contribute to the neuroinflammatory process. | (90, 91) |
| NLRP3 | Microglia, astrocytes, neurons | SC, FroCx, Acb, Hy, SN, ACC, HiF, Amg, Cd, PG, Pu, Cb | To date, it is unclear if SARS-CoV-2 activates the NLRP3 inflammasome. However, SARS-CoV expresses at least three proteins (viroporins) that activate the NLRP3 inflammasome: envelope (E), ORF3a, and ORF8b. The NLRP3 inflammasome activation could trigger inflammatory cell death. | (92–94) |
Neuroanatomic areas and nerve cells in which these receptors or proteins are expressed and their possible neuropathological effects.
Acb, nucleus accumbens; ACC, anterior cingulate cortex; ACE2, angiotensin-converting enzyme 2; Amg, amygdala; ATR1, angiotensin receptor type 1; BBB, blood-brain barrier; BECs, brain endothelial cells; Cat, cathepsin; Cb, cerebellum; Cd, caudate nucleus; DPP4, dipeptidyl peptidase-4; FroCx, frontal cortex; HiF, hippocampal formation; Hy, hypothalamus; ITGB1, integrin subunit beta 1; KGE, Lys-Gly-Glu; MAPK, Mitogen-Activated Protein Kinases; MERS-CoV, Middle East Respiratory Syndrome Coronavirus; MI3K, myo-inositol 3-kinase; MMPs, matrix metalloproteinases; NF-kB, nuclear factor kappa B; NLRP3, nucleotide-binding domain-, leucine-rich repeat-containing receptor, pyrin domain-containing 3; OLGs, oligodendrocytes; PG, pituitary gland; Pu, putamen; RGD, Arg-Gly-Asp; SARS-CoV-2, severe acute respiratory syndrome coronavirus 2; SC, spinal cord (cervical c-1), SN, substantia nigra; TLR, Toll Like Receptor; TMPRSS2, transmembrane protease serine 2.
The GTEx Analysis Release V8 (dbGaP Accession phs000424.v8.p2) was used to obtain the gene expression data (from highest to lowest expression) in several brain areas.
SARS-CoV-2 interaction with ACE2 could cause astrogliosis and microgliosis, increase BBB permeability, allowing monocyte and leukocyte infiltration to the CNS in multiple brain regions (98, 99). These areas include the olfactory bulb, choroid plexus, cerebral cortex, caudate/putamen, ventral striatum, thalamus, hypothalamus (paraventricular nuclei), spinal cord, hippocampus, frontal cortex (52, 95, 100), substantia nigra, middle temporal gyrus (64, 101), and other brain areas (Table 1). Since many viruses have neurotropic properties (102), SARS-CoV-2 could spread through neuroanatomically interconnected pathways (103) and lead to nerve cell dysfunction and neurodegeneration in the CNS.
Can the Systemic Inflammation by COVID-19 Trigger Neurovascular Disturbance?
In this section, we highlight evidence at the systemic level and locally in the respiratory tract tissue of patients with COVID-19. Since this virus induces lung pathology, the detailed information of other organs and systems such as the CNS has yet to be fully investigated. Therefore, the nerve signaling pathways proposed here are based on the systemic evidence from similar viruses.
Channappanavar and Perlman focused on the systemic immune response against pathogenic human coronaviruses such as SARS-CoV and Middle East respiratory syndrome CoV (MERS-CoV). They proposed that a dysregulated immune response in the host is responsible for triggering the pulmonary pathology and fatal clinical manifestations (104).
On the other hand, high levels of viral replication in the host could contribute to tissue damage. Two mechanisms might be responsible: first, the delayed induction of interferon responses and second, the production of interferon inhibitory proteins by the human CoVs. Therefore, early unmitigated viral replication could be responsible for the high and exaggerated production of cytokines and chemokines by infected alveolar epithelial cells, macrophages, and leukocytes infiltrated into the lung tissue, which leads to severe damage (Figure 2A steps 1–3) (104). Other investigators have concluded that COVID-19 is characterized by an extreme hyper-inflammatory process followed by hyper-coagulation (Figure 2A step 4) (105).
CRS is a systemic inflammatory response that can be triggered by SARS CoV-2 infection, characterized by a drastic increase in the levels of the pro-inflammatory cytokines (Figure 2A) (106). The CRS may induce a MODS in COVID-19 patients, which is characterized by acute failure of different organs such as the liver, kidney, heart, and as well as hematological, gastrointestinal, and neurological disorders (Figure 3) (107). Besides, it has been proposed that patients who died from severe COVID-19 have a significant endothelial affectation or “endothelitis,” which may be associated with MODS. It has been suggested that endothelial dysfunction in several organs may be triggered by the interaction between SARS-CoV-2 with ACE2 receptors that express endothelial cells and the subsequent inflammatory response (108, 109). This inflammatory response can contribute to increased vascular permeability, edema, and the synthesis of coagulation factors (110). From a meta-analysis, it has been reported that levels of D-dimer, an indicator of fibrinolysis, have been reported following severe infection by COVID-19 (111). The formation of clots could result in the occlusion of blood vessels and cerebral arteries, which can lead to cerebral venous thrombosis. Therefore, we assume that some of the symptoms and even neurological complications may be caused by the systemic cytokine storm and subsequent endothelium and BBB dysfunction (Figure 2). In this way, systemic hyper-inflammation caused by maladaptive innate immunity may trigger neurovascular function damage, a BBB rupture, and activate the CNS innate immune signaling pathways (112). This BBB disruption could promote immune cell infiltration (113) (Figure 2B steps 1 and 2). The intracerebral cytokine storm also could contribute to the BBB rupture (114, 115), leading to a vicious cycle of increasing pathology. These events may also be responsible for developing other neuropathies such as necrotizing encephalopathy or Guillain-Barré syndrome (GBS) (116, 117). The coagulopathy observed in COVID-19 could make patients prone to thrombotic cerebrovascular or bleeding events (118).
On the other hand, microglia and astrocytes are the main cell lineages that mediate immunological processes within the CNS. Thus, microglia, the macrophage of the CNS par excellence, can also promote states of hyper-inflammation that exacerbate hypercoagulation by infiltration of professional immune cells and coagulation elements. Nevertheless, we hypothesize that SARS-CoV-2 could activate the microglia and, subsequently, induce the reactivation of A1 astrocytes via secreting IL-1α, TNF, and the complement component 1q (C1q), as occurs in other neurological diseases (119) (Figure 2B step 3). Besides, exposure to the viruses or their components promotes the expression and activation of Toll-like receptors (TLR) in astrocytes. This signaling promotes the production and release of pro-inflammatory mediators and induces inflammatory responses in the CNS (Figure 2B step 3), eliminating the pathogen as demonstrated for Flavivirus infections (82, 120). Therefore, this pathological signaling causes neuronal degeneration and dysfunction of the nerve cells short or long term.
Viroporins belong to a family of small transmembrane proteins that include CoV protein E (121, 122), which could generate neurotropism of SARS-CoV. According to previous studies, viroporins can promote the activation of the NLRP3 inflammasome (123, 124). The NLRP3 inflammasome is a subcellular multiprotein complex that is highly expressed in several nerve cells and CNS areas (Table 1). Activation of the NLRP3 occurs after infection by the influenza A virus and SARS-CoV (125) (Figure 2B step 4). After NLRP3 inflammasome activation, caspase-1 and other non-canonical inflammasome caspases (caspase-4, caspase-5, or caspase-11) activate gasdermin-D (GSDMD), which subsequently forms pores in the cell membrane. These pores facilitate the secretion of IL-1β and IL-18 and, importantly, they also enable the simultaneous influx of Na+ and water molecules, facilitating neuroinvasion by causing excessive cellular swelling, membrane rupture, and subsequent pyroptosis, an inflammatory form of cell death (126, 127). Therefore, it is possible that pyroptosis may occur in nerve cells (Figure 2B step 4).
Neurological and Neuropsychiatric Manifestations, Diagnostic, and Treatment in Patients With COVID-19
The respiratory symptoms caused by the SARS-CoV-2 virus are still the most readily identified and studied. However, neurological manifestations are beginning to take on unquestionable importance, mainly in the critically affected patient. Our understanding of the long-term neurological symptoms is limited and presents a real challenge (13, 14, 62, 128). A physiopathological explanation for the neurological and neuropsychiatric manifestations of COVID-19 has yet to be found. Although there are hypotheses about the direct effects of SARS-CoV-2 on the CNS and PNS, evidence suggests that these effects can be attributed to other causes such as: (1) the impact of the systemic inflammatory response caused by the virus and (2) the underlying comorbidities of the patients (62, 129, 130). Patients with mild COVID-19 have been reported to have non-specific neurological disorders such as headache and myalgias, dizziness, dysgeusia, and anosmia with variations in their prevalence (Table 2) (13, 14).
Table 2.
SARS-CoV-2 infection in the central and peripheral nervous system: clinical manifestations, mechanism of pathogenicity, laboratory, and clinical findings and suggested treatment.
| Clinical manifestation | The probable mechanism of pathogenicity | Laboratory and/or clinical alterations | Treatment or recommendations | References |
|---|---|---|---|---|
| Central nervous system | ||||
| Headache: occurs in ~70% of patients, with an average duration of 3 days. | (1) Direct viral invasion of the trigeminal nerve endings in the nasal or oral cavity. (2) An increase in the levels of peptides related to the circulating calcium gene has been linked to the trigeminal vascular activation. | The use of neurological and laboratory imaging techniques is only recommended if the headache is associated with focal neurological symptoms. | (1) NSAIDs and steroids are not recommended as they can exacerbate COVID-19 symptoms. (2) Anticonvulsants may offer benefits. | (131–133) |
| Delayed awakening: has been observed in some patients after ventilation for COVID-19-related ARDS. | A relationship between posterior circulation inflammation and brainstem function may be related to altered consciousness. | (1) Brain MRA: an increase in the abnormal contrast has been observed in the arterial wall associated with endotelialitis. (2) EEG: non-specific changes have been observed. (3) In serum and CSF: oligoclonal bands have been observed. | The use of IV methylprednisolone has been proposed for 5 days, followed by decreasing doses of prednisone. | (130) |
| Encephalopathy: One study Liotta et al. (134) determined that it was present in about a third of patients, and was associated with increased mortality. | It has been proposed that they may be involved in toxic-metabolic processes such as hypoxemia, ROS production, and organ failure. | MRI: intensity changes in the leptomeningeal spaces, in the mesial temporal lobe, and the hippocampus, as well as frontotemporal hypoperfusion. | The use of low potency antipsychotic agents and alpha-2 agonists has been proposed to control psychomotor agitation. | (134–136) |
| Ischemic stroke event: is a life-threatening complication and is associated with cardioembolic events. | (1) Elevated inflammation, DIC, and hypoxia have been associated with a state of hypercoagulability. (2) Complement activation is associated with microvascular damage leading to thrombotic injury. | (1) The neuroimaging patterns observed are extensive vessel thrombosis, embolism, or stenosis, followed by affected multiple vascular territories. (2) Laboratory studies have revealed an increase of D-dimer, fibrinogen, antiphospholipid antibody levels. | Prophylactic or therapeutic anticoagulation therapy, as well as thrombectomy, have been recommended. | (62, 137) |
| Hemorrhagic stroke: has been attributed to COVID-19 and risk factors as anticoagulation, trauma, and hypertension. | Lupus anticoagulant and antiphospholipid antibodies have been suggested to play a role in its pathophysiology. | Imaging studies have revealed microhemorrhage foci, hematomas larger than 5cm, surrounding edema, and even descending hernia. | Reduce risk factors that affect hypertension, aneurysm, and states of anticoagulation. | (62) |
| Peripheral nervous system | ||||
| Olfactory disorders: present around 86% of COVID-19 patients: anosmia (79%), hyposmia (20.4%), phantosmia (12%), and parosmia (32%) Lechien et al. (138). | (1) Nasal epithelial damage is characterized by a reduced number of ORs and abnormal dendrites that do not reach the epithelial surface or lack sensory cilia. (2) Substitution of ONE with metaplastic squamous epithelium. (3) Inflammation can lead to impairment of ORs and also damage of olfactory neurons. | MRI has shown abnormalities in the signaling of one or both olfactory bulbs, edema of the olfactory bulb, and microhemorrhage in one of the olfactory bulbs. | The most widely used treatments for olfactory dysfunction are saline nasal irrigations, nasal corticosteroids, oral corticosteroids, vitamins, and trace elements. | (138–141) |
| Gustatory disorders: present around 88% of COVID-19 patients: hypogeusia (79%) or dysgeusia (21%) Lechien et al. (138) | (1) Diffuse expression of ACE2 receptors (modulation of taste perception) in the oral mucosa, particularly in the tongue. (2) SARS-CoV-2 can bind to sialic acid receptors, accelerating the degradation of taste particles. | Recent evidence suggests that imaging or laboratory studies are not usually done on patients who only manifest gustatory disorders. | Treatment for these disorders has not been established; however, l-carnitine or trace elements and vitamins have been used. | (138, 142) |
| Neuromuscular disorders: myalgia and fatigue affect between 44 and 70% of patients. About 10% of patients have a skeletal muscle injury. | (1) SARS-Cov-2 could trigger viral myositis. (2) Alteration in the expression of ECA2 in skeletal muscle. (3) Skeletal muscle damage from cytokine storm. | (1) Elevated serum creatine kinase levels. (2) Muscle injury has been associated with multiple organ damage, such as liver dysfunction (increased levels of LDH, ALT, and AST) and kidney (increased levels of blood urea nitrogen and creatinine). | The use of corticosteroids has resulted in benefits. | (129, 143) |
| Guillain-Barre Syndrome GBS: has been associated with COVID-19. Interestingly, the interval between the onset of COVID-19 symptoms and the first symptoms of GBS has ranged from 5 to 10 days. | (1) It has been proposed that it serves the same mechanisms as typical GBS, consisting of demyelination of peripheral nerve roots. (2) Peripheral nerve damage can be caused by the immune response to SARS-CoV-2, driven by the production of autoreactive antibodies (anti-ganglioside). | (1) Hematological and biochemical examinations have shown leukocytosis, leukopenia, thrombocytosis, thrombocytopenia, and elevated levels of CRP. (2) CSF tests have shown cytological dissociation of albumin. (3) EMG has been associated with a demyelinating process. (4) MRI has revealed an enhancement in the caudal nerve roots and the facial nerve. | The therapeutic protocol to GBS associated with COVID-19 has been typically used for this pathology: IV immunoglobulin or plasma exchange, supportive care, and antiviral drugs. | (144–146) |
ACE2, angiotensin-converting enzyme 2; ALT, alanine transaminase; ARDS, acute respiratory distress syndrome; AST, aspartate aminotransferase; CNS, central nervous system; CRP, C-reactive protein; CSF, cerebrospinal fluid; DIC, disseminated intravascular coagulation; EEG, electroencephalography; EMG, electromyography; GBS, Guillain-Barre syndrome; IV, intravenous; LDH, lactate dehydrogenase; MRA, magnetic resonance angiography; MRI, magnetic resonance imaging; NSAIDs, non-steroidal anti-inflammatory drugs; ONE, olfactory neuroepithelium; ORs, olfactory receptors; ROS, reactive oxygen species.
Some studies point to headache as the most common neurological symptom and often as the only symptom of COVID-19 (129, 147). However, other authors have defined the headache as a consequence of systemic disease. It has been suggested that the chronic release or exposure of vasoactive peptides such as Calcitonin Gene-Related Peptide (CGRP; pain and migraine-related peptide) (148) can activate trigeminal sensory fibers and thus modulate the transmission of impulses related to headache (149). Besides, in COVID-19, a close link between cytokine storm and headache has been proposed, due to the release of the vasoactive peptides (150).
In contrast, for hospitalized patients, encephalopathy with neuropsychiatric manifestations such as delirium and agitation have been observed. There has also been a considerable increase in the reports of patients with neuromuscular diseases, among which are GBS with some of its variants and several rhabdomyolysis cases. However, it has not been possible to find a clear relationship between these manifestations and COVID-19. An increasing incidence of neurological manifestations has been observed in COVID-19-infected patients that have been associated with severe health conditions and prolonged hospital stays (129, 134). However, there are also reports of neurological manifestations in outpatients with COVID-19 infection (129, 138). Therefore, it is difficult to determine the incidence of each of the neurological manifestations due to the different screening methods applied for each reported case.
Neurological disorders such as multiple sclerosis (MS), encephalopathy, and GBS, have been associated with SARS-CoV2. In some cases, CNS demyelination has occurred shortly after SARS-CoV-2 infection, suggesting a causal relationship between these two pathologies (151). Viruses, such as the Epstein-Barr virus (EBV), have been linked to MS, with high titers of EBV antibodies found in MS patients. Viral induced demyelination could be a direct result of viral infection of oligodendrocytes, which leads to cell death and myelin degeneration, or to the exacerbated inflammatory response caused by virus replication (152, 153). The cytokine storm caused by SARS-CoV-2 may cause the activation of glial cells and the start of the demyelination process (154). Conversely, other studies suggest that SARS-CoV-2 could act as an accelerating factor for MS but not the trigger for the disaese (155). Likewise, several case reports have reported the appearance of GBS after SARS-CoV-2 infection (156–158). Although hypoxic/metabolic changes caused by intense inflammatory response against the virus together with the presence of comorbidities, may result in encephalopathy (159) there is still insufficient evidence to prove that SARS-CoV-2 virus infection invades the CNS directly to provoke encephalopathy (151). In the same way, despite the complications associated with SARS-CoV-2 infection in patients with GBS, there is no clear evidence yet that COVID-19 initiates GBS (151).
Cerebral events have been associated with SARS-CoV-2 patients, with cerebral ischemic events being the most frequent. Cerebral hemorrhages and microhemorrhages are also noticed (62, 144) (Table 2).
As discussed previously, the cranial nerves might also be susceptible to a direct or indirect injury caused by SARS-CoV-2. According to a recent study, about 86 and 88% of patients with COVID-19 develop olfactory and gustatory alterations, respectively (138). These findings might be specific for SARS-CoV-2 infection and be useful to distinguish them from other causes. Interestingly, the presence of these dysfunctions can precede the onset of respiratory symptoms (160, 161) and may predict a mild clinical course of the disease (162) (Table 2). Besides, it has been proposed that pericytes of the olfactory bulb, which express high levels of the ACE2 receptor, may be responsible for triggering the cytokine storm and thus causing olfactory disorders in COVID-19 patients (163).
On the other hand, neuroimaging data could help us understand the pathological effects of SARS-CoV-2 in the CNS and PNS. Unfortunately, published brain imaging findings from confirmed COVID-19 patients are currently scarce and limited to small case series. However, it has been possible to correlate them with the potential pathophysiological mechanisms involved. For example, in a recent study, it was shown that patients with COVID-19 presented multifocal petechial hemorrhages associated with BBB rupture (164). In another study, microhemorrhages and macrohemorrhages were associated with posterior reversible encephalopathy syndrome (165) (Table 2). Although the underlying mechanism of brain abnormalities detected through neuroimaging remains to be understood, these findings provide further evidence that CNS damage can occur in COVID-19 patients. The correct understanding of pathophysiological mechanisms of neurological manifestations may reveal potential therapeutic targets (Table 3). Depending on the neurological complications associated with COVID-19, treatments would need to be adjusted accordingly (Table 2).
Table 3.
Current drugs used against COVID-19.
| Drug | Mechanism of action | Results of clinical case reports | Adverse effects | Dose | References |
|---|---|---|---|---|---|
| Antiviral drugs | |||||
| Remdesivir | The prodrug, belonging to the group of nucleotide analogs, generates an active metabolite capable of entering cells and inhibits viral RNA polymerase. Inhibitory capacity against SARS-CoV-2 in vitro has been observed*. | Decreased recovery time, disease progression, as well as mortality compared to placebo. | -Infusion-related hypotension - Hepatotoxic - Nephrotoxic - Gastrointestinal symptoms |
-First dose of 200 mg -100 mg/day for 5–9 days. | (166) |
| TMPRSS2 antagonist | |||||
| Camostat | Produces GBPA, that inhibits many of the serine proteases that SARS CoV and SARS-CoV-2 use for virus-to-host cell membrane fusion, like TMPRSS2**. | Reduces the likelihood of serious infection, as well as morbidity and mortality. | -Eruption - Pruritus - Oedema - Urticaria |
It has been used at different doses in humans and other pathologies. e.g., : 200 mg every 8 h | (167) |
| Nafamostat mesylate | Inhibited SARS-CoV-2 S protein-mediated entry into host cells with about 15-fold-higher efficiency than camostat, with a 50% effective concentration. | In combination with Favipiravir has shown a decrease in mortality. | Hyperkalemia | 0.2 mg per kg/hour by continuous IV infusion, for 14 days. | (168, 169) |
| Monoclonal antibodies | |||||
| Tocilizumab | IL-6 receptor antagonist | May reduce the hospital stay, the need for ICU admission, and the need for invasive mechanical ventilation. |
- Increased risk of secondary infections. - Hypersensitivity reactions - Neutropenia and thrombocytopenia - Hepatotoxicity |
>75 kg: 600 mg single dose <75 kg: 400 mg single dose*** | (170) |
| Anakinra | IL-1 receptor antagonist | Reduced both needs for invasive mechanical ventilation and mortality in severe COVID-19 patients. |
- Elevation of liver enzymes three times higher than their reference value. - Possible thromboembolic events. |
100 mg every 6 h for a maximum of 15 days. | (171, 172) |
| Mavrilimumab | Binds to GM-CSFRα**** and disrupts downstream signaling. | Fast clinical improvement, decrease both the need for mechanical ventilation and mortality. | No adverse reactions to the infusion were observed. | 6 mg/kg single dose. | (173) |
| Steroids | |||||
| Dexamethasone |
- Anti-inflammatory action. - Inhibits phospholipase A2 and, consequently, prostaglandin, thromboxane, and leukotriene synthesis - Suppresses leukocyte migration - Recovers the BBB by upregulation of ZO-1 tight junction protein |
Decreased mortality in patients requiring oxygen therapy and mechanical ventilatory support when treatment is initiated 7 days after symptom onset. |
- Hyperglycemia - Increased risk of bacterial and fungal infections. |
6 mg/day for 10 days. | (174) |
GBPA, 4-[4-guanidinobenzoyl-oxy] phenylacetic acid; GM-CSF, Granulocyte-macrophage colony-stimulating factor (GM-CSF); TMPRSS2, Transmembrane serine protease 2.
Inhibitory activity against SARS-CoV-1 and MERS-CoV has been demonstrated.
The high expression of TMPRSS2 in different brain areas could be a potential therapeutic target for neurological manifestations and complications.
According to safety criteria and clinical trial data.
GM-CSF is a cytokine with a cardinal role in inflammation modulation. Ligand binding to the GM-CSF receptor-α (GM-CSFRα) activates multiple pro-inflammatory pathways and, in macrophages and neutrophils, results in increased secretion of pro-inflammatory cytokines.
Neurohistopathological Findings by COVID-19
The histopathological analysis of nervous tissue of patients who presented neurological complications and died due to COVID-19 is undoubtedly precious to our understanding of the pathophysiology and potential therapeutic strategies (Table 4).
Table 4.
Neurohistopathological findings in patients infected with SARS-CoV-2 and their association with neurological manifestations.
| Characteristics of the patients | Tissue and PMI | Histopathological findings | Neurological manifestations | References |
|---|---|---|---|---|
| Central nervous system | ||||
|
n = 18 age range: 53–75 years comorbidities: AF, ALL, BPH, CAD, CKD, COPD, DM, ESRD on HD, EtOH use disorder, HF, HTN, ILD, MGUS, NHL, OCD, OSA, PPV, PVD, RA-SLE. |
Inferior-frontal lobe with olfactory tract/bulb, corpus callosum, hippocampus, occipital lobe, anterior basal ganglia, thalamus, cerebellum, midbrain, pons, and medulla. PMI: NS. | Acute hypoxic-ischemic injury with neuronal loss in the cerebral cortex, hippocampus, and cerebellar Purkinje cell layer. Arteriolosclerosis with perivascular rarefaction, a microglial nodule, and perivascular inflammation with scattered microglia were also detected. | It is associated with the confusional state, myalgia, headache or, hypogeusia. | (175) |
|
n = 6 age range: 58–82 years comorbidities: EtOH use disorder, HTN, COPD, CKD, PHT, PVD, CAD, AF. |
Hippocampus, neocortex, cerebellum, and brainstem nuclei. PMI: NS. | Lymphocytic panencephalitis and meningitis. Neuronal cell loss and axon degeneration in the dorsal motor nuclei of the CN X and V, NTS, dorsal raphe nuclei, and medial longitudinal fasciculus. | Associated with altered consciousness. | (176) |
| n = 1 age: 73 years commorbidities: DM and HTN. | Cortex, hippocampus, amygdala, striatum. PMI: NS. | Cerebellar hemorrhage, acute infarcts, global hypoxic changes with scattered hypereosinophilic shrunken neurons in the cerebral cortex, striatum, thalamus, amygdala, hippocampus, and the Purkinje cell layer. | Headache, nausea, vomiting, and loss of consciousness. | (177) |
| Cranial nerves and peripheric nervous system | ||||
|
n = 33 age range: 67–79 years commorbidities: DM, HTN, CVD, HLD, CKD, PS and dementia. |
Olfactory mucosa, bulb and tuber, oral mucosa, trigeminal ganglion, medulla oblongata, and cerebellum. PMI: NS. | High levels of viral SARS-CoV-2 RNA (RT–qPCR) and protein within the olfactory mucosa. Lower levels were found in the cornea, conjunctiva, and oral mucosa; and in only a few COVID-19 autopsy cases, the cerebellum was positive for SARS-CoV-2. | Alterations of smell and taste perception, impaired consciousness, headache, and behavioral changes | (178) |
| n = 2 age: 51 and 94 years commorbidities: COPD, IHD and AML | Glossopharyngeal, vagal nerves and other brain areas. PMI: 3.3 days | SARS-CoV-2 viral proteins mapped to isolated cells. | Ageusia | (179) |
|
n = 21 age range: 41–78 years commorbidities: DM, CVD, COPD, asthma, ASM and AHM. |
Olfactory bulbs, NTS and other brain areas. PMI: NS. | Extensive inflammation and infiltrating immune cells. | Anosmia and dampening of the respiratory system. | (180) |
AF, atrial fibrillation; AHM, active hematological malignancy; ALL, acute lymphoblastic leukemia; AML, acute myeloid leukemia; ASM, active solid malignancy; BPH, benign prostatic hyperplasia; CAD, coronary artery disease; CKD, chronic kidney disease; CN, cranial nerves; COPD, chronic obstructive lung disease; CVD, cardiovascular disease; DM, diabetes mellitus; ESRD on HD, end stage renal disease on dialysis; EtOH use disorder, alcohol use disorder; HF, heart failure; HLD, hyperlipidemia; HTN, hypertension; IHD, ischaemic heart disease; ILD, interstitial lung disease; MGUS, monoclonal gammopathy of undetermined significance; n, number of patients; NHL, non-Hodgkin lymphoma; NS, not specified; NTS, nucleus tractus solitarius; OCD, obsessive compulsive disorder; OSA, obstructive sleep apnea; PHT, pulmonary hypertension; PMI, postmortem interval; PS, prior stroke; PVD, peripheral vascular disease; RA-SLE, rheumatoid arthritis - systemic lupus erythematosus; RT-qPCR, reverse transcription-quantitative polymerase chain reaction.
Solomon et al. analyzed nervous tissue from 18 patients infected with SARS-CoV-2 who had also presented with certain comorbidities such as DM, hypertension, cardiovascular disease, hyperlipidemia, chronic kidney disease, and dementia. The histological examination (Table 4) revealed a greater number of copies of SARS-CoV-2, acute hypoxic-ischemic injury, neuronal loss, and perivascular inflammation in several brain areas, and even pathological features of Alzheimer's disease (AD) were observed (175). A different case report described the brain from a 73-year-old man with unspecified neurological manifestations (Table 4), hypertension and DM and positive for SARS-CoV-2 with cranial computed tomography. The results showed right cerebellar intra-parenchymal hemorrhage, edema, medulla compression, and tonsillar herniation. After 18 h without improvement, the patient died of palliative extubation. Brain histopathology revealed severe global hypoxic changes with scattered hypereosinophilic shrunken neurons in several brain areas and mild perivascular inflammatory infiltrates (Table 4) (177). This study also suggested a preference of the virus to the cerebellar Purkinje cell layer. In addition, astrogliosis was noted in the superior frontal and orbital cortices, while microglial activation in the cortex was not evident (177).
A study focused on describing the SARS-CoV-2 tropism within the olfactory mucosa to the CNS examined autopsy material from 33 patients positive for the virus. The authors showed viral RNA for SARS-CoV-2 within the olfactory mucosa sampled directly beneath the cribiform plate. They also found viral RNA in anatomically distinct regions such as cornea, conjunctiva and oral mucosa. Using immunohistochemistry, in situ hybridization, and electron microscopy, they suggested that SARS-CoV-2 neuroinvasion to the CNS occurs via axonal transport, thus explaining the well-documented neurological symptoms (Table 4) (178). The authors also proposed that SARS-CoV-2 infection in the cerebellar region may occur by the migration of the virus-carrying leukocytes across the BBB, without directly connecting this area to the olfactory mucosa.
Other cranial nerves have been considered as the route for entrance of the virus to the CNS (Figure 3) (181, 182). Regarding ageusia, the pathogenesis may involve an alteration in the glossopharyngeal, facial, vagus nerve, or the nucleus tractus solitarii (NTS), at the brainstem level (183). In an immunohistochemistry analysis of the cranial nerves from two individuals, SARS-CoV-2 and viral proteins were found within the medulla oblongata and in both glossopharyngeal and vagal nerves from the lower brainstem (179), suggesting these areas as a potential route for virus entry into the CNS and peripheral tissue (Table 4).
Other authors found hypereosinophilia or nuclear and cytoplasmic condensation of neurons in the cerebrum and cerebellum of severe COVID-19 patients due to hypoxic brain changes (Table 4). The olfactory bulb histopathological analysis showed many activated microglia with enlarged bodies and T-cell extravasation into the parenchyma and elevated levels of reactive astrocytes (180). Interestingly, the NTS showed astrogliosis and a massive microglial activation with the formation of a microglia nodule and T cells in the leptomeninges of the medulla oblongata (180). This implies extensive inflammation in this area, which results in a dysregulation of the respiratory system (184). One of the main limitations of these studies is that it is not clear whether the histopathological findings are the result of patients' comorbidities/aging, or due to SARS-CoV2 neuro-infection. Further investigations are necessary to make the corresponding comparison with healthy subjects with appropriate age ranges and to understand the neuropathological mechanism of SARS-CoV-2 and its relationship with neurological manifestations and patient comorbidities.
The Potential Role of SARS-CoV-2 in the Pathogenesis of Neurodegenerative Diseases
The SARS-CoV-2 neurotropism has already been documented in several reports (Table 2) (185–187). However, it remains unknown whether SARS-CoV-2 contributes to neurodegenerative pathogenesis. It has been hypothesized that viruses can cause neurological problems by affecting neurotransmitter release, lysing the cells, inducing apoptosis, commanding neuronal transcriptional pathways or indirectly activating the immune response (188).
Neuroinvasive animal CoVs, such as the porcine hemagglutinating encephalitis virus (PHEV) or MHV have been shown to induce different types of neuropathology. Similarly, human CoVs, such as HCoV-229E and HCoV-OC43, have been implicated in establishing or exacerbating neurodegenerative diseases (189–192).
AD is the most common cause of dementia among the elderly. Neuropathological hallmarks of AD include the neurofibrillary tangles, consisting of intraneuronal and hyperphosphorylated tau, and the extracellular accumulation of amyloid β-peptide (Aβ) in the brain parenchyma in the form of neuritic plaques (193, 194). The neurovascular unit (NVU) and BBB dysregulation are also critical pathophysiological events in neurodegenerative diseases, including AD. Previous studies have suggested a relationship between AD and infectious agents. Chlamydia pneumoniae, Helicobacter pylori, Borrelia burgdorferi, and herpes simplex virus have been reported in post-mortem AD brain (195) and a relationship between virus infection and Aβ has been suggested. Soscia et al. noticed that Aβ exerted antimicrobial activity against relevant microorganisms and was modulated in response to some environmental stressors. Thus, transient viral infection could initiate or accelerate Aβ accumulation in the brain and neuronal damage (Figure 2B steps 5 and 6) (196). ACE2 can induce an increase of nitric oxide (NO) in the brain, which becomes neurotoxic. NO and other reactive species, which could be produced as a consequence of viral internalization and impairment of cell organelles (mitochondria, lysosomes), could, in turn, increase misfolding and aggregation of cellular proteins (197).
It has been proposed that SARS-CoV-2 could increase the hyperphosphorylation of tau in the axonal region (52, 198–200), promoting disassembly of microtubules and, subsequently, neuronal degeneration (Figure 2B steps 5 and 6) (201). Likewise, it has been suggested that persistent CoV infections can induce a neuroimmune response and a pro-inflammatory state, and activate glial cells (202). Microglial cells may be chronically activated by a single stimulus, such as pathogen infection, resulting in slow and progressive neuronal loss through multiple neurotoxic factors (203). Interferon (IFN), which has a role in mediating AD pathology, directly activates microglia and stimulates a pro-inflammatory response derived from SARS-CoV-2 infection (204). Therefore, it seems that the neurotropism of SARS-CoV-2 can lead to the activation of microglial cells, trigger chronic neuroinflammation, and finally, neurodegeneration (Figure 2B).
Finally, it has been found that ACE2 is upregulated in the cerebral vasculature of dementia cases. ACE2 increases the intracellular level of angiotensin 2, causing vasoconstriction and promoting brain degeneration (205). Buzhdygan et al. demonstrated that S1 could promote BBB alteration in an advanced 3D microfluidic model of the BBB, being able to induce different types of neuropathology (98).
Like AD, viral agents have been associated with parkinsonism disorders. These include the post-encephalitic parkinsonism linked to the 1918 influenza A H1N1 pandemic (206) and the parkinsonism associated with Epstein Barr, Coxsackie, West Nile, herpes and the human immunodeficiency (HIV) viruses (207–209). Parkinson's disease (PD) is the second most common and fastest-growing neurodegenerative disorder (210). It is characterized by dopaminergic neuronal loss in the substantia nigra pars compacta and the accumulation of misfolded α-synuclein (α-syn), which is found as intracytoplasmic inclusions called “Lewy bodies” (211). SARS-CoV-2 could play a role in the epidemiology of PD, since pro-inflammatory events triggered by viral infections could act as predisposing factors to the development of PD (Figure 2B steps 5 and 6) (Table 2) (212–214). This inflammatory environment can trigger the long-term neuronal loss, misfolding, aggregation, and spread of α-syn through the CNS (215, 216). Interestingly, it has been proposed that α-syn plays an essential role in response to infection, promoting a higher expression of α-syn, as occurs in the West Nile virus encephalitis (217, 218). Furthermore, α-syn aggregation can activate microglia, favoring the pro-inflammatory response and cellular damage signals, leading to slow and progressive neuronal death (219). However, it remains unknown whether SARS-CoV-2 could contribute to neurodegenerative pathogenesis, or whether it only uses the CNS as a reservoir, making it difficult for the virus to replicate, due to the low level of ACE2 receptors expressed in CNS (220).
Conclusion
COVID-19 pandemic has become a real challenge for the scientific community around the world. Although SARS-CoV-2 mainly affects the respiratory tract, more evidence suggests that this virus can also invade the CNS causing neurological manifestations. The possible routes of SARS-CoV-2 neuroinvasion include: (1) the hematopoietic pathway via the BBB, (2) via the B-CSF, (3) via retrograde axonal transport through the cranial nerves, and (4) via the circumventricular organs. Once the virus enters the CNS, it binds to cell receptors, including ACE2. This receptor is expressed in several brain areas and in both neuronal and non-neuronal cell types. The binding of SARS-CoV-2 with ACE2 can promote neuroinflammation, hypercoagulation, microhemorrhages, BBB dysfunction, generation of reactive species, phosphorylation of tau, protein misfolding and aggregation, and neuronal death, features that are closely related to the appearance or progression of neurodegenerative diseases. Further studies on the molecular changes in the brain triggered by SARS-CoV-2 infection would facilitate timely diagnosis and therapeutic approaches.
Author Contributions
MP-H, JL-M, and LS-R contributed to the idea formulation, reviewing of the literature, and writing and revision of the manuscript. YF-M, CH, MV-R, AL-A, PM-G, BC-C, VB-A, RA-P, CC-T, and JD-G contributed to reviewing of the literature and revision of the manuscript. All authors contributed to the article and approved the submitted version.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
We want to express our gratitude to the Union Medical University Clinic, Dominican Republic, for their support and collaboration in the development of this research project. We also want to express our gratitude to the Mexican families who have donated the brain of their loved ones affected with Alzheimer's disease and made our research possible. This work is dedicated to the memory of Professor Dr. José Raúl Mena López†.
1Deceased.
Funding. This work was supported by Fondo Nacional de Ciencia, Tecnologia, FONDOCyT, from the Ministry of Higher Education, Science and Technology, Dominican Republic (2015-3A2-127 to MP-H and 2018-2019-2A3-208 to JL-M and MP-H).
References
- 1.Allam Z. Chapter 1 - The First 50 days of COVID-19: A Detailed Chronological Timeline and Extensive Review of Literature Documenting the Pandemic In: Surveying the Covid-19 Pandemic and its Implications. 1–7 10.1016/B978-0-12-824313-8.00001-2 [DOI] [Google Scholar]
- 2.World Health Organization . Coronavirus Disease (COVID-19). Situation Report. Available online at: https://www.who.int/docs/default-source/coronaviruse/situation-reports/20200730-covid-19-sitrep-192.pdf?sfvrsn=5e52901f_8
- 3.Zhang W, Du RH, Li B, Zheng XS, Yang XL, Hu B, et al. Molecular and serological investigation of 2019-nCoV infected patients: implication of multiple shedding routes. Emerg Microbes Infect. (2020) 9:386–9. 10.1080/22221751.2020.1729071 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Organization WH . COVID-19. (2021). Available online at: https://covid19.who.int/ (accessed 22 February, 2021).
- 5.Wu Y-C, Chen C-S, Chan Y-J. The outbreak of COVID-19: an overview. J Chinese Medical Assoc. (2020) 83:217–20. 10.1097/JCMA.0000000000000270 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Guan WJ, Ni ZY, Hu Y, Liang WH, Ou CQ, He JX, et al. Clinical characteristics of coronavirus disease 2019 in China. N Engl J Med. (2020) 382:1708–20. 10.1101/2020.02.06.20020974 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Wang D, Hu B, Hu C, Zhu F, Liu X, Zhang J, et al. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus-infected pneumonia in Wuhan, China. JAMA. (2020) 323:1061–9. 10.1001/jama.2020.1585 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Kanne JP, Little BP, Chung JH, Elicker BM, Ketai LH. Essentials for radiologists on COVID-19: an update-radiology scientific expert panel. Radiology. (2020) 296:E113–4. 10.1148/radiol.2020200527 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Castelli V, Cimini A, Ferri C. Cytokine storm in COVID-19: “when you come out of the storm, you won't be the same person who walked in.” Front Immunol. (2020) 11:2132. 10.3389/fimmu.2020.02132 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Jin JM, Bai P, He W, Wu F, Liu XF, Han DM, et al. Gender differences in patients with COVID-19: focus on severity and mortality. Front Public Health. (2020) 8:152. 10.3389/fpubh.2020.00152 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Guan WJ, Liang WH, Zhao Y, Liang HR, Chen ZS, Li YM, et al. Comorbidity and its impact on 1590 patients with COVID-19 in China: a nationwide analysis. Eur Respir J. (2020) 55:2020. 10.1183/13993003.00547-2020 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Huang C, Wang Y, Li X, Ren L, Zhao J, Hu Y, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. (2020) 395:497–506. 10.1016/S0140-6736(20)30183-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Guadarrama-Ortiz P, Choreno-Parra JA, Sanchez-Martinez CM, Pacheco-Sanchez FJ, Rodriguez-Nava AI, Garcia-Quintero G. Neurological aspects of SARS-CoV-2 infection: mechanisms and manifestations. Front Neurol. (2020) 11:1039. 10.3389/fneur.2020.01039 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Puccioni-Sohler M, Poton AR, Franklin M, Silva SJD, Brindeiro R, Tanuri A. Current evidence of neurological features, diagnosis, and neuropathogenesis associated with COVID-19. Rev Soc Bras Med Trop. (2020) 53:e20200477. 10.1590/0037-8682-0477-2020 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Baig AM. Neurological manifestations in COVID-19 caused by SARS-CoV-2. CNS Neurosci Ther. (2020) 26:499–501. 10.1111/cns.13372 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Conti P, Ronconi G, Caraffa A, Gallenga CE, Ross R, Frydas I, et al. Induction of pro-inflammatory cytokines (IL-1 and IL-6) and lung inflammation by Coronavirus-19 (COVI-19 or SARS-CoV-2): anti-inflammatory strategies. J Biol Regul Homeost Agents. (2020) 34:327–31. 10.23812/CONTI-E [DOI] [PubMed] [Google Scholar]
- 17.Diao B, Wang C, Tan Y, Chen X, Liu Y, Ning L, et al. Reduction and functional exhaustion of T cells in patients with coronavirus disease 2019 (COVID-19). Front Immunol. (2020) 11:827. 10.3389/fimmu.2020.00827 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Ellul MA, Benjamin L, Singh B, Lant S, Michael BD, Easton A, et al. Neurological associations of COVID-19. Lancet Neurol. (2020) 19:767–83. 10.1016/S1474-4422(20)30221-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Coronaviridae Study Group of the International Committee on Taxonomy of V . The species Severe acute respiratory syndrome-related coronavirus: classifying 2019-nCoV and naming it SARS-CoV-2. Nat Microbiol. (2020) 5:536–44. 10.1038/s41564-020-0695-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Ludwig S, Zarbock A. Coronaviruses and SARS-CoV-2: a brief overview. Anesth Analg. (2020) 131:93–6. 10.1213/ANE.0000000000004845 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Woo PC, Lau SK, Huang Y, Yuen KY. Coronavirus diversity, phylogeny and interspecies jumping. Exp Biol Med. (2009) 234:1117–27. 10.3181/0903-MR-94 [DOI] [PubMed] [Google Scholar]
- 22.Li F. Structure, function, and evolution of coronavirus spike proteins. Annu Rev Virol. (2016) 3:237–61. 10.1146/annurev-virology-110615-042301 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Huang Y, Yang C, Xu XF, Xu W, Liu SW. Structural and functional properties of SARS-CoV-2 spike protein: potential antivirus drug development for COVID-19. Acta Pharmacol Sin. (2020) 41:1141–9. 10.1038/s41401-020-0485-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Sigrist CJ, Bridge A, Le Mercier P. A potential role for integrins in host cell entry by SARS-CoV-2. Antiviral Res. (2020) 177:104759. 10.1016/j.antiviral.2020.104759 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Li W, Moore MJ, Vasilieva N, Sui J, Wong SK, Berne MA, et al. Angiotensin-converting enzyme 2 is a functional receptor for the SARS coronavirus. Nature. (2003) 426:450–4. 10.1038/nature02145 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Lam SD, Bordin N, Waman VP, Scholes HM, Ashford P, Sen N, et al. SARS-CoV-2 spike protein predicted to form complexes with host receptor protein orthologues from a broad range of mammals. Sci Rep. (2020) 10:16471. 10.1038/s41598-020-71936-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Heurich A, Hofmann-Winkler H, Gierer S, Liepold T, Jahn O, Pohlmann S. TMPRSS2 and ADAM17 cleave ACE2 differentially and only proteolysis by TMPRSS2 augments entry driven by the severe acute respiratory syndrome coronavirus spike protein. J Virol. (2014) 88:1293–307. 10.1128/JVI.02202-13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Hoffmann M, Kleine-Weber H, Schroeder S, Kruger N, Herrler T, Erichsen S, et al. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell. (2020) 181:271–80 e278. 10.1016/j.cell.2020.02.052 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Lim YX, Ng YL, Tam JP, Liu DX. Human coronaviruses: a review of virus-host interactions. Diseases. (2016) 4:26. 10.3390/diseases4030026 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Satarker S, Nampoothiri M. Structural proteins in severe acute respiratory syndrome coronavirus-2. Arch Med Res. (2020) 51:482–91. 10.1016/j.arcmed.2020.05.012 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Wong CK, Lam CW, Wu AK, Ip WK, Lee NL, Chan IH, et al. Plasma inflammatory cytokines and chemokines in severe acute respiratory syndrome. Clin Exp Immunol. (2004) 136:95–103. 10.1111/j.1365-2249.2004.02415.x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Fu Y, Cheng Y, Wu Y. Understanding SARS-CoV-2-mediated inflammatory responses: from mechanisms to potential therapeutic tools. Virol Sin. (2020) 35:266–71. 10.1007/s12250-020-00207-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Verdecchia P, Cavallini C, Spanevello A, Angeli F. The pivotal link between ACE2 deficiency and SARS-CoV-2 infection. Eur J Intern Med. (2020) 76:14–20. 10.1016/j.ejim.2020.04.037 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Channappanavar R, Fehr AR, Vijay R, Mack M, Zhao J, Meyerholz DK, et al. Dysregulated type I interferon and inflammatory monocyte-macrophage responses cause lethal pneumonia in SARS-CoV-infected mice. Cell Host Microbe. (2016) 19:181–93. 10.1016/j.chom.2016.01.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Fu B, Xu X, Wei H. Why tocilizumab could be an effective treatment for severe COVID-19? J Transl Med. (2020) 18:164. 10.1186/s12967-020-02339-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Fung SY, Yuen KS, Ye ZW, Chan CP, Jin DY. A tug-of-war between severe acute respiratory syndrome coronavirus 2 and host antiviral defence: lessons from other pathogenic viruses. Emerg Microbes Infect. (2020) 9:558–70. 10.1080/22221751.2020.1736644 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Nieto-Torres JL, Dediego ML, Verdia-Baguena C, Jimenez-Guardeno JM, Regla-Nava JA, Fernandez-Delgado R, et al. Severe acute respiratory syndrome coronavirus envelope protein ion channel activity promotes virus fitness and pathogenesis. PLoS Pathog. (2014) 10:e1004077. 10.1371/journal.ppat.1004077 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Chen N, Zhou M, Dong X, Qu J, Gong F, Han Y, et al. Epidemiological and clinical characteristics of 99 cases of 2019 novel coronavirus pneumonia in Wuhan, China: a descriptive study. Lancet. (2020) 395:507–13. 10.1016/S0140-6736(20)30211-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Liu Y, Yang Y, Zhang C, Huang F, Wang F, Yuan J, et al. Clinical and biochemical indexes from 2019-nCoV infected patients linked to viral loads and lung injury. Sci China Life Sci. (2020) 63:364–74. 10.1007/s11427-020-1643-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Tay MZ, Poh CM, Renia L, Macary PA, Ng LFP. The trinity of COVID-19: immunity, inflammation and intervention. Nat Rev Immunol. (2020) 20:363–74. 10.1038/s41577-020-0311-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Iwasaki A, Yang Y. The potential danger of suboptimal antibody responses in COVID-19. Nat Rev Immunol. (2020) 20:339–41. 10.1038/s41577-020-0321-6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Wang SF, Tseng SP, Yen CH, Yang JY, Tsao CH, Shen CW, et al. Antibody-dependent SARS coronavirus infection is mediated by antibodies against spike proteins. Biochem Biophys Res Commun. (2014) 451:208–14. 10.1016/j.bbrc.2014.07.090 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Thompson BT, Chambers RC, Liu KD. Acute respiratory distress syndrome. N Engl J Med. (2017) 377:562–72. 10.1056/NEJMra1608077 [DOI] [PubMed] [Google Scholar]
- 44.Mahmudpour M, Roozbeh J, Keshavarz M, Farrokhi S, Nabipour I. COVID-19 cytokine storm: the anger of inflammation. Cytokine. (2020) 133:155151. 10.1016/j.cyto.2020.155151 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Sanclemente-Alaman I, Moreno-Jimenez L, Benito-Martin MS, Canales-Aguirre A, Matias-Guiu JA, Matias-Guiu J, et al. Experimental models for the study of central nervous system infection by SARS-CoV-2. Front Immunol. (2020) 11:2163. 10.3389/fimmu.2020.02163 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Gruslin E, Moisan S, St-Pierre Y, Desforges M, Talbot PJ. Transcriptome profile within the mouse central nervous system and activation of myelin-reactive T cells following murine coronavirus infection. J Neuroimmunol. (2005) 162:60–70. 10.1016/j.jneuroim.2005.01.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Dandekar AA, Perlman S. Virus-induced demyelination in nude mice is mediated by gamma delta T cells. Am J Pathol. (2002) 161:1255–63. 10.1016/S0002-9440(10)64402-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Choi KS, Aizaki H, Lai MM. Murine coronavirus requires lipid rafts for virus entry and cell-cell fusion but not for virus release. J Virol. (2005) 79:9862–71. 10.1128/JVI.79.15.9862-9871.2005 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Singh M, Khan RS, Dine K, Das Sarma J, Shindler KS. Intracranial inoculation is more potent than intranasal inoculation for inducing optic neuritis in the mouse hepatitis virus-induced model of multiple sclerosis. Front Cell Infect Microbiol. (2018) 8:311. 10.3389/fcimb.2018.00311 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Iadecola C, Anrather J, Kamel H. Effects of COVID-19 on the nervous system. Cell. (2020) 183:16–27 e11. 10.1016/j.cell.2020.08.028 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Buzhdygan TP, Deore BJ, Baldwin-Leclair A, Mcgary H, Razmpour R, Galie PA, et al. The SARS-CoV-2 spike protein alters barrier function in 2D static and 3D microfluidic in vitro models of the human blood-brain barrier. bioRxiv. (2020). 10.1101/2020.06.15.150912 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Liu JM, Tan BH, Wu S, Gui Y, Suo JL, Li YC. Evidence of central nervous system infection and neuroinvasive routes, as well as neurological involvement, in the lethality of SARS-CoV-2 infection. J Med Virol. (2020) 93:1304–13. 10.1002/jmv.26570 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Perrin P, Collongues N, Baloglu S, Bedo D, Bassand X, Lavaux T, et al. Cytokine release syndrome-associated encephalopathy in patients with COVID-19. Eur J Neurol. (2020) 28:248–58. 10.1111/ene.14491 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Ur A, Verma K. Cytokine storm in COVID19: a neural hypothesis. ACS Chem Neurosci. (2020) 11:1868–70. 10.1021/acschemneuro.0c00346 [DOI] [PubMed] [Google Scholar]
- 55.Pena-Silva RA, Faraci FM, Heistad DD. Response to letter regarding article, “impact of ACE2 deficiency and oxidative stress on cerebrovascular function with aging.” Stroke. (2013) 44:e35. 10.1161/STROKEAHA.111.000481 [DOI] [PubMed] [Google Scholar]
- 56.Maclean MA, Kamintsky L, Leck ED, Friedman A. The potential role of microvascular pathology in the neurological manifestations of coronavirus infection. Fluids Barriers CNS. (2020) 17:55. 10.1186/s12987-020-00216-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Brinker T, Stopa E, Morrison J, Klinge P. A new look at cerebrospinal fluid circulation. Fluids Barriers CNS. (2014) 11:10. 10.1186/2045-8118-11-10 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Desforges M, Le Coupanec A, Stodola JK, Meessen-Pinard M, Talbot PJ. Human coronaviruses: viral and cellular factors involved in neuroinvasiveness and neuropathogenesis. Virus Res. (2014) 194:145–58. 10.1016/j.virusres.2014.09.011 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Fenrich M, Mrdenovic S, Balog M, Tomic S, Zjalic M, Roncevic A, et al. SARS-CoV-2 dissemination through peripheral nerves explains multiple organ injury. Front Cell Neurosci. (2020) 14:229. 10.3389/fncel.2020.00229 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Baig AM, Sanders EC. Potential neuroinvasive pathways of SARS-CoV-2: deciphering the spectrum of neurological deficit seen in coronavirus disease-2019 (COVID-19). J Med Virol. (2020) 92:1845–57. 10.1002/jmv.26105 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Li CW, Syue LS, Tsai YS, Li MC, Lo CL, Tsai CS, et al. Anosmia and olfactory tract neuropathy in a case of COVID-19. J Microbiol Immunol Infect. (2020) 54:93–6. 10.1016/j.jmii.2020.05.017 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Lin E, Lantos JE, Strauss SB, Phillips CD, Campion TR, Jr, Navi BB, et al. Brain imaging of patients with COVID-19: findings at an academic institution during the height of the outbreak in New York City. AJNR Am J Neuroradiol. (2020) 41:2001–8. 10.3174/ajnr.A6793 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 63.Lu S, Wei N, Jiang J, Wu L, Sheng J, Zhou J, et al. First report of manic-like symptoms in a COVID-19 patient with no previous history of a psychiatric disorder. J Affect Disord. (2020) 277:337–40. 10.1016/j.jad.2020.08.031 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 64.Zubair AS, Mcalpine LS, Gardin T, Farhadian S, Kuruvilla DE, Spudich S. Neuropathogenesis and neurologic manifestations of the coronaviruses in the age of coronavirus disease 2019: a review. JAMA Neurol. (2020) 77:1018–27. 10.1001/jamaneurol.2020.2065 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Gosztonyi G. Propagation of viruses along neuron networks by transsynaptic passage–a contribution to the pathogenesis of rabies. Tierarztl Prax. (1986) 14:199–204. [PubMed] [Google Scholar]
- 66.Li YC, Bai WZ, Hirano N, Hayashida T, Taniguchi T, Sugita Y, et al. Neurotropic virus tracing suggests a membranous-coating-mediated mechanism for transsynaptic communication. J Comp Neurol. (2013) 521:203–12. 10.1002/cne.23171 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 67.Li YC, Bai WZ, Hashikawa T. The neuroinvasive potential of SARS-CoV2 may play a role in the respiratory failure of COVID-19 patients. J Med Virol. (2020) 92:552–5. 10.1002/jmv.25728 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Taylor MP, Enquist LW. Axonal spread of neuroinvasive viral infections. Trends Microbiol. (2015) 23:283–8. 10.1016/j.tim.2015.01.002 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Tremblay M-E, Madore C, Bordeleau M, Tian L, Verkhratsky A. Neuropathobiology of COVID-19: the role for Glia. Front Cell Neurosci. (2020) 14:592214. 10.3389/fncel.2020.592214 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Sun SH, Chen Q, Gu HJ, Yang G, Wang YX, Huang XY, et al. A mouse model of SARS-CoV-2 infection and pathogenesis. Cell Host Microbe. (2020) 28:124–33 e124. 10.1016/j.chom.2020.05.020 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 71.Doobay MF, Talman LS, Obr TD, Tian X, Davisson RL, Lazartigues E. Differential expression of neuronal ACE2 in transgenic mice with overexpression of the brain renin-angiotensin system. Am J Physiol Regul Integr Comp Physiol. (2007) 292:R373–381. 10.1152/ajpregu.00292.2006 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Kerslake R, Hall M, Randeva HS, Spandidos DA, Chatha K, Kyrou I, et al. Coexpression of peripheral olfactory receptors with SARSCoV2 infection mediators: potential implications beyond loss of smell as a COVID19 symptom. Int J Mol Med. (2020) 46:949–56. 10.3892/ijmm.2020.4646 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Hamming I, Timens W, Bulthuis ML, Lely AT, Navis G, Van Goor H. Tissue distribution of ACE2 protein, the functional receptor for SARS coronavirus. A first step in understanding SARS pathogenesis. J Pathol. (2004) 203:631–7. 10.1002/path.1570 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 74.Vazana U, Veksler R, Pell GS, Prager O, Fassler M, Chassidim Y, et al. Glutamate-mediated blood-brain barrier opening: implications for neuroprotection and drug delivery. J Neurosci. (2016) 36:7727–39. 10.1523/JNEUROSCI.0587-16.2016 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 75.Merkler AE, Parikh NS, Mir S, Gupta A, Kamel H, Lin E, et al. Risk of ischemic stroke in patients with covid-19 versus patients with influenza. MedRxiv. (2020). 10.1101/2020.05.18.20105494 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Bilinska K, Jakubowska P, Von Bartheld CS, Butowt R. Expression of the SARS-CoV-2 entry proteins, ACE2 and TMPRSS2, in cells of the olfactory epithelium: identification of cell types and trends with age. ACS Chem Neurosci. (2020) 11:1555–62. 10.1021/acschemneuro.0c00210 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Mollica V, Rizzo A, Massari F. The pivotal role of TMPRSS2 in coronavirus disease 2019 and prostate cancer. Future Oncol. (2020) 16:2029–33. 10.2217/fon-2020-0571 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 78.Qiao J, Li W, Bao J, Peng Q, Wen D, Wang J, et al. The expression of SARS-CoV-2 receptor ACE2 and CD147, and protease TMPRSS2 in human and mouse brain cells and mouse brain tissues. Biochem Biophys Res Commun. (2020) 533:867–71. 10.1016/j.bbrc.2020.09.042 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 79.Mentzel S, Dijkman HB, Van Son JP, Koene RA, Assmann KJ. Organ distribution of aminopeptidase A and dipeptidyl peptidase IV in normal mice. J Histochem Cytochem. (1996) 44:445–61. 10.1177/44.5.8627002 [DOI] [PubMed] [Google Scholar]
- 80.Mulvihill EE, Drucker DJ. Pharmacology, physiology, and mechanisms of action of dipeptidyl peptidase-4 inhibitors. Endocr Rev. (2014) 35:992–1019. 10.1210/er.2014-1035 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Meyerholz DK, Lambertz AM, Mccray PB, Jr. Dipeptidyl peptidase 4 distribution in the human respiratory tract: implications for the middle east respiratory syndrome. Am J Pathol. (2016) 186:78–86. 10.1016/j.ajpath.2015.09.014 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 82.Li L, Acioglu C, Heary RF, Elkabes S. Role of astroglial toll-like receptors (TLRs) in central nervous system infections, injury and neurodegenerative diseases. Brain Behav Immun. (2020) 91:740–55. 10.1016/j.bbi.2020.10.007 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 83.Choudhury A, Mukherjee S. In silico studies on the comparative characterization of the interactions of SARS-CoV-2 spike glycoprotein with ACE-2 receptor homologs and human TLRs. J Med Virol. (2020) 92:2105–13. 10.1002/jmv.25987 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Singh KD, Karnik SS. Angiotensin receptors: structure, function, signaling and clinical applications. J Cell Signal. 1:111. 10.4172/jcs.1000111 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 85.Krasniqi S, Daci A. Role of the angiotensin pathway and its target therapy in epilepsy management. Int J Mol Sci. (2019) 20:30726. 10.3390/ijms20030726 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 86.Gurwitz D. Angiotensin receptor blockers as tentative SARS-CoV-2 therapeutics. Drug Dev Res. (2020) 81:537–40. 10.1002/ddr.21656 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 87.D'ardes D, Boccatonda A, Rossi I, Guagnano MT, Santilli F, Cipollone F, et al. COVID-19 and RAS: unravelling an unclear relationship. Int J Mol Sci. (2020) 21:83003. 10.3390/ijms21083003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 88.Maginnis MS. Virus-Receptor interactions: the key to cellular invasion. J Mol Biol. (2018) 430:2590–611. 10.1016/j.jmb.2018.06.024 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 89.Yan S, Sun H, Bu X, Wan G. New strategy for COVID-19: an evolutionary role for RGD motif in SARS-CoV-2 and potential inhibitors for virus infection. Front Pharmacol. (2020) 11:912. 10.3389/fphar.2020.00912 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 90.Stoka V, Turk V, Turk B. Lysosomal cathepsins and their regulation in aging and neurodegeneration. Ageing Res Rev. (2016) 32:22–37. 10.1016/j.arr.2016.04.010 [DOI] [PubMed] [Google Scholar]
- 91.Pezzini A, Padovani A. Lifting the mask on neurological manifestations of COVID-19. Nat Rev Neurol. (2020) 16:636–44. 10.1038/s41582-020-0398-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 92.Johann S, Heitzer M, Kanagaratnam M, Goswami A, Rizo T, Weis J, et al. NLRP3 inflammasome is expressed by astrocytes in the SOD1 mouse model of ALS and in human sporadic ALS patients. Glia. (2015) 63:2260–73. 10.1002/glia.22891 [DOI] [PubMed] [Google Scholar]
- 93.Voet S, Srinivasan S, Lamkanfi M, Van Loo G. Inflammasomes in neuroinflammatory and neurodegenerative diseases. EMBO Mol Med. (2019) 11:10248. 10.15252/emmm.201810248 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 94.Deora V, Lee JD, Albornoz EA, Mcalary L, Jagaraj CJ, Robertson A, et al. The microglial NLRP3 inflammasome is activated by amyotrophic lateral sclerosis proteins. Glia. (2020) 68:407–21. 10.1002/glia.23728 [DOI] [PubMed] [Google Scholar]
- 95.Chen R, Wang K, Yu J, Howard D, French L, Chen Z, et al. The spatial and cell-type distribution of SARS-CoV-2 receptor ACE2 in the human and mouse brains. Front Neurol. (2020) 11:573095. 10.3389/fneur.2020.573095 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 96.Hikmet F, Mear L, Edvinsson A, Micke P, Uhlen M, Lindskog C. The protein expression profile of ACE2 in human tissues. Mol Syst Biol. (2020) 16:e9610. 10.15252/msb.20209610 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 97.Lovren F, Pan Y, Quan A, Teoh H, Wang G, Shukla PC, et al. Angiotensin converting enzyme-2 confers endothelial protection and attenuates atherosclerosis. Am J Physiol Heart Circ Physiol. (2008) 295:H1377–84. 10.1152/ajpheart.00331.2008 [DOI] [PubMed] [Google Scholar]
- 98.Buzhdygan TP, Deore BJ, Baldwin-Leclair A, Bullock TA, Mcgary HM, Khan JA, et al. The SARS-CoV-2 spike protein alters barrier function in 2D static and 3D microfluidic in-vitro models of the human blood-brain barrier. Neurobiol Dis. (2020) 146:105131. 10.1016/j.nbd.2020.105131 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 99.Vargas G, Medeiros Geraldo LH, Gedeao Salomao N, Viana Paes M, Regina Souza Lima F, Carvalho Alcantara Gomes F. Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) and glial cells: insights and perspectives. Brain Behav Immun Health. (2020) 7:100127. 10.1016/j.bbih.2020.100127 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 100.Jha NK, Ojha S, Jha SK, Dureja H, Singh SK, Shukla SD, et al. Evidence of coronavirus (CoV) pathogenesis and emerging pathogen SARS-CoV-2 in the nervous system: a review on neurological impairments and manifestations. J Mol Neurosci. (2021) 19:1–8. 10.1007/s12031-020-01767-6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 101.Chen L, Li X, Chen M, Feng Y, Xiong C. The ACE2 expression in human heart indicates new potential mechanism of heart injury among patients infected with SARS-CoV-2. Cardiovasc Res. (2020) 116:1097–100. 10.1093/cvr/cvaa078 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 102.Ludlow M, Kortekaas J, Herden C, Hoffmann B, Tappe D, Trebst C, et al. Neurotropic virus infections as the cause of immediate and delayed neuropathology. Acta Neuropathol. (2016) 131:159–84. 10.1007/s00401-015-1511-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 103.Sporns O. Structure and function of complex brain networks. Dialogues Clin Neurosci. (2013) 15:247–62. 10.31887/DCNS.2013.15.3/osporns [DOI] [PMC free article] [PubMed] [Google Scholar]
- 104.Channappanavar R, Perlman S. Pathogenic human coronavirus infections: causes and consequences of cytokine storm and immunopathology. Semin Immunopathol. (2017) 39:529–39. 10.1007/s00281-017-0629-x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 105.Merad M, Martin JC. Pathological inflammation in patients with COVID-19: a key role for monocytes and macrophages. Nat Rev Immunol. (2020) 20:355–62. 10.1038/s41577-020-0331-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 106.Zhang C, Wu Z, Li JW, Zhao H, Wang GQ. Cytokine release syndrome in severe COVID-19: interleukin-6 receptor antagonist tocilizumab may be the key to reduce mortality. Int J Antimicrob Agents. (2020) 55:105954. 10.1016/j.ijantimicag.2020.105954 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 107.Mokhtari T, Hassani F, Ghaffari N, Ebrahimi B, Yarahmadi A, Hassanzadeh G. COVID-19 and multiorgan failure: a narrative review on potential mechanisms. J Mol Histol. (2020) 51:613–28. 10.1007/s10735-020-09915-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 108.Bhaskar S, Sinha A, Banach M, Mittoo S, Weissert R, Kass JS, et al. Cytokine storm in COVID-19-immunopathological mechanisms, clinical considerations, and therapeutic approaches: the REPROGRAM consortium position paper. Front Immunol. (2020) 11:1648. 10.3389/fimmu.2020.01648 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 109.Varga Z, Flammer AJ, Steiger P, Haberecker M, Andermatt R, Zinkernagel AS, et al. Endothelial cell infection and endotheliitis in COVID-19. Lancet. (2020) 395:1417–8. 10.1016/S0140-6736(20)30937-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 110.Fotuhi M, Mian A, Meysami S, Raji CA. Neurobiology of COVID-19. J Alzheimers Dis. (2020) 76:3–19. 10.3233/JAD-200581 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 111.Xiong M, Liang X, Wei YD. Changes in blood coagulation in patients with severe coronavirus disease 2019 (COVID-19): a meta-analysis. Br J Haematol. (2020) 189:1050–2. 10.1111/bjh.16725 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 112.Najjar S, Najjar A, Chong DJ, Pramanik BK, Kirsch C, Kuzniecky RI, et al. Central nervous system complications associated with SARS-CoV-2 infection: integrative concepts of pathophysiology and case reports. J Neuroinflammation. (2020) 17:231. 10.1186/s12974-020-01896-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 113.Larochelle C, Alvarez JI, Prat A. How do immune cells overcome the blood-brain barrier in multiple sclerosis? FEBS Lett. (2011) 585:3770–80. 10.1016/j.febslet.2011.04.066 [DOI] [PubMed] [Google Scholar]
- 114.Najjar S, Pahlajani S, De Sanctis V, Stern JNH, Najjar A, Chong D. Neurovascular unit dysfunction and blood-brain barrier hyperpermeability contribute to schizophrenia neurobiology: a theoretical integration of clinical and experimental evidence. Front Psychiatry. (2017) 8:83. 10.3389/fpsyt.2017.00083 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 115.Dantzer R. Neuroimmune interactions: from the brain to the immune system and vice versa. Physiol Rev. (2018) 98:477–504. 10.1152/physrev.00039.2016 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 116.Ottaviani D, Boso F, Tranquillini E, Gapeni I, Pedrotti G, Cozzio S, et al. Early Guillain-Barre syndrome in coronavirus disease 2019 (COVID-19): a case report from an Italian COVID-hospital. Neurol Sci. (2020) 41:1351–4. 10.1007/s10072-020-04449-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 117.Poyiadji N, Shahin G, Noujaim D, Stone M, Patel S, Griffith B. COVID-19-associated acute hemorrhagic necrotizing encephalopathy: imaging features. Radiology. (2020) 296:E119–20. 10.1148/radiol.2020201187 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 118.Al Saiegh F, Ghosh R, Leibold A, Avery MB, Schmidt RF, Theofanis T, et al. Status of SARS-CoV-2 in cerebrospinal fluid of patients with COVID-19 and stroke. J Neurol Neurosurg Psychiatry. (2020) 91:846–8. 10.1136/jnnp-2020-323522 [DOI] [PubMed] [Google Scholar]
- 119.Liddelow SA, Guttenplan KA, Clarke LE, Bennett FC, Bohlen CJ, Schirmer L, et al. Neurotoxic reactive astrocytes are induced by activated microglia. Nature. (2017) 541:481–7. 10.1038/nature21029 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 120.Potokar M, Jorgacevski J, Zorec R. Astrocytes in flavivirus infections. Int J Mol Sci. (2019) 20:30691. 10.3390/ijms20030691 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 121.Madan V, Garcia Mde J, Sanz MA, Carrasco L. Viroporin activity of murine hepatitis virus E protein. FEBS Lett. (2005) 579:3607–12. 10.1016/j.febslet.2005.05.046 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 122.Achar A, Ghosh C. COVID-19-associated neurological disorders: the potential route of CNS invasion and blood-brain relevance. Cells. (2020) 9:112360. 10.3390/cells9112360 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 123.Guo HC, Jin Y, Zhi XY, Yan D, Sun SQ. NLRP3 inflammasome activation by viroporins of animal viruses. Viruses. (2015) 7:3380–91. 10.3390/v7072777 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 124.Farag NS, Breitinger U, Breitinger HG, El Azizi MA. Viroporins and inflammasomes: a key to understand virus-induced inflammation. Int J Biochem Cell Biol. (2020) 122:105738. 10.1016/j.biocel.2020.105738 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 125.Ichinohe T, Pang IK, Iwasaki A. Influenza virus activates inflammasomes via its intracellular M2 ion channel. Nat Immunol. (2010) 11:404–10. 10.1038/ni.1861 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 126.Kovacs SB, Miao EA. Gasdermins: effectors of pyroptosis. Trends Cell Biol. (2017) 27:673–84. 10.1016/j.tcb.2017.05.005 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 127.Lieberman J, Wu H, Kagan JC. Gasdermin D activity in inflammation and host defense. Sci Immunol. (2019) 4:aav1447. 10.1126/sciimmunol.aav1447 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 128.Munhoz RP, Pedroso JL, Nascimento FA, Almeida SM, Barsottini OGP, Cardoso FEC, et al. Neurological complications in patients with SARS-CoV-2 infection: a systematic review. Arq Neuropsiquiatr. (2020) 78:290–300. 10.1590/0004-282x20200051 [DOI] [PubMed] [Google Scholar]
- 129.Mao L, Jin H, Wang M, Hu Y, Chen S, He Q, et al. Neurologic manifestations of hospitalized patients with coronavirus disease 2019 in Wuhan, China. JAMA Neurol. (2020) 77:683–90. 10.1001/jamaneurol.2020.1127 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 130.Pugin D, Vargas MI, Thieffry C, Schibler M, Grosgurin O, Pugin J, et al. COVID-19-related encephalopathy responsive to high-dose glucocorticoids. Neurology. (2020) 95:543–6. 10.1212/WNL.0000000000010354 [DOI] [PubMed] [Google Scholar]
- 131.Arca KN, Starling AJ. Treatment-refractory headache in the setting of COVID-19 pneumonia: migraine or meningoencephalitis? case report. SN Compr Clin Med. (2020) 369:1–4. 10.1007/s42399-020-00369-y [DOI] [PMC free article] [PubMed] [Google Scholar]
- 132.Toptan T, Aktan C, Basari A, Bolay H. Case series of headache characteristics in COVID-19: headache can be an isolated symptom. Headache. (2020) 60:1788–92. 10.1111/head.13940 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 133.Uygun O, Ertas M, Ekizoglu E, Bolay H, Ozge A, Kocasoy Orhan E, et al. Headache characteristics in COVID-19 pandemic-a survey study. J Headache Pain. (2020) 21:121. 10.1186/s10194-020-01188-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 134.Liotta EM, Batra A, Clark JR, Shlobin NA, Hoffman SC, Orban ZS, et al. Frequent neurologic manifestations and encephalopathy-associated morbidity in Covid-19 patients. Ann Clin Transl Neurol. (2020) 7:2221–30. 10.1002/acn3.51210 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 135.Beach SR, Praschan NC, Hogan C, Dotson S, Merideth F, Kontos N, et al. Delirium in COVID-19: a case series and exploration of potential mechanisms for central nervous system involvement. Gen Hosp Psychiatry. (2020) 65:47–53. 10.1016/j.genhosppsych.2020.05.008 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 136.Helms J, Kremer S, Merdji H, Clere-Jehl R, Schenck M, Kummerlen C, et al. Neurologic features in severe SARS-CoV-2 infection. N Engl J Med. (2020) 382:2268–70. 10.1056/NEJMc2008597 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 137.Tan YK, Goh C, Leow AST, Tambyah PA, Ang A, Yap ES, et al. COVID-19 and ischemic stroke: a systematic review and meta-summary of the literature. J Thromb Thrombolysis. (2020) 50:587–95. 10.1007/s11239-020-02228-y [DOI] [PMC free article] [PubMed] [Google Scholar]
- 138.Lechien JR, Chiesa-Estomba CM, De Siati DR, Horoi M, Le Bon SD, Rodriguez A, et al. Olfactory and gustatory dysfunctions as a clinical presentation of mild-to-moderate forms of the coronavirus disease (COVID-19): a multicenter European study. Eur Arch Otorhinolaryngol. (2020) 277:2251–61. 10.1007/s00405-020-05965-1 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 139.Aragao M, Leal MC, Cartaxo Filho OQ, Fonseca TM, Valenca MM. Anosmia in COVID-19 associated with injury to the olfactory bulbs evident on MRI. AJNR Am J Neuroradiol. (2020) 41:1703–6. 10.3174/ajnr.A6675 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 140.Gori A, Leone F, Loffredo L, Cinicola BL, Brindisi G, De Castro G, et al. COVID-19-related anosmia: the olfactory pathway hypothesis and early intervention. Front Neurol. (2020) 11:956. 10.3389/fneur.2020.00956 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 141.Meng X, Deng Y, Dai Z, Meng Z. COVID-19 and anosmia: a review based on up-to-date knowledge. Am J Otolaryngol. (2020) 41:102581. 10.1016/j.amjoto.2020.102581 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 142.Vaira LA, Salzano G, Fois AG, Piombino P, De Riu G. Potential pathogenesis of ageusia and anosmia in COVID-19 patients. Int Forum Allergy Rhinol. (2020) 10:1103–4. 10.1002/alr.22593 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 143.Guidon AC, Amato AA. COVID-19 and neuromuscular disorders. Neurology. (2020) 94:959–69. 10.1212/WNL.0000000000009566 [DOI] [PubMed] [Google Scholar]
- 144.Toscano G, Palmerini F, Ravaglia S, Ruiz L, Invernizzi P, Cuzzoni MG, et al. Guillain-Barre syndrome associated with SARS-CoV-2. N Engl J Med. (2020) 382:2574–6. 10.1056/NEJMc2009191 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 145.Abu-Rumeileh S, Abdelhak A, Foschi M, Tumani H, Otto M. Guillain-Barre syndrome spectrum associated with COVID-19: an up-to-date systematic review of 73 cases. J Neurol. (2020) 25:1–38. 10.1007/s00415-020-10124-x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 146.Zhao H, Shen D, Zhou H, Liu J, Chen S. Guillain-Barre syndrome associated with SARS-CoV-2 infection: causality or coincidence? Lancet Neurol. (2020) 19:383–4. 10.1016/S1474-4422(20)30109-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 147.Ozdag Acarli AN, Samanci B, Ekizoglu E, Cakar A, Sirin NG, Gunduz T, et al. Coronavirus disease 2019 (COVID-19) from the point of view of neurologists: observation of neurological findings and symptoms during the combat against a pandemic. Noro Psikiyatr Ars. (2020) 57:154–9. 10.29399/npa.26148 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 148.Benemei S, Nicoletti P, Capone JG, Geppetti P. CGRP receptors in the control of pain and inflammation. Curr Opin Pharmacol. (2009) 9:9–14. 10.1016/j.coph.2008.12.007 [DOI] [PubMed] [Google Scholar]
- 149.Durham PL. Calcitonin gene-related peptide (CGRP) and migraine. Headache. (2006) 46(Suppl.1):S3–8. 10.1111/j.1526-4610.2006.00483.x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 150.Porta-Etessam J, Matias-Guiu JA, Gonzalez-Garcia N, Gomez Iglesias P, Santos-Bueso E, Arriola-Villalobos P, et al. Spectrum of headaches associated with SARS-CoV-2 infection: study of healthcare professionals. Headache. (2020) 60:1697–704. 10.1111/head.13902 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 151.Zhao F, Han Z, Wang R, Luo Y. Neurological manifestations of COVID-19: causality or coincidence? Aging Dis. (2021) 12:27–35. 10.14336/AD.2020.0917 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 152.Stohlman SA, Hinton DR. Viral induced demyelination. Brain Pathol. (2001) 11:92–106. 10.1111/j.1750-3639.2001.tb00384.x [DOI] [PMC free article] [PubMed] [Google Scholar]
- 153.Savarin C, Bergmann CC. Viral-induced suppression of self-reactive T cells: lessons from neurotropic coronavirus-induced demyelination. J Neuroimmunol. (2017) 308:12–6. 10.1016/j.jneuroim.2017.01.003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 154.Dziedzic A, Saluk-Bijak J, Miller E, Niemcewicz M, Bijak M. The impact of SARS-CoV-2 infection on the development of neurodegeneration in multiple sclerosis. Int J Mol Sci. (2021) 22:1804. 10.3390/ijms22041804 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 155.Palao M, Fernandez-Diaz E, Gracia-Gil J, Romero-Sanchez CM, Diaz-Maroto I, Segura T. Multiple sclerosis following SARS-CoV-2 infection. Mult Scler Relat Disord. (2020) 45:102377. 10.1016/j.msard.2020.102377 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 156.Diez-Porras L, Verges E, Gil F, Vidal MJ, Massons J, Arboix A. Guillain-Barre-Strohl syndrome and COVID-19: case report and literature review. Neuromuscul Disord. (2020) 30:859–61. 10.1016/j.nmd.2020.08.354 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 157.Paybast S, Gorji R, Mavandadi S. Guillain-Barre syndrome as a neurological complication of novel COVID-19 infection: a case report and review of the literature. Neurologist. (2020) 25:101–3. 10.1097/NRL.0000000000000291 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 158.Zito A, Alfonsi E, Franciotta D, Todisco M, Gastaldi M, Cotta Ramusino M, et al. COVID-19 and Guillain-Barre syndrome: a case report and review of literature. Front Neurol. (2020) 11:909. 10.3389/fneur.2020.00909 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 159.Garg RK, Paliwal VK, Gupta A. Encephalopathy in patients with COVID-19: a review. J Med Virol. (2021) 93:206–22. 10.1002/jmv.26207 [DOI] [PubMed] [Google Scholar]
- 160.Lorenzo Villalba N, Maouche Y, Alonso Ortiz MB, Cordoba Sosa Z, Chahbazian JB, Syrovatkova A, et al. Anosmia and dysgeusia in the absence of other respiratory diseases: should COVID-19 infection be considered? Eur J Case Rep Intern Med. (2020) 7:001641. 10.12890/2020_001641 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 161.Spinato G, Fabbris C, Polesel J, Cazzador D, Borsetto D, Hopkins C, et al. Alterations in smell or taste in mildly symptomatic outpatients with SARS-CoV-2 infection. JAMA. (2020) 323:2089–90. 10.1001/jama.2020.6771 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 162.Yan CH, Faraji F, Prajapati DP, Ostrander BT, Deconde AS. Self-reported olfactory loss associates with outpatient clinical course in COVID-19. Int Forum Allergy Rhinol. (2020) 10:821–31. 10.1002/alr.22592 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 163.Brann DH, Tsukahara T, Weinreb C, Lipovsek M, Van Den Berge K, Gong B, et al. Non-neuronal expression of SARS-CoV-2 entry genes in the olfactory system suggests mechanisms underlying COVID-19-associated anosmia. Sci Adv. (2020) 6:abc5801. 10.1126/sciadv.abc5801 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 164.Nicholson P, Alshafai L, Krings T. Reply. AJNR Am J Neuroradiol. (2020) 41:E91. 10.3174/ajnr.A6827 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 165.Coolen T, Lolli V, Sadeghi N, Rovai A, Trotta N, Taccone FS, et al. Early postmortem brain MRI findings in COVID-19 non-survivors. Neurology. (2020) 95:e2016–27. 10.1212/WNL.0000000000010116 [DOI] [PubMed] [Google Scholar]
- 166.Beigel JH, Tomashek KM, Dodd LE, Mehta AK, Zingman BS, Kalil AC, et al. Remdesivir for the treatment of covid-19 - final report. N Engl J Med. (2020) 383:1813–26. 10.1056/NEJMoa2007764 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 167.Breining P, Frolund AL, Hojen JF, Gunst JD, Staerke NB, Saedder E, et al. Camostat mesylate against SARS-CoV-2 and COVID-19-Rationale, dosing and safety. Basic Clin Pharmacol Toxicol. (2021) 128:204–12. 10.1111/bcpt.13533 [DOI] [PubMed] [Google Scholar]
- 168.Doi K, Ikeda M, Hayase N, Moriya K, Morimura N, Group C-US. Nafamostat mesylate treatment in combination with favipiravir for patients critically ill with Covid-19: a case series. Crit Care. (2020) 24:392. 10.1186/s13054-020-03078-z [DOI] [PMC free article] [PubMed] [Google Scholar]
- 169.Hoffmann M, Schroeder S, Kleine-Weber H, Muller MA, Drosten C, Pohlmann S. Nafamostat mesylate blocks activation of SARS-CoV-2: new treatment option for COVID-19. Antimicrob Agents Chemother. (2020) 64:20. 10.1128/AAC.00754-20 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 170.Salama C, Han J, Yau L, Reiss WG, Kramer B, Neidhart JD, et al. Tocilizumab in patients hospitalized with Covid-19 pneumonia. N Engl J Med. (2021) 384:20–30. 10.1056/NEJMoa2030340 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 171.Huet T, Beaussier H, Voisin O, Jouveshomme S, Dauriat G, Lazareth I, et al. Anakinra for severe forms of COVID-19: a cohort study. Lancet Rheumatol. (2020) 2:e393–400. 10.1016/S2665-9913(20)30164-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 172.Kooistra EJ, Waalders NJB, Grondman I, Janssen NaF, De Nooijer AH, Netea MG, et al. Anakinra treatment in critically ill COVID-19 patients: a prospective cohort study. Crit Care. (2020) 24:688. 10.1186/s13054-020-03364-w [DOI] [PMC free article] [PubMed] [Google Scholar]
- 173.De Luca G, Cavalli G, Campochiaro C, Della-Torre E, Angelillo P, Tomelleri A, et al. GM-CSF blockade with mavrilimumab in severe COVID-19 pneumonia and systemic hyperinflammation: a single-centre, prospective cohort study. Lancet Rheumatol. (2020) 2:e465–e473. 10.1016/S2665-9913(20)30170-3 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 174.Group RC, Horby P, Lim WS, Emberson JR, Mafham M, Bell JL, et al. Dexamethasone in hospitalized patients with covid-19. N Engl J Med. (2021) 384:693–704. 10.1056/NEJMoa2021436 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 175.Solomon IH, Normandin E, Bhattacharyya S, Mukerji SS, Keller K, Ali AS, et al. Neuropathological Features of Covid-19. N Engl J Med. (2020) 383:989–92. 10.1056/NEJMc2019373 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 176.Von Weyhern CH, Kaufmann I, Neff F, Kremer M. Early evidence of pronounced brain involvement in fatal COVID-19 outcomes. Lancet. (2020) 395:e109. 10.1016/S0140-6736(20)31282-4 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 177.Al-Dalahmah O, Thakur KT, Nordvig AS, Prust ML, Roth W, Lignelli A, et al. Neuronophagia and microglial nodules in a SARS-CoV-2 patient with cerebellar hemorrhage. Acta Neuropathol Commun. (2020) 8:147. 10.1186/s40478-020-01024-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 178.Meinhardt J, Radke J, Dittmayer C, Franz J, Thomas C, Mothes R, et al. Olfactory transmucosal SARS-CoV-2 invasion as a port of central nervous system entry in individuals with COVID-19. Nat Neurosci. (2020) 24:168–75. 10.1038/s41593-020-00758-5 [DOI] [PubMed] [Google Scholar]
- 179.Matschke J, Lutgehetmann M, Hagel C, Sperhake JP, Schroder AS, Edler C, et al. Neuropathology of patients with COVID-19 in Germany: a post-mortem case series. Lancet Neurol. (2020) 19:919–29. 10.1016/S1474-4422(20)30308-2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 180.Schurink B, Roos E, Radonic T, Barbe E, Bouman CSC, De Boer HH, et al. Viral presence and immunopathology in patients with lethal COVID-19: a prospective autopsy cohort study. Lancet Microbe. (2020) 1:e290–9. 10.1016/S2666-5247(20)30144-0 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 181.Dinkin M, Gao V, Kahan J, Bobker S, Simonetto M, Wechsler P, et al. COVID-19 presenting with ophthalmoparesis from cranial nerve palsy. Neurology. (2020) 95:221–3. 10.1212/WNL.0000000000009700 [DOI] [PubMed] [Google Scholar]
- 182.Jakhmola S, Indari O, Chatterjee S, Jha HC. SARS-CoV-2, an underestimated pathogen of the nervous system. SN Compr Clin Med. (2020) 7:1–10. 10.1007/s42399-020-00522-7 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 183.Luers JC, Rokohl AC, Loreck N, Wawer Matos PA, Augustin M, Dewald F, et al. Olfactory and gustatory dysfunction in coronavirus disease 2019 (COVID-19). Clin Infect Dis. (2020) 71:2262–4. 10.1093/cid/ciaa525 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 184.Chamberlin NL. Functional organization of the parabrachial complex and intertrigeminal region in the control of breathing. Respir Physiol Neurobiol. (2004) 143:115–25. 10.1016/j.resp.2004.03.015 [DOI] [PubMed] [Google Scholar]
- 185.Chao CC, Tsai LK, Chiou YH, Tseng MT, Hsieh ST, Chang SC, et al. Peripheral nerve disease in SARS: report of a case. Neurology. (2003) 61:1820–1. 10.1212/01.WNL.0000099171.26943.D0 [DOI] [PubMed] [Google Scholar]
- 186.Tsai LK, Hsieh ST, Chao CC, Chen YC, Lin YH, Chang SC, et al. Neuromuscular disorders in severe acute respiratory syndrome. Arch Neurol. (2004) 61:1669–73. 10.1001/archneur.61.11.1669 [DOI] [PubMed] [Google Scholar]
- 187.Saad M, Omrani AS, Baig K, Bahloul A, Elzein F, Matin MA, et al. Clinical aspects and outcomes of 70 patients with Middle East respiratory syndrome coronavirus infection: a single-center experience in Saudi Arabia. Int J Infect Dis. (2014) 29:301–6. 10.1016/j.ijid.2014.09.003 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 188.Van Den Pol AN. Viral infection leading to brain dysfunction: more prevalent than appreciated? Neuron. (2009) 64:17–20. 10.1016/j.neuron.2009.09.023 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 189.Fazzini E, Fleming J, Fahn S. Cerebrospinal fluid antibodies to coronavirus in patients with Parkinson's disease. Mov Disord. (1992) 7:153–8. 10.1002/mds.870070210 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 190.Murray RS, Brown B, Brian D, Cabirac GF. Detection of coronavirus RNA and antigen in multiple sclerosis brain. Ann Neurol. (1992) 31:525–33. 10.1002/ana.410310511 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 191.Arbour N, Cote G, Lachance C, Tardieu M, Cashman NR, Talbot PJ. Acute and persistent infection of human neural cell lines by human coronavirus OC43. J Virol. (1999) 73:3338–50. 10.1128/JVI.73.4.3338-3350.1999 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 192.Desforges M, Le Coupanec A, Brison E, Meessen-Pinard M, Talbot PJ. Neuroinvasive and neurotropic human respiratory coronaviruses: potential neurovirulent agents in humans. Adv Exp Med Biol. (2014) 807:75–96. 10.1007/978-81-322-1777-0_6 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 193.Sagare AP, Bell RD, Zlokovic BV. Neurovascular defects and faulty amyloid-beta vascular clearance in Alzheimer's disease. J Alzheimers Dis. (2013) 33(Suppl.1):S87–100. 10.3233/JAD-2012-129037 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 194.Selkoe DJ, Hardy J. The amyloid hypothesis of Alzheimer's disease at 25 years. EMBO Mol Med. (2016) 8:595–608. 10.15252/emmm.201606210 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 195.Harris SA, Harris EA. Herpes simplex virus type 1 and other pathogens are key causative factors in sporadic Alzheimer's disease. J Alzheimers Dis. (2015) 48:319–53. 10.3233/JAD-142853 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 196.Soscia SJ, Kirby JE, Washicosky KJ, Tucker SM, Ingelsson M, Hyman B, et al. The Alzheimer's disease-associated amyloid beta-protein is an antimicrobial peptide. PLoS ONE. (2010) 5:e9505. 10.1371/journal.pone.0009505 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 197.Singh K, Chen YC, Judy JT, Seifuddin F, Tunc I, Pirooznia M. Network analysis and transcriptome profiling identify autophagic and mitochondrial dysfunctions in SARS-CoV-2 infection. bioRxiv. (2020) 2020:092536. 10.1101/2020.05.13.092536 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 198.Bullen CK, Hogberg HT, Bahadirli-Talbott A, Bishai WR, Hartung T, Keuthan C, et al. Infectability of human BrainSphere neurons suggests neurotropism of SARS-CoV-2. ALTEX. (2020) 37:665–71. 10.14573/altex.2006111s [DOI] [PubMed] [Google Scholar]
- 199.Ramani A, Muller L, Ostermann PN, Gabriel E, Abida-Islam P, Muller-Schiffmann A, et al. SARS-CoV-2 targets neurons of 3D human brain organoids. EMBO J. (2020) 39:e106230. 10.15252/embj.2020106230 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 200.Song E, Zhang C, Israelow B, Lu-Culligan A, Prado AV, Skriabine S, et al. Neuroinvasion of SARS-CoV-2 in human and mouse brain. bioRxiv. (2020). 10.1101/2020.06.25.169946 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 201.Gendron TF, Petrucelli L. The role of tau in neurodegeneration. Mol Neurodegener. (2009) 4:13. 10.1186/1750-1326-4-13 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 202.Abate G, Memo M, Uberti D. Impact of COVID-19 on Alzheimer's disease risk: viewpoint for research action. Healthcare. (2020) 8:30286. 10.3390/healthcare8030286 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 203.Lull ME, Block ML. Microglial activation and chronic neurodegeneration. Neurotherapeutics. (2010) 7:354–65. 10.1016/j.nurt.2010.05.014 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 204.Mcnab F, Mayer-Barber K, Sher A, Wack A, O'garra A. Type I interferons in infectious disease. Nat Rev Immunol. (2015) 15:87–103. 10.1038/nri3787 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 205.Kai H, Kai M. Interactions of coronaviruses with ACE2, angiotensin II, and RAS inhibitors—lessons from available evidence and insights into COVID-19. Hypertension Res. (2020) 43:648–54. 10.1038/s41440-020-0455-8 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 206.Jang H, Boltz DA, Webster RG, Smeyne RJ. Viral parkinsonism. Biochim Biophys Acta. (2009) 1792:714–21. 10.1016/j.bbadis.2008.08.001 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 207.Yamada T. Viral etiology of Parkinson's disease: focus on influenza A virus. Parkinsonism Relat Disord. (1996) 2:113–21. 10.1016/1353-8020(96)00006-5 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 208.Limphaibool N, Iwanowski P, Holstad MJV, Kobylarek D, Kozubski W. Infectious etiologies of parkinsonism: pathomechanisms and clinical implications. Front Neurol. (2019) 10:652. 10.3389/fneur.2019.00652 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 209.Wang C, Horby PW, Hayden FG, Gao GF. A novel coronavirus outbreak of global health concern. Lancet. (2020) 395:470–3. 10.1016/S0140-6736(20)30185-9 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 210.Dorsey ER, Sherer T, Okun MS, Bloem BR. The emerging evidence of the parkinson pandemic. J Parkinsons Dis. (2018) 8:S3–8. 10.3233/JPD-181474 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 211.Balestrino R, Schapira AHV. Parkinson disease. Eur J Neurol. (2020) 27:27–42. 10.1111/ene.14108 [DOI] [PubMed] [Google Scholar]
- 212.Baba Y, Kuroiwa A, Uitti RJ, Wszolek ZK, Yamada T. Alterations of T-lymphocyte populations in Parkinson disease. Parkinsonism Relat Disord. (2005) 11:493–8. 10.1016/j.parkreldis.2005.07.005 [DOI] [PubMed] [Google Scholar]
- 213.Ransohoff RM, Perry VH. Microglial physiology: unique stimuli, specialized responses. Annu Rev Immunol. (2009) 27:119–45. 10.1146/annurev.immunol.021908.132528 [DOI] [PubMed] [Google Scholar]
- 214.Ringheim GE, Conant K. Neurodegenerative disease and the neuroimmune axis (Alzheimer's and Parkinson's disease, and viral infections). J Neuroimmunol. (2004) 147:43–9. 10.1016/j.jneuroim.2003.10.013 [DOI] [PubMed] [Google Scholar]
- 215.Franceschi C, Garagnani P, Parini P, Giuliani C, Santoro A. Inflammaging: a new immune-metabolic viewpoint for age-related diseases. Nat Rev Endocrinol. (2018) 14:576–90. 10.1038/s41574-018-0059-4 [DOI] [PubMed] [Google Scholar]
- 216.Caggiu E, Arru G, Hosseini S, Niegowska M, Sechi G, Zarbo IR, et al. Inflammation, infectious triggers, and Parkinson's disease. Front Neurol. (2019) 10:122. 10.3389/fneur.2019.00122 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 217.Lesteberg KE, Beckham JD. Immunology of west nile virus infection and the role of alpha-synuclein as a viral restriction factor. Viral Immunol. (2019) 32:38–47. 10.1089/vim.2018.0075 [DOI] [PubMed] [Google Scholar]
- 218.Massey AR, Beckham JD. Alpha-synuclein, a novel viral restriction factor hiding in plain sight. DNA Cell Biol. (2016) 35:643–5. 10.1089/dna.2016.3488 [DOI] [PubMed] [Google Scholar]
- 219.Gelders G, Baekelandt V, Van Der Perren A. Linking neuroinflammation and neurodegeneration in Parkinson's disease. J Immunol Res. (2018) 2018:4784268. 10.1155/2018/4784268 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 220.Gomez-Pinedo U, Matias-Guiu J, Sanclemente-Alaman I, Moreno-Jimenez L, Montero-Escribano P, Matias-Guiu JA. Is the brain a reservoir organ for SARS-CoV2? J Med Virol. (2020) 92:2354–5. 10.1002/jmv.26046 [DOI] [PMC free article] [PubMed] [Google Scholar]