Abstract
Background
Universal coverage with long-lasting insecticidal nets (LLINs) is an essential component of malaria control programmes. Three-yearly mass distribution of LLINs in Papua New Guinea (PNG) has been successful in reducing infection transmission since 2009, but malaria prevalence ramped up from 2015 onwards. Although LLIN universal coverage is mostly achieved during these campaigns, it may not be related with net use over time. Uses given to LLINs and non-compliance of this strategy were evaluated.
Methods
A knowledge, attitude and practice (KAP) cross-sectional study was conducted in Lihir Islands, PNG, 2–2.5 years after the last LLIN mass distribution campaign. Data on bed net ownership, use and maintenance behaviour was collected using a household questionnaire administered by trained community volunteers. Logistic regression models were used to identify factors associated with owning at least one LLIN and sleeping under a LLIN the previous night.
Results
Among 2694 households surveyed, 27.4 % (95 % CI: 25.8–29.2) owned at least one LLIN and 8.7 % (95 % CI: 7.6–9.8) had an adequate LLIN coverage (at least one LLIN for every two people). Out of 13,595 individuals in the surveyed households, 13.6 % (95 % CI: 13.0-–4.2) reported having slept under a LLIN the preceding night. Determinants for sleeping under LLIN included living in a household with adequate LLIN coverage [adjusted OR (aOR) = 5.82 (95 % CI: 3.23–10.49)], household heads knowledge about LLINs [aOR = 16.44 (95 % CI: 8.29–32.58)], and female gender [aOR = 1.92 (95 % CI: 1.53–2.40)] (all p-values < 0.001). LLIN use decreased with older age [aOR = 0.29 (95 % CI: 0.21–0.40) for ≥ 15 year-olds, aOR = 0.38 (95 % CI: 0.27–0.55) for 5–14 year-olds] compared to < 5 year-olds (p-value < 0.001). Knowledge on the use of LLIN was good in 37.0 % of the household heads. Repurposed nets were reported serving as fishing nets (30.4 %), fruits and seedlings protection (26.6 %), covering up food (19.0 %) and bed linen (11.5 %).
Conclusions
Two years after mass distribution, LLIN coverage and use in Lihir Islands is extremely low. Three yearly distribution campaigns may not suffice to maintain an acceptable LLIN coverage unless knowledge on maintenance and use is promoted trough educational campaigns.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12936-021-03867-z.
Keywords: Bed net, Coverage, Long-lasting insecticidal net, LLIN, Malaria, Papua New Guinea, Repurposing, Vector control
Background
Universal coverage with insecticide-treated mosquito nets (ITNs) is recommended to achieve community-wide protection in malaria endemic areas [1]. In the last 3 years, more than 500 million ITNs have been distributed worldwide and undoubtedly contributed to malaria control efforts. However, coverage, maintenance and use of ITNs is heterogeneous and nets are sometimes misused or repurposed, reducing the efficiency of the overall strategy [2–4].
Long-lasting insecticidal nets (LLINs) have been massively distributed in Papua New Guinea (PNG) since 2004. Regular mass distribution campaigns were initiated in 2009 and are repeated every three years. According to a nationwide survey conducted in 2011 during the second mass distribution, 81.8 % of households retained at least one LLIN from the previous campaign [5]. Overall human malaria prevalence decreased from 15.7 % to 2009 to 4.8 % in 2011, although the reduction was more pronounced for Plasmodium falciparum than for Plasmodium vivax [6]. Moreover, a study conducted in selected sites in PNG, showed a steep decrease in malaria annual incidence: from 20 to 115 cases per 1000 population in 2010, to 1–79 cases per 1000 in 2014. This effect was attributed to LLIN mass coverage and use, rather than to the widespread use of highly effective artemisinin-based combination therapy [7]. Despite the initial success, PNG experienced a large increase of infections in the latest years, with an incidence that ramped up from 118.8 cases per 1000 inhabitants in 2015 to 184.5 cases per 1000 inhabitants in 2018 [8]. Consequently, in 2019, PNG accounted for 80 % of all malaria cases diagnosed in the Western Pacific Region [2, 9].
In view of the established efficacy of LLINs as a malaria control intervention, it is unclear why there was not more of an effect. There are several potential reasons, including insecticide resistance, vector behaviour change, incomplete campaign coverage and non-compliance to LLIN. Anopheles spp phenotypic resistance to pyrethroids, the insecticides commonly used in LLIN, is not yet present in PNG [10], ruling out a contribution of insecticide resistance to the changes observed in malaria epidemiology. In contrast, decreased bioefficacy of LLINs distributed between 2013 and 2019 has been described [11], as well as behavioural adaptation of local malaria vectors towards more frequent outdoor biting earlier in the evening [12, 13]. Lack of use, misuse or repurposing of LLINs may as well be related to the reduced efficacy of this particular malaria control strategy. Studies conducted in different countries have reported that repurposed nets served as fishing nets, gardening, or fencing [3, 4, 14–16]. The main reason for the lack of appropriate use and maintenance of LLIN are dislike and discomfort due to heat and perceived low mosquito density [15, 17, 18].
In this study LLIN ownership, maintenance and use in Lihir Islands were evaluated, two years after the 2016 mass distribution when 10,897 nets were issued and 97 % of individual coverage was achieved [19]. Misuse and misconception of villagers were also assessed as factors that may influence the effectiveness and sustainability of this vector control strategy over time.
Methods
Study setting
This study was conducted in Lihir Islands, located in the Bismarck archipelago, in New Ireland Province, PNG. New Ireland is among the PNG provinces experiencing a higher increase in malaria cases since 2015, with 426 cases per 1000 population in 2018 [20], although in previous years the province had achieved a reduction in cases comparable to other parts of the country [21, 22]. In addition, New Ireland is one of the provinces with lowest LLIN use despite high LLIN coverage according to a national indicator survey conducted in 2017 [23]. During the 2016 mass distribution campaign, 90,948 double nets were distributed by the national program in collaboration with Rotarians Against Malaria PNG (RAM), achieving a coverage ratio of 49 double-size LLINs per 100 population (97 % population coverage) [19].
Lihir islands is a group of four small islands: Aniolam (the largest, with an area of 200 km2), and the smaller outer islands of Malie, Masahet, and Mahur. They are characterised by a tropical rainforest climate with extremely high precipitation figures all year round. There are 8 aid posts, 1 subhealth centre and 2 health centres in the islands. A gold mine located in Aniolam is the main source of employment. Employee migration from other parts of PNG, contributes to more than one third of the population on Aniolam [24]. In 2019, Lihir had a population of approximately 27,500 inhabitants and 6000 households [25]. Households can be permanent (built of bricks, with solid material in the roof and windows with glass), traditional (built of natural materials, especially wood and grass, with open windows) or makeshift (usually made with different kinds of materials from settlement areas, such as cardboard). Malaria is one of the main health issues in Lihir islands. In 2018, 11,267 confirmed malaria cases were reported (annual incidence of 478 cases per 1000 inhabitants) with minimal variation in number of cases per month.
Study design and procedures
A knowledge, attitude and practice (KAP) cross-sectional household survey was conducted between the 3rd of December of 2018 and the 25th of May of 2019 to assess ownership and use of LLIN distributed during 2016, before the following mass distribution campaign scheduled for late 2019.
The data collection was implemented by community volunteers, called Village Malaria Assistants (VMAs). They were selected by community leaders, and trained to implement malaria control activities at the village level, mainly awareness and education on malaria prevention, health-seeking behaviour and compliance with treatment. The VMA network in Lihir islands was established in 2018, after all VMAs were trained. A total of 40 VMAs worked in this study and were instructed to survey all households in their village or catchment area.
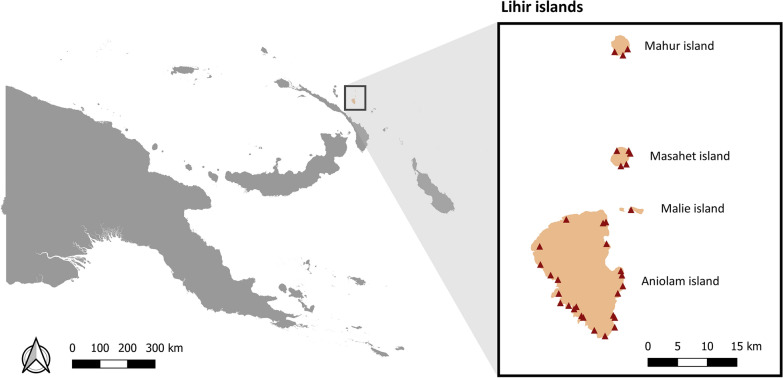
The survey was conducted in a convenient sample of 33 villages out of 40 located in the four islands of the Lihir group (see Fig. 1). Although the goal was set to survey all households in Lihir islands, reaching all households was not possible due to logistical constraints; hence, households were also selected using convenience sampling. A total of 2694 households were enrolled in the survey, which represents approximately half of the households on the Lihir islands [25].
Fig. 1.
Map of the surveyed villages in the Lihir islands, New Ireland province, Papua New Guinea
Data collection and management
Interviews were conducted using structured questionnaires to household heads or, in its absence, to the partner or an adult permanently living in the house. A household was excluded from the study if the head of the household was not willing to participate or if no adults were available to answer the questionnaire after two separate visits.
Interviews included questions on household characteristics, demographic information of all household members (residents and long-term visitors sleeping in the same house), LLIN ownership, individual correct use of LLINs, alternative uses given to the nets, and behavioural questions related to malaria prevention. VMAs were instructed to enter the surveyed house to check the number of reported nets. Strategies to prevent malaria and alternative uses given to LLINs were asked with an open question, and household heads were prompt to list as many options as they considered relevant. After the questionnaires were collected, data were introduced into a database by two independent data clerks. See data collection tool in supplementary material, Additional file 1.
Statistical analysis
A sample size of 379 households was estimated to detect an unknown prevalence (50 %) of having at least 1 LLIN (conservative estimate with maximum imprecision), with a margin of error of ± 5 % and a confidence level of 95 %.
Basic characteristics of participating households and individuals were summarized using descriptive analyses. Different indicators of LLIN ownership and use were calculated following the recommendations of the Roll Back Malaria Monitoring and Evaluation Reference Group [26], including: (i) proportion of households with at least one LLIN, (ii) proportion of households with at least one LLIN for every two people, (iii) proportion of population with adequate access (≥ 1 LLIN/2 individuals) to a LLIN in their household, (iv) proportion of the population that slept under a LLIN the previous night, and (v) proportion of children under five years of age who slept under a LLIN the previous night. Formulae used are shown in supplementary material, Additional file 2. Knowledge of malaria prevention tools and alternative uses given to LLIN revealed by the head of the household were reported using descriptive analyses.
Univariable and multivariable logistic regression analyses were used to identify factors associated with maintaining at least one LLIN in the household. Both models were adjusted for village as a fixed effect parameter. Similarly, univariable and multivariable mixed-effects logistic regression analyses were used to identify factors associated with sleeping under a LLIN the previous night among individuals living in a household with at least one LLIN. These two models were adjusted for household and village as random effects parameters. We have considered village as a fixed effect in the first models and random effect in the second type of models following the recommendations of Green and Tukey [27]. Analysis results are presented as odds ratios (ORs) with 95 % confidence intervals (CIs). The strength of the evidence for the different associations was calculated using likelihood-ratio tests.
Data were analysed using Stata 16 software [28]. All graphs were drawn using Stata 16 software, and a map of the surveyed villages was created using QGIS Desktop v3.16 Hannover software [29].
Ethical considerations
The research protocol was approved by the PNG Medical Research Advisory Committee (MRAC No. 18.07). Permission to conduct this survey was also obtained from village leaders. All household heads orally consented before recording data of each household. No biological samples were collected.
Results
Study population
A total of 2694 households, with 13,595 individuals, were visited and enrolled in the survey. Characteristics of participating households and their residents are described in Table 1. Half of the houses (50.1 %) were permanent, 39.7 % were traditional, and 10.2 % were makeshift. The median number of people per household was 5 (interquartile range [IQR]: 3–7), and a large proportion of the household heads were male (76.6 %). Approximately half of the individuals living in the surveyed households were male (51.9 %), and 62.4 % of the population were aged 15 years and older. Most school-age children attended a local school (78.0 %), and only 22.6 % of the adults were employed.
Table 1.
Household and study population characteristics
| Variable | N (%) |
|---|---|
| Household characteristics (n = 2694) | |
| Type of household | |
| Permanent | 1349 (50.1) |
| Traditional | 1069 (39.7) |
| Makeshift | 276 (10.2) |
| Number of individuals per household | |
| Median (IQR) | 5 (3–7) |
| Sex of the household head | |
| Male | 2063 (76.6) |
| Female | 631 (23.4) |
| Individual chracteristics (n = 13,595) | |
| Gendera | |
| Male | 7056 (51.9) |
| Female | 6537 (48.1) |
| Age [years]b | |
| < 5 | 2088 (15.5) |
| 5–14 | 2979 (22.1) |
| ≥ 15 | 8432 (62.4) |
| Employed [if ≥ 15 years old]c | |
| No | 5411 (77.4) |
| Yes | 1584 (22.6) |
| Studying [if 5–14 years old]d | |
| No | 639 (22.0) |
| Yes | 2267 (78.0) |
an = 13,593 (0.01 % missing)
bn = 13,499 (0.7 % missing)
cn = 6995 (17.0 % missing)
dn = 2906 (2.5 % missing)
LLIN ownership and use
Among the 2694 households responding the survey, 27.4 % (95 % CI: 25.8–29.2) owned at least one LLIN, 2–2.5 years after the mass distribution that took place in the islands. A total of 416 households had one LLIN, 117 had two LLINs, 183 had three LLINs, and 23 had four or more LLINs. Only 8.7 % (95 % CI: 7.6–9.8) of households had at least one LLIN for every two individuals (adequate household coverage). Similarly, the percentage of people with adequate access to a LLIN within their household was estimated to be 6.7 % (95 % CI: 6.2–7.1).
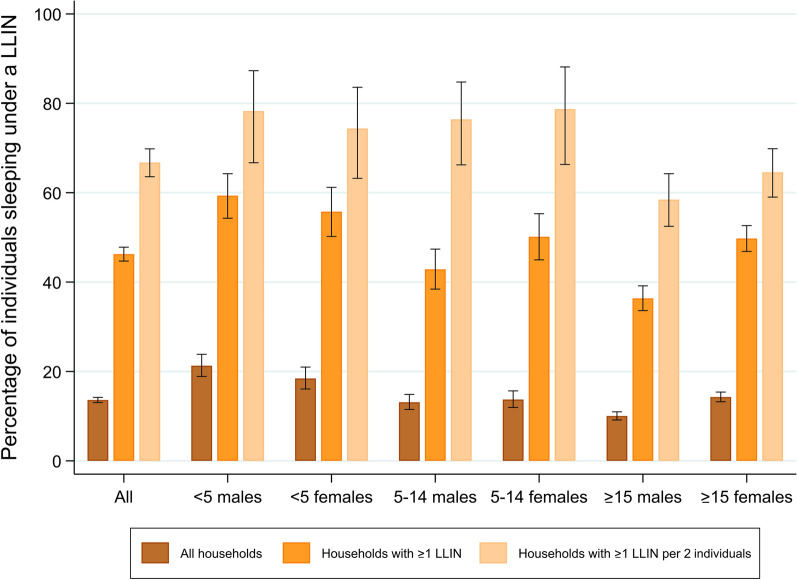
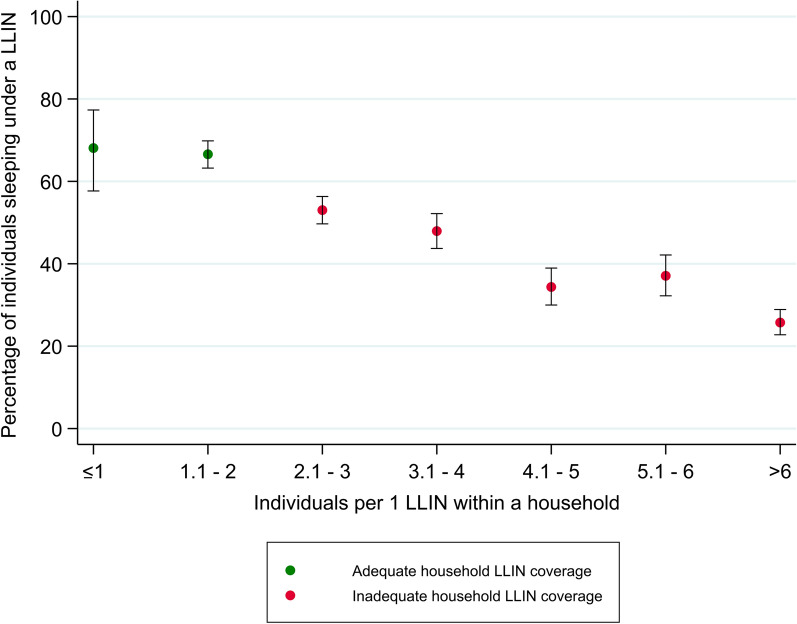
Regarding LLIN use, a total of 1851 individuals [13.6 % (95 % CI: 13.0–14.2)] reported to have slept under a LLIN the previous night. Among individuals living in a household with at least one LLIN, a 46.3 % (95 % CI: 44.7–47.8) slept under a LLIN the previous night. Among individuals living in a household with adequate LLIN coverage, a 66.7 % (95 % CI: 63.6–69.8) did so. A detailed breakdown of individuals using LLIN by age and sex according to household LLIN coverage is shown in Fig. 2. Among the key population of children under five years of age, 19.9 % (95 % CI: 18.2–21.7) reported to have slept under a LLIN the previous night. The percentage of individuals reporting to have slept under a LLIN increased with LLIN availability within a household (Fig. 3).
Fig. 2.
Percentage of individuals reported to sleep under a LLIN the previous night by sex and age groups, among (1) all households, (2) households that have at least 1 LLIN, and (3) households with at least 1 LLIN per 2 individuals
Fig. 3.
Percentage of individuals reported to sleep under a LLIN the previous night by the ratio individuals:LLIN of the household, among the 739 households with at least 1 LLIN
Determinants of owning at least one LLIN
Factors associated with LLIN ownership are shown in Table 2. In the multivariable analysis, owning at least one LLIN was associated with having at least one resident aged < 5 years-old [adjusted OR (aOR) = 1.55 (95 % CI: 1.17–2.06), p-value = 0.002], having at least one resident being an adult woman [aOR = 1.82 (95 % CI: 1.04–3.16), p-value = 0.029], and with the head of the household knowing that sleeping under a LLIN prevents malaria [aOR = 30.32 (95 % CI: 21.25–43.27), p-value < 0.001].
Table. 2.
Factors associated with household ownership of at least one LLIN (n = 2694 households)
| Variable | Total households | Owning ≥ 1 LLIN (%) | Univariable aOR (95 %CI) |
p-value | Multivariable aOR (95 %CI) |
p-value |
|---|---|---|---|---|---|---|
| Type of household | ||||||
| Permanent | 1349 | 360 (26.7) | 1 | 0.099 | 1 | 0.405 |
| Traditional | 1069 | 289 (27.0) | 0.91 (0.74–1.13) | 0.90 (0.67–1.21) | ||
| Makeshift | 276 | 90 (32.6) | 1.34 (0.97–1.85) | 1.21 (0.79–1.86) | ||
| Number of individuals per household | ||||||
| Median (IQR) | 5 (3–7) | 5 (4–7) | 1.07 (1.03–1.12) | 0.001 | 1.02 (0.96–1.09) | 0.529 |
| Household head knows that sleeping under a LLIN prevents malaria | ||||||
| No | 1697 | 117 (10.4) | 1 | < 0.001 | 1 | < 0.001 |
| Yes | 997 | 562 (56.4) | 24.08 (17.96–32.30) | 30.32 (21.25–43.27) | ||
| Gender of the household head | ||||||
| Male | 2063 | 555 (26.9) | 1 | 0.690 | 1 | 0.908 |
| Female | 631 | 184 (29.2) | 1.05(0.83–1.32) | 0.98 (0.71–1.35) | ||
| At least 1 resident aged < 5 yearsa | ||||||
| No | 1320 | 288 (21.8) | 1 | < 0.001 | 1 | 0.002 |
| Yes | 1347 | 443 (32.9) | 1.70 (1.39–2.06) | 1.55 (1.17–2.06) | ||
| At least 1 resident an adult woman [> 15 years old] | ||||||
| No | 241 | 38 (15.8) | 1 | < 0.001 | 1 | 0.029 |
| Yes | 2453 | 701 (28.6) | 2.35 (1.56–3.53) | 1.82 (1.04–3.16) | ||
| At least 1 resident employed [> 15 years old]b | ||||||
| No | 1129 | 268 (23.7) | 1 | 0.022 | 1 | 0.579 |
| Yes | 1122 | 340 (30.3) | 1.29 (1.04–1.61) | 1.08 (0.82–1.43) | ||
| At least 1 resident studying [5–14 years old]c | ||||||
| No | 1342 | 334 (24.9) | 1 | 0.108 | 1 | 0.167 |
| Yes | 1315 | 391 (29.7) | 1.17 (0.97–1.43) | 0.81 (0.61–1.09) | ||
an = 2667 (1.0 % missing)
bn = 2251 (16.4 % missing)
cn = 2657 (1.4 % missing)
Determinants of sleeping under LLIN
Out of 4,002 individuals that lived in a household with at least one LLIN, 46.3 % (95 % CI: 44.7–47.8) reported sleeping under a LLIN the preceding night. Table 3 shows the factors associated with LLIN use. In the multivariable analysis, sleeping under a LLIN the previous night was associated with living in a household with adequate LLIN coverage [adjusted OR (aOR) = 5.82 (95 % CI: 3.23–10.49)], head of household knowing that sleeping under a LLIN prevents from malaria [aOR = 16.44 (95 % CI: 8.29–32.58)], being female [aOR = 1.92 (95 % CI: 1.53–2.40)] and decreasing age [aOR = 0.38 (95 % CI: 0.27–0.55) for 5–14 year-olds, and aOR = 0.29 (95 % CI: 0.21–0.40) for ≥ 15 year-olds, compared both to < 5 year-olds] (all p-values < 0.001).
Table 3.
Factors associated with sleeping under a LLIN among individuals residing in households owning at least one LLIN (n = 4002 individuals)
| Variable | Total individuals | Slept under a LLIN the previous night (%) | Univariable aOR (95 %CI) |
p-value | Multivariable aOR (95 %CI) |
p-value |
|---|---|---|---|---|---|---|
| Gender | ||||||
| Male | 2093 | 879 (42.0) | 1 | < 0.001 | 1 | < 0.001 |
| Female | 1909 | 972 (50.9) | 1.99 (1.64–2.41) | 1.92 (1.53–2.40) | ||
| Age [years]a | ||||||
| < 5 | 721 | 416 (57.7) | 1 | < 0.001 | 1 | < 0.001 |
| 5–14 | 867 | 399 (46.0) | 0.37 (0.27–0.51) | 0.38 (0.27–0.55) | ||
| ≥ 15 | 2373 | 1021 (43.0) | 0.32 (0.24–0.41) | 0.29 (0.21–0.40) | ||
| Type of household | ||||||
| Permanent | 2168 | 917 (42.3) | 1 | 0.021 | 1 | 0.200 |
| Traditional | 1402 | 738 (52.6) | 2.08 (1.26–3.42) | 1.44 (0.82–2.52) | ||
| Makeshift | 432 | 196 (45.4) | 0.99 (0.47–2.06) | 0.66 (0.29–1.53) | ||
| Household LLIN coverage | ||||||
| Inadequate (< 1 LLIN per 2 individuals) | 3097 | 1247 (40.3) | 1 | < 0.001 | 1 | < 0.001 |
| Adequate (≥ 1 LLIN per 2 individuals) | 905 | 604 (66.7) | 6.61 (3.99–10.96) | 5.82 (3.23–10.49) | ||
| Household head knows that sleeping under a LLIN prevents malaria | ||||||
| No | 982 | 211 (21.5) | 1 | < 0.001 | 1 | < 0.001 |
| Yes | 3020 | 1640 (54.3) | 20.84 (11.48–37.85) | 16.44 (8.29–32.58) | ||
| Gender of the household head | ||||||
| Male | 3081 | 1443 (46.8) | 1 | 0.696 | 1 | 0.252 |
| Female | 921 | 408 (44.3) | 0.89 (0.52–1.53) | 0.68 (0.36–1.28) | ||
| At least 1 resident employed [> 15 years old]b | ||||||
| No | 1147 | 623 (54.3) | 1 | 0.028 | 1 | 0.082 |
| Yes | 2044 | 924 (45.2) | 0.54 (0.32–0.90) | 0.62 (0.37–1.04) | ||
| At least 1 resident studying [5–14 years old]c | ||||||
| No | 1399 | 695 (49.7) | 1 | 0.150 | 1 | 0.670 |
| Yes | 2528 | 1124 (44.5) | 0.70 (0.45–1.11) | 0.89 (0.53–1.49) | ||
an = 3961 (1.0 % missing)
bn = 3191 (20.3 %missing)
cn = 3927 (1.9 %missing)
Knowledge of malaria prevention tools
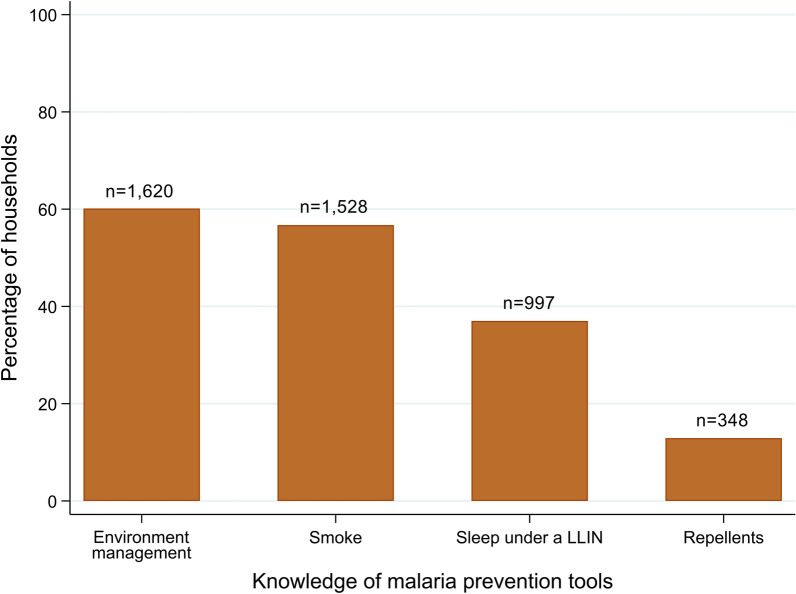
When the head of the household was asked about strategies to prevent malaria, 37.0 % (997/2694) responded that sleeping under a LLIN was effective to prevent malaria. Most of them (1620; 60.1 %) answered that strategies of environmental management are effective, including cleaning the house and removing water from gardens, and/or cleaning villages. Another frequent answer (1528; 56.7 %) was that creating smoke by burning bush material was useful to prevent malaria, while the use of mosquito repellents as a malaria prevention tool was pointed out by only 12.9 % of the household heads. Figure 4 shows the knowledge on malaria prevention tools by household heads.
Fig. 4.
Knowledge of malaria prevention tools reported by the household head (n = 2694 households)
Alternative uses of LLIN
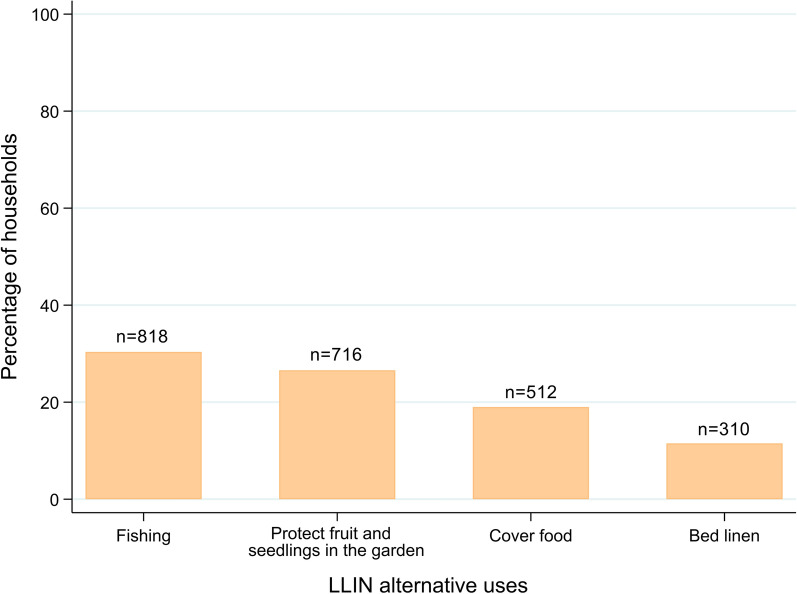
When asked about use of LLINs, a total of 1170 (43.4 %) household heads reported to have used LLINs only for the purpose of sleeping under. Many gave alternative uses (either misuse or repurposing) to the LLINs: 937 (34.8 %) households provided one alternative use, 401 (14.9 %) households provided two alternative uses, 127 (4.7 %) provided three, and 59 (2.2 %) provided four or more. The most common alternative use for LLINs was fishing (818; 30.4 %), followed by protecting fruits and seedlings in gardens (716, 26.6 %). Other uses given to the LLINs included covering food in the house (512, 19.0 %) and using them as bed linen (310, 11.5 %). Figure 5 shows the alternative uses given to the LLINs.
Fig. 5.
Alternative uses of LLIN reported by the household head (n = 2694 households)
Discussion
This study shows a very large reduction over time on the adequate LLIN coverage in Lihir Islands, decreasing from 97 % of individuals having access to LLIN after 2016 mass distribution [19] to less than 7 % in 2–2.5 years (one year prior to the next mass distribution campaign). This reduction in LLIN coverage is rather striking, and significantly different to the relatively high bed net coverage maintained in previous distributions campaigns in the country. As an example, a 2011 study in selected sites in PNG showed that 88.8 % of people still had access to LLIN in villages where the distribution had been conducted during the 2 years preceding the survey, whereas coverage decreased to 67.6 % in those villages where the distribution had been done more than 2 years before the survey [5]. Lack of LLIN maintenance is a common issue in other tropical areas: in Uganda, LLIN population coverage decreased from 65 to 18 % three years after distribution [30]; and in Tanzania, households with at least one LLIN for every two people were below 30 % two years after LLIN distribution [31]. Accordingly, only less than 14 % of the total population surveyed slept under LLIN the previous night; and adequate LLIN coverage was strongly associated with LLIN use as previously reported [5, 32], confirming the importance to achieve high coverage and maintenance to sustain LLIN use.
Interestingly, while adequate LLIN coverage in PNG has improved over time, especially in the islands’ region where Lihir Islands are located (increasing from 46 % to 2009 to 82 % in 2011), use of LLIN still remained poor: 25 % of individuals in this region reported sleeping under LLIN in 2009, which increased to only 40 % in 2011 despite the substantial improve in LLIN coverage [33]. In fact, the villages in the PNG islands’ region are those with better LLIN coverage but worse LLIN use [23]. Hence, achieving adequate LLIN coverage during mass distribution is clearly not sufficient to ensure their use. A qualitative study in PNG found that many environmental, human and nets factors could be linked to the impediments of the adequate use of nets; however, the most important factor that reduced the use was a lack of fear of malaria infection [34]. Promoting LLIN maintenance over time is also key to enhance their use and impact on malaria transmission. Mass LLIN distribution campaigns in PNG, similar as to many other countries, achieve a high coverage in the minimum time possible using strategies that are proven to work such as use of coupons or training of distributors [35]. Including additional strategies to target issues affecting long-term coverage could enhance maintenance and use of LLIN until the following mass distribution.
Households with at least one child under 5 years-old and households with at least one adult woman had a higher odds of owning at least one LLIN similar to other studies in PNG [33]. The scale up of antenatal services in the country, where pregnant women are targeted for prevention strategies and receive LLIN [36], has likely contributed to increase LLIN ownership in their households and probably enhanced maintenance. Antenatal services provide awareness on the importance of pregnant women and children below 5 years old to sleep under LLIN to prevent malaria. Interestingly, gender and age were associated with LLIN use, with women being more likely to sleep under LLIN as well as the younger members of the household.
However, the key factor for LLIN ownership and use was the head of the household’s knowledge about LLIN preventing from malaria infection. Only 37 % of the heads of the households reported that sleeping under a LLIN was effective to prevent malaria. These results suggest that education campaigns on malaria prevention tools targeting the heads of the households could further promote LLIN maintenance and use, as shown in previous studies [37]. Such education campaigns could be included as part of the mass LLIN distribution strategy, which could also look for the support of community leaders, pastors and other influential community members to deliver key awareness messages. In Lihir islands, the VMAs deployed an extensively education campaign at village and hamlet level during the LLIN distribution in 2019, targeting the heads of the households and involving community and church leaders. This intensive education campaign had not been conducted previously and it may have improved LLIN coverage, use and maintenance.
In addition, although an association between a household having at least one resident attending school and increased odds of owning one LLIN or sleeping under a LLIN was not shown, half of the households had at least one child between 5- and 14- years old attending school. Consequently, there is also a big opportunity to promote LLIN maintenance and use through frequent education campaigns in schools. In Tanzania, for example, nets were provided annually to children attending primary and secondary school, which resulted in high level of maintenance (50–75 % of nets given) over the first four years of distribution, even in the absence of a mass distribution campaign [38].
On the other hand, addressing alternative uses and repurposing of LLIN could also enhance maintenance and use. In this study, half of the surveyed households admitted using LLIN for alternative purposes. The study was unable to determine if LLIN used for alternative purposes were those provided in the distribution campaign in 2016 or those remaining from the 2013 campaign. However, since most households did not retain a single LLIN, it is likely that most nets used for other purposes were those given in 2016. The most common alternative use given to LLIN was fishing, which could be related to the low LLIN maintenance and use observed in the PNG islands’ region, among other factors. Another common alternative use was to protect seedlings and food. These common misuses have been also described in sub-Saharan Africa [4, 12–14] and all relate to basic needs like ensuring food supply. LLIN distribution using mass campaigns are proven to increase LLIN ownership [39–41]; however, especially when health education might not be sufficient to reduce alternative uses of LLIN when other basic needs are involved, some creative solutions could be used during mass LLIN distribution campaigns, such as facilitating access of target communities to suitable and without insecticide materials for fishing and gardening. In addition, ensuring high LLIN bioefficacy and teaching communities about the impact of LLIN in reducing mosquito population could further motivate communities to better maintain LLIN.
This study used a community approach that allowed a massive outreach to the Lihirian population but also had some limitations. Although the goal of VMAs was to survey their entire village or assigned part of a village, full coverage of all villages was not possible due to logistical constraints. Hence, it could be subjected to selection bias. However, all statistical models were adjusted for village in order to minimize bias arising from the non-representativeness of a few villages. In addition, our sample size was very large and spatio-geographically and demographically representative. Because data collection was conducted by the VMAs who are living in the same village, sensitive questions such as socioeconomic factors or enquiring about pregnancy status were avoided. These two pieces of information could have given important insight, such as LLIN use during pregnancy or the role of socioeconomic status contributing to repurposing of LLIN. It was observed that, while less than 7 % of individuals had adequate access to LLIN, close to 14 % were reported to sleep under them, which could be due to more than two individuals sharing a double net (as commonly seen for young children) and due to the social desirability bias inherent in self-reported measures. Finally, in order to maximize quality of the results, VMAs received an intensive training and close supervision, and data were carefully reviewed to recode impossible values and minimize missing values.
Conclusions
Although mass LLIN distribution campaigns are a proven health intervention to promote LLIN ownership and use, and reduce the malaria burden, distribution every three years does not seem to be sufficient to maintain an adequate LLIN coverage in the Lihir islands, PNG. Knowledge on malaria prevention tools by household heads is a determinant factor for retention and use of LLINs, as well as strategies targeting risk groups like pregnant women and children below 5 years of age. Thus, it is extremely important to ensure education of local communities in how to use and maintain the LLINs distributed to sustain the achieved high coverage during mass distribution for as long as possible and maximize impact for malaria control. Community approaches to gather information through trained community volunteers are useful to understand and deploy public health strategies. Lack of maintenance and use of LLIN, together with reduced LLIN bioefficacy and changes in mosquito biting behaviour, might altogether explain the recent increase in malaria cases observed in PNG.
Supplementary Information
Additional file 1: Data collection tool used by the village malaria assistants (VMA) tocollect information for this survey.
Additional file 2: Definitions of the LLIN ownership and use indicators, used for thedata analysis.
Acknowledgements
We acknowledge all the Lihirian communities for their acceptance and collaboration in this research. We acknowledge the Village Malaria Assistants that collaborated in the study for the outstanding work they are doing to reduce the burden of malaria in Lihir Islands. ISGlobal receives support from the Spanish Ministry of Science and Innovation through the “Centro de Excelencia Severo Ochoa 2019–2023” Program (CEX2018-000806-S), and support from the Generalitat de Catalunya through the CERCA Program. CISM is supported by the Government of Mozambique and the Spanish Agency for International Development (AECID). NB is supported by an FPU predoctoral fellowship from the Spanish Ministry of Universities (FPU18/04260). BB is a Beatriu de Pinós postdoctoral fellow granted by the Government of Catalonia’s Secretariat for Universities and Research, and by Marie Sklodowska-Curie Actions COFUND Programme (BP3, 801370).
Abbreviations
- aOR
Adjusted odds ratio
- CI
Confidence interval
- IQR
Interquartile range
- ITN
Insecticide-treated net
- KAP
Knowledge, attitude and practice
- LLIN
Long-lasting insecticidal nets
- OR
Odds ratio
- PNG
Papua New Guinea
- RAM
Rotarians Against Malaria
- VMA
Village malaria assistant
Authors’ contribution
PMM: conceptualization, methodology, supervision, data curation, writing-original draft; RG: conceptualization, methodology, supervision; NB: data curation, formal analysis, writing-review and editing; SL: methodology, supervision; SS: formal analysis; SR: investigation; AE: investigation; CW: investigation; BP: investigation; JD: investigation; ST: investigation; SK: conceptualization, methodology, writing-review and editing; ML: conceptualization, methodology, writing-review and editing; WP: conceptualization, methodology, writing-review and editing; OM: conceptualization, methodology, writing-review and editing; BB: Conceptualization, methodology, supervision, writing-review and editing, project administration; QB: Conceptualization, writing-review and editing, project administration. All authors read and approved the final manuscript.
Funding
This research project was funded by the Lihir Malaria Elimination Programme through its alliance between Medicines for Malaria Venture and Newcrest Mining Limited.
Availability of data and materials
The datasets used and analysed during the current study are available from the corresponding author on reasonable request.
Declarations
Ethics approval and consent to participate
Our research protocol was given ethics clearance at the PNG Medical Research Advisory Committee (MRAC No. 18.07). Permissions for this survey were also obtained from village leaders, and head of households orally consented before recording data of each household.
Consent for publication
This manuscript does not contain personal data from any individual person, hence the consent for publication is not applicable.
Competing interest
The authors declare that they have no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Pere Millat-Martínez and Rebecca Gabong contributed equally, and should share primary authorship
References
- 1.WHO . Guidelines for malaria vector control. Geneva: World Health Organization; 2019. [PubMed] [Google Scholar]
- 2.WHO . World malaria report 2019. Geneva: World Health Organization; 2019. [Google Scholar]
- 3.Minakawa N, Dida GO, Sonye GO, Futami K, Kaneko S. Unforeseen misuses of bed nets in fishing villages along Lake Victoria. Malar J. 2008;7:165. doi: 10.1186/1475-2875-7-165. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Dhiman S, Veer V. Culminating anti-malaria efforts at long lasting insecticidal net? J Infect Public Health. 2014;7:457–64. doi: 10.1016/j.jiph.2014.06.002. [DOI] [PubMed] [Google Scholar]
- 5.Hetzel MW, Choudhury AA, Pulford J, Ura Y, Whittaker M, Siba PM, et al. Progress in mosquito net coverage in Papua New Guinea. Malar J. 2014;13:242. doi: 10.1186/1475-2875-13-242. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Hetzel MW, Reimer LJ, Gideon G, Koimbu G, Barnadas C, Makita L, et al. Changes in malaria burden and transmission in sentinel sites after the roll-out of long-lasting insecticidal nets in Papua New Guinea. Parasit Vectors. 2016;9:340. doi: 10.1186/s13071-016-1635-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Rodriguez-Rodriguez D, Maraga S, Lorry L, Robinson LJ, Siba PM, Mueller I, et al. Repeated mosquito net distributions, improved treatment, and trends in malaria cases in sentinel health facilities in Papua New Guinea. Malar J. 2019;18:364. doi: 10.1186/s12936-019-2993-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.WHO. Global Health Observatory data repository. Geneva. World Health Organization; 2021 [Available from: https://apps.who.int/gho/data/view.main.MALARIAINCIDENCEv.
- 9.WHO. Malaria Country profile: Papua New Guinea. Geneva, World Health Organization; 2020 [Available from: https://www.who.int/malaria/publications/country-profiles/profile_png_en.pdf?ua=1.
- 10.Koimbu G, Czeher C, Katusele M, Sakur M, Kilepak L, Tandrapah A, et al. Status of insecticide resistance in Papua New Guinea: an update from nation-wide monitoring of Anopheles mosquitoes. Am J Trop Med Hyg. 2018;98:162–5. doi: 10.4269/ajtmh.17-0454. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Vinit R, Timinao L, Bubun N, Katusele M, Robinson LJ, Kaman P, et al. Decreased bioefficacy of long-lasting insecticidal nets and the resurgence of malaria in Papua New Guinea. Nat Commun. 2020;11:3646. doi: 10.1038/s41467-020-17456-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Reimer LJ, Thomsen EK, Koimbu G, Keven JB, Mueller I, Siba PM, et al. Malaria transmission dynamics surrounding the first nationwide long-lasting insecticidal net distribution in Papua New Guinea. Malar J. 2016;15:25. doi: 10.1186/s12936-015-1067-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Thomsen EK, Koimbu G, Pulford J, Jamea-Maiasa S, Ura Y, Keven JB, et al. Mosquito behavior change after distribution of bednets results in decreased protection against malaria exposure. J Infect Dis. 2017;215:790–7. doi: 10.1093/infdis/jix071. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Vanden Eng JL, Thwing J, Wolkon A, Kulkarni MA, Manya A, Erskine M, et al. Assessing bed net use and non-use after long-lasting insecticidal net distribution: a simple framework to guide programmatic strategies. Malar J. 2010;9:133. doi: 10.1186/1475-2875-9-133. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Doda Z, Solomon T, Loha E, Gari T, Lindtjørn B. A qualitative study of use of long-lasting insecticidal nets (LLINs) for intended and unintended purposes in Adami Tullu, East Shewa Zone, Ethiopia. Malar J. 2018;17:69. doi: 10.1186/s12936-018-2209-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Santos EM, Coalson JE, Munga S, Agawo M, Jacobs ET, Klimentidis YC, et al. "After those nets are torn, most people use them for other purposes”: an examination of alternative bed net use in western Kenya. Malar J. 2020;19:272. doi: 10.1186/s12936-020-03342-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Linn SY, Maung TM, Tripathy JP, Shewade HD, Oo SM, Linn Z, et al. Barriers in distribution, ownership and utilization of insecticide-treated mosquito nets among migrant population in Myanmar, 2016: a mixed methods study. Malar J. 2019;18:172. doi: 10.1186/s12936-019-2800-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Pulford J, Hetzel MW, Bryant M, Siba PM, Mueller I. Reported reasons for not using a mosquito net when one is available: a review of the published literature. Malar J. 2011;10:83. doi: 10.1186/1475-2875-10-83. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Rotarians Against Malaria. Long lasting insecticidal net distribution report: New Ireland Province. Port Moresby: 2016.
- 20.Papua New Guinea National Department of Health. Sector Performance Annual Review for 2019: Government of Papua New Guinea; 2020 [Available from: https://www.health.gov.pg/pdf/SPAR_2019.pdf.
- 21.Papua New Guinea National Department of Health. Sector Performance annual review for 2017. Port Moresby; 2018.
- 22.Hetzel MW, Pulford J, Ura Y, Jamea-Maiasa S, Tandrapah A, Tarongka N, et al. Insecticide-treated nets and malaria prevalence, Papua New Guinea, 2008–2014. Bull World Health Organ. 2017;95:695–705b. doi: 10.2471/BLT.16.189902. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Hetzel M, Saweri O, Kuadima J, Smith I, Tandrapah A, Jamea-Maiasa S, et al. Papua New Guinea Malaria Indicator Survey 2016–2017: Malaria Prevention, Infection, and Treatment. Goroka: Papua New Guinea Institute of Medical Research; 2018 [Available from: https://www.malariasurveys.org/documents/PNGIMR%202018 %20-%20PNG%20MIS%202016-17 %20-%20Final%20Report%2006.04.2018.pdf.
- 24.Mc Dermott R, Ruediger S. The Lihir Island Integrated Strategic Plan, 2013–2017. A Review of the Lihir Island Group Health System and a proposal for a Public Private Partnership (PPP) Health Model and Discussion Paper2012.
- 25.Rotarians Against Malaria. Long lasting insecticidal net distribution report. New Ireland Province, Papua New Guinea; 2019.
- 26.Roll Back Malaria Monitoring and Evaluation Reference Group. Household survey indicators for malaria control 2018 [Available from: Household Survey Indicators for Malaria Control_FINAL.pdf (endmalaria.org).
- 27.Green BF, Tukey JW. Complex analyses of variance: general problems. Psychometrika. 1960;25:127–52. doi: 10.1007/BF02288577. [DOI] [Google Scholar]
- 28.StataCorp . Stata Statistical Software: Release 16. College Station. TX: StataCorp LLC; 2019. [Google Scholar]
- 29.QGIS.org. QGIS Geographic Information System. QGIS Association; 2021.
- 30.Gonahasa S, Maiteki-Sebuguzi C, Rugnao S, Dorsey G, Opigo J, Yeka A, et al. LLIN Evaluation in Uganda Project (LLINEUP): factors associated with ownership and use of long-lasting insecticidal nets in Uganda: a cross-sectional survey of 48 districts. Malar J. 2018;17:421. doi: 10.1186/s12936-018-2571-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Mboma ZM, Overgaard HJ, Moore S, Bradley J, Moore J, Massue DJ, et al. Mosquito net coverage in years between mass distributions: a case study of Tanzania, 2013. Malar J. 2018;17:100. doi: 10.1186/s12936-018-2247-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Ntuku HM, Ruckstuhl L, Julo-Réminiac JE, Umesumbu SE, Bokota A, Tshefu AK, et al. Long-lasting insecticidal net (LLIN) ownership, use and cost of implementation after a mass distribution campaign in Kasaï Occidental Province, Democratic Republic of Congo. Malar J. 2017;16:22. doi: 10.1186/s12936-016-1671-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Hetzel MW, Gideon G, Lote N, Makita L, Siba PM, Mueller I. Ownership and usage of mosquito nets after four years of large-scale free distribution in Papua New Guinea. Malar J. 2012;11:192. doi: 10.1186/1475-2875-11-192. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Pulford J, Oakiva T, Angwin A, Bryant M, Mueller I, Hetzel MW. Indifferent to disease: a qualitative investigation of the reasons why some Papua New Guineans who own mosquito nets choose not to use them. Soc Sci Med. 2012;75:2283–90. doi: 10.1016/j.socscimed.2012.08.030. [DOI] [PubMed] [Google Scholar]
- 35.Arroz JAH, Mendis C, Pinto L, Candrinho B, Pinto J, Martins M. Implementation strategies to increase access and demand of long-lasting insecticidal nets: a before-and-after study and scale-up process in Mozambique. Malar J. 2017;16:429. doi: 10.1186/s12936-017-2086-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Government of Papua New Guinea. National Health Plan 2011–2020, Back to Basic. 2010.
- 37.Augustincic Polec L, Petkovic J, Welch V, Ueffing E, Tanjong Ghogomu E, Pardo Pardo J, et al. Strategies to increase the ownership and use of insecticide-treated bednets to prevent malaria. Cochrane Database Syst Rev. 2015;2015:Cd009186. doi: 10.1002/14651858.CD009186.pub2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Yukich J, Stuck L, Scates S, Wisniewski J, Chacky F, Festo C, et al. Sustaining LLIN coverage with continuous distribution: the school net programme in Tanzania. Malar J. 2020;19:158. doi: 10.1186/s12936-020-03222-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Lengeler C. Insecticide-treated bed nets and curtains for preventing malaria. Cochrane Database Syst Rev. 2004;2:CD000363. doi: 10.1002/14651858.CD000363.pub2. [DOI] [PubMed] [Google Scholar]
- 40.Hawley WA, Phillips-Howard PA, ter Kuile FO, Terlouw DJ, Vulule JM, Ombok M, et al. Community-wide effects of permethrin-treated bed nets on child mortality and malaria morbidity in western Kenya. Am J Trop Med Hyg. 2003;68(4 Suppl):121–7. doi: 10.4269/ajtmh.2003.68.121. [DOI] [PubMed] [Google Scholar]
- 41.Hetzel MW, Morris H, Tarongka N, Barnadas C, Pulford J, Makita L, et al. Prevalence of malaria across Papua New Guinea after initial roll-out of insecticide-treated mosquito nets. Trop Med Int Health. 2015;20:1745–55. doi: 10.1111/tmi.12616. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Additional file 1: Data collection tool used by the village malaria assistants (VMA) tocollect information for this survey.
Additional file 2: Definitions of the LLIN ownership and use indicators, used for thedata analysis.
Data Availability Statement
The datasets used and analysed during the current study are available from the corresponding author on reasonable request.