The currently available epidemiologic reports regarding children with COVID‐19 have suggested that critical cases are concentrated in adolescents rather than in younger children, although respiratory supports were rarely needed. 1 , 2 Above all, neonatal cases requiring mechanical ventilation are quite limited. 3
A 21‐day‐old term neonate, with an uneventful perinatal history, was admitted to a local hospital ward for isolation due to positive polymerase chain reaction test for severe acute respiratory syndrome coronavirus 2 (SARS‐CoV‐2). He was asymptomatic on admission although both parents had already been diagnosed with symptomatic COVID‐19 a few days before.
Six hours after admission, he rapidly developed hypoxemia with oxygen saturation of 89% in ambient air and mild tachypnea (50 breaths/min). Venous blood gas analysis revealed respiratory acidosis with partial pressure of carbon dioxide of 55 mmHg. Concerns about his rapid oxygenation deterioration and young age led to urgent intubation and transportation to the pediatric intensive care unit (PICU). 4
The patient was isolated in a negative‐pressure room in the PICU, and mechanical ventilation was initiated on deep sedation and muscle paralysis along with empiric administration of cefotaxime. Due to poor respiratory system compliance, the patient required high driving pressure of 16 cm of water above a positive end‐expiratory pressure of 8 cm of water to achieve a tidal volume of 6–7 mL/kg of bodyweight. Nevertheless, oxygenation was disproportionately maintained at PaO2/FiO2 ratio of approximately 300–400 mmHg. Chest radiograph and computed tomography revealed extensive bilateral infiltration in the dorsal lung areas, compatible with acute respiratory distress syndrome (Fig. 1), and the patient was diagnosed with severe COVID‐19 pneumonia. On PICU admission, complete blood count (hemoglobin 11.4 g/dL, white cell count 4.7 × 103 /µL, and platelet 3.5 × 105/µL) and inflammatory markers (C reactive protein <0.03 mg/dL) were normal. Liver and kidney function tests were also within normal ranges. Blood culture on admission was negative, and respiratory viral panel (FilmArray® Respiratory Panel 2.1, BioMeriéux, France) was also negative, except for SARS‐CoV‐2.
Fig. 1.
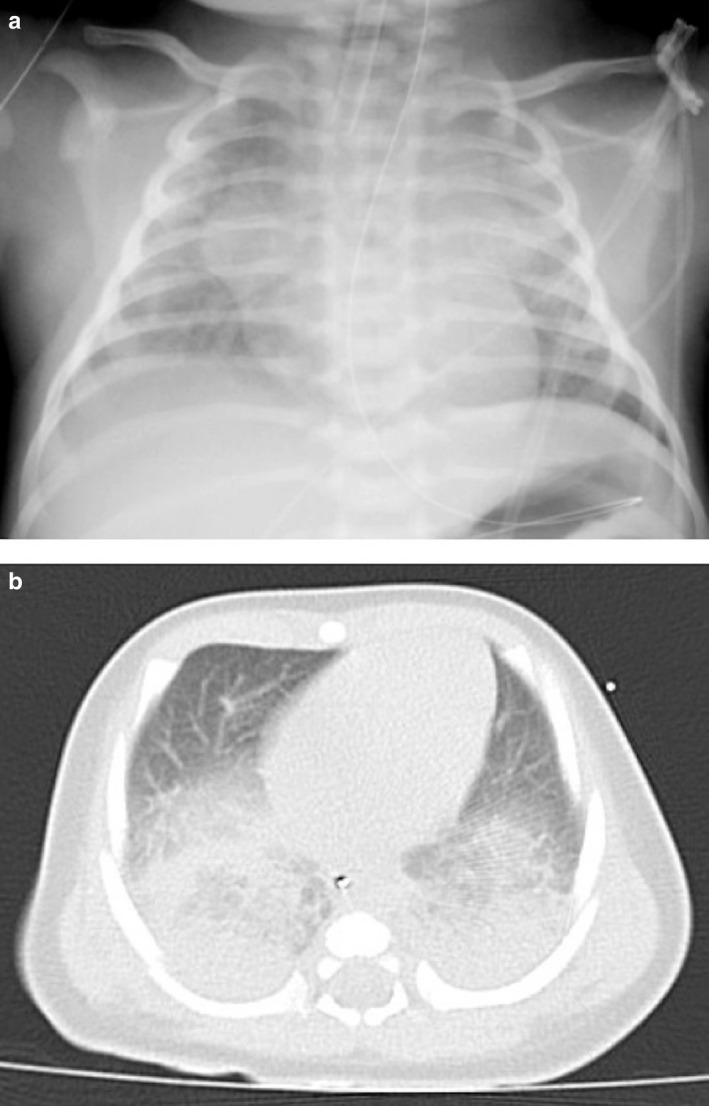
Chest computed tomography and radiograph images on PICU admission. The chest radiograph image showed diffuse opacities in the bilateral lungs (Panel a). The chest computed tomography image showed extensive bilateral infiltration in the dorsal lung areas (Panel b).
The patient was placed in a prone position from the second day of hospitalization for 48 h, aiming at recruitment of the collapsed dorsal lung areas. His oxygenation did not further deteriorate but noradrenaline infusion was needed to counteract hypotension due to deep sedation. No laboratory findings indicated multiorgan dysfunctions induced by hypercytokinemia, and respiratory mechanics gradually improved during ventilation in the prone position, even without pharmaceutical intervention, including dexamethasone and antiviral agents. He was liberated from ventilation on the fifth day, and his respiratory conditions continued to improve subsequently. He was discharged home without sequelae on the eighth day.
Although studies on neonatal COVID‐19 cases requiring invasive ventilation are quite limited, this case illustrates the possibility of rapid deterioration. In Japan, the main strategy for COVID‐19 focuses on cluster control, which leads to early investigation of the association between clusters and family transmission. Our case suggests that it could facilitate early detection of infected children and timely intervention to severe pediatric cases.
Disclosure
The authors declare no conflict of interest.
Author contributions
Ken Yakame, the first author, planned this report, conducted the literature search, and wrote the draft manuscript. Takayo Shoji, the second author, planned this report, conducted the literature search, and revised the manuscript. Takamori Kanazawa and Mitsunori Sato both planned this report and revised the manuscript. Tatsuya Kawasaki, the corresponding author, planned this report, conducted the literature search, and revised the manuscript including arranging English proof reading. All authors read and approved the final manuscript.
Informed consent
Written consent for publication was obtained from the patient’s parents.
References
- 1. Shekerdemian LS, Mahmood NR, Wolfe KK et al. Characteristics and outcomes of children with Coronavirus disease 2019 (COVID‐19) infection admitted to US and Canadian Pediatric Intensive Care Units. JAMA Pediatr. 2020; 174: 868–73. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2. Parri N, Lenge M, Buonsenso D. Children with Covid‐19 in pediatric emergency departments in Italy. N. Engl. J. Med. 2020; 383: 187–90. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Coronado Munoz A, Nawaratne U, McMann D, Ellsworth M, Meliones J, Boukas K. Late‐onset neonatal sepsis in a patient with Covid‐19. N. Engl. J. Med. 2020; 382: e49. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4. Götzinger F, Santiago‐García B, Noguera‐Julián A et al. COVID‐19 in children and adolescents in Europe: a multinational, multicentre cohort study. Lancet Child Adolesc. Heal. 2020; 4: 653–61. [DOI] [PMC free article] [PubMed] [Google Scholar]


