Abstract
Introduction
Understanding how influenza vaccine uptake changed during the 2020/2021 influenza season compared to previous pre-pandemic seasons is a key priority, as is identifying the relationship between prior influenza vaccination and COVID-19 vaccine willingness.
Methods
We analyzed data from a large, nationally representative cohort of Canadian residents aged 50 and older to assess influenza vaccination status three times between 2015 and 2020. We investigated: 1) changes in self-reported influenza vaccine uptake, 2) predictors of influenza vaccine uptake in 2020/2021, and 3) the association between influenza vaccination history and self-reported COVID-19 vaccine willingness using logistic regression models.
Results
Among 23,385 participants analyzed for aims 1–2, influenza vaccination increased over time: 14,114 (60.4%) in 2015–2018, 15,692 (67.1%) in 2019/2020, and 19,186 (82.0%; combining those already vaccinated and those planning to get a vaccine) in 2020/2021. After controlling for socio-demographics, history of influenza vaccination was most strongly associated with influenza vaccination in 2020/2021 (adjusted odds ratio [aOR] 147.9 [95% CI: 120.9–180.9]); this association remained after accounting for multiple health and pandemic-related factors (aOR 140.3 [95% CI: 114.5–171.8]). To a lesser degree, those more concerned about COVID-19 were also more likely to report influenza vaccination in fall 2020, whereas those reporting a very negative impact of the pandemic were less likely to get vaccinated. Among 23,819 participants with information on COVID-19 vaccine willingness during the last quarter of 2020 (aim 3), prior influenza vaccination was most strongly associated with willingness to get a COVID-19 vaccine (aOR 15.1 [95% CI: 13.5–16.8] for those who had received influenza vaccine at all previous timepoints versus none).
Conclusions
Our analysis highlights the importance of previous vaccination in driving vaccination uptake and willingness. Efforts to increase vaccination coverage for influenza and COVID-19 should target individuals who do not routinely engage with immunization services regardless of demographic factors.
Keywords: CLSA, Influenza, Vaccine, Vaccination, COVID-19, SARS-CoV-2, Adults, Canada
Abbreviations: aOR, Adjusted Odds Ratio; CLSA, Canadian Longitudinal Study on Aging; CI, Confidence Interval; CMC, Chronic Medical Conditions; COPD, Chronic Obstructive Pulmonary Disease; COVID-19, Coronavirus Disease 2019; PHAC, Public Health Agency of Canada; SARS-CoV-2, Severe Acute Respiratory Syndrome Coronavirus-2
1. Introduction
Influenza is among the top ten causes of death in Canada, with approximately 12,200 hospitalizations and 3,500 deaths reported annually [1]. Adults 65 years of age and older are at increased risk of severe disease, hospitalization, and death due to influenza compared to younger individuals [2]. In Canada, an influenza vaccine is strongly recommended for people at risk of influenza-related complications or hospitalization including individuals aged 65 years and older and adults aged 18–64 with chronic medical conditions (CMC), and other selected vulnerable populations [3]. Moreover, the Public Health Agency of Canada (PHAC) established ambitious goals to increase influenza vaccine uptake to 80% among these population groups by 2025 [4].
According to the Seasonal Influenza Vaccination Coverage Survey, between the seasons 2016–2017 and 2019–2020 the coverage level has remained relatively stable below the target threshold (around 70%) among Canadian adults 65 years or older [5], [6].
With the spread of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) since the early months of 2020, even greater emphasis has been placed on the importance of influenza vaccination [7], particularly among those at risk of severe influenza outcomes, who are also at increased risk of severe disease, complications, and death due to SARS-CoV-2 infection [8], [9], both to prevent influenza and reduce the burden on the healthcare system. However, the coronavirus disease 2019 (COVID-19) pandemic has prompted the need to re-examine how individuals perceive their disease risk, how individuals interact with health services including vaccination, and attitudes towards existing vaccines and the newly developed COVID-19 vaccines. Many questions remain about how the pandemic may impact the uptake of vaccines designed to protect against other infectious diseases.
For these reasons, it is critical to evaluate how influenza vaccine uptake and willingness to get vaccinated changed during the 2020/2021 influenza season in the Northern Hemisphere compared to previous pre-pandemic seasons. In addition, understanding whether an individual's previous history of influenza vaccination over multiple seasons is associated with willingness to receive a COVID-19 vaccine can provide insight into vaccine decision-making and help identify those who are least likely to receive a COVID-19 vaccine.
The Canadian Longitudinal Study on Aging (CLSA) pre-pandemic datasets [10], together with the 2020 CLSA COVID-19 Questionnaire Study data [11], [12], provide an opportunity to address these questions and identify those who would most benefit from interventions to increase uptake of influenza vaccine, COVID-19 vaccine, or both in order to inform vaccination efforts during the 2021/2022 influenza season and beyond and optimally prevent the morbidity and mortality caused by these diseases.
Our primary aims were to determine whether and the degree to which influenza vaccine uptake among Canadian adults (overall and across subgroups of interest) changed in the 2020/2021 influenza season during the COVID-19 pandemic compared to previous years, to examine factors associated with influenza vaccine uptake in the 2020/2021 influenza season, and to assess whether willingness to receive a COVID-19 vaccine during this same period was associated with prior influenza vaccine uptake based on data collected from the same participants across multiple years.
2. Material and methods
2.1. Study setting and population
The CLSA is a large, nationally generalizable cohort of 51,338 Canadian residents across 10 provinces, who were aged 45–85 years at recruitment (between 2011 and 2015). Biological, medical, psychological, social, lifestyle, and economic data are collected from study participants every three years. With 95% retention, 48,893 individuals completed follow-up 1 (2015–2018). To assess the impact of COVID-19 on the physical, mental, social, and economic well-being of older adults, CLSA participants who were still alive and could be contacted (n = 42,511) were invited to participate in the COVID-19 Questionnaire Study starting on April 15, 2020. In total, 28,559 (67.2%) provided informed consent and completed the baseline survey. Multiple weekly, biweekly and monthly surveys took place after the initial contact, and participants who had responded to any previous survey were asked to complete an exit survey at the end of 2020. Detailed CLSA methods are described elsewhere [10], [13], and all survey questionnaires are accessible on the CLSA website [14]. Supplementary Figure S1 shows participants’ flow over time. The core CLSA study and the CLSA COVID-19 Questionnaire Study were approved by McMaster University Health Integrated Research Ethics Board (HiREB) and by research ethics boards at all collaborating Canadian institutions. The HiREB approval numbers are 10–423 for the Comprehensive Cohort and 09–213 for the Tracking Cohort. The CLSA Consortium data access approval number is 21CON001.
2.2. Data sources
We analysed data collected during the core CLSA baseline study visit (conducted between 2011 and 2015), the core CLSA follow-up 1 study (conducted between 2015 and 2018) as well as the baseline (conducted between April 15 to May 30, 2020) and exit CLSA COVID-19 questionnaires (conducted between September 29 to December 29, 2020) to investigate changes in self-reported influenza vaccine uptake over time and the association with self-reported willingness to get a COVID-19 vaccine at the end of 2020. For simplicity, from now on we will refer to these three data collection time points as T0, T1, T2 and T3, respectively (Supplementary Figure S2).
Outcome data. To address our first two aims, self-reported influenza vaccine uptake was the outcome of interest, assessed at three points in time among CLSA participants: at T1 with respect to the previous 12 months, at T2 with respect to the 2019/2020 season, and at T3 with respect to the 2020/2021 season. Participants could indicate whether they had received influenza vaccine during the relevant period by responding “Yes”, “No” or “I don't know/No answer”. Since the T3 questionnaire occurred during the influenza season, participants could also indicate that they were planning to receive an influenza vaccine if they had not already had received one. For the purpose of this analysis, having received an influenza vaccine in the 2020/2021 season and planning to receive it in the 2020/2021 season (T3) were combined into a single category. This decision was justified because we found almost no difference in terms of sociodemographic characteristics between individuals who had already been vaccinated at the time of the survey and those who reported that they were planning to get a vaccine, the only exception being the distribution of respondents by province of residence. In particular, Quebec residents represented only 4.8% of those already vaccinated at the time of the survey and 19.8% of those planning to receive a vaccine, likely reflecting the later start of the vaccination campaign compared to other provinces (Supplementary Table S1). The outcome of interest for our third aim was self-reported willingness to receive a COVID-19 vaccine once available (i.e. “willingness”), assessed at T3, i.e. between September and December 2020. In line with other work from our group that focused solely on factors associated with COVID-19 vaccine willingness [15], COVID-19 vaccine willingness was categorized as “likely” if participants answered either “very likely” or “somewhat likely”, and “unlikely” if they answered “uncertain”, “somewhat unlikely”, or “very unlikely”.
Influenza vaccination history. To examine the association between history of influenza vaccination and influenza vaccine uptake at T3, we created a composite variable indicating whether participants reported having received an influenza vaccine at any previous timepoint (never, only at T1, only at T2, at both time points). To evaluate the relationship with participants’ willingness to receive a COVID-19 vaccine, prior influenza vaccination history was categorized as “not vaccinated at any timepoint (T1 to T3)”, “vaccinated at one timepoint only (T1 or T2 or T3), “vaccinated at two of three timepoints”, “vaccinated at all three timepoints (T1 to T3)”, or “data not available for one or more timepoints”.
Sociodemographic variables. For each of our analyses, we considered the following sociodemographic variables: sex at birth (male or female), age group (50–54, 55–64, 65–74, 75 and older; years), race (white or other than white), highest education level (less than secondary school graduation, secondary school graduation no post-secondary education, some post-secondary education, post-secondary degree/diploma), annual household income (in Canadian dollars; < $20,000, $20,000 to < $50,000, $50,000 to < $100,000, $100,000 to < $150,000, $150,000 or greater), province of residence (10 provinces), and geographic area of residence (urban or rural). Age categories were obtained from the participants age recorded at T1, T2 or T3 depending on the analysis. Sex, race, and education were obtained from the CLSA baseline study visit (T0); household income data were drawn from the follow-up 1 study visit (T1); province and geographic area of residence were from the COVID-19 baseline survey (T2). These variables were assumed to remain reasonably stable over time among older adults.
COVID-19-related factors. Aside from sociodemographic factors described above, we evaluated the relationship between the outcomes of interest and key factors reflecting the individual’s health status throughout 2020 as well as their experience with the pandemic. These included: self-reported general health status, measured on a scale from 1 (excellent) to 5 (poor); having chronic conditions that are known to increase the risk of severe or fatal COVID-19, i.e. at least one of asthma, chronic obstructive pulmonary disease (COPD), other chronic lung disease, diabetes, hypertension, heart disease, cancer, heart/lung/kidney/liver/pancreas failure; autoimmune disorder, HIV infection; self-reported likelihood of SARS-CoV-2 infection since March 2020, measured on a scale from 1 (very likely) to 5 (very unlikely); having someone close who was ill or died during the COVID-19 pandemic; self-reported concern about COVID-19, measured on a scale from 1 (not at all worried) to 7 (very worried). Finally, we considered self-reported experience of the COVID-19 pandemic impact on participant and household, measured on a scale from 1 (very negative) to 5 (very positive); this variable derived from a question that was intentionally broad in scope, allowing participants to take into account a wide range of experiences related to the pandemic itself and weight the impact of those experiences in the context of their own life. Data about self-reported chronic conditions were collected during the COVID-19 baseline survey (T2), whereas data for all other variables were obtained during the exit survey (T3).
2.3. Sample size and missing data
For aims 1 and 2, we restricted our analyses to CLSA participants who had completed the COVID-19 exit survey (n = 24,112) and had available influenza vaccination status for all three timepoints (n = 23,385). For aim 3, we restricted our analyses to CLSA participants who had complete outcome data (COVID-19 vaccine willingness) regardless of missing covariate data (n = 23,819). Influenza vaccine uptake information was missing at one or more time points for 727 (3.0%) individuals and willingness to receive a COVID-19 vaccine was not available for 293 (1.2%) participants; all outcome data were assumed to be missing at random as no associations were identified between missing values and key sociodemographic factors (e.g., age group, sex, race, education, income). Given the small amount of missing data and the assumption of missingness at random, participants with missing outcome data were excluded from the analyses.
2.4. Statistical analyses
Proportions and 95% confidence intervals (CIs) were estimated to describe influenza vaccine uptake at each point in time, both overall and across subgroups of interest based on age group, sex at birth, race, education, household income and area of residence (province and urban/rural location).
We examined the predictors of influenza vaccine uptake in the 2020/2021 season through multivariable logistic regression models. First, we estimated associations between sociodemographic factors (age group, sex at birth, race, education, income, province of residence and geographic area) and the outcome (influenza vaccination in the 2020/21 season, i.e. T3) (Model 1). Second, we determined the association between influenza vaccination history and the outcome (influenza vaccination in the 2020/21 season, i.e. T3), adjusting for all sociodemographic factors reported above (Model 2). Third, we assessed the effect of COVID-19-related factors on influenza vaccine uptake during the 2020/21 influenza season, also controlling for socio-demographics and influenza vaccination history (Model 3) to determine whether there was an additional association of COVID-19 related factors with the outcome of interest. For all predictors, we reported adjusted odds ratios (aORs) and 95% CIs.
Given the uncertainty about the actual vaccination status of individuals who had not yet been vaccinated against influenza but were planning to get a vaccine at the time of the survey, we also fitted nested multinomial logistic regression models where the outcome was a three-level variable (unvaccinated and unwilling to get influenza vaccine [reference group], already vaccinated, and unvaccinated but planning to get an influenza vaccine).
Finally, we examined factors associated with participants’ willingness to receive a COVID-19 vaccine. To address this objective, we employed a multivariable logistic regression model (Model 4) including history of influenza vaccination and COVID-19-related factors as predictors. In addition, all estimates were adjusted for sociodemographic characteristics as previously noted.
All analyses were pre-specified. Since sampling weights for the CLSA COVID-19 questionnaire study have not been developed, confidence intervals are assumed to capture the precision of the estimates in the sample and reflect what they would be if the sample were a random sample of the Canadian population aged 50 years and older. All analyses were conducted using STATA version 17.0 (StataCorp, College Station, TX, US). The alluvial diagram was generated using R version 4.1.0.
3. Results
3.1. Change in influenza vaccine uptake over time
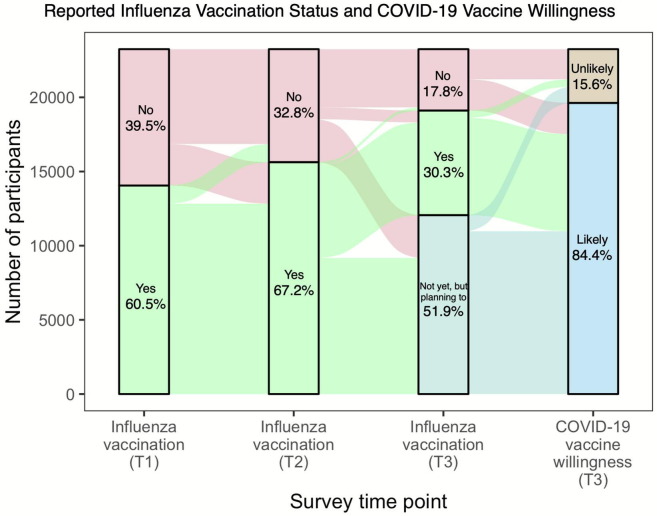
Table 1 summarizes the main characteristics of the 23,385 CLSA participants who reported their influenza vaccination status during the three time points considered in this analysis (T1, T2, and T3). Fig. 1 provides a graphical representation of how influenza vaccine uptake changed over time from T1 to T2 to T3 and how influenza vaccine uptake relates to willingness to receive a COVID-19 vaccine assessed at T3.
Table 1.
Influenza vaccine uptake among 23,385 participants at all timepoints, both overall and by sociodemographic characteristics.
| Characteristic |
Total |
Self-Reported Influenza Vaccination |
|||||
|---|---|---|---|---|---|---|---|
|
T1 |
T2 |
T3* |
|||||
| N (%) | n (%) | 95% CI | n (%) | 95% CI | n (%) | 95% CI | |
| Overall | 23,385 (100) | 14,114 (60.4) | 59.7 – 61.0 | 15,692 (67.1) | 66.5 – 67.7 | 19,186 (82.0) | 81.5 – 82.5 |
| Sex at birth | |||||||
| Female | 12,412 (53.1) | 7,462 (60.1) | 59.3 – 61.0 | 8,264 (66.6) | 65.7 – 67.4 | 10,059 (81.0) | 80.3 – 81.7 |
| Male | 10,973 (46.9) | 6,652 (60.6) | 59.7 – 61.5 | 7,428 (67.7) | 66.8 – 68.6 | 9,127 (83.2) | 82.5 – 83.9 |
| Age group (at final survey Sep-Dec 2020) | |||||||
| 50–54 | 1,067 (4.6) | 431 (40.4) | 37.4 – 43.4 | 499 (46.8) | 43.7 – 49.8 | 754 (70.7) | 67.8 – 73.4 |
| 55–64 | 7,093 (30.3) | 3,200 (45.1) | 44.0 – 46.3 | 3,815 (53.8) | 52.6 – 55.0 | 5,245 (74.0) | 72.9 – 75.0 |
| 65–74 | 8,566 (36.6) | 5,363 (62.6) | 61.6 – 63.6 | 6,053 (70.7) | 69.7 – 71.6 | 7,254 (84.7) | 83.9 – 85.4 |
| 75+ | 6,659 (28.5) | 5,120 (76.9) | 75.9 – 77.9 | 5,325 (80.0) | 79.0 – 80.9 | 5,933 (89.1) | 88.3 – 89.8 |
| Race | |||||||
| White | 22,466 (96.1) | 13,627 (60.7) | 60.0 – 61.3 | 15,167 (67.5) | 66.9 – 68.1 | 18,487 (82.3) | 81.8 – 82.8 |
| Other than white | 890 (3.8) | 472 (53.0) | 49.7 – 56.4 | 507 (57.0) | 53.6 – 60.2 | 676 (76.0) | 73.0 – 78.7 |
| Not available | 29 (0.1) | 15 (51.7) | 32.5 – 70.6 | 18 (62.1) | 42.3 – 79.3 | 23 (79.3) | 60.3 – 92.0 |
| Education level | |||||||
| Less than secondary school graduation | 1,056 (4.5) | 669 (63.4) | 60.4 – 66.3 | 694 (65.7) | 62.8 – 68.6 | 822 (77.8) | 75.2 – 80.3 |
| Secondary school graduation, no post-secondary education | 2,276 (9.7) | 1,311 (57.6) | 55.5 – 59.6 | 1,465 (64.4) | 62.4 – 66.3 | 1,782 (78.3) | 76.5 – 80.0 |
| Some post-secondary education | 1,671 (7.2) | 1,012 (60.6) | 58.2 – 62.9 | 1,123 (67.2) | 64.9 – 69.5 | 1,374 (82.2) | 80.3 – 84.0 |
| Post-secondary degree/diploma | 18,335 (78,4) | 11,098 (60.5) | 59.8 – 61.2 | 12,387 (67.6) | 66.9 – 68.2 | 15,174 (82.8) | 82.2 – 83.3 |
| Not available | 47 (0.2) | 24 (51.1) | 36.1 – 65.9 | 23 (48.9) | 34.1 – 63.9 | 34 (72.3) | 57.4 – 84.4 |
| Annual household income | |||||||
| < $20,000 | 815 (3.5) | 435 (53.4) | 49.9 – 56.8 | 447 (54.9) | 51.4 – 58.3 | 558 (68.5) | 65.2 – 71.6 |
| $20,000 to < 50,000 | 4,700 (20.1) | 2,875 (47.0) | 59.8 – 62.6 | 3,093 (65.8) | 64.4 – 67.2 | 3,741 (79.6) | 78.4 – 80.7 |
| $50,000 to < 100,000 | 8,399 (35.9) | 5,272 (62.8) | 61.7 – 63.8 | 5,830 (69.4) | 68.4 – 70.4 | 6,985 (83.2) | 82.3 – 84.0 |
| $100,000 to < 150,000 | 4,514 (19.3) | 2,630 (58.3) | 56.8 – 59.7 | 3,023 (67.0) | 65.6 – 68.3 | 3,746 (83.0) | 81.9 – 84.1 |
| $150,000 or greater | 3,695 (15.8) | 2,126 (57.5) | 55.9 – 59.1 | 2,443 (66.1) | 64.6 – 67.6 | 3,136 (84.9) | 83.7 – 86.0 |
| Not available | 1,262 (5.4) | 776 (61.5) | 58.7 – 64.2 | 856 (67.8) | 65.2 – 70.4 | 1,020 (80.8) | 78.5 – 83.0 |
| Province of residence | |||||||
| Newfoundland | 1,320 (5.6) | 731 (55.4) | 52.6 – 58.0 | 921 (69.8) | 67.2 – 72.2 | 1,164 (88.2) | 86.3 – 89.9 |
| Prince Edward Island | 373 (1.6) | 246 (66.0) | 60.9 – 70.6 | 285 (76.4) | 71.8 – 80.6 | 320 (85.8) | 81.8 – 89.2 |
| Nova Scotia | 2,093 (9.0) | 1,529 (73.1) | 71.1 – 74.9 | 1,683 (80.4) | 78.6 – 82.1 | 1,884 (90.0) | 88.6 – 91.3 |
| New Brunswick | 440 (1.9) | 281 (63.9) | 59.2 – 68.4 | 303 (68.9) | 64.3 – 73.2 | 367 (83.4) | 79.6 – 86.8 |
| Quebec | 4,226 (18.1) | 1,939 (45.9) | 44.4 – 47.4 | 1,955 (46.3) | 44.7 – 47.8 | 2,730 (64.6) | 63.1 – 66.0 |
| Ontario | 5,426 (23.2) | 3,504 (64.6) | 63.3 – 65.9 | 3,925 (72.3) | 71.1 – 73.5 | 4,651 (85.7) | 84.8 – 86.6 |
| Manitoba | 2,113 (9.0) | 1,242 (58.8) | 56.6 – 60.9 | 1,465 (69.3) | 67.3 – 71.3 | 1,794 (84.9) | 83.3 – 86.4 |
| Saskatchewan | 545 (2.3) | 336 (61.7) | 57.4 – 65.8 | 381 (69.9) | 65.9 – 73.7 | 450 (82.6) | 79.1 – 85.7 |
| Alberta | 2,352 (10.1) | 1,579 (67.1) | 65.2 – 69.0 | 1,767 (75.1) | 73.3 – 76.9 | 2,009 (85.4) | 83.9 – 86.8 |
| British Columbia | 4,497 (19.2) | 2,727 (60.6) | 59.2 – 62.1 | 3,007 (66.9) | 65.5 – 68.2 | 3,817 (84.9) | 83.9 – 85.9 |
| Geographic area of residence | |||||||
| Rural | 4,131 (17.7) | 2,264 (54.8) | 53.2 – 56.3 | 2,521 (51.0) | 59.5 – 62.5 | 3,144 (76.1) | 74.8 – 77.4 |
| Urban | 19,132 (81.8) | 11,775 (61.6) | 60.9 – 62.2 | 13,088 (68.4) | 67.7 – 69.1 | 15,937 (83.3) | 82.8 – 83.8 |
| Not available | 122 (0.5) | 75 (61.5) | 52.2 – 70.1 | 83 (68.0) | 59.0 – 76.2 | 105 (86.1) | 78.6 – 91.7 |
T1 = 12 months prior to CLSA Follow-up 1 study visit (data collected between 2015 and 2018); T2 = During 2019/2020 influenza season, as reported in COVID-19 baseline survey (Apr-May 2020); T3 = During 2020/2021 influenza season, as reported in COVID-19 exit survey (Sep-Dec 2020). Under “Total” (column 2), percentages were calculated among the total sample size (i.e. 23,385 participants); under “T1”, “T2”, and “T3” (columns 3-5), percentages were calculated relative to the total number of individuals in the subgroup (e.g. percent of female participants who reported having received an influenza vaccibe at T1).
Participants who had not yet received an influenza vaccine at the time of the survey but were planning to get one during the 2020/2021 influenza season were combined with those who reported that they had already been vaccinated.
Fig. 1.
Influenza vaccine uptake over time and willingness to receive a COVID-19 vaccine at the end of 2020 (n = 23,244). Strata represent participants’ responses about influenza vaccine uptake or COVID-19 vaccine willingness, and vertical blocks represent different survey timepoints (T1 = follow-up 1 study visit [2015–2018] relative to the previous 12 months, T2=COVID-19 baseline survey (Apr-May 2020) relative to the 2019/2020 influenza season, and T3 = COVID-19 exit survey (Sep-Dec 2020) relative to the 2020/2021 influenza season). Changes in self-reported vaccination status are shown as flows from one block to the next.
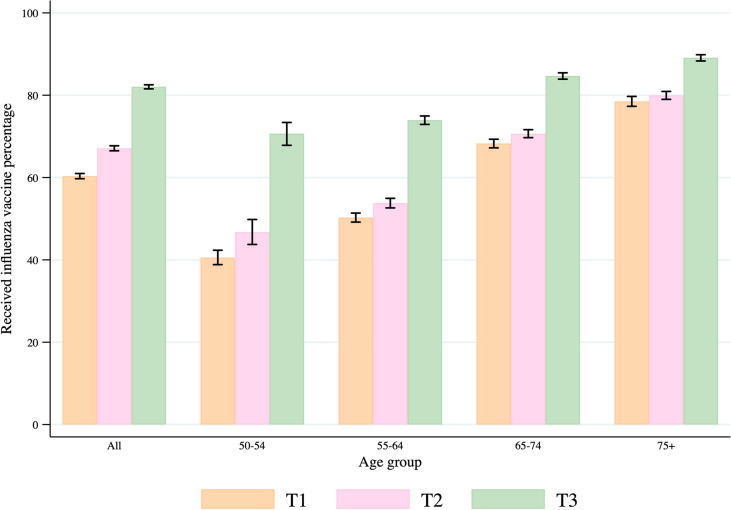
Among the 23,385 participants with data analyzed in aims 1 and 2, 14,114 (60.4%) reported having received an influenza vaccine at T1, and 15,692 (67.1%) did so at T2. Given the time of administration of the COVID-19 exit survey (T3) during the early part of the influenza season, 12,100 (51.7%) participants had not yet received the vaccine but reported that they were planning to get one. Most notably, 81.4% of these individuals completed the survey between September 29 and October 31, 2020, i.e. when the influenza vaccination campaign had not yet begun in some provinces. At the time of the survey, 7,086 (30.3%) participants had already received influenza vaccination. Since we could not assess whether all those planning to get vaccinated actually received a vaccine, we are unable to judge whether influenza vaccine uptake did increase in the 2020/2021 season compared to the previous years. An increase in uptake would be observed if at least 55% of those planning to get vaccinated eventually followed through. As expected, we found higher proportions of vaccinated persons among older age groups at all timepoints (Fig. 2 ). Influenza vaccination was less frequent at all timepoints among those other than white versus white participants, among those living in rural versus urban areas, and among those with lower income (Table 1). Participants residing in Quebec reported having received the vaccine much less frequently than those from other Canadian provinces, a pattern that remained unchanged over time. We did not observe significant differences in influenza vaccine uptake by sex or across education levels at any time point.
Fig. 2.
Influenza vaccine uptake among 23,385 participants, stratified by age group at three timepoints (T1 = follow-up 1 study visit [2015–2018] relative to the previous 12 months, T2=COVID-19 baseline survey (Apr-May 2020) relative to the 2019/2020 influenza season, and T3 = COVID-19 exit survey (Sep-Dec 2020) relative to the 2020/2021 influenza season). For the 2020/21 influenza season, participants who had not yet received an influenza vaccine but were planning to get one were combined with those who had already been vaccinated.
3.2. Factors associated with influenza vaccine uptake in the 2020/2021 season
Fig. 3 (Models 1 and 2) and Supplementary Figure S3 (Model 3) present the results of our analysis of factors associated with influenza vaccine uptake in the 2020/2021 season. We estimated that the odds of receiving or planning to receive an influenza vaccine increased gradually with age as compared to individuals aged 50–54, from aOR 1.3 (95% CI: 1.1–1.5) for people aged 55–64 to aOR 4.8 (95% CI: 4.0–5.6) for people aged 75 or older. Participants who identified as any racial group other than white were less likely to get vaccinated (aOR 0.7; 95% CI: 0.6–0.8) than those who identified as white. No significant differences in influenza vaccine uptake were identified across education levels, except for those with a post-secondary degree versus those with the least education (aOR 1.3; 95% CI: 1.1–1.5). The odds of influenza vaccination increased with income level, reaching an aOR of 3.1 (95% CI: 2.6–3.8) among those with the highest income ($150,000 or higher) as compared to those with a household income below $20,000. Regarding the province of residence, setting Ontario as the reference, only those living in Quebec showed significantly lower odds of influenza vaccination (aOR 0.3; 95% CI: 0.3–0.4), whereas those from Atlantic Canada except for New Brunswick had 1.3 to 1.7 times higher odds of getting vaccinated. Residing in urban areas was also found to favor vaccine uptake relative to residing in a rural area (aOR 1.5; 95% CI: 1.4–1.7).
Fig. 3.
Factors associated with influenza vaccine uptake in the 2020/2021 season (n = 23,385). Adjusted odds ratios (aORs) and their 95% confidence intervals (CIs) were estimated using logistic regression models: Model 1 for sociodemographic characteristics; Model 2 for influenza vaccination history, adjusting for all socio-demographics. All estimates are plotted on the log-odds scale to accommodate extreme values.
Having a history of influenza vaccination was the strongest predictor of influenza vaccine uptake in the 2020/21 season (T3) even after adjusting for all sociodemographic factors (Model 2). Most notably, we estimated a striking aOR of 147.9 (95% CI: 120.9–180.9) for those who reported influenza vaccine uptake both at T1 and T2 compared to those who had not been vaccinated at either of these timepoints.
Based on Model 3 (Supplementary Figure S3), we found that participants who reported that they were more worried about COVID-19 were more likely to report influenza vaccination (aOR 4.0 [95% CI: 3.2–5.1] for very worried individuals versus those who were not at all worried). As for the overall impact of the pandemic experienced by the participant and household, those reporting a very negative experience had significantly lower odds of getting vaccinated relative to those who reported that COVID-19 had no effect (aOR 0.6; 95% CI: 0.5–0.8). Having at least one chronic condition among those investigated was associated with slightly higher odds of vaccination (aOR 1.2; 95% CI: 1.1–1.3) compared to having no such conditions. However, self-reported general health status was not associated with influenza vaccination status at T3. Interestingly, believing one was previously infected with SARS-CoV-2 was not associated with influenza vaccine uptake at T3, and similar findings were observed among participants who reported that someone close to them was ill or died during the pandemic. Even after accounting for all of these covariates related to COVID-19 plus demographic factors, history of influenza vaccination was still the most strongly associated with influenza vaccine uptake in the 2020/21 season. Those who reported influenza vaccine uptake both at T1 and T2 had 140.3 times the odds (95% CI: 114.5–171.8) of influenza vaccination in the 2020/21 season (T3) compared to those who had not been vaccinated at any previous timepoint based on the full model.
Our sensitivity analysis based on multinomial models (Supplementary Table S2) further supports our findings about participants who had already received an influenza vaccine at the time of the survey. Similar associations of a slightly lower magnitude were estimated for those who were unvaccinated at the time of the survey but planning to get the influenza vaccine, suggesting that these individuals were more similar to those already vaccinated in terms of experiences and attitudes towards vaccination compared to unvaccinated participants who did not intend to get an influenza vaccine.
3.3. Relationship between willingness to get vaccinated against COVID-19 and influenza vaccination history
Among 23,819 survey participants who had information on COVID-19 vaccine willingness during the last quarter of 2020, a total of 20,044 (84.2%) responded they were either “somewhat likely” or “very likely” to receive a COVID-19 vaccine once available. The results of our logistic regression model evaluating the association between this outcome and influenza vaccination history and COVID-19-related factors are shown in Fig. 4 . After accounting for sociodemographic characteristics and COVID-19-related factors, history of influenza vaccination was the strongest predictor of participants’ likelihood to be willing to get vaccinated against COVID-19 (aOR 15.1 [95% CI: 13.5–16.8] for those who received an influenza vaccine at all three prior timepoints versus those who had not received it at those timepoints). We also found a stronger association between concern about COVID-19 and participants’ willingness to get a COVID-19 vaccine as concern increased, ranging from aOR 1.7 (95% CI: 1.5–2.0) for those who gave a score of 2 on a 1 to 7 scale, to aOR 4.4 (95% CI: 3.7–5.3) for very worried individuals (score of 7) relative to those who reported that they were not at all worried (score of 1). Respondents indicating that the pandemic had a negative overall impact on themselves or their household (versus no effect) were slightly more likely to be willing to get vaccinated with a COVID-19 vaccine (aOR 1.2; 95% CI: 1.1–1.3). Yet, those reporting a very negative impact showed an opposite pattern (aOR 0.8; 95% CI: 0.6–0.9). Interestingly, having one or more chronic conditions and reporting less than excellent general health status were associated with a lower odds of being willing to receive a COVID-19 vaccine even after accounting for the factors described above.
Fig. 4.
Factors associated with self-reported likelihood of receiving a COVID-19 vaccine at T3 (i.e., during the COVID-19 exit survey conducted in Sep-Dec 2020) among 23,819 participants with available outcome data. Adjusted odds ratios (aORs) and their 95% confidence intervals (CIs) were estimated through logistic regression (Model 4), controlling for sociodemographic factors (age group, sex at birth, race, education, income, province, and geographic area of residence). All estimates are plotted on the log-odds scale to accommodate extreme values.
4. Discussion
Canada is among countries with the some of the highest influenza vaccination coverage levels among older adults, and previous surveys have shown that the vast majority of older Canadians believe in the importance of vaccines [5]. Yet, over the past few years, influenza vaccine uptake has remained below target uptake levels even among high-risk groups, largely reflecting low perceived susceptibility to influenza [5], [16], [17], [18]. With the advent of COVID-19, health risk perception and attitudes towards vaccinations have likely changed. We conducted a comprehensive analysis of data from a large, nationally representative and well-established population-based cohort of older Canadians with the primary aim of better understanding influenza vaccine uptake during the 2020/2021 season. Our analysis suggests that influenza vaccine uptake among Canadians aged 50 and older might have increased during the 2020/2021 season compared to the previous year (from 67.1% [95% CI: 66.5–67.7] to 82.0% [95% CI: 81.6–82.5]), particularly among those aged 50 to 64 years. However, caution is advised when comparing these estimates because, during the 2020/2021 season, individuals who had not yet received an influenza vaccine and were planning to get it were combined with those already vaccinated, thus likely overestimating influenza vaccine uptake if some respondents did not eventually follow through. Yet, it is worth noting that a considerable proportion of the study population expressed their intention to receive an influenza vaccine.
While having previously received an influenza vaccine based on data collected since 2015 was the strongest predictor of influenza vaccine uptake in the 2020/2021 season after adjusting for key sociodemographic characteristics and important COVID-19 related factors (aOR 140.3 [95% CI: 114.5–171.8] for those reporting influenza vaccine uptake in the two previous surveys versus those reporting no influenza vaccination at those timepoints), we also observed associations with selected pandemic-related factors, though the magnitude was modest in comparison. Most notably, the more worried about COVID-19 an individual declared to be, the higher the odds of getting vaccinated against influenza during the 2020/2021 season (aOR 4.0 [95% CI: 3.2–5.1] for very worried participants versus not at all worried). In contrast, those who reported experiencing a very negative overall impact of the pandemic were at lower odds of receiving an influenza vaccine (aOR 0.6; 95% CI: 0.5–0.8).
Furthermore, our work indicates that individuals who identified as any racial group other than white, those with lower education, those with lower income, and those residing in Quebec were less likely to receive an influenza vaccine in 2020/2021. These findings are largely consistent with what was observed in previous surveys conducted in the Canadian population [5], [17], [18]. However, we also found that 83.2% (95% CI: 82.5–83.9) of males and 81.0% (95% CI: 80.3–81.7) of females received or were planning to receive an influenza vaccine in the last quarter of 2020, and no differences in vaccine uptake were detected between sexes after controlling for other sociodemographic factors. This is in contrast with previous reports from the 2013/2014 Canadian Community Health Survey, where – among 33,664 adults aged 65 or older – male participants had significantly higher odds of non-vaccination as compared to females (aOR 1.21; 95% CI: 1.07–1.36) [17]. Similarly, though based on a much smaller sample size (1,950 respondents including 514 aged 65 + from across Canada), the 2015/2016 Influenza Immunization Coverage Survey found lower vaccination rates among males compared to females [18]. Of note, male sex is recognized as a strong risk factor for severe disease and death from COVID-19, which may have altered disease risk perception among males [19]. While CLSA participants were not explicitly asked about the reasons for getting or not getting vaccinated against influenza during the 2020/2021 season, the apparently higher influenza vaccine uptake among males observed in our analysis compared to previous studies could possibly reflect an increased perceived risk among this population group due to the pandemic.
Besides investigating the prevlance and determinants of influenza vaccine uptake, drawing upon previous work we have conducted on this topic [15], we also sought to investigate in greater depth the relationship between influenza vaccination history and COVID-19 vaccine willingness during the last quarter of 2020, i.e. before COVID-19 vaccines became available. In our previous study, we documented a strong association between influenza vaccine uptake in the 2020/2021 season and COVID-19 vaccine willingness in 2020 [15]. In the present study, we further found that a history of multiple previous influenza vaccinations is similarly and strongly associated with participants’ likelihood of getting vaccinated against COVID-19 even after accounting for many other contributing factors. In fact, those who reported receiving an influenza vaccination at all previous timepoints and who had received or planned to receive it also during the 2020/2021 season were 15-fold more likely to be willing to get a COVID-19 vaccine versus those who had not been vaccinated for influenza during any of the timepoints assessed. With respect to other potentially relevant predictors, we found a similar pattern as described for influenza vaccination. While self-reported concern about COVID-19 may have played a role in favoring vaccine uptake for both influenza and COVID-19, these results suggest that history of influenza vaccination is the strongest predictor of both future influenza and COVID-19 vaccination. Thus, interventions that identify those who have not been vaccinated recently and aim to counteract common reasons for vaccine hesitancy and common barriers to vaccination should primarily address underlying determinants of low vaccine uptake rather than focus on socio-demographic factors or pandemic-specific perceptions.
This study is the first to investigate factors accociated with influenza vaccine uptake during the COVID-19 pandemic. Among its major strengths is the use of longitudinal data that were collected at multiple timepoints (before and during the pandemic) from a large and well-established national cohort. This allowed us to track changes in vaccine uptake over time among the same individuals and explore associations with a range of factors, including self-reported experiences related to the ongoing pandemic. Another important strength of this study is the joint availability of data about COVID-19 vaccine willingness and influenza vaccination status during the last quarter of 2020. Since COVID-19 vaccines had not yet been approved for use and made available to the general population at that time, self-reported likelihood of getting vaccinated against COVID-19 presumably reflects many factors including individual past experiences with vaccines.
Our study also has some limitations. First, we could have overestimated the level of influenza vaccine uptake during the 2020/2021 season due to the inclusion of individuals who had not yet been vaccinated but were planning toget vaccination, as a proportion of these respondents may have not followed through. As previously mentioned, we combined these groups because of the timing of administration of the COVID-19 exit survey, which that took place during the first half of the influenza season. At present, no Canadian estimates of influenza vaccine uptake during the 2020/2021 season are available for comparison as we write. Nevertheless, it is worth noting that those planning to receive a vaccine did not significantly differ from those already vaccinated in terms of sociodemographic profile. Second, our surveys did not include specific questions regarding reasons for receiving or not receiving an influenza vaccine. While the factors we evaluated may correlate with an individual’s motivation for getting vaccinated or not, our analyses could not directly address attitudes towards vaccination among participants or how these may have changed over time as these data were not available. Similarly, whether participants had underlying chronic conditions was assessed differently before and during the pandemic, and only the latter was utilized in our analyses. Accounting for the time-varying nature of this confounder in future analyses may address potential residual confounding in the associations observed. Third, vaccination status was assessed through self-report only, thus potentially overestimating the number of individuals who received a vaccine; however, previous studies have shown that this is generally a valid measure of vaccination uptake [20], and it is reassuring that our key findings aligned fairly well with past national surveys. Finally, generalizability of our findings to other countries may be limited to those that share similar sociocultural characteristics as well as those that provide accessibility to and affordability of vaccines across population groups. For instance, as influenza vaccine uptake has been shown to be associated with education level in this and other studies [5], [17], [18], it is important to highlight that, in 2019, the proportion of 25–64 year-old Canadians with a tertiary education was 21.4% above the average of the Organization for Economic Cooperation and Development (OECD) member countries [21]. Furthermore, influenza vaccination is publicly funded for priority population groups (e.g. adults aged 65 and older, individuals with chronic conditions) in all Canadian provinces, and most provinces even provide universal vaccination free of charge [22]. This may not be the case in other settings, thus potentially creating additional barriers to vaccine uptake.
5. Conclusions
With the 2020/2021 influenza season coinciding with ongoing efforts to prevent COVID-19 and the relaxation of many social distancing, masking, and other public health prevention measures, optimizing vaccination campaigns and reaching those subgroups least likely to be vaccinated against both diseases remain key priorities. Our study provides insights into the main determinants of influenza vaccine uptake and willingness to get vaccinated during unprecedented times and could be used to inform and improve current approaches, tailored to increase uptake among populations who do not routinely access influenza vaccination. The finding that having previously received an influenza vaccine is by far the most important predictor of influenza vaccine uptake as well as of COVID-19 vaccine willingness clearly shows that more efforts must be undertaken to target those who do not routinely engage with immunization services. Therefore, rather than focusing on sociodemographic groups, future efforts aimed at increasing vaccine uptake and actively promoting vaccination particularly amongst individuals at high risk for severe outcomes should explore avenues to identify and connect with those who do not have a history of accessing immunization services. To this end, establishing comprehensive immunization registries may be an important step towards improving surveillance for vaccinnation uptake and identifing those who remain unvaccinated year after year and who may benefit most from outreach.
Author contributions
GS and NEB conceived the study, designed the analyses, and prepared the first draft of the manuscript. GS conducted the analyses. NEB, CW, SK, LEG, JM and PR designed the CLSA COVID-19 study and contributed to the revision of the manuscript. The members of the CLSA team have contributed to the collection of the data across Canada. The opinions expressed in this manuscript are the authors’ own and do not reflect the views of the Canadian Longitudinal Study on Aging.
Financial disclosure
Funding for the CLSA COVID-19 Questionnaire study was provided by Juravinski Research Institute, Faculty of Health Sciences, McMaster University, Provost Fund from McMaster University, McMaster Institute for Research on Aging, Public Health Agency of Canada and the Nova Scotia COVID-19 Health Research Funding Coalition. Funding for the Canadian Longitudinal Study on Aging (CLSA) is provided by the Government of Canada through the Canadian Institutes of Health Research (CIHR) under grant reference: LSA 94473 and the Canada Foundation for Innovation, as well as the following provinces: Newfoundland, Nova Scotia, Quebec, Ontario, Manitoba, Alberta, and British Columbia. The funders had no role in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Data availability
Data are available from the Canadian Longitudinal Study on Aging (www.clsa-elcv.ca) for researchers who meet the criteria for access to de-identified CLSA data.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Acknowledgements
This research has been conducted using the CLSA Baseline Data Version 3.7 (tracking cohort) and 5.2 (comprehensive cohort), CLSA follow up 1 Data Version 2.2 (tracking cohort) and 3.0 (comprehensive cohort), and CLSA COVID-19 Data Version 1. The CLSA is led by Drs. Parminder Raina, Christina Wolfson and Susan Kirkland. Parminder Raina holds the Raymond and Margaret Labarge Chair in Optimal Aging and Knowledge Application for Optimal Aging and Tier 1 Canada Research Chair in Geroscience. Lauren E. Griffith is supported by the McLaughlin Foundation Professorship in Population and Public Health. Nicole E. Basta is supported by a Tier 2 Canada Research Chair in Infectious Disease Prevention. Giorgia Sulis is supported by a grant from the National Institute of Allergy and Infectious Diseases of the US National Institutes of Health (NIH) (R01 AI132496 (PI: NEB.). The authors gratefully acknowledge key contribution from all members of the CLSA team: Andrew Costa, Laura Anderson, and Cynthia Balion (McMaster University); Asada Yukiko (Dalhousie University); Benoȋt Cossette and Melanie Levasseur (University of Sherbrooke); Scott Hofer and Theone Paterson (University of Victoria); David Hogan (University of Calgary); Teresa Liu-Ambrose (University of British Columbia); Verena Menec and Philip St. John (University of Manitoba); Gerald Mugford and Zhiwei Gao (Memorial University of Newfoundland); Vanessa Taler and Patrick Davidson (University of Ottawa); Andrew Wister and Theodore Cosco (Simon Fraser University).
Footnotes
Supplementary data to this article can be found online at https://doi.org/10.1016/j.vaccine.2021.11.088.
Appendix A. Supplementary material
The following are the Supplementary data to this article:
References
- 1.Public Health Agency of Canada. Flu (influenza): For health professionals. 2019. Available at: https://www.canada.ca/en/public-health/services/diseases/flu-influenza/health-professionals.html#a8.
- 2.Mauskopf J., Klesse M., Lee S., Herrera-Taracena G. The burden of influenza complications in different high-risk groups: a targeted literature review. J Med Econ. 2013;16(2):264–277. doi: 10.3111/13696998.2012.752376. [DOI] [PubMed] [Google Scholar]
- 3.Young K., Gemmill I., Harrison R. Summary of the NACI Seasonal Influenza Vaccine Statement for 2020–2021. Can Commun Dis Rep. 2020;46(05):132–137. doi: 10.14745/ccdr.v46i05a06. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Vaccination Coverage Goals and Vaccine Preventable Disease Reduction Targets by 2025. Ottawa, Canada: Public Health Agency of Canada; 2019. Available at: https://www.canada.ca/en/public-health/services/immunization-vaccine-priorities/national-immunization-strategy/vaccination-coverage-goals-vaccine-preventable-diseases-reduction-targets-2025.html.
- 5.Seasonal Influenza Vaccination Coverage in Canada, 2019-2020. Ottawa, Canada: Public Health Agency of Canada; 2020. Available at: https://www.canada.ca/content/dam/hc-sc/documents/services/immunization-vaccines/vaccination-coverage/seasonal-influenza-vaccine-coverage-in-canada-en.pdf.
- 6.2016/2017 Seasonal Influenza Vaccine Coverage in Canada. Ottawa, Canada: Public Health Agency of Canada; 2018. Available at: https://publications.gc.ca/collections/collection_2018/aspc-phac/HP40-198-2017-eng.pdf.
- 7.Maltezou H.C., Theodoridou K., Poland G. Influenza immunization and COVID-19. Vaccine. 2020;38(39):6078–6079. doi: 10.1016/j.vaccine.2020.07.058. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.O’Driscoll M., Ribeiro Dos Santos G., Wang L., Cummings D.A.T., Azman A.S., Paireau J., et al. Age-specific mortality and immunity patterns of SARS-CoV-2. Nature. 2021;590(7844):140–145. doi: 10.1038/s41586-020-2918-0. [DOI] [PubMed] [Google Scholar]
- 9.Levin A.T., Hanage W.P., Owusu-Boaitey N., Cochran K.B., Walsh S.P., Meyerowitz-Katz G. Assessing the age specificity of infection fatality rates for COVID-19: systematic review, meta-analysis, and public policy implications. Eur J Epidemiol. 2020;35(12):1123–1138. doi: 10.1007/s10654-020-00698-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Raina P., Wolfson C., Kirkland S., Griffith L.E., Balion C., Cossette B., et al. Cohort Profile: The Canadian Longitudinal Study on Aging (CLSA) Int J Epidemiol. 2019;48(6):1752–1753j. doi: 10.1093/ije/dyz173. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.COVID-19 Questionnaire (Baseline). The Canadian Longitudinal Study on Aging (CLSA). The Canadian Longitudinal Study on Aging (CLSA); 2020. Available at: https://www.clsa-elcv.ca/doc/4263.
- 12.COVID-19 Questionnaire (Exit). The Canadian Longitudinal Study on Aging (CLSA). 2020. Available at: https://www.clsa-elcv.ca/doc/4271.
- 13.Raina P.S., Wolfson C., Kirkland S.A., Griffith L.E., Oremus M., Patterson C., et al. The Canadian longitudinal study on aging (CLSA) Can J Aging. 2009;28(3):221–229. doi: 10.1017/S0714980809990055. [DOI] [PubMed] [Google Scholar]
- 14.Data collection. The Canadian Longitudinal Study on Aging (CLSA). Available at: https://www.clsa-elcv.ca/researchers/data-collection.
- 15.Basta N.E., Sohel N., Sulis G., Wolfson C., Maimon G., Griffith L.E., et al. Factors Associated with Willingness to Receive a COVID-19 Vaccine among Adults Aged 50 years and Older: An Analysis of the Canadian Longitudinal Study on Aging. 2021; Under review. [DOI] [PMC free article] [PubMed]
- 16.Buchan S.A., Kwong J.C. Trends in influenza vaccine coverage and vaccine hesitancy in Canada, 2006/07 to 2013/14: results from cross-sectional survey data. CMAJ Open. 2016;4(3):E455–E462. doi: 10.9778/cmajo.20160050. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Roy M., Sherrard L., Dubé È., Gilbert N.L. Determinants of non-vaccination against seasonal influenza. Health Rep. 2018;29:12–22. [PubMed] [Google Scholar]
- 18.Farmanara N., Sherrard L., Dubé È., Gilbert N.L. Determinants of non-vaccination against seasonal influenza in Canadian adults: findings from the 2015–2016 Influenza Immunization Coverage Survey. Can J Public Health. 2018;109(3):369–378. doi: 10.17269/s41997-018-0018-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Peckham H., de Gruijter N.M., Raine C., Radziszewska A., Ciurtin C., Wedderburn L.R., et al. Male sex identified by global COVID-19 meta-analysis as a risk factor for death and ITU admission. Nat Commun. 2020;11(1) doi: 10.1038/s41467-020-19741-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.King J.P., McLean H.Q., Belongia E.A. Validation of self-reported influenza vaccination in the current and prior season. Influenza Other Respir Viruses. 2018;12(6):808–813. doi: 10.1111/irv.12593. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Education at a Glance 2020. Organization for Economic Cooperation and Development (OECD); 2020. Available at: https://www.oecd-ilibrary.org/content/publication/69096873-en.
- 22.Public Funding for Influenza Vaccination by Province/Territory (as of August 2020). Ottawa, Canada 2020. Available at: https://www.canada.ca/en/public-health/services/provincial-territorial-immunization-information/public-funding-influenza-vaccination-province-territory.html.
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
Data are available from the Canadian Longitudinal Study on Aging (www.clsa-elcv.ca) for researchers who meet the criteria for access to de-identified CLSA data.