Abstract
Introduction
Multiple operative modalities are available for management of unstable intertrochanteric femoral fractures. This meta-analysis was conducted to find out if there is superiority of surgical fixation by proximal femoral plate or surgical fixation by intramedullary nail over hip arthroplasty for management of unstable intertrochanteric femoral fractures in the elderly.
Methods
A search for relevant studies that published from January 2000 to November 2018 through the electronic literature database of Cochrane library, Medline, Trip Database and Wiley online library.
Results
A total of 19 studies including 14 prospective RCTs, and five retrospective studies. This meta-analysis showed that nail group had shorter operative time than plate group (P < 0.0001), and less blood loss than the plate and arthroplasty groups (P < 0.0001), cut-out was higher in nail group than the plate group (P < 0.0001), mortality rate was higher in hip arthroplasty compared to other groups (P < 0.0001), Harris hip score within 6 months of the operation was higher in the arthroplasty group compared with the nail and plate groups, while within 1 year of the operation, nail group had higher Harris hip score than arthroplasty group (P < 0.0001).
Conclusions
This meta-analysis suggested that the intramedullary nail fixation method is a preferred method for management of unstable intertrochanteric femoral fractures in the elderly over hip arthroplasty and proximal femoral plate fixation.
Supplementary Information
The online version contains supplementary material available at 10.1007/s43465-021-00426-1.
Keywords: Intertrochanteric, Extracapsular hip fractures, Intramedullary fixation, Proximal femoral plate, Hip arthroplasty
Introduction
The average lifespan worldwide is increasing, which results in growth of the elderly population and subsequently increase in the incidence of osteoporotic hip fractures. The worldwide incidence of hip fracture was 1.6 million in the year 2000; and the number is expected to reach 6 million in the year 2050 [1, 2]. Intertrochanteric femoral fractures comprise nearly 45% of all hip fractures and out of these, 50–60% are classified as unstable. Multiple operative modalities are available for management of unstable intertrochanteric femoral fractures. However, there is no clear evidence from clinical research to indicate if hip arthroplasty is more superior to surgical fixation and vice versa [1–5]. Therefore, this meta-analysis was performed to find out if there is superiority of surgical fixation by proximal femoral plate or surgical fixation by intramedullary nail over hip arthroplasty and vice versa by comparing the advantages and disadvantages of the devices including patient's morbidity and mortality.
Materials and Methods
Search Strategy
A search for relevant studies that published from January 2000 to November 2018 through the electronic literature database of Cochrane library, Medline, Trip Database, Wiley online library using the following keywords: Intertrochanteric OR Pertrochanteric OR trochanteric, extracapsular hip fractures OR intramedullary fixation OR Proximal femoral plate OR cephalomedullary nail OR hip arthroplasty OR endoprosthesis; Comprehensive meta-analysis program software was used for our meta-analysis.
Inclusion and Exclusion Criteria
We identified literature that met the following inclusion criteria: (1) patients older than 60 years, (2) unstable intertrochanteric femoral fracture, (3) the articles restricted to English language, (4) studies that were designed as interventional studies (Randomized clinical trials or non-randomized clinical trials), and (5) each study has to include at least 20 cases either managed by surgical fixation or hip arthroplasty and a mean follow-up period of 2 years minimum.
While, the exclusion criteria were: (1) stable intertrochanteric femoral fracture, (2) patients had a metastasis or myeloma, infection, or congenital deformity, (3) patients with neurological diseases as Cerebral palsy, Parkinson's disease, etc. (4) type of literature as a “review” and “talk,” “letters,” “commentary,” and “case report”; cadaver or model studies., and (5) data duplicated or overlapped.
Selection of Literature
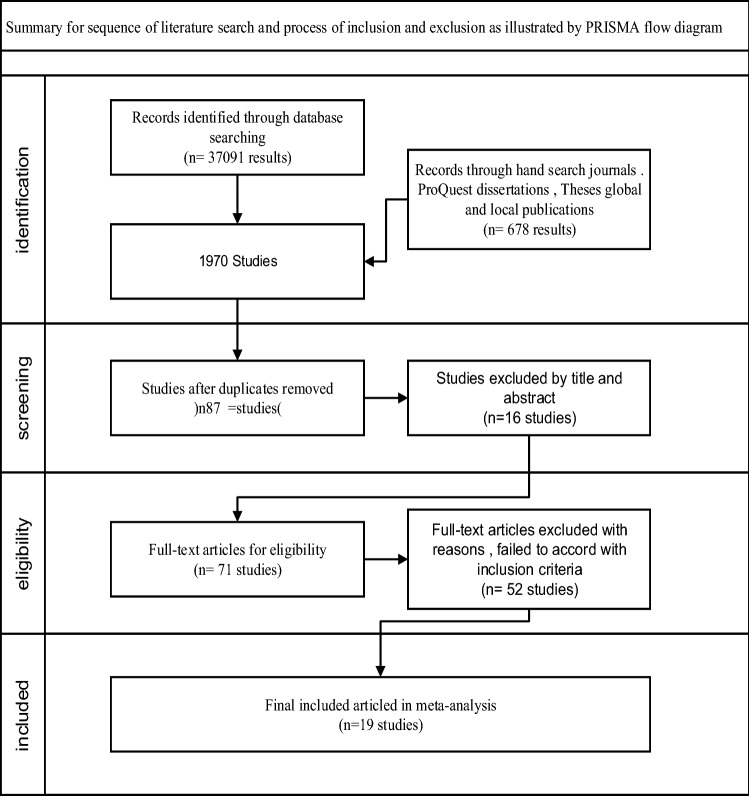
The PRISMA flow diagram was used to select the included studies. All the titles and abstracts of the relevant studies were first categorized, and then the full-text articles that met the eligibility criteria were read and selected for inclusion (Fig. 1).
Fig. 1.
Preferred reporting items for systematic reviews and meta-analyses (PRISMA) flow diagram of study selection
Quality Assessment of Included Studies
The Cochrane tool was used to assess the following items: randomization, allocation concealment, blinding of participants, blinding of outcome assessment, incomplete outcome data, selective outcome reporting and other bias, for each individual item, while assessment of the included non-RCTs was done according to the Newcastle–Ottawa scale (Tables 1, 2).
Table 1.
Risk of bias assessment of the RCTs
| Study | Randomization | Allocation concealment | Blinding of participants | Incomplete outcome data | Selective outcome reporting |
|---|---|---|---|---|---|
| Boldin [6] | Low risk | Low risk | Low risk | Unclear risk | Low risk |
| Miedel [7] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Grimsrud [8] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Bonnevialle [9] | High risk | Low risk | Low risk | Low risk | Low risk |
| Richard Borger [10] | Low risk | Low risk | Low risk | Low risk | Unclear risk |
| LeeYoung-Kyun [11] | Low risk | Low risk | Low risk | Unclear risk | high risk |
| Zha [12] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Tao [13] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Guo [14] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Nishikant [15] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Özkayın [16] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Keizo Wada [17] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Malkesh [18] | Low risk | Low risk | Low risk | Low risk | Low risk |
| Jolly [19] | Low risk | Low risk | Low risk | Low risk | Low risk |
Table 2.
Risk of bias was assessed with use of the Newcastle–Ottawa Scale
| Study | Exposed cohort | Non exposed cohort | Ascertainment of exposure | Outcome of interest | Comparability | Assessment of outcome | Length of follow-up | Adequacy of follow-up | Total score |
|---|---|---|---|---|---|---|---|---|---|
| Herman [20] | * | * | * | * | – | * | * | * | 7 |
| Ming Hui Li Lei [21] | * | * | * | * | – | * | * | * | 7 |
| Zhenhai [22] | * | * | * | * | * | * | * | * | 8 |
| Temiz A [23] | * | * | * | * | * | * | * | * | 8 |
| Güven M [24] | * | * | * | * | – | * | * | * | 7 |
“*”Means a score of 1; “**”means a score of 2; the total score of this scale is 9
A higher overall, score corresponds to a lower risk of bias; a total score of 5 or less indicates a high risk of bias
Statistical Analysis
Weighted mean differences (WMDs) or odds ratios (ORs) corresponding 95% confidence interval (CI) were estimated and pooled across studies to assess the discrepancy between different methods with a value of P < 0.05 as statistically significant. Heterogeneity was assessed using the I2 value and Chi-square test, a random effect model was used.
Results
Included Studies
A total of 1970 potentially relevant articles were identified from the databases.
At first, 87 studies were included, 16 of them are excluded due to duplication, Following closer examination of the remaining 71 studies through reading the full text of each and risk of bias assessment process, further 52 studies are excluded with reasons as they did not fulfill the study's inclusion criteria (Fig. 1).
Clinical Outcomes
According to: there have been many parameters we have worked in the study as mentioned below: Type of intervention, Operative time, Blood loss, Blood transfusion, Hospital stay, Implant related complication, Reoperation, Mortality assessment and Harris hip score.
Type of Intervention
A total of 1764 patients from 19 studies were included.
The majority was managed by intramedullary nail (954 cases) followed by proximal femoral plate (407 cases) and hip arthroplasty (403 cases) for unstable intertrochanteric hip fractures, respectively. This means that up to 54% of cases were managed by intramedullary nails, while about 46% distributed nearly equally between proximal femoral plate and hip arthroplasty.
According to Operative Time
In studies comparing different types of intervention, we found that cases managed by nail shows less operative time than plate [7, 13, 14, 21] (Chi2 = 2.310, P < 0.0001, I2 = 94.674, Supplementary Fig. 2), while systematic reviews of Individual studies [8, 11, 12, 15, 18, 21, 23] found cases managed by nail showed less operative time than plate and hip arthroplasty, respectively.
According to Intraoperative Blood Loss
There was a significant difference in results of meta-analysis according to blood loss between individual studies that managed by either: the plate or the nail group [7, 13, 14, 22], (Supplementary Fig. 3), while it was found that cases managed by intramedullary nail group showed less blood loss than both plate and hip arthroplasty groups with a significant difference (P < 0.0001, I2 = 99.493).
According to Blood Transfusion
Meta-analysis of studies according to blood transfusion could not be assessed because of the smaller-sized results of the studies [7, 9], while systematic review of individual studies that were managed by either: plate, nail or hip arthroplasty according to blood transfusion showed insignificant difference.
According to Hospital Stay
The pooled results indicated that there was insignificant difference in duration of hospital stay between the plate and nail group [13, 14] (Chi2 = 0.335, P = 0.063, I2 = 71.026, Supplementary Fig. 4), and there was insignificant difference in results of meta-analysis according to hospital stay between individual studies that are managed by either: plate or nails [18, 23], (Chi2 = 9.961, P = 0.060, I2 = 97.034).
According to Implant-Related Complications
-
A.
Superficial infection
Meta-analysis of studies found that there was insignificant difference in superficial infection between the plate and nail groups [7, 14] (Chi2 = 0.000, P = 0.976, I2 = 0.000, Supplementary Fig. 5), while meta-analysis of studies found that there was significant difference in superficial infection between the nail and hip arthroplasty groups [16] (P < 0.0001, I2 = 31.138, Supplementary Fig. 6) and systematic review of individual studies found that cases managed by hip arthroplasty had more superficial infection than cases managed by the plate and nail groups [6, 8, 10–12, 15, 17, 18, 20, 21, 23].
-
B.
Deep infection
Meta-analysis of study [16] studies that were managed by nail versus hip arthroplasty according to deep infection showed insignificant difference, (Supplementary Fig. 7), while systematic reviews of studies [6, 8, 15–18, 20, 21] according to deep infection in cases with unstable intertrochanteric femoral fracture in the elderly either managed by plate, nail or hip arthroplasty showed insignificant difference.
-
C.
Cut-out complication
The pooled results showed higher cut-out complication in cases managed by nail than cases managed by plate with significant difference [6, 10–12, 15, 18, 20, 21, 23] according to cut-out complication: (Chi2 = 2.649, P < 0.0001, I2 = 86.881, Supplementary Fig. 8).
-
D.
Implant failure
Meta-analysis of studies and also systematic reviews of individual studies [6, 8, 10–12, 15, 17, 18, 20, 21, 23] according to implant failure in cases either managed by either plate, nail or hip arthroplasty showed insignificant difference (P = 0.015, I2 = 57.901).
-
E.
Deep venous thrombosis
Meta-analysis of studies and also systematic reviews of individual studies [6, 8, 10–12, 15, 17, 18, 20, 21, 23] according to DVT in cases with unstable intertrochanteric femoral fracture in the elderly either plate, nail or hip arthroplasty showed insignificant difference (Supplementary Figs. 9 and 10).
According to the Need for Re-operation
Meta-analysis of studies [7] indicated that there was insignificant difference in the need for re-operation between plate versus nail (Chi2 = 0.000, P = 0.555, I2 = 0.000, Supplementary Fig. 11).While systematic reviews of individual studies [6, 8, 10–12, 15, 17, 23] showed that the need for re-operation was higher in the plate and nail groups than the hip arthroplasty group.
According to Mortality Assessment
Meta-analysis of study [7] indicated that there was insignificant difference in mortality assessment between different groups: (Chi2 = 0.152, P = 0.056, I2 = 56.577 Supplementary Fig. 12). While, systematic reviews [6–8, 17] showed high mortality rate in cases underwent hip arthroplasty within 1 year compared to other groups.
According to Harris Hip Score for Follow-up
The pooled results indicated that there was insignificant difference in HHS for follow-up between cases managed by plate group versus the nail group [13, 14, 16] (Chi2 = 0.000, P = 0.668, I2 = 0.000, Supplementary Fig. 13), while systematic review of individual studies [18, 21, 23] results 6 months postoperatively showed that the HHS was higher in the hip arthroplasty group in comparison with the nail and the plate groups, while 1 year postoperative, it was found that nail group had significantly higher HHS compared with the hip arthroplasty group.
Discussion
This meta-analysis was conducted to find out if there is superiority of surgical fixation by proximal femoral plate or by intramedullary nail over hip arthroplasty for management of unstable intertrochanteric femoral fractures in the elderly from the current literature to provide guidance on the appropriate clinical choice to accommodate individual patients. In this meta-analysis, it was found that intramedullary fixation could achieve significantly shorter operative time, less intraoperative blood loss, also higher post-operative functional hip scores which achieve the long-term operative purposes including restoring the limb functions and early mobilization, and decreasing the re-operation rate in comparison with proximal femoral plate and hip arthroplasty for management of unstable intertrochanteric femoral fractures in the elderly. Wu-Bin Shu et al. [25]concluded that GN has the least total incidence of complications for treating unstable intertrochanteric fractures among the four interventions.
These results were almost consistent with our meta-analysis results. Most of our included studies in this meta-analysis were RCTs (fourteen RCTS with 1217 participants), which, therefore, overcomes the shortcomings of recall or selection bias in non-randomized studies. The methodological quality of included retrospective studies was high; (a total of two studies scored 8 stars, while three studies scored 7 stars) according to the NOS.
However, there was heterogeneity in this meta-analysis results which can be explained by different implant devices of internal medullary nails, surgeon expertise, surgical technique and post-operative rehabilitation.
So after evaluation of all data and reviewing previous systematic reviews that compared different intramedullary nail fixation, proximal femoral plate and hip arthroplasty with exclusion of stable intertrochanteric fractures, we can recommend intramedullary nail fixation for the treatment of unstable femoral intertrochanteric fractures in the elderly, with some modifications and precautions according to type of fracture, quality of bone and the associated medical conditions.
There were several strengths in this network meta-analysis:
The meta-analysis has included prospective randomized clinical trials with large sample size which increases the statistical power.
A random effect model was used to avoid heterogeneous results.
We compared treatment strategies indirectly, when no head-to-head trial existed, more precise efficacy estimates were based on direct and indirect comparisons with various interventions.
The use of the 95% confidence intervals of inconsistency factor values reached zero, demonstrating no substantial inconsistency.
But, undoubtedly, this study had some limitations:
Some of our included articles have not always reported some items which were needed for comparison between different types of interventions or they are reported in various ways (e.g., number and percentage, mean, median and SD, etc.)
The qualities of the studies were quite variable. Some studies were of unclear bias as to randomization sequence generation; some had weak blinding, or imperfect allocation concealment; therefore, selection bias or confounding factors might be present, influencing our results.
Some factors that may affect the post-operative functional outcome were not reported as post-operative physiotherapy and rehabilitation.
Summary and Conclusion
Intertrochanteric femoral fracture is a devastating skeletal injury which is common in elderly osteoporotic patients and it greatly affects the patient lifestyle, physical and psychological conditions. Proximal femoral plate, intramedullary nail and hip arthroplasty are all used for the management of unstable intertrochanteric femoral fractures in the elderly.
In this study, it was concluded that the intramedullary nail fixation is a preferred method for management of unstable intertrochanteric femoral fractures in the elderly over hip arthroplasty and proximal femoral plate fixation as it has shorter operative time and less blood loss, Also, the intramedullary nail fixation shows higher post-operative functional hip scores which achieves the long-term operative purposes include restoring the limb functions and early mobilization and decreasing the re-operation rate.
According to the adverse effects, this study showed that hip arthroplasty group has a higher mortality rate, more blood loss, more superficial infection and longer operation time than the intramedullary nail and proximal femoral plate, while the need for re-operation was higher in proximal femoral plate and intramedullary nail than the hip arthroplasty group.
Supplementary Information
Below is the link to the electronic supplementary material.
Acknowledgements
We would like to thank Prof. Dr. Ibrahim ali Kabbash (Professor of Public Health & Community Medicine—Faculty of Medicine) for providing the statistical analysis for this study.
Authors’ contributions
It has been a teamwork; each one has his specific role: MSEW (Orthopedic surgery resident—Faculty of Medicine, Tanta University, Egypt) and Assist. Prof. Dr. MAER (Assistant Professor of orthopedic surgery—Faculty of Medicine, Tanta University, Egypt) were responsible for data collection for the study including reading full-text articles and exclusion of articles that did not met the inclusion criteria. Assist. Prof. Dr. AMS (Assistant Professor of orthopedic surgery—Faculty of Medicine, Tanta University, Egypt) was responsible for data extraction and writing the original draft. Prof. Dr. LMAEY ( Professor of orthopedic surgery—Faculty of Medicine, Tanta University, Egypt), was responsible for research activity planning and execution in addition to writing review and editing. Prof. Dr. IK (Professor of Public Health & Community Medicine—Faculty of Medicine, Tanta University, Egypt) was responsible for providing the statistical analysis for this study.
Funding
No funding was received.
Availability of Data and Materials
Electronic search was search was done, so data are available.
Declarations
Conflict of Interest
The authors had no conflicts of interest to declare in relation to this article.
Ethical Approval
This article does not contain any studies with human participants performed by any of the authors; thus, no ethical approval is required.
Ethical Standard Statement
This article does not contain any studies with human or animal subjects performed by the any of the authors.
Consent to Publish
Formal written consent to publish before publication of the work has been provided.
Informed Consent
For this type of study, informed consent is not required.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Contributor Information
Mohamed Shawky El Madboh, Email: shawkyelmadboh92@gmail.com.
Lotfy Mohamed Abd ElKader Yonis, Email: lotfyyonis@yahoo.com.
Ibrahim ali Kabbash, Email: Ibrahim.kabbash@med.tanta.edu.eg.
Ahmed Mohamed Samy, Email: dr.ahmedsamy@yahoo.com.
Mohamed Abd Elhamed Romeih, Email: romeih@med.tanta.edu.eg.
References
- 1.Court-Brown CM, Caesar B. Epidemiology of adult fractures: A review. Injury. 2006;37:691–700. doi: 10.1016/j.injury.2006.04.130. [DOI] [PubMed] [Google Scholar]
- 2.Teague DC, Ertl WJ, Hickerson L, et al. What’s new in orthopaedic trauma. The Journal of Bone and Joint Surgery. 2016;98:1142–1149. doi: 10.2106/JBJS.16.00378. [DOI] [Google Scholar]
- 3.Grisso JA, Kelsey JL, Strom BL, Chiu GY, Maislin G, O’Brien LA, Hoffman S, Kaplan F. Risk factors for falls as a cause of hip fracture in women. The Northeast Hip Fracture Study Group. New England Journal of Medicine. 1991;324:1326–1331. doi: 10.1056/NEJM199105093241905. [DOI] [PubMed] [Google Scholar]
- 4.Bonnaire F, Lein T, Bula P. Trochanteric femoral fractures: Anatomy, biomechanics and choice of implants. Der Unfallchirurg. 2011;114:491–500. doi: 10.1007/s00113-011-1973-2. [DOI] [PubMed] [Google Scholar]
- 5.Sambandam SN, Chandrasekharan J, Mounasamy V, et al. Intertrochanteric fractures: A review of fixation methods. European Journal of Orthopaedic Surgery and Traumatology. 2016;26:339–353. doi: 10.1007/s00590-016-1757-z. [DOI] [PubMed] [Google Scholar]
- 6.Boldin C, Seibert FJ, Fankhauser F, Peicha G, Grechenig W, Szyszkowitz R. The proximal femoral nail (PFN)–a minimal invasive treatment of unstable proximal femoral fractures: A prospective study of 55 patients with a follow-up of 15 months. Acta Orthopaedica Scandinavica. 2003;74(1):53–58. doi: 10.1080/00016470310013662. [DOI] [PubMed] [Google Scholar]
- 7.Miedel R, Ponzer S, Törnkvist H, Söderqvist A, Tidermark J. The standard Gamma nail or the Medoff sliding plate for unstable trochanteric and subtrochanteric fractures. A randomised, controlled trial. The Journal of Bone and Joint Surgery. 2005;87(1):68–75. doi: 10.1302/0301-620X.87B1.15295. [DOI] [PubMed] [Google Scholar]
- 8.Grimsrud C, Monzon RJ, Richman J, Ries MD. Cemented Hip arthroplasty with a novel cerclage cable technique for unstable intertrochanteric hip fractures. Journal of Arthroplasty. 2005;20(3):337–344. doi: 10.1016/j.arth.2004.04.017. [DOI] [PubMed] [Google Scholar]
- 9.Bonnevialle P, Saragaglia D, Ehlinger M, Tonetti J, Maisse N, Adam P, Le Gall C, French Hip and Knee Society (SFHG); Trauma Surgery Academy (GETRAUM) Trochanteric locking nail versus arthroplasty in unstable intertrochanteric fracture in patients aged over 75 years. Orthopaedics and Traumatology: Surgery and Research. 2011;97(6):S95–100. doi: 10.1016/j.otsr.2011.06.009. [DOI] [PubMed] [Google Scholar]
- 10.Borger RA, Borger FA, Pires de Araújo R, Pereira TF, Queiroz RD. prospective assessment of the clinical, radiographic and functional evolution of treatment for unstable trochanteric fractures of the femur using a cephalomedullary nail. Revista Brasileira de Ortopedia. 2011;46(4):380–389. doi: 10.1016/S2255-4971(15)30249-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Lee YK, Ha YC, Chang BK, Kim KC, Kim TY, Koo KH. Cementless bipolar hemiarthroplasty using a hydroxyapatite-coated long stem for osteoporotic unstable intertrochanteric fractures. Journal of Arthroplasty. 2011;26(4):626–632. doi: 10.1016/j.arth.2010.05.010. [DOI] [PubMed] [Google Scholar]
- 12.Zha GC, Chen ZL, Qi XB, Sun JY. Treatment of pertrochanteric fractures with a proximal femur locking compression plate. Injury. 2011;42(11):1294–1299. doi: 10.1016/j.injury.2011.01.030. [DOI] [PubMed] [Google Scholar]
- 13.Tao R, Lu Y, Xu H, Zhou ZY, Wang YH, Liu F, et al. Intramedullary versus extramedullary internal fixation for unstable intertrochanteric fracture, a meta-analysis. The Scientific World Journal. 2013 doi: 10.1155/2013/834825.139. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Guo Q, Shen Y, Zong Z, Zhao Y, Liu H, Hua X, Chen H. Percutaneous compression plate versus proximal femoral nail anti-rotation in treating elderly patients with intertrochanteric fractures: a prospective randomized study. Journal of Orthopaedic Science. 2013;18(6):977–986. doi: 10.1007/s00776-013-0468-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Nishikant K, Himanshu K, Chandrashekhar SY, Bharath G, Rishi R. Evaluation of proximal femoral locking plate in unstable extracapsular proximal femoral fractures: Surgical technique & mid term follow up results. Journal of Clinical Orthopaedics and Trauma. 2014;5(3):137–145. doi: 10.1016/j.jcot.2014.07.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Özkayın N, Okçu G, Aktuğlu K, et al. Intertrochanteric femur fractures in the elderly treated with either proximal femur nailing or hemiarthroplasty: A prospective randomised clinical study. Injury. 2015;46(Suppl 2):S3–8. doi: 10.1016/j.injury.2015.05.024. [DOI] [PubMed] [Google Scholar]
- 17.Wada K, Mikami H, Oba K, Yonezu H, Sairyo K. Cementless calcar-replacement stem with integrated greater trochanter plate for unstable intertrochanteric fracture in very elderly patients. Journal of Orthopaedic Surgery (Hong Kong) 2017;25(1):2309499016684749. doi: 10.1177/2309499016684749. [DOI] [PubMed] [Google Scholar]
- 18.Malkesh DS, Chirag SK, Rishit JS, Jagdish JP, Paresh PG. Evaluation of outcome of proximal femur locking compression plate (PFLCP) in unstable proximal femur fractures. Journal of Clinical Orthopaedics and Trauma. 2017;8(4):308–312. doi: 10.1016/j.jcot.2016.11.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Jolly A. Bansal R, More AR Pagadala MB, Comparison of complications and functional results of unstable intertrochanteric fractures of femur treated with proximal femur nails and cemented hemiarthroplasty. Journal of Orthopaedics and Trauma. 2019;10(2):296–301. doi: 10.1016/j.jcot.2017.09.015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Herman A, Landau Y, Gutman G, Ougortsin V, Chechick A, Shazar N. Radiological evaluation of intertrochanteric fracture fixation by the proximal femoral nail. Injury. 2012;43(6):856–863. doi: 10.1016/j.injury.2011.10.030. [DOI] [PubMed] [Google Scholar]
- 21.Li MH, Lei W, Liu Y, Wang CM. Clinical evaluation of the Asian proximal femur intramedullary nail antirotation system (PFNA-II) for treatment of intertrochanteric fractures. Journal of Orthopaedic Surgery and Research. 2014;9:112. doi: 10.1186/s13018-014-0112-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Hou Z, Shi J, Ye H, Pan Z. Treatment of unstable intertrochanteric fractures with percutaneous non-contact bridging plates. International Journal of Surgery. 2014;12(5):538–543. doi: 10.1016/j.ijsu.2014.02.017.140. [DOI] [PubMed] [Google Scholar]
- 23.Temiz A, Durak A, Atici T. Unstable intertrochanteric femur fractures in geriatric patients treated with the DLT trochanteric nail. Injury. 2015;46(Suppl 2):S41–S46. doi: 10.1016/j.injury.2015.05.031. [DOI] [PubMed] [Google Scholar]
- 24.Güven M, Kocadal O, Akman B, Poyanlı OS, Kemah B, Atay EF. Proximal femoral nail shows better concordance of gait analysis between operated and uninjured limbs compared to hemiarthroplasty in intertrochanteric femoral fractures. Injury. 2016;47(6):1325–1331. doi: 10.1016/j.injury.2016.03.009. [DOI] [PubMed] [Google Scholar]
- 25.Wu-BinShu X-b, Hua-yaLu H-H, Guan-HuaLan., Comparison of effects of four treatment methods for unstable intertrochanteric fractures: A network meta-analysis. International Journal of Surgery. 2018;60:173–181. doi: 10.1016/j.ijsu.2018.11.011. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
Electronic search was search was done, so data are available.