Abstract
Aneurysm of the portal vein is a rare type of visceral aneurysm that is largely asymptomatic although some patients may develop symptoms or secondary complications. In this report, we present the first case in the literature of inferior vena cava (IVC) thrombosis arising as a consequence of portal vein aneurysm. A 95-year-old male with past medical history significant for hypertension, hypercholesterolemia, type II diabetes mellitus, benign prostatic hyperplasia, and gastroesophageal reflux presented to the emergency department with several days of altered mental status, disorganized behavior, visual hallucinations, and weight loss. Contrast-enhanced computed tomography of the patient's abdomen and pelvis was performed to assess for infection or malignancy. The study revealed a large saccular aneurysm of the proximal portal vein arising near the portal confluence. Compression of the adjacent IVC was also seen which contained a hypoattenuating filling defect, probably representing thrombus. Incidental large hepatic cysts were seen, and a 6 mm pancreatic cyst was also identified which likely represented an intra-ductal papillary mucinous neoplasm . He was determined not to be a surgical candidate due to age, comorbidities, and absence secondary symptoms. The patient was discharged on quetiapine and enoxaparin for management of agitation and IVC thrombosis, respectively. This case demonstrates the increasing rates of detection of portal vein aneurysm and the range of complications that may arise as a result.
Keywords: Portal vein, Aneurysm, Inferior vena cava, Thrombosis
Introduction
Aneurysm of the portal vein is a rare vascular finding that was first described in 1956 in a patient who was diagnosed at autopsy after aneurysmal rupture [1]. Due to greater utilization of abdominal imaging, detection of portal vein aneurysms is increasing. Most aneurysms are asymptomatic and remain stable in size once discovered but some may manifest as vague abdominal discomfort [2]. A number of complications are known to arise as a result of portal venous aneurysm including portal vein thrombosis, portal hypertension, rupture, and compression of adjacent structures including the common bile duct, duodenum, and inferior vena cava (IVC) [3]. In the following study, we present the first reported case in the literature of IVC thrombosis arising as a complication of compression due to portal vein aneurysm.
Case presentation
A 95-year-old male with past medical history significant for hypertension, hypercholesterolemia, type II diabetes mellitus, benign prostatic hyperplasia, and gastroesophageal reflux presented to the emergency department with several days of altered mental status, disorganized behavior, visual hallucinations, decreased appetite, and weight loss. His daughter had noted that for the past several days, he had been speaking unintelligibly, has had visual hallucinations, loss of appetite, and had been attempting to ingest his glucose test strips. Earlier in the month, the patient had a similar presentation and was discharged with a diagnosis of metabolic encephalopathy of uncertain etiology. At that time, complete blood count and metabolic panel were unremarkable, and resolution of symptoms was achieved with quetiapine. At baseline, the patient was independent of all activities of daily living and cared for his wife at home, who suffered from dementia, with the help of a visiting nurse. The patient denied any other complaints including subjective fevers, nausea, vomiting, diarrhea, chest pain, shortness of breath, and stated he was taking his home medications (linagliptin, carvedilol, amlodipine, atorvastatin, finasteride, tamsulosin, and pantoprazole) as prescribed. He stated that he had not been using any new medications or substances.
At the emergency department, he was afebrile, hypertensive to 180/80 mm Hg, with an oxygen saturation of 99% on room air. Physical examination revealed a frail, elderly male in no apparent distress. Focused neurological, cardiac, lung, and abdominal examinations were performed which were normal. He was awake, alert, and oriented to person and place. The patient was admitted to the inpatient floors for further management of acute encephalopathy and workup was initiated for metabolic and vascular causes, malignancy, trauma, and infection. He was started on his home medications which helped reduce his elevated blood pressure.
Computed tomography (CT) of the abdomen and pelvis with intravenous contrast was performed to assess for malignancy and infection as a potential cause of his symptoms. The study revealed a 3.5 × 3.0 × 3.5 cm (anteroposterior x transverse x craniocaudal) saccular aneurysm of the proximal portal vein arising distal to the confluence of the splenic and superior mesenteric veins. Compression of the adjacent IVC was seen which appeared to contain a hypoattenuating filling defect, probably representing thrombus. Incidental large hepatic cysts were present, and a 6 mm pancreatic cyst was also identified which most likely represented an intra-ductal papillary mucinous neoplasm . (Fis. 1 and 2).
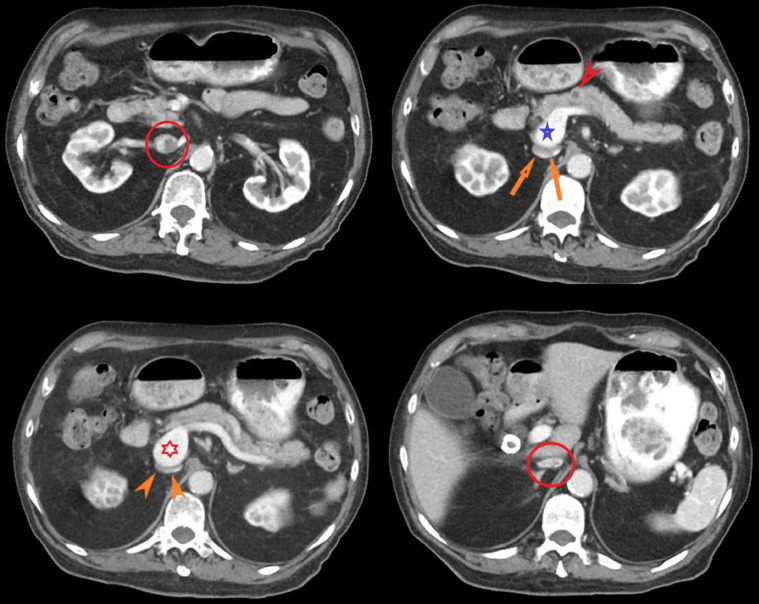
Fig. 1.
Contrast-enhanced axial computed tomography imaging sections illustrate a 3.5 × 3.0 × 3.5 cm saccular aneurysm of the portal vein arising near the portal confluence (blue and red star). Compression of the IVC is also seen posteriorly (orange arrows) with hypoattenuating intra-luminal material (red circles). This is most consistent with thrombus within the IVC. A 6 mm hypoattenuating lesion is seen within the pancreatic body (red arrow) which likely represents an intra-ductal papillary mucinous neoplasm.
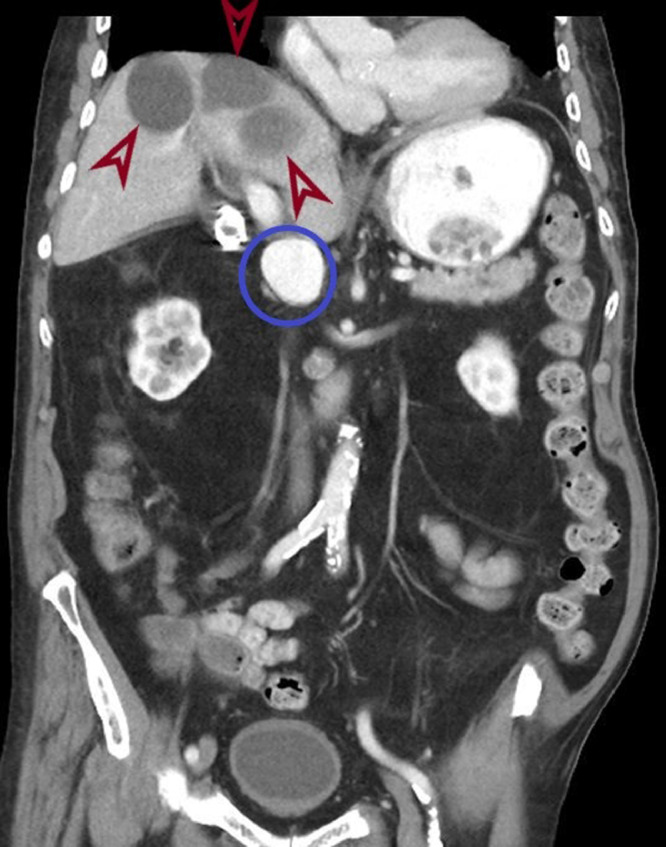
Fig. 2.
Contrast-enhanced coronal CT imaging again shows saccular aneurysm of the portal vein (blue circle). Also present in this image are large hepatic cysts (maroon arrows). This study was slightly degraded by motion artifact.
After other organic causes of altered mental status were ruled out, 12.5 mg quetiapine was started as needed for agitation. The patient was discharged with a diagnosis of acute encephalopathy secondary to possible Lewy body dementia for which he was prescribed quetiapine for agitation and 70 mg of enoxaparin daily for IVC thrombus. A goals of care discussion was held with the patient's family regarding further workup of the portal vein thrombus, and it was decided not to pursue further intervention given his age and comorbidities.
Discussion
Portal vein aneurysm represents less than 3% of all cases of visceral aneurysm [4]. In one study, the maximum portal vein diameter measured 15 mm in healthy subjects and 19 mm in those with cirrhosis [5]. A diameter that exceeds these values is generally regarded as aneurysmal. The most common locations for aneurysm formation are at the splenomesenteric venous confluence, main portal vein, and intrahepatic branches with the majority being fusiform in morphology [2,6]. Both congenital and acquired causes of portal vein aneurysms have been proposed. With respect to the former, supporting evidence includes cases of aneurysm discovered in utero [7]. It is thought that vessel wall weakness or incomplete regression of the right vitelline vein in the area of the proximal superior mesenteric vein could explain a congenital basis [2]. Acquired portal vein aneurysm is most commonly reported to arise as a result of portal hypertension due to intimal thickening, medial hypertrophy, and fibrosis, and weakening of the vessel wall [8]. Other etiologies include venous inflammation due to severe acute pancreatitis, trauma, and invasion of the portal vein by cancer [9,10]. In the patient described above, no suggestion of the latter could be ascertained from his imaging studies.
Portal vein aneurysms may be diagnosed on ultrasound and appear as an anechoic, rounded mass with luminal continuity with the portal vein. Doppler flow may assist in differentiating this and similar appearing lesions like cysts. As the most common complication of portal vein aneurysm is thrombus, echogenic material may be present within the vessel wall. The prevalence of thrombus is estimated to be between 6% and 13% [11]. Although ultrasound is a relatively cheap and safe modality for the diagnosis and monitoring of portal vein aneurysm, contrast-enhanced CT or magnetic resonance angiography is helpful in further characterizing lesions [3].
As previously mentioned, reported complications of portal vein aneurysm include thrombosis, rupture, cholestasis secondary to biliary tract compression, and compression of the duodenum or IVC. Rupture is a rare complication due to relatively low venous pressure, with only a few reported cases in the literature [11,12]. In this study, we have illustrated caval thrombus resulting from aneurysmal mass effect. It is postulated that impedance of blood flow across the site of compression had contributed to the development of a thrombus. It is also possible that induction of a hypercoagulable state by malignancy in this patient increased the risk of clot development.
Surgical management is generally reserved for symptomatic patients, rapidly enlarging aneurysms or those at risk for rupture, and aneurysms with thrombus [13]. One study suggested surgical intervention for asymptomatic aneurysms without thrombus greater than 3 cm to prevent development of complications [14]. Aneurysmal diameter was 3.5 cm in our patient, but intervention was not pursued due to his age, comorbidities, and goals of care. Selection of procedure type is based on the presence or absence of portal hypertension. In the latter case, aneurysmorrhaphy or aneurysmectomy have been successfully used in several instances [15,16]. One review suggested shunt procedures (ie, portocaval shunt) with or without splenectomy, or liver transplantation as viable approaches that have been successful in a few reports [13]. These treatments are meant to achieve portal decompression to curb enlargement instead of primary treatment of the defected vessel.
Author contribution
K.K. and H.A. were responsible for the writing of this paper, data analysis, interpretation, and critical review of the draft.
Patient consent
Written informed consent was obtained from the patient for publication of this case report and accompanying images. A copy of the written consent form is available upon request.
Footnotes
Acknowledgments: None.
Competing interests: The authors of this study have no conflicts of interest to disclose.
References
- 1.Barzilai R, Kleckner MS. Hemocholecyst following ruptured aneurysm of portal vein. AMA Arch Surg. 1956;72:725–727. doi: 10.1001/archsurg.1956.01270220173023. [DOI] [PubMed] [Google Scholar]
- 2.Gallego C, Velasco M, Marcuello P, Tejedor D, De Campo L, Friera A. Congenital and acquired anomalies of the portal venous system. Radiographics. 2002;22(1):141–159. doi: 10.1148/radiographics.22.1.g02ja08141. [DOI] [PubMed] [Google Scholar]
- 3.Rafiq SA, Sitrin MD. Portal vein aneurysm: case report and review of the literature. Gastroenterol Hepatol (N Y) 2007;3(4):296–298. [PMC free article] [PubMed] [Google Scholar]
- 4.Koc Z, Oguzkurt L, Ulusan S. Portal venous system aneurysms: imaging, clinical findings, and a possible new etiologic factor. AJR Am J Roentgenol. 2007;189(5):1023–1030. doi: 10.2214/AJR.07.2121. [DOI] [PubMed] [Google Scholar]
- 5.Doust BD, Pearce JD. Gray-scale ultrasonic properties of the normal and inflamed pancreas. Radiology. 1976;120(3):653–657. doi: 10.1148/120.3.653. [DOI] [PubMed] [Google Scholar]
- 6.Lee Wai-Kit, Chang Silvia D., Duddalwar Vinay A., Comin Jules M., Perera Warren, Lau Wing-Fai E., et al. Imaging assessment of congenital and acquired abnormalities of the portal venous system. RadioGraphics. 2011;31(4):905–926. doi: 10.1148/rg.314105104. [DOI] [PubMed] [Google Scholar]
- 7.Gallagher DM, Leiman S, Hux CH. In utero diagnosis of a portal vein aneurysm. J Clin Ultrasound. 1993;21:147–151. doi: 10.1002/jcu.1870210214. [DOI] [PubMed] [Google Scholar]
- 8.Leonsins AJ, Siew S. Fusiform aneurysmal dilation of the portal vein. Postgrad Med J. 1960;46:570–574. doi: 10.1136/pgmj.36.419.570. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Lau H, Chew DK, Belkin M. Extrahepatic portal vein aneurysm: a case report and review of the literature. Cardiovasc Surg. 2002;10:58–61. doi: 10.1177/096721090201000115. [DOI] [PubMed] [Google Scholar]
- 10.Yang DM, Yoon MH, Kim HS, et al. CT findings of portal vein aneurysm caused by gastric adenocarcinoma invading the portal vein. Br J Radiol. 2001;74:654–656. doi: 10.1259/bjr.74.883.740654. [DOI] [PubMed] [Google Scholar]
- 11.Shrivastava A, Rampal JS, Nageshwar Reddy D. Giant intrahepatic portal vein aneurysm: leave it or treat it? J Clin Exp Hepatol. 2017;7(1):71–76. doi: 10.1016/j.jceh.2016.08.013. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Schwope RB, Margolis DJ, Raman SS, Kadell BM. Portal vein aneurysms: a case series with literature review. J Radiol Case Rep. 2010;4(6):28–38. doi: 10.3941/jrcr.v4i6.431. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Laurenzi A, Ettorre GM, Lionetti R, Meniconi RL, Colasanti M, Vennarecci G. Portal vein aneurysm: what to know. Dig Liver Dis. 2015;47(11):918–923. doi: 10.1016/j.dld.2015.06.003. [DOI] [PubMed] [Google Scholar]
- 14.Moreno JA, Fleming MD, Farnell MB, Gloviczki P. Extrahepatic portal vein aneurysm. J Vasc Surg. 2011;54(1):225–226. doi: 10.1016/j.jvs.2010.05.113. [DOI] [PubMed] [Google Scholar]
- 15.Savadkohi S, Abouljoud M. Outcome with surgical repair of extrahepatic portal vein aneurysms. Ann Vasc Surg. 2011;25(8) doi: 10.1016/j.avsg.2011.02.046. 1140.e1-1140.e11405. [DOI] [PubMed] [Google Scholar]
- 16.He H, Antonopoulos CN, Moulakakis KG, et al. Diagnosis and surgical treatment of extrahepatic portal vein aneurysm: a case report. Vascular. 2015;23(5):553–554. doi: 10.1177/1708538114560464. [DOI] [PubMed] [Google Scholar]