Abstract
Objectives. To estimate the direct and indirect effects of the COVID-19 pandemic on overall, race/ethnicity‒specific, and age-specific mortality in 2020 in the United States.
Methods. Using surveillance data, we modeled expected mortality, compared it to observed mortality, and estimated the share of “excess” mortality that was indirectly attributable to the pandemic versus directly attributed to COVID-19. We present absolute risks and proportions of total pandemic-related mortality, stratified by race/ethnicity and age.
Results. We observed 16.6 excess deaths per 10 000 US population in 2020; 84% were directly attributed to COVID-19. The indirect effects of the pandemic accounted for 16% of excess mortality, with proportions as low as 0% among adults aged 85 years and older and more than 60% among those aged 15 to 44 years. Indirect causes accounted for a higher proportion of excess mortality among racially minoritized groups (e.g., 32% among Black Americans and 23% among Native Americans) compared with White Americans (11%).
Conclusions. The effects of the COVID-19 pandemic on mortality and health disparities are underestimated when only deaths directly attributed to COVID-19 are considered. An equitable public health response to the pandemic should also consider its indirect effects on mortality. (Am J Public Health. 2022;112(1):154–164. https://doi.org/10.2105/AJPH.2021.306541)
Most reports of US mortality associated with the COVID-19 pandemic have focused on deaths caused by infection with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2). Such reports overlook the many indirect pathways through which the pandemic has affected mortality, despite evidence that deaths attributed to COVID-19 accounted for only 66% to 72% of all pandemic-related mortality in 2020.1,2 Estimates of total pandemic-related mortality typically evaluate “excess deaths” (i.e., the difference between the total number of deaths that occurred during the pandemic and the number expected for that same period in absence of the pandemic, given historical trends in all-cause mortality). As of May 20, 2021, the Centers for Disease Control and Prevention (CDC) estimated that between 431 924 and 503 372 excess deaths occurred in the United States in 2020,3 whereas COVID-19 was documented as a primary or underlying cause of 384 098 deaths in 2020,4 implying that between 11% and 24% of pandemic-related deaths in 2020 were not captured in official surveillance data on deaths from COVID-19.
National figures, however, do not reveal how the pandemic has affected different population groups. We know that the risk of dying from COVID-19 varies by age, gender, race, ethnicity, and other sociodemographic characteristics because of differences in exposure probability (e.g., Black, Latinx, and Indigenous people are more likely, as a result of structural racism, to live and work in places that are conducive to the spread of SARS-CoV-25,6) and susceptibility (e.g., older adults are more likely to develop severe COVID-197). The risk of dying from an indirect consequence of the pandemic, such as social isolation, economic insecurity, or disrupted medical care, is also likely to vary across population groups.8 Quantifying group differences in the risks of dying from direct versus indirect effects of the pandemic can lay the groundwork for a more tailored and equitable public health response to the pandemic.
In this analysis, we used surveillance data from 2015 to 2020 to model expected mortality in 2020 and compared it to observed mortality in 2020. Using death certificate data, we estimated the risk of death and proportion of total pandemic-related mortality directly attributed to COVID-19. Under the assumption that the remaining excess deaths represent the social and economic effects of the pandemic on mortality, we present estimates of the risk of death and proportion of total pandemic-related mortality indirectly attributable to the pandemic. We examine group differences in the magnitude and composition of pandemic-related mortality by presenting age- and race/ethnicity‒specific estimates in addition to national estimates.
METHODS
The National Center for Health Statistics (NCHS), a division of the CDC, began releasing provisional counts of deaths from all causes and deaths attributed to COVID-19, grouped by CDC Morbidity and Mortality Weekly Report (MMWR) week, in April 2020.1,9 Deaths attributed to COVID-19 are defined as deaths with COVID-19 listed as an immediate or underlying cause of death on the death certificate, including deaths among people with suspected, but not laboratory-confirmed, COVID-19. Provisional counts of deaths were upweighted to account for incomplete reporting in more recent weeks, with weights estimated based on the completeness of provisional data in the reporting jurisdiction in 2018 to 2019. For this analysis, we used counts of deaths that occurred between January 3, 2015, and December 31, 2020, and were reported to the NCHS by August 1, 2021. Death counts were classified by race/ethnicity as recorded on the death certificate (Hispanic, non-Hispanic White, non-Hispanic Black, non-Hispanic Asian, non-Hispanic American Indian/Alaska Native, non-Hispanic Native Hawaiian/Pacific Islander, and other or unknown) and by age group (0‒14, 15‒19, 20‒24, 25‒29, 30‒34, 35‒39, 40‒44, 45‒49, 50‒54, 55‒59, 60‒64, 65‒69, 70‒74, 75‒79, 80‒84, and ≥ 85 years). Age group was missing for 796 decedents (< 0.01%); race/ethnicity was reported as other or unknown for 101 664 (0.74%). We excluded deaths with missing sociodemographic information only from the relevant group-specific estimates. We obtained monthly population estimates for 2015 to 2020 from the US Census Bureau.10
Estimation of Expected Deaths
We used data on deaths that occurred between January 3, 2015, and February 29, 2020, to estimate expected counts of deaths during the pandemic period (i.e., the number of deaths we expect to have observed in the absence of the pandemic). We assumed that the pandemic period began on March 1, 2020. We modeled deaths in the prepandemic period using quasi-Poisson regression to account for overdispersion of death counts, following the approach used by the CDC.1 We used separate models to predict expected death counts at the national level, overall and for each age group, each racial/ethnic group, and each combination of age group and racial/ethnic group. Each model accounted for secular trends by using a linear term for epidemiological year, and for seasonal trends by using restricted quadratic spline terms for MMWR week, with knots placed at the weeks representing percentiles of the observed distribution of deaths (10th, 25th, 50th, 75th, and 90th). We used the estimated model coefficients to predict death counts for each MMWR week between March 1 and December 31, 2020. Details about the specification and fit of the models are provided in Appendix A (available as a supplement to the online version of this article at http://www.ajph.org), and plots of observed and predicted death counts are provided in Appendix D. While models were fit by epidemiological year (July to June) to more smoothly model the rise and fall in deaths that occurs each winter and spring, the plots show observed and predicted death counts by calendar year (January to December).
Estimation of Risks of Death
Using observed and predicted counts of deaths, we estimated observed and expected risks of death in 2020. We intentionally report risks because of their advantages over more commonly reported mortality rates. Whereas rates are averaged over time, and contrasts of rates (e.g., rate differences and ratios) are noncollapsible, risks are explicitly a function of time, and their contrasts are collapsible, making risks easier to compare across studies and across time periods.11 Moreover, risks of death have a convenient interpretation as the “average” probability of death among individuals alive at the beginning of the risk period (i.e., the probability that a person randomly selected from the population on January 1, 2020, would survive to a particular week of 2020), whereas rates do not apply to individual population members.
To estimate risks, we first accounted for the impacts of aging on age-group membership over the course of the year by adjusting observed and predicted death counts to reflect the age groups of decedents as of January 1, 2020. Details are provided in Appendix B (available as a supplement to the online version of this article at http://www.ajph.org). We then merged the observed and predicted death counts for 2020 with population denominators to estimate the observed risk of death from all causes, the expected risk of death from all causes, and the observed risk of death from COVID-19 for each MMWR week of 2020. The observed risk of death from all causes was estimated as , where Ot indicates the cumulative count of observed deaths through MMWR week t, and N indicates the size of the population on January 1, 2020, as estimated by the US Census Bureau.10 The expected risk of death from all causes was estimated as , where Et indicates the cumulative count of predicted deaths through MMWR week t. We estimated the excess risk of death from all causes as the difference between the observed and expected risks of death from all causes (i.e., F(t)obs ‒ F(t)exp). Finally, we estimated the share of the excess risk of death in 2020 that was indirectly attributable to the pandemic as the difference between the excess risk of death from all causes and the observed risk of death from COVID-19. To estimate the uncertainty around our estimates, we constructed 95% confidence intervals (CIs) based on the empirical distribution of estimates obtained from 10 000 bootstrap samples of the data (details provided in Appendix C, available as a supplement to the online version of this article at http://www.ajph.org). We conducted all analyses in SAS version 9.4 (SAS Institute, Cary, NC).
To interpret our results, we relied on the following assumptions: (1) our statistical models for expected deaths correctly predict the number of deaths that would have occurred during the pandemic period in the absence of the pandemic; (2) if not for the pandemic, individuals who died in 2020 and whose deaths were directly or indirectly attributable to the pandemic would still have been alive on December 31, 2020; and (3) medical examiners are able to correctly distinguish cause of death such that all deaths caused by COVID-19 are captured using International Classification of Diseases, Tenth Revision (https://bit.ly/3xiSWDQ) code U07.1.
RESULTS
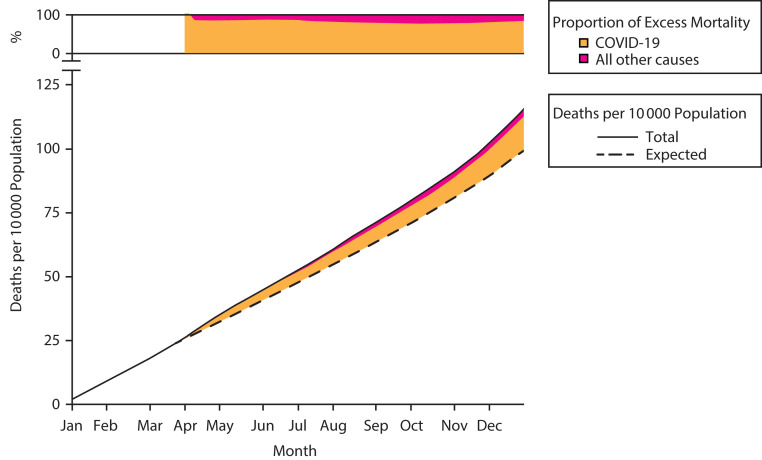
We estimated that US mortality was 17% higher than expected in 2020, corresponding to 16.6 excess deaths per 10 000 population (95% CI = 16.4, 16.7; Table 1; Figure 1). Equivalently, 1 in 602 (95% CI = 1 in 610, 1 in 599) US residents who were alive on January 1, 2020, died as a direct or indirect result of COVID-19 by December 31, 2020. Of those deaths, 84% were directly attributed to COVID-19. The remaining 16% represent deaths indirectly attributable to the pandemic: an absolute risk of 2.7 deaths per 10 000 population (95% CI = 2.5, 2.8).
TABLE 1—
One-Year Observed, Expected, and Excess Risks of Death Among US Residents From January 1 to December 31, 2020
| Observed Risk of Death (O), Deaths per 10 000 Population | Expected Risk of Death (E), Deaths per 10 000 Population | Increase in the Risk of Death, (O–E)/E, % (95% CI) | Excess Risk of Death From All Causes, Deaths per 10 000 Population (95% CI) | Excess Risk of Death Directly Attributed to COVID-19 | Excess Risk of Death Indirectly Attributable to the Pandemic | |||
| Deaths per 10 000 Population (95% CI) | % of All Excess Deaths | Deaths per 10 000 Population (95% CI) | % of All Excess Deaths | |||||
| Overall | 115.8 | 99.2 | 16.7 (16.5, 16.9) | 16.6 (16.4, 16.7) | 13.9 (13.9, 14.0) | 84.0 | 2.7 (2.5, 2.8) | 16.0 |
| By age group, y | ||||||||
| 0–14 | 4.9 | 5.1 | −2.9 (−4.5, −1.3) | 0.0 (0.0, 0.0) | 0.0 (0.0, 0.0) | . . .a | 0.0 (0.0, 0.0) | . . .a |
| 15–19 | 7.0 | 5.9 | 18.7 (16.0, 21.4) | 1.1 (1.0, 1.2) | 0.1 (0.1, 0.1) | 9.2 | 1.0 (0.8, 1.1) | 90.8 |
| 20–24 | 11.6 | 9.6 | 20.8 (18.8, 22.8) | 2.0 (1.8, 2.2) | 0.2 (0.2, 0.3) | 12.2 | 1.7 (1.6, 1.9) | 87.8 |
| 25–29 | 14.7 | 12.6 | 16.5 (14.9, 18.2) | 2.1 (1.9, 2.3) | 0.4 (0.4, 0.5) | 21.5 | 1.6 (1.4, 1.8) | 78.5 |
| 30–34 | 18.6 | 15.5 | 20.0 (18.5, 21.6) | 3.1 (2.9, 3.3) | 0.8 (0.8, 0.8) | 26.0 | 2.3 (2.1, 2.5) | 74.0 |
| 35–39 | 23.0 | 19.4 | 18.6 (17.1, 20.0) | 3.6 (3.3, 3.9) | 1.3 (1.3, 1.3) | 36.4 | 2.3 (2.0, 2.5) | 63.6 |
| 40–44 | 29.5 | 23.7 | 24.2 (22.8, 25.6) | 5.7 (5.4, 6.0) | 2.3 (2.2, 2.4) | 40.0 | 3.4 (3.1, 3.7) | 60.0 |
| 45–49 | 41.1 | 34.4 | 19.6 (18.5, 20.7) | 6.7 (6.4, 7.1) | 3.9 (3.9, 4.0) | 58.3 | 2.8 (2.5, 3.2) | 41.7 |
| 50–54 | 60.6 | 50.2 | 20.8 (20.0, 21.7) | 10.4 (10.0, 10.8) | 6.0 (5.9, 6.1) | 57.6 | 4.4 (4.0, 4.8) | 42.4 |
| 55–59 | 89.3 | 77.4 | 15.3 (14.6, 15.9) | 11.8 (11.3, 12.3) | 9.1 (8.9, 9.2) | 76.6 | 2.8 (2.3, 3.3) | 23.4 |
| 60–64 | 128.3 | 110.9 | 15.7 (15.1, 16.3) | 17.4 (16.8, 18.0) | 14.1 (13.9, 14.2) | 81.1 | 3.3 (2.7, 3.9) | 18.9 |
| 65–69 | 178.9 | 152.0 | 17.7 (17.2, 18.3) | 26.9 (26.1, 27.7) | 21.6 (21.4, 21.8) | 80.4 | 5.3 (4.5, 6.1) | 19.6 |
| 70–74 | 258.1 | 222.5 | 16.0 (15.5, 16.5) | 35.5 (34.5, 36.6) | 33.0 (32.8, 33.3) | 93.0 | 2.5 (1.4, 3.6) | 7.0 |
| 75–79 | 414.1 | 358.1 | 15.7 (15.2, 16.1) | 56.1 (54.9, 57.7) | 55.1 (54.6, 55.5) | 98.2 | 1.0 (0.0, 2.6) | 1.8 |
| 80–84 | 754.1 | 648.1 | 16.4 (15.9, 16.8) | 106.0 (103.8, 108.5) | 103.8 (103.1, 104.4) | 97.9 | 2.2 (0.0, 4.8) | 2.1 |
| ≥ 85 | 1403.0 | 1240.4 | 13.1 (12.8, 13.4) | 180.8 (179.8, 181.8) | 180.8 (179.8, 181.8) | 100.0 | 0.0 (0.0, 0.0) | 0.0 |
| By race/ethnicity | ||||||||
| White | 128.0 | 114.4 | 11.9 (11.7, 12.1) | 13.6 (13.4, 13.8) | 12.1 (12.1, 12.2) | 89.2 | 1.5 (1.2, 1.7) | 10.8 |
| Black | 110.5 | 88.3 | 25.2 (24.6, 25.7) | 22.2 (21.8, 22.6) | 15.2 (15.0, 15.3) | 68.2 | 7.1 (6.6, 7.5) | 31.8 |
| Hispanic | 51.1 | 37.3 | 37.0 (36.2, 37.8) | 13.8 (13.6, 14.1) | 11.6 (11.5, 11.7) | 84.0 | 2.2 (1.9, 2.5) | 16.0 |
| Asian | 48.6 | 40.0 | 21.6 (20.4, 22.8) | 8.6 (8.2, 9.1) | 7.3 (7.2, 7.4) | 84.4 | 1.3 (0.9, 1.8) | 15.6 |
| AIAN | 102.8 | 77.6 | 32.5 (30.0, 35.1) | 25.2 (23.5, 26.9) | 19.3 (18.8, 19.9) | 76.6 | 5.9 (4.1, 7.7) | 23.4 |
| NHPI | 75.4 | 63.0 | 19.7 (14.6, 25.3) | 12.4 (11.3, 15.5) | 11.8 (10.9, 12.7) | 95.3 | 0.6 (0.0, 3.8) | 4.7 |
| By age and race/ethnicity | ||||||||
| 0–29 y | ||||||||
| White | 7.4 | 6.6 | 12.5 (11.1, 14.0) | 0.8 (0.7, 0.9) | 0.1 (0.1, 0.1) | 8.4 | 0.8 (0.7, 0.8) | 91.6 |
| Black | 15.3 | 12.4 | 23.3 (21.0, 25.5) | 2.9 (2.6, 3.1) | 0.3 (0.3, 0.3) | 9.5 | 2.6 (2.4, 2.9) | 90.5 |
| Hispanic | 6.9 | 5.9 | 16.6 (14.2, 19.0) | 1.0 (0.8, 1.1) | 0.3 (0.2, 0.3) | 26.7 | 0.7 (0.6, 0.8) | 73.3 |
| Asian | 3.5 | 3.5 | −0.2 (−5.7, 5.7) | 0.1 (0.1, 0.2) | 0.1 (0.1, 0.1) | . . .a | 0.0 (0.0, 0.1) | . . .a |
| AIAN | 16.2 | 13.0 | 24.4 (15.8, 33.3) | 3.2 (2.1, 4.2) | 0.7 (0.6, 0.9) | 23.5 | 2.4 (1.4, 3.4) | 76.5 |
| NHPI | 11.6 | 11.7 | −0.5 (−15.5, 17.8) | 0.9 (0.6, 1.9) | 0.9 (0.6, 1.3) | 100.0 | 0.0 (0.0, 1.0) | 0.0 |
| 30–49 y | ||||||||
| White | 27.6 | 23.4 | 18.1 (17.2, 19.1) | 4.2 (4.0, 4.4) | 0.8 (0.8, 0.9) | 20.0 | 3.4 (3.2, 3.6) | 80.0 |
| Black | 44.7 | 34.3 | 30.4 (28.6, 32.2) | 10.4 (9.9, 10.9) | 3.7 (3.6, 3.8) | 35.9 | 6.7 (6.1, 7.2) | 64.1 |
| Hispanic | 22.2 | 15.7 | 41.2 (39.0, 43.5) | 6.5 (6.2, 6.8) | 4.3 (4.2, 4.4) | 66.8 | 2.1 (1.8, 2.5) | 33.2 |
| Asian | 9.3 | 7.6 | 23.1 (18.5, 28.1) | 1.8 (1.4, 2.1) | 1.0 (1.0, 1.1) | 59.7 | 0.7 (0.4, 1.0) | 40.3 |
| AIAN | 71.2 | 49.7 | 43.3 (36.8, 50.4) | 21.5 (18.8, 24.3) | 9.7 (8.9, 10.4) | 44.9 | 11.9 (9.0, 14.7) | 55.1 |
| NHPI | 40.3 | 30.2 | 33.4 (18.5, 49.5) | 10.1 (6.5, 14.0) | 6.4 (5.3, 7.5) | 63.4 | 3.7 (0.0, 7.7) | 36.6 |
| 50–69 y | ||||||||
| White | 109.0 | 95.0 | 14.7 (14.3, 15.2) | 14.0 (13.6, 14.4) | 7.7 (7.6, 7.8) | 55.1 | 6.3 (5.9, 6.7) | 44.9 |
| Black | 173.0 | 138.0 | 25.4 (24.5, 26.3) | 35.1 (33.9, 36.2) | 23.9 (23.6, 24.2) | 68.1 | 11.2 (10.0, 12.3) | 31.9 |
| Hispanic | 93.6 | 62.4 | 50.1 (48.6, 51.7) | 31.3 (30.5, 32.0) | 26.8 (26.5, 27.1) | 85.7 | 4.5 (3.6, 5.3) | 14.3 |
| Asian | 51.5 | 40.2 | 28.2 (25.6, 30.9) | 11.4 (10.4, 12.3) | 9.1 (8.8, 9.3) | 79.8 | 2.3 (1.3, 3.3) | 20.2 |
| AIAN | 162.9 | 121.0 | 34.6 (30.3, 39.0) | 41.9 (37.4, 46.3) | 34.2 (32.7, 35.7) | 81.6 | 7.7 (2.9, 12.4) | 18.4 |
| NHPI | 147.0 | 116.5 | 26.1 (17.4, 35.3) | 30.4 (26.4, 39.6) | 28.0 (25.2, 31.0) | 92.1 | 2.4 (0.0, 11.9) | 7.9 |
| ≥ 70 y | ||||||||
| White | 604.7 | 548.2 | 10.3 (10.1, 10.6) | 68.7 (68.4, 69.0) | 68.7 (68.4, 69.0) | 100.0 | 0.0 (0.0, 0.0) | 0.0 |
| Black | 670.7 | 543.5 | 23.4 (22.7, 24.2) | 127.2 (123.5, 131.0) | 112.7 (111.5, 113.8) | 88.6 | 14.6 (10.7, 18.4) | 11.4 |
| Hispanic | 509.2 | 387.1 | 31.5 (30.5, 32.5) | 122.1 (118.7, 125.4) | 116.7 (115.5, 117.9) | 95.6 | 5.4 (1.9, 8.9) | 4.4 |
| Asian | 368.6 | 307.1 | 20.0 (18.6, 21.4) | 61.5 (57.5, 65.4) | 55.9 (54.8, 57.1) | 91.0 | 5.5 (1.3, 9.7) | 9.0 |
| AIAN | 501.6 | 393.9 | 27.4 (23.5, 31.2) | 111.1 (107.4, 121.1) | 111.1 (106.6, 115.8) | 100.0 | 0.0 (0.0, 10.6) | 0.0 |
| NHPI | 428.0 | 380.5 | 12.5 (4.8, 20.6) | 58.7 (52.1, 75.5) | 58.7 (51.4, 66.4) | 100.0 | 0.0 (0.0, 18.3) | 0.0 |
Note. AIAN = American Indian or Alaska Native; CI = confidence interval; NHPI = Native Hawaiian or Pacific Islander. Calculated using provisional death data last updated on August 1, 2021.
Proportions of excess deaths were not calculated when total excess deaths were fewer than 1 in 100 000.
FIGURE 1—
US Excess Mortality Directly Attributed to COVID-19 and From All Other Causes in 2020
In our analyses of age-specific mortality, we found that the magnitude of excess mortality increased dramatically with age, consistent with prepandemic mortality patterns as well as the age distribution of deaths attributed to COVID-19 (Figure 2). The percentage increase in observed mortality relative to expected mortality, which accounts for age differences in prepandemic mortality, was similar across age groups, with the exception of children aged 0 to 14 years. The risk of death was 3% lower than expected among children aged 0 to 14 years (95% CI = −4.5, −1.3), and higher than expected in all other age groups, ranging from 13% higher among adults aged 85 years and older (95% CI = 12.8, 13.4) to 24% higher among adults aged 40 to 44 years (95% CI = 22.8, 25.6). In contrast, the proportion of excess mortality directly attributed to COVID-19 varied widely by age group, from 9% among decedents aged 15 to 19 years to 100% among decedents aged 85 years and older. In the age group with the largest percentage increase in observed versus expected mortality, adults aged 40 to 44 years, only 40% of excess deaths were directly attributed to COVID-19.
FIGURE 2—
US Excess Mortality Directly Attributed to COVID-19 and From All Other Causes in 2020, by Race/Ethnicity
In analyses of race/ethnicity‒specific mortality, we found that the magnitude of excess mortality varied widely across groups (Figure 3). The 1-year risk of excess mortality was higher than the national average among decedents identified as American Indian or Alaska Native (25.2 deaths per 10 000) or Black (22.2 deaths per 10 000), and lower than the national average among decedents identified as Hispanic (13.8 deaths per 10 000), White (13.6 deaths per 10 000), Native Hawaiian or Pacific Islander (12.4 deaths per 10 000), or Asian (8.6 deaths per 10 000).
FIGURE 3—
US Excess Mortality Directly Attributed to COVID-19 and From All Other Causes in 2020, by Age Group
Differences in the magnitude of excess mortality reflect the disproportionate burden of the pandemic on racially minoritized groups as well as prepandemic mortality patterns. These prepandemic mortality patterns are largely driven by differences in the age distributions of different racial/ethnic groups. For example, the expected risk of death among Hispanic Americans (37.3 deaths per 10 000) was a fraction of the expected risk of death among non-Hispanic White Americans (114.4 deaths per 10 000). Comparisons of the percentage increase in observed versus expected mortality account for differences in prepandemic mortality patterns. For example, decedents identified as non-Hispanic White experienced an 11.9% increase in observed versus expected mortality in 2020 (95% CI = 11.7%, 12.1%), whereas decedents identified as Hispanic experienced a 37.0% increase (95% CI = 36.2%, 37.8%)—more than 3 times the increase experienced by White Americans. The percentage increase in observed versus expected mortality was 32.5% among decedents identified as American Indian or Alaska Native (95% CI = 30.0%, 35.1%), 25.2% among those identified as Black (95% CI = 24.6%, 25.7%), 21.6% among those identified as Asian (95% CI = 20.4%, 22.8%), and 19.7% among those identified as Native Hawaiian or Pacific Islander (95% CI = 14.6%, 25.3%).
The proportion of excess deaths directly attributed to COVID-19 also varied substantially across racial/ethnic groups. Deaths indirectly attributable to the pandemic accounted for as much as 32% of excess mortality among decedents identified as Black and as little as 5% of excess mortality among those identified as Native Hawaiian or Pacific Islander. When considering younger age groups (ages 0‒29, 30‒49, and 50–69 years), the proportion of excess mortality indirectly attributable to the pandemic was highest among decedents identified as White (Appendix, Figure A). In these younger age groups, however, the absolute risks of death indirectly attributable to the pandemic were greatest among decedents identified as Black and American Indian or Alaska Native. Among adults aged 30 to 49 years, for example, indirect causes accounted for 6.7 deaths per 10 000 Black decedents aged 30 to 49 years and 11.9 deaths per 10 000 American Indian or Alaska Native decedents aged 30 to 49 years, versus 3.4 deaths per 10 000 White decedents aged 30 to 49 years.
DISCUSSION
We estimate that there were nearly 17 excess pandemic-related deaths in 2020 per 10 000 US residents alive on January 1, 2020. This is an estimate of the net effect of the pandemic on mortality. The net effect accounts for deaths caused by and prevented by the pandemic (i.e., some portion of deaths caused by the pandemic is offset by decreases in influenza deaths, traffic fatalities, and other deaths that would have occurred in the absence of lockdowns and social distancing). We estimate that 84% of excess deaths were directly attributed to COVID-19, while the remaining 16% of excess deaths represent the net indirect effect of the pandemic on mortality in 2020.
Our estimate of excess deaths directly attributable to COVID-19 exceeds an earlier estimate of 66% based on data through October 20201 and a more recent estimate of 72% that did not account for delays in the reporting of death certificates to the NCHS.2 Both earlier estimates were also based on mortality rates, which, unlike risks, do not account for changes in the population denominator as more susceptible individuals die and less susceptible individuals are born into the population, or as individuals age in and out of groups with different mortality risks. In group-specific analyses, we found that the proportion of excess deaths indirectly attributable to the pandemic varied widely by age, and across racial/ethnic groups within strata of age. Our findings reveal that a substantial proportion of pandemic-related mortality has not been captured in surveillance data on deaths from COVID-19, particularly among young people who are not recognized as being at serious risk of death from COVID-19. We also found that racial/ethnic inequities in pandemic-related mortality are likely underestimated when only deaths directly attributed to COVID-19 are considered.
Underdiagnosis of COVID-19 may explain part of the difference between excess deaths and deaths directly attributed to COVID-19. Underdiagnosis is an especially plausible explanation for deaths occurring early in the pandemic period, when testing was not yet widespread, and before the release of federal guidelines for reporting COVID-19 deaths on March 24, 2020.12 These guidelines give some leeway to coroners and medical examiners, who are responsible for confirming cause of death, and it is possible that some have systematically underreported deaths from COVID-19.13 Underdiagnosis is unlikely to account for all excess deaths during the pandemic period, however. In the United Kingdom, hospital autopsies conducted during the first 2 months of lockdown (starting on March 23, 2020) identified reduced access to health care, financial and work pressures, and drug and alcohol misuse as much more frequent causes of death than undiagnosed COVID-19.14 In the United States, documented increases in deaths from chronic diseases like dementia, diabetes, and heart disease9,15 may partially reflect underdiagnosed COVID-19, but they may also, along with increases in deaths from drug overdose15,16 and homicide,17 reflect the sweeping social and economic costs of the pandemic.18 Future validation studies may illuminate what proportion of excess deaths may have been attributable to undiagnosed COVID-19.
In our analysis, we found that excess deaths among older adults were much more likely to be directly attributed to COVID-19 than deaths among people aged younger than 55 years. Our results corroborate a previous study that found that only 38% of excess deaths among adults aged 25 to 44 years from March to July 2020 were directly attributed to COVID-19.19 Inadequate testing among young adults early in the pandemic may have contributed to the low proportion of deaths directly attributed to COVID-19 in this group, although access to testing has since improved. Another plausible explanation is that, while young adults are less susceptible to COVID-19, they are nonetheless dying at alarming rates because of the social and economic effects of the pandemic. For example, school closures and stay-at-home orders have isolated many young adults from their daily activities and social support systems, leading to increases in suicidal ideation and attempts.20 Young working adults are more likely than older working adults to have lost jobs, be underemployed, and be excluded from economic assistance programs,21 resulting in serious physical and mental health harms.22 Whatever the mechanisms linking the pandemic to increases in mortality among young people, it is clear that total pandemic-related mortality in this group is substantially and systematically underestimated in statistics describing deaths from COVID-19.
In addition to differences by age group, the proportion of excess deaths directly attributed to COVID-19 varied substantially across racial/ethnic groups, from 95% among decedents identified as Native Hawaiian or Pacific Islander to only 68% among decedents identified as Black. Our findings corroborate a recent ecological study by Stokes et al., which found that counties with more Black residents had lower proportions of excess deaths attributed to COVID-19,23 and a study by Wrigley-Field et al., which found that racial disparities in excess deaths were greater than racial disparities in deaths attributed to COVID-19 in Minnesota.24 Because the proportion of deaths attributed to COVID-19 was lower in many of the same racial/ethnic groups that experienced disproportionate increases in mortality in 2020, racial/ethnic disparities in pandemic-related mortality are likely to be underestimated in analyses that only consider deaths directly attributed to COVID-19.
One explanation for the lower proportion of excess deaths attributed to COVID-19 among many racially minoritized groups may be inequitable access to testing, resulting in higher rates of undiagnosed COVID-19.25 However, the indirect effects of the pandemic are also likely to be greater among racially minoritized groups because the social and economic impacts of the pandemic have not been uniformly distributed. For example, as a consequence of racial capitalism, Black and Latinx workers are more likely to suffer the physical and mental health consequences of losing jobs, employment benefits, and savings during the pandemic recession, or working in sectors that place them at higher risk of exposure to SARS-CoV-2.26,27 Asian Americans have suffered discrimination and violence as a result of racist narratives about the origins of COVID-19.28 The distributions of these pandemic-related stressors, like the distribution of infections, reflect the pre-existing social context.8,29–31
Historically, marginalized communities have often been disproportionately affected by public health emergencies, from past pandemics to Hurricane Katrina and the Flint water crisis. History has shown us that the effects of such emergencies play out long after the acute threat has passed, exacerbating pre-existing inequities.32 The financial burden of the pandemic, for example, has fallen disproportionately on hourly workers and small business owners, compounding the economic disparities that existed before the pandemic.33 These same economically marginalized communities are often communities of color who, as Cooper and Williams explained in a recent commentary, “have borne the burden of excess deaths from health disparities for generations.”33(p1491)
Accurate estimates of the full scale of pandemic-related mortality in specific population groups are critical to guide the efficient and equitable allocation of resources for the pandemic response. For example, the prioritization and allocation of resources to support safe school reopening should be informed by comprehensive data on how the pandemic affects the health of adolescents, including their mental health. Attribution of excess deaths to the pandemic may also have tangible consequences for families and communities, allowing access to funeral assistance and other funding allocated for disaster relief.34 Moreover, accurate estimates of disparities are needed to expose unjust social structures as a first step toward restorative justice and healing.33 Finally, our finding that the net effect of the pandemic on mortality was consistently underestimated in certain groups reveals an urgent need to improve our national surveillance systems. If these systems are not designed with health equity in mind, they will continue to downplay the effects of emerging pathogens on marginalized groups.35
Limitations
Deaths tend to follow a highly regular seasonal pattern, and mortality data are often more complete than diagnostic data, making excess deaths a revealing indicator of the population health impacts of the pandemic. Nevertheless, interpretation of our findings relies on the assumptions stated in the Methods section. For example, we assumed that people who died of COVID-19 would not have died absent the pandemic. Some people who died of COVID-19 in 2020, particularly adults in the oldest age group, may have died regardless of the pandemic, albeit from different causes. Also, while we modeled expected deaths flexibly, we may have underestimated expected deaths because of recent demographic trends or increases in causes of death unrelated to the pandemic, or overestimated expected deaths because of our linear parameterization of epidemiological year. Finally, self-described race/ethnicity may be misclassified on death certificates, and risks may be slightly underestimated because of missing data on race/ethnicity (0.74% of all deaths in 2020) and overestimated because of deaths among foreign residents (0.2%).
Public Health Implications
Accurate estimates of pandemic-related mortality are essential in guiding an efficient and equitable public health response to COVID-19. The net effect of the pandemic on mortality, and on population disparities in mortality, appears to be severely underestimated when only counting deaths directly attributed to COVID-19. Given differences among racial/ethnic groups in the proportion of excess mortality directly attributed to COVID-19, pandemic response efforts and policies that consider only the biological effects of the pandemic are likely to exacerbate health inequities that existed before 2020.
ACKNOWLEDGMENTS
Funding for this study was provided by National Institutes of Health grant K01AI125087.
CONFLICTS OF INTEREST
The authors have no conflicts of interest to declare.
HUMAN PARTICIPANT PROTECTION
This study used publicly available data and was determined to not be human participant research by the institutional review board at the University of North Carolina at Chapel Hill.
REFERENCES
- 1.Rossen LM, Branum AM, Ahmad FB, Sutton P, Anderson RN. Excess deaths associated with COVID-19, by age and race and ethnicity—United States, January 26–October 3, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(42):1522–1527. doi: 10.15585/mmwr.mm6942e2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Woolf SH, Chapman DA, Sabo RT, Zimmerman EB. Excess deaths from COVID-19 and other causes in the US, March 1, 2020, to January 2, 2021. JAMA. 2021;325(17):1786–1789. doi: 10.1001/jama.2021.5199. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.National Center for Health Statistics; National. 2021. https://www.cdc.gov/nchs/nvss/vsrr/covid19/excess_deaths.htm
- 4.National Center for Health Statistics. 2021. https://www.cdc.gov/nchs/nvss/vsrr/covid19/index.htm
- 5.Wallis C.> Why racism, not race, is a risk factor for dying of COVID-19. Scientific American. June 12, 2020. Available at: https://www.scientificamerican.com/article/why-racism-not-race-is-a-risk-factor-for-dying-of-covid-1912021
- 6.Zalla LC, Martin CL, Edwards JK, Gartner DR, Noppert GA. A geography of risk: structural racism and COVID-19 mortality in the United States. Am J Epidemiol. 2021;190(8):1439–1446. doi: 10.1093/aje/kwab059. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Garcia MA, Homan PA, García C, Brown TH. The color of COVID-19: structural racism and the disproportionate impact of the pandemic on older Black and Latinx adults. J Gerontol B. 2021;76(3):e75–e80. doi: 10.1093/geronb/gbaa114. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Galea S, Keyes K. Understanding the COVID-19 pandemic through the lens of population health science. Am J Epidemiol. 2020;189(11):1232–1237. doi: 10.1093/aje/kwaa142. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.National Center for Health Statistics. 2020. https://www.cdc.gov/nchs/nvss/vsrr/covid19/excess_deaths.htm
- 10.US Census Bureau. 2020. https://www.census.gov/data/tables/time-series/demo/popest/2010s-national-detail.html
- 11.Cole SR, Hudgens MG, Brookhart MA, Westreich D. Risk. Am J Epidemiol. 2015;181(4):246–250. doi: 10.1093/aje/kwv001. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Gill JR, DeJoseph ME. The importance of proper death certification during the COVID-19 pandemic. JAMA. 2020;324(1):27–28. doi: 10.1001/jama.2020.9536. [DOI] [PubMed] [Google Scholar]
- 13.Goldhill O.2021. https://www.statnews.com/2021/01/25/undercounting-covid-19-deaths-greatest-in-pro-trump-areas-analysis-shows
- 14.Pell R, Fryer E, Manek S, Winter L, Roberts ISD. Coronial autopsies identify the indirect effects of COVID-19. Lancet Public Health. 2020;5(9):e474. doi: 10.1016/S2468-2667(20)30180-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Ahmad FB, Anderson RN. The leading causes of death in the US for 2020. JAMA. 2021;325(18):1829–1830. doi: 10.1001/jama.2021.5469. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Katz J, Goodnough A, Sanger-Katz M. In shadow of pandemic, U.S. drug overdose deaths resurge to record. New York Times. July 15, 2020https://www.nytimes.com/interactive/2020/07/15/upshot/drug-overdose-deaths.html
- 17.Bates J. 2020 will end as one of America’s most violent years in decades. Time. December 30, 2020
- 18.Hartnett KP, Kite-Powell A, DeVies J, et al . Impact of the COVID-19 pandemic on emergency department visits—United States, January 1, 2019–May 30, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(23):699–704. doi: 10.15585/mmwr.mm6923e1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Faust JS, Krumholz HM, Du C, et al. All-cause excess mortality and COVID-19–related mortality among US adults aged 25‒44 years, March‒July 2020. JAMA. 2021;325(8):785–787. doi: 10.1001/jama.2020.24243. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Czeisler MÉ, Lane RI, Petrosky E, et al. Mental health, substance use, and suicidal ideation during the COVID-19 pandemic—United States, June 24–30, 2020. MMWR Morb Mortal Wkly Rep. 2020;69(32):1049–1057. doi: 10.15585/mmwr.mm6932a1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Gould E, Kassa M.2020. https://www.epi.org/publication/young-workers-covid-recession
- 22.Vahratian A, Blumberg SJ, Terlizzi EP, Schiller JS. Symptoms of anxiety or depressive disorder and use of mental health care among adults during the COVID-19 pandemic—United States, August 2020–February 2021. MMWR Morb Mortal Wkly Rep. 2021;70(13):490–494. doi: 10.15585/mmwr.mm7013e2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Stokes AC, Lundberg DJ, Elo IT, Hempstead K, Bor J, Preston SH. Assessing the impact of the COVID-19 pandemic on US mortality: a county-level analysis. medRxiv. 2021 doi: 10.1101/2020.08.31.20184036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Wrigley-Field E, Garcia S, Leider JP, Robertson C, Wurtz R. Racial disparities in COVID-19 and excess mortality in Minnesota. Socius. 2020;6:2378023120980918. doi: 10.1177/2378023120980918. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Rader B, Astley CM, Sy KTL, et al. Geographic access to United States SARS-CoV-2 testing sites highlights healthcare disparities and may bias transmission estimates. J Travel Med. 2020;27(7):taaa076. doi: 10.1093/jtm/taaa076. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.McClure ES, Vasudevan P, Bailey Z, Patel S, Robinson WR. Racial capitalism within public health: how occupational settings drive COVID-19 disparities. Am J Epidemiol. 2020;189(11):1244–1253. doi: 10.1093/aje/kwaa126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Matthay EC, Duchowny K, Riley A, Galea S. Projected all-cause deaths attributable to COVID-19–related unemployment in the United States. Am J Public Health. 2021;111(4):696–699. doi: 10.2105/AJPH.2020.306095. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Jeung R.2021. https://stopaapihate.org/wp-content/uploads/2021/05/Stop-AAPI-Hate-Report-National-210316.pdf
- 29.Bailey ZD, Moon JR. Racism and the political economy of COVID-19: will we continue to resurrect the past? J Health Polit Policy Law. 2020;45(6):937–950. doi: 10.1215/03616878-8641481. [DOI] [PubMed] [Google Scholar]
- 30.Laster Pirtle WN. Racial capitalism: a fundamental cause of novel coronavirus (COVID-19) pandemic inequities in the United States. Health Educ Behav. 2020;47(4):504–508. doi: 10.1177/1090198120922942. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Gravlee CC. Systemic racism, chronic health inequities, and COVID‐19: a syndemic in the making? Am J Hum Biol. 2020;32(5):e23482. doi: 10.1002/ajhb.23482. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Dávalos LM,, Austin RM, Balisi MA, et al. Pandemics’ historical role in creating inequality. Science. 2020;368(6497):1322–1323. doi: 10.1126/science.abc8953. [DOI] [PubMed] [Google Scholar]
- 33.Cooper LA, Williams DR. Excess deaths from COVID-19, community bereavement, and restorative justice for communities of color. JAMA. 2020;324(15):1491–1492. doi: 10.1001/jama.2020.19567. [DOI] [PubMed] [Google Scholar]
- 34.Kiang MV, Irizarry RA, Buckee CO, Balsari S. Every body counts: measuring mortality from the COVID-19 pandemic. Ann Intern Med. 2020;173(12):1004–1007. doi: 10.7326/M20-3100. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Noppert GA, Zalla LC. Who counts and who gets counted? Health equity in infectious disease surveillance. Am J Public Health. 2021;111(6):1004–1006. doi: 10.2105/AJPH.2021.306249. [DOI] [PMC free article] [PubMed] [Google Scholar]