Abstract
Background
Most common sought antibiotic-self treated infection globally is pharyngitis (sore throat). The aim of this study is to assess public's acceptance and potential use of Rapid Antigen Detection Test at community pharmacies in the diagnosis of bacterial pharyngitis in children prior to antibiotic dispensing in Saudi Arabia.
Method
A qualitative cross-sectional study was conducted on October 2017. Two self-conducted questionnaires were used. One targeted the public above 21 years old and was distributed via social media. The other randomly targeted community pharmacists in Jeddah.
Result
A total of 689 of the public and 40 community pharmacists completed the survey. Moreover, 571 (82.9%) of the public received antibiotics without a prescription; for symptoms related to sore throat (71%) followed by flu-like symptoms (24%). Only (3.77%) and (5%) of both public and community pharmacies have heard about RADT respectively, however the majority (93.03%) and (90%) of both respectively support its use in community pharmacies. Coded reasons for its use was mainly to decrease antibiotic misuse and/or abuse, increased specificity, decreased antibiotic side effects including bacterial resistance, and ease of use.
Conclusion
Both public and community pharmacists support the idea of using RADT. Future efforts should look into pharmacist's role in providing point of care tests that are cost-effective and convenient for the public.
Keywords: Pharyngitis, Self-medication, Bacterial resistance, Sore throat, Rapid antigen detection test, Point of care test
1. Background
One of the most concerns in pharmacist’s dispensing pattern of medications without a prescription is that of antibiotic (Abx) (Al Rasheed et al., 2016). Most common sought antibiotic-self treated infection globally is known to be pharyngitis (sore throat); despite the fact that 80% is usually viral, self-limiting and does not require antibiotic use (Shulman et al., 2012).
Furthermore, acute pharyngitis (sore throat) is a frequent infectious disease of the oropharynx. It affects mostly children aged 5–15 years old, and is usually viral. However, (20–30%) of pharyngitis in children can also be bacterial; most commonly caused by Streptococcus pyogenes or group A Streptococcus (GAS) (Uphoff et al., 2016).
Bacterial pharyngitis symptoms usually include sudden onset of sore throat that worsens with swallowing, fever, headache, nausea and vomiting; whereas viral pharyngitis symptoms include cough, rhinorrhea, hoarseness and conjunctivitis (Uphoff et al., 2016). Because it is difficult to clinically distinguish between viral and bacterial pharyngitis; CDC guidelines recommend using rapid antigen detection test (RADT) or throat culture to differentiate between them (Shulman et al., 2012).
Unfortunately, many countries including Saudi Arabia, have reported inappropriate dispensing pattern of antibiotics. A simulated study in Jeddah, Saudi Arabia, found that (97.9%) of acquired antibiatoci in community pharmacies, is dispensed readily (Al-Mohamadi et al., 2013). In another study, that was done in Riyadh, the capital of Saudi Arabia; a remarkable 77.6% of pharmacies in Saudi Arabia are dispensing antibiotics without demanding a valid prescription; with 95% doing so without even the patient’s request (Bin Abdulhak et al., 2011).
Inappropriate use of antibiotics without prescription is clearly stated by the World Health Organization (WHO) as an emerging issue throughout the world including both poor and developing countries. Moreover, Saudi Arabia has showed the highest antimicrobial resistance across all Gulf Corporation Council (GCC) countries (El Zowalaty et al., 2016).
Just recently the Ministry Of Health (MOH) has announced a set of rules and regulations condemning Abx dispensing at Community Pharmacies (CP) without requesting a valid prescription (Little et al., 2013). This decision was applauded by most; yet may cause overcrowding of hospitals and increased cost to patients (Al Rasheed et al., 2016). Given the shift of these regulations, one can only contemplate the use of RADT in CPs to overcome these problems.
The aim of this study is therefore, to assess public’s and community pharmacist’s perception of RADT use as a diagnostic tool for bacterial pharyngitis in children prior to Abx dispensing in CPs in Saudi Arabia.
2. Methods
A qualitative cross-sectional observational study was conducted on October 2017. Two self-conducted questionnaires were validated by expert opinion. One targeted the public and was distributed via social media. The other targeted pharmacists in Jeddah and was randomly distributed and filled by them. For better assessment we only included (1) respondents above 21 years old, (2) have children, (3) received a valid antibiotic prescription for their kids and (4) for upper respiratory tract infection.
2.1. Public questionnaire items
The public questionnaire items consisted of 10 questions, under three sections: (1) respondent’s demographics, (2) antibiotic related questions, and (3) RADT related questions.
2.1.1. Public questionnaire items for RADT use in bacterial pharyngitis diagnosis
| Respondent's demographic |
|
| Antibiotic related question |
|
| RADT related question |
|
*The description included a picture of RADT test, followed by the following information: RADT is a tool that can be used to determine whether or not bacteria is present in the patient's throat. It is used in pharyngitis (sore throat). It takes only 5–10 min. It's done by taking a swab from the tonsils (back wall of the mouth). And it costs from 5 to 10$ (19–38 SR)
2.2. Community pharmacist questionnaire items
The community pharmacist questionnaire items consisted of 9 questions under two sections: (1) community pharmacist's demographics and (2) RADT related questions.
2.2.1. Pharmacist survey items on RADT use for bacterial pharyngitis diagnosis
| Community pharmacist' demographics: |
|
| RADT related question: |
|
3. Results
3.1. Public RADT perception
For the public survey, we collected 7368 responses in less than 24 h. A total of (571, 38%) reported that they received antibiotic without prescription at community pharmacies, to treat upper respiratory tract infections; mainly sore throat (405, 71%) followed by influenza/flu-like symptoms (137, 24%) (Fig. 1).
Fig. 1.
Named infections by respondents who received antibiotics without prescription (n = 571). *RTI: Repertory Tract Infection. **Symptoms were described as: cough, influenza, sore throat and common cold.
We narrowed respondents according to inclusion and exclusion criteria to reach a total of 689. Majority were female (629, 90.86%), over the age of 35 years old (395, 57.33%), and with no medical insurance (497, 72.13%) (Table1).
Table 1.
Respondents’ demographics (n = 689).
| Respondent Demographic | n (%) |
|---|---|
| Sex | |
| Female | 629(90.86) |
| Male | 60(8.71) |
| Age | |
| >35 years | 395(57.33) |
| 29–35 years | 188(27.29) |
| 22–28 years | 106(15.38) |
| Medical Insurance | |
| Available | 192(27.87) |
| Not available | 497(72.13) |
Just over half respondent 366 (366, 53.12%) were not aware that pharyngitis is more common in children and is caused by a virus in most cases (70–80%). Moreover, only (26, 3.77%) have heard of RADT that is used to differentiate between viral and bacterial pharyngitis. Following a brief description of the device, place in practice and estimated price; (641, 93.03%) supported their use in CPs as Point of Care Testing to differentiate between bacterial and viral pharyngitis (Table2).
Table 2.
Public’s perception of RADT at community pharmacies (n = 689).
| Question | N (%) |
|---|---|
| Do you know that pharyngitis is more common in children and is only caused by bacteria in 20–30% of cases? | |
| Yes | 366 (53.12) |
| No | 323 (46.88) |
| Have you heard of a product known as a rapid antigen detection test (RADT) that is used to detect bacterial pharyngitis and the need for antibiotics? | |
| Yes | 26 (3.77) |
| No | 663 (96.23) |
| Would you like to have this quick test done for your child to detect if antibiotic is needed in community pharmacies?* | |
| Yes | 641 (93.03) |
| No | 48 (6.97) |
This question followed the brief description of RADT that is mentioned above in methodology. Refer to Table 1 for full description.
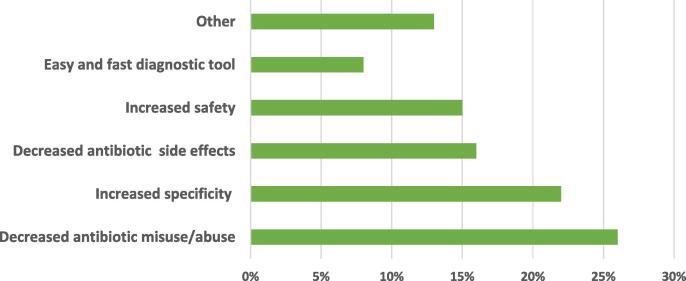
Coded reasons by the public supporting RADT use in community pharmacies were mainly to decrease antibiotic misuse/abuse (26%), followed by increased specificity (152, 22%), decreased antibiotic side effect and complication (110, 15.96%), and increased overall safety (103, 14.95%) (Fig. 2).
Fig. 2.
Percent of coded reasons by the public for RADT use in children, n = 689. Other: Skipped (10%), Cost effectiveness (2%), decreased bacterial resistance (1%).
3.2. Community pharmacy RADT perception
A total of 40 pharmacies were visited randomly within Jeddah, Saudi Arabia. All pharmacist agreed to participate with (40, 100%) response rate. Pharmacists were all non-Saudis, and the majority were between 26 and 30 and 31 to 45 years old (18, 45% each), held a bachelor’s degree (36, 90%) and have had 4–10 years of experience (23, 57.5%) (Table 3).
Table 3.
Community pharmacist’s demographics (n = 40).
| Respondent Demographic | n (%) |
|---|---|
| Nationality | |
| Saudi | 0 |
| Non-Saudi | 40 (100%) |
| Age | |
| 22–25 years | 2 (5) |
| 26–30 years | 18 (45) |
| 31–45 years | 18 (45) |
| >45 years of age | 2 (5) |
| Sex | |
| Female | 0(0) |
| Male | 40 (100) |
| Degree | |
| Bachelor of pharmacy | 36 (90) |
| PharmD | 3 (7.5) |
| Pharmacy resident | 1 (2.5) |
| Years of experience | |
| <1 year | 0 |
| 1–3 years | 9 (22.5) |
| 4–10 years | 23 (57.5) |
| >10 years | 8 (20) |
Almost all respondents (38, 95%) did not hear about RADT. However, after a brief description of the test; majority (35, 87.5%) believed the test would benefit the society. Moreover, (36, 90%) supported its use in community pharmacies to help diagnose bacterial pharyngitis in children (Table 4).
Table 4.
Community Pharmacist’s perception of performing RADT at community pharmacies (n = 40).
| Question | N (%) |
|---|---|
| Have you heard of a product known as a rapid antigen detection test (RADT) that is used to detect bacterial pharyngitis and the need for antibiotics? | |
| Yes | 2 (5) |
| No | 38 (95) |
| Do you think using such a device in community pharmacies may benefit the society? | |
| Yes | 35 (87.5) |
| No | 5 (12.5) |
| Do you support offering this quick test in community pharmacies? | |
| Yes | 36 (90) |
| No | 4 (10) |
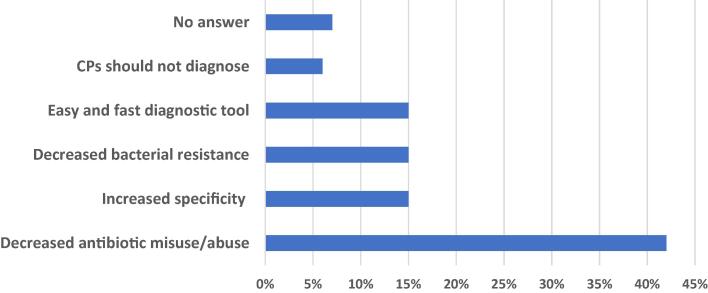
Coded reasons by pharmacist supporting RADT use in community pharmacies were mainly to decrease antibiotic misuse and abuse (17, 42.5%), followed by decreased bacterial resistance (6, 15%), increased specificity (6, 15%) and to obtain an accelerated result easily (6, 15%). Those against using it at community pharmacies (4, 10%) were mainly against pharmacists taking a diagnostic role (3) while one did not provide an answer. Coded reasons are listed in (Fig. 3).
Fig. 3.
Percent of coded reasons by community pharmacists for RADT use in children, n = 40.
4. Discussion
This is the first study to date to assess both public and pharmacist acceptance of point of care testing, particularly RADT in the diagnosis of bacterial pharyngitis in community pharmacies. Antibiotic dispensing without a valid prescription at community pharmacies is a problem that is well documented in the literature, and just recently the Ministry of Health (MOH) has taken stringent steps on antibiotic illegal dispensing without prescription on April of 2018 (MOH News - MOH Warns Against Selling Antibiotics without Prescription, n.d.).
Because this survey was distributed before the MOH new regulations, 38% still received an antibiotic without a valid prescription at community pharmacies. We believe this number may have dropped significantly after the new regulations.
The gold standard for detecting GABHS is a throat-swab culture, however results are available after 24 h (Shulman et al., 2012). Alternatively rapid antigen detection test (RADT) can be done at the point of care (POC), such as in a physician’s office or a community pharmacy, with results available within a few minutes. RADT has reported 97% sensitivity and over 95% specificity. Current guidelines however, recommended that children with negative result still need to confirm the results with a throat-swab culture (Worrall et al., 2007).
Empiric treatment using antibiotic for pharyngitis based on signs and symptoms of the patient would no doubt lead to misuse/overuse of antibiotics. In one study, pediatricians prescribed antibiotics to 79.8% of patients in which the incidence of GAS pharyngitis was only 17%.
In our study, most sought for self-medicated infections with antibiotics without prescription was sore throat (71%) followed by influenza/flu symptoms (24%). Which is consistent with a study in Riyadh that found respiratory diseases such as cough, sore throat, and common colds to be the most frequent infections for self-medication with antibiotics (Al Rasheed et al., 2016).
With the public questionnaire; majority of respondents were female (91%) and over 35 years of age (57.33%) which gives a great representation to our society since women are considered the main caregivers of their children and are more concerned about giving medications; particularly antibiotic to their children.
Some studies have shown that antibiotic self-medication is linked to (1) lack of legislation that prohibits dispensing antibiotics without prescriptions, (2) poor enforcement of regulations, (3) high cost of medical consultation, and (4) lack of health insurance (Dror et al., 2016, Grigoryan et al., 2006). The MOH have taken stringent actions in the enforcing regulations. However, the majority on our sample were not medically insured (72.13%); and this may have an influence on self-medication in our population. Future studies and health authorities should look further into this.
Moreover, over half respondents (53%) did not know pharyngitis could be viral and therefore does not require antibiotics. This mandate educational campaigns targeting the public to raise awareness on viral vs bacterial infections and the prevalence of each. Only (4%) have heard of the RADT and after a brief description of the device, role, and price, (93.32%) supported its use. Their support came mainly to decrease antibiotic misuse/abuse (26%), increased specificity (22%), decreased antibiotics related side effects (16%) and increased overall safety (15%).
On the other hand, 95% of all surveyed pharmacists did not hear of RADT which is only used in some hospitals in Jeddah. Majority of doctors still seem to diagnose based on clinical symptoms, a practice that is not recommended by guidelines, due to reported antibiotic overuse. The utilization of rapid antigen-detection tests (RADT) or Strep A has been associated with lower antibiotic prescribing for patients with sore throat. One study reported 45% reduction in antibiotic prescribing in adults using RADT compared to empirical treatment (Humair et al., 2006). In another primary-care study in Switzerland, RADT reduced antibiotic prescribing from 60% to 37%. Moreover, greater reductions were observed with pediatricians, where streptococcal infection rate is seen higher in children; with antibiotic prescribing percentages of only 22–28% when using RADT (Ayanruoh et al., 2009).
We believe the 40 pharmacists who did participate in the study gave a good representation of CPs in Saudi, with an age range of 25–45 years old and 4–10 years of experience. Furthermore, 90% of surveyed pharmacists supported their use at CPs and coded reasons presented by them aligned with public’s perception of its use. Majority (42%) were stating that it can decrease antibiotic misuse and abuse, and the remaining reasons were (15%) to decrease bacterial resistance and increased specificity.
Finally, one of the major limitations of our study is limiting survey results to RADT use in children. However, we believe we can extrapolate these findings to the use of POCT and RADT to adults too since the pediatric population is the more vulnerable population. Future studies should look into the cost effectiveness of these tools, particularly in CPs; to decrease hospital waiting time and overload. Future studies and the ministry of health can look into the potential role pharmacist or primary care physicians performing a well-trained POCT prior to dispensing antibiotics.
5. Conclusion
Our study strongly suggests public and community pharmacist preparedness and acceptance for CPs Point of Care Testing (POCT), including RADT with the perceived advantages of decreasing antibiotic abuse/misuse. This study paves the way for their use in CPs by well-trained pharmacists. Interventions to reduce over-prescribing antibiotics, including the utilization of such valid, rapid point-of-care tests, in addition to educating the public on microbial resistance with overuse of antibiotics should be enforced. Future efforts should look into pharmacist’s role in providing community service that are cost-effective and convenient for the public as a whole.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Footnotes
Peer review under responsibility of King Saud University.
References
- Al Rasheed, A., et al., 2016. Prevalence and Predictors of Self-Medication with Antibiotics in Al Wazarat Health Center, Riyadh City, KSA [WWW Document]. BioMed Res. Int. 10.1155/2016/3916874. [DOI] [PMC free article] [PubMed]
- Al-Mohamadi A. Dispensing medications without prescription at Saudi community pharmacy: Extent and perception. Saudi Pharm. J. SPJ. 2013;21:13–18. doi: 10.1016/j.jsps.2011.11.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ayanruoh S. Impact of rapid streptococcal test on antibiotic use in a pediatric emergency department. Pediatr. Emerg. Care. 2009;25:748–750. doi: 10.1097/PEC.0b013e3181bec88c. [DOI] [PubMed] [Google Scholar]
- Bin Abdulhak A.A. Non prescribed sale of antibiotics in Riyadh, Saudi Arabia: a Cross Sectional Study. BMC Public Health. 2011;11:538. doi: 10.1186/1471-2458-11-538. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dror D.M. Impact of community-based health insurance in rural India on self-medication & financial protection of the insured. Indian J. Med. Res. 2016;143:809–820. doi: 10.4103/0971-5916.192075. [DOI] [PMC free article] [PubMed] [Google Scholar]
- El Zowalaty M.E. Knowledge, awareness, and attitudes toward antibiotic use and antimicrobial resistance among Saudi population. Int. J. Clin. Pharm. 2016;38:1261–1268. doi: 10.1007/s11096-016-0362-x. [DOI] [PubMed] [Google Scholar]
- Grigoryan L. Self-medication with Antimicrobial Drugs in Europe. Emerg. Infect. Dis. 2006;12:452–459. doi: 10.3201/eid1203.050992. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Humair J.-P. Management of acute pharyngitis in adults: reliability of rapid streptococcal tests and clinical findings. Arch. Intern. Med. 2006;166:640–644. doi: 10.1001/archinte.166.6.640. [DOI] [PubMed] [Google Scholar]
- Little P. PRImary care Streptococcal Management (PRISM) study: identifying clinical variables associated with Lancefield group A β-haemolytic streptococci and Lancefield non-Group A streptococcal throat infections from two cohorts of patients presenting with an acute sore throat. BMJ Open. 2013;3:e003943. doi: 10.1136/bmjopen-2013-003943. [DOI] [PMC free article] [PubMed] [Google Scholar]
- MOH News - MOH Warns Against Selling Antibiotics without Prescription [WWW Document], n.d. URL https://www.moh.gov.sa/en/Ministry/MediaCenter/News/Pages/news-2018-04-17-004.aspx (accessed 12.7.20).
- Shulman S.T. Clinical practice guideline for the diagnosis and management of group A streptococcal pharyngitis: 2012 update by the Infectious Diseases Society of America. Clin. Infect. Dis. Off. Publ. Infect. Dis. Soc. Am. 2012;55:1279–1282. doi: 10.1093/cid/cis847. [DOI] [PubMed] [Google Scholar]
- Uphoff T.S. Multicenter evaluation of the Solana Group A streptococcus assay: comparison with culture. J. Clin. Microbiol. 2016;54:2388–2390. doi: 10.1128/JCM.01268-16. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Worrall G. Diagnosing streptococcal sore throat in adults Randomized controlled trial of in-office aids. Can. Fam. Physician Médecin Fam. Can. 2007;53:666–671. [PMC free article] [PubMed] [Google Scholar]