Abstract
Objective
The coronavirus disease 2019 (COVID-19) has impacted the Kingdom of Saudi Arabia (KSA) as it has other nations. However, length of stay (LOS), as a healthcare quality indicator, has not been examined across the healthcare regions in the KSA. Therefore, this study aimed to examine factors associated with LOS to better understand the Saudi Health System's performance in response to the COVID-19 pandemic in the newly suggested five Saudi regional business units (BUs).
Methods
A retrospective study was conducted using Ministry of Health (MOH) data on hospital LOS during the period from March to mid-July 2020. Participants were adult inpatients (18 years or older) with confirmed COVID-19 (n = 1743 patients). The 13 regions of the KSA were united into the defined five regional BUs during the reorganization of the health system. Covariates included demographics such as age and sex, comorbidities, and complications of COVID-19. A multiple linear regression with stepwise forward selection was used to model LOS for other explanatory variables associated with LOS, including demographic, comorbidities, and complications.
Results
The mean LOS was 11.85 days which differed significantly across the BUs, ranging from 9.3 days to 13.3 days (p value < 0.001). BUs differed significantly in LOS for transferred patients but not for patients in the intensive care unit (ICU) or those who died in-hospital. The multiple regression analysis revealed that the LOS for inpatients admitted in the Eastern and Southern BUs was significantly shorter than for those in the Central BU. (p value < 0.001). Admission to the ICU was associated with lengthier stays (p value < 0.0001). Factors significantly associated with shorter stays (compared to the reference), were being Saudi, death during admission, and patients referred to another hospital (p value < 0.05).
Conclusion
The LOS for patients with COVID-19 differed across the proposed regional healthcare BUs, suggesting regional differences in quality of care under the reorganization of the national health system. Since patient and disease characteristics did not explain these findings, differences in staffing and other resources need to be examined to develop interventions.
Keywords: COVID-19, Hospital admission, Occupational and environmental health, Length of stay, Saudi Arabia, Vision 2030
Abbreviations: KSA, Kingdom of Saudi Arabia; LOS, Length of stay; CI, Confidence interval; OR, Odds Ratio; ICU, Intensive care unit; MOC, Model of care; ARDS, Acute Respiratory Distress Syndrome; MOH, Ministry of Health; GIT, Gastrointestinal tract; COVID-19, Coronavirus disease 2019
1. Introduction
Similar to other nations, the coronavirus disease 2019 (COVID-19) caused by the severe acute respiratory syndrome coronavirus 2, has affected the Kingdom of Saudi Arabia (KSA) (Liu et al., 2020, Singhal, 2020). Demand for hospital care is high as many patients with COVID-19 develop a severe form that can cause acute respiratory distress syndrome (ARDS) and respiratory failure, which carries a 20% mortality rate (Gibson et al., 2020, Abate et al., 2020). As of mid-July 2020, worldwide statistics indicated 13,150,645 total cases and 574,464 deaths, while the KSA had 237,803 total confirmed cases and 2,283 deaths related to COVID-19 (Medicine, 2020). However, as the projected need for hospital care for patients with COVID-19 within the KSA is largely unknown, the length of stay (LOS) for inpatients with confirmed COVID-19 is one of the most critical factors in preparing for the demand for hospital care as the pandemic continues (Medicine, 2020, Rosenbaum, 2020, Rodriguez-Morales, 2020). This study occurred during the initial wave of the pandemic in the KSA when the world was not yet prepared to cope with it’s demands. It will be very useful to plan for successive waves in the allocation of resources to different regions since the regions experienced the peak at different times.
The best health care provision for COVID-19 patients requires an abundance of resources including medical and paramedical staff and non-human resources such as sufficient hospital beds, oxygen support, and technology (Guo et al., 2021). The pandemic created demands and inflicted enormous financial costs on all aspects of healthcare systems worldwide to the point of such costly overburdening that many systems were forced into collapse even in advanced countries such as Italy (Rosenbaum, 2020). LOS in hospitals represented such a large portion of costs, for example with average costs per diem in the USA of 73.300 USD and in China of 17,000 yuan, that this is especially worrying for developing countries with fewer resources to meet such a sudden crisis demand (Guo et al., 2021). Understanding LOS and its consequences on the healthcare system from region to region in the KSA will help delineate the best standards for the medical profession to focus on care of those most likely to require longer LOS to improve health outcomes and shorten LOS reducing the financial burden. The example of Italy and other countries (Rosenbaum, 2020, Rodriguez-Morales, 2020, Rees et al., 2020) served as a wake-up call to the KSA to take early swift action prior to the first case identified in the KSA to prevent the spread of COVID-19, thereby avoiding the collapse of the Saudi hospital system (Komies, et al., 2020). As it has been established that there is significant variation in the quality of care provided to COVID-19 inpatients among regions in the KSA (Alharbi et al., 2021), we focused on LOS as one of the indicators that may measure utilization and provision of services among the 5 regions as proposed by the new Model of Care(MOC) under vision 2030. LOS is also critical for planning purposes for both the COVID-19 and future pandemics considering all factors that influence it, including comorbidities, complications, gender, age, region of residence, and other demographics (Rosenbaum, 2020, Rodriguez-Morales, 2020, Rees et al., 2020, Massonnaud et al., 2020, Castro, 2020, Chen et al., 2020, Wu and McGoogan, 2020).
Several studies have demonstrated the importance of LOS for resource allocation planning in general hospital and ICU settings as well as an indicator of quality. A 2018 large cohort study on LOS in the Emergency Departments among the elderly in the Netherlands found that these patients experienced longer LOS in the emergency department and had a lower quality of care with an increasing demand on limited resources (Sir, 2019). A review of studies on patients with COVID-19 concluded that LOS in general hospitals varied considerably from less than a week to 2 months (Rosenbaum, 2020). An early study conducted in the UK noted a range of 12–19 days in general hospitals among patients with COVID-19 who were not in an ICU (Vekaria, et al., 2020).
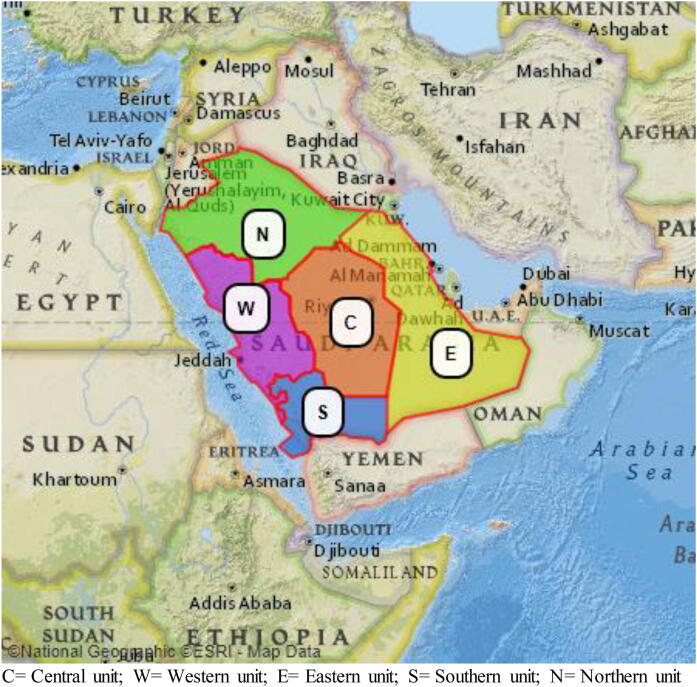
The health care system in the KSA is in the process of being transformed into a 21st century world-class health service governed by the Saudi Vision 2030 (Al-Hanawi et al., 2018, Hazazi and Chandramohan, 2017). Vision 2030 calls for health care reforms to ensure that all citizens have access to high-quality healthcare, that primary care becomes the main engine of the system, and that competition and accountability will render a more efficient system. The reforms contained in this plan include reorganizing the existing 13 administrative regions into five busness units (Fig. 1 and Fig. 2). These are the Central, Northern, Southern, Eastern, and Western, each with its own private holding company charged with administering the healthcare for that region (Health, M.o., VRO Health Sector Transformation Strategy., 2019).
Fig. 1.
The five proposed business units in the KSA. C = Central unit; W = Western unit; E = Eastern unit; S = Southern unit; N = Northern unit.
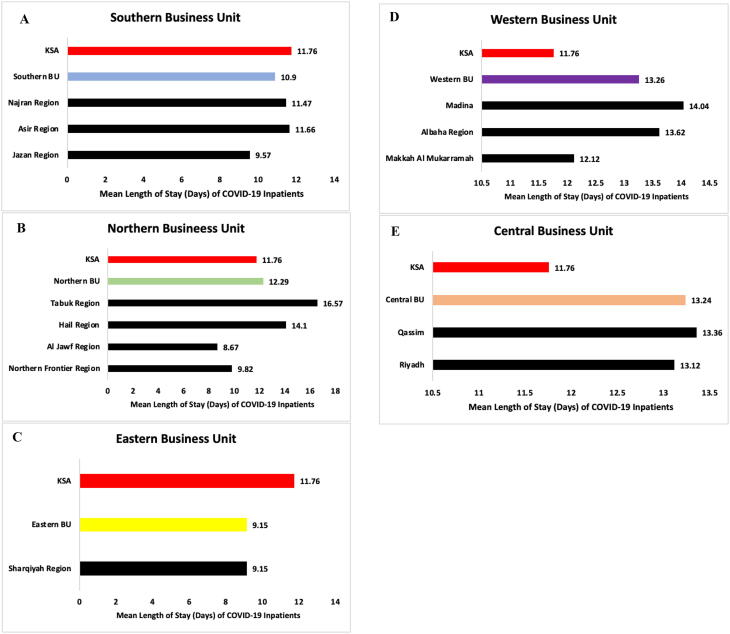
Fig. 2.
Rates of length of stay in the current 13 administrative region model and prospective five administrative unit model of the Kingdom of Saudi Arabia.
The MOH is gradually implementing the system's transition to privatization to comply with Vision 2030 by creating a Vision Realization Office (Health, 2019, Almalki et al., 2011). For this purpose, the National Insurance Center was recently created to assume the responsibility for the financial administration of the entire healthcare system (Health, M.o., VRO Health Sector Transformation Strategy., 2019). Our study has interpreted the data gathered from the existing model of 13 regions to fit the future model of five BUs (Fig. 2). The five BUs in the new MOC are composed of regions as follows: Asir, Jazan, and Najran in the Southern BU (SBU); Al Jawf, Hail, Northern Frontier, and Tabuk in the Northern BU (NBU); Riyadh and Al Qassim in the Central BU (CBU); Makkah, Medina, & Al Baha in the Western BU (WBU), and Sharqiyah in the Eastern BU (EBU).
In the KSA, there are no published reports on the variations in the LOS among inpatients with COVID-19. The main objective of this study was to assess the LOS of inpatients with COVID-19 and its associated factors among the current 13 administrative regions to project the likely healthcare quality for the KSA’s health system once it is reorganized into five BUs. We hypothesized that the LOS for inpatients with COVID-19 would reveal variations among the five proposed BUs under the new model of care (MOC) created by Vision 2030. By assessing LOS among the five BUs as an indicator of the quality of care and demand for hospital care, our study’s findings will assist policymakers in planning for resource allocation and improving the quality of care among the five BUs.
2. Methodology
2.1. Data source, design, and participants
The MOH collected the data from the hospitals assigned to treat inpatients with COVID-19. We restricted our study to those patients with moderate to severe disease as defined by the MOH protocols. This was a cross-sectional retrospective study conducted using data collected by the MOH on hospital LOS for inpatients with confirmed COVID-19 for the period from March 2020 to mid-July 2020. Our study included all adult inpatients with COVID-19 reported to the MOH by hospitals in all 13 regions with a sample size of 1743 adult inpatients (aged 18 years and above) from 30 hospitals in the 13 administrative regions. We targeted only adults in our sample since data on people aged below 18 years is lacking due to fewer hospitalizations of this age group (Alharbi et al., 2021).
2.2. Measurements
Our primary outcome was the LOS, a continuous variable reported as the number of days from admission to either discharge to home, referral to another hospital, or in-hospital death. The primary independent variable of interest was the BU in which the admitting hospital was located, a categorical variable defined as 0 = Central (CBU), 1 = Eastern (EBU), 2 = Western (WBU), 3 = Northern (NBU), and 4 = Southern (SBU) as shown in Fig. 1. Covariates included demographics such as age and gender, comorbidities, and complications of COVID-19. Use of the Central BU as the reference is the most reasonable as it contains Riyadh where the most advanced medical centers are located with more resources so that we can compare other regions to the most advanced (Alharbi et al., 2021).
2.3. Statistical analysis
Using simple descriptive statistics, the BUs were compared in terms of patient characteristics. The BU differences in the LOS of inpatients were assessed using linear regression modeling. Our statistical models assumed that the dependent variable followed a normal distribution and, hence, it was necessary to use the natural log transformation for the LOS. We used multiple linear regression with stepwise forward selection to model LOS for other explanatory variables associated with LOS, including demographic, comorbidities, and complications. Statistical significance was set at p ≤ 0.05 and all statistical analyses were conducted using STATA version 14 (StataCorp, College Station, Texas 77,845 USA). Sensitivity analysis was conducted to assess the robustness of our findings' and we ran five models on selected subsets of our sample. The first model included all the patients who died in the hospital, those admitted to ICU, those transferred to another hospital, or those discharged to home. The second model excluded the patients who were admitted to ICU. The third model excluded patients who died in the hospital during the admission. The fourth model excluded both patients who died in the hospital during the admission or were admitted to ICU. The fifth model excluded transferred cases.
2.4. Ethical considerations
Study participants had signed informed consent forms for the secondary data used for this study, and the privacy and anonymity of study participants were preserved. The Central Institutional Review Board of the MOH approved this study's ethics, with the reference number 20-163E.
3. Results
Table 1 illustrates the demographic characteristics of our sample participants by BU. The highest proportion of patients with COVID-19 were from the WBU and EBU, with the lowest portion from the NBU. Participants were almost equally likely to be Saudi or Non-Saudi with a mean age of 50. Approximately three-quarters of our participants were male..
Table 1.
Demographic characteristics of the study population (N = 1743).
| Units | Age* (years), Mean (SD) | Sex | Nationality | Patients with COVID-19 N (%) |
||
|---|---|---|---|---|---|---|
| Male N (%) |
Female N (%) |
Saudi N (%) |
Non-Saudi N (%) |
|||
| Central | 49 (13.26) | 260 (85) | 47 (15) | 69 (22) | 238 (78) | 307 (18) |
| Northern | 55 (16.08) | 74 (81) | 17 (19) | 46 (51) | 45 (49) | 91 (5) |
| Eastern | 45 (16.28) | 302 (60) | 200 (40) | 361 (72) | 141 (28) | 502 (29) |
| Western | 53 (15.97) | 465 (71) | 190 (29) | 244 (37) | 411 (63) | 655 (37) |
| Southern | 49 (14.44) | 138 (73) | 50 (27) | 109 (58) | 79 (42) | 188 (11) |
| All regions | 50 (0.38) | 1239(71) | 538 (29) | 829 (48) | 914 (52) | 1743 (100) |
Abbreviations: SD = Standard Deviation.
Footnote: * p value < 0.05 based on the one-way-ANOVA test.
Table 2 illustrates the clinical characteristics of the patients with COVID-19 according to the proposed five BUs. Inpatient mortality rates in the WBU (51%) and NBU (53%) were approximately double those in the CBU (25%). In contrast, mortality rates in the EBU were less than one-third the rate of the WBU (8%) and the SBU were less than half the rate (14%). Similarly, compared to the CBU, the ICU admission rates for the Western and Northern BUs were significantly higher, at 71% and 88% respectively, and were markedly lower in the Eastern and Southern BUs Regarding rates of inpatients transferred to another hospital, compared to the CBU, the Western, Northern, and Southern BUs had relatively lower rates while the EBU had a statistically significant higher rate (p < 0.0001). On admission, diabetes (42%) and hypertension (32%) were the two most frequent comorbidities, while immunocompromised and cancer each represented<5%. Participants with pre-existing ARDS accounted for 12% while participants with obesity and cardiac disease were relatively equally distributed at 14% and 13%, respectively. The most frequent complications from COVID-19 were bacterial pneumonia (39%), sepsis (21%), and ARDS (8%). Multi-organ failure and acute kidney injury were significant complications, while arrhythmia, hepatotoxicity, and GIT perforation were less common complications (p value < 0.0001).
Table 2.
Clinical characteristics of the patients with COVID-19 according to the proposed five regional units.
| Characteristics | Total N (%) |
Central N (%) |
Northern N (%) |
Eastern N (%) |
Western N (%) |
Southern N (%) |
p value* |
|---|---|---|---|---|---|---|---|
| Pre-Coexisting Conditions | |||||||
| Diabetes mellitus | 734 (42) | 158 (51) | 49 (54) | 132 (26) | 310 (47) | 85 (45) | <0.001 |
| Hypertension | 566 (32) | 91 (30) | 38 (42) | 128 (25) | 255 (39) | 54 (29) | <0.001 |
| Obesity | 252 (14) | 51 (17) | 7 (8) | 18 (4) | 152 (23) | 24 (13) | <0.001 |
| Heart Diseases | 230 (13) | 30 (10) | 13 (14) | 39 (8) | 129 (20) | 19 (10) | <0.001 |
| ARDS at admission | 212 (12) | 58 (19) | 19 (21) | 11 (2) | 108 (16) | 16 (9) | <0.001 |
| Incompetent immunity | 70 (4) | 9 (3) | 11 (12) | 8 (2) | 38 (6) | 4 (2) | <0.001 |
| History of cancer | 43 (2.5) | 8 (3) | 2 (2) | 7 (1) | 26 (4) | 0 (0) | <0.001 |
| Complications | |||||||
| ICU Admission | 862 (49.5) | 180 (59) | 80 (88) | 62 (12) | 464 (71) | 76 (40) | <0.001 |
| Patient Transferred to another hospital | 434 (25) | 71 (23) | 105 (16) | 223 (44) | 11 (12) | 24 (13) | <0.001 |
| Bacterial Pneumonia | 680 (39) | 155 (50) | 42 (46) | 79 (16) | 312 (48) | 92 (49) | <0.001 |
| ARDS | 534 (31) | 102 (33) | 30 (33) | 38 (8) | 323 (49) | 41 (22) | <0.001 |
| Sepsis | 367 (21) | 70 (23) | 20 (22) | 52 (10) | 2009 (31) | 25 (13) | <0.001 |
| Acute kidney injury | 248 (14) | 38 (12) | 6 (7) | 5 (1) | 177 (27) | 22 (12) | <0.001 |
| Multi-organ failure | 179 (10) | 24 (8) | 8 (9) | 2 (0.5) | 130 (20) | 14 (7) | <0.001 |
| Arrythmia | 131 (8) | 38 (12) | 11 (12) | 2 (0.5) | 74 (11) | 6 (3) | <0.001 |
| Liver toxicity | 41 (2) | 4 (1) | 4 (4) | 0 (0) | 26 (4) | 6 (3) | <0.001 |
| GIT perforation | 34 (2) | 0 (0) | 0 (0) | 0 (0) | 32 (5) | 0 (0) | <0.001 |
| Death during admission: | 525 (30) | 76 (25) | 48 (53) | 39 (8) | 335 (51) | 27 (14) | <0.001 |
Abbreviations: ICU = intensive-care unit; ARDS = acute respiratory distress syndrome; GIT = gastrointestinal tract.
Footnote: * p value based on the Chi-square test.
Pre-existing chronic disease and the occurrence of complications from COVID-19 showed statistically significant regional differences (p value < 0.0001 for all). Significantly higher combined rates of chronic diseases were reported in the Northern and Western BUs compared with the CBU, accompanied by higher mean ages. Conversely, there were significantly lower combined rates of chronic diseases in the Southern and Eastern BUs. Regarding complications from COVID-19, the WBU had a significantly higher sepsis occurrence than other BUs, ARDS, acute kidney injury, hepatotoxicity, GIT perforation, and multi-organ failure. All BUs had a significantly higher occurrence of bacterial pneumonia (39–50%) except the EBU (16%) which was significantly lower. The Eastern and Southern BUs (10 and 13%) had a significantly lower ARDS incidence, while the WBU (49%) was the highest. The Northern and the Central BUs were equal (33%).
Table 3 illustrates the results of the LOS of four subsets of the sample in all the BUs. The mean range of the LOS in all the BUs for the four subsets was 10–14 days distributed as follows: ICU, 14; total sample 11.9; in-hospital deaths, 11.6; and transferred, 10.0. A one-way-ANOVA applied to the total sample suggested that there were statistically significant variations between BUs (p value < 0.0001), in which the Central and Western BUs were the highest, the Eastern and Southern had significantly lower LOSs. When the one-way-ANOVA was applied to the transferred patients it showed statistically significant variations between BUs (p value < 0.0001), in which the Central, Western, and Southern BUs had the highest LOS, and the Eastern had the lowest. There were no significant statistical variations in the LOS between BUs for ICU admissions or patients who died in hospital (p value > 0.05 for both).
Table 3.
Mean of LOS for Inpatient Categories among the five regional units in the Kingdom of Saudi Arabia.
| Mean LOS | All units | Central | Western | Eastern | Northern | Southern | p-value* |
|---|---|---|---|---|---|---|---|
| Total sample | 11.9 | 13.2 | 13.3 | 9.3 | 12.6 | 10.9 | <0.0001 |
| Transferred patients | 10.0 | 12.8 | 12.3 | 7.9 | 9.5 | 12.0 | <0.0001 |
| ICU admissions | 14.0 | 15.2 | 13.8 | 12.5 | 13.2 | 14.7 | 0.1981 |
| In-hospital deaths | 11.6 | 12.2 | 11.9 | 9.4 | 9.6 | 13.3 | 0.0995 |
Abbreviations, LOS = length of stay, ICU = intensive-care unit.
Footnote: Data are presented as means; * p value is based on the one-way-ANOVA test.
Results from the Multiple linear regression analysis of the factors associated with the length of stay are presented in Table 4. Compared to the inpatients admitted in the CBU and controlling for chronic diseases and complications, the estimated average LOS for inpatients admitted in the Eastern and Southern BUs were significantly shorter by 28% and 25 % days respectively (p value < 0.001). The NBU had relatively shorter LOS, while the WBU was associated with lengthier stays compared with the CBU, but without statistical significance (p value > 0.05 for both). Other variables having a significant association with longer LOS (compared to reference) were admission to ICU (50% longer LOS; p value < 0.0001) and age with a 4% longer LOS each year of increase in age (p value = 0.006). Other factors significantly associated with shorter LOSs (compared to the reference) were death during admission (61% shorter LOS), patients referred to other hospitals (24% shorter LOS), admitted with ARDS (13% shorter LOS), and being Saudi (9% shorter LOS).
Table 4.
Multiple linear regression analysis of the factors associated with the length of stay.
| Characteristics | p-value | Coefficients | 95% CI |
|
|---|---|---|---|---|
| Lower | Upper | |||
| Regions (Central unit = REF) | ||||
| Western | 0.725 | 0.02 | −0.08 | 0.12 |
| Eastern | <0.0001 | −0.28 | −0.4 | −0.17 |
| Northern | 0.329 | −0.09 | −0.26 | 0.09 |
| Southern | <0.0001 | −0.25 | −0.39 | −0.12 |
| Demographic and Hospital Factors | ||||
| Age (years) | 0.006 | 0.004 | 0.001 | 0.006 |
| Female (Male = REF) | 0.537 | 0.03 | −0.05 | 0.10 |
| Saudi (Non-Saudi = REF) | 0.028 | −0.09 | −0.17 | −0.01 |
| Admitted with ARDS | 0.026 | −0.13 | −0.25 | −0.02 |
| Admitted to ICU | <0.0001 | 0.49 | 0.39 | 0.59 |
| Died during admission | <0.0001 | −0.61 | −0.74 | −0.49 |
| Patient referred to other hospital | <0.0001 | −0.24 | −0.33 | −0.16 |
| Comorbidities | ||||
| Diabetes | 0.404 | −0.03 | −0.11 | 0.05 |
| Obesity | 0.620 | −0.03 | −0.12 | 0.07 |
| Hypertension | 0.176 | 0.06 | −0.03 | 0.15 |
| Pulmonary diseases | 0.189 | 0.08 | −0.04 | 0.19 |
| Cardiac Diseases | 0.414 | −0.05 | −0.16 | 0.06 |
| History of cancer | 0.750 | 0.04 | −0.19 | 0.27 |
| Immunocompromised | 0.914 | 0.01 | −0.17 | 0.19 |
| Complications | ||||
| Bacterial Pneumonia | 0.054 | 0.08 | −0.002 | 0.16 |
| Sepsis | 0.426 | 0.05 | −0.07 | 0.16 |
| Arrythmia | 0.296 | −0.07 | −0.21 | 0.07 |
| ARDS | 0.396 | 0.05 | −0.07 | 0.17 |
Abbreviations: ICU = intensive-care unit; CI = confidence interval; ARDS = acute respiratory distress syndrome; REF = reference category.
Table 5, shows the results of a sensitivity analysis to perform an in-depth investigation into the differentials in LOS in the proposed five regional BUs. When modeling patient subsets, the results were similar in all models in which we compared the CBU to the other BUs. The Eastern and Southern BUs had significantly shorter LOSs than the CBU (p value < 0.05 for all of the models). Because the results are similar, we can conclude that the patient subsets are unlikely to bias the results obtained from using the entire sample.
Table 5.
Sensitivity analysis models predicting the length of stay in the five units.
| Characteristics | p-value | Coefficient | 95% CI |
|
|---|---|---|---|---|
| Lower | Upper | |||
| Model 1- Univariate analysis (N = 1743) | ||||
| Regions (Central = REF) | ||||
| Western | 0.397 | −0.04 | −0.14 | 0.05 |
| Eastern | <0.0001 | −0.52 | −0.62 | −0.41 |
| Northern | 0.332 | −0.08 | −0.26 | 0.08 |
| Southern | <0.0001 | −0.28 | −0.41 | −0.14 |
| Model 2 (Patients admitted to the ICU were excluded) (N = 881) | ||||
| Regions (Central = REF) | ||||
| Western | 0.077 | 0.15 | −0.02 | 0.33 |
| Eastern | 0.005 | −0.23 | −0.4 | −0.07 |
| Northern | 0.312 | −0.24 | −0.71 | 0.22 |
| Southern | 0.013 | −0.25 | −0.45 | −0.05 |
| Model 3 (Excluded patients who died during admission) (N = 1218) | ||||
| Regions (Central = REF) | ||||
| Western | 0.081 | 0.1 | −0.01 | 0.23 |
| Eastern | <0.0001 | −0.24 | −0.36 | −0.11 |
| Northern | 0.89 | −0.02 | −0.25 | 0.21 |
| Southern | <0.0001 | −0.27 | −0.42 | −0.12 |
| Model 4 (Excluded patients who died or were admitted to the ICU) (N = 865) | ||||
| Regions (Central = REF) | ||||
| West | 0.027 | 0.2 | 0.02 | 0.38 |
| East | 0.023 | −0.2 | −0.36 | −0.27 |
| Northern | 0.313 | −0.24 | −0.72 | 0.22 |
| Southern | 0.033 | −0.22 | −0.42 | −0.02 |
| Model 5 (Excluded patients who were transferred to other hospitals) (N = 1309) | ||||
| Regions (Central = REF) | ||||
| West | 0.332 | 0.05 | −0.05 | 0.16 |
| East | 0.001 | −0.22 | −0.36 | −0.09 |
| Northern | 0.617 | −0.04 | −0.22 | 0.13 |
| Southern | <0.0001 | −0.25 | −0.4 | −0.11 |
Abbreviations: ICU = intensive-care unit; CI = confidence interval; REF = reference category.
4. Discussion
This study examined the variations in the LOS of inpatients with confirmed COVID-19 to assess the demand for healthcare and healthcare quality between the five BUs. We included the analyses of three categories of patient characteristics in our study, demographics, comorbidities, and complications from COVID-19, to consider the factors that might be associated with LOS. The mean LOS for inpatients with COVID-19 in the KSA was almost 12 days. Our resultant mean LOS of 12 fell between that found in an extensive systematic review in which the mean LOS in China was 14 days and outside China was 5 days for inpatients in general hospitals (Rees et al., 2020). The mean LOS for inpatients in the ICU in our study was 14 days; however, in a previous review, the LOS ranged from 5 to 19 days (Rosenbaum, 2020). The difference in protocols for hospitalization and discharges and the extent of the pandemic between countries may account for such a wide range in the LOS of both for general hospital patients and ICU patients.
We adjusted for known patient and disease severity characteristics that may have affected the length of stay among patients with COVID-19. After adjustment, compared to the CBU the Eastern and Southern BUs had significantly lower LOSs; although the NBU had a relatively lower LOS, it was statistically insignificant. Compared to the CBU, the WBU had a relatively higher, but statistically insignificant LOS. Our observation of a difference in LOS between BUs after the adjustments supports our hypothesis that there are variations in terms of quality in the provision of health services that are driven by factors other than patient demographic and clinical characteristics. Our findings of differences in the quality of care among the BUs is consistent with a study of ICU admissions among COVID-19 inpatients in the KSA which found variations in quality among the BUs (Alharbi et al., 2021).
These findings may be explained by hospital practices for patients with COVID-19; in terms of the relationship with region and LOS, using subsets of patients. Consider, for example, transferred patients. We observed that the EBU transferred patients to a second hospital at a significantly higher rate than other BUs, which may mean that they transferred patients with severe conditions to tertiary hospitals where more advanced treatment would be available. This disparity may have resulted from the variability of resources between BUs. However, our findings of a difference in LOS persisted when subsets of patients were eliminated.
Several studies worldwide have indicated the relationship between LOS and the quality of health services (Massonnaud et al., 2020, Sir, 2019). To our knowledge, this study is the first to examine LOS as a healthcare quality indicator in the proposed five BUs of the KSA. Since we controlled for comorbidities, complications, and demographics, these do not explain the variations between the BUs. Therefore, we conclude that LOS is the result of the quality of care in each BU. This study shows that the allocation of resources should be reconsidered carefully for all patients to have equal access to quality care, according to Vision 2030.
It has been well documented that utilization alone is not an adequate measure to determine the quality of healthcare and that significant differences between healthcare quality depends on geography (Corallo et al., 2014, Steinwachs and Hughes, 2008, Wunsch, 2008, Zhou et al., 2019, Kwan et al., 2018, Bos et al., 2007); this highlights the importance of this study. The evidence provided by our study regarding the differences in LOS among the future five BUs in the new MOC can guide policymakers in decisions relating to the provision of resources to help ensure equity in quality healthcare as the KSA moves forward with Vision 2030. As the private administration of each of the five BUs is implemented, the MOH will move to a greater supervision of the overall system and will need a rational basis for providing resources and guidance to the administrators to reduce the large variations in the quality of healthcare services shown in Fig. 2.
As there is complexity in determining all the factors associated with LOS and as our results were adjusted for comorbidities and complications, further studies are needed to describe all the human and non-human resources in each BU that may impact the LOS; both the infrastructural and clinical factors are relevant to the LOS. As our research is based on only three and a half months of MOH reporting during a period where variations reached the peak of cases among the 13 regions, we recommend conducting another study that uses data through December 2020. Moreover, our study did not explore the effect of level of care, i.e., insufficient, or excessive care. For example, does the number of staff involved lead to longer or shorter LOS; further study with an in-depth investigation on this may help understand the interplay between these factors.
4.1. Strengths
Our study's data provided many explanatory variables, including extensive demographics, comorbidities, and complications of COVID-19 among inpatients, for which we were able to control. This strengthened the validity of our study. In seeking to understand the variabilities in the LOS among the five proposed BUs, adjustment for these factors was crucial.
4.2. Limitations
This study's primary limitation is that our data represents a period of only three and a half months. During this time, COVID-19 had not yet peaked, and the BUs peaked at different times. Second, there was the lack of information regarding several factors that needed to be controlled, such as available human resources and sophisticated equipment to treat inpatients with COVID-19. This cross-sectional study design could not establish a direct causal relationship between LOS and the five proposed BUs because this design only allowed for an indirect assessment of relationships.
5. Conclusions
Our study on inpatients with COVID-19 in KSA-MOH hospitals found that the overall average LOS in hospitals is approximately 12 days. The study revealed significant differences in LOS between the BUs indicating quality of care disparities from region to region in descending order: Western, Central, Northern, Southern, and Eastern. The differences in the LOS persisted, even after adjustment for patient and disease factors. Therefore, reasons for the lower LOS duration in the EBU and SBU may relate to differences in human and physical infrastructure. These findings are valuable for implementing the new MOC of Vision 2030 in which one goal is to provide high quality, accessible, and equitable healthcare for all citizens.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments
Acknowledgments
We acknowledge the funding assistance provided by King Abdulaziz City for Science and Technology; whose crucial support enabled us to accomplish our research. With gratitude, we acknowledge the Clinical Excellence General Directorate of the Ministry of Health for their efforts in the data. We thank the Central Institutional Review Board and the General Administration for Research and Studies who facilitated our research. Finally, we thank Jazan University and its Science & Technology Unit for their assistance in guiding the team toward the accomplishment with a good follow-up.
Funding
This work was supported by the King Abdulaziz City for Science and Technology. (Reference number: 5-20-01-105-0011).
Authors’ contributions
Study design: Ab A. A, A Y. A, I M. G, Ab A. Aq, A M. M.
Data collection: Ab A. A.
Data analysis: Ab A. A, A Y. A, I M. G, Ab A. Aq, M A. M.
Manuscript writing: Ab A. A, A Y. A, Ah A. A, M A. M, O A. A.
Footnotes
Peer review under responsibility of King Saud University.
References
- Liu Y.-C., Kuo R.-L., Shih S.-R. COVID-19: The first documented coronavirus pandemic in history. Biomed J. 2020;43(4):328–333. doi: 10.1016/j.bj.2020.04.007. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Singhal T. A Review of Coronavirus Disease-2019 (COVID-19) Indian J. Pediatr. 2020;87(4):281–286. doi: 10.1007/s12098-020-03263-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Gibson P.G., Qin L., Puah S.H. COVID-19 acute respiratory distress syndrome (ARDS): clinical features and differences from typical pre-COVID-19 ARDS. Med. J. Aust. 2020;213(2):54–56 e1. doi: 10.5694/mja2.50674. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Abate S.M., Ahmed Ali S., Mantfardo B., Basu B., Lazzeri C. Rate of Intensive Care Unit admission and outcomes among patients with coronavirus: A systematic review and Meta-analysis. PLoS ONE. 2020;15(7):e0235653. doi: 10.1371/journal.pone.0235653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Medicine, J.H.U. COVID-19 Case Tracker. CORONAVIRUS RESOURSE CENTER 2020 March 11, 2021]; Available from: https://coronavirus.jhu.edu/.
- Rosenbaum L. Facing Covid-19 in Italy - Ethics, Logistics, and Therapeutics on the Epidemic's Front Line. N. Engl. J. Med. 2020;382(20):1873–1875. doi: 10.1056/NEJMp2005492. [DOI] [PubMed] [Google Scholar]
- Rodriguez-Morales A.J. Clinical, laboratory and imaging features of COVID-19: A systematic review and meta-analysis. Travel Med. Infect. Dis. 2020;34 doi: 10.1016/j.tmaid.2020.101623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Guo A., Lu J., Tan H., Kuang Z., Luo Y., Yang T., Xu J., Yu J., Wen C., Shen A. Risk factors on admission associated with hospital length of stay in patients with COVID-19: a retrospective cohort study. Sci. Rep. 2021;11(1) doi: 10.1038/s41598-021-86853-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Rees E.M., Nightingale E.S., Jafari Y., Waterlow N.R., Clifford S., B. Pearson C.A., Group CMMID.W., Jombart T., Procter S.R., Knight G.M. COVID-19 length of hospital stay: a systematic review and data synthesis. BMC Med. 2020;18(1) doi: 10.1186/s12916-020-01726-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Komies, S., et al., COVID-19 Outcomes in Saudi Arabia and the UK: A Tale of Two Kingdoms. medRxiv, 2020.
- Alharbi A.A., Alqassim A.Y., Gosadi I.M., Aqeeli A.A., Muaddi M.A., Makeen A.M., Alhazmi A.H., Alharbi A.A. Regional differences in COVID-19 ICU admission rates in the Kingdom of Saudi Arabia: A simulation of the new model of care under vision 2030. J Infect Public Health. 2021;14(6):717–723. doi: 10.1016/j.jiph.2021.04.012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Massonnaud, C., J. Roux, and P. Crépey, COVID-19: Forecasting short term hospital needs in France. medrxiv, 2020.
- Castro M.C. Demand for hospitalization services for COVID-19 patients in Brazil. MedRxiv. 2020 [Google Scholar]
- Chen S., Zhang Z., Yang J., Wang J., Zhai X., Bärnighausen T., Wang C. Fangcang shelter hospitals: a novel concept for responding to public health emergencies. Lancet. 2020;395(10232):1305–1314. doi: 10.1016/S0140-6736(20)30744-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Wu Z., McGoogan J.M. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72314 Cases From the Chinese Center for Disease Control and Prevention. JAMA. 2020;323(13):1239–1242. doi: 10.1001/jama.2020.2648. [DOI] [PubMed] [Google Scholar]
- Sir O. Risk Factors for Prolonged Length of Stay of Older Patients in an Academic Emergency Department: A Retrospective Cohort Study. Emerg Med Int. 2019;2019:4937827. doi: 10.1155/2019/4937827. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Vekaria, B., et al., Hospital length of stay for COVID-19 patients: Data-driven methods for forward planning. 2020. [DOI] [PMC free article] [PubMed]
- Al-Hanawi M.K., Alsharqi O., Almazrou S., Vaidya K. Healthcare Finance in the Kingdom of Saudi Arabia: A Qualitative Study of Householders' Attitudes. Appl Health Econ Health Policy. 2018;16(1):55–64. doi: 10.1007/s40258-017-0353-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Hazazi A.M., Chandramohan S. Privatization of Saudi health-care system and its significant effect: A review. International Journal of Medical Science and Public Health. 2017;6(12):1652–1655. [Google Scholar]
- Health, M.o., VRO Health Sector Transformation Strategy. 2019.
- Almalki M., Fitzgerald G., Clark M. Health care system in Saudi Arabia: an overview. East Mediterr Health J. 2011;17(10):784–793. doi: 10.26719/2011.17.10.784. [DOI] [PubMed] [Google Scholar]
- Corallo Ashley N., Croxford Ruth, Goodman David C., Bryan Elisabeth L., Srivastava Divya, Stukel Therese A. A systematic review of medical practice variation in OECD countries. Health Policy. 2014;114(1):5–14. doi: 10.1016/j.healthpol.2013.08.002. [DOI] [PubMed] [Google Scholar]
- Steinwachs, D.M. and R.G. Hughes, Health Services Research: Scope and Significance, in Patient Safety and Quality: An Evidence-Based Handbook for Nurses, R.G. Hughes, Editor. 2008: Rockville (MD).
- Wunsch H. Variation in critical care services across North America and Western Europe. Crit. Care Med. 2008;36(10) doi: 10.1097/CCM.0b013e318186aec8. [DOI] [PubMed] [Google Scholar]
- Zhou Yuqi, Yao Xi, Liu Guofeng, Jian Weiyan, Yip Winnie. Level and variation on quality of care in China: a cross-sectional study for the acute myocardial infarction patients in tertiary hospitals in Beijing. BMC Health Serv Res. 2019;19(1) doi: 10.1186/s12913-019-3872-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kwan Ada, Daniels Benjamin, Saria Vaibhav, Satyanarayana Srinath, Subbaraman Ramnath, McDowell Andrew, Bergkvist Sofi, Das Ranendra K., Das Veena, Das Jishnu, Pai Madhukar, Evans Carlton. Variations in the quality of tuberculosis care in urban India: A cross-sectional, standardized patient study in two cities. PLoS Med. 2018;15(9):e1002653. doi: 10.1371/journal.pmed.1002653. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Bos Judith T., Frijters Dinnus H.M., Wagner Cordula, Carpenter G. Iain, Finne-Soveri Harriet, Topinkova Eva, Garms-Homolová Vjenka, Henrard Jean-Claude, Jónsson Pálmi V., Sørbye Liv, Ljunggren Gunnar, Schroll Marianne, Gambassi Giovanni, Bernabei Roberto. Variations in quality of home care between sites across Europe, as measured by home care quality indicators. Aging clinical and experimental research. 2007;19(4):323–329. doi: 10.1007/BF03324709. [DOI] [PubMed] [Google Scholar]