Abstract
This review focuses on complications linked to trans-oral endoscopic thyroidectomy via vestibular approach (TOETVA) and aimed to elucidate the procedure’s initial safety profile. According to the Preferred Reporting Items for Systematic Review and Meta-Analyses (PRISMA), Pubmed, Embase, and the Cochrane databases were screened till May 2021. Twenty-eight articles, nine cohorts and nineteen case series, met the inclusion criteria. Procedure-related complications were analyzed, the most important being hypoparathyroidism: transient (range=0.94-22.2%), permanent (range=1.33-2.22%), and recurrent laryngeal nerve injury: transient (range=1.9-8.8%) and permanent (range=0.59-1.42%). Surgical trauma related complications, the most prevalent being seroma, emphysema, and hematoma accounted for 2.91%. Null mortality was reported. Although current evolving experience indicates that TOETVA is safe and linked to acceptable complication rates, the method needs to be compared with the gold standard of traditional thyroidectomy in the context of sufficiently numbered cohorts and ultimately randomized controlled trials.
Keywords: Trans-oral, vestibule, thyroid surgery, complications, minimal invasive thyroid surgery, TOETVA, TORTVA, review
Surgical procedures addressing thyroid/parathyroid pathology are common in general surgery. to date, a transverse-ellipsoid incision to the neck, named by the Swiss doctor Emil Theodor Kocher (1841-1917), is utilized to gain access to the thyroid gland. Albeit meticulous suturing, a scar and marks remain in the most visible area of the neck region, a measurable drawback especially for young women (1). Aiming at elimination of this “iatrogenic tattoo”, surgeons conceived various minimal invasive endoscopic approaches to operate thyroid. In parallel, vision technology and surgical instruments developed, thus enabling surgeons to perform thyroid surgery from a remote site. Endoscopic and robotic thyroidectomy have evolved during the last decade in the context of minimal invasion pursuing scar-less surgery on the neck. Various proposed remote procedural innovations have been tried such as the axillary, the areola, the breast-chest, and the retro-auricular approach (2-4). Of special interest, being the topic of this short review, is a recently developed technique known as the transoral endoscopic thyroidectomy via the inferior vestibule (TOETVA).
TOETVA is a natural orifice transluminal endoscopic surgical procedure, which nowadays has drawn the attention of both “minimal invasivists” and young aged patients interested in ultimate cosmetic outcomes. TOETVA is realized via three internal incisions in the inferior vestibule, (one 10-mm port for endoscope and two additional 5-mm ports for surgical instruments), thereby avoiding external visible incisions and scars. Carbon dioxide is insufflated under the anterior cervical platysma to create working space extending from the oral vestibule down to the sternal notch. Then, thyroid excisional procedures are executed endoscopically (or robotically assisted, TOVARA) using conventional laparoscopic instruments and energy-based devices (EBD) (4,5).
Compared to other remote approaches, TOETVA claims to be advantageous in terms of cosmetics due to the proximity of entry sites of the working ports to the target organ (thyroid), the median symmetry of the created surgical field and the invisible sites of the scars. On the other hand, the learning curve seems to be more than steep because the learner must train his perception to a new “up to down” endoscopic vision in an unexplored till now anatomic area, undoubtfully a great challenge. New laparoscopic skills, tips and tricks had to develop by field pioneers to avoid disastrous surgical complications (5-10). The primary aim of this review was to assess feasibility and safety profile of this modern, minimally invasive thyroid surgical procedure and secondarily to address provisional complications. Whether such an ambitious modern procedure will survive head-to-head comparison with the gold standard of traditional thyroid operation remains to be proven.
Materials and Methods
Search strategy. Three Databases namely PubMed, EMBASE and Cochrane were meticulously searched for relevant studies. Publication year restrictions were not set and the last search date was May 10, 2021. The search process and elimination steps are both described in Figure 1. Key words used in the electronic research process were: TOETVA, trans-oral vestibular thyroidectomy and complications. Titles and abstracts were inspected and the articles were discarded if not relevant with complications. Duplicates were identified and discarded. Then, any article within the inclusion criteria set was thoroughly read and analyzed to extract data pertinent with TOETVA complications. Trials published from the same center or author, including different set/number of patients in different time periods were separately recorded and not excluded.
Figure 1. Flowchart: selection of articles.
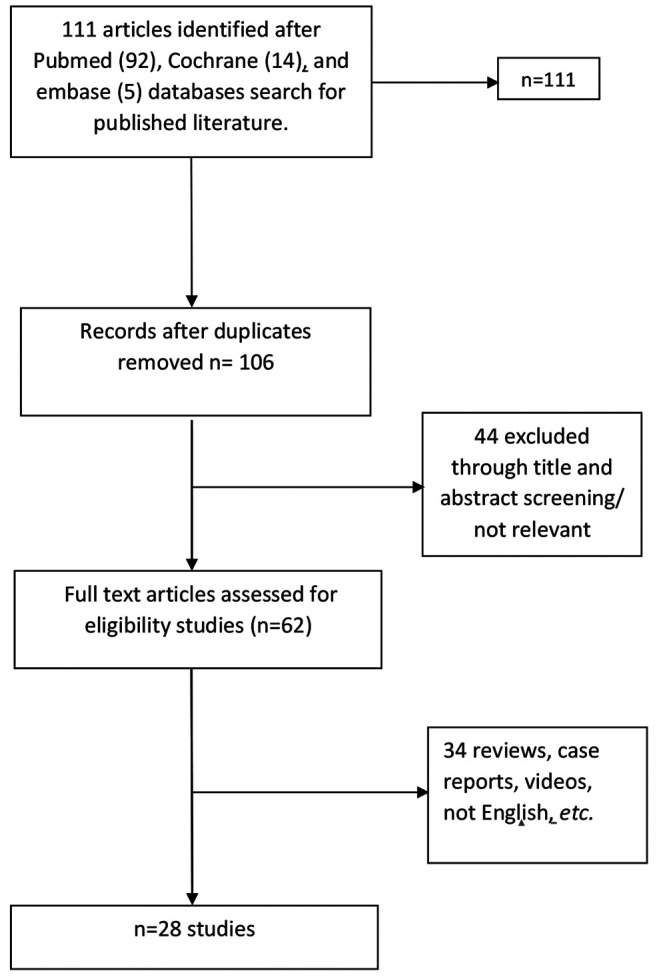
Inclusion and exclusion criteria. Original articles published in English language that assessed or/and described complications following transoral vestibular approach for thyroidectomy were included. Detailed information of patient’s characteristics, surgical procedure and peri-operative complications constituted eligibility criteria as well. Articles not written in the English language, reviews, single case reports, letters, abstracts from conferences, videos, and animal or cadaver studies were excluded.
Data recorded. Variables that were extracted from each included study consisted of: author, study type, patient characteristics such as sex and age, diagnosis, type of surgery, operation time, extracted specimen’s dimensions and length of hospital stay. Regarding complications the following list was tabulated: recurrent laryngeal nerve, superior laryngeal nerve, mental nerve injuries, transient or permanent, hypo-parathyroidism, transient or permanent, surgical site infection, seroma, emphysema, postoperative bleeding, skin flap perforation. Other scarcely reported uncommon complications thus considered miscellaneous were not grouped and thoroughly analyzed (Table I and Table II).
Table I. Clinical information of patients.
GD: Grave’s disease; PH: primary hyperparathyroidism; PTC: papillary thyroid cancer; TC: thyroglossal cyst; A: atypia; FTC: follicular thyroid cancer; NG: nodular goiter; MG: multinodular goiter; B: benign; M: malignancy; TOETVA: trans-oral endoscopic thyroidectomy via vestibular approach.
Table II. Outcome measures of included studies.
Results
Twenty-eight eligible studies, the majority of which were of Eastern hemisphere origin, were analyzed. Regarding the type of publication, there were 19 case series and 9 cohorts including 1,887 patients with a mean age of 33.8±6.6 years. One thousand seven hundred seventy-six (1,776) were women (94.22%) and 111 were men (5.88%). Apart from one mixed series of TOETVA and TOVARA, the remaining patients underwent TOETVA. Surgical indications comprised both benign (n=1088) and malignant (n=799) either thyroid or parathyroid diseases namely: graves (n=78), primary hyperparathyroidism (n=2), goiters (n=583) (single or multiple), neoplasms (n=836) (papillary or follicular and atypical), thyroid adenomas and other various benign pathologies (n=253) (cystic nodule, thyroglossal cyst etc.). Type of resections included cyst or nodule resections (n=3), hemithyroidectomy/lobectomies (n=1174), total/almost total thyroidectomy (n=712), parathyroidectomy (n=2). Thyroid resection of neoplasms was occasionally combined with central and/or lateral neck dissection (n=277). Median operation time in minutes was 130±36.19 and median length of hospital stay in days was 3.15±1.47 hours. Dimension of extracted specimen was expressed either in maximum axis length/diameter (2.85±1.98 cm) or in volume (30.11±18.74 ml). A wide range of procedure-related complications were analyzed: (a) Nerve injuries such as recurrent laryngeal nerve (RLN) (n=85; transient, 79; permanent 6), superior laryngeal nerve (SLN) (n=31; transient, 13; permanent, 18), mental nerve (MN) (n=102; transient, 82; permanent, 20), (b) hypo-parathyroidism (n=118; 116 transient, 2 permanent), (c) surgical trauma related complications such as site infection (n=12), seroma (n=36), emphysema (n=11), skin flap perforation (n=8), postoperative bleeding/hematoma (n=10), (d) miscellaneous: tracheal injury (n=2), skin bruise/injury/dimpling (n=16), swallowing discomfort (n=5), long standing pulling sensation (n=5), horner’s syndrome (n=1), C02 embolism (n=2), dehiscence (n=1), transient lip drop (n=1), chin numbness (n=26) (Table III).
Table III. Adverse events of included studies.
SLN: Superior laryngeal nerve; TOETVA: trans-oral endoscopic thyroidectomy via vestibular approach; RLN: recurrent laryngeal nerve; MN: mental nerve; T: transient; P: permanent.
Discussion
Endoscopic and robotic thyroidectomy have evolved during this last decade in the context of minimal invasion pursuing scar-less surgery on the neck. Of special interest, is a recently developed technique known as the transoral endoscopic thyroidectomy via the inferior vestibule (TOETVA). TOETVA, is a natural orifice transluminal endoscopic surgical procedure, which nowadays has drawn the attention of both “minimal invasivists” and young aged patients interested in ultimate cosmetic outcomes. A recent study aiming at quantification of social perception of neck scars, utilized eye tracking technology and recorded measurable differences in visual attention attracted by a “marked neck” (2,3,4,7). A long neck, covered by white-colored skin, free of any scar/mark consists a key feature of perceived attractiveness and facial beauty especially in eastern cultures. This fact might partly explain the fast-growing interest of eastern female patients in minimal invasive techniques of thyroid surgery. Most studies in the literature are of eastern origin and refer to young women. In this review the results of TOETVA refer to a population of 1,887 patients with a mean age of 33.8±6.6 years, 1,776 of which were women (94.22%) and only 111 were men (5.88%).
Various remote access endoscopic thyroidectomy methods have been proposed, however the rather long distance of entry sites from the thyroid bed demanded extensive tissue dissection paths leading to complications and prolonged operative time (8,11).
TOETVA is realized via three internal incisions in the inferior vestibule, (one 10-mm port for endoscope and two additional 5-mm ports for surgery instruments), thereby avoiding external visible incisions and scars. Carbon dioxide is insufflated under the anterior cervical platysma to create a working space extending from the oral vestibule down to the sternal notch. Then, thyroid excisional procedures are executed endoscopically (or robotically assisted) using conventional laparoscopic instruments and energy-based devices (EBD) (4,5). Cosmetics remain the major driving force of procedure’s innovation. Conventional thyroidectomy inevitably marks patient’s neck. Transoral approach produces no visible incision, neither scar or its physiological variants such as keloid or hypertrophic formation, contracture formation or dehiscence (12-15).
A sufficient number of studies have already been published but long-term follow-up results of TOETVA regarding its surgical and oncologic safety are lacking (16-18). Although preliminary case series report favorable outcomes (19) and shorter learning curves compared to other minimal invasive surgery (MIS) procedures (20), clear and robust data supporting safety issues and a non-inferiority identity compared to conventional thyroidectomy are still pending (4,21,22). Several potential challenges should be considered preceding safe introduction of TOETVA to clinical practice. Expert pioneers, agree on the critical need for adequate training and prevention of novel complications. Safety validation of a surgical procedure should consider both conventional and unconventional complications (23). Unconventional events are further classified into experience-related and procedure-related. Vestibular approach thyroidectomy related complications comprise new risks inherent to two-dimensional visualization, instrument’s rigidity, restricted surgeon’s maneuverability, and confined neck workspace (4).
TOETVA approach access thyroid gland through the oral vestibule of the lower lip transversing the premandibular space. Compared to other “remote access paths”, dissection is minimized and the hypoglossal nerve is not in the operative field (24). This review focuses in TOETVA-related technical and safety issues in an attempt to draw procedure’s identity.
Nerve Injuries
Although most of the nerve injuries are of the transient clinical course, they consist one of the main inherent complications experienced postoperatively by the patient.
Mental nerve injury. Mental nerve (MN) is a sensory nerve providing sensation to the front of the chin and lower lip, buccal gingivae of the mandibular anterior teeth and premolars. It is a common complication with a prevalence ranging 1-5% (25), more often transient, lateral or bilateral, related with site of working trocar placement. It results in postoperative decreased lower lip/chin sensation (numbness and/or paresthesia and/or inability to sense hot liquids).
MN palsy was early reported with an overall incidence of 4.3% (26,27). In this review, in a total of 1,887 patients, MN injury was recorded in 102 patients (5.8%), 82 transient (80.4%) and the rest 20 permanent (19.6%).
Repositioning 5mm port incisions to the vestibular mucosa just in the inner aspect of the inferior lip lateral to the level of the canines might spare tract of MN and avoid this complication (4,25). The clinical condition of altered sensation in the innervated area might persist for more than 6 months and usually occurs with other sensations such as prickling pain tingling or burning (23,26,27).
Recurrent laryngeal nerve injury. Of paramount importance, in any thyroid surgical procedure, is localization and preservation of recurrent laryngeal nerve (RLN). Prevalence of transient and permanent RLN injury in conventional open thyroidectomy ranges from 2.11% to 11.8% and from 0.2% to 5.9% respectively (2,22). In this review, in a total of 1887 patients, RLN injury was recorded in 85 patients (4.5%), 79 transient (92.9%) and the remaining 6 permanent (7.1%).
Attributed to a high definition augmented (X6-X10) “up to down” vision of endoscopic methods, the RLN is rather easily and clearly identified at its most constant location (its insertion) making TOETVA at least theoretically a safe procedure on critical neck structures (23).
However, temporary and overall RLN injury rates in TOETVA seem to be comparable or slightly higher than open procedures (22,25). In the majority or reported TOETVA-associated RLN injuries, full recovery of vocal cord function was observed (2,24,28). Others proposed intraoperative neuromonitoring in TOETVA procedures with good results (29). At present, limited experience and number of patients preclude firm conclusions regarding a provisional prophylactic effect of neuromonitoring in RLN injury. Intraoperative nerve monitoring (IONM) requires training, equipment, troubleshooting algorithms, and training of both surgeons and anesthesiologists. Until then, further trials are needed to elucidate IONM’s role in nerve protection (29,30).
External branch superior laryngeal nerve injury. “Voice symptoms” attributed to injury of the external branch of the superior laryngeal nerve (EBSLN) can occur during dissection in upper thyroid pole area. The external laryngeal nerve is the sole motor nerve supply to the cricothyroid muscle, which is the tensor of vocal folds and raises the pitch of voice. Post-thyroidectomy EBSLN injury symptoms include voice fatigue, breathy voice, and a decrease in voice range. EBSLN injury is sometimes difficult to recognize clinically and its electromyographic incidence ranges from 0% to 58% (31). During meticulous dissection of 1.5 to 2.0 cm of the distal end of the superior thyroid vessels, the external branch of SLN must be recognized and preserved (32). EBSLN can be either visually identified and preserved or functionally localized with the assistance of IONM (cricothyroid muscle twitch) (33,34). In this review, in a total of 1,887 patients, EBSLN injury was recorded in 31 patients (1.9%), 13 transient (41.9%) and the rest permanent (58.1%). Despite high quality vision during TOETVA, trivial over-dissection of the upper pole might explain the above-mentioned percentages of this nerve injury.
Hypoparathyroidism and Hypocalcemia
Hypoparathyroidism, almost solely transient, is one of the commonest complications in thyroid surgery. For obvious reasons, hypocalcemia an indirect index of parathyroid dysfunction, is more common in total thyroidectomy. Theoretically, since partial “ectomies” (lobectomy, nodule ectomy) comprise the majority of TOETVA operations, low percentages of hypoparathyroidism are anticipated (16,20). In our review, transient hypoparathyroidism occurred in 6.11% (range=0.94-22.2%) and permanent in 0.21% (range=1.33-2.22%). These results are comparable to those of standard open thyroidectomy (transient range=0-11%, permanent range=0-5.7%) (2,35-37). Fewins et al. (38) reported an incidence of hypoparathyroidism in thyroid surgery between 6.9% and 46%. Reports of permanent hypoparathyroidism are scarce (39). When a lobectomy is attempted via TOETVA, cutting the gland at midline and proceeding dissection of the lobe to be removed from medial to lateral increase the risk for parathyroid damage. This method might explain considerable rates of calcium metabolism disturbance even in lobectomies. Overzealous application of energy base devises could play a role in transient hypoparathyroid dysfunction through a mechanism of thermic shock.
Skin Complications
Minor injuries to the skin are not a surprise after TOETVA. Ecchymosis of the chin and anterior neck are common in the immediate postoperative period and resolve within 1-2 weeks (21,23,40,41). Other skin damages include tears at the lip commissures from traction and piercing of the skin caused by the Veress needle, electrocautery, or even because of the use of clamps during dissection of the superior neck flap (42). Flap perforation comprises an unconventional experience-related complication occurring while dissecting centrally through the mentalis muscle down to the tip of the chin (23). Dimpling on the chin, sometimes permanent, at the site of trocar insertion has also been reported, especially if the trocar is inserted near the level of the skin. In our review population of 1887 subjects, skin complications were skin flap perforation (n=8) and skin bruise/injury/dimpling (n=16). Although rare, these complications directly and obviously visible to the patient undermine cosmetic expectations and ruins sensation of well-being.
Seroma Formation, Hematoma, Subcutaneous Emphysema
Seroma is a minor complication, occurring in 3.5% to 5% of published cases (n=36 in our review or 36/1,887:1.91%) Its risk increases with the size of flap created to provide adequate working space; aspiration is the indicated treatment option without further sequela (2,43). Hematomas are even rarer, although this might be an underestimate due to limited pertinent literature (42). In our review among 1887 patients, 10 (0.53%) suffered postoperative bleeding or hematoma.
Subcutaneous emphysema should be expected intraoperatively or postoperatively in most patients because of insufflation. Almost always is self-limited and resolves within 3-5 days (39,44). Presentation may be mild, with crepitus confined in the neck area, and usually diminishes in 6-12 hours (44). It may occur despite proper surgical technique and gas flow rate and pressure settings are the most important causal factors (44-49). In our review, 11 (0.58%) patients were reported to suffer subcutaneous emphysema.
Infection
Based on the Centers for disease control and prevention (CDC) wound classification, TOETVA operation is characterized as a clean-contaminated one. The bacterial flora of the oral cavity is diverse comprising both gram positive aerobic and anaerobic bacteria (50). As such, perioperative antibiotic coverage against polymicrobial flora of the mouth is recommended (2,24,50). Amoxicillin-sulbactam or cefazolin combined with clindamycin or metronidazole consist logical choices (50). Careful oral preparation, meticulous technique minimizing tissue trauma and dead space eliminate risk of infection (19,51). A concomitant infectious process (i.e., periodontitis, tooth abscess etc.) consists a contraindication for TOETVA until cured. Fortunately, infection rates reported at TOETVA series are negligible (2). This agrees with the12 cases out of 1,887 patients identified in our review (0.64%).
CO2 Related Complications
Carbon dioxide embolism is a potential serious complication scarcely reported (46,52,53). In our review two cases of this ominous event were recorded among 1887 patients. Either vessel, (especially the vein), micro or macro lacerations while dissecting tissues to create essential “working space”, or prolonged high insufflation pressure consist the two main mechanisms promoting entrance of CO2 into the circulation (23). Insufflation-related adverse events also include pneumomediastinum, pneumothorax or excessive hypercarbia. Continuous end tidal CO2 (et CO2) monitoring by the anesthesiologist (goal <35), CO2 flow rates <15 l/min, CO2 pressure 6 mmHg, intermitted release of gas, precise dissection under subplatysmal plane, and meticulous hemostasis are key proposals to minimize CO2 related complications (41,46-48,54-56). Gasless TOETVA utilized by a special retractor has also been invented as an alternative to avoid CO2 related complications (4). Following extubation, close monitoring and observation in the recovery room is strongly recommended to ensure safe return to homeostasis (39,49).
Pain Pulling Sensation and Neck Swallowing Disorders
It seems that there is a short- and long-term difference in interpretation of pain comparing open thyroidectomy approach (OTA) with TOETVA. In terms of intensity, as assessed by relevant questionnaires/survey tools such as VAS, TOETVA- and OTA- related-postoperative pain was marginally different in terms of statistical significance but of minimum clinical importance (52). TOETVA is also linked with different nature of pains such as “brushing teeth”, lower lip or chin pain. Interestingly, TOETVA is reported to produce reduced cervical back pain as less head hyperextension is essential compared to OTA. Neck pain is also claimed to be less if the right subplatysmal plane is entered as a smaller number of pain receptors are located in the area compared to skin and subcutaneous level (56). Swallowing pain is reported to be equivalent or even lower in TOETVA patients compared with OTA (22,25,56).
Patients undergoing TOETVA repeatedly report a “pulling sensation” below the lower jaw, along the area which coincides with the surgical track created during the surgical procedure. It has been defined as a feeling, a complaint, not linked with a specific clinical sign such as skin retraction or dimpling. It is postulated that extensive dissection and consequent fibrosis might explain this sensation which gradually disappears within 6 months following surgery. Although benign, this bothersome inherent-to-TOETVA symptom affects patient’s quality of life and is referred as a serious reason of regretting their choice to select this approach (4,23). In this current review of 1,887 subjects, only 5 patients experienced intractable long standing pulling sensation, while the rest 1,882 became progressively asymptomatic or acquainted with this symptom. Another five patients reported excessive swallowing discomfort and 36 of them chin numbness, the majority of which faded in time.
Specimen Extraction, Size Restrictions
Thyroid specimen size is a determinant factor in choosing the endoscopic vestibular approach (25,57). Oncologic reasons, (i.e., violation of tumor capsule), and mechanical-technical issues (i.e., size of midline intraoral incision, tightness of tissue in chin area), constitute limiting factors and dictate definition of exclusion criteria. Intending to preserve a malignant specimen intact to avoid spillage (58), ensure “pathology readability” and minimize surgical trauma, an optimum specimen size of ≤20 mm and a volume ≤30 ml is generally suggested as a reasonable limit (58,36) even though larger dimensions have been attempted and proved feasible (19,23,40,41,54,55,59,60). In our review, mean dimension of extracted specimens was expressed either in maximum axis length/diameter (2.85±1.98 cm) or in volume (30.11±18.74 ml). To become extractable, larger in size or hard in consistency specimens warrant fragmentation at the provisional expense of oncologic safety and specimen quality, thus violating size limits should be avoided (58).
Operative Time and Hospital Stay
Operative time of TOETVA, although variable among reports, is longer compared to OT (19) but shorter than other endoscopic techniques (retro auricular, axilla) (22,25,61-63). In various reports, mean operative time varies considerably from less than 100 min (19,40,41,55) to more than 200 min (28,54,64). Surgeon’s experience and shape of the mandible have been suggested as main determinants of operative time in TOETVA. When reaching twenty cases in learning curve, operative time should decrease (55,63). When the mandible has a long and narrow basal arch operation time is prolonged compared to that in cases with a short and wide arch (65). Port placement and flap dissection to create working space are time consuming especially if the surgeon is not familiar with endoscopic instruments and techniques. In our review, median operative time in minutes was 130±36.19.
Length of hospital stay does not seem to differ among TOETVA and OT but several factors may produce wide variability (22,25). Different treatment guidelines, health insurance policies, economic constraints, patient’s culture or personal expectations determine length of hospital time. Series from USA or Europe report discharge after an overnight stay while those of eastern origin usually after 48-72 hours (40,66). In our review median length of hospital stay in days was 3.15±1.47. As more experience builds, and perioperative management improves hospital stay will decrease (61).
Conclusion
In this review, available data relevant to TOETV(R)A were extracted from case series and/or cohort studies. Twenty-eight studies, the majority of which were of Eastern hemisphere origin, were analyzed in this review. Nineteen were case series and nine cohorts summing up to 1,887 patients. Recurrent and superior laryngeal nerve injury, hypoparathyroidism, trauma related complications, operative time, length of hospital stay, pain and postoperative discomfort seem to be acceptable and comparable with open approach. Acceptable safety profile of TOETVA seems to be also valid regarding inherent complications such as CO2 related (emphysema, embolism).
Open thyroid operations remain the gold standard to compare with any novel procedure. Such a comparison in the context of randomized trials remains a future challenge. Until then, novel techniques such as TOETVA are tested in few specialized centers, driving evolution in the field (4). Anatomic considerations (jaw shape), obesity, patient’s culture, health policies, and economics formulate different evolution pathways between the East and West.
Keeping in mind the low level of evidence available, it could be stated that TOETVA is at least not inferior, by means of safety and outcome, compared to OT. It is also realized that it is a highly technically demanding operation with a steep learning curve, requiring previous endoscopic experience and structured training. The number of cases required to achieve minimum mastery is fifteen to twenty in endoscopic experienced operators (20,67). Cadaveric or virtual reality simulation trainings are currently under validation (4). The procedure should not be undertaken by unfamiliar teams in the absence of mentoring and training protocols (2,26).
In conclusion, this review suggests that TOETVA (or TORTVA) may be a safe treatment choice-approach for selected thyroid operative procedures in selected patients. Low level of evidence upon which this review was built is constrictive regarding reliability. Precise common terminology and clear indications remain to be defined. At present, structured training programs, evolution of instrumentation and equipment and analysis of data accumulated under the umbrella of official endocrine surgery associations is the way forward (61,67). Finally, apart from cosmetic, other substantial reasons remain to be clarified before investing and adopting this skill demanding new operation.
Conflicts of Interest
The Authors declare that they have no conflicts of interest in relation to this study.
Authors’ Contributions
E.A contributed by researching electronic databases, reading and sorting articles, and tabularizing results. G.D. contributed by reading, writing and editing this manuscript. E.S. contributed by conceiving the idea and approving this manuscript. G.T., D.D, N.N. contributed by reading and approving the manuscript.
References
- 1.Park JH, Bilegsaikhan SE, Suh YJ. A novel technique for performing transoral endoscopic thyroidectomy vestibular approach (TOETVA): A single-port platform. Surg Laparosc Endosc Percutan Tech. 2020;30(1):e4–e7. doi: 10.1097/SLE.0000000000000739. [DOI] [PubMed] [Google Scholar]
- 2.Anuwong A, Sasanakietkul T, Jitpratoom P, Ketwong K, Kim HY, Dionigi G, Richmon JD. Transoral endoscopic thyroidectomy vestibular approach (TOETVA): indications, techniques and results. Surg Endosc. 2018;32(1):456–465. doi: 10.1007/s00464-017-5705-8. [DOI] [PubMed] [Google Scholar]
- 3.Juarez MC, Ishii L, Nellis JC, Bater K, Huynh PP, Fung N, Darrach H, Russell JO, Ishii M. Objectively measuring social attention of thyroid neck scars and transoral surgery using eye tracking. Laryngoscope. 2019;129(12):2789–2794. doi: 10.1002/lary.27933. [DOI] [PubMed] [Google Scholar]
- 4.Zhang D, Park D, Sun H, Anuwong A, Tufano R, Kim HY, Dionigi G. Indications, benefits and risks of transoral thyroidectomy. Best Pract Res Clin Endocrinol Metab. 2019;33(4):101280. doi: 10.1016/j.beem.2019.05.004. [DOI] [PubMed] [Google Scholar]
- 5.Tan CT, Cheah WK, Delbridge L. “Scarless” (in the neck) endoscopic thyroidectomy (SET): an evidence-based review of published techniques. World J Surg. 2008;32(7):1349–1357. doi: 10.1007/s00268-008-9555-3. [DOI] [PubMed] [Google Scholar]
- 6.Wang Y, Yu X, Wang P, Miao C, Xie Q, Yan H, Zhao Q, Zhang M, Xiang C. Implementation of intraoperative neuromonitoring for transoral endoscopic thyroid surgery: a preliminary report. J Laparoendosc Adv Surg Tech A. 2016;26(12):965–971. doi: 10.1089/lap.2016.0291. [DOI] [PubMed] [Google Scholar]
- 7.Lee HY, Lee JY, Dionigi G, Bae JW, Kim HY. The efficacy of intraoperative neuromonitoring during robotic thyroidectomy: a prospective, randomized case-control evaluation. J Laparoendosc Adv Surg Tech A. 2015;25(11):908–914. doi: 10.1089/lap.2014.0544. [DOI] [PubMed] [Google Scholar]
- 8.Miccoli P, Berti P, Raffaelli M, Materazzi G, Baldacci S, Rossi G. Comparison between minimally invasive video-assisted thyroidectomy and conventional thyroidectomy: a prospective randomized study. Surgery. 2001;130(6):1039–1043. doi: 10.1067/msy.2001.118264. [DOI] [PubMed] [Google Scholar]
- 9.Miccoli P, Rago R, Massi M, Panicucci E, Metelli MR, Berti P, Minuto MN. Standard versus video-assisted thyroidectomy: objective postoperative pain evaluation. Surg Endosc. 2010;24(10):2415–2417. doi: 10.1007/s00464-010-0964-7. [DOI] [PubMed] [Google Scholar]
- 10.Dionigi G, Boni L, Rovera F, Rausei S, Dionigi R. Wound morbidity in mini-invasive thyroidectomy. Surg Endosc. 2011;25(1):62–67. doi: 10.1007/s00464-010-1130-y. [DOI] [PubMed] [Google Scholar]
- 11.Tae K, Ji YB, Song CM, Ryu J. Robotic and endoscopic thyroid surgery: Evolution and advances. Clin Exp Otorhinolaryngol. 2019;12(1):1–11. doi: 10.21053/ceo.2018.00766. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Kurumety SK, Helenowski IB, Goswami S, Peipert BJ, Yount SE, Sturgeon C. Post-thyroidectomy neck appearance and impact on quality of life in thyroid cancer survivors. Surgery. 2019;165(6):1217–1221. doi: 10.1016/j.surg.2019.03.006. [DOI] [PubMed] [Google Scholar]
- 13.Choi Y, Lee JH, Kim YH, Lee YS, Chang HS, Park CS, Roh MR. Impact of postthyroidectomy scar on the quality of life of thyroid cancer patients. Ann Dermatol. 2014;26(6):693–699. doi: 10.5021/ad.2014.26.6.693. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Juarez MC, Ishii L, Nellis JC, Bater K, Huynh PP, Fung N, Darrach H, Russell JO, Ishii M. Objectively measuring social attention of thyroid neck scars and transoral surgery using eye tracking. Laryngoscope. 2019;129(12):2789–2794. doi: 10.1002/lary.27933. [DOI] [PubMed] [Google Scholar]
- 15.Felix C, Russell JO, Juman S, Medford S. Cervical scar satisfaction post conventional thyroidectomy. Gland Surg. 2019;8(6):723–728. doi: 10.21037/gs.2019.11.17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Wilhelm T, Metzig A. Endoscopic minimally invasive thyroidectomy (eMIT): a prospective proof-of-concept study in humans. World J Surg. 2011;35(3):543–551. doi: 10.1007/s00268-010-0846-0. [DOI] [PubMed] [Google Scholar]
- 17.Yi JW, Yoon SG, Kim HS, Yu HW, Kim SJ, Chai YJ, Choi JY, Lee KE. Transoral endoscopic surgery for papillary thyroid carcinoma: initial experiences of a single surgeon in South Korea. Ann Surg Treat Res. 2018;95(2):73–79. doi: 10.4174/astr.2018.95.2.73. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Russell JO, Sahli ZT, Shaear M, Razavi C, Ali K, Tufano RP. Transoral thyroid and parathyroid surgery via the vestibular approach-a 2020 update. Gland Surg. 2020;9(2):409–416. doi: 10.21037/gs.2020.03.05. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Anuwong A, Ketwong K, Jitpratoom P, Sasanakietkul T, Duh QY. Safety and outcomes of the transoral endoscopic thyroidectomy vestibular approach. JAMA Surg. 2018;153(1):21–27. doi: 10.1001/jamasurg.2017.3366. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Razavi CR, Vasiliou E, Tufano RP, Russell JO. Learning curve for transoral endoscopic thyroid lobectomy. Otolaryngol Head Neck Surg. 2018;159(4):625–629. doi: 10.1177/0194599818795881. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Ahn JH, Yi JW. Transoral endoscopic thyroidectomy for thyroid carcinoma: outcomes and surgical completeness in 150 single-surgeon cases. Surg Endosc. 2020;34(2):861–867. doi: 10.1007/s00464-019-06841-8. [DOI] [PubMed] [Google Scholar]
- 22.Witzel K, von Rahden BH, Kaminski C, Stein HJ. Transoral access for endoscopic thyroid resection. Surg Endosc. 2008;22(8):1871–1875. doi: 10.1007/s00464-007-9734-6. [DOI] [PubMed] [Google Scholar]
- 23.Bakkar S, Al Hyari M, Naghawi M, Corsini C, Miccoli P. Transoral thyroidectomy: a viable surgical option with unprecedented complications-a case series. J Endocrinol Invest. 2018;41(7):809–813. doi: 10.1007/s40618-017-0808-6. [DOI] [PubMed] [Google Scholar]
- 24.Anuwong A. Transoral endoscopic thyroidectomy vestibular approach: a series of the first 60 human cases. World J Surg. 2016;40(3):491–497. doi: 10.1007/s00268-015-3320-1. [DOI] [PubMed] [Google Scholar]
- 25.Kim HK, Chai YJ, Dionigi G, Berber E, Tufano RP, Kim HY. Transoral robotic thyroidectomy for papillary thyroid carcinoma: Perioperative outcomes of 100 consecutive patients. World J Surg. 2019;43(4):1038–1046. doi: 10.1007/s00268-018-04877-w. [DOI] [PubMed] [Google Scholar]
- 26.Colella G, Giudice A, Siniscalchi G, Falcone U, Guastafierro S. Chin numbness: a symptom that should not be underestimated: a review of 12 cases. Am J Med Sci. 2009;337(6):407–410. doi: 10.1097/MAJ.0b013e31819299fa. [DOI] [PubMed] [Google Scholar]
- 27.Ewbank RL. Mental nerve neuropathy. Oral Surg Oral Med Oral Pathol. 1980;50(4):325–326. doi: 10.1016/0030-4220(80)90415-6. [DOI] [PubMed] [Google Scholar]
- 28.Udelsman R, Anuwong A, Oprea AD, Rhodes A, Prasad M, Sansone M, Brooks C, Donovan PI, Jannitto C, Carling T. Trans-oral vestibular endocrine surgery: a new technique in the United States. Ann Surg. 2016;264(6):e13–e16. doi: 10.1097/SLA.0000000000002001. [DOI] [PubMed] [Google Scholar]
- 29.Dionigi G, Wu CW, Tufano RP, Rizzo AG, Anuwong A, Sun H, Carcoforo P, Antonino C, Portinari M, Kim HY. Monitored transoral endoscopic thyroidectomy via long monopolar stimulation probe. J Vis Surg. 2018;4:24. doi: 10.21037/jovs.2017.12.25. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Dionigi G, Boni L, Rovera F, Bacuzzi A, Dionigi R. Neuromonitoring and video-assisted thyroidectomy: a prospective, randomized case-control evaluation. Surg Endosc. 2009;23(5):996–1003. doi: 10.1007/s00464-008-0098-3. [DOI] [PubMed] [Google Scholar]
- 31.Gavid M, Dubois MD, Larivé E, Prades JM. Superior laryngeal nerve in thyroid surgery: anatomical identification and monitoring. Eur Arch Otorhinolaryngol. 2017;274(9):3519–3526. doi: 10.1007/s00405-017-4666-9. [DOI] [PubMed] [Google Scholar]
- 32.Loré JM Jr, Kokocharov SI, Kaufman S, Richmond A, Sundquist N. Thirty-eight-year evaluation of a surgical technique to protect the external branch of the superior laryngeal nerve during thyroidectomy. Ann Otol Rhinol Laryngol. 1998;107(12):1015–1022. doi: 10.1177/000348949810701204. [DOI] [PubMed] [Google Scholar]
- 33.Gurleyik E, Gurleyik G. Intraoperative monitoring of external branch of the superior laryngeal nerve: Functional identification, motor integrity, and its role on vocal cord function. J Invest Surg. 2018;31(6):509–514. doi: 10.1080/08941939.2017.1362489. [DOI] [PubMed] [Google Scholar]
- 34.Tan Y, Guo B, Deng X, Ding Z, Wu B, Niu Y, Hou J, Zhang Y, Fan Y. Transoral endoscopic selective lateral neck dissection for papillary thyroid carcinoma: a pilot study. Surg Endosc. 2020;34(12):5274–5282. doi: 10.1007/s00464-019-07314-8. [DOI] [PubMed] [Google Scholar]
- 35.Song CM, Jung JH, Ji YB, Min HJ, Ahn YH, Tae K. Relationship between hypoparathyroidism and the number of parathyroid glands preserved during thyroidectomy. World J Surg Oncol. 2014;12:200. doi: 10.1186/1477-7819-12-200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Ywata de Carvalho A, Chulam TC, Kowalski LP. Long-term results of observation vs. prophylactic selective level VI neck dissection for papillary thyroid carcinoma at a cancer center. JAMA Otolaryngol Head Neck Surg. 2015;141(7):599–606. doi: 10.1001/jamaoto.2015.0786. [DOI] [PubMed] [Google Scholar]
- 37.Selberherr A, Scheuba C, Riss P, Niederle B. Postoperative hypoparathyroidism after thyroidectomy: efficient and cost-effective diagnosis and treatment. Surgery. 2015;157(2):349–353. doi: 10.1016/j.surg.2014.09.007. [DOI] [PubMed] [Google Scholar]
- 38.Fewins J, Simpson CB, Miller FR. Complications of thyroid and parathyroid surgery. Otolaryngol Clin North Am. 2003;36(1):189–206, x. doi: 10.1016/s0030-6665(02)00129-9. [DOI] [PubMed] [Google Scholar]
- 39.Shan L, Liu J. A systemic review of transoral thyroidectomy. Surg Laparosc Endosc Percutan Tech. 2018;28(3):135–138. doi: 10.1097/SLE.0000000000000512. [DOI] [PubMed] [Google Scholar]
- 40.Dionigi G, Bacuzzi A, Lavazza M, Inversini D, Boni L, Rausei S, Kim HY, Anuwong A. Transoral endoscopic thyroidectomy: preliminary experience in Italy. Updates Surg. 2017;69(2):225–234. doi: 10.1007/s13304-017-0436-x. [DOI] [PubMed] [Google Scholar]
- 41.Yang J, Wang C, Li J, Yang W, Cao G, Wong HM, Zhai H, Liu W. Complete endoscopic thyroidectomy via oral vestibular approach versus areola approach for treatment of thyroid diseases. J Laparoendosc Adv Surg Tech A. 2015;25(6):470–476. doi: 10.1089/lap.2015.0026. [DOI] [PubMed] [Google Scholar]
- 42.Fernandez-Ranvier G, Meknat A, Guevara DE, Inabnet WB 3rd. Transoral endoscopic thyroidectomy vestibular approach. JSLS. 2019;23(4):e2019.00036. doi: 10.4293/JSLS.2019.00036. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Shan CX, Zhang W, Jiang DZ, Zheng XM, Liu S, Qiu M. Prevalence, risk factors, and management of seroma formation after breast approach endoscopic thyroidectomy. World J Surg. 2010;34(8):1817–1822. doi: 10.1007/s00268-010-0597-y. [DOI] [PubMed] [Google Scholar]
- 44.Zhang D, Wu CW, Inversini D, Kim HY, Anuwong A, Bacuzzi A, Dionigi G. Lessons learned from a faulty transoral endoscopic thyroidectomy vestibular approach. Surg Laparosc Endosc Percutan Tech. 2018;28(5):e94–e99. doi: 10.1097/SLE.0000000000000555. [DOI] [PubMed] [Google Scholar]
- 45.Bellantone R, Lombardi CP, Rubino F, Perilli V, Sollazzi L, Mastroianni G, Gagner M. Arterial PCO2 and cardiovascular function during endoscopic neck surgery with carbon dioxide insufflation. Arch Surg. 2001;136(7):822–827. doi: 10.1001/archsurg.136.7.822. [DOI] [PubMed] [Google Scholar]
- 46.Kim SH, Park KS, Shin HY, Yi JH, Kim DK. Paradoxical carbon dioxide embolism during endoscopic thyroidectomy confirmed by transesophageal echocardiography. J Anesth. 2010;24(5):774–777. doi: 10.1007/s00540-010-0992-4. [DOI] [PubMed] [Google Scholar]
- 47.Ochiai R, Takeda J, Noguchi J, Ohgami M, Ishii S. Subcutaneous carbon dioxide insufflation does not cause hypercarbia during endoscopic thyroidectomy. Anesth Analg. 2000;90(3):760–762. doi: 10.1097/00000539-200003000-00046. [DOI] [PubMed] [Google Scholar]
- 48.Gottlieb A, Sprung J, Zheng XM, Gagner M. Massive subcutaneous emphysema and severe hypercarbia in a patient during endoscopic transcervical parathyroidectomy using carbon dioxide insufflation. Anesth Analg. 1997;84(5):1154–1156. doi: 10.1097/00000539-199705000-00040. [DOI] [PubMed] [Google Scholar]
- 49.Anuwong A. Strategy to prevent subcutaneous emphysema and gas insufflation-related complications in transoral endoscopic thyroidectomy vestibular approach: Reply. World J Surg. 2017;41(10):2649–2650. doi: 10.1007/s00268-017-4042-3. [DOI] [PubMed] [Google Scholar]
- 50.Salmerón-Escobar JI, del Amo-Fernández de Velasco A. Antibiotic prophylaxis in Oral and Maxillofacial Surgery. Med Oral Patol Oral Cir Bucal. 2006;11(3):E292–E296. [PubMed] [Google Scholar]
- 51.Liu N, Chen B, Li L, Zeng Q, Lv B. Subplatysmal or subfascial approach in totally endoscopic thyroidectomy has better postoperative efficacy for voice, sensory, swallowing symptoms and cosmetic result. Cohort study. Int J Surg. 2018;60:22–27. doi: 10.1016/j.ijsu.2018.10.034. [DOI] [PubMed] [Google Scholar]
- 52.Hong YT, Ahn JH, Kim JH, Yi JW, Hong KH. Bi-institutional experience of transoral endoscopic thyroidectomy: Challenges and outcomes. Head Neck. 2020;42(8):2115–2122. doi: 10.1002/hed.26153. [DOI] [PubMed] [Google Scholar]
- 53.Fu J, Luo Y, Chen Q, Lin F, Hong X, Kuang P, Yan W, Wu G, Zhang Y. Transoral endoscopic thyroidectomy: Review of 81 cases in a single institute. J Laparoendosc Adv Surg Tech A. 2018;28(3):286–291. doi: 10.1089/lap.2017.0435. [DOI] [PubMed] [Google Scholar]
- 54.Nakajo A, Arima H, Hirata M, Mizoguchi T, Kijima Y, Mori S, Ishigami S, Ueno S, Yoshinaka H, Natsugoe S. Trans-Oral Video-Assisted Neck Surgery (TOVANS). A new transoral technique of endoscopic thyroidectomy with gasless premandible approach. Surg Endosc. 2013;27(4):1105–1110. doi: 10.1007/s00464-012-2588-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Wang C, Zhai H, Liu W, Li J, Yang J, Hu Y, Huang J, Yang W, Pan Y, Ding H. Thyroidectomy: a novel endoscopic oral vestibular approach. Surgery. 2014;155(1):33–38. doi: 10.1016/j.surg.2013.06.010. [DOI] [PubMed] [Google Scholar]
- 56.Zhang D, Caruso E, Sun H, Anuwong A, Tufano R, Materazzi G, Dionigi G, Kim HY. Classifying pain in transoral endoscopic thyroidectomy. J Endocrinol Invest. 2019;42(11):1345–1351. doi: 10.1007/s40618-019-01071-0. [DOI] [PubMed] [Google Scholar]
- 57.You JY, Kim HY, Chai YJ, Kim HK, Anuwong A, Tufano RP, Dionigi G. Transoral robotic thyroidectomy versus conventional open thyroidectomy: comparative analysis of surgical outcomes in thyroid malignancies. J Laparoendosc Adv Surg Tech A. 2019;29(6):796–800. doi: 10.1089/lap.2018.0587. [DOI] [PubMed] [Google Scholar]
- 58.Wu YJ, Chi SY, Elsarawy A, Chan YC, Chou FF, Lin YC, Wee SY, Pan CC, Cheng BC, Lin CC. What is the appropriate nodular diameter in thyroid cancer for extraction by transoral endoscopic thyroidectomy vestibular approach without breaking the specimens? A surgicopathologic study. Surg Laparosc Endosc Percutan Tech. 2018;28(6):390–393. doi: 10.1097/SLE.0000000000000563. [DOI] [PubMed] [Google Scholar]
- 59.Park JO, Sun DI. Transoral endoscopic thyroidectomy: our initial experience using a new endoscopic technique. Surg Endosc. 2017;31(12):5436–5443. doi: 10.1007/s00464-017-5594-x. [DOI] [PubMed] [Google Scholar]
- 60.Chen S, Zhao M, Qiu J. Transoral vestibule approach for thyroid disease: a systematic review. Eur Arch Otorhinolaryngol. 2019;276(2):297–304. doi: 10.1007/s00405-018-5206-y. [DOI] [PubMed] [Google Scholar]
- 61.Johri G, Chand G, Mishra A, Mayilvaganan S, Agarwal G, Agarwal A, Mishra SK. Endoscopic versus conventional thyroid surgery: A comparison of quality of life, cosmetic outcomes and overall patient satisfaction with treatment. World J Surg. 2020;44(12):4118–4126. doi: 10.1007/s00268-020-05732-7. [DOI] [PubMed] [Google Scholar]
- 62.Jeong JJ, Kang SW, Yun JS, Sung TY, Lee SC, Lee YS, Nam KH, Chang HS, Chung WY, Park CS. Comparative study of endoscopic thyroidectomy versus conventional open thyroidectomy in papillary thyroid microcarcinoma (PTMC) patients. J Surg Oncol. 2009;100(6):477–480. doi: 10.1002/jso.21367. [DOI] [PubMed] [Google Scholar]
- 63.Liu S, Qiu M, Jiang DZ, Zheng XM, Zhang W, Shen HL, Shan CX. The learning curve for endoscopic thyroidectomy: a single surgeon’s experience. Surg Endosc. 2009;23(8):1802–1806. doi: 10.1007/s00464-009-0332-7. [DOI] [PubMed] [Google Scholar]
- 64.Kim HY, Chai YJ, Dionigi G, Anuwong A, Richmon JD. Transoral robotic thyroidectomy: lessons learned from an initial consecutive series of 24 patients. Surg Endosc. 2018;32(2):688–694. doi: 10.1007/s00464-017-5724-5. [DOI] [PubMed] [Google Scholar]
- 65.Shulutko AM, Semikov VI, Osmanov EG, Gryaznov SE, Gorbacheva AV, Patalova AR, Mansurova GT, Kazaryan AM. Evaluation criteria and surgical technique for transoral access to the thyroid gland: experimental study. J Invest Surg. 2019;32(5):421–427. doi: 10.1080/08941939.2018.1424271. [DOI] [PubMed] [Google Scholar]
- 66.Witzel K, Messenbaeck F, Weitzendorfer M, Benhidjeb T. Transoral thyroidectomy: limitations, patients’ safety, and own experiences. Updates Surg. 2017;69(2):193–198. doi: 10.1007/s13304-017-0457-5. [DOI] [PubMed] [Google Scholar]
- 67.Russell JO, Razavi CR, Garstka ME, Chen LW, Vasiliou E, Kang SW, Tufano RP, Kandil E. Remote-access thyroidectomy: A multi-institutional North American experience with transaxillary, robotic facelift, and transoral endoscopic vestibular approaches. J Am Coll Surg. 2019;228(4):516–522. doi: 10.1016/j.jamcollsurg.2018.12.005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 68.Karakas E, Klein G, Schopf S. Transoral thyroid surgery vestibular approach: does size matter anymore. J Endocrinol Invest. 2020;43(5):615–622. doi: 10.1007/s40618-019-01149-9. [DOI] [PubMed] [Google Scholar]
- 69.Xu Z, Song J, Wang Y, Tan L, Sun S, Meng Y. A comparison of transoral vestibular and bilateral areolar endoscopic thyroidectomy approaches for unilateral papillary thyroid microcarcinomas. Wideochir Inne Tech Maloinwazyjne. 2019;14(4):501–508. doi: 10.5114/wiitm.2019.84759. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 70.Wang T, Wu Y, Xie Q, Yan H, Zhou X, Yu X, Chen Y, Xiang C, Yan H, Zhao Q, Zhang M, Qi M, Wang P, Wang Y. Safety of central compartment neck dissection for transoral endoscopic thyroid surgery in papillary thyroid carcinoma. Jpn J Clin Oncol. 2020;50(4):387–391. doi: 10.1093/jjco/hyz195. [DOI] [PubMed] [Google Scholar]
- 71.Guo F, Wang W, Zhu X, Xiang C, Wang P, Wang Y. Comparative study between endoscopic thyroid surgery via the oral vestibular approach and the areola approach. J Laparoendosc Adv Surg Tech A. 2020;30(2):170–174. doi: 10.1089/lap.2019.0562. [DOI] [PubMed] [Google Scholar]
- 72.Kadem SG, Habash SM, Jasim AH. Transoral Endoscopic Thyroidectomy via Vestibular Approach: A series of the first ten cases in Iraq. Sultan Qaboos Univ Med J. 2019;19(1):e68–e72. doi: 10.18295/squmj.2019.19.01.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 73.Park JO, Park YJ, Kim MR, Sun DI, Kim MS, Koh YW. Gasless transoral endoscopic thyroidectomy vestibular approach (gasless TOETVA) Surg Endosc. 2019;33(9):3034–3039. doi: 10.1007/s00464-019-06826-7. [DOI] [PubMed] [Google Scholar]
- 74.Peng X, Li Z, Li H, Peng W, Zhou X, Song D, Zhou B, Lv C. The clinical application of mental nerve dissection in transoral endoscopic thyroidectomy via an oral vestibular approach. Surg Endosc. 2020;34(1):153–158. doi: 10.1007/s00464-019-06743-9. [DOI] [PubMed] [Google Scholar]
- 75.Tesseroli MAS, Spagnol M, Sanabria Á. Transoral endoscopic thyroidectomy by vestibular approach (TOETVA): initial experience in Brazil. Rev Col Bras Cir. 2018;45(5):e1951. doi: 10.1590/0100-6991e-20181951. [DOI] [PubMed] [Google Scholar]
- 76.Bian C, Liu H, Yao XY, Wu SP, Wu Y, Liu C, Huang TS. Complete endoscopic radical resection of thyroid cancer via an oral vestibule approach. Oncol Lett. 2018;16(5):5599–5606. doi: 10.3892/ol.2018.9369. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 77.Wang Y, Zhang Z, Zhao Q, Xie Q, Yan H, Yu X, Xiang C, Zhang M, Wang P. Transoral endoscopic thyroid surgery via the tri-vestibular approach with a hybrid space-maintaining method: A preliminary report. Head Neck. 2018;40(8):1774–1779. doi: 10.1002/hed.25157. [DOI] [PubMed] [Google Scholar]
- 78.Chen HK, Chen CL, Wen KS, Lin YF, Lin KY, Uen YH. Application of transoral continuous intraoperative neuromonitoring in natural orifice transluminal endoscopic surgery for thyroid disease: a preliminary study. Surg Endosc. 2018;32(1):517–525. doi: 10.1007/s00464-017-5656-0. [DOI] [PubMed] [Google Scholar]
- 79.Jitpratoom P, Ketwong K, Sasanakietkul T, Anuwong A. Transoral endoscopic thyroidectomy vestibular approach (TOETVA) for Graves’ disease: a comparison of surgical results with open thyroidectomy. Gland Surg. 2016;5(6):546–552. doi: 10.21037/gs.2016.11.04. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Sivakumar T, Amizhthu RA. Transoral endoscopic total thyroidectomy vestibular approach: A case series and literature review. J Minim Access Surg. 2018;14(2):118–123. doi: 10.4103/jmas.JMAS_3_17. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 81.Lira RB, Ramos AT, Nogueira RMR, de Carvalho GB, Russell JO, Tufano RP, Kowalski LP. Transoral thyroidectomy (TOETVA): Complications, surgical time and learning curve. Oral Oncol. 2020;110:104871. doi: 10.1016/j.oraloncology.2020.104871. [DOI] [PubMed] [Google Scholar]
- 82.Le QV, Ngo DQ, Tran TD, Ngo QX. Transoral endoscopic thyroidectomy vestibular approach: an initial experience in Vietnam. Surg Laparosc Endosc Percutan Tech. 2020;30(3):209–213. doi: 10.1097/SLE.0000000000000764. [DOI] [PubMed] [Google Scholar]
- 83.Dinç B, İlker Turan M, Rıza Gündüz U, Haluk Belen N. Transoral endoscopic thyroidectomy vestibular approach (TOETVA): Our outcomes from Turkey. Turk J Surg. 2020;36(4):340–346. doi: 10.47717/turkjsurg.2020.4765. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 84.Russell JO, Razavi CR, Shaear M, Liu RH, Chen LW, Pace-Asciak P, Tanavde V, Tai KY, Ali K, Fondong A, Kim HY, Tufano RP. Transoral thyroidectomy: Safety and outcomes of 200 consecutive North American cases. World J Surg. 2021;45(3):774–781. doi: 10.1007/s00268-020-05874-8. [DOI] [PubMed] [Google Scholar]
- 85.Deroide G, Honigman I, Berthe A, Branger F, Cussac-Pillegand C, Richa H, Anuwong A. Trans oral endoscopic thyroidectomy (TOETVA): First French experience in 90 patients. J Visc Surg. 2021;158(2):103–110. doi: 10.1016/j.jviscsurg.2021.02.001. [DOI] [PubMed] [Google Scholar]
- 86.Chai YJ, Chae S, Oh MY, Kwon H, Park WS. Transoral endoscopic thyroidectomy vestibular approach (TOETVA): Surgical outcomes and learning curve. J Clin Med. 2021;10(4):863. doi: 10.3390/jcm10040863. [DOI] [PMC free article] [PubMed] [Google Scholar]





