The article by Lee et al 1 showed that the current use of proton pump inhibitors (PPIs) increased the risk of severe clinical outcomes of COVID-19 rather than the susceptibility to SARS-CoV-2 infection in a Korean nationwide cohort. Instead, a significant association between susceptibility to SARS-CoV-2 infection and current use of PPIs, either one time or two times a day, was found by another recent study2 based on US nationwide data. The conflicting results of these two large-scale observational studies may be due to regional epidemiological differences or considerable between-study variance and might compromise clinical decision-making. As the impact of PPI use on SARS-CoV-2 infection has very relevant clinical implications, we performed a meta-analysis to address the aforementioned discrepancies, which could lead to better informed clinical decision-making on PPI use during the ongoing pandemic.
We scrutinised 3413 records retrieved from a comprehensive search using the COVID-19 Research Articles Downloadable Database maintained by the US CDC (https://www.cdc.gov/library/researchguides/2019novelcoronavirus/researcharticles.html) and ultimately included 16 studies1–16 from 10 countries or regions reporting comparative data on PPI use and clinical outcomes of COVID-19 (online supplemental figure 1 and table). We pooled the data using an inverse variance-weighted random-effect model. Pooled estimates are presented as OR, HR or mean difference (MD), with associated 95% CIs. Intensive care unit admission, mechanical ventilation, acute respiratory distress syndrome or death were considered severe outcomes of COVID-19.
gutjnl-2020-323366supp001.pdf (918KB, pdf)
Six studies1–6 including 318 261 participants reported data on PPI usage and the risk of SARS-CoV-2 infection. Among them, five studies had information of current PPI users compared with non-users and four on past PPI users versus non-users. Analysis of five studies1–5 encompassing 145 428 patients who were tested for SARS-CoV-2 showed that the risk of SARS-CoV-2 infection was higher, although not significantly, among current PPI users (OR 1.33, 95% CI 0.86 to 2.07, p=0.20; figure 1) compared with PPI non-users, with evidence of substantial between-study heterogeneity (I 2=97%). Moreover, in a subgroup analysis of non-Korean cohorts,2–4 we found a significant association between current use of PPIs and increased risk of SARS-CoV-2 infection (OR 1.94, 95% CI 1.59 to 2.36, p<0.0001; online supplemental figure 2). Furthermore, a leave-one-out sensitivity analysis revealed that the summary estimate of the association between current PPI usage and SARS-CoV-2 infection was overly influenced by a single Korean study5 (online supplemental figure 3).
Figure 1.
Forest plot showing the association between PPI use and SARS-CoV-2 infection. PPI, proton pump inhibitor.
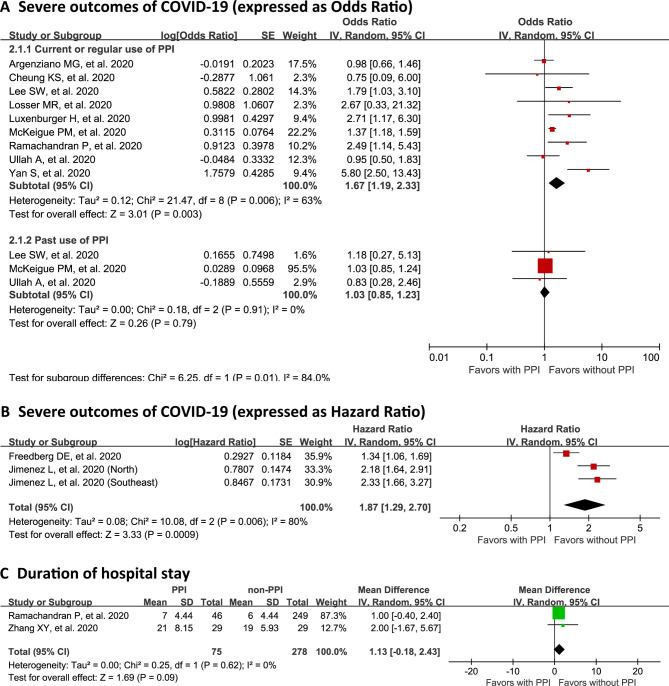
Instead, current or regular PPI users were more likely to have severe outcomes of COVID-19 than PPI non-users, with a pooled OR of 1.67 (95% CI 1.19 to 2.33, p=0.003; n=42 405 from nine studies;1 3 7–13 I 2=63%; figure 2) and a pooled HR of 1.87 (95% CI 1.29 to 2.70, p<0.001; n=2977 from two studies;15 16 I 2=80%; figure 2). These results were consistent with our leave-one-out sensitivity analysis (online supplemental figure 4), indicating that this association was strong. Furthermore, current PPI users tended to hospitalised longer than PPI non-users, although not by a statistically significant margin (n=353 from two studies;7 14 MD 1.13, 95% CI −0.18 to 2.43, p=0.09; figure 2). Finally, past use of PPIs was not associated with increased susceptibility to SARS-CoV-2 infection (n=1 72 833 from four studies;1 3 5 6 OR 0.85, 95% CI 0.57 to 1.27, p=0.43; I 2=92%; figure 1) or with severe outcomes of COVID-19 (n=40 097 from three studies;1 3 9 OR 1.03, 95% CI 0.85 to 1.23, p=0.79; I 2=0%; figure 2).
Figure 2.
Forest plot showing the association of PPI use with severe outcomes of COVID-19 (A, OR; B, HR) or duration of hospital stay (C). PPI, proton pump inhibitor.
In summary, this meta-analysis shows that regional differences can explain the heterogeneous findings concerning the association between current PPI use and incidence of SARS-CoV-2 infection and further underscores the increased risk of severe COVID-19 outcomes associated with current PPI use, highlighting that caution should be exercised when treating patients receiving PPIs during the COVID-19 pandemic. Further studies investigating different dosing regimens and durations of PPI use on COVID-19 outcomes should be warranted.
Footnotes
Contributors: Concept and design: G-FL and GY. Acquisition, analysis and interpretation of data: G-FL, X-XA, GY, YY, L-RJ, D-NW, YX. Drafting of the manuscript: GFL. Supervision: GY. Critical revision of the manuscript: DC, G-FL, GW and YY. Final approval: all authors.
Funding: This work was supported by Jiangsu Provincial Medical Youth Talent programme (QNRC2016323), Jiangsu Province 333 Project (to GY) and Jiangsu Provincial Science Fund for Distinguished Young Scholars (to GY).
Competing interests: None declared.
Provenance and peer review: Not commissioned; externally peer reviewed.
Supplemental material: This content has been supplied by the author(s). It has not been vetted by BMJ Publishing Group Limited (BMJ) and may not have been peer-reviewed. Any opinions or recommendations discussed are solely those of the author(s) and are not endorsed by BMJ. BMJ disclaims all liability and responsibility arising from any reliance placed on the content. Where the content includes any translated material, BMJ does not warrant the accuracy and reliability of the translations (including but not limited to local regulations, clinical guidelines, terminology, drug names and drug dosages), and is not responsible for any error and/or omissions arising from translation and adaptation or otherwise.
Ethics statements
Patient consent for publication
Not required.
References
- 1.Lee SW, Ha EK, Yeniova Abdullah Özgür. Severe clinical outcomes of COVID-19 associated with proton pump inhibitors: a nationwide cohort study with propensity score matching. Gut 2021;70:807–9. 10.1136/gutjnl-2020-322248 [DOI] [PubMed] [Google Scholar]
- 2.Almario CV, Chey WD, Spiegel BMR, et al. Increased risk of COVID-19 among users of proton pump inhibitors. Am J Gastroenterol 2020;115:1707–15. 10.14309/ajg.0000000000000798 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Ullah A, Sivapalan L, Chelala PC, et al. COVID-19 in patients with hepatobiliary and pancreatic diseases in East London: a single-centre cohort study. medRxiv 2020. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Vila-Corcoles A, Satue-Gracia E, Ochoa-Gondar O, et al. Use of distinct anti-hypertensive drugs and risk for COVID-19 among hypertensive people: a population-based cohort study in southern Catalonia, Spain. J Clin Hypertens 2020. 10.1111/jch.13948. [Epub ahead of print: 25 Jul 2020]. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Huh K, Ji W, Kang M, et al. Association of previous medications with the risk of COVID-19: a nationwide claims-based study from South Korea. medRxiv 2020. [Google Scholar]
- 6.Tarlow B, Gubatan J, Khan MA, et al. Are proton pump inhibitors contributing to SARS-COV-2 infection? Am J Gastroenterol 2020. 10.14309/ajg.0000000000000933. [Epub ahead of print: 11 Sep 2020]. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Ramachandran P, Perisetti A, Gajendran M, et al. Prehospitalization proton pump inhibitor (PPI) use and clinical outcomes in COVID-19. medRxiv 2020. [DOI] [PubMed] [Google Scholar]
- 8.Luxenburger H, Sturm L, Biever P, et al. Treatment with proton pump inhibitors increases the risk of secondary infections and ARDS in hospitalized patients with COVID-19: coincidence or underestimated risk factor? J Intern Med 2020. 10.1111/joim.13121. [Epub ahead of print: 01 Jul 2020]. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.McKeigue PM, Kennedy S, Weir A, et al. Associations of severe COVID-19 with polypharmacy in the REACT-SCOT case-control study. medRxiv 2020. [Google Scholar]
- 10.Argenziano MG, Bruce SL, Slater CL, et al. Characterization and clinical course of 1000 patients with coronavirus disease 2019 in New York: retrospective case series. BMJ 2020;369:m1996. 10.1136/bmj.m1996 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Cheung KS, Hung IFN, Leung WK. Association between famotidine use and COVID-19 severity in Hong Kong: a territory-wide study. Gastroenterology 2020. 10.1053/j.gastro.2020.05.098 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Losser M-R, Lapoix C, Delannoy M, et al. Almitrine as a non-ventilatory strategy to improve intrapulmonary shunt in COVID-19 patients. Anaesth Crit Care Pain Med 2020;39:467–9. 10.1016/j.accpm.2020.05.013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Yan S, Song X, Lin F, et al. Clinical characteristics of coronavirus disease 2019 in Hainan, China. medRxiv 2020. [Google Scholar]
- 14.Zhang XY, HB W, Ling Y, et al. Analysis of the effect of proton pump inhibitors on the course of common COVID-19. MedRxiv 2020. [Google Scholar]
- 15.Jimenez L, Codo AC, Sampaio VS, et al. The influence of pH on SARS-CoV-2 infection and COVID-19 severity. MedRxiv 2020. [Google Scholar]
- 16.Freedberg DE, Conigliaro J, Wang TC, et al. Famotidine use is associated with improved clinical outcomes in hospitalized COVID-19 patients: a propensity score matched retrospective cohort study. Gastroenterology 2020;159:1129–31. 10.1053/j.gastro.2020.05.053 [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
gutjnl-2020-323366supp001.pdf (918KB, pdf)