Abstract
Background:
COVID-19 brought significant challenges to public health. It changed the view of global health and safety, trust in the healthcare system, and clients’ willingness to seek healthcare. To contain the course of the COVID-19 pandemic and its detrimental effects, understanding peoples’ health behavior, especially healthcare-seeking, and determining the community risk perception is very important. Thus, this study aimed to determine the health-seeking behavior, community’s risk perception to COVID-19 pandemics, and factors influencing the community risk perception in Harari regional state, Ethiopia.
Methods:
Community-based cross-sectional study was conducted from 5 to 30 February 2021. A total of 1320 adult (>18 years) participants were selected using systematic random sampling. The data were collected using an online kobo collect toolbox and analyzed using descriptive statistical tests. Chi-square test and multiple binary logistic regression were applied to examine the difference between variables. A p-value < 0.05 was considered to be of statistical significance.
Results:
The study included 1296 respondents >18 years old. The overall prevalence of willingness to seek healthcare in the study area was 35.6% (95% CI: 33%–38.3.0%). The mean cumulative score of risk perception was 30.5 (SD ± 7.25) with the minimum and maximum score of 13 and 63, respectively. A total of 656 (50.6%) of the participants had low-risk perceptions concerning COVID-19. The study found a statistically significant association between risk perception and sociodemographic characteristics (age, educational status, and income), and knowledge of the respondents.
Conclusion:
The overall prevalence of willingness to seek healthcare was 35.6%. Healthcare intervention aimed to contain the COVID-19 pandemic should consider the factors associated with the study area. Similarly, the study found a low-risk perception among the community that needs critical action to manage the COVID-19 pandemic and to protect the community as a whole. Thus, it is necessary to improve community risk perception through health education.
Keywords: Risk perception, COVID-19, coronavirus, 2019, SARS-CoV-2, community risk perception
Background
The global epidemic of coronavirus disease 2019 (COVID-19) has presented a major threat to public health worldwide. 1 COVID-19 is the result of an infection with severe acute respiratory syndrome, coronavirus 2 (SARS-CoV-2) that was first isolated and identified in patients who were exposed to a seafood market in Wuhan City, China, in December 2019. 2 Similar to the findings related to SARS-CoV and Middle East respiratory syndrome coronavirus (MERS-CoV), SARS-CoV-2 is believed to cross species to initiate primary human infections; it is now spread primarily by human-to-human transmission. 3 Due to its rapid spread from China to many countries worldwide, COVID-19 was declared a global pandemic by the World Health Organization (WHO) 4 on 11 March 2020.
The disease is highly infectious, and its main clinical symptoms include fever, cough, and dyspnea. Approximately 20% of those hospitalized needed to be admitted to the intensive care unit (ICU) for critical management for severe stage, which is characterized by acute respiratory distress syndrome, acute cardiac injury, acute kidney injury, shock, and secondary infections. 5 Epidemiologically, the distribution of the disease is exponentially growing across the globe. Since the first reported case on 31 December 2019, it has resulted in over 2,465,517 deaths and over 111 million infections globally as of 20 February 2020. 6
In Ethiopia, the first confirmed COVID-19 case was reported on 13 March 2020, of a 48-year-old Japanese man, who had traveled from Japan to Burkina Faso and who then arrived in Ethiopia,. Three weeks into the outbreak, cases were noted among people without a history of travel to COVID-19 endemic countries but who were in contact with confirmed cases. 7 As of 16 February 2021, there were 148,490 confirmed cases of COVID-19 and a total of 2223 deaths. 8 The Government of Ethiopia has implemented a variety of policy actions and precautionary measures to control the spread and mitigate the impact of the COVID-19 pandemic. Despite efforts to scale-up public health interventions to contain and mitigate the spread of coronavirus in Ethiopia, new cases have continued to emerge. Gaps and negligence in applying the COVID-19 preventive measures among the public have been observed.9,10
Understanding individuals’ perceived risk is important in terms of effective control of an outbreak of infectious diseases. 11 The motivation to protect oneself from disease is related to the perceived threat. The perceived threat is derived from both how people feel vulnerable to develop a certain condition and how severe it would be for them to be affected. 12 A lower perceived risk leads to lower adherence, whereas people with higher levels of risk perception are significantly more likely to be willing to comply with specific public health behaviors.11,13
The primary aim of this study was to assess the community risk perception of COVID-19 infection and factors influencing this risk perception among adult residents of Harari regional state.
Materials and methods
Study area and period
The study was conducted in Harari regional state, which is one of the 10 regional states found in Ethiopia, from 5 to 30 February 2021. The region is located 510 km far away from Addis Ababa, the capital city of Ethiopia. The region is divided into nine woredas with three of them being rural and six being urban.
The urban districts are subdivided into 19 kebeles (the lowest administrative division in the country), and the rural districts are subdivided into 17 peasant associations (which is equivalent to kebeles in urban cases). The total population (2021 projection based on the 2007 Census, CSA) of the region is 270,000 of which 136,000 are males and 134,000 are females.
Study design
Community-based cross-sectional study design was employed.
Source population
Harari regional state adult residents were a source population.
Study population
All adult residents living in selected kebeles of Harari regional state aged ⩾18 years old formed the study population.
Inclusion and exclusion criteria
Inclusion criteria
Residents living in selected households as heads or any other household members >18 years old and available during data collection were included in the study.
Exclusion criteria
People who left their house for some reason and were seriously ill during data collection were excluded from the study.
Sample size determination and sampling technique
The sample size was calculated by using the single population proportion formula (n = (Zα/2)2p (1–p)/d2), where n is the minimum sample size required, p is the estimated proportion of risk perception, and Zα/2 is the value of the standard score at 95% confidence interval (1.96); the assumptions of confidence level are at 95% = 1.96, a margin of error (d) = 0.03, design effect = 2, and non-retrieval rate = 10%. For this study, p = 53.4% (the proportion of community risk perception in Ethiopia) was used. 14 The number of households included in the study was calculated as
Thus n = 2(1.96)2 × 0.534(1–0.534)/(0.04)2 =1195.
Including 10% contingency (non-response rate) which is 120, the sample size was 1315. Therefore, the final sample size was 1315 households.
A multistage sampling technique was used for sampling the study participants. From 9 woredas, 13 kebeles were selected using the simple random sampling (lottery) method. Then from the selected kebeles, 1315 households were allocated proportionally. Each study participant (HH) was selected using a systematic random sampling method, and then, an eligible individual within the selected household was included in the study. Using this technique, a total of 1315 eligible individuals for the study were obtained from the households included in the survey.
Data collection method
A questionnaire was created online by the investigators using an online survey portal, Kobo toolbox (Harvard Humanitarian Initiative, Cambridge, MA). The questionnaire was valid and reliable as it was adapted from the WHO and UNICEF documents relating to COVID-19 preparedness and response 15 and similar researches.7,14,16 Furthermore, the data collection tool (questionnaire) was pretested to check its clarity, sequence, applicability, and validity. A brief introductory orientation was given to the study participants by data collectors about the purpose of the study. An explanation was given about the importance of their involvement, volunteer individuals were interviewed, and then the data were filled in by data collectors using an online survey portal. The data were collected by 30 well-trained undergraduate students under the guidance of 8 MSc holding superiors and 8 investigators.
Operational definitions
Knowledge of the participants regarding COVID-19 was determined based on the questions developed for the knowledge section by calculating the sum score. 17 Participants who correctly answered below or equal to the mean were considered as having poor knowledge, whereas those who had answered above the mean were considered as having good knowledge.
Risk perception regarding COVID-19 was measured using Likert-type scales. The respondents rated their levels of agreement with different statements. Furthermore, the cumulative risk perception score was computed. Based on the mean score, the risk perception is categorized as high for those who score above the mean, and low for those who score mean or below.17,18
The practice of COVID-19 prevention method was measured using 10 questions. The respondents rated how often they were following the preventive methods recommended by WHO on five scales: none (1), rarely (2), sometimes (3), frequently (4), and always (5). Then, the cumulative practice score was computed. Based on the mean score, the practice of COVID-19 preventive methods was categorized as good for those who scored above the mean, and poor for those who scored mean or below. 18
Data analysis and quality control
A descriptive statistical test was used to provide a clear distribution of the data. Numerical variables were measured as mean, median, interquartile range, and standard deviations, while categorical variables were expressed as frequency and percentages. Chi-square test was done to examine the differences between the categorical variables. Finally, multiple binary logistic regression was applied to examine the effects of independent variables on community risk perception and expressed as odds ratio (OR) and 95% confidence interval (CI). A p-value < 0.05 was considered as statistically significant.
Results
Sociodemographic characteristics
A total of 1296 respondents participated in the study at a response rate of 98.03%. The median age of the study participants was 32 years with an interquartile range of 14 years.
There were 657 (50.7%) male respondents, 953 (73.5%) of the participants were married, 785 (60.6%) were urban residents, 403 (31.1%) had attended primary, and 513 (39.6%) had completed secondary education or above. The average monthly income of the study participants was 3120 Ethiopian birrs. A total of 1246 (96.1%) study participants were living with one or more persons in the house (Table 1).
Table 1.
Sociodemographic characteristics of the study participants in Harari regional state, Ethiopia, 2021 (n = 1296).
| Variables (n = 1296) | Category | Frequency | % |
|---|---|---|---|
| Age | 18–25 | 311 | 24 |
| 26–35 | 501 | 38.7 | |
| 36–45 | 310 | 23.9 | |
| Above 45 | 174 | 13.4 | |
| Sex | Male | 657 | 50.7 |
| Female | 639 | 49.3 | |
| Address | Urban | 785 | 60.6 |
| Rural | 511 | 39.4 | |
| Marital status | Single | 228 | 17.6 |
| Married | 953 | 73.5 | |
| Widowed | 43 | 5.6 | |
| Divorced | 72 | 3.3 | |
| Educational status | No education | 380 | 29.3 |
| Primary school | 403 | 31.1 | |
| Secondary school | 263 | 20.3 | |
| College and above | 250 | 19.3 | |
| Occupational status | Housewife | 273 | 21.1 |
| Merchant | 279 | 21.5 | |
| Government employee | 123 | 9.5 | |
| Private employee | 278 | 21.5 | |
| Farmer | 220 | 17 | |
| Others | 123 | 9.5 | |
| Number of family living together | Alone | 50 | 3.9 |
| More than one | 1246 | 96.1 | |
| Average monthly income | ⩽5000 ETB | 1064 | 82.1 |
| 5001–10,000 ETB | 209 | 16.1 | |
| >10,000 ETB | 23 | 1.8 |
ETB: Ethiopian Birr; Others: student, no job.
Knowledge of the community regarding COVID-19
Among 1296 study participants, 1274 (98.3%) of them had heard about the new emerging coronavirus and 1040 (80.2%) knew that COVID-19 was the name of the virus; for 900 of the participants (69.3%), the kind of information that they received about the disease was about the symptoms of the new coronavirus disease; while 989 (76.3%) of the participants got information from TV, which was the most trusted source of information, at 912 (70.4%).
Among the study participants, n = 1296 gave the response for the current study, 781 (60.3%), 752 (58%), 885 (68.3%), and 454(35%) of the participants were those who answered that COVID-19 could be transmitted via inhalation of a droplet from infected people, through airborne, through direct contact with infected people, and through touching of infected surfaces, respectively.
The mean sum score of knowledge items was 9.3 (SD ± 3.21) with minimum and maximum scores of 0 and 20, respectively. Among the 1296 respondents, 707 (54.6%) of them had poor knowledge while 589 (45.4%) had good knowledge (Table 2).
Table 2.
Knowledge of COVID-19 among adult residents of Harari regional state, Ethiopia, 2021 (n = 1296).
| Variables (n = 1296) | Category | Frequency | % |
|---|---|---|---|
| Have you ever heard about the new coronavirus disease (COVID 19)? | Yes | 1274 | 98.3 |
| No | 22 | 1.7 | |
| Cause of disease | Correct | 1040 | 80.2 |
| Incorrect | 256 | 19.8 | |
| Can the virus transmit through the following routes? | |||
| Blood transfusion | Yes | 66 | 5.1 |
| No | 1230 | 94.9 | |
| Droplet from infected person | Yes | 781 | 60.3 |
| No | 515 | 39.7 | |
| Airborne | Yes | 752 | 58 |
| No | 544 | 42 | |
| Direct contact with the infected person | Yes | 885 | 68.3 |
| No | 411 | 31.7 | |
| Touching contaminated object | Yes | 454 | 35 |
| No | 842 | 65 | |
| Mosquito bite | Yes | 24 | 1.9 |
| No | 1272 | 98.1 | |
| Eating contaminated food/drinking contaminated water | Yes | 61 | 4.7 |
| No | 1235 | 95.3 | |
| Are the following the symptoms of coronavirus? | |||
| Fever | Yes | 1017 | 78.5 |
| No | 279 | 21.5 | |
| Cough | Yes | 1179 | 91 |
| No | 117 | 9 | |
| Shortness of breath and difficulty in breathing | Yes | 670 | 51.7 |
| No | 626 | 48.3 | |
| Muscle pain | Yes | 233 | 18 |
| No | 1063 | 82 | |
| Headache | Yes | 650 | 50.2 |
| No | 646 | 49.8 | |
| Diarrhea | Yes | 90 | 6.9 |
| No | 1206 | 93.1 | |
| Are the following measures/methods used to prevent COVID 19? | |||
| Wash hand regularly with alcohol or soap and water | Yes | 1093 | 84.3 |
| No | 203 | 15.7 | |
| Cover mouth and nose when coughing or sneezing | Yes | 110 | 8.5 |
| No | 1186 | 91.5 | |
| Avoid contact with anyone who has a cough and fever | Yes | 726 | 56 |
| No | 570 | 44 | |
| Maintain physical distance | Yes | 54 | 4.2 |
| No | 1242 | 95.8 | |
| Avoid unprotected direct contact | Yes | 63 | 4.9 |
| No | 1233 | 95.1 | |
| Cook food/drink treated water | Yes | 809 | 62.4 |
| No | 487 | 37.6 | |
| Sleep under mosquito net | Yes | 27 | 2.1 |
| No | 1269 | 97.9 | |
Source of information about COVID-19
Respondents were asked their source of information about the status of COVID-19 and the means of prevention methods to reduce the risk of COVID-19 infection. It was found that 76.3%, 54.6%, 43%, and 43.4% of the respondents reported that they got information about COVID-19 from television, radio, families, and friends, and health professionals, respectively. The participants reported that the kind of information they received from those media were about the symptoms of the disease (69.4%), mode of transmission of the disease (69.3%), how to protect themselves from disease (62.7%), preventive mechanisms (34.3%), and risks and complications (18.2%).
Risk perception regarding COVID-19
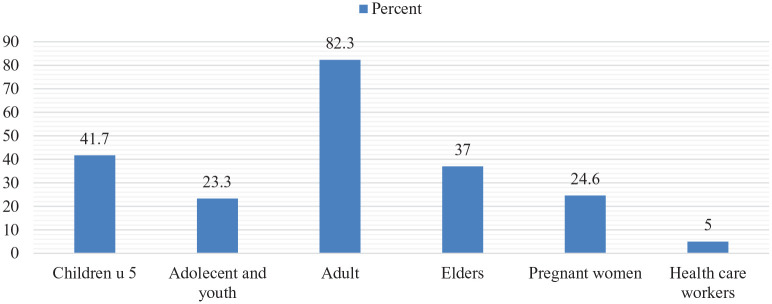
In all, 1067 (82.3%) of the respondents perceived that adults were more at risk than others, while 41.7% of the participants believed that children aged <5 years were more at risk than others (Figure 1).
Figure 1.
Perception of the participants regarding who are at most risk to get the coronavirus 2019.
In all, 790 (61.0%) of the respondents strongly agreed that the risk of new coronavirus is very dangerous; 424 (32.7%) of the study participants agreed that they are more likely to become sick with the new coronavirus; 626 (48.3%) of the participants strongly agreed that COVID-19 causes more deaths than other respiratory diseases; and 550 (42.4%) of the participants agreed that their health would be severely damaged if they contracted coronavirus. The mean cumulative score of risk perception was 30.5 (SD ± 7.25) with the minimum and maximum scores of 13 and 63, respectively; 656 (50.6%) of the participants had low-risk perceptions concerning COVID-19 (Table 3).
Table 3.
Risk perception toward COVID-19 among adult residents of Harari regional state, Ethiopia, 2021 (1296).
| Statements (n = 1296) | Category | Frequency | % |
|---|---|---|---|
| New coronavirus risk is very dangerous | Strongly agree | 790 | 61.0 |
| Agree | 383 | 29.6 | |
| Neutral | 70 | 5.4 | |
| Disagree | 39 | 3.0 | |
| Strongly disagree | 14 | 1.1 | |
| I think that I am likely to become sick with the new coronavirus | Strongly agree | 399 | 30.8 |
| Agree | 424 | 32.7 | |
| Neutral | 248 | 19.1 | |
| Disagree | 170 | 13.1 | |
| Strongly disagree | 55 | 4.2 | |
| I think that COVID-19 causes more deaths than other respiratory diseases | Strongly agree | 626 | 48.3 |
| Agree | 446 | 34.4 | |
| Neutral | 148 | 11.4 | |
| Disagree | 50 | 3.9 | |
| Strongly disagree | 26 | 2.0 | |
| I think that work exposes me more to COVID-19 | Strongly agree | 436 | 33.6 |
| Agree | 632 | 48.8 | |
| Neutral | 156 | 12.0 | |
| Disagree | 3 | 2.0 | |
| Strongly disagree | 69 | 5.3 | |
| I think getting sick with the coronavirus can be serious | Strongly agree | 593 | 45.8 |
| Agree | 517 | 39.9 | |
| Neutral | 94 | 7.3 | |
| Disagree | 74 | 5.7 | |
| Strongly disagree | 18 | 1.4 | |
| I think my health will be severely damaged if you contract coronavirus | Strongly agree | 431 | 33.3 |
| Agree | 550 | 42.4 | |
| Neutral | 122 | 9.4 | |
| Disagree | 137 | 10.6 | |
| Strongly disagree | 56 | 4.3 | |
| I think it is not possible to recover from coronavirus disease | Strongly agree | 155 | 12.0 |
| Agree | 311 | 24.0 | |
| Neutral | 144 | 11.1 | |
| Disagree | 493 | 38.0 | |
| Strongly disagree | 193 | 14.9 | |
| I think If I am caught with coronavirus, I cannot manage my daily activities | Strongly agree | 333 | 25.7 |
| Agree | 554 | 42.7 | |
| Neutral | 177 | 13.7 | |
| Disagree | 207 | 16.0 | |
| Strongly disagree | 23 | 1.9.0 | |
| I think people may stigmatize me if I get sick due to coronavirus | Strongly agree | 527 | 40.7 |
| Agree | 527 | 40.7 | |
| Neutral | 149 | 11.5 | |
| Disagree | 67 | 5.2 | |
| Strongly disagree | 26 | 2.0 | |
| I think that I will contract coronavirus if I do not take any preventive measure | Strongly agree | 401 | 30.9 |
| Agree | 651 | 50.2 | |
| Neutral | 141 | 10.9 | |
| Disagree | 91 | 7.0 | |
| Strongly disagree | 12 | 0.9 | |
| I think that I will contract coronavirus if I come into contact with a coronavirus patient | Strongly agree | 444 | 34.3 |
| Agree | 680 | 52.5 | |
| Neutral | 115 | 8.9 | |
| Disagree | 47 | 3.6 | |
| Strongly disagree | 10 | 0.8 | |
| I think that the coronavirus will not affect very many people in the area I am currently living | Strongly agree | 266 | 20.5 |
| Agree | 490 | 37.8 | |
| Neutral | 241 | 18.6 | |
| Disagree | 243 | 18.8 | |
| Strongly disagree | 56 | 4.3 |
Willingness to seek healthcare among the study participants
In all, 462 (35.6%) (95% CI: 33%–38.3.0%) of the participants showed willingness to seek healthcare if they developed any kind of disease symptoms during the COVID-19 pandemic. Of these, 39.4%, 33.8%, 14.9%, and 11.9% of the participants preferred a health center, hospital, private clinic, and traditional healer for seeking the treatment, respectively. Among those participants who showed willingness to seek health care, 364 (78.8%) were reported to seek healthcare immediately as the illness started. Furthermore, 890 (68.7%) of the participants reported self-treatment practice.
Practice of COVID-19 preventive measure and self-efficacy
A total of 479 (37.0%) of the respondents wash their hands with water and soap sometimes and 153 (11.2%) of the respondents were not wearing a facemask at work or outside the home always. Out of the total respondents (n = 1296), 738 (56.9%) did not wear a glove at all, while 223 (17.2%) wore it rarely, 7.1% wore it frequently, and 3.8% wore gloves always (Table 4).
Table 4.
Practice of COVID-19 preventive measure among adult residents of Harari regional state, Ethiopia, 2021 (n = 1296).
| Questions (n = 1296) | None |
Rarely |
Sometimes |
Frequently |
Always |
|---|---|---|---|---|---|
| N (%) | N (%) | N (%) | N (%) | N (%) | |
| How often do you maintain physical distance? | 310 (23.9) | 453 (35.0) | 393 (30.3) | 86 (6.6) | 54 (4.2) |
| How often do you avoid larger gatherings? | 332 (25.6) | 484 (37.3) | 364 (28.1) | 84 (6.5) | 32 (2.5) |
| How often do you avoid touching your face, eyes, mouth, and nose? | 270 (20.8) | 392 (30.2) | 410 (31.6) | 173 (13.3) | 51 (3.9) |
| How often do you wash your hands with water and soap or sanitizers? | 102 (7.9) | 277 (21.4) | 479 (37.0) | 281 (21.7) | 157 (12.1) |
| How often do you avoid contact with people who had fever and cough? | 156 (12.0) | 319 (24.6) | 333 (25.7) | 265 (20.4) | 223 (17.2) |
| How often do you wear a facemask when you are at work or outside the home? | 153 (11.8) | 289 (22.3) | 471(36.3) | 238 (18.4) | 145 (11.2) |
| How often do you avoid using public transportation? | 482 (37.2) | 328 (25.3) | 319 (24.6) | 132 (10.2) | 35 (2.7) |
| How often do you avoid unprotected contacting (touching) of frequently contacted surfaces? | 318 (24.5) | 371 (28.6) | 424 (32.7) | 134 (10.3) | 49 (3.8) |
| How often do you stay home to prevent COVID-19 infection? | 464 (35.8) | 384 (29.6) | 285 (22.0) | 103 (7.9) | 60 (4.6) |
| How often do you use gloves at work? | 738 (56.9) | 223 (17.2) | 194 (15.0) | 92 (7.1) | 49 (3.8) |
| Self-efficacy to COVID-19 preventive measures | |||||
| Questions | Certainly not | Probably not | Perhaps not–Perhaps | Probably yes | Most certainly |
| Do you think that you manage to handwash with water and soap or sanitizer frequently? | 144 (11.1) | 266 (20.5) | 132 (10.2) | 548 (42.3) | 206 (15.9) |
| Do you think that you manage to stay at home? | 255 (19.7) | 366 (28.2) | 205 (15.8) | 361 (27.9) | 109 (8.4) |
| Do you think that you manage to maintain distancing anywhere? | 196 (15.1) | 353 (27.2) | 201 (15.5) | 422 (32.6) | 124 (9.6) |
N: sample size.
The mean cumulative score of the practices of COVID-19 preventive measures was 24.7 (SD ± 7.8); 664 (51.2%) of the respondent’s practice of preventive measures was poor.
Out of the 1296 respondents, only 206 (15.9%) were almost certain that they can wash their hands with water and soap or with sanitizers; 124 (9.6%) of the respondents reported that they certainly maintain distancing anywhere. The mean of the cumulative score of self-efficacy items was 9.03(SD ± 3.07) (Table 4).
Factors associated with risk perception toward COVID-19
In the bivariate model, risk perception was significantly associated with the age of the participants, address, educational status, marital status, income level, and knowledge of COVID-19. To control the effect of confounders, variables including age, address, educational status, marital status, income, knowledge of COVID-19, the practice of COVID-19 preventive measures, and self-efficacy on preventive measures of COVID 19 were selected for multivariate logistic regression. Age of the respondents, address, educational status, marital status, income, and knowledge of COVID-19 were significantly associated with risk perception.
The age of the respondents was significantly associated with risk perception regarding COVID-19. Respondents aged 18–25 and 26–35 were 1.8 times (AOR = 1.8, 95% CI (1.163, 2.8)) and 1.8 times (AOR = 1.84, 95% CI (1.27, 2.66)) more likely to have low-risk perception regarding COVID-19 when compared with those aged 45 years old, respectively. However, respondents aged 36–45 years were 0.64 (AOR = 0.64, 95% CI (0.43, 0.95) times less likely to have low-risk perception compared to those who aged >45 years.
The address of the respondents was significantly associated with risk perception. Respondents who came from the rural areas was 1.62 times (AOR = 1.62, 95% CI (1.24, 2.10)) more likely to have low-risk perception regarding COVID-19 compared with respondents who came from the urban areas. Educational status was also significantly associated with risk perception regarding COVID-19. Participants who had no formal education and primary education were 1.9 times (AOR = 1.93, 95% CI (1.29, 2.87)) and 1.44 times (AOR = 1.44, 95% CI (1.01, 2.05)) more likely to have low-risk perceptions compared with those respondents having college and above educational status, respectively. Similarly, participants with income of ⩽5000 ETB and 5001–10,000 ETB had 0.15- and 0.22-times lower odds of having low-risk perception regarding COVID-19 compared with those who had an income >10,000 ETB (AOR = 0.15, 95% CI (0.05,0.45)) and (AOR = 0.22, 95% CI (0.07, 0.69)), respectively.
The odds of having a lower risk perception regarding COVID-19 among participants who had poor knowledge was 0.50 times that of participants who had good knowledge (0.39, 0.63) (Table 5).
Table 5.
Factors associated with community risk perception toward COVID-19 among adult residents of Harari regional state, Ethiopia (n = 1296).
| Variables (n = 1296) | Risk perception |
AOR (95% CI) | |||
|---|---|---|---|---|---|
| Low | High | COR (95% CI) | |||
| Age | 18–25 | 177 | 134 | 1.66 (1.145, 2.42)* | 1.81 (1.163, 2.8)** |
| 26–35 | 289 | 212 | 1.72 (1.12, 2.43)* | 1.84 (1.27, 2.66)** | |
| 36–45 | 113 | 197 | 0.72 (0.50, 1.1)* | 0.64 (0.43, 0.95)* | |
| Above 45 | 77 | 97 | 1 | 1 | |
| Address | Rural | 294 | 217 | 1.58 (1.27, 1.98)** | 1.62 (1.24, 2.10)** |
| Urban | 362 | 423 | 1 | 1 | |
| Educational status | No formal education | 204 | 176 | 1.45 (1.05, 2.0)* | 1.93 (1.29, 2.87)** |
| Primary | 206 | 197 | 1.31 (1.00, 1.80) | 1.44 (1.01, 2.05)* | |
| Secondary | 135 | 128 | 1.3 (0.9, 1.87) | 1.40 (0. 6, 2.03) | |
| Collage and above | 111 | 139 | 1 | 1 | |
| Marital status | Widowed/divorced | 41 | 74 | 0.49 (0.31, 0.77)* | 0.84 (0.58, 1.22) |
| Married | 493 | 460 | 0.94 (0.70, 1.26) | 0.66 (0.43, 1.01) | |
| Single | 121 | 106 | 1 | 1 | |
| Income | ⩽5000 ETB | 529 | 535 | 0.21 (0.07, 0.62)** | 0.15 (0.05, 0.45)** |
| 5001–10,000 ETB | 108 | 101 | 0.225 (0.074, 0.68)** | 0.22 (0.07, 0.69)** | |
| >10,000 ETB | 19 | 4 | 1 | 1 | |
| Knowledge level | Poor | 315 | 392 | 0.58 (0.47, 0.73)** | 0.50 (0.39, 0.63)** |
| Good | 341 | 248 | 1 | 1 | |
| Practice of preventive measures | Poor | 328 | 335 | 1.1 (0.88, 1.49) | 0.94 (0.73, 1.20) |
| Good | 328 | 305 | 1 | 1 | |
| Self-efficacy to preventive measures | Poor | 343 | 362 | 1.19 (0.955, 1.50) | 0.86 (0.67, 1.09) |
| Good | 313 | 278 | 1 | 1 | |
COR: crude odds ratios; AOR: adjusted odds ratio; CI: confidence interval; ETB: Ethiopian Birr.
Significant at ⩽ 0.05; **significant at < 0.01.
Discussion
The current study aimed to determine the community risk perception toward COVID-19 among the community in Harari Regional State, Eastern Ethiopia. Among the study participants interviewed, 501(38.7%) were aged ranging from 26 to 35 years, and 380 (29.3%) had no formal education. However, another study conducted in Nigeria reported a higher proportion of study participants who had completed a degree 471 (30.35%). 19 The difference may be due to the data collection tools employed to collect data, since the current study was conducted using a questionnaire (face-to-to-face interview).
Among the study participants (1296), 781 (60.3%) answered that COVID-19 could be transmitted via inhalation of a droplet from infected people, which was lower than the finding of another study conducted in China, which reported that 2734 (96.1%) of the respondents knew that COVID-19 could be transmitted from person to person. 20 Similarly, the current study found 752 (58.0%) of the respondents reported airborne as a transmission route for COVID-19; this was lower than the finding of another study conducted in China, which found that 2730 (96.0%) of respondents reported breathing and droplets as a transmission route for COVID-19. 20 The variation may be related to the difference in sources of information, educational status of the respondents, and timely access to the information that can all play a major role in controlling the COVID-19 pandemic.
The current study found that 1173 (90.5%) of the respondents perceived (strongly agreed and agreed) that the risk of new coronavirus was very dangerous, which was in line with the finding of another study conducted in Ethiopia that reported 87.5% of respondents to perceive that COVID-19 is a serious disease. 7 However, another study conducted in China found 94.4% of respondents reported a high level of perceived severity of COVID-19 that was agreed with the findings of the current study. 21 The difference may be related to the variation in the health information system, educational status of the respondents, and rumors in the community that contributes to COVID-19 pandemic management.
In all, 424 (32.7%) of the study participants agreed that they were more likely to become sick with the new coronavirus, which was inconsistent with the finding of another study conducted in Ethiopia reporting that 446 (85.6%) of respondents perceived that COVID 19 is a serious disease. 7 The difference may be related to the scope of the study and increasing rumors in the community, which can all be obstacles in controlling the COVID-19 pandemic.
The current study found that 656 (50.6%) of the respondents had low-risk perceptions concerning COVID-19, which was in line with the finding of another study which reported that 222 (53.4%) of respondents had high-risk perceptions concerning COVID-19. 14 In all, 626 (48.3%) of the participants strongly agreed that COVID-19 causes more deaths than other respiratory diseases, which was relatively consistent with the finding that another study conducted in Ethiopia found more than half (53.4%) of respondents agreed that COVID-19 causes more deaths than other respiratory diseases. 14
Furthermore, more than 1067 (2.3%) of the respondents perceived that adults were more at risk than others, while 41.7% of the participants believed that children aged <5 years were more at risk than others. However, another study conducted in Ethiopia reported that 149 (45.1%) of the respondents perceived that children were at moderate risk of COVID-19 and 578 (62.2%) of respondents perceived that youth are at a moderate risk of COVID-19 respectively. 22
The study also found that 1051 (81.17%) of respondents believed that they would contract COVID-19, which was higher than the finding of another study conducted in Nigeria, which found that 89 (26.0%) of respondents reported that they could contract COVID-19. 23 Furthermore, the current study found 651 (50.2%) of respondents who believed that they would contract COVID-19, which was higher than the finding of another study conducted in India which reported that 16.3% of the respondents perceived that they were at risk of contracting COVID-19. 24 The variation may be related to the misunderstanding or rumors in the community regarding COVID-19.
Furthermore, the current study found 76.3% of respondents got information about COVID-19 from the TV, which was in line with the findings of another study conducted in Ethiopia which found that 81.0% of respondents reported TV to be a source of COVID-19-related information. However, another study conducted in Malawi reported radio and conversations with friends as the most common sources of COVID-19-related information. 25
The prevalence of healthcare-seeking behavior in the current study is consistent with the previous findings reported in Brazil (33.6%), 20 Bangladesh (35.1%), 26 and China (35.4%). 27 However, the result of the current study is lower than the findings reported in Hubei, China (85.7%), 28 Iran (75.2%), 29 United Kingdom (64.3%), 30 and Egypt (60%). 31 The possible explanation may be due to the differences in the communication platform to inform the people about where to go if they developed the symptoms and institutional trust among the study participants. Better information access may enhance participants’ decision making, which in turn positively affects their healthcare-seeking behaviors. 23
On the contrary, the current study shows an association of risk perception with some sociodemographic variables (age and educational status). That is, respondents who had no formal education were 1.9 times more likely to have low-risk perceptions compared with those respondents having college and above educational status. This may be due to access to false information and rumors from various social medias that may lead to low-risk perception in the community. The result of the current study agreed with the findings of other studies conducted in India, which reported a statistical association between risk perception and age and educational status. 24 Similar to the current study, the study conducted in Iran 32 also reported a correlation between risk perception and knowledge of the respondents.
According to a study done in south Ethiopia, 14 risk perception was associated with age (β = 0.10; 95% CI: 0.02, 0.18) and knowledge of COVID-19 (β = 0.50, 95% CI: 0.23, 0.76), which was in line with the finding of the current study which found a statistically significant association between age (ranged from AOR; 0.64 to 1.81) and knowledge of the respondents (AOR: 0.50). Respondents aged 36–45 years are 0.64 times less likely to have low-risk perceptions compared with those aged >45 years. Overall, the study found low-risk perception among the community and various determinant factors related to COVID-19. Thus, the local and federal governments should take appropriate measures such as giving health education to increase positive attitudes, to increase community risk perception. The limitation of this study is that it might not indicate a cause–effect relationship because the study design was cross-sectional. Due to the nature of this study design, we cannot assess how risk perceptions change over time. Also, there might be the risk of social desirability bias since individual behaviors have public health implications and the data were collected through self-reports.
Conclusion
In general, the current study found that about half (50.6%) of the respondents had low-risk perceptions concerning COVID-19 and significant differences in risk perception among different ages, educational statuses, and knowledge of the respondents. Thus, it is necessary to improve community risk perception to manage the COVID-19 pandemic.
Supplemental Material
Supplemental material, sj-pdf-1-smo-10.1177_20503121211036132 for Community risk perception and health-seeking behavior in the era of COVID-19 among adult residents of Harari regional state, eastern Ethiopia by Addis Eyeberu, Dechasa Adare Mengistu, Belay Negash, Addisu Alemu, Degu Abate, Temam Beshir Raru, Alemayehu Deressa Wayessa, Adera Debela, Nebiyu Bahiru, Helina Heluf, Mohammed Abdurke Kure, Ahmedmenewer Abdu, Amanuel Oljira Dulo, Habtamu Bekele, Kefelegn Bayu, Saron Bogale, Genanaw Atnafe, Tewodros Assefa, Rabuma Belete, Mohammed Muzeyin, Haftu Asmerom, Mesay Arkew, Anumein Mohammed, Henock Asfaw, Barkot Taddesse, Daniel Alemu, Dawit Yihun, Shambel Nigussie Amare, Jemal Yusuf Kebira, Siraj Aliyi Adem, Gebisa Dirirsa, Saba Hailu Girmay, Abduro Godana, Deribe Bekele Dechasa and Yadeta Dessie in SAGE Open Medicine
Acknowledgments
The authors extend their deepest thanks to Haramaya University, College of Health and Medical Science staff for providing their constructive support.
Footnotes
Author contributions: A.E. conceived the idea and contributed to data analysis. D.A.M., B.N., T.B.R., A.D.W., A.D., N.B., H.H., M.A.K., A.A., A.O.D., H.B., K.B., S.B., G.A., T.A., and R.B. contributed to the data review and data analysis. D.A.M., M.M., H.A., M.A., A.M., H.A., B.T., D.A., D.Y., S.N.A., J.Y.K., S.A.A., G.D., S.A.G., A.G., and D.B.D. contributed to drafting or writing, and editing the article. A.E., D.A.M., D.A., A.A., and Y.D. contributed to writing, editing, and critically revising the article. All co-authors contributed to data analysis and drafting. Finally, all authors read and approved the final version of the article to be published and agreed on all aspects of this work.
Availability of data and materials: Almost all data are included in this study. However, additional data will be available from the corresponding author on reasonable request.
Declaration of conflicting interests: The author(s) declared no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Ethical approval: Ethical approval for this study was obtained from the Institutional Health Research Ethics Review Committee (IHRERC) of College of Health and Medical Sciences of Haramaya University (protocol number: IHRERC/015/2021).
Funding: The author(s) received no financial support for the research, authorship, and/or publication of this article.
Informed consent: Written informed consent was obtained from legally authorized representatives before the study. Written informed consent was obtained from all subjects before the study.
ORCID iDs: Addis Eyeberu  https://orcid.org/0000-0002-3147-3770
https://orcid.org/0000-0002-3147-3770
Dechasa Adare Mengistu  https://orcid.org/0000-0002-0076-5586
https://orcid.org/0000-0002-0076-5586
Ahmedmenewer Abdu  https://orcid.org/0000-0002-0477-2206
https://orcid.org/0000-0002-0477-2206
Habtamu Bekele  https://orcid.org/0000-0001-9839-1908
https://orcid.org/0000-0001-9839-1908
Mohammed Muzeyin  https://orcid.org/0000-0003-1492-7512
https://orcid.org/0000-0003-1492-7512
Supplemental material: Supplemental material for this article is available online.
References
- 1. Wang J, Sato T, Sakuraba A. Coronavirus disease 2019 (COVID-19) meets obesity: strong association between the global overweight population and COVID-19 mortality. J Nutr 2021; 151(1): 9–10. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Wu F, Zhao S, Yu B, et al. A new coronavirus associated with human respiratory disease in China. Nature 2020; 580(7803): E7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Shi Y, Wang G, Cai XP, et al. An overview of COVID-19. J Zhejiang Univ Sci B 2020; 21: 343–360. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. World Health Organization. WHO coronavirus disease (COVID-19) dashboard, 2020, https://www.who.int/
- 5. Rodriguez-Morales AJ, Cardona-Ospina JA, Gutiérrez-Ocampo E, et al. Clinical, laboratory and imaging features of COVID-19: a systematic review and meta-analysis. Travel Med Infect Dis 2020; 34: 101623. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Worldometer. Real time world statistics, https://www.worldometers.info/
- 7. Asnakew Z, Asrese K, Andualem M. Community risk perception and compliance with preventive measures for COVID-19 pandemic in Ethiopia. Risk Manag Healthc Policy 2020; 13: 2887–2897. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8. EPHI. Status update on COVID19 Ethiopia February 16, 2021, http://www.covid19.ephi.gov.et/status-update-on-covid19-ethiopia-february-16-2021/
- 9. Deressa W, Worku A, Amogne W, et al. Knowledge and perceptions of COVID-19 among government employees in Ethiopia, 2020, pp. 1–31, https://www.medrxiv.org/content/10.1101/2020.11.12.20230615v1.full.pdf
- 10. Deressa W, Worku A, Abebe W, et al. Risk perceptions and preventive practices of COVID-19 among healthcare professionals in public hospitals in Ethiopia, 2020, pp. 1–33, https://www.medrxiv.org/content/medrxiv/early/2020/11/03/2020.10.30.20223180.full.pdf [DOI] [PMC free article] [PubMed]
- 11. Cvetković VM, Nikolić N, Radovanović Nenadić U, et al. Preparedness and preventive behaviors for a pandemic disaster caused by COVID-19 in Serbia. Int J Environ Res Public Health 2020; 17(11): 4124. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Vai B, Cazzetta S, Ghiglino D, et al. Risk perception and media in shaping protective behaviors: insights from the early phase of COVID-19 Italian outbreak. Front Psychol 2020; 11: 563426. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. De Wilton A, Kilich E, Chaudhry Z, et al. Delayed healthcare seeking and prolonged illness in healthcare workers during the COVID-19 pandemic: a single-centre observational study. BMJ Open 2020; 10(11): e040216. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14. Asefa A, Qanche Q, Hailemariam S, et al. Risk perception towards COVID-19 and its associated factors among waiters in selected towns of southwest Ethiopia. Risk Manag Healthc Policy 2020; 13: 2601–2610. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. UNICEF. RCCE action plan guidance: COVID-19 preparedness and response, 2019, https://www.unicef.org/media/65936/file/Preparedness
- 16. Azene ZN, Merid MW, Muluneh AG, et al. Adherence towards COVID-19 mitigation measures and its associated factors among Gondar city residents: a community-based cross-sectional study in northwest Ethiopia. PLoS ONE 2020; 15(12): e0244265. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17. Fetansa G, Etana B, Tolossa T, et al. Knowledge, attitude, and practice of health professionals in Ethiopia toward COVID-19 prevention at early phase. SAGE Open Med 2021; 9: 1–9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Wolff K, Larsen S, Øgaard T. How to define and measure risk perceptions. Ann Tour Res 2019; 79: 102759. [Google Scholar]
- 19. Iorfa SK, Ottu IF, Oguntayo R, et al. COVID-19 knowledge, risk perception, and precautionary behavior among Nigerians: a moderated mediation approach. Front Psychol 2020; 11: 566773. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20. Macinko J, Woolley NO, Seixas BV, et al. Health care seeking due to COVID-19 related symptoms and health care cancellations among older Brazilian adults: the ELSI-COVID-19 initiative. Cad Saude Publica 2020; 36(Suppl. 3): e00181920. [DOI] [PubMed] [Google Scholar]
- 21. Ning L, Niu J, Bi X, et al. The impacts of knowledge, risk perception, emotion and information on citizens’ protective behaviors during the outbreak of COVID-19: a cross-sectional study in China. BMC Public Health 2020; 20: 1751. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22. Kebede Y, Birhanu Z, Fufa D, et al. Myths, beliefs, and perceptions about COVID-19 in Ethiopia: a need to address information gaps and enable combating efforts. PLoS ONE 2020; 15(11): e0243024. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23. Ilesanmi O, Afolabi A. Perception and practices during the COVID-19 pandemic in an urban community in Nigeria: a cross-sectional study. PeerJ 2020; 8: e10038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24. Kuang J, Ashraf S, Das U, et al. Awareness, risk perception, and stress during the COVID-19 pandemic in communities of Tamil Nadu, India. Int J Environ Res Public Health 2020; 17(19): 7177. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25. Banda J, Dube AN, Brumfield S, et al. Knowledge, risk perceptions, and behaviors related to the COVID-19 pandemic in Malawi. Demogr Res 2021; 44: 459–480. [Google Scholar]
- 26. Lopez-Pena P, Davis CA, Mobarak AM, et al. Prevalence of COVID-19 symptoms, risk factors, and health behaviors in host and refugee communities in Cox’s Bazar: a representative panel study. Bull World Health Organ 2020, https://www.who.int/bulletin/online_first/20-265173.pdf
- 27. Yang J, Gong H, Chen X, et al. Health-seeking behaviors of patients with acute respiratory infections during the outbreak of novel coronavirus disease 2019 in Wuhan, China. Influenza Other Respir Viruses 2021; 15: 188–194. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28. Wong LP, Wu QH, Chen X, et al. The role of institutional trust in preventive and treatment-seeking behaviors during the 2019 novel coronavirus (2019-nCoV) outbreak among residents in Hubei, China, 2020, https://www.medrxiv.org/content/10.1101/2020.02.15.20023333v1.full.pdf [DOI] [PMC free article] [PubMed]
- 29. Kakemam E, Ghoddoosi-Nejad D, Chegini Z, et al. Knowledge, attitudes, and practices among the general population during COVID-19 outbreak in Iran: a national cross-sectional online survey. Front Public Health 2020; 8: 585302. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30. Geldsetzer P. Knowledge and perceptions of COVID-19 among the general public in the United States and the United Kingdom: a cross-sectional online survey. Ann Intern Med 2020; 173(2): 157–160. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31. Abdelhafiz AS, Mohammed Z, Ibrahim ME, et al. Knowledge, perceptions, and attitude of Egyptians towards the novel coronavirus disease (COVID-19). J Community Health 2020; 45(5): 881–890. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Honarvar B, Lankarani KB, Kharmandar A, et al. Knowledge, attitudes, risk perceptions, and practices of adults toward COVID-19: a population and field-based study from Iran. Int J Public Health 2020; 65(6): 731–739. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Supplemental material, sj-pdf-1-smo-10.1177_20503121211036132 for Community risk perception and health-seeking behavior in the era of COVID-19 among adult residents of Harari regional state, eastern Ethiopia by Addis Eyeberu, Dechasa Adare Mengistu, Belay Negash, Addisu Alemu, Degu Abate, Temam Beshir Raru, Alemayehu Deressa Wayessa, Adera Debela, Nebiyu Bahiru, Helina Heluf, Mohammed Abdurke Kure, Ahmedmenewer Abdu, Amanuel Oljira Dulo, Habtamu Bekele, Kefelegn Bayu, Saron Bogale, Genanaw Atnafe, Tewodros Assefa, Rabuma Belete, Mohammed Muzeyin, Haftu Asmerom, Mesay Arkew, Anumein Mohammed, Henock Asfaw, Barkot Taddesse, Daniel Alemu, Dawit Yihun, Shambel Nigussie Amare, Jemal Yusuf Kebira, Siraj Aliyi Adem, Gebisa Dirirsa, Saba Hailu Girmay, Abduro Godana, Deribe Bekele Dechasa and Yadeta Dessie in SAGE Open Medicine