ABSTRACT
Objectives:
Recently, the dart-throwing motion (DTM) has attracted attention as a functional direction of wrist joint motion. Consequently, we devised a new artificial muscle-type dynamic orthosis (Dynamic Traction Splint by Artificial Muscle, DTSaM) to reproduce DTM. This study analyzed the automatic motion of the wrist joint using a three-dimensional motion analysis system to assess how closely the DTSaM replicates DTM.
Methods:
The DTSaM orthosis incorporates two McKibben-type rubber artificial muscles, and measurements were performed using image analysis software and a three-dimensional motion analysis system. The wrist radial angle (WRA) was defined as the angle between the line connecting the head of the index finger metacarpal to the radial styloid process and the line connecting the radial styloid process to the lateral epicondyle of the humerus. WRAs were investigated from 60° of palmar flexion to 60° of dorsiflexion.
Results:
For dorsiflexion, comparisons of radial deviation and wrist ulnar angle (WUA) between the motion obtained using the DTSaM orthosis and active DTM showed a significant difference (P <0.05) at 30° and 60°, respectively. For palmar flexion, the same comparison showed a significant difference for both the ulnar and radial deviations (30°, P <0.05; and 60°, P <0.01, respectively). Furthermore, WUA showed a significant difference at 50° (P <0.05). Intraclass correlation coefficient analyses yielded good reliability with an average value of ≥0.8.
Conclusion:
The DTSaM orthosis produces a motion similar to the DTM. It is hoped that the use of the DTSaM orthosis will help to shorten the treatment period for patients with wrist disease.
Keywords: dart-throwing motion, hand therapy, motion analyzer, wrist joint angle
INTRODUCTION
Wrist disease causes pain, swelling, and contracture and significantly impairs activities of daily living and quality of life.1) Sequelae associated with wrist joint diseases, such as pain, often remain; moreover, some patients with wrist joint disorders develop contractures.
Contractures are treated by identifying the limiting factors and employing focused treatment. Sustained stretching is effective for contracted tissue.2) The application of dynamic orthoses is known to be an effective therapy for improving the range of motion.3) Similarly, dynamic orthoses are effective and widely accepted for improving finger function after trauma, and their use is expected to shorten the treatment period.4) Conventional dynamic orthoses for wrist joints5) are unidirectional; therefore, there is a risk of increased pain. Moreover, such orthoses may be ineffective because of the difficulty in adopting an approach adjusted to the limiting factors.
Overall wrist joint movement is essentially the sum of the movements of the carpometacarpal joint (C-L joint) and the radiocarpal joint (R-L joint).6) The movement ratio of these two joints to the movement of the entire wrist joint is called the contribution ratio. There are characteristic tendencies in the contribution ratio. In rehabilitation, it is important to improve the contracture of each joint and to normalize the contribution ratio.6,7,8) Recently, application of the dart-throwing motion (DTM) to contracted hands has been studied. DTM exercise is reportedly effective for C-L joints,9,10,11) suggesting that motion in the DTM plane can be preserved following wrist surgery, as in radiocarpal fusion, provided that mid-carpal motion is permitted.12,13,14) DTM has been shown to require minimal relative rotation of the scaphoid and lunate.9,14,15,16) Therefore, DTM may be permitted during early mobilization following injury. However, an accurate measurement of DTM is required before it is used in clinical practice because deviation from the DTM path reportedly increases the relative motion of the carpal bones.15)
Moreover, the development and clinical effects of dynamic orthoses, including those that reproduce the DTM, should be considered.17,18) However, to enable active movements, orthoses are usually made of rigid materials, and this makes them difficult to use when treating diseases such as contractures that require tissue expansion.
Therefore, based on a dynamic orthosis that has a clinical effect on wrist contracture,5) we devised a new orthodontic orthosis that combines the DTM with traction effects, thereby addressing the common problems. The resulting orthosis incorporates pneumatic artificial muscles (PAMs), which generate superior tension as the power source of the straightening action to achieve traction at the wrist and effective passive DTM. The device is an artificial muscle-type traction orthosis (novel Dynamic Traction Splint by Artificial Muscle: DTSaM)19) developed for exercising the wrist joint. The authors previously assessed the clinical effects of using the DTSaM orthosis in patients with painful wrist contracture.19) The present study aimed to analyze the automatic motion of the wrist joint during DTM using three-dimensional motion analysis to assess the accuracy with which the DTSaM replicates DTM.
MATERIALS AND METHODS
Structure and Characteristics of the DTSaM Orthosis
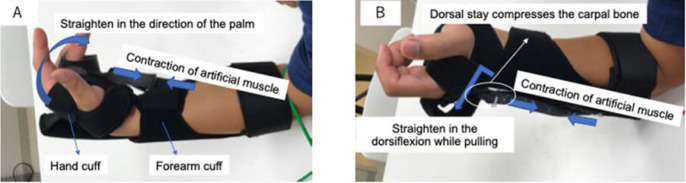
Figure 1 shows the features and mounting attachments of the McKibben artificial muscles. The DTSaM includes a controller, a palm finger cuff, a wrist cuff, a forearm cuff (made by Daiya Industry Co., Ltd., Japan), a dorsal stay, McKibben artificial muscles (two palms, two dorsals), and elbow joint and forearm fixtures (thermoplastic Orfit material, produced in-house). The orthosis works by using PAMs to correct the dorsiflexion and the palmar flexion while performing traction. The PAMs were arranged such that the rubber tube was constrained by the elastic material in the longitudinal direction of the finger. In the resulting structure, the rubber tube expands toward the center point and contracts when pressurized (Fig. 2).
Fig. 1.
Essential parts of the DTSaM wrist orthosis: ① forearm cuff (made by Daiya Industry Co., Ltd., Japan), ② hand cuff (made by Daiya Industry Co., Ltd., Japan), ③ artificial muscle for palmar flexion (two), ④ artificial muscle for dorsiflexion (two), and ⑤ controller.
Fig. 2.
Wrist orthosis mechanism for (A) wrist palmar flexion and (B) dorsiflexion. (A) For palmar flexion, the finger cuff for flexion was attached to the middle and ring fingers and the wrist cuff was also attached. The pneumatic artificial muscle (PAM) was attached from the finger cuff to the lateral epicondyle of the humerus. When the PAM contracted, palmar flexion movement was performed, and the dart-throwing motion was reproduced. (B) The artificial muscle expands and the dorsal stay of the wrist joint restricts the movement of the carpal bone and presses the carpal bone in the volar direction. Thereby, traction is added to the metacarpal bone, and traction and dorsiflexion of the wrist joint are performed.
For palmar flexion, the finger cuff for flexion was attached to the middle finger and the ring finger and the wrist cuff was also attached. The finger cuff and PAMs were connected, and the artificial muscles were attached from the finger cuff to the lateral epicondyle of the humerus. As the PAMs contracted, palmar flexion movement was performed, and DTM was reproduced (Fig. 2A).
For dorsiflexion, the artificial muscle expanded, as shown in Fig. 2 B, and the dorsal stay of the wrist joint restricted the movement of the carpal bone and pressed the carpal bone in the volar direction. Consequently, traction was added to the metacarpal bone, and traction and dorsiflexion of the wrist joint were performed. This traction method is very different from conventional wrist traction devices. To reproduce DTM, the PAMs were attached, and traction was initiated to perform the dorsiflexion motion.
Subjects
Twenty healthy forearms from 12 men and 8 women with an average age of 26.2 years (range, 25–28 years) were evaluated. The average forearm height was 162.5 ± 7.8 cm, the body weight was 70.1 ± 10.1 kg, and all subjects were right-handed. The traction force was unified and measured at 300 kPa using the PAMs. To avoid affecting the blood flow and causing pain, the study was conducted after confirming the skin color and assessing subjective symptoms after the subject had worn the cuff for 3 min.20,21) We previously examined the effects of the orthosis cuff on blood flow and myoelectrical activity and have proven its safety.22) For the cuff shape, we used a wrist cuff covering the entire circumference of the wrist to obtain complete compression on the dorsal and volar arches.23)
This research was approved by the Kansai Welfare Science University Ethics Committee (Approval number 17–19). Written informed consent was obtained before patient enrollment from all volunteers who agreed to participate in the research protocol.
Measurement Method
The forearm muscles that are directly involved in generating DTM are the extensor carpi radialis brevis and longus (ECRL-B) and the flexor carpi ulnaris (FCU).17) Therefore, the McKibben-type rubber artificial muscles were arranged along the running direction of the muscle by palpating the two palmar sides of the FCU and the two dorsal sides of the ECRL-B. The wrist joint cuff was made of polyurethane. Care was taken to avoid any deviation between individuals. We prepared a fixture exclusively for this research to fix the measured limb position at 90° flexion of the elbow joint and 45° pronation of the forearm. The movement of the wrist joint was measured using a three-dimensional motion analysis system (Opti Track Japan: Motive Tracker) and image analysis software (SKYCOM, Japan). Three Flex3 cameras were used for motion capture, and the camera settings were frame rate (FPS) 100, exposure (EXP) 480, threshold (THR) 255, and LED illumination (LED) 15.
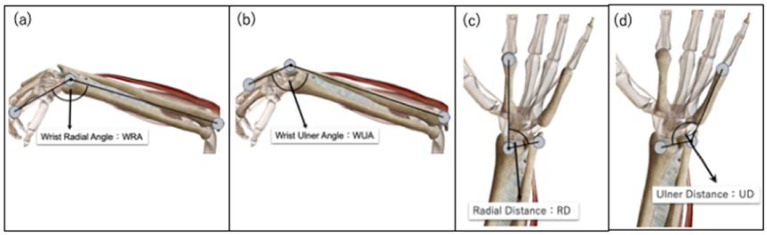
The measurement angle of the wrist joint was based on the wrist radial angle (WRA), i.e., the angle formed by the line between the index phalanx head and the radial styloid process and the line between the radial styloid process and the lateral epicondyle of the humerus (Fig. 3a). The changes in other anatomical variables were estimated for units of 10° of WRA from 60° of palmar flexion to 60°of dorsiflexion. We also analyzed the wrist ulnar angle (WUA), i.e., the angle formed by the line between the phalangeal head of the little finger and the ulnar styloid process and the line between the ulnar styloid process and the lateral epicondyle of the humerus; the ulnar deviation (UD), i.e., the angle formed by the line between the phalanx of the index finger and the radial styloid process and the line between the radial styloid process and the ulnar styloid process; and the radial deviation (RD) i.e., the angle formed by the line between the phalangeal head of the little finger and the ulnar styloid process and the line between the ulnar styloid process and the radial styloid process. Measurements were taken three times each for the following three scenarios: active exercise, the motion produced by the DTSaM, and passive exercise performed by a skilled occupational therapist with more than 10 years of experience with consideration of DTM. The average values were subsequently measured and calculated.
Fig. 3.
Definition of wrist angles for measurement. (A) Wrist radial angle (WRA): the angle formed by the line connecting the index finger head of the metacarpal bone to the styloid process of the radius and the line connecting the lateral epicondylus of the humerus to the styloid process of the radius. (B) Wrist ulnar angle (WUA): the angle formed by the line connecting the little finger head of the metacarpal bone to the styloid process of the ulna and the line from the lateral epicondyle of the humerus to the styloid process of the ulna. (C) Radial deviation (RD): the angle between the line connecting the index finger metacarpal head to the styloid process of the radius and the line connecting the styloid process of the radius to the styloid process of the ulna. (D) Ulnar deviation (UD): the angle between the line connecting the little finger head of the metacarpal bone to the styloid process of the ulna and the line connecting the styloid process of the ulna to the styloid process of the radius.
Statistical Analysis
Statistical analysis was performed using analysis of variance and Friedman’s test. Post-tests were performed using Scheffe’s multiple comparison test. Furthermore, the validity was calculated from the passive motion and the measured values of DTSaM, but not for active motion, using the intraclass correlation coefficient (ICC).
RESULTS
Dorsiflexion
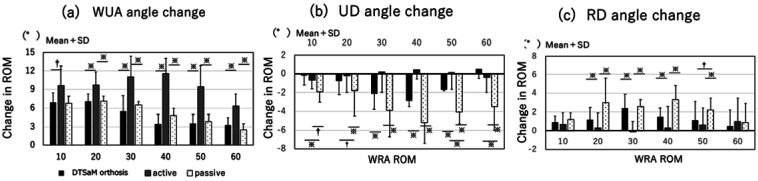
For dorsiflexion, there were significant differences in WUA between DTSaM and active exercise for all WRA angles from 10° (P<0.01) to 60° (P<0.05) (Fig. 4). For the same comparison, UD showed significant differences between 30° and 50° (P<0.05). For RD, significant differences were found at 20°–40° (P<0.05). For active compared with passive exercise, WUA showed significant differences between 20° and 60° (P<0.05). UD showed significant differences at all angles from 10° to 60° (P<0.01, P<0.05), and RD showed significant differences between 20° and 50° (P<0.05). A comparison of DTSaM and passive movement showed significant differences in UD at 10° (P<0.05), 20° (P<0.01), 50°, and 60° (P<0.05). For RD, there was a significant difference at 50° only (P<0.01). The ICC of passive movement and DTSaM for WUA increased from 0.81 to 0.83; for UD, ICC increased from 0.78 to 0.88, and for RD, ICC increased from 0.75 to 0.81 (Table 1).
Fig. 4.
Changes in anatomical angles in the dorsiflexion direction for WRA in the range 10°–60°: (A) wrist ulnar angle (WUA), (B) ulnar deviation (UD), and (C) radial deviation (RD). Analysis of variance and the Friedman test were performed. A post-hoc test was performed using Scheffe’s multiple comparison test. *P<0.05, †P<0.01. ROM, range of motion.
Table 1. . Intra-rater reliability for measurements.
| Angle analysis | Direction of movement | Intra-rater reliability | ||
| ICC 1,1 (95% CI) | ICC 1,2 (95% CI) | ICC 1,3 (95% CI) | ||
| WUA | Flexion | 0.78 (0.68–0.88) | 0.81 (0.72–0.90) | 0.77 (0.69–0.88) |
| Extension | 0.81 (0.76–0.92) | 0.83 (0.77–0.91) | 0.81 (0.74–0.90) | |
| UD | Flexion | 0.76 (0.68–0.90) | 0.75 (0.67–0.88) | 0.77 (0.69–0.88) |
| Extension | 0.88 (0.78–0.92) | 0.78 (0.71–0.85) | 0.82 (0.71–0.91) | |
| RD | Flexion | 0.77 (0.63–0.89) | 0.79 (0.71–0.83) | 0.81 (0.74–0.90) |
| Extension | 0.78 (0.71–0.83) | 0.75 (0.68–0.91) | 0.81 (0.81–0.92) | |
ICC, intraclass correlation coefficient; CI, confidence interval; WUA, wrist ulnar angle; RD, radial deviation; UD, ulnar deviation.
Palmar Flexion
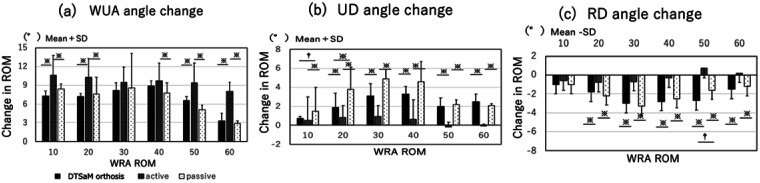
For palmar flexion (Fig. 5), there were significant differences in WUA between DTSaM and active exercise for WRA angles of 10°, 20°, 50°, and 60° (P<0.05). For the same comparison, UD showed significant differences for all angles in the range 20°–60° (P<0.05). For RD, significant differences were also found in the range 20°–60° (P<0.05). For active compared with passive movement, WUA showed significant differences at WRA angles of 10°, 20°, 40°, 50°, and 60° (P<0.05). UD showed significant differences at all angles from 10° to 60° (P<0.05), and RD showed significant differences for WRA angles in the range 20°–60° (P<0.05). A comparison of DTSaM and passive movement showed a significant difference in UD at 10° (P<0.01) and 20° (P<0.05). Additionally, a significant difference was observed in RD at 50° (P<0.01). The ICCs for passive movement and DTSaM for WUA, UD, and RD were 0.77 to 0.81, 0.75 to 0.77, and 0.77 to 0.81, respectively (Table 1).
Fig. 5.
Changes in (A) WUA, (B) UD, and (C) RD in the palmar flexion direction for WRA in the range 10°–60°. Analysis of variance and the Friedman test were performed. A post-hoc test was performed using Scheffe’s multiple comparison test. *P<0.05, †P<0.01.
DISCUSSION
We devised a new orthosis that can stretch tissues using a highly flexible clothing material and PAMs. From our results, no radial or ulnar flexion movements were observed between WRA angles of 10° and 60° during automatic movements for both flexion and dorsiflexion. Therefore, even if the pronation position was approximately 45°, the movement would not be similar to DTM, unless the subject was under instruction.
In passive DTM movements, the ulnar flexion angle during palmar flexion and during dorsiflexion changed by an average of 33.2° and 22.2°, respectively. Under DTSaM, the ulnar flexion angle during palmar flexion and during dorsiflexion were, on average, 32.3° and 21.4°, respectively. There was a significant difference in both the flexion and dorsiflexion directions.
Early mobilization of the wrist is important to prevent the development of fibrosis and secondary stiffness and to regain proprioception more quickly, thereby ensuring a faster return to function. To date, wrist joint motion has been evaluated and analyzed mainly in two directions: dorsiflexion/palmar flexion and radial/ulnar flexion. However, the motion from radial dorsiflexion, which is a diagonal movement combining radial flexion and dorsiflexion, to palmar ulnar flexion (i.e., the DTM) has been recently included in the analysis.
Furthermore, the diagonal movement of ulnar dorsiflexion, which combines ulnar and dorsiflexion, to radial flexion, which in turn combines radial and palmar flexion, has been used in functional anatomy.14,23) Cadaveric and in vivo studies demonstrated that both lunate motion and scaphoid motion are minimal during motion in the true DTM plane.9,14,15) Early post-surgical rehabilitation of the wrist along a plane that is not consistent with DTM may result in excessive scaphoid and lunate motion, thereby compromising the surgical reconstruction. Therefore, the accurate measurement of DTM in the clinic is important for both clinical assessment and the use of DTM in the design of rehabilitation tools, such as dynamic orthoses. Such measurement would also facilitate strengthening programs that allow mobilization of the wrist along the DTM plane only.24) “Dart orthoses” may be utilized in postoperative rehabilitation protocols wherein it is necessary to immobilize the radio-carpal joint, such as following surgical repair or reconstruction of radio-carpal ligaments, scapholunate ligaments, midcarpal instability, and radioscapho-lunate fusion. Moreover, dart orthoses can be recommended for the conservative treatment of several types of predynamic and dynamic scapho-lunate interosseous ligament instability and palmar midcarpal instability. Currently, the basic characteristics of DTM and the effectiveness of dart orthoses are inconclusive. However, such orthoses need to be rigid orthotics and should be focused on active motion. Therefore, it is problematic to apply dart orthoses to diseases such as contractures, which require tissue expansion.
Generally, PAMs enable effective treatment to be delivered under conditions of relatively low pressure and reduced tension; consequently, PAMs were used to provide powered torque for DTSaM orthoses. Additionally, PAM utilization results in orthoses that are flexible, lightweight, easily maintained, and inexpensive. Recent studies have quantified in detail the force-length, force-velocity, force-activation, and bandwidth properties of artificial pneumatic muscles.25,26,27,28) PAMs, which can generate high power at low pressures, are well suited for mimicking natural gait movements,26,27) as in the current DTSaM orthosis, and for providing power-assisted gloves.29)
The current DTSaM results are similar to those of a previous study,30) and DTM movements may be closely reproduced. However, it takes time for the artificial muscle to expand after the pressure is applied to the entire rubber tube. The comparison between passive movement and DTSaM movement revealed a difference in the radial flexion angle between the palmar flexion and dorsiflexion motions during the initial motion. However, ICC analyses yielded good reliability, with an average value of ≥0.8 between WUA, RD, and UD for both dorsiflexion and palmar flexion in DTSaM movement and passive movement. Consequently, the DTSaM orthosis may enable reproduction of the DTM movement. The results of the current study are novel in that we developed an orthosis with a movement similar (as judged by optical motion capture) to the DTM performed by skilled occupational therapists in previous studies.
This study has several limitations. First, the research was conducted in healthy young individuals and did not include elderly or disabled persons; therefore, the feasibility of its application in the clinical setting should be examined. Second, the neutral position of the range of motion in the 90° pronation condition cannot be defined theoretically, and the measurements may be inappropriate for high pronation angles. Third, while intra-rater reliability was evaluated, inter-rater reliability could not be assessed. Therefore, the characteristics and biases of the examiner may be reflected in the data. In the future, it will be important to compare DTSaM to conventional orthoses, to evaluate inter-examiner reliability in terms of the feel and ease of wearing the orthoses, and to obtain results based on sound scientific evidence. Furthermore, we would like to examine the clinical effect of using the DTSaM to treat patients with contractures and deformities. Moreover, the durability of the equipment has not been examined. It will be necessary to investigate the degree of fatigue of the McKibben rubber tube in relation to air pressure and the strength of the cuff.
CONCLUSION
The DTSaM orthosis reproduces a motion similar to the DTM. It is hoped that the use of DTSaM orthoses will contribute significantly to shortening the treatment period for patients with wrist disease.
Footnotes
CONFLICTS OF INTEREST : Dr. Ogawa Kazunori is employed by Daiya Industrial Inc, the manufacturer of some components of the DTSaM orthosis. The other authors declare that there are no conflicts of interest.
REFERENCES
- 1.Glasgow C,Tooth LR,Fleming J,Peters S: Dynamic splinting for the stiff hand after trauma: predictors of contracture resolution. J Hand Ther 2011;24:195–206, quiz 206. 10.1016/j.jht.2011.03.001 [DOI] [PubMed] [Google Scholar]
- 2.Wong JM: Management of stiff hand: an occupational therapy perspective. Hand Surg 2002;07:261–269. 10.1142/S0218810402001217 [DOI] [PubMed] [Google Scholar]
- 3.Flowers KR,LaStayo P: Effect of total end range time on improving passive range of motion. J Hand Ther 1994;7:150–157. 10.1016/S0894-1130(12)80056-1 [DOI] [PubMed] [Google Scholar]
- 4.Judith A: Rehabilitation of the hand. The C. V. Mosby Company, 1978, pp 591–598. [Google Scholar]
- 5.Colditz JC: Principles of splinting and splint prescription. In: Surgery of the hand and upper extremity. 1996, pp 2401–2410.
- 6.Arino K,Nemoto K: Wrist joints / hands − biomechanics useful in rehabilitation. J Jpn Clin Rehab 2005;14:958–961. [Google Scholar]
- 7.Imamura K: Analysis of wrist movement by cineradiography. J Jpn Orthop 1987;61:45–56. [Google Scholar]
- 8.Kajisako M,Sanada S,Ikeda K,Hayashi N: Kinetic analysis of the wrist with the X-ray lateral images: joint movement in flexion and extension. IEICE Technical Report 2003;M12003-51:29–34.
- 9.Werner FW,Green JK,Short WH,Masaoka S: Scaphoid and lunate motion during a wrist dart throw motion. J Hand Surg Am 2004;29:418–422. 10.1016/j.jhsa.2004.01.018 [DOI] [PubMed] [Google Scholar]
- 10.Kasubuchi K,Fujita H,Fukumoto T,Dohi Y,Fujita H,Imagita H: A relationship between dart-throwing motion plane ROM and the DASH score after distal radius fracture. J Jpn Phys Ther 2003;40:169–175. [Google Scholar]
- 11.Omori S: Biomechanics of the wrist. Jpn J Rehabil Med 2016;53:762–764. 10.2490/jjrmc.53.762 [DOI] [Google Scholar]
- 12.Arimitsu S,Murase T,Hashimoto J,Yoshikawa H,Sugamoto K,Moritomo H: Three-dimensional kinematics of the rheumatoid wrist after partial arthrodesis. J Bone Joint Surg Am 2009;91:2180–2187. 10.2106/JBJS.H.01445 [DOI] [PubMed] [Google Scholar]
- 13.Calfee RP,Leventhal EL,Wilkerson J,Moore DC,Akelman E,Crisco JJ: Simulated radioscapholunate fusion alters carpal kinematics while preserving dart-thrower’s motion. J Hand Surg Am 2008;33:503–510. 10.1016/j.jhsa.2007.12.013 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Moritomo H,Apergis EP,Garcia-Elias M,Werner FW,Wolfe SW: International Federation of Societies for Surgery of the Hand 2013 Committee’s report on wrist dart-throwing motion. J Hand Surg Am 2014;39:1433–1439. 10.1016/j.jhsa.2014.02.035 [DOI] [PubMed] [Google Scholar]
- 15.Crisco JJ,Coburn JC,Moore DC,Akelman E,Weiss AP,Wolfe SW: In vivo radiocarpal kinematics and the dart thrower’s motion. J Bone Joint Surg Am 2005;87:2729–2740. 10.2106/JBJS.D.03058 [DOI] [PubMed] [Google Scholar]
- 16.Edirisinghe Y,Troupis JM,Patel M,Smith J,Crossett M: Dynamic motion analysis of dart throwers motion visualized through computerized tomography and calculation of the axis of rotation. J Hand Surg Eur Vol 2014;39:364–372. 10.1177/1753193413508709 [DOI] [PubMed] [Google Scholar]
- 17.Braidotti F,Atzei A,Fairplay T: Dart-Splint: an innovative orthosis that can be integrated into a scapho-lunate and palmar midcarpal instability re-education protocol. J Hand Ther 2015;28:329–335, quiz 335. 10.1016/j.jht.2015.01.007 [DOI] [PubMed] [Google Scholar]
- 18.Feehan L,Fraser T: Dart-throwing motion with a twist orthoses: design, fabrication, and clinical tips. J Hand Ther 2016;29:205–212. 10.1016/j.jht.2015.12.009 [DOI] [PubMed] [Google Scholar]
- 19.Nakayama J,Denno K: Clinical experience of artificial muscle type dynamic splint for patients with painful wrist contracture. Community Caring 2020;22:30–33.
- 20.Shibata K,Ikuta M,Nomura T: Effect of rubber band compression on the peripheral blood flow when using dynamic orthoses. Mem Kanazawa Univ Sch Paramedicine 1987;11:15–21. [Google Scholar]
- 21.Shibata K,Ikuta M,Nomura T: Relation between traction force and cuff shape of orthoses on the peripheral blood flow of the digits. Mem Kanazawa Univ Sch Paramedicine 1987;12:39–42. [Google Scholar]
- 22.Nakayama J,Ogawa K,Oka H: Investigation of wrist joint cuff material and shape in new pneumatic-type dynamic splint for wrist joint disease − using blood flow and electromyogram. Bull Jpn Soc Prosthet Orthot 2021;37:40–47. [Google Scholar]
- 23.Dohi Y,Kasubuchi K,Yamaguchi F,Ono H, Omokawa S, Tanaka Y. Dart throw motion after distal radius fracture: comparison with wrist dynamic X-ray [in Japanese]. J Jpn Hand Surg 2013;29:505–509. [Google Scholar]
- 24.Garcia-Elias M: The non-dissociative clunking wrist: a personal view. J Hand Surg Eur Vol 2008;33:698–711. 10.1177/1753193408090148 [DOI] [PubMed] [Google Scholar]
- 25.Davis S,Tsagarakis N,Canderle J,Caldwell DG: Enhanced modelling and performance in braided pneumatic muscle actuators. Int J Robot Res 2003;22:213–227. 10.1177/0278364903022003006 [DOI] [Google Scholar]
- 26.Klute GK,Czerniecki JM,Hannaford B: Artificial muscles: actuators for biorobotic systems. Int J Robot Res 2002;21:295–309. 10.1177/027836402320556331 [DOI] [Google Scholar]
- 27.Klute GK,Hannaford B: Accounting for elastic energy storage in McKibben artificial muscle actuators. J Dyn Syst Meas Control 2000;122:386–388. 10.1115/1.482478 [DOI] [Google Scholar]
- 28.Reynolds DB,Repperger DW,Phillips CA,Bandry G: Modeling the dynamic characteristics of pneumatic muscle. Ann Biomed Eng 2003;31:310–317. 10.1114/1.1554921 [DOI] [PubMed] [Google Scholar]
- 29.Stewart KM: Review and comparison of current trends in the postoperative management of tendon repair. Hand Clin 1991;7:447–460. 10.1016/S0749-0712(21)01097-0 [DOI] [PubMed] [Google Scholar]
- 30.Vardakastani V,Bell H,Mee S,Brigstocke G,Kedgley AE: Clinical measurement of the dart throwing motion of the wrist: variability, accuracy and correction. J Hand Surg Eur Vol 2018;43:723–731. 10.1177/1753193418773329 [DOI] [PMC free article] [PubMed] [Google Scholar]