Abstract
The aim of this study is to examine the association between patient characteristics and primary care telemedicine choice among integrated delivery system patients self-scheduling visits during the COVID-19 pandemic. We used multivariate logistic regression to examine the association between the choice of video versus telephone and patient sociodemographic characteristics and technology access among patient-initiated primary care telemedicine visits scheduled online from March to October 2020. Among 978 272 patient-scheduled primary care telemedicine visits, 39% were video visits. Patients of Black or Hispanic race/ethnicity, or living in low socioeconomic status or low internet access neighborhoods were less likely to schedule video visits. Patients 65 years or older, with prior video visit experience or mobile portal access, or visiting their own personal provider were more likely to schedule video visits. While video adoption was substantial in all patient groups examined, differences in telemedicine choice suggest the persistence of a digital divide, emphasizing the importance of maintaining a telephone telemedicine option.
Keywords: telemedicine, digital divide, video visit, access to care, COVID-19
Lay Summary
We examined the association between patient characteristics and primary care telemedicine choice among patient-initiated primary care telemedicine visits scheduled online in a large integrated health care delivery system during the COVID-19 pandemic at a time when patient portal self-scheduled visit types were limited to telephone or video (March–October 2020). Among 978 272 patient-scheduled primary care telemedicine visits, 39% were video and 61% were telephone visits. Patients of Black or Hispanic race/ethnicity, living in neighborhoods with low socioeconomic status or low internet access were more likely to schedule telephone visits. Older patients, those with prior video visit experience or mobile portal access, or those visiting their own personal care provider were more likely to schedule video visits. While video adoption was substantial in all patient groups examined, differences in telemedicine choice suggest the persistence of a digital divide, emphasizing the importance of maintaining a telephone telemedicine option.
OBJECTIVE
The COVID-19 pandemic has dramatically changed the way health care is delivered, with telemedicine broadly promoted and widely adopted for social distancing.1–3 While live patient–physician video telemedicine more closely approximates an in-person visit, telephone telemedicine also offers patients convenient real-time access to care without potential exposure to the virus. There is limited evidence on patient preference for video or telephone telemedicine primary care visits during the pandemic. In this time of crisis-based practice change, we studied patient characteristics associated with the choice of video versus telephone telemedicine among members of an integrated care delivery system who self-scheduled primary care visits.
METHODS
This study was conducted in Kaiser Permanente Northern California (KPNC), which had adopted telephone visits over a decade ago and implemented video visit technology in 2014 with strong patient satisfaction.4,5 In early March 2020, in order to support social distancing, medical group leadership removed the option for patients to self-schedule in-person visits through the online patient portal. All patients self-scheduling an appointment had to choose either a telephone or a video visit with comparable scheduling availability. In-person visits were still available, but only based on a physician’s recommendation after an initial telemedicine visit. These protocols continued throughout the study period.
We examined all patient-initiated primary care telemedicine visits scheduled through the patient portal from March 16 (start of local shelter-in-place order) to October 31, 2020, and used multivariate logistic regression to examine the associations between patient choice of video versus telephone visit and patient sociodemographic characteristics (age, sex, race/ethnicity, and neighborhood socioeconomic status), technology access (neighborhood-level residential high-speed internet access, prior video visit, prior mobile portal use), and whether the visit was with patient’s own personal primary care provider (PCP). Based on the patients’ residential addresses, we defined low neighborhood socioeconomic status (SES) if at least 20% of residents have household incomes below the federal poverty level or at least 25% of residents 25 years of age or older have less than a high school education in the census block group using 2010 US census measures,6 and low neighborhood residential high-speed internet access level if less than 80% of households have a residential fixed high-speed connection (at least 10 Mbps downstream and at least 1 Mbps upstream) in the census tract using Federal Communications Commission data. As additional measures of prior technology access, we captured patients’ mobile portal use in the prior 365 days as a measure of prior mobile device access and use of any video visit in the prior 365 days as a measure of prior video visit experience. The multivariate model controlled for patient medical problem (ICD10 code grouping7 of primary diagnosis), time trend (an indicator variable for week), and KPNC Medical Center, with standard errors adjusted for repeated visits within patients. For easier interpretation, we calculated the adjusted rate of video visits in telemedicine by patient characteristics using the coefficients from multivariate logistic regression. We used Stata 14.2 (StataCorp, Texas) for all analyses.
The study was approved by the Kaiser Foundation Research Institute’s Institutional Review Board. Waiver of informed consent was obtained due to the observational nature of the study.
RESULTS
There were 978 272 primary care telemedicine visits scheduled using the patient portal during the study period. Overall, 11.0% of patients were pediatric (age< 18) and 15.7% were 65 years or older, 42.4% were male, and 47.5% were patients of White race/ethnicity; 20.3% lived in a neighborhood categorized as low SES and 40.1% lived in a neighborhood with low internet access level; 29.0% of patients had at least one video visit in prior 365 days and 60.6% had mobile portal access in prior 365 days; 75.9% of the visits were with patients’ own personal PCP (Table 1).
Table 1.
Patient characteristics by type of telemedicine visit
| Patient characteristic | All visits |
Telephone visits |
Video visits |
||||
|---|---|---|---|---|---|---|---|
| N | Col% | N | Col% | N | Col% | ||
| Total | 978 272 | 592 294 | 385 978 | ||||
| Age | <18 | 107 192 | 11.0 | 55 915 | 9.4 | 51 277 | 13.3 |
| 18–<45 | 443 567 | 45.3 | 277 199 | 46.8 | 166 368 | 43.1 | |
| 45–<65 | 273 865 | 28.0 | 172 218 | 29.1 | 101 647 | 26.3 | |
| 65+ | 153 648 | 15.7 | 86 962 | 14.7 | 66 686 | 17.3 | |
| Sex | Male | 414 300 | 42.4 | 244 389 | 41.3 | 169 911 | 44.0 |
| Race/ethnicity | White | 464 481 | 47.5 | 278 833 | 47.1 | 185 648 | 48.1 |
| Black | 72 192 | 7.4 | 47 320 | 8.0 | 24 872 | 6.4 | |
| Hispanic | 201 453 | 20.6 | 134 661 | 22.7 | 66 792 | 17.3 | |
| Asian | 222 132 | 22.7 | 120 447 | 20.3 | 101 685 | 26.3 | |
| Neighborhood SES | Low | 198 485 | 20.3 | 130 742 | 22.1 | 67 743 | 17.6 |
| Neighborhood Internet Access | Low | 392 428 | 40.1 | 251 309 | 42.4 | 141 119 | 36.6 |
| Prior Video Visit | Yes | 283 523 | 29.0 | 135 390 | 22.9 | 148 133 | 38.4 |
| Prior Mobile Portal Access | Yes | 592 376 | 60.6 | 354 993 | 59.9 | 237 383 | 61.5 |
| Visit with PCP | Yes | 742 041 | 75.9 | 440 452 | 74.4 | 301 589 | 78.1 |
Abbreviations: PCP: primary care provider; SES: socioeconomic status.
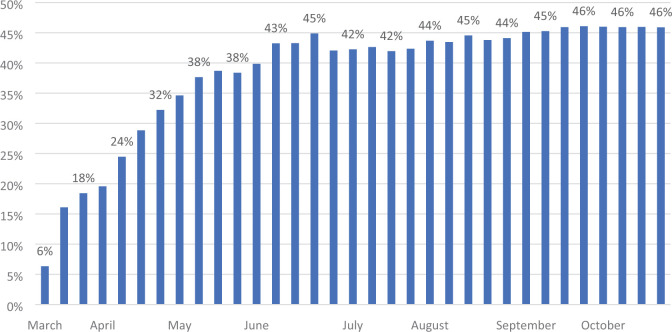
Overall, 39.4% of the patient-scheduled visits during the study period were scheduled as video visits and 60.6% were scheduled as telephone visits. The highest rate of video visits (60.9%) was found among visits with diagnosis of skin problems (ICD10: L00-L99), followed by 57.6% among visits with diagnosis of eye problems (ICD10: H00-H59). The rate of video visits varied significantly by diagnoses (P < .05). The proportion of video visits in telemedicine increased dramatically over time during the study period, from less than 7% in the first week of the study period to 40% in the first week of June, and 46% by the end of the study period in last week of October (Figure 1).
Figure 1.
Percent of video visits among telemedicine in 2020.
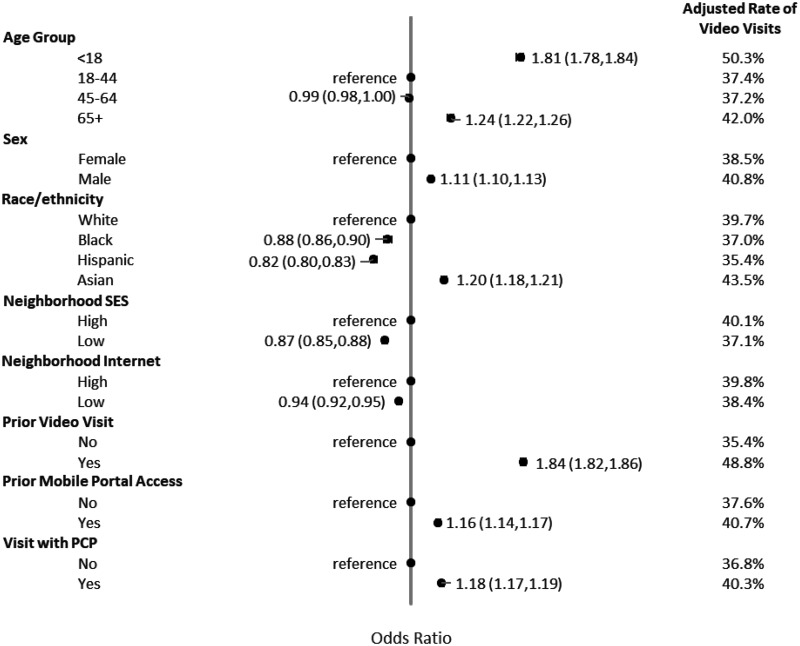
After adjustment, all the patient characteristics examined were statistically significantly associated with the choice of video versus telephone visits (Figure 2). Compared with patients who were 18–44 years old, patients who were younger than 18 years (OR: 1.81, 95% CI: 1.78–1.84) or 65 years or older (OR: 1.24, 95% CI: 1.22–1.26) were more likely to choose a video visit (no statistically significant difference between patients who were 45–64 years old and 18–44 years old, OR: 0.99, 95% CI: 0.98–1.00). Compared with patients of white race/ethnicity, Black (OR: 0.88, 95% CI: 0.86–0.90) or Hispanic (OR: 0.82, 95% CI: 0.80–0.83) patients were less likely to choose video visits, while Asians (OR: 1.20, 95% CI: 1.18–1.21) were more likely to choose video visits. Patients living in neighborhoods with lower SES (OR: 0.87, 95% CI: 0.85–0.88) or lower internet access level (OR: 0.94: 95% CI: 0.92–0.95) were less likely to choose video visits. Patients with at least one video visit in the prior 365 days (OR: 1.84, 95% CI: 1.82–1.86) were more likely to choose video visits than those without, as were patients who used a mobile device to access the portal in the prior 365 days (OR: 1.16, 95% CI: 1.14–1.17). Patients were more likely to choose a video visit if they were seeing their own personal PCP (OR: 1.18, 95% CI: 1.17–1.19).
Figure 2.
Association of choice of video visits versus telephone visits and patient characteristics.
DISCUSSION
With the ongoing COVID-19 pandemic, telemedicine provides patients the option to seek primary care without the potential virus exposure, but preference and capability for video telemedicine may be different between patients. Among patient-scheduled primary care telemedicine visits in a large integrated health care delivery system, we found patients’ choice of video versus telephone appointment varied by patient demographics and technology access. For example, Black or Hispanic patients or patients living in low SES or low internet access neighborhoods were less likely to choose video visits. Those with technology access, either prior video visit experience or mobile device access, were more likely to choose video visits. Still, while we found different adoption rates of video visits by patient characteristics, ranging from 35.4% to 50.3% across specific patient subgroups, the adoption rates were relatively high in all examined groups and no specific group was completely left out of video telemedicine.
The findings from this large study represent unique pandemic-related shifts in use of telemedicine, at a time when patient visits scheduled using the portal were limited to telephone or video. While this study confirmed the association of Black or Hispanic race/ethnicity and low SES neighborhood with low video visit use from other studies during the pandemic,8–11 some of the findings appear different from previous studies. We found Asian patients were more likely to choose video visits as compared with patients of White race, which is different from another study examining video visit during the pandemic.9 In this study, where the option for a patient-initiated in-person visit was unavailable during the pandemic-affected time period, patients who were 65 years or older were significantly more likely than younger patients (ages 18–44) to choose a video visit over a telephone visit. This finding is different from studies that examined the choice of video visits when the option for an in-person visit is available,8–13 including our prior study14 which found that older patients generally preferred an in-person visit to either a video or a telephone visit before the pandemic and older patients were associated with lower video use during the pandemic.9 In the current study, the preference for video visits among older patients may be because video visits can more closely approximate the visual interaction of an in-person visit.12 Reimbursement differences between video and telephone visits, including from federal programs, may also encourage video visit use among elderly patients during the pandemic. Our distinct findings related to age and race/ethnicity during the pandemic may reflect the impact of differences in study settings, patient populations, geographic areas, and telemedicine implementation. Further, different health care settings likely also vary in their degree of outreach to promote and support telemedicine visits, and patients’ technological readiness for telemedicine.
There are several limitations in this study. First, this study was conducted in an integrated health delivery system and the majority of visits were with the patient’s own PCP, and the findings from this study setting may not directly generalize to other less-integrated telemedicine delivery settings or fee for service systems or other direct-to-consumer telehealth programs or different patient-initiated appointment workflows. Second, while KPNC members are representative of the Northern California population in terms of age, gender, and race/ethnicity, they tend to have higher education attainment, are less likely to have low/high extremes in income, and are more likely to have experience in health-related internet use.15 Third, this study used electronic medical records and administrative data and did not include information on patients’ perspective regarding personal preference and barriers to the type of telemedicine. Moreover, patients who use the portal for scheduling visits generally have more technology access and are more likely to be e-literate,16 and the findings from this study do not represent patients who had no ability to access to the online portal. We do not have information on whether family members help to set up or participate in the telemedicine visit. Also, in deriving patient characteristics such as internet access and SES status, we did not have access to individual level measures and used general area characteristics based on patient’s neighborhood. Finally, we used a broad categorization for the primary diseases based on ICD10 grouping.
Both telephone and video telemedicine visits can provide patients with a convenient and safe way to access health care without the risk of being exposed to the virus during the pandemic. At a time when patient visits scheduled using the portal were limited to telephone or video, we found that the rate of video visits increased over time and patients’ choice of video versus telephone appointment varied by patient characteristics. The difference in telemedicine choice by technology access suggests the persistence of a digital divide8–11,14,16,17 may act as a barrier to video telemedicine. Moreover, it emphasizes the importance of maintaining a telephone telemedicine option, which may often be sufficient to address patients’ health concerns. Pandemic-related shifts in visit availability and preferences may spur longer term changes in patient care-seeking preferences, but the degree to which these shifts persist remains to be seen. Further research is needed to examine the patients’ perspective on preference and barriers for using telemedicine, and quality and clinical outcomes associated with telemedicine modality.
FUNDING
This work was supported by the Agency for Healthcare Research and Quality (grant number R01HS025189).
AUTHOR CONTRIBUTIONS
Conception and design were done by JH, IG, AM, AG, CL, EM, and MER. Acquisition, analysis, or interpretation of data for the work: JH and MER. Drafting the work: JH and MER. Revising it critically for important intellectual content: JH, IG, AM, AG, CL, EM, and MER. Final approval of the version to be published: JH, IG, AM, AG, CL, EM, and MER. Agreement to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved: JH, IG, AM, AG, CL, EM, and MER.
CONFLICT OF INTEREST STATEMENT
None declared.
DATA AVAILABILITY
Individual level data may not be made publicly available due to Institutional Review Board (IRB) and privacy concerns. The data used for this study contain protected health information (PHI) and access is protected by the Kaiser Permanente Northern California IRB. Data are available from the Kaiser Permanente Division of Research for researchers who meet the criteria for access to confidential data. For more information about data access and criteria for access to confidential data, please contact Kaiser Permanente Division of Research: DOR.IRB.Submissions@kp.org.
REFERENCES
- 1.Hollander JE, Carr BG.. Virtually perfect? Telemedicine for Covid-19. N Engl J Med 2020; 382 (18): 1679–81. [DOI] [PubMed] [Google Scholar]
- 2.Using telehealth to expand access to essential health services during the COVID-19 pandemic. https://www.cdc.gov/coronavirus/2019-ncov/hcp/telehealth.html. Accessed June 10, 2020.
- 3.Early impact of CMS expansion of medicare telehealth during COVID-19. Health Affairs Blog. https://www.healthaffairs.org/do/10.1377/forefront.20200715.454789/abs. Accessed July 15, 2020
- 4.Reed ME, Huang J, Parikh R, et al. Patient–provider video telemedicine integrated with clinical care: patient experiences. Ann Intern Med 2019; 171 (3): 222–4. [DOI] [PubMed] [Google Scholar]
- 5.Reed ME, Parikh R, Huang J, et al. Real-time patient–provider video telemedicine integrated with clinical care. N Engl J Med 2018; 379 (15): 1478–9. [DOI] [PubMed] [Google Scholar]
- 6.Krieger N, Gordon D.. Use of census-based aggregate variables to proxy for socioeconomic group: evidence from national samples. Am J Epidemiol 1999; 150 (8): 892–6. [DOI] [PubMed] [Google Scholar]
- 7.https://www.icd10data.com/ICD10CM/Codes
- 8.Gilson SF, Umscheid CA, Laiteerapong N, et al. Growth of ambulatory virtual visits and differential use by patient sociodemographics at one urban academic medical center during the COVID-19 pandemic: retrospective analysis. JMIR Med Inform 2020; 8 (12): e24544. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Eberly LA, Kallan MJ, Julien HM, et al. Patient characteristics associated with telemedicine access for primary and specialty ambulatory care during the COVID-19 pandemic. JAMA Netw Open 2020; 3 (12): e2031640. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Lam K, Lu A, Shi Y, et al. Assessing telemedicine unreadiness among older adults in the United States during the COVID-19 pandemic. JAMA Intern Med 2020; 180 (10): 1389–91. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Rodriguez JA, Betancourt JR, Sequist TD, Ganguli I.. Differences in the use of telephone and video telemedicine visits during the COVID-19 pandemic. Am J Manag Care 2021; 27 (1): 21–6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Hammersley V, Donaghy E, Parker R, et al. Comparing the content and quality of video, telephone, and face-to-face consultations: a non-randomised, quasi-experimental, exploratory study in UK primary care. Br J Gen Pract 2019; 69 (686): e595–604. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Donaghy E, Atherton H, Hammersley V, et al. Acceptability, benefits, and challenges of video consulting: a qualitative study in primary care. Br J Gen Pract 2019; 69 (686): e586–94. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Reed ME, Huang J, Graetz I, et al. Patient characteristics associated with choosing a telemedicine visit vs office visit with the same primary care clinicians. JAMA Netw Open 2020; 3 (6): e205873. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Gordon NP. Similarity of the Adult Kaiser Permanente Membership in Northern California to the insured and general population in Northern California: statistics from the 2011–12 California Health Interview Survey. Kaiser Permanente Division of Research, Oakland, CA, June 2015. http://www.dor.kaiser.org/external/chis_non_kp_2011/
- 16.Graetz I, Gordon N, Fung V, Hamity C, Reed ME.. The digital divide and patient portals. Med Care 2016; 54 (8): 772–9. [DOI] [PubMed] [Google Scholar]
- 17.Whaley CM, Pera MF, Cantor J, et al. Changes in health services use among commercially insured US populations during the COVID-19 pandemic. JAMA Netw Open 2020; 3 (11): e2024984. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Data Availability Statement
Individual level data may not be made publicly available due to Institutional Review Board (IRB) and privacy concerns. The data used for this study contain protected health information (PHI) and access is protected by the Kaiser Permanente Northern California IRB. Data are available from the Kaiser Permanente Division of Research for researchers who meet the criteria for access to confidential data. For more information about data access and criteria for access to confidential data, please contact Kaiser Permanente Division of Research: DOR.IRB.Submissions@kp.org.