Abstract
Background
There is a dearth of studies on intermittent fasting in Saudi Arabia outside of Ramadan. The aim of this research was to study and describe the practice of intermittent fasting outside of Ramadan among Saudi people.
Methods
A web-based survey that focused on intermittent fasting practices—specifically the use of intermittent fasting applications, goal setting, and the effects of fasting on an individual’s state of health—was administered, collected, and analyzed.
Results
The study revealed that 58% (298/514) of the respondents practiced intermittent fasting for a duration of less than 3 months. The most-practiced pattern of intermittent fasting was a 16/8 fasting pattern (43.8%, 225/514). About 88.3% (454/514) of those who followed intermittent fasting drank fluids while fasting. Additionally, the amount of weight loss after intermittent fasting was less than 2.2 kg for 35% (180/514) of the participants. The primary goal of intermittent fasting for 44.9% (231/514) of the respondents was to lose weight. The majority of the participants (84.6%, 435/514) did not use any fasting applications.
Conclusion
The results of the current research on intermittent fasting outside of Ramadan are preliminary and inconclusive. The findings of the present study advance the idea that for some Saudis, the practice of intermittent fasting does not necessarily begin and end with Ramadan; this finding may present a strategic opportunity for Saudi health professionals who are focused on the obesity epidemic and other public health issues in Saudi Arabia. This study sought to help start a discussion on this topic and fill the knowledge gap.
Supplementary Information
The online version contains supplementary material available at 10.1186/s12889-022-12908-4.
Keywords: Intermittent fasting; Saudis; Ramadan; Cross-sectional, Saudi Arabia; Fasting
Background
Fasting practices have been part of human life for religious, cultural, or health reasons for thousands of years. For Muslims, the culturally intrinsic practice of fasting has been around for centuries. The Muslim community worldwide, including Muslims in Saudi Arabia, fasts for an entire lunar month during Ramadan.
Islamic fasting studies based in Muslim countries have particularly focused on intermittent fasting during Ramadan [1–6]. Although the research [7–12] has included an analysis of practices and outcomes, these studies were also limited to a focus on intermittent fasting during Ramadan.
Furthermore, the majority of the research on intermittent fasting based in Muslim countries has been limited to the study of the physiological effects of fasting during Ramadan, for example, the effect of fasting during Ramadan on diabetes treatment [10, 13, 14], cardiovascular disease [1, 15, 16], body weight [17–19], athletic performance [20–22] and sleep [23].
A review of the current international literature reveals very limited descriptive research focused on intermittent fasting practices. As Cuccolo notes [24], there is a wealth of literature focused very specifically on whether and how intermittent fasting produces clinical changes in different contexts and with different biomarkers. For instance, in terms of lipid profiles, intermittent fasting was shown to be effective in improving total cholesterol, low-density lipoprotein cholesterol, and triacylglycerol concentrations [25, 26]. Intermittent fasting was associated with greater weight loss in patients with diabetes compared with a regular diet [27]. In terms of body composition, intermittent fasting was positively correlated with short-term weight loss [28–30]. Despite the abundance of specifically targeted studies concentrated on the apparent and ranging physiological advantages of intermittent fasting, there is limited research that is more broadly directed at intermittent fasting practices, and the implementation, motivation, and perceptions of these practices. Moreover, because these and other studies have confirmed the multiple and varying benefits of intermittent fasting for human health, this body of research is pertinent to the current study and relevant for the continuation and expansion of a dialog on intermittent fasting practices.
In terms of motivation and perceptions, the study by Potter and colleagues [31] compared individuals who implemented intermittent fasting in the past and individuals who were currently practicing intermittent fasting, revealing that a person’s beliefs about a traditional three-meals-a-day lifestyle may play a key role in adherence to dietary practices.
Given the limited literature, little is still known about how people in general and the Saudi community, in particular, are practicing intermittent fasting. Therefore, to fill the research gap and augment the limited body of descriptive research on intermittent fasting, the aim of this research was to study and describe the practice of intermittent fasting outside of Ramadan among Saudi people.
Methods
Study design andsample
This cross-sectional web-based survey was conducted with Saudi adults who used social networks. The questionnaire link was publicized through social media (Twitter, WhatsApp, and Telegram), and responses were collected over 1 month. When participants accessed the web-based survey, they were greeted with the name and purpose of the study, as well as a statement about the anonymity and confidentiality of the information collected. Next, the screening criteria (18 years old or older, practicing intermittent fasting outside of Ramadan, etc.) were presented. If a participant met the criteria, s/he was directed to a statement of informed consent that asked them to check agree/disagree. Once a participant agreed to provide informed consent, s/he was able to complete the survey.
All information—from the study name to the final question—was presented textually. The participants reported no issues with survey access, understanding the language within the study, or the informed consent statement.
The inclusion and exclusion criteria of the study and the responses given by the participants are shown in Table 1.
Table 1.
The inclusion and exclusion criteria of the study and the responses given by the participants
| Inclusion/Exclusion | Category | Criteria |
|---|---|---|
| Inclusion | Survey period | 11 March 2021–8 April 2021 |
| Nationality | Saudi | |
| Sex | Male or female | |
| Age | At least 18 years old | |
| Region of research | Saudi Arabia, but Saudis living abroad could also participate | |
| Methodology | Web-based questionnaire | |
| Topic of research | Intermittent fasting practices among Saudis | |
| Exclusion | Age | Younger than 18 years |
| Responses | Responses that were illogical or incomplete | |
| Intermittent fasting | Participants that did not practice intermittent fasting |
A sample size of 385 was generated via the Raosoft sample size calculator [32] with a 95% confidence level, 5% margin error and response rate of 50%, which was comparable to another Saudi-based study [33], to represent Saudi Arabia’s current population of 12.6 million adults aged ≥ 18 years old [34].
Questionnaire development
Given the scarcity of descriptive studies on intermittent fasting practices, as noted by Cuccolo and colleagues [24], a questionnaire was developed with the aim of addressing this gap and to better understand intermittent fasting practices. The questionnaire was created after reviewing the existing literature. An examination of multiple sources yielded a pool of questions deemed relevant to the study goals [31, 35].
Regarding content validity, the questionnaire was sent to five health and academic professionals who had collectively published numerous studies that included survey-based research. Based on their recommendations, the survey was rewritten for clarity, relevance, and consistency. For the evaluation of face validity, before conducting the study, the questionnaire was tested with a sample of Saudi adults (n = 10) and was revised based on their feedback. Finally, during the piloting process of the questionnaire, Cronbach’s alpha was used to determine internal consistency reliability. A good value of 0.80 was obtained. The final web-based questionnaire was published on Google Forms with the idea that answers to the questions and respondent feedback could be given in real time.
The questionnaire consisted of 22 close-ended questions (Additional file 1) that encompassed the following determinants and was developed in compliance with the Checklist for Reporting Results of Internet E-Surveys (CHERRIES) guidelines [10, 36] and the Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines [37]:
Demographic characteristics (age, sex, residency, education, employment status, weight, height and medical diagnoses)
Intermittent fasting practices (patterns of intermittent fasting, type of food)
The effect of fasting on a person’s state of health (post-fasting portion sizes, weight loss, hunger, health status, physical symptoms)
Fasting goals (cause and duration of the practice, plans, sources of knowledge about intermittent fasting, resources on intermittent fasting)
Use of technology in fasting (name of the app if applicable)
Data analysis
Data were analyzed using the Statistical Package of Social Sciences (SPSS) system (Version 22.0). Descriptive statistics (frequency, percentages, and cross-tabulation), the chi-square test, and linear regression were applied. The P value significance was set at P < 0.05 and 95% confidence intervals (CIs) were reported.
Results
Socioeconomic characteristics and health status
The survey was completed by 575 respondents according to the inclusion and exclusion criteria (shown in Table 1). Sixty-one respondents reported information (age, height, etc.) that excluded them from the study. Even after identifying as Saudi, over 18 years of age, and practicing intermittent fasting outside of Ramadan, participants were asked in two later survey checkpoint questions if they 1) practiced intermittent fasting outside of Ramadan and 2) to report their specific age and height for the calculation of body mass index (BMI); 47 respondents reported that they did not practice intermittent fasting outside of Ramadan, which excluded them from the study, and ten respondents entered values for height or age that excluded them from the study. Ultimately, 514 respondents were selected for analysis, of which 11.9% (61/514) were male and 88.1% (453/514) were female. The majority of the respondents were aged between 18 and 31 years (56.2%, 289/514) and were residents of the central region of Saudi Arabia, including Riyadh (37.7%, 194/514). It was interesting to observe that 67.3% (346/514) of the respondents considered themselves to be in good or excellent health, and nearly the same percentage of respondents either reported themselves as being overweight or suffering from moderate or severe obesity, or were calculated as such based on their reported height and weight. These results are in agreement with findings from the Saudi National Survey, which showed that risk factors such as obesity were not associated with Saudis’ self-rated health [38].
The most prevalent medical conditions that the respondents reported were obesity (7.6%, 39/514), high blood cholesterol and triglyceride levels (5.3%, 27/514), and hypothyroidism (2.3%, 12/514). A total of 30.5% (157/154) of the respondents had a BMI in the normal range, and 67.3% (346/514) had a BMI in the overweight or moderate or severe obesity range (as shown in Table 2).
Table 2.
Sociodemographic characteristics of the study subjects by sex
| Variables | Sex | Total | P Value | |
|---|---|---|---|---|
| Female | Male | |||
| Age, years (mean ± SD) | 31.43 ± 8.89 | 35.23 ± 10.59 | 31.88 ± 9.18 | 0.002* |
| Age group (years) | ||||
| 18–31 | 264 (51.4%) | 25 (4.9%) | 289 (56.2%) | 0.013* |
| 32–45 | 154 (30.0%) | 26 (5.1%) | 180 (35.0%) | |
| 46 and older | 35 (6.8%) | 10 (1.9%) | 45 (8.8%) | |
| Region of the Country | ||||
| Central | 173 (33.7%) | 21 (4.1%) | 194 (37.7%) | 0.134* |
| Southern | 47 (9.1%) | 7 (1.4%) | 54 (10.5%) | |
| Eastern | 132 (25.7%) | 11 (2.1%) | 143 (27.8%) | |
| Northern | 21 (4.1%) | 6 (1.2%) | 27 (5.3%) | |
| Western | 7 (13.8%) | 13 (2.5%) | 84 (16.3%) | |
| Living abroad | 9 (1.8%) | 3 (0.6%) | 12 (2.3%) | |
| Education level | ||||
| Up to high school | 85 (16.5%) | 15 (2.9%) | 100 (19.4%) | < 0.001** |
| Undergraduate | 322 (62.3%) | 40 (7.7%) | 362 (70.4%) | |
| Graduate and postgraduate | 46 (8.9) | 6 (1.2%) | 52 (10.1%) | |
| Employment | ||||
| Student | 99 (19.3%) | 9 (1.8%) | 108 (21.0%) | < 0.001** |
| Employee | 141 (27.4%) | 42 (8.2%) | 183 (35.6%) | |
| Not employed | 192 (37.4%) | 4 (0.8%) | 196 (38.1%) | |
| Retired | 21 (4.1%) | 6 (1.2%) | 27 (5.3%) | |
| BMI | ||||
| Underweight | 10 (1.9%) | 1 (0.2%) | 11 (2.1%) | 0.302* |
| Normal weight | 137 (26.7%) | 20 (3.9%) | 157 (+ 30.5%) | |
| Overweight | 184 (35.8%) | 19 (3.7%) | 203 (39.5%) | |
| Obesity | 122 (23.7) | 14 (4.1%) | 143 (27.8%) | |
| Have you ever been diagnosed with any of the following conditions by a health professional? | ||||
| None | 315 (61.3%) | 31 (6.0%) | 346 (67.3%) | 0.01* |
| Yes | 138 (26.8%) | 30 (5.9%) | 168 (32.7%) | |
| Total Count (%) | 453 (88.1%) | 61 (11.9%) | 514 (100%) | |
P < 0.05: Significant, * statistically significant, ** highly statistically significant
Intermittent fasting practices
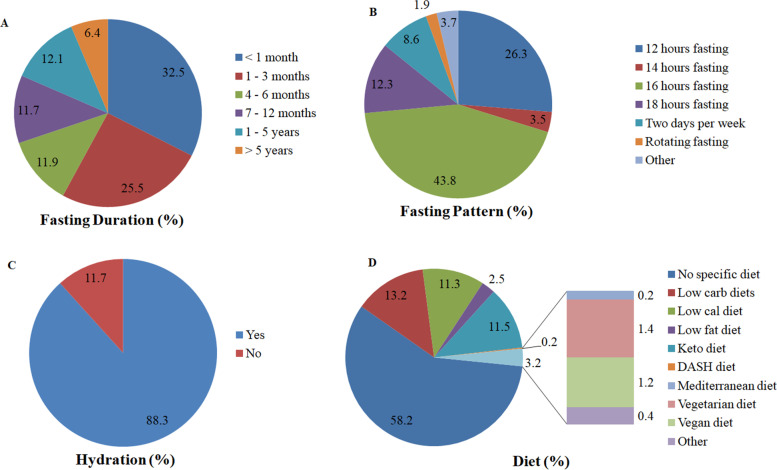
The survey focused on intermittent fasting practices with a particular focus on four factors: months/years of fasting, the fasting practice pattern, hydration during fasting (if any), and the diet plan. A duration of less than 1 month (32.5%) and a 16 h fasting pattern (43.8%, 225/514) was the most practiced approach among Saudis. Intermittent fasting for one to 3 months (25.5%) was the most prevalent duration, and a 12-h (26.3%, 135/514) fasting pattern was the second most prevalent pattern.
In terms of hydration during fasting, 88.3% (454/514) of the respondents kept themselves hydrated by drinking fluids during intermittent fasting. On the other hand, 11.7% (60/514) of the respondents did not drink any fluids for religious reasons (63.3%, 38/60), because they forgot to hydrate (11.6%, 7/60) and/or (25%, 15/60) or for other reasons such as sleep and laziness. The results related to intermittent fasting patterns, practices, and diets are shown in Fig. 1.
Fig. 1.
Fasting practices among Saudi adults. A Fasting duration, B Fasting pattern, C Hydration status and D Diet. Data are represented as an overall percentage
It was noteworthy that among the respondents, the majority of Saudi adults did not follow any specific diet plan (58.2%, 299/514). Only a small number of respondents followed a specialized diet plan, such as a low-carb diet (13.2%, 68/514), a keto diet (11.5%, 59/514), and a low calorie diet (11.3%, 58/514).
The effect of fasting on state of health
To evaluate the full impact of intermittent fasting, weight loss was studied. The physical impact of intermittent fasting on eating habits, health status, and the changes felt by the participants were also studied. Most participants (62.5%, 321/514) reported consuming less food than usual. The eating habits of 34% (175/514) of the respondents were not changed. However, 18 (3.5%) participants responded that they ate more food than usual after intermittent fasting, and 60.7% (312/514) of the participants lost less than 5 kg after intermittent fasting (as shown in Table 3).
Table 3.
Impact of fasting on the participants’ health
| Variables | Total |
|---|---|
| After intermittent fasting, is the amount of food you eat: | |
| Less than usual | 321 (62.5%) |
| Unchanged | 175 (34.0%) |
| More than usual | 18 (3.5%) |
| After intermittent fasting, did your weight change, and by how much? | |
| Less than 2.2 kg | 180 (35.0%) |
| 2.2–4.9 kg | 132 (25.7%) |
| 5–9.9 kg | 52 (10.1%) |
| 10–14.9 kg | 15 (2.9%) |
| 15–19.9 kg | 4 (0.8%) |
| More than 2.0 kg | 16 (3.1%) |
| I did not lose weight | 109 (21.2%) |
| I gained weight | 6 (1.2%) |
| After practicing intermittent fasting, my level of hunger has become | |
| Less | 383 (74.5%) |
| More | 28 (5.4%) |
| Unchanged | 103 (20.0%) |
| After intermittent fasting, my health status is: | |
| Better | 315 (61.3%) |
| Worse | 17 (3.3%) |
| Unchanged | 179 (34.8%) |
| Other - please specify | 3 (0.6%) |
| Have you experienced any of these physical symptoms during fasting? | |
| Hunger | 38 (7.4%) |
| Lethargy | 47 (9.1%) |
| Headaches | 25 (4.9%) |
| Feeling dizzy | 16 (3.1%) |
| Constipation | 14 (2.7%) |
| Sensation of being cold | 11 (2.1%) |
| I had no symptoms. | 188 (36.6%) |
| I had more than one symptom | 175 (34.0%) |
| Total Count (%) | 514 (100%) |
The majority of the participants (61.3%, 315/514) felt that their health was improved after practicing intermittent fasting, and 34.8% (179/514) did not feel they experienced any changes.
In terms of reported physical symptoms during intermittent fasting, 36.6% (188/514) of the participants did not experience any physical effects during intermittent fasting, and a small number (7.4%, 38/514) experienced hunger while practicing intermittent fasting.
Fasting goals and the use of technology
The primary goal of practicing intermittent fasting was to lose weight among 44.9% (231/514) of the respondents who reported that they wanted to lose some weight (as shown in Table 4). However, the rest of the respondents practiced intermittent fasting for multiple reasons, such as the optimization of health preservation and religious reasons. In addition, approximately 36.8% (189/514) of the participants were planning to continue practicing fasting until they reached their goals, and 21.4% (110/514) planned to continue to practice intermittent fasting for the rest of their lives. It is possible that the simplicity of the intermittent fasting regimen—as well as the complex relationship among intermittent fasting, religious practices, health, weight goals, and lifestyle—may explain why more than one-fifth of the participants planned to continue intermittent fasting throughout their lives.
Table 4.
Knowledge about fasting goals and the use of technology among the study population
| Variables | Total | |
|---|---|---|
| Why do you practice intermittent fasting? | ||
| To lose weight | 231 (44.9%) | |
| To be healthy | 56 (10.9%) | |
| Religious reasons | 36 (7.0%) | |
| Multiple reasons | 172 (33.5%) | |
| Other | 19 (3.7%) | |
| How long do you plan to continue to practice fasting? | ||
| < 1 year | 52 (10.1%) | |
| > 1 year | 26 (5.1%) | |
| Until I reach my goals | 189 (36.8%) | |
| For the rest of my life | 110 (21.4%) | |
| I do not know | 137 (26.7%) | |
| How did you learn about this practice of fasting? | ||
| From a health program on TV | 24 (4.7%) | |
| Through social networking sites | 320 (62.3%) | |
| Discussed with health professionals | 33 (6.4%) | |
| Through friends and family | 105 (20.4%) | |
| Other | 21 (4.1%) | |
| Which app do you use for fasting? | ||
| Zero | 28 (5.4%) | |
| Body Fast | 5 (1.0%) | |
| In Fasting | 2 (0.4%) | |
| LIFE Fasting Tracker | 10 (1.9%) | |
| Fastient | 2 (0.4%) | |
| Fast Habit | 4 (0.8%) | |
| I do not use any app for fasting | 435 (84.6%) | |
| Other | 28 (5.4%) | |
| If you responded no to the last question, why don’t you use an intermittent fasting phone app? | ||
| No applications in Arabic are available | 17 (3.3%) | |
| I did not know there were applications for intermittent fasting | 192 (37.4%) | |
| I do not need apps to fast | 226 (44.0%) | |
| Total Count (%) | 514 (100%) | |
The majority (62.3%, 320/514) of the respondents learned about the practice of fasting through social networking sites, while a minority (6.4%, 33/514) learned through discussion with health professionals. Almost 84.6% (435/514) of the participants did not use any smartphone application for fasting, while 37.4% (192/514) were not even aware of applications that help manage intermittent fasting. Most participants who used intermittent fasting management applications reported using the Zero app (35.4%, 28/79).
Body mass index (BMI)
BMI is a metric used by clinicians and public health organizations in predicting and determining overweight and obesity (weight status category). In addition to self-reported weight change (or stasis), BMI was used for determining any post-intermittent fasting weight changes. Linear regression was used to determine the interaction between the fasting status and pattern and hydration status with BMI among the study population (F = 8.199, p < 0.001; adjusted R-Square = 0.040; as shown in Table 5). Approximately 4.0% of the variance in the BMI scores could be explained by the fasting status and pattern and hydration status of the participants. The findings show that the overall BMI status of the respondents was significantly (P < 0.05) affected by practicing intermittent fasting for a long period of time and by hydration status (P < 0.001 and 0.005, respectively). Respondents who were not new to intermittent fasting had a significantly lower BMI (OR = 0.55) than those who had not practiced intermittent fasting. In addition, respondents who hydrated during fasting had a significantly lower BMI than those who did not hydrate during fasting (OR = 2.3).
Table 5.
The interaction between fasting status and pattern with BMI among the study population
| a | Predictors | Beta | 95% confidence intervals beta coefficient | P value | Adjusted R | F | P Value |
|---|---|---|---|---|---|---|---|
| BMI | For how long have you practiced intermittent fasting? | −0.55 | −0.870 to −0.241 | < 0.001 | 0.040 | 8.199 | < 0.001** |
| What is your intermittent fasting pattern? | 0.199 | −0.142 to 0.541 | 0.289 | ||||
| Are you hydrating during fasting? | −2.39 | −3.996 to − 0.792 | 0.005 |
a. Dependent variable (BMI), ** highly statistically significant
The duration of intermittent fasting practices
Moreover, linear regression was used to determine the effect of sociodemographic characteristics on the duration of intermittent fasting practices among the study population (F = 4.901, p < 0.001, adjusted R-squared = 0.037). Approximately 3.7% of the variance in intermittent fasting practices could be explained by the sociodemographic characteristics of the participants (Table 6). The findings show that the overall duration of the respondents’ intermittent fasting practices was significantly (P < 0.05) affected by the sex and age of the participants (P value = 0.002 and 0.008, respectively). However, women practiced longer periods of intermittent fasting than men (OR = 0.143). Furthermore, older respondents practiced longer periods of intermittent fasting than younger respondents (OR = 0.123) (Table 6).
Table 6.
The effect of sociodemographic characteristics on the duration of intermittent fasting practices among the study population
| a | Predictors | Beta | 95% confidence intervals beta coefficient | P value | Adjusted R | F | P Value |
|---|---|---|---|---|---|---|---|
|
The duration of intermittent fasting practices |
Sex | 0.143 | 0.274 to 1.158 | 0.002* | 0.037 | 4.901 | < 0.001** |
| Age | 0.123 | 0.006 to 0.038 | 0.008* | ||||
| Region | −0.071 | −0.165 to 0.016 | 0.108 | ||||
| Education level | 0.030 | −0.097 to 0.198 | 0.502 | ||||
| Employment status | 0.034 | −0.080 to 0.172 | 0.476 |
a. Dependent variable (the duration of intermittent fasting), * statistically significant, ** highly statistically significant
Discussion
The study sought to explore intermittent fasting patterns among a sample of Saudis to better understand the practice of intermittent fasting. Intermittent fasting has shown an increase in popularity as a method for weight loss and health optimization, and previous research has found promising results for its utility [39]. The current study collected data on intermittent fasting duration and habits, as well as health perceptions, and aggregated data exploring intermittent fasting trends and impacts. Unsurprisingly, although this study was not focused on sex, it should be noted that the majority of the participants were female; it is well known that males are less likely to participate in surveys [40, 41].
The results found in the present study align with the previous literature in a myriad of ways. Most participants (43.8%) reported that they followed a 16/8 fasting pattern, which is supported by a recent systematic review [30]. Welton and colleagues reported that the ideal period of a fast for positive weight change appears to be 16 h [24, 30]; our results are in accordance with these findings and indicate that the optimum intermittent fasting period is already inherent to Saudi intermittent fasting practices. Furthermore, consistent with the findings of previous research that noted that long-term intermittent fasting and hydration with noncaloric beverages contributed to a reduction in BMI and stomach circumference [39], we observed that the overall BMI status of the respondents was significantly affected (P < 0.05) by the hydration status and duration of intermittent fasting. Finally, Haines [42] found, as the current study concluded, that at least 50% of participants planned to continue the practice of intermittent fasting for some duration beyond the time of the survey.
In terms of studies focused on intermittent fasting in Arabic-speaking countries, in another study on voluntary fasting in Saudi Arabia [43], survey participants identified that the most common reasons for fasting were weight loss (47.59%; 44.9% in our study). However, another study on intermittent fasting in Saudi Arabia [35] also found that intermittent fasting was “useful and effective for weight loss.” The same study also identified a predisposition toward using intermittent fasting as a culturally familiar weight-loss tool in the Middle East and noted that intermittent fasting “was prevalent among Arabs because of their habituation toward it.” In the present study, more than half of the participants reported that they lost less than 5 kg after intermittent fasting. It is well known that a weight loss of 5% is defined as clinically meaningful weight loss that lowers the risk of many diseases [44] and can be a measure of lifestyle weight-loss program efficacy [45].
Sutton and colleagues [46] observed no significant change in self-reported hunger during a two- or four-week period of intermittent fasting. In another study [47], researchers noted a significant increase in participant hunger levels. However, our study found that after practicing intermittent fasting, the majority (75%) of the participants reported decreased hunger levels. A small number of our participants also reported other physical symptoms in response to intermittent fasting, such as headaches, dizziness, a sensation of being cold, and constipation after intermittent fasting.
Further clinical studies are warranted to assess the risks associated with long-term intermittent fasting, and factors such as protein malnutrition, vitamins, and mineral malnutrition should also be considered [48]. It has been reported that long-term intermittent fasting could adversely affect health, and due to insufficient energy intake, it may cause potential side effects such as dizziness, nausea, headaches, weakness, and excessive hunger [48]. Therefore, studies on the short- and long-term physical symptoms related to intermittent fasting have shown mixed results and justify more research and discussion.
Although most participants learned about the practice of fasting through social networking sites, surprisingly, smartphone applications did not play a significant role in intermittent fasting management for Saudis. Given that Saudi Arabia has the most social network users in the Middle East and is ranked second worldwide in terms of the percentage of social media users [49], clinicians should consider using social networking as a public awareness and community health information tool. A culturally adapted and religiously sensitive fasting application that is available in Arabic might attract more users from Arabic countries, particularly Saudi Arabia [50].
Study analyses have revealed that there is a relationship between hydration status and BMI. Our finding was in agreement with a previous national survey of 9528 adults [51] (Chang et al., 2016) that also found a strong association between poor hydration levels and a higher BMI. Another recent study among 8699 adults [52] from the National Health and Nutrition Examination Survey discovered a greater probability of hypohydration in participants with a BMI ≥30 kg/m2.
Our study revealed that the overall duration of intermittent fasting practices was significantly impacted by the sex and age of the participants. The results showed that women practiced longer periods of intermittent fasting than men. Additionally, the analyses pointed out that older respondents practiced longer periods of intermittent fasting than younger participants. In another study [53], researchers found a positive correlation between intermittent fasting and body composition in women aged 60 and older. Gupta & Singh [54], curiously, found that more men than women practiced intermittent fasting. Interestingly, contrary to our findings, they also observed that young adults practiced intermittent fasting more than middle-aged or older adults. Future research into sex, age, and intermittent fasting practices might help provide valuable insights into the sociodemographics of intermittent fasting practices and motivations.
The limitations of our study include the following. First, the use of purposive sampling was one of the study’s main limitations. Although this is a cost- and time-effective sampling strategy, its main limitation is that the results are not representative of the population and are not generalizable [55, 56]. Second, information bias, or reporting bias more specifically, may have negatively affected the accuracy of our survey, which was reliant on self-reported data. Self-reported data, such as weight loss and BMI data, might be biased and misreported. It is well documented [57] that self-reported body weight, for instance, is often underestimated. Additionally, because we could not independently verify participants’ self-reported values, self-reported bias must be considered. Third, 61 participants reported information that excluded them from the study, so this also limited the scope of the research and further limited any potential generalizability of the study. Fourth, the design of the Google Forms questionnaire did allow for the determination of a response rate. Finally, because of time and financial considerations and COVID-19 restrictions, the study relied on single-mode online data collection. As such, we could not ensure that a wider pool of potential participants was reached through a variety of survey opportunities and data collection modes. Additionally, online data collection may be a barrier for individuals with physical or internet accessibility issues, those who are not on social media or infrequent users of social media. Therefore, selection bias occurred in this study and is one of the study’s limitations. To overcome the limitations encountered in the present study and to gain a more in-depth understanding of intermittent fasting practices, future research should consider qualitative approaches, such as participant focus groups and interviews, as well as mixed-mode or multimodal data collection methods, such as mail, phone, and online survey access.
Conclusion
This research sought to assess and better understand the Saudi practices of intermittent fasting outside of Ramadan, and hoped to continue the conversation on intermittent fasting practices. We discovered that most participants practiced intermittent fasting for a duration of less than 3 months. It was observed that 16-h intermittent fasting was the most common intermittent fasting practice among Saudi individuals. Additionally, weight loss was found to be the main purpose for practicing intermittent fasting. In fact, the data showed that intermittent fasting significantly reduced weight and BMI among participants who were practicing intermittent fasting for a long period of time, with or without hydration. Furthermore, our findings indicated that the majority of the participants were satisfied with the outcomes of their fasting practices and noted a general improvement in their health. Finally, smartphone applications did not play any notable role in intermittent fasting practices among Saudi people.
Supplementary Information
Acknowledgments
This research project was supported by a grant from the “Research Center of the Female Scientific and Medical Colleges”, Deanship of Scientific Research, King Saud University.
Code availability
Not applicable.
Abbreviations
- BMI
Body Mass Index
Authors’ contributions
A.A. and M.A. conceived the presented idea. A.A. and M.A. developed the survey. M.A. carried out the survey. A.A. supervised the data collection. M.A. analyzed the data. A.A. contributed to the data analysis and data interpretation. M.A. wrote the first draft of the paper. A.A. revised and wrote the final manuscript. The authors read and approved the final manuscript.
Availability of data and materials
The data that supported the findings of this study are available from the corresponding author on request.
Declarations
Ethics approval consent to participate
The study was approved by the Institutional Review Board of King Saud University (Ref. No: KSU-HE-21-162, March 2021).
An online consent form to participate in the study was included on the survey website.
Consent for publication
Not applicable.
Competing interests
The authors declare that they have no competing interests.
Footnotes
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
References
- 1.Jahrami HA, Faris ME, I Janahi A, I Janahi M, Abdelrahim DN, Madkour MI, et al. Does four-week consecutive, dawn-to-sunset intermittent fasting during Ramadan affect cardiometabolic risk factors in healthy adults? A systematic review, meta-analysis, and meta-regression. Nutr Metab Cardiovasc Dis. 2021. 10.1016/j.numecd.2021.05.002. [DOI] [PubMed]
- 2.Abdelrahim D, Faris MAIE, Hassanein M, Shakir AZ, Yusuf AM, Almeneessier AS, et al. Impact of Ramadan Diurnal Intermittent Fasting on Hypoglycemic Events in Patients With Type 2 Diabetes: A Systematic Review of Randomized Controlled Trials and Observational Studies. Front Endocrinol (Lausanne) 2021;12:624423. doi: 10.3389/fendo.2021.624423. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 3.Faris MAIE, Alsibai J, Jahrami HA, Obaideen AA, Jahrami HA, Obaideen AA. Impact of Ramadan diurnal intermittent fasting on the metabolic syndrome components in healthy, non-athletic Muslim people aged over 15 years: A systematic review and meta-analysis. Br J Nutr. 2020;123:1–22. doi: 10.1017/S000711451900254X. [DOI] [PubMed] [Google Scholar]
- 4.Aloui A, Baklouti H, Chtourou H. Effects of Ramadan fasting on body composition in athletes: a systematic review Countermeasurement to sleep deprivation View project Effects of sleep deprivation on diurnal variations of hematological, immune and inflammatory responses during physical exercise View project. https://www.researchgate.net/publication/333149687. Accessed 30 Jun 2021.
- 5.Boukhris O, Trabelsi K, Chtourou H. Evolution of Dietary Intake Between Before, During and After Ramadan Observance in Tunisian Physically Active Men: A Systematic Review. Int J Sport Stud Heal. 2018;1. 10.5812/intjssh.83782.
- 6.Hajek P, Myers K, Dhanji AR, West O, McRobbie H. Weight change during and after Ramadan fasting. J Public Heal (United Kingdom) 2012;34:377–381. doi: 10.1093/pubmed/fdr087. [DOI] [PubMed] [Google Scholar]
- 7.Kridli SAO. Health beliefs and practices of Muslim women during Ramadan. MCN Am J Matern Nurs. 2011;36:216–221. doi: 10.1097/NMC.0B013E3182177177. [DOI] [PubMed] [Google Scholar]
- 8.Al-Balhan E, Khabbache H, Laaziz A, Watfa A, Mhamdi A, Del PG, et al. To fast or not to fast during the month of Ramadan? A comprehensive survey on religious beliefs and practices among Moroccan diabetic patients. Diabetes Metab Syndr Obes Targets Ther. 2018;11:633–640. doi: 10.2147/DMSO.S171990. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 9.Saro S, Tanawattanacharoen S. Knowledge, attitudes and practices of ramadan fasting in pregnant thai-muslim women. Thai J Obstet Gynaecol. 2018:83–95. 10.14456/TJOG.2018.11.
- 10.Beshyah SA, Badi A, El-Ghul AM, Eledrisi MS. The year in “Ramadan Fasting and Health”(2018). Ibnosina J Med. Biomed Sci. 2019;11:151. [Google Scholar]
- 11.Seiermann AU, Al-Mufti H, Waid JL, Wendt AS, Sobhan S, Gabrysch S. Women’s fasting habits and dietary diversity during Ramadan in rural Bangladesh. Matern Child Nutr. 2021;17. 10.1111/MCN.13135. [DOI] [PMC free article] [PubMed]
- 12.Moghadam MT, Taati B, Paydar Ardakani SM, Suzuki K. Ramadan Fasting During the COVID-19 Pandemic; Observance of Health, Nutrition and Exercise Criteria for Improving the Immune System. Front Nutr. 2021;7:349. doi: 10.3389/fnut.2020.570235. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13.Beshyah SA, Ali KF, Hafidh K, Hajjaji IM. Ramadan fasting and diabetes 2019: The year in review. Diabetes Res Clin Pract. 2021;172:108593. doi: 10.1016/j.diabres.2020.108593. [DOI] [PubMed] [Google Scholar]
- 14.Gad H, Al-Muhannadi H, Purra H, Mussleman P, Malik RA. The effect of Ramadan focused education on patients with type 2 diabetes: A systematic review and meta-analysis. Diabetes Res Clin Pract. 2020;162. 10.1016/J.DIABRES.2020.108122. [DOI] [PubMed]
- 15.Hammami R, Bahloul A, Charfeddine S, Gargouri R, Ellouze T, Abid L, et al. Cardiovascular disease and Ramadan. A literature review. Ann Cardiol Angeiol (Paris). 2022. 10.1016/J.ANCARD.2021.09.011. [DOI] [PubMed]
- 16.Refaat M, El Jamal N, El-Rayess H, Gebran A, Salam A. The Impact of Diurnal Fasting During Ramadan on Patients with Established Cardiac Disease: A Systematic Review. Int Cardiovasc Forum J. 2019;15. 10.17987/icfj.v15i0.549.
- 17.Correia JM, Santos I, Pezarat-Correia P, Silva AM, Mendonca GV. Effects of Ramadan and Non-ramadan Intermittent Fasting on Body Composition: A Systematic Review and Meta-Analysis. Front Nutr. 2021;7:372. doi: 10.3389/fnut.2020.625240. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 18.Jahrami HA, Alsibai J, Clark CCT, Faris MAIE. A systematic review, meta-analysis, and meta-regression of the impact of diurnal intermittent fasting during Ramadan on body weight in healthy subjects aged 16 years and above. Eur J Nutr. 2020;59:2291–2316. doi: 10.1007/S00394-020-02216-1. [DOI] [PubMed] [Google Scholar]
- 19.Fernando HA, Zibellini J, Harris RA, Seimon RV, Sainsbury A. Effect of ramadan fasting on weight and body composition in healthy non-athlete adults: a systematic review and meta-analysis. Nutrients. 2019;11. 10.3390/NU11020478. [DOI] [PMC free article] [PubMed]
- 20.Trabelsi K, Bragazzi N, Zlitni S, Khacharem A, Boukhris O, El-Abed K, et al. Observing Ramadan and sleep-wake patterns in athletes: a systematic review, meta-analysis and meta-regression. Br J Sports Med. 2020;54. 10.1136/BJSPORTS-2018-099898. [DOI] [PubMed]
- 21.Abaïdia AE, Daab W, Bouzid MA. Effects of Ramadan fasting on physical performance: a systematic review with meta-analysis. Sports Med. 2020;50:1009–1026. doi: 10.1007/S40279-020-01257-0. [DOI] [PubMed] [Google Scholar]
- 22.Trabelsi K, Shephard RJ, Boukhris O, Ammar A, Khanfir S, Hakim A, et al. Effects of Ramadan fasting on athletes’ hematological indices: a systematic review. Tunis Med. 2019;97:1104–1113. [PubMed] [Google Scholar]
- 23.Faris MAIE, Jahrami HA, Alhayki FA, Alkhawaja NA, Ali AM, Aljeeb SH, et al. Effect of diurnal fasting on sleep during Ramadan: a systematic review and meta-analysis. Sleep Breath. 2020;24:771–782. doi: 10.1007/S11325-019-01986-1. [DOI] [PubMed] [Google Scholar]
- 24.Cuccolo K, Kramer R, Petros T, Thoennes M. Intermittent fasting implementation and association with eating disorder symptomatology. Eat Disord. 2021;1–21. 10.1080/10640266.2021.1922145. [DOI] [PubMed]
- 25.Meng H, Zhu L, Kord-Varkaneh H, O Santos H, Tinsley GM, Fu P. Effects of intermittent fasting and energy-restricted diets on lipid profile: A systematic review and meta-analysis. Nutrition. 2020;77. 10.1016/j.nut.2020.110801. [DOI] [PubMed]
- 26.Ahmed N, Farooq J, Siddiqi HS, Meo SA, Kulsoom B, Laghari AH, et al. Impact of Intermittent Fasting on Lipid Profile–A Quasi-Randomized Clinical Trial. Front Nutr. 2020;7:596787. doi: 10.3389/FNUT.2020.596787. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 27.Borgundvaag E, Mak J, Kramer CK. Metabolic Impact of Intermittent Fasting in Patients With Type 2 Diabetes Mellitus: A Systematic Review and Meta-analysis of Interventional Studies. J Clin Endocrinol Metab. 2021;106:902–911. doi: 10.1210/CLINEM/DGAA926. [DOI] [PubMed] [Google Scholar]
- 28.Vitale R, Kim Y. The Effects of Intermittent Fasting on Glycemic Control and Body Composition in Adults with Obesity and Type 2 Diabetes: A Systematic Review. Metab Syndr Relat Disord. 2020;18:450–461. doi: 10.1089/MET.2020.0048. [DOI] [PubMed] [Google Scholar]
- 29.Pinto FCS, Silva AAM, Souza SL. Repercussions of intermittent fasting on the intestinal microbiota community and body composition: a systematic review. Nutr Rev. 2022. 10.1093/NUTRIT/NUAB108. [DOI] [PubMed]
- 30.Welton S, Minty R, O’Driscoll T, Willms H, Poirier D, Madden S, et al. Intermittent fasting and weight loss Systematic review. Can Fam Physician. 2020;66:117–125. [PMC free article] [PubMed] [Google Scholar]
- 31.Potter C, Griggs RL, Brunstrom JM, Rogers PJ. Breaking the fast: Meal patterns and beliefs about healthy eating style are associated with adherence to intermittent fasting diets. Appetite. 2019;133:32–39. doi: 10.1016/j.appet.2018.10.020. [DOI] [PubMed] [Google Scholar]
- 32.Sample Size Calculator by Raosoft, Inc. http://www.raosoft.com/samplesize.html. Accessed 26 Jan 2022.
- 33.Al-Rawashdeh N, Damsees R, Al-Jeraisy M, Al Qasim E, Deeb AM. Knowledge of and attitudes toward clinical trials in Saudi Arabia: a cross-sectional study. BMJ Open. 2019;9. 10.1136/BMJOPEN-2019-031305. [DOI] [PMC free article] [PubMed]
- 34.Population Estimates. The General Authority for statistics. 2020. https://www.stats.gov.sa/en/43. Accessed 3 Feb 2021.
- 35.Almoraie N, Alkarimi A, Alosaimi R. The Effects of Intermittent Fasting on Weight Loss for Overweight and Obese Men and Woman in Saudi Arabia. Int J Sci Basic Appl Res. 2019;46:150–159. [Google Scholar]
- 36.Eysenbach G. Improving the quality of web surveys: The Checklist for Reporting Results of Internet E-Surveys (CHERRIES) J Med Internet Res. 2004;6:e132. doi: 10.2196/jmir.6.3.e34. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 37.Vandenbroucke JP, von Elm E, Altman DG, Gøtzsche PC, Mulrow CD, Pocock SJ, et al. Strengthening the Reporting of Observational Studies in Epidemiology (STROBE): explanation and elaboration. Int J Surg. 2014;12:1500–1524. doi: 10.1016/J.IJSU.2014.07.014. [DOI] [PubMed] [Google Scholar]
- 38.Moradi-Lakeh M, El Bcheraoui C, Tuffaha M, Daoud F, Al Saeedi M, Basulaiman M, et al. Self-rated health among saudi adults: findings from a national survey, 2013. J Community Health. 2015;40:920–926. doi: 10.1007/s10900-015-0014-4. [DOI] [PubMed] [Google Scholar]
- 39.Wilhelmi de Toledo F, Grundler F, Sirtori CR, Ruscica M. Unravelling the health effects of fasting: a long road from obesity treatment to healthy life span increase and improved cognition. Ann Med. 2020;52:147–161. doi: 10.1080/07853890.2020.1770849. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 40.Dillman DA, Eltinge JL, Groves RM, Little RJA. Evaluating Nonresponse Error in Mail Surveys. In: Groves RM, Dillman DA, Eltinge JL & Little RJA editors. Survey Nonresponse, New York: Wiley; 2002. p. 197–211. ISBN: 978-0-471-39627-7.
- 41.Singer E, Van Hoewyk J, Maher MP. Experiments with incentives in telephone surveys. Public Opin Q. 2000;64:171–188. doi: 10.1086/317761. [DOI] [PubMed] [Google Scholar]
- 42.Haines RE. The Effect of Time-Restricted Feeding on Body Weight, Energy, The Effect of Time-Restricted Feeding on Body Weight, Energy, Mood, Sleep, and Hunger Levels of Adults on Social Media. Louisiana Tech University. 2020; https://digitalcommons.latech.edu/theses. Accessed 26 Jan 2022.
- 43.Alhussain MH, Almarri DM, Arzoo S. Study on the Effect of Intermittent Fasting on Body Mass Index, Physical Activity and Sleep in Adults. J Clin Diagnostic Res. 2021;34–7. 10.7860/JCDR/2021/49940.15067.
- 44.Williamson DA, Bray GA, Ryan DH. Is 5% weight loss a satisfactory criterion to define clinically significant weight loss? Obesity. 2015;23:2319–2320. doi: 10.1002/oby.21358. [DOI] [PubMed] [Google Scholar]
- 45.Perry KJ, Hickson M, Thomas J. Factors enabling success in weight management programmes: systematic review and phenomenological approach. J Hum Nutr Diet. 2011;24:301–302. doi: 10.1111/j.1365-277x.2011.01175_32.x. [DOI] [Google Scholar]
- 46.Sutton EF, Beyl R, Early KS, Cefalu WT, Ravussin E, Peterson CM. Early time-restricted feeding improves insulin sensitivity, blood pressure, and oxidative stress even without weight loss in men with prediabetes. Cell Metab. 2018;27:1212–1221.e3. doi: 10.1016/j.cmet.2018.04.010. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 47.Stote KS, Baer DJ, Spears K, Paul DR, Harris GK, Rumpler WV, et al. A controlled trial of reduced meal frequency without caloric restriction in healthy, normal-weight, middle-aged adults. Am J Clin Nutr. 2007;85:981–988. doi: 10.1093/AJCN/85.4.981. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 48.Grajower MM, Horne BD. Clinical management of intermittent fasting in patients with diabetes mellitus. Nutrients. 2019;11. 10.3390/nu11040873. [DOI] [PMC free article] [PubMed]
- 49.The Ministry of Communications and Information Technology. No Title 2019. https://www.mcit.gov.sa/en/. Accessed 3 Feb 2021.
- 50.Alnasser AA, Alkhalifa AS, Sathiaseelan A, Marais D. What overweight women want from a weight loss app: a qualitative study on arabic women. JMIR mHealth uHealth. 2015;3:e4409. doi: 10.2196/mhealth.4409. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 51.Chang T, Ravi N, Plegue MA, Sonneville KR, Davis MM. Inadequate Hydration, BMI, and Obesity Among US Adults: NHANES 2009–2012. Ann Fam Med. 2016;14:320–324. doi: 10.1370/AFM.1951. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 52.Ehlert AM, Wilson PB. The Associations between Body Mass Index, Estimated Lean Body Mass, and Urinary Hydration Markers at the Population Level. 2020. pp. 163–170. [Google Scholar]
- 53.Domaszewski P, Konieczny M, Pakosz P, Baczkowicz D, Sadowska-Krępa E. Effect of a Six-Week Intermittent Fasting Intervention Program on the Composition of the Human Body in Women over 60 Years of Age. Int J Environ Res Public Heal. 2020;17:4138. doi: 10.3390/IJERPH17114138. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 54.Gupta S, Singh N. Comparative study on nutritional status of intermittent fasting Vs. Non-intermittent fasting practice in adults across gender. Indian J Prev Soc Med. 2021;52:152–160. [Google Scholar]
- 55.Klar S, Leeper TJ. Identities and intersectionality: a case for purposive sampling in survey-experimental research. Exp Methods Surv Res Tech Comb Random Sampl Random Assign. 2019:419–33. 10.1002/9781119083771.CH21.
- 56.Brick JM. Explorations in Non-Probability Sampling Using the Web. Proc Stat. Canada Symp. 2014.
- 57.Gorber SC, Tremblay M, Moher D, Gorber B. A comparison of direct vs. self-report measures for assessing height, weight and body mass index: a systematic review. Obes Rev. 2007;8:307–326. doi: 10.1111/J.1467-789X.2007.00347.X. [DOI] [PubMed] [Google Scholar]
Associated Data
This section collects any data citations, data availability statements, or supplementary materials included in this article.
Supplementary Materials
Data Availability Statement
The data that supported the findings of this study are available from the corresponding author on request.