Abstract
We describe a patient with of acute right ventricular dysfunction secondary to right ventricular isolated Takotsubo syndrome (TTS). The importance of appropriate differential diagnosis for acute right ventricular dysfunction differential diagnosis of acute right ventricular dysfunction and the differences in diagnosis and management of right ventricular TTS and typical left ventricular TTS are highlighted. (Level of Difficulty: Intermediate.)
Key Words: cardiac magnetic resonance, cardiogenic shock, right ventricle, stress cardiomyopathy, Takotsubo syndrome
Abbreviations and Acronyms: AMI, acute myocardial infarction; ECG, electrocardiogram; LV, left ventricle; MRI, magnetic resonance imaging; RV, right ventricle; TTS, Takotsubo syndrome
Graphical abstract
This study describes a case of acute right ventricular dysfunction secondary to right ventricular isolated Takotsubo syndrome (TTS). The importance…
History of Presentation
An 82-year-old female patient presented to the emergency department with nonspecific discomfort and in poor general condition. Physical examination demonstrated normal chest and cardiac auscultation. The patient showed signs of cardiogenic shock and respiratory failure: blood pressure 90/60 mm Hg, 110 beats/min, arterial oxygen saturation 80%, and lactate levels 7.3 mmol/l. An electrocardiogram (ECG) indicated sinus rhythm with no repolarization abnormalities. Right-sided ECG showed nondeep T waves in leads V3R to V6R (Figure 1). Transthoracic echocardiography revealed normal left ventricular (LV) systolic function but dilation and severe systolic dysfunction of the right ventricle (RV) with apical dyskinesia and basal hypercontractility, also known as the reverse McConnell sign (1).
Learning Objectives
-
•
To review the differential diagnosis of acute RV dysfunction and highlight the importance of the clinical history.
-
•
To understand the differences in clinical presentation and evolution of RV TTS and classic left ventricular TTS.
-
•
Phosphodiesterase-3 inhibitors could be useful in cases of TTS complicated with cardiogenic shock.
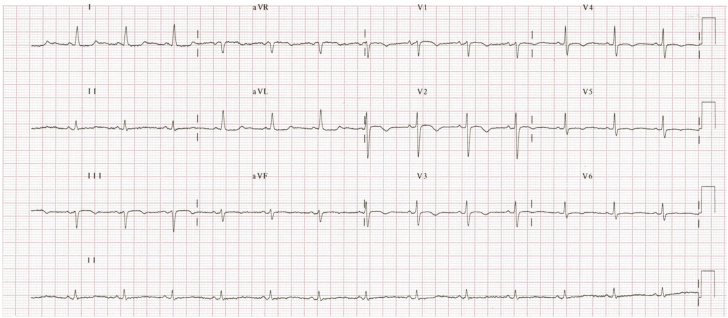
Figure 1.
Initial ECG
(A) ECG at admission showing precordial leads with no repolarization abnormalities. (B) Right-sided precordial leads (right) showing nondeep negative T waves in leads V3R to V6R. ECG = electrocardiogram.
Past Medical History
The patient had a chronic depressive affective disorder. Four days earlier, she had suffered a Colles fracture and coccyx fracture with persistent low back pain in the following days.
Differential Diagnosis
Taking into consideration the initial presentation with respiratory failure and RV dysfunction the initial differential diagnosis should include acute pulmonary embolism and acute myocardial infarction (AMI).
Investigations
Chest computed tomographic scan ruled out pulmonary embolism as the first suspected etiology. High sensitivity troponin T and creatine kinase levels were markedly elevated, with significant dynamic change (high sensitivity troponin T: 469 to 556 to 368 ng/dl; creatine kinase: 354 to 516 to 202 U/l), as was the N-terminal pro–B-type natriuretic peptide level (9,116 ng/l). Coronary angiography performed to rule out RV AMI showed normal coronary arteries (Figure 2). Right ventriculography confirmed midapical dyskinesia (Video 1).
Figure 2.
Right Coronary Angiography, Chest CT Scan, and Cardiac MRI
(Top row) Angiography (left) showing normal right coronary artery (RCA) with no presence of lesions and chest computed tomographic (CT) scan (right) showing no evidence of pulmonary thromboembolism and normal diameter pulmonary trunk. (Middle, bottom rows) Four-chamber cine images by cardiac magnetic resonance imaging (MRI) in diastole (left) and systole (right) with dilated right ventricle (RV) and dyskinesia of the RV free wall at admission and recovery of the volumes and contractility of the RV at cardiac MRI performed 10 days after. LVEDV = left ventricular end-diastolic volume; LVEF = left ventricular ejection fraction; RVEDV = right ventricular end-diastolic volume; RVEF = right ventricular ejection fraction.
Online Video 1.
Right Ventriculography
Right ventriculography performed at admission after coronary angiography showing midapical dyskinesia of the right ventricle.
Management
The patient was admitted to the coronary care unit. Oxygen therapy and administration of milrinone were initiated, with hemodynamic improvement. A pulmonary artery catheter was implanted and revealed pulmonary artery pressures of 34/14 mm Hg, central venous pressure 9 mm Hg, and cardiac index 2.5 l/min/m2. In the following 24 h, the patient demonstrated progressive clinical improvement with resolution of respiratory failure and hemodynamic stability, allowing the withdrawal of inotropic support. Evolutionary ECG on day 2 showed the appearance of negative T waves in leads V1 to V4 with a slight QT-interval prolongation (Figure 3).
Figure 3.
Evolutionary ECG
ECG performed on day 2 showing evolutionary negative T waves in leads V1 to V4 with slight QT-interval prolongation. ECG = electrocardiogram.
Cardiac magnetic resonance imaging (MRI) performed on day 2 showed a nonhypertrophic but dilated RV with dyskinetic movement of the apex and midanterior wall segments, conditioning mild RV systolic dysfunction (Figure 2, Video 2). Sequences to evaluate for the presence of myocardial edema could not be performed because the patient had low back pain due to prolonged recumbency.
Online Video 2.
Cardiac MRI Cine Sequence at Admission
Four-chamber cine images by cardiac magnetic resonance imaging on day 2 of hospitalization showing dilated right ventricle (RV) and dyskinesia of the RV free wall.
On day 3, the patient was transferred to the cardiology ward. Control transthoracic echocardiography and cardiac MRI (days 7 and 10 after admission) showed normalization of volumes and regional/global RV systolic function without late gadolinium enhancement (Figure 2, Video 3).
Online Video 3.
Cardiac MRI Cine Sequence at Follow-Up
Four-chamber cine images by cardiac magnetic resonance imaging on day 10 showing normalization of right ventricular volumes and contractility.
After pulmonary embolism, acute coronary syndrome, and other pathologies associated with transient acute RV dysfunction (e.g., acute myocarditis) were ruled out and considering the typical clinical scenario of a post-menopausal woman with a previous stressful situation and a compatible ECG evolution, the diagnosis of Takotsubo syndrome (TTS) with isolated RV involvement was finally established.
Discussion
TTS, also known as stress cardiomyopathy, is an acute heart failure syndrome that usually affects post-menopausal women with a recent physical or psychological stressor. Unlike AMI, TTS is characterized by the absence of significant coronary lesions and the reversibility of cardiac dysfunction. However, because of the similar acute clinical presentations, it often triggers a differential diagnosis with AMI. TTS is increasingly recognized and reported, probably because of better knowledge of the disease and its particular characteristics, but the precise incidence is unknown (2,3). The apical and midregional systolic defect is the most frequent form of LV regional wall motion abnormality. It is classified as the typical anatomic variant of TTS, but other atypical forms have been described. Nevertheless, the isolated involvement of the RV is exceptional, and few cases have been reported to date (4,5), so this variant has not yet been included as a type of TTS in expert consensus (2,3). Unlike classic forms of TTS affecting the LV, some specific characteristics present in this case that we found in common with previously reported cases of isolated RV TTS are: 1) development of nondeep negative T waves in leads V1 to V4 on the evolutionary ECGs, in opposition to the deep and predominantly anterolateral negative T waves generally observed in the typical form of TTS; 2) dilation of the affected ventricle, which is not commonly observed in the LV forms of TTS, with characteristic systolic impairment resembling the reverse McConnell sign (i.e., apical dyskinesia and hyperkinesia of the basal segments); and 3) frequent severe clinical presentation, with a reasonably rapid clinical recovery in accordance with the rapid improvement of RV systolic dysfunction seen in the imaging tests. Interestingly, this recovery seems to occur faster than in patients with LV involvement.
In this case, some particular characteristics were noted. First, the initial ECG showed nonpathological negative T waves limited to lead V1. The initial ECG can be normal in up to 14% of patients with classic LV TTS (6), and usually these patients develop deep negative T waves over the course of several days. This fact, in conjunction with the low magnitude of ECG changes reflecting RV pathology in the standard leads, could explain the normal ECG upon admission of this patient. Second is the choice of milrinone treatment and its successful response. We decided to administer a phosphodiesterase-3 inhibitor rather than dobutamine to avoid the use of catecholamines. Use of phosphodiesterase-3 inhibitors has been described for treatment of TTS complicated by cardiogenic shock, with successful results (7,8). Dobutamine use has been described as a trigger of TTS (9). Nonetheless, there is a lack of evidence on the benefit of using milrinone over dobutamine in clinical practice.
Follow-Up
Within 2 years follow up with cardiology the patient is in New York Heart Association functional class I. Ambulatory echocardiography demonstrated normal biventricular function with no recurrence of TTS episodes.
Conclusions
Although very uncommon, RV TTS has to be considered in the differential diagnosis of acute right heart failure. This entity has several specific features that differentiate it from typical LV TTS. Previously reported cases describe a frequent severe clinical presentation, usually cardiogenic shock, with more rapid recovery than cases of LV TTS.
Footnotes
The authors have reported that they have no relationships relevant to the contents of this paper to disclose.
The authors attest they are in compliance with human studies committees and animal welfare regulations of the authors’ institutions and Food and Drug Administration guidelines, or patient consent where appropriate. For more information, visit the JACC: Case Reportsauthor instructions page.
Appendix
For supplemental videos, please see the online version of this paper.
References
- 1.Liu K., Carhart R. “Reverse McConnell’s sign?”: a unique right ventricular feature of Takotsubo cardiomyopathy. Am J Cardiol. 2013;111:1232–1235. doi: 10.1016/j.amjcard.2012.12.007. [DOI] [PubMed] [Google Scholar]
- 2.Lyon A.R., Bossone E., Schneider B. Current state of knowledge on Takotsubo syndrome: a position statement from the Taskforce on Takotsubo Syndrome of the Heart Failure Association of the European Society of Cardiology. Eur J Heart Fail. 2016;18:8–27. doi: 10.1002/ejhf.424. [DOI] [PubMed] [Google Scholar]
- 3.Ghadri J.-R., Wittstein I.S., Prasad A. International expert consensus document on Takotsubo syndrome (part I): clinical characteristics, diagnostic criteria, and pathophysiology. Eur Heart J. 2018;39:2032–2046. doi: 10.1093/eurheartj/ehy076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Stähli B.E., Ruschitzka F., Enseleit F. Isolated right ventricular ballooning syndrome: a new variant of transient cardiomyopathy. Eur Heart J. 2011;32:1821. doi: 10.1093/eurheartj/ehr079. [DOI] [PubMed] [Google Scholar]
- 5.Sumida H., Morihisa K., Katahira K., Sugiyama S., Kishi T., Oshima S. Isolated right ventricular stress (Takotsubo) cardiomyopathy. Intern Med. 2017;56:2159–2164. doi: 10.2169/internalmedicine.8323-16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Frangieh A.H., Obeid S., Ghadri J.-R. ECG criteria to differentiate between Takotsubo (stress) cardiomyopathy and myocardial infarction. J Am Heart Assoc. 2016;5 doi: 10.1161/JAHA.116.003418. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Mrozek S., Srairi M., Marhar F. Successful treatment of inverted Takotsubo cardiomyopathy after severe traumatic brain injury with milrinone after dobutamine failure. Heart Lung. 2016;45:406–408. doi: 10.1016/j.hrtlng.2016.06.007. [DOI] [PubMed] [Google Scholar]
- 8.Padayachee L. Levosimendan: the inotrope of choice in cardiogenic shock secondary to takotsubo cardiomyopathy? Heart Lung Circ. 2007;16 Suppl 3:S65–S70. doi: 10.1016/j.hlc.2007.03.018. [DOI] [PubMed] [Google Scholar]
- 9.Hajsadeghi S., Rahbar M.H., Iranpour A., Salehi A., Asadi O., Jafarian S.R. Dobutamine-induced takotsubo cardiomyopathy: a systematic review of the literature and case report. Anatol J Cardiol. 2018;19:412–416. doi: 10.14744/AnatolJCardiol.2018.78642. [DOI] [PMC free article] [PubMed] [Google Scholar]