Abstract
Background
Most clinicians would probably agree that what patients think will happen can influence what does happen over the clinical course. Yet despite useful narrative reviews on expectancy of therapeutic gain >and the mechanisms by which expectancy can affect health outcomes, we were unable to locate a systematic review of the predictive relation between patients' recovery expectations and their health outcomes.
Methods
We searched MEDLINE for English-language articles published from 1966 to June 1998 with a title or abstract containing at least 1 of the medical subject headings (MeSH) “self-assessment,” “self-concept” or “attitude to health,” or the MeSH subheading “psychology,” and at least 1 word from each of 3 sets: “patient” and similar words; a form of “expectation,” “belief” or “prediction”; and a form of “recover,” “outcome,” “survival” or “improve.” Relevant articles contained original research data, measured patients' recovery expectations, independently measured a subsequent health outcome and analyzed the relation between expectations and outcomes. We assessed internal validity using quality criteria for prognostic studies based on 6 categories (case definition; patient selection; extent of follow-up; objective outcome criteria; measurement and reporting of recovery expectations; and analysis).
Results
A total of 1243 titles or abstracts were identified through the computer search, and 93 full-text articles were retrieved. Forty-one of these articles met the relevance criteria, along with 4 additional articles identified through other means. Agreement beyond chance on quality assessments of 18 randomly selected articles was high (kappa = 0.87, p = 0.001). Sixteen of the 45 articles provided moderate-quality evidence and included a range of clinical conditions and study designs; 15 of the 16 showed that positive expectations were associated with better health outcomes. The strength of the relation depended on the clinical conditions and the measures used.
Interpretation
Consistency across the studies reviewed and the evidence they provided support the need for clinicians to clarify patients' expectations and to assist them in having appropriate expectations of recovery. The understanding of the nature, extent and clinical implications of the relation between expectations and outcomes could be enhanced by more conceptually driven and methodologically sound research, including evaluations of intervention effectiveness.
Clinicians have long been aware of the placebo effect1 and of the influence of patient expectations in psychotherapy.2 Patient psychological factors, including expectation of outcome, have been found to be crucial to the success of rehabilitation3 and linked to levels of postoperative pain and recovery.4 On the basis of such evidence, most clinicians would probably agree that what patients think will happen (their recovery expectations) can influence what actually happens (their health outcomes).
Yet despite useful narrative reviews on expectancy of therapeutic gain5 and the mechanisms by which expectancy can affect outcomes,6 we were unable to locate a systematic review of the predictive relation between patients' recovery expectations and subsequent health outcomes. In this article we report on such a review we conducted using accepted procedures for locating, selecting and evaluating the quality of evidence.7 We summarize qualitatively the results of studies in the medical literature that provide at least moderate-quality evidence, comment on approaches to utilization of existing evidence and suggest fruitful research avenues.
Methods
We searched the MEDLINE database for English-language articles published from 1966 to June 1998 that contained in the title or abstract each of the following: (a) at least 1 of “patient,” “survivor,” “client,” “self-,” “subject,” “participant” or “outpatient”; (b) a form of at least 1 of “expectation,” “belief” or “prediction”; and (c) a form of “recover,” “outcome,” “survival” or “improve.” In addition, the word from (a) had to appear within 4 words of the word from (b), and the citation had to have at least 1 of the medical subject headings (MeSH) “self-assessment,” “self concept” or “attitude to health” or the MeSH subheading “psychology.” The titles and abstracts identified by this search strategy were perused by one of us (M.V.M.) to determine whether the articles contained original research results (i.e., were primary studies), measured patients' recovery expectations, independently measured a health outcome at a later point and analyzed the relation between these measures. If these relevance criteria were all met or there was some uncertainty as to whether they were met, the full-text article was obtained. A few additional relevant articles were identified through other means (e.g., reference lists, suggestions by colleagues). A review of the full articles by 2 of us (M.V.M. and D.C.C.) permitted consensus agreement on the application of the relevance criteria. We subsequently conducted a parallel search of the PsychInfo database, which unearthed equivalent numbers of potentially relevant abstracts. We decided not to pursue retrieval and inclusion of them for this report because the abstract contents corroborated the findings from our MEDLINE search.
A quality assessment modelled after approaches described elsewhere8,9 was used to assess the internal validity of the identified studies (Table 1). To be considered as providing moderate-quality evidence, the studies had to have a follow-up of 80% of the total sample, have outcome criteria appropriate to the research question, clearly describe the instrument used to measure recovery expectations, and have a stratified analysis, adjustment for a single confounder or presentation of data in a manner that would allow analysis of subsets. One of us (M.V.M.) assessed the validity of each of the selected articles. Another (D.C.C.), who was blind to the assessment of the first author, independently evaluated 18 randomly selected articles for quality of evidence. Agreement beyond chance between assessors on a dichotomous classification of moderate versus weak quality was calculated using Cohen's kappa statistic.10 The second reviewer subsequently assessed the validity of all the articles deemed by the first author as having provided moderate-quality evidence. Disagreements in assessments of quality of evidence at this stage were resolved by consensus.
Table 1
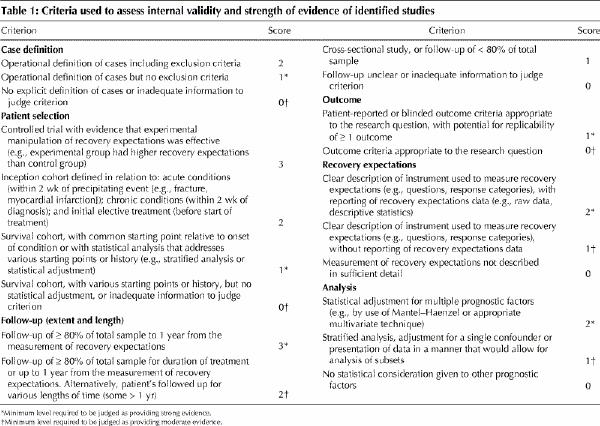
Substantial differences in conditions, questions, outcomes and analytic strategies prevented more formal quantitative summation of effect sizes. Qualitative interpretation of effect sizes was done in keeping with Cohen's approach.11 Synthesis thus relied on the qualitative approach of reflecting on commonalities and differences, and on linking with conceptual work and research findings.12
Results
The MEDLINE search identified 1243 titles and abstracts, and 93 full-text articles were retrieved. Forty-one of these articles met the relevance criteria, along with 4 additional articles identified by other means. Agreement beyond chance between the 2 reviewers on quality assessments of the randomly selected articles produced a kappa value of 0.87 (17 of 18 studies, p = 0.001). Although weak studies provided a wider range of interesting examples of expectations predicting outcomes, they raised sufficient validity concerns that we elected not to rely on them further (the list and quality assessments of these 29 articles are available from the authors upon request). The lack of statistical control for the effects of other potential prognostic factors (e.g., severity of condition) either through stratified or multivariate analysis was the most common weakness (19 of the 29 studies). Incompleteness of follow-up or cross-sectional character (6 studies) and unclear descriptions of the measurement of recovery expectations (5 studies) were the other weaknesses; 8 weak studies had more than one problem. Sixteen articles were deemed by both reviewers to provide evidence of at least moderate quality (Table 2). Although each study presented different strengths and weaknesses, the lack of exclusion criteria in case definition, the reliance on survival cohorts, the limited duration of follow-up and the limited reporting of data on recovery expectations were the most common problems that prevented an assessment of strong evidence in these 16 studies.
Table 2
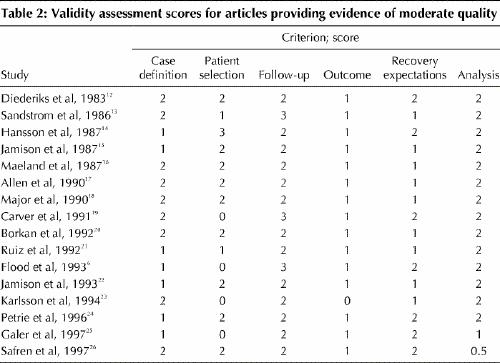
Table 3 describes the questions, results and effect sizes for the different clinical conditions in the 16 studies that provided moderate-quality evidence. Fifteen of the studies were observational, and 1 was experimental.15 Myocardial infarction was the most commonly studied condition (in 3 of the studies);13,17,25 the next most commonly studied conditions were cardiac surgery,18,22 chronic pain14,26 and psychiatric conditions15,27 (each in 2 studies). Only 2 studies shared a common question regarding expectations (anticipation of postoperative pain on a scale ranging from “not at all” to “extremely”).16,23 Studies tended to include a minimum of 1 variable covering at least 2 of the biologic and physiologic, psychological or social domains (e.g., peak creatinine kinase and mental health index in myocardial infarction patients,25 or Nottingham Health Profile and occupation in prostatectomy cases6).
Table 3
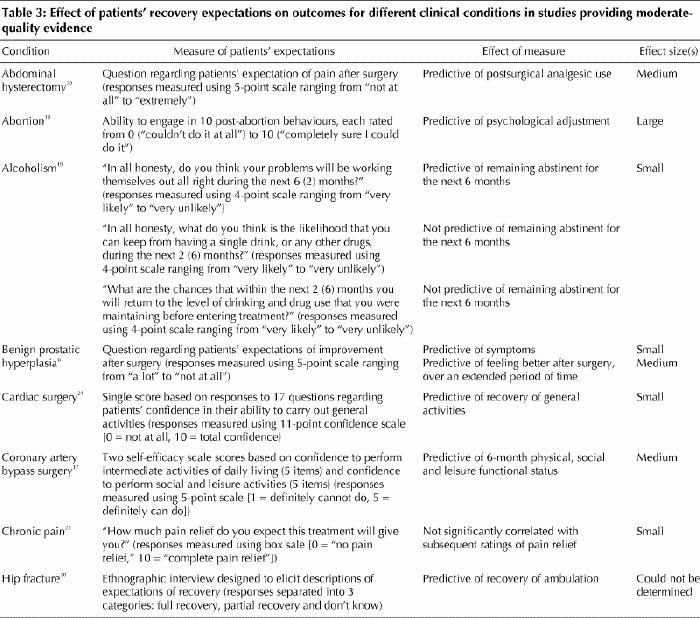
Table 3 continued
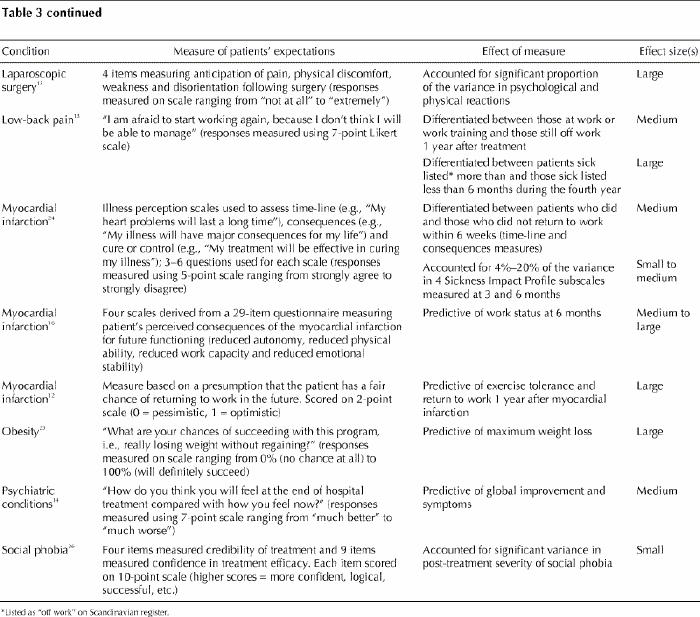
Simultaneous control for the effects of biologic and physiologic variables or of psychological or social variables6,13,15,16,17,19,22,25 usually had little effect on the strength of the relation between expectations and outcome, which indicated an independent influence of recovery expectations on health outcomes. Maximum effect sizes within a study for differences in recovery expectations, estimable for all but one of the studies, ranged from small (4 of 15 studies) through medium (5 studies) to large (6 studies). Little differentiation in effect size by type of condition was apparent, although smaller effect sizes tended to be more common for psychological conditions (e.g., social phobia), and larger effect sizes for medical conditions (e.g., obesity). Measures of the predictive utility of measurements of recovery expectations were minimal (only 1 study reported on the sensitivity and specificity of a question [68% and 71% respectively], which asked patients with chronic low-back pain to predict the outcome of a vocational rehabilitation program14). Estimates of relative risks of a given outcome for various levels of recovery expectations were absent. Emphasis was on statistical inference testing rather than on predictive utility.28,29
Interpretation
The 16 studies providing moderate-quality evidence invoked a variety of explanations for the role of patients' recovery expectations in predicting outcome. Bandura's concept of self-efficacy30 was the most common theoretical framework (in 4 of 16 articles). Previous experience, vicarious learning, verbal persuasion and social support were all thought to contribute to recovery expectations.19 Flood and colleagues6 summarized 5 mechanisms by which expectations can affect outcomes: “triggering of a physiologic response, acting to help motivate patients to achieve better outcomes, conditioning the patient psychologically to observe certain types of symptoms and ignore others, changing the understanding of the disease, or acting in concert with anxiety to heighten or reduce symptoms.” Such alternative explanations are consistent with evidence that feelings and perceptions may profoundly affect biological disease processes through behavioural and nonbehavioural mechanisms.31,32 Studies in psychoneuroimmunology and psychoneuroendocrinology have documented mechanisms by which negative-affect states, and the experiences that cause them (e.g., recovery slower or less complete than one expects), can translate into pathogenetic processes.33,34,35,36 Hence “recovery disappointment” may act through mind–body pathways and result in less than optimal outcomes across illness or injury processes.
Most authors suggested ways to apply their research; for example, patients who expect complications should be “targeted for psychological support and patient education prior to surgery,”16 and the assessment of illness perceptions may help to identify which patients “may benefit from another intervention before attending a rehabilitation programme.”25 Uncertainty about the causal versus the predictive role of patients' recovery expectations, hesitation in deliberately manipulating expectations, and limited rigorous evaluation of interventions to modify expectations (in 1 of the studies we reviewed) may limit such suggestions. Yet the consistency across studies and the supporting body of corroborative evidence argue for more confidence in the research findings. While avoiding the generation of false hopes and assisting patients with appropriate recovery expectations, physicians may improve adherence to treatment regimens and foster patient behaviours that “not only require positive motivation but also the knowledge and skills to pursue the desired goals.”17
Considerable scope exists for improving the validity and utility of research into the effect of recovery expectations on health outcomes. Ways to achieve this could include working toward a core set of reliable and valid measures of recovery expectations, bearing in mind that “the best prediction of outcome would be an expectancy-measure whose domain of behaviour matches that of the outcome”;17 including such measures in prognostic models37,38,39,40 while articulating better the effect size associated with such measures for clinical audiences;8,41,42 and incorporating such measures into trials that treat recovery expectations as an intermediate variable, measured at baseline and modified through interventions. Such research should improve treatment recommendations for effective methods of fostering more positive recovery expectations and of ultimately improving patient health outcomes.
Footnotes
This article has been peer reviewed.
Acknowledgements: We thank Emma Irvin, Sandro Mosnia and Julie Lucas for library assistance, and Linda Harlowe for help in preparing the manuscript.
This project was sponsored by the Institute for Work and Health. The institute, an independent, not-for-profit research organization, receives support from the Ontario Workplace Safety and Insurance Board.
Competing interests: None declared.
Correspondence to: Dr. Donald C. Cole, Institute for Work and Health, 702–250 Bloor St. E, Toronto ON M4W 1E6; dcole@iwh.on.ca
References
- 1.Beecher HK. The powerful placebo. JAMA 1955;159:1602-6. [DOI] [PubMed]
- 2.Goldstein AP. Participant expectancies in psychotherapy. Psychiatry 1962;25: 72-9. [DOI] [PubMed]
- 3.Albrecht GL, Higgins PC. Rehabilitation success: the interrelationships of multiple criteria. J Health Soc Behav 1977;18:36-45. [PubMed]
- 4.Taenzer P, Melzack R, Jeans ME. Influence of psychological factors on postoperative pain, mood and analgesic requirements. Pain 1986;24:331-42. [DOI] [PubMed]
- 5.Wilkins W. Expectancy of therapeutic gain: an empirical and conceptual critique. J Consult Clin Psychol 1973;40(1):69-77. [DOI] [PubMed]
- 6.Flood AB, Lorence DP, Ding J, McPherson K, Black NA. The role of expectations in patients' reports of post-operative outcomes and improvement following therapy. Med Care 1993;31:1043-56. [DOI] [PubMed]
- 7.Oxman AD, Guyatt GH. Guidelines for reading literature reviews. CMAJ 1988;138(8):697-703. [PMC free article] [PubMed]
- 8.Laupacis A, Wells G, Richardson WS, Tugwell P. Users' guides to the medical literature. V. How to use an article about prognosis. Evidence-Based Medicine Working Group. JAMA 1994;272:234-7. [DOI] [PubMed]
- 9.Hudak PL, Cole DC, Haines AT. Understanding prognosis to improve rehabilitation: the example of lateral elbow pain. Arch Phys Med Rehabil 1996;77:586-93. [DOI] [PubMed]
- 10.Cohen J. A coefficient of agreement for minimal scales. Educ Psychol Measure 1960;20:37.
- 11.Cohen J. A power primer. Psychol Bull 1992;112(1):155-9. [DOI] [PubMed]
- 12.Light RJ, Pillemer DB. Summing up: the science of reviewing research. Cambridge (MA): Harvard University Press; 1984.
- 13.Diederiks JP, van der Sluijs H, Weeda HW, Schobre MG. Predictors of physical activity one year after myocardial infarction. Scand J Rehabil Med 1983;15:103-7. [PubMed]
- 14.Sandstrom J, Esbjornsson E. Return to work after rehabilitation. The significance of the patient's own prediction. Scand J Rehabil Med 1986;18:29-33. [PubMed]
- 15.Hansson L, Berglund M. Factors influencing treatment outcome and patient satisfaction in a short-term psychiatric ward. A path analysis study of the importance of patient involvement in treatment planning. Eur Arch Psychiatry Neurol Sci 1987;236:269-75. [DOI] [PubMed]
- 16.Jamison RN, Parris WC, Maxson WS. Psychological factors influencing recovery from outpatient surgery. Behav Res Ther 1987;25:31-7. [DOI] [PubMed]
- 17.Maeland JG, Havik OE. Psychological predictors for return to work after a myocardial infarction. J Psychosom Res 1987;31:471-81. [DOI] [PubMed]
- 18.Allen JK, Becker DM, Swank RT. Factors related to functional status after coronary artery bypass surgery. Heart Lung 1990;19:337-43. [PubMed]
- 19.Major B, Cozzarelli C, Sciacchitano AM, et al. Perceived social support, self-efficacy, and adjustment to abortion. J Pers Soc Psychol 1990;59:452-63. [DOI] [PubMed]
- 20.Carver CS, Dunham RG. Abstinence expectancy and abstinence among men undergoing inpatient treatment for alcoholism. J Subst Abuse 1991;3:39-57. [DOI] [PubMed]
- 21.Borkan JM, Quirk M. Expectations and outcomes after hip fracture among the elderly. Int J Aging Hum Dev 1992;34:339-50. [DOI] [PubMed]
- 22.Ruiz BA, Dibble SL, Gilliss CL, Gortner SR. Predictors of general activity 8 weeks after cardiac surgery. Appl Nurs Res 1992;5:59-65. [DOI] [PubMed]
- 23.Jamison RN, Taft K, O'Hara JP, Ferrante FM. Psychosocial and pharmacologic predictors of satisfaction with intravenous patient-controlled analgesia. Anesth Analg 1993;77:121-5. [PubMed]
- 24.Karlsson J, Hallgren P, Kral J, Lindroos AK, Sjostrom L, Sullivan M. Predictors and effects of long-term dieting on mental well-being and weight loss in obese women. Appetite 1994;23:15-26. [DOI] [PubMed]
- 25.Petrie KJ, Weinman J, Sharpe N, Buckley J. Role of patients' view of their illness in predicting return to work and functioning after myocardial infarction: longitudinal study. BMJ 1996;312:1191-4. [DOI] [PMC free article] [PubMed]
- 26.Galer BS, Schwartz L, Turner JA. Do patient and physician expectations predict response to pain-relieving procedures? Clin J Pain 1997;13:348-51. [DOI] [PubMed]
- 27.Safren SA, Heimberg RG, Juster HR. Clients' expectancies and their relationship to pretreatment symptomatology and outcome of cognitive-behavioral group treatment for social phobia. J Consult Clin Psychol 1997;65:694-8. [DOI] [PubMed]
- 28.Kazis LE, Anderson JJ, Meenan RF. Effect sizes for interpreting changes in health status. Med Care 1989;27(3):178-89. [DOI] [PubMed]
- 29.Fletcher RH, Fletcher SW, Wagner EH. Clinical epidemiology: the essentials. Baltimore: Williams & Wilkins; 1996. p. 1-276.
- 30.Bandura A. Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev 1977;84:191-215. [DOI] [PubMed]
- 31.Cohen S, Herbert TB. Health psychology: psychological factors and physical disease from the perspective of human psychoneuroimmunology [review]. Annu Rev Psychol 1996;47:113-42. [DOI] [PubMed]
- 32.Adler R, Felten DL, Cohen N. Psychoneuroimmunology. 2nd ed. New York: Academic Press; 1991.
- 33.Kaplan HB. Social psychology and the immune system: a conceptual framework and review of the literature. Soc Sci Med 1991;33:909-23. [DOI] [PubMed]
- 34.Sternberg EM, Gold PW. The mind-body interaction in disease. Sci Am 1997;7:8-15.
- 35.Kelly S, Hertzman C, Daniels M. Searching for the biological pathways between stress and health. Annu Rev Public Health 1997;18:437-62. [DOI] [PubMed]
- 36.Coe C. Psychosocial factors and psychoneuroimmunology within a lifespan perspective. In: Keating DP, Hertzman C, editors. Developmental health and the wealth of nations. New York: Guilford Press; 1999. p. 201-19
- 37.Engel GL. The need for a new medical model: a challenge for biomedicine. Science 1977;196:129-36. [DOI] [PubMed]
- 38.Waddell G. Biopsychosocial analysis of low back pain. Baillieres Clin Rheumatol 1992;6(3):523-57. [DOI] [PubMed]
- 39.Wilson IB, Cleary PD. Linking clinical variables with health-related quality of life. A conceptual model of patient outcomes. JAMA 1995;273:59-65. [PubMed]
- 40.Talo S, Rytökoski U, Hämäläinen A, Kallio V. The biospychosocial disease consequence model in rehabilitation: model development in the Finnish ‘Work hardening’ programme for chronic pain. Int J Rehabil Res 1996;19:93-109. [PubMed]
- 41.Mitchell PH. The significance of treatment effects: Significance to whom? Med Care 1995;33:AS280-5. [PubMed]
- 42.Deyo RA, Patrick DL. The significance of treatment effects: the clinical perspective [review]. Med Care 1995;33:AS286-91. [PubMed]


