Abstract
Aim
LISA is a promising method in improving preterm outcome. The aim of this study was to assess whether the INSURE (intubation‐surfactant extubation) technique or LISA (less invasive surfactant administration) procedure for surfactant administration is associated with more pain‐relieving interventions after the intervention in preterm infants.
Methods
Preterm infants born at <32 weeks gestational age admitted to the Neonatal Intensive Care Unit of Innsbruck University hospital between Jan 2012 and June 2017 subjected to INSURE or LISA were included in the study, which was performed as a retrospective analysis of routinely collected data. Pain assessments were made bedside using the Bernese Pain Scale for Neonates.
Results
During the study period 15 preterm infants (median gestational age 30.7 weeks; range: 25.9‐32.0 weeks) were subjected to INSURE technique and 59 (median gestational age 29.4 weeks; range: 25.1‐31.4 weeks) to LISA. Infants subjected to LISA showed a higher need for nonpharmacological pain‐relieving interventions in the first three days of life.
Conclusion
LISA procedure compared to INSURE technique was associated with a higher need for pain‐relieving interventions in the first three days of life. Prospective randomized controlled trials are needed to optimize this less invasive method for surfactant application with special focus on pain in neonates.
Abbreviations
- INSURE
intubation‐surfactant‐extubation
- LISA
less invasive surfactant administration
1. INTRODUCTION
Pain is a complex and unpleasant sensory and emotional experience. Pain responses include biological, environmental and psychosocial factors. All children, even those who are considered to be healthy, undergo painful procedures after birth as part of routine care and practice. The overall principle is to reduce the number of painful interventions by routine assessments for the detection of pain. In adults self‐report is the standard for pain detection, however, in newborns, a more distinct evaluation, based on responses in different systems of the body should form the base for pain assessment. Furthermore, in neonates reliable pain assessment should take gestational age (preterm versus term) and medical status (severe illness, sleep‐wake state) into account. Until the late eighties newborns were supposed to feel no pain. 1 Since then many studies have been performed to verify the extent of neonatal pain perception, to develop measurements of pain and treatments.
During their stay in the neonatal intensive care unit, newborn infants undergo 10 to 15 painful procedures per day. 2 Preterm infants are those, who are most frequently exposed to numerous painful stimuli due to their medical condition as a result to intensive care treatment. 3 This is of importance, because immaturity affects the ability to react adequately to pain and to protect the body from further damage. Repeated pain exposure could limit pain thresholds and make the infant more succeptible to subsequent painful events. 4 Changes in sensitivity to pain persist after the neonatal period and might put neonates at risk to develop adverse events and may result in poorer brain development. 5 Neonatal pain management is based on pain prevention, routine pain assessment, minimizing the number of painful procedures performed and treatment. 6 Pain treatment includes nonpharmacological pain management and pharmacologic therapies. Pharmacological care is not always ideal for pain management, therefore procedures, especially when regarded minimally invasive, are often performed without premedication. 7
Respiratory distress syndrome, due to surfactant deficiency, has been associated with high morbidity and mortality. 8 Surfactant treatment has been a major achievement in the care of preterm infants and has been shown to substantially improve outcome. 9 With more than 5.000 reports listed on PubMed, surfactant treatment is currently the best‐investigated treatment option in neonatal intensive care. In an effort to reduce mechanical lung damage, alternative approaches to deliver surfactant have been developed. The intubation‐surfactant extubation (INSURE) technique involves surfactant administration during brief mechanical ventilation followed by immediate extubation and includes by standard analgosedative medication. The less invasive surfactant administration (LISA) technique involves administering surfactant while maintaining spontaneous breathing using a thin catheter. 10 Endotracheal intubation in preterm infants is regarded painful and has a negative impact on brain development. 11 Illness severity in the first 24 hours of life together with pain exposure contributes to a slower microstructural brain development (corticospinal tract) up to term‐equivalent age. 12 Premedication is used for all nonemergency endotracheal intubations in neonates. Despite being considered minimally invasive, LISA involves using a laryngoscope to visualize the vocal cords. Awake laryngoscopy has been associated with physiological changes such as systemic and pulmonary hypertension, bradycardia and hypoxia that might put neonates at risk to develop adverse events. Currently, there is no consensus whether or not to use analgosedative medication for LISA. 13 , 14 Our aim was to evaluate LISA and INSURE with respect to pain‐relieving interventions after the intervention in the first days of life in preterm infants.
2. METHODS
The study survey area was Tyrol, a state in western Austria with 680,000 inhabitants and about 7,000 live births per year. Infants born at Innsbruck University Hospital, the only Neonatal Intensive Care Unit in the geographical region, were included in the study. The study was performed as a retrospective analysis of routinely collected data. Data from 74 preterm infants born at ≤ 32 weeks and admitted to our Neonatal Intensive Care Unit between January 2012 to June 2017 were retrospectively analyzed. The study was approved by the Ethics Committee of the Medical University of Innsbruck (Approval No. AN213‐0086333/4.2).
Clinical characteristics of all study participants were collected during hospital stay and defined as described in detail in our previous paper. 15 Neonatal characteristics included gestational age, birth weight, Clinical Risk Index for Babies score, low‐dose prophylactic treatment of patent ductus arteriosus (paracetamol 10 mg/kg birthweight, every eight hours within the first 24 hours until echocardiography), small for gestational age, sex, antenatal steroid use, patent ductus arteriosus, necrotizing enterocolitis, diagnosis of early‐ and late‐onset sepsis, intraventricular hemorrhage, periventricular leukomalacia and retinopathy of prematurity. 16 , 17
As per clinical practice at our Neonatal Intensive Care Unit surfactant was administered in case of clinical signs of respiratory distress (tachypnoea or dyspnoea), need for supplemental oxygen or radiographic findings consistent with respiratory distress syndrome. During LISA a soft and thin catheter was inserted into the larynx via a laryngoscope while the patient was awake and spontaneously breathing on continuous positive end‐expiratory airway pressure with 5 cm water. We used either a Leadercath (Vygon, Ecouen, France) or LISAcath (Chiesi, Parma, Italy). Surfactant was administered at a dose of 200 mg/kg over 1‐2 min in small fractions adapted to the respiratory rate of the preterm infant. Infants subjected to the INSURE technique received surfactant (200 mg/kg) during brief mechanical ventilation followed by immediate extubation. The decision to administer bolus analgosedation before surfactant administration was at the discretion of the attending neonatologist.
For the assessment of pain and discomfort in neonates, we used the Bernese Pain Scale for Neonates, 18 which includes two physiological and seven subjective items, with scores of more than 11 indicating greater pain‐related distress. The score was evaluated every 6‐8 hours starting on the first day of life, or when indicated (during painful intervention or ongoing pain therapy, after surgery, disease pattern like asphyxia, necrotizing enterocolitis, hematomas or need for continuous positive airway pressure, installations or drains), during routine nursing care, which has been performed every 3‐4 hours in all infants. We analyzed the routinely assessed Bernese pain score for day 1, 2, 3 and 4. Nonpharmacological pain management included facilitated‐tucking, swaddling and non‐nutritive sucking. Pain therapy consisted of oral 33% glucose solution for mild to moderate pain and systemic analgesia with paracetamol for mild pain. We used opioid analgesics like morphine or fentanyl or S‐ketamine for strong pain as recommended. 19
2.1. Statistical methods
All statistical analyses were performed by using IBM© SPSS© Statistics, Version 24.0 for Windows (SPSS Inc, Chicago, IL, USA). For group comparisons of normally distributed continuous data Student's t tests were performed; for data not adhering to a particular distribution Mann‐Whitney U tests were applied. Categorical data were compared using the Chi‐Square test. Data are presented as absolute numbers and percentages, medians with interquartile ranges or means with standard deviations. Results were regarded as statistically significant when two‐sided P < .05.
3. RESULTS
The median gestational age of the participants was 29.6 (range 25.1‐32.1) weeks and the median birth weight was 1300 (400‐2080) grams. Of those, 59 infants received surfactant delivered via LISA and 15 infants via INSURE. Neonatal characteristics were similar for both groups, except for more paracetamol‐patent ductus arteriosus prophylaxis in the LISA group (66.1% versus 20%, P = .001) and a lower mean birth weight in the LISA group (1227.9 ± 389.6 versus 1466.7 ± 383.5, P = .037). There were no significant differences between the two groups regarding gestational age, being born small for gestational age, sex or antenatal steroid use (table 1) and CRIB score (Figure 1). There were no significant differences between groups in terms of patent ductus arteriosus, necrotizing enterocolitis, early‐onset sepsis or late‐onset sepsis, intraventricular hemorrhage, periventricular leukomalacia, retinopathy of prematurity (P > .05). Bernese pain scores between groups are shown in Figure 2.
Table 1.
Analysis of baseline characteristics
| Variable |
LISA group n = 59 |
INSURE group n = 15 |
P value |
|---|---|---|---|
| Gestational age [weeks]; median (IQR) | 29.43 (27.86;31.43) | 30.71 (28.57;31.86) | .163 a |
| Birthweight [grams]; mean (SD) | 1227.90 ± 389.58 | 1466.73 ± 383.55 | .037 b |
| Small for gestational age; n (%) | 6 (10.2) | 1 (6.7) | .679 c |
| Prophylactic treatment of patent ductus arteriosus; n (%) | 39 (66.1) | 3 (20.0) | .001 c |
| Male; n (%) | 39 (66.1) | 8 (53.3) | .359 c |
| Antenatal steroids; n (%) | 55 (94.8) | 15 (100.0) | .368 c |
| Patent ductus arteriosus; n (%) | 14 (23.7) | 4 (26.7) | .813 c |
| Necrotizing enterocolitis; n (%) | 2 (3.4) | 0 (0.0) | .470 c |
| Early‐onset sepsis; n (%) | 4 (6.8) | 0 (0.0) | .300 c |
| Late‐onset sepsis; n (%) | 3 (5.1) | 0 (0.0) | .373 c |
| Intraventricular hemorrhage; n (%) | 5 (8.5) | 0 (0.0) | .243 c |
| Intraventricular hemorrhage grade 3 or 4; n (%) | 2 (3.4) | 0 (0.0) | .470 c |
| Periventricular leukomalacia; n (%) | 1 (1.7) | 0 (0.0) | .612 c |
| Retinopathy of prematurity; n (%) | 7 (11.9) | 1 (6.7) | .563 c |
| CRIB score; median (IQR), range | 1 (0;2), 0‐9 | 1 (0;1), 0‐6 | .898 a |
CRIB indicates Clinical Risk Index for Babies; IQR, interquartile range; SD, standard deviation.
Population characteristics of preterm infants subjected to LISA (Less Invasive Surfactant Administration) procedure or INSURE (Intubation‐surfactant‐extubation) technique. In all variables, the proportion of missing data was < 5%.
Mann‐Whitney U test.
Student's t test.
Chi‐square test.
P values <0.05 were marked as bold.
Figure 1.
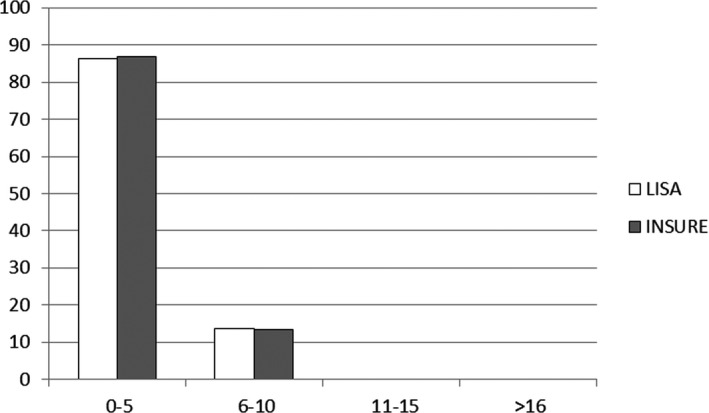
CRIB score (percentage, %) by group
Figure 2.
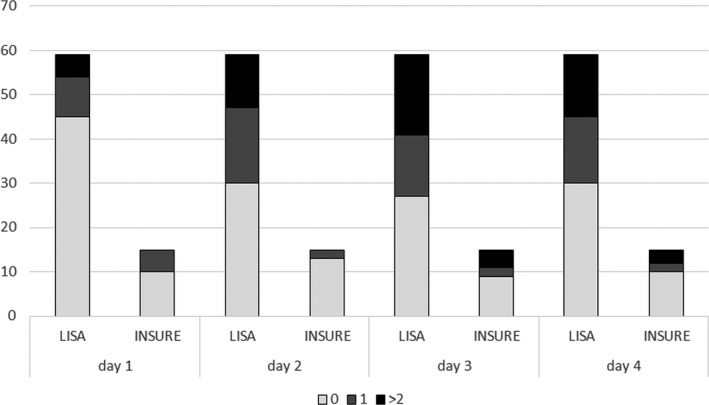
Bernese pain scale. Y‐axis shows number of infants. with a Bernese pain score of 0, 1 or more than 2 points by group
Our study revealed that preterm infants receiving surfactant via LISA procedure required nonpharmacological pain relief interventions twice as often than their peers subjected to the INSURE technique in the first three days of life. Significance was lost on day 4 of life. There was no significant difference in pharmacologic interventions after birth on day 1, 2, 3 and 4 of life (P > .05) (table 2).
Table 2.
Primary outcome between groups
|
LISA group n = 59 |
INSURE group n = 15 |
P value | |
|---|---|---|---|
| Primary outcome parameter | |||
| Day 1 | |||
| NPPRI | 6.93 ± 6.20 | 3.27 ± 2.34 | 0.025 a |
| Glucose 33% | 1.10 ± 1.17 | 1.20 ± 1.08 | 0.626 a |
| Systemic analgesics | 0.05 ± 0.29 | 0.00 ± 0.00 | 0.473 a |
| Day 2 | |||
| NPPRI | 13.63 ± 9.41 | 6.47 ± 5.60 | 0.002 a |
| Glucose 33% | 1.76 ± 1.87 | 2.33 ± 3.70 | 0.831 a |
| Systemic analgesics | 0.10 ± 0.44 | 0.00 ± 0.00 | 0.303 a |
| Day 3 | |||
| NPPRI | 13.53 ± 7.32 | 8.14 ± 5.85 | 0.009 a |
| Glucose 33% | 1.81 ± 1.63 | 1.93 ± 1.64 | 0.801 a |
| Systemic analgesics | 0.12 ± 0.42 | 0.00 ± 0.00 | 0.263 a |
| Day 4 | |||
| NPPRI | 11.07 ± 7.64 | 8.54 ± 5.25 | 0.391 a |
| Glucose 33% | 1.53 ± 1.50 | 1.62 ± 1.12 | 0.572 a |
| Systemic analgesics | 0.24 ± 0.73 | 0.00 ± 0.00 | 0.195 a |
Primary outcomes of preterm infants treated with surfactant via LISA (Less Invasive Surfactant Administration) procedure or INSURE (Intubation‐surfactant‐extubation) technique. NPPRI, nonpharmacological pain‐relieving intervention. Study group by outcome with mean number of interventions (standard deviation). In all variables, the proportion of missing data was < 5%.
Mann‐Whitney U test.
P values <0.05 were marked as bold.
All infants in the INSURE group received premedication, compared to 12% of the LISA group. Seven infants in the LISA group received premedication with ketamine (0.59 ± 0.34 mg, maximum dose 0.7 mg) and lorazepam (0.05 ± 0 mg, maximum dose 0.05 mg), but exclusion of these seven patients did not change significance levels. In the INSURE group, all 15 infants received premedication (fentanyl 3.96 ± 1.59 µg, maximum dose 6 µg; lorazepam 0.17 ± 0.28 mg, maximum dose 0.21 mg and ketamine 1.7 ± 1.1 mg, maximum dose 3.5 mg).
The need for secondary intubation was similar between the LISA group and the INSURE group (27.1% versus 13.3%, P = .267). Sixteen (21.6%) infants in the LISA group and three (20.0%) in the INSURE group developed bronchopulmonary dysplasia (P = .573). Infants in both groups received similar amounts of standard procedures in the first three days of life (insertion of a peripheral venous line: LISA group and INSURE group (98.3% versus 100%, P = .614); insertion of a percutaneous venous line: LISA group and INSURE group (98.3% versus 93.3%, P = .292); insertion of a peripheral arterial line (LISA group and INSURE group (15.3% versus 13.3%, P = .853).
Preterm infants subjected to LISA procedure showed no significant difference in terms of mortality, the duration of mechanical ventilation and continuous positive airway pressure treatment as compared to infants treated with the INSURE technique (table 3).
Table 3.
Secondary outcome between groups
|
LISA group n = 59 |
INSURE group n = 15 |
P value | |
|---|---|---|---|
| Secondary outcome parameter | |||
| Neonatal mortality; n (%) | 3 (5.1) | 0 (0.0) | .373 a |
| Secondary intubation; n (%) | 16 (27.1) | 2 (13.3) | .267 a |
| Duration of CPAP [days]; median (IQR) | 9 (4;23) | 6 (4;30) | .618 b |
| Duration of mechanical ventilation [hours]; median (IQR) | 45.5 (13.0;88.5) |
23.5 (23.0;‐‐) |
.471 b |
| Bronchopulmonary dysplasia; n (%) | 16 (27.1) | 3 (20.0) | .573 a |
CPAP, continuous positive airway pressure; IQR, interquartile range; SD, standard deviation.
Secondary outcomes of preterm infants treated with surfactant via LISA (Less Invasive Surfactant Administration) procedure or INSURE (Intubation‐surfactant‐extubation) technique. In all variables, the proportion of missing data was < 5%.
Chi‐square test.
Mann‐Whitney U test,
4. DISCUSSION
Neonatal respiratory distress syndrome is one of the most frequent morbidities associated with preterm birth. Multiple concepts have been developed to reduce intubation‐ and mechanical ventilation‐related complications, such as desaturations, tracheal injury, volutrauma, barotrauma and atelectotrauma. 20 Several observational studies and randomized controlled trials have been carried out, showing that surfactant administration via LISA procedure was associated with an improved pulmonary outcome as well as reduced rates of mechanical ventilation and bronchopulmonary dysplasia. 10 , 21 , 22 Despite the observed benefits of this technique to administer surfactant even in extremely immature infants, several aspects of this procedure still are controversially discussed. 23 One of the main questions is whether to use sedative/analgesic medication prior to/during LISA. As reported by Aldana‐Aguiree et al, in most of the trials and reports evaluating LISA premedication (except for atropine and caffeine citrate) was not administered, in order to maintain respiratory drive. 14 , 24 As recently pointed out by Herting et al most centers in Germany perform the first LISA attempt without analgesia. At present, no consensus about whether to sedate routinely for LISA is available and attending neonatologists must decide for themselves, as we did. There is a current lack of a standard operating procedure including adequate pain management for this procedure and practice patterns whether to use drugs vary widely, which might be at least partly, be due to a lack of awareness.. 25 Pain management in preterm infants starting immediately after birth and in the first days of life is important, to avoid subsequent responses to painful procedures 26 and because repeated painful stimuli early in life lead to serious sequelae. 5 , 12 These include abnormal brain development, with lower cognitive scores and altered somatosensory and stress response systems. 11 , 12 The main finding of our study was that the LISA group required significantly more nonpharmacological pain relief in the first three days of life than the INSURE group, which might reflect an ongoing preterm stress response. Repeated pain exposure could limit pain thresholds, make the infant more susceptible to subsequent painful events and might put neonates at risk to develop adverse events and poor development. 5 , 6 It might also strengthen the fact, that every procedure, even when regarded minimally invasive should be supported by nonpharmacological and if necessary pharmacological therapies, to limit painful experiences in preterm infants. To test the assumption, that a minimally invasive procedure like LISA, could have long‐term effects by increasing painful experiences in preterm infants, our study was not designed for and a prospective randomized study is needed in the future.
Even though surfactant is applied during spontaneous respiration, the LISA procedure includes laryngoscopy and intratracheal catheter placement, which is potentially painful. 27 According to a recent European survey, more than a half of neonatologists performed LISA procedure without any sort of pharmacological treatment, but two‐thirds used a Magill forceps to introduce the catheter into the trachea. 28 Premedication is recommended for nonemergency intubations in neonates by the American Academy of Pediatrics, 29 however spontaneous breathing plays a key role in the distribution of surfactant via LISA procedure, hence the reduction of breathing effort through sedatives may create a major disadvantage. 30 In 2019 the European consensus guidelines on the management of respiratory distress syndrome stated that the use of a low‐dose sedation prior to laryngoscopy for LISA is feasible and will make the infant less uncomfortable, but concern has been raised, that sedation will increase the risk of continuous positive airway pressure failure. 31
A major strength was the comprehensive data from a cohort that was highly representative of the general population, as we have the only high‐level neonatal intensive care in our region. Thus, all preterm infants born at ≤ 32 gestational weeks in this region receiving surfactant via LISA procedure or INSURE technique were included in this study. The retrospective design was a limitation and we could not investigate Bernese pain scores during (before and after) LISA/INSURE procedure. This should be evaluated in future prospectively designed studies. Neonatal characteristics were similar for both groups, but birth weight was lower in the LISA group. This reflects a change of practice, by implementing LISA technique into our standard care, even to the smallest infants. There were no other major changes in medical treatment during the study, except for introducing paracetamol for patent ductus arteriosus prophylaxis, which was introduced in October 2014.
With this study, we were able to compare two treatment regimens for surfactant application regarding pain levels in preterm infants. We demonstrated that infants receiving surfactant via LISA had a higher need for nonpharmacological pain‐relieving interventions in the first three days of life. Besides technical aspects, performing a potentially distressing procedure without adequate pain management constitutes an ethical issue. Our results should encourage prospective randomized controlled trials, 32 to examine the severity of respiratory distress and pain, perhaps also including measurements of stress hormone levels and inform strategies for reducing pain for preterm infants undergoing LISA and optimize the use of this less invasive method for surfactant application, to further optimize this less invasive method for surfactant application in neonates. A premedication protocol that does not affect spontaneous breathing should be developed.
CONFLICTS OF INTEREST
The authors have no conflicts of interest to declare. We declare that the research is the original work of the authors. The study was approved by the Ethics Committee of the Medical University of Innsbruck. No.AN213‐0086333/4.2. This study did not receive any specific funding.
AUTHOR CONTRIBUTIONS
All authors (Michaela Höck, Maria Waltner‐Romen, Anna Posod, Ursula Kiechl‐Kohlendorfer, Elke Griesmaier) declare that they participated in the design, execution, and analysis of this paper entitled “Less invasive surfactant administration is associated with a higher need for nonpharmacological pain‐relieving interventions compared to the intubation‐surfactant extubation technique in preterm infants”. All authors drafted the work or revised it critically for important intellectual content. All authors have seen and approved the final version of the manuscript. This work has neither been published nor submitted elsewhere. Dr Hoeck had primary responsiblity for protocol development, patient screening, preliminary data analysis and writing the manuscript. Drs Hoeck, Waltner‐Romen and Kiechl‐Kohlendorfer participated in the development of the protocol and analytical framework for the study and contributed to the writing of the manuscript. Drs Griesmaier, Posod and Kiechl‐Kohlendorfer supervised the design and execution of the study, performed the final data analyses and contributed to the writing of the manuscript.
Höck M, Posod A, Waltner‐Romen M, Kiechl‐Kohlendorfer U, Griesmaier E. Less invasive surfactant administration is associated with a higher need for nonpharmacological pain‐relieving interventions compared to the intubation‐surfactant extubation technique in preterm infants. Paediatr Neonatal Pain. 2021;3:29–35. 10.1002/pne2.12042
REFERENCES
- 1. Anand KJ, Hickey PR. Pain and its effects in the human neonate and fetus. N Engl J Med. 1987;317(21):1321‐1329. [DOI] [PubMed] [Google Scholar]
- 2. Carbajal R, Rousset A, Danan C, et al. Epidemiology and treatment of painful procedures in neonates in intensive care units. JAMA. 2008;300(1):60‐70. [DOI] [PubMed] [Google Scholar]
- 3. Burnett AC, Cheong JLY, Doyle LW. Biological and social influences on the neurodevelopmental outcomes of preterm infants. Clin Perinatol. 2018;45(3):485‐500. [DOI] [PubMed] [Google Scholar]
- 4. Brummelte S, Grunau RE, Chau V, et al. Procedural pain and brain development in premature newborns. Ann Neurol. 2012;71(3):385‐396. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 5. Ranger M, Chau CM, Garg A, et al. Neonatal pain‐related stress predicts cortical thickness at age 7 years in children born very preterm. PLoS One. 2013;8(10):e76702. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 6. Ranger M, Grunau RE. Early repetitive pain in preterm infants in relation to the developing brain. Pain Manag. 2014;4(1):57‐67. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 7. Johnston C, Barrington KJ, Taddio A, Carbajal R, Filion F. Pain in Canadian NICUs: have we improved over the past 12 years? Clin J Pain. 2011;27(3):225‐232. [DOI] [PubMed] [Google Scholar]
- 8. Isayama T, Chai‐Adisaksopha C, McDonald SD. Noninvasive ventilation with vs without early surfactant to prevent chronic lung disease in preterm infants: a systematic review and meta‐analysis. JAMA Pediatr. 2015;169(8):731‐739. [DOI] [PubMed] [Google Scholar]
- 9. Mehler K, Grimme J, Abele J, Huenseler C, Roth B, Kribs A. Outcome of extremely low gestational age newborns after introduction of a revised protocol to assist preterm infants in their transition to extrauterine life. Acta Paediatr. 2012;101(12):1232‐1239. [DOI] [PubMed] [Google Scholar]
- 10. Kribs A, Pillekamp F, Hunseler C, Vierzig A, Roth B. Early administration of surfactant in spontaneous breathing with nCPAP: feasibility and outcome in extremely premature infants (postmenstrual age </=27 weeks). Paediatr Anaesth. 2007;17(4):364‐369. [DOI] [PubMed] [Google Scholar]
- 11. Coviello C, Popple Martinez M, Drovandi L, et al. Painful procedures can affect post‐natal growth and neurodevelopment in preterm infants. Acta Paediatr. 2018;107(5):784‐790. [DOI] [PubMed] [Google Scholar]
- 12. Zwicker JG, Grunau RE, Adams E, et al. Score for neonatal acute physiology‐II and neonatal pain predict corticospinal tract development in premature newborns. Pediatr Neurol. 2013;48(2):123‐9 e1. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 13. Dekker J, Lopriore E, van Zanten HA, Tan R, Hooper SB, Te Pas AB. Sedation during minimal invasive surfactant therapy: a randomised controlled trial. Arch Dis Child Fetal Neonatal Ed. 2019;104(4):F378‐F383. [DOI] [PubMed] [Google Scholar]
- 14. Aldana‐Aguirre JC, Pinto M, Featherstone RM, Kumar M. Less invasive surfactant administration versus intubation for surfactant delivery in preterm infants with respiratory distress syndrome: a systematic review and meta‐analysis. Arch Dis Child Fetal Neonatal Ed. 2017;102(1):F17‐F23. [DOI] [PubMed] [Google Scholar]
- 15. Neubauer V, Griesmaier E, Ralser E, Kiechl‐Kohlendorfer U. The effect of sex on outcome of preterm infants ‐ a population‐based survey. Acta Paediatr. 2012;101(9):906‐911. [DOI] [PubMed] [Google Scholar]
- 16. Hock M, Brunner B, Rier V, et al. Prophylactic low‐dose paracetamol administration associated with lowered rate of patent ductus arteriosus in preterm infants ‐ Impact on outcome and pain perception. Pediatr Neonatol. 2019. [DOI] [PubMed] [Google Scholar]
- 17. The CRIB (clinical risk index for babies) score: a tool for assessing initial neonatal risk and comparing performance of neonatal intensive care units . The International Neonatal Network. Lancet. 1993;342(8865):193‐198. [PubMed] [Google Scholar]
- 18. Cignacco E, Mueller R, Hamers JP, Gessler P. Pain assessment in the neonate using the Bernese pain scale for neonates. Early Hum Dev. 2004;78(2):125‐131. [DOI] [PubMed] [Google Scholar]
- 19. Walter‐Nicolet E, Annequin D, Biran V, Mitanchez D, Tourniaire B. Pain management in newborns: from prevention to treatment. Paediatr Drugs. 2010;12(6):353‐365. [DOI] [PubMed] [Google Scholar]
- 20. Polin RA, Carlo WA, Committee on fetus and Newborn . American Academy of P. Surfactant replacement therapy for preterm and term neonates with respiratory distress. Pediatrics. 2014;133(1):156‐163. [DOI] [PubMed] [Google Scholar]
- 21. Kribs A, Vierzig A, Hunseler C, et al. Early surfactant in spontaneously breathing with nCPAP in ELBW infants–a single centre four year experience. Acta Paediatr. 2008;97(3):293‐298. [DOI] [PubMed] [Google Scholar]
- 22. Gopel W, Kribs A, Ziegler A, et al. Avoidance of mechanical ventilation by surfactant treatment of spontaneously breathing preterm infants (AMV): an open‐label, randomised, controlled trial. Lancet. 2011;378(9803):1627‐1634. [DOI] [PubMed] [Google Scholar]
- 23. Rigo V, Lefebvre C, Broux I. Surfactant instillation in spontaneously breathing preterm infants: a systematic review and meta‐analysis. Eur J Pediatr. 2016;175(12):1933‐1942. [DOI] [PubMed] [Google Scholar]
- 24. Kanmaz HG, Erdeve O, Canpolat FE, Mutlu B, Dilmen U. Surfactant administration via thin catheter during spontaneous breathing: randomized controlled trial. Pediatrics. 2013;131(2):e502‐e509. [DOI] [PubMed] [Google Scholar]
- 25. Herting E, Hartel C, Gopel W. Less invasive surfactant administration (LISA): chances and limitations. Arch Dis Child Fetal Neonatal Ed. 2019;104(6):F655‐F659. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 26. Grunau R. Early pain in preterm infants. A model of long‐term effects. Clin Perinatol. 2002;29(3):373‐394, vii‐viii. [DOI] [PubMed] [Google Scholar]
- 27. Ancora G, Lago P, Garetti E, et al. Evidence‐based clinical guidelines on analgesia and sedation in newborn infants undergoing assisted ventilation and endotracheal intubation. Acta Paediatr. 2019;108(2):208‐217. [DOI] [PubMed] [Google Scholar]
- 28. Klotz D, Porcaro U, Fleck T, Fuchs H. European perspective on less invasive surfactant administration‐a survey. Eur J Pediatr. 2017;176(2):147‐154. [DOI] [PubMed] [Google Scholar]
- 29. Kumar P, Denson SE, Mancuso TJ. Committee on F, Newborn SoA, Pain M. Premedication for nonemergency endotracheal intubation in the neonate. Pediatrics. 2010;125(3):608‐615. [DOI] [PubMed] [Google Scholar]
- 30. Bourgoin L, Caeymaex L, Decobert F, Jung C, Danan C, Durrmeyer X. Administering atropine and ketamine before less invasive surfactant administration resulted in low pain scores in a prospective study of premature neonates. Acta Paediatr. 2018;107(7):1184‐1190. [DOI] [PubMed] [Google Scholar]
- 31. Sweet DG, Carnielli V, Greisen G, et al. European consensus guidelines on the management of respiratory distress syndrome ‐ 2019 update. Neonatology. 2019;115(4):432‐450. [DOI] [PMC free article] [PubMed] [Google Scholar]
- 32. Chevallier M, Durrmeyer X, Ego A, Debillon T, Group PS . Propofol versus placebo (with rescue with ketamine) before less invasive surfactant administration: study protocol for a multicenter, double‐blind, placebo controlled trial (PROLISA). BMC Pediatr. 2020;20(1):199. [DOI] [PMC free article] [PubMed] [Google Scholar]


