Conflict of interest
All authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Editor
The COVID‐19 pandemic has caused more than 168 million people to be infected and 3 million people to die. 1 Although the COVID‐19 vaccination work for the general population has been started, herd immunity cannot be achieved in the short term. 2 Wearing masks is still the most effective means for the public to prevent and control the spread of COVID‐19. However, the occurrence of facial skin problems caused by wearing masks may, under some conditions, influence the maintenance of mask wearing among the public. We conducted a cross‐sectional survey through online and offline questionnaires to explore the characteristics of facial skin problems and microbiome variation during wearing masks for fighting against COVID‐19, from 30 May to 1 July 2020. Among them, 19 subjects were recruited for microbiome detection. Facial skin problems were defined as suffering from itching, stress injury, allergic dermatitis, fungal skin disease and skin maceration while wearing masks against COVID‐19.
A total of 4385 valid questionnaires were finally obtained and analysed. Among them, 1981 (45.2%) were male. The average age of the participants was 31.1 ± 11.6 years. Overall, 1323 (33.1%) participants reported having facial skin problems while wearing masks. The incidence of facial skin problems was the highest in the age group of 20–30 years (38.4%), those living in suburbs (35.2%) and those with an occupation in the public services (44.5%). Medical personnel had a high incidence of facial skin problems (40.0%). The incidence was also significantly different among different skin types (Fig. 1). The most common type of facial skin problem was indentation/crush (13.2%), followed by allergic dermatitis (11.1%) and acne/worsening of acne (9.9%). More than half of the patients with facial skin problems experienced healing within a week (54.7%). Although there was no significant difference in genus Simpson index and number of genus (P > 0.05), the diversity of the facial microbiome showed a decreasing trend after wearing masks. We found a significant change in the functional pathways of the microbiome (P = 0.0095 and P = 0.011) and a remarkable decrease in distance after wearing masks in both the dry and oily zones (P < 0.05; Fig. 2).
Figure 1.
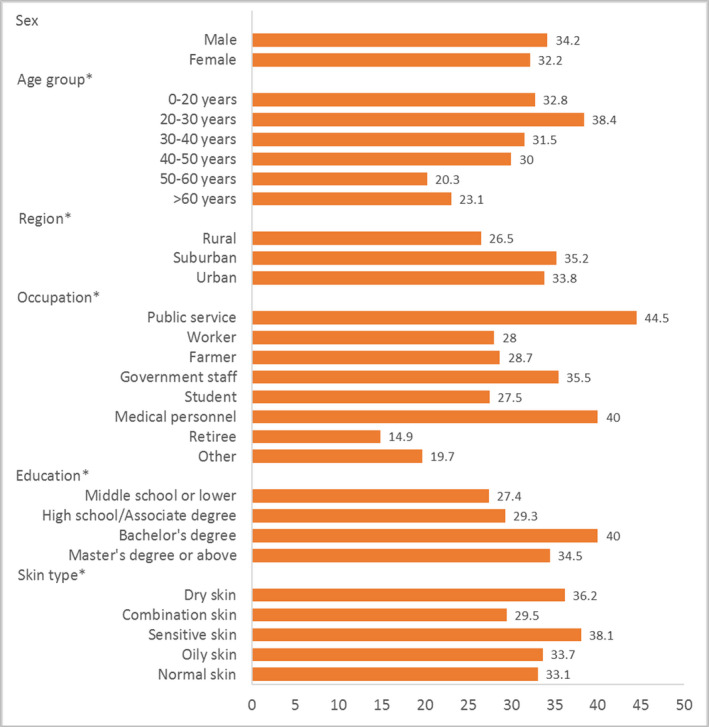
The incidence of facial problems among subgroups.
Figure 2.
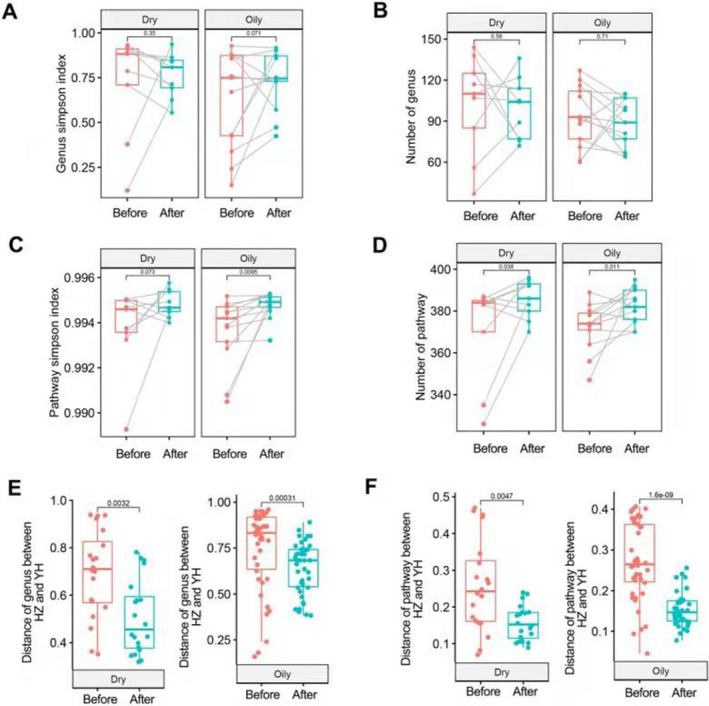
Changing of facial microbiome related to wearing masks.
Facial skin problems are noticeable public health problems for individuals wearing masks. 3 Although there is consensus on the importance of protection against skin injuries among medical staff fighting against COVID‐19, there were no unified protection guidelines for the general population so far. We found that more than 34% of participants experienced skin problems occurring on the cheek and the bridge of the nose, which was consistent with the results of Jiang et al. 4 The incidence of indentation was the highest. This was caused by habits such as wearing the mask for too long or wearing it too tightly, but this issue disappears by itself under normal circumstances. Indentation experienced by medical staff is usually associated with close contact with the protruding parts of the stiff structure of the masks, so it is usually found in the cheekbones, behind the ears and on the bridge of the nose. The incidence of allergic dermatitis was the second highest. Although mild skin indentations may recover completely on their own, it is still recommended to actively use drug treatment and moisturizing cream for prevention.
There were significant differences in the incidence of skin problems between groups with different skin types. Those with sensitive skin had the highest incidence due to the extreme sensitivity to external stimuli. 5 Those with dry skin had a slightly higher incidence of facial skin problems than those with oily skin. Changes in the facial microbiome might partly explain the skin problems caused by long‐term mask wearing.
Funding source
This study was supported by grants from the National Natural Science Foundation of China (81672005, 81001271), the Mega‐Project of National Science and Technology for the 12th and 13th Five‐Year Plans of China (2018ZX10715‐014‐002, 2014ZX10004008, 2013ZX10004901, 2013ZX10004904 and 2011ZX10004‐901), the Key Joint Project for the Data Center of the National Natural Science Foundation of China (U1611264) and the Fundamental Research Funds for the Central Universities (2017FZA7004).
C. Huang, Q. Sun contributed equally to this study.
Contributor Information
L. Li, Email: ljli@zju.edu.cn.
A. Li, Email: lia@zju.edu.cn.
X. Liu, Email: hzliuxiaoyan@zju.edu.cn.
S. Yang, Email: yangshigui@zju.edu.cn.
References
- 1. WHO . WHO Coronavirus Disease (COVID‐19) Dashboard. 2020.
- 2. Gostin LO, Salmon DA. The dual epidemics of COVID‐19 and Influenza: vaccine acceptance, coverage, and mandates. JAMA 2020; 324: 335–336. [DOI] [PubMed] [Google Scholar]
- 3. Foo CCI, Goon ATJ, Leow Y‐H, Goh C‐L Adverse skin reactions to personal protective equipment against severe acute respiratory syndrome ? a descriptive study in Singapore. Contact Dermatitis. 2006; 55: 291–294. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Yan Y, Chen H, Chen L et al. Consensus of Chinese experts on protection of skin and mucous membrane barrier for health‐care workers fighting against coronavirus disease 2019. Dermatol Ther 2020; 33: e13310. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Misery L. Sensitive skin, reactive skin. Ann Dermatol Venereol 2019; 146: 585–591. [DOI] [PubMed] [Google Scholar]


