Abstract
A 59-year-old woman was referred with weakness, paraesthesia, numbness and clawing of the little and ring fingers for the last 2 years. MRI of the cervical spine was normal and nerve conduction velocity revealed abnormality of the ulnar nerve. Ultrasound and MRI showed medial osteophytes and effusion of the elbow joint with stretched and thinned ulnar nerve in the cubital tunnel. The patient underwent release and anterior transposition of the ulnar nerve with significant relief of symptoms.
Keywords: musculoskeletal and joint disorders, peripheral nerve disease, plastic and reconstructive surgery
Background
Ulnar nerve palsy can cause debilitating symptoms and interfere with activities of daily living. Primary elbow osteoarthritis is an uncommon condition rarely associated with ulnar nerve palsy and claw hand. Focused investigation of the spine and nerve may delay diagnosis of cause of ulnar claw hand. Infectious neuritis or extrinsic compression of the ulnar nerve can be imaged by ultrasound and MRI.
We present a case of ulnar claw hand due to compression of the ulnar nerve by osteophytes in a patient with previously undiagnosed primary osteoarthritis of the elbow and the outcome of surgical management with ulnar nerve release and transposition.
Case presentation
A 59-year-old obese woman (Body Mass Index 35.6) presented with weakness of the hand with paraesthesia and numbness in the ring and little fingers of the right hand for 2 years. She had a poor grip, with inability to cut and cook. There was no history of prior or recent trauma. She did not complain of pain or restriction of motion in the elbow joints. She had osteoarthritis of bilateral knees for which she was on non-steroidal anti-inflammatory drugs. She had no history of diabetes, hypothyroidism or inflammatory arthritis.
On examination, the patient had mild ulnar pattern of clawing of hand (ring and small finger clawing) with weakened grasp and decreased sensation in ulnar 1-1/2 digits.
Investigations
The patient initially underwent an MRI of the cervical spine without any evidence of cervical spondylosis, radiculopathy, syringomyelia or focal lesion. Nerve conduction study showed non-recordable sensory and motor velocity in the right ulnar nerve suggestive of right ulnar axonal neuropathy.
The patient was referred for ultrasound and MR neurography of the ulnar nerve.
On ultrasound, there was bowing of the nerve in the cubital tunnel with focal thickening with normal calibre and echogenicity proximal and distal to the tunnel. Synovial thickening and joint effusion were also observed, along with irregular cortical margins and medial osteophytes from the olecranon process (figures 1 and 2). There was atrophy of the flexor carpi ulnaris and medial fibres of the flexor digitorum with reduced muscle bulk and increased echogenicity due to denervation oedema. On dynamic ultrasound, there was no subluxation of the nerve. Radiographs of her right elbow showed extensive degenerative changes with loss of joint space and large marginal osteophytes seen originating from the medial aspect of the ulnohumeral joint (figure 3). Axial proton density (PD) and T2-weighted (T2W) sequences revealed ulno-trochlear joint osteophytes projecting medially into the cubital tunnel, along with synovial effusion, with displacement of the ulnar nerve and obliteration of the surrounding fat (figure 4). On T2W images the nerve showed focal moderate hyperintensity in the cubital tunnel with significant surrounding soft tissue oedema(figure 5). MR neurography depicted the focal thickening and hyperintensity of the ulnar nerve in the cubital tunnel (figure 6). There were no loose bodies or periarticular ganglion cysts. A combined effect of the osteophytes along with the thickened synovium and joint effusion causing compression, traction and friction of the nerve can been implicated as the cause for cubital tunnel syndrome in our patient.
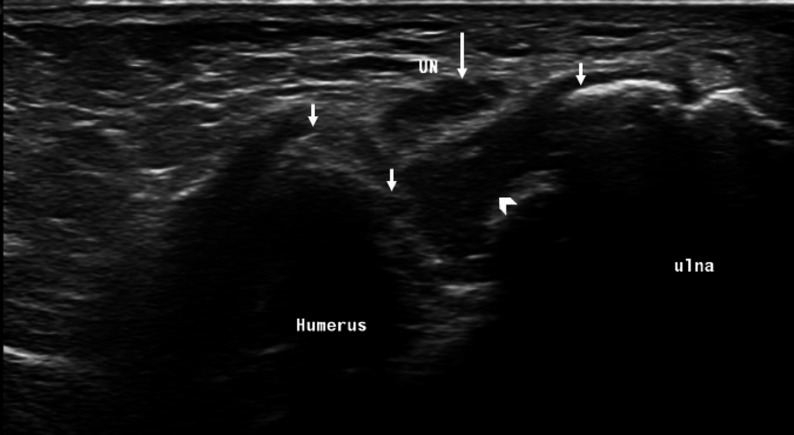
Figure 1.
Ultrasound of the cubital tunnel showing the UN in transverse section (large arrow). Ulnotrochlear portion of the elbow joint shows multiple bony spurs (small arrows) and joint effusion (arrowhead). The ulnar nerve is flattened, thickened and superficially displaced by the effusion. UN, ulnar nerve.
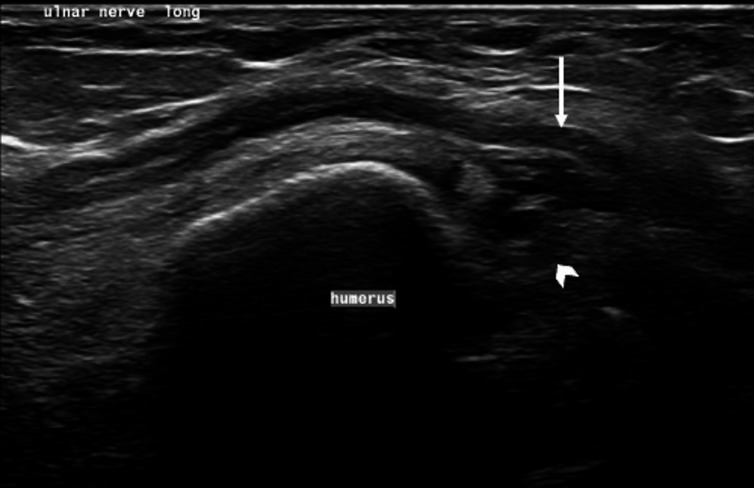
Figure 2.
Ultrasound of the ulnar nerve in the longitudinal axis in the cubital tunnel shows mild displacement and bowing (arrow) of the nerve. Synovial thickening (arrowhead) with adjacent joint effusion is seen.
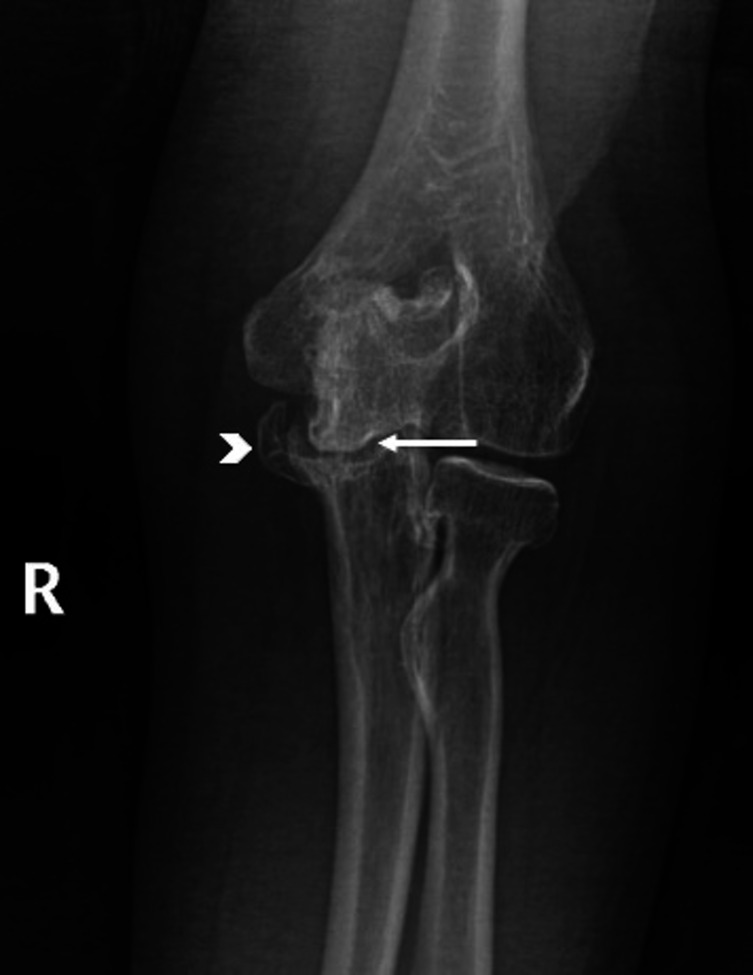
Figure 3.
Plain radiograph anteroposterior view of the elbow joint showing reduction in joint space (arrow) predominantly in the ulnotrochlear joint, subchondral sclerosis and large medially projecting osteophyte formation (arrowhead).
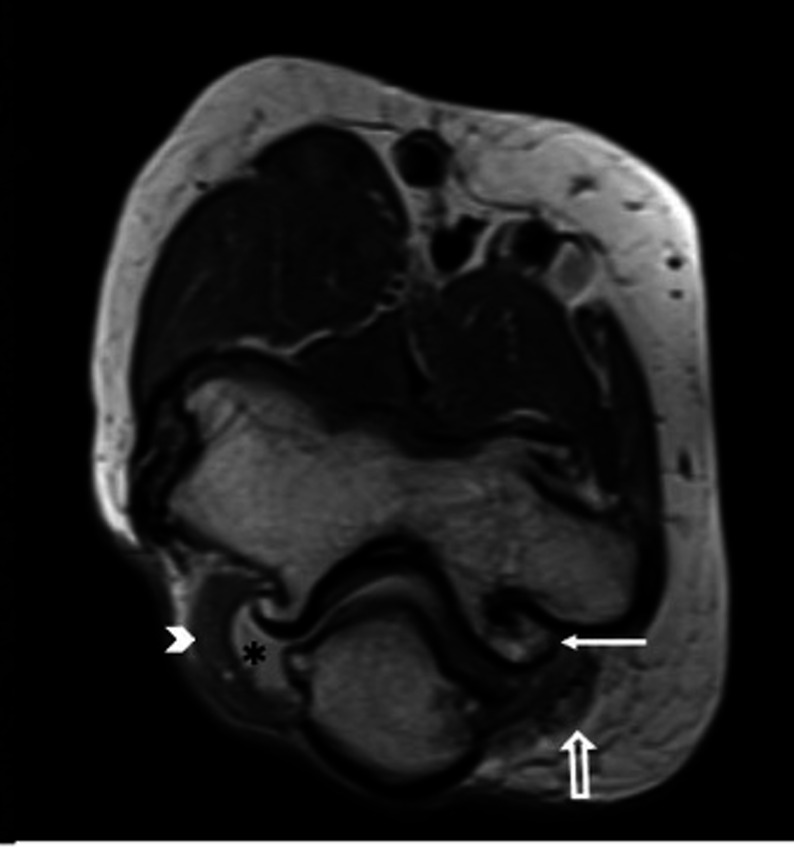
Figure 4.
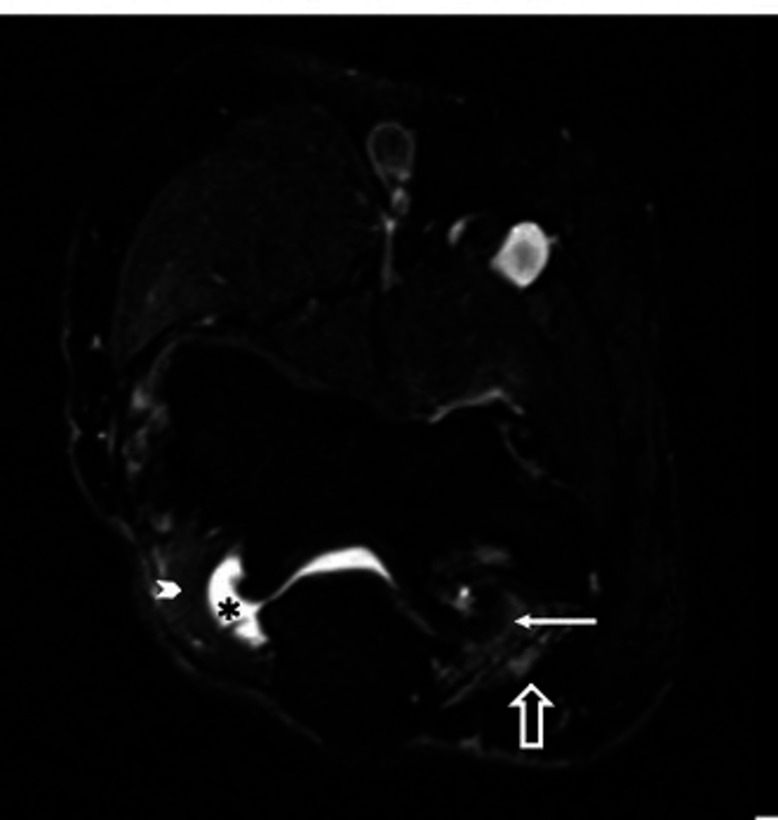
Axial proton density-weighted non-fat suppressed image reveals large marginal osteophytes arising from the ulnotrochlear joint (arrow) with minimal joint effusion (*) and synovits(arrowhead) within elbow joint. There is obliteration of fat in the cubital tunnel. The ulnar nerve (empty arrow) appears hyperintense and is displaced laterally.
Figure 5.
Axial T2-weighted fat suppressed image reveals large marginal osteophytes arising from ulnotrochlear joint (arrow) with minimal joint effusion (*) and synovits(arrowhead) within elbow joint. There is obliteration of fat in the cubital tunnel. The ulnar nerve (empty arrow) appears hyperintense and is displaced laterally.
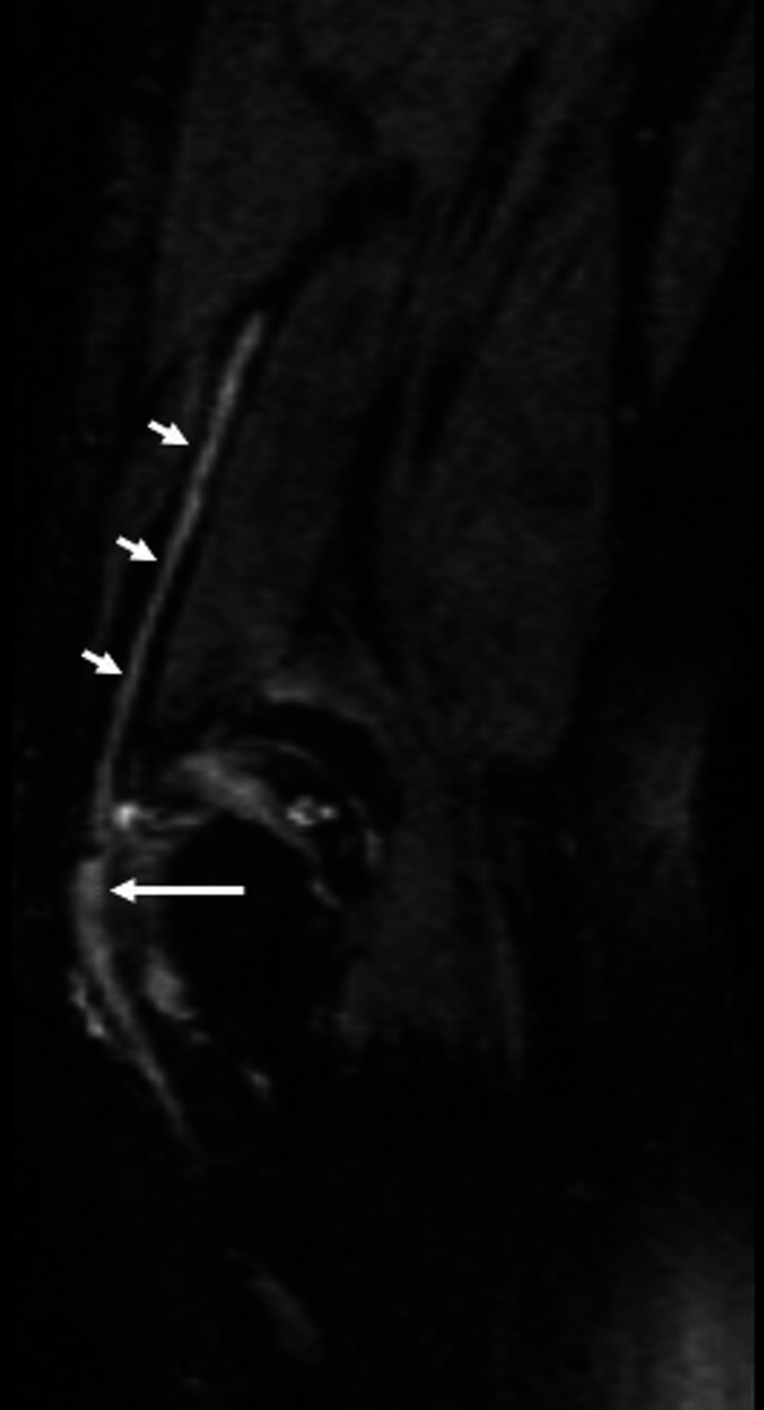
Figure 6.
MR neurography (PSIF-reverse TRUFISP) sagittal sequence of the elbow joint shows the course of the ulnar nerve (small arrows) with focal thickening and hyperintensity in the cubital tunnel (large arrow). TRUFISP, True Fast Imaging with Steady-state free Precession.
Differential diagnosis
Cervical spondylosis with cervical osteophytes or disc protrusions causing compression of the C8 and T1 nerve roots of ulnar nerve can present as ulnar claw hand and it was ruled out by a cervical MRI. Hansen’s disease, a common cause of ulnar neuropathy in the Indian subcontinent was ruled out by ultrasound. The ulnar nerve can be thickened and hypoechoic in the cubital tunnel and an abscess of the ulnar nerve can also be seen on ultrasound. Tardy ulnar nerve palsy is a delayed onset ulnar neuropathy in patients with a remote history of trauma (with fracture and callus formation or cubitus valgus or varus)and secondary osteoarthritis. Other common causes like accessory anconeus epitrochlearis, ganglion cyst and loose bodies from the elbow joint can be detected and differentiated on imaging. Osteophytes which appear as osseous projections and synovial effusion or synovitis compressing the ulnar nerve in the cubital tunnel are also well visualised on ultrasound and MRI.
Treatment
The patient underwent ulnar nerve release and transposition (figure 7). A 15 cm long incision was given between the medial epicondyle and the olecranon process along the cubital tunnel region under tourniquet control. The ulnar nerve was exposed proximally at the intramuscular septum and decompressed distally after opening the tight distal cubital tunnel. The nerve was exposed between the two heads of flexor carpi ulnaris. It was released from the distal tendinous edge of the muscle. It was found to be thickened and oedematous at the cubital tunnel region. After ensuring complete release of the nerve distally and proximally along its course, it was transposed anteriorly and was kept in a submuscular pocket as it was found to subluxate on flexing the elbow. The flexor pronator mass was incised and a submuscular pocket was created. The transposed ulnar nerve was kept inside the space thus created. The muscle was then reattached back with non-absorbable sutures after achieving haemostasis after release of tourniquet. A bulky dressing was applied. Range of motion exercises were started a week after surgery.
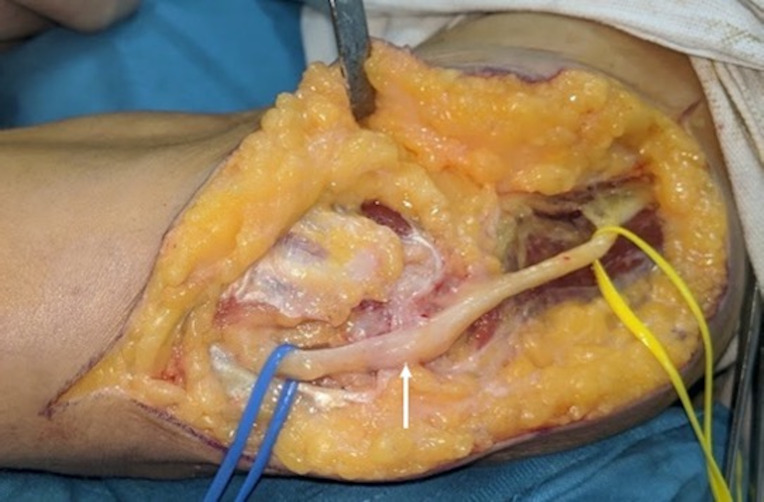
Figure 7.
Intraoperative image after ulnar nerve decompression shows the focally thickened ulnar nerve (arrow) at the cubital tunnel.
Outcome and follow-up
The patient was highly satisfied in terms of pain relief and decrease in the compression symptoms such as the pins and needles, paraesthesia, and numbness along the distribution of the ulnar nerve. We have a follow-up of 3 months.
Discussion
Primary osteoarthritis of the elbow is uncommon but can be associated with cubital tunnel syndrome and ulnar nerve palsy. However, not all patients with elbow osteoarthritis develop ulnar neuropathy. Increased cubital tunnel pressure in flexion, decreased size of the cubital tunnel, position of the medial osteophytes, and changes in shape of the cubital tunnel during flexion and extension have been implicated as causes of ulnar neuropathy due to osteoarthritis.1 Symptomatic patients have been reported to have larger humeral osteophyte areas within the cubital tunnel or a cubital tunnel divided by humeral osteophytes.1
Anteromedial osteophytes from humerus also cause more symptoms than posterior osteophytes, possibly due to impaction with medial coronoid process and trochlea during flexion.2
Ulnohumeral joint osteophytes are also more common in primary osteoarthritis as in our patient, due to disproportionate axial load bearing ranging from two times the body weight through the ulnohumeral joint on lifting even 2 kg weights.3
Ulnar nerve palsy due to osteoarthritis of the elbow is more commonly secondary to post-traumatic degenerative arthritis of the elbow and presents as a delayed ulnar neuropathy long after the injury has occurred, sometimes in childhood, and is known as tardy ulnar nerve palsy. Cubitus valgus deformity due to fractures of lateral condyle or cubitus varus due to supracondylar fractures or of medial epicondyle, radial head fractures and dislocations cause stretching of the ulnar nerve as it traverses through the cubital tunnel are implicated as one of the mechanisms of ulnar nerve palsy.4
The cubital tunnel is located between the olecranon process and medial epicondyle of humerus. The floor of the tunnel is formed by the joint capsule and the medial collateral ligament (posterior band) of the elbow joint and by the cubital retinaculum which straddles between the medial epicondyle and the olecranon process forms the roof.5 The ulnar nerve traverses within this limited space and repeated flexion movement of the elbow further exaggerates the space constraint resulting in both stretching and sliding of the nerve.
Among the peripheral nerve entrapment neuropathies of the upper limb, cubital tunnel syndrome is the second most common after carpal tunnel syndrome. Causes of extrinsic compression of the nerve in the cubital tunnel besides osteophytes include humeral fracture with loose bodies, accessory muscle, ganglion, infection. The nerve may also be injured at the elbow from repetitive ulnar nerve subluxation/dislocation.6 Most common cause of ulnar neuropathy is Hansen’s disease in the Indian subcontinent.
Clinically, both flexor digitorum profundus and superficialis palsy of the ring and little finger and sensory loss of the dorsum of the medial one and a half fingers with a weak grip strength of the hand indicate a high ulnar nerve involvement and not at Guyon’s canal. In our case, the patient did not complain of pain in the elbow region nor did she have any history of injury to the elbow in the past or valgus deformity to suggest a tardy ulnar nerve palsy; hence, localisation of the pathology at the elbow level could have been overlooked since primary osteoarthritis of elbow is relatively uncommon.
Imaging plays a crucial role not only in localising the site of nerve involvement as well as the exact cause of the neuropathy. High resolution ultrasonography of the nerve allows the nerve to be traced along its course with the advantage of allowing dynamic manoeuvres to be carried out especially to evaluate the subluxation and dislocation of the nerve across the medial humeral epicondyle in real time. Ultrasound can help localise the site of pathology when the exact site is unclear and help in planning MR neurography.
On MRI, a normal peripheral nerve is either similar or smaller than the accompanying artery, appears isointense to skeletal muscle on T1W images with well-outlined perineural fat and isointense to minimally hyperintense on T2 weighted fat-suppressed (T2FS) or Short Tau Inversion Recovery (STIR) images.7 Reverse FISP-Fast Imaging in Steady-state free Precession (PSIF) is a steady-state gradient echo sequence which optimally increases the conspicuity of nerve tissue signal by supressing signal from rest of the soft tissues including adjacent vessels.8 Abnormal nerves appear hyperintense to skeletal muscle. MRI also depicts the denervation changes in the muscles supplied by the nerve.
Conservative management is the first line of therapy. In patients with moderate to severe palsy, surgical management is preferred. Endoscopic approach to release the ulnar nerve is a reliable treatment for those with mild to moderate symptoms.9 Large osteophytes with the synovial thickening can also be debrided, with ulnar nerve release.10 Medial epicondylectomy is also an option for decompressing the area around the ulnar nerve but can lead to instability, flexor–pronator weakness and stiffness.11
The purpose of this case was to highlight our experience of primary elbow osteoarthritis presenting as compressive ulnar neuropathy in a patient without diabetes. In high ulnar nerve palsy, impingement of nerve due to osteoarthritis should be considered. One must be aware of the relevant anatomy and the possibility of the nerve entrapment due to degenerative changes especially in elderly individuals even in the absence of clinical manifestations of degenerative joint disease. Surgical treatment with ulnar nerve transposition was associated with good outcome.
Patient’s perspective.
I came to the neurology department for treatment of the troublesome folding of the fingers which was hampering my daily work. First investigation was cervical spine MRI, which was normal. They found some abnormality of the nerve on nerve conduction study but could not find the cause. Ultimately, ultrasound and X-ray were done and MRI confirmed my disease, which was not really causing much pain in my elbows, though I have arthritis of the knees. After this, I was immediately referred for surgery for releasing the ulnar nerve, which gave me a lot of relief and I could resume my household work.
Learning points.
Primary osteoarthritis of the elbow joint can present as ulnar neuropathy with claw hand.
Investigations should not be limited to the ulnar nerve but also evaluate the elbow joint.
Ultrasound can detect osteophytes and effusion within the elbow joint and demonstrate the cause of extrinsic ulnar nerve compression.
Footnotes
Contributors: SS: data acquisition, literature search and writing. AS: data acquisition, literature search, writing and editing. MP: literature search and writing. ST: data acquisition, clinical management, literature search and writing.
Funding: The authors have not declared a specific grant for this research from any funding agency in the public, commercial or not-for-profit sectors.
Competing interests: None declared.
Provenance and peer review: Not commissioned; externally peer reviewed.
References
- 1.Kawanishi Y, Miyake J, Omori S, et al. The association between cubital tunnel morphology and ulnar neuropathy in patients with elbow osteoarthritis. J Shoulder Elbow Surg 2014;23:938–45. 10.1016/j.jse.2014.01.047 [DOI] [PubMed] [Google Scholar]
- 2.Lim YW, van Riet RP, Mittal R, et al. Pattern of osteophyte distribution in primary osteoarthritis of the elbow. J Shoulder Elbow Surg 2008;17:963–6. 10.1016/j.jse.2008.03.012 [DOI] [PubMed] [Google Scholar]
- 3.Chadwick EK, Nicol AC. Elbow and wrist joint contact forces during occupational Pick and place activities. J Biomech 2000;33:591–600. 10.1016/S0021-9290(99)00184-0 [DOI] [PubMed] [Google Scholar]
- 4.Rubin G, Orbach H, Bor N, et al. Tardy ulnar nerve palsy. J Am Acad Orthop Surg 2019;27:717–25. 10.5435/JAAOS-D-18-00138 [DOI] [PubMed] [Google Scholar]
- 5.Cutts S. Cubital tunnel syndrome. Postgrad Med J 2007;83:28–31. 10.1136/pgmj.2006.047456 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Jacobson JA, Fessell DP, Lobo LDG, et al. Entrapment neuropathies I: upper limb (carpal tunnel excluded). Semin Musculoskelet Radiol 2010;14:473–86. 10.1055/s-0030-1268068 [DOI] [PubMed] [Google Scholar]
- 7.Kim S, Choi J-Y, Huh Y-M, et al. Role of magnetic resonance imaging in entrapment and compressive neuropathy--what, where, and how to see the peripheral nerves on the musculoskeletal magnetic resonance image: part 2. Upper extremity. Eur Radiol 2007;17:509–22. 10.1007/s00330-006-0180-y [DOI] [PubMed] [Google Scholar]
- 8.Thawait SK, Chaudhry V, Thawait GK, et al. High-Resolution MR neurography of diffuse peripheral nerve lesions. AJNR Am J Neuroradiol 2011;32:1365–72. 10.3174/ajnr.A2257 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Hoffmann R, Siemionow M. The endoscopic management of cubital tunnel syndrome. J Hand Surg Am 2006;31:23–9. 10.1016/J.JHSB.2005.08.008 [DOI] [PubMed] [Google Scholar]
- 10.Yan H, Cui G-Q, Wang J-Q, et al. Arthroscopic debridement of osteoarthritic elbow in professional athletes. Chin Med J 2011;124:4223–8. [PubMed] [Google Scholar]
- 11.Gaspar MP, Jacoby SM, Osterman AL, et al. Risk factors predicting revision surgery after medial epicondylectomy for primary cubital tunnel syndrome. J Shoulder Elbow Surg 2016;25:681–7. 10.1016/j.jse.2015.10.024 [DOI] [PubMed] [Google Scholar]