Abstract
Background
School and Physical Education classes (PEC) are privileged spaces, promoters of positive changes for the rest of life. High-Intensity Interval Training (HIIT) is presented as a time-efficient alternative to aerobic training, as it leverages the number of exercise participants, resulting in improvements in health outcomes. Despite the widespread interest in the advantages that the HIIT methodology reveals, there is a lack of randomized controlled studies investigating the impact on adolescents, mainly adressing adolescents’ environment, such as schools. This study aims to evaluate the utility of a HIIT program integrated into high-school PEC, as a strategy that allows students to improve their Physical Fitness, Physical Activity (PA) level, and Motivation for Exercise.
Methods
This study is a two-arm randomized controlled trial design with adolescents from the 10th to 12th grades (15–17 years). The trial will aim to recruit 300 students from 1 secondary school. The HIIT sessions will be applied in the first 10–15 min of each PEC, twice a week, for 16 weeks, ranged from 14 to 20 all-out bouts intervals, adopting a 2:1 work to rest ratio. A cut-point of ≥ 90% of maximal heart rate will be a criterion for satisfactory compliance to high-intensity exercise. A rated perceived exertion scale will be measured in each exercise session to estimate effort, fatigue, and training load. The control group will continue the usual programmed PEC. Study outcomes will be measured at baseline and after the HIIT program. Cardiorespiratory fitness is the primary outcome. Secondary outcomes include: muscular fitness, PA and motivation for exercise.
Discussion
HIIT protocols presents wide applicability in PEC and great adaptation to the facilities. The authors aim to provide novel HIIT protocols for schools.
Keywords: Fitness, Health, HIIT, Physical education, Sedentary behaviour
1. Introduction
Insufficient physical activity (PA), overweight and obesity, poor diet, low cardiorespiratory fitness (CRF), hypertension, chronic inflammation, and dyslipidemia are increasingly evident in the adolescent population [1]. Over 50% of obese children will become obese adults, with a significant increase in the risk of developing asymptomatic diseases including cardiovascular diseases, cancer and type 2 diabetes mellitus [2]. In most Western countries, children and adolescents spend too much time in sedentary behaviors, which is worsening every decade [1,[3], [4], [5]]. Data related to Health Behavior in School-Aged Children (HBSC) associate a sedentary lifestyle with headaches, sadness, irritability, and nervousness [5]. Moreover, adolescents tend to become more inactive as their age increase [6]. Short leisure time, reduced access to facilities, and low motivation to engage in physical activities, are frequently reported barriers to poor adherence to exercise programs [[7], [8], [9]]. Interventions designed to increase moderate-to-vigorous PA in Physical Education classes (PEC) indicate that interventions can increase the proportion of time students spend in higher intensities during PEC and reduce sedentary behavior, since motivational climates that emphasize effort and improvement and provide opportunities to demonstrate leadership and make decisions have a positive impact on PA [10]. Physical self-perception could be considered for adherence to PA, although Rey et al. [11] suggest that the adolescents’ psychological perception and health might be improved in response to morphological adaptations, without concomitant improvements in objectively measured physical characteristics or performances.
Therefore, High-Intensity Interval Training (HIIT) is presented as a time-efficient alternative to aerobic training [1,[12], [13], [14]], as it leverages the number of exercise participants, resulting in improvements in health outcomes, mainly from adolescents [4,[15], [16], [17]]. HIIT is characterized by relatively short periods of very intense exercise, interspersed with periods of pause or low-intensity exercise [18,19], the purpose of HIIT is that physiological systems may perform exercises of higher intensity than those achieved during a gradual maximal test [20]. HIIT is a powerful stimulus in improving body composition and preventing cardiometabolic risk in adults [21]. Preliminary studies conducted with adolescents have shown promising results on body composition and cardiometabolic health, and more effective and time-efficient intervention for improving blood pressure and aerobic capacity levels [3,6,15,22,23]. According to Bond et al. [24], time spent in high-intensity activities is the most important factor in promoting vascular health and autonomic cardiac modulation. Intense efforts have been considered inappropriate and not motivating for the general/sedentary population due to feelings of incompetence [25,26]. However, children and adolescents have expressed a clear preference for time efficiency and pleasure, and the “stop-start” nature of HIIT seems to reflect the activities traditionally observed in childhood [[1], [2], [3],14]. No negative associations in recent studies applying intense efforts are also encouraging [27,28].
Adolescents, especially older ones, are underrepresented in studies implemented in the school context [29]. Despite the widespread interest in the advantages that the HIIT methodology reveals, there is a lack of randomized controlled studies investigating the impact on adolescents [1,28], mainly adressing adolescents’ environment, such as schools [4,16]. It is known that School and PEC are privileged spaces, promoters of positive changes for the rest of life [30]. Recently, some studies presents HIIT programs targeting school-aged children [[31], [32], [33], [34]], and in a scoope of 10 years we find dozens of works with students aged 10–19 years, but only a few were implemented in the school setting. Notwithstanding some studies have been implemented in the school setting, only a few [9,27,[33], [34], [35], [36], [37], [38]] were implemented in PEC, some of which replaced the entire session with the intervention [9,36], or were applied in a classroom [39]. This study aims to investigate whether 16-weeks of HIIT implemented on PEC warm-up, compared to 16-weeks of usual PEC warm-up, can improve Physical Fitness, PA, and Motivation for Exercise in high-school adolescents.
The present manuscript details a protocol for a randomized controlled trial examining the effect of HIIT in PEC. CRF is the primary outcome and secondary outcomes includes: muscular fitness, PA and motivation for exercise. Also we aim to provide a rationale of design considerations for HIIT, such as appropriate length, intensity, and modality.
2. METHODS
2.1. Study design
This project is registered on ClinicalTrials.gov (ID: NCT04022642) and has been approved by the Ethics Committee of the University of Évora (doc. 19017). In all aspects, this trial will be conducted according to the Declaration of Helsinki on Human Research. Two public schools in the city of Beja (Portugal) will be invited to participate. Written consent will be obtained before participation from the school principal and parents. Any protocol modifications will be communicated and registered on ClinicalTrials.gov.
2.2. Study population
This study is a two-arm randomized controlled trial design with adolescents from the 10th to 12th grades (15–17 years old). This age group has been selected because it is underrepresented in studies implemented in the school context [28].
2.3. Recruitment
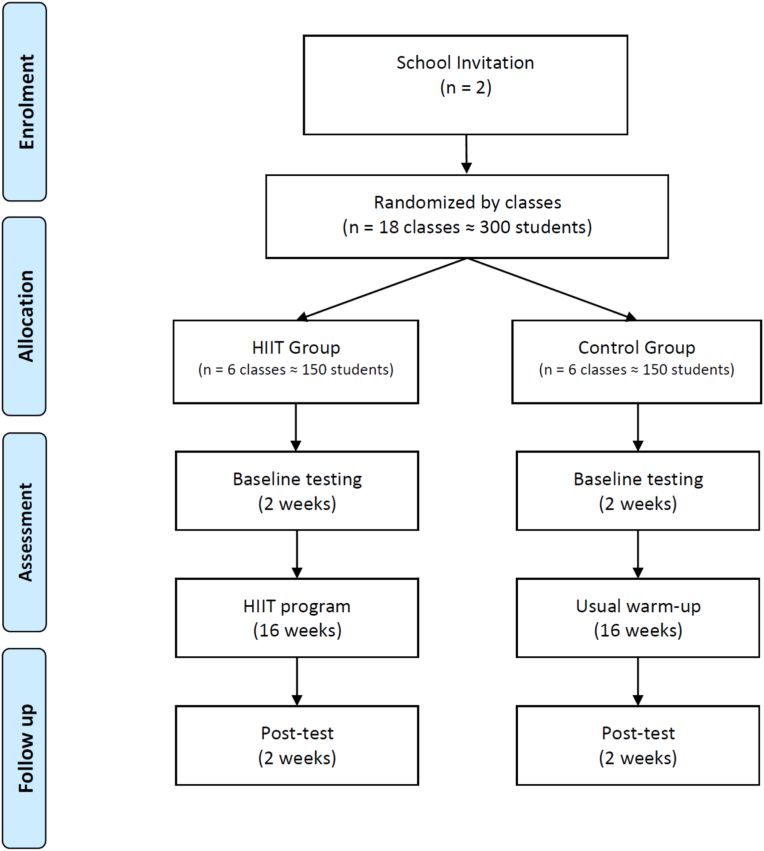
Twelve from a total of 18 classes with an average of 25 students each, recruited from a public school in the city of Beja, Portugal (Fig. 1) will be randomized to either a 16-weeks of HIIT (HIIT-G, n ≈ 150 students) implemented on PEC warm-up or a control group (CON-G, n ≈ 150 students) of usual PEC warm-up. After an invitation, the researchers will meet with the school principal to provide information on the whole project. After accepting to participate, adolescents and their parents will be informed of a full description of the scientific background, objectives, and safety.
Fig. 1.
Study design.
2.4. Randomization
School principal, as a person independent of the study, will conceal participant allocation by shaking a bag with all 18 classes, before baseline testing. Classes will be randomized such that two classes from each grade will be allocated to the intervention condition and the other two to the control condition. Using this approach, each class will have an equal chance of being allocated to the intervention condition, while maintaining an appropriate balance of grades across the two conditions.
2.5. Inclusion/exclusion criteria
As stated above, girls and boys from the 10th to 12th grades (15–17 years old) taking part in the regular PEC will be included in the study. For ethical reasons, adolescents who have any physical, psychiatric, and/or psychological disability will also be included in the intervention if both children and parents approve their participation. Once the evaluation process is concluded, these children could be excluded from the main analysis. Students will be ineligible if they do not provide parental consent to participate, have physical limitations, or reveal intellectual disabilities.
2.6. Sample size
Power calculations were based on the primary outcome of CRF, assessed using the Yo-Yo Intermittent Endurance Test level one [40]. To detect a clinically meaningful baseline-adjusted between-group difference of six laps [27,41] with 80% power at a 5% significance level will require 158 students per treatment group (ie, 12 classes of 13 students from each school), for a potential drop-out rate of 15% at our primary study end point (i.e., 16 weeks).
2.7. Intervention group
Throughout the 16-weeks intervention period the HIIT-G will take part in the regular 90min PEC twice a week, conducted by the schools’ PEC teachers following the regular curriculum. The HIIT-G replaces the warm-ups established in the PEC curriculum with the proposed HIIT training sessions. After the HIIT sessions, students will complete the planned PEC.
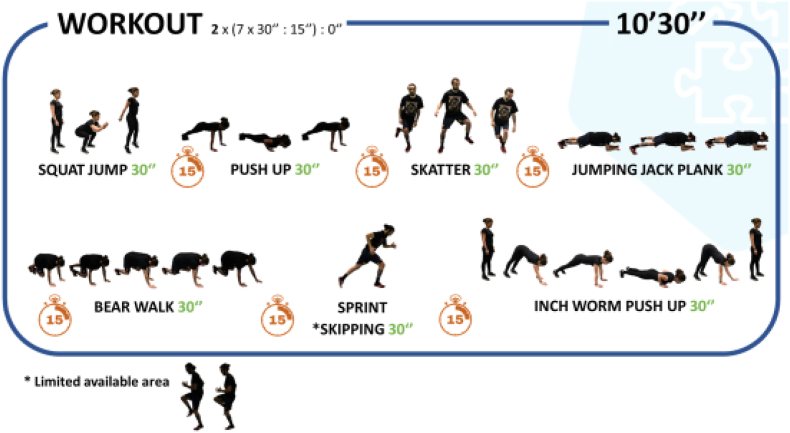
The HIIT sessions will be applied in the first 10–15 min of each PEC, including a brief warm-up, ranged from 14 to 20 all-out bouts intervals, adopting a 2:1 work to rest ratio, involving a combination of aerobic and body weight muscle-strengthening exercises, and designed to be fun and engaging as well as vigorous in nature (Fig. 2). Most protocols in the literature opted for 1:1 density and SPRINT as modality [23]. Some, recording large effect sizes on CRF [9,36], PA [9], strength, power, and speed [39], needed only 6 min three [9,36] and four times [39] a week, and chose to use all-out bouts instead of a percentage of Maximal Aerobic Speed (MAS). In adults, previous findings suggest that a 2:1 work-to-rest ratio is optimal during HIIT for both men and women [42]. We aim to provide novel HIIT protocols for schools with less volume (only twice a week) and higher density (less rest in each interval), to implement PA interventions that retain the health-enhancing effects and satisfy the adolescents’ desire for enjoyment and variety.
Fig. 2.
Graphical description of an example session.
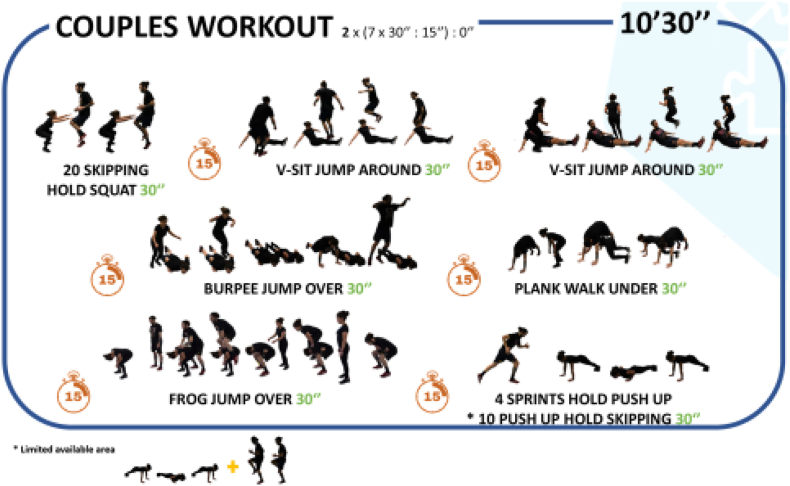
To promote exercise adherence, sessions were designed progressively from 4 min in week zero to 10 min in week three using the Tabata protocol (20s intense work, followed by 10s rest). From week four to week seven, the same volume but using 30s intense work, followed by 15s rest. From weeks eight to 16, sessions will be completed in pairs (Fig. 3). Participants will be able to give additional elements of choice, such as music, exercises, and workouts.
Fig. 3.
Graphical description of an example session (couples).
A cut-point of ≥ 90% of maximal HR will be a criterion for satisfactory compliance to high-intensity exercise. HR has become one of the most used outcomes to assess the intensity, and several authors suggest that each interval corresponds to a value equal to or greater than 90%HRmax [[43], [44], [45]]. An optimal stimulus that promotes cardiovascular and peripheral adaptations implies several minutes per session in the so-called red zone, which usually means a minimum intensity of 90%VO2max [46]. It is expected that HR reaches maximum values (>90–95% HRmax) close to the speed/power associated with VO2max, which does not always happen, especially in very short exercises (<30 s) [43,44]. It may be related to the known delay in HR response at the beginning of exercise, which is slower than the VO2 response. During the supervised intervention, the researchers will record HR using a technology based on forearm plethysmography (Scosche Industries, CA, USA) to ensure compliance with the exercise stimulus at the predetermined target HR zone. Besides, rating perceived exertion (RPE) will also be measured in each exercise session to estimate effort, fatigue, and training load, targeting >17 on the 6–20 Borg scale [47,48].
2.8. Control group
Throughout the 16-weeks intervention period the CON-G will take part in the regular 90min PEC twice a week, conducted by the schools’ PEC teachers following the regular curriculum.
2.9. Outcome measures (primary and secondary)
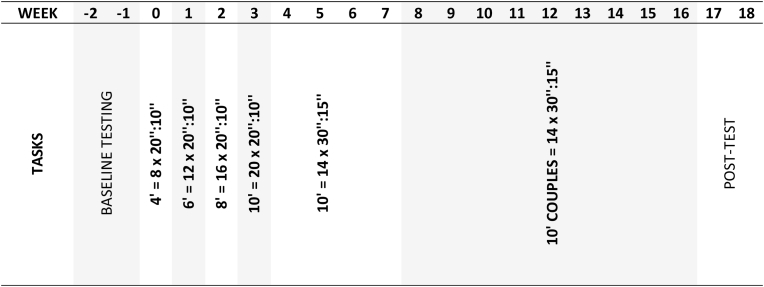
All primary and secondary outcomes will be measured at baseline two weeks prior the intervention, and after 16-weeks of the HIIT program (Fig. 4). CRF is the primary outcome. Secondary outcomes includes: muscular fitness, PA and motivation for exercise. All assessments will be conducted by the Principal Investigator at the schools participating in the study. Anthropometric assessments will be conducted sensitively by the presence of a same-sex research staff when possible. The Principal Investigator will provide a brief verbal description and demonstration of each fitness test before commencement. Measures and data collection will be evaluated by the authors, not blinded for group allocation.
Fig. 4.
Schedule of assessment and HIIT intervention. (‘) Total work in minutes, (‘’:’’) ration ON:OFF in seconds.
2.9.1. Physical fitness assessment
CRF will be assessed using the Yo-Yo Intermittent Endurance Test level one. This test has been previously confirmed as valid and reliable to assess aerobic fitness and intermittent high-intensity endurance in 9-to 16-year-old children [40]. This test consists of incremental shuttle running starting from the speed of 8 km·h−1 until exhaustion. The maximum running speed is 14.5 km·h−1. Each shuttle run consists of 2 × 20 m interspersed by 10 s of active recovery (slow jog or walk) for a short 2.5 m shuttle. Within each speed stage, there are several shuttle runs. Running speed is prescribed by a pre-recorded audio track. Participants must reach the 20 m line by the time each audio is heard. The test is terminated if the participant is unable to maintain the required speed for the second time during the shuttle running bout. The total number of laps will be used to estimate maximal aerobic capacity (i.e., VO2 max), using the following equation: IRT1 distance (m) x 0.0084 + 36.4 (ml.kg−1.min−1) [49]. Heart Rate (HR) will be monitored by telemetric HR during testing. The peak HR recorded during the test will be assumed to be representative of maximal HR [50].
FITescola® is a battery used to assess physical fitness in the Portuguese school setting [51]. Upper body muscle force will be assessed through the push‐up test. The test starts with the participant's hands and feet touching the floor, and the body in a plank position, with feet apart and the hands positioned below the shoulder line. The participants should lower the body until forming a 90° angle between the arm and the forearm and then return to the starting position. This action will be repeated with a previously defined cadence of 20 push‐ups per minute.
Participants’ body composition and body mass will be measured to the nearest 0.1 kg in light sportswear on an electrical weight scale (Tanita MC -780), and height will be measured to the nearest 1 mm using a portable stadiometer (Seca 213 Portable Height Measuring Rod Stadiometer). Both weight and height will be measured twice to reduce the risk of measurement error. A third measurement will occur should there be a difference of >0.1 kg for weight and >0.3 cm for height between the first and second measurements. Considering that the portable stadiometer has a precision of 3 mm and the scale of 0.1 kg, making a third measurement when the difference between the first and the second exceeds these precision levels can be justified by the objective of reducing to the maximum the technical error of measurement (TEM) and, consequently, the reliability of the results to attain. TEM should not be higher than 1.5% (intra-observer) or 2.0% (inter-observer) [52]. BMI will be calculated using the standard formula (weight [kg]/height [m2]).
2.9.2. Physical activity, motivation, and dietary registration
Before the exercise intervention, both HIIT-G and CON-G participants will be instructed to maintain their dietary or lifestyle behaviors during the intervention period, so that, in this way, possible changes in eating habits may not contaminate the results. Daily dietary intake will be estimated with a validated self-reported food frequency questionnaire [53], which list food types and meals typical of a Portuguese diet. Will be assessed using a semiquantitative food frequency questionnaire of the previous month, covering 82 food items or beverage categories, and a frequency section with nine possible responses ranging from never to six or more times per day.
As has been recommended in a recent systematic review [54], triaxial accelerometers will be used to determine PA levels, sedentary time, and sleeping time during 24 h (seven days). Participants will be instructed to wear an ActiGraph wGT3X-BT accelerometer on their waist for 24 h/day (will be only removed during shower time or swimming activities), fixed to an elasticized belt and placed on the right side of the participant's hip, for seven consecutive days. Adolescents will be encouraged to wear accelerometers on their dominant wrist [55] during the night to assess the time and quality of sleep. At least three weekdays and one weekend day will be considered as a minimum recording time for valid registers. Physical activity will be calculated separately on weekdays and weekend days (i.e., mean minutes per day), using existing thresholds for categorizing physical activity into a light, moderate and vigorous intensity.
Moreover, a self-reported questionnaire – the International Physical Activity Questionnaire (i-PAQ) – will assess the participants’ physical activity behavior during the prior seven days, including the number of days spent engaged in sporting activity, physical activity during the school day, and physical activity out-with the school day. This questionnaire has been validated in different countries [56], and has shown acceptable psychometric properties to assess PA levels with good reliability.
Motivation will be assessed with the Behavioral Regulation in Exercise Questionnaire 3 (BREQ-3) [57]. BREQ-3 is a valid and reliable measurement instrument to measure behavior regulation underlying the self-determination theory in the exercise domain and consists of 24 items with a five-point Likert scale, which varies between 1 (“Strongly Disagree”) and 4 (“Strongly Agree”).
2.10. Statistical analyses
The final data will be analyzed using IBM SPSS 26.0 (SPSS, Inc., Chicago, IL, USA). An exploratory analysis will be performed to determine the frequency, range, variability, and distribution type for each variable, to use the most appropriate statistical test when comparisons will be necessary. According to the subjects’ recruitment, cluster analyses (a-priori segmentation approach) will be also considered.
If necessary, analyses will be adjusted for baseline differences. In order to avoid outcomes baseline imbalance, analysis of covariance should be used to adjust for baseline in the data analysis stage. Moreover, a post-hoc cluster analysis could be performed using interrelated variables from which subjects could be clustered into groups whose average within-group similarity is high while between-group similarity is low. The primary analysis of the data set will be carried out according to the ‘intention to treat’ principle. Analyses will include standard descriptive statistics, t tests, correlation, regression and two-way repeated measures ANOVA or the comparable non-parametric test as necessary to examine differences between and within groups. Missing data will be handled by multiple imputation approach [58].
With the aim to minimize threats to internal validity, thereby strengthening external validity and improving the generalizability of results, an independent statistician will be in charge of the data analysis.
3. DISCUSSION
On adolescents, despite differences in protocols on intensity like all-out bouts or % of MAS, modality (sprints vs calisthenics), and volume (6min–35min/session), most of them opted for 1:1 density [23]. Almost all programs are limited to sprints, but some were designed to be implemented in couples [27,28,37], or individually [38] through calisthenic exercises and plyometrics. Some studies that exceed 10 min per session [8,28,59], for 12 weeks, did not go beyond the moderate effect on body composition and physical fitness, compared to protocols below 10 min and with the same Effect Size [7,27,38,60,61]. Interestingly, other protocols record Large Effect Size on CRF [9,36], PA [9], strength, power, and speed [39], needed only 6 min three [9,36] and four times [39] a week, for only four [9,39] and seven weeks [36]. It should be also emphasized that the same three studies that record Large Effect Sizes chose to use all-out bouts instead of a percentage of MAS, reinforcing the importance of including resistance training as a HIIT modality.
Few studies have objectively measured internal load by monitoring HR [8,9,28,37,38,59,60] or RPE [38,39]. Most studies opted to set intensity through external load, expressed in speed or distances. The more traditional HIIT methodology reflects a temporal efficiency in the improvement of several health markers and aerobic/anaerobic performance but lowered impact strength, muscle strength, and power. New protocols that also include resistance exercises, can induce a higher amount of beneficial adaptations in young people [62].
Optimal exercise duration and rest intervals remain ambiguous [23]. Some studies that did not report improvements in body composition [7,60] revealed that the CON-G significantly worsened, which gives HIIT a possible protective effect on body composition in these populations. Like body composition, a possible protective effect of HIIT was observed when the improvements in physical fitness were not significant, as the CON-G significantly worsened the performance [9,35,36,60]. Ultimately, it can serve as protective factor against loss of functional capacity in youth, weight gain, and risk factors associated with physical inactivity, as teenagers tend to become more inactive as their age increases.
Despite some limitations, as the absence of a detailed evaluation to determine intervention fidelity to confirm treatment/protocol adherence, this project aims to evaluate the utility of a HIIT program integrated into high-school PEC, on Physical Fitness, PA, and Motivation for Exercise. Although some studies have been implemented in the school setting, only a few [9,27,[35], [36], [37], [38]] were implemented in PEC. With this study, the authors aim to provide novel HIIT protocols for schools with less volume (only twice a week) and higher density (less rest in each interval), to implement PA interventions, which retain the health-enhancing effects and satisfy the adolescents’ desire for enjoyment and variety. The efficiency seems evident that HIIT protocols implemented in schools reflects in the improvement of physical fitness and reduction of sedentary behaviors, compared to other types of less intense and higher volume activities. This efficiency, resulting from the reduced time required (on average, about 10 min), reflects the wide applicability that these protocols could have in PEC and the great adaptation to the facilities (including classrooms). The introduction of HIIT in the school context has a high potential for improving physical fitness [7,8,29,38,39,59,60,[63], [64], [65], [66]] and PA [37,66,67], and a moderate effect on improving body composition in adolescents [7,38,59,63,65,68]. Moreover, exercise protocols that result in physiological improvements and adaptations in terms of health in a short time are of interest to physical education teachers, as well as to rehabilitation, health, and exercise professionals.
Author contributions
Conceptualization, A.B., L.C., and A.R.; methodology, L.C., and A.R.; software, A.B. validation, A.B. and A.R.; ormal analysis, A.B. and L.C. investigation, A.B., and A.R.; resources, A.B., and L.C.; data curation, A.B. and A.R.; writing—original draft preparation, A.B.; writing—review and editing, A.B., L.C. and A.R.; visualization, A.B., L.C. and A.R.; supervision, L.C., and A.R.; project administration, A.B., L.C., and A.R.; funding acquisition, A.B., L.C., and A.R. All authors have read and agreed to the published version of the manuscript.
Declaration of competing interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgments
Funding: This work was supported by the Portuguese national funding agency for science, research, and technology, Fundação para a Ciência e Tecnologia [grant numbers SFRH/BD/136869/2018]
Contributor Information
André Filipe Paulino da Silva Bento, Email: andresbento@uevora.pt.
Luis Carrasco Páez, Email: lcarrasco@us.es.
Armando Manuel de Mendonça Raimundo, Email: ammr@uevora.pt.
References
- 1.Logan G.R., et al. A review of adolescent high-intensity interval training. Sports Med. 2014;44(8):1071–1085. doi: 10.1007/s40279-014-0187-5. [DOI] [PubMed] [Google Scholar]
- 2.Dias K.A., et al. Effects of exercise intensity and nutrition advice on myocardial function in obese children and adolescents: a multicentre randomised controlled trial study protocol. BMJ Open. 2016;6(4):e010929. doi: 10.1136/bmjopen-2015-010929. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Herget S., et al. High-intensity interval training for overweight Adolescents: program acceptance of a media supported intervention and changes in body composition. Int. J. Environ. Res. Publ. Health. 2016;13(11) doi: 10.3390/ijerph13111099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Logan G.R., et al. Low-active male adolescents: a dose response to high-intensity interval training. Med. Sci. Sports Exerc. 2016;48(3):481–490. doi: 10.1249/MSS.0000000000000799. [DOI] [PubMed] [Google Scholar]
- 5.Marques A., et al. Health complaints among adolescents: associations with more screen-based behaviours and less physical activity. J. Adolesc. 2015;44:150–157. doi: 10.1016/j.adolescence.2015.07.018. [DOI] [PubMed] [Google Scholar]
- 6.Bluher S., et al. Cardiometabolic risk markers, adipocyte fatty acid binding protein (aFABP) and the impact of high-intensity interval training (HIIT) in obese adolescents. Metabolism. 2017;68:77–87. doi: 10.1016/j.metabol.2016.11.015. [DOI] [PubMed] [Google Scholar]
- 7.Lau P.W.C., et al. Effects of high-intensity intermittent running exercise in overweight children. Eur. J. Sport Sci. 2015;15(2):182–190. doi: 10.1080/17461391.2014.933880. [DOI] [PubMed] [Google Scholar]
- 8.Cvetkovic N., et al. Exercise training in overweight and obese children: recreational football and high-intensity interval training provide similar benefits to physical fitness. Scand. J. Med. Sci. Sports. 2018;28(Suppl 1):18–32. doi: 10.1111/sms.13241. [DOI] [PubMed] [Google Scholar]
- 9.Martin-Smith R., et al. Sprint interval training and the school curriculum: benefits upon cardiorespiratory fitness, physical activity profiles, and cardiometabolic risk profiles of healthy adolescents. Pediatr. Exerc. Sci. 2019;31(3):296–305. doi: 10.1123/pes.2018-0155. [DOI] [PubMed] [Google Scholar]
- 10.Lonsdale C., et al. A systematic review and meta-analysis of interventions designed to increase moderate-to-vigorous physical activity in school physical education lessons. Prev. Med. 2013;56(2):152–161. doi: 10.1016/j.ypmed.2012.12.004. [DOI] [PubMed] [Google Scholar]
- 11.Rey O., et al. Effects of combined vigorous interval training program and diet on body composition, physical fitness, and physical self-perceptions among obese adolescent boys and girls. Pediatr. Exerc. Sci. 2017;29(1):73–83. doi: 10.1123/pes.2016-0105. [DOI] [PubMed] [Google Scholar]
- 12.Kong Z., et al. Short-term high-intensity interval training on body composition and blood glucose in overweight and obese young women. J Diabetes Res. 2016:4073618. doi: 10.1155/2016/4073618. 2016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Zhang H., et al. Comparable effects of high-intensity interval training and prolonged continuous exercise training on abdominal visceral fat reduction in obese young women. J. Diabetes Res. 2017:9. doi: 10.1155/2017/5071740. 2017. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Kilian Y., et al. Markers of biological stress in response to a single session of high-intensity interval training and high-volume training in young athletes. Eur. J. Appl. Physiol. 2016;116(11–12):2177–2186. doi: 10.1007/s00421-016-3467-y. [DOI] [PubMed] [Google Scholar]
- 15.Garcia-Hermoso A., et al. Is high-intensity interval training more effective on improving cardiometabolic risk and aerobic capacity than other forms of exercise in overweight and obese youth? A meta-analysis. Obes. Rev. 2016;17(6):531–540. doi: 10.1111/obr.12395. [DOI] [PubMed] [Google Scholar]
- 16.Harris N.K., et al. Acute responses to resistance and high-intensity interval training in early adolescents. J. Strength Condit Res. 2017;31(5):1177–1186. doi: 10.1519/JSC.0000000000001590. [DOI] [PubMed] [Google Scholar]
- 17.Lazzer S., et al. Effects of high-intensity interval training on physical capacities and substrate oxidation rate in obese adolescents. J. Endocrinol. Invest. 2017;40(2):217–226. doi: 10.1007/s40618-016-0551-4. [DOI] [PubMed] [Google Scholar]
- 18.Fisher G., et al. Lymphocyte enzymatic antioxidant responses to oxidative stress following high-intensity interval exercise. J. Appl. Physiol. 2011;110(3):730–737. doi: 10.1152/japplphysiol.00575.2010. 1985. [DOI] [PubMed] [Google Scholar]
- 19.Gibala M.J., Jones A.M. Physiological and performance adaptations to high-intensity interval training. Nestle. Nutr. Inst. Workshop. Ser. 2013;76:51–60. doi: 10.1159/000350256. [DOI] [PubMed] [Google Scholar]
- 20.Stuckey M.I., et al. Autonomic recovery following sprint interval exercise. Scand. J. Med. Sci. Sports. 2012;22(6):756–763. doi: 10.1111/j.1600-0838.2011.01320.x. [DOI] [PubMed] [Google Scholar]
- 21.Sim A.Y., et al. Effects of high-intensity intermittent exercise training on appetite regulation. Med. Sci. Sports Exerc. 2015;47(11):2441–2449. doi: 10.1249/MSS.0000000000000687. [DOI] [PubMed] [Google Scholar]
- 22.Costigan S.A., et al. High-intensity interval training for improving health-related fitness in adolescents: a systematic review and meta-analysis. Br. J. Sports Med. 2015;49(19):1253–1261. doi: 10.1136/bjsports-2014-094490. [DOI] [PubMed] [Google Scholar]
- 23.Eddolls W.T.B., et al. High-intensity interval training interventions in children and adolescents: a systematic review. Sports Med. 2017;47(11):2363–2374. doi: 10.1007/s40279-017-0753-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Bond B., et al. Two weeks of high-intensity interval training improves novel but not traditional cardiovascular disease risk factors in adolescents. Am. J. Physiol. Heart Circ. Physiol. 2015;309(6):H1039–H1047. doi: 10.1152/ajpheart.00360.2015. [DOI] [PubMed] [Google Scholar]
- 25.Hardcastle S.J., et al. Why sprint interval training is inappropriate for a largely sedentary population. Front. Psychol. 2014;5:1505. doi: 10.3389/fpsyg.2014.01505. 1505. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Biddle S.J.H., Batterham A.M. High-intensity interval exercise training for public health: a big HIT or shall we HIT it on the head? Int. J. Behav. Nutr. Phys. Activ. 2015;12(1):95. doi: 10.1186/s12966-015-0254-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Costigan S.A., et al. Preliminary efficacy and feasibility of embedding high intensity interval training into the school day: a pilot randomized controlled trial. Prev. Med. Rep. 2015;2:973–979. doi: 10.1016/j.pmedr.2015.11.001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Leahy A.A., et al. Feasibility and preliminary efficacy of a teacher-facilitated high-intensity interval training intervention for older adolescents. Pediatr. Exerc. Sci. 2019;31(1):107–117. doi: 10.1123/pes.2018-0039. [DOI] [PubMed] [Google Scholar]
- 29.Leahy A.A., et al. Feasibility and preliminary efficacy of a teacher-facilitated high-intensity interval training intervention for older adolescents. Pediatr. Exerc. Sci. 2019;31(1):107–117. doi: 10.1123/pes.2018-0039. [DOI] [PubMed] [Google Scholar]
- 30.Mura G., et al. Physical activity interventions in schools for improving lifestyle in European countries. Clin. Pract. Epidemiol. Ment. Health : CP & EMH. 2015;11(Suppl 1 M5):77–101. doi: 10.2174/1745017901511010077. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Sharp C.A., et al. Identifying facilitators and barriers for adolescents participating in a school-based HIIT intervention: the eXercise for asthma with commando Joe's® (X4ACJ) programme. BMC Publ. Health. 2020;20(1):609. doi: 10.1186/s12889-020-08740-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Tottori N., et al. Effects of high intensity interval training on executive function in children aged 8-12 years. Int. J. Environ. Res. Publ. Health. 2019;16(21):4127. doi: 10.3390/ijerph16214127. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Bogataj Š., et al. Effects of school-based exercise and nutrition intervention on body composition and physical fitness in overweight Adolescent girls. Nutrients. 2021;13(1) doi: 10.3390/nu13010238. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Ketelhut S., et al. Effectiveness of multi-activity, high-intensity interval training in school-aged children. Int. J. Sports Med. 2020;41(4):227–232. doi: 10.1055/a-1068-9331. [DOI] [PubMed] [Google Scholar]
- 35.Buchan D.S., et al. The effects of a novel high intensity exercise intervention on established markers of cardiovascular disease and health in Scottish adolescent youth. J. Publ. Health. Res. 2012;1(2):155–157. doi: 10.4081/jphr.2012.e24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Martin R., et al. Sprint interval training (SIT) is an effective method to maintain cardiorespiratory fitness (CRF) and glucose homeostasis in Scottish adolescents. Biol. Sport. 2015;32(4):307–313. doi: 10.5604/20831862.1173644. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Costigan S.A., et al. Exploring the impact of high intensity interval training on adolescents' objectively measured physical activity: findings from a randomized controlled trial. J. Sports Sci. 2018;36(10):1087–1094. doi: 10.1080/02640414.2017.1356026. [DOI] [PubMed] [Google Scholar]
- 38.Alonso-Fernández D., et al. Impact of a HIIT protocol on body composition and VO2max in adolescents. Sci. Sports. 2019;34(5):341–347. [Google Scholar]
- 39.Engel F.A., et al. Classroom-based micro-sessions of functional high-intensity circuit training enhances functional strength but not cardiorespiratory fitness in school children-A feasibility study. Front. Pub. Health. 2019;7:9. doi: 10.3389/fpubh.2019.00291. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Póvoas S.C., et al. Reliability and validity of Yo-Yo tests in 9- to 16-year-old football players and matched non-sports active schoolboys. Eur. J. Sport Sci. 2016;16(7):755–763. doi: 10.1080/17461391.2015.1119197. [DOI] [PubMed] [Google Scholar]
- 41.Weston K.L., et al. Effect of novel, school-based high-intensity interval training (HIT) on cardiometabolic health in adolescents: project FFAB (fun fast activity blasts) - an exploratory controlled before-and-after trial. PLoS One. 2016;11(8):e0159116. doi: 10.1371/journal.pone.0159116. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Laurent C.M., et al. Sex-specific responses to self-paced, high-intensity interval training with variable recovery periods. J. Strength Condit Res. 2014;28(4):920–927. doi: 10.1519/JSC.0b013e3182a1f574. [DOI] [PubMed] [Google Scholar]
- 43.Hanssen H., et al. Acute effects of interval versus continuous endurance training on pulse wave reflection in healthy young men. Atherosclerosis. 2015;238(2):399–406. doi: 10.1016/j.atherosclerosis.2014.12.038. [DOI] [PubMed] [Google Scholar]
- 44.Helgerud J., et al. Aerobic high-intensity intervals improve VO2max more than moderate training. Med. Sci. Sports Exerc. 2007;39(4):665–671. doi: 10.1249/mss.0b013e3180304570. [DOI] [PubMed] [Google Scholar]
- 45.Bonsu B., Terblanche E. The training and detraining effect of high-intensity interval training on post-exercise hypotension in young overweight/obese women. Eur. J. Appl. Physiol. 2016;116(1):77–84. doi: 10.1007/s00421-015-3224-7. [DOI] [PubMed] [Google Scholar]
- 46.Buchheit M., Laursen P.B. High-intensity interval training, solutions to the programming puzzle: Part I: cardiopulmonary emphasis. Sports Med. 2013;43(5):313–338. doi: 10.1007/s40279-013-0029-x. [DOI] [PubMed] [Google Scholar]
- 47.Borg G. Perceived exertion as an indicator of somatic stress. Scand. J. Rehabil. Med. 1970;2(2):92–98. [PubMed] [Google Scholar]
- 48.Williams J.G., Eston R.G., Stretch C. Use of the Rating of Perceived Exertion to Control Exercise Intensity in Children. 1991;3(1):21. [Google Scholar]
- 49.Tanner R.K., Gore C.J. second ed. Australian Institute of Sport: Human Kinetics; 2014. Physiological Tests for Elite Athletes. [Google Scholar]
- 50.Krustrup P., et al. The yo-yo intermittent recovery test: physiological response, reliability, and validity. Med. Sci. Sports Exerc. 2003;35(4):697–705. doi: 10.1249/01.MSS.0000058441.94520.32. [DOI] [PubMed] [Google Scholar]
- 51.Henriques-Neto D., et al. Test–retest reliability of physical fitness tests among young athletes: the FITescola® battery. Clin. Physiol. Funct. Imag. 2020;40(3):173–182. doi: 10.1111/cpf.12624. [DOI] [PubMed] [Google Scholar]
- 52.Talita Adão P., et al. Technical error of measurement in anthropometry. Rev. Bras. Med. do Esporte. 2005;11(1):81–85. [Google Scholar]
- 53.Lopes C., et al. Intake and adipose tissue composition of fatty acids and risk of myocardial infarction in a male Portuguese community sample. J. Am. Diet Assoc. 2007;107(2):276–286. doi: 10.1016/j.jada.2006.11.008. [DOI] [PubMed] [Google Scholar]
- 54.Migueles J.H., et al. Accelerometer data collection and processing criteria to assess physical activity and other outcomes: a systematic review and practical considerations. Sports Med. 2017;47(9):1821–1845. doi: 10.1007/s40279-017-0716-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Sadeh A., Sharkey K.M., Carskadon M.A. Activity-based sleep-wake identification: an empirical test of methodological issues. Sleep. 1994;17(3):201–207. doi: 10.1093/sleep/17.3.201. [DOI] [PubMed] [Google Scholar]
- 56.Craig C.L., et al. International physical activity questionnaire: 12-country reliability and validity. Med. Sci. Sports Exerc. 2003;35(8):1381–1395. doi: 10.1249/01.MSS.0000078924.61453.FB. [DOI] [PubMed] [Google Scholar]
- 57.Cid L., et al. The behavioral regulation in exercise questionnaire (BREQ-3) Portuguese-version: evidence of reliability, validity and invariance across gender. Front. Psychol. 2018;9:1940. doi: 10.3389/fpsyg.2018.01940. 1940. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Rubin D.B. Wiley; New York: 1987. Multiple Imputation for Nonresponse in Surveys. [Google Scholar]
- 59.Racil G., et al. Effects of high vs. moderate exercise intensity during interval training on lipids and adiponectin levels in obese young females. Eur. J. Appl. Physiol. 2013;113(10):2531–2540. doi: 10.1007/s00421-013-2689-5. [DOI] [PubMed] [Google Scholar]
- 60.Buchan D.S., et al. High intensity interval running enhances measures of physical fitness but not metabolic measures of cardiovascular disease risk in healthy adolescents. BMC Publ. Health. 2013;13:498. doi: 10.1186/1471-2458-13-498. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Racil G., et al. Greater effects of high- compared with moderate-intensity interval training on cardio-metabolic variables, blood leptin concentration and ratings of perceived exertion in obese adolescent females. Biol. Sport. 2016;33(2):145–152. doi: 10.5604/20831862.1198633. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Bento A., Loureiro V. High-intensity interval training: monitoring and effect between genders. J. Strength Condit Res. 2018;32(9):e42–e43. [Google Scholar]
- 63.Racil G., et al. Plyometric exercise combined with high-intensity interval training improves metabolic abnormalities in young obese females more so than interval training alone. Appl. Physiol. Nutr. Metabol. 2016;41(1):103–109. doi: 10.1139/apnm-2015-0384. [DOI] [PubMed] [Google Scholar]
- 64.Buchan D.S., et al. The effects of a novel high intensity exercise intervention on established markers of cardiovascular disease and health in Scottish adolescent youth. J. Publ. Health. Res. 2012;1(2):155–157. doi: 10.4081/jphr.2012.e24. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 65.Racil G., et al. Greater effects of high- compared with moderate-intensity interval training on cardio-metabolic variables, blood leptin concentration and ratings of perceived exertion in obese adolescent females. Biol. Sport. 2016;33(2):145–152. doi: 10.5604/20831862.1198633. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 66.Martin-Smith R., et al. Sprint interval training and the school curriculum: benefits upon cardiorespiratory fitness, physical activity profiles, and cardiometabolic risk profiles of healthy adolescents. Pediatr. Exerc. Sci. 2019;31(3):296–305. doi: 10.1123/pes.2018-0155. [DOI] [PubMed] [Google Scholar]
- 67.Martin R., et al. Sprint interval training (SIT) is an effective method to maintain cardiorespiratory fitness (CRF) and glucose homeostasis in Scottish adolescents. Biol. Sport. 2015;32(4):307–313. doi: 10.5604/20831862.1173644. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Costigan S.A., et al. Preliminary efficacy and feasibility of embedding high intensity interval training into the school day: a pilot randomized controlled trial. Prev. Med. Rep. 2015;2:973–979. doi: 10.1016/j.pmedr.2015.11.001. [DOI] [PMC free article] [PubMed] [Google Scholar]