Abstract
Objectives
Public health interventions for adolescent “obesity prevention” have focused predominantly on individualistic health behaviours (e.g., diet and physical activity) at the expense of recognizing body weight diversity and the array of social factors (e.g., stigma and discrimination of marginalized identities) that may be linked to weight status. Research is needed to examine the extent to which individualistic health behaviours versus social factors contribute to weight status in adolescents. As such, the aim of this study was to investigate the relative contribution of individualistic health behaviours versus social factors to objective and perceptual indices of weight status.
Methods
Cross-sectional survey data were collected as part of the Toronto Public Health Student Survey and comprised students 12 to 19 years of age (N = 5515). Measures included perceived and objective weight status, social and demographic factors (e.g., gender, sexual orientation, school connectedness), and health behaviours (e.g., physical activity, nutritious consumption).
Results
Findings from latent variable regression models partially supported hypotheses, whereby social factors (i.e., age, sex, socio-economic access, sexual minority status) contribute similar amounts of variance, or relatively more variance in weight indices, compared to health behaviours (e.g., physical activity, nutritious consumption).
Conclusion
Contrary to traditional views of adolescent weight status, physical activity (i.e., school-based, individual, active transport) and nutritious consumption (i.e., fruits, vegetables, milk) were not associated with weight status, when considering social factors. These findings challenge the utility of public health approaches that target individualistic behaviours as critical risk factors in “obesity prevention” efforts in adolescence.
Keywords: Weight perception, Youth, Obesity, Health behaviour
Résumé
Objectifs
En matière de « prévention de l’obésité » chez les adolescents, les interventions en santé publique ont essentiellement porté leur attention sur les comportements de santé individualistes (par exemple, alimentation et activité physique), aux dépens de la valorisation de la diversité des poids corporels et de l’ensemble des facteurs sociaux (par exemple, stigmatisation et discrimination des identités marginalisées), qui sont parfois associés au statut pondéral. Des recherches sont toutefois indispensables afin de déterminer le degré de corrélation entre les comportements de santé individualistes et les facteurs sociaux susceptibles de favoriser le poids chez les adolescents. Par conséquent, il convient de se pencher sur le rôle joué par les comportements de santé individualistes face aux facteurs sociaux dans la détermination des indices objectifs et perceptifs du poids.
Méthodes
Les données recueillies lors de cette étude transversale ont été obtenues dans le cadre du Toronto Public Health Student Survey et ont été recueillies auprès d’étudiants âgés de 12 à 19 ans (N = 5 515). Les mesures prises comprenaient le statut de poids perçu et objectif, les facteurs sociaux et démographiques (par exemple, le sexe, l’orientation sexuelle, les rapports avec l’école) et les comportements liés à la santé (par exemple, l’activité physique, la consommation de substances nutritives).
Résultats
Les conclusions tirées des modèles de régression à variables latentes ont confirmé en partie les hypothèses selon lesquelles les facteurs sociaux (âge, sexe, accès socio-économique, statut de minorité sexuelle) apportent une variance similaire, ou relativement plus importante, aux indices de poids comparativement aux comportements liés à la santé (par exemple, l’activité physique, la consommation d’aliments nutritifs).
Conclusion
À la différence des vues traditionnelles sur le statut pondéral des adolescents, l’activité physique (c’est-à-dire à l’école, individuellement, dans les transports actifs) et la consommation de substances nutritives (c’est-à-dire de fruits, de légumes, de lait) n’ont pas fait l’objet d’une corrélation avec le statut pondéral, compte tenu des facteurs sociaux. Ces résultats contestent l’utilité des approches de santé publique axées sur les comportements individualistes à titre de facteurs de risque déterminants dans les efforts de « prévention de l’obésité » à l’adolescence.
Mots-clés: Perception du poids, jeunesse, obésité, comportements liés à la santé
Introduction
Public health efforts aimed at “obesity prevention” predominantly focus on individualistic health behaviour change, such as nutritious consumption and physical activity (WHO 2017). While enhancing health behaviours in adolescence contributes to favourable health outcomes in the long term, this approach overlooks the highly complex and dynamic systems (e.g., genetic, social, cultural, environmental) that contribute to weight status in adolescence (Rutter et al. 2017) and relies on the assumption that weight status is a reliable and accurate proxy for health (Tylka et al. 2014). Even though this mainstream weight-normative approach aligning health behaviours with weight status has been critiqued (Tomiyama et al. 2018), public health strategies largely focus on individualistic prevention efforts at the expense of addressing the complex array of factors and systems that might contribute to adolescents’ weight status and perceptions of their weight.
Due to the declines in physical activity and nutritious consumption during adolescence, and the normative classification of these behaviours as “modifiable risk factors” (Patton et al. 2016), adolescence is deemed as the target period for “obesity prevention.” Yet, these prevention efforts have historically yielded small and unsustainable weight-related outcomes in adolescents (Laska et al. 2012). “Obesity prevention” interventions may fail to produce sustained effects due to the underlying assumption that diet and physical activity behaviours are directly related to body mass index (BMI), the stigmatizing nature of messaging against higher weight individuals, and the conflation of weight with health (Bristow et al. 2020). While adolescence is a critical developmental period where health behaviours are cemented (Halfon and Hochstein 2002), positioning health behaviours as primary targets for “obesity prevention” ignores the harmful side effects that can result from a focus on weight-based outcomes (e.g., eating disorders, poor body image), while also overlooking the dynamic macro-level forces (e.g., household food insecurity, socio-economic status, and weight stigma) that determine the health behaviours in which they are able to engage (Patton et al. 2016).
Critical social factors that have been shown to contribute to an adolescent’s weight status include age, sex, socio-economic access (Barriuso et al. 2015), sexual and gender minority status (Grammer et al. 2019), country of birth (Beydoun and Wang 2010), and extent to which individuals feel connected to their social context (e.g., school; Sinton et al. 2012). Underlying these social factors are structural forces that discriminate against marginalized social identities and cause health inequities (Marmot 2005). For example, gender and sexual minority adolescents may experience unique stressors such as oppression, stigmatization, and bullying, which are associated with behavioural and physiological stress responses that have been shown to impact weight (Grammer et al. 2019; Puhl et al. 2019). Meanwhile, adolescents living in low-income neighbourhoods may have less access to nutritious foods, safe recreational areas, and health care (Larson et al. 2009; Lee and Cardel 2019), thereby potentially influencing weight status. An individual’s country of birth may also present confounding issues such as being a part of a racial or ethnic minority and acculturation adjustment for immigrants (Beydoun and Wang 2010), both of which have been linked to higher adolescent weight. Finally, an adolescent’s perception of school connectedness is important to consider given that feelings of loneliness or reduced level of social engagement are linked to higher weight (Sinton et al. 2012). Importantly, these social factors represent proxies by which social inequities can impact weight status (Marmot 2005). For most individuals, achieving sustained weight loss by focusing solely on reducing caloric intake and increasing exercise is highly unlikely over the long term (Laska et al. 2012) given that individual health behaviours are embedded in complex social structures. Social factors are uncontrollable at an individual level and can thwart an adolescent’s ability to access and engage in health-promoting behaviour.
To date, most weight-based research in adolescents has used body mass index (BMI) as a proxy for physical health, even though the BMI metric has been criticized for not representing any direct indication of health status (e.g., physical strength, metabolic fitness, blood sugar, blood pressure) (Burkhauser & Burkhauser and Cawley 2008). Weight and BMI metrics are highly problematic when used as the sole or primary indicators of health, in that they preclude considerations that individuals live within a wider socio-cultural context that impacts health, and that the perception of one’s weight can be uniquely linked to health outcomes. For example, the perception of one’s weight has been linked to health behaviours including type and level of food consumption, even after accounting for BMI (Gaylis et al. 2020). In school-based adolescent samples, weight perceptions have been shown to predict health behaviour, irrespective of objective weight status (Patte et al. 2016). Additionally, differences in weight perception can vary as a function of an individual’s sex, race/ethnicity, and socio-economic status (SES) (Paeratakul et al. 2002). As such, in order to inform public health interventions, it is critical to consider how social factors and health behaviours are associated with perceived as well as objective weight status.
The present research aimed to understand how engagement in traditional health behaviours (i.e., diet and physical activity) compared to social factors (i.e., age, sex, sexual orientation, gender identity, SES, country of birth, school connectedness) was related to perceived and objective weight status in a school-based sample of adolescents. Since the focus on behavioural interventions for youth has been a measurably futile endeavour in sustainably reducing weight (Stice et al. 2006), it was hypothesized that social factors would predict greater variance in both perceived and objective weight status relative to diet and physical activity behaviour.
Methods
Participants and procedures
The 2014 Toronto Public Health (TPH) Student Survey assessed the health and well-being of students in grades 7 to 12 enrolled in Toronto’s four public school boards. Using a stratified two-stage cluster design, one class per grade for each of the 165 selected schools was randomly selected to participate. Stratifications at the school level were based on school board, school size, and school SES. Active parental consent and student assent were obtained separately for the paper-and-pencil questionnaire (response rate of 50%, n = 6053) and for a physical assessment of height and weight which was conducted by a public health nurse (response rate of 46%, n = 5515). Measurement tools were informed by Toronto Public Health institutional priorities, and the present study consists of a secondary analysis of the data collected for these purposes. Full details of the methodology are published elsewhere (Corson et al. 2015). Approval was granted by the TPH research ethics review process, University of Toronto Research Ethics Board, as well as the research ethics departments of the four participating school boards. The ethical approval has been performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Measures
Weight indices
Height and weight were objectively assessed using scale and stadiometer. Weight perception was assessed using a previous World Health Organization instrument for adolescents (Currie et al. 2001) by selecting one of the following options in response to “I think my body is…” (e.g., much too thin, a bit too thin, about the right size, a bit too fat, much too fat).
Social factors
Participants reported current age, sex (i.e., male, female), gender identity (i.e., boy, girl, trans or other gender identity, not sure), sexual orientation (i.e., heterosexual, lesbian, gay, bisexual, other orientation, not sure),1 socio-economic access (i.e., family’s ease of access to basic goods and services, ranging from 1 = difficult to access to 10 = easiest to access), and country of birth. School connectedness was indicated by (i) closeness to peers at school, (ii) inclusion in school environment, (iii) happiness at school, (iv) fairness of adults at school, (v) feeling safe at school, and (vi) importance of academic grades (Likert scale ranging from 1 = strongly disagree to 4 = strongly agree).
Health behaviours
Physical activity indices comprised (i) engagement in organized school physical activity (i.e., yes, no, not offered), (ii) organized non-school physical activity (i.e., yes, no), (iii) individual physical activities outside of school (i.e., yes, no), and (iv) active transportation (i.e., walk/bicycle vs. motorized vehicle such as school bus, public transit, or passenger/driver in a car). Nutritious consumption was indicated by consumption of (i) vegetables, (ii) fruits, and (iii) milk, which were assessed by the number of times per day (i.e., never/sometimes but not daily, once a day, twice a day, 3 times a day, 4 times a day, 5 times a day, 6 times a day, 7 times a day, 8 or more times a day). Eating behaviour was indicated by (i) family meals per day/week (i.e., never, rarely, once a week, 2 to 3 times per week, 4 to 6 times per week, every day), (ii) breakfast on weekdays (i.e., never, 1 day, 2 days, 3 days, 4 days, 5 days), (iii) breakfast on weekends (i.e., no weekend day, only one weekend day, both weekend days), and (iv) going to bed hungry (i.e., never, rarely, once a week, 2 to 3 times per week, 4 to 6 times per week, every day).
Data analysis
Participant demographics (Table 1) and interfactor correlations (Table 2) were assessed. Relationships between behavioural and social determinant predictors were examined in relation to perceived weight and BMI-for-age through use of latent variable regression (LVR) analysis, which is a specific type of confirmatory structural equation model that includes latent variables as independent variables. LVR allows for unique weighting of each item in the construction of unobserved/latent variables (e.g., eating behaviour) from observed variables (e.g., BMI-for-age) and simultaneously models the structural paths (i.e., relationships between variables) and measurement paths (i.e., relationships between a latent variable and its indicators). LVR analysis is preferable to techniques such as multiple regression analysis because it is not based on the assumption that measurement of the variables is error-free, and therefore avoids potentially producing biased estimates (Muthén 2002). The LVR analyses were conducted using Mplus (Version 6.11) software and account for the ordered categorical nature of the scores.
Table 1.
Participant demographics (N = 5515)
| Variable | Score range | Mean (SD) or percentage |
|---|---|---|
| Age | 12–19 | 14.9 (1.9) |
| Sex | 46.8% male, 53.2% female | |
| BMI-for-age | 7.31–50.24 | 21.48 (4.20) |
| Sexual orientation | ||
| Heterosexual | 34.7% | |
| Lesbian/gay/bisexual/other/unsure | 3.9% | |
| Not asked | 60.0% | |
| Gender identity | ||
| Cisgender | 33.8% | |
| Gender non-conforming | 0.2% | |
| Not sure | 0.3% | |
| Not asked | 65.1% | |
| Socio-economic access ladder | ||
| Low access | 8.4% | |
| Middle access | 22.2% | |
| High access | 69.4% | |
| Born in Canada | 67.9% | |
| Born outside of Canada | 32.1% | |
| School connectedness | 1–4 | 3.27 (.44) |
| Physical activity (PA), % yes | ||
| Organized school PA | 52.3% | |
| Organized non-school PA | 49.9% | |
| Individual PA outside school | 74.0% | |
| Active transportation | 36.4% | |
| Nutrition consumption | ||
| Consumption of vegetables | 0–8 | 1.77 (1.77) |
| Consumption of fruits | 0–8 | 1.73 (1.84) |
| Consumption of milk | 0–8 | 2.12 (2.02) |
| Eating behaviours | ||
| Family meals (days/week) | 1–6 | 4.94 (1.50) |
| Breakfast on weekdays | 1–6 | 4.59 (1.90) |
| Breakfast on weekends | 1–3 | 2.66 (.64) |
| Going to bed hungry | 1–6 | 1.47 (.89) |
| Perceived weight | ||
| Much too thin | 2.1% | |
| A bit too thin | 14.4% | |
| About the right size | 42.5% | |
| A bit too fat | 27.7% | |
| Much too fat | 4.6% | |
| I do not think about it | 7.7% | |
Table 2.
Interfactor correlations
| Variable | 1 | 2 | 3 | 4 | 5 | 6 | 7 | 8 | 9 | 10 | 11 | 12 |
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| 1. Age | – | |||||||||||
| 2. Sex | − .02 | – | ||||||||||
| 3. Sexual orientation | − .61** | .02 | – | |||||||||
| 4. Gender identity | − .61** | .02 | .99** | – | ||||||||
| 5. Socio-economic access | .01 | .00 | .02 | .02 | – | |||||||
| 6. Born in Canada | .01 | − .02 | .02 | .02 | .05** | – | ||||||
| 7. Physical activity | .25** | .21** | .16** | .07* | − .23** | .18** | – | |||||
| 8. Nutritious consumption | − .11** | − .08** | − .02 | − .01 | .19** | − .09** | − .53** | – | ||||
| 9. Eating behaviours | − .31** | − .12** | − .18** | − .05 | .27** | − .01 | − .45** | .39** | – | |||
| 10. School connectedness | − .22** | − .06 | − .12** | − .03 | .25** | − .04* | − .31** | .19** | .35** | – | ||
| 11. Perceived weight | .01 | .01 | .04** | .04** | .06** | .06** | .08** | .04 | − .08** | − .05* | – | |
| 12. BMI-for-age | .01 | − .01 | − .04** | − .04** | .03* | − .00 | .14** | − .04* | .20** | − .10** | − .01 | – |
*p < 0.05; **p < 0.01. CR values were calculated for scores of independent variables and were found to be .80, .54, .63, and .55 for school connectedness, physical activity, nutritious consumption, and eating behaviours respectively. All other variables were single item indicators. Sex was coded as male = 1 and female = 2. Gender identity was coded as cisgender = 1, gender non-conformity = 2, trans or other gender identity = 3, and not sure = 4. Sexual orientation was coded as heterosexual = 1 and lesbian/gay/bisexual/other/not sure = 2. Country of birth was coded as Canadian-born = 1 and non-Canadian-born = 2. Physical activity indices were coded as yes = 1 and no or not offered = 2. Dietary variables were coded as number of times per day 0 = never/sometimes but not daily to 8 = eight or more times a day
A series of LVRs were conducted to examine the relative importance of behavioural and social determinants of body weight. First, physical activity, nutritious consumption, and eating behaviours were assessed as predictors of perceived weight and BMI-for-age. Second, social factors were added to the model to assess the relative importance of determinants of weight. Finally, a subanalysis was conducted with participants who completed sexual orientation and gender identity items on the survey. Pratt indices were calculated to compare relative variance between health behaviours and social determinant predictor variables.
Weighted least squares means and variance-adjusted (WLSMV) estimation was used with a polychoric correlation matrix to model ordered categorical data (Beauducel and Herzberg 2006). Missing data were estimated using pairwise-present and based on all of the available data, using the WLSMV algorithm within Mplus. To assess the model, models were compared using χ2 goodness of fit indices, comparative fit indices (CFI), Tucker-Lewis indices (TLI), and the root mean square error of approximation (RMSEA). Criterion for evaluating good model-data fit was designated as CFI and TLI values > .90, and RMSEA values < .08, and excellent fit for CFI and TLI values > .95, and RMSEA values < .06. Reliability was assessed via composite reliability (CR).
Results
Relationships between behavioural predictors and weight indices (model 1)
The behavioural predictor model (N = 5515) had good fit (χ2 (46) = 348.46, p < 0.001, CFI = .964, TLI = .948, RMSEA = .035, 90% CI [.031–.038]). Together, health behaviours explained 2% of the variance in perceived weight. Specifically, physical activity (β = .10), nutritious consumption (β = .13), and eating behaviours (β = − .09) were significant predictors of perceived weight (p < 0.01). Of the 2% of variance accounted for by the model, physical activity, nutritious consumption, and eating behaviours accounted for 40%, 36%, and 26% respectively. Physical activity (β = .09), nutritious consumption (β = .08), and eating behaviours (β = − .19) were significant predictors of BMI-for-age (p range 0.001 to 0.003) and explained 4.8% of the variance in BMI-for-age. Of the 4.8% of variance accounted for by the model, physical activity, nutritious consumption, and eating behaviours accounted for 26%, 7%, and 79% respectively.
Relationships between behavioural and social factors with weight indices (model 2)
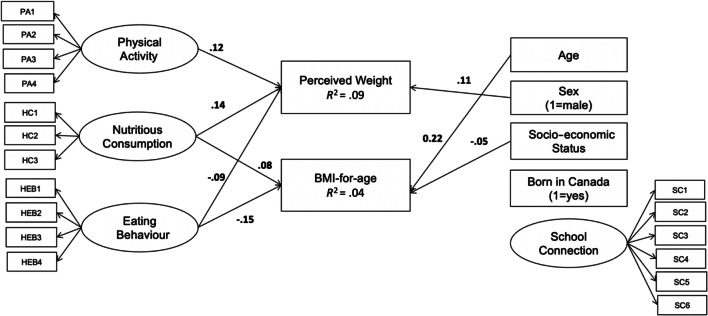
The behavioural and social predictor model (n = 4456) fit was (χ2 (186) = 3599.00, p < 0.001, CFI = .846, TLI = .813, RMSEA = .064, 90% CI [.062–.066]) and is presented in Table 3. Physical activity, nutritious consumption, eating behaviours, and sex were significant predictors of perceived weight, explaining 4% of the variance. Relative to each other, physical activity, nutritious consumption, eating behaviours, and sex accounted for 24%, 14%, 18%, and 3% respectively. Behavioural and social predictors explained 8% of the variance in BMI-for-age. Specifically, nutritious consumption, eating behaviours, age, and socio-economic access were found to be significant predictors of BMI-for-age. Of the 8% of variance accounted for by the model, nutritious consumption, eating behaviours, age, and socio-economic access accounted for 4%, 1%, 3%, and 4% respectively. For model summary, see Fig. 1.
Table 3.
Model 2 direct associations of behavioural and social factors on perceived weight and body mass index (n = 4456)
| β | Beta | Std error | p | 95% BCCI | |
|---|---|---|---|---|---|
| Physical activity | .12 | .16 | .13 | 0.001 | .06, .20 |
| .05 | .60 | .49 | 0.146 | − .02, .11 | |
| Nutritious consumption | .14 | .14 | .07 | < 0.001 | .08, .20 |
| .08 | .35 | .26 | 0.004 | .03, .13 | |
| Eating behaviours | − .09 | − .08 | .13 | 0.002 | − .15, − .03 |
| − .15 | − .30 | .49 | < 0.001 | − .20, − .09 | |
| School connectedness | − .02 | − .08 | .04 | 0.239 | − .06, .02 |
| − .02 | − .14 | .17 | 0.266 | − .06, .02 | |
| Age | − .02 | .01 | .02 | 0.259 | − .05, .01 |
| .22 | .43 | .08 | < 0.001 | .19, .25 | |
| Sex | .11 | .30 | .05 | < 0.001 | .08, .14 |
| − .01 | − .52 | .20 | 0.514 | − .04, .02 | |
| Socio-economic access | .01 | .01 | .02 | 0.542 | − .02, .04 |
| − .05 | − .16 | .07 | 0.003 | − .08, − .01 | |
| Born in Canada | .02 | .04 | .05 | 0.343 | − .02, .05 |
| .01 | − .12 | .21 | 0.614 | − .02, .04 |
Values associated with perceived weight are listed first; values associated with BMI-for-age are listed second
Fig. 1.
Model 2 results from latent and observed behavioural and socio-demographic health determinant predictors of perceived weight and BMI-for-age. Only significant (p < 0.05) paths are shown
Relationships between behavioural and social factors (including gender and sexual orientation) with weight indices (model 3)
Sexual orientation was added as a social factor in model 3 (Table 4). This was a subanalysis with n = 1669 participants who reported their sexual orientation. Gender identity was not included in the model due to collinearity with sexual orientation (r = .996, p < 0.001) and limited variability (i.e., 99% of sample reported identifying as cisgender (boy/girl)). The model fit was as follows: χ2 (202) = 1494.84, p < 0.001, CFI = .840, TLI = .808, RMSEA = .062, 90% CI [.059–.065], and predicted 4.1% of the variance in perceived weight, and 4.1% of the variance in BMI-for-age. Sex and sexual orientation were found to be significant predictors of perceived weight. Relative to each other, sex and sexual orientation accounted for 9% and 8% of the variance, respectively. Age, sex, sexual orientation, and socio-economic access were found to be significant predictors of BMI-for-age. Of the 4.1% of variance accounted for by the model, age, sex, sexual orientation, and socio-economic access accounted for 3%, 2%, 7%, and 4% respectively.
Table 4.
Model 3 subanalysis of direct associations of behavioural and social factors, including sexual orientation on perceived weight and body mass index (n = 1669)
| β | Beta | Std error | p | 95% BCCI | |
|---|---|---|---|---|---|
| Physical activity | .07 | .16 | .13 | 0.214 | − .04, .17 |
| .06 | .60 | .49 | 0.210 | − .04, .16 | |
| Nutritious consumption | .09 | .14 | .07 | 0.049 | .00, .18 |
| .06 | .35 | .26 | 0.180 | − .03, .15 | |
| Eating behaviours | − .03 | − .08 | .13 | 0.511 | − .14, .07 |
| − .03 | − .30 | .49 | 0.532 | − .13, .07 | |
| School connectedness | − .05 | − .08 | .04 | 0.086 | − .11, .01 |
| − .02 | − .14 | .17 | 0.416 | − .08, .03 | |
| Age | .01 | .01 | .02 | 0.617 | − .04, .06 |
| .14 | .43 | .08 | < 0.001 | .09, .19 | |
| Sex | .15 | .30 | .05 | < 0.001 | .10, .20 |
| − .06 | − .52 | .20 | 0.008 | − .11, − .02 | |
| Socio-economic status | .02 | .01 | .02 | 0.573 | − .04, .07 |
| − .06 | − .16 | .07 | 0.023 | − .12, − .01 | |
| Born in Canada | .02 | .04 | .05 | 0.429 | − .03, .07 |
| − .01 | − .12 | .21 | 0.562 | − .06, .03 | |
| Sexual orientation | .08 | .26 | .09 | 0.005 | .02, .13 |
| .07 | 1.03 | .39 | 0.008 | .02, .13 |
Values associated with perceived weight are listed first; values associated with BMI-for-age are listed second
Discussion
Contrary to traditional views of adolescent “obesity prevention,” the present findings partially supported the hypotheses, whereby social factors contributed either similar or slightly more variance in predicting weight perceptions and BMI-for-age compared with health behaviours. Notably, associations in the structural model were unique from interfactor correlations, indicating the importance of considering the interplay between factors when health behaviour and social factors are modelled simultaneously. However, the effect sizes in all models were consistently small (i.e., models predicting ≤ 8% total variance in weight indicators), suggesting that unmeasured factors (e.g., experienced and internalized weight stigma, mental health, household income) may be more important in predicting variance in adolescent weight status, and should be explored in future research.
Contrary to hypotheses, social factors (e.g., age, socio-economic access) contributed less (3.4%) relative variance in BMI-for-age compared with the health behaviours (5%), although difference in these relative contributions was minor. Specifically, when including social factors, physical activity was no longer a significant predictor of higher BMI-for-age. Although social factors explained less relative variance in BMI-for-age, they did predict unique variance in the weight indices above and beyond health behaviours, despite the small overall magnitude of effects. The finding that socio-economic access was related to objective weight status corroborates previous research in Canadian adolescents (Janssen et al. 2006). Given the present findings show that health behaviours contribute nearly negligible variability in weight status, and relatively less compared to social factors, the utility of nutrition and physical activity as risk factors is called into question. Rather, it may be valuable to reconstruct public health strategies to focus on factors related to the social inequities that may drive health outcomes directly.
Findings that girls are more vulnerable to worsened weight perceptions compared with boys have been reliably documented and may reflect gendered forces for socio-cultural weight ideals (Patte et al. 2016). Regardless of gender, engaging in more physical activity was associated with higher perceived weight status, but not with objective weight status. One explanation for this finding is that adolescents who use and endorse physical activity as a weight management strategy perceive their weight to be higher than it “should be,” or that those who engage in different types of physical activity perceive that type of physical activity (e.g., weight-lifting) to be related to a higher weight (Eisenberg et al. 2012). A closer look at different types of physical activity related to perceived weight status in future research may help clarify this relationship. Furthermore, it is possible that physical activity is a less reliable predictor of weight than conventionally hypothesized (Butryn et al. 2010).
As expected, higher frequency of health-promoting eating behaviour (e.g., family meals, breakfast consumption, not going to bed hungry) was associated with lower perceived and objective weight status, whereas unexpectantly, nutritious consumption (e.g., consuming vegetables, fruits, milk) was associated with higher perceived and objective weight. Engaging in higher frequency of regularly eating breakfast and eating with family may be more indicative of other factors that are associated with lower weight status (e.g., accessibility of food, spending more time with family, and overall socio-economic status), which are robustly associated with weight status (Fulkerson et al. 2008). Whereas, the type of food intake alone may be indicative of higher caloric intake and does not capture important social, cultural, and contextual factors that are integral to dietary practices. Given that age and socio-economic access predicted unique variance in the weight indices above and beyond health behaviours (despite small effects), greater emphasis on social factors versus individual health behaviours may be valuable.
A key study finding is in the subsample of participants with data on sexual orientation whereby none of the health behaviours were significant predictors of perceived weight or BMI-for-age. Specifically, female and sexual minority status were associated with higher perceptions of weight; and higher age, lower socio-economic access, male sex, and sexual minority status predicted higher BMI-for-age. Previous research in adolescents and young adults has reported that sexual minority females have higher BMI-for-age compared with non-minority females (Grammer et al. 2019), whereas the relationship between BMI-for-age in sexual minority males is confounded by age, with sexual minority males having higher BMI-for-age early in adolescence and then lower BMI-for-age later in adolescence compared with non-minority males (Deputy and Boehmer 2010). These unique associations regarding sexual minority status have been predominantly explained using a minority stress model, whereby exposure to prejudice and discrimination on the basis of minority status has a negative impact on health (Grammer et al. 2019). It is noteworthy that the original study hypothesis was only supported in the subsample that modelled sexual orientation as a predictor, thereby urging future research to consider sexual minority status as an important social factor of weight status, above and beyond health behaviours.
The current study has several limitations which should be considered for future research. First, the results are based on cross-sectional data, and therefore, causal direction cannot be inferred. Second, given that the measure of socio-economic access was self-reported and relative to peers, future research ought to utilize parental objective assessments of socio-economic access, such as income. Third, ethno-racial identity was pragmatically excluded from the analysis despite being assessed as a study variable due to the complexity of including a nominal or dichotomous set of variables in the structural equation model. Similarly, sexual orientation status was dichotomized due to the small sample sizes in the disaggregated categories. Since weight-related outcomes vary by ethno-racial identity and sexual orientation status and stigma associated with marginalized identities (Barriuso et al. 2015; Beydoun and Wang 2010), future research is needed to better represent these groups. Fourth, this study only examined social factors that may impact weight status (e.g., socio-economic access, age, sexual orientation) as proxies of the social forces that drive these relationships (e.g., experienced and internalized stigma related to weight and/or other marginalized social identities). It is critical to directly study how social inequities, stigma, and discrimination associated with marginalized identities are associated with weight status. Fifth, the operationalization of the health behaviour variables was limited to population-based items that were deemed acceptable to the school boards and public health agency disseminating the questionnaires. By examining the underlying latent constructs, some measurement error was reduced; however, conclusions are limited to the method in which the latent constructs were developed (e.g., capacity to include an item indicator in multiple constructs). As such, future research would benefit from using full-length questionnaires with validity evidence to assess the health behaviours in this study, such as dietary logs or recalls and full-length physical activity surveys, which can be corroborated with objective accelerometer-based metrics.
Conclusion
This research contributes to the emerging literature that recognizes the need to consider social factors beyond individual health behaviours in understanding adolescent weight status. Using a large and diverse sample of Canadian adolescents, the present findings challenge weight-normative approaches for the utility of health behaviour as the most critical factor in public health prevention and intervention targets. Considerations of the complex array of factors (e.g., socio-economic access, age, and sexual minority status) are necessary to understand the factors that impact adolescent weight status at a population level.
Acknowledgements
We would like to acknowledge the support of Dr. David McKeown, Paul Fleiszer, Vincenza Pietropaolo, Loren Vanderlinden, and Toronto Public Health staff involved in project planning and data collection and processing. The methodology pertaining to the present study has been published in a government report (Corson et al. (2015). Toronto Public Health: 2014 Toronto Public Health Student Survey: Research Methods. https://www.toronto.ca/wp-content/uploads/2017/12/8c33-tph-student-health-survey-web-final-aoda.pdf), and all contributors have agreed to this publication.
Authors’ contribution
EP: conceptualization; writing—original draft, review, and editing
BDS: conceptualization; formal analysis
LC: conceptualization; writing—review and editing
CF: conceptualization; writing—review and editing
KLH: writing—literature review and components of original draft
CMS: supervision; writing—review and editing
Compliance with ethical standards
Conflict of interest
The authors declare that they have no conflict of interest.
Footnotes
Survey questions regarding gender identity and sexual orientation were only asked to a subset of students, depending on school policies.
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- Barriuso L, Miqueleiz E, Albaladejo R, Villanueva R, Santos JM, Regidor E. Socioeconomic position and childhood-adolescent weight status in rich countries: a systematic review, 1990–2013. BMC Pediatr. 2015;15(1):129. doi: 10.1186/s12887-015-0443-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Beauducel, A., & Herzberg, P. Y. (2006). On the performance of maximum likelihood versus means and variance adjusted weighted least squares estimation in CFA. Struct Equ Model. 10.1207/s15328007sem1302_2.
- Beydoun MA, Wang Y. Pathways linking socioeconomic status to obesity through depression and lifestyle factors among young US adults. J Affect Disord. 2010;123(1–3):52–63. doi: 10.1016/j.jad.2009.09.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bristow, C., Meurer, C., Simmonds, J., & Snell, T. (2020). Anti-obesity public health messages and risk factors for disordered eating: a systematic review. Health Promot Int. [DOI] [PubMed]
- Burkhauser RV, Cawley J. Beyond BMI: the value of more accurate measures of fatness and obesity in social science research. J Health Econ. 2008;27(2):519–529. doi: 10.1016/j.jhealeco.2007.05.005. [DOI] [PubMed] [Google Scholar]
- Butryn, M. L., Wadden, T. A., Rukstalis, M. R., Bishop-Gilyard, C., Xanthopoulos, M. S., Louden, D., & Berkowitz, R. I. (2010). Maintenance of weight loss in adolescents: current status and future directions. J Obes. 10.1155/2010/789280. [DOI] [PMC free article] [PubMed]
- Corson L, Khandor E, Yue C. Toronto Public Health: 2014 Toronto Public Health Student Survey: research methods. 2015. [Google Scholar]
- Currie, C., Samdal, O., Boyce, W., & Smith, R. (2001). Health behaviour in school-aged children: a WHO cross-national study (HBSC), research protocol for the 2001/2002 survey. Child and Adolescent Health Research Unit (CAHRU), University of Edinburgh, 20.).
- Deputy, N. P., & Boehmer, U. (2010). Determinants of body weight among men of different sexual orientation. Prev Med. 10.1016/j.ypmed.2010.05.010. [DOI] [PubMed]
- Eisenberg, M. E., Wall, M., & Neumark-Sztainer, D. (2012). Muscle-enhancing behaviors among adolescent girls and boys. Pediatrics.10.1542/peds.2012-0095. [DOI] [PMC free article] [PubMed]
- Fulkerson, J. A., Neumark-Sztainer, D., Hannan, P. J., & Story, M. (2008). Family meal frequency and weight status among adolescents: cross-sectional and 5-year longitudinal associations. Obesity.10.1038/oby.2008.388. [DOI] [PubMed]
- Gaylis JB, Levy SS, Hong MY. Relationships between body weight perception, body mass index, physical activity, and food choices in Southern California male and female adolescents. Int J Adolesc Youth. 2020;25(1):264–275. doi: 10.1080/02673843.2019.1614465. [DOI] [Google Scholar]
- Grammer AC, Byrne ME, Pearlman AT, Klein DA, Schvey NA. Overweight and obesity in sexual and gender minority adolescents: a systematic review. Obes Rev. 2019;20(10):1350–1366. doi: 10.1111/obr.12906. [DOI] [PubMed] [Google Scholar]
- Halfon N, Hochstein M. Life course health development: an integrated framework for developing health, policy, and research. Milbank Q. 2002;80(3):433–479. doi: 10.1111/1468-0009.00019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Janssen, I., Boyce, W. F., Simpson, K., & Pickett, W. (2006). Influence of individual- and area-level measures of socioeconomic status on obesity, unhealthy eating, and physical inactivity in Canadian adolescents. Am J Clin Nutr. 10.1093/ajcn/83.1.139. [DOI] [PubMed]
- Larson NI, Story MT, Nelson MC. Neighborhood environments. American Journal of Preventive Medicine: Disparities in Access to Healthy Foods in the U.S; 2009. [DOI] [PubMed] [Google Scholar]
- Laska MN, Murray DM, Lytle LA, Harnack LJ. Longitudinal associations between key dietary behaviors and weight gain over time: transitions through the adolescent years. Obesity. 2012;20(1):118–125. doi: 10.1038/oby.2011.179. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Lee, A. M., & Cardel, M. I. (2019). Social status and adolescent physical activity: expanding the insurance hypothesis to incorporate energy expenditure. American Journal of Lifestyle Medicine. 10.1177/1559827618815449. [DOI] [PMC free article] [PubMed]
- Marmot M. Social determinants of health inequalities. Lancet. 2005;365(9464):1099–1104. doi: 10.1016/S0140-6736(05)71146-6. [DOI] [PubMed] [Google Scholar]
- Muthén, B. O. (2002). Beyond SEM: General latent variable modeling. Behaviormetrika. 10.2333/bhmk.29.81.
- Paeratakul S, White MA, Williamson DA, Ryan DH, Bray GA. Sex, race/ethnicity, socioeconomic status, and BMI in relation to self-perception of overweight. Obes Res. 2002;10(5):345–350. doi: 10.1038/oby.2002.48. [DOI] [PubMed] [Google Scholar]
- Patte, K. A., Laxer, R. E., Qian, W., & Leatherdale, S. T. (2016). An analysis of weight perception and physical activity and dietary behaviours among youth in the COMPASS study. SSM - Population Health. 10.1016/j.ssmph.2016.10.016. [DOI] [PMC free article] [PubMed]
- Patton GC, Sawyer SM, Santelli JS, Ross DA, Afifi R, Allen NB, et al. Our future: a Lancet Commission on adolescent health and wellbeing. Lancet. 2016;387(10036):2423–2478. doi: 10.1016/S0140-6736(16)00579-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Puhl, R. M., Himmelstein, M. S., & Watson, R. J. (2019). Weight-based victimization among sexual and gender minority adolescents: findings from a diverse national sample. Pediatric Obesity, 14(7), e12514. [DOI] [PMC free article] [PubMed]
- Rutter, H., Bes-Rastrollo, M., De Henauw, S., Lahti-Koski, M., Lehtinen-Jacks, S., Mullerova, D., et al. (2017). Balancing upstream and downstream measures to tackle the obesity epidemic: a position statement from the European Association for the Study of Obesity. Obesity Facts, 10(1), 61–63. [DOI] [PMC free article] [PubMed]
- Sinton, M. M., Goldschmidt, A. B., Aspen, V., Theim, K. R., Stein, R. I., Saelens, B. E., et al. (2012). Psychosocial correlates of shape and weight concerns in overweight pre-adolescents. Journal of Youth and Adolescence. 10.1007/s10964-011-9686-y. [DOI] [PMC free article] [PubMed]
- Stice, E., Shaw, H., & Marti, C. N. (2006). A meta-analytic review of obesity prevention programs for children and adolescents: the skinny on interventions that work. Psychol Bull. 10.1037/0033-2909.132.5.667. [DOI] [PMC free article] [PubMed]
- Tomiyama AJ, Carr D, Granberg EM, Major B, Robinson E, Sutin AR, Brewis A. How and why weight stigma drives the obesity ‘epidemic’ and harms health. BMC Med. 2018;16(1):123. doi: 10.1186/s12916-018-1116-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Tylka, T. L., Annunziato, R. A., Burgard, D., Daníelsdóttir, S., Shuman, E., Davis, C., & Calogero, R. M. (2014). The weight-inclusive versus weight-normative approach to health: evaluating the evidence for prioritizing well-being over weight loss. J Obes, 983495. [DOI] [PMC free article] [PubMed]
- World Health Organization . Adolescent obesity and related behaviours: trends and inequalities in the WHO European region, 2002–2014. 2017. [Google Scholar]