Abstract
Mucormycosis, is an invasive infection caused by fungi. Mainly it affects patients with immunosuppressive conditions but can occur in immuncompetent host in specific situation such us direct skin inoculation by traumatic injury. We present a 56-year-old patient who hospitalized due to left orbital cellulitis and necrotizing fasciitis post traumatic injury. A diagnosis of invasive mucormycosis was established by tissue histopathology and culture. Despite daily surgical debridement and amphotericin B, the infection disseminated to central nervous system led to fatal outcome. We conclude that mucormycosis can disseminate in immunocompetent population and leads to death.
Keywords: Mucormycosis, Invasive, Immunocompetent, Trauma
Introduction
Mucurmycosis commonly seen with blunt trauma like in motor vehicle accidents [1]. The average time from first symptoms to diagnosis is two weeks, and mortality rates range from 22 % in the cutaneous to 79 % in the disseminated form [2]. It is an invasive and rapidly progressing fungal infection caused by Mucorales organisms of the Zygomycota family. The ubiquitous filamentous fungi (molds) are usually found in soil, decaying plants and on animals. More than 200 species belong to the Mucorales order, like Sporodiniella, Syzygites, and Rhizopus of the Rhizopodaceae family [3,4]. Usually, it affects immunocompromised patients but may rarely occur in immunocompetent hosts especially with traumatic injury. We present a fatal case of muormycosis in immunocompetent patient post traumatic injury.
Case presentation
A-56 year old female presented after 10 days history of fall in a stagnant water with sustained left eye traumatic injury. On first day of hospitalization, the patient was alert and oriented but could open or move her left eye. Her symptoms were associated with headache and loss of sensation of left facial side.
Pertinent positive on physical examination; left eye ptosis and proptosis, loss of light perception on left eye, total left ophthalmoplegia with moderate conjunctival chemosis with blackish crust on the conjunctiva (Fig. 1).
Fig. 1.
Left eye ecchymosis and swelling on first day of hospitalization.
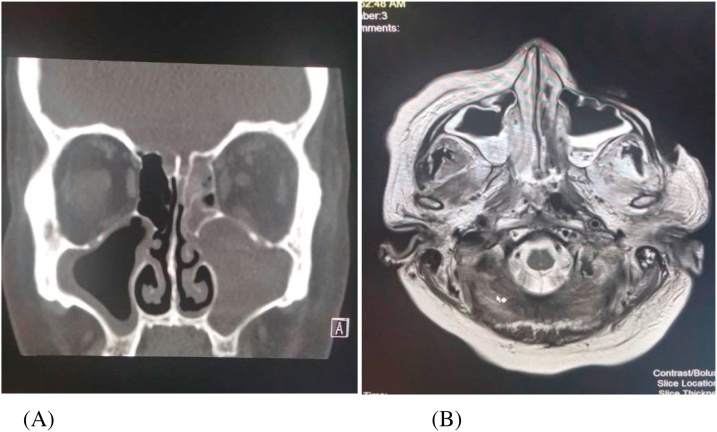
Total leucocyte count on the day of presentation was 33,500/mm3, differential leucocytes count was 21.775 109 Neutrophils, serum creatinine level was 59.8 umol/L. Arterial blood gas analysis showed metabolic acidosis with pH of 7.22. CT of the head showed signs of left facialsinusitis with left preiorbital/preseptal inflammatory changes with proptosis (Fig. 2A). MRI of the head showed pan-sinusitis and inflammatory changes of the adjacent left infra-temporal fossa and left masticator (Fig. 2B).
Fig. 2.
(A) CT of head showed opacification of left frontal, sphenoid, ethmoid and maxillary sinuses suggestive for sinusitis. (B) MRI of head showed inflammatory changes of left infra-temporal fossa and left masticator along with signs left sinusitis.
Patient underwent to operation room for emergent surgical debridement. Signs of necrotizing fasciitis of left eye globe and surrounded muscles ended by debridement and complete left inoculation. Histopathology of left orbital tissue showed fungal hyphae and signs of angioinvasion (Fig. 3). Broad spectrum intravenous (IV) antibiotics were started along with IV amphotericin B. On post-operative day 2, facial examination revealed extensive necrosis of left facial tissues with blackish discoloration (Fig. 4). Patient underwent for second surgical debridement then scheduled for daily surgical debridement. Unfortunately on day 5, patient developed hypotension and right hemiparesis then rapidly progressed to complete loss of brainstem reflexes. At that time, family decided end-of-life care and patient passed away. Lately, left orbital tissue culture was positive for Mucor spp. (Fig. 5).
Fig. 3.
Histopathology of multiple fungal hyphae with angioinvasion.
Fig. 4.
Left facial necrotic tissues with blackish discoloration.
Fig. 5.
Mucor spp. grew from orbital tissue culture.
Discussion
Mucormycosis, is most commonly caused by species of Rhizpus, Absidia, and Rhizomucor. Mostly present with patients who has predisposing factor that reduce their immunity and make them more susceptible to the infection, as well as there’re cases have been reported in immunocompetent individuals. Most common predisposing factors that have been associated with mucormycosis include hematological malignancy, diabetes mellitus, corticosteroid therapy, trauma [5]. In our case the patient was immunocompetent present to hospital with eye trauma invaded by fungal infection known as mucor. The mucorales fungi invade the blood vessels of the soft tissue and obstruct the blood flow to the wound. This process cause necrotic tissues of the wound. Mucor occurs due to inoculation of spores into damaged area with contaminated material at a time of trauma. The pathogenesis of Mucorales followed trauma was explained by number of spores that present in soil contaminated wounds and lead to infection [6]. Our case is one of the rare cases reported in literature due to post traumatic mucormycosis in healthy patient while invasion of subcutaneous tissues, muscles, and fascias. The clinical manifestations of mucormycosis are variable, ranging from mild to severe fatal infection. The classical features of mucor infection are angioinvasion, necrosis, infarction and thrombosis [7]. The definitive method for diagnosis by wound culture or biopsy. The treatment depend on early detection, surgical debridement of infected tissue and start appropriate anti- fungal therapy [8]. In our patient diagnosed by histopathological examination and culture, started on antifungal agent amphotericin B and aggressive surgical debridement. Mortality rate is more than 50 % and to 100 % in disseminated form. The rates of morbidity and mortality related to rapidly vascular invasions, tissue necrosis and infarction [9]. Nonsurvivors usually had rapidly progressive infection, whereas survivors had minor disease [10]. In our patient the disseminated of the severe infection (Mucor spp.) lead to fatal outcome. Despite systemic antifungal therapy (Amphotracin B) and aggressive surgical debridement.
In conclusion, post-traumatic mucormycosis remains a rare condition especially in healthy patient. The highly suspicious index of clinical diagnosis of any trauma patient should be made earlier and start a combination of anti-fungal therapy and surgical intervention may be lifesaving that lower the mortality, but it can be fatal as in our patient despite of started on appropriate treatment the outcome end by death.
Consent
Informed consent obtained.
Funding
None.
Author contributions
LA and FA contributed to conception and design of the study, acquisition and analysis of data, and drafting a significant portion of the manuscript. ST, NR, and WE contributed to conception and design of the study, and acquisition and analysis of data. MS contributed to conception and design of the study, acquisition and analysis of data, and drafting a significant portion of the manuscript.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgement
None.
References
- 1.Ingram P.R., Suthananthan A.E., Rajan R., Pryce T.M., Sieunarine K., Gardam D.J. Cutaneous mucormycosis and motor vehicle accidents: findings from an Australian case series. Med Mycol. 2014;52(November (8)):819–825. doi: 10.1093/mmy/myu054. [DOI] [PubMed] [Google Scholar]
- 2.Lanternier F., Dannaoui E., Morizot G., Elie C., Garcia-Hermoso D., Huerre M. A global analysis of mucormycosis in France: the RetroZygo study (2005-2007) Clin Infect Dis. 2012;54(Suppl. 1):S35–S43. doi: 10.1093/cid/cir880. [DOI] [PubMed] [Google Scholar]
- 3.Hoffmann K., Pawlowska J., Walther G., Wrzosek M., de Hoog G.S., Benny G.L. The family structure of the Mucorales: a synoptic revision based on comprehensive multigene-genealogies. Persoonia. 2013;30:57–76. doi: 10.3767/003158513X666259. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Katragkou A., Walsh T.J., Roilides E. Why is mucormycosis more difficult to cure than more common mycoses? Clin Microbiol Infect. 2014;20(Suppl. 6):74–81. doi: 10.1111/1469-0691.12466. [DOI] [PubMed] [Google Scholar]
- 5.Geller J.D., Peters M.S., Su W.P. Cutaneous mucormycosis resembling superficial granulomnatous pyoderma in an immunocompetent host. J Am Acad Dermatol. 1993;29:462–465. doi: 10.1016/0190-9622(93)70211-b. [DOI] [PubMed] [Google Scholar]
- 6.Marchevsky A.M., Bottone E.J., Geller S.A., Giger D.K. The changing spectrum of disease, etiology, and diagnosis of mucormycosis. Hum Pathol. 1980;11(5):457–464. doi: 10.1016/s0046-8177(80)80054-2. [DOI] [PubMed] [Google Scholar]
- 7.Kline M.W. Mucormycosis inchildren: review of the literature and report of cases. Pediat Infect Dis. 1985;4:672–676. doi: 10.1097/00006454-198511000-00015. [DOI] [PubMed] [Google Scholar]
- 8.Meyer R.D., Armstrong D. Mucormycosis-changing states. CRC Crit Rev Clin Lab Sci. 1973;4:421. doi: 10.3109/10408367309151561. [DOI] [PubMed] [Google Scholar]
- 9.Adam R.D., Hunter G., DiTomasso J., Comerci G. Mucormycosis: emerging prominence of cutaneous infection. Clin Infect Dis. 1994;19:67–76. doi: 10.1093/clinids/19.1.67. [DOI] [PubMed] [Google Scholar]
- 10.Everett E.D., Pearson S., Rogers W. Rhizopus surgical wound infectio associated with elasticized adhesive tape dressings. Arch Surg. 1979;114:738–739. doi: 10.1001/archsurg.1979.01370300092019. [DOI] [PubMed] [Google Scholar]