Abstract
Sepsis disproportionally affects people over the age of 65, and with an exponentially increasing older population, sepsis poses additional risks for cognitive decline. This review summarizes published literature for (1) authorship qualification; (2) the type of cognitive domains most often assessed; (3) timelines for cognitive assessment; (4) the control group and analysis approach, and (5) sociodemographic reporting. Using key terms, a PubMed database review from January 2000 to January 2021 identified 3050 articles, and 234 qualified as full text reviews with 18 ultimately retained as summaries. More than half (61%) included an author with an expert in cognitive assessment. Seven (39%) relied on cognitive screening tools for assessment with the remaining using a combination of standard neuropsychological measures. Cognitive domains typically assessed were declarative memory, attention and working memory, processing speed, and executive function. Analytically, 35% reported on education, and 17% included baseline (pre-sepsis) data. Eight (44%) included a non-sepsis peer group. No study considered sex or race/diversity in the statistical model, and only five studies reported on race/ethnicity, with Caucasians making up the majority (74%). Of the articles with neuropsychological measures, researchers report acute with cognitive improvement over time for sepsis survivors. The findings suggest avenues for future study designs.
Keywords: sepsis, cognitive assessment, aging
1. Introduction
Sepsis is one of the most common, expensive, and inadequately managed syndromes. A 2016 task force introduced an updated definition (Sepsis-3), explaining that sepsis is “a life-threatening organ dysfunction caused by a dysregulated host response to infection” [1,2,3,4]. Approximately 2 million adults are affected by sepsis within the United States annually with sepsis being responsible for one out of three hospital deaths [5,6]. Although the sepsis-associated hospitalization frequency has minimally changed for young individuals aged 18–49 years old, the hospitalization frequency has risen dramatically for those aged 65 and older, such that sepsis is currently considered a “disease of the aged” [2]. With increasing age, individuals with sepsis are more likely to endure critical illness with major organ damage resulting in chronic care conditions.
For the brain, sepsis might act as a major inflammatory stimulus and potentially increase the brain’s susceptibility to neurodegenerative disease [7,8]. Fitting with postulates of a brain reserve theory and threshold, sepsis may stimulate the deterioration of cognitive ability or enhance the risk for future progressive cognitive deterioration [9]. Brain health and cognition is also relevant to the risk of developing acute organ dysfunction [10]. By 2050, people aged 65 and older will reach 1.6 billion worldwide [11] and our healthcare system will face greater numbers of individuals with early to late-stage neurodegenerative disorders such as Alzheimer’s disease (AD) [12].
To assist sepsis cognitive research going forward, we conducted the current review to provide insight into the strengths and weaknesses of published research addressing cognition following sepsis. We summarize study designs, the inclusion of a cognitive expert on the team, if authors considered the impacts of education, sex, race/ethnicity, the timeline of testing and inclusion of a baseline, the time of testing, the type of cognitive measures, the statistical approach, and findings. We provide conclusions regarding current limitations and strengths of this literature.
2. Materials and Methods
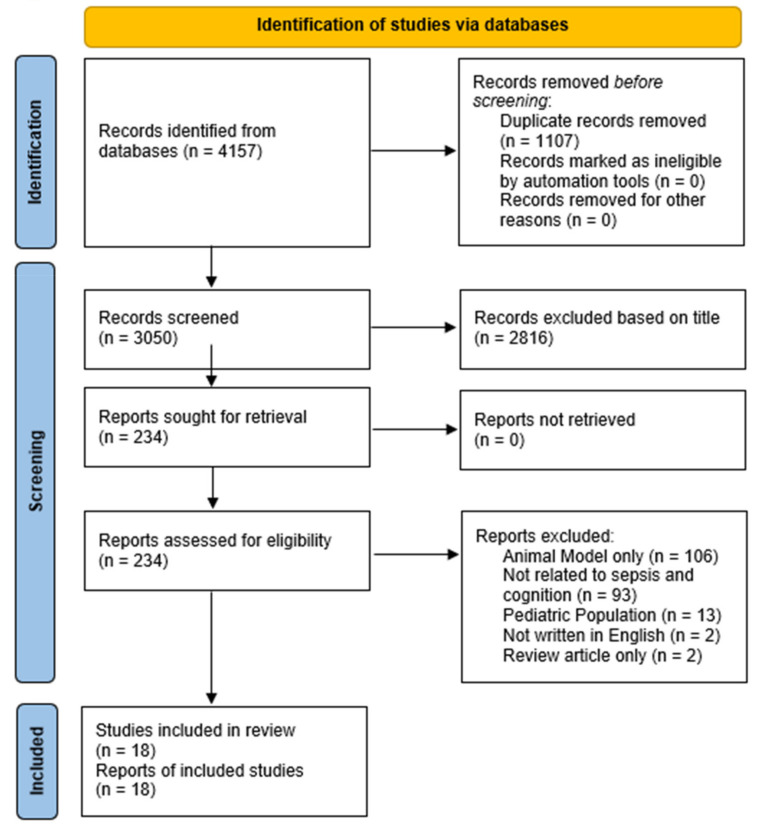
The literature review process included a thorough PubMed search for publications up to 13 January 2021 (See Figure 1). Key terms included: “sepsis and cognition”, which yielded 850, “sepsis and cognitive” (850), “sepsis and memory” (699), “sepsis and thinking” (642), and “sepsis and attention” (1962). Across these search terms a total of 3050 unique articles were identified, with 2816 articles removed based on keywords missing from the article titles, and with 234 qualifying as full text reviews. Of these, 18 met all inclusion criteria. To be eligible for inclusion, articles needed to have a population with a mean age of ≥18 years, a quantitative assessment of a cognition post-septic episode, they needed to be peer-reviewed (i.e., no dissertations), and they needed to be written in English. No limits were placed on the date of publication or timeframe of the cognitive assessment.
Figure 1.
Publication Identification Process.
3. Results
3.1. Author Inclusion of Neuropsychology Expert and Study Design
Of the 18 retained articles [13,14,15,16,17,18,19,20,21,22,23,24,25,26,27,28,29,30], 61% of them included a neuropsychologist as a co-author. 66.7% of studies used longitudinal designs, while 33.3% used cross-sectional designs.
3.2. Age, Education, Sex, Race and Ethnicity
The mean age ranged from 49 to 80.81 years across all studies, for a grand mean of 58.30 years. Analytically, 35% of studies considered premorbid intellectual abilities such as education, with a wide educational attainment range. Three studies (16.7%) reported a 7th grade education on average, four studies (22.2%) were comprised mainly of high school graduates (12 years), and two studies (11.1%) included mainly college graduates (16 years).
Fifteen studies (83.3%) reported on sex, which were generally evenly split across sexes with slightly more females (n = 1067) than males (n = 995).
Only five studies (27.8%) reported on race and/or ethnicity, with the majority of patients identifying as Caucasians (79.5%). Only three studies (16.7%) reported on the inclusion of patients identifying as Black/African-American, one study (5.6%) reported on individuals identifying as Hispanic, and one study (5.6%) reported on individuals identifying as Native American or other Pacific Islanders. See Table 1 for additional demographic information.
Table 1.
Demographic characteristics of the retained studies.
| 1st Author | Year | Sepsis Sample (n) | Control Sample (n) | Neuro Expert | Mean Age | Education Reported | Sex (male:female) |
Race/Ethnicity |
|---|---|---|---|---|---|---|---|---|
| Regazzoni [13] | 2008 | 137 | No | No | 80.81 | NR | 67:70 | NR |
| Girard [14] | 2010 | 77 | No | Yes | 61 | Median = 12 (IQR = 10–13) years | 40:37 | NR |
| Iwashyna [15] | 2010 | 623 | No | No | 76.9 | NR | 281:362 | Black: 128 Hispanic: 44 White: 451 |
| Davydow [16] | 2012 | 517 | No | No | 76.1 | ≤HS = 38.5%; Some College = 34.8; >College degree = 26.7% | 235:282 | White: 416 Black: 95 Other: 6 |
| Merli [17] | 2013 | 31 | Yes (23) | No | NR | NR | NR | NR |
| Semmler [18] | 2013 | 25 | Yes (19) | Yes | 55.64 | NR | 13:12 | NR |
| Götz [19] | 2015 | 36 | Yes (30) | Yes | 59.8 | NR | 24:12 | NR |
| Götz [20] | 2016 | 36 | Yes (30) | Yes | 59.8 | NR | 24:12 | NR |
| Needham [21] | 2016 | 83 | Yes (106) | Yes | 52 | Mean = 13.9 ± 2.2 years | 39:44 | White: 68 Non-White: 15 |
| Pierrakos [22] | 2017 | 28 | No | Yes | 67.3 | NR | NR | NR |
| Brown [23] | 2018 | 40 | No | Yes | NR | <HS = 13%; HS = 20%; Associate degree = 18%; Higher education = 10% | 19:21 | NR |
| Calasavara [24] | 2018 | 33 | No | Yes | 49 | Mean = 7 (IQR = 4–8) years | 14:19 | NR |
| Kang [25] | 2018 | 36 | No | No | 67.8 | Mean = 7.4 ± 5.8 years | 29:7 | NR |
| Orhun [26] | 2019 | MMSE < 24 = 7 MMSE 24–30 = 14 |
Yes (33) | Yes | MMSE < 24: 57.3 ± 3.1 MMSE 24–30: 53.2 ± 3 |
MMSE < 24: Mean = 7.1 ± 1.1 years MMSE 24–30: Mean = 8.7 ± 1.0 years |
MMSE < 24 = 4:3 MMSE 24–30 = 8:6 |
NR |
| Seidel [27] | 2019 | 20 | Yes (44) | Yes | 53.8 | NR | 9:11 | NR |
| Mankowski [28] | 2020 | 328 | No | No | Young group = 35 Middle group = 58 Old group = 72 |
NR | 176:152 | White: 293 African American: 30 American Indian: 1 Other: 1 Unknown: 1 |
| Brown [29] | 2021 | 30 | No | Yes | 56 | <HS = 10%; HS = 23%; Some College = 33%; Associate degree = 7%; Bachelor degree = 17%; >Bachelor degree = 10% | 13:17 | Asian: 1 Native Hawaiian/other pacific islander: 1 White: 28 |
| Wang [30] | 2021 | 840 | Yes (20,893) | No | 64.3 | <HS = 12.7%; HS = 26.8%; Some College = 29.3%; >College = 31.2% | NR in the final sample | NR in the final sample |
Abbreviations: HS = High School; IQR = Interquartile Range; MMSE = Mini-Mental State Exam; NR = Not Reported.
3.3. Baseline and Time of Testing
Few studies (17%) included baseline cognitive testing (pre-sepsis data), making it difficult to accurately identify cognitive change from premorbid abilities. Initial cognitive testing occurred within two months of hospital discharge for nine studies (50%), with seven of those assessments being within 48 h of discharge. Twelve articles (66.7%) had at least one follow-up assessment, and eleven of them conducted at least two follow-up testing sessions, providing data for the course of cognitive changes and recovery post sepsis. See Table 2 for more information on cognitive testing.
Table 2.
Study designs and cognitive testing measures.
| 1st Author | Year | Baseline Testing | Time of Testing | Tests (Estimated Length) | Cognitive Domains | Reported Score |
|---|---|---|---|---|---|---|
| Regazzoni [13] | 2008 | No | Admit | MMSE (10’) | Global | Raw score |
| Girard [14] | 2010 | No | 3 months, 12 months post sepsis | MMSE, WAIS-III DS, TMT A&B, Coding, RAVLT, RCFT (Copy & Delay), VF (70’) | Global, ATT, DM, PS, VC, WM |
T-scores (age and education adjusted based on specific population norms) |
| Iwashyna [15] | 2010 | Yes | 1998—death or 2006 | M-TICS (10’) | Global | % of cognitive impairment in sample |
| Davydow [16] | 2012 | Yes | Mean = 7y post sepsis | TICS or TICS-27 (10’) | Global | TICS raw score |
| Merli [17] | 2013 | No | Admit, 3 months post discharge | MMSE, TMT A & B, Digit Symbol (18’) | Global, ATT, PS, WM | Z-Scores (test specific population norms) |
| Semmler [18] | 2013 | No | 6–24 months post discharge |
German Vocab. Test, NeuroCogFx, TMT A&B, AVLT, RCFT (70’) | ATT, DM, FM, PI, STM, VF | Mean unweighted score, (zDiff) = ((Cognitive Test z-score) − (Multiple Choice Word Test-B z-score))) (test specific population norms) |
| Götz [19] | 2015 | No | 0–2 months, 5–8 months, 10–15 months post ICU discharge | DemTect & CDT (15’) | Global | DemTect raw score |
| Götz [20] | 2016 | No | 0–2 months, 5–8 months, 10–15 months post ICU discharge | DemTect & CDT (15’) | Global | DemTect raw score |
| Needham [21] | 2016 | No | 6 months and 12 months post ICU discharge | Hayling Sentence Completion Test, VF, WAIS-III Similarities & DS, WMS-III LM (50’) | ATT, DM, EF, VR, WM | Percentage of scores 1.5 SD below the mean |
| Pierrakos [22] | 2017 | No | Sepsis discharge (~8d post sepsis onset) | MMSE, CDT (15’) | Global | MMSE raw score & MMSE recall sub-score |
| Brown [23] | 2018 | No | Sepsis discharge, 3 months, 6 months | MoCA, VF, WAIS-IV DS Similarities, WMS-IV LM, Hayling Sentence Completion Test (70’) | Global, ATT, DM, EF, VF, VR, WM | Percentage of scores 1.5 SD and 2.0 SD below the mean (test specific population norms) |
| Calasavara [24] | 2018 | No | 24 h post discharge, 1 year (median 393 days) | MMSE, CERAD (Verbal Fluency, TMT A&B, BNT, List Learning, Praxis, List Recall & Recognition, Praxis Recall) (70’) | Global, DM, EF, Language (naming, comprehension), PS, VF | MMSE raw score, CERAD mean scores |
| Kang [25] | 2018 | No | 48 hours after ICU admit | K-MoCA; K-MMSE; CoSAS-S (30’) | Global | Raw scores |
| Orhun [26] | 2019 | No | 0, 3 months, 12 months post sepsis | MMSE & ACE-R (Orientation-attention, Memory, VF, Language, Visuospatial Function) (35’) | Global | MMSE raw scores; ACE-R Sub-scores means |
| Seidel [27] | 2019 | No | 2.6 ± 1.9 years post sepsis | TAP, Go-No-Go paradigm, German version of AVLT (40’) | ATT, DM, WM | T-scores (age-adjusted based on test specific population norms) |
| Mankowski [28] | 2020 | No | 3, 6, 12 months post discharge | MMSE, HVLT-R (Total recall, Delayed recall, Retention), COWA (30’) | Global, DM, VF | Mean raw scores |
| Brown [29] | 2021 | No | 6 months post discharge | Hayling Sentence Completion Test (5’) | EF | Mean raw scores |
| Wang [30] | 2021 | Yes | 6 months post sepsis; every 2 years (2006–2017) | SIS, CERAD: WLL, WLD, AFT (20’) | Global | Mean raw scores |
Abbreviations: ACE-R = Addenbrooke’s Cognitive Examination Revised; AFT = Animal Fluency Test, ATT = Attention; AVLT = Auditory Verbal Learning Test; BNL = Below Normal Limits; BNT = Boston Naming Test; CERAD = Consortium to Establish a Registry for Alzheimer’s Disease, CoSAS-S = Computer Cognitive Senior Assessment System-Screen; COWA = Controlled Oral Word Association; DM = Declarative Memory; DS = Digit Span; EF = Executive Functioning; FM = Figural Memory; HS = High School; HVLT-R = Hopkins Verbal Learning Test - Revised; K-MMSE = Korean Mini Mental State Exam; K-MoCA = Korean-Montreal – Cognitive Assessment; MMSE = Mini Mental State Exam; MoCA = Montreal – Cognitive Assessment; NP = Neuropsychological; NR = Not Reported; PI = Premorbid Intelligence; RAVLT = Rey Auditory Verbal Learning Test; RCFT = Rey-Osterreith Complex Figure; SD = Standard Deviation; SIS = Six-Item Screener; STM = Short Term Memory; TAP = Test of Attentional Performance; TICS-27 = Telephone Interview for Cognitive Status-Modified; Six-Item Screener = TICS-M = Telephone Interview for Cognitive Status-Modified; TMT = Trail Making Test; VF = Verbal Fluency Test; VR = Verbal Reasoning; WM = Working Memory; WAIS-III = Weschler Adult Intelligence Scale Third Edition; WAIS-IV = Weschler Adult Intelligence Scale Fourth Edition; WLD = Word List Delayed Recall; WLL = Word List Learning; WM = Working Memory; WMS-III LM = Weschler Memory Scale Third Edition Logical Memory; WMS-IV LM = Weschler Memory Scale Fourth Edition Logical Memory.
3.4. Type of Measures, Congitive Domains, and Reported Scores
Seven studies (39%) only administered cognitive screening tools, with the remaining using a combination of standard neuropsychological measures. Cognitive domains typically included declarative memory, attention and working memory, processing speed, and executive function. Eleven studies (61%) used raw scores or mean raw scores, two studies (11.1%) reported percentages of scores falling 1.5 or 2 standard deviations below the mean, one study (5.6%) reported the percentage of cognitive impairment, two studies (11.1%) included t-scores (age and/or education adjusted), and two studies (11.1%) included z-scores.
3.5. Statistical Analyses
Studies varied in terms of the statistical modeling employed: correlation/regression models (50%), structural equation modeling (5.6%), general estimating equations (11.1%), survival models (5.6%), parametric and nonparametric tests for group comparisons (33.3%), concordance rate models (5.6%), receiver operating characteristics (5.6%), weighted network analyses (5.6%), and linear mixed models (5.6%). Three studies (16.7%) statistically corrected for education, two studies (11.1%) reported age-adjusted t-scores, and one study (5.6%) reported education-adjusted t-scores. See Table 3 for further detail on the statistical analyses.
Table 3.
Statistical Analyses and Corrections, and Summary of Cognitive Findings.
| 1st Author | Year | Statistical Method | Education Correction | Sex and/or Race Correction | Findings |
|---|---|---|---|---|---|
| Regazzoni [13] | 2008 | Cox proportional hazard model and Kaplan-Meier test | No | No | Sepsis survivor MMSE mean = 20.14; scores predicted 1-year mortality. |
| Girard [14] | 2010 | Multiple nonlinear regression, propensity score matching | Yes | No | Cognitive impairment at 3 months: 79% (62% severe); 12 months: 79% (36% severe). As duration of delirium increased, cognition decreased. |
| Iwashyna [15] | 2010 | Latent growth curve models, random effects models, and logistic regressions. | No | No | Rate of moderate or severe cognitive impairment among survivors (pre-sepsis) increased from 6.1% (95% CI: 4.2%, 8.0%) before severe sepsis to 16.7% (95% CI: 13.8%, 19.7%) at the 1st assessment after severe sepsis. |
| Davydow [16] | 2012 | Paired t-test, Pearson’s correlation, logistic regression. | No | No | Cognitive impairment in 18% of severe sepsis survivors. Pre-sepsis depression was the greatest predictor of post-sepsis cognitive impairment. |
| Merli [17] | 2013 | Logistic regression. | Yes | No | No sepsis survivors were cognitively impaired, but 42% of sepsis survivors showed a decline in performance. |
| Semmler [18] | 2013 | Student t-tests, Pearson’s correlation, ANOVA, and MANCOVA. | No; Estimated premorbid verbal abilities instead. | No | Sepsis survivors impaired in 8 of 9 subtests (mainly learning and memory). Non-septic ICU survivors showed deficits in 6 subtests. |
| Götz [19] | 2015 | General estimating equations. | No | No | Sepsis survivors were impaired on periodic visual stimulation (familiar and unfamiliar pictures) and scored lower than HCs on the DemTect and CDT at all time points. |
| Götz [20] | 2016 | General estimating equations. | No | No | Sepsis survivors scored lower than HCs on the DemTect and CDT at all time points. |
| Needham [21] | 2016 | Joint survival models, linear regressions and logistic random intercept regression models. | No | No | 38% at 6m post-sepsis had cognitive impairment; 28% at 12m. |
| Pierrakos [22] | 2016 | Multivariable linear regression. | If education >12 years, no MMSE was given; CDT only. | No | 50% of sepsis survivors had cognitive decline, with greatest decline in information recall. |
| Brown [23] | 2018 | Concordance correlation coefficient and Fisher’s exact tests. | No | No | At discharge, 90% of survivors had MoCA< 25 (BNL). At 3 months, 70% BNL; 6 months, 57% BNL. Neuropsychology: 3 months, 43% impaired; 6 months, 57% impaired. WAIS-IV DS was the one test performance that did not improve from 3 to 6 months. |
| Calasavara [24] | 2018 | Student t-test, Mann-Whitney U, chi-square test, one sample t-test, marginal models, stepwise regression. | No | No | At discharge, survivors had lower MMSE and poor constructional praxis (p < 0.001). At 1 year, all performances normalized except for the BNT (p = 0.193) and constructional praxis (p < 0.001). |
| Kang [25] | 2018 | Receiver Operating Characteristics. | No | No | 53.1% of sepsis survivors were cognitively impaired on MMSE; 65.6% of sepsis survivors were cognitively impaired on MoCA |
| Orhun [26] | 2019 | Mann-Whitney U or Kruskal-Wallis tests, Dunn’s post-hoc test, Spearman correlation. | No | No | Initial mean MMSE = 25.4 ± 3.9; 3 months: 27.8 ± 2.8; 12 months: 28.4 ± 1.4 |
| Seidel [27] | 2019 | Two-tailed student t-test, Pearson correlation. | No | No | 55% of survivors had deficits in 1–2 domains and 20% in 3 or more domains. Primary difficulties in learning, alertness, working memory, and memory decay rate. |
| Mankowski [28] | 2020 | Fisher exact test and Kruskal-Wallis test. | No | No | Young adults performed better than middle-aged and older adults. No group differences between the middle-aged and older adults. |
| Brown [29] | 2020 | Weighted network analysis. | No | No | 20% of survivors had impairment in executive domain according to the Hayling Sentence Completion Test |
| Wang [30] | 2021 | Multivariable linear mixed-effects models. | Yes | No | SIS scores of sepsis survivors improved. AFT scores decreased, while WLD and WLL scores increased. |
Abbreviations: AFT = Animal Fluency Test, ANOVA = Analysis of Variance; BNL = below normal limits; CDT = clock drawing test; CI = confidence interval; HC = Healthy Controls; ICU = Intensive Care Unit; MANCOVA = Multiple Analysis of Covariance; MoCA = Montreal Cognitive Assessment; MMSE = Mini Mental State Examination; SD = Standard Deviation; SIS = Six-Item Screener; WLD = Word List Delayed Recall; WLL = Word List Learning.
4. Discussion
Relevant research articles reviewed herein span 13 years (February 2008 to January 2021). The 18 publications addressing cognition varied with regards to the study design, demographic reporting, cognitive test type, and statistical approach. Despite 18 published articles, we continue to have a limited understanding of sepsis and cognition. Strengths include the number of studies considering cognitive domains in addition to general cognitive screeners, as well as the inclusion of an expert in cognitive assessment as part of the study team panel. Eleven studies report at least two follow-up testing sessions. Initial cognitive testing occurred within two months of hospital discharge for nine studies, with seven of those assessments being within 48 h of discharge. Across the publications, the themes suggest an acute decrease in cognitive function, with follow-up assessments showing cognitive improvement from acute levels. However, few studies considered premorbid or demographic factors within the statistical model, and less than half included a non-sepsis peer group to calculate practice effects. These design limitations challenge the accuracy of study findings, for there are associations between premorbid status and cognitive change [31,32,33,34], and there is a value to considering practice effects in post-trauma cognitive change models [35,36,37]. Our review findings suggest avenues for improvement as the field of sepsis and cognitive research moves forward.
Although more than one third of studies limited their investigation to global cognitive screening tools, the remaining studies used a combination of neuropsychological measures primarily assessing attention/working memory and declarative memory. These domains involve neurological systems typically assaulted by common comorbidities often associated with sepsis and small vessel vascular disease such as hypertension and diabetes [38,39,40]. Two studies additionally considered subdomains of measures of language (semantics) [21,23], and two looked at subdomains of higher cortical abstract reasoning [21,29], but they were limited in sample size. Hypothetically, within larger samples, comparing semantics and higher order functions to the more “vulnerable” cognitive domains would guide insight into cortical versus subcortical/white matter contributions, neuronal vulnerability, and potential mechanisms [41,42]. Longitudinal studies comparing cognitive domains in larger samples are needed.
Control groups are discussed in eight of the published investigations. Control groups used within a statistical design can provide information on “non-disease” practice effects as well as provide normative reference sources for calculating a standardized individual composite reliable change score [34,36,37,42]; the change is larger than reasonably expected due to the measurement error alone [43]. Control groups provide a reference for the expected performance. This information is particularly valuable when a researcher is concerned about the psychometric properties of cognitive measures (e.g., range of possible scores, normal distribution) and the test appropriateness for the population of interest (i.e., one would not administer a 16-word verbal list learning test to individuals with moderate cognitive impairment, for this would likely result in a poor performance and a floor effect). Patients who are acutely ill or cognitively compromised may perform at floor level; the test may be too difficult or not appropriate for identifying further deterioration. By contrast, individuals with a superior premorbid cognitive reserve who acquire sepsis may not be challenged appropriately with general cognitive screening tests. Control groups provide the research team with an external comparison to examine expected patterns of performance without complication from the disease state [37,42].
There was also a notable absence in the publications of the reporting of the years of education. Half of the publications reported this variable, and three considered education years in the statistical model. Given the wealth of research showing how education is a proxy for cognitive reserve, we consider the absence of educational reporting a concerning finding. The years of education have been used repeatedly in aging studies to help explain variability in cognition relative to pathology [44,45]. Cognitive reserve proxies, such as education, are shown to protect against impairment from traumatic brain injury [31,32,33] or operative/anesthesia exposure [34]. Considering education in analytical approaches may explain important variabilities in the outcome. The years of education are also a vital consideration if research teams are unable to acquire a premorbid/pre-sepsis cognitive estimation using formal test tools [46].
Sociodemographic considerations were limited, as was a consideration of medical comorbidities. Animal models [47] and some human studies [48,49] report sex as an important predictor of sepsis recovery. However, no study reported findings relative to participants’ sex. Although race or ethnicity were reported in five of the 18 studies, no study considered these variables relative to the cognitive trajectory. Today, we appreciate how race and ethnicity are surrogates for appreciating health disparities’ contribution to neurobiological responses [50]. Social determinants of health, including systemic racism experienced by many communities of color, are known to have negative ramifications on health outcomes and recovery [51,52,53]. It remains unknown if or how the cognitive sequela of sepsis differentiates across sex, race, and ethnicity. Sex, race, and ethnicity are proxies for health disparities and may modify neurobehavioral responses. This is an important area for future research. Further, individuals within different sociodemographics have a unique risk of sepsis (i.e., renal disease, congestive heart failure, myocardial infarction, chronic pulmonary disease, liver disease, peripheral vascular disease, peptic ulcer disease, and connective tissue disease) [38], and these are worthy of consideration relative to the pre-sepsis neuronal vulnerability status. We also identified a considerable patient heterogeneity in the current state of the literature with regards to the demographic characteristics and origin of sepsis. These are relevant design considerations.
Based on the current review, the authors consider sepsis cognitive research to be in an early developmental stage. There are noticeable methodological study design weaknesses that limit confidence in study findings. We encourage future researchers to consider study design suggestions from the fields of epilepsy (see [54] for a review of neuropsychology and epilepsy) and perioperative cognitive research—both of which have aggressively addressed challenges in longitudinal cognitive study design problems since the 1990s [42]. While sepsis poses a unique challenge due to the unexpected nature of the illness, researchers may wish to consider the benefits of including a control group, premorbid intellectual estimates, education, and other sociodemographic factors in future investigations. It should be noted that our review spanned a considerable timeframe (from February 2008 to January 2021), where the definition and management of sepsis rapidly evolved. We encourage a repeated literature review over the next 5 years.
Author Contributions
Conceptualization: L.C.J., C.C.P. and P.A.E.; Methodology: L.C.J., C.D. and C.C.P.; Data Curation: L.C.J. and C.D.; Writing—original draft preparation: L.C.J.; Writing—review and editing: C.D. and C.C.P.; Supervision: C.C.P. and P.A.E. All authors have read and agreed to the published version of the manuscript.
Funding
This research was supported by NIH K07 AG066813.
Institutional Review Board Statement
Not applicable.
Informed Consent Statement
Not applicable.
Conflicts of Interest
The authors declare no conflict of interest.
Footnotes
Publisher’s Note: MDPI stays neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Gotts J., Matthay M. Sepsis: Pathophysiology and clinical management. BMJ. 2016;353:i1585. doi: 10.1136/bmj.i1585. [DOI] [PubMed] [Google Scholar]
- 2.Kumar G., Kumar N., Taneja A., Kaleekal T., Tarima S., McGinley E., Jimenez E., Mohan A., Khan R.A., Whittle J., et al. Nationwide Trends of Severe Sepsis in the 21st Century (2000–2007) Chest. 2011;140:1223–1231. doi: 10.1378/chest.11-0352. [DOI] [PubMed] [Google Scholar]
- 3.Martin G.S., Mannino D., Eaton S., Moss M. The Epidemiology of Sepsis in the United States from 1979 through 2000. N. Engl. J. Med. 2003;348:1546–1554. doi: 10.1056/NEJMoa022139. [DOI] [PubMed] [Google Scholar]
- 4.Singer M., Deutschman C.S., Seymour C.C., Shankar-Hari M., Annane D., Bauer M., Bellomo R., Bernard G.R., Chiche J.-D., Coopersmith C.C.M., et al. The Third International Consensus Definitions for Sepsis and Septic Shock (Sepsis-3) JAMA. 2016;315:801–810. doi: 10.1001/jama.2016.0287. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Hajj J., Blaine N., Salavaci J., Jacoby D. The “Centrality of Sepsis”: A Review on Incidence, Mortality, and Cost of Care. Healthcare. 2018;6:90. doi: 10.3390/healthcare6030090. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Rhee C., Jones T.M., Hamad Y., Pande A., Varon J., O’Brien C., Anderson D.J., Warren D.K., Dantes R.B., Epstein L., et al. Prevalence, Underlying Causes, and Preventability of Sepsis-Associated Mortality in US Acute Care Hospitals. JAMA Netw. Open. 2019;2:e187571. doi: 10.1001/jamanetworkopen.2018.7571. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Brummel N.E., Balas M.C., Morandi A., Ferrante L., Gill T., Ely E.W. Understanding and Reducing Disability in Older Adults Following Critical Illness. Crit. Care Med. 2015;43:1265–1275. doi: 10.1097/CCM.0000000000000924. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Hawkins R.B., Raymond S.L., Stortz J.A., Horiguchi H., Brakenridge S., Gardner A., Efron P.A., Bihorac A., Segal M., Moore F.A., et al. Chronic Critical Illness and the Persistent Inflammation, Immunosuppression, and Catabolism Syndrome. Front. Immunol. 2018;9:1511. doi: 10.3389/fimmu.2018.01511. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Satz P. Brain reserve capacity on symptom onset after brain injury: A formulation and review of evidence for threshold theory. Neuropsychologia. 1993;7:273–295. doi: 10.1037/0894-4105.7.3.273. [DOI] [Google Scholar]
- 10.Shen H.-N., Lu C.-L., Li C.-Y. Dementia Increases the Risks of Acute Organ Dysfunction, Severe Sepsis and Mortality in Hospitalized Older Patients: A National Population-Based Study. PLoS ONE. 2012;7:e42751. doi: 10.1371/journal.pone.0042751. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Wan H., Goodkind D., Kowal P.U.S. Census Bureau, International Population Reports. U.S. Government Publishing Office; Washington, DC, USA: 2016. P95/16-1, An Aging World: 2015. [Google Scholar]
- 12.Hebert L.E., Scherr P.A., Bienias J.L., Bennett D.A., Evans D.A. Alzheimer Disease in the US Population Prevalence Estimates Using the 2000 Census. [(accessed on 30 July 2021)];Arch. Neurol. 2003 60:1119–1122. doi: 10.1001/archneur.60.8.1119. Available online: https://jamanetwork.com. [DOI] [PubMed] [Google Scholar]
- 13.Regazzoni C.J., Zamora R.J., Petrucci E., Pisarevsky A.A., Saad A.K., Mollein D.D., Luna C.M., Poderoso J.J., De Mollein D. Hospital and 1-Year Outcomes of Septic Syndromes in Older People: A Cohort Study. J. Gerontol. Ser. A Boil. Sci. Med. Sci. 2008;63:210–212. doi: 10.1093/gerona/63.2.210. [DOI] [PubMed] [Google Scholar]
- 14.Girard T.D., Jackson J.C., Pandharipande P., Pun B.T., Thompson J.L., Shintani A.K., Gordon S.M., Canonico A.E., Dittus R.S., Bernard G.R., et al. Delirium as a predictor of long-term cognitive impairment in survivors of critical illness. Crit. Care Med. 2010;38:1513–1520. doi: 10.1097/CCM.0b013e3181e47be1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Iwashyna T.J., Ely E.W., Smith D.M., Langa K. Long-term Cognitive Impairment and Functional Disability Among Survivors of Severe Sepsis. JAMA. 2010;304:1787–1794. doi: 10.1001/jama.2010.1553. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Davydow D.S., Hough C.L., Langa K., Iwashyna T. Presepsis Depressive Symptoms Are Associated with Incident Cognitive Impairment in Survivors of Severe Sepsis: A Prospective Cohort Study of Older Americans. J. Am. Geriatr. Soc. 2012;60:2290–2296. doi: 10.1111/jgs.12001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Merli M., Lucidi C., Pentassuglio I., Giannelli V., Giusto M., Di Gregorio V., Pasquale C., Nardelli S., Lattanzi B., Venditti M., et al. Increased risk of cognitive impairment in cirrhotic patients with bacterial infections. J. Hepatol. 2013;59:243–250. doi: 10.1016/j.jhep.2013.03.012. [DOI] [PubMed] [Google Scholar]
- 18.Semmler A., Widmann C.N., Okulla T., Urbach H., Kaiser M., Widman G., Mormann F., Weide J., Fliessbach K., Hoeft A., et al. Persistent cognitive impairment, hippocampal atrophy and EEG changes in sepsis survivors. J. Neurol. Neurosurg. Psychiatry. 2013;84:62–69. doi: 10.1136/jnnp-2012-302883. [DOI] [PubMed] [Google Scholar]
- 19.Götz T., Baumbach P., Huonker R., Kranczioch C., Witte O.W., Debener S., Klingner C., Brunkhorst F.M., Günther A. Slowed peak resting frequency and MEG overactivation in survivors of severe sepsis and septic shock. Clin. Neurophysiol. 2015;127:1247–1253. doi: 10.1016/j.clinph.2015.07.021. [DOI] [PubMed] [Google Scholar]
- 20.Götz T., Baumbach P., Reuken P., Huonker R., Kranczioch C., Debener S., Brunkhorst F.M., Witte O.W., Klingner C., Günther A. The loss of neural synchrony in the post septic brain. Clin. Neurophysiol. 2016;127:2200–2207. doi: 10.1016/j.clinph.2016.02.006. [DOI] [PubMed] [Google Scholar]
- 21.Needham D.M., Colantuoni E., Dinglas V.D., Hough C.L., Wozniak A.W., Jackson J.C., E Morris P., A Mendez-Tellez P., Ely E.W., O Hopkins R. Rosuvastatin versus placebo for delirium in intensive care and subsequent cognitive impairment in patients with sepsis-associated acute respiratory distress syndrome: An ancillary study to a randomised controlled trial. Lancet Respir. Med. 2016;4:203–212. doi: 10.1016/S2213-2600(16)00005-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Pierrakos C., Attou R., Decorte L., Velissaris D., Cudia A., Gottignies P., Devriendt J., Tsolaki M., De Bels D. Cerebral perfusion alterations and cognitive decline in critically ill sepsis survivors. Acta Clin. Belg. 2017;72:39–44. doi: 10.1080/17843286.2016.1191851. [DOI] [PubMed] [Google Scholar]
- 23.Brown S., Collingridge D.S., Wilson E.L., Beesley S., Bose S., Orme J., Jackson J., Hopkins R.O. Preliminary Validation of the Montreal Cognitive Assessment Tool among Sepsis Survivors: A Prospective Pilot Study. Ann. Am. Thorac. Soc. 2018;15:1108–1110. doi: 10.1513/AnnalsATS.201804-233OC. [DOI] [PubMed] [Google Scholar]
- 24.Calsavara A.J.C., Costa P.A., Nobre V., Teixeira A.L. Factors Associated With Short and Long Term Cognitive Changes in Patients With Sepsis. Sci. Rep. 2018;8:1–10. doi: 10.1038/s41598-018-22754-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Kang E.-Y., Jee S.J., Kim C.-S., Suh K.-S., Wong A.W., Moon J.Y. The feasibility study of Computer Cognitive Senior Assessment System-Screen (CoSAS-S) in critically ill patients with sepsis. J. Crit. Care. 2018;44:128–133. doi: 10.1016/j.jcrc.2017.10.005. [DOI] [PubMed] [Google Scholar]
- 26.Orhun G., Tuzun E., Ozcan P.E., Ulusoy C., Yildirim E., Küçükerden M., Gürvit H., Ali A., Esen F. Association between inflammatory markers and cognitive outcome in patients with acute brain dysfunction due to sepsis. Arch. Neuropsychiatry. 2018;56:63–70. doi: 10.29399/npa.23212. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Seidel G., Gaser C., Götz T., Günther A., Hamzei F. Accelerated brain ageing in sepsis survivors with cognitive long-term impairment. Eur. J. Neurosci. 2020;52:4395–4402. doi: 10.1111/ejn.14850. [DOI] [PubMed] [Google Scholar]
- 28.Mankowski R.T., Anton S.D., Ghita G.L., Brumback B., Cox M.C., Mohr A.M., Leeuwenburgh C., Moldawer L.L., Efron P.A., Brakenridge S.C., et al. Older Sepsis Survivors Suffer Persistent Disability Burden and Poor Long-Term Survival. J. Am. Geriatr. Soc. 2020;68:1962–1969. doi: 10.1111/jgs.16435. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Brown S.M., Beesley S.J., Stubben C., Wilson E.L., Presson A.P., Grissom C., Maguire C., Rondina M.T., Hopkins R.O. Postseptic Cognitive Impairment and Expression of APOE in Peripheral Blood: The Cognition After SepsiS (CASS) Observational Pilot Study. J. Intensiv. Care Med. 2021;36:262–270. doi: 10.1177/0885066619897604. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Wang H.E., Kabeto M.M., Gray M., Wadley V.G., Muntner P., Judd S.E., Safford M.M., Kempker J., Levine D.A. Trajectory of Cognitive Decline After Sepsis. Crit. Care Med. 2021;49:1083–1094. doi: 10.1097/ccm.0000000000004897. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Donders J., Stout J. The Influence of Cognitive Reserve on Recovery from Traumatic Brain Injury. Arch. Clin. Neuropsychol. Off. J. Natl. Acad. Neuropsychol. 2019;34:206–213. doi: 10.1093/arclin/acy035. [DOI] [PubMed] [Google Scholar]
- 32.Krch D., Frank L.E., Chiaravalloti N.D., Vakil E., DeLuca J. Cognitive reserve protects against memory decrements associated with neuropathology in traumatic brain injury. J. Head Trauma Rehabil. 2019;34:E57–E65. doi: 10.1097/HTR.0000000000000472. [DOI] [PubMed] [Google Scholar]
- 33.Steward K.A., Kennedy R., Novack T.A., Crowe M., Marson D.C., Triebel K.L. The Role of Cognitive Reserve in Recovery From Traumatic Brain Injury. J. Head Trauma Rehabil. 2018;33:E18–E27. doi: 10.1097/HTR.0000000000000325. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Monk T.G., Weldon B.C., Garvan C.W., Dede D.E., van der Aa M.T., Heilman K.M., Gravenstein J.S. Predictors of cognitive dysfunction after major noncardiac surgery. Anesthesiology. 2008;108:18–30. doi: 10.1097/01.anes.0000296071.19434.1e. [DOI] [PubMed] [Google Scholar]
- 35.Funder K.S., Steinmetz J., Rasmussen L.S. Methodological Issues of Postoperative Cognitive Dysfunction Research. Semin. Cardiothorac. Vasc. Anesthesia. 2010;14:119–122. doi: 10.1177/1089253210371520. [DOI] [PubMed] [Google Scholar]
- 36.Rasmussen L.S. Defining postoperative cognitive dysfunction. Eur. J. Anaesthesiol. 1998;15:761–764. doi: 10.1097/00003643-199811000-00026. [DOI] [PubMed] [Google Scholar]
- 37.Selnes O.A., Gottesman R.F., Grega M.A., Baumgartner W.A., Zeger S.L., McKhann G.M. Cognitive and Neurologic Outcomes after Coronary-Artery Bypass Surgery. N. Engl. J. Med. 2012;366:250–257. doi: 10.1056/NEJMra1100109. [DOI] [PubMed] [Google Scholar]
- 38.Yang Y., Yang K.S., Hsann Y.M., Lim V., Ong B.C. The effect of comorbidity and age on hospital mortality and length of stay in patients with sepsis. J. Crit. Care. 2010;25:398–405. doi: 10.1016/j.jcrc.2009.09.001. [DOI] [PubMed] [Google Scholar]
- 39.Lamar M., Price C., Libon D.J., Penney D.L., Kaplan E., Grossman M., Heilman K.M. Alterations in working memory as a function of leukoaraiosis in dementia. Neuropsychologia. 2007;45:245–254. doi: 10.1016/j.neuropsychologia.2006.07.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Price C.C., Jefferson A.L., Merino J.G., Heilman K.M., Libon D.J. Subcortical vascular dementia: Integrating neuropsychological and neuroradiologic data. Neurology. 2005;65:376–382. doi: 10.1212/01.WNL.0000168877.06011.15. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Price C.C., Tanner J.J., Monk T.G., Lydic R. Postoperative Cognitive Disorders. Neurosci. Found. Anesthesiol. 2011;19:255–269. doi: 10.1093/med/9780195398243.003.0135. [DOI] [Google Scholar]
- 42.Rasmussen L.S., Larsen K., Houx P., Skovgaard L.T., Hanning C.D., Moller J.T., ISPOCD Group The assessment of postoperative cognitive function. Acta Anaesthesiol. Scand. 2001;45:275–289. doi: 10.1034/j.1399-6576.2001.045003275.x. [DOI] [PubMed] [Google Scholar]
- 43.Jacobson N.S., Truax P. Clinical significance: A statistical approach to defining meaningful change in psychotherapy research. J. Consult. Clin. Psychol. 1991;59:12–19. doi: 10.1037/0022-006X.59.1.12. [DOI] [PubMed] [Google Scholar]
- 44.McQuail J.A., Dunn A.R., Stern Y., Barnes C.A., Kempermann G., Rapp P.R., Kaczorowski C.C., Foster T.C. Cognitive Reserve in Model Systems for Mechanistic Discovery: The Importance of Longitudinal Studies. Front. Aging Neurosci. 2021;12:532. doi: 10.3389/fnagi.2020.607685. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Stern Y., Arenaza-Urquiljo E.M., Bartrés-Faz D., Belleville S., Cantillon M., Chetelat G., Ewers M., Franzmeier N., Kempermann G., Kremen W.S., et al. Whitepaper: Defining and investigating cognitive reserve, brain reserve, and brain maintenance. J. Alzheimer’s Assoc. 2020;16:1305–1311. doi: 10.1016/j.jalz.2018.07.219. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 46.Lezak M.D., Howieson D.B., Loring D.W., Fischer J.S. Neuropsychological Assessment. Oxford University Press; New York, NY, USA: 2004. [Google Scholar]
- 47.Barter J., Kumar A., Stortz J.A., Hollen M., Nacionales D., Efron P.A., Moldawer L.L., Foster T.C. Age and Sex Influence the Hippocampal Response and Recovery Following Sepsis. Mol. Neurobiol. 2019;56:8557–8572. doi: 10.1007/s12035-019-01681-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Chicco D., Jurman G. Survival prediction of patients with sepsis from age, sex, and septic episode number alone. Sci. Rep. 2020;10:1–12. doi: 10.1038/s41598-020-73558-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Xu J., Tong L., Yao J., Guo Z., Lui K.Y., Hu X., Cao L., Zhu Y., Huang F., Guan X., et al. Association of Sex With Clinical Outcome in Critically Ill Sepsis Patients: A Retrospective Analysis of the Large Clinical Database MIMIC-III. Shock. 2019;52:146–151. doi: 10.1097/SHK.0000000000001253. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Tanner J.J., Johnson A.J., Terry E.L., Cardoso J., Garvan C., Staud R., Deutsch G., Deshpande H., Lai S., Addison A., et al. Resilience, pain, and the brain: Relationships differ by sociodemographics. J. Neurosci. Res. 2021;99:1207–1235. doi: 10.1002/jnr.24790. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Bagby S.P., Martin D., Chung S.T., Rajapakse N. From the Outside In: Biological Mechanisms Linking Social and Environmental Exposures to Chronic Disease and to Health Disparities. Am. J. Public Health. 2019;109:S56–S63. doi: 10.2105/AJPH.2018.304864. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Hill C.V., Pérez-Stable E.J., Anderson N.A., Bernard M.A. The National Institute on Aging Health Disparities Research Framework. Ethn. Dis. 2015;25:245–254. doi: 10.18865/ed.25.3.245. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Kaplan J.B., Bennett T. Use of race and ethnicity in biomedical publication. JAMA. 2003;289:2709–2716. doi: 10.1001/jama.289.20.2709. [DOI] [PubMed] [Google Scholar]
- 54.Loring D.W. History of neuropsychology through epilepsy eyes. Arch. Clin. Neuropsychol. 2010;25:259–273. doi: 10.1093/arclin/acq024. [DOI] [PMC free article] [PubMed] [Google Scholar]