Abstract
Objective
Mechanical circulatory support (MCS) devices are widely used for cardiogenic shock (CS). This network meta-analysis aims to evaluate which MCS strategy offers advantages.
Methods
A systemic search of PubMed, EMBASE, and the Cochrane Central Register of Controlled Trials was performed. Studies included double-blind, randomized controlled, and observational trials, with 30-day follow-ups. Paired independent researchers conducted the screening, data extraction, quality assessment, and consistency and heterogeneity assessment.
Results
We included 39 studies (1 report). No significant difference in 30-day mortality was noted between venoarterial extracorporeal membrane oxygenation (VA-ECMO) and VA-ECMO plus Impella, Impella, and medical therapy. According to the surface under the cumulative ranking curve, the optimal ranking of the interventions was surgical venting plus VA-ECMO, medical therapy, VA-ECMO plus Impella, intra-aortic balloon pump (IABP), Impella, Tandem Heart, VA-ECMO, and Impella plus IABP. Regarding in-hospital mortality and 30-day mortality, the forest plot showed low heterogeneity. The results of the node-splitting approach showed that direct and indirect comparisons had a relatively high consistency.
Conclusions
IABP more effectively reduce the incidence of 30-day mortality compared with VA-ECMO and Impella for the treatment of CS.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12872-022-02493-0.
Keywords: Cardiogenic shock, Mechanical circulatory support, Venoarterial extracorporeal membrane oxygenation, Intra-aortic balloon pump, Impella, Tandem heart
Introduction
Cardiogenic shock (CS) is a state of low cardiac output and hypoperfusion that is highly associated with organ damage [1]. The progress made in the field of mechanical circulatory support (MCS) has led to considerable changes in the management and treatment of CS; however, CS remains associated with a certain degree of mortality [2]. In clinical practice, venoarterial extracorporeal membrane oxygenation (VA-ECMO) has been frequently used to treat CS caused by different aetiologies such as postcardiotomy shock, acute myocardial infarction (AMI), end-stage heart failure, and acute myocarditis [1, 3–7].
CS continues to be associated with high rates of mortality and morbidity, causing a therapeutic challenge for clinicians [1, 8–10]. Although the mortality of CS patients may decrease over time, the short-term mortality rate remains 35–40% [11–13]. The main cause of CS is myocardial infarction (MI) [11]. Nevertheless, even after active treatment, there is a high mortality rate, so it is particularly important to reduce short-term mortality [11, 14]. MCS has achieved considerable advances in the treatment of CS and MCS has a theoretical basis for the treatment of CS. Moreover, this treatment has been accepted by clinicians. Therefore, the purpose of this study was to evaluate the in-hospital mortality and 30-day mortality of CS patients who underwent MCS treatment, to provide the best intervention strategy for clinicians.
Methods
This network meta-analysis (NMA) complies with the Preferred Reporting Items of Systematic Reviews and Meta-Analyses (PRISMA) guidelines [15]. All aspects involved in this study were independently conducted by at least two researchers.
Inclusion criteria
Study types: Studies included double-blind, randomized controlled, and observational trials, with 30-day follow-ups.
Participants: Patients included adults and children diagnosed with CS. CS diagnostic criteria have been debated over the years. Clinicians established the presence of CS by combining evidence of end-organ dysfunction and abnormal haemodynamic parameters. Most patients were diagnosed based on some combination of the following diagnostic criteria: (I) severe hypotension with systolic blood pressure (BP) < 80–90 mmHg for at least 30 min, the mean BP decreases by 30 mmHg or more from baseline, and vasoactive medications are needed to maintain the systolic BP above 90 mmHg in spite of sufficient fluid resuscitation; (II) elevated biventricular filling pressures with pulmonary capillary wedge pressure (PCWP) exceeding 15 mmHg and central venous pressure above 10 mmHg; (III) significantly reduced cardiac index (< 1.8 L/min/m2 or < 2.2 L/min/m2 with haemodynamic support); (IV) low mixed venous blood oxygen saturation signalling increased peripheral oxygen extraction due to hypoperfusion [13, 16].
Interventions: The interventions for CS included Tandem Heart(Cardiac Assist, Pittsburgh, PA, USA)plus Impella, medical therapy, VA-ECMO plus intra-aortic balloon pump(IABP), Tandem Heart, IABP, Impella, VA-ECMO, VA-ECMO plus Impella, Impella plus IABP, and Surgical Venting plus VA-ECMO.
Retrieval strategy
To identify relevant clinical trials, we searched PubMed, EMBASE, and the Cochrane Central Register of Controlled Trials. To expand the number of included studies, the search terms “cardiogenic shock” and “mechanical circulatory support” were used. The researchers screened the literature according to the inclusion criteria of this study. After two researchers determined that an article satisfied the preliminary inclusion criteria by reading the title and abstract, the researchers proceeded to read the full text independently to finally determine whether the article met the inclusion criteria. When differences were noted, the two researchers discussed the inclusion qualification of the article until they reached an agreement. If no agreement could be reached, a third researcher acted as an arbitrator to determine whether the article met the inclusion criteria. The reference lists of all included studies were also screened to examine relevant articles and discover other related published and unpublished research. To minimize publication bias, clinical trial registries (ClinicalTrials.gov[http://clinicaltrials.gov/]) were searched. Any discrepancies in the selected papers were resolved by consensus.
Data extraction and clinical outcome
A data extraction form was used by two pairs of reviewers to extract data independently and duplicate them. The name of the project or the last name of the first author, the time of publication, study design, setting, aetiology of CS, and interventions (VA-ECMO plus IABP, IABP, VA-ECMO, medical therapy, VA-ECMO plus Impella, percutaneous left ventricular (LV) assist devices (PLVADs)) were extracted. We considered “no MCS used” described by the study authors as “medical therapy” and extracted quantitative data from the studies. The number of patients who died in the hospital, those who died within 30 days, and the total number of patients receiving treatment were extracted. The primary outcomes were in-hospital mortality and 30-day mortality.
Meta-analysis methods and quality assessment
Using fixed-effects models [17], a Bayesian NMA was conducted using netmeta [18]. The NMA was used to estimate the relative effectiveness of all interventions for the primary outcomes by using a fixed-effects model combined with direct and indirect evidence. The model assumes that the between-study heterogeneity parameters and frequency theory methods of the whole network are common. We conducted NMA using the package netmeta in R software (Version 4.0.3, http://www.r-project.org/). The design-by-treatment test (global) and the node-splitting approach were used to perform a statistical evaluation of consistency. The Bayesian analyses estimated rank probabilities. The probability of each treatment obtaining each possible rank is shown by their relative effects. Odds ratios (ORs) and 95% confidence intervals (CIs)were used to evaluate the efficacy of various MCS equipment for adverse clinical events. To visualize heterogeneity, prediction intervals were used in the forest plots for the primary outcomes. We assessed network heterogeneity by the I2 statistic. I2 > 50% indicated higher heterogeneity. The fixed-effects model was used first. When I2 was > 50%, a random-effects model was used for statistical analysis. Subgroup analysis was performed to explore the causes of heterogeneity. Sensitivity analysis was performed by omitting each study to evaluate the reliability and stability of all studies. The methodological quality of the included articles was assessed according to the Cochrane Risk of Bias criteria [19]. Cumulative ranking plots and the surface under the cumulative ranking (SUCRA) were used to rank the advantages and disadvantages of interventions. The quality of retrospective and randomized controlled trials was evaluated by the Newcastle–Ottawa Scale and the Jadad score, respectively. Funnel plots were used to assess potential bias. Finally, the results were incorporated into the CINeMA application to assess the credibility of the results from each NMA [20]. CINeMA grades the confidence for the results of each intervention comparison as high, moderate, low, or very low. The statistical analyses in this NMA were performed using a combination of R software (Version 4.0.3, http://www.r-project.org/), STATA statistical software (version 16; StataCorp, College Station, Texas, USA), and Review Manager software (Version 5.3; Copenhagen; The Nordic Cochrane Center, The Cochrane Collaboration, 2014).
Results
Study characteristics
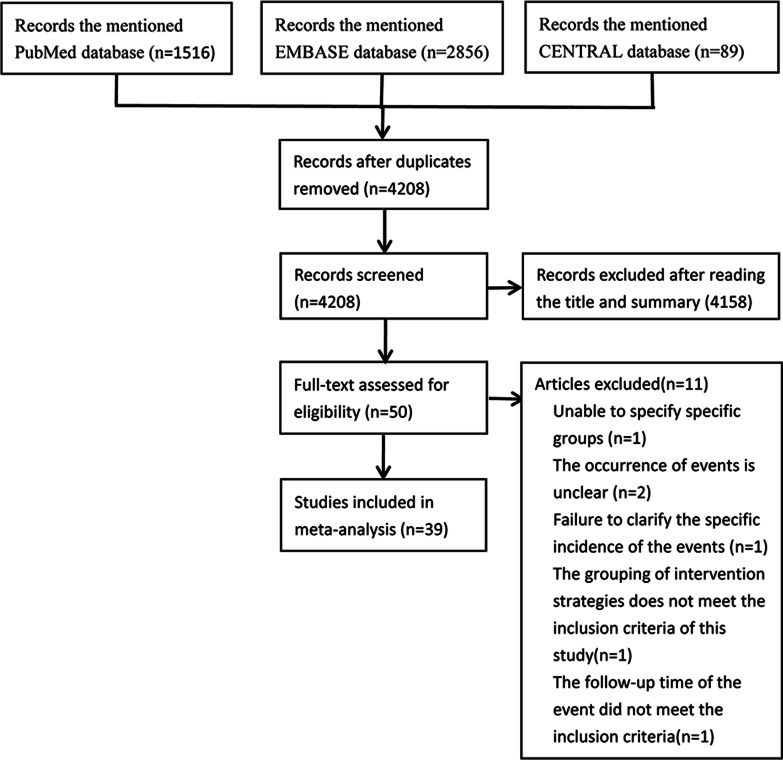
A total of 4461 articles were retrieved by searching relevant online databases. Of these,253 articles were eliminated due to duplication. By retrieving the references of previous meta-analyses, 26 additional articles met the inclusion criteria. After reading the title and abstract, 4158 articles were excluded and 50 were identified. Thereafter, 11 articles were removed after reading the full text. The flow chart of literature retrieval and reasons for article exclusion are shown in Fig. 1. Finally, we included 39 studies (including 1 report) in this NMA [11, 21–57]. The quality assessment of studies that met the inclusion criteria is shown in Additional file 1: Figure S1.
Fig. 1.
The flow chart of literature retrieval and reasons for article exclusion
A total of 10,985 patients were included in this meta-analysis. 9 double-blind, randomized controlled trials and 30 observational trials were identified. The interventions included VA-ECMO plus IABP, VA-ECMO, IABP, medical therapy, VA-ECMO plus Impella, and PLVADs (Impella, Tandem Heart). The clinical safety of VA ECMO plus IABP and IABP, PLVADs with IABP, VA-ECMO plus IABP with VA-ECMO, PLVAD with medical therapy, IABP with medical therapy, Impella plus VA-ECMO with Impella, VA-ECMO plus Impella with VA-ECMO, and VA-ECMO with Impella was compared in 3, 8, 4, 1, 11, 1, 6, and 5 articles, respectively. The characteristics of all studies that met the inclusion criteria are summarized in Table 1. The study designs of all randomized controlled trials were of high quality according to the Cochrane Risk of Bias criteria.
Table 1.
The characteristics of all studies
| Study | Year | No. of participants | Study design | Setting | Etiology of CS | Quality assessment |
|---|---|---|---|---|---|---|
| ECMO plus IABP vs. IABP | ||||||
| Perazzolo Marra et al. | 2013 | 35 | Obs | Europe | AMI | 5 |
| Tsao et al. | 2012 | 58 | Obs | Asia | AMI | 7 |
| Sheu et al. | 2010 | 219 | Obs | Asia | STEMI | 9 |
| PLVADs vs IABP | ||||||
| Seyfarth et al. (ISAR-SHOCK) | 2008 | 26 | RCT | Europe | AMI | 7 |
| Schrage et al | 2018 | 352 | Obs | Europe | AMI | 9 |
| Bochaton et al | 2019 | 13 | RCT | Europe | AMI | 4 |
| Dagmar et al. (IMPRESS trial) | 2016 | 48 | RCT | Europe | AMI | 7 |
| Shah et al | 2012 | 27 | Obs | United States | STEMI or UA/NSTEMI | 6 |
| Thiele et al | 2005 | 41 | RCT | Europe | AMI | 7 |
| Manzo-Silberman et al. | 2013 | 78 | Obs | Europe | ACS | 9 |
| Burkhoff et al. | 2006 | 33 | RCT | United States, Europe | AMI (70%) | 5 |
| Schwartz et al. | 2012 | 76 | Obs | United States | STEMI (68%) | 7 |
| ECMO plus IABP vs. ECMO | ||||||
| Park et al. | 2014 | 96 | Obs | Asia | AMI | 8 |
| Chung et al. | 2011 | 20 | Obs | Asia | AMI | 5 |
| Aoyama et al. | 2014 | 38 | Obs | Asia | AMI, INCA (2 pts, OHCA 7 pts) | 6 |
| PLVAD vs. medical therapy | ||||||
| Feistritzer et al. | 2020 | 1024 | RCT | Europe | AMI | 7 |
| IABP vs medical therapy | ||||||
| Sanborn et al. (SHOCK Registry) | 2000 | 383 | Obs | United States, Canada, Europe, New Zealand | AMI | 9 |
| Anderson et al. (GUSTO-I) | 1997 | 310 | Obs | United States, Europe | STEMI | 9 |
| Barron et al. (NRMI-2) | 2001 | 2990 | Obs | United States | AMI | 8 |
| Gu et al | 2010 | 91 | Obs | Asia | STEMI | 5 |
| Prondzinsky et al. (IABP-SHOCK) | 2010 | 40 | RCT | Europe | AMI | 7 |
| Zeymer et al. (Euro Heart Survey PCI) | 2012 | 653 | Obs | Europe | STEMI or NSTEMI | 8 |
| Dziewierz et al. (EUROTRANSFER registry) | 2014 | 51 | Obs | Europe | STEMI | 5 |
| Brunner et al. | 2019 | 42 | Obs | Europe | AMI | 5 |
| Thiele et al. (IABP-SCHOCK II) | 2012 | 598 | RCT | Europe | AMI | 7 |
| Kim et al. (KAMIR) | 2015 | 1214 | Obs | Asia | AMI | 8 |
| ECMELLA vs. Impella | ||||||
| Castro et al. | 2020 | 27 | Obs | Europe | ICMP(53.3%), DCM (26.7%) | 6 |
| ECMELLA vs. ECMO | ||||||
| Pappalardo et al. | 2016 | 63 | Obs | Europe | STEMI (54%) | 9 |
| PATEL et al | 2019 | 66 | Obs | United States | STEMI (32%), NSTEMI (14%) | 6 |
| Tepper et al | 2016 | 45 | Obs | United States | AMI (26%), PCS (28%) | 7 |
| Schrage et al. (STOP-SHOCK) | 2020 | 510 | Obs | Europe | AMI (63%) | 9 |
| MOURAD et al | 2018 | 16 | Obs | Europe | AMI | 5 |
| AKANNI et al | 2019 | 225 | Obs | United States |
AMI (25.78%), PCS (36.44%) |
6 |
| ECMO vs. Impella | ||||||
| Wernly et al | 2021 | 149 | Obs | Europe | AMI (51%) | 8 |
| Lamarche et al | 2010 | 61 | Obs | Europe | ACS (39.3%) | 8 |
| Lemor et al. | 2020 | 900 | Obs | United States | AMI | 7 |
| Karami et al. | 2020 | 128 | Obs | Europe | AMI | 8 |
| Karatolios et al. | 2020 | 166 | Obs | Europe | AMI (86%) | 8 |
| ECMO plus IABP vs. PLVADs | ||||||
| Kagawa et al. | 2012 | 73 | Obs | Asia | ACS, INCA, OHCA | 9 |
Primary outcomes
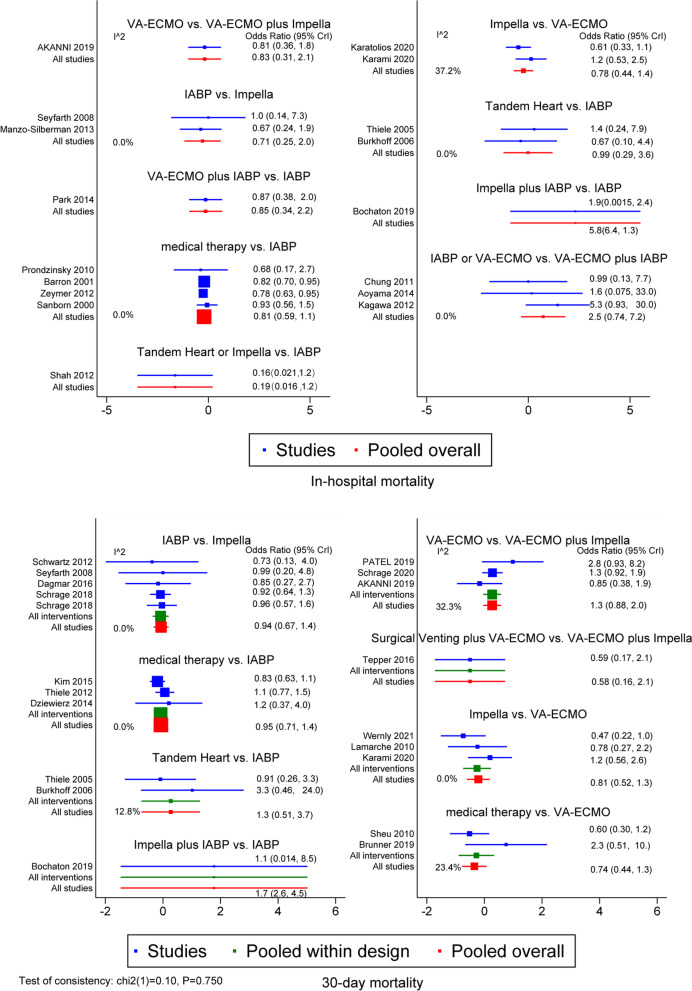
Regarding in-hospital mortality, the results showed no significant differences between IABP and Impella, VA-ECMO plus IABP, Tandem Heart, and medical therapy (Fig. 2). According to the results of the SUCRA and cumulative ranking plots, the optimal ranking among the interventions was as follows: Tandem Heart or Impella, medical therapy, VA-ECMO plus IABP, PLVAD (Tandem Heart), IABP, Impella, VA-ECMO, IABP or VA-ECMO, VA-ECMO plus Impella, and Impella plus IABP (Additional file 1: Figures S2 and S3).
Fig. 2.
The forest plots of MCS for in-hospital mortality and 30-day mortality
Based on the in-hospital mortality and mortality within 30 days, we constructed two network diagrams (Fig. 3). The contribution of each study to the indirect comparison of interventions is shown in Additional file 1: Figure S4. Regarding 30-day mortality, the results showed no significant differences between VA-ECMO and VA-ECMO plus Impella, Impella, and medical therapy. In addition, no significant differences were noted between IABP, Tandem Heart, Impella, and medical therapy (Fig. 2). According to the results of the SUCRA and cumulative ranking plots, the optimal ranking among the interventions was as follows: surgical venting plus VA-ECMO, medical therapy, VA-ECMO plus Impella, IABP, Impella, Tandem Heart, VA-ECMO, and Impella plus IABP (Additional file 1: Figures S2 and S3).
Fig. 3.
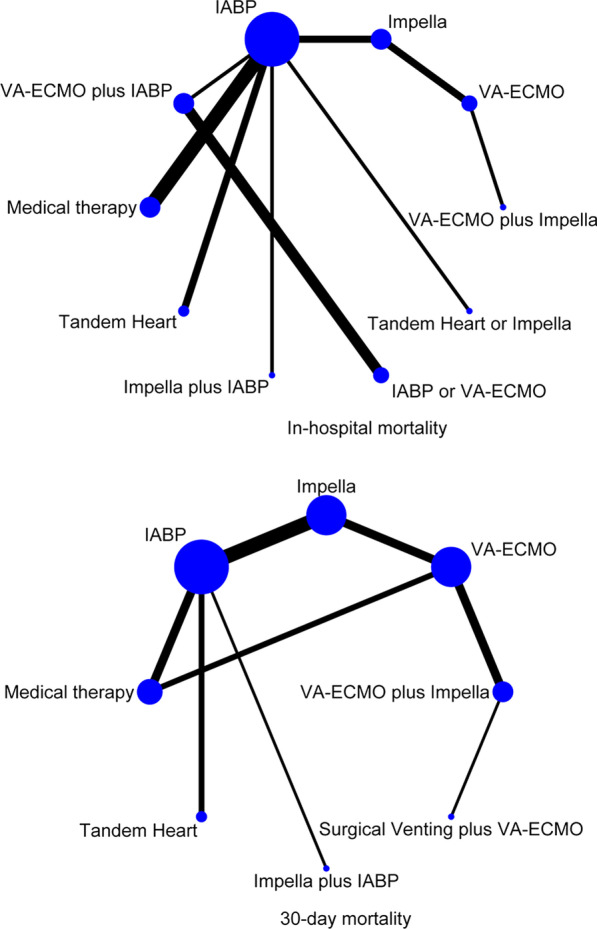
The network diagrams
Heterogeneity and consistency
The forest plots showed that the heterogeneity of all results was low (Fig. 2). The results of the node-splitting approach showed relatively high consistency in direct and indirect comparisons (Fig. 4). P values were greater than 0.05. Density plots were used to judge the degree of convergence of the model. Additional file 1: Figure S5 demonstrates that the shape of the curve is close to a normal distribution. However, the intermediate value is far from “1”; the left side of the graph shows a better coincidence rate. In summary, the model had a good degree of fit.
Fig. 4.
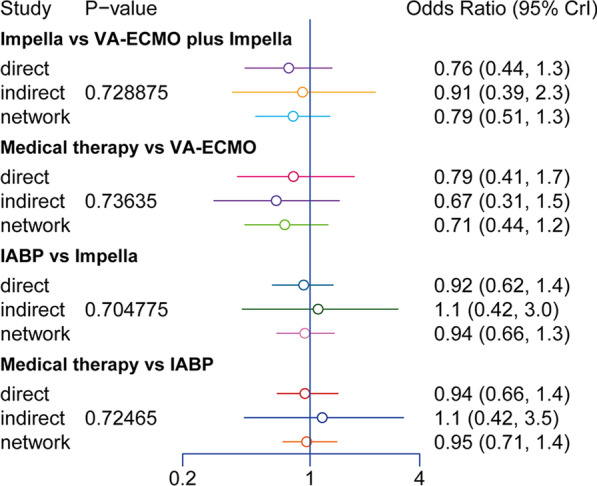
The consistency in direct and indirect comparisons of 30-day mortality
Bias detection and evidence for the NMA graded by the CINeMA system
Regarding 30-day mortality, the funnel plot showed no significant bias in the included studies (Fig. 5). Given that this NMA includes observational trials and double-blind, randomized controlled trials, the evidence level of comparison between some interventions is low according to the CINeMA system.
Fig. 5.
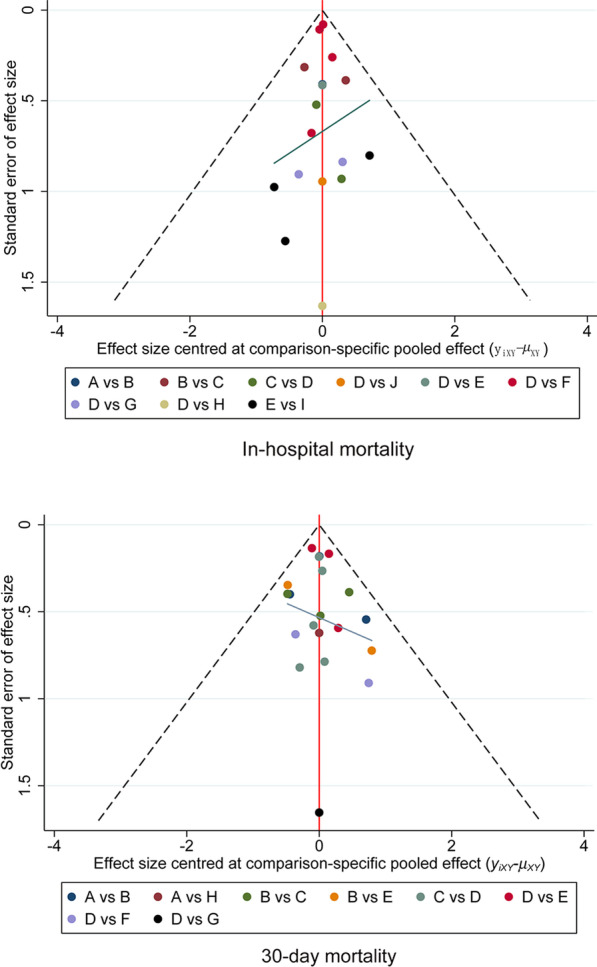
The funnel plot of all studies. (A) Venoarterial extracorporeal membrane oxygenation concomitant with Impella; (B) Venoarterial extracorporeal membrane oxygenation; (C) Impella; (D) Intra-aortic balloon pump; (E) Venoarterial extracorporeal membrane oxygenation plus Intra-aortic balloon pump; (F Medical therapy; (G) Tandem Heart; (H) Impella plus Intra-aortic balloon pump; (I) Venoarterial extracorporeal membrane oxygenation or Intra-aortic balloon pump; (J) Tandem Heart or Impella; (K) Surgical Venting
Discussion
Regarding 30-day mortality, the results of network comparison of VA-ECMO plus Impella versus VA ECMO, VA ECMO versus Impella, and IABP versus medical therapy showed high heterogeneity. Subsequently, sensitivity analysis was performed by omitting each study. Through sensitivity analysis, upon elimination of articles with a low-quality score, all results of the heterogeneity test showed low heterogeneity. Paired researchers reassessed the three articles with low-quality scores [21, 23, 56]. We believe that the reasons for the high heterogeneity may be related to the different aetiologies of CS and the different designs of the studies. For in-hospital mortality, the results of network comparison of VA-ECMO plus Impella versus VA ECMO, VA ECMO versus Impella, and IABP versus medical therapy also showed high heterogeneity. Subsequently, we also conducted a sensitivity analysis. Paired researchers reassessed the four articles with low-quality scores [23, 56, 58, 59]. The heterogeneity for all interventions was low following the exclusion of these four studies. Similarly, paired researchers discussed the reasons for the high heterogeneity. We agreed that the reason for the high heterogeneity may be the variations in the aetiology of CS and the study designs. After elimination of studies with low-quality scores, this NMA had a very favourable consistency, and the model had a comparatively favourable degree of conformity. In addition, most of the evidence levels of intervention comparison remained above medium. Regarding in-hospital mortality, the results of the SUCRA and cumulative ranking plots showed that Tandem Heart or Impella was superior to other interventions reducing in-hospital mortality. However, the studies of in-hospital mortality had a certain degree of publication bias. This notion reduced the level of evidence of Tandem Heart or Impella. In addition, compared with IABP plus Impella, IABP had a lower risk of in-hospital mortality (OR 5.89, 95% CI 1.33–6.4) and 30-day mortality (OR 1.78, 95% CI 2.6–4.56). After discussion among the researchers, the above results were considered to be less convincing. Only one study compared IABP plus Impella and IABP. Paired researchers reassessed the article with low-quality scores [60]. We cannot draw a conclusion from one study, which is unconvincing.
In this NMA, we included 39 clinical trials and evaluated the safety of various MCSs using the Bayesian method. For patients with CS, IABP is associated with the lower incidence of 30-day mortality than VA-ECMO and Impella.
VA-ECMO is a temporary mechanical circulatory support system that provides immediate and complete cardiopulmonary support in the event of CS and cardiac arrest [61].The centrifugal pump of VA-ECMO can propelup to 8 L/min of blood and promote cannula arterial return and venous drainage. A hollow fibre membrane oxygenator is spliced into the circuit, which not only provides blood oxygenation but also carbon dioxide (CO2) clearance via sweep gas flow. The latter function differentiates other MCS strategies, such as PLVADs and IABP [16]. Previously, strategies for LV unloading mainly included pulmonary vein or septal left atrial intubation, atrial septostomy, percutaneous mechanical circulatory support, transapical cannulation, or concomitant MCS devices, including IABP or PLVADs, such as Tandem-Heart [62–65]. However, many strategies require more difficult and invasive procedures with a considerable degree of correlation with serious complications [63]. Impella PLVAD (Abiomed, Danvers, MA) has been approved for use in the United States; in addition, it is also approved for the treatment of CS. The safety and effectiveness of VA-ECMO concomitant with Impella has been increasingly evaluated by several studies.
An increasing number of MCS devices have been developed for treating CS to enhance efficacy or to replace medical therapy to avoid potentially detrimental effects [66]. MCS devices can be classified based on the site of blood return, the sites from which blood is withdrawn from the body, their mechanism of action, and whether the devices provide carbon dioxide and oxygen gas exchange [66]. Devices include PLVADs, ECMO devices, percutaneous left atrial decompression devices, and aortic counterpulsation pumps. It should be noted that despite comparable effects on cardiac output and blood pressure, the effects of different forms of MCS on the heart and lung may be significantly different, specifically as determined by myocardial oxygen demand and pulmonary capillary wedge pressure (which is related to LV end-diastolic pressure) [67]. In addition, a scientific statement from the American Heart Association in 2017 noted little evidence for the selection of patients with CS who are suitable for MCS devices [68]. Therefore, in view of the feasibility and controversy of MCS in the treatment of CS patients, it is necessary to evaluate which type of MCS equipment has the superiority to better reduce mortality. MCS devices improve the systemic haemodynamics of CS patients by pumping blood from one vascular compartment to another, demonstrating the feasibility of MCS in the treatment of CS patients [67].
VA-ECMO has become a frequently used therapy for circulatory support during CS [69]. The clinical application of VA-ECMO has been widely accepted by doctors. However, VA-ECMO is still not easier to perform in the clinical setup with the improvement of peripheral cannulation. In addition, VA-ECMO might cause haemodynamic changes due to femoral artery retrograde flow, which can increase cardiac afterload and may also cause an increase in pulmonary capillary wedge pressure and left ventricular end diastolic pressure(LVEDP), which will eventually lead to the occurrence of pulmonary oedema and an increase in myocardial oxygen consumption [70, 71]. Furthermore, the associated phenomenon of LV distention cannot be ignored. LV distention is typically associated with ventricular arrhythmias and stasis of blood in the LV. Therefore, during the use of VA-ECMO, the use of a second MCS device offers great potential theoretical advantages, which play an important role in reducing myocardial oxygen consumption, pulmonary oedema, and LV distention [70, 72]. For traditional LV unloading strategies, in addition to surgical venting, IABP has always been considered a mainstream intervention. However, sufficient evidence is not available to demonstrate the capacity of IABP to reduce the occurrence of vascular adverse events. More researchers believe that the effectiveness of IABP in CS is reduced because the haemodynamic support produced by IABP is closely related to the cardiac output produced by the ventricle itself [73–75]. With the advancement of Impella technology, an Impella rotary pump can generate 2.5–3.5 L of blood flow, which plays a considerable role in improving coronary perfusion, and can greatly improve haemodynamic endpoints, thereby compensating for the shortcomings of IABP [51, 76]. Although Impella can significantly improve coronary perfusion, there is still a risk of haemolysis, which is a common problem noted among pump devices [77]. Therefore, the VA-ECMO plus Impella intervention strategy can be more beneficial in the treatment of CS patients as it can significantly reduce the central venous pressure compared with VA-ECMO alone [31, 38]. Related studies have shown that among AMI patients complicated by CS, the use of PLVAD is associated with a significantly higher risk of in-hospital mortality and haemorrhage compared with IABP [68]. However, it can not be ignored that despite the early use of IABP, the prognosis of patients with CS remains poor [78].
Regarding the use of Impella, haemolysis is a known common complication associated with acute renal failure and increased demand for blood transfusions [77]. In addition, bleeding is also a common complication of the use of MCS equipment during CS, which is related to vascular damage caused by arterial and venous cannulation [79]. When using VA-ECMO and Impella, it is necessary to administer a sufficient dose of anticoagulants to prevent thrombosis. This process enhances the risk of bleeding [80]. Acute renal failure is also a treatment challenge faced by clinicians. However, prolonging survival is considered to be the ultimate goal of CS management. Therefore, it is of great significance to evaluate the safety of various MCSs for CS patients. The various aetiologies of CS included in the NMA may have a certain degree of influence on the results of this study. Therefore, it is necessary to discuss the baseline data of this study. The aetiologies of CS in this NMA include unstable angina (UA), acute myocardial infarction (AMI), in-of-hospital cardiac arrest (INCA), out-of-hospital cardiac arrest (OHCA), ischaemic cardiomyopathy (ICMP), and dilative cardiomyopathy (DCM). However, after the exclusion of studies with low-quality scores, the heterogeneity, consistency, and convergence of the model had good results, which may be related to the analysis of the sole event of death in this NMA. However, MCS equipment is adopted for the treatment of CS patients, and mortality data provide a very important reference for clinicians to specify the diagnosis and treatment plans. This study compared the pros and cons of various MCS interventions. In addition, in this NMA, some interventions have been included in a small number of clinical trials, resulting in a small sample size for those interventions. However, as the applications of MCS are gradually recognized by clinicians, further clinical studies on MCS devices will emerge, to assess their clinical safety.
The present study is the first network meta-analysis of various MCS interventions, and it explores the best intervention strategy for the treatment of CS. In addition, the study makes an indirect comparison between interventions that were not included in clinical research. In addition, 39 articles and 10,985 patients were included in this NMA, which makes our results more credible. However, the aetiologies of CS that are not fully controlled may represent the shortcomings of our research.
Conclusions
IABP is recommended to reduce 30-day mortality in CS patients.
Review registration
PROSPERO, CRD42021282526
Supplementary Information
Additional file 1. Supplemental Figures.
Acknowledgements
None.
Authors' contributions
QZ, BW, and SW made substantial contributions to the conception of the study; QZ, YH, and SS contributed to the design of the work; QZ, CZ, BW and SW made substantial contributions to the acquisition and analysis of the data and to the interpretation of data; QZ, BW, HL, and SW drafted the work; and all authors have substantively revised the draft. All authors have approved the submitted version. All authors have agreed both to be personally accountable for the author’s own contributions and to ensure that questions related to the accuracy or integrity of any part of the work, even ones in which the author was not personally involved, are appropriately investigated, resolved, and the resolution documented in the literature. All authors read and approved the final manuscript.
Funding
This study was supported by the National Natural Science Foundation of China (82072141), Key R&D Program of Shandong Province (2019GSF108261), Natural Science Foundation of Shandong Province (ZR2020MH030), and Clinical Research Foundation of Shandong University (2020SDUCRCC014).
Availability of data and materials
All data generated or analyzed during this study are included in this manuscript and its additional files.
Declarations
Ethics approval and consent to participate
This work was approved by the Ethics Committee of Qilu Hospital of Shandong University and conducted in accordance with the Helsinki declaration. Patient consent was waived by the review board as all the data were collected from published data.
Consent for publication
Not applicable.
Competing interests
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Footnotes
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.van Diepen S, Katz JN, Albert NM, Henry TD, Jacobs AK, Kapur NK, Kilic A, Menon V, Ohman EM, Sweitzer NK, et al. Contemporary management of cardiogenic shock: a scientific statement from the American Heart Association. Circulation. 2017;136(16):e232–e268. doi: 10.1161/CIR.0000000000000525. [DOI] [PubMed] [Google Scholar]
- 2.Rihal CS, Naidu SS, Givertz MM, Szeto WY, Burke JA, Kapur NK, Kern M, Garratt KN, Goldstein JA, Dimas V, et al. 2015 SCAI/ACC/HFSA/STS Clinical Expert Consensus Statement on the Use of Percutaneous Mechanical Circulatory Support Devices in Cardiovascular Care: Endorsed by the American Heart Assocation, the Cardiological Society of India, and Sociedad Latino Americana de Cardiologia Intervencion; Affirmation of Value by the Canadian Association of Interventional Cardiology-Association Canadienne de Cardiologie d'intervention. J Am Coll Cardiol. 2015;65(19):e7–e26. doi: 10.1016/j.jacc.2015.03.036. [DOI] [PubMed] [Google Scholar]
- 3.Vallabhajosyula S, Dunlay SM, Prasad A, Kashani K, Sakhuja A, Gersh BJ, Jaffe AS, Holmes DR, Jr, Barsness GW. Acute noncardiac organ failure in acute myocardial infarction with cardiogenic shock. J Am Coll Cardiol. 2019;73(14):1781–1791. doi: 10.1016/j.jacc.2019.01.053. [DOI] [PubMed] [Google Scholar]
- 4.Vallabhajosyula S, Arora S, Lahewala S, Kumar V, Shantha GPS, Jentzer JC, Stulak JM, Gersh BJ, Gulati R, Rihal CS, et al. Temporary mechanical circulatory support for refractory cardiogenic shock before left ventricular assist device surgery. J Am Heart Assoc. 2018;7(22):e010193. doi: 10.1161/JAHA.118.010193. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Vallabhajosyula S, Arora S, Sakhuja A, Lahewala S, Kumar V, Shantha GPS, Egbe AC, Stulak JM, Gersh BJ, Gulati R, et al. Trends, predictors, and outcomes of temporary mechanical circulatory support for postcardiac surgery cardiogenic shock. Am J Cardiol. 2019;123(3):489–497. doi: 10.1016/j.amjcard.2018.10.029. [DOI] [PubMed] [Google Scholar]
- 6.Vallabhajosyula S, Patlolla SH, Sandhyavenu H, Vallabhajosyula S, Barsness GW, Dunlay SM, Greason KL, Holmes DR, Jr., Eleid MF. Periprocedural cardiopulmonary bypass or venoarterial extracorporeal membrane oxygenation during transcatheter aortic valve replacement: a systematic review. J Am Heart Assoc. 2018, 7(14). [DOI] [PMC free article] [PubMed]
- 7.Le Gall A, Follin A, Cholley B, Mantz J, Aissaoui N, Pirracchio R. Veno-arterial-ECMO in the intensive care unit: From technical aspects to clinical practice. Anaesthesia Crit Care Pain Med. 2018;37(3):259–268. doi: 10.1016/j.accpm.2017.08.007. [DOI] [PubMed] [Google Scholar]
- 8.Kolte D, Khera S, Aronow WS, Mujib M, Palaniswamy C, Sule S, Jain D, Gotsis W, Ahmed A, Frishman WH, et al. Trends in incidence, management, and outcomes of cardiogenic shock complicating ST-elevation myocardial infarction in the United States. J Am Heart Assoc. 2014;3(1):e000590. doi: 10.1161/JAHA.113.000590. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Berg DD, Bohula EA, van Diepen S, Katz JN, Alviar CL, Baird-Zars VM, Barnett CF, Barsness GW, Burke JA, Cremer PC, et al. Epidemiology of shock in contemporary cardiac intensive care units. Circul Cardiovasc Quality Outcomes. 2019;12(3):e005618. doi: 10.1161/CIRCOUTCOMES.119.005618. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Hunziker L, Radovanovic D, Jeger R, Pedrazzini G, Cuculi F, Urban P, Erne P, Rickli H, Pilgrim T. Twenty-year trends in the incidence and outcome of cardiogenic shock in AMIS plus registry. Circ Cardiovasc Interv. 2019;12(4):e007293. doi: 10.1161/CIRCINTERVENTIONS.118.007293. [DOI] [PubMed] [Google Scholar]
- 11.Thiele H, Zeymer U, Neumann FJ, Ferenc M, Olbrich HG, Hausleiter J, Richardt G, Hennersdorf M, Empen K, Fuernau G, et al. Intraaortic balloon support for myocardial infarction with cardiogenic shock. N Engl J Med. 2012;367(14):1287–1296. doi: 10.1056/NEJMoa1208410. [DOI] [PubMed] [Google Scholar]
- 12.Thiele H, Akin I, Sandri M, Fuernau G, de Waha S, Meyer-Saraei R, Nordbeck P, Geisler T, Landmesser U, Skurk C, et al. PCI strategies in patients with acute myocardial infarction and cardiogenic shock. N Engl J Med. 2017;377(25):2419–2432. doi: 10.1056/NEJMoa1710261. [DOI] [PubMed] [Google Scholar]
- 13.Hochman JS, Sleeper LA, Webb JG, Sanborn TA, White HD, Talley JD, Buller CE, Jacobs AK, Slater JN, Col J, et al. Early revascularization in acute myocardial infarction complicated by cardiogenic shock. SHOCK Investigators. Should We Emergently Revascularize Occluded Coronaries for Cardiogenic Shock. N Engl J Med. 1999;341(9):625–634. doi: 10.1056/NEJM199908263410901. [DOI] [PubMed] [Google Scholar]
- 14.Thiele H, Ohman EM, Desch S, Eitel I, de Waha S. Management of cardiogenic shock. Eur Heart J. 2015;36(20):1223–1230. doi: 10.1093/eurheartj/ehv051. [DOI] [PubMed] [Google Scholar]
- 15.Hutton B, Salanti G, Caldwell DM, Chaimani A, Schmid CH, Cameron C, Ioannidis JP, Straus S, Thorlund K, Jansen JP, et al. The PRISMA extension statement for reporting of systematic reviews incorporating network meta-analyses of health care interventions: checklist and explanations. Ann Intern Med. 2015;162(11):777–784. doi: 10.7326/M14-2385. [DOI] [PubMed] [Google Scholar]
- 16.Tsangaris A, Alexy T, Kalra R, Kosmopoulos M, Elliott A, Bartos JA, Yannopoulos D. Overview of Veno-Arterial Extracorporeal Membrane Oxygenation (VA-ECMO) support for the management of cardiogenic shock. Front Cardiovasc Med. 2021;8:686558. doi: 10.3389/fcvm.2021.686558. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.DerSimonian R, Laird N. Meta-analysis in clinical trials. Control Clin Trials. 1986;7(3):177–188. doi: 10.1016/0197-2456(86)90046-2. [DOI] [PubMed] [Google Scholar]
- 18.Rücker G, Petropoulou M, Schwarzer G. Network meta-analysis of multicomponent interventions. Biometrical J Biometrische Zeitschrift. 2020;62(3):808–821. doi: 10.1002/bimj.201800167. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Cumpston M, Li T, Page MJ, Chandler J, Welch VA, Higgins JP, Thomas J. Updated guidance for trusted systematic reviews: a new edition of the Cochrane Handbook for Systematic Reviews of Interventions. Cochrane Database Systematic Rev. 10:Ed000142 [DOI] [PMC free article] [PubMed]
- 20.Salanti G, Del Giovane C, Chaimani A, Caldwell DM, Higgins JP. Evaluating the quality of evidence from a network meta-analysis. PLoS ONE. 2014;9(7):e99682. doi: 10.1371/journal.pone.0099682. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Castro L, Zipfel S, Braunsteiner J, Schaefer A, Sill B, Söffker G, Kluge S, Lubos E, Rybczinski M, Grahn H, et al. Switching to Impella 5.0 decreases need for transfusion in patients undergoing temporary mechanical circulatory support. J Crit Care. 2020;57:253–258. doi: 10.1016/j.jcrc.2019.11.007. [DOI] [PubMed] [Google Scholar]
- 22.Park TK, Yang JH, Choi S-H, Song YB, Hahn J-Y, Choi J-H, Sung K, Lee YT, Gwon H-C. Clinical impact of intra-aortic balloon pump during extracorporeal life support in patients with acute myocardial infarction complicated by cardiogenic shock. BMC Anesthesiol. 2014;14(1):27. doi: 10.1186/1471-2253-14-27. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Gu J, Hu W, Xiao H, Feng X, Chen Y, Zhang D. Intra-aortic balloon pump improves clinical prognosis and attenuates C-reactive protein level in acute STEMI complicated by cardiogenic shock. Cardiology. 2010;117(1):75–80. doi: 10.1159/000319618. [DOI] [PubMed] [Google Scholar]
- 24.Prondzinsky R, Lemm H, Swyter M, Wegener N, Unverzagt S, Carter JM, Russ M, Schlitt A, Buerke U, Christoph A, et al. Intra-aortic balloon counterpulsation in patients with acute myocardial infarction complicated by cardiogenic shock: The prospective, randomized IABP SHOCK Trial for attenuation of multiorgan dysfunction syndrome*. Crit Care Med. 2010;38(1):152–160. doi: 10.1097/CCM.0b013e3181b78671. [DOI] [PubMed] [Google Scholar]
- 25.Sheu J-J, Tsai T-H, Lee F-Y, Fang H-Y, Sun C-K, Leu S, Yang C-H, Chen S-M, Hang C-L, Hsieh Y-K, et al. Early extracorporeal membrane oxygenator-assisted primary percutaneous coronary intervention improved 30-day clinical outcomes in patients with ST-segment elevation myocardial infarction complicated with profound cardiogenic shock. Crit Care Med. 2010;38(9):1810–1817. doi: 10.1097/CCM.0b013e3181e8acf7. [DOI] [PubMed] [Google Scholar]
- 26.Kagawa E, Dote K, Kato M, Sasaki S, Nakano Y, Kajikawa M, Higashi A, Itakura K, Sera A, Inoue I, et al. Should we emergently revascularize occluded coronaries for cardiac arrest? Circulation. 2012;126(13):1605–1613. doi: 10.1161/CIRCULATIONAHA.111.067538. [DOI] [PubMed] [Google Scholar]
- 27.Schrage B, Schneider S, Zeymer U, Thiele H, Westermann D. Response by Schrage et al to Letter Regarding Article, "Impella Support for Acute Myocardial Infarction Complicated by Cardiogenic Shock: A Matched-Pair IABP-SHOCK II Trial 30-Day Mortality Analysis". Circulation. 2019;140(11):e559–e560. doi: 10.1161/CIRCULATIONAHA.119.041637. [DOI] [PubMed] [Google Scholar]
- 28.Schrage B, Becher PM, Bernhardt A, Bezerra H, Blankenberg S, Brunner S, Colson P, Cudemus Deseda G, Dabboura S, Eckner D, et al. Left ventricular unloading is associated with lower mortality in patients with cardiogenic shock treated with venoarterial extracorporeal membrane oxygenation. Circulation. 2020;142(22):2095–2106. doi: 10.1161/CIRCULATIONAHA.120.048792. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Mourad M, Gaudard P, De La Arena P, Eliet J, Zeroual N, Rouvière P, Roubille F, Albat B, Colson PH. Circulatory support with extracorporeal membrane oxygenation and/or impella for cardiogenic shock during myocardial infarction. ASAIO J. 2018;64(6):708–714. doi: 10.1097/MAT.0000000000000704. [DOI] [PubMed] [Google Scholar]
- 30.Schwartz. Treating refractory cardiogenic shock with the tandemheart and Impella devices: a single center experience. Cardiol Res. 2012. [DOI] [PMC free article] [PubMed]
- 31.Akanni OJ, Takeda K, Truby LK, Kurlansky PA, Chiuzan C, Han J, Topkara VK, Yuzefpolskaya M, Colombo PC, Karmpaliotis D, et al. EC-VAD: combined use of extracorporeal membrane oxygenation and percutaneous microaxial pump left ventricular assist device. ASAIO J. 2019;65(3):219–226. doi: 10.1097/MAT.0000000000000804. [DOI] [PubMed] [Google Scholar]
- 32.Wernly B, Karami M, Engström AE, Windecker S, Hunziker L, Lüscher TF, Henriques JP, Ferrari MW, Binnebößel S, Masyuk M, et al. Impella versus extracorporal life support in cardiogenic shock: a propensity score adjusted analysis. ESC Heart Failure. 2021;8(2):953–961. doi: 10.1002/ehf2.13200. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Karami M, den Uil CA, Ouweneel DM, Scholte NTB, Engström AE, Akin S, Lagrand WK, Vlaar APJ, Jewbali LS, Henriques JPS. Mechanical circulatory support in cardiogenic shock from acute myocardial infarction: Impella CP/5.0 versus ECMO. Eur Heart J: Acute Cardiovasc Care. 2019;9(2):164–172. doi: 10.1177/2048872619865891. [DOI] [PubMed] [Google Scholar]
- 34.Pappalardo F, Schulte C, Pieri M, Schrage B, Contri R, Soeffker G, Greco T, Lembo R, Müllerleile K, Colombo A, et al. Concomitant implantation of Impella®on top of veno-arterial extracorporeal membrane oxygenation may improve survival of patients with cardiogenic shock. Eur J Heart Fail. 2017;19(3):404–412. doi: 10.1002/ejhf.668. [DOI] [PubMed] [Google Scholar]
- 35.Thiele H, Sick P, Boudriot E, Diederich K-W, Hambrecht R, Niebauer J, Schuler G. Randomized comparison of intra-aortic balloon support with a percutaneous left ventricular assist device in patients with revascularized acute myocardial infarction complicated by cardiogenic shock. Eur Heart J. 2005;26(13):1276–1283. doi: 10.1093/eurheartj/ehi161. [DOI] [PubMed] [Google Scholar]
- 36.Bochaton T, Huot L, Elbaz M, Delmas C, Aissaoui N, Farhat F, Mewton N, Bonnefoy E. Mechanical circulatory support with the Impella® LP5.0 pump and an intra-aortic balloon pump for cardiogenic shock in acute myocardial infarction: The IMPELLA-STIC randomized study. Arch Cardiovasc Diseases. 2020;113(4):237–243. doi: 10.1016/j.acvd.2019.10.005. [DOI] [PubMed] [Google Scholar]
- 37.Burkhoff D, Cohen H, Brunckhorst C, O'Neill WW. A randomized multicenter clinical study to evaluate the safety and efficacy of the TandemHeart percutaneous ventricular assist device versus conventional therapy with intraaortic balloon pumping for treatment of cardiogenic shock. Am Heart J. 2006;152(3):469.e461–469.e468. doi: 10.1016/j.ahj.2006.05.031. [DOI] [PubMed] [Google Scholar]
- 38.Tepper S, Masood MF, Baltazar Garcia M, Pisani M, Ewald GA, Lasala JM, Bach RG, Singh J, Balsara KR, Itoh A. Left Ventricular Unloading by Impella Device Versus Surgical Vent During Extracorporeal Life Support. Ann Thorac Surg. 2017;104(3):861–867. doi: 10.1016/j.athoracsur.2016.12.049. [DOI] [PubMed] [Google Scholar]
- 39.Shah R, Thomson A, Atianzar K, Somma K, Mehra A, Clavijo L, Matthews RV, Shavelle DM. Percutaneous left ventricular support for high-risk PCI and cardiogenic shock: Who gets what? Cardiovasc Revascul Med. 2012;13(2):101–105. doi: 10.1016/j.carrev.2012.01.003. [DOI] [PubMed] [Google Scholar]
- 40.Lemor A, Hosseini Dehkordi SH, Basir MB, Villablanca PA, Jain T, Koenig GC, Alaswad K, Moses JW, Kapur NK, O'Neill W. Impella versus extracorporeal membrane oxygenation for acute myocardial infarction cardiogenic shock. Cardiovasc Revasc Med. 2020;21(12):1465–1471. doi: 10.1016/j.carrev.2020.05.042. [DOI] [PubMed] [Google Scholar]
- 41.Seyfarth M, Sibbing D, Bauer I, Fröhlich G, Bott-Flügel L, Byrne R, Dirschinger J, Kastrati A, Schömig A. A randomized clinical trial to evaluate the safety and efficacy of a percutaneous left ventricular assist device versus intra-aortic balloon pumping for treatment of cardiogenic shock caused by myocardial infarction. J Am Coll Cardiol. 2008;52(19):1584–1588. doi: 10.1016/j.jacc.2008.05.065. [DOI] [PubMed] [Google Scholar]
- 42.Ouweneel DM, Eriksen E, Sjauw KD, van Dongen IM, Hirsch A, Packer EJS, Vis MM, Wykrzykowska JJ, Koch KT, Baan J, et al. Percutaneous mechanical circulatory support versus intra-aortic balloon pump in cardiogenic shock after acute myocardial infarction. J Am Coll Cardiol. 2017;69(3):278–287. doi: 10.1016/j.jacc.2016.10.022. [DOI] [PubMed] [Google Scholar]
- 43.Brunner S, Guenther SPW, Lackermair K, Peterss S, Orban M, Boulesteix A-L, Michel S, Hausleiter J, Massberg S, Hagl C. Extracorporeal life support in cardiogenic shock complicating acute myocardial infarction. J Am Coll Cardiol. 2019;73(18):2355–2357. doi: 10.1016/j.jacc.2019.02.044. [DOI] [PubMed] [Google Scholar]
- 44.Tsao N-W, Shih C-M, Yeh J-S, Kao Y-T, Hsieh M-H, Ou K-L, Chen J-W, Shyu K-G, Weng Z-C, Chang N-C, et al. Extracorporeal membrane oxygenation–assisted primary percutaneous coronary intervention may improve survival of patients with acute myocardial infarction complicated by profound cardiogenic shock. J Crit Care. 2012;27(5):530.e531–530.e511. doi: 10.1016/j.jcrc.2012.02.012. [DOI] [PubMed] [Google Scholar]
- 45.Kim HK, Jeong MH, Ahn Y, Sim DS, Chae SC, Kim YJ, Hur SH, Seong IW, Hong TJ, Choi DH, et al. Clinical outcomes of the intra-aortic balloon pump for resuscitated patients with acute myocardial infarction complicated by cardiac arrest. J Cardiol. 2016;67(1):57–63. doi: 10.1016/j.jjcc.2015.04.007. [DOI] [PubMed] [Google Scholar]
- 46.Lamarche Y, Cheung A, Ignaszewski A, Higgins J, Kaan A, Griesdale DEG, Moss R. Comparative outcomes in cardiogenic shock patients managed with Impella microaxial pump or extracorporeal life support. J Thorac Cardiovasc Surg. 2011;142(1):60–65. doi: 10.1016/j.jtcvs.2010.07.075. [DOI] [PubMed] [Google Scholar]
- 47.Manzo-Silberman S, Fichet J, Mathonnet A, Varenne O, Ricome S, Chaib A, Zuber B, Spaulding C, Cariou A. Percutaneous left ventricular assistance in post cardiac arrest shock: comparison of intra aortic blood pump and IMPELLA Recover LP2.5. Resuscitation. 2013;84(5):609–615. doi: 10.1016/j.resuscitation.2012.10.001. [DOI] [PubMed] [Google Scholar]
- 48.Feistritzer H-J, Desch S, Freund A, Poess J, Zeymer U, Ouarrak T, Schneider S, de Waha-Thiele S, Fuernau G, Eitel I, et al. Prognostic impact of active mechanical circulatory support in cardiogenic shock complicating acute myocardial infarction, results from the culprit-shock trial. J Clin Med. 2020;9(6):1976. doi: 10.3390/jcm9061976. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Karatolios K, Chatzis G, Markus B, Luesebrink U, Ahrens H, Divchev D, Syntila S, Jerrentrup A, Schieffer B. Comparison of mechanical circulatory support with venoarterial extracorporeal membrane oxygenation or Impella for patients with cardiogenic shock: a propensity-matched analysis. Clin Res Cardiol. 2020;110:1404. doi: 10.1007/s00392-020-01777-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Chung ES, Lim C, Lee H-Y, Choi J-H, Lee J-S, Park K-H. Results of Extracorporeal Membrane Oxygenation (ECMO) support before coronary reperfusion in cardiogenic shock with acute myocardial infarction. Korean J Thorac Cardiovasc Surg. 2011;44(4):273–278. doi: 10.5090/kjtcs.2011.44.4.273. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Patel SM, Lipinski J, Al-Kindi SG, Patel T, Saric P, Li J, Nadeem F, Ladas T, Alaiti A, Phillips A, et al. Simultaneous venoarterial extracorporeal membrane oxygenation and percutaneous left ventricular decompression therapy with impella is associated with improved outcomes in refractory cardiogenic shock. ASAIO J. 2019;65(1):21–28. doi: 10.1097/MAT.0000000000000767. [DOI] [PubMed] [Google Scholar]
- 52.Barron HV, Every NR, Parsons LS, Angeja B, Goldberg RJ, Gore JM, Chou TM. The use of intra-aortic balloon counterpulsation in patients with cardiogenic shock complicating acute myocardial infarction: data from the National Registry of Myocardial Infarction 2. Am Heart J. 2001;141(6):933–939. doi: 10.1067/mhj.2001.115295. [DOI] [PubMed] [Google Scholar]
- 53.Dziewierz A, Siudak Z, Rakowski T, Kleczyński P, Zasada W, Dudek D. Impact of intra-aortic balloon pump on long-term mortality of unselected patients with ST-segment elevation myocardial infarction complicated by cardiogenic shock. Adv Interv Cardiol. 2014;3:175–180. doi: 10.5114/pwki.2014.45144. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Zeymer U, Hochadel M, Hauptmann K-E, Wiegand K, Schuhmacher B, Brachmann J, Gitt A, Zahn R. Intra-aortic balloon pump in patients with acute myocardial infarction complicated by cardiogenic shock: results of the ALKK-PCI registry. Clin Res Cardiol. 2012;102(3):223–227. doi: 10.1007/s00392-012-0523-4. [DOI] [PubMed] [Google Scholar]
- 55.Sanborn TA, Sleeper LA, Bates ER, Jacobs AK, Boland J, French JK, Dens J, Dzavik V, Palmeri ST, Webb JG, et al. Impact of thrombolysis, intra-aortic balloon pump counterpulsation, and their combination in cardiogenic shock complicating acute myocardial infarction: a report from the SHOCK Trial Registry. SHould we emergently revascularize Occluded Coronaries for cardiogenic shocK? J Am Coll Cardiol. 2000;36(3):1123–1129. doi: 10.1016/s0735-1097(00)00875-5. [DOI] [PubMed] [Google Scholar]
- 56.Anderson RD, Ohman EM, Holmes DR, Jr, Col I, Stebbins AL, Bates ER, Stomel RJ, Granger CB, Topol EJ, Califf RM. Use of intraaortic balloon counterpulsation in patients presenting with cardiogenic shock: observations from the GUSTO-I Study. Global Utilization of Streptokinase and TPA for Occluded Coronary Arteries. J Am Coll Cardiol. 1997;30(3):708–715. doi: 10.1016/s0735-1097(97)00227-1. [DOI] [PubMed] [Google Scholar]
- 57.Aoyama N, Imai H, Kurosawa T, Fukuda N, Moriguchi M, Nishinari M, Nishii M, Kono K, Soma K, Izumi T. Therapeutic strategy using extracorporeal life support, including appropriate indication, management, limitation and timing of switch to ventricular assist device in patients with acute myocardial infarction. J Artif Organs. 2013;17(1):33–41. doi: 10.1007/s10047-013-0735-z. [DOI] [PubMed] [Google Scholar]
- 58.Pappalardo F, Schulte C, Pieri M, Schrage B, Contri R, Soeffker G, Greco T, Lembo R, Müllerleile K, Colombo A, et al. Concomitant implantation of Impella(®) on top of veno-arterial extracorporeal membrane oxygenation may improve survival of patients with cardiogenic shock. Eur J Heart Fail. 2017;19(3):404–412. doi: 10.1002/ejhf.668. [DOI] [PubMed] [Google Scholar]
- 59.Lemor A, Hosseini Dehkordi SH, Basir MB, Villablanca PA, Jain T, Koenig GC, Alaswad K, Moses JW, Kapur NK, O'Neill W. Impella versus extracorporeal membrane oxygenation for acute myocardial infarction cardiogenic shock. Cardiovasc Revascul Med. 2020;21(12):1465–1471. doi: 10.1016/j.carrev.2020.05.042. [DOI] [PubMed] [Google Scholar]
- 60.Bochaton T, Huot L, Elbaz M, Delmas C, Aissaoui N, Farhat F, Mewton N, Bonnefoy E. Mechanical circulatory support with the Impella® LP5.0 pump and an intra-aortic balloon pump for cardiogenic shock in acute myocardial infarction: The IMPELLA-STIC randomized study. Arch Cardiovasc Dis. 2020;113(4):237–243. doi: 10.1016/j.acvd.2019.10.005. [DOI] [PubMed] [Google Scholar]
- 61.Telukuntla KS, Estep JD. Acute mechanical circulatory support for cardiogenic shock. Methodist Debakey Cardiovasc J. 2020;16(1):27–35. doi: 10.14797/mdcj-16-1-27. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 62.Vallabhajosyula S, O'Horo JC, Antharam P, Ananthaneni S, Vallabhajosyula S, Stulak JM, Dunlay SM, Holmes DR, Jr, Barsness GW. Venoarterial extracorporeal membrane oxygenation with concomitant impella versus venoarterial extracorporeal membrane oxygenation for cardiogenic shock. ASAIO J. 2020;66(5):497–503. doi: 10.1097/MAT.0000000000001039. [DOI] [PubMed] [Google Scholar]
- 63.Russo JJ, Aleksova N, Pitcher I, Couture E, Parlow S, Faraz M, Visintini S, Simard T, Di Santo P, Mathew R, et al. Left ventricular unloading during extracorporeal membrane oxygenation in patients with cardiogenic shock. J Am Coll Cardiol. 2019;73(6):654–662. doi: 10.1016/j.jacc.2018.10.085. [DOI] [PubMed] [Google Scholar]
- 64.Conrad SA, Grier LR, Scott LK, Green R, Jordan M. Percutaneous cannulation for extracorporeal membrane oxygenation by intensivists: a retrospective single-institution case series. Crit Care Med. 2015;43(5):1010–1015. doi: 10.1097/CCM.0000000000000883. [DOI] [PubMed] [Google Scholar]
- 65.Keebler ME, Haddad EV, Choi CW, McGrane S, Zalawadiya S, Schlendorf KH, Brinkley DM, Danter MR, Wigger M, Menachem JN, et al. Venoarterial extracorporeal membrane oxygenation in cardiogenic shock. JACC Heart failure. 2018;6(6):503–516. doi: 10.1016/j.jchf.2017.11.017. [DOI] [PubMed] [Google Scholar]
- 66.Burkhoff D, Sayer G, Doshi D, Uriel N. Hemodynamics of mechanical circulatory support. J Am Coll Cardiol. 2015;66(23):2663–2674. doi: 10.1016/j.jacc.2015.10.017. [DOI] [PubMed] [Google Scholar]
- 67.Saxena A, Garan AR, Kapur NK, O'Neill WW, Lindenfeld J, Pinney SP, Uriel N, Burkhoff D, Kern M. Value of hemodynamic monitoring in patients with cardiogenic shock undergoing mechanical circulatory support. Circulation. 2020;141(14):1184–1197. doi: 10.1161/CIRCULATIONAHA.119.043080. [DOI] [PubMed] [Google Scholar]
- 68.Dhruva SS, Ross JS, Mortazavi BJ, Hurley NC, Krumholz HM, Curtis JP, Berkowitz A, Masoudi FA, Messenger JC, Parzynski CS, et al. Association of use of an intravascular microaxial left ventricular assist device vs intra-aortic balloon pump with in-hospital mortality and major bleeding among patients with acute myocardial infarction complicated by cardiogenic shock. JAMA. 2020;323(8):734–745. doi: 10.1001/jama.2020.0254. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 69.Squiers JJ, Lima B, DiMaio JM. Contemporary extracorporeal membrane oxygenation therapy in adults: Fundamental principles and systematic review of the evidence. J Thorac Cardiovasc Surg. 2016;152(1):20–32. doi: 10.1016/j.jtcvs.2016.02.067. [DOI] [PubMed] [Google Scholar]
- 70.Truby LK, Takeda K, Mauro C, Yuzefpolskaya M, Garan AR, Kirtane AJ, Topkara VK, Abrams D, Brodie D, Colombo PC, et al. Incidence and implications of left ventricular distention during venoarterial extracorporeal membrane oxygenation support. ASAIO J. 2017;63(3):257–265. doi: 10.1097/MAT.0000000000000553. [DOI] [PubMed] [Google Scholar]
- 71.Ostadal P, Mlcek M, Kruger A, Hala P, Lacko S, Mates M, Vondrakova D, Svoboda T, Hrachovina M, Janotka M, et al. Increasing venoarterial extracorporeal membrane oxygenation flow negatively affects left ventricular performance in a porcine model of cardiogenic shock. J Transl Med. 2015;13:266. doi: 10.1186/s12967-015-0634-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 72.Bréchot N, Demondion P, Santi F, Lebreton G, Pham T, Dalakidis A, Gambotti L, Luyt CE, Schmidt M, Hekimian G, et al. Intra-aortic balloon pump protects against hydrostatic pulmonary oedema during peripheral venoarterial-extracorporeal membrane oxygenation. Eur Heart J Acute Cardiovasc Care. 2018;7(1):62–69. doi: 10.1177/2048872617711169. [DOI] [PubMed] [Google Scholar]
- 73.Cheng R, Hachamovitch R, Makkar R, Ramzy D, Moriguchi JD, Arabia FA, Esmailian F, Azarbal B. Lack of survival benefit found with use of intraaortic balloon pump in extracorporeal membrane oxygenation: a pooled experience of 1517 patients. J Invasive Cardiol. 2015;27(10):453–458. [PubMed] [Google Scholar]
- 74.Vallabhajosyula S, O'Horo JC, Antharam P, Ananthaneni S, Vallabhajosyula S, Stulak JM, Eleid MF, Dunlay SM, Gersh BJ, Rihal CS, et al. Concomitant intra-aortic balloon pump use in cardiogenic shock requiring veno-arterial extracorporeal membrane oxygenation. Circ Cardiovasc Interv. 2018;11(9):e006930. doi: 10.1161/CIRCINTERVENTIONS.118.006930. [DOI] [PubMed] [Google Scholar]
- 75.Esposito ML, Kapur NK. Acute mechanical circulatory support for cardiogenic shock: the "door to support" time. F1000Research. 2017;6:737. doi: 10.12688/f1000research.11150.1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 76.Thiele H, Jobs A, Ouweneel DM, Henriques JPS, Seyfarth M, Desch S, Eitel I, Pöss J, Fuernau G, de Waha S. Percutaneous short-term active mechanical support devices in cardiogenic shock: a systematic review and collaborative meta-analysis of randomized trials. Eur Heart J. 2017;38(47):3523–3531. doi: 10.1093/eurheartj/ehx363. [DOI] [PubMed] [Google Scholar]
- 77.Badiye AP, Hernandez GA, Novoa I, Chaparro SV. Incidence of hemolysis in patients with cardiogenic shock treated with Impella Percutaneous left ventricular assist device. ASAIO J (Am Soc Artif Internal Organs : 1992). 2016;62(1):11–14. [DOI] [PubMed]
- 78.Mandawat A, Rao SV. Percutaneous mechanical circulatory support devices in cardiogenic shock. Circ Cardiovasc Interv. 2017; 10(5). [DOI] [PMC free article] [PubMed]
- 79.Chen Z, Zhang J, Kareem K, Tran D, Conway RG, Arias K, Griffith BP, Wu ZJ. Device-induced platelet dysfunction in mechanically assisted circulation increases the risks of thrombosis and bleeding. Artif Organs. 2019;43(8):745–755. doi: 10.1111/aor.13445. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 80.Sy E, Sklar MC, Lequier L, Fan E, Kanji HD. Anticoagulation practices and the prevalence of major bleeding, thromboembolic events, and mortality in venoarterial extracorporeal membrane oxygenation: a systematic review and meta-analysis. J Crit Care. 2017;39:87–96. doi: 10.1016/j.jcrc.2017.02.014. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Additional file 1. Supplemental Figures.
Data Availability Statement
All data generated or analyzed during this study are included in this manuscript and its additional files.