Abstract
Objective
Malalignment of the cervical spine can result in cord compression, leading to a myelopathy diagnosis. Whether deformity or myelopathy severity is stronger predictors of surgical outcomes is understudied.
Methods
Surgical cervical deformity (CD) patients with baseline (BL) and up to 1-year data were included. Modified Japanese Orthopaedic Association (mJOA) score categorized BL myelopathy (mJOA = 18 excluded), with moderate myelopathy mJOA being 12 to 17 and severe myelopathy being less than 12. BL deformity severity was categorized using the mismatch between T1 slope and cervical lordosis (TS-CL), with CL being the angle between the lower endplates of C2 and C7. Moderate deformity was TS-CL less than or equal to 25° and severe deformity was greater than 25°. Categorizations were combined into 4 groups: group 1 (G1), severe myelopathy and severe deformity; group 2 (G2), severe myelopathy and moderate deformity; group 3 (G3), moderate myelopathy and moderate deformity; group 4 (G4), moderate myelopathy and severe deformity. Univariate analyses determined whether myelopathy or deformity had greater impact on outcomes.
Results
One hundred twenty-eight CD patients were included (mean age, 56.5 years; 46% female; body mass index, 30.4 kg/m2) with a BL mJOA score of 12.8±2.7 and mean TS-CL of 25.9°±16.1°. G1 consisted of 11.1% of our CD population, with 21% in G2, 34.6% in G3, and 33.3% in G4. At BL, Neck Disability Index (NDI) was greatest in G2 (p=0.011). G4 had the lowest EuroQol-5D (EQ-5D) (p<0.001). Neurologic exam factors were greater in severe myelopathy (p<0.050). At 1-year, severe deformity met minimum clinically important differences (MCIDs) for NDI more than moderate deformity (p=0.002). G2 had significantly worse outcomes compared to G4 by 1-year NDI (p=0.004), EQ-5D (p=0.028), Numerical Rating Scale neck (p=0.046), and MCID for NDI (p=0.001).
Conclusion
Addressing severe deformity had increased clinical weight in improving patient-reported outcomes compared to addressing severe myelopathy.
Keywords: Myelopathy, Correction, Cervical, Deformity, Outcomes
INTRODUCTION
The skull rests on the cervical spine to maintain erect posture and horizontal gaze [1,2]. Additionally, cervical spine offers range of motion and protects neurologic and vascular structures [3]. Therefore, optimal alignment of the cervical spine is vital to its functionality. Degenerative malalignment of the cervical spine leads to cervical or cervicothoracic kyphosis, which often results in severe axial neck pain and spinal cord compression, ultimately leading to a diagnosis of cervical spondylotic myelopathy (CSM) [4,5].
The main goal of cervical deformity (CD) surgery with neurologic compromise is to perform decompression and restoration of cervical lordosis (CL) which results in realignment of the spine. These corrective procedures have a significant impact on patient-reported and complication outcomes [6,7]. However, it is not fully understood whether deformity severity or the degree of myelopathy is the most significant predictors of these outcomes [5]. For instance, if the patient’s main complaint is gaze disturbance or dysphagia, both of which could be directly attributed to cervical kyphosis therefore, deformity correction is prioritized to restore these functions [8,9]. In contrast, when surgery is indicated mainly for compressive myelopathy, the primary goal is to ensure sufficient decompression and it is unclear whether deformity correction may impact the outcomes of these patients [10].
When accounting for initial deformity severity and myelopathic severity of a patient at baseline, it is unclear whether the malalignment of the cervical spine or the neurologic deficits put more impact on surgical outcome and/or patient satisfaction, postoperatively. Main objective of this study was to investigate the simultaneous impact of myelopathy and baseline deformity stratified by severity of each, upon postoperative outcomes.
MATERIALS AND METHODS
1. Study Inclusion Criteria
Consecutive adult patients (≥ 18 years) with cervical spine deformity undergoing cervical fusion by a single spine surgeon at an academic center were included. Database inclusion criteria for CD were defined using radiographic imaging and the following established parameters: cervical kyphosis (C2–7 sagittal Cobb angle ≥ 10), cervical scoliosis (C2–7 coronal Cobb angle ≥ 10), C2–7 sagittal vertical axis (C2–7 SVA)≥ 4 cm, or chin-brow vertical angle ≥ 25. Patient consent and Institutional Review Board (IRB) approval was obtained at the Center for Neuromuscular Care at Hospital for Joint Diseases (IRB number: i14-000) prior to enrolling patients.
2. Data Collection
Patients included had baseline and up to 1-year health-related quality of life (HRQoL) data. Baseline and 3-month radiographic measurements were maintained for these patients as well. Demographic data included age, sex, body mass index (BMI), and baseline comorbidity index as described the Charlson Comorbidity Index (CCI). Surgical data collected included number of levels fused, surgical approach, decompression type (discectomy, foraminotomy, corpectomy, laminectomy), and osteotomy type (Smith-Peterson, incomplete/complete facet). Clinical outcomes including neck disability (as assessed by the Neck Disability Index [NDI], EuroQol 5-Dimension Questionnaire [EQ-5D], and pain Numerical Rating Scale [NRS]), and myelopathy score (as assessed by the modified Japanese Orthopaedic Assocation [mJOA]) were obtained via patient surveys at baseline up to 1 year. For the purposes of this study, the EQ-5D-3 Level was used as an unweighted total score. Each response was scored between 1 and 3, with a maximum score of 15 indicating extreme problems and a minimum score of 5 indicating no problems. Previously published criteria for meeting minimum clinically important differences (MCIDs) for these metrics were also used to assess patient outcomes [11-14].
Radiographs were measured using validated software programming (SpineView; ENSAM Laboratory of Biomechanics, Paris, France) at a single academic center. Cervical sagittal alignment and balance were evaluated using C2–7 Cobb angle for CL (angle between the lower endplates of C2 and C7), cervical SVA (cSVA: C2 plumbline offset from the posterosuperior corner of C7), and the mismatch between T1 slope and CL (TS-CL).
3. Patient Grouping: Myelopathy vs. Deformity Severity
The mJOA was utilized to assess baseline myelopathy severity. Patients with a baseline mJOA of 18 were excluded to account for the ceiling effect. Moderate myelopathy was defined as having a score of 12–17 at baseline, while a severe myelopathy: patient presented with a baseline score of < 12. In terms of deformity severity, patients were classified with moderate deformity with a TS-CL≤ 25°, and severe deformity when baseline values of TS-CL mismatch exceeded 25°. Patients were stratified into 4 groups based upon their myelopathy and deformity severity as described: group 1 (G1), severe myelopathy and severe deformity; group 2 (G2), severe myelopathy and moderate deformity; group 3 (G3), moderate myelopathy and moderate deformity; group 4 (G4), moderate myelopathy and severe deformity. G2 and G4 were identified as mismatched myelopathy/deformity groups, and were assessed accordingly (Table 1).
Table 1.
Patients stratified by groups based upon their myelopathy and deformity severity
| Severity & group | Percentage |
|---|---|
| Myelopathy and deformity severity | |
| Moderate myelopathy | 69.5 |
| Severe myelopathy | 30.5 |
| Moderate deformity | 35.2 |
| Severe deformity | 64.8 |
| Groups | |
| 1: severe myelopathy and severe deformity | 11.1 |
| 2: severe myelopathy and moderate deformity | 21.0 |
| 3: moderate myelopathy and moderate deformity | 34.6 |
| 4: moderate myelopathy and severe deformity | 33.3 |
4. Statistical Analysis
Statistical analysis was performed using licensed IBM SPSS Statistics ver. 23.0 (IBM Co., Armonk, NY, USA). Univariate analyses were performed with a statistical cutoff p<0.05 to determine whether myelopathy severity or deformity severity had a greater impact on patient-reported outcomes via means comparison and analysis of variance analyses.
RESULTS
1. Demographic and Surgical Data
One hundred twenty-eight CD patients met inclusion criteria (mean age, 56.5 years; 46% female; BMI, 30.4 kg/m2, CCI, 0.56±0.85). Eighteen percent of patients were current smokers. Most patients underwent a posterior-only approach (47.5%), followed by a combined (24.6%) or anterior-only approach (27.9%). Mean total number of levels fused for the cohort was 5±3.2, mean operative time was 588.5 minutes, and mean estimated blood loss was 766.9 mL. Demographic and surgical data by myelopathy and deformity grouping is shown in Table 2.
Table 2.
Surgical details by deformity/myelopathy grouping
| Variable | Group 1 | Group 2 | Group 3 | Group 4 | p-value |
|---|---|---|---|---|---|
| Age (yr) | 59.0 | 55.1 | 54.8 | 59.4 | 0.203 |
| % Female | 56% | 35% | 30% | 56% | 0.201 |
| Body mass index (kg/m2) | 31.2 | 29.8 | 30.7 | 28.6 | 0.706 |
| Levels fused | 4.5 | 4.6 | 5.0 | 5.5 | 0.765 |
| Anterior-only approach | 33.3% | 25.0% | 25.9% | 11.5% | > 0.05 |
| Posterior-only approach | 44.4% | 50.0% | 51.9% | 61.5% | > 0.05 |
| Combined approach | 22.2% | 25.0% | 22.2% | 26.9% | > 0.05 |
| Any fusion | 55.6% | 64.7% | 42.8% | 37.0% | 0.308 |
| Anterior discectomy | 22% | 18% | 7% | 7% | 0.456 |
| Anterior corpectomy | 33.3% | 35.3% | 14.3% | 14.8% | 0.238 |
| Posterior osteotomy | 22% | 35% | 36% | 19% | 0.470 |
| Posterior decompression | 22% | 18% | 21% | 19% | 0.985 |
| Posterior foraminotomy | 22.2% | 41.2% | 35.7% | 22.2% | 0.504 |
| Posterior laminectomy | 22.2% | 29.4% | 32.1% | 25.9% | 0.933 |
Surgical approach data are given as a percentage within the group.
Group 1, severe myelopathy and severe deformity; group 2, severe myelopathy and moderate deformity; group 3, moderate myelopathy and moderate deformity; group 4, moderate myelopathy and severe deformity.
2. Overall Cohort Alignment
Baseline cervical alignment in our cohort was as follows: C2–7 CL was 1.30°±17.7°, mean C2–7 SVA was 28.8±16.4 mm, mean TS-CL was 25.9°±16.1°. Spinopelvic alignment at baseline included a mean T2–12 angle of -46.8±14.0, mean C7-S1 SVA of 0.74±57.2 mm, mean pelvic tilt (PT) of 18.3±10.1, and mean pelvic incidence minus lumbar lordosis (PI–LL) of -0.87±15.3.
At 3 months following surgery, patients saw significant improvement in cervical sagittal realignment. CL increased significantly (p=0.002) and TS-CL improvement trended towards significance (p=0.056). Cervical translation (cSVA) did not change significantly from baseline (p=0.883). No significant differences in spinopelvic alignment were observed between pre- and postoperative PT, PI–LL, and SVA (all p>0.05).
3. Myelopathy vs. TS-CL Groups.
Baseline mJOA score was 12.8±2.7, with a mean TS-CL of 25.9°±16.1°, as stated above. 30.5% of patients had severe baseline myelopathy, 69.5% moderate myelopathy, via the mJOA guidelines noted in the methods.
By baseline deformity severity, 35.2% were moderately deformed per TS-CL measurements, while 64.8% were severely deformed (Table 1).
Patients were then categorized into the 4 myelopathy/deformity groups, which found that G1 consisted of 11.1% of our CD population, with 21% in G2, 34.6% in G3, and 33.3% in G4 (Table 1). Table 3 details radiographic measurements by grouping at baseline and postoperatively. Case examples for each of these groupings can be seen in Figs. 1-4.
Table 3.
Radiographic measurements by grouping at baseline and 3 months
| Radiographic measurement | Group 1 | Group 2 | Group 3 | Group 4 | p-value |
|---|---|---|---|---|---|
| Cervical lordosis (C2–7) | |||||
| Baseline | -4.52 | 2.59 | 4.59 | -4.79 | 0.085 |
| 3 Months | 6.57 | 13.99 | 9.94 | 12.31 | 0.756 |
| TS-CL | |||||
| Baseline | 43.79 | 16.35 | 15.79 | 36.54 | < 0.001 |
| 3 Months | 33.07 | 23.19 | 23.10 | 24.56 | 0.317 |
| cSVA | |||||
| Baseline | 39.53 | 22.26 | 21.24 | 44.24 | < 0.001 |
| 3 Months | 39.35 | 39.75 | 31.82 | 32.65 | 0.600 |
Group 1, severe myelopathy and severe deformity; group 2, severe myelopathy and moderate deformity; group 3, moderate myelopathy and moderate deformity; group 4, moderate myelopathy and severe deformity; TS-CL, T1 slope and cervical lordosis; cSVA, cervical sagittal vertical axis.
Fig. 1.
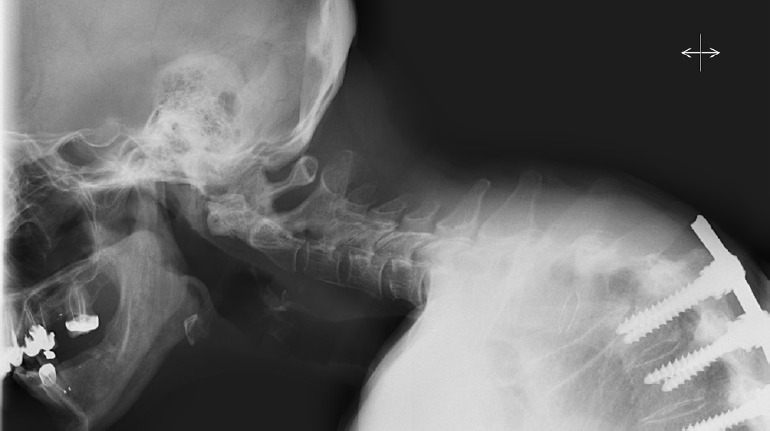
Group 1 (severe myelopathy and severe deformity) patient example.
Fig. 2.
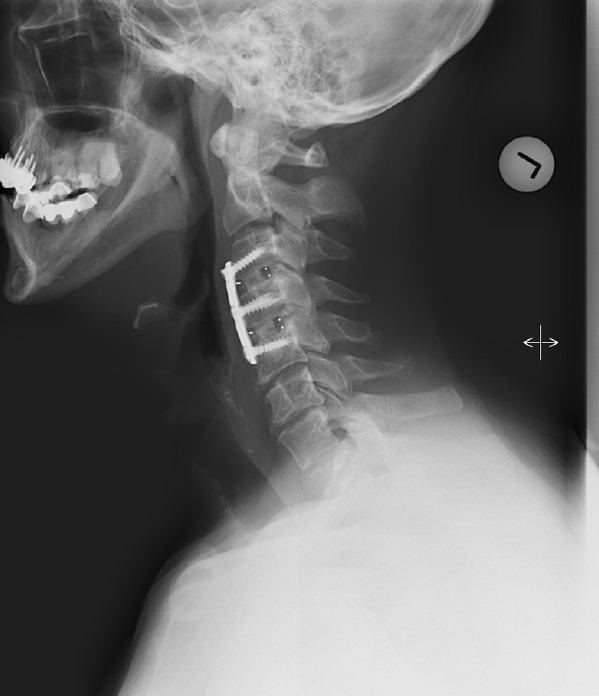
Group 2 (severe myelopathy and moderate deformity) patient example.
Fig. 3.
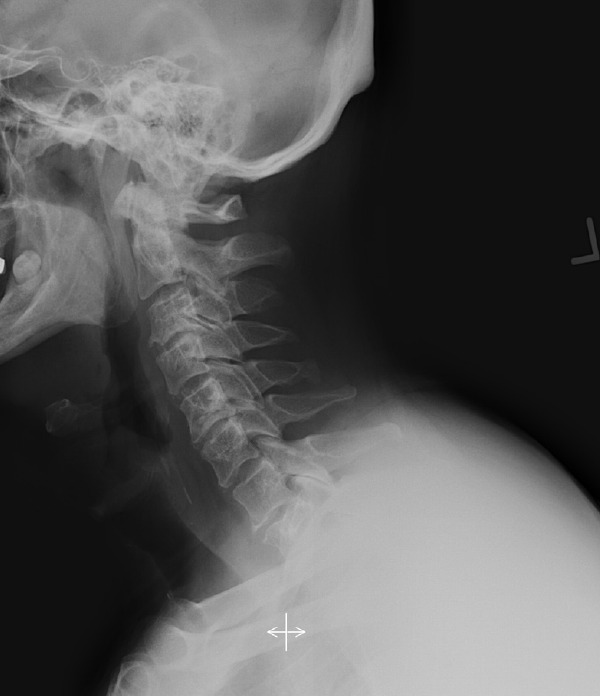
Group 3 (moderate myelopathy and moderate deformity) patient example.
Fig. 4.
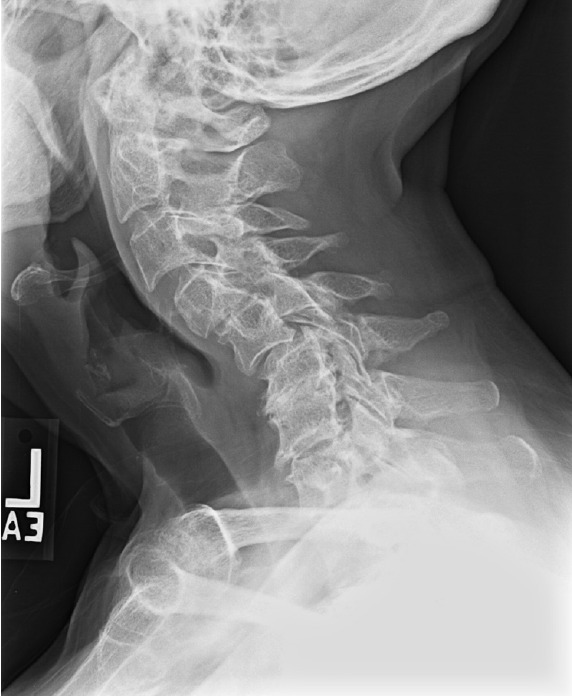
Group 4 (moderate myelopathy and severe deformity) patient example.
4. Myelopathy/Deformity Group HRQoL Comparison
At baseline, NDI score was the greatest in G2 at 69.4 (G1: 69.1, G3: 57.1, G4: 52.6, p=0.011), whereas G4 had the lowest EQ-5D scores (p<0.001). G2 had the lowest mJOA score at baseline (9.35), while G4 had the greatest (14.5) (p<0.001) (Table 4). According to baseline neurologic exam factors were significantly greater in the groups with severe myelopathy (G1 and G2, p<0.05).
Table 4.
Baseline mean health-related quality of life measures by group
| NDI score |
EQ-5D score |
mJOA score |
||||
|---|---|---|---|---|---|---|
| Mean ± SD | p-value | Mean ± SD | p-value | Mean ± SD | p-value | |
| Group | 0.011 | < 0.001 | < 0.001 | |||
| 1 | 69.1 ± 13.9 | 10.4 ± 3.85 | 10.3 ± 1.00 | |||
| 2 | 69.4 ± 14.7 | 10.8 ± 1.80 | 9.35 ± 1.73 | |||
| 3 | 57.1 ± 21.0 | 10.1 ± 2.96 | 13.6 ± 1.35 | |||
| 4 | 52.6 ± 17.4 | 6.14 ± 4.88 | 14.5 ± 1.53 | |||
Group 1, severe myelopathy and severe deformity; group 2, severe myelopathy and moderate deformity; group 3, moderate myelopathy and moderate deformity; group 4, moderate myelopathy and severe deformity; NDI, Neck Disability Index; EQ-5D, Euro-Quality of Life-5 Dimension; mJOA, modified Japanese Orthopaedic Association; SD, standard deviation.
At 1 year, 55.6% of patients with severe myelopathy and severe deformity, G1, met MCID for NDI, while 6.9% of G2, 25% G3, and 55.6% G4 met the threshold for MCID for the NDI, p=0.002. There were no significant differences between the groups in meeting MCID for neither EQ-5D nor mJOA. Additionally, while differences between groups were maintained at 1-year HRQoL measures by the NDI and EQ-5D, groups were not significantly different in their mJOA scores 1 year postoperatively (Table 5). Indeed, the severe myelopathy groups improved their mJOA scores after surgery while the moderate myelopathy group scores remained stagnant, bringing all of the groups to relatively similar mJOA scores at 1 year. Mismatch myelopathy/deformity analysis determined that a greater myelopathy over deformity, G2, had significantly worse patient-reported outcomes compared to G4 in terms of 1-year NDI (G2: 57 vs. G4: 28.1; p=0.004), EQ-5D (p=0.028), and NRS neck (G2: 5.9, G4: 3.6; p=0.046), as well as meeting MCID for NDI (G2: 5.9%, G4: 55.6%; p=0.001).
Table 5.
Year 1 mean health-related quality of life measures by group
| NDI score |
EQ-5D score |
mJOA score |
||||
|---|---|---|---|---|---|---|
| Mean ± SD | p-value | Mean ± SD | p-value | Mean ± SD | p-value | |
| Group | 0.001 | 0.001 | 0.268 | |||
| 1 | 43.7 ± 18.5 | 9.57 ± 1.99 | 12.3 ± 4.99 | |||
| 2 | 57.0 ± 21.9 | 9.67 ± 1.37 | 12.2 ± 2.14 | |||
| 3 | 51.8 ± 17.5 | 9.80 ± 2.99 | 13.8 ± 2.98 | |||
| 4 | 28.1 ± 18.3 | 5.22 ± 4.51 | 14.5 ± 2.57 | |||
Group 1, severe myelopathy and severe deformity; group 2, severe myelopathy and moderate deformity; group 3, moderate myelopathy and moderate deformity; group 4, moderate myelopathy and severe deformity; NDI, Neck Disability Index; EQ-5D, Euro-Quality of Life-5 Dimension; mJOA, modified Japanese Orthopaedic Association; SD, standard deviation.
DISCUSSION
A diagnosis of CD presents symptomatically as poor horizontal gaze, dysphagia, axial neck pain, neurological dysfunction, and functional disabilities [3]. With an increasing degree of malalginment of the cervical spine anterior to the cervical segment of the spinal cord, CSM results [2]. Myelopathy combined with deformity is a severe threat to a patient’s spinal health and treatment requires complex surgical procedures. Patients who meet this criteria require simultaneous surgical decompression and correction surgery [5,15]. The case for which optimal surgical strategy is often debated and the various approaches (anterior, posterior, or combined) carry different risks and benefits. After surgical intervention, it is unclear the impact that preoperative factors of deformity severity and neurologic compromise from myelopathy have on postoperative HRQoL metrics [2,8].
When encountering CSM, a thorough understanding of etiological factors is important. During the normal aging process, disc desiccation leads to progressive disc degeneration, resulting in disc collapse and a decrease in disc height [1]. Sequential mechanical endplate damage results in formation of disc osteophytic complexes by subperiosteal bone formation. This creates more stress on the facet joints leading to facet arthropathy. This change gets accentuated during both static and dynamic states [2]. Degenerative changes are further accentuated by the ligamentum flavum hypertrophy accounting for an additional spinal stenosis [3,4]. During normal range of cervical spine motion, any flexion or extension can lead to an intermittent compression which further worsens spinal stenosis. All these changes have cumulative effect on impedance of blood supply to the spinal cord and therefore cause additional progressive neurological deficits [5-7].
When treating minor spinal deformity, the surgeons should understand the goal of postoperative alignment and its implication on the outcomes when myelopathic symptoms prevail. Kyphosis in the cervical spine plays an important role in development of myelopathy, as it decreases the space between the anterior compressive pathology and the spinal cord [9]. Major causative factors are multilevel disc herniations, spondylotic disc osteophyte complexes, and an ossified posterior longitudinal ligament [2,16]. Therefore, cervical realignment aims to increase this space and relieve compression and tension on the spinal cord. It has been previously shown that sufficient decompression can be achieved even in minor deformity and severe myelopathic patients [17]. Thus, our study may reflect the severe spondylitic changes seen in major myelopathic CD patients who present with mild deformity (group 2).
In our study, we sought to investigate the impact of myelopathy severity on outcomes and satisfaction postoperatively over baseline deformity severity. The results showed that when assessing greater baseline myelopathy over deformity severity, significantly worse patient-reported outcomes occurred compared to patients with greater deformity over myelopathy severity. In the literature, we see that surgical restoration of sagittal alignment and balance appears to correlate with functional outcomes [5]. In 2018, a study by Ailon et al. [18] investigated how surgical correction affected 77 CD patients postoperatively in terms of their HRQoLs. They found significant improvement in NDI, NRS neck, and EQ-5D, despite minimal change in myelopathy outcomes. This study suggested that improvement across multiple quality of life measures without significant recovery of neurologic function may be related to the pathophysiology and chronicity of myelopathy in the setting of cervical kyphosis. Kato et al. [19] showed in their 2018 study, that preoperative CD was associated with postoperative HRQoL scores in an entirely myelopathic cohort. These results may be true within our cohort as well. The patients who met criteria for severe myelopathy and moderate deformity may have been neurologically impaired beyond improvement, ultimately resulting in minimal functionality return.
Severe deformity correction, in the setting of moderate baseline myelopathic symptoms, directly impacted patient-reported outcomes postoperatively. With better improvement in NDI, EQ-5D, and NRS neck, our study supports the literature on surgical intervention for majorly deformed patients for ultimate improvement of quality of life.
The retrospective nature of the cohort can inherently lead to potential reporting or observer bias. Using data collected from a one surgeon operating in an academic setting may not be representative of the average physician and average hospital a primary cervical diagnoses patient receives treatment at in the United States. Furthermore, a study of this nature cannot examine causality and both sagittal spinal alignment parameters and HRQoL may be influenced by another confounding factor such as the underlying spinal diagnoses for which the patient was receiving spinal fusion surgery. At 1 year postoperative, this study may be hindered by a relatively short follow-up time. Additionally, myelopathy severity was defined via mJOA scores rather than magnetic resonance imaging findings, which may not accurately reflect the physiologic actuality of the patient’s disease.
CONCLUSION
CSM and the spinal deformity are strongly related. Patients who present with more severe myelopathy than deformity have worse patient-reported outcomes than the opposite case. In moderate deformity, myelopathy decompression and symptomatic alleviation are substantial. However, this intervention is inadequate in the case of severe deformity, where realignment is necessary due to cord tension. Surgical intervention to address severe deformity had increased clinical weight with respect to improving patient-reported outcomes in comparison to addressing severe myelopathy, which further indicates the gravity of deformity as a formidable and complex illness.
Footnotes
The authors have nothing to disclose.
REFERENCES
- 1.Moses MJ, Tishelman JC, Zhou PL, et al. McGregor’s slope and slope of line of sight: two surrogate markers for Chin-Brow vertical angle in the setting of cervical spine pathology. Spine J. 2019;19:1512–7. doi: 10.1016/j.spinee.2019.04.021. [DOI] [PubMed] [Google Scholar]
- 2.Chi JH, Tay B, Stahl D, et al. Complex deformities of the cervical spine. Neurosurg Clin N Am. 2007;18:295–304. doi: 10.1016/j.nec.2007.01.003. [DOI] [PubMed] [Google Scholar]
- 3.Dru AB, Lockney DT, Vaziri S, et al. Cervical spine deformity correction techniques. Neurospine. 2019;16:470–82. doi: 10.14245/ns.1938288.144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Cho SK, Safir S, Lombardi JM, et al. Cervical spine deformity: indications, considerations, and surgical outcomes. J Am Acad Orthop Surg. 2019;27:e555–67. doi: 10.5435/JAAOS-D-17-00546. [DOI] [PubMed] [Google Scholar]
- 5.Passias PG, Horn SR, Bortz CA, et al. The relationship between improvements in myelopathy and sagittal realignment in cervical deformity surgery outcomes. Spine (Phila Pa 1976) 2018;43:1117–24. doi: 10.1097/BRS.0000000000002610. [DOI] [PubMed] [Google Scholar]
- 6.Tang JA, Scheer JK, Smith JS, et al. The impact of standing regional cervical sagittal alignment on outcomes in posterior cervical fusion surgery. Neurosurgery. 2012;71:662–9. doi: 10.1227/NEU.0b013e31826100c9. [DOI] [PubMed] [Google Scholar]
- 7.Kim YC, Cui JH, Kim KT, et al. Novel radiographic parameters for the assessment of total body sagittal alignment in adult spinal deformity patients. J Neurosurg Spine. 2019;31:372–9. doi: 10.3171/2019.3.SPINE18703. [DOI] [PubMed] [Google Scholar]
- 8.Yeh KT, Chen IH, Lee RP, et al. Two surgical strategies for treating multilevel cervical spondylotic myelopathy combined with kyphotic deformity. Medicine (Baltimore) 2020;99:e19215. doi: 10.1097/MD.0000000000019215. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Mummaneni PV, Deutsch H, Mummaneni VP. Cervicothoracic kyphosis. Neurosurg Clin N Am. 2006;17:277–87. doi: 10.1016/j.nec.2006.05.007. vi. [DOI] [PubMed] [Google Scholar]
- 10.Al-Tamimi YZ, Guilfoyle M, Seeley H, et al. Measurement of long-term outcome in patients with cervical spondylotic myelopathy treated surgically. Eur Spine J. 2013;22:2552–7. doi: 10.1007/s00586-013-2965-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Young IA, Cleland JA, Michener LA, et al. Reliability, construct validity, and responsiveness of the neck disability index, patient-specific functional scale, and numeric pain rating scale in patients with cervical radiculopathy. Am J Phys Med Rehabil. 2010;89:831–9. doi: 10.1097/PHM.0b013e3181ec98e6. [DOI] [PubMed] [Google Scholar]
- 12.Passias PG, Segreto FA, Lafage R, et al. Recovery kinetics following spinal deformity correction: a comparison of isolated cervical, thoracolumbar, and combined deformity morphometries. Spine J. 2019;19:1422–33. doi: 10.1016/j.spinee.2019.03.006. [DOI] [PubMed] [Google Scholar]
- 13.Steinhaus ME, Iyer S, Lovecchio F, et al. Minimal clinically important difference and substantial clinical benefit using PROMIS CAT in cervical spine surgery. Clin Spine Surg. 2019;32:392–7. doi: 10.1097/BSD.0000000000000895. [DOI] [PubMed] [Google Scholar]
- 14.Pool JJ, Ostelo RW, Hoving JL, et al. Minimal clinically important change of the Neck Disability Index and the Numerical Rating Scale for patients with neck pain. Spine (Phila Pa 1976) 2007;32:3047–51. doi: 10.1097/BRS.0b013e31815cf75b. [DOI] [PubMed] [Google Scholar]
- 15.Grosso MJ, Hwang R, Mroz T, et al. Relationship between degree of focal kyphosis correction and neurological outcomes for patients undergoing cervical deformity correction surgery. J Neurosurg Spine. 2013;18:537–44. doi: 10.3171/2013.2.SPINE12525. [DOI] [PubMed] [Google Scholar]
- 16.Ichihara K, Taguchi T, Sakuramoto I, et al. Mechanism of the spinal cord injury and the cervical spondylotic myelopathy: new approach based on the mechanical features of the spinal cord white and gray matter. J Neurosurg. 2003;99(3 Suppl):278–85. doi: 10.3171/spi.2003.99.3.0278. [DOI] [PubMed] [Google Scholar]
- 17.Chen J, Liu Z, Zhong G, et al. Surgical treatment for cervical spondylotic myelopathy in elderly patients: a retrospective study. Clin Neurol Neurosurg. 2015;132:47–51. doi: 10.1016/j.clineuro.2015.02.012. [DOI] [PubMed] [Google Scholar]
- 18.Ailon T, Smith JS, Shaffrey CI, et al. Outcomes of operative treatment for adult cervical deformity: a prospective multicenter assessment with 1-year follow-up. Neurosurgery. 2018;83:1031–9. doi: 10.1093/neuros/nyx574. [DOI] [PubMed] [Google Scholar]
- 19.Kato S, Nouri A, Wu D, et al. Impact of cervical spine deformity on preoperative disease severity and postoperative outcomes following fusion surgery for degenerative cervical myelopathy: sub-analysis of AOSpine North America and International Studies. Spine (Phila Pa 1976) 2018;43:248–54. doi: 10.1097/BRS.0000000000002307. [DOI] [PubMed] [Google Scholar]


