Abstract
Objectives:
To explore the effects of a hypnotic communication (HC) training for paediatric nurses in decreasing patients’ pain and distress during venipunctures.
Methods:
A 4-day theoretical and practical HC training was offered to five paediatric oncology nurses. The effects of HC were tested with 22 young cancer patients (13 girls, 9 boys, 10 ± 4 years) over four time points, with 88 encounters being video-recorded and coded in stable professional-patient dyads. Patients’ pain and distress were rated by patients and parents with visual analogue scales and coded from recordings using the Faces, Legs, Activity, Cry and Consolability (FLACC) scale.
Results:
We observed a significant decrease in pre-post distress reported by parents (d = 0.45, p = 0.046). Two out of five nurses with higher skills acquisition had larger reduction in patients’ self-reported pain (d = 1.03, p = 0.028), parents perceived pain (d = 1.09, p = 0.042), distress (d = 1.05, p = 0.043) as well as observed pain (d = 1.22, p = 0.025). Favourable results on pain and distress did not maintain at follow-up.
Conclusion and clinical implications:
Training nurses in HC may translate into improved pain and distress in patients, both self-rated and observed provided that skills are used in practice. HC training is a promising non-pharmacological intervention to address pain in paediatrics.
Keywords: Procedural pain, distress, paediatric, haematology oncology, hypnotic communication, nurses’ training
Introduction
Children with cancer experience repetitive painful needle procedures along the trajectory.1 Previous studies have observed that medical procedures can cause significant medical stress and may complicate care, yield avoidance or adherence issues.2 It is therefore crucial to manage pain and distress from an early age. Pharmacological interventions, such as local anaesthetic (EMLA cream®),3 and non-pharmacological interventions (e.g. Buzzy®,4 distraction,5 hypnosis1,6) are typically used by the healthcare team to prevent and manage procedural pain.
Among non-pharmacological interventions, hypnosis has been considered as highly relevant due to the high suggestibility of children.7 Previous studies have demonstrated the efficacy of hypnosis as a single or combined intervention, in reducing procedural pain7–17 and distress7,8,11–15 in children with cancer. In these studies, healthcare professionals performed the medical procedure while another professional (e.g. hypnotherapist) provided the hypnosis talk. This setting is a major barrier to the use of these techniques in day-to-day paediatric clinics.18 Recently, nurses have themselves used the hypnotic communication (HC) skills while performing the painful procedure.19 To date, such studies are extremely rare and have not linked the professional’s behaviour with patient’s level of pain/distress.
Mizrahi et al.19 developed and evaluated a short training course in HC for nurses in paediatric haematology-oncology. A hypnosis-certified psychologist conducted four 5-hour sessions of HC training (Figure 1). The content was adapted from manuals of hypnotic intervention in children and is available in previous reports.19,20 When studying skills acquisition in nurses, authors found medium-large desirable behavioural changes following the training in a group of nurses.21 In this study, we aim at reporting changes at the patients’ level. First, we assessed whether training in HC was associated with expected improvements in pain and distress. Second, we explored whether such improvements would be related to the use of HC techniques in practice.
Figure 1.
Content of the hypnotic communication techniques (HCTech) training sessions.
Methods
This exploratory study was conducted at the Haematology-Oncology day care clinic at a large tertiary Canadian hospital. Ethical approval was received by our local Research Ethics Committee (#2015-849) and all participants (patients and nurses) provided written informed consent. The reporting of this study was previously published and is compliant with the TREND Statement.19,22
Inclusion and exclusion criteria
To be included in this study, cancer patients had to be aged between 5 and 18 years old and have regular follow-up at the clinic and understand French. Patients who had previously been exposed to hypnosis or hypnosis-derived communication were excluded, as were those who came to the clinic for an unexpected appointment or those with a psychiatric disorder. Nurses were required to work at the outpatient haematology-oncology day care clinic, have previous experience performing venipuncture (VP) in paediatrics and have no prior experience in hypnosis or hypnosis-derived communication.
Participants and setting
We invited 6 nurses and 36 patients to participate in this study. Nurses took part in the 4-day HC training at our hospital. Using a convenience sampling method, the research assistant assigned six patients from the clinic’s computer database to each nurse. The first six patients meeting the criteria were contacted by phone and received preliminary information on the study. Patients and their parent(s) subsequently met with a researcher (T.M. or J.A.) to obtain additional information about the study and sign their consent. Then, patients were received at the day care haematology-oncology clinic by the nurses for a VP, which was video-recorded. After the VP, patients, parents and the researcher completed evaluation scales.
Patients’ distress and pain, and nurses’ HC skills were assessed at four time points: two in pre-training (T1 and T2 on average, respectively, 119 and 148 days before the training) and two in post-training (T3 and T4 on average, respectively, 137 and 203 days after the training). The training took place on 16, 17, 23 and 24 September 2015 and data collection was carried out from March 2015 to November 2016.
Measures
Socio-demographic and medical information
For nurses, we collected age and years of service. For patients, we collected age, sex, cancer diagnosis and the date of diagnosis.
Self-reported pain and distress
Visual analogue scale (VAS) was used in this study to assess fear and pain of VP rated by children and their parents. The VAS is a well-validated, appropriate, efficient and easy-to-use scale in children from 5 to 18 years old.23–25 As the concept of distress is not expected to be mastered by the younger children of this sample, we used self-report with anchor term referring to levels of fear.26 Respondents were asked ‘how much you/your child feared the venipuncture’, from 0 to 10, ‘no fear at all’ to ‘a lot of fear’, respectively. To assess pain (children) and perception of pain (parents), respondents replied to the item ‘how much pain did you/your child feel during the venipuncture?’, 0 being ‘no pain at all’, and 10 ‘extreme pain’.
Observed pain
We used the FLACC (Faces, Legs, Activity, Cry and Consolability) Scale to code pain from video-recorded encounters.27–29 This internationally validated scale measures procedural pain and distress in children from birth to 18 years. Research has identified substantial levels of pain and distress in young children using FLACC during commonly performed emergency department procedures.19 Inter-rater reliability of FLACC in this dataset was excellent (median intraclass correlation coefficient (ICC) = 0.789).
Sainte-Justine Hypnotic Communication Assessment Scale
This scale was used to assess communication behaviours in video-recorded nurse–patient encounters.20 It is based on 11 core items of hypnosis-derived communication to prevent pain and distress in children. For each item, an independent rater evaluates whether the behaviour is present (1) or absent (0). Two count scores are computed, one on the quality of the relationship (subscore 0–5) and one on the quality of the communication technique (subscore 0–6). A total score is computed by adding all 11 items (range, 0–11). The score is transformed to a percentage. In this dataset, we had excellent inter-rater reliability for the total score and the two subscores (median ICC = 0.879), when raters were blind of assessment time points and when raters had different professional backgrounds.20 At the same time, nurses were asked to answer a question related to the technique used: 0 = ‘no technique’, 1 = ‘guided imagery’, 2 = ‘switch’, 3 = ‘pain transformation’.
Data analysis
To explore stability between the two pre-training time points, we computed differences (Cohen’s d) and absolute stability30 on the VAS measures and the FLACC. For comparisons of pain and distress over time, we used the non-parametric Wilcoxon test. Effect sizes (Cohen’s d) were calculated to compare the differences between pre-training and post-training assessment for the whole sample and for each nurse in particular. An alpha level of 0.05 was set for inference statistics. As the sample size was limited, and consistent with the exploratory nature of the study, we put more emphasis on effect sizes. Analyses were performed with the SPSS 25 software.
Results
Final sample and preliminary analyses
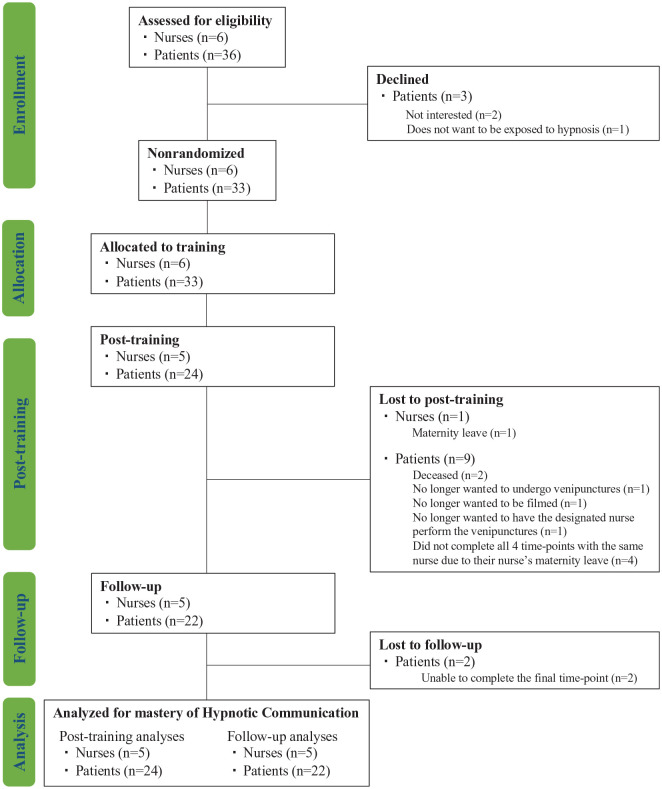
We included 6 female paediatric oncology nurses aged 33 ± 6 years and 33 of their cancer patients (16 boys, 17 girls) aged 10 ± 4 years. Among these participants, one nurse stopped training for maternity leave, and seven patients did not complete the study: two passed away and five dropped out (see Figure 2). Five nurses aged 33 ± 5 years completed the full HC training. Twenty-two patients (13 girls, 9 boys) aged 10 ± 4 years participated in all time points with the same nurse and were available for complete pre-, post- and follow-up analyses. Data were derived from 88 stable dyad nurse–patient encounters.
Figure 2.
Flow chart.
When considering data points before training, we observed stability in all measures: Sainte-Justine Hypnotic Communication Assessment Scale (SJ-HCAS) scores (ICCs = 0.630–0.766, d = 0.141–0.167), VAS scales (ICCs = 0.681–0.862, d = −0.216 to 0.000) and the FLACC score (ICCs = −0.058, d = −0.058). Consequently, we averaged both pre-training time points to form one baseline value for each outcome.
Changes in pain and distress following the training
When considering all available nurse–patient interactions (n = 88), no significant change on pain or distress reported by patient, pain reported by parent, and observed pain was detected, either in post-training or follow-up (ds = 0.26–0.32). We found a significant reduction in post-training distress scores as perceived by parents (Z = −1.993, p = 0.046, d = 0.45, small), not maintained in follow-up.
However, when investigating the same results across nurses, we found heterogeneity in the sample, with significant changes for nurses C and D. For these nurses, pre-post comparisons showed large differences on self-reported pain (ds = 0.94–1.03), parent-reported pain (ds = 0.90–1.19), observed pain (ds = 0.95–1.43) and medium-large differences on parent-reported distress (ds = 0.73–1.82). We did not observe changes on pre-post self-reported distress (ds = 0.23–0.28) and the maintenance of these effects in follow-up. In contrast, in nurses A, B and F, we observed negligible changes, with the exception of patient’s self-report distress pre-post in Nurse A (d = 0.84) and Observed pain pre-follow-up in Nurse F (d = 0.96) (Supplemental material – Figure S1).
Role of HC skills acquisition and technique use
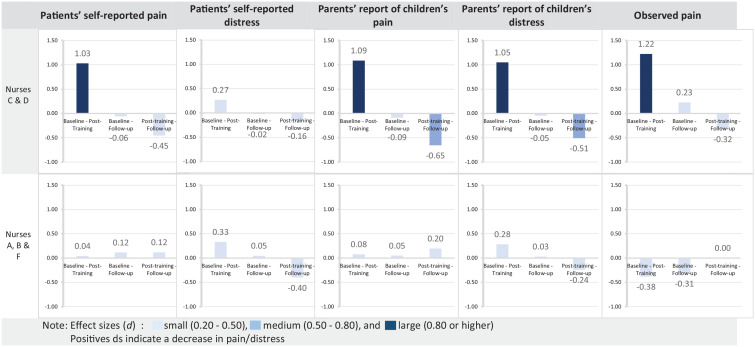
The observed changes in effect sizes among these nurses were consistent with the results demonstrated in the skills acquisition study, showing larger scores of HC techniques among nurses C and D (ds = 1.21–1.51), as compared to A, B and F (ds = 0.32–0.71).21 When comparing changes at the patient’s level for the two groups of nurses [C, D] versus [A, B, F], we found a large reduction in self-reported pain (Z = −2.201, p = 0.028, d = 1.03), parent-reported pain (Z = −2.032, p = 0.042, d = 1.09), observed pain (Z = −2.243, p = 0.025, d = 1.22) and parent-reported distress (Z = −2.023, p = 0.043, d = 1.05) for [C, D], while no significant results were observed for the other group [A, B, F]. In summary, nurses who improved most on their communication skills also demonstrated greater changes on pain and distress (Figure 3). Yet, effects were limited to post-training and did not maintain over time.
Figure 3.
Cohen’s d across time points for patients’ pain and distress scores for nurses C and D compared to nurses A, B and F.
To further document the relationship between the use of techniques with the observed outcomes at the patient level, we focused on video-recorded interactions and compared the observed pain (FLACC scores) in encounters demonstrating desired communication techniques (proportions of encounters post: n = 9, 42%, follow-up: n = 8, 40%) versus encounters with no such techniques. When selecting encounters demonstrating the use of HC techniques, we found a maintained reduction in observed pain in the former group (pre-post: Z = −2.255, p = 0.024, d = 1.05; pre-follow-up: Z = −2.028, p = 0.043, d = 0.93). This was not observed when techniques were not used (pre-post: Z = −1.350, p = 0.177, d = −0.41; pre-follow-up: Z = −1.548, p = 0.122, d = −0.43). Notably, only the ‘guided imagery’ technique was used by nurses.
Discussion
The management of procedural pain requires the evaluation of simple and easily applicable techniques in healthcare networks.2,31 The present project aimed to meet this need by exploring patient-level effects of a HC training for paediatric nurses.19 Following training, we found a reduction on self-reported pain, parent-reported pain, parent-reported distress and observed pain, but only when nurses showed high skills acquisition.
While our first objective was to evaluate whether training in HC was associated with improvements in pain and distress, we found little support for this when considering the whole group. Yet, there was heterogeneity among the participating nurses, and when isolating those who showed higher skills acquisition, we observed favourable short-time reduction in self-reported pain, parent-reported pain, observed pain and parent-reported distress. This is coherent with the model of the training and is an encouragement to use and refine this type of training. Yet, changes did not hold overtime at the patient level in those who improved their skills in HC. Although disappointing, this result is consistent with the Nurse Competency Acquisition Study.21 In this study, after completing the training, the results showed a decrease in nurses’ HC skills. This suggests that skills should be reinforced to maintain benefits in the long term. To address this limitation, continuing education and supervision will probably be important. As it is observed in medical pedagogy, follow-up training is often required to enhance health caregivers’ skills.32 One important output of this research points to a refinement of the training in adding supervision, or reorganizing future training over time so that sessions may better benefit from application to practice (e.g. four weekly sessions instead of 4 consecutive days). Additional refinements were also suggested by nurses in a previous qualitative survey.21
Interestingly, when focusing on encounters where nurses actually used the communication techniques, we found improvements in observed pain, both post-training and at follow-up. This means that patients who encountered a nurse who used the HC technique experienced a significant reduction in observed video-coded pain, whereas this was not the case when the nurse did not practice HC. It is the first time that nurses’ hypnotic behaviour is directly associated with pain reduction and strongly suggests that it would be beneficial to use adequate HC techniques to prevent pain in children. Importantly, this result was evaluated by tracking stable dyads over time and thereby controlling for several interpersonal biases. Although we know that hypnotic techniques are very effective in reducing pain according to the literature, previous studies demonstrating the positive effects of HC have been evaluated with two separate providers: the nurse and a hypnotherapist.10–15 In this study, we observed self-initiated HC effects. This highlights the potential impact of an inexpensive and easy-to-implement non-pharmacological intervention on pain and procedural distress.
Despite these encouraging results, we must recognize the study limitations. First, the samples were small and analyses lacked power. We tried to deal with this issue by emphasizing effect sizes in our interpretations, as it is usual in exploratory studies. The study should be replicated in a larger pilot design with a comparison to a control group, following recommendations for programme development.33 However, the results lend support to favourable outcomes when skills are used in practice. Second, we had a significant dropout rate, particularly due to the maternity leave of a nurse, which caused the exclusion of several patients from the study. This important feasibility aspect should be anticipated in future trials aiming at testing the effects of HC training. Finally, we were unable to control the time laps between encounters due to the clinical work organization. To limit time bias, it would be important in future trials to better standardize time points. As this appeared difficult to do in practice when stable dyads were observed, one could observe nurses’ skills in controlled simulation protocols.
In conclusion, this exploratory study with 22 stable dyads followed over time showed that a HC training of nurses was associated with a short-time reduction in procedural pain and distress of patients in nurses who acquired skills following training. Notably, there was a more durable change in observed pain in encounters where the nurse effectively used the HC communication techniques. This supports further developments of simple HC training to meet the increasing demand for non-pharmacological, low-cost and easy-to-implement techniques in paediatric oncology. Future research should refine HC training and further explore the link between HC communication behaviours in professionals and the pain response in paediatric patients.
Supplemental Material
Supplemental material, Figure_S1 for Does practising hypnosis-derived communication techniques by oncology nurses translate into reduced pain and distress in their patients? An exploratory study by David Ogez, Jennifer Aramideh, Terry Mizrahi, Marie-Claude Charest, Caroline Plante, Michel Duval and Serge Sultan in British Journal of Pain
Acknowledgments
The authors wish to thank Cybelle Abate for her help with the data collection.
Footnotes
Conflict of interest: The author(s) declared no potential conflicts of interest with respect to the research, authorship and/or publication of this article.
Contributorship: D.O. and J.A. wrote the first draft of the manuscript. All authors reviewed and edited the manuscript and approved the final version of the manuscript.
Ethical approval: Ethical approval for this study was obtained from Sainte-Justine Research Ethics Committee.
Funding: The author(s) disclosed receipt of the following financial support for the research, authorship and/or publication of this article: Support for this research came from the Sainte-Justine UHC Foundation through the Centre of Psycho-Oncology (recipient Serge Sultan) and the Fonds pour la Recherche du Québec – Santé (FRQs) through a post-doctoral fellowship to D.O.
Guarantor: S.S. is the guarantor of this article.
Informed consent: Written informed consent was obtained from all subjects before the study.
ORCID iDs: David Ogez  https://orcid.org/0000-0002-7441-9678
https://orcid.org/0000-0002-7441-9678
Serge Sultan  https://orcid.org/0000-0002-7520-1734
https://orcid.org/0000-0002-7520-1734
Supplemental material: Supplemental material for this article is available online.
References
- 1. Birnie KA, Noel M, Parker JA, et al. Systematic review and meta-analysis of distraction and hypnosis for needle-related pain and distress in children and adolescents. J Pediatr Psychol 2014; 39(8): 783–808. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Pai AL, Kazak AE. Pediatric medical traumatic stress in pediatric oncology: family systems interventions. Curr Opin Pediatr 2006; 18(5): 558–562. [DOI] [PubMed] [Google Scholar]
- 3. Rogers TL, Ostrow CL. The use of EMLA cream to decrease venipuncture pain in children. J Pediatr Nurs 2004; 19(1): 33–39. [DOI] [PubMed] [Google Scholar]
- 4. Şahiner NC, İnal S, Akbay AS. The effect of combined stimulation of external cold and vibration during immunization on pain and anxiety levels in children. J Perianesth Nurs 2015; 30(3): 228–235. [DOI] [PubMed] [Google Scholar]
- 5. Koller D, Goldman RD. Distraction techniques for children undergoing procedures: a critical review of pediatric research. J Pediatr Nurs 2012; 27(6): 652–681. [DOI] [PubMed] [Google Scholar]
- 6. Accardi MC, Milling LS. The effectiveness of hypnosis for reducing procedure-related pain in children and adolescents: a comprehensive methodological review. J Behav Med 2009; 32(4): 328–339. [DOI] [PubMed] [Google Scholar]
- 7. Kuttner L, Bowman M, Teasdale M. Psychological treatment of distress, pain, and anxiety for young children with cancer. J Dev Behav Pediatr 1988; 9(6): 374–381. [PubMed] [Google Scholar]
- 8. Hawkins PJ, Liossi C, Ewart BW, et al. Hypnosis in the alleviation of procedure related pain and distress in paediatric oncology patients. Contemporary Hypnosis 1998; 15: 199–207. [Google Scholar]
- 9. Hilgard JR, LeBaron S. Relief of anxiety and pain in children and adolescents with cancer: quantitative measures and clinical observations. Int J Clin Exp Hypn 1982; 30(4): 417–442. [DOI] [PubMed] [Google Scholar]
- 10. Katz ER, Kellerman J, Ellenberg L. Hypnosis in the reduction of acute pain and distress in children with cancer. J Pediatr Psychol 1987; 12(3): 379–394. [DOI] [PubMed] [Google Scholar]
- 11. Liossi C, Hatira P. Clinical hypnosis versus cognitive behavioral training for pain management with pediatric cancer patients undergoing bone marrow aspirations. Int J Clin Exp Hypn 1999; 47(2): 104–116. [DOI] [PubMed] [Google Scholar]
- 12. Liossi C, Hatira P. Clinical hypnosis in the alleviation of procedure-related pain in pediatric oncology patients. Int J Clin Exp Hypn 2003; 51(1): 4–28. [DOI] [PubMed] [Google Scholar]
- 13. Liossi C, White P, Hatira P. Randomized clinical trial of local anesthetic versus a combination of local anesthetic with self-hypnosis in the management of pediatric procedure-related pain. Health Psychol 2006; 25(3): 307–315. [DOI] [PubMed] [Google Scholar]
- 14. Liossi C, White P, Hatira P. A randomized clinical trial of a brief hypnosis intervention to control venepuncture-related pain of paediatric cancer patients. Pain 2009; 142(3): 255–263. [DOI] [PubMed] [Google Scholar]
- 15. Smith JT, Barabasz A, Barabasz M. Comparison of hypnosis and distraction in severely ill children undergoing painful medical procedures. J Counsel Psychol 1996; 43: 187–195. [Google Scholar]
- 16. Wall VJ, Womack W. Hypnotic versus active cognitive strategies for alleviation of procedural distress in pediatric oncology patients. Am J Clin Hypn 1989; 31(3): 181–191. [DOI] [PubMed] [Google Scholar]
- 17. Zeltzer L, LeBaron S. Hypnosis and nonhypnotic techniques for reduction of pain and anxiety during painful procedures in children and adolescents with cancer. J Pediatr 1982; 101(6): 1032–1035. [DOI] [PubMed] [Google Scholar]
- 18. Yeh VM, Schnur JB, Montgomery GH. Disseminating hypnosis to health care settings: applying the RE-AIM framework. Psychol Conscious 2014; 1(2): 213–228. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Mizrahi T, Sultan S, Charest M-C, et al. Training nurses in basic hypno-analgesia techniques to reduce procedural distress and pain in children: a feasibility trial. Cogent Med 2016; 3: 1165083. [Google Scholar]
- 20. Aramideh J, Mizrahi T, Charest M-C, et al. Development and inter-rater reliability of a tool assessing hypnotic communication behaviours adopted by nurses caring for children with cancer: the Sainte-Justine hypnotic communication assessment scale. Complement Ther Med 2018; 37: 178–184. [DOI] [PubMed] [Google Scholar]
- 21. Aramideh J, Ogez D, Mizrahi T, et al. Do professionals change their communication behaviours following a training in hypnosis-derived communication? A feasibility study in pediatric oncology. Complement Ther Med 2020; 52: 102426. [DOI] [PubMed] [Google Scholar]
- 22. Des Jarlais DC, Lyles C, Crepaz N, et al. Improving the reporting quality of nonrandomized evaluations of behavioral and public health interventions: the TREND statement. Am J Public Health 2004; 94(3): 361–366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Crandall M, Lammers C, Senders C, et al. Initial validation of a numeric zero to ten scale to measure children’s state anxiety. Anesth Analg 2007; 105(5): 1250–1253. [DOI] [PubMed] [Google Scholar]
- 24. Babl FE, Mandrawa C, O’Sullivan R, et al. Procedural pain and distress in young children as perceived by medical and nursing staff. Paediatr Anaesth 2008; 18(5): 412–419. [DOI] [PubMed] [Google Scholar]
- 25. Ortiz MI, Lopez-Zarco M, Arreola-Bautista EJ. Procedural pain and anxiety in paediatric patients in a Mexican emergency department. J Adv Nurs 2012; 68(12): 2700–2709. [DOI] [PubMed] [Google Scholar]
- 26. Dufresne A, Dugas MA, Samson Y, et al. Do children undergoing cancer procedures under pharmacological sedation still report pain and anxiety? A preliminary study. Pain Med 2010; 11(2): 215–223. [DOI] [PubMed] [Google Scholar]
- 27. Willis MH, Merkel SI, Voepel-Lewis T, et al. FLACC behavioral pain assessment scale: a comparison with the child’s self-report. Pediatr Nurs 2003; 29(3): 195–198. [PubMed] [Google Scholar]
- 28. Nilsson S, Finnstrom B, Kokinsky E. The FLACC behavioral scale for procedural pain assessment in children aged 5-16 years. Paediatr Anaesth 2008; 18(8): 767–774. [DOI] [PubMed] [Google Scholar]
- 29. Blount RL, Loiselle KA. Behavioural assessment of pediatric pain. Pain Res Manag 2009; 14(1): 47–52. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Cicchetti DV. Guidelines, criteria, and rules of thumb for evaluating normed and standardized assessment instruments in psychology. Psychol Asses 1994; 6: 284–290. [Google Scholar]
- 31. Po’ C, Benini F, Sainati L, et al. The management of procedural pain at the Italian centers of pediatric hematology-oncology: state-of-the-art and future directions. Support Care Cancer 2012; 20(10): 2407–2414. [DOI] [PubMed] [Google Scholar]
- 32. Snowdon DA, Leggat SG, Taylor NF. Does clinical supervision of healthcare professionals improve effectiveness of care and patient experience? A systematic review. BMC Health Serv Res 2017; 17: 786. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33. Czajkowski SM, Powell LH, Adler N, et al. From ideas to efficacy: the ORBIT model for developing behavioral treatments for chronic diseases. Health Psychol 2015; 34(10): 971–982. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, Figure_S1 for Does practising hypnosis-derived communication techniques by oncology nurses translate into reduced pain and distress in their patients? An exploratory study by David Ogez, Jennifer Aramideh, Terry Mizrahi, Marie-Claude Charest, Caroline Plante, Michel Duval and Serge Sultan in British Journal of Pain