Abstract
Background
Patient safety is recognised as an important aspect of the undergraduate medical curriculum. However, packed medical curricula have been slow to evolve despite repeated mandates and large-scale tragedies resulting from unlearnt lessons. The aim of this work was to explore students’ perspectives on patient safety to inform curriculum re-design.
Methods
Using a qualitative approach, medical students from year 2 and year 4 of the undergraduate course were invited to participate in focus groups to consider: their personal conceptualisation of patient safety, their perceptions of patient safety education in the existing curriculum and their collective preferences for future teaching in this area. Transcripts of the focus groups were subjected to thematic analysis.
Results
Six focus groups were convened with a total of 77 students. Thirteen major themes were identified which included conceptual ambiguity, healthcare culture, error theory, specific safety topics (such as infection prevention and control, medication safety, technical/procedural safety, communication and other non-technical skills), self-awareness, patient-centredness, low student morale and raising concerns. Students were more aware of technical than non-technical competence. They wanted learning aligned to the realities of practice, a clearer concept of patient safety and improved visibility of patient safety topics within an integrated curriculum.
Conclusions
Students are keen to engage with safety topics but frequently feel disempowered as future change agents. Educators need to advocate a clear definition of patient safety and consider the implication of the theory-practice gap on students’ evolving attitudes.
Keywords: Patient safety, undergraduate curriculum, medical students
Introduction
Over the last 20 years, healthcare has become more aware that it is not risk averse [1]. Researchers continue to investigate and hold practitioners to account for an estimated 10% of clinical errors including medication, diagnostic and procedural errors which may lead to patient death [2–5]. The analysis of errors has begun to unpack concerns relating to human behaviour especially because practitioners fail to place the needs of patients as central to all they do [6]. In addition, there is a growing understanding of the impact of human factors, including how to work collaboratively with each other and, importantly, the part played by the working environment and the systems which govern care delivery [7–10]. In this way, health care has moved from a position of thinking about safety as a technical complexity to a position of thinking about service re-design with the patient in the midst of all we do; hence the term ‘patient safety’.
The part played by education was raised with Kohn and colleagues in 1999, recommending ‘professional societies… should develop a curriculum on patient safety and encourage its adoption into training and certification requirements’ [3]. Similarly in the UK ‘An Organisation with a Memory’ pointed to the need to develop a learning culture within the NHS, and a consequent change from passive to active learning, including team-based safety training [4]. In order to help guide these learning aspirations, there were a number of publications from the World Health Organisation (WHO), including a multi-disciplinary guide on a patient safety curriculum [11]. Recently, the UK report into care at the Mid Staffordshire NHS Foundation Trust uncovered a catalogue of patient errors resulting in calls for continuous learning with patients and a focus on quality of care delivery [6, 12]. There has been an international growth in qualified practitioners seeking to learn about quality improvement, team working and the psychology, sociology and ergonomics of human factors [13–16].
So where does this leave medical education? In 2006, an international symposium of medical educators reported that the provision of patient safety education was largely inadequate [17]. This is exemplified in a large-scale, multi-centre study of medical students’ and junior doctors’ knowledge of patient safety topics [18]. The study involved 693 medical trainees and identified significant deficiencies and a lack of insight into these. A cross-sectional survey of 1247 new graduates in medicine, nursing and pharmacy in Canada reported that overall levels of confidence indicated that more training in patient safety topics is required [19]. In particular, healthcare graduates reported lower levels of confidence in the management of safety risks and human factors topics. A systematic review by Nie et al. in 2010 reported that the academic literature contained a very limited number of high-quality studies relating to patient safety education [20]. Despite the growth in research on patient safety and recurrent global policy documents, medical education has been trying to define the attributes of a qualifying doctor and to consider post-qualified training requirements. In the most recent consultation documents on undergraduate medical education, emphasis is placed on ‘human factors’ [21]. However, translation into curriculum time and integration throughout a curriculum of these new non-technical competencies has been slow.
The opportunity to influence an undergraduate medical curriculum renewal led to research to listen to the views of medical students on patient safety and related teaching in the existing curriculum. We wanted to understand if the patient safety content of the medical curriculum, presented as a spiral progressive pathway of learning underpinned by educational theory, was adequate. The curriculum was built on the presumptions of medical students as adult learners and on solid educational theory [22]. The learning came from content designed and delivered through lectures and assimilated through group learning using social constructivist principles, later affirmed through experiential learning and reflection when in practice [23–25]. Our prior mapping exercise had identified a range of content on patient safety but this was not labelled directly as such but rather seen as a corpus of knowledge relevant to the well understood principles of safe practice.
Methodology
This research set out to discover how one UK medical school translated ‘patient safety’ into teaching design and delivery. In particular, we were interested to understand the concepts used by medical students, such as ‘sense making’ and ‘coherence’ for this learning; therefore, a qualitative approach was taken [26]. The research takes a phenomenological theoretical stance in that the medical students’ understandings—subjective consciousness, of patient safety will be shared as conversations with the researcher and interpreted at face value [27]. Data collection was using focus groups designed to enable the students to discuss topics presented and to make meaning through their interactions with one another. The number of meetings was dependent upon the researchers’ (AB and ES) continuous analysis of the content and agreement on saturation.
The sample included medical students at two points in their curriculum journey after 2 years of study and after 4 years of study. Selection was through a faculty member who acted as a gatekeeper, inviting students to participate in the research study through contact in a variety of elements of the medical curriculum. Participation was entirely voluntary and students who consented were randomly allocated to focus group meetings, staying in their year groups. Students were informed the focus groups would be recorded and assured of anonymity. The topic guide for the interviews was informed by a literature search on educational content on patient safety and from guidance of the WHO curriculum and GMC outcomes previously used in a mapping exercise of curriculum content relating to patient safety. The final schedule aimed to enable debate and discussion between participants and not to be researcher led. It consisted of three open questions:
-
i)
What does the term “patient safety” mean to you?
-
ii)
What have you been taught about patient safety?
-
iii)
Do you have any suggestions about how patient safety should be taught?
Analysis included verbatim translation into Microsoft Word. The transcripts were proof read in entirety by AB and ES to ensure that they were an accurate representation of the discussions with students mapped against notes made by the researchers while hosting the conversations. Data from the focus groups were analysed inductively using thematic analysis [28]. The audio recordings and transcripts were repeatedly reviewed in order to ensure familiarity with the data, to facilitate the identification of themes within it. Codes were identified in the printed text, and these were organised into concepts, without the use of computer software. The concepts were arranged into broader categories or themes to create a coding tree and were agreed iteratively by the two researchers.
Ethical permission for this study was granted by the University of Nottingham Medical School Research Ethics Committee.
Results
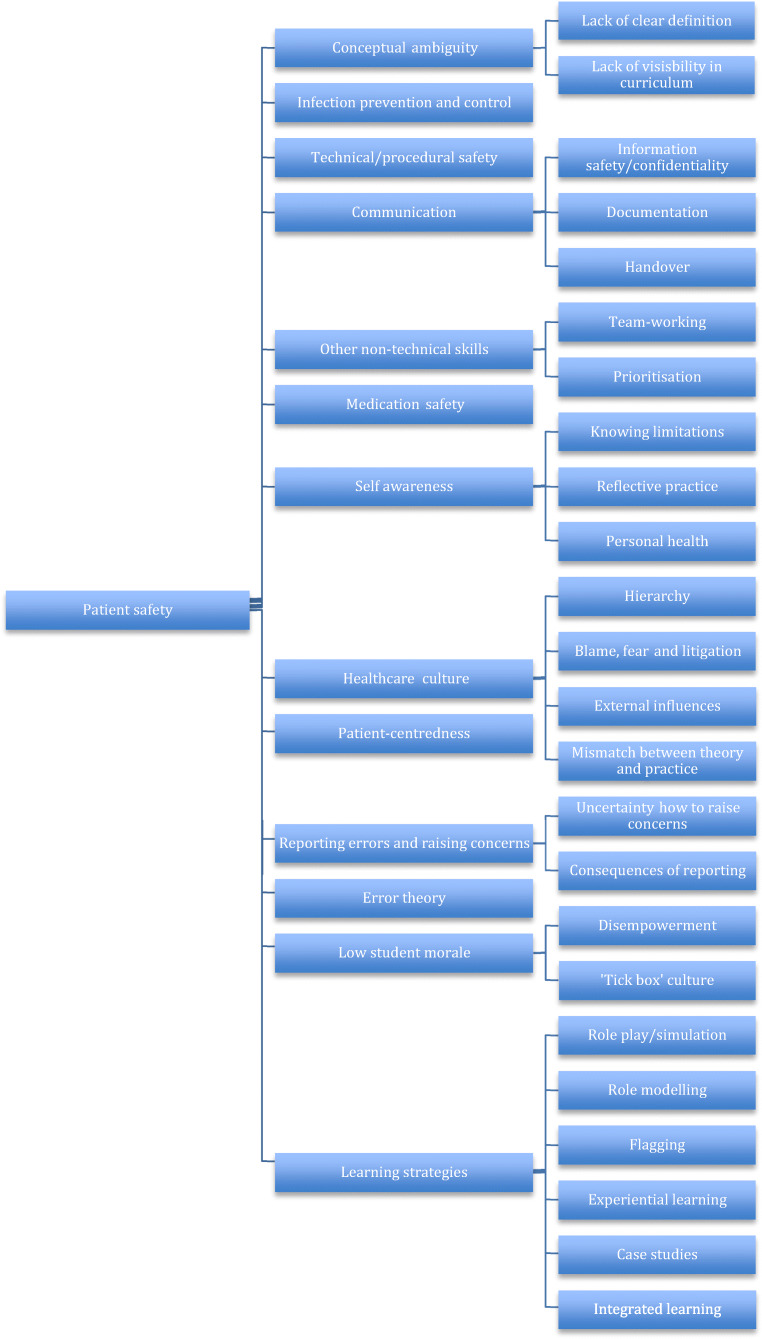
A total of 6 focus groups were convened, with 49 students from year 2 of the course and 28 students from year 4 of the course. Thematic analysis identified a total of 13 major themes and 25 sub-themes and these are demonstrated in the coding tree shown in Fig. 1. Individual themes are discussed in more detail below and examples of students’ comments (transcribed verbatim) are demonstrated in Table 1.
Fig. 1.
Coding tree created from thematic analysis
Table 1.
Examples of students’ comments on some of the patient safety themes identified by thematic analysis
| Theme/sub-theme | Comment |
|---|---|
| Conceptual ambiguity | |
| Lack of clear definition | ‘I do not think it’s anything that we have really been given a definition of so far on the course. We have never been given one but you can kind of take a bit of a guess yourself.’ |
| ‘I think impressions are formed mainly from outside of the Medical School; so from obviously what’s going on in the media with Stafford, from maybe those who have probably got previous clinical experience, what they have seen and experienced in their sort of previous working lives.’ | |
| “I think generally it’s quite ill defined and as a cohort, maybe, as students we do not really understand fully the concept of patient safety. And I think a lot of people tend to kind of switch off because it’s seen as, like, potentially quite a boring thing but if we knew a bit more about, sort of, what it fully entailed and what was encompassed by patient safety then we might pay a bit more attention to it.” | |
| Lack of visibility in the curriculum | ‘It’s not really clear that that’s what we are learning about, as a theme.’ |
| ‘It’s kind of been incorporated into whatever it seems most suitable to incorporate it into.’ | |
| ‘It’s kind of as though patient safety is lost in the other events, like the IPE—it’s almost like the interprofessional is more important than it. I just felt that this was all about spending time with the pharmacists, who rarely turn up, and the actual message of it wasn’t important. It’s just the fact that you were working with the other professions. Whereas if we knew it was a patient safety event and this was the main take-home message from it I think you would absorb it a lot better rather than, kind of, what are we doing here? We are just being spoken to, is this kind of a box-ticking exercise for me to work with other professions?’ | |
| Technical and procedural safety | ‘Something that sticks out in my mind is when we did manual handling. It’s a bit off the topic but we were taught, like, if a patient falls there’s no way you can catch them safely yourself. And obviously the NHS cannot have everyone hurting their back but as someone with family members in hospital, like, that’s not patient safety. But it’s a hard thing to do because it’s, like, staff safety as well. That was shocking.’ |
| ‘The triple check when you are doing a, like cannulating or whatever—checking the identity in three different places.’ | |
| Communication | |
| Information safety and confidentiality | ‘If we are ever making notes about a patient you just use their initials and ‘male’ or ‘female’ rather than actually writing their name or taking paper away like that.’ |
| ‘I think I would like to know more about what would constitute a breach of confidentiality because I am not really sure. Yeah, I am aware that saying somebody’s name, date of birth and hospital number is probably a bit much, is probably breaking their confidentiality but I am not sure how much information one could reveal to a colleague, you know, at home without breaking confidentiality.’ | |
| Documentation | ‘Everything that is sort of done for the patient should be written down. You are not only protecting yourself if something goes wrong but everyone else knows what’s been done and what needs to be done.’ |
| ‘I think the one thing that they have not taught us very well, unless I have just missed something or forgotten, is actually how to write notes while you are on a ward round. You are just sort of handed the book and told to get on with it and you have just picked up on how the juniors have written it before... if you do not know how to write a clear, concise set of notes and how to transmit that information then how are you going to transmit information safely?’ | |
| Handover | ‘When shifts are coming on and off that transition must be quite difficult to make sure that the patient is safe throughout when the care is not always continuous.’ |
| Other non-technical skills | |
| Team-working | ‘It’s a running theme, like, the importance of good team work throughout the whole thing because talking to other members of staff, running through a complete check list when you are prescribing, just like everything’s revolving around kind of making sure communication’s good so things do not slip through the net. The importance of that kind of relationship as well.’ |
| Prioritisation | ‘Something that’s quite overwhelming on the ward when you first get on is, kind of, priorities. In terms of safety, you know this patient’s about to fall out of the bed but I have got a needle in my hand, you know, what do I do in this situation?’ |
| Medication safety | ‘In Cancer Care we got teaching about how to prescribe morphine on TTOs because that is a little bit different, because you have to do it in words and numbers and things. They explicitly told us, “This is how you prescribe for a TTO” and we did lots of practice on that, so that was quite good. But apart from that I do not think I have ever been sat down and explicitly told, “This is how you prescribe safely”. I mean you probably pick most of it up but that is probably not the best way to learn it really.’ |
| Self-awareness | |
| Knowing limitations | ‘It’s your responsibility to recognise when you are unable to carry out a procedure and get someone else to do it if you think that by you doing it it would compromise their safety.’ |
| Reflective practice | ‘You need to have time to think about it a bit, come back a day or two later when—I hate to say the word “reflect” as obviously we are going to get bombarded with it, but it is that you need to just think, “What did I get wrong?” And you can go back and watch a video or read something else about it and then come back and it’s like, “OK, it makes a bit more sense now”.’ |
| Personal health | ‘[You need to be] fit to do your job. If your health is impaired in any way then you are not going to be able to make sure that what you are doing is not going to compromise patient safety’. |
| Healthcare culture | |
| Hierarchy | ‘We are just medical students and we are the bottom the pile’. |
| ‘If I saw something really bad and there were other people there I might assume that someone else would report it. Um, like, I don’t necessarily feel at the moment like that responsibility is all on us as a medical student because even a nurse, you know, nurses are more superior than us’. | |
| Blame, fear and litigation | ‘I find it, like, scary. It’s just, like, you know you are all responsible and, you know, it’s that thing where they say, “You are responsible. You need to be accountable for your actions.” But then they leave out the part of what would happen, what kind of mistakes do you have to make before you lose your whole career?’ |
| ‘If you are going to have a very litigious society people are not going to be jumping over each other to be honest about mistakes they have made.’ | |
| Mismatch between theory and practice | ‘I think there is a mismatch between the theory and the reality as everyone is talking about. Because my experience with the, when I went to the venepuncture session, you clean the tray and you leave it for 3 min to dry up but on the ward you would never have this chance to do it.’ |
| ‘I was going to do one of the blood cultures in the proper way that I was trained to and there was a health care assistant who was also trained to do blood cultures as well and I was trying to do it in the right way and she was like, “No, just use the syringe—that’s how it’s been done and it’s been done in that way for years and we did not have any problems so just forget about that blue vac”. They were very stressed, I was very stressed – I was getting told off for trying to do the right thing. And I just did not know what to do and I was really upset that day actually about it.’ | |
| Patient-centredness | ‘It’s the number one rule whenever you do anything in a hospital: patients should be at the centre of that decision.’ |
| Reporting errors and raising concerns | |
| Uncertainty how to raise concerns | ‘There’s 200 of us in our year in medical practice and we do not know who to go to.’ |
| Consequences of reporting | ‘I know of an issue that a friend of mine had whilst in X, that they had and they saw clinical practice that they thought was absolutely shocking and awful and they thought the patient was made to feel really really uncomfortable. I do not think their safety was a stake but certainly their dignity was stomped all over by a clinician and so they went to the undergraduate coordinator because that’s who they felt most comfortable to talk to, to talk about it and mention it. And then they kind of got, the undergraduate coordinator was very nice about it, but they got a little telling off almost from the clinical lead for that area who said, “You should not have gone to that person; you should have come to us first”, basically so they were saying so that we can keep it in-house because the undergraduate coordinator there is someone not medical and we do not want them knowing about it—we want to deal with it ourselves.’ |
| Low student morale | |
| Disempowerment | ‘Its almost like the Med School do not empower you as a person, to build up your self-confidence. One of the examples, I know it’s a Phase 1 example, but you’d got all these yellow forms going around and all of a sudden you have got a yellow form slapped on you and if you challenge it you get another one slapped on you. Can I find out about why? Can I give my own opinion? Can I express the reason as to why this has happened? Maybe there was crossed wires or, or maybe I just need to be sat down and explained, “OK, this is not acceptable because it does not...” But the minute you go, “Excuse me”, you get another one. And if you try again then you have to write an essay and it’s like, it’s almost like you are treating me like a child. Especially for the grads who, it’s like, “Hang on a minute—I am not straight from school.” I want to be responsible but to be an adult and actually ask in a respectful way, you just, you are not treated like an adult.’ |
|
Student 1: ‘Part of the thing that I would like to see is them [the Medical School] actually sort of encouraging that in us, instilling that belief that we are important enough to help with patient safety, or if we do recognise something they can equip us to deal with it effectively because we are important in that. And I know that I certainly do not feel important here in anyway at all. Well no, I do not know about anybody else but I have seen medical students on the wards before in hospitals where I have worked and they are...’ Student 2: ‘They are an inconvenience are not they?’ | |
| ‘Tick box’ culture | ‘For my venepuncture she sees me do it once, big tick all the way through for all the boxes and that’s the end of that. And nobody knows how good I am at venepuncture in this entire medical school.’ |
| Learning strategies | |
| Role modelling | ‘I think it’s more about models, I mean consultants teaching us, in practice what we do. It’s not about teaching things, like in slides, and say, “You do this and this”, but also seeing these things in practice. Not explicitly saying, “You have to do this” but just showing things to encourage learning.’ |
| Flagging | ‘I’d have found it quite useful just in the first few months if somebody had said to me patient safety is going to come up again and again and this is what it is. Watch out for it. Keep an eye on it. You are going to have a question in the exam on it.’ |
| Case studies | ‘We are all human, but to look into learning those kind of lessons might help in getting across what can go wrong. Cos dry teaching, you know, sort of does not go in but when you can, when you can enable someone to picture it and conjure it in their own mind and think, “OK, what can I put into my practice that would maybe prevent me from slipping down that road?”’ |
Theme: Conceptual Ambiguity
Most students’ understanding of the term ‘patient safety’ focussed upon the avoidance of harm. For example, one student defined patient safety as, ‘making sure the patient doesn’t come to any further harm whilst in the care of clinicians’. Another commented that it is about, ‘trying not to make them [the patient] any worse than when they came in’. Whilst many students emphasised the avoidance of harm to patients, a significant number professed to a lack of clarity regarding what patient safety encompasses and where it features in the existing curriculum. Several students suggested that this lack of clarity had implications for students’ engagement with the topic. In a number of the focus groups, students described how patient safety topics were not explicitly identified within the curriculum. A year 2 student commented, ‘It’s not labelled. It’s not sort of introduced with: “This is patient safety”’. Students noted that, unlike other learning units, the patient safety longitudinal theme does not have an associated workbook or a clear structure; similarly, it is not identified by a single assessment.
Theme: Healthcare Culture
A variety of different aspects of healthcare culture were discussed and the five sub-themes identified were the hierarchy within healthcare and specifically within the medical profession; a blame culture and fear of the consequences of error, including litigation; the effect of external influences; the physical healthcare environment; and a perceived mismatch between the theory and application of clinical practice. Students at all stages of their training were keenly aware of their own positions within the hierarchy of healthcare. This perceived lack of importance impacted upon medical students’ willingness to intervene or report errors. Students had also observed that this hierarchy has a significant impact on junior doctors with potential implications for patient safety. One student commented:
They’ve literally just qualified as doctors and all of a sudden, you know, they’ve got this weight of expectation where they’re in this situation where they want to keep the patient safe but at the same time they don’t want to upset their seniors by coming to them with every single little query and it’s a very difficult balancing act and it’s quite scary, I think.
Students acknowledged that they had been taught that the appropriate response to error is to evaluate the system, as a whole, rather than seeking to attribute blame to an individual clinician. Nevertheless, this was perceived as a theory not borne out in practice. There were many comments made by students in year 2 and year 4 expressing concern that they might inadvertently harm patients and uncertainty about the consequences of making a mistake. It was noted that a trend towards increasing litigation in the wider society may also be contributing to creating a culture of blame. Throughout the focus groups, students made reference to factors external to healthcare. These included accounts of healthcare stories in the mass media, documentaries following junior doctors in training and a guest lecture given by a Member of Parliament related to the Francis Report (2013). The discussions between students suggested that external influences have a significant impact on shaping students’ understanding of patient safety.
Theme: Low Student Morale
Throughout the focus groups, particularly amongst year 4 students, it was apparent that morale was poor. Many students’ comments indicated low self-esteem, disgruntlement with the education system or disquiet about what the future held. Two sub-themes that became apparent were student disempowerment and an overly goal-driven educational system, typically referred to as a ‘tick box’ culture. Students repeatedly commented that they felt undervalued and several highlighted some of the implications this might have in terms of contributing to patient safety, as demonstrated by the quotations in Table 1. Students frequently lamented an emphasis on producing evidence of exposure to teaching rather than genuine meaningful learning. As a consequence of this ‘tick box’ culture, students reported that they wasted time pursuing signatures for skills they perceived themselves to be competent at, and conversely, were deprived of opportunities to practice other skills because they have already been ‘signed off’, despite not perceiving themselves to be competent.
Theme: Reporting Errors and Raising Concerns
There was extensive discussion between students on the subject of raising concerns. Students were conscious of their duty to report malpractice; however, the two sub-themes identified were a lack of clarity on how to raise concerns and the general perception that these may not be acted upon or students may be punished for doing so. Students in both year 2 and year 4 were not aware of mechanisms for reporting concerns. In addition, year 2 students, in particular, indicated uncertainty about what constituted a valid concern. A number of student shared anecdotes of their experiences of raising concerns. The majority of these stories described either punitive consequences for the student who reported the concerns or a lack of meaningful response.
Theme: Infection Control and Prevention
Students frequently identified aspects of infection control and prevention as an important element of patient safety. The year 2 students interviewed had recently received teaching relating to handwashing and the use of personal protective equipment; the recency of this teaching may have contributed to its prevalence in the focus groups. In addition to hand hygiene, students also reported teaching about utilising an aseptic, non-touch technique when carrying out procedural skills. However, students noted that the infection control and prevention measures that they were being taught were often not adhered to in the clinical setting; this mismatch between the educational and clinical contexts was identified as a further sub-theme.
Theme: Technical/Procedural Safety
Students repeatedly identified clinical skills as another aspect of patient safety. Several facets of procedural safety were highlighted, for example, cannulation and venepuncture. One student talked about checking habits and another described post-procedural monitoring. Students expressed anxiety about a lack of opportunity to practice clinical skills and the importance of simulated practice prior to undertaking procedures on patients. Another aspect of technical safety highlighted was the safe handling of patients and equipment. One student described the scenario of a patient falling and acknowledged that under certain circumstances, a compromise must be reached between patient safety and personal safety. The students’ responses suggested that they struggled with this dilemma.
Theme: Communication
Students identified communication and related facets as important elements of patient safety. The most common sub-theme within the topic of communication was information safety and confidentiality. Several students included information safety as part of their own definitions of patient safety; for example, one year 2 student said, ‘I think patient safety means taking care of the patient and that it encompasses many dimensions... Keeping confidentiality and also trying to maintain the health of the patient’. Nevertheless, several year 2 students expressed uncertainty about the application of what they had been taught.
Additionally, students recognised the importance of good documentation; however, writing in medical notes appeared to be a source of concern for a number of year 4 students. Some students feel ill equipped to do this and others expressed discontent that they were not provided with adequate time to document information in the clinical environment, for example, on a ward round. Finally, students also highlighted the role of adequate handover of clinical information. It was noted that the provision of teaching varied depending upon the locality at which the student was based for particular clinical placements.
Theme: Other Non-technical Skills
In addition to communication, students in the focus groups offered comment on a number of other non-technical skills; these included team-working and clinical prioritisation. Interprofessional events are frequently used to enable students to develop the skills required to work effectively as part of a team. Students expressed a mixture of responses to these teaching episodes; some were highly critical whilst others described what they had gained from them. Nevertheless, the importance of good team work to the safe operation of clinical work was acknowledged by year 2 and year 4 students alike. However, some students in year 4 reported that they did not consider themselves part of the healthcare team during clinical placements because they were not treated as such. One student suggested that, except on the rare occasion that a particular clinician intervened, ‘You are just sort of on the edge’.
Theme: Medication Safety
Aspects of prescribing and administering medications safely were a frequent topic of discussion including checking habits, patient identification and avoidance of unnecessary medications. A number of year 4 students lamented the lack of teaching about how to prescribe safely. Other students in the same focus group commented on a lack of opportunities to practice prescribing, particularly with appropriate supervision, and another noted that the growing use of electronic prescribing tools may limit opportunities on wards yet further.
Theme: Self-awareness
Students identified a number of different aspects of self-awareness that are important for patient safety. Three sub-themes were noted; knowing one’s limitations, reflective practice and personal health. In general, students described a keen awareness of their own limitations and this was frequently reflected in a lack of confidence in undertaking tasks in the clinical environment. Students volunteered phrases such as ‘working within your competence’ and ‘accepting that you might need to educate yourself’. One student stated that, ‘as a doctor or any part of the medical team, regardless of their status, you need to keep mindful of the fact that you need to do your part in terms of continually reflecting on what you’ve done wrong and so forth’. Curiously, some students have developed a degree of apathy towards reflection in clinical practice, although the reasons were not readily apparent from these focus groups. Year 2 students frequently identified an awareness of personal health as being important in maintaining patient safety. Interestingly, this sub-theme was not mentioned by year 4 students; this may be as a consequence of exposure to the different attitudes towards personal health that exist in the clinical environment.
Theme: Patient-Centredness
During the discourse on the definition of patient safety, one phase 1 student volunteered that patient-centredness lies at its core: ‘I think it’s just basically putting the patient first, like you do in terms of treatment, in terms of security and everything that you do’. Students identified this concept as being grounded in professional guidance from the General Medical Council.
Theme: Error Theory
When asked about what they had been taught on the topic of patient safety, a number of students made reference to theoretical aspects of error. These included the typology of errors, a systems approach and the Swiss cheese model of error propagation. Year 4 students observed that the relevance of teaching on error theory had not become apparent to them until the later stages of the medical course, when exposed to the clinical environment.
Theme: Learning Strategies
Unsurprisingly in a discourse on education, learning strategies provoked a great deal of discussion. Students often emphasised a desire to learn and expressed concern about their own failure to recognise key learning points. They offered suggestions on how to increase the visibility of patient safety as a critical overarching theme. They described teaching events they would welcome, including role play and simulation. Simulation exercises were noted to be intimidating but the anxiety they created was perceived to augment the memorability of the material being taught. In addition, they highlighted that simulation offers the opportunity for feedback following observed practice, something that is perceived to be lacking throughout the medical course. The observed behaviours of qualified clinicians serve as a powerful learning tool for students who lamented that there were few positive role models. Several students in both year 2 and year 4 talked about negative role models demonstrating sub-optimal practice and thereby encouraging students to develop ‘bad habits’.
Many students highlighted how their clinical experiences brought patient safety alive. One student commented, ‘Every time I think of patient safety I think of things that have happened to me on the job’. Students frequently made reference to case studies to develop their arguments during discussions. In the focus groups, students related examples such as the failings at the Mid Staffordshire NHS Foundation Trust, the Bristol heart scandal, wrong-site surgery, administration of chemotherapy via an incorrect route and the death of Elaine Bromiley.
In several of the focus groups with year 2 students, attendees initially appeared tentative about their understanding of patient safety. However, as discussions proceeded and they began to identify how patient safety was being taught in the existing curriculum, students became increasingly cognisant of the magnitude of the subject. This dawning of awareness is exemplified by a student who said, ‘It’s, like, been integrated into everything’ and another that commented, ‘As far as I can tell it’s [patient safety] absolutely across the board in everything we do, whether or not it’s explicit’. When asked to make suggestions about how patient safety education might be delivered, many students recommended that topics should be distributed throughout the course. Suggestions to achieve this included daily or weekly case studies on patient safety incidents in the early part of the course, forums to discuss students’ experiences relating to patient safety at the end of each clinical rotation and simulation exercises at a variety of points during the medical course.
Discussion
Listening to the perspective of medical students in the middle and latter stages of their training offered insights into how they understood the term ‘patient safety’ within their learning and preparation for practice. Medical students lacked clarity and understanding especially for the non-technical human factors, being more aware of technical competence. Although lectures and workshops in the early curriculum from social scientists had covered the theory of human behaviour, these non-technical concepts were not revisited and as a result appeared to be poorly understood. Similarly, we could not clearly identify where students would learn about factors which underpinned the importance of patient-centred safe practice. There was a clear distinction between early (year 2) and later (year 4) student’s understandings and foci. It was the senior students who raised concerns about the mismatch between what they were taught and what they observed in clinical practice, for example, poor adherence to infection control standards. The stance of qualified doctors towards patient safety also confused them especially about speaking up to raise concerns about poor practice.
It is crucial that medical students, as the change agents of the future, feel empowered to safeguard the welfare of patients and are able to raise safety concerns without fear of reprisal. Of concern was the feeling of disempowerment by students overwhelmed by a ‘culture of blame’ and of hierarchies leaving them with a lack of confidence in what to do when things go wrong and how to learn from error. Even more concerning was their fear that they themselves might be at the centre of something going wrong. Students felt disempowered to either challenge others in order to avoid errors or to report their concerns. This was most notable amongst year 4 students who were close to qualification and subsequent independent practice. Rees suggests that student disempowerment is one of the fundamental problems of outcomes-based or product-orientated curricula [29]. This correlates well with students’ frustrations at what they describe as a ‘tick box’ culture and a perceived lack of responsiveness to feedback. Tensions can arise between achieving co-operative student engagement in curriculum design and meeting the requirements of accrediting bodies.
The ideas from the students on teaching design were limited, although they perceived the value of early theoretical concepts contextualised in clinical practice, asking for case studies, role play and simulation. These aspirations require sufficient resource and investment in physical facilities such as simulation centres, trained faculty and adequate curriculum space. There has been a great deal of concern about the lack of opportunity to learn in interprofessional team-based settings which can address issues of hierarchy, changing attitudes and resulting in greater shared professional responsibility [15, 30]. Students will, however, continue to pick up the messages of what they see and hear. Medical school faculty members must act as positive role models cascading change to effect safer care.
As with all of these aspirations, faculty development is essential. There have been concerns that not enough faculty members understand the essential components for a patient safety curriculum, and there has been a failure to understand the associated skills which need to be taught [31, 32]. Real clinical episodes relating to patient safety offer a meaningful vehicle for learning from error, and this may be augmented by sharing with other team members, for example, in interprofessional morbidity and mortality meetings. Faculty staff require professional development sessions on the value of interprofessional practice learning, the pedagogical principles for interprofessional education, simulation and quality improvement.
Reassuringly, many students could relate topics as covered in the WHO Patient Safety Curriculum Guide, although the recent introduction of quality improvement was not understood. Patient safety remains a cross curriculum integration component with poor articulation of what is required at graduation and is often not labelled as safety in assessments; these students did not mention assessment. Students displayed a worrying apathy towards personal reflection which offers an assessment vehicle using electronic portfolios. This is not surprising as reflection is a difficult concept to grasp and is often used artificially.
The data produced by this study were used to inform curriculum re-design and, in particular, the way in which patient safety education is structured and delivered. We have set up a dedicated faculty patient safety team to integrate and align content across the science, professional practice and professionalism elements of our undergraduate medical curriculum. These outcomes offer a steer for how to integrate this important set of learning topics within a curriculum map. Curriculum design needs to align definitions and understandings of patient safety and related terms, for example, human factors, service improvement and related teaching to a readily-visible, assessed curriculum map.
The study has several limitations. It offers insights from a single medical school based on the curriculum set up to meet the GMC outcome standards as set out in 2009. The researchers practised reflexivity and were not seen as senior or significant figures with responsibility for curriculum design. The students were selected through a faculty member acting as a gatekeeper and, although larger samples were anticipated, were felt to be representative of their year groups. Students’ discussions during this study encompassed the majority of the major topic areas. Those omitted closely correlated with those identified as being incompletely taught during a synchronous review of the curriculum content, providing credibility for these findings.
Conclusion
A number of barriers have been described that have impeded progress in improving patient safety education. Patient safety is a subject that is unfamiliar to many educators and falls outside the traditional biopsychosocial sphere of teaching. Historically, medical teachers have not recognised patient safety as an essential component of the curriculum and there has been a failure to appreciate the associated skills to be taught. In addition, there has been a lack of a framework describing patient safety competencies, although the WHO Patient Safety Curriculum Guide now offers a clear steer for all caring professions.
Compliance with Ethical Standards
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
Ethical approval was granted for this study from the University of Nottingham Medical School Research Ethics Committee (Reference: CLT13122012MEU).
Informed Consent
Informed written consent was obtained from all study participants.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Andrew J. Batchelder, Phone: +44 (0)116 252 4730, Email: ajb80@le.ac.uk
Liz Anderson, Phone: +44 (0)116 252 3767, Email: esa1@le.ac.uk.
References
- 1.Brennan T, Leape L, Laird N, Herbert L, Localio A, Lawthers A. Incidence of adverse events and negligence in hospitalized patients. N Engl J Med. 1991;234:370–376. doi: 10.1056/NEJM199102073240604. [DOI] [PubMed] [Google Scholar]
- 2.Vincent C, Neale G, Woloshynowych M. Adverse events in British hospitals: preliminary retrospective record review. BMJ. 2001;322:517–519. doi: 10.1136/bmj.322.7285.517. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Kohn L, Corrigan J, Donaldson M. To err is human: building a safer health system. Washington DC: National Academies Press; 2000. [PubMed] [Google Scholar]
- 4.Department of Health . An organisation with a memory: report of an expert group on learning from adverse events in the NHS. London: HMSO; 2000. [Google Scholar]
- 5.Health Foundation . The measurement and monitoring of safety. London: Health Foundation; 2013. [Google Scholar]
- 6.Francis R. Report of the mid Staffordshire NHS Foundation trust public inquiry. London: HMSO; 2013. [Google Scholar]
- 7.Manser T. Teamwork and patient safety in dynamic domains of healthcare: a review of the literature. Acta Anaesthesiol Scand. 2009;53:143–151. doi: 10.1111/j.1399-6576.2008.01717.x. [DOI] [PubMed] [Google Scholar]
- 8.Reeves S, Lewin S, Espin S, Zwarenstein M. Interprofessional teamwork for health and social care. Oxford: Wiley-Blackwell; 2010. [Google Scholar]
- 9.Dekker S. The field guide to understanding ‘human error’. Farnham: Ashgate; 2014. [Google Scholar]
- 10.Dekker SWA, Leveson NG. The systems approach to medicine: controversy and misconceptions. BMJ Qual Saf. 2014;24:7–9. doi: 10.1136/bmjqs-2014-003106. [DOI] [PubMed] [Google Scholar]
- 11.World Health Organization . Patient safety curriculum guide: multi-professional edition. Geneva: WHO Press; 2011. [Google Scholar]
- 12.Berwick D. A promise to learn—a commitment to act: improving the safety of patients in England. London: Department of Health; 2013. [Google Scholar]
- 13.Gurses AP, Ozok AA, Provonost PJ. Time to accelerate integration of human factors and ergonomics in patient safety. BMJ Qual Saf. 2012;21:347–351. doi: 10.1136/bmjqs-2011-000421. [DOI] [PubMed] [Google Scholar]
- 14.Bleakley A. Broadening conceptions of learning in medical education: the message from teamworking. Med Educ. 2006;40:150–157. doi: 10.1111/j.1365-2929.2005.02371.x. [DOI] [PubMed] [Google Scholar]
- 15.Anderson ES, Gray R, Price K. Patient safety and interprofessional education: a report of key issues from two interprofessional workshops. J Interprof Care. 2016;31:154–163. doi: 10.1080/13561820.2016.1261816. [DOI] [PubMed] [Google Scholar]
- 16.Waterson P, Catchpole K. Human factors in healthcare: welcome progress, but still scratching the surface. BMJ Qual Saf. 2016;25:480–484. doi: 10.1136/bmjqs-2015-005074. [DOI] [PubMed] [Google Scholar]
- 17.Sandars J, Bax N, Mayer D, Wass V, Vickers R. Educating undergraduate medical students about patient safety: priority areas for curriculum development. Med Teach. 2007;29:60–61. doi: 10.1080/01421590601087546. [DOI] [PubMed] [Google Scholar]
- 18.Kerfoot BP, Conlin PR, Travison TT, McMahon GT. Patient safety knowledge and its determinants in medical trainees. J Gen Intern Med. 2007;22:1150–1154. doi: 10.1007/s11606-007-0247-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Ginsburg LR, Tregunno D, Norton PG. Self-reported patient safety competence among new graduates in medicine, nursing and pharmacy. BMJ Qual Saf. 2013;22:147–154. doi: 10.1136/bmjqs-2012-001308. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Nie Y, Li L, Duan Y, Chen P, Barraclough BH, Zhang M, Li J. Patient safety education for undergraduate medical students: a systematic review. BMC Med Educ. 2011;11:33. doi: 10.1186/1472-6920-11-33. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.General Medical Council . About the outcomes for graduates: working with doctors and working for patients. Consultation document. London: GMC; 2017. [Google Scholar]
- 22.Knowles M. The adult learner: a neglected species. Houston: Gulf Publishing; 1973. [Google Scholar]
- 23.Bandura A. Social foundations of thought and action: A social cognitive theory. Englewood Cliffs: Prentice Hall; 1986. [Google Scholar]
- 24.Schön DA. The reflective practitioner: how professionals think in action. New York: Basic Books; 1983. [Google Scholar]
- 25.Kolb DA. Experiential learning: experience as the source of learning and development. Englewood Cliffs: Prentice Hall; 1984. [Google Scholar]
- 26.Denzin NK, Lincoln YS. The sage handbook of qualitative research. 3. Thousand Oaks: Sage Publications; 2005. Introduction: the discipline and practice of qualitative research; pp. 1–32. [Google Scholar]
- 27.Kuper A, Reeves S, Levinson W. An introduction to reading and appraising qualitative research. BMJ. 2008;337:404–407. doi: 10.1136/bmj.a288. [DOI] [PubMed] [Google Scholar]
- 28.Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3:77–101. doi: 10.1191/1478088706qp063oa. [DOI] [Google Scholar]
- 29.Rees CE. The problem with outcomes-based curricula in medical education: insights from educational theory. Med Educ. 2004;38:593–598. doi: 10.1046/j.1365-2923.2004.01793.x. [DOI] [PubMed] [Google Scholar]
- 30.Newton J. Group conformity: the legacy continues. Med Educ. 2014;48:842–843. doi: 10.1111/medu.12531. [DOI] [PubMed] [Google Scholar]
- 31.Walton MM. Teaching patient safety to clinicians and medical students. Clin Teach. 2007;4:1–8. doi: 10.1111/j.1743-498X.2007.00187.x. [DOI] [Google Scholar]
- 32.Ladden MD, Bednash G, Steves DP, Moore GP. Educating interprofessional learners for quality, safety and systems improvement. J Interprof Care. 2006;20:497–505. doi: 10.1080/13561820600935543. [DOI] [PubMed] [Google Scholar]