Abstract
Objectives:
The aim of this paper is to determine the empirical formula for calculating the incident air kerma (Ki), used as a patient dose descriptor in the intraoral radiographic imaging.
Methods:
The data for the formula were collected during the regular annual inspection of intraoral dental X-ray units in 2018, 2019 and early 2020. The measurement data of 50 X-ray units were processed to develop the formula. Exposure factors for imaging molars of the upper jaw of an average patient in a clinical setting were used in the measurement. The formula validity was statistically evaluated using coefficient of correlation, standard error of the fitted function and the mean relative percentage deviation.
Results:
The measurement values of the radiation doses and calculated values obtained by using the final formula showed good agreement – the mean relative percentage deviation values less than ±15%.
Conclusions:
Although there are differences in X-ray units, voltages, manufacturers and device architectures (single-phase and high-frequency), the measurement data comply well with computed ones in all cases.
Keywords: Intraoral, Ionising Radiation, Dental x-ray, Air kerma
Introduction
It is well known that the medical exposure is the single largest category of population exposure to ionising radiation.1 The frequency of dental X-ray procedures is high, but the effective dose per procedure is low. It has been reported that the frequency of dental radiographic procedures in the European Union is about 32% of all plain radiography procedures. Nevertheless, the low mean effective doses of these procedures make their contribution to the collective effective dose insignificant, typically only 2–4% of the total collective effective dose for the plain radiography.2 According to 2012 data, more than 25% of all X-ray machines in the Republic of Serbia are intraoral dental X-ray units.3 There is a regular quality control by licensed out-of-hospital services.4 The majority of examinations were found to be periapical radiography (recordings spanning two to four teeth), while other bitewing, occlusal oblique lateral techniques were almost non-existent.5 Procedures are usually performed by X-ray technicians, although when there is the only one device in a practice, the procedure is usually performed by a dentist with insufficient radiation protection awareness. It has been shown that the patient dose recording could raise radiation protection awareness.
Because dose indices are unknown for many dental radiographic units in Serbia, we propose the empirical formula to calculate the incident air kerma (Ki) and kerma–area-product (KAP). This can provide an insight into the unmeasured doses and can be used to calculate the diagnostic reference level (DRL). The DRL has proven to be an effective tool for optimisation of the patient protection related to medical exposure of patients in diagnostic and interventional procedures.6 It can also be used to determine staff doses and to calculate protective barriers in the practice.
There are references of mathematical formulas for calculating incident air kerma (Ki) (or similar quantities) for conventional radiography X-ray units.7–12 However, no data of the same formula for calculating the Ki of intraoral radiography could be found. Therefore, the aim of this paper is to determine an empirical formula for calculating the Ki in the intraoral radiography.
Methods and materials
The performance testing of dental X-ray units was performed by a calibrated multimeter (semiconductor detector) MPD Barracuda (RTI Electronics AB, Sweden). The multimeter is calibrated on an annual basis at Secundary Standard Dosimetry Laboratory (SSDL) INN Vinča Laboratory for Radiation Protection, Belgrade, Serbia. The measurement uncertainty of Barracuda MPD multimeter is ±7%. All performance testing measurements were repeated five times.
Exposure parameters of 50 intraoral X-ray units were collected during the regular annual inspections in 2018, 2019 and early 2020 in public and private facilities. Then, these parameters were used for measurements, in a clinical settings, as in the imaging molars of the upper jaw of an average patient. When measuring, the tip of the tube was placed on the detector.
The parameters checked, with tolerances, are given in the Table 1 and the list of examined intraoral dental X-ray devices with technical characteristics in the Table 2.13
Table 1.
Performance testing of the dental X-ray units
| Parameter | Tolerancies |
|---|---|
| kVp reproducibility (%) | <±10 |
| Timer accuracy (%) | <±10 |
| Timer reproducibility (%) | <±10 |
| Tube output reproducibility at FSD | <±10 |
| Half-value layer (HVL) | |
| For voltage <70 kV | ≥1.5 mmAl |
| For voltage >70 kV | ≥2.5 mmAl |
Table 2.
List of examined intraoral dental X-ray devices and their basic technical characteristics
| No | Model (Manufacturer) | Nominal X-ray tube potential (kV) | X-ray tube current (mA) | The source-skin distance (cm) | Total filtration (mm Al) |
|---|---|---|---|---|---|
| 1. | CCX Digital (Trophy) | 70 | 8 | 31 | 2.5 |
| 2. | RXDC (MYRAY) | 60 | 7 | 20 | 2.0 |
| 3. | Elitys (Trophy) | 60 | 7 | 20 | 1.5 |
| 4. | Expert DC (Gendex) | 65 | 7 | 20 | 1.5 |
| 5. | Heliodent DS (Sirona) | 60 | 3.5 | 20 | 1.5 |
| 6. | HeliodenVario (Sirona) | 70 | 7 | 20 | 1.5 |
| 7. | Heliodent 70 (Siemens) | 70 | 7 | 20 | 1.5 |
| 8. | Vario DG (Sirona) | 70 | 3.5 | 20 | 1.5 |
| 9. | Dent (EiNiš) | 50 | 10 | 10 | 1.5 |
| 10. | Minray (Soredex) | 70 | 7 | 20 | 2 |
| 11. | Gnatus (Gnatus) | 70 | 7 | 20 | 1.5 |
| 12. | CS 2100 (Carestream) | 60 | 7 | 20 | 2 |
| 13. | Intra (Planmeca) | 63 | 8 | 20 | 1.5 |
| 14. | Focus (Kavo) | 70 | 7 | 20 | 2 |
| 15. | XDC (Fona) | 70 | 7 | 20 | 1.5 |
| 16. | Xgenus (De Götzen) | 70 | 8 | 20 | 1.5 |
| 17. | CS 2200 (Carestream) | 70 | 7 | 20 | 2 |
| 18. | Endos DC (DentX) | 65 | 5 | 20 | 2 |
| 19. | Endos AC (DentX) | 70 | 8 | 20 | 2 |
| 20. | ANTHOS AC | 70 | 7 | 20 | 1.5 |
| 21. | Leadex 70 (Ritter) | 70 | 7 | 20 | 1.5 |
50 intraoral dental x-ray units in use in the public and private sector in Serbia.
It is worth to notice that all the devices given in the Table 2 have round collimators with a diameter of 6 cm, except Dent (EiNiš) which has a diameter of 5 cm. Also, in Serbia, the use of devices having a voltage of 50 kV (single-phase generator X-ray units (also Dent EiNiš)) is still permitted by law.4,13
It should be emphasised that there are differences in X-ray units, voltages, manufacturers, device architectures (single-phase and high-frequency), but also in the image receptors (analogue: film (classes D and E) and digital: (CCD compound), CMOS (complementary metal oxide semiconductor) and PSP (phosphor storage plate)), which is also shown in Table 3.
Table 3.
Measurement results of X-ray tube voltage (kV) and time (s) compared to nominal values and measurement and calculated results of Ki (mGy and mR) of the 50 intraoral dental X-ray units in Serbia, with the displayed image receptors for each device separately
| No | Set X-ray tube Volt. (kV) |
Measured X-ray tube Volt. (kV) |
Set It (mAs) | Set t (s) |
Meas. t (s) | Image recep. | Measur.Ki (mGy) | Calc. Ki (mGy) |
Measur.Ki (mR) | Calc.Ki (mR) | Avr. RPDa (%) |
|---|---|---|---|---|---|---|---|---|---|---|---|
| 17. | 70 | 71.58 ± 0.03 | 4.41 | 0.63 | 0.63 ± 0.00 | E film | 5.70 ± 0.01 | 4.49 | 0.65 ± 0.01 | 0.50 | 23.67 |
| 8. | 70 | 65.3 ± 0.2 | 3.5 | 0.5 | 0.5 ± 0.0 | D film | 4.39 ± 0.02 | 3.42 | 0.50 ± 0.02 | 0.39 | 21.10 |
| 16. | 70 | 63.43 ± 0.09 | 4 | 0.8 | 0.83 | E film | 4.12 ± 0.02 | 3.95 | 0.47 ± 0.02 | 0.45 | 3.53 |
| 10. | 70 | 69.58 ± 0.02 | 3.5 | 0.5 | 0.5 ± 0.0 | D film | 4.04 ± 0.01 | 3.42 | 0.46 ± 0.01 | 0.39 | 15.15 |
| 10. | 70 | 70.36 ± 0.02 | 3.5 | 0.5 | 0.5 ± 0.0 | E film | 3.95 ± 0.01 | 3.42 | 0.45 ± 0.01 | 0.39 | 12.69 |
| 21. | 70 | 69.46 ± 0.05 | 5.04 | 0.63 | 0.58 ± 0.05 | E film | 3.86 ± 0.05 | 5 | 0.44 ± 0.05 | 0.57 | 29.00 |
| 3. | 60 | 60.8 ± 0.1 | 4.41 | 0.63 | 0.63 ± 0.00 | D film | 3.77 ± 0.02 | 3.6 | 0.43 ± 0.02 | 0.41 | 3.62 |
| 18. | 70 | 69.9 ± 0.6 | 4 | 0.5 | 0.52 ± 0.03 | E film | 3.51 ± 0.03 | 3.95 | 0.40 ± 0.03 | 0.45 | 13.02 |
| 10. | 70 | 69.0 ± 0.2 | 2.8 | 0.4 | 0.4 ± 0.0 | E film | 3.33 ± 0.01 | 2.81 | 0.38 ± 0.01 | 0.32 | 17.77 |
| 11. | 70 | 65.9 ± 0.0 | 3.5 | 0.5 | 0.5 ± 0.0 | E film | 3.25 ± 0.01 | 3.42 | 0.37 ± 0.01 | 0.39 | 5.60 |
| 21. | 70 | 67.4 ± 0.2 | 4 | 0.5 | 0.46 ± 0.09 | E film | 3.16 ± 0.05 | 3.95 | 0.36 ± 0.05 | 0.45 | 25.83 |
| 10. | 70 | 71.5 ± 0.1 | 2.8 | 0.5 | 0.49 ± 0.02 | E film | 3.16 ± 0.05 | 2.81 | 0.36 ± 0.05 | 0.32 | 12.68 |
| 6. | 70 | 66.5 ± 0.5 | 3.5 | 0.5 | 0.5 ± 0.0 | CCD | 3.07 ± 0.04 | 3.42 | 0.37 ± 0.04 | 0.39 | 7.25 |
| 6. | 70 | 68.1 ± 0.2 | 3.5 | 0.5 | 0.5 ± 0.0 | CCD | 3.07 ± 0.05 | 3.42 | 0.36 ± 0.05 | 0.39 | 10.51 |
| 10. | 70 | 72.5 ± 0.1 | 3.5 | 0.5 | 0.5 ± 0.0 | PSP | 3.07 ± 0.03 | 3.42 | 0.36 ± 0.03 | 0.39 | 10.39 |
| 6. | 70 | 65.1 ± 0.5 | 3.5 | 0.5 | 0.5 ± 0.0 | CCD | 2.81 ± 0.05 | 3.42 | 0.32 ± 0.05 | 0.39 | 21.41 |
| 7. | 70 | 68.6 ± 0.0 | 3.5 | 0.5 | 0.5 ± 0.0 | CCD | 2.72 ± 0.01 | 3.42 | 0.31 ± 0.01 | 0.39 | 25.09 |
| 7. | 70 | 66.7 ± 0.02 | 3.5 | 0.5 | 0.5 ± 0.0 | CCD | 2.72 ± 0.02 | 3.42 | 0.35 ± 0.02 | 0.39 | 14.03 |
| 6. | 70 | 66.6 ± 0.3 | 3.5 | 0.5 | 0.5 ± 0.0 | CCD | 2.72 ± 0.01 | 3.42 | 0.35 ± 0.01 | 0.39 | 13.02 |
| 18. | 65 | 65.1 ± 0.4 | 2.5 | 0.48 | 0.48 ± 0.00 | E film | 2.46 ± 0.01 | 2.02 | 0.28 ± 0.01 | 0.23 | 16.50 |
| 4. | 65 | 64.5 ± 0.6 | 2.24 | 0.32 | 0.32 ± 0.00 | E film | 2.46 ± 0.01 | 1.84 | 0.28 ± 0.01 | 0.21 | 25.53 |
| 4. | 65 | 65.1 ± 0.0 | 2.24 | 0.32 | 0.32 ± 0.00 | E film | 2.46 ± 0.01 | 1.84 | 0.28 ± 0.01 | 0.21 | 25.02 |
| 4. | 65 | 63.8 ± 0.2 | 2.24 | 0.32 | 0.32 ± 0.00 | E film | 2.46 ± 0.01 | 1.84 | 0.28 ± 0.01 | 0.21 | 24.42 |
| 16. | 70 | 71.1 ± 0.1 | 2.8 | 0.35 | 0.32 ± 0.01 | PSP | 2.46 ± 0.01 | 2.81 | 0.28 ± 0.01 | 0.32 | 13.15 |
| 9. | 50 | 45.7 ± 0.2 | 5 | 0.5 | 0.45 ± 0.08 | D film | 2.37 ± 0.01 | 2.1 | 0.27 ± 0.01 | 0.24 | 9.28 |
| 3. | 70 | 71.8 ± 0.1 | 2.43 | 0.347 | 0.348 ± 0.002 | CCD | 2.37 ± 0.01 | 2.37 | 0.27 ± 0.01 | 0.27 | 2.73 |
| 16. | 70 | 65.6 ± 0.3 | 2.56 | 0.32 | 0.32 ± 0.00 | CCD | 2.28 ± 0.03 | 2.54 | 0.26 ± 0.03 | 0.29 | 11.07 |
| 6. | 70 | 64.6 ± 0.4 | 2.8 | 0.5 | 0.5 ± 0.0 | CCD | 2.19 ± 0.06 | 2.81 | 0.25 ± 0.06 | 0.32 | 26.98 |
| 11. | 70 | 66.6 ± 0.3 | 2.24 | 0.32 | 0.32 ± 0.00 | PSP | 2.19 ± 0.04 | 2.19 | 0.25 ± 0.04 | 0.25 | 0.83 |
| 15. | 70 | 70.2 ± 0.0 | 2.52 | 0.36 | 0.36 ± 0.00 | PSP | 2.02 ± 0.01 | 2.46 | 0.23 ± 0.01 | 0.28 | 21.13 |
| 10. | 70 | 70.3 ± 0.0 | 1.75 | 0.25 | 0.25 ± 0.00 | PSP | 2.02 ± 0.01 | 1.75 | 0.23 ± 0.01 | 0.20 | 13.27 |
| 20. | 70 | 70.4 ± 0.0 | 2 | 0.25 | 0.28 ± 0.04 | CCD | 1.93 ± 0.01 | 2.02 | 0.22 ± 0.01 | 0.23 | 2.43 |
| 8. | 70 | 67.6 ± 0.1 | 2.24 | 0.64 | 0.62 ± 0.04 | PSP | 1.84 ± 0.02 | 2.19 | 0.21 ± 0.02 | 0.25 | 19.59 |
| 12. | 60 | 62.5 ± 0.4 | 1.75 | 0.25 | 0.25 ± 0.00 | E film | 1.56 ± 0.03 | 1.35 | 0.18 ± 0.03 | 0.13 | 24.90 |
| 1. | 70 | 70.1 ± 0.0 | 1.6 | 0.2 | 0.18 ± 0.02 | CCD | 1.56 ± 0.01 | 1.56 | 0.18 ± 0.01 | 0.18 | 1.78 |
| 10. | 70 | 70.5 ± 0.0 | 1.4 | 0.2 | 0.2 ± 0.0 | PSP | 1.49 ± 0.00 | 1.4 | 0.17 ± 0.00 | 0.16 | 9.24 |
| 5. | 60 | 61.8 ± 0.1 | 1.75 | 0.25 | 0.25 ± 0.00 | E film | 1.36 ± 0.02 | 1.31 | 0.16 ± 0.02 | 0.13 | 14.03 |
| 14. | 70 | 70.0 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.32 ± 0.00 | 1.14 | 0.15 ± 0.00 | 0.13 | 14.01 |
| 14. | 70 | 71 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.32 ± 0.01 | 1.14 | 0.15 ± 0.01 | 0.13 | 15.84 |
| 10. | 70 | 70.3 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | PSP | 1.32 ± 0.01 | 1.14 | 0.15 ± 0.01 | 0.13 | 14.50 |
| 2. | 60 | 61.6 ± 0.2 | 1.4 | 0.2 | 0.2 ± 0.0 | CCD | 1.25 ± 0.02 | 1.13 | 0.14 ± 0.02 | 0.11 | 24.90 |
| 13. | 63 | 60.2 ± 0.4 | 2 | 0.25 | 0.25 ± 0.00 | PSP | 1.23 ± 0.04 | 1.5 | 0.14 ± 0.04 | 0.23 | 56.45 |
| 4. | 65 | 66.7 ± 0.1 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.23 ± 0.03 | 0.88 | 0.14 ± 0.03 | 0.1046 | 23.35 |
| 4. | 65 | 65.3 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.23 ± 0.03 | 0.88 | 0.14 ± 0.03 | 0.10 | 24.35 |
| 4. | 65 | 64.1 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.23 ± 0.01 | 0.88 | 0.14 ± 0.01 | 0.10 | 23.31 |
| 14. | 70 | 69.9 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.23 ± 0.01 | 1.14 | 0.14 ± 0.01 | 0.13 | 12.67 |
| 10. | 70 | 70.6 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.23 ± 0.01 | 1.14 | 0.14 ± 0.01 | 0.13 | 12.04 |
| 8. | 70 | 71.3 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | CCD | 1.14 ± 0.01 | 1.14 | 0.13 ± 0.01 | 0.13 | 6.23 |
| 10. | 70 | 69.8 ± 0.0 | 1.12 | 0.16 | 0.16 ± 0.00 | PSP | 1.14 ± 0.01 | 1.14 | 0.13 ± 0.01 | 0.13 | 4.87 |
| 10. | 70 | 70.6 ± 0.0 | 0.7 | 0.1 | 0.1 ± 0.00 | CCD | 0.79 ± 0.00 | 0.7 | 0.09 ± 0.00 | 0.08 | 9.09 |
Relative percent difference.
The results of the performance testing were statistically analysed and shown in Table 3.4
The information on Ki, together with the beam area, can be used to calculate KAP and to determine diagnostic reference levels (DRL).6,14 Furthermore, the effective dose can be estimated based on KAP and coefficients from references.15
The results of the QC measurements showed12:
The nominal tube voltage was accurate within 5%, except for two measured X-ray units.
The measured time was accurate within 5%, except for two measured X-ray units.
The largest deviation from the mean Ki was 6%.
The Table 3 shows that the measured Ki is strongly influenced by the time/current product and voltage of the device. Following the results from the Table 3 and the mathematical model used by Kothan et al8 (the equation in this case referred to classical radiography), an empirical formula of Ki in milliroentgen (mR) can be set:
| (1) |
where U is X-ray peak tube voltage, I is the current, t is the exposure time, d the source-chamber distance and n the constant value. All the source-chamber distances are normalised to 20 cm using the quadratic law. The value of the constant k is taken to be one. One of the reasons for this is the impossibility of changing the voltage value on the measured intraoral dental X-ray units.
The coefficient n of Eq. (1) was estimated by the multiple nonlinear regression method using measured values of radiation doses at set points values V and Ixt. The MATLAB 2013a (MathWorks) was used for surface fitting (non-linear regression method) of the Eq. (1). MATLAB is a high-performance language for technical computing. It integrates computation, visualisation and programming in an easy-to-use environment where problems and solutions are expressed in familiar mathematical notation.16
The Eq. (1) validity was statistically evaluated using a coefficient of correlation (R), standard error (SE) of the fitted function and the mean relative percentage deviation (MRPD).17,18 These parameters are defined by the following equations:
| (2) |
| (3) |
| (4) |
where yi is experimental data, fi is fitted data, yav is the average of experimental data and N is the number of data points.
Results and discussion
Experimental data obtained by measurement (Table 3) and data from reference show that the final measured dose is certainly influenced by the age and architecture of the dental device, the choice of image receptors and the operator’s training and knowledge of the device. 19–22 In the case of films, it depends on whether development is done manually or automatically. The data from reference indicate that, depending on the architecture of a device, the exposure time can vary up to five times resulting in final dose variations (Table 3).19–21,23,24 The choice of image receptors can reduce the dose up to nine times (comparison of D film as image receptors (analog) and PSP and CCD receptors (digital).19–21,23,24 Table 3 also shows the differences in doses up to four times in the case of devices that use the same image receptors and have a similar device architecture (CCD, 70 kV, 20 cm tube). The final result is also affected by the age of the device and insufficient operator training. Finally, it should be mentioned that the dose may be affected by irregular maintenance. The influence of difference in the shape of the collimator on the dose is not discussed in this paper though it exists, but all investigated units had cylindrical collimator.22
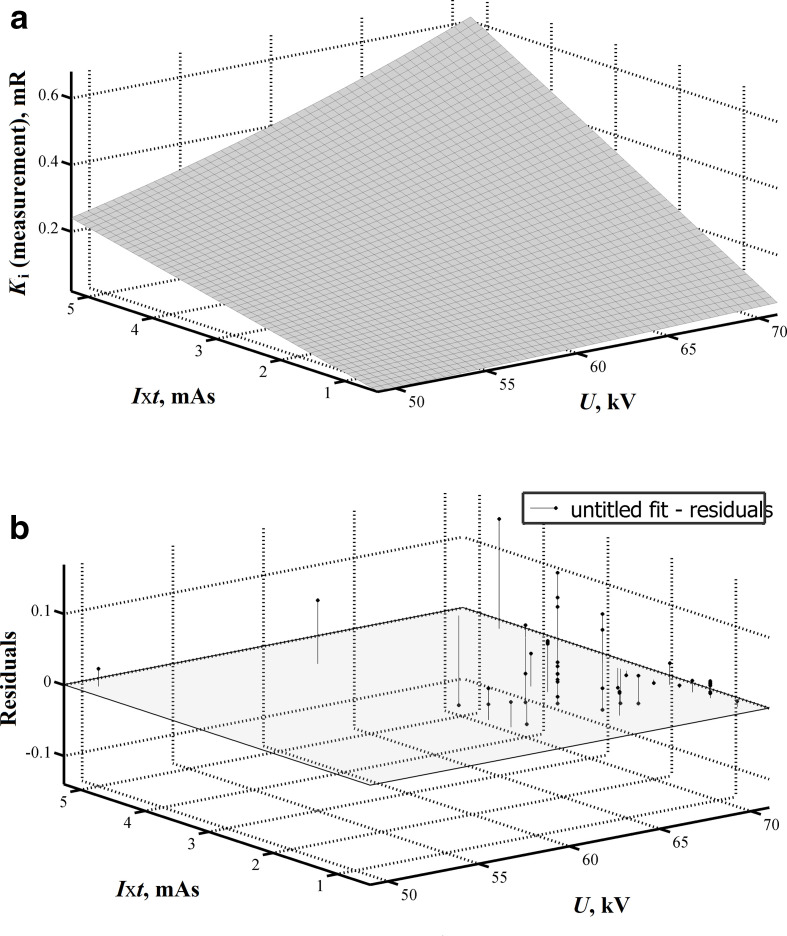
The experimental data on Ki were analyzed by the multiple nonlinear regression model based on the actual levels of the exposure conditions (V and Ixt), whereas Eq. (1) was used to fit the radiation dose data. The goal of the multiple nonlinear regression model is to model a non-linear relationship (Eq. 1) between the independent (Ki) and dependent (U and Ixt) variables. Figure 1 shows the surface fitting of the Eq. (1) and the residual plot. The Eq. (1) describes the dependence of Ki on U, Ixt and d, but not on the architecture of the unit. Based on the results of the measured Ki for devices of different architecture, the coefficient n in Eq. (1) was determined by fitting. This gave a universal formula of Ki for devices of different architecture.
Figure 1.
The 3D plots for measured radiation doses (Ki) as a function of the X-ray peak tube voltage (V) and the exposure current and time product, (Ixt), visual representation in support of an empirical formula (1); surface fitting (a) and residual plot (b).
The mathematical model describing relationship between the radiation dose, X-ray peak tube voltage (V) and the exposure current/time product (Ixt) is presented by Eq. (5). Value of the coefficient n is given in Eq. (5). The values of R = 0.897 and SE = 0.003 show that the model of Eq. (5) fitted the measurement data very well. The effect of the X-ray peak tube voltage and the exposure current/time product on radiation dose is shown in Figure 1. With the increase in the exposure current/time product, the radiation doses increase linearly (Figure 1). Radiation doses increase with increasing the U2.5.
| (5) |
For easier insight and comparison of the obtained results, the Table 3 shows calculated Ki (mGy, mR) values (columns 9 and 11) and measured Ki (mGy, mR) values.
The accuracy of the models of Eq. (5) was estimated by calculating the MRPD. Measurement values of the radiation doses and calculated values obtained by using Eq. (5) showed good agreement, as illustrated in Figure 2. The MRPD between calculated and measured values was less than 15% indicating validity of Eq. (5).
Figure 2.
Diagnostic plots of measurement and calculated values of radiation doses (R).
The obtained formula for empirical calculation of incident kerma in air shows good matches with measured values in all X-ray units, whose deviations of measured nominal voltage does not exceed the value more than 10%. On the other hand, if deviations were higher than 10% calculated doses did not match the measured ones.
Conclusion
The empirical formula found in this work to calculate Ki shows good matches with the measured values and can be used in practice. It can help dentists to determine Ki of the procedure, if devices does not estimate it. The Ki deviation can mean wrong mode of operation, that is, poorly set parameter. Also, if the Ki is known, typical value could be set in order to compare to DRL and optimize the practice. It can also be used in other aspects of radiological protection, that is, dose calculation of occupationally exposed persons who are close to the patient during imaging. This can facilitate the calculation of protective barriers.
REFERENCES
- 1.United Nations Scientific Committee on the Effects of Atomic Radiation .Sources and effect of ionizing radiation. UNSCEAR 2008 Report, Vol. 1. New York: United Nations; 2008. http://www.unscear.org/docs/reports/2008/09-86753_Report_2008_Annex_A.pdf. [Google Scholar]
- 2.Commission E. Radiation protection No. 180. Medical radiation exposure of the european population. 2014. Available from: https://ec.europa.eu/energy/content/rp-180-medical-radiation-exposure-european-population-part-1-part-2_en.
- 3.Košutić D, Božović P. Distribution of X ray units in Serbia. XXVII symposium DZZ SCG, Vrnjačka Banja, Serbia. In: In Proc. XXVII Symposium DZZ SCG, Vrnjačka Banja, Serbia; 2013. pp. 197–200. [Google Scholar]
- 4.Mirkov Z. Quality control in dental radiology in Serbia: preliminary results. Rad Conference Proceedings 2017; 2: 95–8. [Google Scholar]
- 5.Bushberg JT, Seibert JA, Leidholdt EM, Boone JM. The essential physics for medical imaging (2nd edn). Philadelphia, USA: Lippincott Williams & Wilkins Publisher; 2002. [Google Scholar]
- 6.ICRP. Diagnostic reference levels in medical imaging. ICRP publication 135. Ann ICRP 2017; 46. [DOI] [PubMed] [Google Scholar]
- 7.Tsapaki V, Ahmed NA, AlSuwaidi JS, Beganovic A, Benider A, BenOmrane L, et al. Radiation exposure to patients during interventional procedures in 20 countries: initial IAEA project results. AJR Am J Roentgenol 2009; 193: 559–69. doi: 10.2214/AJR.08.2115 [DOI] [PubMed] [Google Scholar]
- 8.Tungjai M. An estimation of x-radiation output using Mathematic model. American Journal of Applied Sciences 2011; 8: 923–6. doi: 10.3844/ajassp.2011.923.926 [DOI] [Google Scholar]
- 9.Alghoul A, Abdalla MM, Abubaker HM. Mathematical evaluation of entrance surface dose (ESD) for patients examined by diagnostic x-rays. Open Access J Sci 2017; 1: 8–11. [Google Scholar]
- 10.Tung CJ, Cheng CY, Chao TC, Tsai HY. Determination of entrance skin doses and organ doses for medical X ray examinations. Radiat Prot Dosimetry 1999; 85: 417–20. doi: 10.1093/oxfordjournals.rpd.a032886 [DOI] [Google Scholar]
- 11.Ciraj O, Marković S, Kosutić D. First results on patient dose measurements from conventional diagnostic radiology procedures in Serbia and Montenegro. Radiat Prot Dosimetry 2005; 113: 330–5. doi: 10.1093/rpd/nch469 [DOI] [PubMed] [Google Scholar]
- 12.Tsapaki V, Tsalafoutas IA, Chinofoti I, Karageorgi A, Carinou E, Kamenopoulou V, et al. Radiation doses to patients undergoing standard radiographic examinations: a comparison between two methods. Br J Radiol 2007; 80: 107–12. doi: 10.1259/bjr/87150291 [DOI] [PubMed] [Google Scholar]
- 13.Rulebook on application of the radiation sources in medicine (Official Gazette RS 1/12 from 11.01.2012), Belgrade, Serbia, 2012. 2012. Available from: http://www.srbatom.gov.rs/srbatomm/wp-content/uploads/2019/11/RULEBOOK-ON-APPLICATION-OF-IONIZING-RADIATION-SOURCES-IN-MEDICINE.pdf.
- 14.Helmrot E, Alm Carlsson G. Measurement of radiation dose in dental radiology. Radiat Prot Dosimetry 2005; 114(1-3): 168–71. doi: 10.1093/rpd/nch502 [DOI] [PubMed] [Google Scholar]
- 15.Looe HK, Eenboom F, Chofor N, Pfaffenberger A, Steinhoff M, Rühmann A, et al. Conversion coefficients for the estimation of effective doses in intraoral and panoramic dental radiology from dose-area product values. Radiat Prot Dosimetry 2008; 131(Issue 3): 365–73Volume. doi: 10.1093/rpd/ncn172 [DOI] [PubMed] [Google Scholar]
- 16.Mathworks.com. What Is MATLAB? Available from: https://www.mathworks.com/discovery/what-is-matlab.html.
- 17.Rajković K, Bačić G, Ristanović D, Milošević NT. Mathematical model of neuronal morphology: prenatal development of the human dentate nucleus. Biomed Res Int 2014; 2014: 1–8. doi: 10.1155/2014/812351 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Milić PS, Rajković KM, Stamenković OS, Veljković VB. Kinetic modeling and optimization of maceration and ultrasound-extraction of resinoid from the aerial parts of white lady's bedstraw (Galium mollugo L.. Ultrason Sonochem 2013; 20: 525–34. doi: 10.1016/j.ultsonch.2012.07.017 [DOI] [PubMed] [Google Scholar]
- 19.Gail FW. Digital radiography in dentistry: moving from film-based to digital imaging. Chicago: American Dental Assistants Association; 2014. pp. 7–13. [Google Scholar]
- 20.Poppe B, Looe HK, Pfaffenberger A, Eenboom F, Chofor N, Sering M, et al. Radiation exposure and dose evaluation in intraoral dental radiology. Radiat Prot Dosimetry 2007; 123: 262–7. doi: 10.1093/rpd/ncl113 [DOI] [PubMed] [Google Scholar]
- 21.Mirkov Z, Nikolov J, Ciraj-Bjelac O, Rafajlovic S. Preliminary test level of dose for patients for various types of image receiver of intraoral dental radiology in Serbia. In: Symposium of the Croatian Radiation Protection Association; Osijek (Croatia); 2017. pp. 134–9. http://www.hdzz.hr/wp-content/uploads/2017/04/11HDZZ_zbornik.pdf. [Google Scholar]
- 22.Svenson B, Söderfeldt B, Gröndahl HG. Attitudes of Swedish dentists to the choice of dental X-ray film and collimator for oral radiology. Dentomaxillofac Radiol 1996; 25: 157–61. doi: 10.1259/dmfr.25.3.9084265 [DOI] [PubMed] [Google Scholar]
- 23.Anas A, Asaad J, Tarboush K. A comparison of intra-oral digital imaging modalities: charged couple device versus storage phosphor plate. Int J Health Sci 2010; 4: 156–67. [PMC free article] [PubMed] [Google Scholar]
- 24.van der Stelt PF. Filmless imaging: the uses of digital radiography in dental practice. J Am Dent Assoc 2005; 136: 1379–87. doi: 10.14219/jada.archive.2005.0051 [DOI] [PubMed] [Google Scholar]