Abstract
Injury to the medial compartment of the knee is the most common ligament injury to this joint. The medial approach must consider the presence of associated anteromedial instability. Untreated injury of these instabilities can result in failure of the other reconstructed ligaments. As treatment is usually associated with other ligaments, it is relevant that the technique could save grafts and synthetic material. This article aims to describe a technique for the treatment of anteromedial instabilities through semimembranosus tendon tenodesis in a more anterior and distal position, promoting the tensioning of the posteromedial structures.
Technique Video
Reconstruction of a posteromedial structure of a left knee. The patient is in a supine position. The medial approach starts over the medial epicondyle up to 7 cm distal to the joint interline in the medial tibia surface. At this moment, the semitendinosus and gracilis tendons are removed and prepared to serve as a graft for the (MCLs). The direct tibial insertion of the semimembranosus (SM) tendon is individualized and reinserted from the tibia. Anterodistalization of this tendon is carried out, and posterior oblique ligament is tensioned on this anchor with knee flexed at 5°, neutral rotation, and without adduction. Finally, the MCLs are reconstructed and fixed in 30° of flexion using interference screws.
Introduction
Medial collateral ligament (MCL) injury is the most common ligament injury of the knee.1 This ligament is anatomically divided into superficial medial collateral ligament (MCLs) and deep medial collateral ligament (MCLd), and it is considered the primary stabilizer in abduction and secondary to the external knee rotation, acting in conjunction with the posteromedial corner (PMC). PMC is composed of the posterior oblique ligament (POL), the posterior horn of the medial meniscus, the capsular joint, and the insertions of the semimembranosus tendon that secondarily operates as restrictors of anteroposterior translation, external rotation, and valgus. PMC is also known as the semimembranosus corner, since all the structures in this region are directly related to it. Patients with MCL injury associated with PMC injury have rotational anteromedial instability of the knee (AMRI), described by Slocum and Larson, characterized by excess valgus movement associated with external rotation.2, 3, 4, 5, 6 PMC injuries are often undiagnosed or neglected. This fact can generate residual instability, and it has been described as being responsible for the treatment failure of the cruciate ligament due to generating mechanical overload.3 The techniques described for the treatment of PMC injuries include repair or reconstruction, however, always looking for static stability.7, 8, 9, 10, 11, 12, 13, 14, 15, 16 Nonetheless, these structures have a dynamic function in restraining knee rotation and translation, especially in amplitudes close to extension.17,18 Yet, it is not clear in literature when the technique of reconstructing medial structures should or should not contain the reconstruction of posteromedial structures.4,5,19, 20, 21, 22, 23, 24, 25 The reinsertion and retensioning of posteromedial structures could establish stability in this region of the knee preserving the dynamic function of the SM muscle tendon. This study aims to describe a technique for the treatment of AMRI associated with MCL reconstruction through the tenodesis of the SM tendon in a more anterior and distal position.
Methods
Diagnosis
This case is part of a retrospective cohort of individuals diagnosed with AMRI who underwent reconstruction of the anterior cruciate ligament (ACL) and tibial collateral ligament associated with tenodesis of the SM, being approved by the ethics committee of this institution under the number 83352118.9.0000.5486. Patients were clinically evaluated for the diagnosis of AMRI and those, who presented positive tests for anterior drawer with external rotation, dial test at 30°. and opening in abnormal abduction with an extended knee, were considered to have AMRI. All patients had knee magnetic resonance that presented damage to the anterior cruciate ligament and damage to the medial structures and stress radiographs showing abnormal medial opening when compared to the contralateral knee.
Surgical Technique
The objective of this technique is to retension the posteromedial structures related to the SM tendon through the tenodesis of this tendon in a more anterior and distal position. (Video 1) The procedure is initiated by knee arthroscopy through conventional, anteromedial, and anterolateral portals for the joint inventory and the diagnosis of associated injuries. In the evaluation of the medial compartment, the magnitude of the opening in abduction is observed by the distance between the medial condyle and the tibial plateau and the presence of associated medial meniscal lesions, and the presence of floating meniscus.26,27 ACL reconstruction was performed using the anatomical technique through the anteromedial portal with a 10-mm diameter quadriceps tendon graft. The fixation of the femoral tunnel is performed with an 8 × 25 mm interference screw (BIOSURE HA-Smith & Nephew, Andover MA). Tibial fixation will only be performed after fixation of the medial ligament complex. The medial approach starts over the medial epicondyle up to 7 cm distal to the joint interline in the medial tibia surface. After dissection, the longitudinal opening of the sartorius muscle fascia and the medial retinaculum is performed (Fig 1). At this moment, the semitendinosus and gracilis tendons are removed and prepared to serve as a graft for the MCLs (Figs 2 and 3). The direct tibial insertion of the SM tendon is individualized and deinserted from the tibia. Through deep dissection, the remnants of the POL and the meniscotibial ligaments are individualized (Fig 3).
Fig 1.
Medial aspect of the access route to the posteromedial region of a left knee. Patient is in supine position. (A) Medial approach starts over the medial epicondyle up to 7 cm distal to the joint interline in the medial tibia surface. This approach is more posterior than the usual to facilitate deep dissection. (B) The longitudinal opening of the Sartorius muscle fascia and the medial retinaculum is performed. At this moment in the procedure, it is not frequently possible to visualize the ligament injury.
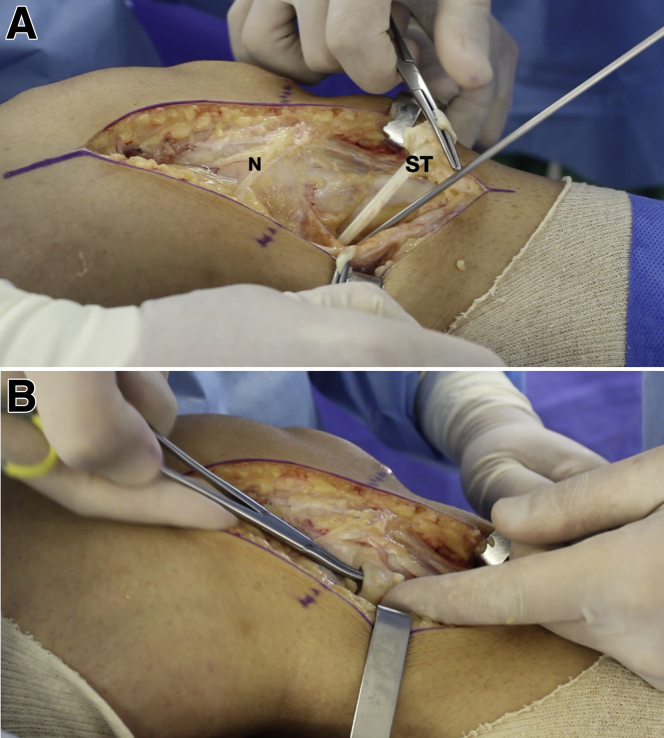
Fig 2.
Medial aspect of the access route to the posteromedial region of a left knee. Patient is in supine position. (A) The semitendinosus (ST) and gracilis tendons are removed. N denotes the cutaneous branch of the saphenous nerve. (B) Identification of the direct tibial insertion of the semimembranosus tendon is individualized.
Fig 3.
Medial aspect of the access route to the posteromedial region of a left knee. Patient is in supine position. After opening the superficial layers and removing the tendons from the semitendinosus and gracilis muscles, the posterior oblique ligament (POL) is identified, as well as the tendon of the semimembranosus muscle. N denotes the cutaneous branch of the saphenous nerve.
A K-wire is placed 10 mm anteriorly and 10 mm distally from the direct insertion of the SM tendon and a temporary suture of this tendon is made, testing the flexion-extension of the knee to verify there is no extension restriction (Fig 4). After finding the point where tendon tension is sufficient and does not restrict full extension, a 5.0-mm metallic anchor is placed at this point (TWINFIX /ULTRABRAID-Smith &Nephew, Andover MA). Anterodistalization of this tendon is carried out, and the POL is tensioned on this anchor with the knee flexed at 5°, neutral rotation, and without adduction (Figs 5 and 6). The meniscotibial ligaments of the medial meniscus and its posterior horn must also be properly reinserted using a 5.0 metal anchor (TWINFIX / ULTRABRAID - Smith & Nephew, Andover MA) (Figs 6 and 7). The anatomical points for the execution of the tunnels in the reconstruction of the MCL were those described by LaPrade et al. The femoral insertion is located 3.2 mm proximal and 4.8 mm posterior to the medial epicondyle, and the tibial insertion is located as posterior as possible along the medial surface of the proximal tibia 7 mm away from the medial articular surface (Fig 8) (24). Using two 2.0-mm Kirschner wires at these points, we tested the isometry of the future ligament. A thread of Ethibond 2 (Ethicon, Somerville, NJ) is passed through those K-wires and marked with a pen. We perform the flexion extension of the knee, and observe the movement of the Ethibond 2 Ethicon, Somerville, NJ); the mobility of this up to 5 mm is considered isometric. The tunnels are then carried out (Fig 8). The previously prepared grafts are passed and fixed with 2 8 × 25-mm interference screws (BIOSURE HA, Smith & Nephew, Andover, MA) with the knee flexed at a 30º, neutral rotation without adduction (Figs 9 and 10). Finally, the tibial ACL fixation is performed with a 11 × 30 mm interference screw (BIOSURE HA, Smith & Nephew, Andover MA) with the knee extended. After that, the remaining MCLs are repaired in the graft, and the subsequent layers are closed and suction drains are placed (Fig 10).
Fig 4.
Medial aspect of the access route to the posteromedial region of a left knee. Patient is in a supine position. A K-wire is placed 10 mm anteriorly and 10 mm distally from the direct insertion of the SM tendon, and a temporary suture of this tendon is made, testing the flexion-extension of the knee to verify that there is no extension restriction. T denotes the direct tibial insertion of the semimembranosus tendon. N denotes the cutaneous branch of the saphenous nerve.
Fig 5.
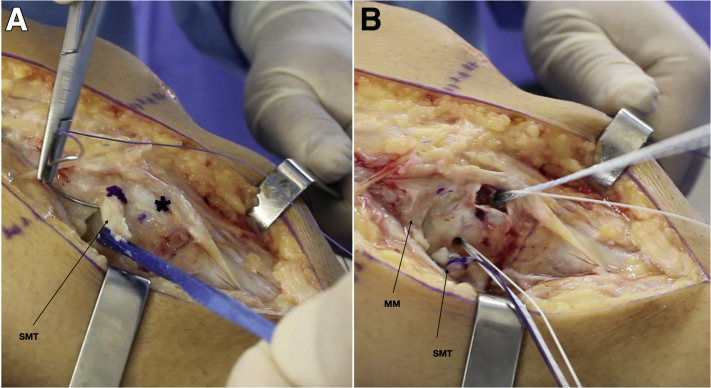
Preparation for tenodesis of the tendon of the semimembranosus muscle (SMT). Medial aspect of the posteromedial region of a left knee. Patient is in the supine position. (A) SMT is repaired with suture threads after being identified in its tibial portion in the posteromedial region of the tibia. A 10-mm distal and anterior spot (∗) is identified. (B) The two 5.0-mm metallic anchors are inserted. The most proximal tendon is shown immediately below the joint surface for the repair of the meniscotibial ligaments, and the second tendon is located at the point where the SMT tenodesis will be performed.
Fig 6.
Position of the anchors. Medial aspect of the posteromedial region of a left knee. Patient is in the supine position. (A) The most anterior and distal anchor at the point where the SMT tenodesis will be performed. (B) The most proximal anchor immediately below the joint surface and posterior for the repair of the meniscotibial ligaments. Anchor used is made with TWINFIX / ULTRABRAID (Smith & Nephew, Andover, MA).
Fig 7.
Position of the anchors. Medial aspect of the posteromedial region of a left knee. Patient is in the supine position. Final aspect of the semimembranosus tendon (SMT). Advancement and the medial meniscus (MM) repaired in the second anchor.
Fig 8.
Reconstruction of the superficial medial collateral ligament. Medial aspect of the left knee. Patient is in supine position (A) Guide wires showing anatomical points for the construction of tunnels for ligament reconstruction. (B) Final aspect of ligament reconstruction with quadruple hamstring autograft.
Fig 9.
Reconstruction of the superficial medial collateral ligament. Medial aspect of the left knee. Patient is in supine position, knee flexed at a 30º, neutral rotation without adduction. An 8×25 mm interference screw is placed to fix the new ligament.
Fig 10.
Medial aspect of the left knee. Patient is in the supine position. (A) Final aspect of the graft placed, total extension is tested. (B) The remaining medial collateral ligament is repaired in the graft, and the subsequent layers are closed.
The postoperative regimen is based on early mobility assisted by a physiotherapist from the 7th day onward. We maintain a brace for 45 days and partial load for 60 days.
Discussion
The importance of identifying and treating PMC injuries is based on the fact that posteromedial instabilities increase the external rotation of the knees and cause mechanical stress on newly reconstructed ligaments. Thus, the correct treatment of these structures serves to prevent the failure of cruciate ligament reconstruction and chondral and meniscal injuries.20,21,23,24,27, 28, 29 There are several techniques for the reconstruction of medial structures. They are based on repair by retensioning the injured ligaments or static reconstruction with a tendon graft. However, the technical difficulty of repairing a friable and barely identifiable tissue makes it difficult to establish a good anatomical parameter, so they are not very reproducible and may be related to failures. On the other hand, although static reconstructions have good clinical results, they are not able to maintain the normal mechanics of the medial compartment and, therefore, there is no evidence that these reconstructions can provide in the long term, the prevention of joint degeneration. In addition, there is a risk of confluence with the tibial cruciate ligament reconstruction tunnels.10,12, 13, 14,16,20,30, 31, 32, 33, 34, 35, 36 Given these facts, we developed a method that aims to reestablish posteromedial stability while maintaining the dynamic function of the semimembranosus muscle and, at the same time, provide the surgeon with viable tissue through a technique of easy reproducibility, based on an easy-to-use anatomical structure that already has a stabilized function in the knee joint (Table 1) (25). The risks of this technique are related to the risk of limiting knee extension and arthrofibrosis due to excessive tension in the tenodesis of the SM tendon and the impossibility of using the SM tendon due to extensive injuries to the medial compartment. The risk of slackening over time must be considered and is the subject of longitudinal studies. The use of interference screws in the tibial cortex is also a concern, as it can cut the graft during its introduction (Table 2). Some strategies can be used to minimize this risk, for example, tapping the screw hole before its insertion through a blunt device or changing the type of tibial fixation to a cortical fixation with a button, screws, washers, or staples. The advantages of this technique are related to the possibility of maintaining the dynamic function of posteromedial structures, the lower risk of a tunnel confluence, the need to use tendon grafts, which for places where there is no autologous graft available, may be a technical limitation—and finally, the possibility of being associated with any MCLs reconstruction technique (Table 1). The primary outcome of this study was to present a new possibility of treatment for the anteromedial knee instability with autologous grafts. Thus, anterodistalization of the semimembranosus muscle tendon is a viable and reproducible technique that can be part of the therapeutic arsenal in the treatment of multiligament knee injuries.
Table 1.
Advantages and Disadvantages of Semimembranosus Tendon Advancement for the Anteromedial Knee Rotatory Instability Treatment
| Advantages | Disadvantages |
|---|---|
| It does not need a posteromedial bone tunnel avoiding many tibial tunnels and the risk of their confluence. | Need for postoperative immobilization |
| It provides an easily identifiable landmark for repairs making repair techniques more reproducible. | Fixing the graft with an interference screw in the tibia can be difficult. |
| It can be used in association with any technique for medial reconstruction | |
| It can also be used with biotenodesis anchors (i.e., Swivelock-Arthrex, Naples FL) |
Table 2.
Pearls and Pitfalls of Semimembranosus Tendon (SMT) Advancement for the Anteromedial Knee Rotatory Instability Treatment
| Pearls | Pitfalls |
|---|---|
| You can perform the incision more posterior than usual. | In extensive lesions, it may be difficult to locate the SMT. |
| You can check the extension before final tendon fixation. | In associated meniscal injuries, it may be necessary an outside-in meniscal repair |
| Fixing the semimembranosus tendon with a slight flexion facilitates suturing. | In a multiligamentary injury, care must be taken not to fix the tendon with the subluxated knee. |
| Doing a tibial scarification before placing the anchor helps the tendon-bone healing. | In acute injuries, the tendon can be damaged, which can make its individualization difficult. |
Footnotes
Full ICMJE author disclosure forms are available for this article online, as supplementary material.
Supplementary Data
Reconstruction of a posteromedial structure of a left knee. The patient is in a supine position. The medial approach starts over the medial epicondyle up to 7 cm distal to the joint interline in the medial tibia surface. At this moment, the semitendinosus and gracilis tendons are removed and prepared to serve as a graft for the (MCLs). The direct tibial insertion of the semimembranosus (SM) tendon is individualized and reinserted from the tibia. Anterodistalization of this tendon is carried out, and posterior oblique ligament is tensioned on this anchor with knee flexed at 5°, neutral rotation, and without adduction. Finally, the MCLs are reconstructed and fixed in 30° of flexion using interference screws.
References
- 1.Jungmann P.M. [Posteromedial corner of the knee] Radiologe. 2019;59:155–168. doi: 10.1007/s00117-018-0488-z. [DOI] [PubMed] [Google Scholar]
- 2.Robinson J.R., Sanchez-Ballester J., Bull A.M., ReW Thomas, Amis A.A. The posteromedial corner revisited. An anatomical description of the passive restraining structures of the medial aspect of the human knee. J Bone Joint Surg Br. 2004;86:674–681. doi: 10.1302/0301-620x.86b5.14853. [DOI] [PubMed] [Google Scholar]
- 3.Lundquist R.B., Matcuk G.R., Schein A.J., et al. Posteromedial corner of the knee: The neglected corner. Radiographics. 2015;35:1123–1137. doi: 10.1148/rg.2015140166. [DOI] [PubMed] [Google Scholar]
- 4.Lubowitz J.H., MacKay G., Gilmer B. Knee medial collateral ligament and posteromedial corner anatomic repair with internal bracing. Arthrosc Tech. 2014;3:e505–508. doi: 10.1016/j.eats.2014.05.008. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Dold A.P., Swensen S., Strauss E., Alaia M. The posteromedial corner of the knee: Anatomy, pathology, and management strategies. J Am Acad Orthop Surg. 2017;25:752–761. doi: 10.5435/JAAOS-D-16-00020. [DOI] [PubMed] [Google Scholar]
- 6.Cavaignac E., Carpentier K., Pailhé R., Luyckx T., Bellemans J. The role of the deep medial collateral ligament in controlling rotational stability of the knee. Knee Surg Sports Traumatol Arthrosc. 2015;23:3101–3107. doi: 10.1007/s00167-014-3095-1. [DOI] [PubMed] [Google Scholar]
- 7.Wymenga A.B., Kats J.J., Kooloos J., Hillen B. Surgical anatomy of the medial collateral ligament and the posteromedial capsule of the knee. Knee Surg Sports Traumatol Arthrosc. 2006;14:229–334. doi: 10.1007/s00167-005-0682-1. [DOI] [PubMed] [Google Scholar]
- 8.Van der Wal W.A., Van Gennip S., Heesterbeek P.J., Busch V.J., Wymenga A.B. Anatomical superficial medial collateral ligament reconstruction with posteromedial capsule reefing successfully restores valgus knee laxity. Acta Orthop Belg. 2020;86:69–76. [PubMed] [Google Scholar]
- 9.Ng J.W.G., Myint Y., Ali F.M. Management of multiligament knee injuries. EFORT Open Rev. 2020;5:145–155. doi: 10.1302/2058-5241.5.190012. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Mehl J.T., Kia C., Murphy M., et al. Posteromedial ligament repair of the knee with suture tape augmentation: A biomechanical study. Am J Sports Med. 2019;47:2952–2959. doi: 10.1177/0363546519868961. [DOI] [PubMed] [Google Scholar]
- 11.Maxwell G.T., Warth R.J., Amin A., et al. Multiple ligament knee injuries: Does the knee dislocation classification predict the type of surgical management? J Knee Surg. 2021;34:273–279. doi: 10.1055/s-0039-1695739. [DOI] [PubMed] [Google Scholar]
- 12.Malinowski K., Hermanowicz K., Góralczyk A., LaPrade R.F. Medial collateral ligament reconstruction with anteromedial reinforcement for medial and anteromedial rotatory instability of the knee. Arthrosc Tech. 2019;8:e807–e814. doi: 10.1016/j.eats.2019.03.019. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Lind M., Jakobsen B.W., Lund B., Hansen M.S., Abdallah O., Christiansen S.E. Anatomical reconstruction of the medial collateral ligament and posteromedial corner of the knee in patients with chronic medial collateral ligament instability. Am J Sports Med. 2009;37:1116–1122. doi: 10.1177/0363546509332498. [DOI] [PubMed] [Google Scholar]
- 14.Kim M.S., Koh I.J., In Y. Superficial and deep medial collateral ligament reconstruction for chronic medial instability of the knee. Arthrosc Tech. 2019;8:e549–e554. doi: 10.1016/j.eats.2019.01.016. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Jiang K.N., West R.V. Management of chronic combined ACL medial posteromedial instability of the knee. Sports Med Arthrosc Rev. 2015;23:85–90. doi: 10.1097/JSA.0000000000000056. [DOI] [PubMed] [Google Scholar]
- 16.Fanelli G.C., Harris J.D. Surgical treatment of acute medial collateral ligament and posteromedial corner injuries of the knee. Sports Med Arthrosc Rev. 2006;14:78–83. doi: 10.1097/01.jsa.0000212301.80496.dc. dc. [DOI] [PubMed] [Google Scholar]
- 17.D’Ambrosi R., Corona K., Guerra G., Rubino M., Di Feo F., Ursino N. Biomechanics of the posterior oblique ligament of the knee. Clin Biomech (Bristol, Avon) 2020;80:105205. doi: 10.1016/j.clinbiomech.2020.105205. [DOI] [PubMed] [Google Scholar]
- 18.Sonnery-Cottet B., Serra Cruz R., Vieira T.D., Goes R.A., Saithna A. Ramp lesions: An unrecognized posteromedial instability? Clin Sports Med. 2020;39:69–81. doi: 10.1016/j.csm.2019.08.010. [DOI] [PubMed] [Google Scholar]
- 19.Wada K., Hamada D., Tamaki S., Higashino K., Fukui Y., Sairyo K. Influence of Medial collateral ligament release for internal rotation of tibia in posterior-stabilized total knee arthroplasty: A cadaveric study. J Arthroplasty. 2017;32:270–273. doi: 10.1016/j.arth.2016.06.013. [DOI] [PubMed] [Google Scholar]
- 20.Stannard J.P. Medial and posteromedial instability of the knee: Evaluation, treatment, and results. Sports Med Arthrosc Rev. 2010;18:263–268. doi: 10.1097/JSA.0b013e3181eaf713. [DOI] [PubMed] [Google Scholar]
- 21.Robinson J.R., Bull A.M., Thomas R.R., Amis A.A. The role of the medial collateral ligament and posteromedial capsule in controlling knee laxity. Am J Sports Med. 2006;34:1815–1823. doi: 10.1177/0363546506289433. [DOI] [PubMed] [Google Scholar]
- 22.Robinson J.R., Sanchez-Ballester J., Bull A.M.J., Thomas R.D.M., Amis A.A. The posteromedial corner revisited—An anatomical description of the passive restraining structures of the medial aspect of the human knee. J Bone Joint Surg Br. 2004;86B:674–681. doi: 10.1302/0301-620x.86b5.14853. [DOI] [PubMed] [Google Scholar]
- 23.Ritchie J.R., Bergfeld J.A., Kambic H., Manning T. Isolated sectioning of the medial and posteromedial capsular ligaments in the posterior cruciate ligament-deficient knee. Influence on posterior tibial translation. Am J Sports Med. 1998;26:389–394. doi: 10.1177/03635465980260030801. [DOI] [PubMed] [Google Scholar]
- 24.Peltier A., Lording T., Maubisson L., Ballis R., Neyret P., Lustig S. The role of the meniscotibial ligament in posteromedial rotational knee stability. Knee Surg Sports Traumatol Arthrosc. 2015;23:2967–2973. doi: 10.1007/s00167-015-3751-0. [DOI] [PubMed] [Google Scholar]
- 25.Kittl C., Becker D.K., Raschke M.J., et al. Dynamic restraints of the medial side of the knee: The semimembranosus corner revisited. Am J Sports Med. 2019;47:863–869. doi: 10.1177/0363546519829384. [DOI] [PubMed] [Google Scholar]
- 26.Black A.K. Editorial Commentary: Don’t float away—Medial collateral ligament and medial meniscus will protect your anterior cruciate ligament reconstruction if you respect them. Arthroscopy. 2019;35:938–939. doi: 10.1016/j.arthro.2019.01.019. [DOI] [PubMed] [Google Scholar]
- 27.Funchal L.F.Z., Astur D.C., Ortiz R., Cohen M. The Presence of the arthroscopic “floating meniscus” sign as an indicator for surgical intervention in patients with combined anterior cruciate ligament and grade II medial collateral ligament injury. Arthroscopy. 2019;35:930–937. doi: 10.1016/j.arthro.2018.10.114. [DOI] [PubMed] [Google Scholar]
- 28.LaPrade R.F., Engebretsen A.H., Ly T.V., et al. The anatomy of the medial part of the knee. J Bone Joint Surg Am. 2007;89:2000–2010. doi: 10.2106/JBJS.F.01176. [DOI] [PubMed] [Google Scholar]
- 29.Svantesson E., Hamrin Senorski E., et al. Increased risk of ACL revision with non-surgical treatment of a concomitant medial collateral ligament injury: A study on 19,457 patients from the Swedish National Knee Ligament Registry. Knee Surg Sports Traumatol Arthrosc. 2019;27:2450–2459. doi: 10.1007/s00167-018-5237-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Tibor L.M., Marchant M.H., Taylor D.C., Hardaker W.T., Garrett W.E., Sekiya J.K. Management of medial-sided knee injuries. Part 2: Posteromedial corner. Am J Sports Med. 2011;39:1332–1340. doi: 10.1177/0363546510387765. [DOI] [PubMed] [Google Scholar]
- 31.Roth J., Taylor D.C. Management of acute isolated medial and posteromedial instability of the knee. Sports Med Arthrosc Rev. 2015;23:71–76. doi: 10.1097/JSA.0000000000000065. [DOI] [PubMed] [Google Scholar]
- 32.Moulton S.G., Bhatia S., Civitarese D.M., Frank R.M., Dean C.S., LaPrade R.F. Surgical techniques and outcomes of repairing meniscal radial tears: A systematic review. Arthroscopy. 2016;32:1919–1925. doi: 10.1016/j.arthro.2016.03.029. [DOI] [PubMed] [Google Scholar]
- 33.Fanelli G.C., Fanelli D.G. Management of chronic combined PCL medial posteromedial instability of the knee. Sports Med Arthrosc Rev. 2015;23:96–103. doi: 10.1097/JSA.0000000000000061. [DOI] [PubMed] [Google Scholar]
- 34.DeLong J.M., Waterman B.R. Surgical techniques for the reconstruction of medial collateral ligament and posteromedial corner injuries of the knee: A systematic review. Arthroscopy. 2015;31:2258–2272.e1. doi: 10.1016/j.arthro.2015.05.011. [DOI] [PubMed] [Google Scholar]
- 35.DeLong J.M., Waterman B.R. Surgical repair of medial collateral ligament and posteromedial corner injuries of the knee: A systematic review. Arthroscopy. 2015;31:2249–2255.e5. doi: 10.1016/j.arthro.2015.05.010. [DOI] [PubMed] [Google Scholar]
- 36.Bauer K.L., Stannard J.P. Surgical approach to the posteromedial corner: Indications, technique, outcomes. Curr Rev Musculoskelet Med. 2013;6 doi: 10.1007/s12178-013-9161-3. 124-131. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Reconstruction of a posteromedial structure of a left knee. The patient is in a supine position. The medial approach starts over the medial epicondyle up to 7 cm distal to the joint interline in the medial tibia surface. At this moment, the semitendinosus and gracilis tendons are removed and prepared to serve as a graft for the (MCLs). The direct tibial insertion of the semimembranosus (SM) tendon is individualized and reinserted from the tibia. Anterodistalization of this tendon is carried out, and posterior oblique ligament is tensioned on this anchor with knee flexed at 5°, neutral rotation, and without adduction. Finally, the MCLs are reconstructed and fixed in 30° of flexion using interference screws.
Reconstruction of a posteromedial structure of a left knee. The patient is in a supine position. The medial approach starts over the medial epicondyle up to 7 cm distal to the joint interline in the medial tibia surface. At this moment, the semitendinosus and gracilis tendons are removed and prepared to serve as a graft for the (MCLs). The direct tibial insertion of the semimembranosus (SM) tendon is individualized and reinserted from the tibia. Anterodistalization of this tendon is carried out, and posterior oblique ligament is tensioned on this anchor with knee flexed at 5°, neutral rotation, and without adduction. Finally, the MCLs are reconstructed and fixed in 30° of flexion using interference screws.