Abstract
OBJECTIVE
Continuous glucose monitoring (CGM) is increasingly used in type 1 diabetes management; however, funding models vary. This study determined the uptake rate and glycemic outcomes following a change in national health policy to introduce universal subsidized CGM funding for people with type 1 diabetes aged <21 years.
RESEARCH DESIGN AND METHODS
Longitudinal data from 12 months before the subsidy until 24 months after were analyzed. Measures and outcomes included age, diabetes duration, HbA1c, episodes of diabetic ketoacidosis and severe hypoglycemia, insulin regimen, CGM uptake, and percentage CGM use. Two data sources were used: the Australasian Diabetes Database Network (ADDN) registry (a prospective diabetes database) and the National Diabetes Service Scheme (NDSS) registry that includes almost all individuals with type 1 diabetes nationally.
RESULTS
CGM uptake increased from 5% presubsidy to 79% after 2 years. After CGM introduction, the odds ratio (OR) of achieving the HbA1c target of <7.0% improved at 12 months (OR 2.5, P < 0.001) and was maintained at 24 months (OR 2.3, P < 0.001). The OR for suboptimal glycemic control (HbA1c ≥9.0%) decreased to 0.34 (P < 0.001) at 24 months. Of CGM users, 65% used CGM >75% of time, and had a lower HbA1c at 24 months compared with those with usage <25% (7.8 ± 1.3% vs. 8.6 ± 1.8%, respectively, P < 0.001). Diabetic ketoacidosis was also reduced in this group (incidence rate ratio 0.49, 95% CI 0.33–0.74, P < 0.001).
CONCLUSIONS
Following the national subsidy, CGM use was high and associated with sustained improvement in glycemic control. This information will inform economic analyses and future policy and serve as a model of evaluation diabetes technologies.
Introduction
Most children and adolescents with type 1 diabetes (T1D) do not achieve recommended glycemic targets (1,2). Although early studies of the use of continuous glucose monitoring (CGM) did not demonstrate significant clinical improvement with CGM use (3), more recent reports have shown benefit (4,5). Concurrently, there has been increased uptake and use of CGM, especially in children, as reported from the U.S. and Germany (6).
Randomized controlled trials, although essential, are often short-term, recruit-selected populations, often with more optimal diabetes self-management, and are frequently insufficiently powered to examine hypoglycemia and diabetic ketoacidosis (DKA) rates. Furthermore, device education and usage are likely to differ between a strictly controlled trial environment and routine outpatient clinical practice. As a result, measuring outcomes in the real world is important to assess the impact of CGM in the clinic.
CGM is expensive, and funding models vary. A recent report and commentary highlighted the significant disparities in pediatric T1D care and the potential impact of this on outcomes (7–9). This presents another confounding factor when analyzing the impact of new diabetes technologies. Further, as noted above, there are multiple funding models to provide access to CGM in people with T1D and few data to inform funders on the most effective approach. A recent commentary in Lancet highlighted the complexity, variation, and frustration around reimbursement of CGM (10).
In April 2017, the Australian Government fully funded CGM products for young people living with T1D aged <21 years through a national scheme. Prior to funding, the usage rate of CGM was ∼5% nationally. This sudden change in availability provided a unique opportunity to examine the real-world effect of the introduction of fully subsidized CGM available to a whole population. Because the funding was universal, the effect of socioeconomic status was potentially reduced. The aim of this study was to evaluate the effect of the policy change on the rate of uptake and ongoing use of the devices and the impact, if any, on glycemic control and hypoglycemia and ketoacidosis rates, information of importance to funders, policy makers, clinicians, and people living with T1D.
Research Design and Methods
Study Subjects
The study sample consisted of young people living with T1D aged <21 years who attended an Australasian Diabetes Database Network (ADDN) center in Australia between April 2016 and December 2019 and therefore had visit data provided to the ADDN registry.
Sociodemographic and clinical data were obtained from the ADDN registry. Other fields extracted included sex, age at visit, age at diabetes diagnosis, diabetes duration, HbA1c, hypoglycemia and DKA events, and insulin therapy. For those using CGM, the start date and percentage of time that CGM was actively used was documented (as a percentage of time between visits) and recorded at each visit.
Rates of CGM uptake nationally, for the same time period, were obtained from the National Diabetes Supply Scheme (NDSS) registry (see below).
Data Sources
1. The NDSS
The NDSS is an Australian Government-funded program that provides support services to people living with diabetes in Australia. In order to receive subsidized diabetes supplies, such as glucose monitoring strips, needles, and insulin, an individual with diabetes is required to register with the NDSS. As a result, nearly all people living with T1D are registered on the NDSS database. In 2017, the NDSS was given responsibility for administering the supply of fully subsidized CGM products to eligible individuals with T1D. Data were obtained from NDSS on the number of people with T1D <21 years registered with NDSS and, of those, the number who applied for subsidized CGM products. This registry provided the data that was used to determine rates of uptake.
2. The ADDN
The ADDN, established in 2012, is a prospective longitudinal registry that captures clinical data from a sample of diabetes centers across Australia and New Zealand (11). There are 18 centers contributing data to ADDN—11 tertiary pediatric and 7 tertiary adult centers. Data are collected locally and uploaded at 6-month intervals to the central database. Data from the two New Zealand centers and those centers that had incomplete documentation of CGM start dates were not included. This registry was the source of the outcome data used in the analysis.
CGM Eligibility
Individuals were able to receive fully subsidized CGM products if they met the following criteria:
T1D <10 years of age, or
- Individuals aged 10 to <21 years meeting one or more of the following criteria:
- frequent significanthypoglycemia—more than one episode a year of significant hypoglycemia requiring external, third-party assistance; and/or
- impaired awareness of hypoglycemia; and/or
- inability to recognize or communicate about symptoms of hypoglycemia; and/or
- significant fear of hypoglycemia for the child/young person or a family member/carer, which was seriously affecting the health and well-being of the child or young person or contributing to hyperglycemia as a reaction to this fear.
Eligible products at the time of the study included Dexcom G5 Mobile, Medtronic Guardian Connect, Medtronic MiniLink, Medtronic Guardian 2 Link, Medtronic Guardian Sensor 3, and Medtronic Guardian Link (3).
Outcome Measures
Glycemic Control
Mean HbA1c was assessed at 3-month intervals 12 months before the start of CGM to 24 months after. The proportion of participants who achieved the HbA1c target (<7.0%) and those with HbA1c well above target (≥9.0%) was assessed at 3-month intervals—from 12 months before the start of CGM to 24 months after start of CGM for the CGM cohort. Because residual insulin secretion has a potential impact on glycemic control in the period following diagnosis, HbA1c values within the first 12 months after diagnosis were excluded.
Hypoglycemia
Hypoglycemic events were recorded at each clinic visit. These were defined as an event associated with severe cognitive impairment (including coma and convulsions) requiring external assistance by another person to actively administer carbohydrates, glucagon, or take other corrective actions (12).
DKA
This was documented from the medical record, and standard criteria based on the International Society for Pediatric and Adolescent Diabetes (ISPAD) Guidelines (12) were used to define DKA. Biochemical criteria for the diagnosis of DKA were hyperglycemia (blood glucose >11 mmol/L), venous pH <7.3 or bicarbonate <15 mmol/L, ketonemia, and/or ketonuria.
Analyses
Firstly, the calculated mean HbA1c levels were grouped into the following HbA1c range categories: <7.0% and ≥9.0% for 12 months before CGM and for the 24 months after CGM. The odds of patients achieving the recommended glycemic target of <7.0% were analyzed before and after the introduction of CGM by using the generalized estimating equation (GEE) model. A binomial distribution with a logit link function and an exchangeable correlation matrix was specified. The same analysis was repeated for determining the odds of patients having a mean HbA1c of ≥9.0% before and after the introduction of CGM.
Secondly, we used the conditional negative binomial regression model to compare the incidence rate ratio of severe hypoglycemia and DKA for post-CGM start date compared with pre-CGM (maximum 2 years prior). The negative binomial model was chosen over the Poisson model because of overdispersion in the counts. The actual incidence rates for severe hypoglycemia and DKA were calculated based on the total number of events reported at each outpatient visit for the 12-month period preceding the CGM start date (before CGM) and following the CGM start date (after CGM). Incidence rates were then expressed as number of events per 100 patient-years.
Lastly, in those for whom a percentage use was available, changes in mean HbA1c over time before and after CGM was introduced were compared among three groups: 1) those who started on CGM and reported that they had been using CGM for ≥75% of the time; 2) those who started on CGM but had either not continued using CGM or only used CGM for <25% of the time; and 3) those who did not start on CGM (non-CGM). CGM use of 75% was selected based on published data suggesting that 75% usage is an important metric associated with glycemic outcomes (3). Percentage use was determined by the clinician at the clinic visit using downloaded data. The non-CGM group was defined as individuals <21 years with T1D who did not have a documented CGM start date in ADDN after 1 April 2017; for these individuals, the CGM subsidy start date (1 April 2017) was used as the surrogate “start of intervention” date.
Mean and 95% CIs for HbA1c are presented for each 3-month period. Differences in the mean HbA1c between different groups at each time period were assessed using the GEE model with a Gaussian family distribution and an exchangeable correlation matrix with identity link function. Data were analyzed in Stata 14 software (StataCorp, College Station, TX), and P values <0.05 were considered statistically significant.
Data and Resource Availability
This research was conducted as part of the ADDN. The CGM uptake data were sourced from the NDSS. The NDSS is an initiative of the Australian Government administered by Diabetes Australia.
Results
Uptake Rates
Prior to the commencement of the CGM subsidy in April 2017, CGM usage was recorded as <5% in people with T1D <21 years of age. Up to 31 Dec 2019, 14,367 individuals <21 years were listed on the NDSS database, of these 11,159 (79%) registered for CGM supply. Uptake was lower in those aged 15–21 years (75%) compared with younger age-groups, who had similar rates of uptake across the age span (85%, 89%, and 88% in 0–5 years, 6–10 years, and 10–15 years, respectively).
The ADDN registry captured 3,060 of 14,367 individuals (21%) with T1D <21 years in Australia and CGM data on 2,625 of 11,159 individuals (23%) who were registered for CGM supply. Demographic characteristics of ADDN registrants <21 years is summarized in Table 1. Those choosing not to use CGM were older, had longer duration of diabetes, were more likely to be managed with a multiple daily insulin (MDI) regimen, and had higher baseline HbA1c compared with those who elected to commence CGM use.
Table 1.
Demographic and clinical characteristics of the CGM and non-CGM cohorts
| Variable | CGM | Non-CGM* | All | P value‡ | Test |
|---|---|---|---|---|---|
| n = 2,625 | n = 435 | N = 3,060 | |||
| Sex | 0.067 | Pearson χ2 | |||
| Female | 1,283 (48.9) | 192 (44.1) | 1,475 (48.2) | ||
| Male | 1,342 (51.1) | 243 (55.9) | 1,585 (51.8) | ||
| Age at baseline,† mean (SD), years | 11.5 (4.1) | 13.9 (3.8) | 11.8 (4.1) | <0.001 | Two-sample t test |
| Age at diagnosis, mean (SD), years | 7.7 (3.9) | 8.5 (4.3) | 7.9 (4.0) | <0.001 | Two-sample t test |
| Diabetes duration at baseline,† years | 2.6 (0.3, 6.1) | 4.5 (1.9, 8.1) | 2.9 (0.3, 6.4) | <0.001 | Wilcoxon rank sum |
| Insulin regimen | <0.001 | Pearson χ2 | |||
| MDI | 1,113 (49.4) | 242 (61.6) | 1,355 (51.2) | ||
| CSII | 933 (41.4) | 116 (29.5) | 1,049 (39.6) | ||
| BD | 201 (8.9) | 35 (8.9) | 236 (8.9) | ||
| HbA1c at baseline,† mean (SD), % | 8.3 (1.5) | 8.6 (1.9) | 8.4 (1.6) | <0.001 | Two-sample t test |
Data are presented as n (%), median (interquartile range), or as indicated. MDI defined as basal bolus, long-acting plus rapid insulin with meals; CSII, continuous subcutaneous insulin infusion; BD, twice-daily insulin (NPH/Rapid with breakfast and long acting/rapid with evening meal).
The non-CGM cohort is defined as having a clinic visit after 1 April 2017 (CGM subsidy start date) and not registering for CGM.
Baseline age, diabetes duration, and HbA1c for the CGM cohort is defined as the value on the closest clinic visit before the CGM start date and for the non-CGM cohort is defined as the value on the closest clinic visit before 1 April 2017 (when the subsidy became available).
CGM vs. non-CGM.
Glycemic Control
Table 2 shows the results of the analysis of the impact of CGM on glycemic control using the GEE model. As shown in Table 2, there was an increase in the odds of young people having optimal glycemic control (HbA1c <7.0%) from 6 months post-CGM start. The odds ratio (OR) continued to improve and more than doubled the reference rate at baseline from 12 months, and this was maintained to 24 months post-CGM commencement.
Table 2.
OR of HbA1c <7% and HbA1c ≥9% from 6 months before CGM start to 24 months after CGM start
| OR | 95% CI | P value | ||
|---|---|---|---|---|
| HbA1c <7.0% (53 mmol/mol) | ||||
| Before CGM | ||||
| 6 months | 1.07 | 0.89 | 1.28 | 0.470 |
| 3 months | 1.01 | 0.85 | 1.20 | 0.933 |
| CGM start | Reference | |||
| After CGM | ||||
| 3 months | 1.16 | 0.99 | 1.37 | 0.061 |
| 6 months | 1.42 | 1.21 | 1.66 | <0.001 |
| 9 months | 1.78 | 1.53 | 2.08 | <0.001 |
| 12 months | 2.49 | 2.13 | 2.90 | <0.001 |
| 15 months | 2.31 | 1.97 | 2.71 | <0.001 |
| 18 months | 2.35 | 2.00 | 2.77 | <0.001 |
| 21 months | 2.36 | 1.99 | 2.80 | <0.001 |
| 24 months | 2.30 | 1.93 | 2.75 | <0.001 |
| HbA1c ≥9.0% (75 mmol/mol) | ||||
| Before CGM | ||||
| 6 months | 0.78 | 0.70 | 0.87 | <0.001 |
| 3 months | 0.83 | 0.75 | 0.92 | <0.001 |
| CGM start | Reference | |||
| After CGM | ||||
| 3 months | 0.80 | 0.72 | 0.88 | <0.001 |
| 6 months | 0.71 | 0.64 | 0.79 | <0.001 |
| 9 months | 0.54 | 0.49 | 0.61 | <0.001 |
| 12 months | 0.31 | 0.28 | 0.35 | <0.001 |
| 15 months | 0.28 | 0.24 | 0.31 | <0.001 |
| 18 months | 0.29 | 0.25 | 0.33 | <0.001 |
| 21 months | 0.35 | 0.31 | 0.40 | <0.001 |
| 24 months | 0.34 | 0.30 | 0.39 | <0.001 |
Conversely, as shown in the same table, there was a significant reduction in the OR of having an HbA1c ≥9% apparent from 3 months after introduction of CGM. At 12 months, there was a reduction to one-third from baseline of the proportion of individuals with HbA1c ≥9%, and this was largely maintained at 2 years after commencement of CGM.
Clinically Severe Hypoglycemia and DKA Rates
Absolute rates of severe hypoglycemia were 10.7 events/100 patient-years at baseline and 6.8 events/100 patient-years at 24 months post-CGM start. At 2 years after commencement, the OR compared with baseline of a severe event was 0.59 (95% CI 0.48–0.78; P < 0.001). Rates of DKA were analyzed in adolescent and preadolescent age-groups. In preadolescents (<12 years age), the rate of DKA was 1.7 at baseline and 2.2 events/100 patient-years 2 years post-CGM. In the adolescent age-group, the rates were 2.1 events/100 patient-years pre-CGM and 3.4 events/100 patient-years 2 years post-CGM (P = 0.02).
Rates of Usage in the CGM Uptake Group and Glycemic Outcomes
In the ADDN registry, 2,625 of 3,060 participants (79%) used CGM. Reported usage was recorded at each visit as a percentage. In the ADDN data set, of those with documented CGM percentage use, 65% used CGM ≥75% of the time and 31% used CGM <25% of the time. Few (4%) had documented usage rates between 25 and 75%. Usage rates were similar across the age-groups.
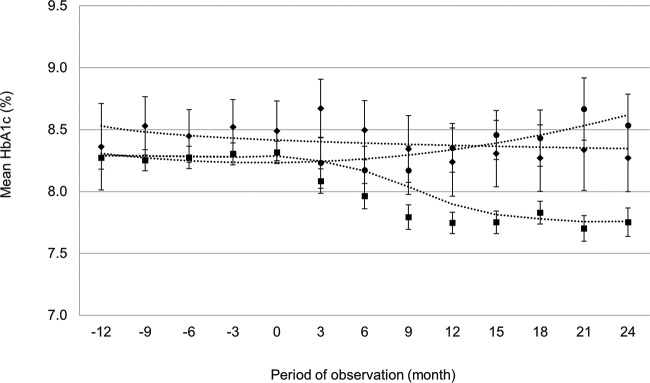
Figure 1 shows the mean HbA1c in the 12 months prior to introduction of CGM and the first 2 years following CGM uptake in those using CGM ≥75% of the time compared with nonusers and those registered as using CGM but with usage <25% of the time. As shown, there was a continued fall in HbA1c with CGM use ≥75% over the first 18 months and a significant difference at 24 months compared with CGM use <25% (7.8% ± 1.3% vs. 8.6% ± 1.8%, use >75% vs. use <25% respectively, P < 0.001).
Figure 1.
Mean HbA1c over time. The diamonds (♦) represent individuals with diabetes who did not use CGM (non-CGM), the circles (●) represent those who were using CGM <25% of the time, and the squares (▪) represent patients who were using CGM >75% of the time. Data are mean ± 95% CIs.
DKA rates were reduced in the >75% usage group compared with the <25% usage (incidence rate ratio 0.49, 95% CI 0.33–0.74, P < 0.001).
Table 3 shows HbA1c at baseline and at 12 and 24 months following CGM subsidy in three age-groups (0 to <10 years, 10 to <15 years, and 15 to 21 years of age). As shown, the greatest improvement in glycemic control was seen in the older age-group (1.2% HbA1c difference at 12 months and 0.8% difference at 24 months).
Table 3.
Mean HbA1c by age-group and CGM usage at baseline and 12 and 24 months after CGM start
| CGM usage | Age-group (years) | Baseline | 12 months | 24 months |
|---|---|---|---|---|
| HbA1c (%) | HbA1c (%) | HbA1c (%) | ||
| <25% | 0–10 | 7.8 (1.1) | 7.5 (1.2) | 7.7 (1.3) |
| 10–15 | 8.2 (1.4) | 8.1 (1.6) | 8.5 (1.8) | |
| 15–21 | 8.5 (1.6) | 9.0 (2.0)* | 8.8 (1.8)* | |
| >75% | 0–10 | 7.8 (1.1) | 7.5 (1.0)* | 7.4 (0.9)* |
| 10–15 | 8.2 (1.4) | 7.9 (1.3) | 7.9 (1.3) | |
| 15–21 | 8.5 (1.6) | 7.8 (1.3)* | 8.0 (1.6)* |
Data are mean (SD). P values for comparison between the baseline and 12 months post-CGM start and baseline and 24 months post-CGM start were calculated using the GEE model with a Gaussian family distribution and an exchangeable correlation matrix with identity link function.
Denotes having a P value of <0.05.
Conclusions
Although multiple well-controlled clinical trials have demonstrated significant glycemic benefits with CGM use (4,13,14), long-term, real-world, population-based studies are limited (2,15), with very few published outcomes for children and young people (16). The introduction of fully subsidized CGM in Australia for all young people with T1D aged <21 years provided a unique opportunity to determine the impact of the introduction of universal unrestricted access to CGM on glycemic measures in a real-world setting. Evaluation of this policy change was facilitated by the availability of prospective national registries. The outcomes are of interest, not only because the study is population based but also because access to CGM was equitable, and the effect of socioeconomic disparities between participants might be reduced (7,8).
Rates of uptake and continued use are of particular interest. Prior to the subsidy, <5% of youth <21 years with T1D were using CGM. It is noteworthy that following the introduction of the subsidy, this increased to 79% in this age-group nationally. Of these, 65% of registrants continued to use CGM >75% of the time (or 55% of all with T1D aged <21 years), with higher rates in the younger children. The rates of uptake and continued use are higher than in past reports from, for example, the JDRF CGM trial (3) and the 2014 report from the T1D Exchange (17). Although the increased rates of use may reflect improvements in the technology and usability (15,18–20), it can be speculated that the absence of a cost to the person or family living with T1D and the simplicity of access and administration of the products also contributed to the change.
A major finding in this report was the improvements in glycemic outcomes, which were sustained over time in those using CGM following the national subsidy. The likelihood of achieving the internationally defined target HbA1c of <7% increased more than twofold from baseline, and the mean HbA1c was reduced by 0.3–0.5% overall. This order of reduction in HbA1c is concordant with results from the majority of randomized controlled trials, which have demonstrated improvements in HbA1c of 0.3–0.6% (3,19,21–24). The improvement in likelihood of achieving optimal glycemic control is paralleled by a reduced likelihood of a suboptimal HbA1c (arbitrarily defined as ≥9% for this analysis) confirmed by a reduction of the adjusted OR to one-third of baseline. It is important to note that in the 6 months prior to uptake of CGM, there was a rise in HbA1c to baseline and that following CGM introduction, the improvement in glycemic control was sustained over the 2 years of follow-up.
The analyses described above did not include a comparison with the cohort that did not take up CGM. The non-CGM group was significantly different from the CGM cohort in age, duration of diabetes, glycemic control at baseline, and use of MDI versus continuous subcutaneous insulin infusion. A comparison of HbA1c change over time in CGM users versus nonusers would reflect differences in the characteristics of those electing to use CGM, as well as the effect of CGM itself, and this would have introduced major bias. The analysis used is an important strength of the study as the CGM participants were used as their own controls.
It can be speculated that those not taking up CGM are already experiencing difficulty with diabetes management, and it will be important to further characterize this group with the aim of improving uptake with, for example, targeted programs. In those who elected not to register for use of CGM (CGM nonusers), there was an increase in HbA1c over the 2 years of analysis in all age-groups, an increase that is well described, particularly in adolescence (25). In the CGM users, the adolescent subgroup showed the greatest degree of absolute HbA1c reduction, while the nonusers, conversely, had the greatest increase in HbA1c over the 2 years following the time point of introduction of subsidized CGM. There are few interventions that have been shown to improve glycemia in adolescents and young adults, and it is promising that the real-world data from this report mirror recent trial data (4). Considering the reduced risk of diabetic complications with improved glycemic control, it could be speculated that the benefits will justify the costs of the subsidy, but this will have to await detailed health economic analysis.
The reduction in the incidence of severe hypoglycemia after CGM introduction is consistent with results from randomized trials that have shown significant improvements in time in hypoglycemia with use of CGM (18,19). Although older trials that included pediatric studies did not show a reduction in severe hypoglycemia events (Cochrane review in 2012 [26]) with CGM compared with self-monitoring of blood glucose, the technology has changed significantly with alerts and ability for a third party to monitor. The increasing use of suspend-before-low algorithms means that going forward, we will be increasingly unable to determine whether reductions in hypoglycemia are a result of CGM per se or the suspend algorithms, although both depend on CGM availability. The rates of hypoglycemia may reduce further with integration of CGM and insulin delivery.
We did not find a clinically significant change in rates of DKA in the of analysis of the overall sample, and this could be because the baseline rates were low and lower than published rates from large samples (27). Other studies examining CGM impact on DKA had very low rates of DKA events, perhaps due to the nature of patient selection for clinical trials (19,24). Although a definitive answer regarding the impact of CGM on DKA rates could not be determined from the analysis of the overall sample, when the outcomes were limited to those with >75% CGM usage, a reduction in DKA rates was detected, a result consistent with a 1-year study from the Diabetes-Patienten-Verlaufsdokumentation (DPV) registry (28).
The current report has a number of strengths and limitations. Strengths include the study design, a multisite national evaluation, and a longitudinal prospective study over a longer time period than has been reported previously. The core analysis did not require comparison with those choosing not to use CGM, thus removing a potential major bias. The universal nature of the subsidy allowed the analysis of CGM use without the confounding factor of health disparity in access. A limitation results from the multisite nature and the lack of information on models of care used in each center, and because of the rapid introduction of the subsidy, each site will have had different approaches to patient education.
This study suggests that universal funding of CGM in a population results in rapid uptake and continued use in the majority. To date, improvements in clinical measures of glycemic outcomes have been demonstrated and, importantly, maintained. This information will inform comprehensive economic analyses, future policy decisions, and serve as a model of evaluation for future new diabetes technologies.
Article Information
Acknowledgments. The authors are grateful to JDRF Australia, the Australian Research Council, and to the children and young people with diabetes and their families who provided the data.
Funding. This research was supported by JDRF Australia (4-SRA-2016-169-M-B), the recipient of the Australian Research Council Special Research Initiative in Type 1 Juvenile Diabetes.
The study funders had no role in study design, data collection, analysis, interpretation, or the manuscript preparation.
Duality of Interest. No potential conflicts of interest relevant to this article were reported.
Author Contributions. S.R.J., D.J.H.-W., and T.W.J. contributed to conceptualization, literature search, data collection and verification, data analysis and interpretation, and writing the draft and review of the manuscript. M.C. contributed to data curation, data analysis and interpretation, and writing the draft and review of the manuscript. A.E. contributed to data verification, analysis and interpretation, and writing the draft and review of the manuscript. T.W.J. is the guarantor of this work and, as such, had full access to all of the data in the study and takes responsibility for the integrity of the data and the accuracy of the data analysis.
Footnotes
This article contains supplementary material online at https://doi.org/10.2337/figshare.16940740.
This article is featured in a podcast available at diabetesjournals.org/journals/pages/diabetes-core-update-podcasts.
A list of members of the ADDN Study Group can be found in the supplementary material online.
Contributor Information
Collaborators: ADDN Study Group:, Maria Craig, Kym Anderson, Geoff Ambler, Helen Barrett, Jenny Batch, Philip Bergman, Fergus Cameron, Peter Colman, Louise Conwell, Chris Cooper, Jennifer Couper, Elizabeth Davis, Martin de Bock, Kim Donaghue, Jan Fairchild, Gerry Fegan, Spiros Fourlanos, Sarah Glastras, Leonie Gray, Shane Hamblin, Paul Hofman, Dianne Jane Holmes-Walker, Neville Howard, Michelle Jack, Steven James, Craig Jefferies, Stephanie Johnson, Jeff Kao, Bruce R. King, Antony Lafferty, Michelle Martin, Robert McCrossin, Mark Pascoe, Ryan Paul, Dorota Pawlak, Alexia Peña, Sarah Price, Darrell Price, Christine Rodda, David Simmons, Richard Sinnott, Alan Sive, Carmel Smart, Monique Stone, Steve Stranks, Elaine Tham, Charles Verge, Glenn Ward, Ben Wheeler, Judy Williams, Helen Woodhead, Nick Woolfield, and Anthony Zimmermann
References
- 1. Phelan H, Clapin H, Bruns L, et al. The Australasian Diabetes Data Network: first national audit of children and adolescents with type 1 diabetes. Med J Aust 2017;206:121–125 [DOI] [PubMed] [Google Scholar]
- 2. Foster NC, Beck RW, Miller KM, et al. State of type 1 diabetes management and outcomes from the T1D Exchange in 2016-2018. Diabetes Technol Ther 2019;21:66–72 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3. Juvenile Diabetes Research Foundation Continuous Glucose Monitoring Study Group; Tamborlane WV, Beck RW, Bode BW, et al. Continuous glucose monitoring and intensive treatment of type 1 diabetes. N Engl J Med 2008;359:1464–1476 [DOI] [PubMed] [Google Scholar]
- 4. Laffel LM, Kanapka LG, Beck RW, et al.; CGM Intervention in Teens and Young Adults with T1D (CITY) Study Group; CDE10 . Effect of continuous glucose monitoring on glycemic control in adolescents and young adults with type 1 diabetes: a randomized clinical trial. JAMA 2020;323:2388–2396 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Cardona-Hernandez R, Schwandt A, Alkandari H, et al.; SWEET Study Group . Glycemic outcome associated with insulin pump and glucose sensor use in children and adolescents with type 1 diabetes. Data from the international pediatric registry SWEET. Diabetes Care 2021;44:1176–1184 [DOI] [PubMed] [Google Scholar]
- 6. Miller KM, Hermann J, Foster N, et al.; T1D Exchange and DPV Registries . Longitudinal changes in continuous glucose monitoring use among individuals with type 1 diabetes: international comparison in the German and Austrian DPV and U.S. T1D Exchange registries. Diabetes Care 2020;43:e1–e2 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Lipman TH, Hawkes CP. Racial and socioeconomic disparities in pediatric type 1 diabetes: time for a paradigm shift in approach. Diabetes Care 2021;44:14–16 [DOI] [PubMed] [Google Scholar]
- 8. Addala A, Auzanneau M, Miller K, et al. A decade of disparities in diabetes technology use and HbA1c in pediatric type 1 diabetes: a transatlantic comparison. Diabetes Care 2021;44:133–140 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9. Lai CW, Lipman TH, Willi SM, Hawkes CP. Racial and ethnic disparities in rates of continuous glucose monitor initiation and continued use in children with type 1 diabetes. Diabetes Care 2021;44:255–257 [DOI] [PubMed] [Google Scholar]
- 10. Nørgaard K, Schmidt S. Is reimbursement for alerts and real-time continuous glucose monitoring needed? Lancet 2021;397:2230–2232 [DOI] [PubMed] [Google Scholar]
- 11. Clapin H, Phelan H, Bruns L Jr, et al.; Australasian Diabetes Data Network (ADDN) Study Group . Australasian Diabetes Data Network: building a collaborative resource. J Diabetes Sci Technol 2016;10:1015–1026 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12. Wolfsdorf JI, Glaser N, Agus M, et al. ISPAD Clinical Practice Consensus Guidelines 2018: diabetic ketoacidosis and the hyperglycemic hyperosmolar state. Pediatr Diabetes 2018;19(Suppl. 27):155–177 [DOI] [PubMed] [Google Scholar]
- 13. Thabit H, Prabhu JN, Mubita W, et al. Use of factory-calibrated real-time continuous glucose monitoring improves time in target and HbA1c in a multiethnic cohort of adolescents and young adults with type 1 diabetes: the MILLENNIALS Study. Diabetes Care 2020;43:2537–2543 [DOI] [PubMed] [Google Scholar]
- 14. Battelino T, Phillip M, Bratina N, Nimri R, Oskarsson P, Bolinder J. Effect of continuous glucose monitoring on hypoglycemia in type 1 diabetes. Diabetes Care 2011;34:795–800 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15. Charleer S, Mathieu C, Nobels F, et al.; RESCUE Trial Investigators . Effect of continuous glucose monitoring on glycemic control, acute admissions, and quality of life: a real-world study. J Clin Endocrinol Metab 2018;103:1224–1232 [DOI] [PubMed] [Google Scholar]
- 16. Cherubini V, Bonfanti R, Casertano A, et al. Time in range in children with type 1 diabetes using treatment strategies based on nonautomated insulin delivery systems in the real world. Diabetes Technol Ther 2020;22:509–515 [DOI] [PubMed] [Google Scholar]
- 17. Wong JC, Foster NC, Maahs DM, et al.; T1D Exchange Clinic Network . Real-time continuous glucose monitoring among participants in the T1D Exchange clinic registry. Diabetes Care 2014;37:2702–2709 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18. Ólafsdóttir AF, Polonsky W, Bolinder J, et al. A randomized clinical trial of the effect of continuous glucose monitoring on nocturnal hypoglycemia, daytime hypoglycemia, glycemic variability, and hypoglycemia confidence in persons with type 1 diabetes treated with multiple daily insulin injections (GOLD-3). Diabetes Technol Ther 2018;20:274–284 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 19. Beck RW, Riddlesworth T, Ruedy K, et al.; DIAMOND Study Group . Effect of continuous glucose monitoring on glycemic control in adults with type 1 diabetes using insulin injections: the DIAMOND randomized clinical trial. JAMA 2017;317:371–378 [DOI] [PubMed] [Google Scholar]
- 20. Burckhardt MA, Abraham MB, Mountain J, et al. Improvement in psychosocial outcomes in children with type 1 diabetes and their parents following subsidy for continuous glucose monitoring. Diabetes Technol Ther 2019;21:575–580 [DOI] [PubMed] [Google Scholar]
- 21. Beck RW, Bergenstal RM, Laffel LM, Pickup JC. Advances in technology for management of type 1 diabetes. Lancet 2019;394:1265–1273 [DOI] [PubMed] [Google Scholar]
- 22. Beck RW, Riddlesworth TD, Ruedy KJ, et al.; DIAMOND Study Group . Effect of initiating use of an insulin pump in adults with type 1 diabetes using multiple daily insulin injections and continuous glucose monitoring (DIAMOND): a multicentre, randomised controlled trial. Lancet Diabetes Endocrinol 2017;5:700–708 [DOI] [PubMed] [Google Scholar]
- 23. Lind M, Polonsky W, Hirsch IB, et al. Continuous glucose monitoring vs conventional therapy for glycemic control in adults with type 1 diabetes treated with multiple daily insulin injections: the GOLD randomized clinical trial. JAMA 2017;317:379–387 [DOI] [PubMed] [Google Scholar]
- 24. Heinemann L, Freckmann G, Ehrmann D, et al. Real-time continuous glucose monitoring in adults with type 1 diabetes and impaired hypoglycaemia awareness or severe hypoglycaemia treated with multiple daily insulin injections (HypoDE): a multicentre, randomised controlled trial. Lancet 2018;391:1367–1377 [DOI] [PubMed] [Google Scholar]
- 25. Miller KM, Beck RW, Foster NC, Maahs DM. HbA1c levels in type 1 diabetes from early childhood to older adults: a deeper dive into the influence of technology and socioeconomic status on HbA1c in the T1D Exchange clinic registry findings. Diabetes Technol Ther 2020;22:645–650 [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Langendam M, Luijf YM, Hooft L, Devries JH, Mudde AH, Scholten RJ. Continuous glucose monitoring systems for type 1 diabetes mellitus. Cochrane Database Syst Rev 2012;1:CD008101. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27. Maahs DM, Hermann JM, Holman N, et al.; National Paediatric Diabetes Audit and the Royal College of Paediatrics and Child Health, the DPV Initiative, and the T1D Exchange Clinic Network . Rates of diabetic ketoacidosis: international comparison with 49,859 pediatric patients with type 1 diabetes from England, Wales, the U.S., Austria, and Germany. Diabetes Care 2015;38:1876–1882 [DOI] [PubMed] [Google Scholar]
- 28. Tauschmann M, Hermann JM, Freiberg C, et al.; DPV Initiative . Reduction in diabetic ketoacidosis and severe hypoglycemia in pediatric type 1 diabetes during the first year of continuous glucose monitoring: a multicenter analysis of 3,553 subjects from the DPV registry. Diabetes Care 2020;43:e40–e42 [DOI] [PubMed] [Google Scholar]