Abstract
Background
COVID-19 patients may experience “cytokine storm” when human immune system produces excessive cytokines/chemokines. However, it remains unclear whether early responses of inflammatory cytokines would lead to high or low titers of anti-SARS-CoV-2 antibodies.
Methods
This retrospective study enrolled a cohort of 272 hospitalized patients with laboratory-confirmed SARS-CoV-2. Laboratory assessments of serum cytokines (IL-2R, IL-6, IL-8, IL-10, TNF-α), anti-SARS-CoV-2 IgG/IgM antibodies, and peripheral blood biomarkers were conducted during hospitalization.
Results
At hospital admission, 36.4% patients were severely ill, 51.5% patients were ≥ 65 years, and 60.3% patients had comorbidities. Higher levels of IL-2R and IL-6 were observed in older patients (≥65 years). Significant differences of IL-2R (week 2 to week ≥5 from symptom onset), IL-6 (week 1 to week ≥5), IL-8 (week 2 to week ≥5), and IL-10 (week 1 to week 3) were observed between moderately-ill and severely ill patients. Anti-SARS-CoV-2 IgG titers were significantly higher in severely ill patients than in moderately ill patients, but such difference was not observed for IgM. High titers of early-stage IL-6, IL-8, and TNF-α (≤2 weeks after symptom onset) were positively correlated with high titers of late-stage IgG (≥5 weeks after symptom onset). Deaths were mostly observed in severely ill older patients (45.9%). Survival analyses revealed risk factors of patient age, baseline COVID-19 severity, and baseline IL-6 that affected survival time, especially in severely ill older patients.
Conclusion
Early responses of elevated cytokines such as IL-6 reflect the active immune responses, leading to high titers of IgG antibodies against COVID-19.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12979-022-00271-2.
Keywords: SARS-CoV-2, COVID-19, IgG, IgM, Cytokine dynamics
Introduction
Severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) is the aetiological agent of coronavirus disease 2019 (COVID-19), causing severe pneumonia, multiorgan dysfunction, or even death [1]. During SARS-CoV-2 infection, a large family of cytokines and chemokines are produced by host cells to initiate inflammatory responses and to mediate innate immune responses [2, 3]. Although most COVID-19 patients are asymptomatic or have mild signs [4, 5], those with severe disease may experience a hyperinflammatory state called a “cytokine storm” in which the immune system produces excessive inflammatory cytokines/chemokines that may cause acute respiratory distress, pulmonary edema, and multiorgan failure [6–9].
Previous studies suggest that serum levels of cytokines and chemokines are likely associated with the disease severity and clinical outcomes of COVID-19 [10–19]. Many COVID-19 patients have been diagnosed with abnormal production of serum cytokines and chemokines such as interleukin-6 (IL-6) [10, 19], IL-1α [11], IL-1β [12], IL-2 receptor (IL-2R) [13], IL-3 [14], IL-7 [20], IL-8 [15], IL-10 [21], IL-13 [22], IL-18 [12], IL-37 [18], tumor necrosis factor-α (TNF-α) [19] and transforming growth factor-β [23], especially in severe and critical cases.
Among the long list of cytokines/chemokines, IL-6 has been recognized as a key COVID-19-associated cytokine. First, IL-6 may serve as an early biomarker to monitor inflammatory and immune responses in COVID-19 patients. Early diagnosis of serum IL-6 can be achieved within the first 10 days after symptom onset; other cytokines are often detected at the later stage [2]. The early responses of elevated IL-6 expression might drive activation of T cell immunity against COVID-19 [24]. Second, baseline IL-6 is a promising predictor of disease severity and mortality during hospitalization of COVID-19 patients [19]. Elevated production of IL-6 in severe cases is likely associated with reduced levels of granzyme A-expressing natural killer cells, indicating impaired immune cell cytotoxicity [25]. Even at 8 months after viral infection, inflammatory biomarkers such as IL-6, interferon-β, and interferon-λ2/3 remain persistently high in COVID-19 survivors [26]. Third, IL-6 has been identified as a COVID-19-associated cytokine by many independent studies [10, 11, 24, 27], while other biomarkers have not been consistently reported in the literature. Overall, elevated expression of serum IL-6 is associated with adverse clinical outcomes and mortality in COVID-19 patients [19], and the IL-6 receptor antagonists such as tocilizumab may reduce 28-day all-cause mortality in hospitalized patients with COVID-19 [28]. Moreover, higher expressions of epithelial cell-derived IL-6 and myeloid-derived IL-1β in lung tissues are distinguishing features of COVID-19 compared with healthy controls, influenza pneumonia, bacterial pneumonia, and acute respiratory distress syndrome [29]. Despite this knowledge, it remains unclear to date whether serum levels of cytokines such as IL-6 are associated with anti-SARS-CoV-2 antibody responses.
During the innate immune response to SARS-CoV-2 infection, inflammatory cytokines are produced at the early stage [30]. Later, emergence of adaptive immune responses leads to production of anti-SARS-CoV-2 antibodies, such as IgM and IgG, which ideally deliver long-term protection [31]. Although the importance of IgM and IgG antibodies is known, it remains unclear whether the late-stage responses of anti-SARS-CoV-2 IgG/IgM antibodies could be predicted by the early responses of inflammatory cytokines. To investigate this hypothesis, we conducted this retrospective study. To avoid the impact of different vaccines, cytokine inhibitors and circulating SARS-CoV-2 variants, we evaluated a cohort of laboratory-confirmed COVID-19 patients who received neither vaccines nor cytokine inhibitors.
Methods
Study design and participants
We performed a retrospective study to collect cytokine and antibody records of hospitalized COVID-19 patients during the early outbreak of the pandemic (January to March 2020) when approved vaccines and cytokine-targeted drugs were not available or administered. We analyzed a cohort of 272 COVID-19 patients who were hospitalized from 2020/02/01 to 2020/03/31 in the Sino-French New-City Tongji Hospital in Wuhan, China. At hospital admission, all patients were confirmed to have SARS-CoV-2 infection based on real-time RT–PCR tests of nasopharyngeal swab specimens. During their hospitalization, all patients received neither vaccines nor cytokine-targeted drugs, according to the COVID-19 guidelines before 2020 April. Archived records during the inpatient hospital stay were analyzed in this retrospective study; thereby, written informed consent was waived. This study was conducted under the Helsinki Declaration and was approved by the Ethics Committees of The Second Xiangya Hospital (approval ID: LYF2020060).
Based on the New Coronavirus Diagnosis and Treatment Guidelines in China, a severely ill case was identified if any of the following five conditions were fulfilled at baseline or during hospitalization: (i) the breathing rate of ≥30 breaths per minute; (ii) oxygen saturation of ≤93% at rest; (iii) PaO2/FiO2 (artery partial pressure of oxygen / inspired oxygen fraction) ≤300 mmHg; (iv) chest imaging tests that exhibit > 50% progression of lung lesions within 48 h; and (v) shock or organ failure that requires intensive care unit, or respiratory failure that requires mechanical ventilation. Moderately ill cases were defined based on mild/moderate symptoms of fever, respiratory difficulties, and/or radiological findings of pneumonia.
Data collection
Electronic medical records of COVID-19 patients were retrieved to collect datasets of epidemiological and demographic information, laboratory biomarkers, onset symptoms, disease severity and clinical comorbidities at hospital admission. All medical records were retrieved based on a standard collection form from the Sino-French New-City Tongji Hospital. Two authors (XJ, TY) cross-checked the medical records and communicated with doctors for data accuracy.
Laboratory examinations
Real-time RT–PCR tests were performed to detect SARS-CoV-2 nucleic acid; the detailed protocols were described previously [32]. During hospitalization, serial monitoring of 30 laboratory biomarkers (Table S1) was conducted for each COVID-19 patient, and blood samples were collected at different time points when laboratory biomarkers were requested by physicians to monitor disease progression. Laboratory biomarkers, such as routine peripheral blood biomarkers, inflammatory biomarkers, coagulation biomarkers, serum biochemical biomarkers, and anti-SARS-CoV-2 IgG and IgM antibodies, were assessed during hospitalization. Peripheral blood was collected for routine blood tests using an automated hematology analyzer. Biochemical biomarkers such as albumin, alanine aminotransferase, aspartate aminotransferase, and creatinine were measured using a Roche automated clinical chemistry analyzer (Roche Diagnostics). Coagulation tests were conducted with a new coagulation analyzer, STAR Max® (Diagnostica Stago). Serum quantitative measurements of anti-SARS-CoV-2 IgM and IgG antibodies were conducted using commercial chemiluminescence kits of iFlash-SARS-CoV-2 IgM (Cat. No. C86095M) and iFlash-SARS-CoV-2 IgG (Cat. No. C86095G) from Shenzhen YHLO Biotech. Seroconversion was defined by the cutoff of IgG ≥ 10 AU/mL or IgM ≥ 10 AU/mL.
Statistical analysis
We analyzed either the proportion of categorical variables or the median/interquartile range (IQR) of continuous variables. Chi-square tests were applied to compare proportions of categorical variables, and Fisher’s exact tests were applied within the context of limited data. Logarithmic transformation of continuous variables with all-positive data was conducted, and normality tests of continuous variables on the original scale and the log-transformed scale were performed using Shapiro-Wilk tests. We employed two-tailed t-tests for continuous variables following normal distributions, Wilcoxon rank-sum tests for non-normal continuous variables in paired groups, and Kruskal-Wallis tests for non-normal continuous variables in unpaired groups. To analyze correlations between biomarkers, Pearson’s and Spearman’s correlation coefficients were measured for normal and non-normal continuous variables, respectively. Hierarchical clustering analysis was applied to show clustering of correlating biomarkers. Cox proportional hazards models were utilized in survival analyses to assess hazard ratios (HR) indicating the effects of risk factors on survival outcomes: either death for non-survivors or hospital discharge for survivors. Baseline values of all factors were initiated in univariate survival analysis, and significant variables were subsequently used as inputs in stepwise multivariate survival analyses. Kaplan-Meier curves were built to show survival time and log-rank tests were used to compare survival distributions between different groups. The pairwise deletion approach was applied to handle missing data. All statistical analyses were descriptive, and no random sampling was conducted. For all statistical tests, two-sided tests at the level of < 0.05 were considered significant. Above statistical analyses were performed using MATLAB R2016.
Results
Baseline characteristics of COVID-19 patients
A cohort of 272 hospitalized patients with laboratory-confirmed COVID-19 were enrolled in this retrospective study. At hospital admission, 99 (36.4%) patients were severely ill, 139 (51.1%) were males, and 164 (60.3%) had comorbidities (Table 1). Moreover, 64.6% (64/99) of the severely ill patients were males, and most males (66%) had comorbidities. The most common symptom was fever (85.3%), followed by cough (62.1%), fatigue (37.9%), and shortness of breath (33.5%).
Table 1.
A cohort of hospitalized patients with laboratory-confirmed COVID-19
| Characteristics | Total (N = 272) |
Patients aged < 65 y (N = 132) |
Patients aged ≥ 65 y (N = 140) |
P-value* | ||
|---|---|---|---|---|---|---|
| Moderate (N = 95) |
Severe (N = 37) |
Moderate (N = 78) |
Severe (N = 62) |
|||
| Male gender | 139 (51.1%) | 36 (37.9%) | 25 (67.6%) | 39 (50%) | 39 (63%) | 0.003 |
| Age (years) | 65 (56–72) | 54 (43–60) | 57 (50–62) | 70 (68–75) | 72 (69–78) | < 0.01 |
| Baseline symptoms | ||||||
| Fever | 232 (85.3%) | 83 (87.4%) | 29 (78.4%) | 67 (85.9%) | 53 (85.5%) | 0.62 |
| Cough | 169 (62.1%) | 57 (60.0%) | 24 (64.9%) | 49 (62.8%) | 39 (62.9%) | 0.95 |
| Fatigue | 103 (37.9%) | 33 (34.7%) | 16 (43.2%) | 25 (32.1%) | 29 (46.8%) | 0.25 |
| Shortness of breath | 91 (33.5%) | 27 (28.4%) | 16 (43.2%) | 21 (26.9%) | 27 (43.5%) | 0.07 |
| Chills | 72 (26.5%) | 24 (25.3%) | 10 (27.0%) | 18 (23.1%) | 20 (32.3%) | 0.67 |
| Diarrhea | 71 (26.1%) | 25 (26.3%) | 9 (24.3%) | 19 (24.4%) | 18 (29.0%) | 0.93 |
| Myalgia | 63 (23.2%) | 24 (25.3%) | 10 (27.0%) | 15 (19.2%) | 14 (22.6%) | 0.74 |
| Headache | 35 (12.9%) | 15 (15.8%) | 5 (13.5%) | 6 (7.7%) | 9 (14.5%) | 0.43 |
| Nausea | 30 (11.0%) | 12 (12.6%) | 5 (13.5%) | 6 (7.7%) | 7 (11.3%) | 0.71 |
| Vomit | 18 (6.6%) | 6 (6.3%) | 2 (5.4%) | 4 (5.1%) | 6 (9.7%) | 0.72 |
| Abdominal pain | 11 (4.0%) | 5 (5.3%) | 1 (2.7%) | 3 (3.8%) | 2 (3.2%) | 0.88 |
| Blood cough | 5 (1.8%) | 1 (1.1%) | 0 (0.0%) | 1 (1.3%) | 3 (4.8%) | 0.36 |
| Baseline comorbidity | ||||||
| Hypertension | 114 (41.9%) | 21 (22.1%) | 16 (43.2%) | 42 (53.8%) | 35 (56.5%) | < 0.01 |
| Diabetes mellitus | 71 (26.1%) | 18 (18.9%) | 9 (24.3%) | 20 (25.6%) | 24 (38.7%) | 0.05 |
| Cardiovascular disease | 22 (8.1%) | 2 (2.1%) | 1 (2.7%) | 10 (12.8%) | 9 (14.5%) | 0.008 |
| Cancer | 13 (4.8%) | 4 (4.2%) | 0 (0.0%) | 6 (7.7%) | 3 (4.8%) | 0.34 |
| Cerebrovascular disease | 10 (3.7%) | 1 (1.1%) | 1 (2.7%) | 3 (3.8%) | 5 (8.1%) | 0.15 |
| Chronic bronchitis | 8 (2.9%) | 2 (2.1%) | 0 (0.0%) | 3 (3.8%) | 3 (4.8%) | 0.50 |
| Cholecystitis | 3 (1.1%) | 0 (0.0%) | 0 (0.0%) | 2 (2.6%) | 1 (1.6%) | 0.44 |
| COPD# | 2 (0.7%) | 1 (1.1%) | 0 (0.0%) | 0 (0.0%) | 1 (1.6%) | 0.65 |
| Comorbidity count | < 0.01 | |||||
| 0 | 108 (40%) | 62 (65%) | 15 (40%) | 18 (23%) | 13 (21%) | |
| 1 | 95 (35%) | 18 (19%) | 17 (46%) | 35 (45%) | 25 (40%) | |
| 2 | 46 (17%) | 12 (13%) | 4 (11%) | 17 (22%) | 13 (21%) | |
| ≥3 | 23 (8%) | 3 (3%) | 1 (3%) | 8 (10%) | 11 (18%) | |
| Clinical outcome | ||||||
| Death | 42 (15.4%) | 2 (2.2%) | 11 (29.7%) | 1 (1.3%) | 28 (45.2%) | < 0.01 |
| Length of hospital stay (days) | 21 (12–29) | 17 (10–23) | 19 (13–31) | 23 (18–33) | 25 (10–33) | < 0.01 |
*: P-values were measured by multigroup tests of variables in four patient groups (discrete variables: chi-squared tests, continuous variables: Kruskal-Wallis tests)
#: COPD: chronic obstructive pulmonary disease
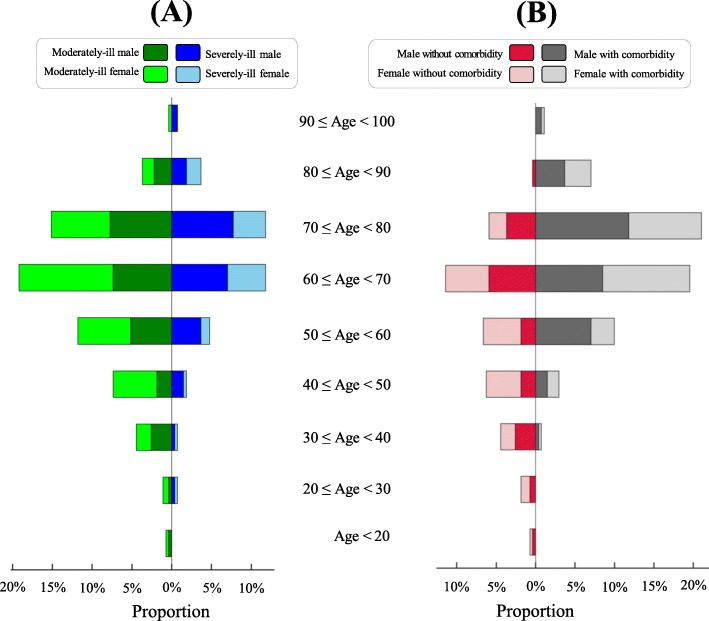
Age distribution is shown in Fig. 1. The median age was 65 years (interquartile range: 56 to 72 years); the youngest patient was a 14-year-old female and the oldest a 92-year-old male. Subsequently, two patient groups were defined: age < 65 years (N = 132) and age ≥ 65 years (N = 140). The proportion of males was higher in patients aged ≥65 years than in those aged < 65 years (55.7% versus 46%, p-value = 0.12). Compared with patients aged < 65 years, older patients had more severe cases (44.3% versus 28%, p-value < 0.01) and comorbidities (77.9% versus 41.7%, p-value < 0.01). In patients aged ≥65 years, highly prevalent comorbidities included hypertension (55%), diabetes mellitus (31.4%), and cardiovascular disease (13.6%, Table 1).
Fig. 1.
Age distribution of 272 hospitalized patients with COVID-19. A Proportions of COVID-19 males/females who were moderately-ill (left) or severely-ill (right) at hospital admission. B Proportions of COVID-19 males/females without any comorbidity (left) or with comorbidity (right) at hospital admission
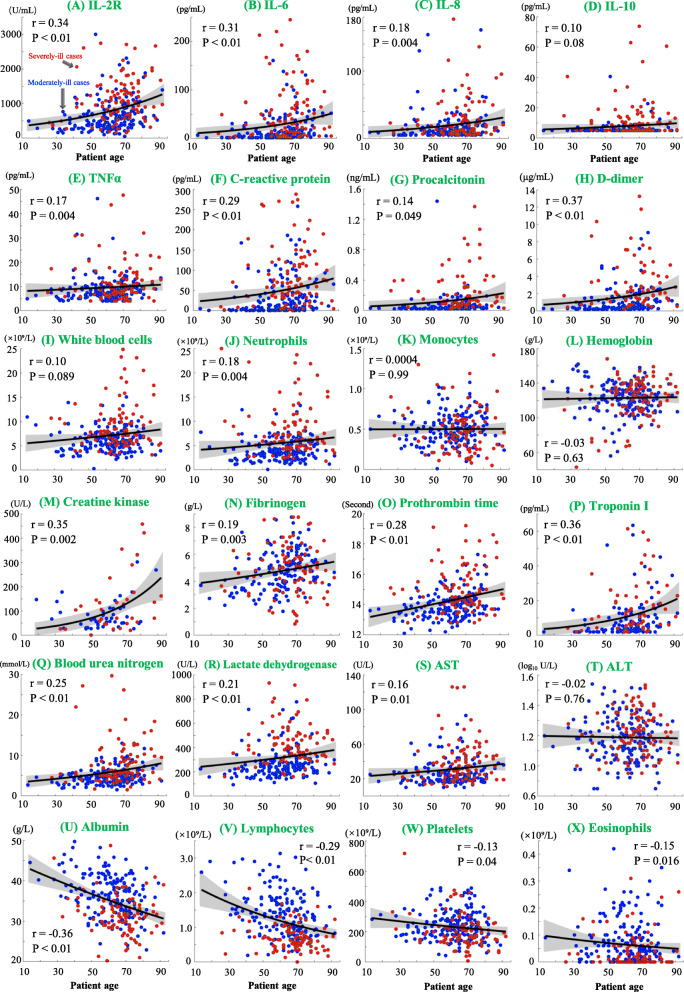
Baseline levels of blood biomarkers were associated with patient age in subsets of moderately ill patients and severely ill patients. As shown in Fig. 2, increasing age correlated positively with serum levels of individual biomarkers, including IL-2R, IL-6, C-reactive protein, D-dimer, creatine kinase, and troponin I (p-values < 0.05). In contrast, patient age correlated negatively with the decreasing levels of biomarkers, including albumin, lymphocytes, eosinophils, and platelets (p-values < 0.05).
Fig. 2.
Correlation of baseline biomarkers with patient age. Red and blue dots indicate results from severely-ill and moderately-ill patients, respectively. The fitted linear polynomial curves and 95% confidence interval bounds are shown by black lines and gray area, respectively. Pearson’s correlation coefficients were measured for albumin (g/L), fibrinogen (g/L) and ALT (log10 U/L), while Spearman’s correlation coefficients were measured for other biomarkers whose distributions were not normal. Correlation coefficients (r) and their p-values (P) are shown
Dynamics of cytokines and blood biomarkers during disease progression
To monitor disease progression, 1769 blood samples were collected from 272 COVID-19 patients to measure the serum levels of cytokines (IL-2R, IL-6, IL-8, IL-10, TNF-α) and blood biomarkers during the hospitalization. Blood samples were collected at the time of physician requests (usually once per week). Because patient age plus disease severity may play a role in biomarker dynamics, our subsequent analyses focused on the weekly dynamics of the above biomarkers in four subgroups: (i) moderately ill patients aged < 65 years, (ii) severely ill patients aged < 65 years, (iii) moderately ill patients aged ≥65 years, and (iv) severely ill patients aged ≥65 years.
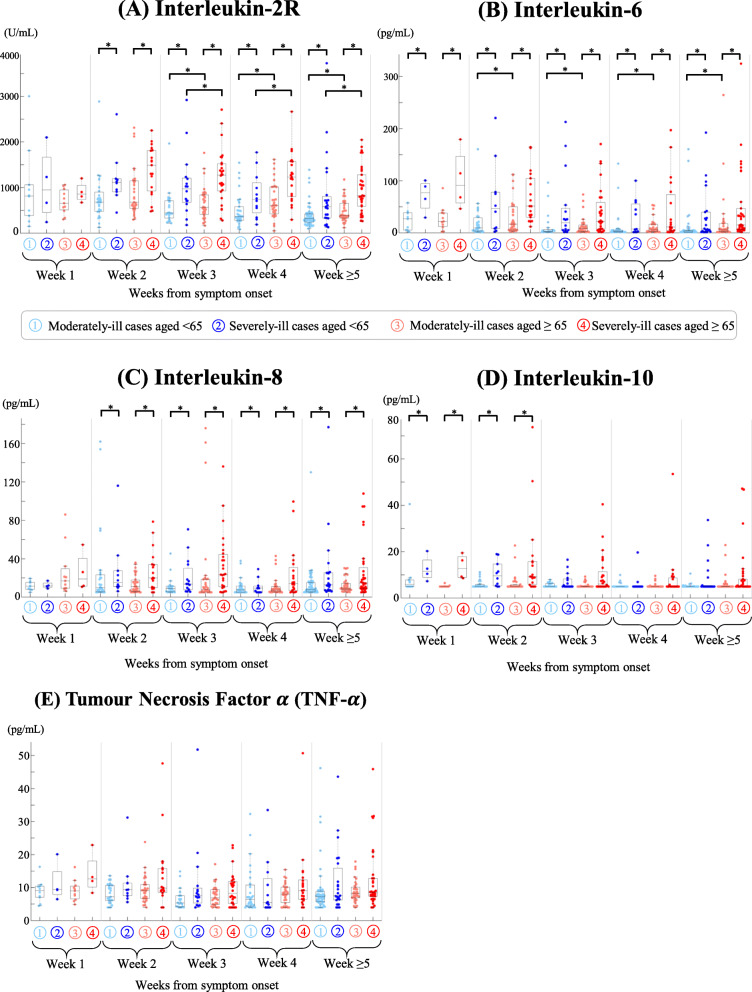
Serum levels of IL-2R, IL-6, IL-8, and IL-10 were higher in severely-ill patients than in moderately ill patients. Significant differences in IL-2R (week 2 to week ≥5, Fig. 3A), IL-6 (week 1 to week ≥5, Fig. 3B), IL-8 (week 2 to week ≥5, Fig. 3C), and IL-10 (week 1 to week 2, Fig. 3D) were observed in the comparison of moderately ill versus severely ill patients aged < 65 as well as moderately ill versus severely ill patients aged ≥65 years. Serum levels of TNF-α were slightly higher in severely ill patients, but no significant difference was found within the context of COVID-19 severity and patient age (Fig. 3E).
Fig. 3.
Dynamics of five cytokines (IL-2R, IL-6, IL-8, IL-10, TNF-α) in COVID-19 patients during hospitalization. Four patient groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patient aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patient aged ≥65 years). Due to their non-normality, cytokine levels were compared using Wilcoxon rank-sum tests. A significant difference (p-value < 0.05) was highlighted by an asterisk *. One sample from each patient was obtained from week 1, week 2, week 3, week 4 to week ≥5 after symptom onset. If one patient had multiple tests within one week, median results were obtained for our analysis
Analyses of 24 non-cytokine biomarkers revealed their possible associations with disease severity and patient age (Fig. S1-S4). Among these biomarkers, serum levels of six biomarkers (D-dimer, C-reactive protein, procalcitonin, lymphocytes, neutrophils, albumin) consistently showed increasing or decreasing patterns in the four patient subgroups (Fig. S1).
IgG and IgM dynamics during disease progression
Serum levels of anti-SARS-CoV-2 IgG and IgM antibodies were measured in a subcohort of 162 patients with COVID-19. The earliest date and the latest date of IgG/IgM tests was 10 days and 76 days after symptom onset, respectively. Note that all blood samples were collected during the hospitalization, such that IgG/IgM tests were not conducted before hospital admission or after hospital discharge.
Based on the collection of blood samples during hospitalization, IgG titers were higher in severely ill patients than in moderately ill patients (median: 187.7 versus 137.5 AU/mL, p-value < 0.01, Fig. 4A). The dynamics of IgG titers changed during disease progression, and with a steady IgG increase in the first 4 weeks (Fig. 4B). From week 5 to week 10, a decline in IgG titers was observed in moderately ill patients, whereas severely ill patients maintained relatively higher levels of IgG titers even at week 10 (Fig. 4B). Comparisons of IgM titers showed no significant difference with regard to patient age and COVID-19 severity (Fig. 4C). A similar pattern of IgM dynamics was observed in both moderately-ill and severely-ill patients, though IgM was almost undetectable at week 10 (Fig. 4D). In total, 86.7% of survivors and 100% of non-survivors experienced IgG seroconversion (IgG ≥10 AU/mL) and/or IgM seroconversion (IgM ≥10 AU/mL).
Fig. 4.
Serum levels of anti-SARS-CoV-2 IgG and IgM antibodies. A IgG levels in four patient groups: moderately-ill patients aged < 65 years (light blue), severely-ill patients aged < 65 years (blue), moderately-ill patients aged ≥65 years (light red), and severely-ill patients aged ≥65 years (red). IgG data was collected across all timepoints. B Polynomial regression of IgG was applied to fit the dynamic patterns of IgG from symptom onset to clinical outcomes (hospital discharge or death). C IgM levels in four patient groups. D Polynomial regression of IgM dynamics from symptom onset to clinical outcomes
Anti-SARS-CoV-2 IgG responses are associated with early-stage cytokines
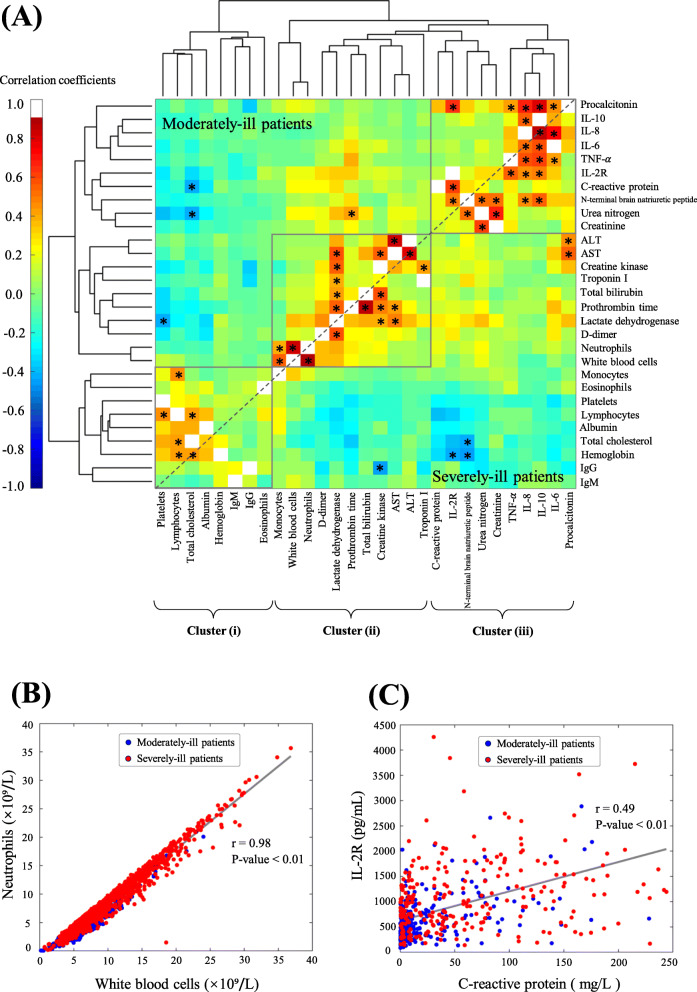
Given that many blood biomarkers are assessed in clinical diagnosis, we determined whether these biomarkers correlate with each other within the context of COVID-19 severity. Pairwise correlation coefficients were measured based on all available data for moderately ill and severely-ill patients (Fig. 5A). The highest correlation coefficient (r = 0.98, p-value < 0.01) was identified between white blood cells and neutrophils (Fig. 5B), and this is confirmed by the fact that neutrophils represent the most plentiful type of white blood cells. Clustering analyses further revealed three major clusters of biomarkers: (i) IgG, IgM, eosinophils, platelets, lymphocytes, albumin, total cholesterol, and hemoglobin; (ii) AST, ALT, D-dimer, lactate dehydrogenase, prothrombin time, total bilirubin, troponin I, and creatine kinase; and (iii) IL-2R, IL-6, IL-8, IL-10, TNF-α, procalcitonin, creatinine, C-reactive protein, N-terminal brain natriuretic peptide, creatinine, and urea nitrogen (Fig. 5A). In cluster (i), IgG and IgM were closely correlated in the same branch. In cluster (ii), known biomarkers such as white blood cells and neutrophils were clustered. Four cytokines (IL-6, IL-8, IL-10, and TNF-α) were clustered in the cluster (iii). IL-2R correlated positively with C-reactive protein (Fig. 5C), a biomarker known for its response to infection and/or inflammation.
Fig. 5.
Clustering analyses of biological biomarkers in COVID-19 patients. A Hierarchical clustering of 29 biological biomarkers based on the subsets of moderately-ill patients (top left) and severely-ill patients (bottom right). The significance of any correlation coefficient (absolute value > 0.4 and p-value < 0.05) was highlighted by an asterisk *. Three clusters (i), (ii), and (iii) were indicated based on the hierarchical clustering. B Plots of white blood cells versus neutrophils. C Plots of C-reactive protein versus IL-2R
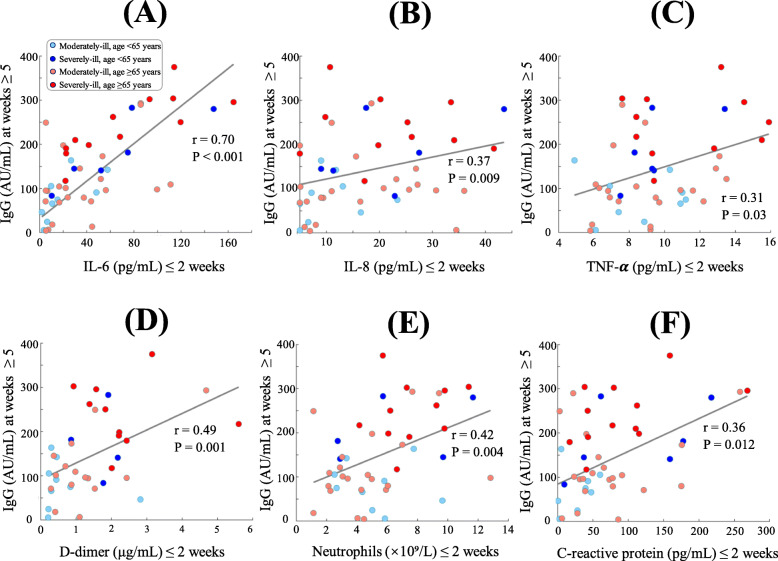
We next asked whether late-stage IgG responses (from week 5 to 10) are associated with early-stage biomarker responses (≤ 2 weeks) in COVID-19 patients. To this end, we analyzed a subcohort of 47 hospitalized patients whose blood samples were tested within two weeks after symptom onset and whose late-stage IgG titers were also tested from weeks 5 to 10. Among all available biomarkers, early responses of six biomarkers (IL-6, IL-8, TNF-α, D-dimer, neutrophils, C-reactive protein) correlated significantly with high titers of anti-SARS-CoV-2 IgG antibodies (p-values < 0.05) (Fig. 6). Of note, the pairwise correlation coefficient between early-stage IL-6 and late-stage IgG was 0.70 (p-value < 0.001, Fig. 6A) and a linear regression model could be built as Y = 71.62 + 1.62X (R2: 49.26%) to predict late-stage IgG responses (the variable Y) based on early-stage IL-6 levels (the variable X). This significant correlation was independently observed in the subsets of moderately-ill patients (r = 0.62, p-value < 0.001) and severely-ill patients (r = 0.83, p-value < 0.001). Due to a steady decrease in IgM titers from ≥5 weeks, significant correlations of IgG titers with early-stage biomarkers were not observed.
Fig. 6.
Scatter plots of early-stage biomarkers (≤ 2 weeks from symptom onset) versus late-stage IgG (≥ 5 weeks from symptom onset) in COVID-19 patients. Serum levels of cytokines IL-6 (A), IL-8 (B), TNF-α (C) at the early stage of ≤2 weeks from symptom onset are positively correlated with the response of IgG at the late stage of ≥5 weeks from symptom onset. Positive correlations with IgG responses were also observed for D-dimer (D), neutrophils (E), and C-reactive protein (F). Spearman’s correlation coefficients (r) and their p-values (P) are shown
Risk factors associated with the mortality of COVID-19 patients
In our cohort of 272 hospitalized patients, 42 (15.4%) died, and the median length of hospital stay was 21 days (Table 1). Deaths mostly occurred in severely ill patients, both aged ≥65 years (45.9%) and < 65 years (31.4%). In contrast, few deaths were observed in moderately-ill patients aged < 65 years (2.2%) and ≥ 65 years (1.3%). Moreover, the median length of hospital stay was longer in patients aged ≥65 than in those aged < 65 years (23 versus 18 days, p-value = 0.0003).
Using 62 baseline parameters (patient age, gender, baseline disease severity, symptoms, comorbidities, blood biomarkers) as predictors, Cox proportional hazards models were applied to analyze risk factors potentially associated with the clinical outcome of either death for non-survivors or hospital discharge for survivors (Table 2). Univariate survival analyses identified 24 of 62 baseline parameters as risk factors, such as male sex, patient age, and baseline severity (p-values < 0.05, Table 2). These 24 risk factors were used as inputs in multivariate survival analyses, which further identified four risk factors: patient age (hazard ratio (HR): 1.07, p-value = 0.002), baseline severity (HR: 33.7, p-value = 0.0009), baseline D-dimer (HR: 1.09, p-value = 0.008), and baseline IL-6 (HR: 1.12, p-value = 0.025).
Table 2.
Risk factors associated with the clinical outcome (death or hospital discharge) of COVID-19 patients using Cox proportional hazards models
| Univariate analysis* | Multivariate analysis | |||
|---|---|---|---|---|
| HR (95% CI) | P-value | HR (95% CI) | P-value | |
| Male gender | 2.23 (1.60 to 3.12) | 0.016 | ||
| Patient age & | 1.05 (1.03 to 1.06) | 9.8 × 10−4 | 1.07 (1.04 to 1.09) | 0.002 |
| Baseline disease severity | 24.2 (13.3 to 44.1) | 1.1 × 10−7 | 38.0 (12.9 to 111.3) | 7 × 10− 4 |
| Baseline symptoms | ||||
| Fatigue | 2.02 (1.48 to 2.75) | 0.023 | ||
| Baseline comorbidity | ||||
| Cardiovascular disease | 2.33 (1.54 to 3.53) | 0.041 | ||
| Blood routine biomarkers | ||||
| White blood cells | 1.18 (1.15 to 1.21) | 3 × 10−10 | ||
| Neutrophils | 1.14 (1.11 to 1.16) | 2.2 × 10−9 | ||
| Lymphocytes | 0.03 (0.02 to 0.06) | 6 × 10− 10 | ||
| Coagulation biomarkers | ||||
| D-dimer | 1.10 (1.08 to 1.12) | 5.4 × 10−8 | 1.09 (1.06 to 1.13) | 0.006 |
| Prothrombin time | 1.57 (1.43 to 1.72) | 9.6 × 10−7 | ||
| Biochemistry biomarkers | ||||
| Albumin | 0.85 (0.82 to 0.87) | 4.8 × 10−4 | ||
| Aspartate aminotransferase | 1.02 (1.01 to 1.03) | 6.2 × 10− 4 | ||
| Total cholesterol | 0.56 (0.46 to 0.67) | 0.0017 | ||
| Total bilirubin | 1.08 (1.06 to 1.11) | 0.0001 | ||
| Blood urea nitrogen | 1.15 (1.12 to 1.17) | 8.3 × 10−3 | ||
| Creatinine | 1.02 (1.01 to 1.02) | 6.3 × 10−5 | ||
| Cardiac biomarkers | ||||
| Troponin I | 1.03 (1.02 to 1.03) | 5 × 10−3 | ||
| Myocardial creatine kinase | 1.38 (1.29 to 1.49) | 7.6 × 10−6 | ||
| Inflammatory biomarkers | ||||
| C-reactive protein | 1.01 (1.01 to 1.01) | 5.9 × 10−9 | ||
| Procalcitonin | 8.38 (5.56 to 12.6) | 2.2 × 10−7 | ||
| IL-6 | 1.11 (1.10 to 1.13) | 3 × 10−14 | 1.12 (1.10 to 1.14) | 0.025 |
| IL-8 | 1.02 (1.01 to 1.02) | 6.2 × 10−7 | ||
| IL-10 | 1.03 (1.02 to 1.04) | 2.7 × 10−4 | ||
| TNF-α | 1.04 (1.03 to 1.06) | 6.6 × 10−3 | ||
*: A total of 62 biomarkers were tested in our survival analysis and only variables with a significant hazard ratio (HR) at the significance level of p-value < 0.05 are listed in the table
&: Increase per year
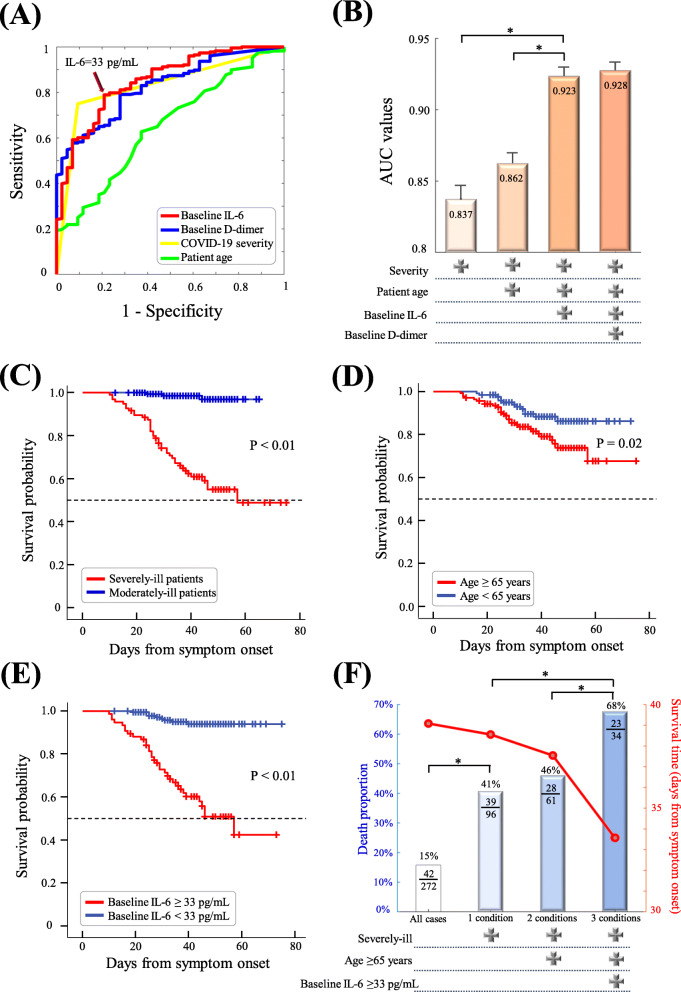
In predicting COVID-19 mortality, Fig. 7A shows the area under the curve for each individual factor, including patient age (AUC: 0.65, p-value = 0.001), baseline severity (AUC: 0.837, p-value < 0.01), baseline D-dimer (AUC: 0.827, p-value < 0.01), and baseline IL-6 (AUC: 0.856, p-value < 0.01). Of note, the area under the curve for three factors (patient age, baseline severity, baseline IL-6) reached 0.923 (Fig. 7B). Kaplan-Meier curves were subsequently evaluated to examine whether these three risk factors affect the survival time from symptom onset. The mean survival time was significantly different in comparisons of severely-ill versus moderately-ill patients (p-value < 0.01, Fig. 7C), patients aged ≥65 versus < 65 (p-value =0.02, Fig. 7D), and patients with baseline IL-6 ≥ 33 pg/mL versus IL-6 < 33 pg/mL (p-value < 0.01, Fig. 7E). Compared with the overall cohort, the mortality rate was significantly higher in the subgroup of patients with these risk factors, especially severely-ill old patients with IL-6 ≥ 33 pg/mL at baseline (Fig. 7F).
Fig. 7.
Survival analysis and area under the curves of risk factors. A Area under the curves (AUC) of baseline factors in the prediction of COVID-19 mortality. The cutoff of IL-6 at 33 pg/mL (sensitivity: 79%, specificity: 81%) was optimized by the highest point of AUC based on the Cutoff Finder tool (https://molpathoheidelberg.shinyapps.io/CutoffFinder_v1/). B AUC values in the stepwise combination of four baseline factors. Kaplan-Meier curves are shown for severely-ill versus moderately-ill patients (C), patients aged < 65 versus ≥65 years (D), patients with baseline IL-6 ≥ 33 pg/mL versus patients with IL-6 < 33 pg/mL (E). F Mortality rate and survival time of patients with the combined conditions of severely-ill, age ≥ 65, and baseline IL-6 ≥ 33 pg/mL
Discussion
At the early stage, invasion of SARS-CoV-2 leads to activation of innate immunity and dendritic cells with excessive release of cytokines (e.g., IL-6, TNF-α) and chemokines (e.g., CCL20, CXCL1, CXCL2), thereafter driving induction of SARS-CoV-2-specific B cell and T cell responses [33]. Subsequently, plasma B cells are responsible for production of anti-SARS-CoV-2 IgG and IgM antibodies that act in adaptive immune responses [2, 3]. Our study was initiated to test the hypothesis of whether early responses of cytokines are associated with late-stage responses of anti-SARS-CoV-2 IgG/IgM antibodies. As of January 2022, the majority of the populations has been vaccinated (> 90% in China), and many cytokine-targeted drugs (e.g., tocilizumab [34]) are widely used in clinical practice [35]. For this reason, we decided to perform a retrospective study to collect detailed cytokine and antibody records for hospitalized COVID-19 patients during the early outbreak of the pandemic when vaccines and cytokine-targeted drugs were not available or administered. Based on detailed records of hospitalized patients, our findings can be briefly summarized, as indicated below. (i) Serum levels of certain cytokines and antibodies are associated with patient age and COVID-19 severity at baseline. Older patients with severe COVID-19 usually have higher levels of serum IL-6 and IgG antibodies. (ii) Baseline factors such as patient age, disease severity, and IL-6 are early predictors of clinical outcomes among COVID-19 patients. (iii) Early-stage cytokines such as IL-6 correlate positively with late-stage IgG responses, especially in older patients.
In agreement with previous studies [36–38], our analyses of cytokine profiles revealed different dynamics of IL-2R, IL-6, IL-8, IL-10, and TNF-α during the disease progression of COVID-19. We observed that serum IL-6 exhibited an early response to disease severity even at the first week after symptom onset, supporting its role as an early predictor of severe disease (Fig. 3B). This is in agreement with previous studies that showed IL-6 to be a sensitive and specific predictor of disease severity [19, 39] and clinical outcomes such as death and respiratory failure [40–42]. Moreover, we observed that IL-6 and IL-2R were associated with older age and disease severity (Fig. 3A, B). A meta-analysis also reported that older age might significantly influence the association of IL-6 with clinical outcomes [43]. Such age-severity association indicates the existence of age-associated immune signatures and the need for better clinical management of severely-ill older patients [44]. In addition to IL-6 and IL-2R, we observed associations of serum IL-8 and IL-10 with disease severity, which is in agreement with previous studies [19, 37, 45]. Our univariate survival analyses suggested that IL-6, IL-8, IL-10, and interferon-α are risk factors significantly associated with the clinical outcome of death; IL-6 remained a key factor in the multivariate survival model (Table 2). The role of IL-6 in the disease progression of COVID-19 has been widely recognized [46], and IL-6 blockade possibly reduce the systemic inflammation [47]. Although an IL-6 inhibitor called tocilizumab offered a modest reduction in mortality (31% vs. 35%) in the RECOVERY trial [48], other clinical trials (e.g., the REMAP-CAP trial) showed no benefit of IL-6 inhibition in reducing mortality [47, 49]. Future studies are needed to address whether antagonists of IL-6 and its receptor would be beneficial for better clinical outcomes.
Responses to anti-SARS-CoV-2 antibodies are associated with many baseline factors such as COVID-19 severity, patient age, and baseline symptoms [50–53]. Our analyses showed a steady increase in anti-SARS-CoV-2 IgG titers in the first month after symptom onset, and severely ill patients maintained relatively high levels of IgG even at week 10 (Fig. 4). In contrast, IgM peaked at nearly 5 weeks after symptom onset and almost disappeared by week 10. In agreement with previous results, IgM antibodies, accounting for approximately 10% of human immunoglobulins, are often produced during the early phase of acute infection [50]. IgG antibodies, accounting for approximately 75% of human immunoglobulins, provide long-term immunity after viral infection [50]. In an Italian study of asymptomatic to critically ill patients, IgM seroconversion disappeared at 4 months and 47% of IgG seroconversion was observed at 10 months after symptom onset [51]. A Brazilian study reported a 30.4% loss of IgG reactivity after 90 days of symptom onset [52]. A Chinese study also showed the maintenance of IgG responses even up to 10 months after infection [53]. In agreement with our findings, a previous study observed higher titers of IgG antibodies in severely ill older patients, and the antibody decline was associated with antibody titers and symptoms at baseline [51].
Age-related features of COVID-19 cytokine profiles and immune responses have been observed by our study and in other studies [54–56]. We detected different levels of serum IL-6, IL-2R, albumin, D-dimer, and C-reactive protein between young and older patients (Fig. 3, Fig. S1). Patient age was also a key risk factor in our survival analysis (Table 2). Ageing is associated with elevated systemic levels of inflammatory cytokines (e.g., IL-6, IL-8, TNF-α, IL-13, interferon-γ) as well as acute-phase proteins [57]. Older patients ≥65 years may experience impaired adaptive responses with the scarcity of naïve T cells, therefore failing to activate antigen-specific responses to control COVID-19 [55]. Older patients may experience immunosenescence with ineffective viral responses to fight COVID-19 due to age-related biological changes (e.g., impaired innate immune responses), chronic disease states (e.g., cardiovascular disease, diabetes), and environmental risk factors (e.g., smoking) [9, 54]. In addition to patient age and cytokines, other factors, such as sex [58, 59] and lymphocytes [10], might be associated with the disease outcomes of COVID-19 patients. The mortality risk of COVID-19 was often higher in males than females [59]. Serum levels of CD8+ T lymphocytes were significantly lower in severe cases than in mild and moderate cases with COVID-19 [10]. Moreover, a severity-associated decrease in CD4+ T lymphocytes was observed in males with COVID-19 [10].
There are several limitations to this study. First, this retrospective study analyzed a cohort of COVID-19 patients hospitalized during the early pandemic to avoid the potential impact of different vaccines, cytokine antagonists, and SARS-CoV-2 variants. Although our study sought to analyze immune responses of different variants (e.g., omicron, alpha, beta, gamma, delta) [60], > 90% of citizens in Wuhan have been vaccinated, and only a few cases (N < 100 in total) have been reported after December 2020 because of the strict adherence to a zero-COVID-19 policy in China. Second, our study reported the interplay between early-stage cytokines and late-stage IgG due to active immune responses, but any causal effect remains unclear and future studies need to address the exact molecular mechanisms. Third, blood samples in our retrospective study were not collected prior to SARS-CoV-2 infection due to the sudden outbreak in early 2020. Future studies should address the baseline impact of inflamm-ageing in older patients with COVID-19. Fourth, more than 10 cytokines/chemokines are possibly involved in the disease progression of COVID-19, but our study was limited to those biomarkers that had been tested in our hospital laboratory. It is worth examining a full panel of cytokines/chemokines in future studies. Whether cytokine antagonists reduce the risk of cytokine storms and improve the clinical outcomes of different variants should also be addressed.
Conclusion
Based on a cohort of hospitalized COVID-19 patients with detailed records of cytokines, antibodies, and blood biomarkers, this retrospective study supports the hypothesis that early responses of elevated cytokines such as IL-6 may reflect active responses of the humoral immune system (Fig. S5). Active immune responses drive production of high IgG titers at the late stage, ideally delivering long-term protection. IL-6 can be used as an early predictor of IgG responses and cytokine storms, which may cause fatal symptoms such as acute respiratory distress syndrome. With a limited number of antiviral therapies against COVID-19 [61–64], future studies need to investigate whether antagonists of IL-6 and its receptor significantly improve the clinical outcomes of COVID-19.
Supplementary Information
Additional file 1: Table S1. Summary of laboratory-confirmed biomarkers in our study. Fig. S1. Dynamics of albumin (A), D-dimer (B), lymphocytes (C), C-reactive protein (D), neutrophils (E), procalcitonin (F) in COVID-19 patients. Four groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S2. Dynamics of creatine (A), creatine kinase (B), prothrombin time (C), total cholesterol (D), urea nitrogen (E), total bilirubin (F), troponin I (G), N-terminal brain natriuretic peptide (H) in COVID-19 patients. Four groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S3. Dynamics of monocytes (A), platelets (B), eosinophils (C), white blood cells (D), hemoglobin (E), and fibrinogen (F) in COVID-19 patients. Four patient groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S4. Dynamics of aspartate aminotransferase (A), alanine aminotransferase (B), lactate dehydrogenase (C), and erythrocyte sedimentation rate (D) in COVID-19 patients. Four patient groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S5. Our hypothesis of the cytokine - antibody associations during the disease progression of COVID-19. This figure is adapted from previous publications. Briefly, the disease progression of SARS-CoV-2 can be intuitively divided into the early stage (nearly 2 weeks after symptom onset) and the late stage (> 2 weeks after symptom onset). During the early stage, SARS-CoV-2 infects airway epithelial cells with the surface receptors such as ACE2 and TMPRSS2. The active replication and release of viral particles cause host cells to trigger the generation of pro-inflammatory cytokines (e.g., IL-6, IL-10, TNF), chemokines (e.g., CCL2, CCL3, CCL5, CXCL10), and interferons (type I/III interferons). This attracts monocytes, macrophages, and T cells to the infected cells and establish a pro-inflammatory feedback loop. The innate immunity responses to SARS-CoV-2 by activating many signaling pathways during the early stage of infection, while the adaptive immune responses take over during the late stage with production of antibodies such as anti-SARS-CoV-2 IgG. The defective immune response causes the overproduction of cytokines, resulting in cytokine storm that causes fatal symptoms such as acute respiratory distress syndrome (ARDS), severe pneumonia, multiorgan failure, and coagulation damage. The red lines indicate findings of our study that early responses of cytokines are associated with IgG responses at the late stage, and baseline cytokines and other factors such as older age can be early predictors of death outcome.
Acknowledgments
We thank Dr. Lewis F Buss for his helpful suggestions to improve this study. The authors acknowledge the study investigators, coordinators, nurses, and patients for their contributions to this study.
Abbreviations
- ALT
alanine aminotransferase
- ARDS
acute respiratory distress syndrome
- AST
aspartate aminotransferase
- AUC
area under the curve
- CCL20
C-C motif chemokine ligand 20
- COPD
chronic obstructive pulmonary disease
- COVID-19
coronavirus disease 2019
- CXCL
C-X-C motif chemokine receptor
- HR
hazard ratios
- IgG
immunoglobulin G
- IgM
immunoglobulin M
- IL
interleukin
- IL-2R
interleukin-2 receptor
- IQR
interquartile range
- RT-PCR
reverse transcription polymerase chain reaction
- SARS-CoV-2
severe acute respiratory syndrome coronavirus 2
- TNF-α
tumor necrosis factor-alpha
Authors’ contributions
XJ, MX and DS performed statistical analyses and drafted the manuscript; XJ, MX and TY performed data acquisition; DS, MX, YZ and MZ conducted clinical practice and data interpretation; XJ, YW and PZ performed statistical analyses; TTL, NRF and EDC contributed with discussions of the manuscript; GL supervised the study, obtained funding, and revised the manuscript. All authors contributed to the final article. The author(s) read and approved the final manuscript.
Funding
This research was funded by the National Nature Science Foundation of China (31871324, 81730064, 31571368), the National Science and Technology Major Project (2018ZX10715004), and the NSFC Excellent Young Scientists Fund (Hong Kong and Macau) (31922087). The funders had no role in study design, data collection, data analysis, data interpretation, or writing of the report.
Availability of data and materials
All data are contained within the article and available upon request after the approval of proposals by the Ethics Committees of The Second Xiangya Hospital.
Declarations
Competing interests
The authors disclose no conflicts.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Xixi Jing, Min Xu and Deye Song contributed equally to this work.
References
- 1.Hu B, Guo H, Zhou P, Shi ZL. Characteristics of SARS-CoV-2 and COVID-19. Nat Rev Microbiol. 2021;19(3):141–154. doi: 10.1038/s41579-020-00459-7. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Schultze JL, Aschenbrenner AC. COVID-19 and the human innate immune system. Cell. 2021;184(7):1671–1692. doi: 10.1016/j.cell.2021.02.029. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Tay MZ, Poh CM, Renia L, MacAry PA, Ng LFP. The trinity of COVID-19: immunity, inflammation and intervention. Nat Rev Immunol. 2020;20(6):363–374. doi: 10.1038/s41577-020-0311-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 4.Johansson MA, Quandelacy TM, Kada S, Prasad PV, Steele M, Brooks JT, Slayton RB, Biggerstaff M, Butler JC. SARS-CoV-2 transmission from people without COVID-19 symptoms. JAMA Netw Open. 2021;4(1):e2035057. doi: 10.1001/jamanetworkopen.2020.35057. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Jiang C, Wang Y, Hu M, Wen L, Wen C, Wang Y, Zhu W, Tai S, Jiang Z, Xiao K, Faria NR, de Clercq E, Xu J, Li G. Antibody seroconversion in asymptomatic and symptomatic patients infected with severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2) Clin Transl Immunology. 2020;9(9):e1182. doi: 10.1002/cti2.1182. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Fajgenbaum DC, June CH. Cytokine Storm. N Engl J Med. 2020;383(23):2255–2273. doi: 10.1056/NEJMra2026131. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Liuzzo G, Patrono C. COVID 19: in the eye of the cytokine storm. Eur Heart J. 2021;42(2):150–151. doi: 10.1093/eurheartj/ehaa1005. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Bektas A, Schurman SH, Franceschi C, Ferrucci L. A public health perspective of aging: do hyper-inflammatory syndromes such as COVID-19, SARS, ARDS, cytokine storm syndrome, and post-ICU syndrome accelerate short- and long-term inflammaging? Immun Ageing. 2020;17(1):23. doi: 10.1186/s12979-020-00196-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Wang Y, Pang SC, Yang Y. A potential association between immunosenescence and high COVID-19 related mortality among elderly patients with cardiovascular diseases. Immun Ageing. 2021;18(1):25. doi: 10.1186/s12979-021-00234-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Jurado A, Martin MC, Abad-Molina C, Orduna A, Martinez A, Ocana E, Yarce O, Navas AM, Trujillo A, Fernandez L, et al. COVID-19: age, Interleukin-6, C-reactive protein, and lymphocytes as key clues from a multicentre retrospective study. Immun Ageing. 2020;17(1):22. doi: 10.1186/s12979-020-00194-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Thwaites RS, Sanchez Sevilla Uruchurtu A, Siggins MK, Liew F, Russell CD, Moore SC, Fairfield C, Carter E, Abrams S, Short CE, et al. Inflammatory profiles across the spectrum of disease reveal a distinct role for GM-CSF in severe COVID-19. Sci Immunol. 2021;6(57):eabg9873. doi: 10.1126/sciimmunol.abg9873. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Rodrigues TS, de Sa KSG, Ishimoto AY, Becerra A, Oliveira S, Almeida L, Goncalves AV, Perucello DB, Andrade WA, Castro R, et al. Inflammasomes are activated in response to SARS-CoV-2 infection and are associated with COVID-19 severity in patients. J Exp Med. 2021;218(3):e20201707. doi: 10.1084/jem.20201707. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ma A, Zhang L, Ye X, Chen J, Yu J, Zhuang L, Weng C, Petersen F, Wang Z, Yu X. High levels of circulating IL-8 and soluble IL-2R are associated with prolonged illness in patients with severe COVID-19. Front Immunol. 2021;12:626235. doi: 10.3389/fimmu.2021.626235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 14.Benard A, Jacobsen A, Brunner M, Krautz C, Klosch B, Swierzy I, Naschberger E, Podolska MJ, Kouhestani D, David P, et al. Interleukin-3 is a predictive marker for severity and outcome during SARS-CoV-2 infections. Nat Commun. 2021;12(1):1112. doi: 10.1038/s41467-021-21310-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Nagant C, Ponthieux F, Smet J, Dauby N, Doyen V, Besse-Hammer T, De Bels D, Maillart E, Corazza F. A score combining early detection of cytokines accurately predicts COVID-19 severity and intensive care unit transfer. Int J Infect Dis. 2020;101:342–345. doi: 10.1016/j.ijid.2020.10.003. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 16.Henry BM, Benoit SW, Vikse J, Berger BA, Pulvino C, Hoehn J, Rose J. Santos de Oliveira MH, Lippi G, Benoit JL: the anti-inflammatory cytokine response characterized by elevated interleukin-10 is a stronger predictor of severe disease and poor outcomes than the pro-inflammatory cytokine response in coronavirus disease 2019 (COVID-19) Clin Chem Lab Med. 2021;59(3):599–607. doi: 10.1515/cclm-2020-1284. [DOI] [PubMed] [Google Scholar]
- 17.Orlov M, Wander PL, Morrell ED, Mikacenic C, Wurfel MM. A case for targeting Th17 cells and IL-17A in SARS-CoV-2 infections. J Immunol. 2020;205(4):892–898. doi: 10.4049/jimmunol.2000554. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Li A, Ling Y, Song Z, Cheng X, Ding L, Jiang R, Fu W, Liu Y, Hu H, Yuan S, Chen J, Zhu C, Fan J, Wang J, Jin Y, Zhang M, Zhu L, Sun P, Zhang L, Qin R, Zhang W, Qiu C, Shen Y, Zhang L, Shi Z, Zhao C, Zhu T, Lu H, Zhang X, Xu J. Correlation between early plasma interleukin 37 responses with low inflammatory cytokine levels and benign clinical outcomes in severe acute respiratory syndrome coronavirus 2 infection. J Infect Dis. 2021;223(4):568–580. doi: 10.1093/infdis/jiaa713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19.Del Valle DM, Kim-Schulze S, Huang HH, Beckmann ND, Nirenberg S, Wang B, Lavin Y, Swartz TH, Madduri D, Stock A, et al. An inflammatory cytokine signature predicts COVID-19 severity and survival. Nat Med. 2020;26(10):1636–1643. doi: 10.1038/s41591-020-1051-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Wang GL, Gao HX, Wang YL, Wei X, Liu YZ, Lu JH, Li L, Wang HB, Zhao L, Rong YX, Yao L, Duan LJ, Anderson BD, Ma MJ, Dai EH, Zhao XN. Serum IP-10 and IL-7 levels are associated with disease severity of coronavirus disease 2019. Cytokine. 2021;142:155500. doi: 10.1016/j.cyto.2021.155500. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Zhao Y, Qin L, Zhang P, Li K, Liang L, Sun J, Xu B, Dai Y, Li X, Zhang C, Peng Y, Feng Y, Li A, Hu Z, Xiang H, Ogg G, Ho LP, McMichael A, Jin R, Knight JC, Dong T, Zhang Y. Longitudinal COVID-19 profiling associates IL-1RA and IL-10 with disease severity and RANTES with mild disease. JCI Insight. 2020;5(13):e139834. doi: 10.1172/jci.insight.139834. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Donlan AN, Sutherland TE, Marie C, Preissner S, Bradley BT, Carpenter RM, Sturek JM, Ma JZ, Moreau GB, Donowitz JR, Buck GA, Serrano MG, Burgess SL, Abhyankar MM, Mura C, Bourne PE, Preissner R, Young MK, Lyons GR, Loomba JJ, Ratcliffe SJ, Poulter MD, Mathers AJ, Day AJ, Mann BJ, Allen JE, Petri Jr WA. IL-13 is a driver of COVID-19 severity. JCI Insight. 2021;6(15):e150107. doi: 10.1172/jci.insight.150107. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Ferreira-Gomes M, Kruglov A, Durek P, Heinrich F, Tizian C, Heinz GA, Pascual-Reguant A, Du W, Mothes R, Fan C, et al. SARS-CoV-2 in severe COVID-19 induces a TGF-beta-dominated chronic immune response that does not target itself. Nat Commun. 2021;12(1):1961. doi: 10.1038/s41467-021-22210-3. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Youngs J, Provine NM, Lim N, Sharpe HR, Amini A, Chen YL, Luo J, Edmans MD, Zacharopoulou P, Chen W, Sampson O, Paton R, Hurt WJ, Duncan DA, McNaughton AL, Miao VN, Leaver S, Wyncoll DLA, Ball J, Hopkins P, Oxford Immunology Network Covid-19 response T cell Consortium. Oxford Protective T cell Immunology for COVID-19 (OPTIC) Clinical team. Skelly DT, Barnes E, Dunachie S, Ogg G, Lambe T, Pavord I, Shalek AK, Thompson CP, Xue L, Macallan DC, Goulder P, Klenerman P, Bicanic T. Identification of immune correlates of fatal outcomes in critically ill COVID-19 patients. PLoS Pathog. 2021;17(9):e1009804. doi: 10.1371/journal.ppat.1009804. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Mazzoni A, Salvati L, Maggi L, Capone M, Vanni A, Spinicci M, Mencarini J, Caporale R, Peruzzi B, Antonelli A, Trotta M, Zammarchi L, Ciani L, Gori L, Lazzeri C, Matucci A, Vultaggio A, Rossi O, Almerigogna F, Parronchi P, Fontanari P, Lavorini F, Peris A, Rossolini GM, Bartoloni A, Romagnani S, Liotta F, Annunziato F, Cosmi L. Impaired immune cell cytotoxicity in severe COVID-19 is IL-6 dependent. J Clin Invest. 2020;130(9):4694–4703. doi: 10.1172/JCI138554. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Phetsouphanh C, Darley DR, Wilson DB, Howe A, Munier CML, Patel SK, Juno JA, Burrell LM, Kent SJ, Dore GJ, Kelleher AD, Matthews GV. Immunological dysfunction persists for 8 months following initial mild-to-moderate SARS-CoV-2 infection. Nat Immunol. 2022;23(2):210–216. doi: 10.1038/s41590-021-01113-x. [DOI] [PubMed] [Google Scholar]
- 27.Xiao N, Nie M, Pang H, Wang B, Hu J, Meng X, Li K, Ran X, Long Q, Deng H, Chen N, Li S, Tang N, Huang A, Hu Z. Integrated cytokine and metabolite analysis reveals immunometabolic reprogramming in COVID-19 patients with therapeutic implications. Nat Commun. 2021;12(1):1618. doi: 10.1038/s41467-021-21907-9. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.WHO Rapid Evidence Appraisal for COVID-19 Therapies Working Group. Shankar-Hari M, Vale CL, Godolphin PJ, Fisher D, JPT H, Spiga F, Savovic J, Tierney J, Baron G, et al. Association Between Administration of IL-6 Antagonists and Mortality Among Patients Hospitalized for COVID-19: A Meta-analysis. JAMA. 2021;326(6):499–518. doi: 10.1001/jama.2021.11330. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Melms JC, Biermann J, Huang H, Wang Y, Nair A, Tagore S, Katsyv I, Rendeiro AF, Amin AD, Schapiro D, Frangieh CJ, Luoma AM, Filliol A, Fang Y, Ravichandran H, Clausi MG, Alba GA, Rogava M, Chen SW, Ho P, Montoro DT, Kornberg AE, Han AS, Bakhoum MF, Anandasabapathy N, Suárez-Fariñas M, Bakhoum SF, Bram Y, Borczuk A, Guo XV, Lefkowitch JH, Marboe C, Lagana SM, del Portillo A, Tsai EJ, Zorn E, Markowitz GS, Schwabe RF, Schwartz RE, Elemento O, Saqi A, Hibshoosh H, Que J, Izar B. A molecular single-cell lung atlas of lethal COVID-19. Nature. 2021;595(7865):114–119. doi: 10.1038/s41586-021-03569-1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 30.Ragab D, Salah Eldin H, Taeimah M, Khattab R, Salem R. The COVID-19 cytokine storm; What We Know So Far. Front Immunol. 2020;11:1446. doi: 10.3389/fimmu.2020.01446. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Nielsen SS, Vibholm LK, Monrad I, Olesen R, Frattari GS, Pahus MH, Hojen JF, Gunst JD, Erikstrup C, Holleufer A, et al. SARS-CoV-2 elicits robust adaptive immune responses regardless of disease severity. EBioMedicine. 2021;68:103410. doi: 10.1016/j.ebiom.2021.103410. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Chen T, Wu D, Chen H, Yan W, Yang D, Chen G, Ma K, Xu D, Yu H, Wang H, Wang T, Guo W, Chen J, Ding C, Zhang X, Huang J, Han M, Li S, Luo X, Zhao J, Ning Q. Clinical characteristics of 113 deceased patients with coronavirus disease 2019: retrospective study. BMJ. 2020;368:m1091. doi: 10.1136/bmj.m1091. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Cox RJ, Brokstad KA. Not just antibodies: B cells and T cells mediate immunity to COVID-19. Nat Rev Immunol. 2020;20(10):581–582. doi: 10.1038/s41577-020-00436-4. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Saavedra D, Ane-Kouri AL, Sanchez N, Filgueira LM, Betancourt J, Herrera C, Manso L, Chavez E, Caballero A, Hidalgo C, et al. An anti-CD6 monoclonal antibody (itolizumab) reduces circulating IL-6 in severe COVID-19 elderly patients. Immun Ageing. 2020;17(1):34. doi: 10.1186/s12979-020-00207-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Kim JS, Lee JY, Yang JW, Lee KH, Effenberger M, Szpirt W, Kronbichler A, Shin JI. Immunopathogenesis and treatment of cytokine storm in COVID-19. Theranostics. 2021;11(1):316–329. doi: 10.7150/thno.49713. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 36.Mulchandani R, Lyngdoh T, Kakkar AK. Deciphering the COVID-19 cytokine storm: systematic review and meta-analysis. Eur J Clin Investig. 2021;51(1):e13429. doi: 10.1111/eci.13429. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Liu QQ, Cheng A, Wang Y, Li H, Hu L, Zhao X, Wang T, He F. Cytokines and their relationship with the severity and prognosis of coronavirus disease 2019 (COVID-19): a retrospective cohort study. BMJ Open. 2020;10(11):e041471. doi: 10.1136/bmjopen-2020-041471. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Hou H, Zhang B, Huang H, Luo Y, Wu S, Tang G, Liu W, Mao L, Mao L, Wang F, Sun Z. Using IL-2R/lymphocytes for predicting the clinical progression of patients with COVID-19. Clin Exp Immunol. 2020;201(1):76–84. doi: 10.1111/cei.13450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Laguna-Goya R, Utrero-Rico A, Talayero P, Lasa-Lazaro M, Ramirez-Fernandez A, Naranjo L, Segura-Tudela A, Cabrera-Marante O. Rodriguez de Frias E, Garcia-Garcia R et al: IL-6-based mortality risk model for hospitalized patients with COVID-19. J Allergy Clin Immunol. 2020;146(4):799–807. doi: 10.1016/j.jaci.2020.07.009. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Santa Cruz A, Mendes-Frias A, Oliveira AI, Dias L, Matos AR, Carvalho A, Capela C, Pedrosa J, Castro AG, Silvestre R. Interleukin-6 is a biomarker for the development of fatal severe acute respiratory syndrome coronavirus 2 pneumonia. Front Immunol. 2021;12:613422. doi: 10.3389/fimmu.2021.613422. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 41.Zhang J, Hao Y, Ou W, Ming F, Liang G, Qian Y, Cai Q, Dong S, Hu S, Wang W, Wei S. Serum interleukin-6 is an indicator for severity in 901 patients with SARS-CoV-2 infection: a cohort study. J Transl Med. 2020;18(1):406. doi: 10.1186/s12967-020-02571-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 42.Chen LYC, Biggs CM, Jamal S, Stukas S, Wellington CL, Sekhon MS. Soluble interleukin-6 receptor in the COVID-19 cytokine storm syndrome. Cell Rep Med. 2021;2(5):100269. doi: 10.1016/j.xcrm.2021.100269. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 43.Yonas E, Alwi I, Pranata R, Huang I, Lim MA, Yamin M, Nasution SA, Setiati S, Virani SS. Elevated interleukin levels are associated with higher severity and mortality in COVID 19 - a systematic review, meta-analysis, and meta-regression. Diabetes Metab Syndr. 2020;14(6):2219–2230. doi: 10.1016/j.dsx.2020.11.011. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 44.Angioni R, Sanchez-Rodriguez R, Munari F, Bertoldi N, Arcidiacono D, Cavinato S, Marturano D, Zaramella A, Realdon S, Cattelan A, et al. Age-severity matched cytokine profiling reveals specific signatures in Covid-19 patients. Cell Death Dis. 2020;11(11):957. doi: 10.1038/s41419-020-03151-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 45.Li J, Rong L, Cui R, Feng J, Jin Y, Chen X, Xu R. Dynamic changes in serum IL-6, IL-8, and IL-10 predict the outcome of ICU patients with severe COVID-19. Ann Palliat Med. 2021;10(4):3706–3714. doi: 10.21037/apm-20-2134. [DOI] [PubMed] [Google Scholar]
- 46.Jones SA, Hunter CA. Is IL-6 a key cytokine target for therapy in COVID-19? Nat Rev Immunol. 2021;21(6):337–339. doi: 10.1038/s41577-021-00553-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Rubin EJ, Longo DL, Baden LR. Interleukin-6 receptor inhibition in Covid-19 - cooling the inflammatory soup. N Engl J Med. 2021;384(16):1564–1565. doi: 10.1056/NEJMe2103108. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Recovery Collaborative Group Tocilizumab in patients admitted to hospital with COVID-19 (RECOVERY): a randomised, controlled, open-label, platform trial. Lancet. 2021;397(10285):1637–1645. doi: 10.1016/S0140-6736(21)00676-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 49.Yang C, Zhao H. Tocilizumab in COVID-19 therapy: who benefits, and how? Lancet. 2021;398(10297):299. doi: 10.1016/S0140-6736(21)01380-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 50.Jacofsky D, Jacofsky EM, Jacofsky M. Understanding antibody testing for COVID-19. J Arthroplast. 2020;35(7S):S74–S81. doi: 10.1016/j.arth.2020.04.055. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Peghin M, De Martino M, Fabris M, Palese A, Visintini E, Graziano E, Gerussi V, Bontempo G, D'Aurizio F, Biasotto A, et al. The fall in antibody response to SARS-CoV-2: a longitudinal study of asymptomatic to critically ill patients up to 10 months after recovery. J Clin Microbiol. 2021;59(11):e0113821. doi: 10.1128/JCM.01138-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Bichara CDA, da Silva Graca Amoras E, Vaz GL, da Silva Torres MK, MAF Q, IPC d A, Vallinoto I, CNC B, ACR V. Dynamics of anti-SARS-CoV-2 IgG antibodies post-COVID-19 in a Brazilian Amazon population. BMC Infect Dis. 2021;21(1):443. doi: 10.1186/s12879-021-06156-x. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 53.Wang H, Yuan Y, Xiao M, Chen L, Zhao Y, Haiwei Z, Long P, Zhou Y, Xu X, Lei Y, et al. Dynamics of the SARS-CoV-2 antibody response up to 10 months after infection. Cell Mol Immunol. 2021;18(7):1832–1834. doi: 10.1038/s41423-021-00708-6. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Nidadavolu LS, Walston JD. Underlying vulnerabilities to the cytokine storm and adverse COVID-19 outcomes in the aging immune system. J Gerontol A Biol Sci Med Sci. 2021;76(3):e13–e18. doi: 10.1093/gerona/glaa209. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 55.Rydyznski Moderbacher C, Ramirez SI, Dan JM, Grifoni A, Hastie KM, Weiskopf D, Belanger S, Abbott RK, Kim C, Choi J, Kato Y, Crotty EG, Kim C, Rawlings SA, Mateus J, Tse LPV, Frazier A, Baric R, Peters B, Greenbaum J, Ollmann Saphire E, Smith DM, Sette A, Crotty S. Antigen-specific adaptive immunity to SARS-CoV-2 in acute COVID-19 and associations with age and disease severity. Cell. 2020;183(4):996–1012. doi: 10.1016/j.cell.2020.09.038. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 56.Martin MC, Jurado A, Abad-Molina C, Orduna A, Yarce O, Navas AM, Cunill V, Escobar D, Boix F, Burillo-Sanz S, et al. The age again in the eye of the COVID-19 storm: evidence-based decision making. Immun Ageing. 2021;18(1):24. doi: 10.1186/s12979-021-00237-w. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 57.Meftahi GH, Jangravi Z, Sahraei H, Bahari Z. The possible pathophysiology mechanism of cytokine storm in elderly adults with COVID-19 infection: the contribution of "inflame-aging". Inflamm Res. 2020;69(9):825–839. doi: 10.1007/s00011-020-01372-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 58.Marquez EJ, Trowbridge J, Kuchel GA, Banchereau J, Ucar D. The lethal sex gap: COVID-19. Immun Ageing. 2020;17(1):13. doi: 10.1186/s12979-020-00183-z. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 59.Li G, Liu Y, Jing X, Wang Y, Miao M, Tao L, Zhou Z, Xie Y, Huang Y, Lei J, Gong G, Jin P, Hao Y, Faria NR, Clercq E, Zhang M. Mortality risk of COVID-19 in elderly males with comorbidities: a multi-country study. Aging. 2020;13(1):27–60. doi: 10.18632/aging.202456. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 60.Miao M, Clercq E, Li G. Genetic diversity of SARS-CoV-2 over a one-year period of the COVID-19 pandemic: a global perspective. Biomedicines. 2021;9(4):412. doi: 10.3390/biomedicines9040412. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 61.Li G, De Clercq E. Therapeutic options for the 2019 novel coronavirus (2019-nCoV) Nat Rev Drug Discov. 2020;19(3):149–150. doi: 10.1038/d41573-020-00016-0. [DOI] [PubMed] [Google Scholar]
- 62.Li G, De Clercq E. A medicinal chemist who reshaped the antiviral drug industry: John Charles Martin (1951-2021) Med Res Rev. 2021;42(2):647–653. doi: 10.1002/med.21858. [DOI] [PubMed] [Google Scholar]
- 63.Li G, Wang Y, De Clercq E. Approved HIV reverse transcriptase inhibitors in the past decade. Acta Pharm Sin B. 2021. 10.1016/j.apsb.2021.11.009. [DOI] [PMC free article] [PubMed]
- 64.Tao K, Tzou PL, Nouhin J, Bonilla H, Jagannathan P, Shafer RW. SARS-CoV-2 antiviral therapy. Clin Microbiol Rev. 2021;34(4):e0010921. doi: 10.1128/CMR.00109-21. [DOI] [PMC free article] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Additional file 1: Table S1. Summary of laboratory-confirmed biomarkers in our study. Fig. S1. Dynamics of albumin (A), D-dimer (B), lymphocytes (C), C-reactive protein (D), neutrophils (E), procalcitonin (F) in COVID-19 patients. Four groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S2. Dynamics of creatine (A), creatine kinase (B), prothrombin time (C), total cholesterol (D), urea nitrogen (E), total bilirubin (F), troponin I (G), N-terminal brain natriuretic peptide (H) in COVID-19 patients. Four groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S3. Dynamics of monocytes (A), platelets (B), eosinophils (C), white blood cells (D), hemoglobin (E), and fibrinogen (F) in COVID-19 patients. Four patient groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S4. Dynamics of aspartate aminotransferase (A), alanine aminotransferase (B), lactate dehydrogenase (C), and erythrocyte sedimentation rate (D) in COVID-19 patients. Four patient groups were visualized in light blue (moderately-ill patients aged < 65 years), blue (severely-ill patients aged < 65 years), light red (moderately-ill patients aged ≥65 years), and red (severely-ill patients aged ≥65 years). Fig. S5. Our hypothesis of the cytokine - antibody associations during the disease progression of COVID-19. This figure is adapted from previous publications. Briefly, the disease progression of SARS-CoV-2 can be intuitively divided into the early stage (nearly 2 weeks after symptom onset) and the late stage (> 2 weeks after symptom onset). During the early stage, SARS-CoV-2 infects airway epithelial cells with the surface receptors such as ACE2 and TMPRSS2. The active replication and release of viral particles cause host cells to trigger the generation of pro-inflammatory cytokines (e.g., IL-6, IL-10, TNF), chemokines (e.g., CCL2, CCL3, CCL5, CXCL10), and interferons (type I/III interferons). This attracts monocytes, macrophages, and T cells to the infected cells and establish a pro-inflammatory feedback loop. The innate immunity responses to SARS-CoV-2 by activating many signaling pathways during the early stage of infection, while the adaptive immune responses take over during the late stage with production of antibodies such as anti-SARS-CoV-2 IgG. The defective immune response causes the overproduction of cytokines, resulting in cytokine storm that causes fatal symptoms such as acute respiratory distress syndrome (ARDS), severe pneumonia, multiorgan failure, and coagulation damage. The red lines indicate findings of our study that early responses of cytokines are associated with IgG responses at the late stage, and baseline cytokines and other factors such as older age can be early predictors of death outcome.
Data Availability Statement
All data are contained within the article and available upon request after the approval of proposals by the Ethics Committees of The Second Xiangya Hospital.