Abstract
Aims
Diabetes mellitus (DM) and atrial fibrillation (AF) commonly co-exist. Oral anticoagulants (OACs) are widely used in patients with DM. This review aims to summarise the available literature on the safety (hypoglycaemia or bleeding) and efficacy (stroke or systemic embolism) of the use of OACs in patients with DM.
Methods
We searched the Medline, the Excerpta Medica dataBASE (Embase) and Cochrane databases up to the 10th of December 2020. The search strategy was conducted using both keywords and MeSH terms. We included randomised controlled trials (RCTs) and observational studies that reported on the safety and efficacy of the use of OACs in patients with diabetes from all age groups. Study selection, data extraction and quality assessment were conducted independently by two reviewers.
Results
A total of 3,976 articles were identified through the search process, of which seven studies met the inclusion criteria of the systematic review: four observational studies and three studies that were randomised controlled trials, with a total of 703,855 patients. Two observational studies reported that the use of warfarin was associated with a higher risk of hypoglycaemic events, specifically with sulfonylurea. One observational study and three randomised controlled trials reported that the use of warfarin compared to other oral anticoagulants was associated with a higher risk of bleeding. In addition, three randomised controlled trials reported that the use of warfarin compared to other oral anticoagulants was associated with a lower risk of stroke or systemic embolism.
Conclusions
This systematic review found that DOACs had a better efficacy outcome and safer clinical outcomes in comparison to warfarin in patients with diabetes.
Keywords: Anticoagulant, Safety, Systematic review, Diabetes mellitus
1. Introduction
Atrial fibrillation (AF) is considered one of the most prevalent types of arrhythmia and is a major risk factor for stroke(Wolf et al., 1991). Patients with diabetes mellitus (DM) are at higher risk of developing this condition compared to other patients(Huxley et al., 2011a, Huxley et al., 2011b). Patients with DM are at higher risk of costly complications due to the nature of their disease and often need combination therapy to manage their disease(Naser et al., 2018, Naser et al., 2020). The co-existence of DM and AF increases the risk of various critical cardiovascular events, bleeding, and mortality (Kannel and Mc Gee 1979). Moreover, increasing haemoglobin A1c levels and diabetes duration have been reported to raise thromboembolism risk (Bell et al., 2013). Diabetes is also a stroke independent risk factor, and in contrast with non-diabetic patients, patients with DM have more disabilities and an increased mortality risk. In addition, other stroke risk factors in AF patients are more prevalent in patients with diabetes, such as peripheral vascular disease and renal failure. The probability of the development of thromboembolic events increases by 70% in patients with diabetes (group. 2007); therefore, CHADS2 and CHA2DS2‐ VASc scores consider the presence of DM in the prediction of thromboembolic risk (Hart et al., 2008, Lip and N. R., Pisters R, Lane DA, Crijns HJ., , 2010). Treatment guidelines recommend the use of oral anticoagulation therapy in patients with DM and AF (Camm et al., 2012). Direct oral anticoagulants (DOACs) are considered to be an important advanced pharmacological option for the prevention of thromboembolic events such as stroke in patients with AF. DOACs are characterised by better and safer pharmacokinetic and pharmacodynamic profiles. In previous randomised controlled trials, patients who were using DOACs had a 14% reduction in the incidence of bleeding compared to patients who were on warfarin therapy (Giugliano et al., 2013, Ruff et al., 2014, Brambatti et al., 2015, Ezekowitz et al., 2015). Atrial fibrillation is an independent risk factor for diabetes (Dublin et al., 2010). Several reports have highlighted that the prevalence of AF in patients with diabetes ranges from 8% to 14% (Movahed et al., 2005, Murphy et al., 2007). Knowing that DM and AF commonly co-exist and, therefore, the use of oral anticoagulants (OACs) is a common combination in this population of patients, it is necessary to assess the safety and efficacy of OACs in patients with DM due to the high number of patients and the potential association with serious adverse outcomes such as bleeding and hypoglycaemia (Ament P 2000).
No previous systematic review and meta-analysis have investigated the safety and efficacy of the use of anticoagulant medications therapy in patients with type 2 DM in combined observational and randomised controlled trial (RCT) studies. One previous meta-analysis explored the safety of OACs in patients with T2DM in phase III randomised trials only (Giuseppe Patti et al., 2017). Exploring the safety of the use of anticoagulant medications therapy in patients with DM from combined observational and RCT studies enable us to have more robust evidence from both real-life data (observational studies) and well-controlled conditions (RCTs). This review aimed to summarise the available literature on the safety and efficacy of the use of OACs (including warfarin and DOACs) in patients with DM.
2. Method
2.1. Data sources
We searched the Medline, the Excerpta Medica dataBASE (Embase) and the Cochrane databases up to the 10th of December 2020 for studies that examined the safety and the efficacy of the use of anticoagulant medications therapy in patients with type 2 DM. We used a combination of MeSh (Medical Subject Heading)/ Emtree terms and keywords during the search process. The study protocol was registered with PROSPERO (Ref: CRD42021260169).
2.2. Search strategy and study selection
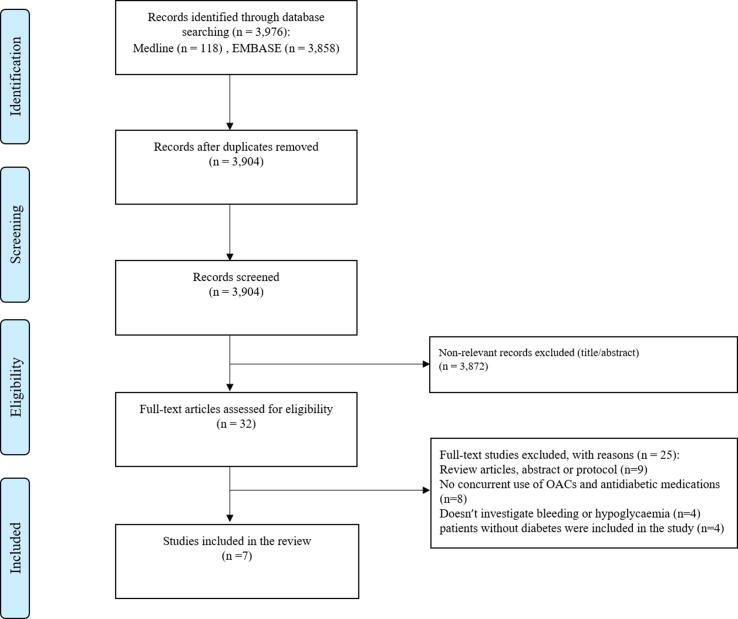
The Preferred Reporting Items for Systematic Review and Meta-Analysis (PRISMA) guidelines were implemented throughout the search process (Moher et al., 2009). In addition, this study followed the Meta-analysis of Observational Studies in Epidemiology (MOOSE) guidelines (Stroup et al., 2000). The following keywords were used in the search process: “Adverse Drug Events OR Adverse Drug Reactions OR Side Effects OR Risk Factors” AND “Insulin OR Agents OR Antidiabetic Medications” AND “Anticoagulants OR Oral Anticoagulants OR Direct Oral Anticoagulants OR DOAC OR NOAC”. Our search process considered suffix variations and all the synonyms for each keyword. In addition, we combined the search results of the keywords with those of the available “MeSH term”. The search strategy was based on an extensive literature search and was confirmed by an expert physician. Endnote X7 software was used to manage the search process. Further details about the search process are available in Appendix 1. The selection process of the studies was conducted by two reviewers (HA and BA) and was summarised using the PRISMA diagram, Fig. 1. We included studies that explored the safety of the use of anticoagulant medications in patients with DM only. RCT or non-randomised studies that investigated the safety and efficacy of OACs in patients with DM were included. We did not have any restrictions on gender or age to make our conclusion more generalisable and robust. Studies not related to the topic and deemed irrelevant were excluded. OACs included warfarin and DOACs (including apixaban, dabigatran, rivaroxaban and edoxaban).
Fig. 1.
PRISMA diagram.
2.3. Study outcomes
Safety outcomes of interest were hypoglycaemia and bleeding from any type or severity. Efficacy outcomes were cardiovascular events, including stroke and systemic embolism.
2.4. Data extraction and quality assessment
Two reviewers (HA, BA) independently extracted data from the included studies using a data extraction form. The data extraction was checked by a third reviewer (AN). Extracted information included the following study characteristics: the author's name (publication year), country, study design, sample size, sample source, type of diabetes among the study population, mean/ median age of the patients, sex, diabetes duration, treatment regimens, the definition of hypoglycaemia, bleeding, and cardiovascular outcomes in the study (stroke and systemic embolism). The outcome of interest was the effect size (such as OR, RR, HR, or the frequency and percentage of events in each treatment group).
2.5. Quality assessment
The Cochrane handbook of systematic reviews of intervention guidelines was used to assess the quality of the included RCTs (Higgins and Green 2011). The quality assessment for the included observational studies was conducted using the Newcastle-Ottawa quality assessment scale [14], which was modified to meet the requirement of this review (Herzog et al., 2013, Alwafi et al., 2020a, Alwafi et al., 2020b, Alwafi et al., 2020c, Park et al., 2020). A total of seven criteria were evaluated: representativeness of the population, sample size, statistical analysis, confounders, missing data, methodology to report the outcome of interest, and methods to detect or report the outcome of interest. Each criterion was rated using a scale ranging from 0 to 3, where 3 represented the highest quality; the highest possible overall score was 21. In addition, we categorised the quality assessment score into three categories: good quality (>14 points), moderate quality (>7 points) and low quality (≤7 points) (Wells et al., 2000). Further details on the quality assessment tools that were used are available in Appendix 2.
3. Results
A total of 3,976 articles were identified through the search process of the two databases: Medline (n = 118), EMBASE (n = 3,858). After removing duplicates, a total of 3,904 articles remained for the screening stage. After that, the title and abstract of the remaining articles were screened, through which a total of 3,872 articles were deemed irrelevant and were immediately excluded. The remaining 32 articles were assessed according to the inclusion/exclusion criteria after reading the full text. At this stage, a total of 25 articles were excluded for different reasons which included review articles, abstracts or protocols (n = 9), no use of oral anticoagulant medications (n = 8), does not investigate hypoglycaemia, bleeding, or cardiovascular outcomes (n = 4), and patients without diabetes were included in the study (n = 4). A total of seven studies met the inclusion criteria of the systematic review. The results are presented using narrative synthesis and tabulation of the data.
3.1. Description of studies
Out of the seven relevant articles that were included in this systematic review, four studies were observational studies (two cohort studies (Baker et al., 2019, Lip et al., 2020) and two self-controlled case series studies (Romley et al., 2015, Nam et al., 2019a, Nam et al., 2019b)) and three studies were randomised controlled trials (Bansilal et al., 2015, Brambatti et al., 2015, Ezekowitz et al., 2015). A total of 703,855 patients (661,846) patients were identified from the observational studies and 42,009 patients were identified from the RCTs. The sample size in the included studies ranged between 3,467 to 465,918. The four observational studies used medical claims data from medical databases in the USA (Romley et al., 2015, Baker et al., 2019, Nam et al., 2019a, Nam et al., 2019b, Lip et al., 2020). Two observational studies explored the safety in terms of hypoglycaemic events (Romley et al., 2015, Nam et al., 2019a, Nam et al., 2019b), and two studies explored the safety and efficacy of OACs in patients with DM (Baker et al., 2019, Lip et al., 2020). All the studies used data from electronic health records databases. The three trials explored the safety and efficacy of the OACs in patients with DM (Bansilal et al., 2015, Brambatti et al., 2015, Ezekowitz et al., 2015). Full details about the included studies are available in Table 1.
Table 1.
Details of the included studies.
| Study details | Country | Study design | Sample size | Mean age | Gender (M/F) | Treatment regimens | Definition of hypoglycaemia | Definition of bleeding | Definition of cardiovascular outcomes (efficacy) | Effect size (OR,RR,HR) |
|---|---|---|---|---|---|---|---|---|---|---|
| Ezekowitz et al. 2015 | Multinational | Double-blind, double-dummy, Randomized trial | 18,201 | Median age: 69 years (IQR 63–75) | 65.1% males | Comparing apixaban 5 mg twice daily (or 2.5 mg twicedaily for patients with ≥ 2 of the following three criteria: age ≥ 80 years, body weight ≤ 60 kg, or serum creatinine level ≥ 1.5 mg/dL) with warfarin [dosed by the investigator to achieve a target international normalized ratio (INR), 2.0–3.0] | N/A | Major bleeding was defined as acute or subacute clinically overt bleeding accompanied by one or more of the following: (i) decrease in the haemoglobin level of ≥ 2 g/dL, (ii) transfusion of ≥ 2 U of packed red blood cells, and/or (iii) bleeding that is fatal or occurs in at least one of the following critical sites: intra-cranial, intra-spinal, intra-ocular, pericardial, intra-articular, intra-muscular with compartment syndrome, or retroperitoneal. | Stroke or systemic embolism | Comparing apixaban with warfarin:- major bleeding: 0.961 (0.740–1.247).- Any bleeding: 0.727 (0.655–0.807).Cardiovascular outcomes and death-Stroke:0.746 (0.529–1.053) |
| Bansilal et al. 2015 | Multinational | An international multicentre, double-blind, double-dummy, randomized non-inferiority trial | 5,695 patients | Median age: 71 years (IQR 64–77). | 60.6% males | Comparing rivaroxaban—20 mg once daily (or 15 mg daily in patients with creatinine clearance 30–49 mL/min)—with adjusted-dose warfarin (target INR 2.5, range 2.0–3.0) | N/A | Major or non-major clinically relevant (NMCR) bleeding. | Stroke or systemic embolism | Rates of major bleeding in patients with DM randomized to rivaroxaban vs warfarin (3.79 vs 3.90 per 100 patient years). Rates of NMCR bleeding (14.81 vs 15.44 per 100 patient-years in patients with DM.Cardiovascular outcomes and death:- Stroke: Rivaroxaban vs Warfarin / 100pt-yrs: 0.23 vs 0.46- Vascular death: Rivaroxaban vs Warfarin / 100pt-yrs: 2.83 vs 3.65 |
| Brambatti et al. 2015 | Multinational (44 countries) | A randomized trial, blinded, open-label | 18,113 patients | 70.9 years ± 8.0 | 65.8 % males | Comparing two fixed doses of dabigatran versus warfarin | N/A | N/A | Stroke or systemic embolism | Compared to warfarinMajor bleeding:− 110 mg dabigatran: 0.91 (0.70, 1.19).− 150 mg dabigatran: 1.12 (0.87, 1.44).Intracranial bleeding:− 110 mg dabigatran: 0.26 (0.11, 0.65).− 150 mg dabigatran: 0.58 (0.29, 1.16).Cardiovascular outcomes and death:Compared to warfarin1- Stroke or systematic embolism.− 110 mg dabigatran:0.74(0.51,1.07).− 150 mg dabigatran:0.61 (0.41, 0.91).2- Ischemic stroke− 110 mg dabigatran:0.97 (0.64,1.40).− 150 mg dabigatran:0.76 (0.49,1.19).3- Haemorrhagic stroke− 110 mg dabigatran:0.29 (0.10,0.90).− 150 mg dabigatran:0.15 (0.03,0.67). |
| Nam et al. 2019 | United states | Observational study (self-controlled case series design) | 3,467 patients | Median age: From 74.7 years (66.3 – 82.9) to 65.1 (52.1 – 74.2) | 35.3 % males | Sulfonylurea (glimepiride, glipizide and glyburide) plus warfarin compared to metformin plus warfarin | N/A | N/A | N/A | Warfarin was associated with an elevated rate of serious hypoglycaemia when given concomitantly with glimepiride (RR , 1.47; 95% confidence interval (CI), 1.07–2.02) and metformin (RR , 1.73; 95% CI, 1.38–2.16). |
| Romley et al. 2015 | United states | Observational study (retrospective cohort analysis) | 465,918 patients | Mean: 74.6 years (7.5). | 42.2 % males | concurrent use f warfarin and glipizide/glimepiride | Events that required hospital admission or emergency department visit. | N/A | N/A | - Admissions or emergency department visits for hypoglycaemia were more common in person quarters with concurrent warfarin use compared with quarters without warfarin use adjusted odds ratio 1.22, 95% confidence interval 1.05 to 1.42). |
| Baker et al. 2019 | United states | Observational study (retrospective cohort analysis) | 24,646 patients | The median (25%, 75% range) age was 70 (62, 79) years | 63.5 % males | Rivaroxaban compared to warfarin | N/A | Major bleeding (intracranial or gastrointestinal) | Stroke or systemic embolism | Rivaroxaban was associatedwith a 25% (95% CI 4–41) reduced risk of major adverse cardiovascular events (MACE) and a 63% (95% CI 35–79) reduced risk of major adverse limb events (MALE) compared to warfarin. Major bleeding risk did not significantly differ between cohorts (HR 0.95). The event rates of major bleeding were 2.38 per 100 person-years among rivaroxaban users and 3.37 per 100 person-years among warfarin users. |
| Lip, et al, 2020 | United states | Observational retrospective | 167,815 | N/A | 55.0 % males | apixaban, dabigatran, rivaroxaban, and warfarin | N/A | MB/ gastrointestinal (GI) bleeding, intracranial haemorrhage, and bleeding at other key sites | Stroke or systemic embolism | Compared with warfarin, apixaban (HR, 0.60; 95% CI, 0.56–0.65) and dabigatran (HR, 0.78; 95% CI, 0.69–0.88) were associated with a lower risk of MB. Compared with warfarin, rivaroxaban was associated with a similar risk of MB (HR, 1.02; 95% CI, 0.94–1.10). Dabigatran was associated with a similar risk of stroke/SE (HR, 1.11; 95%, 0.85–1.46) and lower risk of MB (HR, 0.76; 95% CI, 0.66–0.86) compared with rivaroxaban |
3.2. Safety measures of anticoagulants medications
3.2.1. Hypoglycaemia
A study by Nam et al. reported that the co-administration of warfarin and sulfonylurea or metformin was associated with a higher risk of hypoglycaemic events (Nam et al., 2019a, Nam et al., 2019b). The co-administration of glimepiride with warfarin was associated with a higher risk of hypoglycaemic events compared to metformin (HR:1.47 (95 %CI 1.07 – 2.02) vs. 1.73 (95 %CI 1.38 – 2.16).
The second study by Romely et al. found that patients who were using warfarin with sulfonylurea (glipizide or glimepiride) were at higher risk of hypoglycaemia compared to patients who were not using warfarin (HR: 1.22 (95 %CI 1.05 – 1.42).
3.2.2. Bleeding
Baker et al. found that the risk of major bleeding events did not differ significantly between patients with DM who were using rivaroxaban or warfarin (HR: 0.95 (95 %CI 0.79 – 1.15) (Baker et al., 2019). The other study, by Lip et al., reported that compared with warfarin, apixaban (HR, 0.60; 95% CI, 0.56–0.65) and dabigatran (HR, 0.78; 95% CI, 0.69–0.88) were associated with a lower risk of major bleeding (MB). Compared with warfarin, rivaroxaban was associated with a similar risk of MB (HR, 1.02; 95% CI, 0.94–1.10). Apixaban was associated with a lower risk of MB compared with dabigatran (HR, 0.73; 95% CI, 0.63–0.84) and rivaroxaban (HR, 0.59; 95% CI, 0.54–0.65), both driven by GI bleeding. Dabigatran was associated with a similar risk of stroke/SE (HR, 1.11; 95%, 0.85–1.46) and a lower risk of MB (HR, 0.76; 95% CI, 0.66–0.86) compared with rivaroxaban. The three randomised controlled trials in this systematic review confirmed that the use of warfarin as an anticoagulant therapy was associated with a higher risk of bleeding compared to other anticoagulant options.
Ezekowitz et al. reported that patients who were using apixaban had a lower rate of any type of bleeding compared to patients on warfarin (HR: 0.727 (95 %CI 0.655 – 0.807)(Ezekowitz et al., 2015). Bansilal et al., in their study, reported that the rate of MB events was lower among users of rivaroxaban compared to warfarin users (3.79 vs. 3.90 / per 100 patient years) (Bansilal et al., 2015). In addition, Brambatti et al. reported that dabigatran had a lower risk of intracranial bleeding at a low dose (110 mg) compared to warfarin (HR: 0.26 (95 %CI 0.11 – 0.65) (Brambatti et al., 2015).
3.2.3. Efficacy (cardiovascular) outcomes
Ezekowitz et al. observed that patients on apixaban had a lower incidence of stroke or systematic embolism compared to patients on warfarin (HR: 0.746 (95 %CI 0.529–1.053)) and that apixaban showed a lower rate of cardiovascular mortality against the warfarin cohort (HR: 0.888 (95 %CI 0.655–1.203)). Bansilal et al. demonstrated the safety of rivaroxaban vs warfarin as the stroke endpoint ratios were 0.23 vs 0.46/100pt-yrs, which demonstrates that rivaroxaban has a favourable safety profile compared to warfarin. Brambatti et al. reported that patients on dabigatran had a lower risk of stroke or systematic embolism, with ratios against warfarin being (HR: 0.74(95 %CI 0.51, 1.07)) and (HR: 0.61 (95 %CI 0.41, 0.91)) for 110 mg and 150 mg cohorts, respectively.
3.2.4. Risk of bias in included studies
The quality of the included studies was high. All included studies had a sample size of 3,467 patients and above. The study objectives were mentioned in all studies. In addition, the study population was clearly defined in all studies. The inclusion and exclusion criteria were pre-specified, and the intervention/control and outcome measures were clearly defined in all studies. For further details about quality assessment for the included studies, refer to Appendix 2.
4. Discussion
This systematic review aimed to assess the safety and efficacy of OACs in patients with DM. Our study reveals the variation between oral anticoagulants in the safety profile among different oral anticoagulants in patients with DM. Previous large, randomised trials on the general population reported that DOACs are superior to warfarin in terms of embolic and haemorrhagic stroke but inferior in terms of gastrointestinal bleeding events. In our review, three randomised trials reported a similar conclusion when comparing warfarin to DOACs among patients with DM. In this review, one observational study by Baker et al. also reported non-inferior efficacy and better safety when comparing warfarin to DOACs. Moreover, Lip et al. reported that rivaroxaban and apixaban when compared to warfarin were associated with lower stroke rates. Furthermore, apixaban and dabigatran have been associated with lower MB values in comparison to warfarin. These results were conclusive on patients with DM, and they are also consistent with previous studies on the general population. A study by Vinogradova et al. reported that both apixaban and rivaroxaban were associated with a better safety profile and less associated with MB. However, this study also reported that rivaroxaban was associated with an increased risk of all-cause mortality (Vinogradova et al., 2018). Other studies also reported a similar conclusion for DOACs being safer and more efficacious compared to warfarin (Xian et al., 2019).
In this review, two observational studies reported that the concurrent use of warfarin with sulfonylurea exacerbated the odds of hypoglycaemia contrary to sulfonylurea monotherapy(Romley et al., 2015, Nam et al., 2019a, Nam et al., 2019b). This could be explained by pharmacokinetic and pharmacodynamic interactions among these agents. The displacement of sulfonylurea from their protein-binding sites is exacerbated by warfarin; subsequently, the high fraction of unbound sulfonylureas will pronounce the hypoglycaemic effect (Triplitt 2006). Another explanation is the attenuated metabolism of sulfonylureas due to the competitive inhibition of warfarin on CYP2C9(Romley et al., 2015). The co-administration of DOACs and antidiabetic agents requires further investigation to detect the prevalence of hypoglycaemia.
The correlation between bleeding and rivaroxaban or warfarin did not reach the significance threshold in one observational study. Nevertheless, three different RCT’s have demonstrated the tolerability of bleeding in apixaban, rivaroxaban and dabigatran cohorts set against the warfarin cohort. Furthermore, warfarin has pharmacogenetic variations, specifically in the CYP2C9 enzyme, and this is related to the single nucleotide polymorphisms (SNP) (Al-Eitan et al., 2018). The unpredictable response of warfarin among the patients necessitates the implementation of routine international normalised ratio (INR) testing to tackle concerns about bleeding(Bussey et al., 2013). Consequently, tedious clinical visits will interrupt the patient’s quality of life. On the other hand, DOACs have a predictable pharmacokinetic profile and tolerable safety issues. Henceforth, DOACs would be a convenient choice for selected patients. Regardless of the increasing utilisation of DOACs, they are more expensive than warfarin, thus judicious utilisation is the cornerstone in the pharmacotherapy plan for Afib patients. Although this paper is in line with the literature, our findings require careful interpretation to yield a better clinical outcome.
As indicated by Chan YH et al., the effectiveness of using non-vitamin K oral anticoagulants over warfarin in Afib patients with DM includes a lower risk of major adverse cardiovascular events, major adverse limb events, and all major bleeding. Additionally, they reduce major adverse cardiovascular events in Afib patients with DM with a high atherosclerotic risk, including elderly patients, and they reduce the presence of ischaemic heart disease or peripheral artery disease (Chan et al., 2020). Furthermore, a previous study in the US on 11,278 patients reported that warfarin was associated with a higher risk of death, myocardial infarction, and stroke compared to DOACs. In this study, warfarin was consistently connected with a higher risk of developing adverse events compared to DOACs: OR (95% confidence interval) for the composite of mortality, myocardial infarction, and stroke were 1.91 (1.76–2.07) versus apixaban, 1.92 (1.81–2.03) versus dabigatran, 4.09 (3.38–4.37) versus rivaroxaban, and 2.64 (2.53–2.76) versus all DOACs combined (all P < 0.001). Warfarin, compared to all DOACs combined, demonstrated higher rates of all-cause mortality [OR = 2.69 (95% confidence interval, 2.49–2.90)], myocardial infarction [5.30 (4.17–6.74)], stroke [OR = 8.85 (6.61–11.84)], and ischaemic stroke [OR = 12.73 (8.87–18.27); all P < 0.001](von Lueder et al., 2019) . Another observational cohort study on 116,804 oral anticoagulant naïve nonvalvular patients with AF reported that all DOACs were associated with lower risks of ischaemic stroke, intracranial haemorrhage, gastrointestinal bleeding, major bleeding, and composite outcomes. Apixaban and edoxaban showed a lower rate of ischaemic stroke compared to rivaroxaban and dabigatran. Apixaban, dabigatran, and edoxaban had a lower rate of gastrointestinal bleeding and major bleeding compared with rivaroxaban. The composite clinical outcome was not significantly different for apixaban versus edoxaban(Lee et al., 2019) .
As reported by Yamagishi SI, due to the unstable anticoagulant activity of warfarin on matrix Gla protein and osteocalcin, the use of warfarin carries a potentially detrimental risk of vascular calcification and osteoporotic fracture, which both contribute to the reduction in quality of life in patients with DM. Despite the high cost of non-vitamin K oral anticoagulants, they may be superior to warfarin when treating Afib patients with DM (Yamagishi 2019).
A meta-analysis done by Giuseppe et al. concluded that the vascular death rate with non-vitamin K oral anticoagulants was significantly reduced in patients with DM when compared to warfarin (Patti et al., 2017a, Patti et al., 2017b). In contrast, Frappe et al. concluded that in general practice, vitamin K antagonists and DOACs were comparably safe and effective (Frappé et al., 2020).
The efficacy of warfarin has been studied extensively in the literature, and for many years, it was the main OAC that has been used for the prevention and treatment of multiple cardiac diseases, including AF. However, doctors and researchers have expressed their concern about the safety of the use of warfarin in patients with T2DM (Yamagishi 2019). These concerns arise from the fact that warfarin is a problematic medication, with multiple drug interactions(Ament P 2000), increased risk of bleeding(Snipelisky and Kusumoto 2013), and it has a narrow therapeutic window (Teklay et al., 2014). In general, OAC treatment is likely to be indicated for old age patients with DM(Alwafi et al., 2020a, Alwafi et al., 2020b, Alwafi et al., 2020c). Patients with DM are likely to suffer from AF and other comorbidities when they are older (Alwafi et al., 2020a, Alwafi et al., 2020b, Alwafi et al., 2020c) and, therefore, to be at risk of polypharmacy and drug-drug interactions (Mallet et al., 2007). The findings reported in this review can ultimately support and guide health care providers to prescribe the optimal therapy of OACs for patients with T2DM. Doctors and clinical pharmacists must be vigilant when prescribing OACs in patients with DM, especially when warfarin is prescribed, and they must be alert to both immediate and delayed-onset hypoglycaemia and bleeding when prescribing this drug combination. Clinical surveillance, frequent blood glucose measurements, INR monitoring, diet changes and patient education may be necessary to reduce the risk of hypoglycaemia or bleeding if patients are prescribed these medications together (Wolpert, 2007, Snipelisky and Kusumoto, 2013). Similar measures may be applied to patients receiving warfarin and sulfonylureas.
Given that DOACs are currently widely available, they may be an alternative therapeutic when OACs and sulfonylureas are indicated in patients with DM. DOACs have a more predictable pharmacokinetic profile and have fewer drug-drug interactions (Melkonian et al., 2017). However, they are more expensive than warfarin (Melkonian et al., 2017) and, in many cases, warfarin remains the treatment of choice for many patients. In cases where warfarin is still prescribed, other oral hypoglycaemic agents (OHAs), such as metformin, SGLT2 and GLP-1, may be an alternative treatment for other than SU in patients requiring both OACs and OHAs in their management plan, especially given the decline in the use of SUs in general this could be an additional caution for their use.
This review has highlighted several research gaps regarding the efficacy and safety of OACs in patients with diabetes. Future studies to investigate the efficacy and safety of OACs in patients with diabetes with a longer follow-up period and on different populations than the US population are needed. Future studies to explore the drug-drug interaction between DOACs and OHAs are needed. We also recommend future studies be directed at investigating the cost-effectiveness of OACs in patients with diabetes.
This systematic review and meta‐analysis have several strengths. Our findings are derived from observational and RCT studies, which provides us with evidence from both real-life and controlled settings. The included studies had a large sample size, which gave us statistically robust findings. However, there are some limitations. First, we were not able to conduct a meta-analysis because of the clinical and methodological heterogeneity in outcomes between the included studies. In addition, we only included seven studies, although we had an extensive literature search that should have captured all the studies in the literature.
5. Conclusion
In conclusion, this systematic review found that DOACs have better efficacy outcomes compared to warfarin and demonstrate a favourable safety profile with a lower risk of bleeding and minimal drug-drug interaction in patients with diabetes. The only concern facing clinicians is the higher cost of DOACs compared to warfarin.
Authors Contributions
Alwafi and Naser, had full access to all the data in the study and take responsibility for the integrity of the data and the accuracy of the data analysis. Alwafi, and Naser had the original idea for this study. Alwafi, and Naser contributed to the design of the study. Alwafi, Naser and Alotaibi contributed to their literature screening, data extraction and quality assessment of the studies included. Alwafi, Alotaibi, Qadus, Salawati, Dairi, Samannodi and Naser wrote the first draft. All the authors contributed to interpretation and edited the draft report.
Funding
No fund
Data Availability Statement
Data sharing is not applicable to this article as no new data were created or analysed in this study.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Footnotes
Peer review under responsibility of King Saud University.
Supplementary data to this article can be found online at https://doi.org/10.1016/j.jsps.2021.11.001.
Appendix A. Supplementary data
The following are the Supplementary data to this article:
References
- Al-Eitan L.N., Almasri A.Y., Khasawneh R.H. Impact of CYP2C9 and VKORC1 Polymorphisms on Warfarin Sensitivity and Responsiveness in Jordanian Cardiovascular Patients during the Initiation Therapy. Genes (Basel). 2018;9:578. doi: 10.3390/genes9120578. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Alwafi H., Alsharif A.A., Wei L.i., Langan D., Naser A.Y., Mongkhon P., Bell J.S., Ilomaki J., Al Metwazi M.S., Man K.K.C., Fang G., Wong I.C.K. Incidence and prevalence of hypoglycaemia in type 1 and type 2 diabetes individuals: A systematic review and meta-analysis. Diabetes Research and Clinical Practice. 2020;170:108522. doi: 10.1016/j.diabres.2020.108522. [DOI] [PubMed] [Google Scholar]
- Alwafi H., Wei L.i., Naser A.Y., Mongkhon P., Tse G., Man K.K.C., Bell J.S., Ilomaki J., Fang G., Wong I.C.K. Trends in oral anticoagulant prescribing in individuals with type 2 diabetes mellitus: a population-based study in the UK. BMJ Open. 2020;10(5):e034573. doi: 10.1136/bmjopen-2019-034573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Alwafi H., Wong I.C.K., Banerjee A., Mongkhon P., Whittlesea C., Naser A.Y., Lau W.C.Y., Wei L.i. Epidemiology and treatment of atrial fibrillation in patients with type 2 diabetes in the UK, 2001–2016. Scientific Reports. 2020;10(1) doi: 10.1038/s41598-020-69492-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ament P, B. J., Liszewski J. , 2000. Clinically Significant Drug Interactions. American Family Physician. 15, 1745-1754. [PubMed]
- Baker W.L., Beyer‐Westendorf J., Bunz T.J., Eriksson D., Meinecke A., Sood N.A., Coleman C.I. Effectiveness and safety of rivaroxaban and warfarin for prevention of major adverse cardiovascular or limb events in patients with non-valvular atrial fibrillation and type 2 diabetes. Diabetes, Obesity and Metabolism. 2019;21(9):2107–2114. doi: 10.1111/dom.13787. [DOI] [PubMed] [Google Scholar]
- Bansilal S., Bloomgarden Z., Halperin J.L., Hellkamp A.S., Lokhnygina Y., Patel M.R., Becker R.C., Breithardt Günter, Hacke W., Hankey G.J., Nessel C.C., Singer D.E., Berkowitz S.D., Piccini J.P., Mahaffey K.W., Fox K.A.A. Efficacy and safety of rivaroxaban in patients with diabetes and nonvalvular atrial fibrillation: the Rivaroxaban Once-daily, Oral, Direct Factor Xa Inhibition Compared with Vitamin K Antagonism for Prevention of Stroke and Embolism Trial in Atrial Fibrillation (ROCKET AF Trial) Am Heart J. 2015;170(4):675–682.e8. doi: 10.1016/j.ahj.2015.07.006. [DOI] [PubMed] [Google Scholar]
- Bell E.J., Selvin E., Lutsey P.L., Nambi V., Cushman M., Folsom A.R. Glycemia (hemoglobin A1c) and incident venous thromboembolism in the Atherosclerosis Risk in Communities cohort study. Vasc Med. 2013;18(5):245–250. doi: 10.1177/1358863X13506764. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Brambatti M., Darius H., Oldgren J., Clemens A., Noack H.H., Brueckmann M., Yusuf S., Wallentin L., Ezekowitz M.D., Connolly S.J., Healey J.S. Comparison of dabigatran versus warfarin in diabetic patients with atrial fibrillation: Results from the RE-LY trial. International journal of cardiology. 2015;196:127–131. doi: 10.1016/j.ijcard.2015.05.141. [DOI] [PubMed] [Google Scholar]
- Bussey H.I., Bussey M., Bussey-Smith K.L., Frei C.R. Evaluation of warfarin management with international normalized ratio self-testing and online remote monitoring and management plus low-dose vitamin k with genomic considerations: a pilot study. Pharmacotherapy. 2013;33(11):1136–1146. doi: 10.1002/phar.2013.33.issue-1110.1002/phar.1343. [DOI] [PubMed] [Google Scholar]
- Camm, A., G. Lip and R. e. a. De Caterina, 2012. 2012 focused update of the ESC Guidelines for the management of atrial fibrillation: an update of the 2010 ESC Guidelines for the management of atrial fibrillation. Developed with the special contribution of the European Heart Rhythm Association. Eur Heart J. 33, 2719 - 2747. [DOI] [PubMed]
- Chan Y.-H., Lee H.-F., Li P.-R., Liu J.-R., Chao T.-F., Wu L.-S., Chang S.-H., Yeh Y.-H., Kuo C.-T., See L.-C., Lip G.Y.H. Effectiveness, safety, and major adverse limb events in atrial fibrillation patients with concomitant diabetes mellitus treated with non-vitamin K antagonist oral anticoagulants. Cardiovascular Diabetology. 2020;19(1) doi: 10.1186/s12933-020-01043-2. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Dublin S., Glazer N.L., Smith N.L., Psaty B.M., Lumley T., Wiggins K.L., Page R.L., Heckbert S.R. Diabetes Mellitus, Glycemic Control, and Risk of Atrial Fibrillation. Journal of General Internal Medicine. 2010;25(8):853–858. doi: 10.1007/s11606-010-1340-y. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ezekowitz J.A., Lewis B.S., Lopes R.D., Wojdyla D.M., McMurray J.J.V., Hanna M., Atar D., Cecilia Bahit M., Keltai M., Lopez-Sendon J.L., Pais P., Ruzyllo W., Wallentin L., Granger C.B., Alexander J.H. Clinical outcomes of patients with diabetes and atrial fibrillation treated with apixaban: results from the ARISTOTLE trial. European heart journal. Cardiovascular pharmacotherapy. 2015;1(2):86–94. doi: 10.1093/ehjcvp/pvu024. [DOI] [PubMed] [Google Scholar]
- Frappé P., Cogneau J., Gaboreau Y., Abenhaïm N., Bayen M., Guichard C., Jacquet J.-P., Lacoin F., Liébart S., Bertoletti L., Bosson J.-L. Anticoagulants' Safety and Effectiveness in General Practice: A Nationwide Prospective Cohort Study. Ann Fam Med. 2020;18(2):131–138. doi: 10.1370/afm.2495. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Giugliano, R., C. Ruff and E. e. a. Braunwald, 2013. Antman EM; ENGAGE AFTIMI 48 Investigators. Edoxaban versus warfarin in patients with atrial fibrillation. . N Engl J Med. 369, 2093 - 2104. [DOI] [PubMed]
- Patti G., Di Gioia G., Cavallari I., et al. Safety and efficacy of nonvitamin K antagonist oral anticoagulants versus warfarin in diabetic patients with atrial fibrillation: A study-level meta-analysis of phase III randomized trials. Diabetes Metab Res Rev. 2017;33:1–8. doi: 10.1002/dmrr.2876. [DOI] [PubMed] [Google Scholar]
- group., S. r. i. a. f. w., 2007. Independent predictors of stroke in patients with atrial fibrillation: a systematic review. . Neurology. 69, 546 - 554. [DOI] [PubMed]
- Hart RG, P. L., Halperin JL, et al. , 2008. Comparison of 12 risk stratification schemes to predict stroke in patients with nonvalvular atrial fibrillation. Stroke. 39, 1901- 1910. [DOI] [PubMed]
- Herzog R., Álvarez-Pasquin M.J., Díaz C., et al. Are healthcare workers’ intentions to vaccinate related to their knowledge, beliefs and attitudes? a systematic review. BMC Public Health. 2013;13:154. doi: 10.1186/1471-2458-13-154. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Higgins J.P., Green S. Assessing risk of bias in included studies; The Cochrane Collaboration: 2011. Cochrane Handbook for Systematic Reviews of Interventions. [Google Scholar]
- Huxley R.R., Filion K.B., Konety S., et al. Meta-analysis of cohort and case-control studies of type 2 diabetes mellitus and risk of atrial fibrillation. Am J Cardiol. 2011;108:56–62. doi: 10.1016/j.amjcard.2011.03.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Huxley R.R., Lopez F.L., Folsom A.R., et al. Absolute and attributable risks of atrial fibrillation in relation to optimal and borderline risk factors: the Atherosclerosis Risk in Communities (ARIC) study. Circulation. 2011;123:1501–1508. doi: 10.1161/CIRCULATIONAHA.110.009035. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Kannel W., Mc Gee D. Diabetes and Cardiovascular Disease: The Framingham Study. JAMA. 1979;241:2035–2038. doi: 10.1001/jama.241.19.2035. [DOI] [PubMed] [Google Scholar]
- Lee S.R., Choi E.K., Kwon S., et al. Effectiveness and Safety of Contemporary Oral Anticoagulants Among Asians With Nonvalvular Atrial Fibrillation. Stroke. 2019;50:2245–2249. doi: 10.1161/strokeaha.119.025536. [DOI] [PubMed] [Google Scholar]
- Lip GY, N. R., Pisters R, Lane DA, Crijns HJ. , 2010. Refining clinical risk stratification for predicting stroke and thromboembolism in atrial fibrillation using a novel risk factor‐based approach: the euro heart survey on atrial fibrillation. Chest. 137, 263 - 272. [DOI] [PubMed]
- Lip G.Y.H., Keshishian A.V., Kang A.L., et al. Effectiveness and Safety of Oral Anticoagulants in Patients With Nonvalvular Atrial Fibrillation and Diabetes Mellitus. Mayo Clin Proc. 2020;95:929–943. doi: 10.1016/j.mayocp.2019.05.032. [DOI] [PubMed] [Google Scholar]
- Mallet L., Spinewine A., Huang A. The challenge of managing drug interactions in elderly people. Lancet. 2007;370:185–191. doi: 10.1016/s0140-6736(07)61092-7. [DOI] [PubMed] [Google Scholar]
- Melkonian M., Jarzebowski W., Pautas E., et al. Bleeding risk of antiplatelet drugs compared with oral anticoagulants in older patients with atrial fibrillation: a systematic review and meta-analysis. Journal of thrombosis and haemostasis : JTH. 2017;15:1500–1510. doi: 10.1111/jth.13697. [DOI] [PubMed] [Google Scholar]
- Moher D., Liberati A., Tetzlaff J., et al. Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLOS Medicine. 2009;6 doi: 10.1371/journal.pmed.1000097. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Movahed M.R., Hashemzadeh M., Jamal M.M. Diabetes mellitus is a strong, independent risk for atrial fibrillation and flutter in addition to other cardiovascular disease. International journal of cardiology. 2005;105:315–318. doi: 10.1016/j.ijcard.2005.02.050. [DOI] [PubMed] [Google Scholar]
- Murphy N.F., Simpson C.R., Jhund P.S., et al. A national survey of the prevalence, incidence, primary care burden and treatment of atrial fibrillation in Scotland. Heart (British Cardiac Society). 2007;93:606–612. doi: 10.1136/hrt.2006.107573. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nam Y.H., Brensinger C.M., Bilker W.B., et al. Serious Hypoglycemia and Use of Warfarin in Combination With Sulfonylureas or Metformin. Clinical Pharmacology and Therapeutics. 2019;105:210–218. doi: 10.1002/cpt.1146. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Nam Y.H., Brensinger C.M., Bilker W.B., Leonard C.E., Han X., Hennessy S. Serious Hypoglycemia and Use of Warfarin in Combination With Sulfonylureas or Metformin. 2019;105(1):210–218. doi: 10.1002/cpt.1146. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Naser A.Y., Alwafi H., Alsairafi Z. Cost of hospitalisation and length of stay due to hypoglycaemia in patients with diabetes mellitus: a cross-sectional study. Pharmacy practice. 2020;18:1847. doi: 10.18549/PharmPract.2020.2.1847. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Naser A.Y., Wong I.C.K., Whittlesea C., et al. Use of multiple antidiabetic medications in patients with diabetes and its association with hypoglycaemic events: a case-crossover study in Jordan. BMJ Open. 2018;8 doi: 10.1136/bmjopen-2018-024909. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Park J.Y.E., Howren A.M., Zusman E.Z., et al. The incidence of depression and anxiety in patients with ankylosing spondylitis: a systematic review and meta-analysis. BMC Rheumatology. 2020;4:12. doi: 10.1186/s41927-019-0111-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Patti G., Di Gioia G., Cavallari I., et al. Safety and efficacy of nonvitamin K antagonist oral anticoagulants versus warfarin in diabetic patients with atrial fibrillation: A study-level meta-analysis of phase III randomized trials. Diabetes Metab Res Rev. 2017;33 doi: 10.1002/dmrr.2876. [DOI] [PubMed] [Google Scholar]
- Romley J.A., Gong C., Jena A.B., et al. Association between use of warfarin with common sulfonylureas and serious hypoglycemic events: retrospective cohort analysis. Bmj. 2015;351 doi: 10.1136/bmj.h6223. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Ruff, C., R. Giugliano and E. e. a. Braunwald, 2014. Comparison of the efficacy and safety of new oral anticoagulants with warfarin in patients with atrial fibrillation: a meta‐analysis of randomised trials. . Lancet. 383, 955 - 962. [DOI] [PubMed]
- Snipelisky D., Kusumoto F. Current strategies to minimize the bleeding risk of warfarin. J Blood Med. 2013;4:89–99. doi: 10.2147/JBM.S41404. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Stroup D.F., Berlin J.A., Morton S.C., et al. Meta-analysis of Observational Studies in EpidemiologyA Proposal for Reporting. JAMA. 2000;283:2008–2012. doi: 10.1001/jama.283.15.2008. [DOI] [PubMed] [Google Scholar]
- Teklay G., Shiferaw N., Legesse B., et al. Drug-drug interactions and risk of bleeding among inpatients on warfarin therapy: a prospective observational study. Thrombosis Journal. 2014;12:20. doi: 10.1186/1477-9560-12-20. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Triplitt C. Drug Interactions of Medications Commonly Used in Diabetes. Diabetes Spectrum. 2006;19:202–211. doi: 10.2337/diaspect.19.4.202. [DOI] [Google Scholar]
- Vinogradova Y., Coupland C., Hill T., et al. Risks and benefits of direct oral anticoagulants versus warfarin in a real world setting: cohort study in primary care. 2018;362 doi: 10.1136/bmj.k2505. [DOI] [PMC free article] [PubMed] [Google Scholar]
- von Lueder T.G., Atar D., Agewall S., et al. All-Cause Mortality and Cardiovascular Outcomes With Non-Vitamin K Oral Anticoagulants Versus Warfarin in Patients With Heart Failure in the Food and Drug Administration Adverse Event Reporting System. Am J Ther. 2019;26:e671–e678. doi: 10.1097/mjt.0000000000000883. [DOI] [PubMed] [Google Scholar]
- Wells, G., B. Shea, D. O'Connell, et al., 2000. The Newcastle–Ottawa Scale (NOS) for Assessing the Quality of Non-Randomized Studies in Meta-Analysis.
- Wolf P., Abbott R., Kannel W. Atrial fibrillation as an independent risk factor for stroke: the Framingham Study. Stroke. 1991:983–988. doi: 10.1161/01.str.22.8.983. [DOI] [PubMed] [Google Scholar]
- Wolpert H.A. Use of continuous glucose monitoring in the detection and prevention of hypoglycemia. J Diabetes Sci Technol. 2007;1:146–150. doi: 10.1177/193229680700100126. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Xian Y., Xu H., O’Brien E.C., et al. Clinical Effectiveness of Direct Oral Anticoagulants vs Warfarin in Older Patients With Atrial Fibrillation and Ischemic Stroke: Findings From the Patient-Centered Research Into Outcomes Stroke Patients Prefer and Effectiveness Research (PROSPER) Study. JAMA Neurology. 2019;76:1192–1202. doi: 10.1001/jamaneurol.2019.2099. [DOI] [PMC free article] [PubMed] [Google Scholar]
- Yamagishi S.-I. Concerns about clinical efficacy and safety of warfarin in diabetic patients with atrial fibrillation. Cardiovascular Diabetology. 2019;18:12. doi: 10.1186/s12933-019-0818-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.