Highlights
-
•
The presence of stress-related (Takotsubo) cardiomyopathy has also been demonstrated in COVID-19.
-
•
The proposed mechanisms of cardiac damage during the acute phase of COVID-19 include both direct -viral penetration- and indirect routes -hypoxic injury and systemic inflammation.
-
•
SARS-CoV-2 infection, especially in its severe form, is associated with an increased risk for venous thromboembolism (VTE).
-
•
Unfractionated heparin (UFH) is the first-line treatment for hemodynamic instability and emergency reperfusion for PASC.
-
•
Further studies are needed to offer current screening for the occurrence of cardiovascular problems especially myocardial infarction and heart failure in COVID-19 patients.
Keywords: COVID-19, Cardiovascular diseases, Myocardial infarction, Post covid sequelae
Abbreviations: SARS-CoV 2, severe acute respiratory syndrome coronavirus 2; COVID-19, Coronavirus disease 2019; WHO, World health organization; PACS, Post-Acute COVID-19 syndrome; TTE, transthoracic echocardiogram; ACE2, Angiotensin-converting enzyme 2; TMPRS2, transmembrane protease serine 2; RAAS, Renin-Angiotensin Aldosterone System dysregulation; IL, interleukin; TNF-Alpha, Tumor necrosis factor-alpha; DAMPs, damage-associated molecular patterns; CVD, Cardiovascular disease; CAMKII, calmodulin-dependent protein kinase II; CMR, Cardiac magnetic resonance imaging; VTE, venous thromboembolism; UFH, Unfractionated heparin; NOAC, novel oral anticoagulation
Abstract
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV 2) or coronavirus disease 2019 (COVID-19) initially surfaced in December 2019 from Wuhan, China, sweeping the world with various strains, forcing the WHO to declare a pandemic epidemic in March 2020. Furthermore, COVID-19 manifests with a wide array of presentations from fever and fatigue to severe respiratory and cardiovascular complications. Post-COVID-19 syndrome is poorly understood affecting COVID-19 survivors at all levels of disease severity. The disease is most associated with post-discharge dyspnea and fatigue. However, other persistent symptoms as chest pains, palpitations, smell, and taste dysfunctions. Patients with high concentrations of CRP and creatinine in the acute phase of Covid-19 are more prone to cardiac sequelae. Therefore, high levels of cardiac-sensitive troponin and hypokalaemia can also be used for risk stratification. Furthermore, Cardiac damage can manifest as myocarditis, pericarditis, rhythm abnormalities. The use of different diagnostic modalities like electrocardiogram (ECG), echocardiogram, and cardiac magnetic resonance imaging (MRI)(CMR) to evaluate the myocardial damage were studied. However, Cardiovascular complications are a common manifestation of PASC, classification of severity of cardiac symptoms and the emergence of CMR as a diagnostic tool needs more evidence.
1. Introduction
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV 2) or coronavirus disease 2019 (COVID-19) initially surfaced in December 2019 from Wuhan, China, sweeping the world with various strains, forcing the WHO to declare a pandemic epidemic in March 2020 [1]. COVID-19 is a novel viral disease that primarily affects the upper and lower respiratory tracts. However, mounting evidence suggests that COVID-19 can cause a wide range of clinical manifestations by affecting multiple systems. COVID-19 can range from asymptomatic to severe organ affection and tissue damage (Table 1), (Fig. 1).
Table 1.
Classification of COVID.
| Mild Illness | Moderate Illness | Severe Illness | Critical illness |
|---|---|---|---|
| Fever, cough, sore throat, malaise, headache, myalgia, nausea, vomiting, diarrhea, loss of taste, and smell) | Evidence of lower respiratory Tract Infection during clinical assessment or imaging | Same as before | Respiratory failure, septic shock, and/or multiple organ dysfunction. |
| No SOB OR imaging findings | SOB or Positive imaging findings | lung infiltrates > 50%. | – |
| – | SpO2 ≥ 94% | SpO2 < 94% , (PaO2/FiO2) < 300 mm Hg And /Or respiratory rate > 30 | Intubated or ICU admitted |
Fig. 1.
Post-acute COVID-19 syndrome: An overview and approach to classification.
COVID-19 manifests with a wide array of presentations, which ranges from fever, fatigue, and diarrhea to severe respiratory and cardiovascular complications and multiple organ failure leading to mortality [1]. More recently, various reports from around the globe have reported the persistence of symptoms and SARS-CoV-2 virus beyond the defined acute phase timeline [2]. Therefore, the Royal College of General Practitioners (RCGP) has divided COVID-19 infection into 3 timeframe points—signs and symptoms of COVID-19 infection persistent up to 4 weeks called Acute COVID-19, from 4 till 12 weeks called ongoing symptomatic COVID-19, and if signs and symptoms persist after 12 weeks it is called a post-COVID-19 syndrome.[3] The term ‘Long-COVID-19′ is given to the signs and symptoms that continue or develop after the ‘acute COVID-19′ phase and include both ‘ongoing symptomatic COVID-19′ and ‘post COVID-19 syndrome’[3], [4]. While many people with mild-moderate disease recover within 2 weeks, there is a percentage of the population which do not return to baseline even after 14–21 days [3]. Tenforde et al. found this percentage to be about 35% of symptomatic respondents, of which 47% were>50 years old [4]. The entire spectrum of the post-acute COVID-19 syndrome has been given numerous terms, including long COVID, long-haul COVID, and post-acute COVID syndrome [2], [3].
Post-COVID-19 syndrome is poorly understood as it affects COVID-19 survivors at all levels of disease severity and across all age ranges. The disease is most associated with post-discharge dyspnea and fatigue. However, other persistent symptoms as chest pains, palpitations, myalgia, smell and taste dysfunctions, cough, headache, and gastrointestinal and cardiac-related problems. All of which may persist for up to six months post-discharge or from disease onset [2], [3]. The emergence of post-COVID 19 cardiovascular manifestations is expected to impose a further detrimental effect on the incidence, prevalence, and economic projections of heart disease. Limited elucidation of its clinical course has prompted the requirement to ascertain the persistent symptoms and clinical outcomes. Therefore, our focus in this review is more on the post-acute COVID-19 syndrome, especially the cardiovascular effects.
2. Methods:
We performed a thorough literature review based on the PubMed electronic bibliographic database, Scopus, EMBASE, Web of science. The following descriptors were used in the search engines advanced tool: “COVID-19”, “SARS-CoV”, “Cardiovascular Risk Factors”, “Hypertension”, “Arrhythmias”, “Myocarditis”, “post-covid sequels”, “post-covid syndrome”. We included retrospective studies, prospective studies, meta-analyses regarding the cardiovascular implications related to COVID-19. Articles with a central theme diverging or not related to the cardiovascular complications associated with post-COVID-19 infection were excluded from the revision. Articles that were not in English were also excluded.
3. Discussion:
To the best of our knowledge, this is the first review article to intensely investigate the cardiovascular complications of post-acute COVID-19 syndrome.
3.1. Cardiac complications:
The most accepted pathophysiology to date is long-term tissue damage not only in the lungs but also in other vital organs due to pathological inflammation which is due to a variety of intercalated causes as viral persistence, immune dysregulation, and autoimmunity. it is important to note that replication-competent virus is rarely recovered beyond 20 days after symptom onset [3]; this suggests that persistent symptoms are driven primarily by immunological phenomena. Another possibility is that lingering virus continues to be present in immunologically privileged sites within the body, where it can be difficult for the immune system to eradicate.
A frequent consequence of the COVID-19 disease is myocardial damage, which is linked with a poor prognosis. Patients with myocardial damage were also shown to have a more severe acute illness. As indicated by higher inflammatory markers such as c-reactive protein, higher serum creatinine, more pulmonary infiltrates and opacities on chest imaging, and greater rates of non-invasive and invasive ventilation. Furthermore, older patients with comorbidities such as coronary artery disease, hypertension, diabetes, and chronic renal disease were found to have a higher likelihood of having a severer disease [1], [2], [3] TTE imaging indicated regional wall motion anomalies, systolic left or right ventricular dysfunction, diastolic dysfunction, and pericardial effusion during the acute phase of COVID-19. [4]
The mortality and morbidity due to cardiovascular complications in COVID-19 patients are higher when there is evidence of myocardial involvement, as implicated by Mitrani et al [10] Chest pain was reported in up to ∼ 20% of COVID-19 survivors at 60 d follow-up while ongoing palpitations and chest pain were reported in 9 and 5%, respectively, at 6 months follow-up in the post-acute COVID-19 Chinese study. In their follow-up study, Carvalho-Schneider, C. et al. found that out of 150 study participants, chest pain was reported in 27 (18.0) participants at 30 days follow-up and 17 (13.1) participants at 60 days. Palpitations were reported in 9 (6.5) and 14 (10.9) participants, while Dyspnea/shortness of breath in 16 (10.7) and 10 (7.7) participants at 30 and 60 days follow up, respectively [11].
Nannoni et al in a pooled meta-analysis calculated a total incidence of 1.4% acute cardiovascular complications with COVID-19 [9]. In the earliest study of 138 hospitalized patients of Wuhan, China, cardiac symptoms in acute COVID-19 were documented, with acute cardiac damage in 7.2%, shock in 8.7%, and arrhythmias in 16.7% [5]. According to Puntmann et al., in a matched prospective cohort analysis that lasted a median of 71 days after COVID-19 diagnosis, 78 % of patients had cardiac involvement. Irrespective of preexisting conditions, 60% of which showed cardiac inflammation, regional scarring, and pericardial enhancement on cardiac magnetic resonance imaging [6]. Participants who recovered from COVID-19 had lower left ventricular ejection fraction (57 % vs. 62 %; P < .001) and were more likely to have detectable high-sensitive troponin T (>3 pg/mL; 71% vs. 31%) in comparison with risk factor–matched control patients.
In addition, Another study of 52 critically ill patients from Wuhan, China, with COVID-19 showed myocardial injury, as indicated by high-sensitivity troponin>28 ng/L in 29% of the patients, the study showed development significant cardiac diastolic impairment without systolic involvement was observed in patients who experienced a myocardial injury but not in patients without cardiac involvement within 30 days following the infection as well as at six months after the acute COVID-19 phase were [7]. A study of 416 COVID-19 patients showed 20% with myocardial injury, as indicated by troponin I>0.04 ng/mL [2]. All these findings established a clear connection between COVID-19 infection and myocardial damage, necessitating cardiac assessment of post-COVID-19 patients, particularly those who suffered cardiac troponin rise during the acute phase.
3.2. Mechanisms of cardiac complications:
To better grasp the acute and post-acute pathophysiological manifestations of SARS-CoV2 on the Cardiac system, it is fundamental to understand the underlying molecular and biological processes that result in cardiac dysfunction. Initially thought of predominantly as respiratory disease, COVID-19 is now regarded as a wide spectrum syndrome ranging from asymptomatic infection to critical life-threatening infection [5]
The severe acute respiratory syndrome coronavirus 2 (SARS-CoV2) is the largest known RNA virus like other viral infections, the establishment of the acute infection requires the entry of the SARS-CoV2 into the host cell [6], [7]. The required entry is dependent upon the interaction between the viral spike glycoprotein, the host cell membrane ACE2 receptor, and the host cell protease systems such as the transmembrane protease serine 2 (TMPRSS2) [7]. The ACE2 receptor is a transmembrane aminopeptidase that is responsible for various physiological functions in the cardiovascular system [8]. From the perspective of physiology, ACE2 mediates a vital role in the neurohumoral regulation of the cardiovascular system. Its expression is mostly noted in the vascular endothelium, oral mucosa, tongue, gut, lungs, kidneys, heart, and testis [9]. In an RNA sequencing study, ACE2 expression was noted in 9.87% of cardiomyocytes of the failing heart [9]. Its expression was also noted in the healthy human heart at an enrichment rate of 6.75% [9]. More specifically, the highest expression of ACE2 was noted in the cardiomyocytes and pericytes, while the lowest expression of ACE2 was noted in cardio-fibroblasts, endothelial cells, epicardial adipose tissue, and other various cardio-specific immunoregulatory cells [9].
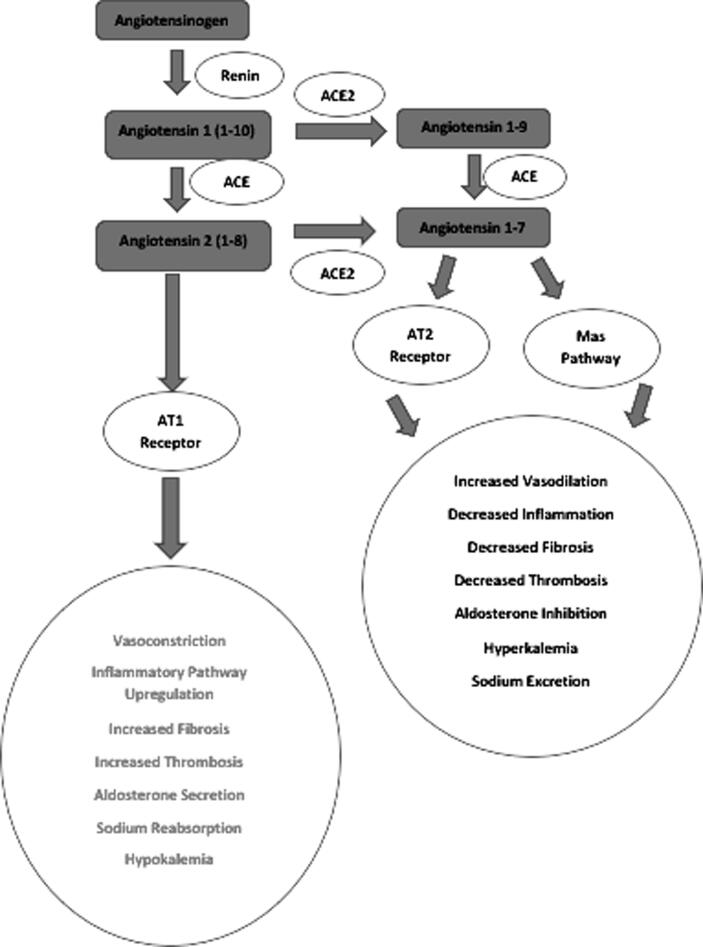
The proposed mechanisms of cardiac damage during the acute phase of COVID-19 include both direct and indirect routes. Direct cardiac injury occurs via the viral infiltration of cardiomyocytes [10]. Whereas indirect injury is known to be mediated by respiratory failure induced hypoxic injury, overwhelming cytokine release, systemic inflammation, hypercoagulability, Renin-Angiotensin-Aldosterone System dysregulation (RAAS), plaque destabilization, and myocardial supply–demand mismatch [10] (Fig. 2). Concerning the post-acute COVID-19 syndrome, the potential pathophysiological mechanisms remain unknown. However, it has been hypothesized that mechanisms implicated in PACS are thought to be ramifications of altered physiological states and mechanical/anatomical damage to the cardiac system during the acute phase of COVID-19. These mechanisms include post-inflammation residual damage, immune system dysregulation, post-critical illness complications, inadequate antibody response, and ongoing underlying viral infection [3].
Fig. 2.
RAAS pathway regulation and its cardio-specific effects.
Upon interaction of viral S protein and ACE2, S1 and S2 subunits are generated by host TMPRSS2 mediated cleavage at the arginine residue site [11]. Further entry into the cell is mediated by the S2 subunit-induced membrane fusion and viral endocytosis [11]. Upon entry into the cell, the cytoplasmic replication of viral RNA results in the production of virion particles, which further attach to the cell membrane and act as a source of infection amplification [11]. Physiologically, ACE2 is known to convert angiotensin 1 and 2 into cardioprotective peptides such as angiotensin 1–7/angiotensin 1–9 [11]. SARS-CoV2 mediated downregulation of ACE2 has been reported in the literature [12]. Therefore, this abolishes the synthesis of cardioprotective peptides (angiotensin 1–7/angiotensin 1–9) and predisposes to cardiac and vascular damage [13], [14].
In addition, the enhanced activity of the angiotensin 2/AT1 pathway results in hypertrophy, fibrosis, hyper inflammation, and cardiac remodeling [15]. These pathological changes in the histological and gross morphology of the heart can predispose patients to various cardiac insults in the post-acute phase of COVID-19. In a cohort study, Chen et al. reported that hypokalemia was prevalent in COVID patients and associated with a poor prognosis [16]. Therefore, one hypothesized biomarker of this RAAS alteration can be hypokalemia [13], [16]. On the other hand, factors that promote ACE2 upregulation can increase susceptibility to COVID by enhancing cellular viral loading [12].
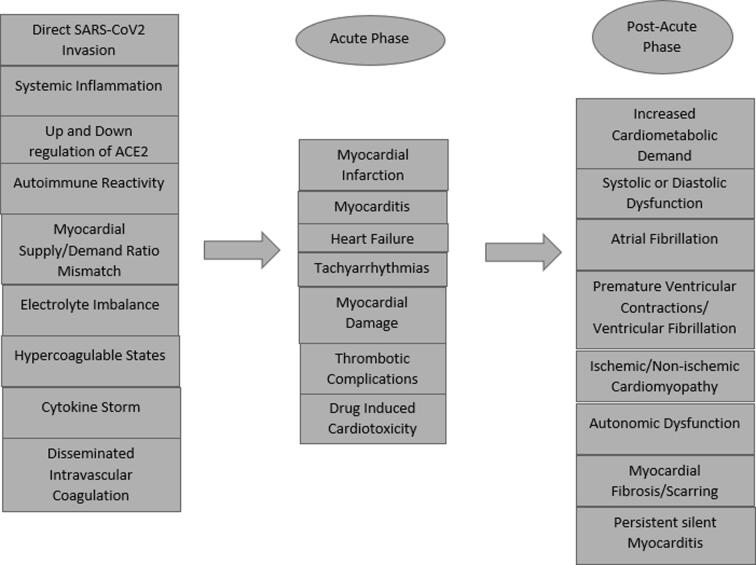
The notion of myocardial involvement in patients with COVID-19 has also been reported. In an analysis of 39 cases conducted by Linder et al., SARS-CoV2 was reported in the myocardium of 24 cases (61.5%) [17]. In addition, SARS-CoV2 was mostly localized to the interstitial cells and macrophages invading the myocardium [17]. Referring to the subsequent release of cytokines and immune system dysregulation which can result in myocardial damage [18], [19]. In COVID- 19 patients, cytokine storm has been a consistent finding among patients [20], [21]. The implicated cytokines include IL-2, IL-6, IL-7, IL-10, GM-CSF, TNF-Alpha, IP-10, MCP-1 and MIP-1A [22], [23]. Myocardial damage due to cytokine-induced generation of reactive oxygen species results in the leakage of intracellular histones, damage-associated molecular patterns (DAMPs), and oxidized lipoproteins [23]. These released molecules activate the inflammatory cascade in a vicious cycle resulting in extensive myocardial damage [23] (Fig. 3).
Fig. 3.
The pathophysiological mechanisms of cardiac involvement in Acute COVID-19 and post-acute COVID-19 syndrome.
Clinically relevant myocardial dysfunction can present as myocarditis, heart failure, stress cardiomyopathy, and cardiogenic shock [24]. Direct myocardial damage can also occur because of loss of protein translational capabilities and cellular homeostasis [24]. In the post-acute phase of COVID-19, the cytokine-mediated damage can translate into thrombogenesis, decreased oxygen supply, coronary plaque destabilization, progression of chronic CVD into unstable disease, increased metabolic demand, and reduced cardiac reserve [25].
Interestingly, ACE2 is also detected in the stromal fibroblasts located in the spongiosa layer of the heart valves [26]. More specifically, the ACE2/Angiotensin-(1–7)/Mas receptor pathway is expressed in the aortic valve cusps [32]. Decreased expression of ACE2 in stenotic valves has been noted from RT-PCR [26]. Downregulation of ACE2/Angiotensin-(1–7)/Mas receptor pathway can promote valvular fibrosis, inflammation, and sclerosis [27]. Angiotensin 2-AT1R pathway-derived pro-inflammatory cytokines can further promote valvular inflammation [27]. Over time, these pathological changes may also alter the stability of pre-existing valvular lesions and may act as a source of emboli for cardioembolic stroke.
The presence of stress-related Takotsubo cardiomyopathy has also been demonstrated in COVID-19 [28]. Due to the overwhelming stress and systemic inflammation, catecholamine surge and coronary vasculature dysfunction can result in myocardial stunning [28]. The surge in catecholamines further enhances immune cell alpha-1 adrenergic receptor-mediated production of pro-inflammatory cytokines such as IL-6 [28]. Supra-physiological catecholamine serum concentrations can induce a shift in beta 2 receptor coupling from Gs to Gi [29]. This shift downregulates the contractile function and is manifested usually as apical hypokinesia in the ECG [29]. Furthermore, the supraphysiological levels of catecholamines further exacerbate the hyper contraction of the LV apex, LV outflow obstruction, and the myocardial oxygen demand [29]. On the contrary, the switch from Gi to Gs coupling can protect the myocytes from Gs overstimulation mediated by myocyte apoptosis [30].
As per a worldwide survey of COVID-19 associated arrhythmias, the most noted cardiac electrical disturbances include atrial arrhythmias, ventricular arrhythmias, and bradyarrhythmias [31]. Multiple mechanisms have been hypothesized for the development of arrhythmias, including the COVID-19 associated electrolyte disturbances in the form of hypomagnesemia and hypokalemia [32]. Other predisposing factors include drug-induced toxicity, direct oxidized Ca2+/calmodulin-dependent protein kinase II (CAMKII), and systemic inflammation [33], [34]. Furthermore, COVID-19 vaccines have been recently debated about the risk the hold for cardiac complications, in a systematic review by Fazlollahi et al. there was an association between cardiac complications and COVID-19 vaccines with myocarditis/myopericarditis being the most cardiac complications (n = 227) among their 243 patients. Pericarditis was reported in seven patients and myocardial infarction in three patients, yet authors called for larger observational studies to draw a valid statistical correlation [35]
3.3. Diagnosis of cardiac complications:
Clinical indicators of myocardial damage include elevated cardiac biomarkers such as troponin I, ST-segment, and T wave changes on electrocardiogram (ECG), and newly reduced left ventricular ejection fraction (LVEF) on cardiac imaging [8]. Furthermore, modified scanning protocols in the pandemic setting reduce the risk of exposure while providing critical data regarding cardiac tissue injury and remodeling in both acute and chronic settings. Cardiac magnetic resonance imaging (CMR) is the preferred imaging modality for non-invasive evaluation in acute myocarditis [14], [17].
Therefore, the use of CMR in COVID-19 related cardiac affection is highly mandated and rapidly growing owing to its ability not only to diagnose acute and chronic sequelae of myocardial inflammation, but also to provide a more detailed understanding of the pathophysiological phenomenon behind cardiac involvement, and differentiate them from other various pathological etiologies, which can be used for risk stratification and optimizing the patients care.
Moreover, myocardial inflammation can lead to tissue edema with increased water content T2 mapping is useful to rule out active inflammation with a sensitivity of 89% [18]. T1 relaxation time is sensitive to acute and chronic inflammation, resulting in T1 mapping's high negative predictive value of 92% for detecting inflammation. The revised LLC recommendation showed a more detailed quantitative aspect of CMR in COVID-19 myocardial inflammation and fibrosis than the 2009 recommendations where in respect to T1 and T2 relaxation times analysis, pooled studies have shown a higher quantitate descriptive role for T2 relaxation time mapping in the analysis of edemas. T2 has higher specificity than in T1 relaxation times mapping that also is increased in chronic tissue changes like [19], [20]
3.4. Management of cardiac complications:
There has not been a single study that has proven a single distinct treatment that treats post-COVID-19 associated heart damage. Rehabilitation may not be appropriate for survivors of catastrophic COVID-19 who have a substantial pulmonary or cardiac impairment, according to systematic and comprehensive reviews. When addressing those patients for rehabilitation, special caution should be used. patients with a resting heart rate (>100 beats/min), Blood pressure (<90/60or > 140/90 mmHg), SaO2 (<95%) should be excluded [21]. Nonetheless, no studies or proposals for specific pharmacological treatments that target PACS-related heart damage have been published.
3.5. Vascular Complications:
SARS-CoV-2 infection, especially in its severe form, is associated with an increased risk for venous thromboembolism (VTE) [16]. The long-term risk of VTE, based on current knowledge, is less well defined. A retrospective observational cohort study of 163 patients, of whom 42 (26%) required ICU admission, had a 30-day post-discharge cumulative incidence of VTE of 0.6% (95% CI, 0.2%–4.6%) [12]. The cumulative incidence of all thrombosis (including pulmonary embolism, left ventricular thrombus, central retinal artery occlusion, thrombosis of arterio-venous dialysis fistula, and ischemic stroke) was 2.5% (95% CI, 0.8%–7.6%). The 30-day cumulative rates of major bleeding and clinically relevant nonmajor bleeding (using the International Society of Thrombosis and Hemostasis definitions for these conditions) were 0.7% and 2.9%, respectively.
On the other hand, These rates are comparable to the post-discharge hospital-acquired VTE (HA-VTE) and bleeding rates, 0.3%–2.5% and 0.7%–2.0%, respectively, that have been observed in patients with comparable forms of non-COVID-19 acute medical illness [12], [18], [19]. However, Engelen et al. report a low rate of VTE (<1%) at a mean of 44 days after hospitalization due to COVID-19 [20], these findings were consistent with a large review of HA-VTE in patients with COVID-19 discharged from King's College Hospital in the United Kingdom [21]. HA-VTE in this study was defined as VTE diagnosed in the hospital at least 48 h after admission, or postoperatively, and occurring up to 90 days post-discharge.
A total of 1877 patients discharged after hospitalization for COVID-19 were included in the analysis, including 84 HA-VTE episodes that occurred during the study period. Overall, 9/84 (11%) occurred after discharge, at a median of 8 days. Therefore, the authors calculated the frequency of discharged patients who developed HA-VTE to be 4.8 per 1000 discharges. By comparison, the rate was found to be 3.1 per 1000 discharges in 2019, which occurred within 42 days of discharge. The odds ratio of HA-VTE associated with COVID-19 compared with rates observed in 2019 before COVID-19 was 1.6 (95% CI, 0.8–3.1) and was not statistically significant [36].
The exact causes of VTE in COVID-19 patients are disputed and uncertain; nevertheless, higher VTE events are found in critically sick ICU patients regardless of diagnosis, as clearly characterized by the traditional Virchow's triad from inevitable stasis and endothelial damage [33]. However, in COVID patients, several mechanisms have been postulated: immobilization, diffuse intravascular coagulation (DIC), lung vessel inflammation (endothelitis), and angiogenesis, as well as COVID-19- associated coagulopathy. COVID-19-associated coagulopathy is due to the associated prothrombotic profile that makes it different from other RNA viruses where bleeding is usually seen [33], [34]. Furthermore, localized clot formation rather than diffuse thrombi is also a unique feature in COVID-19 and is seen primarily in the lung vessels. The mechanism behind that prothrombotic profile is mostly theorized based on etiology cytokine storm from excessive inflammation-causing endothelial injury and platelet activation.
Tang et al. were the first to shed light on the aberrant coagulopathy associated with COVID-19 infection in February 2020, with a total death rate of 11.5 percent among 183 patients, besides COVID-19 patients met the disseminated intravascular coagulation criteria by 71.4% compared to only 0.6% of survivors [37]. Guan et al. -observed 1099 COVID-19 patients from Wuhan, China- found increased d-dimer levels and decreased platelet count among seriously sick patients compared to non-severe diseased patients (137,500/mm3 vs 172,000/mm3, respectively) [38]. Moreover, Acanfora et al. further discussed the cross-talk between coagulation and inflammation which is facilitated by protease-activated receptors (PARs). COVID-19 targets these receptors, which are effectively able to activate local and circulating coagulation factors, thus inducing the generation of disseminated coagulopathies [39]. However, vaccinations were found to have no statistically significant higher risk of developing venous thrombosis, pulmonary embolism, or stroke [40].
3.6. Management of vascular complications:
Unfractionated heparin (UFH) is the first-line treatment for hemodynamic instability and emergency reperfusion when the parenteral route is preferred, excessive obesity, or significantly decreased renal function (creatinine clearance 30 mL/min). However, Patients with PE who are hemodynamically stable, valvular disease-free, or do not have AF can begin novel oral anticoagulation (NOAC) treatment with one of the novel oral anticoagulants, which are recommended over vitamin K antagonists.
COVID-19, on the other hand, predisposes to a prothrombotic condition, unlike other RNA viruses which cause bleeding problems. As a result, with no demonstrated efficacy for vitamin K antagonists and little literature support, most hospitalized patients should begin with parental anticoagulation treatment, using LMWH or IV UFH if hemodynamic instability is evident. Patients in the recovery phase are better treated with one of the NOAC, while patients in the acute phase are better treated with NOAC, and regular renal function tests should be performed, considering the potential interactions with experimental therapy for COVID-19.
3.7. Future research:
Further studies are needed to offer current screening for the occurrence of cardiovascular problems especially myocardial infarction and heart failure in patients with PASC cardiovascular problems and to investigate the possible mechanisms behind such occurrence. Furthermore, we need studies that not only propose management methods to directly target COVID and COVID-related myocardial damage but also investigate the prognostic factors and hazards in COVID-19 patients who are at risk of CVS problems, as well as the identification of groups at risk for closer monitoring throughout the illness course and frequent CVS screening recommendations for crucial prevention of the PACS CVS diseases.
4. Conclusion:
Cardiovascular complications are a common manifestation of PACS. Classification of severity of cardiac symptoms and the emergence of CMR as a diagnostic tool needs more evidence. Although PACS is managed symptomatically, more studies are to be conducted to halt the progression of the disease, and the efficacy of cardiac rehabilitation needs to be studied more. In addition, the risk factors for Covid related hypercoagulability and the difference in onset of HA-VTE and Covid VTE, and the efficacy of vitamin K antagonists as a treatment modality needs more attention.
Funding
None.
Declaration of Competing Interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
References
- 1.Shi S., Qin M.u., Shen B.o., Cai Y., Liu T., Yang F., Gong W., Liu X.u., Liang J., Zhao Q., Huang H.e., Yang B.o., Huang C. Association of Cardiac Injury with Mortality in Hospitalized Patients With COVID-19 in Wuhan. China. JAMA Cardiol. 2020;5(7):802. doi: 10.1001/jamacardio.2020.0950. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 2.Shaobo S., Qin M., Cai Y., Liu T., Shen B., Yang F., Cao S. Characteristics and clinical significance of myocardial injury in patients with severe coronavirus disease 2019. Eur. Heart J. 2020;41:2070–2079. doi: 10.1093/eurheartj/ehaa408. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Shah, W.; Hillman, T.; Playford, E.D.; Hishmeh, L. Managing the long term effects of COVID-19: Summary of NICE, SIGN, and RCGP rapid guideline. BMJ2021,372, n136. [DOI] [PubMed]
- 4.Hendren N.S., Drazner M.H., Bozkurt B., Cooper L.T. Description and Proposed Management of the Acute COVID-19 Cardiovascular Syndrome. Circulation. 2020;141(23):1903–1914. doi: 10.1161/CIRCULATIONAHA.120.047349. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5.Wang D., Hu B.o., Hu C., Zhu F., Liu X., Zhang J., Wang B., Xiang H., Cheng Z., Xiong Y., Zhao Y., Li Y., Wang X., Peng Z. Clinical characteristics of 138 hospitalized patients with 2019 novel coronavirus–infected pneumonia in Wuhan. China. JAMA. 2020;323(11):1061. doi: 10.1001/jama.2020.1585. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6.Puntmann V.O., Carerj M.L., Wieters I., Fahim M., Arendt C., Hoffmann J., Shchendrygina A., Escher F., Vasa-Nicotera M., Zeiher A.M., Vehreschild M., Nagel E. Outcomes of Cardiovascular Magnetic Resonance Imaging in Patients Recently Recovered From Coronavirus Disease 2019 (COVID-19) JAMA Cardiol. 2020 Nov 1;5(11):1265–1273. doi: 10.1001/jamacardio.2020.3557. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7.Yang X., Yu Y., Xu J., Shu H., Xia J., Liu H., Wu Y., Zhang L.u., Yu Z., Fang M., Yu T., Wang Y., Pan S., Zou X., Yuan S., Shang Y. Clinical course and outcomes of critically ill patients with SARS-CoV-2 pneumonia in Wuhan, China: A single-centered, retrospective, observational study. Lancet Respir. Med. 2020;8(5):475–481. doi: 10.1016/S2213-2600(20)30079-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 8.Weckbach L.T., Curta A., Bieber S., Kraechan A., Brado J., Hellmuth J.C., Muenchhoff M., Scherer C., Schroeder I., Irlbeck M., Maurus S., Ricke J., Klingel K., Kääb S., Orban M., Massberg S., Hausleiter J., Grabmaier U. Myocardial Inflammation and Dysfunction in COVID-19-Associated Myocardial Injury. Cardiovasc. Imaging. 2021;14(1) doi: 10.1161/CIRCIMAGING.120.011713. [DOI] [PubMed] [Google Scholar]
- 9.Nannoni S., de Groot R., Bell S., Markus H.S. Stroke in COVID-19: a systematic review and meta-analysis. Int J Stroke. 2021;16(2):137–149. doi: 10.1177/1747493020972922. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 10.Mitrani R.D., Dabas N., Goldberger J.J. COVID-19 cardiac injury: implications for long-term surveillance and outcomes in survivors. Heart Rhythm. 2020;17(11):1984–1990. doi: 10.1016/j.hrthm.2020.06.026. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 11.Carvalho-Schneider C., Laurent E., Lemaignen A., Beaufils E., Bourbao-Tournois C., Laribi S., Flament T., Ferreira-Maldent N., Bruyère F., Stefic K., Gaudy-Graffin C., Grammatico-Guillon L., Bernard L. Follow-up of adults with noncritical COVID-19 two months after symptom onset. Clinical Microbiology and Infection. 2021;27(2):258–263. doi: 10.1016/j.cmi.2020.09.052. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 12.Ni W., Yang X., Yang D., Bao J., Li R., Xiao Y., Hou C., Wang H., Liu J., Yang D., Xu Y.u., Cao Z., Gao Z. Role of angiotensin-converting enzyme 2 (ACE2) in COVID-19. Crit Care. 2020;24(1) doi: 10.1186/s13054-020-03120-0. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Ponikowski P., Voors A.A., Anker S.D., Bueno H., Cleland J.G.F., Coats A.J.S., Falk V., González-Juanatey J.R., Harjola V.-P., Jankowska E.A., Jessup M., Linde C., Nihoyannopoulos P., Parissis J.T., Pieske B., Riley J.P., Rosano G.M.C., Ruilope L.M., Ruschitzka F., Rutten F.H., van der Meer P. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure: The Task Force for the diagnosis and treatment of acute and chronic heart failure of the European Society of Cardiology (ESC) Eur. Heart J. 2016;37(27):2129–2200. doi: 10.1093/eurheartj/ehw128. [DOI] [PubMed] [Google Scholar]
- 14.Gheblawi M., Wang K., Viveiros A., Nguyen Q., Zhong J.-C., Turner A.J., Raizada M.K., Grant M.B., Oudit G.Y. Angiotensin-Converting Enzyme 2: SARS-CoV-2 Receptor and Regulator of the Renin-Angiotensin System: Celebrating the 20th Anniversary of the Discovery of ACE2. Circ Res. 2020;126(10):1456–1474. doi: 10.1161/CIRCRESAHA.120.317015. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 15.Verma K, Pant M, Paliwal S, Dwivedi J, Sharma S. An Insight on Multicentric Signaling of Angiotensin II in Cardiovascular system: A Recent Update. Front Pharmacol. 2021;12:734917. Published 2021 Aug 20. doi:10.3389/fphar.2021.734917. [DOI] [PMC free article] [PubMed]
- 16.Chen D., Li X., Song Q., Hu C., Su F., Dai J., Ye Y., Huang J., Zhang X. Assessment of hypokalemia and clinical characteristics in patients with coronavirus disease 2019 in Wenzhou. China. JAMA Network Open. 2020;3(6):e2011122. doi: 10.1001/jamanetworkopen.2020.11122. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 17.Lindner D., Fitzek A., Bräuninger H., Aleshcheva G., Edler C., Meissner K., Scherschel K., Kirchhof P., Escher F., Schultheiss H.-P., Blankenberg S., Püschel K., Westermann D. Association of Cardiac Infection With SARS-CoV-2 in Confirmed COVID-19 Autopsy Cases. JAMA Cardiol. 2020;5(11):1281. doi: 10.1001/jamacardio.2020.3551. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Ragab D, Salah Eldin H, Taeimah M, Khattab R, Salem R. The COVID-19 Cytokine Storm; What We Know So Far. Front Immunol. 2020;11:1446. Published 2020 Jun 16. doi:10.3389/fimmu.2020.01446. [DOI] [PMC free article] [PubMed]
- 19.Sanghvi S.K., Schwarzman L.S., Nazir N.T. Cardiac MRI and Myocardial Injury in COVID-19: Diagnosis, Risk Stratification and Prognosis. Diagnostics. 2021 Jan 15;11(1):130. doi: 10.3390/diagnostics11010130. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 20.Yong S.J. Long COVID or post-COVID-19 syndrome: putative pathophysiology, risk factors, and treatments. Infectious Diseases. 2021;53(10):737–754. doi: 10.1080/23744235.2021.1924397. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 21.Carfì A., Bernabei R., Landi F. Gemelli Against COVID-19Post-Acute Care Study Group. Persistent symptoms inpatients after acute COVID-19. JAMA. 2020;324(6):603. doi: 10.1001/jama.2020.12603. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 22.Dennis A., Wamil M., Alberts J., et al. Multiorgan impairment in low-risk individuals with post-COVID-19 syn-drome: a prospective, community-based study. BMJ Open. 2021;11(3) doi: 10.1136/bmjopen-2020-048391. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 23.Huang C., Huang L., Wang Y., Li X., Ren L., Gu X., Kang L., Guo L.i., Liu M., Zhou X., Luo J., Huang Z., Tu S., Zhao Y., Chen L.i., Xu D., Li Y., Li C., Peng L.u., Li Y., Xie W., Cui D., Shang L., Fan G., Xu J., Wang G., Wang Y., Zhong J., Wang C., Wang J., Zhang D., Cao B. 6-month consequences of COVID-19 in patients discharged from hospital: a cohort study. The Lancet. 2021;397(10270):220–232. doi: 10.1016/S0140-6736(20)32656-8. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 24.Liang L., Yang B., Jiang N., Fu W., He X., Zhou Y., Ma W.-L., Wang X. Three-month Follow-up Study of Survivors of Coronavirus Disease 2019 after Discharge. J. Korean Med. Sci. 2020;35(47) doi: 10.3346/jkms.2020.35.e418. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 25.Hoffmann M., Kleine-Weber H., Schroeder S., Krüger N., Herrler T., Erichsen S., Schiergens T.S., Herrler G., Wu N.-H., Nitsche A., Müller M.A., Drosten C., Pöhlmann S. SARS-CoV-2 cell entry depends on ACE2 and TMPRSS2 and is blocked by a clinically proven protease inhibitor. Cell. 2020;181(2):271–280.e8. doi: 10.1016/j.cell.2020.02.052. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26.Li X., Yu S. Cardiac valves: Another “Disaster-hit area” of COVID-19 patients? Heart Lung. 2020;49(6):890–891. doi: 10.1016/j.hrtlng.2020.05.004. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Sattar Y., Ullah W., Rauf H., Virk H.u.H., Yadav S., Chowdhury M., Connerney M., Mamtani S., Pahuja M., Patel R.D., Mir T., Almas T., Moussa Pacha H., Chadi Alraies M. COVID-19 cardiovascular epidemiology, cellular pathogenesis, clinical manifestations and management. IJC Heart & Vasculature. 2020;29:100589. doi: 10.1016/j.ijcha.2020.100589. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 28.Ackermann M., Verleden S., Kueknel M., et al. Pulmonary vascular endothlialitis, thombosis, and angiogenesis in Coivd-19. NEJM. 2020;383:120–128. doi: 10.1056/NEJMoa2015432. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 29.Sarfraz Z, Sarfraz A, Barrios A, Garimella R, Dominari A, Kc M, Pandav K, Pantoja JC, Retnakumar V, Cherrez-Ojeda I. Cardio-Pulmonary Sequelae in Recovered COVID-19 Patients: Considerations for Primary Care. J Prim Care Community Health. 2021 Jan-Dec;12:21501327211023726. doi: 10.1177/21501327211023726. PMID: 34096390; PMCID: PMC8188976. [DOI] [PMC free article] [PubMed]
- 30.Błyszczuk P. Myocarditis in humans and in experimental animal models. Front Cardiovasc. Med. 2019;6:64. doi: 10.3389/fcvm.2019.00064. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 31.Coromilas E.J., Kochav S., Goldenthal I., Biviano A., Garan H., Goldbarg S., Kim J.-H., Yeo I., Tracy C., Ayanian S., Akar J., Singh A., Jain S., Zimerman L., Pimentel M., Osswald S., Twerenbold R., Schaerli N., Crotti L., Fabbri D., Parati G., Li Y.i., Atienza F., Zatarain E., Tse G., Leung K.S.K., Guevara-Valdivia M.E., Rivera-Santiago C.A., Soejima K., De Filippo P., Ferrari P., Malanchini G., Kanagaratnam P., Khawaja S., Mikhail G.W., Scanavacca M., Abrahão Hajjar L., Rizerio B., Sacilotto L., Mollazadeh R., Eslami M., Laleh far V., Mattioli A.V., Boriani G., Migliore F., Cipriani A., Donato F., Compagnucci P., Casella M., Dello Russo A., Coromilas J., Aboyme A., O’Brien C.G., Rodriguez F., Wang P.J., Naniwadekar A., Moey M., Kow C.S., Cheah W.K., Auricchio A., Conte G., Hwang J., Han S., Lazzerini P.E., Franchi F., Santoro A., Capecchi P.L., Joglar J.A., Rosenblatt A.G., Zardini M., Bricoli S., Bonura R., Echarte-Morales J., Benito-González T., Minguito-Carazo C., Fernández-Vázquez F., Wan E.Y. Worldwide Survey of COVID-19-Associated Arrhythmias. Circ. Arrhythm. Electrophysiol. 2021;14(3) doi: 10.1161/CIRCEP.120.009458. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32.Tavazzi G., Pellegrini C., Maurelli M., Belliato M., Sciutti F., Bottazzi A., Sepe P.A., Resasco T., Camporotondo R., Bruno R., Baldanti F., Paolucci S., Pelenghi S., Iotti G.A., Mojoli F., Arbustini E. Myocardial localization of coronavirus in COVID-19 cardiogenic shock. Eur. J. Heart Fail. 2020;22(5):911–915. doi: 10.1002/ejhf.1828. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 33.Varga Z., Flammer A.J., Steiger P., Haberecker M., Andermatt R., Zinkernagel A.S., Mehra M.R., Schuepbach R.A., Ruschitzka F., Moch H. Endothelial cell infection and endotheliitis in COVID-19. Lancet. 2020;395(10234):1417–1418. doi: 10.1016/S0140-6736(20)30937-5. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 34.Bose R.J.C., McCarthy J.R. Direct SARS-CoV-2 infection of the heart potentiates the cardiovascular sequelae of COVID-19. Drug. Discov. Today. 2020;25(9):1559–1560. doi: 10.1016/j.drudis.2020.06.021. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 35.Fazlollahi A, Zahmatyar M, Noori M, et al. Cardiac complications following mRNA COVID-19 vaccines: A systematic review of case reports and case series [published online ahead of print, 2021 Dec 17]. Rev Med Virol. 2021;e2318. doi:10.1002/rmv.2318. [DOI] [PubMed]
- 36.Go A.S., Reynolds K., Tabada G.H., Prasad P.A., Sung S.H., Garcia E., Portugal C., Fan D., Pai A.P., Fang M.C. COVID-19 and Risk of VTE in Ethnically Diverse Populations. Chest. 2021;160(4):1459–1470. doi: 10.1016/j.chest.2021.07.025. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Tang N., Li D., Wang X., Sun Z. Abnormal coagulation parameters are associated with poor prognosis in patients with novel coronavirus pneumonia. J. Thromb. Haemost. 2020;18(4):844–847. doi: 10.1111/jth.14768. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 38.Guan W.-J., Ni Z.-y., Hu Y.u., Liang W.-H., Ou C.-Q., He J.-X., Liu L., Shan H., Lei C.-L., Hui D.S.C., Du B., Li L.-J., Zeng G., Yuen K.-Y., Chen R.-C., Tang C.-l., Wang T., Chen P.-Y., Xiang J., Li S.-Y., Wang J.-L., Liang Z.-J., Peng Y.-X., Wei L.i., Liu Y., Hu Y.-H., Peng P., Wang J.-M., Liu J.-Y., Chen Z., Li G., Zheng Z.-J., Qiu S.-Q., Luo J., Ye C.-J., Zhu S.-Y., Zhong N.-S. Clinical characteristics of Coronavirus disease 2019 in China. N. Engl. J. Med. 2020;382(18):1708–1720. doi: 10.1056/NEJMoa2002032. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 39.Acanfora D, Acanfora C, Ciccone MM, et al. The Cross-Talk between Thrombosis and Inflammatory Storm in Acute and Long-COVID-19: Therapeutic Targets and Clinical Cases. Viruses. 2021;13(10):1904. Published 2021 Sep 23. doi:10.3390/v13101904. [DOI] [PMC free article] [PubMed]
- 40.Jabagi M.J., Botton J., Bertrand M., Weill A., Farrington P., Zureik M., Dray-Spira R. Myocardial Infarction, Stroke, and Pulmonary Embolism After BNT162b2 mRNA COVID-19 Vaccine in People Aged 75 Years or Older. JAMA. 2022;327(1):80. doi: 10.1001/jama.2021.21699. [DOI] [PMC free article] [PubMed] [Google Scholar]